Академический Документы
Профессиональный Документы
Культура Документы
Chemotherapy and Diagnostic Toxicology
Загружено:
SunilАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Chemotherapy and Diagnostic Toxicology
Загружено:
SunilАвторское право:
Доступные форматы
RATIONAL ANTIMICROBIAL THERAPY IN DOMESTIC
ANIMALS
A.G.REDDY
The choice of antimicrobial agent in the clinical practice should be based upon
susceptibility of the infecting organism to the drug concentrations achieved in the tissue
and pharmacokinetic characteristics of the drug and its dosing protocol. Although,
several class of antimicrobials are readily available, the clinical cure may not be always
successful and its partially attributable to lack of culture and sensitivity tests under field
conditions. Therefore, atleast, one can bank upon certain pharmacokinetic principles in
the routine clinical practice as well as in serious infections like meningitis, endocarditis
and in immuno-compromised hosts.
Pharmacokinetics:
Pharmacokinetics deals with absorption, distribution, metabolism and excretory pattern
of a given therapeutic agent. Selection of antimicrobial agent based on its
pharmacokinetic characteristics aid in achieving optimal concentration at the desired
site. For example, the location of infection can have a major influence on the drug
concentration achieved there, as some sites (eg: CNS) are protected by barriers to drug
penetration, while others (eg. mammary gland, urinary tract) local pH may favour drug
accumulation. Knowledge of pharmacokinetic data is also useful to avoid possible
toxicity in a given species as well to take necessary precautions during physiological
stress (eg. pregnancy, lactation) or pathological conditions (eg: hepatic failure, renal
dysfunction). The probable antimicrobial agent that can be employed in the clinical
practice should be selected after giving due considerations to following issues:
i.organ/s is/are involved ii.Most likely pathogen iii. Antibiotic likely to be effective
iv. Drug concentrations at the site of infection v. Drug/route likely to achieve that
concentration
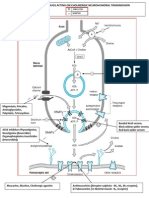
Absorption: The absorption and disposition of antimicrobial agents in the body
arelargely governed by their chemistry and certain physiochemical properties as well as
status of the animal (Fig.1). The various antimicrobials are basically grouped into
weak organic electrolytes (acids/bases), amphoteric or neutral compounds. The
absorption is primarily dependent on extent of lipid solubility and degree of ionization,
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
which are determined by pKa of the drug and pH of the biological fluid in question.
These factors also determine the extent of distribution and elimination process for
antimicrobials. Only non-ionized forms of drugs are passively diffuses across GIT or
can pass across blood-brain or blood-milk barrier. For acidic drugs, a fall in 1 pH unit
results in a 10 fold increase in the concentration of the non-ionized form and converse
applies for organic bases.
Distribution and elimination: Some of the lipophilic antimicrobials listed below
enter most tissues of the body and penetrate cellular barriers and can generally reach
infection foci. Chloramphenicol,Trimethoprim,Erythromycin,Metronidazole,3rd
generation cephalosporins like moxalactam,Fluoroquinolones:Enrofloxacin, Pefloxacin,
Ofloxacin, Norfloxacin.These antimicrobials are eliminated mainly by hepatic
metabolism and/or carrier mediated biliary exertion. This rate of elimination varies
with species, but obeys first order kinetics when therapeutic doses are administered.
Tetracyclins: The lipid solubility of tetracyclins varies with the compound but enter
most tissues and body fluids except CSF. The more lipophilic number, minocycline
attain effective concentration at relatively inaccessible infection site, such as the
prostate. As a result of chelation with calcium, tetracyclins become bound at active
sites of ossification and in developing teeth. Long acting tetracyclins (doxycyline,
minocycline) undergo biliary excretion and may adversely affect indigenous microbes
in the caecum/colon of horses. However, they are suited for biliary and upper intestinal
tract infection in farm animals. Oxytretracyclin in 2-PVP base (IM only) exert long
duration of action over propylene glycol base. Because of poor water solubility,
oxytetracyclin dihydrade must be given in much higher dose (50 mg/kg) than the
hydrochloride salt to produce equivalent tissue concentration.
Sulfonamides: Most of the sulfonamides predominantly non-ionized in biological fluid
of pH below their pKa value (sulfisoxzole = 5; sulfonilamide = 10.4). Commonly used
compounds like sulfamethazine (pka = 7.4) and sulfadimethoxin (pKa = 6.1) enter most
tissues of the body and eliminated by a combination of metabolic reactions
(acetylation) and renal exertion (filteration and pH - dependent passive tubular
reabsorption). Cats are poor acetylators and therefore sulfonamides are contraindicated.
Sulfisoxazole (pKa = 5.0) is more ionized in the plasma and widely distributed and
eliminated mainly by glomerular filtration (best suited for UTI), but their exerction is
dependent on urinary pH.
Penicillins: Distributions of penicillin are limited due to high ionization and they
attain low concentration in cells and do not penetrate well into transcellular fluids.
Protein binding varies among penicillin over a wide range (80%-cloxacillin, 22%-
ampicillin) and this is responsible for low extra-vascular distribution. However,
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
penicillin and/or in combination with streptomycin is best suited for lower respiratory
tract infection (unknown pathogen) with exudation. Penicillins are rapidly eliminated
by kidney. Probencid compete with their excretion (for tubular excretion) and delays
penicillins excretion.
Antibiotic Desired environment for optimal action
Penicillins,Hexamine(only UTI) Acidic pH
Nitrofurazones,Cephalosporins
Tetracyclins,Fluoroquinalones,Aminoglycosi Alkaline pH
des
Ampicillin, amoxicillin and naficillin undergoes enterohepatic circulation and
therefore their half-lives are longer than penicillin-G. Penicillins and cephalosporins
(beta-lactams) are highly active during logarithmic phase of bacterial growth (time
dependent action). Dosing of beta-lactams should be aimed to keep serum
concentration over MIC to prevent regrowth. Penicillins retains their activity even in
the presence of fibrin and abscess formation.
Antibiotic Factors decrease their action
Sulfonamides Pus, blood clot
Penicillin,Cephalosporins,Aminoglycosides Intracellular organisms
Gentamicin,Polymyxin Pus
Aminoglycosides DecreasedpH,anaerobiasis, hyperosmalarity
Aminoglycosides :
Aminoglycosides does not attain therapeutic levels in CSF and ocular fluid. Poor
diffusibility is attributed to this low degree of lipid solubility. Hafl-lives are short (1-2
hr) in domestic animals. Inspite of limited distribution, selective binding to renal tissue
(cortex) occurs. Their bacteriocidal action is rapid but killing of Gm-ve aerobes is
concentration dependent and produce a prolonged post-antibiotic effect. Due to this
biphasic mode of action, serum concentration continuously exceeding MIC are not
required unlike penicillins. Loop diuretics and impaired renal function delays their
renal excretion and it is necessary to adjust maintenance dosage to prevent ototoxicity
and nephrotoxicity. One should not administer large IV dose or multiple injections in
dehydration or ureamic conditions. Intravenous eg: neomycin) must be restricted to
one or two occasions only. Systemic administration does not give satisfactory levels in
milk and therefore local (intramammary) route should be employed in mastitis cows.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Chloramphenicol: In pre-ruminant calves, chloromphenicol is well absorbed from
GIT following systemic administration. The drug readily pass through cellular barriers
and attain sustained concentration in CSF and aqueous humor. The drug can readily
cross placenta. Penetration of the blood: prostate barrier is relatively poor. Due to
lipophilic nature, the apparent volume of distribution is large (> 1L/kg) in all species
and its distribution is independent of pH. It possess short half-lives in most species
except cat (poor in conjugation with glucoronic acid). Due to short of half-life
chloromphenicol (sodium succinate) at the rate of 50 mg/kg (priming dose) followed by
maintenance doses of 25 mg/kg at 8-12 interval is suggested in ruminants.
Fluoroquinolones:
These are amphoteric compounds and having low degree of ionization. Therefore, their
distribution is widespread and even penetrate well into CSF (>50% serum levels in
meningitis), bronchial secretions, bone and cartilage and prostatic tissue. Partially
metabolised in liver and bile concentrations are 2-10 times the serum levels and even
enterohepatic circulation may occur. Plasma half-lives varies with species and urinary
concentration exceed serum concentration by several hundred times and remain high
for 24 hr after administration. Clearance of certain drugs like theophylline get reduced
leading to adverse effects and one should not administer concurrently. They have
affinity for weight bearing cartilages and therefore do not administer to puppies (before
8 months of age) or foals (below 1 year of age). Reduction of dosage is required in
animals with impaired renal function.
Antimicrobial combinations and their effect
Bacteriostatic (systemic) + bacteriocidal (systemic) Antagonistic
Bacteriostatic (local) + bacteriocidal (systemic) Antagonistic
Bacteriocidal (local) + bacteriostatic (systemic) Antagonistic
Chloramphenicol + Aminoglycosides Antagonistic
Macrolid + Chloramphenicol Antagonistic
Conclusion:
The antimicrobial chemotherapy particularly in the absence of antibiotic sensitivity
testing facility under field conditions is a difficult task. In the routine clinical practice
as well as in the absence of microbial sensitivity pattern, one can adopt certain
pharmacological principles discussed here so as to obtain clinical and/or bacterological
cure. The veterinarian must update their knowledge pertaing toclinical pharmacology
of newer antimicrobials released in to market.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
*****
CLINICAL ASPECT OF ANTIMICROBIAL THERAPY IN
RUMINANTS
N.A.PATIL
Drug passage through the ruminant gastrointestinal tract is much different than
that of mono-gastric animals. The drug residence time in rumino-reticulum, that greatly
alters drug blood level profiles as compared to those observed in monogastric. A drug
reaches, the intestine at a rate primarily determined by the rate of rumen emptying. The
drug is then absorbed and enters the general circulation or passes out the faces.
Although the rumen is lined with stratified squamous epithelium, the
nonionized form of weak organic acids and passes passively diffuses through the
mucosa and intraruminal drug administration provides low blood levels and greatly
extended duration when compared to monogastric animals. This is caused by slow rate
of rumen emptying. In ruminants long times (3-5 days) are needed to achieve steady-
state blood levels during multiple oral dosing. But in some cases, extended duration of
activity caused by slow rumen emptying is advantageous for prolonging blood levels.
This principle contributes greatly to the long-lasting properties of many sulfa drugs in
ruminants. Chronic oral dosage with a broad spectrum antimicrobial agent can suppress
activity of ruminal microflora, there by interferes with carbohydrate digestion. The
ruminal microflora also can activate drugs by hydrolytic or reductive reactions
(Trimethoprim).
Sick animals may demonstrate decreased rumen activity. This inturn will result
in a greatly increased rumen mean residence time, which will result in even longer
duration and lower peak blood levels. For example, lower will be peak sulfamethazine
blood levels in diseased cattle compared to normal animals. Decreased rumen motility
of a sick or starved animal may result in subtherapeutic blood levels, even while
therapeutic levels are obtained with the same dose in normal animals. On the other
hand, increasing the dose sufficiently to sick animals can result in therapeutic blood
levels for a much longer duration than that observed in normal animals. In this case
depressed rumen motility enhances therapy.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Antimicrobial therapy: Stability towards chemical and metabolic inactivation within
the reticulo-rumen and abomasum of ruminant species determines the amount of oral
dose which is potentially available for absorption.
Erythromycin is a valuable antibiotic for use against a variety of gram positive bacterial
pathogens. Recent reports indicate that high proportions of pasturella haemolytica
isolates are sensitive to erythromycin in vitro. IM route of administration is the only
acceptable route in cattle at the dose rate of 15 mg / kg body weight. Apart from the
adverse effects like diarrhea there is little reason to use erythromycin orally in
ruminants because of negligible drug absorption. Uses of erythromycin in preruminant
calves require higher dosage due to the limitations in absorption. Serious adverse
gastrointestinal effects associated with the oral administration may occure with
parentral administration since a high proportion of erythromycin apparently is
eliminated by biliary secretion.
Tetracyclines will interfere with bacterial flora in the rumen, so they should not
be given to ruminants. The use of intramuscular and intraabdominal sodium ampicillin
is suitable during abdominal surgery in calves. Ampicillin will appear in milk and urine
for at least 48 hours post administration. Trimethoprim will be metabolized by the
microflora in the gastrointestinal tract of ruminants within 48 minutes; thus oral dosing
is not effective.
Chloramphenicol in ruminants will be inactivated by a reductive reaction in the
rumen. Since the rumen takes 8-12 weeks to develop and become functional, the
bioavailable profile of drugs administered orally to neonatal valves is similar to that
obtained in monogastric species. So the chloramphenicol administered as oral solution
is well absorbed in neonatal calves and oral dosage (26 mg /kg at 12 hour intervals)
will maintain therepeutical effective plasma concentrations. The half life of
chloramphenicol which is 14 hours in one day old calf, decrease to 4.2 hours in 10-12
weeks old calves. This decrease is caused partly by increasing drug “trapping” in the
developing rumen and partly by development of metabolic capacity. Similar changes
noticed in the case of Trimethoprim therapy of goats.
However Furaltadone @10 mg/kg body weight twice daily orally is found to be
effective for simple indigestion, ruminal simple impaction, acid indigestion and
enteritis. Long acting parenteral preparations are most convenient dosage form in farm
animals. A single dose of (25,000 units/kg body weight) of procaine penicillin-G (in
buffered aqueous suspension) injected either intramuscularly or subcutaneously can
maintain effective levels of penicillin-G for 24 hours although the half life of penicillin-
Gis less than an hour.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Passage of antimicrobial agents into milk: In milk weak acids (Benzyl penicillin,
ampicillin, cephalosporin, sulfamethazine and cloxacillin) produces ratios of milk ultra-
filtrate concentration to plasma ultrafiltrate concentration that are less than or equal to
unity and organic bases (Erythromycin, Tylocin, Lincomycin, Trimethoprim) excluding
aminoglycoside antibiotics (which are) polar attain concentration ratios greater than
one.
*****
ANTIMICROBIAL THERAPY OF PROTOZOAL AND
RICKETTSIAL INFECTIONS
B.G. RAVINDRA
Protozoan and Rickettsial diseases are responsible for considerable mortality
and morbidity in animals leading to devastating losses. Protozoan parasites are
unicellular, eukaryotic organisms present in blood cells, tissues, skin and intestines.
The Rickettsial organisms are minute, lack cytoplasm and are present in blood cells.
Attempts to develop vaccines aginst these have been greatly handicapped due to
complexity of different parasitic stages and their life cycle. Few vaccines are available
against these diseases. Drugs currently available are effective, if they are used
specifically with proper dose, route and course of treatment. Integrated method of
control is very important by using vaccines, drugs and other managemental practices.
PROTOZOAL DISEASES
BABESIOSIS (PIROPLASMOSIS, RED WATER FEVER): The viable protozoa
are present in blood stream of animals only in active stages of infection. Ticks
(Boophilus spp.) are natural vectors in which transovarial transmission
occurs.Contaminated needles and surgical instruments can physically transmit the
infection.
Clinicla signs: acute syndrome- high fever (up to 106oF), anorexia, depression,
weakness, suspension of rumination, decrease in milk yield, increased heart and
respiration rates. Conjuctiva brick red but soon changes to extreme pale due to severe
anaemia. In terminal stages, severe jaundice, urine dark red/ brownish and produces
stable froath. Many severely affected animals die after 24 hours and which survive
febrile reaction last for week; pregnant animals often abort, course of disease is 3
weeks. In subacute infection- mild fever, hemoglobinuria absent
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
.B. bigemina- cerebral babesiosis- incoordination, posterior paralysis, mania,
convulsions and coma. High mortality inspite of treatment in cerebral form.
B. divergens- additional sign is spasm of anal sphincter and feces expelled with greater
force in long thin stream referred to as “pipe-stem feces”.
Dogs: Signs vary from mild fever lasting for several days to sudden high fever, marked
anemia, hemoglobinuria and jaundice.There may be cerebral form (hyperexcitability),
alimentary form (stomatitis, gastritis, enteritis), respiratory form (dyspnea), circulatory
form (edema), ocular form (keratitis, iritis) and muscular form (muscular weakness).
Therapy: a) Quinoronium sulphate derivatives- Acaprin (@ 1ml/50 Kg BW s/c,
maximum dose 6ml otherwise salivation, panting, diarrhoea), Babesan, Piroparv,
Piroplasmin. b) Acridine derivatives- Acriflavin (50-100ml i/v as 1% solution),
Gonacrine, Trypan blue, Euflavine c) Aromatic diamidines- Diminazine aceturate
(Berenil- 0.8-1.6 gm/100 Kg BW deep i/m), Stilbamidine, Propamidine, Phenamidine.
d) Imidocarbs- Imizole @ 1mg/Kg BW s/c. (Imidocarb hydrochloride and Imidocarb
dipropionate)
In horses- Berenil @ 11mg/Kg BW deep i/m.; Imidocarb- most favoured drug. B.equi-
@ 4mg/Kg BW four IM injections of 10% solution at 72 hour interval. B.caballi- @
2mg/Kg BW two injections at 24 hour interval. In donkeys- maximum @ 2mg/Kg
BW.; Buparvaquone @ 4-6mg/Kg BW to control B.equi infection.In sheep- Berenil @
3.5mg/Kg BW on two successive days or 12mg/Kg single dose. Supportive treatment-
blood transfusion, Vitamin B complex.
THEILIEROISIS: Theileria parva, T. annulata- tropical theileriosis, T. mutans- less
pathogenic, T. ovis, T. hirci- sheep and goat.T. camelensis- camel. Mainly transmitted
by Hyalomma spp ticks; the organism pass trans-stadially through stages of larva,
nymph and adult. No transovarian transmission.
Clinical signs: Initial sign- enlargement of superficial lymph nodes (prescapular,
prefemoral, parotid) within 7-10 days of tick attachment. After 1-2 days, fever (105-
106oF), depression, anorexia and decrease in milk yield. In later stages- nasal and
ocular discharges, dyspnea, generalized lymph node enlargement and splenomegaly. In
severe cases- emaciation, weakness and recumbency followed by death due to
asphyxia. Ocassional cerebral theileriosis- circling, tremors, convulsions, profuse
salivation and head pressing. T. annulata infection- additional signs of anemia and
jaundice.
Treatment: a) Halofuginone lactate- coccidiostat but also has schizonticidal effect @
1.2-2.0 mg/Kg orally for two days. Higher doses may be toxic- salivation, diarrhea,
conjunctivitis, subnormal temperature and even death. b) Parvaquone @ 10 mg/Kg,
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
may be repeated after 48 hours. c) Buparvaquone (Butalex) @ 2.5 mg/Kg i/m, may be
repeated after 48 hours. d) Tetracyclines, Nivaquine act only on the piroplasm stages.
e) Supportive treatment- blood transfusion, liver tonics, diuretics (to check pulmonary
edema).
TRYPANOSOMIASIS (SURRA): Trypanosoma evansi- highly pathogenic, produce
surra/ murrina/ mal de caders affect cattle, buffalo, sheep, goat, horse, camel and dogs.
Horses and dogs most commonly affected, camel are carriers (chronic disease- Tibersa
in camels- 3 year sickness). Transmission is through biting flies- Tabanus, Stomoxys,
Lyperosia, Glossina, Hematopota even vampire bats help in transmission from one
animal to other.Dogs may contract disease by eating infected meat (after 20 days of
eating placenta of affected cattle).
Clinical signs: i) Peracute form- sudden death within 2-3 hours, animal dies showing
some convulsions. Ii) Acute- Intermittant fever (103-105oF), animal dull and
depressed, eyes are starring and wide open, breathing hard and noisy, staggering gait,
circling movements, cattle stretches the rope to which it is tied, animal strikes head
against wall or manger, stamping of feet, apparent blindness, frequent micturition,
profuse salivation, muscular twitching followed by stage of comma and death within 6-
12 hours. iii) Subacute/chronic- dullness, lacrimation, animal show progressive
emaciation, rapid pulse, intermittent fever, edema of legs, wasting of muscles, loss of
weight, occasionally diarrhea, some animal remain standing with neck extended even
throughout the day. Dogs: may be acute form of disease, intermittent fever, anemia,
edema and corneal opacity.
Camel: in chronic form and may last for 3 years, first sign is weakness of all quarters,
eyes dull, alopecia, mucus membranes pale and show petechial hemorrhages, edema of
legs, abortion common, mange is frequently seen in surra affected cases.
Treatment: a) Quinapyramine sulphate (Antrycide) curative @ 5mg/Kg BW;
Quinapyramine sulphate and chloride (Antrycide prosalt); prophylactic @7.4 mg/Kg
BW. In horses- give injection at 2-3 sites, in weak animals there may be salivation,
restlessness and muscular tremors. b) Suramin @ 10mg/Kg BW i/v as 10% solution in
horses and camels. c) Diminazine aceturate- against T.vivax and T.congolense @ 3.5-
7.0 mg/Kg, toxic to horses and camels. d) Homidium- bromide and chloride salts @
1mg/Kg BW. e) Isometamidium @ 0.25-1.0mg/Kg BW. f) Pyrithidium bromide @
2mg/Kg BW.
COCCIDIOSIS: Eimeria bovis and Eimeria zurnii are the common species,
transmited by Feco-Oral route .Sub-clinical coccidiosis occur in 95% of the cases of
ruminants. The other 5% are clinical cases.Anorexia, Diarrhoea (may or may not
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
contain blood), dehydration, weakness, depression, weight loss, cachexia, Anaemia and
death, Nervous coccidiosis-muscle tremors, staggering, convulsions and occasionally
blind nes.
Amprolium @ 10 mg/Kg BW for five days, 1.25% crumble, 9.6%solution, 20%
soluable powder ; Sulphaquinoxaline @ 8-70 mg/ kg BW for five days, as soluable
powder or feed alternative; Monensin @ 1 mg/ kg daily for 30 days, as feed additive is
effective.
GIARDIOSIS: It is a chronic protozoal disease, common in dogs caused by Giardia
canis and characterized by diarrhea, dysentery and abdominal pain. Treatment is with:
Chloroquin or Metronidazole 250 mg/kg for 10 days are effective.
BALANTIDIOSIS: Balantidium coli exist as a commensal in the large intestine of
pigs. Infection of cattle occurs by ingestion of the cysts. The organisms cause
ulceration of the mucosa and diarrhea. Diagnosis is based on the detection of
cysts/trophozoites in the faeces. Tetracyclines and Metronidazole are effective.
TOXOPLASMOSIS: It is contagious disease of all species including man and is
manifested by abortions and stillbirths in ewes and in all species characterized by
encephalitis, pneumonia and neonatal mortality.
Clinical signs: cattle: in acute form marked by fever, dyspnoea, ataxia,
hyperexcitability in early stages followed by extreme lethargy, stillborn or weak calves
die soon after birth. The parasite plays no significant role in bovine abortion.
Congenitally affected calves show fever, dyspnoea, sneezing, coughing, nasal
discharge, clonic convulsions and grinding of teeth. The death may occur after 2-6
days.; Pigs: highly susceptible, all ages affected. Adults show debility, weakness,
incoordination, coughing, tremors and diarrhea but no fever. In young pigs, high fever,
diarrhoea, dyspnoea, coughing and ataxia. The pregnant sows abort and piglets are
premature or stillborn; Sheep: abortion at last 4 week of gestation and neonatal death.
is fever, dyspnoea and generalized tremors whereas lambs show fever and dyspnoea.
Goats: abortion and stillbirths; Horses- mainly nervous signs including ataxia, circling
movement, paresis, myeloencephalitis that may be positive factor for Wobbler
syndrome.
Treatment: a) A combination of sulpha drugs @200 mg/Kg BW i/v for 3-5 days
(sulphadiazine, sulphadimidine, sulphamerazine, sulphapyrazine) and pyrimethamine
@ 1-2 mg/Kg BW orally is quite effective b) Sulfomoyl diamino diphenyl sulphon
(SDDS) tried in pigs only @ 5 mg/Kg BW, not used clinically.c) Linomycin and
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Clindamycin are reported to be quite effective. D) Treatment of anemia as there is
blood loss.
BOVINE TRICHOMINIASIS: It is a non-febrile protozoal disease of cattle leading
to irregular estrus intervals, early fetal deaths and cases of pyometra.Trichomonas
(Tritrichomonas) fetus, the etiological agent. Clinical signs: The parasite normally
persists for 3 months in female genital tract after infection and a mild vaginitis is seen
after the infective coitusThere is death of fetus within 2-4 months of conception leading
to cases of repeat breeding and infertility.Abortions are usually not detected and main
feature is failure of animals to hold to service.In bulls, infection is confined to penile
and prepucial surface and cause mild inflammatory response.
Treatment: a) The majority of infected cows recover and clear the infection within 3
months so not normally treated. In bulls- douches of prepuce and penis with acriflavin.
Dimetridazole @ 50 mg/Kg/day orally for five days is quite affective. Ipronidazole can
be administered IM but priorl, bulls should be treated with broad spectrum antibiotic to
reduce preputial commensal bacteria which might inactivate the ipronidazole.
RICKETTSIAL DISEASES
ANAPLASMOSIS (GALL SICKNESS) : A non-contagious disease of ruminants
caused by obligate intraerythrocytic parasites: Anaplasma marginale, A. centrale, A.
ovis. Mainly transmitted by ticks: Boophilus spp., Dermacentor spp, tabanid flies;
infected hypodermic needles, blood transfusions
Clinical signs: Subacute (in younger ones): Temperature rises slowly up to 105oF-
remain elevated or fluctuate, partial anorexia, animal may die at this stage or survive in
an emaciated condition- mucous membranes become pale, urine may be brown but no
haemoglobinuria. Peracute cases: sudden onset of high fever, anemia, jaundice, severe
dyspnea and death within 24 hours; animals become hyperexcited and may attack
pregnant animals may abort. Recovered bulls- testicular function depressed for several
months. Sheep and Goat- usually subclinical infection but sometime severe anaemia in
goats.
Treatment: a) Oxytetracycline @ 6-10 mg/Kg BW for three days or single injection
of long acting oxytetracycline @ 20 mg/Kg BW i/m. b) Imidocarb @ 3 mg/Kg BW
s/c. The problem of carriers can be avoided by using tetracycline @ 10-30 mg/Kg BW
i/m daily for 10-15 days or 22 mg/Kg BW i/v daily for 5 days or long acting
tetracycline @ 20 mg/Kg BW i/m weekly for 2-4 times or two injections of imidocarb
@ 5 mg/Kg BW i/m or s/c. The oral use of chlortetracycline @ 11 mg/Kg BW for 30-
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
60 days or 1.1 mg/Kg BW for 120 days also eliminates carrier animals. c) Supportive
treatment- blood transfusion if PCV less than 15%.
EHRLICHIOSIS: Ehrlichia canis, Ehrlichia bovis are the etiological agents,
commonly transmitted by ticks: Rhipicephalus sanguineus. Clinical signs: Anorexia,
fever, incordination and enlargement of lymphnodes. The disease is of low significance
in indigenous cattle, however it is serious problem in imported and newly introduced
cattle. In dogs: Anorexia, fever, respiratory distress, Limb oedema, enlargement of
lymphnodes, bleeding tendacy (epistaxis, hematuria), and petichial haemorrhages on
mucus membrane, Progressive weight loss and Neurological disorder may be seen.
Treatment: Doxcycline @ 5-10 mg/Kg BW per oral for about 10-14 days for four
days ; Oxytetracycline @ 5-10 mg/Kg BW for four days ; Chloromphenicol, @ 5
mg/Kg BW for four days, Enrofloxacin @ 2.5-5 mg/Kg BW for four days may also be
effective
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
ANTIMICROBIAL THERAPY OF IMPORTANT DISEASES
OF ZOONOTIC IMPORTANCE
PRADEEPKUMAR
The antimicrobial therapy of important diseases of zoonotic importance are
discussed in brief in this article.
ANTHRAX:Penicillin, the drug of choice for years other drugs from penicillin family
such as amoxicillin should be equally effective. Doxycycline, one of the tetracyclines,
most recently listed as the drug of choice in treating anthrax. Ciprofloxacin, one of the
quinolone antibiotics and is also effective. is recommended as the first drug to use until
the sensitivities of the organisms are known Lung infections may be treated with IV
antibiotics.If untreated, cutaneous anthrax may result in death. Untreated inhalation
anthrax always results in death.
BRUCELLOSIS: Use of surgical hand gloves is recommended during vaccination and
yhe vaccine should be handled properly. Vials, syringes, needles and gloves used
during vaccination should be discarded by suitably disinfecting them.Streptomycin is
the drug of choice. Doxycycline (per oral dosage) is also effective. Flouroquinolones
can also be used.
TUBERCULOSIS:Tuberculosis is curable only with a combination of chemotherapy,
in which a medley of three or four anti-tubercular drugs is administered. The first line
drugs are Isoniazid, Rifampicin, Ethambutal, Pyrizinamite, and Streptomycin. The
treatment is streamlined over a period of 6-9 months.Azithromycin, clarithromycin,
ciprofloxacin are the second line agents, used in cases of resistance and toxicity tio first
line drugs.
TOXOPLASMOSIS:From acute maternal infection during pregnancy;
incidence/severity related to trimester of infection; may cause abortion, stillbirth, and
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
premature birth. Manifestations varied: if not evident at birth, usually develop in later
life (85%) and may include: microcephaly, hydrocephaly, neurologic disease/mental
retardation, ocular disease, pneumonitis, hepatomegaly, splenomegaly, icterus, anemia,
thrombocytopenia. Clindamycin; sulfa trimethoprim; monitor for evidence of bone
marrow suppression. Do not feed raw or undercooked meat to cats, keep cats inside and
do not let them hunt.
PLAGUE (BUBONIC, PNEUMONIC, SEPTICEMIC) : The etiological agent
is: Yersinia pestis (gram-negative coccobacillus); Rodents (dog, ground squirrel, rock
squirrel) are the major reservoirs. Bubonic form (most common; 80 - 90% of cases):
enlarged, painful lymph nodes (axillary, cervical, inguinal), fever, chills, weakness, GI
signs, headache, myalgia. Septicemic: septic shock, meningitis,
coma, .Pneumonic (least common: severe pneumonia, fever, dyspnea, and hemoptysis).
Aminoglycosides, fluoroquinolones, are effective agents with supportive care.Insect
repellent, appropriate clothing, flea control for pets and environment, rodent control.
Avoid contact of cats with reservoir hosts.
RINGWORM: Patchy pruritic dermatitis that may be multifocal. Many possible
etiologies in people (zoophilic, geophilic, anthrophilic dermatophytes); M. canis most
common zoophilic dermatophyte and infections are from cats. Keeping the affected
part of the body dry and clean and antifungal agents like griseofulvin, terbinafine,
miconazole, ketoconazole are used.
CRYPTOSPORIDIOSIS : Cattle, rodents, dogs, cats, birds, raccoons are the
reservoirs. Immunocompetent ones: Self-limited acute watery diarrhea, epigastric pain,
nausea, anorexia requiring fluid therapy. Immunocompromised: chronic profuse watery
diarrhea, fever, epigastric pain, nausea, anorexia. Gall bladder infection possible.
Respiratory tract infection may occur. Azithromycin may be effective. Evaluate for
concurrent immunosuppressive conditions if prolonged treatment needed. Clean and
disinfect environment (100% ethanol or 50% bleach with 30 minutes of contact
effective after removal of organic matter)
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Q-FEVER : Coxiella burnetii is the etiological agent. Cattle, sheep, and goats are the
primary reservoirs. Inhalation of organisms from air that contains airborne barnyard
dust contaminated by dried placental material, birth fluids, and excreta of infected herd
animals. Outbreaks occur mainly from occupational exposure involving veterinarians,
meat processing plant workers, sheep and dairy workers, livestock farmers, and
researchers at facilities housing sheep.
Acute: high fever (up to 104-105° F), severe headache, general malaise, malign,
confusion, sore throat, chills, sweats, non-productive cough, nausea, vomiting, diarrhea,
abdominal pain, hepatitis and chest pain. 1-2% mortality in humans. Chronic:
Endocarditis, generally involving the aortic heart valves, less ommonly the mitral
valve. Patients who recover can develop lifelong immunity. Incubation period: 2-3
weeks. Doxycycline is the treatment of choice for acute Q fever. Antibiotic treatment is
most effective when initiated within the first 3 days of illness. A dose of 100 mg of
doxycycline taken orally twice daily for 15-21 days is a frequently prescribed therapy.
Quinolone antibiotics have demonstrated good in vitro activity against C. burnetii and
may be considered.
INFLUENZA : Two antiviral agents: zanamivir (TN: Relenza) and oseltamivir (TN:
Tamiflu) are used to prevent or reduce influenza A and B symptoms. These should not
be used indiscriminately, because viral resistance to them can and has occurred. Also,
they are not recommended if the flu symptoms already have been present for 48 hours
or more. Severe infections in some patients may require additional supportive measures
such as ventilation support and treatment of other infections like pneumonia that can
occur in patients with a severe flu infection.
General precautions to prevent zoonotic infections:
Hand hygiene: Consistent thorough hand hand washing with plain (nonantimicrobial)
soap and running water mechanically removes organic material and reduces the number
of transient organisms on the skin, whereas antimicrobial soap kills or inhibits growth
of transient and resident flora.To reduce the opportunity for cross-contamination, liquid
or foam soap products should be selected rather than bar soaps. Hands should be
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
washed between animal contacts and after contact with feces, blood, body fluids, and
exudates. Alcohol-based hand rubs are highly effective against bacteria and enveloped
viruses and may be used if hands are not visibly soiled.
Use of gloves and sleeves: reduce the risk of pathogen transmission by providing
barrier protection; though, wearing gloves is not a substitute for hand washing. Gloves
are available in a variety of materials. Choice of gloves depends on their intended use.
If allergic reactions to latex are a concern, acceptable alternatives include nitrile or
vinyl gloves.
Facial protection: prevents exposure of mucous membranes of eyes, nose, and mouth
to infectious materials. Whenever exposures to splashes or sprays are likely to occur,
such as those generated during lancing of abscesses, flushing wounds, dentistry,
suctioning, lavage, and necropsy, facial protection- surgical mask worn with goggles or
a face shield is used..
Respiratory tract protection: designed to protect the airways of the wearer from
infectious agents that are transmitted via inhalation of small particles.It may be
appropriate in certain situations, such as during investigations of abortion storms in
small ruminants (Q fever), high mortality rates among poultry (avian
influenza),positive herd (bovine tuberculosis), and avian chlamydiosis. Disposable
particulate respirators often resemble surgical or dust masks but fit closely to the
wearer’s face and are designed to filter smaller particles (surgical masks are not
designed to prevent inhalation of small particles).
Protective outerwear: a. Nonsterile gowns: Gowns provide better barrier protection
than laboratory coats. Permeable gowns- used for general care of animals in isolation.
Impermeable gowns should be used when splashes or large quantities of body fluids are
present or anticipated.. b. Footwear: Footwear should be suitable for the specific
working conditions (eg, rubber boots for farm work) and should protect personnel from
exposure to infectious material as well as from trauma. Recommendations include
shoes or boots with thick soles and closed-toe construction that are impermeable to
liquid and easy to clean.. d. Head covers: Disposable head covers provide a barrier
when gross contamination of the hair and scalp is expected. Bite and other animal-
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
related injury prevention: Use of physical restraints, bite-resistant gloves, muzzles,
sedation or anesthesia, and reliance on experienced veterinary personnel rather than
owners to restrain animals
*****
RATIONAL USE OF HORMONES IN ANIMAL
REPRODUCTION
M.K.TANDLE
The following is a brief description of various harmones used in animal
reproductive disorders
1. Oxytocin: The effect of oxytocin on uterus is to change the weak, spontaneous
and irregular contractions. Physiologically oxytocin has shorter half-life
(about 2 minutes) due to its cleavage in plasma by oxytocinase. Therapeutic response
to oxytocin is always better when administered as slow intravenous drip rather than
given as a single bolus dose. The binding of oxytocin to specific receptors present in
mammary gland and myometrium.stimulates smooth muscle contractions promoting
uterine motility and milk let down. The efficacy of exogenously administered oxytocin
is more in estrogen-sensitized uterus and the response to oxytocin is greatest when
circulatory estrogen levels are high.
Indications: Induction of parturition ( only in case of sufficient cervical dilation),
expulsion of last fetus in polytocous animal, post caesarian section- to speed up
involution and control bleeding after removal of fetus , as local infiltration,
expulsion of placental debris, uterine inertia and post repositioned uterine
prolapse ( to reduce enlargement and facilitate contraction ).Dosage : Mare 75-125
IU ; Cow 75-100 IU ;Sow, Ewe 30-50 IU ;Bitch 5-25 IU;cat 5-10 IU. Route IM or
IV
Precautions: Generally oxytocin preparations contain sodium sulfite as a
preservative therefore it should not be infused with solutions containing higher
concentration of dextrose to overcome possible drug interaction. Administration of
oxytocin in dystocia without sufficient cervical dilation is contraindicated.
Intravenous administration may be done by diluting oxytocin with distilled water in
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
1:10 ratio.Products: Inj. Pitocin (Parke –Davis) 5 IU / 0.5 ml , Inj. Syntocinon
(Novartis) 5 IU / ml
2. Prostaglandins :
a. Cloprostenol sodium (PGF2 α analogue) : It has potent luteolytic action that
brings about regression of corpus luteum (CL) and induces fertile estrus following
luteolysis.
Indications: Cow, buffalo: sub estrum, luteal cyst, synchronized breeding, removal of
mummified fetus, chronic endometritis, pyometra and induction of parturition
Dosage: IM, IV, SC; Cattle, Buffalo: 2 ml IM, SC; 1.3 ml IV. Contra indicated in
pregnancy except for termination of pregnancy.Keep away from pregnant woman
veterinarian, persons suffering with asthma or other diseases of respiratory tract
Products: Inj. Juramate 263 µg / ml,2 ml (Vetcare); Inj. Synchromate 263 µg / ml, 4
ml (Prima Vetcare), Inj Cyclix, Intervet, 2 mL and 20 mL vials ; Inj Clostenol,
Sarabhai Zydus. 2 mL
b. Luprostiol (PGF2α analogue) -Dosage: Cow 15 mg, heifer and Horse 7.5
mg;Products: Inj. Prosolvin 7.5 mg / ml 2 ml, 10 ml, 20 ml (Intervet)
c. Tiaprost (PGF2α analogue)-Products: Inj. Iliren 0.196 mg / ml, 10 ml (Intervet);
Dosage:Bovine 3.5 ml IV, 5 ml SC IM, Equine 3 ml IV, Caprine 1-1.5 ml SC
d. Dinoprost (PGF2 α analogue) : Dosage: Pyometra, chronic endometritis: Cattle 5
ml IM’; Induction of parturition: Cattle 3.5 ml IV, Horse 3 ml IM, Pig 2-4 ml
IM; MTP: Cattle 3.5 ml IV .Products : Inj. Hormo P2α 5 mg / ml, 5
ml(BCAHP) ; Inj. Lutalyse 5 mg / ml10 ml (Novartis)
3. Estrogens: Natural estrogens include oestradiol, estrone and oestriols. They have
low bioavailability following postoperative administration. Simple esters of steroidal
estrogens such as benzoates or valerate are used in therapeutics as they release parent
molecule on hydrolysis. Potency of estrogen is enhanced adding ethinyl groups to the
molecule.
Indications: Misalliance, urinary incontinence in old, spayed bitches, uterine
infections, anal adenoma and to induce estrus in bitches. Dosage: Dog 1-3 mg daily
orally / 0.5 – 1 ml, IM. Precautions: Polydypsia, polyuria, GI upsets, suppression of
red cell production, chronic use may lead to hypogonadism and cystic ovary in
females. Products:Tab Evalon,30s (Infar); TabProgynon-C30’s ;Inj. Progynon
Depot 1 ml amp. (German Remedies)
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
4. Conjugated estrogens: To prevent conception in small animal (misalliance) as it
delays transport of zygote from oviduct into the uterus. In uterine infections,
estrogens facilitate uterine drainage through cervix
provided cervix is dilated. Indications: Misalliance (within one week
following breeding), urinary incontinence in spayed / old bitches, anal adenoma,
lactation, suppression and uterine infections . Precaution: Pregnancy, feminization in
male and large doses may cause aplastic anemia. Products: Premarin (Wyeth lederle)
Dosage: Dog, Cat 3 tabs daily for 3 days, 1 ml IM , Tab 0.625 mg; Inj. 25 mg / ml)
II. Hormones used to treat reproductive disorders :The choice of hormones and
drugs acting on reproductive system are important as therapeutic agents during
reproductive disorders like anoestrus, metritis, pyometra, repeat breeder, retention of
fetal membranes, delayed puberty, ovarian disorders etc. The dosage, route, frequency
and indications of hormones acting on reproductive system are mentioned in tabular
form as below.
Note: Trade names mentioned by the authors are only examples and in any form
the author is not promoting or recommending any pharmaceutical products for
treatment.
Particulars Indications Dosage and Commercial
preparations
route in cow
and buffalo
DRUGS ACTING ON FEMALE GENITAL SYSTEM-OVARIES
Buserelin-GnRH Anoestrus, 2.5 mL, IM, IV Inj Receptal,
analogue Intervet
stimulates Delayed ovulation
follicular 0.0042 mg/mL,
development, Trueanoestrus,Follicular 5mL, IM, IV
estrus and cyst 10 mL vial
ovulation by
enhancing release
of FSH and LH
Gonadorelin- Cystic ovarian disease 100 mcg IM, IV Inj Cystorelin,
GnRH analogue BCAHP,50 mcg/ml,
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
stimulates Delayed ovulation,Repeat 250 mcg IM, IV 2 mL, 10 mL vials
follicular breeder,Improvement of
development, post partum fertility
estrus and
ovulation by
enhancing release
of FSH and LH
PITUITARY GONADOTROPINS
Follicle Superovulation in ETT 50 mg BID for 4 Inj Folltropin-V,
stimulating days Vetrepharm Inc400
hormone mg/vial + 20 mL
diluent
FSH induces
folliculogenesis in
mature female
ovaries
Luteinizing Anovulation 25 mg, IV Inj Lutropin-V,
hormone Vetrepharm Inc,25
Delayed ovulation mg vial + 5 mL
induces diluent
maturation, Cystic ovaries,Repeat
estrogen breeding
production and
finally ovulation of
Graafian follicles
and also the growth
of CL
NON-PITUITARY GONADOTROPHINS
Human chorionic Repeat breeding 1500-3000 IU, IM Inj Chorulon,
gonadotrophin Intervet,1500 IU
Cystic ovaries 1500-3000 IU, IV vial
mimics the effect
of pituitary LH Inj Coriogan,
Delayed ovulation 1500-3000 IU, IM
causing ovulation. Intervet,250 IU/mL
repeat on day 8
It promotes the
formation and 1000 IU, 2000 IU
maintenance of CL Post partum lactation failure 1500-3000 IU, IM vials
, q 24 h with
Inj Corion,Win
synthetic oxytocin
Medicare,1000 IU,
Early abortion 1500-3000 IU /
2000 IU, 5000 IU
week for 4 weeks
vials
as IM
Pregnant mare Superovulation in ETT 1500-3000 IU Inj Folligon,
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
serum IM, IV Intervet1000 IU vl;
gonadotrophin Inj Synchro part
(FSH like action) 400, 500, 600,
induce follicular 700, 6000
growth in inactive IU,BCAHP
ovaries of mature
animals
Other To improve quality and Day 1, 6 mL Inj Ovaset, BCAHP
combinations yield of superovulation in BID ;Day 2, 5 mL
ETT n bovines BID;Day 3, 3 mL 9 mL vial FSH + 3
FSH 0.48 mg/9 BID;Day 4, 2 mL mL vial LH +12 mL
mL, LH 0.42 BID diluent
mg/3mL
hCG 3000 IU, Cystic ovarian syndrome 1 vial as slow IV Inj Nymfalon,
Progesterone Intervet;hCG 3000
125mg/ vial IU, Progesterone
125 mg/ vial
Ovarian steroids
Hydroxy- Delayed ovulation,Post 500 mg, IM Inj Duraprogen,
Progesterone partum anoestrus Unichem;Inj
caproate Proluton Depot,
Cystic ovarian disease 500 mg, IM German Remedies
Stimulates luteal
action and cause Habitual abortion (late) 500 mg for 3 days Inj Uniprogestin
quieting of followed by 500 Depot, Foreva;Inj
myometrium, mg/week, IM Vetaprogen, Prima
enhances Vet care;Inj P-
endometrial Habitual abortions (early) 500 mg after 11/2 Depot, Sarabhai
glandular monthpregnancy, Zydus;Inj
secretions, thus repeat every 10 Dinolutin,
favour in days, IM ;Alved250 mg/ mL,
maintenance of 2 mL ampoule
pregnancy. At
lower doses it
induces ovulation
by its indirect
effects on LH
release
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Progestagen Crestar implant,
Norgestomet- Intervet
Synthetic
Progestagen (Norgestomet 3 mg
Control/ induce/synchronize 3 mg implant SC + (estradiol valerate
Administered as ovulation in normal healthy on ear (to be kept 5 mg, Norgestomet
ear implant to animals for 9 days) + 2 mL 3 mg) per mL)
control/induce/ Inj IM
synchronize
ovulation in
normal healthy
animals. In
conjunction with 6 mg implant SC Synchromate-B
estradiol act as a on ear (to be kept implant, BCAHP
strong negative for 9
feed back complex (Norgestomet 6 mg
on hypothalamic days) + 2 mL Inj + (estradiol valerate
hypophyseal IM 5 mg, Norgestomet
system preventing 3 mg) per mL)
final growth and
maturation of
follicles. Sudden
withdrawal of
Progestagen
releasing implant
lead to an increase
of LH pulse
frequency resulting
in estrus and
ovulation within 2-
3 days
Prostaglandins
Dinoprost- PGF2α Sub-estrum 5 mL, IM Inj Hormo P2α,
analogue BCAHP5mg/mL,
Luteal cyst
Potent luteolytic 5 mL vial;Inj
action by Timing and synchronization Lutalyse,
constriction of of estrus Novartis5mg/mL,
utero-ovarian 10 mL vial
vessels. It enhances
cervical dilation
and also has
selective
spasmogenic
action.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Luprostiol- Sub-estrus,Anoestrus, 15 mg, IM Inj Prosolvin,
PGF2α analogue Intervet.7.5mg/mL,2
Luteal cystPersistent mL, 10 mL,
It causes regression CL,Estrus synchronization
of CL followed by 20 mL vials
follicle growth,
estrus and
ovulation in sub-
estrus and
anoestrus.
Tiaprost- PGF2α Sub-estrus,Luteal cyst 3.5 mL, IV or Inj Iliren, Intervet
analogue
Estrus synchronization 5 mL SC/IM 0.196 mg/mL, 10
Luteolytic activity; mL vial
enhances cervical
dilation and has
selective
spasmogenic
action.
Estrogens Induction of estrus 1.5 mL on day1 Inj Progynon
and 1.5 mL after 3 Depot, Zydus
Natural steroidal Cadila,1 mL
estrogens- 3 mL amp,Inj Heatreg ,
estradiol, estrone, Induction of (di-ethyl stilboestrol
estriols. Low oral parturition,Pyometra,RFM 10 mg/mL),
activity, Potency is Novitech ,3 mL
enhanced adding ampoule
Ethinyl groups to
the molecules
Hydroxy Pre partum uterine/ vaginal 500 mg,alternate Inj Duraprogen,
Progesterone prolapse days for 3 times, Unichem
caproate IM
Inj Proluton
Progesterone acts Depot, German
Post partum prolapse 500 mg for 3
on the Remedies
days ; 500
endometrium
mg/week for 3 Inj Uniprogestin
inhibiting weeks, IM Depot, Foreva
myometrial activity
and thus quieting Prolapse due to pronounced 500 mg for 2
uterus Inj Vetaprogen,
heat days, repeat on 3rd Prima Vet care
day, IM
Inj P-Depot,
Habitual pronounced heat 500 mg at the Zydus AHL
beginning of
estrus, IM 250 mg/ mL,
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
2 mL ampoule
Miscellaneous drugs / products
Eazi Breed CIDR Post partum and suckling Inserted for 7 Eazi Breed CIDR,
anoestrus days; Saideep,
Cystic ovaries Inserted for 12 10,s
days
Silent estrus
Inserted for 10
Estrus synchronization days along with
estradiol benzoate
cap 10 mg or
insert for 7 days
and administer
PGF2α on 6th day
or at the time of
removal
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
THERAPEUTIC CONSIDERATIONS IN HELMINTHIC
INFECTIONS OF FARM ANIMALS
P.M.THIMMAREDDY
Chemicals/Drugs used to treat helminthic infections are called Anthelmintics;
are classified in to antitrematodal, anticestodal and antinematodals. The Ideal drug
should be active against all stages, least toxic to host, have wide therapeutic index,
economical and environment friendly. The principle sites of drug action in parasite
include neuromuscular system, biochemical reactions involved in energy metabolism
and those related to reproduction.
A. Antitrematodal drugs: Drugs used against liver flukes, rumen flukes, lung
flukes and Blood flukes
1. Carbon tetrachloride : Effective against mature Fasciola hepatica but not
against Dicrocoelium dentriticum. Sheep – 3 ml P.o or S.c. Cattle 20 ml S.c. or
5 ml P.o. This drug is hepatotoxic. Hyperaesthesia, convulsions and coma may
occur. More toxicity in hypocalcemic animals. In toxicity, give calcium
compounds and reduce the protein intake.
2. Hexachlorethane: Effective against mature Fasciola sp Haemonchus sp and
Trichostrongylus sp. The dose is 20 gm/100 kg. Monthly dosing in areas of
repeated infestations.
3. Hexachlorphene : 10 mg/kg
4. Triclabendazole : Acting on both mature and immature liver flukes. Cattle –
12mg / kg, Sheep and goat 10 mg/kg.
5. Nitroxynil : Active against mature and immature stages (4 to 6 wks) of Fasciola
sp and gape worms in birds. Reaction at the infection site is common. Induce
yellow staining of the skin and wool. It is not used in lactating cows.
6. Rafaxanide : Effective against mature and immature flukes, oetsum ovis larva
and Haemonchus contortus. 10 mg/kg P.o. Toxicity rare but not used lactating
cows.
7. Oxyclozanide : 10 mg/kg. P.o. Safe for lactating, young and pregnant animals.
Toxicity: Transient diarrhoea and hypogalactia. Others from this group for
subacute and chronic fascioliasis are brotianide (22.5 mg+ thiophanate 200
mg/ml) closantel – 5 mg/kg I. M or 15 mg /kg. P.o. Effective against flukes,
Haemonchus sp, larval flies & ticks.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
8. Diamphenithide : 180 mg/ml susp. 100 mg/kg against mature and immature
flukes
9. Bithiona : 50 mg/kg in divided doses on alternate days for 3 or 4 weeks is
effective against paragonimiasis, fascioliasis and clonorchiasis, taeniosis and
Diphyllobothrium latum
10. Chlorsulon : A sulphonamide 100 mg + Ivermectin 10 mg/ml inj. S.c.
Good for biliary fascioliasis in lactating cattle
11. Resorantel : 65 mg/kg P.o. in cattle and sheep against only intestinal
paramphistomes.
12. Albendazole : 7.5 mg/kg in cattle, sheep and goat, for the control of
Fasciola sp 15 mg/kg b.wt for the treatment of Dicrocoelium dentriticum in
sheep.
13. Lithium Antimony thiomalate 6%. Cattle 15-20 ml i.m 2-3 doses at
weekly intervals against nasal schistosomiosis.
14. Praziquantel : used in human schistosomiosis, clonorchis sinsensis and
opisthorchis viveroni.
B. Anticestodals
1. Natural compounds : The earliest anticestodal drugs used were of plant origin, like
minced pumpkin seeds, powdered rhyzome of male fern, kamala and Arecholine
2. Inorganic Compounds : a) Tin compounds were used against human, dog and
poultry tapeworms. Stannous chloride – man, dog-0.5 gm daily for 8 days. b) Di-n-
butyl tin dilaurate : 1ml for poultry c) Lead arsenate : used for treating Moneizia in
lambs and calves.
3. Synthetic organic compounds : i). Hexachlorophene : 100 mg tab
ii). Bunamidine hydrochloride : Used against Echinococcus granulosus : second dose
after 6 weeks to eliminates those which were immature, Also, effective against
Dipylidium caninum and moniezia expansa.
iii) Dichlorophen : Dogs : 300 mg/kg ,Cats : 100-200 mg/kg
iv) Niclosamide : Dogs & cats: 100-157 mg/kg ,Cattle : 50 mg/kg ,Sheep, Goat,
rabbit and monkey : 100 mg/kg
v). Paramomycin Sulphate :
vi) Praziquantel : 2.5 to 7.5 mg/kg P.o or S.c against Diphyllobothrium latum,
Hymenolepis nana, Taenia saginata etc. Dipylidium caninum, Taenia sp, E. granulosus
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Spirometra, Side effects: Malaise, dizziness, headache, abdominal discomfort with or
without nausea. Not used in puppies or kittens younger than 4 wks.
vii). Nitroscanate : 50 mg/kg used against Dipyllidium caninum, Taenia
viii) Benzimidazoles : a) Mebendazole b) Albendazole c) Fenbendazole
d) Oxfendazoel e) Febantel etc are effective against
tapeworms.
C. Antinematodals
1. Phenothiazine : 10 gm/45kg used in strongyles, Triodontophorus, Haemonchus,
Ostertagia and Trichonema. On exposure to light, it causes photosensitization keratitis
manifested by ulceration of the cornea. So, avoid sun for 2-3 days.
(a) Piperazine : 75 mg/kg P.o. for mammals ,3g/bird in water for 3d in poultry
(b) Bephenium hydroxynaphthoate : irritant and poor absorption from the gut. 80%.
Cure of Trichostrongylus in man, Ancylostoma in man and dogs and nematodirus in
ruminants.
(c). n-Butyl chloride : 90% effective against ascarids and 60% against hookworms.
(d) Toluene : 0.2 ml/kg P.o. 98% effective in ascarids and hookworms in dogs and
cats, Emesis, tremors and ataxia in pups and kitten.
(e) Tetrachloroethylene : Removes 90% hookworms. To prevent toxicity give fat free
diet 48h before dosing. It is hepatotoxic, causes dizziness, inco-ordination and death.
Contraindicated in tapeworm infection as the tapeworms may ball up due to irritation
and occlude the intestinal passage.
(f) Methyridine : 200 mg/kg P.o., S.c, or I.P. Twice the normal dose is toxic.
Diethylcarbamazine potentiates toxicity.
(g) Diethyl Carbamazine citrate: 6 mg/kg P.o or S.c in dogs in Spirocerca lupi,
human wucheria bancrofti or Loa loa, onchocerca volvulus, cutaneous larva migrans
and tropical eosinophilia. 22 mg/kg i.m for 3 days in early cases of Dictyocaulus
viviparous infection in cattle, 5mg/kg daily or alternate day commencing before
exposure and continuing 60 days after exposure.
(h) Disophenol : 10 mg/kg P.o., S.c. or i.m. Effective against hookworms and
spirocerca lupi of dogs, syngamus trachea in turkeys. It causes pyrexia, tachycardia,
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
polypnoea, corneal and lens opacity in dogs which regress within 7 days. Non blood
sucking and histotropic parasites are unaffected, orally administered drug is more toxic.
(i) Phtholofyne : 200 mg/kg for whip worm. 24hour fast followed by light meal after
dosing. Toxicity leads to emesis, ataxia, and death.
(j) Hygromycin-B : An antibiotic in feed for swine and poultry against ascarids,
capillaria, oesophagostomum and Heterakis gallinarum. Feed 6 weeks prior to
farrowing in swine.
3. Tertrahydropyrimidines : Less active against larval stages and have minimal
action on hypobiotic larvae. Not ovicidal.
a) Morantel citrate : Not effective against adult lung worms. 10 mg/kg P.o in
cattle & sheep
b) Pyrantel pamoate : used for round worms in horses, dog and man. Due to
mutual antagonism, piperazine and pyrantel compounds should not be
combined.
c) Oxantel : Specific single dose treatment of Trichuriasis in dog at 55 mg/kg.
4. Benzimidazoles :Benzimidazoles have a high therapeutic index, but not to be used
in the first month of pregnancy (teratogenic).
a) Thiabendazole : Not widely used now
b) Mebendazole : Generally not used in cattle, sheep and horse 10 mg/kg. 25-50
mg/kg twice daily for 5 days for round worms and tapeworms in dogs.
c) Parbendazole : 30 mg/kg P.o
d) Albendazole : It is used in the treatment of roundworms, tapeworms and
flukes. 5 mg/kg for roundworms and 7.5 mg/kg for flukes in sheep and goats .
7.5 mg/kg for round worms and 10 mg/kg for flukes in cattle. 5 mg/kg in horses
e) Fenbendazole : In addition to important roundworms, it is effective against
hypobiotic larva and also on tapeworms in sheep, Goat and dogs.
f) Oxfendazole : Active against round worms, their inhibited larva and tapeworms
4.5 mg/kg P.o as a single dose to cattle, sheep and pig. 10mg/kg daily for 3 days
in horses and dogs
g) Oxibendazole : Effective against roundworms and lung worms in horses 10
mg/kg P.o.
h) Flubendazole : 5 mg/kg P.o. mainly used in pigs against round worms
i) Luxabendazole : Effective against round worms and flukes .7.5 mg/kg for
round worms
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
5. Benzimidazole pro-drugs.These are converted in vivo to benzimidazoles. The drugs
are ovicidal, larvicidal and affect adults including some tape worms (Taenia sp)
a) Febantel : Converted to fenbendazole and oxfendazole, 7.5 mg/kg in cattle and
5 mg/kg in sheep
b) Thiophanate : Converted to lobendazole 50 mg/kg
c) Netobin : Converted to albendazole 7.5 mg/kg P.o in cattle & sheep
6. Imidazothiazoles :
a) di-Tetramisole b) Levamisole (1-Tertramisole) : Effective against larvae (but not
hypobiotic and not ovicidal) and adults. anthelmithic dose is immunostimulant. The
drug is non-teratogenic and hence can be used in pregnant animals. The dose is 7.5
mg/kg Antidote is Atropine
7. Macrolides (macrocyclic lactones)
a) Ivermectin : 0.2mg/kg single oral or P.o.Effective against nematodes and
ectoparasites. Used at 6 ug/kg at one month intervals for prevention of Dirofilaria
immitis infestation in dogs. Other macrolides includes Doramectin, milbomycin-D,
milbomycin oxime, Eprinomectin, Moxidectin and selamectin.
8. Organophosphorus compounds : The use is restricted to the treatment of
round worms of dogs, cats, pigs and especially horses where they also control the
stomach bots.
a) Dichlorovos : 20 -40 mg/kg in horses ,30-40 mg/kg in pigs,27-33 mg/kg in
Dogs. They may be incorporated into polyvinyl chloride resin pellets for slow
release and safety
b) Coumaphos : 2 mg/kg/day for 6 days in feed
c) Trichlorofon : A prodrug of dichlorvos used in horses at 40 mg/kg
d) Napthalofos : Narrow margin of safety
e) Crufomate: used for warble fly control.
Broad Spectrum Combinations
1. Clorsulon and Ivermectin : For use in cattle 1 ml/50 kg. S.C.
2. Dichlorophene and Toluene: used in dogs against cestodes and nematodes
3. Diethylcarbamazine and oxibendazole : used in dogs for prevention of
infection with D. immitis and A. caninum, and for the removal of T. canis and
T.vulpis
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
4. Febantel, praziquantel, and pyrautel: A single dose is given to dogs to
remove D. caninum, T. pisiformis, E.granulosus, A. caninum, U. stenocephala,
T. canis, T. vulpis
5. Milbemycin oxime and Lufenuron :This is given once every mouth to remove
G I worms and control of flea population
6. Praziquantel and pyrantel : A single dose is given to cats and kittens to
remove D. caninum, Taenia sp Ancylostoma sp and T. cati
7. Ivermectin and pyrantel pamoate : This is given orally to dogs every 30 days
to prevent D. immitis and for the treatment & control of T. canis, T. leonina,
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
CLINICAL PROTOCOLS IN ANTINEOPLASTIC THERAPY
OF SMALL ANIMALS
D.DILIP KUMAR
The effectiveness of a chemotherapeutic agent is measured in terms of
concentration and exposure time. Routes of administration and absorption may
influence the efficacy of an administered drug.The chemotherapeutic agents can be
administered orally, subcutaneously, intramuscularly and intravenously for systemic
effects.Local effects can be obtained by topical,intrapleural/peritoneal ,intra
cystic/intrathecal into the CSF.All the chemotherapeutic agents can not be given by
each and every route hence proper selection of route of administration can maximize
the efficacy . Biotransformation of the drug also should be taken into consideration in
chemotherapy.Prednisone used in chemotherapy has to be converted into prednisolone
by the liver to be effective. Distribution of drugs partially determines its effectiveness.
If the drug donot reach to the tumour,the exposure of tumour cells to chemotherapeutic
agent will be nil. Some drugs will be effective during first time administration while
they may not be so effective during their subsequent administration Drug resistance
may develop by several means such as acquired resistance of the tumour may occur
owing to decreased activation or increased deactivation of drug reducing its effective
contact time..Toxicity: GI toxicity, bonemarrow suppression and immunosuppression.
Principles of combinations of chemotherapy: 1. Effective single agent used. 2. Two
drugs with different mechanisms of actions should be used. 3. Intermittent treatment
schedule
Guidelines for chemotherapy: Thorough clinical examination, history collection and
appropriate data base are necessary for chemotherapy.
1. Histological diagnosis of tumour is must to know whether it is begnin or malignant
2. Biological behavior of tumors should be understood
3. Drug toxicities,dose level ,species limitations should be understood.
4. Monitoring of toxicities is essential.
5. Therapy should be undertaken with properly explaining the pros and cons to the
owners.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Chemotherapeutic agents can be classified as : 1. Alkalyting agent’s 2.Antimetabolites
3.Plant alkaloids 4. Antibiotics 5.Hormones 6.Miscelaneous
1. Alkalyting agents: These are the compounds that substitute an alkyl radical (R-CH2-
CH2+) for hydrogen atom on some organic compounds. These agents interfere with
DNA replication and RNA transcription.There are five class of alkylating agents
a) Nitrogen mustard derivatives: Methchloethamine,Cyclophosphamide,Chlorambucil
and Melphalan; b) Ethenimine derivatives:Triethylenethiophospharamide; c)Alkyl
Sulfonate:Busulfan d) Triazene derivatives:Dacarbazine; e) Nitrosoureas: Carmustine,
Lomustine, and Somustine
Cyclophosphamide is the most commonly used alkylating agent in Veterinary
practice.It is used for lymphoreticular neoplasms,carcinomas,mast cell
tumour,TVT,Cyclophophamide requires activation to its active metabolite 4-hydroxy
Cyclophosphamide by liver.Dose 50mg/ M2 per orally or weekly once for four times
intravenously. Chlorambucil is used in canine lymphosarcoma.Dose rate is 2mg/ M 2
Per orally or at weekly intervals for two to four weeks.
2. Antimetabolites: The antimetabolites are structural analogues of normal metabolite
required for cell function and replication.They damage cells by interacting with cell
enzymes (1).By substituting for a metabolite needed in key molecule,rendering it
functionally abnormal (2.)By competing successfully with a normal metabolite that acts
at an enzyme regulatory site to alter the catalytic rate of a key enzyme.
The important antimetabolite drugs are Methotrixate, 6-Mercaptopurine,)5-Flurouracil
and Cytosine Arabinoside. The antimetabolite drugs are S-phase specific.
Methotrixate acts in S-phase to inhibit dihydroxy foliate reductase compitatively and
interferes with both DNA and RNA synthesis.The folic acid antagonists are used in the
treatment of lymphoreticular neoplasms,myeloproliferative disorders,transitional
metastatic cell tumours,TVT,sertoli cell tumour and ostesarcoma.Methotrixate dose
2.5mg/ M2 per orally daily until response or toxicity.
3.Plant alkaloids: Vincristine and Vinblastine are the alkaloids extracted from the
periwinkle plant.Vinca Rosea.They act specifically in M phase by binding with
microtubular protein tubulin and blocking mitosis by interfering with chromosomal
separation in metaphase.Both the drugs are used in the treatment of lymphoreticular
neoplasms Vincristine is the treatment of choice for TVT and has been used for the
treatment of carcinomas and mast cell tumour.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
4.Antibiotics : They are derived from soil fungus( Streptomyces).They are cell cycle
non –specific drugs.They damage the DNA.Inhibit DNA or RNA
synthesis.Doxorubicin is a cytotoxic drug.Vomiting,diarrhea,myelosuprression,cardiac
toxicity are the side effects.Doxorubicin must be given slowly when given
intravenously.Pretreatment with histamine helps in avoiding complications.Dose:30mg/
M2 at three week interval for TVT,lymphosarcoma,carcinoma.
5.Hormones: Peptide hormones convert ATP to c-AMP(cyclic AMP).c-AMP is a
secondary messenger to deliver and amplify signals to intracellular site.Steroid
hormones enter cell and bind to specific receptor protein. “Transformation”
(activation) of this newly formed complex allows it to pass the nuclear membranes
where it binds to DNA.This binding alters transcription of cell messenger
RNA,resulting in synthesis of new protein.Steroid induced increase in fatty acids may
cause dissolution of the nuclear membrane,leading to cell death.
Adrenal corticoids are used for treatment of lymphosarcomas and mast cell
tumours.Sex hormones are used in the treatment of mammary ,prostate and perineal
gland tumours.Hormones have valuable role in replacement therapy following
abalation surgery,in the management of some metastatic problems.Prednisolone 60
to20mg/ M2 per orally every 48 hours used in Lymphoreticular tumors mast cell
tumour,and CNS tumours.Diethyl Stilbestrol 1.1mg/kg (not more than 25mg)- used for
perianal adenomas, prostatic tumours.
6. Miscellaneous agents: examples: L-Asparginase o,p-DDD. L-Asparginase enzyme
preparation is derived from the bacteria.L-asparginase deprives the neoplastic cells that
lack the ability to synthesise L-asparginase of extracellular source there by inhibiting
protein synthesis.L-asparginase acts against cells in G1 phase.Used for the treatment of
lymphoreticular neoplasms @20,000units/ M2 intraperitoneally.Side effects are
anaphylaxis and leukaemia. o,p-DDD: Directly suppresses normal and neoplastic
adrenocortical cells,used in adrenocortical insufficiency @50mg /kg PO, to effect.
Drugs used in Chemotherapy:Chemotherapeutic agents dose is expressed in terms of
mg per square meters of body surface area.This is physiologically more accurate
method of determining the dose.Weight in grams is converted to body surface
area(meter square) as follows: M2 = Km xW2/3 / 104; wherein: M2 - Body surface area
in square meters; W-Weight in grams; Km- Species specific constant (10 for cats and
10.1 for dogs).The relation of body weight to surface area in square meters for dogs is
given in this table:
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
m2 m2 m2
Kg
Kg kg m2 Kg kg m2
0.5 0.06 6 0.33 12 0.52 18 0.69 24 0.83
1 0.10 7 0.36 13 0.55 19 0.71 25 0.85
2 0.15 8 0.40 14 0.58 20 0.74 26 0.88
3 0.20 9 0.43 15 0.60 21 0.76 27 0.90
4 0.25 10 0.46 16 0.63 22 0.78 28 0.92
5 0.29 11 0.49 17 0.66 23 0.81 29 0.94
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
DRUGS MAJOR INDICATIONS Dose& Route of Admn.
Cyclophosphamide Lymphoma, sarcomas, mammary
adenocarcinoma,lymphocytic leukemia
60mg/kgBW daily oral
Melphalan Multiple myeloma 150mcg/kgBW/day or
250mcg/kgBW daily 4 weeks
oral
Chlorambucil Chronic lymphocyticleukemia, 100mcg/kgBW daily oral
lymphoma
Carboplastin CNS neoplasm,GI carcinomas 300-360mg/m2 BSA by IV
Dacarbazine Lymphoma 2-4.5mg/kgBW for 10 days
IV10-15mg/day for 4-8days
oral
Busulfan Chronic myelogenous leukemia, 60mcg/kg BW daily oral
polycythemia vera
Methotrexate Lymphoma, Sertoli cell tumor, 10-15mg/day for 4-8 days
osteosarcoma, metastatic TVT oral
Fluorouracil GI, lung, liver, and mammary 15mg/kgBW once a week
carcinomas (systemic); cutaneous oral15mg/kgBW in 500ml
carcinomas (topical) DNS
Dactinomycin Choriocarcinoma, testicular carcinoma, 15mcg/kgBW per day or400-
(Actinomycin D) rhabdomyosarcoma, lymphoma 600 mcg/m2 BSA IV
Doxorubicin Lymphoma, acute lymphocytic 60-75mg/ m2 BSA IV
granulocyticleukemia, sarcomas
carcinomas,
Bleomycin Carcinomas (testicular, squamous cell – 15,000IU thrice a week
head,neck,seminoma,malignant IM/IV
teratoma
Vinblastine Lymphoma and leukemias, 0.1-0.5mg/kgBW IV
mastocytoma
Vincristine TVTs, lymphoma and leukemias,CNS 25-75 mcg/kg or 1.4mg/m2
tumors, mammary carcinoma
IV
Cisplatin Osteosarcoma, carcinomas (transitional 50-120mg/m2 BSA with %
cell, testicular, squamous cell of head NS, IV
and neck, ovarian, cervical, bladder
L-Asparaginase Acute lymphocytic and lymphoblastic 1000units/kg BW/10days
leukemia and lymphoma with NSor Dextrose 5%
Hydroxyurea Polycythemia vera, mastocytoma, 20-30 mg/kgBW oral
granulocytic and basophilic leukemia,
KVC Sponsored CVE training programme on “Chemotherapy and
thrombocythemia
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary
Prednisolone College,Bidar,from
Lymphoma, 23rd to60mg/m
mast cell tumors, palliative 28th 2November
IM,IV
2009 treatment of brain tumors
Tamoxifen Estrogen-receptor-positive mammary 20mg/day single dose oral 76
carcinomas
Flutamide Testosterone-receptor-positive prostatic 250mg TID oral
tumors; surgical castration preferred
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
ANTIMICROBIAL THERAPY IN HEPATIC
IMPAIREMENTS
M. VIJAY KUMAR
Liver has very complicated functions and one of the most important function is
the detoxification of drugs such as antibiotics and its metabolites. Some antibiotics can
cause allergic reactions while others can cause direct damage to their liver, which can
be quite severe in patients with chronic liver disease. For patients with a pre-existing
liver disorder, the detoxification function of the liver is already compromised and
substances that would normally be metabolized could actually accumulate in the liver
or in the bloodstream.Liver disease may have a variable effect on drug clearance. There
are no tests for hepatic function that will reliably predict drug clearance.
Antibiotics that accumulate in this manner could become toxic to the body and
its functions can change drastically from its original purpose. For the most part in
treating patients with preexisting liver disease who develop infections outside the liver,
one should use caution in prescribing drugs known to be dependent on liver for
inactivation or excretion. Usually a safer substitute drug can be found. If a potentially
toxic drug must be used, blood levels can be useful in monitoring the dose to within
safe limits. One should also take care to avoid use of hepatotoxic non-antibiotic drugs
concomitantly. On the other hand, drugs metabolized and/or excreted by the liver are
theoretically ideal for treatment of acute infections of liver and biliary tract. Each one
of the ollowing antibiotic is ordered according to their potential harmful effects on the
liver, the top group being the most potentially harmful and the last group being the
least.
Tetracyclines: Used in larger doses, cause jaundice, fever, and fatty liver. Hepatitis
patients should not be administered with these agents. All tetracyclines are
concentrated in liver and excreted via bile into intestine, where they are reabsorbed.
Variable amounts of each member of this drug family are thereafter eliminated in
urine.; have prolonged half-lives in the serum because of slower renal clearance than
that of tetracycline or oxytetracycline. With excess parenteral dose, liver toxicity
progresses to acidosis, shock, coma and death.Other organs which may suffer
simultaneous toxicity are pancreas, kidneys and brain. Pregnancy and chronic renal
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
disease seem to predispose patients to this type of hepatotoxicity. Dosage adjustment is
necessary, avoid exceeding a blood level of 10mcg/ml. Tetracyclines have adverse
effects on several hepatic enzymes. Inactivated chlortetracycline causes same toxic
hepatic changes as the active drug, so hepatic toxicity appears not related to
antibacterial activity; thus to be avoided completely in liver disease
Macrolides : Erythromycin: It causes damage to the liver via cholestasis (bile
retention) and jaundice. The harmful effects usually start to show after 10 to 14 days
use and the incidence rate is approximately 5 to 10%. Clinically, patients may develop
abdominal pain, nausea, vomiting, jaundice, and elevation of liver enzymes. These
conditions are often considered allergic reactions since the incidence rate is not very
high Liver toxicity is caused by only estolate form. Avoid estolate form in liver disease
and other forms in usual dosage. Estolate-induced hepatitis is a dose dependent.
hypersensitivity reaction.
Lincosasmides: Lincomycin: is excreted and re-excreted via enterohepatic circulation.
Bile levels are high upto 10-20x the serum level. Occasional jaundice and/or abnormal
liver function tests which clear rapidly, sometimes even while drug is continued. Half-
life of drug is doubled in liver disease accordingly drug dose should be reduced, or
drug avoided entirely.
Kanamycin : Not Metabolised by liver.No change in dose in case of parenteral liver
disease.in case of oral dose kanamycin at 8 Gm/day eventually builds serum levels to
therapeutic range. This effect is even greater with hepatic disease and azotemia.
Accordingly, such patients on gut sterilization with kanamycin should be watched for
deafness and increasing nephropathy. Neomycin: Not metabolised by liver. No more
than 6 Gm P.o in liver disease for gut sterilization. If azotemia also present,kanamycin
is preferred.
Chloramphenicol: When metabolized in the liver, they combined with glucoronic
acid and lose their anti-microbial effects. This combination of antibiotics and
glucoronic acid can accumulate in the bloodstream, which can cause bone marrow
inhibition. As a result, WBC and RBC counts can drop and patients with hepatitis
should try to avoid this group if they can. Metabolism by liver. 85-95% is conjugated in
liver to monoglucuronide and 3% is further converted to aryl amines and aryl nitro
derivatives.Most of above is secreted then by kidney tubules. Significant concentration
in liver tissue levels and average bile levels,that of plasma. Liver toxicity is rare. Use
with caution in liver disease. If ascites or jaundice is present, use under 25 mg/kg/ day
or another drug. Newborns are vulnerable to "grey syndrome"due to immature hepatic
and renal function.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Penicillins: These antibiotics cause the least liver damage and only patients who are
allergic may experience some side effects. Generally, antibiotics in the penicillin family
are the most "liver friendly" and safe for chronic hepatitis patients to use.
Penicillin G: . Metabolism by liver: Only minor fraction is ordinarily handled by liver,
but in impaired renal function the liver may be a major excretion route via bile. Attains
significant liver tissue levels and also bile levels.Liver toxicity is rare, as part of a
generalized hypersensitivity reaction. No change in dose in liver diseases if renal
function is good and reduce dose in circumstances of combined kidney and liver
disease.
Generally the information for penicillin G applies also for Alpha-phenoxy-
peniclllins Methicillin., Oxacillin methicillin. Cloxacillin and broad spectrum
penicillins: ampicillin, hetacillin, carbenicillin and nafcillin.
Streptomycin and Dihydrostreptomycin: Metabolism by liver.Small fraction is
secreted into bile. Bile levels up to 10-20mcg/ ml on high doses. Liver toxicity is rare
and also may aggravate existing liver disease. No change in dose in liver disease.
Cephalosporins: Cephalothin: Metabolism by liver, 70-80% usually excreted
unchanged in urine. However, it can be inactivated by deacetylation (presumably in
liver), then excreted in urine. Advisable to decrease in presence of combined renal-
hepatic disease.
Nitrofurantoin: Metabolism by liver: 50-60% is metabolized at unknown site. Rarely,
causes a hypersensitivity hepatitis with cholestasis, focal necrosis,
infiltrates,eosinophils.
Sulphonamides: Metabolism is significantly, but not solely by liver (acetylation,
glucuronidation, and/or oxidation), then excreted into urine. Not influenced by dose:
direct hepatotoxicity and hypersensitivity. Either may go on to acute yellow atrophy.
Best to avoid dose in liver disease. Pre-existing nutritional liver disease may predispose
to sulfonamide hepatotoxicity. Kidneys appear to be more susceptible to damage by
sulfas in patients with chronic liver disease.Neonate require less dose for therapeutic
blood levels.
Metronidazole and related drugs (tinidazole, ronidazole): are sometimes used in
patients with hepatic disease because of the anaerobic spectrum. The most serious
problem caused by high dose of metronidazole has been attributed to CNS toxicity and
include seizures, ataxia, nystagmus, tremors, and rigidity.4 These signs have been
attributed to inferring with the inhibitory neurotransmitter GABA. Because animals
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
with hepatic disease also may be prone to CNS disorders that also share these clinical
signs, veterinarians should understand the risks of metronidazole, and become familiar
with the signs associated with toxicity.
Fluoroquinolones: The fluoroquinolones (enrofloxacin, marbofloxacin, orbifloxacin,
difloxacin) have had a good safety record and increased risk of toxicity in animals with
hepatic disease has not been documented. Although some of these drugs are
metabolized, the clearance is low and probably not affected unless there is substantial
loss of hepatic function. These drugs are also cleared by the kidneys
A common dilemma for veterinarians is which nonsteroidal antiinflammatory
drug (NSAID) to administer to a patient with hepatic disease. The six approved
NSAIDs for dogs: carprofen, etodolac, Meloxicam (cats), tepoxalin, deracoxib, and
firoxixib. Because studies have not been conducted in animals with hepatic disease,
there is no single drug shown to be safer than another. However, All NSAIDs have the
potential to: (1) induce liver injury. (2) Pre-existing elevations in liver enzymes has not
been shown to increase an animal’s risk for NSAID-induced liver injury, but a sharp
increase in liver enzymes and/or bilirubin after instituting NSAID therapy is cause for
alarm. (3) cause gastrointestinal injury, including erosions, ulcers, and bleeding.
Patients with hepatic disease have an increased risk of these problems. (4) There is no
NSAID yet to be shown safe for long-term administration for cats and hepatic reactions
have been one of the problems associated with NSAID administration in cats. Tramadol
and opiate analgesic drugs have high clearance and their metabolism is not likely to be
affected by a loss in hepatic function or changes in hepatic enzymes. These drugs have
a high safety margin and can be used safely in patients with hepatic disease.
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
ANTIMICROBIAL THERAPY OF OCULAR INFECTIONS
M.VIJAY KUMAR
Corneal epithelium is the main site of resistance to drug penetration.. As a result, the
epithelium and endothelium are relatively impermeable to electrolytes but are readily
penetrated by fat-soluble substances. Drugs that have the ability to exist in equilibrium
in solution as ionized (water soluble; polar) and unionized (lipid soluble;nonpolar)
forms are ideal for topical use, i.e., chloramphenicol, fluoroquinolones. Topical
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
administration is used for treatment of eyelids, conjunctiva, cornea, iris, and anterior
uvea. Following which , up to 80% of the applied drug(s) is absorbed systemically
across the highly vascularized nasopharyngeal mucosa. Because absorption via this
route bypasses the liver, there is no large first-pass metabolism seen after
administration PO.
2. Subconjunctival (bulbar conjunctiva): This technique requires only topical
anesthesia and a tuberculin syringe with a 25- or 27-gauge needle. Volumes should not
exceed 0.25 ml in cats and dogs and 1.0 ml in horses and cows. Subconjunctival
medication reaches the cornea by slowly leaking out of the injection site. Intraocular
drug levels are attained by diffusion through the cornea and sclera. This is used for
diseases of the cornea, anterior, uvea, anterior vitreous, and sclera.Drugs with low
solubility such as corticosteroids may provide a repository of drug lasting days to
weeks. Appropriate amounts must be used, as large amounts, especially of long-acting
salts, can cause a significant inflammatory reaction. For sub-Tenon’s injections, 0.5
ml/site is usually safe and effective in small animals and ≤1 ml in large animals such as
the horse and cow.
3.Retrobulbar medications:are used infrequently for therapeutics. In cattle, the
retrobulbar tissues can be anaesthetized with local anesthetic (lidocaine) for
enucleations. Whenever any medication is placed into the orbit, extreme care must be
taken to ensure that the medication is not inadvertently injected into a blood vessel, the
optic nerve, or one of the orbital foramen. Retrobulbar injection has a high risk of
adverse effects and should not be used unless the clinician is experienced and the
animal is appropriately restrained.
4. Intravitreal-used infrequently: Antibiotics,antifungal drugs have been effectively
used in microgram dosages. Generally injected at the pars plana for infectious
endophthalmitis.
5. Systemic-P.O., I.V. or I.M: Systemic administration is required for treatment of
diseases of the retina, optic nerve, and vitreous., for posterior segment therapy and to
complement topical therapy for the anterior segment. The blood-ocular barriers can
limit absorption of less lipophilic drugs, but inflammation initially allows greater drug
concentrations to reach the site. As the eye starts to heal, these barriers become more
effective and can limit further drug penetration. This should be considered when
treating posterior segment disease, eg, blastomycosis in small animals with hydrophilic
drugs such as itraconazole.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Ocular dosage forms : Topical ophthalmic drugs are formulated as ointments,
suspensions and solutions. Deciding which formulations to be used depends on the
several practical considerations.Ocular contact time of ointment is longer than solutions
or suspensions,so they are more practical when the owner cannot follow a frequent
administration regimen.avoid ointments on penetrating wounds or descemetocele,and
prior to intraocular surgery,as their petroleum base elicits severe granulomatous
reaction when in direct contact with intraocular tissue. The frequency of topical
application depends on disease and formulation.One drop of an antimicrobial solution
applied four times daily is usally sufficient in uncomplicated corneal ulcers and
bacterial conjunctivitis.When ointment is used a , 5mm strip is applied to the
conjunctiva a minimum of three times a day. If more than one drug is involved in the
therapeutic regimen,then 3 to 5 minutes should be allowed between application of each
medication to avoid dilution or chemical incompatability.antimicrobial therapy is
typically continued for seven days or until the ocular infection is resolved.
Antibacterial ocular drug therapy
Topical antibiotics are indicated for the treatment of corneal ulcers, corneal
perforations, conjunctivitis,and blepharitis.. Ideal choice of appropriate therapy begins
with identification of the organism and its sensitivity. Culture or cytologic examination
of material from the affected area is necessary.Minor bacterial conjunctivitis infection
may not justify routine culture and may be amendable to initial therapy with broad
spectrum antibiotics. Normal ocular flora is predominantly gram positive;a
predominance of gram negative organisms is indicative of an abnormal condition.
Chloramphenicol: Broad spectrum, bacteriostatic. Soluble in both water and fat so it
penetrates intact cornea with topical administration-thus may be considered for initial
treatment of intraocular infections (penetrates the cornea).it is good first choice
antimicrobial for corneal ulcers and bacterial conjunctivitis.it is having poor efficacy
against gram negative bacteria and pseudomonas spp.Frequency of administration- q4
hours for full therapeutic levels. Toxicity- risk of aplastic anemia
Aminoglycosides: a.. Neomycin: Usually found in combination with other antibiotics.
Broad spectrum-bacteriocidal impairs protein synthesis.Frequency of administration-
BID-TID. Toxicity- Topical-localized sensitivity; conjunctival irritant.Systemic-
ototoxicity-possible head tilt. b. Gentamicin: Broad spectrum bactericidal activity
including Streptococcus, Staphylococcus, Proteus spp, and Pseudomonas aeruginosa.
Effective topically and subconjunctivally for external ocular infections. It is available
as solution and ointment because of its chemical characteristics does not readily cross
lipid membranes,but readily enters the stroma when the corneal epithelium is
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
damaged. Renal toxicity with concurrent oral therapy, may be toxic to surface
epithelium. c. Tobramycin.: Two to four times more effective against Pseudomonas
spp. and betalactamase producing staphylococci than gentamicin and effective against
gentamicin-resistant microbes.
Polypeptides:a.Bacitracin: Bactericidal, active against gram positive microorganisms.
Used in combination with other antibiotics. Poor corneal penetration. b. Polymyxin B:
Poor penetration. Bactericidal. Effective mainly against gram-negative bacilli and
Pseudomonas spp. Should not be given subconjunctivally.
Cephalosporins: a.Cefazolin: Broad spectrum, first generation cephalosporin.Topical
use for gram + cocci resistant to other antimicrobials. Can be administered
subconjunctivally-does penetrate intact cornea. Usually diluted to 50 - 100 mg/ml
concentration. Mix with artificial tears to a concentration of 33 mg/ml for treatment of
meibomitis
Fluoroquinolones: Eg: Ciprofloxacin ,Levofloxacin, Ofloxacin etc. Broad spectrum,
active against gram positive and gram negative microorganims. Drug of choice for
betalactamase producing staphylococcus and aminoglycoside resistant pseudomonas
spp. Generally preferred in corneal, conjunctival, and intraocular infections. Excellent
corneal penetration.not effective against streptococci spp. Because of their spectrum of
activity these agents should never be used as empirical treatment.
Antiviral ocular drug therapy
The topical antiviral agents are static in action and topically irritating,so frequent
dministration is necessary and client compliance and patient tolerance are issues.
Idoxuridine: Frequency of administration is 1 drop every 4hrs until corneal re-
epithelialization occurs. Doesnot penetrate the cornea unless the epithelial barrier is
broken. Acts by altering the viral replication by substituting for thymidine in the viral
DNA chain therefore prolonged or too frequent administration may damage the corneal
epithelium and prevent the ulcer healing.
Vidarabine: 3%Ointment-it is poorly lipid soluble,so corneal penetration is minimal
unless ulceration is present.Penetrates the cornea better than Idoxuridine. Frequency of
administration is to apply small amount of ointment 5 times daily until corneal re-
epithelialization is complete,the every 12 hours for 7 days.
Trifluridine: 1%Solution-Current drug of choice for feline herpetic keratitis. Antiviral
potency reported as over twice that of idoxuridine and 5 times greater than Vidarabine.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
s.penetrates the intact cornea,and ulceration and uveitis increase its intraocular
penetration.; administered 4-8 times/day for 2 days, and reduced over next 2-3 weeks.
Antifungal ocular drug therapy
Topical antifungal agents are used more commonly to treat fungal keratitis in horses
than in small animals. Penetration of the intact cornea is poor with all antifungals.
Polyenes : Natamycin : Used against Candida spp. and Fusarium spp. Amphotericin
B: Fungistatic. Generally used systemically for fungal endophthalmitis. May be given
as an intravitreal injection in mcg dosages.
Imidazoles. Miconazole 1%: the drug of choice for most veterinary fungal
keratitis.Tolerated well as subconjunctival injection. 1 ml SID x 3-5 days if tolerated.
Treatment frequency of a fungal keratitis may warrant 1 to 4hour treatment
intervals.lotions or sprays that contain ethyl alcohol should not be applied to the
eye. .Fluconazole is the synthetic triazole, fungistatic.currently drug of choice for
topical use, subpalpebral lavage unit, and intracameral (100 μg) injection. Treatment
for fungal keratitis may warrant 2 to 4hour treatment intervals.
Anti-inflammatory ocular drug therapy:
Corticosteroids: Subconjunctival injection of corticosteroids provide a greater local
anti-inflammatory effect than can be achieved by topical or systemic administration.
Posterior segment inflammation requires systemic corticosteroid therapy. In general,
topical therapy should be continued two weeks beyond resolution of clinical signs.
Local side effects of corticosteroid use include delayed corneal healing, increased
corneal collagenase activity, and an increased incidence of bacterial and mycotic
keratitis. In addition, topical corticosteroids may result in systemic changes. These
include reduced baseline cortisol levels, suppression of the adrenocorticotropic
hormone response curve, and altered carbohydrate metabolism. Frequency of
administration-dependent on clinical signs and the type of steroid used..
Nonsteroidal anti-inflammatory ocular drugs : Some degree of GI intolerance may
occur such as gastroduodenal ulceration and hemorrhage-when NSAIDs are used
systemically.
Aspirin: dog-10 to 20 mg/kg, BID; cat-10 mg/kg, q 48 hours. Carprofen :. May have
fewer side effects.Do not use in Labrador retrievers - may cause liver disease. Dosages:
2.2mg/kg BID. Not approved for use in cats. Etodolac :: dog-10 - 15 mg/kg, PO SID.
Should not be used in dogs < 5 kg in the horse and dog , although not currently
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
approved for use in dogs.: dog-0.75 to 1.20 mg/kg, IV, SID, not to exceed 2 days.
Commonly given 30 minutes prior to surgery to minimize postoperative swelling and
inflammation .; Not to be used. In cat. Flurbiprofen: Used topically preoperatively to
stabilize the blood-aqueous barrier in inflammation (in diabetes mellitus), decrease
production of ocular prostaglandins and maintain pupil size. Used to treat anterior
uveitis and in the presence of corneal ulceration.
Ocular topical Anesthetics : To be effective, local anesthetics must have properties
similar to drugs that penetrate the cornea. They must be capable of existing in ionized
(water-soluble) and nonionized (lipid soluble) forms. Local anesthesia is less effective
in inflamed tissue which has more acidic pH than normal. Most topical anesthetics are
effective within 30 seconds to 3 minutes to facilitate procedures such as tonometry,
corneal and conjunctival scrapings, and subconjunctival injections. Microbial cultures
should be taken prior to application of topical anesthetics as inhibition of
microorganisms has been attributed to topical anesthetic agents. The agents used are
Proparacaine - 0.5%, . Tetracaine - 0.5% to 2%.. Topical anesthetics should not be
used on a regular basis with painful eyes because: Animal may scratch off corneal
epithelium (feels no pain) and may inhibit mitosis (thus healing) in corneal cells.
a. Osmotic Agents (topical) : 2-5% NaCl (hypertonic saline). Indicated primarily for
treatment of severe chronic corneal edema originating from superficial epithelial
disruption and for severe cornea bullae formation. Side effect-localized irritation.
b.Tear Film Supplements : Many tear film supplements currently exist today. All are
indicated to control keratitis sicca. May provide temporary comfort to corneal irritation
resulting from distichia, entropion, or sutures, and as a vehicle for delivery of
medications. Tear supplements are available in solution and ointment form and are
intended to replace the aqueous or lipid layer of the tear film. Preservative-free
products generally recommended.
c.Lacrimogenics: These are drugs potentially capable of stimulating tear secretion.
1. Pilocarpine: May be effective in the rare case of neurogenic KCS. Prescribed as 2
drops of 2% Pilocarpine per 4.5kg body weight added to the food twice daily.
2. Cyclosporine A 0.2% ointment : Cyclosporine is a potent suppressor of T-cell
growth factor and of the cytotoxic T-cell response to this growth factor.
3. Tacrolimus 0.02%, 0.03% ointment or solution : Effective alternative to
cyclosporine. T-cell surpressor with a distinct receptor site to cyclosporine.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Anticollagenase/Mucolytic Agents :Collagenase inhibitors are indicated for the
treatment of melting corneal ulcers. Acetylcysteine : Diluted from 10 to 20% with
artificial tears to a 5 to 8% concentration. Administered every 1 to 4 hours until desired
effect is achieved.
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
ANTIMICROBIAL THERAPY OF FUNGAL SKIN
INFECTIONS
SANTOSH .P SARANGAMATH
The ideal antifungal agent would be one that targets structures present
in fungal pathogens that are absent in other eukaryotic cells. The fungal cell wall, a
structure that is both unique and essential to fungi, would seem to be such a target. The
vast majority of traditional antifungal drugs selectively target ergosterol, an essential
component of the fungal cell membrane, with greater affinity than for cholesterol in
the mammalian cell membrane. New antifungals have evolved especially azoles and
triazoles, which selectively target fungal cell wall with least toxic effect on the body.
Compounds that interfere with the synthesis of important fungal cell wall components
such as glucan, chitin and mannoproteins have become a focus in the development of
new antifungal agents.
Among the cutaneous diseases fungal diseases involving skin and appendages
(Dermatophytosis) i.e cutaneous mycosis are commonly encountered as compared to
the deep mycosis involving deeper organs of the body. Fungal infections involving the
keratinized layers of the skin and its appendages like hoof, nails, and horns caused by
group of mycelial keratinophilic fungi are called dermatophytes, The term
dermatophytosis indicates the relationship of the disease with dermatophytes as
etiological agents. Dermatophytes of dog and cats mainly belong to T.
mentagrophytes, M. canis, M. gypseum.
The clinical signs of dermatophytosis are extremely variable; lesions are
circular, irregular and vary from scaly patches of alopecia to inflammed to nodular
erythematous patch of alopecia. Hairs partially broken/ fallen with bran like scales and
crusts, signs like erythema, scales, crusts, thinning of hairs frequently in the form of
broken hairs with secondary folliculitis with pruritus are usually observed.
Diagnosis is based on clinical signs, skin scraping examination, examination of
hairs by wood’s lamp, and finally by fungal culture on saborauds dextrose agar or
dermatophyte test medium. The gold standard for diagnosis is a fungal culture. Wood's
light examinations are only screening tools, and direct hair examinations, although
inexpensive, are only practical when infected hairs fluoresce on Wood's light
examination. Finding these hairs allows rapidly diagnosing the infection and starting
therapy. However, if the hairs are not present, this tool is time-consuming and not cost-
effective in practice.
Another type of fungal or yeast disease is malassezia dermatitis; the clinical
signs of which may be localized or generalized. Involving the external ear canal,
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
interdigital skin, ventral neck, axillae, and inguinal region. Affected areas are
erythematous, alopecic and often lichenified with or without hyperpigmentation. The
lesions surface is often greasy and affected dogs have musty or malodour.
Diagnosis of malassezia dermatitis is by cytological examination or acetate
tape impressions, stained with methylene blue which will be examined for the presence
of round to oval monopolar budding yeasts.
ANTIFUNGAL THERAPY
Dermatophytosis will spontaneously resolve in most healthy cats, but treatment is
recommended as the disease is zoonotic and highly contagious. The end point of
therapy will go up to the achievement of mycological cure as well as decontaminated
environment but not the clinical cure on the animal itself so as to prevent re-infection.
A mycological cure is defined as two or three consecutive negative fungal culture
results at weekly or biweekly intervals, and treatment should continue until all these
negative culture results are obtained.
Treatment recommendations:
1) Clipping the coat:. Clipping the coat removes infected hairs , minimizes continued
shedding of hair fragments and spores; also makes topical therapy application easier
and allows for more thorough penetration of topical antifungal agent. In addition,
clipping helps shorten the duration of therapy and ultimately decreases the cost of
treatment. It may temporarily worsen the infection by causing microtrauma to the skin.
Also, it may result in environmental contamination if appropriate efforts to capture
infected hairs and spores are not taken.Dipping is required in pets that live with
children and elderly or immunosuppressed people, as well as in shorthaired breeds with
generalized lesions and in longhaired cats regardless of lesion severity
2) Administering topical antifungal therapy twice weekly: The most effective
topical antifungal agents are lime-sulfur, enilconazole, and miconazole. Lime-sulfur is
suitable for sole therapy; combined topical and systemic therapy is the treatment of
choice. It is important to note that fungicidal efficacy does not imply that one
application of any of these products is 100% fungicidal. These products are fungicidal
with repeated application. Lime-sulfur (8 oz/gal water ) has been used as the topical
therapy of choice, and in some cases as the sole therapy. Enilconazole topical solution
10% concentrated solution (100 mg/ml) is effective against M. canis. It is associated
with hypersalivation, anorexia, weight loss, emesis, idiopathic muscle weakness, and
slightly elevated serum alanine aminotransferase activity. Miconazole, as a sole
therapeutic agent or in combination with chlorhexidine, the shampoo needing a contact
time of 10 minutes for the therapeutic effect. This product can be irritating to the eyes
and can cause skin irritation. Other dips like povidone-iodine, chlorhexidine have
been consistently found to be ineffective against M. canis.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
3) Administer systemic antifungal therapy - Systemic therapy is the treatment of
choice for feline dermatophytosis. The efficacy of griseofulvin, itraconazole,
terbinafine hydrochloride, and lufenuron alone or in combination with other therapies
showed that griseofulvin, itraconazole and terbinafine are most effective agents
Griseofulvin : is fungistatic that inhibits nucleic acid synthesis and cell mitosis
metaphase by interfering with function of spindle microtubules.Its absorption is
enhanced by administering it with fatty meal or by using formulations containing
polyethylene glycol.
It is teratogenic and should not be given to pregnant animals. also may interfere with
spermatogenesis, so it is best avoided in breeding males. Anorexia, vomiting, and
diarrhea are seen, which can be managed by dividing the dose into twice-daily
administrations. Bone marrow suppression and neurologic side effects are most likely
idiosyncratic reactions. Do not use griseofulvin in cats that have feline
immunodeficiency virus (FIV) infections, because severe neutropenic reactions have
been seen in cats with FIV.
The most commonly used dosing regimen is daily: griseofulvin microsize at a
dosage of 25 to 50 mg/kg given orally once a day or divided twice a day; griseofulvin
ultramicrosize at a dosage of 5 to 10 mg/kg given orally once a day or divided twice a
day. Higher doses may be needed in refractory cases.
Ketoconazole : is administered at the rate of 5 to 10 mg/kg b.wt. orally once daily for
21 days. Available in the form of tablets or shampoos, this will be useful for topical as
well as systemic use. This drug is also tolerated in dogs, but long term therapy may
involve the potential risk of causing liver as well as renal damage.
Itraconazole : is a triazole derivative that alters fungal cell membrane permeability by
inhibiting ergosterol synthesis; is fungistatic at low doses, fungicidal at higher doses.It
is well-tolerated in cats and dogs, with vomiton, anorexia being most common adverse
effects a) Daily dosing: 10 mg/kg orally once a day; b) Combined continuous/pulse
therapy: 10 mg/kg given orally once day for 28 days and then on an alternate week
regimen (one week off and one week on) . c) Short-term cycle therapy: 10 mg/kg
given orally once a day for 15 days, followed by fungal cultures 10 -15 days later, this
cycle is repeated until the cure. . It has replaced griseofulvin as the drug of choice for
treating dermatophytosis
Terbinafine : is the newest systemic antifungal agent to be used in treating
dermatophytosis. It is an allylamine antifungal agent that suppresses the biosynthesis of
ergosterol by inhibiting the fungal enzyme squalene epoxidase.31 The drug is
considered to be fungicidal against dermatophytes.
Fluconazole : Fluconazole is also hepatotoxic and nephrotoxic, but its elimination
from the stratum corneum is approximately 2 to 3 times slower than the plasma. Also,
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
due to its rapidity in accumulation the skin after oral ingestion makes the drug to be
administered once a week or daily for 2 to 4 weeks will help in improvement of the
condition. This is administered safely at a dosage of 5 mg/kg/day which is well
tolerated in both dogs and cats.
Lufenuron : is a benzoylphenylurea drug that disrupts chitin synthesis and is used for
flea control. Chitin is a critical component of the outer cell wall of fungi, and it is
possible that drugs that disrupt chitin synthesis might also have antifungal activity. One
report suggested it is useful in treating variety of fungal diseases including
dermatophytosis. But still, lufenuron has been a widely debated topic in veterinary
practice.
4) Considering Fungal vaccines: Intense interest in developing a fungal vaccine to
prevent and possibly treat dermatophytosis continues. Fungal vaccines as sole therapy
are not effective in treating dermatophytosis, but they may be a useful adjuvant therapy
when combined with appropriate topical and systemic therapy and environmental
control or a practical alternative to topical therapy in situations in which topical therapy
cannot be used.
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
CLINICAL PHARMACOLOGY OF MISCELLANEOUS CLASS OF
ANTIBACTERIALS
GANESH. B. KUMBHAR
The following is a brief description of various miscellaneous class of
antibacterials
Polymyxins : Two members- .Colistin (Polymyxin E)(Available as sulphates for oral
and topical use) and Polymyxin B. The spectrum is gram negative bactericidal. They
are commonly used topically due to their systemic toxicity(nephrotoxic, neurotoxic,
neuromuscular blocking effects) . They are synergestic t with sulfonamide and
trimethoprim against variety of enterobacteriaceae.colistin is synergestic with rifampin
(In vivo) against multidrug resistant P.aeruginosa and is employed in coliform mastitis.
Vancomycin-: The spectrum is gram positive aerobic cocci and bacilli bactericidal. It
is used against staphylococcal bone and soft tissue.infections in in dog.Dogs-3 mg/kg
PO, 2 to3 times daily & 10-20 mg/kg IV , 3 to 4 times daily. Ototoxicity and
nephrotoxicity, and thrombophlebitis are the adverse effects. Its administration along
with aminoglcosides should be avoided as it may potentiate the toxicity of
aminoglycosides.
Spectinimycin: is an aminicyclitol antibiotic, bacteristatic against many gram
nagative bacteria, mycoplasmas.. It is used in dog cat, horse pigs for the treatment of
enteric & respiratory infections.. Dogs & cats- 5-10 mg/kg IM, 2 times daily.; Cattle- 8-
12 mg/kg IM, 3 times daily; Calves- 20-30 mg/kg IM, once times daily.; Horses- 20
mg/kg IM, 3 times daily.; Pigs-10 mg/kg PO, 2 times daily.No significant adverse
effects have been obseveved (by parenteral route). On high doses may produce
neuromuscular blockade. Concurrent use along with tetracyclines or chloramphenicol
may produce antagonistic effect.
Rifampicin: is a semisynthetic bactericidal for both intracellular & extracellular
organisms. High activity against gram positive bacteia & mycobacteria also against
some gram negative organisms like Brucella, shows activity against yeast & fungal
microorganisms when combined with amphoterecin B.It is used for treating
Rhodococcus equi and other bacterial infections in Foals- 5 mg/kg PO, 2 times daily
(in combination with erythromycin 25 mg/kg, PO, 3 times daily.; Dogs & Cats - 5
mg/kg PO, 1- 2 times daily.; For CNS fungal infections; Dogs & Cats-10-20 mg/kg PO,
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
3 times daily in combination with amphotericin B & flucytocine. Hepatotoxicity in
animals with pre-exsiting liver diseases. In horse ( IV ) CNS depression, sweating,
heamolysis anorexia. In few cases partial immunosuppression of lymphocytes. GIT
disturbances – nausea, vomition, anorexia, abdominal cramps, diarrhea &
hypersensitivity reactions are the avderse ffects. As a potent inducer of hepatic
microsomal enzymes it may enhances elimination half life of several drugS viz.
digitalis, coticosteroides etc.Synegestic effect with amphotericin B against some fungi.
Furazolidone is bacteriostatic , broad spectrum activity ( both gram positive &
negative organisms).Also active against giardia toxoplasmas. Coccidia & histomonas.
It is used for enteric infectios: Dogs – 2.2 mg/kg PO, 3 times daily for 7 days.; Cats- 4
mg/kg PO, 2 times daily for 7-10 days.; Horses- 4 mg/kg PO, 3times daily; GIT
disturbances – inappetence, nausea, vomition, anorexia, abdominal cramps, diarrhea.
And CNS effects- tremors, ataxia, convulsions, visual impirement. May be seen
Fusidic acid (Sodium fusidate) : is bacteriostatic effective only on gram-positive
bacteria such as Staph. and Corynebacterium. It is used topically for minor local skin
infections, wounds. It should not be used with quinolones, with which they are
antagonistic
Methanamine (Hexamine) : a urinary antiseptic have antibacterial activity is due to
release of formaldehyde in water. It is bacteriostatic agent but becomes cidal in acidic
urine. Active against both gram positive & negative organisms.Methamine mandalate
- Dogs – 10-20 mg/kg PO, 1-2 times daily.GI disturbances (nausea, vomiting &
diarrhea), gastritis, painful & frequent micturation, albinuria, hamaturia, cystitis, CNS
symptoms produced occasionally.Use of urinary alkanizing drugs e.g. Na bicarbonate,
carbonic anhydrase inhibitors may antagonise its action.Sulphonamides combine
chemically with hexamine in urine leads to antagonism.Concurrent use of urinary
acidifires such as ascorbic acid, methionine enhances its action.
Tiamulin: Is a semi-synthetic derivative of pleuromutilin. It is typically available for
oral use as the tiamulin base or the hydrogen fumarate salt. Tiamuli nHCl as injectable..
It is bacteriostatic against gram positive pathogens including Mycoplasma spp.,
Spirochaetes (e.g. Treponema) and obligate anaerobes. It is useed for enteric
pneumonia complex-Pigs-15 mg/kg IM, once daily for 3 days & 8.8 mg/kg PO, 3-
5days
In chickens and turkeys-reductions in water intake. Rarely, redness of the skin,
primarily over the ham, may occur in which case it is recommended that medication is
discontinued and the affected animals moved to clean pens. In oral overdose tiamulin
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
may cause transient salivation, vomiting and CNS depressions (calming effect), in
which case the drug should be removed and affected animals should be treated
symptomatically and supportively if necessary. Tiamulin should not be administered to
animals having access to feeds containing polyether ionophore antibiotics (monensin,
lasalocid, narasin, salinomycin, and maduramycin) as adverse reactions may occur.
Concomitant use with other drugs that bind to the 50S ribosomal sub-unit (e.g.
lincomycin, erythromycin, and tylosin) may lead to decreased efficacy as a result of
competition at the active site.
Virginiamycin:is bactericidal against a wide range of organisms
including staphylococci, streptococci and enterococci. It is commonly used as feed
additive Overdose may result in gastric disturbances, dyspnea, emesis, tremor and
ataxia.
Novobiocin: Spectrum mainly gram positive; Most gram negative resistant; but some
Haemophilus sp., Neisseria sp., and Proteus sp. may be susceptible.Dogs: 10 mg/kg
q8h PO; Cattle:For treatment of mastitis in dry cows:Infuse contents of one syringe
into each quarter at the time of drying off; not later than 30 days prior to calving. For
treatment of mastitis in lactating cows-using the penicillin/novobiocinproduct. Fever,
GI disturbances , rashes and blood dyscrasias after systemic use. It acts similarly to
probenecid by blocking the tubular transport of drugs. thus the elimination rates of
drugs excreted in this manner (e.g., penicillins, cephalosporins) could be decreased and
half-lives prolonged.
Mupirocin: gram positive bactericidal spectrum; is used topically for staphylococcal
and streptocococcal skin infections, wounds, burns etc
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
HANDLING OF VETEROLEGAL POISONING
CASES
B. KALAKUMAR
Generally every veterinarian is encountered with two types of cases in
poisoning of farm animals. Accidental and Malicious poisoning. The necropsy of the
animals and the rapid diagnosis is helpful in the treatment of other affected animals in
case of accidental poisoning. In case of malicious poisoning, which may turn up into
medico legal case, the identification of poison is a must to establish the cause of death.
In all poisonous cases, chemical analysis of the biological specimens is essential to
know the cause of death or illness. Therefore, every veterinarian should know the
salient points in collection and despatch of toxicological specimens to a laboratory.
History of the case is of great importance in the diagnosis of poisoning. This
includes the number of animals in the farm, number of affected, method of feeding,
regularity of feeding, recent changes in the rations or attendants, whether pastures have
been sprayed with pesticides or fertilizers, if rodenticides have been used and remnants
of the bait removed and disposed properly, storage of poisonous substances etc.
Inspection of the surroundings for empty pesticides or paint containers that are not
really empty, presence of poisonous plants in the farm environment. Also, the
possibility of industrial effluents coming in contact with grazing/watering sources
should be given thought of.
POST MORTEM: Necropsy by routine procedure is to be performed as soon as
possible after the death of animal. Examine the animal externally and note incisions
(for sui poisoning, snake bite etc.,) on the skin or mucous membranes. Examine the oral
cavity for corrosive lesions (acids/alkali) or changes in colour of mucous membrane
(nitrate, co, cyanide poisoning). As most of the toxins gain entry through gut,
examination of gut mucosa, the contents, their smell, colour and pH (acids, alkali, urea)
is a valuable guide in diagnosing toxicoses. Poisoning by salts of heavy metals results
in significant post mortem lesions but poisoning by alkaloids like strychnine produces
very feeble lesions.
The natural orifices, sub-cutaneous fat tissue, muscles, bones and teeth (in
fluorine poisoning), body cavities, and internal organs should be examined. The
stomach should be punctured rather than cut open for organoleptic examination to note
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
the character of smell. Puncture ensures greater accuracy and a longer time smell.
Some of the poisons which emit characteristic smell are: bitter almond -hydrogen
cyanide poisoning, garlic odour - phosphorus poisoning, rotten garlic or horse radish
smell - selenium, tobacco odour –nicotine, acetylene odour - zinc phosphide and
ammoniacal odour- urea.
Check the pH of the stomach contents by pH paper. Any variation in the normal
pH of the sps. being examined indicates abnormality. (In urea poisoning-alkaline pH is
observed in rumen liquor due to release of ammonia).
The colour of stomach contents also indicates the cause of poisoning. Copper
salts impart a greenish blue colour whereas picric and nitric acid impart yellow colour
to the contents. The contents of the stomach vary from traces to flakes of paints or lead
objects, grains or baits, seeds etc., like wise small and large intestine should be
examined. Blood should be examined for its colour and clotting characters. Cyanide
poisoning imparts cherry red colour, arsenic imparts rose red colour and nitrate
poisoning turns blood brown in colour. In abrus and cyanide poisoning-blood remains
fluid after death.Examination of other visceral organs should be done in relation to their
size, colour etc. eg: - spleen size is decreased and colour is changed to dark brown or
black in copper poisoning and spleen size is increased in T-2 mycotoxicoses.Lymph
nodes are swollen, haemorrhagic, oedematous and dark upon exposure to radiation.
Bone marrow becomes pale and gelatinous with yellowish tint.The description of
morphological changes should be noted clearly and absence of changes should be
notified. The most important lesions found should be underlined.
In case of small animals (poultry, small dogs, lab animals) the cadavers are sent
as it is, in case of large animals the stomach contents are collected from the vicinity of
patho anatomic changes in the gastric mucosa. If there are no changes a representative
sample is collected, but in medium sized animals the stomach tied at oesophageal and
duodenal end, intestine tied at both ends and bladder with tied ends is sent separately.
Collection of samples: A successful toxicological investigation requires appropriate
specimens, history and clinical signs, necropsy lesions and circumstantial evidences.
All the specimens are to be taken in separate containers (polythene jars/covers),
securely tied, properly labelled with particulars of date, case No., organs collected,
species, name of preservative used etc. A sample of the preservative used, brief history
of the case along with treatment given particulars should be sent. It is always preferable
to send the specimens through a special messenger. In medico legal cases, the
specimens should be sealed in the presence of a witness. The quantity for the kind of
sample to be sent is as follows.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Wholeblood:10-20ml; Serum:10-20ml;Milk:50-100ml;Urine:50-100 ml;Water: 200 ml;
Faeces : 50 g ; Feed : 0.5 - 1kg.
Mode of preservation : 1. Ice for about 72 hrs. 2. Alcohol (95% ethyl alcohol) 1 ml/g
of tissue is the ideal preservative for toxicological specimens. Formaline should never
be used as it hardens the tissue without giving scope for scraping and interferes in the
analysis. Blood and serum should be refrigerated and never frozen. A sample of the
preservative used should be sent. It is always better to have a duplicate sample stored
properly in a refrigerator for future reference Sample for analysis should include a
suspected source material; often gut contents, so that ingestion of suspected material
can be proved. Secondly, a sample of tissue (depending on tissue affinity of the
suspected poison) must be included, to prove that absorption of the poison has
occurred. It is always advisable to include a sample of liver to confirm absorption of
orally ingested poison. In survival cases the following materials may be sent for
analysis:Stomach wash, ruminal contents, vomitus, blood, urine, saliva, dung, water
and feed, suspected forage/ poisonous plant/s is the ideal samples for laboratory
analysis. Most xenobiotics are ingested. Therefore, one of the unique advantages of
analyzing gastrointestinal contents is that qualitative tests can be easily carried out in
order to determine the animal has oral access or not. Guidelines for submitting
specimen for toxicological examination is listed in Table 1.
Table 1: Toxicological specimens for laboratory examination
Sl.No. Suspected Specimen required Remarks
poison
1. HCN/Cyanide Forage / ingesta, whole Rush samples frozen in air
blood tight bottle to laboratory
Liver GIT/ Stomach contents in 1%
mercuric chloride is ideal
2. Organochlorine Cerebrum, fat, liver, Use only glass containers,
pesticides/ kidney, ingesta
Avoid aluminum foil for
Chlorinated wrapping specimens
hydrocarbons
3. Organophosphates Feed, ingesta, liver, urine -
&Carbamates
4. Znic phosphide Liver, kidney, gastric -
contents
5. Nitrate/nitrite Forage, ingesta, body Ingesta in chloroform or
fluids, Serum . Ocular fluid formalin filled air tight
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
water samples container
6. Oxalates Fresh forage, kidneys Fix in formalin
7. Ammonia/Urea Whole blood or serum, Frozen / 1-2 drops of
urine Rumen contents saturated solution of
mercuric chloride
8. Heavy metals(Lead, Kidney, whole blood, liver Heparinized, do not use
Mercury) and urine EDTA
9. Mycotoxins Forages, feed sample, liver, Use airtight containers or
kidney, brain plastic bags. Cloth bags for
dry feeds
Note: Always send a sample of preservative if used in separate container with
proper label *****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
GENERAL LINE OF TREATMENT OF POISONINGS
M. VIJAY KUMAR
In majority of cases of poisonings, treatment with an antidote is not
possible, instead prompt medical intervention to improve the condition of the animal
can ensure its survival. These practices focus on promoting the removal of the poison
or neutralizing it, whilst maintaining the vital functions of the animal.
Decontamination of the skin: Some substance (hydrocarbons, acids, alkalis,
agrochemicals, etc.) may, as a result of an accident or a spillage, contaminate the
feathers or fur of animals. In general it is important that in such circumstances the
following are undertaken:
• Epidermal structures (wings, nails, claws, feathers, fur) should be cleaned with the
greatest care, paying particular attention to areas such as the ears, between toes, etc.
• Avoid licking and ingestion of the poison, and to limit cutaneous absorption.Use
soapy water (preferably a soap with a low pH), rinsing repeatedly with copious tap
water
• Dry carefully and thoroughly (e.g. with a hair dryer)The following must never be
used: organic solvents (alcohol, white spirit, etc.) or oily substances which may
actually increase percutaneous absorption of the toxin.
• Do not rub the area vigorously; cleaning and drying must be gentle but thorough
Gastric emptying: Emetics:Use emetics if ingestion has taken place within the
preceding 2-3 hours. Never induce vomiting in following circumstances: If caustics or
hydrocarbons have been ingested; If the condition of the animal does not allow such
treatment, specifically if the patient is presenting with convulsions (unless controlled),
coma or severe respiratory difficulties; this avoids any secondary complications due to
aspiration.; in pregnancy and ingestion of slow releasing drug formulations.
Apomorphine: a central depressive effect and the possibility of cardio-toxicity
(arrhythmias) -Dogs: 0.05-0.1 mg/kg s.c or im; contraindicated in cats or pigs;
Xylazine: acts within 10-20 minutes; 0.25-0.5 ml of a 2% sol.,s.c.Ipecachuana (10%
syrup) for dogs and cats: Acts in 20-30 minutes; orally, 10-20 ml for a dog, 2-5 ml for a
cat administered in a phased manner. Alternatives: Sodium chloride (salt), p.o, 1-3
teaspoons in warm water; Hydrogen peroxide, by mouth, 1 ml/kg; Copper sulphate is
not recommended as it is an irritant and facilitates the absorption of poisons. Preferred
in pigs (4% solution, max: 60ml,p.o)
Gastric lavage in dogs is indicated: if ingestion has taken place in the preceding 2-4
hours and on anaesthetized animals with endotracheal intubation. Use 10 ml/kg of an
isotonic solution of sodium chloride (occasionally sodium bicarbonate); repeat the
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
procedure until the washout fluids is clear. Emergency gastrotomy with manual
emptying may be necessary in some cases of plant poisoning or indigestible materials
(such as plastic, polyurethane foam).
Purgatives: Never use irritant purgatives and oil-based purgatives as they facilitate
absorption. Sodium sulphate, magnesium sulphate are preferred; PO, as enema, using
solutions of various strengths (make up to 20%):Small animals : 2-25 g, Large animals:
100-200 g (max: 300 – 400g); Liquid paraffin (mineral oil), by mouth:Dogs: 5-15ml,
Cats: 2-6ml
Diuretics: Increase glomerular filtration by instituting a forced diuresis or osmotic
diuresis: 5% glucose solution, by slow IV infusion: Large animals: 2-5 ml/kg
per 24h, Small animals: 5-20 ml/kg per 24hr; 10% glucose solution, by slow IV
infusion: Large animals: 0.5-1 ml/kg per 24 h, Small animals: 1-2 ml/kg per 24
hr; 10% mannitol solution, by IV infusion:Large animals: 1-2 ml/kg per 24 h, Small
animals: 2 ml/kg per 24 hr; :Frusemide (im or iv), Large animals: 0.5-1 mg/kg, Small
animals: 2.5-5 mg/kg
Reduce tubular reabsorption by modifying urinary pH.: Forced acid diuresis to
eliminate weak bases can be done by:Ammonium chloride, PO: Large animals: 20-40
g, Small animals: 2-5 g; Arginine chloride, im, or iv-Large animals: 7-10 g, Small
animals: 0.1-0.2 g/kg; Ascorbic acid, iv, all species: 40 mg/kg
Forced alkaline diuresis to eliminate weak acids: Sodium bicarbonate, 1.4%w/v, iv
infusion, Large animals: 2-4 ml/kg per 24 hr; Small animals: by regular monitoring of
the acid – base balance (number of ml to perfuse = base deficit (in mmol) x 0.6 x body
wt in (kg)ringer’s lactate, IV: all species: 5-10 ml/kg per hr; Use a diuretic such as
acetazolamide
Dialysis: In cats and dogs peritoneal dialysis with an appropriate dialysate 20-25
ml/kg is suggested. Repeat the procedure several Times as necessary. Very effective in
case of renal failure/renotoxicity. Commercial preparations meant for human use can be
employed
Neutralization of poisons with in the gastrointestinal tract
Adsorbents Activated vegetable charcoal (fine medicinal charcoal).-the most effective
and most highly polyvalent adsorbents. They can be administered preferably as a
suspension in water, several minutes to 24 hours after ingestion, if possible before any
emetic. Large animals: 250-500 g, Small animals: 5-50 g; Other adsorbents:
Magnesium oxide (magnesia), Kaolin, Universal antidote (vegetable charcoal 10g+
magnesia 5g + kaolin 5g + tannin 5g with water added up to 200 ml)
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
General chemical antidotes: Substances which form a complex or insoluble
precipitate with poisons and neutralize them in the gastrointestinal tract. The effects
are often limited and debatable. This category includes: Water-containing albumens
(proteins which are capable of forming insoluble complexes with heavy metals and
which neutralize acids and bases); Tannins (these precipitate heavy metals aluminum,
lead, silver and some alkaloids) ; Less useful against copper, mercury and nicotine),
Lugol’s iodine can partially precipitate heavy metals like Pb, Hg, Ag and Strychnine.
and Ferric hydrate .
Milk is commonly believed to act as the best general antidote; in fact, milk promotes
the absorption of liposoluble poisons. A cardinal rule, therefore, is “never administer
milk”.
Additional treatment measures: vary according to the symptoms observed, important
agents used to support vital functions (respiration and circulation) are: Doxapram: A
respiratory stimulant, Dog/Cat: 2 mg/kg, iv, repeat as required ; Caffeine and
theophylline: Cardiovascular and respiratory stimulants, with diuretic action. Dosage:
100-250 mg iv, im, hypodermally or as required and Nikethamide:. Dog: 22-44 mg/kg,
im, iv.
Rational Use of Charcoal : Charcoal is ineffective against cyanide. It can adsorb
vitamins/minerals and continued use may prove to be harmful. Make slurry of the
activated charcoal using lukewarm water. 2-8 g/kg should be given in a concentration
of 1g/5-10ml water by a stomach tube using either a funnel or a large syringe.
Administer a cathartic (sodium sulphate or magnesium sulphate) 30 minutes after the
administration of charcoal. In pet animals this technique can be modified if the charcoal
is used in conjunction with an emetic or gastric lavage (Normal saline: 10 ml/kg) with
endotracheal intubation.
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
CLINICAL MANAGEMENT OF POISONINGS OF
VETERINARY IMPORTANCE
M.VIJAY KUMAR
In veterinary field toxicities are often found as a result of ingestion of poisonous
substances while grazing or through water. Suspicion of poisoning is also aroused when
illness occurs in a number of previously healthy animals, all affected at a same time,
sharing the same signs, necropsy findings, to the same degree of severity. Poisoning in
most occasions is accidental in farm animals, but may occasionally be deliberate .
SOURCE OF POISONINGS
1. Insecticides:Insecticides are the major source of poisonings in livestock.. Most of
the insecticides are basically ‘neurotoxic’, hence they may share some of the clinical
signs, Insecticides can be classified in to following categories: 1. Organochlorines: Eg:
Aldrin, Endosulfan, Lindane, Dicofol etc 2. Oraganophosphates. Eg: Acephate,
Malathion, Parathion, Methyl parathion, Dimethoate, Phosphamidon,, Chlorpyriphos,
Chlorfenvinphos, Monocrotophos etc 3. Carbamates. Eg: Carbaryl, Metacil, Dimetan,
Pyramat etc. 4. Pyrethroids (Synthetic): Deltamethrin, Cypermethrin,Permethrin,
Allerthrin etc. 5. Miscellaneous: Chloro-nicotinic acid (nicotine), Arsenic
compounds,Captan
Organochlorines: By virtue of their high lipid solubility these agents can enter the
neuronal membrane with ease and therefore interfere with normal functioning of the
nerve membrane sodium channel. The clinical signs of toxicity can be broadly
categorized in to:
Behavioural signs - Anxiety, aggressiveness, abnormal posturing, maniac symptoms
like jumping over inanimate objects, wall climbing etc. Neurological signs –
Hypersensitive to external stimuli, spasm and twitching of fre-and hind quarter
muscles, fascicualtions of facial and eye lid muscles and variations in body temperature
(subnormal temperature to hyperthermia, up to 116°F). Autonomic effects: Marked
salivation (normally thick/ sticky saliva), Mydriasis, frequent urination, defecation and
lacrimation.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Organophosphates: Clinical essentially appears as a result of irreversible inhibition of
AChE, causing accumulation of acetylcholine in the neuro-muscular junction leading to
‘spastic paralyses. The cause of death is due to respiratory collapse. Muscaranic signs
(miosis, watery, drooling saliva, urination, colic and /or defecation, lacrimation are the
common signs followed by nicotinic effects (muscle fasciculations, tremors) and
C.N.S effects( ataxia, convulsions and later depression of respiratory and circulatory
centers). Hypotension, bradycardia and dyspnoea are observed in poisoned animals.
Carbamates: The inhibition of AChE enzyme by carbamates is ‘reversible’, therefore,
on most occasions animals recovers on own unless ingested large quantity of pesticide.
Synthetic pyrethroids: Although these compound process low insect: mammalian
toxicity ratio, treatment of poisoned animals may be a difficult task probably because
of multiple mechanisms involved in toxicity and variations among pyrethroid class
(type-I & type-II). Hypersalivation, lacrimation, mucoid nasal discharge, excitement,
in-coordination, extension of limbs are observed in deltamethrin toxicity in buffalo
calves. Few pyrethroids also cause contact dermatitis.
2. Rodenticides:.
Anticoagulant rodenticides: These include warfarin (less used now a days) and second
generation anticoagulant rodenticides viz: Bromadiolone , brodifucoum. The main
source of poisoning is the ingestion of residues of the rodenticides or baits intended
for killing rodents.. The poor coagulation mechanism cause massive internal
haemorrhages over aperiod of time. Normally after period of about 2-5 days clinical
signs appears and these include anorexia, pulmonary coughing (epitaxis,
dyspnoea),hypothermia, haematuria, stiffness of hind quarters and sudden death.
Internal haemorrhage, blood in the GIT(gastroenteritis), haemopericardium and
menigeal/cerebral bleeding and haemorrhages in joints are the pathological lesions one
can observe during necropsy. The affected animals should be shifted to quiet and warm
place and the line of treatment include Vitamin-K1 in physiological saline (Vitamin-K3
not recommended) and cardio-vascular support.
Zinc phosphide/ Aluminium phosphide: It is one of the cheapest and quite effective
rodenticide. Monogastric species are more sensitive rather than ruminants. Clinical
signs include anorexia, lethargy, abdominal pain, bloat (in ruminants), deep respiration,
ataxia, prostration and dyspnoea, gasping, convulsions and death. Post-mortum lesions
include pulmonary congestion, edema, sub-pleural haemorrhages, congestion of liver
and kidneys. Acetylene odour may be detected in stomach. No specific treatment is
possible, however symptomatic and supportive care maybe given. Gastric lavage with
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
5% Sodium bicarbonate, Calcium boro-gluconate injection, anticonvulsants and
measures to prevent shock can be undertaken as a life saving measure.
3. Herbicides & Fungicides:Dinitro-compounds: Dinitrophenol, DNP; dinitro-orthro
cresol, DNOC); are some of the commonly used as herbicides. Accidental ingestion of
foliage sprayed with these compounds may lead to toxicity in ruminants. These
compounds induce methaemoglobinemia (intravascular haemolysis),hyperthermia, dark
coloured blood and gastroenteritis. Rapid onset of rigor mortis, yellowish-green
coloured tissues/urine may be recorded during post mortem examination.
Zeneb & Thiram: Zeneb (Zinc-ethylene dithiocarbonate) and Thiram (Tetra-methyl
thiuron sulfide) are the two most commonly used fungicides in agricultural practice.
Although acute poisonings is less likely to observe in field, chronic toxicities may get
unnoticed. Zeneb can induce thyroid hyperplasia, hypothyroidism, degenerative
changes in myocardial, skeletal tissues and depletion of testicular germ cells. Thiram
exposure may cause conjunctivitis, rhinitis, bronchitis, abortion (ewes) and teratogenic
effects.
4. Hydrocyanic acid (HCN) /Cyanide:The most prevalent form of HCN poisoning in
livestock is caused by various cyanogeneetc plants capable of producing hydrocyanic
acid. Such plants contain cyanogenetic glucocides (dhurrin in sorghum, amygdalin in
bitter almond etc.) which hydrolyzed in to HCN in ruminants. Wilted, drought affected,
injured (chopping, rinsing etc.) plants are more dangerous than fresh plants because of
their preformed HCN. Any plants possessing 20mg HCN per 100gm (wet wt.) may
serve as potential source of HCN poisoning. Other source of cyanide poisonings are:
industrial grade Na/K and calcium cyanide (also fertilizer) and effluents from vicinity
of electroplating/metal coating industries workshop.
Hyperoxygention of blood would lead to cherry red/ bright red colour of venous
blood . Intoxicated animals shows salivation (frothy), bradypnoea, mydriasis,
ataxia,tremors, epileptiform scizure, cardiac arrhythmia and clonic-tonic convulsions.
Invariably loss of conscious, coma and death with several jerky and convulsive
movements if poisoned animals are not attended with in a with in 1 hour after the
appearance of clinical initial signs. Odour of the breath is ammonical/ bitter almond
due to benzaldehyde production (often bloating, regurgitation is observed). Opening of
rumen during post-mortem examination impart similar odour. Animals suspected for
HCN poisoning must be differentiated from nitrite and other sr milar agents before
initiating antidote therapy . In addition to antidotes, per oral administration of Cobalt
chloride(10 mg/kg)and glucose is also indicated.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
5. Nitrate/Nitrite:Drought is one of the root causes of nitrite toxicity in
cattle/buffaloes. Nitrates are reduced to nitrite in ruminates. Otherwise, pigs are most
sensitive species for nitrate toxicity. Contamination of drinking water with sewage,
several plants species (Amarantus sps,Palak etc.), plants grown in highly acidic soil,
water logging and rich nitrated fields / effluents zone, deep well water or pond water
originated from leaching of top soil (after -nitrate fertilizer application) are some of the
common source of nitrite poisonings. Water soaked/entry of moisture may also render
paddy hays/ corn in to nitrite rich within 18-22 hours. Frequent application of fields
with non-toxic weed killer 2,4-D and nitratic fertilizer favour accumulation of nitrtes in
plants. Any forage that contains over 1.5% nitrate (expressed as pot. nitrite) is
considered relatively unsafe for livestock and should be fed with extreme caution.
Nitrite ions induce meth-haemoglobenaemia as well as marked vasodilatation. Clinical
signs include cyanosis, staggering gait, muscular tremors, rapid pulse, dyspnoea and
dilated pupil. Opisthotonus, polyurea, chocolate brown colour of the blood and
cyanotic mucous membranes are the characteristic features of nitrite toxicity. Untreated
animals die with out a struggle. Reducing agents like Methylene blue or Ascorbic acid
are the antidotes (see table 2 for details). Mineral oil or mucilaginous substances and
diluted vinegar (4-5 lt. in cold water, per os) must be administered to counter GI
irritation and further reduction of nitrates in the rumen respectively. Cardiovascular
support (vasoconstrictor); and stimulants to counter prostration.
6. Poisonous plants: Toxicities/ death due to ingestion of poisonous plants are also
often being the etiology of poisoning in the farm animals. Commonly with plant
poisonings there are perplexing epidemiological features. For example, animal already
grazing in the dangerous field are often unaffected while recently introduced may be
poisoned. Drought, starved, ailing from pica, hungry, ravenous animals, curiously
excited animals (often do not eat), and young animals less discriminate plants with
different texture (attraction). Poisonous plants often show geographical limitations in
their distribution, particularly industrial enterprises may create ‘poison hazard’ in local
areas (Ipomea carnea, Amaranthus spinosus) and certain agricultural practices / soil
type may also pose toxicities (eg. Nitrite, Selenium). Severe drought followed by
rain/moisture/humid atmosphere favour accumulation nitrite in many plants. Similarly
re-emergence of fresh leaves following harvesting also contains dangerous levels of
HCN.
Essentially the source of plant poisoning can be classified into: a. naturally occurring b.
Commercial crops/byproducts and c. Conventional and non-conventional fodders.
Immature sorghum, maize, flax (linseed); Manihot esculenta (tapioca) newly emerging
bamboo shoots and rubber leaves are the common source of HCN poisonings.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Accidental ingestion of castor bean, rotten beat roots, adult nicotine leaves,Mimosa
invisa (used to increase nitrogen fixation in soil) may become fatal.. Plants or foliage
belonging to Brassicaceae sps.(Cruciferae) family i.e kale, rape,turnip,
cabbage,reddish plants and mustard seeds or meal may elicit severe toxicities in
animals when fed /ingested large quantity due to the presence of glucosinolates in such
plants..Digestive disturbance(enteritis),goiter polioencephalomalacia (rape blindness),
pulmonary emphysema are the sequelae. Bloat, photosensitization is also observed.
Affected animals are to be treated symptomatically.
Feeding of urea treated straws in excess/or fed to un-acclimatized animals may lead to
urea poisoning, long term feeding of subabul may lead to hypothyrodism and feeding
of fungus infested straws (sorghum, paddy or leguminous fodders) may pose threat of
mycotoxicosis when fed relatively for a long period. Ficus tsjhela (Karnataka-Kerala
boarder, Western Ghats); Acccia leucopholea (HCN), Amaranthus spinosus (nitrite);
Jatropa curcus (purging nut); Crotalaria juncia (hepatotoxic pyrrolizidine alkaloids:
monocrotaline);Flax(linseed, HCN); Ipomea carnea (LSD alkaloid like effects, also
source of nitrite and cause photosensitization). Strychnous nux-vomica (coastal
Karnataka); Abrus precatorius (Gulaganji); marking nut, Calitropis gigantica (yakka),
croton oil and Yellow oleander are also some of the plant source of accidental
poisonings and/or recorded in case of malicious poisoning in animals.
Antidotes and supportive treatments for common poisonings in large animals
Poison/toxicity Antidote/ treatment Dosage and method of treatment
Hydrocyanic acid Sodium nitrite followed Administer 1% sodium nitrite @ 15-
(HCN) /Cyanide by Sodium thiosulfate 25mg/kg,i.v followed by 25% sodium
thiosulphate @ 1.25gm , slow i.v
Na nitrite + Na thiosulfateCattle:
3gm + 15gm in 20ml water, s.c;
Sheep/goats: 2gm+5gm in 15ml
water,s.c. Cobalt chloride @10.2
mg/kg, per os; Approx. 4 lt. vinegar in
10-20lt. cold water; A large dose of
vitamin B12 and anticonvulsants, if
necessary. Give cobalt chloride
10mg/kg per-orally. Fluid therapy with
dextrose-saline is ideal
Nitrate/nitrite Methylene blue 1% Methylene blue @ 8.8mg/kg, i.v
and repeat 30 min later and if
Or necessary administer at 6-8hr. interval
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Ascorbic acid Broad spectrum antibiotics intra-
ruminally; Administer 8-10L cold
water and give osmotic purgatives
Treat for hypotension/shock,
(vasoconstrictors like 1:1000, 0.5 ml
adrenaline, slow iv); Blood
transfusion, if possible
Heavy metals British anti- BAL: 3mg/kg as 5% mixture of 10%
Lewisite(BAL) benzyl benzoate in mineral oil. Give
(Arsenic,antimony, deep i.m injection every 4hr. on first
mercury) two days, every 6hr. on third day and
then b.i.d for next 10 days. In cattle
Arsenic/Mercurial
and horse sodium thiosulfate can also
insecticides)
be used @ 8-10gram in the form of 10-
20%solution (i.v) or 20-30gram per-
orally in 300ml water.
Arsenic poisoning
d-penicillamine Fluid therapy and other supportive
treatment as required. Administer @
30-40mg ,i..v + 60-80mg/kg; P.O,
b.i.d or t.i.d for 3-4 days
Urea No antidote Administer 20-30lt. water and drench
4-6lt. 5 % acetic acid ;
Reduce the rumen pH Anticonvulsants, if required
Strychnine Phenobarbital sodium Phenobarbitone sodium,30mg/kg,i.v
(Strychnous- nux Chloral hydrate Chloral hydrate @ 5g/45 kg, i.v
vomica)
Drench tannic acid and then purgative
Rest the animal in cool, noise free & in
dark room after a dose of purgative
Lead Calcium disodium EDTA Make 6.6% solution and administer @
73 mg/kg,i.v (repeat or two treatment
daily for 3 days if required).
Combined thrapy with thiamine HCl
@2-4mg/kg/day, s.c is more effective,
Anticonvulsants, if required
Warfarine Vitamin- K1 Vitamin-K1: 300-500mg, S.C,every 4-
6hr.Blood transfusion transfusion @
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Bromodiolone 20ml/kg or plasma @ 9ml/kg body wt;
Sedatives/tranquilizer
Pyrethroids No specific antidote, but Diazepam: 0.5-2 mg/kg, i.vAtropine
SO4 as required
(Deltamethrin, Diazepam HCl +
Atropine SO4 Activated charcoal (1-2kg), P.O Fluid
Cypermethrin etc.) therapy
Carbamate insecticides Atropine sulphate 0.25mg-0.5mg/kg,give ¼ intravenously
and remaining ¾ by intra-muscular or
sub-cutaneous route
Organophosphates Atropine sulphate + Atropinization: 0.25mg-0.5mg/kg,give
¼ i.v,remaining ¾ by i.m or s.c for
2-PAM every 3-6 hours. Observe for papillary
dilatation and recovery symptoms and
Or
continue treatment as required.
DAM(diacetyl
2-PAM: 20%solution @ 25-
-monoxime)
50mg/kg,i.v or intra-muscualrly,
Activated charcoal,P.O
Fluid therapy and supportive care
Organochorines Pentobarbitone sodium 30mg/kg,i.v and supportive care
( D.D.T;, B.H.C & Or Chloral hydrate
endosulphan etc.,) 5g/45 kg ,i.v and supportive care
Dinitro-herbicides In ruminants only: Treat Methylene blue: 2-4%,8-10mg/kg,i.v
(Dinitro-orthocresol- for Methaemoglobinemia every 8hr. Or Ascorbic
DNOC & with methylene blue acid: 5-10mg/kg,i.v; every8hr. for first
Dinitrophenol-DNP) 24-48hr.Note: Do not give antipyretics
Or to control hyperthermia. Administer
saline purgatives. Fluid therapy with
Ascorbic acid
DNS
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
CARE AND MANAGEMENT OF CRITICAL PATIENTS IN
CLINICS
VIVEK .R. KASARALIKAR
Critically ill patient is special challenge to the clinician because the underline
problem is not evident for about 24 to 48 hours after initial presentation. Expeditious
therapy in right time can be life saving, whereas delayed adequate therapy may be
ineffective therapeutic failure. Most common clinical conditions in ambulatory patients
are trauma with internal/ external hemorrhage, poisoning and post surgical
complication. In fact, specialized care of emergent patient begins with initial phone call
from the owner and instructions to be given regarding first aid and transport
procedures. Level of consciousness, breathing pattern and external hemorrhage should
be enquired on priority.
The important first aid measures are:
• Immobility and transport on firm flat surface
• Mouth to nose resuscitation in critical patient which is unconscious and not
breathing (Ten to twelve times per minute)
• Pulsating arterial bleeding is controlled by digital pressure and pressure bandage
• Penetrating foreign objects should be left in place till specialized help is available
• Head elevated by 200 in altered mental status after head or spinal injury
Evaluation and initial treatment: Three important assessment criterion in
emergency patients are A, B and C by evaluating certain parameters .
A – Airway: Airway patency should be evaluated on priority. Noisy breathing
without need of stethoscope suggests Large airway problem e.g. trachea and
bronchus, whereas, inspiratory dyspnoea implies extra-thoracic airway compromise.
Loud expiratory sounds reflect towards pathology of intra-thoracic airway including
bronchioles and lung parenchyma.
B – Breathing: Sequence of respiratory compromise is increased in respiratory rate
initially, followed by change in respiratory pattern. Laboured open mouth breathing
with development of cyanosis suggests significant compromised pulmonary function.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
In both the above conditions, immediate Oxygen administration is the priority. Intra-
nasal catheter is the best choice for compromised breathing patients, whereas slash
tracheotomy with endotracheal intubation is preferred in unconscious and apneic
patients (Nasal Oxygen flow rate should be kept at 50 – 100 ml/kg/min).
C– Circulation: Hemodynamic and cellular changes that occur as a result of
abnormality in circulation is referred as shock or peripheral circulatory failure.; is
clinically classified in to four main categories.
Hypovolemic: occurs due to atleast 15-25 % t deficit in circulatory blood volume
Cardiogenic shock: occurs due to failure of heart to pump requisite quantity of
blood in to circulation
Distributive shock: due to impaired distribution of circulatory blood volume as a
result of peripheral vasodialatation
Septic shock: This is endotoxin mediated shock
Therapeutic management of critically ill patient:
1. Cardio-pulmonary Resuscitation (CPR):Hallmarks of Cardio-pulmonary arrest are
a) stage of apnea with cyanosis of visible mucous membranes b) absence of
palpable pulse c) absence of heart sounds and d) dilatation of pupils
Guidelines for Cardio-pulmonary resuscitation
a) Positioning of animal:Lateral recumbency on small animal examination table is
optimal position in small sized dogs (< 7 kgs), whereas dorsal recumbency is
preferred for large sized dogs.
b) Resuscitation:Chest compression coupled with mouth to nose ventilation should
be performed in patients in apneic stage.Compression rate should be 60 to 120 per
minute and the compression – ventilation ratio should be 15:2. It means for every
15 compressions 2 cycles of ventilation should be performed.
2. Management of shock: Assessment of shock is governed by these parameters
• Pale to cyanotic mucous membranes
• Tachycardia with weak pulse
• Significant fall in Systolic blood pressure (Below 60 mm of Hg)
• Central Venous Pressure (CVP) less than 5 mm of H2O
• Elevated level of Blood lactate (> 80 mg/dl)
• Significant increase in Capillary Refill Time (CRT)
Therapeutic management: Emphasis should be given to
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Fluid therapy:The main aim of fluid therapy is to restore circulation and improve
the tissue perfusion. Choice between crystalloid and colloidal solutions should be
determined. Crystalloid supplements fluid along with electrolytes, whereas colloidal
solutions expand the plasma volume.Commonly used colloidal solutions are:
Dextran 70, Hexastarch,Gelatin polymers, Frozen plasma, Packed cell component.
Commonly used crystalloids are: Normal Saline, Lactated Ringer’s solution,
Dextrose Normal Saline, 7.5 % Normal saline and Hypertonic dextrose solution
Corticosteroids:Stabilization of cell membrane, blocking of arachidonic acid
metabolism and gluconeogenesis are few important roles of corticosteroids in the
treatment of shock
Cyclo-oxygenase inhibitors:These decrease the prostaglandin synthesis and other
vaso-active amines.Eg; Flunixin Meglumin( 0.25 mg/kg); Ketoprofen(0.5- 2.2 mg/kg)
Antibiotic therapy in septic shock: Broad spectrum antibiotic therapy has
additional advantage in endotoxin related shock. Anti-bacterials with synergistic action
are also preferred in septic shock. III to IV generation ceophalosporin like cefoperazone,
ceftrioxone and cefixim are frequently used in small animal practice.
Control of hemorrhage and blood transfusion: Antifibrinolytic drugs are
preferred to counteract extensive hemorrhage. PAMBA (Para amino methyl benzoic
acid), EACA (Epsilon amino caproic acid) and Botropase have fast styptic activity
Alpha Adrenergic agonist: These drugs help in improving cardiac output and
thereby improve tissue perfusion. Dopamine used @ 5 – 10 µg/kg/min as constant
infusion has positive ionotropic effect and increase the systolic pressure.
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
MANAGEMENT OF MYCOTOXINS AND ZOOTOXINS OF
VETERINARY IMPORTANCE
M.VIJAY KUMAR
Mycotoxins are the toxic metabolites released by moulds under certain
conditions conducive for their growth. Acute or chronic toxicoses can result from
exposure to feed or bedding contaminated with toxins that may be produced during
growth of various saprophytic or phytopathogenic fungi or molds on cereals, hay,
straw, pastures, or any other fodder. The principles that characterize mycotoxic
diseases: the cause may not be immediately identified; they are not transmissible from
one animal to another; treatment with drugs or antibiotics has little effect on the course
of the disease; outbreaks are usually seasonal because particular climatic sequences
may favor fungal growth and toxin production and study indicates specific association
with a particular feed.
There are various types of mycotoxins and are classified as follows. Based on the
causative organism: Aflatoxins - Aspergillus flavus, A. parasiticus.;Rubratoxins -
Penicillium rubrum, P.purpurogenum.; T-2 toxins - Fusarium sp. F.gramaenareum
and F. roseum.; Ergotoxins – Claviceps purpurea and C. paspali.Among these most
common are aflatoxins. Aspergillus moulds grow rapidly when the moisture is
<15%and the temperature is 24-25ºC.They commonly affect GNC, CSC, coconut cake,
sunflower cake, wheat, sorghum, millets, soybean, peas and almonds.
Susceptibility:Ducks, rabbits, dogs, pigs, calves, chicken, cows, quail and sheep are
susceptible in the order of preference. Broilers are more susceptible than layers. Calves
are more susceptible than adult dairy cattle. Maximum allowable conc. in dairy cattle is
20 ppb (0.02 ppm)Depending on fluorescence aflatoxins are classified into B1, B2, and
G1, G2. B1 is most toxic and need to be converted into its active metabolites.Toxicity is
through ingestion of aflatoxin-contaminated feed. Aflatoxins are not accumulated to
any appreciable extent by animal tissues with the exception of milk.
Signs:Acute - sudden death or anorexia, depression, dyspnoea, coughing, nasal
discharge, anaemia, epistaxis, bloody faeces, possible convulsions and death. Subacute
- jaundice, hypoprothrombinemia, haematomas and haemorrhagic enteritis. Chronic -
decreased feed efficiency, decreased productivity and weight gain, rough hair coat,
anaemia, enlarged abdomen, mild jaundice, depression and anorexia. Abortions may
occur.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Postmortem Lesions: Wide spread heamorhages,Icterus,Gastroenteritis,Hepatic
necrosis,Massive centrilobular necrosis,fibrosis of bile duct,Enlarged
liver,Hydrothorax, Ascites,Oedema of Gall bladder wall,Pericellular cirrhosis
Diagnosis: based on History,Clinical signs,PM findings,Detection of Aflatoxin M1 in
milk & urine,liver, kidney,Serum liver enzymes SGOT,SGPT,ALP elevated,Reduced
prothrombin activity,Hyperbilerubinemia,Tlc,HPLC,RIA,ELISA
Differential diagnosis: Warfarin (haemorrhages), coal tar (mottling of liver)
Copper poisoning (haemoglobinuria, hemolysis); Pyrrozolidine alkaloids
(present in plants), CCl4, blue-green algae, crotalaria are hepatotoxic.
Treatment: 1. Avoidance of contaminated feed. 2. Hydrated sodium calcium alumino
silicate (HSCAS) adsorb aflatoxins @5kg /ton 3. Stanozolol (2 mg / kg) I/M decreases
hepatic necrosis 4. Oxytetracycline (10mg / kg) I/M decreases hepatic necrosis.( Never
administer oxytetracycline and stanzolol combination, they are mutually antagonistic)
5. Activated charcoal 6.7 mg / Kg I/R as 30% W/V slurry in M/15, PH 7 PBS(Along
with charcoal,stanzolol/oxytetracycline(any one) ) 6. GSH Precursors
Cysteine,methionine @2.2mg/kgi/p 7. Multi vitamins Like E,K & Selenium 8. Feeding
easily digestible and low fat diet containing adequate protein
Sample collection : Samples can be taken at various stages:growing crops or during
transport or storage. Whenever possible, samples should be taken after particulate size
has been reduced (Ex: by shelling or grinding) and soon after blending has occurred (as
in harvesting, loading, or grinding).Most effective if small samples are taken at
periodic, predetermined intervals from a moving stream of grain or feed. These
individual stream samples should be combined and mixed thoroughly, after which a
subsample of 10 lb (4.5 kg) should be taken.. A suggested method of probe sampling is
to sample at 5 locations, each 1 ft (30 cm) from the periphery of a bin, plus once in the
center. This should be done for each 6 ft (2 m) of bin depth. Thus, taller bins would
require more samples, and the total weight should be >10kg.
Dry samples are preferable for transport and storage. Samples should be dried at 176-
194°F (80-90°C) for > 3 hr to reduce moisture to 12-13%. If mold studies are to be
done, drying at 140°F (60°C) for 6-12 hr should preserve fungal activity.Containers
should be appropriate for the nature of the sample. For dried samples, paper or cloth
bags are recommended. Plastic bags should be avoided unless grain is dried thoroughly.
Plastic bags are useful for high-moisture samples only if refrigeration, freezing, or
chemicals are used to retard mold growth during transport and storage. Once a sample
has been cooled or frozen, warming may induce condensation and allow mold growth.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Zootoxins :Out of 236 species of snakes in India, only 50 are venomous, However, the
common poisonous snakes of India that man and animal come into contact, are : Cobra,
Krait, Russel’s viper and Sea scaled viper, Apart from these, the other venomous
snakes found in India includes Sea snakes, Pit viper and King cobra.. In animals, many
a time incidence of snakes bite is near leg region and nostrils.
Sensitivity: Horse>Man>Sheep>Cattle>Goat>Dog>Pig>Cat
Venom composition: The venom compositions vary significantly among various class
of poisonous snakes. Therefore, the course of toxicity as well as well as cause of
death will be different, and obviously therapeutic approach will also vary. On
most occasions, the identification of snake is not available or doubtful. The
nature of toxicity of poisonous snakes are: Elapidae: Cobra , King Cobra, Krait-
Neurotioxic; Viparidae: Russel viper- Haemotoxic; Crotalidae: Pit Viper-
Neutrotoxic Haemotoxic. All the bites from venomous snakes do not lead to
death due to “dry bites” which means that no venom was injected. But, some
snake venoms (krait) do not have immediate effect even in a bad bite, it is wise
to give veterinary/medical care.
Cobra:. identified by their “defence display” by spreading their long bones to their
famous hood. ; are most active at dust, having along the wedges of agricultural fields in
search of rats/mice. For this reason they live mostly in cultivated area.. The cobra
venom is rich in enzymes, cardiotoxic, neurotoxic factors. The cobra venom is rich in
enzyme acetylcholinesterase. Therefore, rapid depletion of acetylcholine (ACh) at
neuromuscular junction occurs following envenomation. This leads to “muscular
paralysis” (flacid paralysis). In addition to it, the alpha-neurotoxin is a powerful
cholinoceptor blocker (nicotinic receptors). These factors hinder the function of
muscles involved in respiration and consequently death occurs due to “respiratory
paralysis”. It is important to identify the “big four” dangerous snakes. At first sight
cobra looks like a non-venomous rat snake, but, remember that the rat snake has a
pointed head and larger eyes and it can run faster.
Krait: The common krait has bluish-bluck body with white cross bands and the head is
short and blunt. Kraits venom is 10 times as powerful as that of the cobra and of all the
Asian snakes its venom is the most toxic (neurotoxic). Kraits are noctoural. They are
active at night and rest during the day. They are found throughout India and live mostly
in sandy soil in rat burrows. Their favarite hiding places are piles of wood (on bricks
which provide many pray to shelter in. They are canibalistic- eat snakes, rats, lizards
and birds. Famale lays eggs (10-15) and stays with them until hatch.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Russel viper: is a fat and bulky snake, but it can move with surprising speed when in
danger. Its regular chain-like pattern and flat arrow shaped head make it easy to
recognise. Its fangs are along and curved.. Venom is rich in proteolytic enzymes,
hemolytic factors.
Pit vipers: are forest snakes and feed on frogs and lizards. Commonly found in coffee
and tea plantations in India. Pit vipes have a small “pits” between nostrils and eyes.
They are heat sensitive and can detect change in temperature when warm blooded
animal comes near. Venom is not powerful and seldom results in death.
First-Aid treatment: The first aim, in case of cobra/krait bite is to retard the
absorption of venom from the site of bite. ;done by applying a torniquet, provided site
of bite is suitable for that. Do not disturb/ or/excite the animal with little care incise the
area (1/4) and bleed. It is always better to avoid KMnO 4 solution for wound wash and
instead use 5% soap wash in 30 min. after bite. It is not advisible to apply torniquet in
case of vipers bite as this venom is rich in spreading factors (local tissue necrosis).
Hospital treatment: The nature of hospital treatment practically depends on identity
of the poisonous snake. Polyvalent antivenin is the drug of choce in the absence of
identity. It is better to avoid administration of antihistaminic as they are found to
increase toxic potential of certain vipers venom. Popularly, hospital treatment can be
remembered as “AAA”: A = Antivenin.; A = Antibiotic (broad spectrum) andA =
Antitetanus / Gas gnagrene antitoxins.
The antivenin (monovalent/polyvalent) should be administered IV at the rate of
100 ml. (small animals) or 10-50ml. (large animals). Administer antivenom with 1:00
epinephrine (0.5-1 ml. s/c) to avoid shock. Apply 1-2ml. of antivenin over the wound
(site of bite in case of viper bite. Monitor the cardio vascular activity constantly.
Narcotic analeptic is recommended in case of cobra bite to counteract intense pain.
Epinephrine and corticosteroid to overcome hypotension and shock. Employ plasma
volume expander (6% dextran-40) and calcium gluconate to reduce hemolysis. In case
of viper bite, even if the patient survive, amputation may be performed to avoid spread
of local tissued necrosis or gangrene formation.
Note: - Anitivenom should be stored at 40C. Do not administer if they are discoloured
or after the date of expiry.
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
CLINICAL CONSIDERATIONS IN ADVERSE EFFECTS OF
DRUGS
U. SUNILCHANDRA
Adverse drug effects includes all adverse /side effects associated with a drug;
including that observed in overdose/poisoning with drugs or effects that may occur
during therapy. The mportant adverse effects of the drugs, in general are discussed in
this article.
Drug allergy/ hypersensitivity : Most common drug allergens implicated in producing
anaphylactic reactions in domestic animals include penicillins, cephalosporins,
sulfonamides, streptomycin, tranquliisers, vancomycin, vitamins, insulin, tetracyclines,
quinolones, salicylates, phenothiazines, chloramphenicol, heoparin, lidocaine,
erythromycin, angiotensin converting enzyme inhibitors, methyl dopa, vitamin K, iron
injections, exogenously administered repeated injections of
hormones(LH,hCG,PMSG),thiopentone, suxamethonium,non-depolarising
muscle relaxants, ester local anaesthetics and plasma expanders (dextrans, starches and
gelatins). Other agents that can cause anaphylactoid reactions include vaccines, food
and insect stings.
Clinical signs are manifested by the involving various organ systems.Cardiovascular
system:hypotension and cardiovascular collapse. tachycardia, arrhythmias, cardiac arrest.;
Respiratory System :oedema of the glottis, tongue and airway structures may cause
stridor and airway obstruction. Bronchospasm - may be severe.; Gastrointestinal:
abdominal pain, diarrhoea or vomiting.; Haematological.: coagulopathy. ; Cutaneous :
flushing, erythema, urticaria. signs may be seen. Adrenaline (1:1000 epinephrine) is the
most useful drug for treating anaphylaxis as it is effective in bronchospasm and
cardiovascular collapse. The dose of 0.01ml/kg.IV or 0.2 – 0.5ml/kg, IM is repeated in
10-15minutes if clinical signs are not resolving. Ensure adequate breathing. Intubation
and ventilation may be required.Venous return may be aided by lifting the patient's legs
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
or tilting the patient head down Antihistamine agents: H1 blockers and corticosteroids
are also administered
Hepatotoxicity : Drug-induced liver damge is manifested by highly variable, ranging
from asymptomatic elevation of liver enzymes to fulminant hepatic failure. The type of
drug induced hepatotoxicity is often accompanied by fatigue, fever, and rash, usually
developing after few weeks of therapy. The clinically important potential hepatotoxic
drugs:
acetaminophen,amoxicillin,chlorpromazine,ciprofloxacin,diclofenac,erythromycin,flucon
azole, isoniazid,methyldopa,rifampin, tetracycline,phenobarbitone, phenytoin,
primidone,diazepam (in cats), mebendazole, carprofen, diethylcarbamazine,
oxibendazole, sulfonamides, anabolic steroids, vincristine etc. Treatment is to
discontinue the suspected drug. Specific therapy against is limited to the use of N -
acetylcysteine (acetaminophen toxicity) and L-carnitine( valproate toxicity).
Nephrotoxicity:
The most common drugs with nephrotoxic potentiality are aminoglycosides, NSAIDs,
sulfonamides, tetracyclines, amphotericin B, antiviral agents, methotrexate, the older
cephalosporins, cimetidine, ciprofloxacin, furosemide, penicillins, phenytoin, rifampin,
thiazide diuretics, polymixin etc. Crystalluria, hematuria and obstruction of renal tubules
occurring with sulfonamides are prevented by adequate water intake during the therapy
and alkalinisation of the urine with urinary alkaliser (eg: sodium bicarbonate)
supplementation. The prevention or minimizing the drug induced nephrotoxicity is by
administering single daily dose; reducing the treatment course ; avoiding concurrent
administration of other nephrotoxic drugs or reducing the doses in conditions of renal
insufficicency/impairment.
Drug interactions:. may lead to diminished or an enhanced effect of a drug or may lead
to toxicity. Some pharmacodynamic drug interactions include : GC and NSAIDs
(increased gastrointestinal toxicity), furosemide and ACE inhibitors (increased diuretic
effect), sucralfate and gastric acid secretion inhiobitors( decerased efficacy of sucralfate),
NSAIDs and anticoagulants(increased bleeding), opioids and general
anaesthetics(enhanced respiratory depression by opioids) etc.
Some pharmacokinetic drug interactions that may affect negatively the absorption of the
administered former drug include: fluoroquinolones with cations Na+ and Cl-. Al and
Mg,, Orally active penicillins with antacids, tetracyclines with milk, antacid, laxatives,
digitalis with phenolphthalein (laxative), erythromycin with anti-cholinergic drugs,
linocomycin with kaolin, and orally administered antibiotics with large dose of atropine.
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
The examples of pharmacokinetic drug interactions during metabolism: phenobarbital
with
griseofulvin(decreasedefficacy),chloramphenicol(decreasedefficacy),primidone/phenytoin
(increasedhepatotoxcity),corticosteroids(decreased efficacy);fluoroquinolones with
theophylline (theophylline toxicity-CNS stimulation) etc.
Teratogenicity: Typical manifestations include congenital malformations( birth
defects), intrauterine growth restriction, carcinogenesis and fetal demise. Interference in
the formation process of major body structures(first 12 weeks of conception) cause
teratogenic effect.Classes of teratogens include radiation, maternal
infections,chemicals,and drugs Cytotoxic drugs (antineoplastic
drugs),anticoagulants(warfarin),vitamin A analogues (etretinate, isotretinoin),
anticonvulsants(carbamazepine,phenytoin,sodiumvalproate),Cardiovasculardrugs(Angiot
ensin-convertingenzymeinhibitors,AngiotensinIIinhibitors,losartan,spironolactone),
Endocrinological drugs (carbimazole,propylthiouracil,chlopropamide, sulphonylureas),
Antifungaldrugs(griseofulvin,ketoconazole,triazolesfluconazole,itraconazole,terbinafine),
cardiovasculardrugs(betablockers,minoxidil),Antiinflammatorydrugs(NSAIDs;3rdtrimest
er),antibiotics(tetracycline,ciprofloxacin, chloramphenicol, nitrofurantion, vancomycin,
aminoglycosides), antihelminthics (mebendazole,albendazole, oxfendazole) and others
( misoprostol ,statins). Before using a drug, consideration must be given to any
potentially harmful effects on the fetus or mother. To minimize the fetal risks, the lowest
possible effective dose should be used. Antineoplastic drugs, radio isotopes and
oestrogens are the potential carcinogens and mutagens.
CNS disturbances:. Antibiotics to avoid, or use with care in patients with seizures
include enrofloxacin, cephalosporins and penicillins (in renal disease), and imipenum.
Metronidazole in higher doses; more common in cats. Ivermectin (related drugs
-milbemycin, moxidectin), loperamide and vincristine are expelled from the CNS by p-
glycoprotein. Collies, Shetland sheepdogs, English sheepdogs, and Australian shepherds
are susceptible to these drugs when administered at normally therapeutic concentrations.
The other common drugs with potentiality of CNS disturbances:
levamisole,tetramisole,loperamide,tinidazole,metoclopramide,promethazine,
prochlorperazine, terbutaline,chlorpromazine, methylxanthines, piperazine, respiratory
stimulants (doxapram,nikethamide)and antihistaminics (sedation,also possible), all of
which may result in transcient CNS stimulation depending on the dose and condition.
Photosensitization: Photosensitivity reactions or photosensitization is a clinical condition
in which skin (areas exposed to light and lacking significant protective hair, wool, or
pigmentation) is hyperreactive to sunlight due to the presence of photodynamic agents.
Tissue injury is thought to result from the production of reactive oxygen intermediates or
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
from alterations in cell membrane permeability. It is most commonly seen in
cattle,sheep,goats,and
horses.Tetracyclines,fluoroquinolones,sulophonamides,antihistaminics,diuretics(thiazides
,loop),tricyclicantidepressants,phenothiazines and corticosteroids are examples of drugs
with phototoxic potentiality. Photosensitive animals on prolonged exposure to sunlight-
scratch or rub lightly pigmented, exposed areas of skin (ears, eyelids, muzzle), inducing
typical skin lesions : erythema, edema, serum exudation, scab formation, and skin
necrosis . In cattle, and especially in deer, exposure of the tongue while licking may result
in glossitis, ulceration and deep necrosis. Treatment involves palliative measures
(steroids, topical antibiotic)
Gastrointestinal disturbances: manifested by nausea, vomition, diarrhoea, abdominal
pain are most commonly observed after the oral administration of macrolides,
tetracyclines, piperazine, cephalosporins, oxyclozanide, fluoroquinolones, penicillins,
nitrofurans, rafoxanide, NSAIDs, sulphonamides, antineoplastic drugs. Unless severe as
in case of anticancerous drugs, most of them are transcient and are self limiting.
Local pain, tissue injury and irritation :. Bleeding from the injection site and
hematoma formation can occur if blood vessels are injured during particularly
intramuscular injections.. Skin necrosis, neurological damage, and loss of limb can
follow. The sciatic nerve is commonly injured by gluteal IM injections and the radial
nerve injury at the shoulder, commonly manifested by paresis, necrosis etc. Numerous
drugs like quinpyramine salts, suramin, diminazine, b complex injectables, multivitamin
injectables,cephalosporins, tetracyclines, NSAIDS, oil based injectables, the long-acting
injectable medications may result in complications at IM injection sites. The
extravasation of anticancerous drugs outside the vein may result in thrombophlebitiis and
tissue necrosis.
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
DIAGNOSTIC TESTS FOR DETECTION OF COMMON
TOXICANTS IN SAMPLES
M.VIJAY KUMAR
Detection of Heavy metals: Place 10g of tissue (finely minced) in a beaker or test
tube.Add 10 ml of 10% HCl.Introduce a copper wire into the test tube Boil for 10-15
min. (Do not inhale fumes) Remove the copper wire and place it on a filter paper
Observe the colour of the copper wire. Inference: Black coloration - Arsenic or
Bismuth; Shining silver deposit – Mercury; Dull white deposit – Silver; Dark colour
with purple to blue; violet green - Antimony.
Depending on the colour of copper wire the confirmatory test is conducted.If the
deposit is black it can be confirmed whether it is due to arsenic or bismuth by placing
the copper strip in 1-2 ml. of 10 % potassium cyanide. If the deposit is due to arsenic, it
will dissolve, but if it is due to bismuth or antimony, it will persist.In mercury, colour
of the deposit ranges grayish (50 mg) to shiny silver (100 mg).
Detection of lead : Mince the liver/kidney piece or collect a small amount of scraping
from stomach wall.Add a few drops of conc. nitric acid and heat gently till dry, (never
over heat the sample as it turns black making reading difficult). Add a few drops of
water and two drops of 10% pot. iodide solution.Development of yellow colour
indicates presence of lead.
Detection of Cyanide: a) in biological material: Take 50 g of finely ground tissue or
stomach contents in a 100 ml flask and acidify thecontents with tartaric acid. Take a
filter paper previously moistened with 10 % of guaiacol in alcohol and 0.1% of aqueous
copper sulfate solution.Plug the mouth of flask and warm gently. Allow it to stand for
30 minutes. Observe the colour of paper. If cyanide is present, a blue colour develops.
b) in the plant sample: Preparation of sodium picrate paper-Dissolve sodium
bicarbonate 5 g and picric acid 0.5 g in 100 ml of distilled water. Cut filter paper into
strips of 2. x 6. size. Dip the strips in the reagent and dry in cool place.
Take the given sample in a test tube and add a few drops of water and chlorofom. Plug
the test tube with cotton, hanging the dried picrate paper inside the test tube. The paper
should not touch the fluid in the tube. Heat the tube gently till fumes evolve. Observe
the colour of paper.If the colour of paper changes from yellow to brown it indicates that
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
the plant sampleis positive for cyanide.(The leaves and stomach contents are to be
frozen immediately after collection inpolythene bag as CN is likely to evaporate).
Detection of fluorides: To a small quantity (1-3 ml) of urine or stomach contents add
3 ml of sodium hydroxide solution in a glass or porcelain dish. Add a little quantity of
powdered glass and mix thoroughly. Apply moderate heat till dry. Add 10 ml of
concentrated sulfuric acid and cover the dish with a small plate from the under surface
of which is suspended a drop of 5% sodium chloride solution. Place a small piece of ice
on top of the plate to prevent evaporation of the drop. Heat gently for 3-5 min.,
carefully remove the drop and examine under low power of microscope. If the given
specimen contains fluorides, silicon fluoride is formed which appears as small light
pink hexagonal crystals along the rim of the drop, whereas the crystals of sodium
chloride are large and square.
Detection of Nitrite: a) Draw blood (10 ml) without anticoagulant from an affected
animal and also from a known normal animal in 20 ml capacity test tubes.Place them in
boiling water bath for 45 minutes. Cool them.Observe the colour of the blood and the
surface.Blood sample containing nitrite is Salmon pink in colour, does not pull away
fromthe side and the surface is level or concave. Normal blood sample is chocolate
brown,pulls away from the side of tube and the surface is convex.
b)In a plant sample: Dissolve 0.5 g of diphenylamine in 20 ml of distilled water and
make up the volume to 100 ml with sulfuric acid. Store it in amber colored bottle. This
is a full strength solution and can be made into half strength by diluting with equal
parts of 80% sulfuric acid. To test a plant, place a drop of the reagent on the cut surface
of plant. Observe the colour.A green to blue colour indicates the presence of nitrate.(A
green to blue colour with a half strength solution indicates positive (++) for nitrate,
which could be toxic to animal).
*****
KVC Sponsored CVE training programme on “Chemotherapy and
Diagnostic Toxicology” organized by the Dept.of Pharmacology
&Toxicology,Veterinary College,Bidar,from 23rd to 28th November
2009
76
Вам также может понравиться
- Advances in Veterinary Antimicrobial Therapy and Forensic ToxicologyДокумент230 страницAdvances in Veterinary Antimicrobial Therapy and Forensic ToxicologySunilОценок пока нет
- Trepanier2013 Applying Pharmacokinetics To Veterinary Clinical PracticeДокумент14 страницTrepanier2013 Applying Pharmacokinetics To Veterinary Clinical PracticeSarahОценок пока нет
- Handbook of Drug Interaction and the Mechanism of InteractionОт EverandHandbook of Drug Interaction and the Mechanism of InteractionРейтинг: 1 из 5 звезд1/5 (1)
- FlucanДокумент7 страницFlucanDr.2020Оценок пока нет
- PharmacokineticsДокумент83 страницыPharmacokineticsdv94gw9zd8Оценок пока нет
- Quinolones: Submitted by Jithin GДокумент12 страницQuinolones: Submitted by Jithin GJithin GangadharanОценок пока нет
- 5 Antimicrobial AgentsДокумент47 страниц5 Antimicrobial AgentsNguyên Cao ChíОценок пока нет
- Anticancer DrugДокумент29 страницAnticancer DrugAnjana PaudelОценок пока нет
- Pharmacokinetics - DrdhritiДокумент83 страницыPharmacokinetics - Drdhritidbrahma100% (1)
- Tuberculosis: Robert L. Copeland, JR., PH.DДокумент43 страницыTuberculosis: Robert L. Copeland, JR., PH.Dkristine umamingОценок пока нет
- Unit - 3Документ39 страницUnit - 3ujjwalОценок пока нет
- Cephalosporins, Flouroquinolones and SulfonamidesДокумент7 страницCephalosporins, Flouroquinolones and SulfonamidesErum JanОценок пока нет
- 6 - Farmako - Obat Penyakit MataДокумент68 страниц6 - Farmako - Obat Penyakit MatalenypsОценок пока нет
- Antimicrobial Therapy: Principles of Drug ManagementДокумент64 страницыAntimicrobial Therapy: Principles of Drug ManagementMalueth AnguiОценок пока нет
- Smart Polymer AssДокумент8 страницSmart Polymer AssbawokeОценок пока нет
- Flucil: Product InformationДокумент7 страницFlucil: Product InformationaaОценок пока нет
- Cyclophosphamide Tablets: Drug MonographДокумент2 страницыCyclophosphamide Tablets: Drug MonographShane PangilinanОценок пока нет
- Pharmaco KineticsДокумент10 страницPharmaco KineticsVithyaah ParameswaranОценок пока нет
- Treatment: Visceral Leishmaniasis: Visceral Leishmaniasis (VL), Also Known As Kala-Azar, Black Fever, and Dumdum FeverДокумент3 страницыTreatment: Visceral Leishmaniasis: Visceral Leishmaniasis (VL), Also Known As Kala-Azar, Black Fever, and Dumdum FeverbournvilleeaterОценок пока нет
- 9 - Anti Fungal DrugsДокумент73 страницы9 - Anti Fungal Drugszynab123Оценок пока нет
- Pharmacokinetics of Anti-Epileptic Drugs and Their Clinical SignificanceДокумент12 страницPharmacokinetics of Anti-Epileptic Drugs and Their Clinical Significancerozina mulatОценок пока нет
- Assignment On Pharmacokinetic Drug Interaction: Teerthanker Mahaveer UniversityДокумент8 страницAssignment On Pharmacokinetic Drug Interaction: Teerthanker Mahaveer Universityt24008882Оценок пока нет
- Chloramphenicol: Ayen University - Al College of PharmacyДокумент7 страницChloramphenicol: Ayen University - Al College of Pharmacyمحمد حميد عطيةОценок пока нет
- Anti Fungal TableДокумент4 страницыAnti Fungal TableMaebritt TibubosОценок пока нет
- KSR Pai Antitubercular DrugsДокумент81 страницаKSR Pai Antitubercular Drugswolverine12309Оценок пока нет
- Selection of Antimicrobials To Treat Infectious DiseasesДокумент14 страницSelection of Antimicrobials To Treat Infectious DiseasesInoxcent MoonОценок пока нет
- Awji Et Al-2012-Veterinary DermatologyДокумент7 страницAwji Et Al-2012-Veterinary DermatologyEliud RománОценок пока нет
- Aspects of Pharmacology in The Neonatal FoalДокумент26 страницAspects of Pharmacology in The Neonatal FoalAristoteles Esteban Cine VelazquezОценок пока нет
- Baru 2Документ8 страницBaru 2Nazihan Safitri AlkatiriОценок пока нет
- Hobden Antibiotics II 09Документ12 страницHobden Antibiotics II 09lovelyc95Оценок пока нет
- Antibiotics CompiledДокумент30 страницAntibiotics CompiledJoanne Chu100% (1)
- ReportingДокумент8 страницReportingJanus SantosОценок пока нет
- Introduction To PharmacologyДокумент25 страницIntroduction To PharmacologyGaurav SaxenaОценок пока нет
- Inmunosupresores Caninos y FelinosДокумент22 страницыInmunosupresores Caninos y FelinosJuan Daniel Serrano GuerreroОценок пока нет
- Preformulation Study of Moxifloxacin Hydrochloride 2Документ20 страницPreformulation Study of Moxifloxacin Hydrochloride 2زياد سلمانОценок пока нет
- Pharmacokinetics in PregnancyДокумент10 страницPharmacokinetics in PregnancyCyrel Alexandra I. DiolazoОценок пока нет
- AntifungalДокумент41 страницаAntifungalDeribe BekeleОценок пока нет
- MoxiquinДокумент50 страницMoxiquinpabitraОценок пока нет
- Drug StudyДокумент6 страницDrug StudyMarielle Denise Tagtag BugtongОценок пока нет
- ANtifungal 240522Документ30 страницANtifungal 240522Smita DabadeОценок пока нет
- A Review of The Clinical Pharmacokinetics of MeloxicamДокумент4 страницыA Review of The Clinical Pharmacokinetics of MeloxicamkwadwobrosОценок пока нет
- Clinical PharmacologДокумент81 страницаClinical PharmacologSHILOTAОценок пока нет
- Milta 2 - MarcadoДокумент4 страницыMilta 2 - MarcadoVictor RoticivОценок пока нет
- PharmacДокумент101 страницаPharmacpai.parthjana2020Оценок пока нет
- Inhibicion de AcidosДокумент24 страницыInhibicion de AcidosItzel JuОценок пока нет
- Ceutics CAT 2Документ9 страницCeutics CAT 2Ria KitlerОценок пока нет
- Lecture 2 - Basic Concepts of PharmacokineticsДокумент63 страницыLecture 2 - Basic Concepts of Pharmacokineticsahmadslayman1Оценок пока нет
- Basic Principles of Pharmaceutical Systems Lec1Документ15 страницBasic Principles of Pharmaceutical Systems Lec1sadanalzoubiОценок пока нет
- Kusum D.V., Bhosale U.V. - Formulation and Optimization of Polymeric Nano Drug Delivery System of Acyclovir Using 3 (2) Full Factorial DesignДокумент10 страницKusum D.V., Bhosale U.V. - Formulation and Optimization of Polymeric Nano Drug Delivery System of Acyclovir Using 3 (2) Full Factorial DesignJordy CanalesОценок пока нет
- Pharmacokinetic and Pharmacodynamic2021Документ12 страницPharmacokinetic and Pharmacodynamic2021STEFANIA AYA DIAZОценок пока нет
- Keto Vs Mikonazol PharmacologyДокумент6 страницKeto Vs Mikonazol PharmacologyRanda NovalinoОценок пока нет
- Antifungal Drugs: Evi Sovia Pharmacology DepartementДокумент55 страницAntifungal Drugs: Evi Sovia Pharmacology DepartementKresna Denta ElygioОценок пока нет
- Claforan (Cefotaxime) PDFДокумент18 страницClaforan (Cefotaxime) PDFdinniОценок пока нет
- Ghannoum 2013Документ8 страницGhannoum 2013Aldana JaraОценок пока нет
- Sulfonamides, Trimethoprim-Sulfamethoxazole, Quinolones, and Agents For Urinary Tract InfectionsДокумент35 страницSulfonamides, Trimethoprim-Sulfamethoxazole, Quinolones, and Agents For Urinary Tract InfectionsHanung PujanggaОценок пока нет
- Met Hamido PhosДокумент2 страницыMet Hamido PhosesposibleОценок пока нет
- Bayer 3rd Proc'99 - BOOTHE2Документ8 страницBayer 3rd Proc'99 - BOOTHE2sergioОценок пока нет
- Mycotoxins in Animal HealthДокумент103 страницыMycotoxins in Animal HealthSunil100% (1)
- Classification of AmphibiansДокумент22 страницыClassification of AmphibiansSunilОценок пока нет
- Household Hazards To PetsДокумент16 страницHousehold Hazards To PetsSunilОценок пока нет
- Endocrine Vety PharmaДокумент16 страницEndocrine Vety PharmaSunilОценок пока нет
- Fluorosis Phosphorous Nitrate Toxicity in AnimalsДокумент55 страницFluorosis Phosphorous Nitrate Toxicity in AnimalsSunilОценок пока нет
- Drugs in ReptilesДокумент71 страницаDrugs in ReptilesSunil100% (1)
- VPT MCQ ForДокумент10 страницVPT MCQ ForSunilОценок пока нет
- Carbon Monoxide PoisoningДокумент22 страницыCarbon Monoxide PoisoningSunilОценок пока нет
- Antiseptics and Disinfectants For Veterinary ClinicsДокумент3 страницыAntiseptics and Disinfectants For Veterinary ClinicsSunil100% (5)
- Drugs in Behavioural Disorders of PetsДокумент5 страницDrugs in Behavioural Disorders of PetsSunilОценок пока нет
- Toxicological Investigation and Its Significance in Animal Health DiagnosisДокумент8 страницToxicological Investigation and Its Significance in Animal Health DiagnosisSunilОценок пока нет
- Classification and Dosage of Antimicrobial Agents in Veterinary MedicineДокумент24 страницыClassification and Dosage of Antimicrobial Agents in Veterinary MedicineSunil0% (1)
- Nsaids and Other Antinflammatory Agents in Veterinary PracticeДокумент44 страницыNsaids and Other Antinflammatory Agents in Veterinary PracticeSunil100% (2)
- VCI MSVE 2008 RegulationsДокумент136 страницVCI MSVE 2008 RegulationsSunil50% (2)
- Behavioural Modifying Drugs in PetsДокумент33 страницыBehavioural Modifying Drugs in PetsSunilОценок пока нет
- Mercury Lead Arsenic Cadmium ToxicityДокумент171 страницаMercury Lead Arsenic Cadmium ToxicitySunilОценок пока нет
- Drugs Acting On Respiratory System of AnimalsДокумент8 страницDrugs Acting On Respiratory System of AnimalsSunil100% (4)
- Drugs Acting On Haematopoietic System of AnimalsДокумент28 страницDrugs Acting On Haematopoietic System of AnimalsSunil100% (1)
- Drugs Acting On Genitourinary System of AnimalsДокумент44 страницыDrugs Acting On Genitourinary System of AnimalsSunilОценок пока нет
- Drugs Acting On Digestive System of AnimalsДокумент11 страницDrugs Acting On Digestive System of AnimalsSunil100% (3)
- LATHYRISM AND PHOTOSENSiTIZATIONДокумент33 страницыLATHYRISM AND PHOTOSENSiTIZATIONSunilОценок пока нет
- GENERAL LINE of Treatment UREA AMMONIA SALT - poISONINGДокумент49 страницGENERAL LINE of Treatment UREA AMMONIA SALT - poISONINGSunil0% (1)
- Toxicokinetics DynamicsДокумент76 страницToxicokinetics DynamicsSunil100% (1)
- Site of Action of Drugs Acting On Cholinergic Neurohumoral Transmission PDFДокумент1 страницаSite of Action of Drugs Acting On Cholinergic Neurohumoral Transmission PDFSunilОценок пока нет
- Mycotoxins in Animal HealthДокумент103 страницыMycotoxins in Animal HealthSunil100% (1)
- ZOOTOXINSДокумент72 страницыZOOTOXINSSunil83% (6)
- Environmental PollutantsДокумент32 страницыEnvironmental PollutantsSunilОценок пока нет
- Fluorosis Phosphorous ToxicityДокумент55 страницFluorosis Phosphorous ToxicitySunilОценок пока нет
- AntiConvulsants Drugs in Brief PDFДокумент28 страницAntiConvulsants Drugs in Brief PDFSunilОценок пока нет
- Site of Action of Drugs Acting On Adrenergic Neurohumoral Transmission PDFДокумент1 страницаSite of Action of Drugs Acting On Adrenergic Neurohumoral Transmission PDFSunilОценок пока нет
- Laboratory Technician TrainingДокумент3 страницыLaboratory Technician TrainingVincent MuhayimanaОценок пока нет
- Ospe PyДокумент20 страницOspe Pyipop_001Оценок пока нет
- CANCERДокумент11 страницCANCERMuhammed IbrahimОценок пока нет
- Pediatric Critical Care MedicineДокумент107 страницPediatric Critical Care Medicinerahmawatusayu100% (1)
- Perioperative NursingДокумент13 страницPerioperative NursingTobiDaОценок пока нет
- Alvine Discharge DiseasesДокумент1 страницаAlvine Discharge DiseasesApril Rose AlivioОценок пока нет
- Org - Telegram.messenger - Provider Media Telegram Telegram Documents 4 5920093559716840840 PDFДокумент32 страницыOrg - Telegram.messenger - Provider Media Telegram Telegram Documents 4 5920093559716840840 PDFsameeОценок пока нет
- Swine Health: Beth Ferry MSU Extension Pork EducatorДокумент30 страницSwine Health: Beth Ferry MSU Extension Pork EducatorGooo PoooОценок пока нет
- English Course: Instructor'S Contact Info Ahmad Ridho Rojabi, S.PD, M.PDДокумент62 страницыEnglish Course: Instructor'S Contact Info Ahmad Ridho Rojabi, S.PD, M.PDeliahapsaОценок пока нет
- Human T-Cell Lymphotropic Virus Type 1 and StrongyДокумент9 страницHuman T-Cell Lymphotropic Virus Type 1 and StrongyThais TorresОценок пока нет
- Antibacerials PharmacolgyДокумент53 страницыAntibacerials PharmacolgyHamid AryanОценок пока нет
- Nclex Exam 2010Документ28 страницNclex Exam 2010Mtobs Mukhaini82% (17)
- MUMPSДокумент14 страницMUMPScicichepiОценок пока нет
- Case Study: by Misty ArhelgerДокумент3 страницыCase Study: by Misty ArhelgerPhanVHОценок пока нет
- Project Coc (Cleanliness On Comfort Rooms)Документ6 страницProject Coc (Cleanliness On Comfort Rooms)Dhivinne PerezОценок пока нет
- Infectious Bronchitis and Its Effect On Egg Production and Egg QualityДокумент2 страницыInfectious Bronchitis and Its Effect On Egg Production and Egg QualityPrima Puji RaharjoОценок пока нет
- Graphic EraДокумент1 страницаGraphic EraPharmacy On FingerTipsОценок пока нет
- Airborne Diseases PDFДокумент5 страницAirborne Diseases PDFZegera MgendiОценок пока нет
- Treatmnt HerpesДокумент8 страницTreatmnt HerpesZakky FebrianОценок пока нет
- Records & Reports Maintained at Sub-Centre and PHCДокумент32 страницыRecords & Reports Maintained at Sub-Centre and PHCLakshmi Seth87% (15)
- Antibody Structure & Function AtfДокумент6 страницAntibody Structure & Function Atfnofov45585Оценок пока нет
- 7.epidemiology of Communicable DiseasesДокумент23 страницы7.epidemiology of Communicable DiseasesBada InandanОценок пока нет
- Neisseria Meningitidis PDFДокумент8 страницNeisseria Meningitidis PDFmulyadiОценок пока нет
- Atlas of Uveitis and Scleritis PDFДокумент179 страницAtlas of Uveitis and Scleritis PDFLeslie Stewart100% (1)
- Rhizoctonia BulletinДокумент6 страницRhizoctonia BulletinMarlene RosalesОценок пока нет
- Feline Panleukopenia VirusДокумент9 страницFeline Panleukopenia VirusridhanoidОценок пока нет
- TBL PaedsДокумент10 страницTBL PaedsHo Yong WaiОценок пока нет
- اسئلة امتحان الهيئة ميكروبيولوجى ومختبرات PDFДокумент18 страницاسئلة امتحان الهيئة ميكروبيولوجى ومختبرات PDFMaaryMeee RMT0% (1)
- Euroimmun ManualДокумент4 страницыEuroimmun ManualAFWОценок пока нет
- Epidemiologic Mass Treatment 2014Документ11 страницEpidemiologic Mass Treatment 2014TivHa Cii Mpuzz MandjaОценок пока нет
- The Obesity Code: Unlocking the Secrets of Weight LossОт EverandThe Obesity Code: Unlocking the Secrets of Weight LossРейтинг: 4 из 5 звезд4/5 (6)
- The Age of Magical Overthinking: Notes on Modern IrrationalityОт EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityРейтинг: 4 из 5 звезд4/5 (28)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsОт EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsОценок пока нет
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeОт EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeРейтинг: 2 из 5 звезд2/5 (1)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDОт EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDРейтинг: 5 из 5 звезд5/5 (1)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionОт EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionРейтинг: 4 из 5 звезд4/5 (404)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsОт EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsРейтинг: 5 из 5 звезд5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisОт EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisРейтинг: 4.5 из 5 звезд4.5/5 (42)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedОт EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedРейтинг: 5 из 5 звезд5/5 (81)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsОт EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsРейтинг: 3.5 из 5 звезд3.5/5 (3)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisОт EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisРейтинг: 4 из 5 звезд4/5 (1)
- Why We Die: The New Science of Aging and the Quest for ImmortalityОт EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityРейтинг: 4 из 5 звезд4/5 (3)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaОт EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningОт EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningРейтинг: 4 из 5 звезд4/5 (3)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)От EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Оценок пока нет
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisОт EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisРейтинг: 3.5 из 5 звезд3.5/5 (2)
- Gut: the new and revised Sunday Times bestsellerОт EverandGut: the new and revised Sunday Times bestsellerРейтинг: 4 из 5 звезд4/5 (392)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryОт EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryРейтинг: 4 из 5 звезд4/5 (44)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.От EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Рейтинг: 4.5 из 5 звезд4.5/5 (110)
- The Marshmallow Test: Mastering Self-ControlОт EverandThe Marshmallow Test: Mastering Self-ControlРейтинг: 4.5 из 5 звезд4.5/5 (58)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessОт EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessРейтинг: 4.5 из 5 звезд4.5/5 (328)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingОт EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingРейтинг: 4 из 5 звезд4/5 (1138)
- Troubled: A Memoir of Foster Care, Family, and Social ClassОт EverandTroubled: A Memoir of Foster Care, Family, and Social ClassРейтинг: 4.5 из 5 звезд4.5/5 (26)