Академический Документы
Профессиональный Документы
Культура Документы
Autoimmune Disease - Aetiopathogenesis PDF
Загружено:
manoj_rkl_07Оригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Autoimmune Disease - Aetiopathogenesis PDF
Загружено:
manoj_rkl_07Авторское право:
Доступные форматы
Autoimmune Disease: Aetiology and Pathogenesis
JGM Rosmalen, Erasmus University, Rotterdam, The Netherlands PJM Leenen, Erasmus University, Rotterdam, The Netherlands HA Drexhage, Erasmus University, Rotterdam, The Netherlands
Unfortunate combinations of genetic susceptibility and exogenous factors (microbial, toxic, stress) lead to full-blown autoimmune disease
Secondary article
Article Contents
. Introduction . Multifactorial Nature of Autoimmune Diseases . Development of Organ-specific Autoimmune Diseases . Development of Rheumatoid Arthritis: Various Signs of Immunodysregulation . Effects of Age and Gender . Effects of Environmental Factors . Conclusion
Introduction
One of the important functions of the immune system is the discrimination between self and nonself, or perhaps better between danger and nondanger. Currently, such distinction is thought to be made in a series of complicated and multistep interactions between various cells and components of the immune system. Erroneously, immune cells sometimes build an immune reaction towards self during conditions of apparent nondanger. When such immune reaction is so aberrantly and vigorously selfdirected, pathological damage is inicted on tissues. Socalled autoimmune diseases are the consequence. Autoimmune diseases can be divided into two main categories: the organ-specic and the systemic autoimmune diseases. In organ-specic autoimmune diseases, the immune attack is conned to one organ or organ system. In the majority of organ-specic autoimmune diseases, target tissues are of neuroendocrine character. Among these target tissues are the thyroid, the islets of Langerhans, the intrinsic factor-producing gastric parietal cells, the steroidproducing cells of the adrenal, ovary and testis, the pituitary, the neuromuscular junction in striated muscles, and the myelin sheaths in the central nervous system. The most extensively studied and well characterized organspecic autoimmune diseases are listed in Table 1, and include disorders such as Hashimoto thyroiditis, type 1 diabetes mellitus, Addison disease and Sjo gren syndrome. In systemic autoimmune diseases, target tissues and molecules are widespread in the body. Examples are nuclear components, collagen components and immunoglobulin G (IgG) itself. Hallmarks of the systemic autoimmune diseases are vasculitis and arthritis. Prototypes are systemic lupus erythematosus (SLE) and rheumatoid arthritis (RA) (Table 1). This article is designed to give a birds eye view of the aetiology and pathogenesis of autoimmune diseases. As this is a topic with an extensive body of gathered knowledge and theories, we must necessarily restrict ourselves and give a perhaps biased view, mainly highlighting two prototypic forms of organ-specic and
systemic autoimmunity respectively: the endocrine autoimmune diseases and RA.
Multifactorial Nature of Autoimmune Diseases
In humans, study of the aetiology and pathogenesis of the various autoimmune diseases is logically restricted. Autoimmune diseases often show long nonclinical prodromal phases, which can hardly be studied as clinical signs and symptoms are (still) absent. Over the past 30 years various inbred animal models of spontaneously occurring variants of the human autoimmune diseases have become available (Table 1). These models have greatly contributed to knowledge of the aetiology and pathogenesis of the various autoimmune diseases, most notably of the events that occur in the very early prodromal phases. Studies of the spontaneous animal models have reinforced the idea that the various autoimmune diseases are distinct in nature. Animal models of spontaneously occurring organ-specic autoimmune disease, for instance, hardly show signs of systemic autoimmunity. The animals do, however, often suer from more than one organspecic autoimmune disease. Conversely, models of systemic autoimmunity hardly ever show signs of organspecic autoimmune disease, except for Sjo gren syndrome (sialoadenitis). This strongly suggests a clearly dierent aetiopathogenesis for organ-specic and systemic autoimmune diseases. Furthermore, an inbred animal model of spontaneously occurring RA is lacking, and the two inbred animal models for spontaneously occurring SLE (i.e. the MRL/lpr mouse and the New Zealand White/New Zealand Black (NZW/ NZB) mouse) never show the severe form of destructive arthritis that is characteristic of RA. This suggests that the aetiopathogenesis of RA and SLE are dierent too, and that environmental factors play a prominent role in the development of RA. Indeed, animal models of RA often involve the experimental induction of the disease via
1
ENCYCLOPEDIA OF LIFE SCIENCES / & 2001 Macmillan Publishers Ltd, Nature Publishing Group / www.els.net
2 Autoimmune Disease: Aetiology and Pathogenesis
Table 1 Overview of major autoimmune diseases Animal models Effector mechanisms and resulting autoantibodies/and T cells ADCC and TH1-mediated thyrocyte destruction Antibodies blocking TSH-R Antibodies stimulating TSH-R TH1-mediated destruction of cells Experimental (allergic) Clinical symptoms Goitre, followed by thyroid failure Hypothyroidism and thyroid atrophy Goitre and hyperthyroidism Hyperglycaemia BB rat NOD mouse Spontaneous BB rat NOD mouse OS chicken Antigen/procedure Thyroglobulin in FCA Animal Normal rats and rabbits Disease
ENCYCLOPEDIA OF LIFE SCIENCES / & 2001 Macmillan Publishers Ltd, Nature Publishing Group / www.els.net
Major autoantigens Thyroperoxidase Thyroglobulin
Organ-specific autoimmune diseases Hashimoto thyroiditis
Primary hypothyroidism TSH-R Graves disease TSH-R
TSH-R ECD
NOD mouse
TSH-R+ MHC class II+ fibroblasts AKR/N mouse TSH-R ECD Balb-C mouse Streptozotocin Normal rats and mice
Type 1 diabetes mellitus Insulin GAD IA-2 ICA-69 Pernicious anaemia Na+/H+ ATPase Intrinsic factor 21-Hydroxylase 17-Hydroxylase Tyrosinase
TH1-mediated destruction of gastric parietal cells and neutralization of intrinsic factor by antibodies TH1-mediated destruction of steroidproducing cells Disappearance of melanocytes
Atrophic gastritis Anaemia Adrenalitis and oophoritis Depigmentation Dry eyes Dry mouth Diverse neurological symptoms
Tx (3 day)
Balb/C mouse A/J mouse Balb/C mouse A/J mouse Melanoma therapy (human) NFS/sld mouse Lewis/DA rat SJL mouse Marmoset monkey
Addison disease Vitiligo Sjgren syndrome Multiple sclerosis
Tx (3 day) Smyth-line chicken Melanosomal proteins + IL-2/DC NOD None Tx (3 day) MBP, PLP or MOG in FCA
Destruction/blockade of salivary/ Phodrin lacrimal glands (sialoadenitis) M3-muscarinic receptor MBP, PLP, MOG TH1-mediated destruction of myelin sheaths
Systemic autoimmune diseases Systemic lupus erythematosus dsDNA Other nucleoproteins Antigenantibody reaction Vasculitis (Sjgren syndrome) MRL/lpr mouse Glomerulonephritis NZW/NZB mouse Mild arthritis Sialoadenitis Skin erythema None Mycobacteria Anaerobic bacteria Lewis rat SJL mouse
Rheumatoid arthritis
lgG Collagen type II
Excessive lymphoid tissue developSevere arthritis with ment in synovium (pannus formation) deformations Excessive cytokine and rheumatoid factor production in pannus Destruction of cartilage/bone
ADCC, antibody-dependent cell-mediated cytotoxicity; ECD, extracellular domain; FCA, Freund complete adjuvants; GAD, glutamic acid decarboxylase; IA-2, tyrosine phosphatase; ICA, islet cell autoantigen; Ig, immunoglobulin; IL, interleukin; MBP, myelin basic protein; MHC, major histocompatibility complex; MOG, myelin oligodendrocyte glycoprotein; PLP, proteolipid protein; TH, T helper (cell); TSH-R, thyroid-stimulating hormone receptor; Tx, 3-day thymectomy model (see text).
Autoimmune Disease: Aetiology and Pathogenesis
immunizations with mycobacteria, anaerobic bacteria or antigens derived from these microbial agents. Nevertheless, a genetic susceptibility for the disease, as observed in the Lewis rat and the SJL mouse, is a prerequisite for inducibility (Table 1). Collectively, studies over the past 20 years, in both patients and in the various animal models, have culminated in the awareness that autoimmune diseases must be regarded as polygenic diseases, of which the penetrance is strongly inuenced by environmental factors. Multiple genes (e.g. more than 15 in the nonobese diabetic (NOD) mouse model of type 1 diabetes) determine part of the aberrant immune response towards self. Most important are the genes of the major histocompatibility complex (MHC) region. However, other genes are also involved. These genes include those playing a role in the regulation of the metabolism of the target tissue (e.g. the insulin gene in type 1 diabetes) and genes involved in general regulation of the immune system (e.g. the cytotoxic T lymphocyteassociated antigen 4 (CTLA-4) gene) (Todd and Farrall, 1996). However, genetic polymorphisms are not the whole story. Monozygotic twin studies in type 1 diabetes, for example, have shown a concordance rate of, at best, 45 50% between twins. This demonstrates the additional importance of environmental eliciting factors. In particular, microbial agents of the gut environment and environmental substances toxic for the target tissue and/or the immune system involved. Although detailed pathogenic mechanisms are far from clear for the individual autoimmune diseases, some generalizations can be made. The odds are in favour of the following hypothetical scenarios: 1. Organ-specic autoimmune diseases are characterized mainly by organ failure as a result of target cell destruction in which T helper (TH) 1 cells and activated macrophages play a dominant role. Abnormalities in the structure, growth, metabolism, antigenicity or homeostasis of the organ or organ-system trigger the initial autosensitization to the various organ-specic antigens. Further immunodysregulations are then prerequisite for the development of full-blown disease. Both the early eliciting target abnormalities as well as the immunodysregulations may be genetically or environmentally determined. 2. SLE-like diseases are due mainly to vascular antigen antibody complex reactions in, for example, the skin and kidney. Antibodies are directed mainly towards nuclear components released in apoptotic processes (nucleosomes), and the excessive antibody production towards these nuclear components is probably the result of an abnormal B-cell hyperplasia in a T celldysregulated individual. 3. RA is the consequence of an excessive T and B cellmediated reaction towards microbial antigens of the gut and/or lung environment. These antigens are
probably spread to and trapped in the joints, where the hypersensitization is continued in locally formed lymphoid tissue (the pannus). In this lymphoid tissue, the immune reaction is amplied, and spreads to autoantigens of the joint, such as collagen type II and IgG itself. As the authors have experience mainly of the study of organ-specic autoimmune diseases and environmental agents in RA models, and as space is limited, the aetiology and pathogenesis of only organ-specic autoimmune diseases and RA will be covered in more detail.
Development of Organ-specific Autoimmune Diseases
Afferent, central and efferent phases
The pathogenesis of autoimmune thyroiditis, autoimmune diabetes, autoimmune sialoadenitis and autoimmune vitiligo have been studied in detail in animals that spontaneously develop forms of these autoimmune diseases, such as the obese strain of chicken (OS chicken) (Wick et al., 1989), the biobreeding (BB) rat (Delemarre et al., 1996), the NOD mouse (Bach and Mathis, 1997) and the Smyth-line chicken (Shresta et al., 1997) (Table 1). A synopsis of the outcomes of these studies is given here. A word of caution is necessary when trying to extrapolate data obtained in these animal models to the human situation. The animal models clearly show caricatural, homogeneous and extreme forms of the various diseases, which already dier between the various models for a single disease (let alone from patients). Hence, general conclusions drawn on the basis of studies in one of the animal models should always be veried in the other animal models and in humans. The study of the animal models has shown that the pathogenesis of the autoimmune failure of a gland or tissue is a multistep process, requiring several genetic and environmental abnormalities (or variants) to converge before full-blown autoimmune disease develops. Hence, organ-specic autoimmune diseases are the outcome of an unfortunate combination of various genetic traits and environmental circumstances that by themselves do not need to be harmful, and may even be advantageous. In short, the following stages in the pathological immune process can be distinguished: 1. An initial aerent phase of an accumulation of antigen-presenting cells (APCs), particularly of dendritic cells (DCs) and subclasses of macrophages in the putative target tissue (Figure 1). 2. A later central phase of an apparently uncontrolled production of autoreactive CD4 1 T cells, CD8 1 T cells and of autoantibodies of the IgG class (Figure 1).
3
ENCYCLOPEDIA OF LIFE SCIENCES / & 2001 Macmillan Publishers Ltd, Nature Publishing Group / www.els.net
Autoimmune Disease: Aetiology and Pathogenesis
Phase
Time Afferent phase Central phase CD8 + APC E E E Ag + Cy TH2 Cy APC + IFN E E M Effector phase Receptor Aabs ADCC E Radicals Cy
Cy
APC
Target tissue
TH1 T 1 H CD8 TH1 en TGF Tr IL-4 TH1 IFN IL-4 TH2 + B
mo
mo Aabs en
TH2
Draining lymph node
APC P
APC influx induced by: 1. Aspecific necrosis of target cells (virus, toxins)
Aberrant regulation of immune response:
Pathological reaction of target cells:
Combination of conditions generating autoimmune disease
1. Defects in intrathymic 1. Excessive accumulation generation of T cells of lymphoid cells and their products. Effects of: 2. Defects in T-cell a. receptor antibodies 2. Altered metabolism deletion (AICD) b. ADCC or growth of target c. blocking/toxic effects 3. TH1 : TH2 dysbalance cells of cytokines and macrophage-derived 4. Defects in Tr circuits radicals due to altered APC d. CD8 cytotoxicity function 2. Excessive susceptibility of target cells
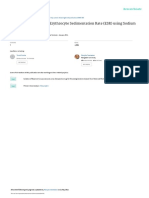
Figure 1 The immunopathogenic events that take place during the development of autoimmunity and ultimately lead to autoimmune glandular failure. In a first afferent phase, antigen-presenting cells (APCs), probably mostly monocyte derived, accumulate in the putative target gland. The APC influx can be induced by aspecific inflammatory stimuli, such as necrosis of target cells by viruses or toxins. Altered metabolism or growth of the target cells may also be an induction factor for APC accumulation (see text). The accumulated APCs take up relevant autoantigens and leave the tissues to travel to the draining lymph nodes. In a second central phase the APCs seek contact with T and B cells in the draining lymph nodes. Apparently, an aberrant immune response results. Instead of reinforcing tolerance, the APCs generate an autoimmune reaction. The figure lists the various abnormalities found in animal models underlying this aberrant regulation of the autoimmune response. In a final afferent phase the generated autoreactive T cells, B cells and antibodies have their effect on the target cells after having gained access to the target gland (see text for various mechanisms). mo, monocyte; en, endothelial cell; Ag (red triangle), autoantigen; Cy, cytokines; E, endocrine cell; Mf, macrophage; ADCC, antibody-dependent cell-mediated cytotoxicity; P, plasma cell; TH1, T helper cell type 1; TH2, T helper cell type 2; Tr, T regulator cell; B, B cell; Aabs, autoantibodies; AICD, activation-induced cell death; IFN, interferon; IL, interleukin; 1 , stimulation, 2 , suppression:!, traffic.
Initially this production of immune eectors takes place in the draining lymph nodes, but later also in a locally developed lymphoid tissue in the diseased tissue itself. 3. A nal eerent phase in which the target tissue becomes susceptible to the autoimmune attack exerted
4
by the generated autoreactive T cells and autoantibodies (Figure 1). This commonly results in the destruction of the tissue or the blockade of its function or growth. Occasionally, it may also result in stimulation of the target tissue, as is the case in Graves disease.
ENCYCLOPEDIA OF LIFE SCIENCES / & 2001 Macmillan Publishers Ltd, Nature Publishing Group / www.els.net
Autoimmune Disease: Aetiology and Pathogenesis
Target abnormalities related to the afferent phase
Blood monocytes are able to mature into various subsets of macrophages as well as into various subsets of DCs (Peters et al., 1996). DCs are the APCs par excellence, and are essential for stimulation of naive T cells, leading to clonal expansion of the latter. Macrophages have various functions, ranging from the phagocytosis and degradation of unwanted material, via the regulation of immune responses, to the production of factors for wound healing and remodelling of bone (Leenen and Campbell, 1993). Increased numbers of MHC class II-positive DCs and specic subsets of macrophages have been found both inside and outside lymphocytic accumulations in the thyroid of patients with Graves disease or Hashimoto goitre, in the islets of diabetics, in the salivary glands of patients with Sjo gren disease, and in the thyroids, islets and salivary glands of the animal models of these diseases (Drexhage et al., 1999). In the animal models, the rst sign of a developing autoimmune reaction is, in fact, an increase in the number of DCs and macrophages in the future target glands, as well as a local homotypic clustering of these cells. The potential APCs, accumulated in these tissues, subsequently enter the lymphatics to travel to the draining lymph nodes while transporting self antigens. What attracts these DCs and macrophages to the target glands? First, attraction signals may simply be inammatory in character. An early necrosis of future target cells due to a viral or bacterial infection, or to toxins and drugs, with the concomitant release of self antigens have been described as eliciting factors (Figure 1). The variety of eliciting factors already indicates the heterogeneity in causal factors at the level of induction of an organ-specic autoimmune disease. Second, DCs and macrophages may accumulate not to exert an immune function, but to regulate the growth and function of endocrine cells or to play a role in tissue homeostasis. It is relevant to note that DCs and macrophages are normal constituents of almost all tissues. In endocrine tissues, the cells regulate the growth and function (in both a positive and a negative way) of neighbouring hormone-producing cells (Hoek et al., 1997). In other tissues, DCs and macrophages are involved in homeostasis during, for example, regeneration processes such as wound healing. The recognition that monocytederived cells constitute a recruitable cell system that, on the one hand, is capable of regulating tissue homeostasis, but on the other hand is also capable of initiating immune responses has implications for our understanding of the induction phase of an endocrine autoimmune reaction. Alterations in the structure, growth and function of tissues may necessitate an inux of DCs and macrophages to regulate tissue homeostasis. This noninammatory inux may, however, be a rst step on the way to autoimmunity. There are arguments for such a concept:
. Iodine deciency leads to goitre formation and to simultaneous inuxes of DCs in the goitre, which is followed by a mild thyroid autoimmune reaction. . Very early (and even fetal) abnormalities in the proliferative capability and hormone production of thyrocytes and pancreatic islet cells have been described in the OS chicken (Sundick et al., 1996), the BB rat, and the NOD mouse (Homo-Delarche, 1997). Also, the salivary glands of NOD mice and the melanocytes of the Smyth-line chicken show inborn errors of growth and metabolism. . The preautoimmune islet abnormalities in the NOD mouse can in part be corrected by prophylactic insulin therapy. Such an early correction of the preautoimmune target cell abnormality leads to a lower inux of DCs and an attenuation of the subsequent autoimmune reaction. The early DC and macrophage inux does not, however, suce for the full development of an endocrine autoimmune disease. In addition, aberrations at the DC, macrophage and lymphocyte level are required to initiate the inappropriate and pathological autoimmune response.
Dysregulations of the immune system in the central phase
In endocrine autoimmune diseases the initial phase of the tissue accumulation of DCs and macrophages is followed by a phase of clonal expansion and maturation of autoreactive eector T and B cells in the draining lymph nodes. In the diabetes prone (DP) BB rat, the NOD mouse and the OS chicken, there are strong indications for genetically determined immunodysregulations that lead to an intolerance for the presented self antigens, explaining the apparently uncontrolled clonal expansion of lymphocytes. These immunodysregulations are partly associated with the presence of particular MHC class I and class II haplotypes, but other genes are also involved. The exact mechanisms of maintaining tolerance in nonautoimmune individuals are far from clear. There exist mechanisms of central tolerance induction (e.g. T-cell deletion in the thymus), mechanisms of peripheral tolerance induction (e.g. activation-induced T-cell death (AICD) and the suppressor activity of regulatory T cells), mechanisms of anergy induction, and immunological ignorance. A variety of defects in these mechanisms has been described in animal models. The BB-DP rat lacks a particular regulator (suppressor) population of T cells in its peripheral immune system, the so-called RT6 1 T cells. Interestingly, it is particularly this subset of T cells that is weakly stimulated by splenic DCs of the BB-DP rat. In this and other aspects, this important splenic APC population also appears to be abnormal. Thymic abnormalities are also evident in the BB-DP rat, suggesting deviations at the level of central tolerance as
5
ENCYCLOPEDIA OF LIFE SCIENCES / & 2001 Macmillan Publishers Ltd, Nature Publishing Group / www.els.net
Autoimmune Disease: Aetiology and Pathogenesis
well. Interestingly, the OS strain of chickens also has defects in its regulatory T-cell system (Wick et al., 1989), as has the neonatally thymectomized Balb/C mouse (see Table 1). The NOD mouse has clear defects in T-cell apoptosis, leading to a decreased ability of the cells to undergo AICD, a major mechanism in both central and peripheral tolerance induction. Moreover, NOD mice are characterized by an abnormal thymic architecture. Whether there are similar (inborn) defects in the lymphoid organs and immunoregulatory cells of patients needs to be investigated. There are, however, numerous reports of human studies showing both numerical and functional decits in T cells with a suppressive function. Also, various DC and macrophage defects have been described in patients with autoimmune thyroid disease and type 1 diabetes. Decits in immunoregulation do not exist only on a genetic basis. They can also be acquired by viral infection. When viruses infect mice (e.g. Encephalomyocarditis virus (EMCV) D in susceptible mice), or when viruses infect rats (e.g. Kilham virus in diabetes-resistant (DR)-BB rats), macrophages are aected, leading in the latter rat model to diabetes (Yoon, 1990). Whether similar viruses or retroviruses with an anity for immune cells are operative in human organ-specic autoimmune diseases has been speculated upon, but has not been proven.
Enhanced susceptibility of target cells for the excessive autoimmune response in the efferent phase
After the excessive generation of autoreactive T cells and IgG autoantibodies, yet another factor or factors, at least in the OS chicken and probably in the NOD mouse, determine whether or not a full-blown autoimmune disease will develop (Wick et al., 1989). A prerequisite for clinical failure is a susceptibility of the target tissue for an autoimmune attack by the generated autoreactive T cells, macrophages and IgG autoantibodies. Experiments have shown that, in the OS chicken, this susceptibility factor is genetically determined, and it has been speculated that this factor might be an abnormality induced by an endogenous retrovirus. Whether such susceptibility factors are also important in human autoimmune disease needs further investigation.
autoimmune arthritis are not spontaneous, but need an articial sensitization. Sensitizing agents, such as microbial antigens (particularly mycobacteria and peptidoglycans of anaerobic bacteria) or other arthritogenic antigens (collagen type II), are used in strains of rats and mice with a genetic tendency to develop the disease, most notably the Lewis rat and the SJL mouse (Melief et al., 1995; van Eden et al., 1996). The proneness to the chronic arthritic autoimmune reaction in the Lewis rat has, amongst other mechanisms, been attributed to subnormal activity of the hypothalamicpituitaryadrenal (HPA) axis, i.e. a low adrenocorticotrophic hormone output and glucocorticoid tonus upon interleukin 1 (IL-l) stimulation of the hypothalamus (Wilder, 1996). Interestingly, the OS chicken, the NOD mouse and the BB rat have similar neuroendocrine abnormalities. The most eye-catching histological nding in human RA synovitis is the development of a secondary lymphoid tissue (pannus) often with active germinal centre reactions in the inamed synovium (Kavanaugh and Lipsky, 1996). In contrast, the arthritis of SLE shows only a very mild synovial inltration. DCs are a conspicuous part of the Tcell zones of this secondary lymphoid tissue in the RA synovium. Specic lymphocyte-homing venules, the high endothelial venules (HEVs), are also components of this synovium-associated lymphoid tissue. Given this histological picture, it is not surprising that increased numbers of T cells and activated DCs can be isolated from RA synovial tissue, and that T and DC-like cell clones have been generated from RA synovial tissue. The synovial DCs are loaded with microbial gut-derived antigens (Melief et al., 1995). These antigens may subsequently be presented to the locally accumulated T cells. Peptidoglycans of the anaerobic gut ora, heat-shock protein (hsp)-like antigens of mycobacteria, and microbial superantigens may all play a role in this intrasynovial expansion of memory T cells. There are also indications that the DCs accumulated in the RA synovium may be abnormal, or in another state of maturation compared with bloodborne DCs: their cluster behaviour with T cells is altered, and the DCT cell clusters fall apart more easily. Nevertheless, DCs present in the RA synovial tissue are excellent accessory cells. In patients suering from RA, there are even signs of a hyperactivity of DC progenitors in the peripheral blood: . There is increased monocyte adhesiveness, integrin expression and cytokine release in patients with RA. . In vitro stimulation of blood precursors with granulocytemacrophage colony-stimulating factor, tumour necrosis factor and stem cell factor produce an increased DC progeny in patients with RA. . IL-1a-containing dendritic-like cells can be found in the peripheral blood of patients with RA in a proportion as high as 7.5%.
Development of Rheumatoid Arthritis: Various Signs of Immunodysregulation
Animal models have provided much insight into the pathogenic process of the systemic autoimmune diseases. However, the experimental animal models of severe
6
ENCYCLOPEDIA OF LIFE SCIENCES / & 2001 Macmillan Publishers Ltd, Nature Publishing Group / www.els.net
Autoimmune Disease: Aetiology and Pathogenesis
The functionally strong local DCT cell interaction in the synovium of patients with RA has its consequences: it creates a milieu with excessive local cytokine production. This cytokine milieu further attracts T cells to the spot, as well as monocytes and macrophages, which accumulate particularly at the periphery of the secondary lymphoid tissues at the synoviumcartilage interphase. The cytokines will also activate these macrophages close to the cartilage and bone to produce IL-1, prostaglandin E2 and other products detrimental to these tissues, leading to at least some of the signs and symptoms of the disease. B cells also inltrate the synovial lymphoid tissue via the newly formed HEVs and will take part in the germinal centre reaction or become plasma cells. Indeed, in the synovial lymphoid tissue of patients with RA, production of autoantibodies does occur (Otten et al., 1993). These autoantibodies are directed, in particular, towards type II collagen or are rheumatoid factors; both are serological hallmarks of RA. Theoretically, epitope spreading from the initial elicitating microbial antigens towards such local autoantigens may be the cornerstone for this autoreactivity in RA. In summary, a local lymphoid tissue (pannus) with a strong germinal centre reaction and macrophage activation in the RA synovium is the hallmark of the disease. Enhanced local DCT-cell interactions, probably involving locally trapped microbial antigens of the gut environment, may be essential for the early pannus formation. Inborn abnormalities in DCs, T cells and B cells, and abnormalities in the HPA axis contribute to the local excessive immune reaction in the synovium. The excessive cytokine, autoantibody and rheumatoid factor production in the pannus are probably the factors leading to cartilage and bone destruction via further local macrophage activation, complement activation and polymorphonuclear cell inltration.
TPO antibody positive (> 100 U ml1) (%)
20
10
1020 2030 3040 4050 5060 6070 7080 8090 Age (years)
Figure 2 Prevalence of thyroperoxidase (TPO) antibody positivity in the normal population according to age and gender. TPO antibodies determined by Lumitest (Henning, Berlin, Germany). Red bars, females; blue bars, males.
Effects of Age and Gender
Some organ-specic (e.g. thyroid and adrenal) and systemic autoimmune diseases (e.g. RA) have a predeliction for the older aged and/or the female gender. This is well illustrated in the prevalence rate of thyroperoxidase (TPO) antibody positivity (a serological sign of mild to severe autoimmune thyroiditis) in the general population (Figure 2). It must, however, also be noted that there are clear exceptions to this rule (e.g. type 1 diabetes). The eect of ageing on the incidence of certain autoimmune diseases is generally ascribed to the decline in immune function in old age, so-called immunosenescence. Signs of immunosenescence are thymus involution, and the involution and brosis of secondary lymphoid tissues. Interestingly, serum levels of dehydroepiandrostenedione (DHEA), which is quantitatively the most
abundant adrenal steroid hormone, also show a steady decline with ageing (Svec, 1997). There are reports showing that when DHEA is administered to aged individuals, whether animals or humans, their immune function is activated: they become more resistant to infections, their secretion of T-cell cytokines is enhanced, and monocyte numbers are increased. There are, however, also reports that refute such immunostimulating action of pharmacological doses of DHEA (Sirrs and Bebb, 1999). In this respect, it is worth noting that DHEA administration does not lead to an attenuation of autoimmune thyroiditis in the ageing BB-DP rat. With regard to the female preponderance in autoimmunity, the mode of action of sex steroids in the spontaneous autoimmune models still remains to be elucidated. Experimental studies show that the course of these autoimmune diseases can be modulated by procedures interfering with sex steroid levels, such as by castration or administration of sex steroids (Homo-Delarche et al., 1991). In chicken and mouse models for autoimmune thyroid disease, oestrogen treatment of female or male animals, as well as castration of male animals, results in increased autoantibody levels. When castrated animals are treated with testosterone, autoantibody levels and autoimmunity decrease again. However, results dier between distinct animal strains. Also, extrapolation of concepts derived from such animal studies to the human situation is problematic, because animal studies in general are performed in a genetically homogeneous population. To illustrate this, we recently completed a study on male to female transsexuals; castration followed by treatment with female hormones of these individuals did not lead to an increased prevalence of TPO antibodies up to the level found in the normal female population.
ENCYCLOPEDIA OF LIFE SCIENCES / & 2001 Macmillan Publishers Ltd, Nature Publishing Group / www.els.net
Autoimmune Disease: Aetiology and Pathogenesis
What are the eects of sex steroids on the normal human immune system? A sexual dimorphism of the immune response has been recognized for some time (HomoDelarche et al., 1991): females in general have a stronger primary and secondary immune response compared with males. Females also have a higher thymus weight and higher serum immunoglobulin concentrations. Moreover, females are more resistant to the induction of immunological tolerance and have a greater ability to reject tumours and allografts. Sex steroids, such as oestrogens and testosterone, may aect leucocyte function directly. Binding sites (probably receptors) for these sex steroids are present in some subpopulations of leucocytes. Moreover, sex steroids can be metabolized in immunocompetent cells, and the intermediary products may inuence the metabolism and function of the cells. The immune eects of sex steroids can be observed particularly during pregnancy. Then, many patients with established autoimmune disease experience an improvement. This applies in particular to thyroid autoimmune diseases and RA. A likely explanation may be found in the increased level of immune tolerance induced by the pregnant state. Adaptation of the immune system of the mother is required to tolerate the fetus immunologically, since the fetus expresses maternal and paternal human leucocyte antigen (HLA) molecules. Despite extensive research, the precise mechanisms of the immune tolerance for these fetal antigens remain unclear. Both local placental and systemic alterations in the immune system contribute to the enhanced tolerance. In early pregnancy, an accumulation of natural killer (NK) cells (with distinctive phenotype CD56 1 CD16 2 CD3 2 ) and of DCs and macrophages occurs in the decidua. These cells are supposed to play a role in the acceptance of the embryo and in the downregulation of the local immune response (Beer et al., 1996). It is well established that these local immune adaptations are associated with various alterations in the number and activity of circulating leucocytes. Recent research further suggests that a normal pregnancy is accompanied by a shift from predominant TH1 to predominant TH2 immune responses to avoid rejection of the antigenically foreign fetus by a cell-mediated immune attack (Wegmann et al., 1993). The shift towards a TH2 response may be triggered by increased circulating levels of 17b-oestradiol and progesterone during pregnancy. The NK cell cytotoxicity is inversely correlated with serum 17boestradiol levels and, in vitro, is inhibited by diethylstilboestrol and enhanced by the oestrogen receptor antagonist tamoxifen. Apart from these sex steroids, placental human chorionic gonadotrophin (HCG)-like gonadotrophins may also play a role in pregnancy-associated immune alterations. Together, these incompletely understood immune alterations apparently lead to an amelioration of some of the existing autoimmune syndromes.
Effects of Environmental Factors
In addition to internal factors such as genotype, gender and age, environmental factors also play a role in the pathogenesis of autoimmune disease. The most important of these external factors are infectious agents, dietary intake, toxic agents and stress.
Infectious agents
The role of infectious agents from the gut in the development of RA was discussed above. With regard to the role of infectious agents in organ-specic autoimmune diseases, noteworthy studies have been carried out in type 1 diabetes and autoimmune thyroiditis. Epidemiological studies have suggested a negative correlation between the pathogen weight in a population and the incidence of type 1 diabetes. In NOD mice and BBDP rats, vaccination with Mycobacterium bovis, strain rin (BCG), or Mycobacterium Bacillus CalmetteGue tuberculosis-containing preparations protect from developing diabetes in the animals, provided the treatment is initiated during the rst 2 weeks of life. Staphylococcal enterotoxins have also been shown to prevent diabetes in NOD mice. Viruses can prevent diabetes too, and a plethora of viral strains such as EMCV-B, Lymphochoriomeningitis virus (LCMV) and others have been shown to interfere favourably with diabetes development in the rodent models of the disease. Although the mechanisms behind this protection are far from clear, it has been suggested that the viruses or bacteria act via antigenic competition, or via a direct superantigenic stimulation of T cells, releasing antiinammatory cytokines. Independently of these potential protective roles, viruses and bacteria can also play a disease-promoting role. At least four mechanisms may contribute to autoimmune pathogenesis in this respect: 1. A virus may specically infect a b cell or a thyrocyte, leading to destruction of the cell. In this way, a nonspecic inammation of the target is induced, attracting APCs, which subsequently trigger an autoimmune response in susceptible (immunodysregulated) hosts (see above). Insulinotrophic viruses include EMCV-D, reoviruses, rubella and various enteroviruses, most notably Coxsackie B virus (Horwitz et al., 1998). Thyrotrophic viruses are less well known, yet reoviruses may infect thyrocytes. Particular attention should be paid to an earlier observation that nuclear core (gag)-2 protein-like material of Human foamy retrovirus is specically present in Graves thyrocytes, Graves orbital broblasts and Graves orbital fat cells. 2. Viral or bacterial proteins sometimes share sequences with important organ-specic autoantigens. This has been suggested for Coxsackie B virus and glutamic acid
ENCYCLOPEDIA OF LIFE SCIENCES / & 2001 Macmillan Publishers Ltd, Nature Publishing Group / www.els.net
Autoimmune Disease: Aetiology and Pathogenesis
decarboxylase (GAD), but has recently been disputed. Cross-reactivity (mimicry) has also been suggested between Yersinia enterocolitica serotype 3 and the thyroid-stimulating hormone receptor. Cross-reactive epitopes could bypass existing T-cell tolerance to autoantigens to give rise to autoimmune responses. 3. A virus could induce the expression of neoantigens by future target cells. Reovirus type 1 induces an antibody-positive lymphocytic thyroiditis in mice. The infection is thought to introduce new epitopes next to, or as part of, thyroid autoantigens. This makes an immune reaction possible to these new epitopes, additionally eliciting an immune reaction to the coupled or adjacent thyroid autoantigen (bypass mechanism). 4. Finally, viruses and bacteria may directly inuence the cells of the immune system, thus disturbing the delicate immune regulatory balance. Avian leucosis virus induces a lymphocytic thyroiditis with germinal centres in fetally infected chickens. The virus infects stem cells of the immune system, and has a direct eect on thymus and bursa development. Retroviruses and bacterial products might also disturb the immune balance by acting as superantigens, which causes expansion of subsets of T cells with T-cell receptors containing particular Vb chains. It is conceivable that such T cells would include autoimmune reactive TH1 or TH2 cells.
Dietary factors
A second source of exogeneous factors contributing to autoimmune pathogenesis is constituted of specic food components. Both iodine excess and iodine deciency are capable of disturbing the tolerance for thyroid autoantigens that exist in the healthy state. This sometimes leads to clinically overt thyroid autoimmune disease. An acute excessive iodine intake (e.g. the iodine treatment after the Chernobyl incident) in individuals with a predisposition for thyroid autoimmune disease induces a rise in the titre of TPO and thyroglobulin antibodies, and an outburst of Hashimoto-like lymphocytic thyroiditis in a proportion of such individuals with increased susceptibility. Proposed pathogenic mechanisms are: . An iodine-induced thyrocyte necrosis with a concomitant attraction of DCs and macrophages, and a release of autoantigens. . A higher antigenicity of thyroglobulin due to a higher iodination grade. . An enhanced maturation of DCs from monocytes due to a stimulating eect of iodinated compounds. . A direct stimulation of B cells, T cells and macrophage peroxidase activity by iodine.
Any of these mechanisms may, by itself or in combination, break the existing tolerance for thyroid autoantigens and cause disease development. Iodine deciency induces goitre formation and a diminished thyroid hormone production. In aected populations this leads to disease entities such as endemic goitre and endemic cretinism. In these environmentally induced thyroid disorders, local thyroid autoimmune phenomena have been described. These phenomena include an intrathyroidal DC accumulation and clustering, and a rise in the titre of anti-TPO and antithyroglobulin antibodies. In the BB-DP rat, a mild iodine deciency leads to acceleration of the disease. Severe iodine deciency leads, however, to a severe immunodeciency in this animal, and hence to an ameloriation of the thyroid autoimmune response. In the induction of type 1 diabetes, dietary factors also play an important role. Standard rodent chow contains wheat, soybeans and alfalfa, which are probably all trigger factors for diabetes in the BB-DP rat and NOD mouse. Biochemical analysis has suggested that the proteins or the peptides of these food components might be the triggering factors. Indeed, protein- and peptide-free diets, as well as diets with restricted amounts of essential fatty acids, prevent the development of diabetes in the BB-DP rat. The addition of 1% gliadin or 1% skim milk to a protein-free diet partially abrogates its protective eect. Furthermore, a diet containing hydrolysed casein as an amino acid source also prevents diabetes in NOD mice and BB rats. Recently, an alteration of the intra-islet cytokine prole has been found in these alternatively fed BB-DP rats, suggesting that diet-induced disease protection is the result of the activation of immune cells with a suppressor function. In NOD mice, this diet elicits spleen cells that interfere with diabetes development in an adoptive transfer experiment. In humans, evidence is emerging that a premature introduction of dietary proteins (and in particular dairy proteins) accelerates type 1 diabetes development in susceptible children (Akerblom and Knip, 1998). With regard to the mechanisms underlying the association between the intake of dairy products and type 1 diabetes, two main concepts have emerged (Kolb and Pozzilli, 1999): 1. An antigenic mimicry has been suggested between bovine serum albumin (BSA) and one of the identied islet cell autoantigens, namely ICA-69. The shared epitope is the ABBOS peptide. In this concept, BSAcontaining diets sensitize susceptible individuals to ICA-69 via the gut immune system. In support of this view, recent-onset type 1 diabetics often show raised antibody titres to BSA. 2. A second concept proposes that digestion of bovine casein with intestinal enzymes yields a bioactive peptide with opioid properties including stimulating eects on immune cells. Digestion of human caseins does not produce such a peptide. It is thus conceivable
9
ENCYCLOPEDIA OF LIFE SCIENCES / & 2001 Macmillan Publishers Ltd, Nature Publishing Group / www.els.net
Autoimmune Disease: Aetiology and Pathogenesis
that (early) introduction of bovine caseins would disturb the developing mucosal immune system in such a way that pancreatic autoimmunity also develops more rapidly. It must, however, also be kept in mind that any particular change in diet inuences the composition of the gut ora. The acidalkali balance of the alimentary tract will be inuenced, and consequently the balance between the anaerobic and aerobic ora and the proneness to enteroviral infection. It is thus conceivable that the mucosal immune system is triggered via such mechanisms, and that this contributes to the development of type 1 diabetes or RA.
Also a heavy metal, such as mercury, is able to induce a SLE-like syndrome and nephritis in rats. Mechanisms underlying such autosensitization are still poorly understood. Possibly, the physical coupling of the drugs to cells and cell membranes creates neo-epitopes, recognized as foreign by the immune system. Alternatively, these drugs may directly inuence cells of the immune system, leading to the disturbance of the delicate balance between responsiveness and tolerance.
Stress
A nal putative external factor that modulates autoimmune pathogenesis is stress. BB rats exposed to daily stress, such as rotation, vibration or restraint stress, develop diabetes with a higher incidence than unaected control animals. In contrast, in NOD mice, chronic stress introduced between 6 and 8 weeks of age, as well as repeated injections of saline, decreases the incidence of diabetes. Prenatal stress, however, accelerates the onset of diabetes (Homo-Delarche et al., 1991). These examples illustrate the complex eects of stressors. It is suspected that stressors modulate the development of organ-specic autoimmunity by altering setpoints in the HPA axis and the IL-l system. This notion is supported by recent ndings in patients with manic-depressive psychosis and severe melancholia. In these patients, the immune system is severely dysregulated, and the HPA axis and IL-1 system are grossly activated. Interestingly, the incidence of TPO antibodies is high in such patients.
Toxic agents or drugs
Chemical toxins or drugs constitute a third source of pathogenic factors in the development of autoimmunity. Exposure to methylcholanthrene enhances the thyroid autoimmune response in Bualo rats, a strain of rats genetically susceptible to experimentally induced autoimmune thyroid disease. Methylcholanthrene is thought to have a direct toxic action on the immunoregulatory system rather than on the thyroid tissue of the rats. Among other toxic factors, components from tobacco smoke have appeared to be most important in the development of Graves disease and autoimmune thyroiditis. In the UK, almost two-thirds of patients with Graves ophthalmopathy smoke cigarettes, in contrast to 1020% of the normal healthy population. The mechanisms behind the association are not clear. Smoking might lead to immune dysregulations akin to the alterations seen in inherited forms of thyroid autoimmune disease. As such, smoking does lead to clear alterations in DC and macrophage function in the lung environment, and to an altered production of proinammatory cytokines in the lung. Whether this is reected in systemic monocyte, DC and macrophage dysfunction, or in a dysfunction of such cells in the thyroid, needs to be investigated. Alternatively, smoking might also lead to thyrocyte necrosis or thyroid metabolic abnormalities, processes that might also be driving forces behind a thyroid-specic autoimmunization. Concerning type 1 diabetes induction, several agents and drugs (e.g. streptozotocin, alloxan and N-3-pyridyl methyl-N1-p-nitrophenyl urea (rodenticide vacor) are toxic to b cells and able to induce insulitis and diabetes in rats and mice. In diabetes-prone animal models, such as the NOD mouse or the BB-DP rat, the compounds amplify and accelerate the autoimmune response towards the b cells. Also, systemic autoimmunity, in particular SLE, is inuenced by chemical compounds. Certain drugs, such as a-methyldopamine, hydralazine, procainamide and antiepileptics, are able to elicit so-called drug-induced SLE.
10
Conclusion
Autoimmune diseases are complex, polygenic aictions of which the penetrance is heavily dependent on various environmental inuences. In their pathogenesis, an aerent stage (enhanced autoantigen presentation), a central stage (excessive expansion and maturation of autoreactive T and B cells) and an eerent stage (eects of autoreactive T and B cells on their targets) can be discerned. In each stage, a plethora of inborn, endogenous or exogenous factors is able to elicit the abnormalities characteristic of that stage, thus opening the gateway to autoimmunity. Only unfortunate combinations of genetic susceptibility and exogenous factors thus lead to full-blown disease.
References
Akerblom HK and Knip M (1998) Putative environmental factors in type 1 diabetes. Diabetes Metabolism Reviews 14: 3167. Bach JF and Mathis D (1997) The NOD mouse. Research in Immunology 148: 285286. Beer AE, Kwak JYH and Ruiz J (1996) Reproductive immunology. In: Rich RR, Fleisher TA, Schwartz BD et al. (eds) Clinical Immunology: Principles and Practice, pp. 15371540. St Louis: Mosby Year Book.
ENCYCLOPEDIA OF LIFE SCIENCES / & 2001 Macmillan Publishers Ltd, Nature Publishing Group / www.els.net
Autoimmune Disease: Aetiology and Pathogenesis
Delemarre FGA, Simons PJ, Drexhage HA (1996) Histomorphological aspects of the development of thyroid autoimmune disease: consequences for our understanding of endocrine ophthalmopathy. Thyroid 6: 369377. Drexhage HA, Delemarre FGA, Rados evic K and Leenen PJM (1999) Dendritic cells in autoimmunity. In: Lotze MT and Thomson AW (eds) Dendritic Cells. Biology and Clinical Applications, pp. 361401. San Diego: Academic Press. van Eden W, Anderton SM, van der Zee A et al. (1996) (Altered) self peptides and the regulation of self reactivity in the peripheral T cell pool. Immunological Reviews 149: 5573. Hoek A, Allaerts W, Leenen PJM, Schoemaker J and Drexhage HA (1997) Dendritic cells and macrophages in the pituitary and the gonads. Evidence for their role in the ne regulation of the reproductive endocrine response. European Journal of Endocrinology 136: 824. Homo-Delarche F (1997) Beta-cell behaviour during the prediabetic stage. Part II. Non-insulin-dependent and insulin-dependent diabetes. Diabete et Metabolisme 23: 473505. Homo-Delarche F, Fitzpatrick F, Christe N et al. (1991) Sex steriods, glucocorticoids, stress and autoimmunity. Journal of Steroid Biochemistry and Molecular Biology 40: 619637. Horwitz MS, Bradley LM, Harbertson J et al. (1998) Diabetes induced by Coxsackie virus: initiation by bystander damage and molecular mimicry. Nature Medicine 4: 781785. Kavanaugh AF and Lipsky PE (1996) Rheumatoid arthritis. In: Rich RR, Fleisher TA, Schwartz BD, Shearer WT and Strober W (eds) Clinical Immunology: Principles and Practice, vol. II, pp. 10931116. St Louis: Mosby. Kolb H and Pozzilli P (1999) Cows milk and type I diabetes: the gut immune system deserves attention. Immunology Today 20: 108110. Leenen PJM and Campbell PA (1993) Heterogeneity of mononuclear phagocytes. An interpretative review. In: Horton MH (ed.) Blood Cell Biochemistry, vol. 5, pp. 2984. New York: Plenum Press.
Melief MJ, Hoijer MA, van Paasen HC and Hazenberg MP (1995) Presence of bacterial ora-derived antigen in synovial tissue macrophages and dendritic cells. British Journal of Rheumatology 34: 1112 1116. Otten HG, Daha MR, Dolhain RJ et al. (1993) Rheumatoid factor production by mononuclear cells derived from dierent sites of patients with rheumatoid arthritis. Clinical Experimental Immunology 94: 236240. Peters JH, Gieseler R, Thiele B and Steinbach F (1996) Dendritic cells: from ontogenetic orphans to myelomonocytic descendants. Immunology Today 17: 273278. Shresta S, Smyth JR Jr and Erf GF (1997) Proles of pulp inltrating lymphocytes at various times throughout feather regeneration in Smyth line chickens with vitiligo. Autoimmunity 25: 193201. Sirrs SM and Bebb RA (1999) DHEA: panacea or snake oil. Canadian Family Physician 45: 17231728. Sundick RS, Bagchi N and Brown TR (1996) The obese strain chicken as a model for human Hashimotos thyroiditis. Experimental and Clinical Endocrinology and Diabetes 104: 46. Svec F (1997) Ageing and adrenal cortical function. Baillie`res Clinical Endocrinology and Metabolism 11: 271287. Todd JA and Farrall M (1996) Panning for gold: genome wide scanning for linkage in type 1 diabetes. Human Molecular Genetics 5: 1443 1448. Wegmann TG, Lin H, Guilbert L and Mosmann TR (1993) Bidirectional cytokine interactions in the maternalfetal relationship: is successful pregnancy a Th2 phenomenon? Immunology Today 14: 353356. Wick G, Brezinschek HP, Hala K et al. (1989) The obese strain of chickens: an animal model with spontaneous autoimmune thyroiditis. Advances in Immunology 47: 433500. Wilder RL (1996) Hormones and autoimmunity: animal models of arthritis. Ballie`res Clinical Rheumatology 10: 259271. Yoon JW (1990) The role of viruses and environmental factors in the induction of diabetes. Current Topics in Microbiology and Immunology 164: 95123.
ENCYCLOPEDIA OF LIFE SCIENCES / & 2001 Macmillan Publishers Ltd, Nature Publishing Group / www.els.net
11
Вам также может понравиться
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Easy Anti Inflammatory Diet - Fast and Simple Recipes For The 15 Best Anti-Inflammatory Foods (PDFDrive)Документ247 страницThe Easy Anti Inflammatory Diet - Fast and Simple Recipes For The 15 Best Anti-Inflammatory Foods (PDFDrive)Rogerio AraujoОценок пока нет
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Innoculations The True Weapons of Mass DestructionДокумент3 страницыInnoculations The True Weapons of Mass DestructionRedza100% (3)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Jean Seignalet DietДокумент28 страницJean Seignalet Dietdevabakhti100% (2)
- Reader's Digest Asia - August 2023Документ116 страницReader's Digest Asia - August 2023Jeena Jabez100% (1)
- Bioplasm-NLS Use Manual (Training) - InglesДокумент136 страницBioplasm-NLS Use Manual (Training) - InglesMarcus Vinicius RibeiroОценок пока нет
- Paleo Book PDFДокумент679 страницPaleo Book PDFsindza100% (17)
- Plant Macro-And Micronutrient MineralsДокумент5 страницPlant Macro-And Micronutrient Mineralsmanoj_rkl_07Оценок пока нет
- 2,4-Thiazolidinedione As Antimicrobial and Cytotoxic AgentsДокумент10 страниц2,4-Thiazolidinedione As Antimicrobial and Cytotoxic Agentsmanoj_rkl_07Оценок пока нет
- BMP Antags &nural Inducna0000805-001-000 PDFДокумент5 страницBMP Antags &nural Inducna0000805-001-000 PDFmanoj_rkl_07Оценок пока нет
- Ca Binding Proteins A0001347-001-000 PDFДокумент8 страницCa Binding Proteins A0001347-001-000 PDFmanoj_rkl_07Оценок пока нет
- Evolution of Genome Organizn1699-001-000 PDFДокумент5 страницEvolution of Genome Organizn1699-001-000 PDFmanoj_rkl_07Оценок пока нет
- Ephrins: Ru Diger KleinДокумент6 страницEphrins: Ru Diger Kleinmanoj_rkl_07Оценок пока нет
- Electroporation: Jac A NickoloffДокумент3 страницыElectroporation: Jac A Nickoloffmanoj_rkl_07Оценок пока нет
- Evolution of Ecosystems - Terrestrial PDFДокумент4 страницыEvolution of Ecosystems - Terrestrial PDFmanoj_rkl_07Оценок пока нет
- Evolution of Development A0001661-001-000 PDFДокумент4 страницыEvolution of Development A0001661-001-000 PDFmanoj_rkl_07Оценок пока нет
- DNA Repair by Reversal of Damage PDFДокумент8 страницDNA Repair by Reversal of Damage PDFmanoj_rkl_07100% (1)
- Cyanogenesis in Higher Plant and InsectsДокумент3 страницыCyanogenesis in Higher Plant and Insectsmanoj_rkl_07Оценок пока нет
- Electron Carriers PDFДокумент8 страницElectron Carriers PDFmanoj_rkl_07100% (1)
- Calibration of A Transillumanator For UV Fixation of DNA To PDFДокумент2 страницыCalibration of A Transillumanator For UV Fixation of DNA To PDFmanoj_rkl_07Оценок пока нет
- DNA Damage: Paul W DoetschДокумент7 страницDNA Damage: Paul W Doetschmanoj_rkl_07Оценок пока нет
- Genetic Code Introduction PDFДокумент10 страницGenetic Code Introduction PDFmanoj_rkl_07Оценок пока нет
- Immunologival Tolerance Therpeutic Induction PDFДокумент6 страницImmunologival Tolerance Therpeutic Induction PDFmanoj_rkl_07Оценок пока нет
- FGF1Документ9 страницFGF1manoj_rkl_07Оценок пока нет
- Forward-Cristopher Reeve PDFДокумент1 страницаForward-Cristopher Reeve PDFmanoj_rkl_07Оценок пока нет
- Flocyt Anal Nstem Cel in DevДокумент11 страницFlocyt Anal Nstem Cel in Devmanoj_rkl_07Оценок пока нет
- Phyllosphere PDFДокумент8 страницPhyllosphere PDFmanoj_rkl_07Оценок пока нет
- Capillary Blotting of RNA and DNA Gels PDFДокумент3 страницыCapillary Blotting of RNA and DNA Gels PDFmanoj_rkl_07Оценок пока нет
- Heavy Metal Adaptation PDFДокумент4 страницыHeavy Metal Adaptation PDFmanoj_rkl_07Оценок пока нет
- Dideoxy Sequencing of DNA PDFДокумент16 страницDideoxy Sequencing of DNA PDFmanoj_rkl_07Оценок пока нет
- Calibration of A Transillumanator For UV Fixation of DNA To PDFДокумент2 страницыCalibration of A Transillumanator For UV Fixation of DNA To PDFmanoj_rkl_07Оценок пока нет
- Dideoxy Sequencing of DNA PDFДокумент16 страницDideoxy Sequencing of DNA PDFmanoj_rkl_07Оценок пока нет
- Closteroviridae: Historical PerspectiveДокумент6 страницClosteroviridae: Historical Perspectivemanoj_rkl_07Оценок пока нет
- Gertrude Belle Elion PDFДокумент1 страницаGertrude Belle Elion PDFmanoj_rkl_07Оценок пока нет
- Heavy Metal Adaptation PDFДокумент4 страницыHeavy Metal Adaptation PDFmanoj_rkl_07Оценок пока нет
- Root Nodules (Rhizobium Legumes) PDFДокумент2 страницыRoot Nodules (Rhizobium Legumes) PDFmanoj_rkl_07Оценок пока нет
- Terpenoids Lower PDFДокумент7 страницTerpenoids Lower PDFmanoj_rkl_07Оценок пока нет
- Tesi Dottorato Catamo - PHDДокумент87 страницTesi Dottorato Catamo - PHDkamil mahdiОценок пока нет
- A Comparative Study of Erythrocyte Sedimentation Rate (Esr) UsingДокумент5 страницA Comparative Study of Erythrocyte Sedimentation Rate (Esr) UsingRaffaharianggaraОценок пока нет
- Parasite DetoxДокумент42 страницыParasite Detoxedurodica7Оценок пока нет
- Dr. Nanang PB 00 Autoimmune Disease Planary KONAS Bandung 2014Документ60 страницDr. Nanang PB 00 Autoimmune Disease Planary KONAS Bandung 2014Anton HilmanОценок пока нет
- Autoimmune DiseaseДокумент3 страницыAutoimmune DiseasePearl AudeОценок пока нет
- Clinical Atlas of Canine and Feline Dermatology - 2019 - Coyner - IndexДокумент12 страницClinical Atlas of Canine and Feline Dermatology - 2019 - Coyner - Indexnabal22Оценок пока нет
- Ditmar - Enzyme TherapyДокумент10 страницDitmar - Enzyme TherapyniobiyОценок пока нет
- Aging Archives - DR William LiДокумент6 страницAging Archives - DR William LiMariana GrecuОценок пока нет
- Leukocytosis LeukopeniaДокумент4 страницыLeukocytosis LeukopeniandrfernandezОценок пока нет
- Rheumatoid ArthritisДокумент16 страницRheumatoid ArthritisDeepak GhimireОценок пока нет
- Catalog Werfen Reagent - Tiếng AnhДокумент24 страницыCatalog Werfen Reagent - Tiếng AnhDau TranvanОценок пока нет
- C1933-GL Global Pharmaceuticals Medicine Manufacturing Industry ReportДокумент69 страницC1933-GL Global Pharmaceuticals Medicine Manufacturing Industry Reportsamuel.p.collingsОценок пока нет
- Alopecia Areata in Covid 19 Case ReportДокумент2 страницыAlopecia Areata in Covid 19 Case ReportAnti TjahyaОценок пока нет
- Autoimmune Hepatitis HandoutДокумент2 страницыAutoimmune Hepatitis HandoutClarisse SantosОценок пока нет
- Lymphatic & Body DefensesДокумент11 страницLymphatic & Body DefensesJeah LourraineОценок пока нет
- Immunology Mcqs-4: InstructionsДокумент22 страницыImmunology Mcqs-4: InstructionsadehkordiОценок пока нет
- Body SystemsДокумент116 страницBody SystemskarunaОценок пока нет
- Autoimmune DisordersДокумент6 страницAutoimmune DisordersMaquille Ann CervalesОценок пока нет
- The Philippine Medicines Policy 2017 202Документ82 страницыThe Philippine Medicines Policy 2017 202Ren PastelОценок пока нет
- Cause of DiseaseДокумент29 страницCause of DiseaseTariku olanaОценок пока нет
- What Is An Autoimmune DiseaseДокумент7 страницWhat Is An Autoimmune DiseaseBISHOP MBILIОценок пока нет
- Prurigo-Nodular Ro 383Документ10 страницPrurigo-Nodular Ro 383Alexandru Ionut SavuОценок пока нет
- Immunology TA v.01 Paramita Mycomments v.01Документ80 страницImmunology TA v.01 Paramita Mycomments v.01Miral Sandipbhai MehtaОценок пока нет
- Immunology - 2022 - Chen - New Onset Autoimmune Phenomena Post COVID 19 Vaccination-1Документ17 страницImmunology - 2022 - Chen - New Onset Autoimmune Phenomena Post COVID 19 Vaccination-1Ivan StojanovicОценок пока нет