Академический Документы
Профессиональный Документы
Культура Документы
Prelims
Загружено:
Jess FabraИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Prelims
Загружено:
Jess FabraАвторское право:
Доступные форматы
TOPIC: Ischemic Heart Disease
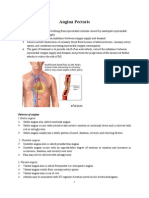
THERAPEUTIC DIFFICULTY: Level 3 Kevin M. Sowinski and Brian R. Overholser Scenario Patient and Setting: AD, a 60-year-old woman presents for follow-up at cardiology clinic Chief Complaint: Follow-up appointment for coronary artery disease/post-myocardial infarction care; presents with increasing chest pain, shortness of breath, and leg swelling History of Present Illness Presents to cardiology clinic complaining of increased chest pain after climbing two flights of stairs or walking three blocks. All episodes of chest pain are relieved by sublingual nitroglycerin. AD reports that they occur a bit more often than before her myocardial infarction (MI); also complains of occasional shortness of breath, mainly when climbing stairs or walking, swelling in her ankles and lower legs, and having to get up several times during the night to go to the bathroom; she claims that the shortness of breath and leg swelling are new and have been occurring over the past several weeks. Medical History: Came to the emergency department 6 months ago with an anterior-wall MI; received fibrinolytic therapy for the MI; has a long history of uncontrolled hypertension. Surgical History: Tonsillectomy and adenoidectomy, age 9; appendectomy, age 22 Family/Social History: Family History: Mother died at age 55 of lung cancer; father died at age 61 of heart failure Social History: Married with three children, all alive and well; active smoker, has smoked approximately one and a half packs of cigarettes per day for 40 years; drinks alcohol occasionally (- 12 drinks per day, 5 x a week) Medications: Aspirin, 325 mg PO daily Atenolol, 50 mg PO once daily Nitroglycerin, 0.4 mg SL as needed for chest pain Nifedipine XL, 30 mg PO daily Hydrochlorothiazide (HCTZ), 50 mg PO twice daily Potassium chloride, 10 mEq PO daily Beclomethasone nasal inhaler Conjugated estrogens, 0.625 mg PO daily Medroxyprogesterone acetate, 2.5 mg PO daily Allergies: PCN and novocaine Physical Examination GEN: Slightly obese female, in moderate distress, increased leg edema, nocturia, and SOB VS: BP 145/105, HR 85, T 37.3, RR 24, Wt 80 kg, Ht 158 cm HEENT: AV nicking and narrowing, retinal exudates COR: Normal S1, S2, + S3, and + S4 with gallop, + JVD, + HJR CHEST: Bilateral rales ABD: Soft, nontender, hepatomegaly, abdominal striae GU: Deferred RECT: Heme (-) EXT: 1+ ankle edema NEURO: WNL
Results of Pertinent Laboratory Tests, Serum Drug Concentrations, and Diagnostic Tests
Na 137 (137) Hct 0.37 (37) AST 0.42 (25) K 4.7 (4.7) Hgb 123 (12.3) ALT 0.32 (19) Cl 103 (103) Lkcs 4.8 x 109 (4.8 x 103) LDH 1.30 (78) HCO3 23 (23) Plts 220 x 109 (220 x 103) Ca 2.27 (9.1) BUN 8.57 (24) PO41.0 (3.2) SCr 177 (2.0) Cholesterol Panel (7 months ago) Mg 0.9 (1.8) Glu 7.05 (127) TC: 249 mg/dL LDL-C: 155 mg/dL HDL-C: 38 mg/dL TG: 280 mg/dL ECG: Old Q waves in leads V1V4, voltage changes consistent with LVH, rate of 85 bpm with occasional premature ventricular contractions
Problem List Identify principal problems from the scenario in priority order (see Answers in back of book for correct list of problems). 1. Coronary artery disease (ischemic heart disease) 2. Coronary artery disease (post-MI/secondary prevention) 3. Heart failure 4. Hypertension 5. Dyslipidemia 6. Renal insufficiency 7. Allergic rhinitis SOAP Note To be completed by the student (see Answers in back of book for correct SOAP Note). SOAP NOTE S: AD complaining of increased chest pain after climbing two flights of stairs or walking three blocks; also complains of leg edema, nocturia, and shortness of breath; all episodes of chest pain are relieved by sublingual nitroglycerin. O: Wt 80 kg, Ht 158 cm, calculated BMI -32, ECG shows occasional premature ventricular contractions. Positive S3, positive S4 with gallop, positive JVD, hepatomegaly, bilateral rales, and 1+ ankle edema, BP 145/105, AV nicking and narrowing, retinal exudates; SCr 177 mmol/L (2.0 mg/dL), BUN 8.57 mmol/L (24 mg/dL) Cholesterol Panel (7 months ago) TC: 249 mg/dL LDL-C: 155 mg/dL HDL-C: 38 mg/dL TG: 280 mg/dL A: PROBLEM 1: Coronary artery disease/chronic stable angina: AD currently receiving atenolol (in addition to providing protection from sudden cardiac death post-MI), nifedipine XL chronically, and sublingual nitroglycerin acutely for anginal symptoms; complaining of increased chest pain after climbing two flights of stairs or walking several blocks; episodes of chest pain are relieved by nitroglycerin; also complaining of new-onset heart failure symptoms. Both increased chest pain and heart failure symptoms can be suggestive of worsening ischemia. Atenolol is appropriate treatment for preventing angina in patients with coronary disease but is not indicated to treat heart failure, which is now likely present in AD. Available choices are metoprolol XL, carvedilol, and bisoprolol (although bisoprolol is not approved in the United States for heart failure treatment). Goal resting heart rate is 50 to 60 bpm; current resting heart rate is 85
bpm. Nifedipine XL is reasonable choice for preventing angina (and treating hypertension) but does not reduce the risk of future events in a patient with a history of MI, nor do any data exist regarding its use in patients with heart failure. In addition, nifedipine XL is associated with a high incidence of peripheral edema If a dihydropyridine calcium channel blocker is desired, either amlodipine or felodipine would be more appropriate as both have been used safely in heart failure patients. AD appears to be taking the sublingual nitroglycerin appropriately, as it is relieving her symptoms. P: PROBLEM 1: Coronary Artery Disease (Ischemic Heart Disease) Change atenolol 50 mg daily to metoprolol XL 50 mg daily and titrate to goal of 100 to 200 mg daily (based on heart failure symptoms) and/or heart rate of 50 to 60 bpm at rest (ischemic heart disease). Discontinue nifedipine XL. Educate AD regarding cardiovascular risk factor reduction: HTN treatment, cholesterol management, dietary modification, exercise, and smoking cessation. Educate about the risk factors of coronary artery disease and stress smoking cessation, weight control, and medication compliance. Continue sublingual nitroglycerin as needed. Remind AD to continue to keep track of the number of anginal attacks and the number of weekly sublingual nitroglycerin tablets used. If exhibiting anginal symptoms on current -blocker therapy, consider adding a long-acting nitrate (ISDN 10 mg tid, NTG patch daily, ISMN 20 mg bid, etc.); coordinate hypertension and anginal symptom control by using agents that benefit both disease states. PROBLEM 2: Coronary artery disease/post-MI/ secondary prevention: In addition to treatment of her underlying angina secondary to her coronary artery disease, AD requires therapy to reduce the risk of a second MI or death secondary to coronary artery disease; currently receiving aspirin and atenolol for this purpose. However, other drugs are indicated for this purpose that she is not receiving, including ACE inhibitors, aldosterone antagonists, and HMG CoA-reductase inhibitors (statins). Because she likely has left-ventricular systolic dysfunction, the ACE inhibitor is indicated, although the use of an aldosterone antagonist (e.g., eplerenone) is controversial and less clear. Statins are discussed below in Problem 4, dyslipidemia. AD is receiving estrogen replacement therapy for an unknown reason, either treatment of dyslipidemia or postmenopausal symptoms. Data suggest that hormone replacement therapy is indicated only for reducing postmenopausal symptoms, not for the prevention of future coronary events or dyslipidemia. These agents should be used for the shortest possible duration due to their risk of increasing vascular events in patients with vascular disease. The issue of dyslipidemia will be addressed in Problem 4. Finally, based on the American College of Cardiology/American Heart Association 2002 guidelines, the approach to coronary artery disease (chronic stable angina/post-MI/secondary prevention) should follow the
mnemonic ABCDE: A (anti-anginals and aspirin), B (blockers and blood pressure), C (cholesterol and cigarettes), D (diet and diabetes treatment), and E (education and exercise). Given ADs underlying conditions (obesity as defined by BMI >30, hypertension, and dyslipidemia) and behaviors (smoking), these should be addressed; she also requires appropriate education regarding her disease and drug regimen and the importance of exercise. PROBLEM 2: Coronary Artery Disease (Post-MI/ Secondary Prevention) See plan for Problem 1 above. Change EC ASA from 325 mg to 81 mg daily. See ACE inhibitor therapy below. See lipid-lowering therapy below. PROBLEM 3: Heart failure: ADs heart failure is secondary to coronary artery disease/acute MI and longstanding hypertension; she complains of new symptoms associated with heart failure. Given previous MI history, it is presumed to be associated with systolic dysfunction. However, evaluation of systolic function (ejection fraction measurement) is essential to determine appropriate therapy. The following discussion of treatment will be based on the assumption that reduced left-ventricular systolic function has been observed. Given the sppearance of heart failure symptoms, she is currently receiving suboptimal diuretic therapy with HCTZ. Diuretic therapy likely is suboptimal for several reasons: first, estimated CrCl of -25 mL per min, and second, thiazide diuretics usually do not provide adequate control of heart failure symptoms except in patients with mild heart failure. Given the dose of HCTZ that she is currently receiving (50 mg BID), increasing the dose is not an option. Most heart failure patients require loop diuretic therapy to reduce heart failure symptoms. Because of the presence of reduced renal function she may require higher doses of loop diuretics than would be required in patients with normal renal function. AD is not receiving ACE inhibitor therapy, which should be initiated and titrated to the target dose immediately. The selection of one particular ACE inhibitor over another is most likely not important in terms of clinical benefits, although regimen and cost are important issues to consider. The addition of ACE inhibitor therapy will also be beneficial in treating the patients hypertension and for reducing remodeling following an acute MI. As described above, since heart failure symptoms are present, -blocker therapy should be changed to either metoprolol XL or carvedilol, since all -blockers are effective for reducing ischemia, but only carvedilol and metoprolol XL are approved for treating heart failure. Given the discussion above regarding nifedipine XL, other dihydropyridine calcium channel blockers are more appropriate in a patient with concomitant heart failure, namely amlodipine or felodipine. The ACE inhibitor and the increase in blocker dose will replace the nifedipine for hypertension treatment. If AD continues to have anginal symptoms on the -blocker therapy alone, either addition of a long-acting nitrate or appropriate calcium channel blocker (felodipine or amlodipine) will be necessary.
PROBLEM 3: Heart Failure Discontinue HCTZ; start furosemide 40 mg QAM. Discontinue Procardia XL. Start enalapril 2.5 mg BID (or captopril 12.5 mg TID or lisinopril 5 mg QD). Since it is likely that all ACE inhibitors are effective in this area, choice of one agent should be based on compliance (once daily versus multiple doses), cost, and other issues. Assess ACE inhibitor therapy in 1 week; measure BP and serum K, BUN, and Cr and adjust therapy accordingly. Goal doses: enalapril 5 mg PO BID; lisinopril 10 mg daily; captopril 25 mg TID (due to reduced renal function), and the dose should be titrated up over several weeks. Discontinue the potassium supplement due to ACE inhibitor therapy in a patient with renal insufficiency; consider need for chronic potassium therapy when the goal dose of ACE inhibitor is achieved. PROBLEM 4: Hypertension: Longstanding, uncontrolled HTN. End-organ damage is evidenced by AV nicking and narrowing, retinal exudates, and poor renal function. Given the accompanying coronary artery disease, the JNC-VII guidelines suggest a goal BP of 130/85 to 140/90 mm Hg. However, because of the accompanying reduced renal function, the JNC-VII recommendations suggest the goal BP is below 130/80 mm Hg. The current therapy is suboptimal and requires considerable attention. See above discussion about antihypertensive therapy in the heart failure section; ultimate goal in this patient is to use therapies to manage the hypertension that benefit the concomitant disorders that are present, particularly heart failure and coronary artery disease. Currently AD is receiving a -blocker (dose to be increased), an ACE inhibitor (drug added) and furosemide (HCTZ discontinued). PROBLEM 4: HTN Goal BP more aggressively due to presence of renal dysfunction and numerous other risk factors. Control HTN with heart failure and coronary artery disease medications. PROBLEM 5: Dyslipidemia: Lipoprotein analysis was obtained in the clinic 1 month prior to ADs MI. Based on the most recent update of the National Cholesterol Education Program guidelines and recent clinical trials, her current goal for LDLC is at least 100 mg per dL and perhaps less than 70 mg per dL. Given her LDL-C of 155 mg per dL prior to her MI, intensive therapy is required to lower her LDL-C by 35% to 55%. Only statin therapy (either alone or in combination) can achieve those goals. Statins are also desirable as they reduce morbidity and mortality. To accurately determine the appropriate treatment strategy, a fasting lipoprotein analysis should be obtained. Baseline AST and ALT levels have been documented. PROBLEM 5: Dyslipidemia Discontinue hormone replacement therapy (conjugated estrogen/medroxyprogesterone acetate). Obtain fasting lipoprotein analysis. Initiate simvastatin 40 mg daily or atorvastatin 20 mg daily in the evening.
Explain to patient that the most common adverse effects of statins are GI related, such as diarrhea, nausea, vomiting, and flatulence. Counsel AD to report muscle pain, tenderness, or weakness, especially if accompanied by fever or malaise. Follow up in 4 to 6 weeks with lipoprotein analysis and liver function testing. Initiate therapeutic lifestyles diet and lifestyle modifications, as described above.
PROBLEM 6: Renal insufficiency: Estimated CrCl of -25 mL per min secondary to poorly controlled hypertension. Renal insufficiency can affect the dosing of medication excreted unchanged by the kidneys. PROBLEM 6: Renal Insufficiency Monitor and adjust dosing of all medications as necessary. PROBLEM 7: Allergic rhinitis: Well controlled. PROBLEM 7: Allergic Rhinitis Currently well controlled. QUESTIONS (See Answers in back of book for correct responses.) 1. Identify and list evidence of end-organ damage secondary to hypertension in AD. (EO-1, 2) AV nicking and narrowing, renal insufficiency, and left-ventricular hypertrophy 2. Which of the following is a sign or symptom of left-sided heart failure? (EO-2) a. Bilateral rales b. +JVD c. Hepatomegaly d. Splenomegaly 3. Which of the following is the most likely etiology of ADs heart failure? (EO-1, 3) a. Coronary artery disease b. Renal insufficiency c. Estrogen replacement therapy d. Hypertension 4. AD is to be started on ACE inhibitor therapy. Which of the following ACE inhibitor regimens will provide this patient with a dose shown to reduce mortality ostmyocardial infarction in controlled clinical trials? (EO-8, 10, 12) a. Captopril 25 mg TID b. Enalapril 5 mg BID c. Lisinopril 20 mg daily d. Benazepril 10 mg daily
5. Six weeks after AD is initiated on enalapril therapy she develops a dry nonproductive cough that keeps her awake at night. Which of the following changes to her antihypertensive regimen is most appropriate for treating her hypertension, alleviating her cough, and reducing heart failure symptoms? (EO-10, 11, 12) a. Continue enalapril and add dextromethorphan at bedtime b. D/C enalapril and initiate lisinopril therapy c. D/C enalapril and initiate valsartan therapy d. D/C enalapril and initiate terazosin therapy 6. Which of the following physical assessment findings is most consistent with a prior myocardial infarction? (EO-2) a. ECG findings of old Q waves in leads V1V4 b. S3 heart sound c. ECG findings of voltage changes d. Chest pain with exertion 7. Given ADs risk factors and previous myocardial infarction, which of the following is the most appropriate LDL goal in this patient? (EO-5, 12) a. <70 mg/dL b. <110 mg/dL c. <130 mg/dL d. <150 mg/dL 8. Which of the following anti-ischemic drugs have been shown to affect long-term outcome in patients who are postmyocardial infarction? (EO-8, 12) a. Carvedilol b. Amlodipine c. Isosorbide mononitrate d. Diltiazem 9. Your medical team wants to initiate digoxin therapy for this patient. What is an appropriate maintenance dose for AD? (EO-6, 8, 12) a. 0.125 mg PO every other day b. 0.125 mg PO daily c. 0.25 mg PO daily d. 0.375 mg PO daily 10. When communicating medication instructions to AD, which of the following is NOT a reason to immediately contact her health care provider? (EO-14, 15, 16) a. Shortness of breath that does not go away with rest b. Weight gain of 2 to 3 pounds in 1 week c. Swelling in ankles, feet, and/or legs d. Persistent cough and/or wheezing 11. To help AD stop smoking, she is started on nicotine gum. What should you tell AD about the proper use of nicotine gum? (EO-14, 16) AD should be provided with the following information for using her nicotine gum correctly: a. The nicotine gum is used to help you stop smoking. It has a better efficacy rate if you enroll in a stop-smoking program. b. The gum should never be swallowed.
c. Chew one piece of gum whenever you have the urge to smoke. d. Chew the gum very slowly until the taste of nicotine or a slight tingling in the mouth is perceived (about 15 chews). Then stop chewing the gum and put it to the side of your mouth. e. Once the tingling in the mouth is gone (usually about 1 minute), the chewing procedure should be repeated. This cycle should be repeated intermittently for about 30 minutes, and then the gum should be thrown away. f. To get the best results from the gum, follow the instructions carefully. Do not chew as you would regular gum. g. Do not use more than 30 pieces of gum per day. (Average daily use is 10 to 12 pieces.) 12. What patient education would you give AD about the proper use of her sublingual nitroglycerin tablets? (EO-12, 14, 15) There is much information for AD to learn about the correct use of nitroglycerin (NTG). Present the information before she is to be discharged, along with a written copy of the instructions. a. When experiencing chest pain, AD should sit down and dissolve one NTG tablet under her tongue. The tablet should not be swallowed, and she should not have food in her mouth at the same time. b. Sublingual NTG rapidly relieves the chest pain, usually within 3 to 5 minutes. She should take one tablet; if the pain has not resolved in 5 minutes, she should take another tablet. If the pain has not resolved in an additional 5 minutes, AD should take a third NTG tablet and proceed to an emergency room. Educate AD and her family regarding the new American Heart Association guidelines, which recommend that patients take one NTG dose sublingually in response to chest discomfort/pain. If chest discomfort/pain is unimproved or worsening 5 minutes after one NTG dose has been taken, the patient or family member/friend should call 911 immediately to access EMS. c. When she takes NTG, AD may get a headache, which may be relieved with acetaminophen (she should take the acetaminophen after the episode of chest pain has resolved). d. The NTG may make AD dizzy and lightheaded and increase her heart rate, so she should sit down when taking the medication. e. The NTG may produce a burning sensation under the tongue. This is not an indication of potency. f. AD may take the NTG prophylactically 5 to 10 minutes before activities that usually precipitate anginal attacks (e.g., climbing stairs). g. AD should have her NTG with her at all times. h. After each use, the cap of the bottle should immediately be closed tightly. i. The cotton filler should be discarded after the initial opening of the bottle. j. The NTG should be kept away from hot, humid places to prevent loss of potency. k. The NTG should be kept in the original container, without other medications in the same bottle. l. AD should get a new bottle of NTG 6 months after opening the bottle for the first time.
13. Summarize the risk-factor reduction therapies for this patients ischemic heart disease. (EO- 12, 14, 15) a. Correction and treatment of all modifiable cardiovascular risk factors is essential in an effort to reduce the risk for future vascular events. b. Risk-factor reduction should focus on hypertension management, smoking cessation, lipid-lowering therapy, antiplatelet therapy, cardiac rehabilitation, and exercise. c. Treatment of HTN reduces cardiovascular morbidity and mortality. d. Smoking cessation is especially important in patients with ischemic heart disease. Smoking is associated with increased morbidity and mortality, silent ischemia, arrhythmias, and coronary vasospasm in patients with coronary artery disease. Pharmacologic and nonpharmacologic approaches are available for assisting patients with smoking cessation. e. Lipid-lowering drug therapy in patients with angina and/or prior MI with average and elevated serum cholesterol concentrations has been shown to reduce cardiovascular morbidity and mortality. f. Exercise training reduces cardiovascular mortality, improves functional capacity, and attenuates myocardial ischemia and thus is an important lifestyle modification. g. Other cardiovascular risk factor reductions should include weight loss if overweight, alcohol use only in moderation. 14. Summarize the nonpharmacologic treatment options for this patients heart failure. a. Patient/family education 1) Discussions/pamphlets on signs and symptoms of heart failure and medications 2) Emphasis on compliance with complete treatment agenda 3) Instructions on when to contact health care providers b. Diet 1) Daily weight chart 2) Individualized diet according to needs/ preferences/lifestyle 3) Sodium restriction: mild (<3 g/day) or moderate (<2 g/day) 4) Information regarding sodium and potassium content in foods 5) Alcohol restriction 6) Fluid restriction: - 2 L per day 7) Nutritional supplements (e.g., vitamins) 8) Emphasize importance of compliance. c. Pharmacologic treatment of hyperlipidemia and hypertension d. Exercise program e. Intensive follow-up: telephone calls, home visits, outpatient clinic visits 15. Summarize therapeutic, pathophysiologic, and disease management concepts related to the treatment of heart failure/myocardial infarction in this patient utilizing a key points format. (EO-18) KEY POINTS Heart failure a. Heart failure is a clinical syndrome that progresses to worsening symptoms and death largely as a consequence
of maladaptive effects triggered by neurohormones and cytokines. b. Heart failure can result from abnormalities in either systolic or diastolic dysfunction. c. Participation in cardiac rehabilitation programs can improve exercise tolerance and quality of life and may reduce mortality in heart failure patients. d. Patient education is extremely important, especially with respect to facilitating compliance with dietary and medication treatment plans. e. Based on their ability to consistently improve both the clinical status of patients and their longevity, ACE inhibitors are considered first-line therapy in the management of heart failure patients. ACE inhibitor therapy should begin with low doses that are slowly titrated to target doses. f. Alternative vasodilator therapy such as ARBs or the combination of nitrates plus hydralazine should be reserved for patients intolerant of ACE inhibitors. g. The use of -blockers is currently advocated in the management of all stable heart failure patients based on their ability to reduce mortality and hospitalization rates. blocking therapy begins with low doses that are slowly and carefully increased. Since this patient has angina, these agents are particularly useful in the prevention of anginal episodes. h. Diuretics are used in the management of heart failure to relieve symptoms. i. Digoxin can be used safely in most patients with heart failure due to systolic dysfunction, with target serum digoxin concentrations between 0.7 and 1.2 ng per mL. j. Anticoagulant therapy is indicated in heart failure patients with coexisting atrial fibrillation or other conditions that predispose them to thromboembolic conditions. Status post-MI a. MI is one of the most common reasons for hospitalization in the Western world. The actual mortality rate is about 15%; approximately 10% of patients will die during the first year after their acute MI. b. Short-term and long-term survival depends on the extent and location of the coronary obstructive lesions and the prompt correction of post-MI complications. c. Information about the presence or absence of mechanical, electrical, ischemic, and vascular abnormalities is needed to institute approximate medical and/or surgical treatment. d. Correction and treatment of all modifiable cardiovascular risk factors is essential in an effort to reduce the risk for future vascular events. e. Risk factor reduction should focus on hypertension management, smoking cessation, lipid-lowering therapy, antiplatelet therapy, and cardiac rehabilitation and exercise. f. Treatment of hypertension reduces cardiovascular morbidity and mortality. g. Smoking cessation is especially important in patients with ischemic heart disease. Smoking is associated with increased morbidity and mortality, silent ischemia, arrhythmias, and coronary vasospasm in patients with coronary artery disease. Pharmacologic and nonpharmacologic approaches are available for assisting patients with smoking cessation.
h. Lipid-lowering drug therapy in patients with angina and/or prior MI with average and elevated serum cholesterol concentrations has been shown to reduce cardiovascular morbidity and mortality. i. Exercise training reduces cardiovascular mortality, improves functional capacity, and attenuates myocardial ischemia and thus is an important lifestyle modification. j. Other cardiovascular risk factor reductions should include weight loss if overweight, alcohol use only in moderation.
TOPIC: Hypertension and Congestive Heart Failure
THERAPEUTIC DIFFICULTY: Level 2 Sarah B. Karish and Joseph M. Calomo Chapter 20: Hypertension Chapter 21: Congestive Heart Failure Scenario Patient and Setting: WJ, a 59-year-old African American male; ambulatory care clinic Chief Complaint: Increased shortness of breath (SOB) this past week; WJ attributes SOB to his cold History of Present Illness Requires two pillows to sleep, swollen legs, malaise, weakness, and weight gain; furosemide dose was decreased 2 weeks ago due to hypokalemia; increasing SOB; paroxysmal nocturnal dyspnea (PND); and ankle edema Medical History: Heart failure (ejection fraction, 15%; New York Heart Association Class II); orthopnea; ventricular tachycardia (controlled with amiodarone); coronary artery disease (CAD); diabetes mellitus (DM) type 2 for 5 years; hypertension (HTN) for 30 years; chronic renal insufficiency Surgical History: None Family/Social History: Family History: Mother with heart failure (HR) Social History: Prior cigarette smoker 34 packs/ week; quit 30 years ago; 6 cans of beer/week Medications: Amiodarone, 200 mg PO QD Furosemide, 80 mg PO QAM Avandia, 8 mg PO QD Spironolactone, 12.5 mg PO QD Carvedilol, 25 mg PO QAM, 12.5 mg PO QPM Coumadin, 6 mg PO QD Digoxin, 0.125 mg PO QD initiated at todays visit Allergies: No known drug allergies; ACEI-induced cough Physical Examination GEN: Well-developed, well-nourished man with noticeable SOB VS: BP 153/91, HR 82, RR 25, T 37C, Wt 78 kg (Wt 2 months earlier 71 kg), Ht 172 cm HEENT: + jugular venous distension COR: rrr, s1s2, no m/r/g CHEST: Bibasilar rales ABD: Hepatomegaly GU: Deferred RECT: Deferred EXT: 2+ edema bilat LE NEURO: Alert and 0 x 3 Results of Pertinent Laboratory Tests, Serum Drug Concentrations, and Diagnostic Tests
Fasting Na 139 (139) Hct 0.33 (33) Lkcs 8.2 _ 109 K 4.0 (4.0) Hgb 140 (14) (8.2 _ 103) CI 103 (103) AST 0.5 (30) Plts 171 _ 109 HCO3 25 (25) ALT 0.5 (30) (171 _ 103) BUN 11.4 (32) Alb 20 (2.0) MCV 80 (80) Glu 11.6 (210) SCr 168 (1.9) Alk Phos 1.5 (90) Uric Acid 190 (3.2) T Bili 3.4 (0.2) Ca 2.2 (8.8) HgA1C: 7.2 % PO4 0.92 (3.0) INR: 3.0
Mg 1.2 (2.5) Lkc differential: WNL Urinalysis: 2_ protein Chest x-ray films: Enlarged cardiac silhouette
Problem List Identify principal problems from the scenario in priority order (see Answers in back of book for correct list of problems). 1. CHF exacerbation 2. Drug interactions: Amiodarone and Coumadin Amiodarone and digoxin 3. Poorly controlled BP 4. Chronic renal insufficiency 5. DM type 2 SOAP Note To be completed by the student (see Answers in back of book for correct SOAP Note). S: I am having increasing difficulty breathing, swollen legs, weakness, and weight gain. This all started 2 weeks ago when my furosemide dose was decreased. O: SOB; 3+ ankle edema; 7 kg weight gain; BP 153/91; CR 1.9; BUN 32; urinalysis: 2+ protein; chest x-ray: enlarged cardiac silhouette; left ventricular ejection fraction (LVEF) 15%, +S1, S2 A: PROBLEM 1: CHF exacerbation secondary to decreased dose of furosemide Increase furosemide daily dose: add PM dose; change regimen to 80 mg PO QAM and 40 mg PO QPM. Monitor weight q24h. Monitor K_ level. Discuss importance of daily weights (same time of day, preferably on arising, in similar clothes); maintain a diary of weights and report increases in weight. Analyze dietary intake of sodium and use of potassiumcontaining salt substitutes. Discuss importance of adhering to dietary restrictions; praise and encourage to continue sodiumrestricted diet (2 g Na/day). Assess adherence to entire heart failure medication regimen. If heart failure continues to worsen, consider adding nitrates or blocker. PROBLEM 2: Drug interaction with amiodarone and digoxin: dose adjustment needed for digoxin. Monitor interaction with amiodarone and coumadin; INR stable; no need to adjust dose Decrease dose of digoxin by 50%: change regimen to 0.125 mg PO Q 3 days Continue digoxin; monitor digoxin level (goal: 1 ng/mL). Counsel regarding need to report nausea, blurred vision Monitor INR (goal: 23) PROBLEM 3: Poorly controlled BP Goal BP for adult hypertensive diabetic patients is below 130/80 Add ARB (ACE inhibitor induced cough). Add Cozaar CHF: initial, 12.5 mg orally PO once daily; titrate at 7-day intervals to 25 mg, then 50 mg daily (based on response) If BP remains elevated with increases in furosemide and addition of Cozaar, add a nitrate
PROBLEM 4: Chronic renal insufficiency secondary to heart failure No interventions needed at this time Use caution with renally cleared medications; doses should be adjusted for decreased renal function Consider metolazone if renal function becomes markedly reduced PROBLEM 5: Poorly controlled DM type 2 Add glyburide 5 mg PO QD. Rule out use of metformin due to increased SCr level (>1.5). Discontinue Avandia 8 mg QD due to possible fluid retention QUESTIONS (See Answers in back of book for correct responses.) 1. The most probable cause for WJs heart failure exacerbation: (EO-1) a. Increased weight b. Decrease in furosemide dose c. Poorly controlled blood pressure d. Inability to take an ACE ihibitor due to cough 2. Which of the following is a sign and symptom of leftsided HF exacerbation currently present in WJ? (EO-2) a. Swollen legs b. Shortness of breath c. Altered mental status d. Increased body weight 3. Which of the following is a nonspecific symptom of HF noted in WJ: (EO-2) a. Swollen legs b. Shortness of breath c. Altered mental status d. Increased body weight 4. Which of the following is a contributing factor to WJs heart failure? (EO-3) a. Gender b. Patients age c. Hypertension d. Increased body weight 5. Which of the following disease processes is LEAST likely to be contributing to WJs HF? (EO-1) a. Hypertension b. Increased age c. Atrial fibrillation d. Coronary artery disease 6. Which of the following is WJs goal blood pressure based on JNC-VII guidelines? (EO-5) a. <120/80 b. < 130/80 c. <140/80 d. <140/90
7. Identify factors to consider when selecting current medication therapy for WJ. (EO-8) a. Diuretic - loop because CrCl is below 50 mL per min b. Spironolactone added because still symptomatic c. ARB not ACE inhibitor because of cough from ARB d. ASA for coronary artery disease e. Add sulfonylurea due to poor control of blood sugar; avoid metformin due to serum creatinine above 1.5. Consider discontinuation of Avandia due to risk of edema 8. WJ should be monitored for factors that predispose him to digoxin toxicity. Based on the information presented, which of the following is a current factor that would potentially predispose WJ to digoxin toxicity? (EO-4, 6, 8, 9) a. Increased age b. Hypokalemia c. Spironolactone d. Hypomagnesemia 9. Describe the mechanisms of action of the pharmacologic interventions in this case. (EO-7) A. Avandia: member of the thiazolidinedione class of antidiabetic agents; improves glycemic control by improving insulin sensitivity. Rosiglitazone is a highly selective and potent agonist for the peroxisome proliferator activated receptor- (PPAR). In humans, PPAR receptors are found in key target tissues for insulin action such as adipose tissue, skeletal muscle, and liver. Activation of PPAR nuclear receptors regulates the transcription of insulin-responsive genes involved in the control of glucose production, transport, and utilization. In addition, PPARresponsive genes also participate in the regulation of fatty acid metabolism. B. Spironolactone: steroid with a structure resembling that of the natural adrenocortical hormone aldosterone, acts on the distal portion of the renal tubule as a competitive antagonist of aldosterone. It acts as a potassium- sparing diuretic, increasing sodium and water excretion and reducing potassium excretion. C. Carvedilol: nonselective -adrenergic blocking agent with -1 blocking activity, moderate membrane-stabilizing activity (MSA), no intrinsic sympathomimetic activity (ISA), and high lipid solubility D. Coumadin: acts by inhibiting the synthesis of vitamin Kdependent clotting factors, which include factors II, VII, IX, and X, and the anticoagulant proteins C and S E. Amiodarone: classified as a class III antiarrhythmic agent, but it is now most appropriate to suggest that it encompasses the entire spectrum of antiarrhythmic classification. Amiodarone slows intraventricular conduction by blocking the sodium channel, slows the heart rate, and impedes AV node conduction by blocking -adrenergic receptors and calcium channels, and it prolongs atrial and ventricular repolarization by inhibiting potassium channels. F. Furosemide: a short-acting sulfonamide loop diuretic. Believed to reversibly bind to the sodium, potassium, chloride cotransport mechanism on the luminal side of the ascending loop of Henle, thereby inhibiting the active reabsorption of these ions; also inhibits reabsorption of sodium and chloride in the proximal and distal tubules.
G. Digoxin: inhibits sodium-potassium ATPase, an enzyme that regulates the quantity of sodium and potassium inside cells. Inhibition of the enzyme leads to an increase in the intracellular concentration of sodium and thus (by stimulation of sodiumcalcium exchange) an increase in the intracellular concentration of calcium. The beneficial effects of digoxin result from direct actions on cardiac muscle, as well as indirect actions on the cardiovascular system mediated by effects on the autonomic nervous system. Positive inotropic and negative chronotropic effects. 10. List the current pharmacological and nonpharmacological treatment problems with WJs treatment plan. Explain your reasoning and provide solutions to therapy. (EO-11) a. Poorly controlled hypertension. Based on JNC-VII, the patients goal BP is 130/80 mm Hg because she also has diabetes. Consider adding ARB agent rather than an ACE inhibitor due to ACE inhibitorinduced cough b. Poorly controlled type 2 DM. Consider adding a secretagogue such as glyburide or repaglinide. Avoid adding biguanide due to renal insufficiency c. Hepatomegaly. While the amount of ETOH currently consumed by WJ might not be cause for alarm, with hepatomegaly and the number of medications currently being used, consider a discussion about decreased ETOH consumption 11. Describe what psychosocial factors may affect WJs adherence to therapy. (EO-15) A. Patient issues 1. Reduced activity due to current symptoms 2. Number and complexity of current medication therapy 3. Dietary restrictions due to current complications may be difficult 4. Cost of medications: assess patients health care coverage and ability to pay for medications B. Potential emotional issues: Based on the number of issues and number of medications being taken, monitor: 1. Anxiety 2. Panic disorders 3. Depression C. Other barriers 1. Unknown family dynamics and support; needs further analysis 2. Assess other potential stressors in WJs life at this time 3. Ability to travel to and from pharmacy or to and from clinic for follow-up 12. Summarize therapeutic, pathophysiologic, and disease management concepts for hypertension utilizing a key points format. (EO-18) The JNC-VII defines hypertension as a systolic BP greater than 140 mm Hg or a diastolic BP greater than 90 mm Hg. The pathogenesis of essential hypertension remains unknown. BP is controlled through a multifaceted interplay of neurohormonal, renal, vascular, adrenal, and genetic manipulations. Target organ disease from arterial hypertension can be cardiac, cerebrovascular, peripheral vascular, renal, and ocular.
The treatment of hypertension requires a multiintervention approach that encompasses nonpharmacologic treatments such as weight reduction through appropriate physical activity and dietary habits, dietary sodium reduction, and moderate alcohol consumption as well as the appropriate individualization of pharmacotherapy. Comorbid treatment options consist of:
Heart failure ACE inhibitor, loop diuretic, -blocker, spironolactone Status post-MI -blocker DM type 2 with microalbuminuria ACE inhibitor, ARB DM with microalbuminuria ACE inhibitor Chronic kidney disease ACE inhibitor
TOPIC: Thromboembolic Disease
THERAPEUTIC DIFFICULTY: Level I Laurie J. Schmitt Chapter 25: Thromboembolic Disease Scenario Patient and Setting: GS, an 89-year-old Hispanic male, hospital Chief Complaint: Hospitalized after 1 week of fever, vomiting, and mental status changes for empirical treatment of pneumonia. GS is not ambulating due to his illness and had one episode of vomiting in the past 24 hours. Renal function has improved since admission when BUN was 23 (65) and CR 186 (2.1); baseline CR 110 (1.2). GS is being given IV fluids for hydration and an albuterol inhaler PRN for shortness of breath (SOB). History of Present Illness GS has received 3 days of IV moxifloxacin 400 mg daily for treatment of pneumonia Medical History: None Surgical History: None Family/Social History: Family History: Noncontributory Social History: Lives alone at home, denies smoking or ETOH use Medications: MVI daily Allergies: No known drug allergies Physical Examination GEN: Very pleasant, comfortable VS: BP 138/76, HR 78, RR 18, T 37_C, Wt 62 kg, Ht 170 cm HEENT: WNL COR: RRR CHEST: Diffuse rales present bilaterally, diminished breath sounds ABD: WNL GU: Deferred RECT: Deferred EXT: No edema NEURO: Alert and oriented _ 3 Results of pertinent Laboratory Tests, Serum Drug Concentrations, and Diagnostic Tests
Na 141 (141) U/A: negative T Bili 3.4 (0.2) K 4.5 (4.5) Hct 0.36 (36) CI 105 (105) Hgb 130 (13) HCO3 28 (28) Lkcs 10 _ 109 AST 0.50 (30) Glu 6.1 (110) (10 _ 103) BUN 14 (38) ALT 0.50 (30) Ca 2.2 (8.8) CR 168 (1.9) Plts 221 _ 109 LDH 1.7 (100) PO4 0.92 (3.0) (221_ 103) Alk Phos 1.5 Mg 1.2 (2.5) (90) MCV 93.8 (93.8) Alb 3.5 (3.5) Uric Acid 190 (3.2) Chest x-rayLLL infiltrate Factor V LeidenWNL Protein C & SWNL Factor VIIIWNL Urine culture: negative ECG: normal
SOAP Note To be completed by the student (see Answers in back for book for correct SOAP Note). S: Patient has no current complaints. O: Chest x-ray LLL infiltrate, diffuse rales bilaterally, diminished breath sounds, RR 18, Lkcs 10 x 109 (10 x 103), T 37C, BUN 14 (38), CR 168 (1.9) P: PROBLEM 1: Pneumonia Continue IV moxifloxacin 400 mg daily for 10 to 14 days. Change IV moxifloxacin to PO once N/V has resolved and patient is afebrile for 24 to 48 h. Monitor temp q24h. Monitor Lkcs q24h. PROBLEM 2: Acute Renal Dysfunction due to Dehydration From N/V Continue IV fluids. Encourage slow PO intake. Monitor I and O. Monitor BUN and Cr q24h. Goal is to return Cr to baseline and hydrate patient to BUN/Cr ratio less than 20:1. PROBLEM 3: VTE Prophylaxis Required Secondary to Hospital Stay and Immobility Patient is at risk for VTE due to age and immobility in the hospital. Check baseline aPTT, PT, hemoglobin, hematocrit, and complete blood count (platelets). Add unfractionated heparin starting with an IV bolus 80 units per kg (5,000 units) followed by IV infusion of 1,000 units per hour to prevent VTE until patient is ambulating. Avoid using LMWH as patient has renal dysfunction. Monitor aPTT 4 to 6 hours after beginning infusion to a goal of 1.5 to 2.5 times the control. Continue to monitor aPTT q6h for 24 h and then q24h. Continue to monitor PT, hemoglobin, hematocrit, and complete blood count (platelets) q24h. Monitor for signs and symptoms of bleeding and VTE q24h, including calf pain/tenderness, LE swelling, venous distention and Homans sign, dyspnea, tachypnea, sinus tachycardia, and pleuritic chest pain. Alternative therapy VFH 5000 units SQ BID-TID until ambulating. QUESTIONS (See Answers in back of book for correct responses.) 1. Which of the following is the likely etiology for the risk of developing VTE in GS? (EO-1) a. Venous stasis as a result of hospitalization b. Hypercoagulable state as a result of Factor V Leiden mutation c. Endothelial damage as a result of surgery d. Increased clearance of clotting factors as a result of renal disease 2. List 3 of the most common signs/symptoms to monitor that may indicate the presence of both DVT and PE in GS. (EO-2) DVT: calf pain/tenderness, LE swelling, venous distention and Homans sign; Pulmonary embolism: dyspnea, tachypnea, sinus tachycardia; pleuritic chest pain
Problem List Identify principal problems from the scenario in priority order (see Answers in back of book for correct list of problems). 1. Pneumonia 2. Acute renal dysfunction 3. VTE prophylaxis
3. List the clinical risk factors that GS has for venous thromboembolic disease. (EO-3) Age, prolonged immobility due to hospitalization 4. What is the diagnostic test that is preferred to diagnose both DVT and PE? (EO-5) DVT: Compression ultrasonography; Pulmonary embolism; no one test is preferred; test of choice is based on presence of risk factors 5. Which of the following statements is most accurate regarding the treatment options available to prevent VTE? (EO-6) a. The onset of UFHs antithrombotic effects may take up to 4 days. b. LMWHs do not require any laboratory monitoring. c. Warfarin is not associated with any drug-drug interactions. d. LMWHs are available in an oral formulation. 6. Which of the following represents the appropriate monitoring for each medication? (EO-5) a. Enoxaparin efficacy is monitored with an Aptt. b. Warfarin efficacy is monitored with an aPTT. c. Warfarin efficacy is monitored with an INR. d. UFH efficacy is monitored with an INR. 7. Which statement below is correct? (EO-7) a. LMWHs inhibit antithrombin III only. b. Unfractionated heparin inhibits thrombin and factor Xa. c. Warfarin interferes with clotting factors II, VII, IX, and X. d. Fibrinolytics inactivate plasminogen. 8. List two nonpharmacologic measures that can be used to help prevent VTE. (EO-7) Support garments including elastic stockings or intermittent compression devices; surgery; avoid prolonged sitting, leg crossing; constrictive garments 9. Which of the following is an adverse drug effect that should be monitored when using UFH and LMWHs? (EO10) a. Hyperaldosteronism b. Hypercalcemia c. Thrombocytopenia d. Hypertension 10. What is an appropriate dose of enoxaparin (Lovenox) for the prevention of VTE? (EO-11) a. 1 mg/kg SQ q12 hrs b. 1.5 mg/kg SQ q24 hrs c. 5000 units SQ q12 hrs d. 40 mg SQ q24 hrs 11. Which of the following is the most appropriate agent to be used in a patient being administered UFH who becomes overanticoagulated?(EO-11) a. Protamine sulfate b. Danaparoid c. Vitamin K d. Alteplase
12. Summarize therapeutic, pathophysiologic, and disease management concepts for thromboembolic disease utilizing a key points format. (EO-18) Hospitalized patients who are not ambulating are at an increased risk for developing VTE. There are several medication treatment options, including UFH, LMWHs, and warfarin, with different advantages and disadvantages. Use should be tailored to individual patients. UFH can be administered SQ or IV and has a quick onset of action. The IV infusion allows for quick titration and ability to stop drug quickly. aPTT should be monitored when using UFH. LMWHs can be administered BID or once daily and do not require laboratory monitoring due to a predictable doseresponse. LMWHs should be used cautiously in patients with renal dysfunction. Warfarin is available orally. Warfarins antithrombotic effects may take up to 4 days, so its administration should be overlapped with another agent with a quick onset of action such as UFH or LMWH. Warfarins effects are influenced by many factors that are variable, including patient diet, liver function, and drugdrug interactions; INR should be monitored carefully
Вам также может понравиться
- Atrial Fibrillation A Simple Guide to The Condition, Treatment And Related DiseasesОт EverandAtrial Fibrillation A Simple Guide to The Condition, Treatment And Related DiseasesРейтинг: 4 из 5 звезд4/5 (1)
- Flashcards - QuizletДокумент7 страницFlashcards - QuizletNEsreОценок пока нет
- AAFP Family Med Board QuestionsДокумент96 страницAAFP Family Med Board QuestionsKamil Hanna100% (2)
- ModMed CardiologyДокумент77 страницModMed CardiologyLee Tzong YewОценок пока нет
- Unstable AnginaДокумент5 страницUnstable AnginaAria AlysisОценок пока нет
- Care of Patient With CADДокумент22 страницыCare of Patient With CADBader ZawahrehОценок пока нет
- 978190medicine5635856 PDFДокумент18 страниц978190medicine5635856 PDFMuhammad TariqОценок пока нет
- NullДокумент11 страницNullKareem SaeedОценок пока нет
- 9 CsaДокумент34 страницы9 Csaمحمد بن الصادقОценок пока нет
- Unit 4 Coronary Artery Disease and Ischaemic Heart Disease: StructureДокумент37 страницUnit 4 Coronary Artery Disease and Ischaemic Heart Disease: StructurebtaleraОценок пока нет
- What Symptoms Should Lead The Nurse To Suspect The Pain May Be Angina?Документ5 страницWhat Symptoms Should Lead The Nurse To Suspect The Pain May Be Angina?Dylan Angelo AndresОценок пока нет
- Clinical Exposure Vi Assignment: Faculty of Medicine Universitas Pelita HarapanДокумент16 страницClinical Exposure Vi Assignment: Faculty of Medicine Universitas Pelita HarapanSteven MatualiОценок пока нет
- Cardiology: Ischemic Heart DiseaseДокумент33 страницыCardiology: Ischemic Heart DiseaseMysheb SSОценок пока нет
- Client With AnginaДокумент3 страницыClient With AnginavitaceeОценок пока нет
- Question 1 of 10: AAFP Board Review Clinchers Cardio Quiz 1Документ53 страницыQuestion 1 of 10: AAFP Board Review Clinchers Cardio Quiz 1angel_sagun_1Оценок пока нет
- CardiologyДокумент9 страницCardiologyAbi RajasingamОценок пока нет
- Questions & Answers: CardiologyДокумент77 страницQuestions & Answers: CardiologyDev Yadav100% (1)
- Lec 4Документ8 страницLec 4Sajjad FalahОценок пока нет
- Care of Clients With Cardiovascular DisordersДокумент67 страницCare of Clients With Cardiovascular DisordersMatt Lao DionelaОценок пока нет
- SID For 4th YrsДокумент76 страницSID For 4th YrsABREHAM BUKULOОценок пока нет
- Ischemic Heart Diease PDFДокумент33 страницыIschemic Heart Diease PDFMahamed Wefkey OmranОценок пока нет
- Question 1 of 10: AAFP Board Review Clinchers Cardio Quiz 1Документ60 страницQuestion 1 of 10: AAFP Board Review Clinchers Cardio Quiz 1pramesh1Оценок пока нет
- Unstable Angina PectorisДокумент28 страницUnstable Angina PectorisLissaberti AmaliahОценок пока нет
- Presentor: John Hommer E. Dy M.D. Moderator: Joy Marchadesch M.DДокумент57 страницPresentor: John Hommer E. Dy M.D. Moderator: Joy Marchadesch M.DJohn Hommer DyОценок пока нет
- Angina PectorisДокумент11 страницAngina Pectorisjialin80% (5)
- Emergency Management of Acute Myocardial Infarction: Simon MaxwellДокумент15 страницEmergency Management of Acute Myocardial Infarction: Simon MaxwellMaram AbdullahОценок пока нет
- Cardiac DisordersДокумент80 страницCardiac Disordersscan1993Оценок пока нет
- 3 Ischemic Heart Disease - PPTX Year 3 2Документ40 страниц3 Ischemic Heart Disease - PPTX Year 3 2Danny DesuОценок пока нет
- 10-Primary Care - AAFP Flashcards - Quizlet PDFДокумент870 страниц10-Primary Care - AAFP Flashcards - Quizlet PDFehabb350% (2)
- Clin Cardiology CasesДокумент34 страницыClin Cardiology CasesSunny Singh0% (1)
- Angina PectorisДокумент8 страницAngina PectorisPrince DuОценок пока нет
- Cardiovascular Agents: Florianne E. Adlawan, R.NДокумент31 страницаCardiovascular Agents: Florianne E. Adlawan, R.NadlawanflorianneОценок пока нет
- Angina PectorisДокумент11 страницAngina PectorisJohn Matley CaampuedОценок пока нет
- Case Analysis: Medical Surgical NursingДокумент7 страницCase Analysis: Medical Surgical NursingMaria ThereseОценок пока нет
- Internal Medicine 1 Step 2 (All Subjects)Документ50 страницInternal Medicine 1 Step 2 (All Subjects)Sumer AhmedОценок пока нет
- SG001 - Jore, Julianna RheavenДокумент9 страницSG001 - Jore, Julianna RheavenJulianna Rheaven JoreОценок пока нет
- ADHF Wecoc FinalДокумент27 страницADHF Wecoc FinalNovrian Ali YlberОценок пока нет
- Acute Miocard InfarkДокумент32 страницыAcute Miocard InfarkhansОценок пока нет
- Pharmacotherapy of CADДокумент27 страницPharmacotherapy of CADhams elaklamОценок пока нет
- Coronary Artery Disease-Cad OR Ischaemic Heart Disease - IhdДокумент99 страницCoronary Artery Disease-Cad OR Ischaemic Heart Disease - IhdMwanja MosesОценок пока нет
- Coronary Artery Disease-Cad OR Ischaemic Heart Disease - IhdДокумент99 страницCoronary Artery Disease-Cad OR Ischaemic Heart Disease - IhdMwanja MosesОценок пока нет
- Lec 2 Heart Failure, Angina and Arryth2Документ19 страницLec 2 Heart Failure, Angina and Arryth2Adel AlomarОценок пока нет
- CardioДокумент9 страницCardioVirgilio Reyes ManuelОценок пока нет
- CH F ManagementДокумент38 страницCH F ManagementShafid HamzabОценок пока нет
- Presentation 3Документ42 страницыPresentation 3Max ZealОценок пока нет
- Myocardial InfarctionДокумент4 страницыMyocardial InfarctionLetecia MooreОценок пока нет
- Case 1 & 2Документ4 страницыCase 1 & 2Adeel ShahidОценок пока нет
- Yash 18ll8a CopyxxДокумент13 страницYash 18ll8a CopyxxPatel YashОценок пока нет
- Angina Pectoris: Ischemic Heart DiseaseДокумент17 страницAngina Pectoris: Ischemic Heart DiseaseMahum SohailОценок пока нет
- Care of The Patient With A Cardiac Mechanical DisorderДокумент8 страницCare of The Patient With A Cardiac Mechanical DisorderthubtendrolmaОценок пока нет
- Cad CommerДокумент2 страницыCad CommerWhatDoYouSeriesОценок пока нет
- Perfusion. Cad - Acs.miДокумент47 страницPerfusion. Cad - Acs.miMichael S. PetryОценок пока нет
- Heart Failure 20Документ160 страницHeart Failure 20jorge corolla montesОценок пока нет
- Drugs Uses For Heart FailureДокумент45 страницDrugs Uses For Heart FailureJoshua ObrienОценок пока нет
- Myocardial Infarction: Coronary Heart Disease (CHD) Coronary Artery Disease (CAD) Ischaemic Heart Disease (IHD)Документ29 страницMyocardial Infarction: Coronary Heart Disease (CHD) Coronary Artery Disease (CAD) Ischaemic Heart Disease (IHD)Mahum SohailОценок пока нет
- End-Stage Heart DiseaseДокумент44 страницыEnd-Stage Heart DiseaseCyrille AgnesОценок пока нет
- AnginaДокумент6 страницAnginaArslan SaeedОценок пока нет
- Cardiovascular DiseasesДокумент67 страницCardiovascular DiseasesokaciaОценок пока нет
- Pipe Cleaner Lesson PlanДокумент2 страницыPipe Cleaner Lesson PlanTaylor FranklinОценок пока нет
- Hazardous Locations: C.E.C. ClassificationsДокумент4 страницыHazardous Locations: C.E.C. ClassificationsThananuwat SuksaroОценок пока нет
- Maritime Academy of Asia and The Pacific-Kamaya Point Department of AcademicsДокумент7 страницMaritime Academy of Asia and The Pacific-Kamaya Point Department of Academicsaki sintaОценок пока нет
- Haier in India Building Presence in A Mass Market Beyond ChinaДокумент14 страницHaier in India Building Presence in A Mass Market Beyond ChinaGaurav Sharma100% (1)
- Beyond "The Arc of Freedom and Prosperity": Debating Universal Values in Japanese Grand StrategyДокумент9 страницBeyond "The Arc of Freedom and Prosperity": Debating Universal Values in Japanese Grand StrategyGerman Marshall Fund of the United StatesОценок пока нет
- Product Manual 26086 (Revision E) : EGCP-2 Engine Generator Control PackageДокумент152 страницыProduct Manual 26086 (Revision E) : EGCP-2 Engine Generator Control PackageErick KurodaОценок пока нет
- Multimodal Essay FinalДокумент8 страницMultimodal Essay Finalapi-548929971Оценок пока нет
- Epreuve Anglais EG@2022Документ12 страницEpreuve Anglais EG@2022Tresor SokoudjouОценок пока нет
- Types of Water Pump and Applications in Power Plant.Документ6 страницTypes of Water Pump and Applications in Power Plant.abbas bilalОценок пока нет
- BIAN How To Guide Developing Content V7.0 Final V1.0 PDFДокумент72 страницыBIAN How To Guide Developing Content V7.0 Final V1.0 PDFميلاد نوروزي رهبرОценок пока нет
- List of Iconic CPG Projects in SingaporeДокумент2 страницыList of Iconic CPG Projects in SingaporeKS LeeОценок пока нет
- The Privatization PolicyДокумент14 страницThe Privatization PolicyRIBLEN EDORINAОценок пока нет
- Final WMS2023 HairdressingДокумент15 страницFinal WMS2023 HairdressingMIRAWATI SAHIBОценок пока нет
- General Chemistry 2 Q1 Lesson 5 Endothermic and Exotheric Reaction and Heating and Cooling CurveДокумент19 страницGeneral Chemistry 2 Q1 Lesson 5 Endothermic and Exotheric Reaction and Heating and Cooling CurveJolo Allexice R. PinedaОценок пока нет
- Organization Culture Impacts On Employee Motivation: A Case Study On An Apparel Company in Sri LankaДокумент4 страницыOrganization Culture Impacts On Employee Motivation: A Case Study On An Apparel Company in Sri LankaSupreet PurohitОценок пока нет
- Matka Queen Jaya BhagatДокумент1 страницаMatka Queen Jaya BhagatA.K.A. Haji100% (4)
- Famous Little Red Book SummaryДокумент6 страницFamous Little Red Book SummaryMatt MurdockОценок пока нет
- Dominion Wargame RulesДокумент301 страницаDominion Wargame Rules4544juutf100% (4)
- Iphone and Ipad Development TU GrazДокумент2 страницыIphone and Ipad Development TU GrazMartinОценок пока нет
- Faa Data On B 777 PDFДокумент104 страницыFaa Data On B 777 PDFGurudutt PaiОценок пока нет
- BARUДокумент53 страницыBARUhueuaОценок пока нет
- Understanding and Teaching Fractions: Sybilla BeckmannДокумент26 страницUnderstanding and Teaching Fractions: Sybilla Beckmannjhicks_mathОценок пока нет
- Analytical Chem Lab #3Документ4 страницыAnalytical Chem Lab #3kent galangОценок пока нет
- 52 - JB CHP Trigen - V01Документ33 страницы52 - JB CHP Trigen - V01July E. Maldonado M.Оценок пока нет
- Upes School of Law Lac & Adr Association: PresentsДокумент7 страницUpes School of Law Lac & Adr Association: PresentsSuvedhya ReddyОценок пока нет
- Aakriti 1Документ92 страницыAakriti 1raghav bansalОценок пока нет
- Acc116 Dec 2022 - Q - Test 1Документ6 страницAcc116 Dec 2022 - Q - Test 12022825274100% (1)
- Odisha State Museum-1Документ26 страницOdisha State Museum-1ajitkpatnaikОценок пока нет
- in 30 MinutesДокумент5 страницin 30 MinutesCésar DiazОценок пока нет
- Csu Cep Professional Dispositions 1Документ6 страницCsu Cep Professional Dispositions 1api-502440235Оценок пока нет