Академический Документы
Профессиональный Документы
Культура Документы
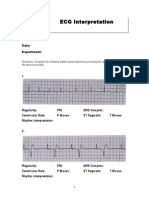
ECG Booklet PDF
Загружено:
yuhuma_qyu6841Исходное описание:
Оригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
ECG Booklet PDF
Загружено:
yuhuma_qyu6841Авторское право:
Доступные форматы
Basic Principles of ECG Booklet
Basic Principles of
Electrocardiography
Nursing Program, Medicine Faculty Brawijaya University 2004
References
Atwood,Stanton, Storey (1996). Pengenalan Dasar Disritmia Jantung. Yogyakarta : Gajah Mada University Press. Emergency Nurses Chapter (2001). Basic ECG Course. 3rd edition. Singapore : Singapore Nurses Association Ginger & Melvin Ochs (1997). Recognition & Interpretation : ECG RHYTHMS. 3rd edition. USA: Appleton & Lange. Thaler (2000). Satu-satunya BUKU EKG yang Anda Perlukan. Edisi 2. Jakarta : Hipokrates.
Alfrina Hany,S.Kp/Brawijaya University
Basic Principles of ECG Booklet
Learning Objectives
General Objectives
After studying this subject in about 2 x 3 x 50 menit, the students expected to be able to use ECG machine and interpret the ECG result. Composition : 15 Pre test 90 Presentation & Discussion 15 Post test
Specific Objectives
1. Fundamentals of EKG (20)
a. Introduction b. Hearts conducting system c. EKG Machine d. EKG Waveform Analysis
2. Obtaining 12 leads EKG (20)
a. About 12-Lead EKG b. Recording 12-Lead EKG c. Troubleshooting (problems&solutions) d. Care & Cleaning
3. Interpreting Basic EKG (50)
a. 5 Steps of Arrhythmia Interpretation b. Classification of Arrythmias c. Recognition & Treatment
Alfrina Hany,S.Kp/Brawijaya University
Basic Principles of ECG Booklet
Fundamentals of EKG
Introduction Hearts conducting system EKG Machine EKG Waveform Analysis
During the late 1800's and early 1900's, Dutch physiologist Willem Einthoven developed the early electrocardiogram. He won the Nobel prize for its invention in 1924. Hubert Mann first uses the electrocardiogram to describe electrocardiographic changes associated with a heart attack in 1920. Electrocardiography - graphic recording of the electrical activity (potentials) produced by the conduction system and the myocardium of the heart during it depolarization / repolarization cycle.
Alfrina Hany,S.Kp/Brawijaya University
Basic Principles of ECG Booklet
Fundamentals of ECG
Hearts Conducting System
(Ginger & Melvin Och, 1997)
Normally electrical impulses that causes rythmic contraction of heart muscles arises in the SA Node as the intrinsic pacemaker of the heart. From the SA Node, impulse spreads over the atrial muscles causing atrial contraction. The impulse is also conducted to the AV Node & it takes 0.03 sec to travel from SA to AV Node. From AV Node the electrical impulse is conducted to ventricular muscles via the bundle of his, the bundle branches & the purkinje fibres. The bundle branches & the purkinje fibres are collectively called the ventricular conduction system
Alfrina Hany,S.Kp/Brawijaya University
Basic Principles of ECG Booklet
Fundamentals of ECG
A heart controlled by the SA Node is said to be in normal sinus rhythm. The SA Node under influence of the autonomic nervous system (Sympathetic which increases the heart rate via B1 adrenergic receptors; Parasympathetic which slows the heart rate via vagus nerve) The rhythm originates from SA Node because the SA Node depolarizes more frequently (60100 beats/min) than AV Node (40-60 b/m) & ventricular conducting system (30-40 b/m), so the AV Node & ventricular conducting system are captured by the sinus impulse and driven at 60-100 b/m
Fundamentals of ECG
The electrical impulse from the SA node is conducted through the AV node because the atria & ventricles are separated by a fibrous connective tissue ring that has poor conductivity. The AV node provides a path for the impulse to proceed from the atria to ventricles. The AV node together with bundle of His make up the AV junctional tissue. The AV Junc Tissue has its own intrinsic pacemaker activity at 40-60 b/m. if SA node are injured,
the AV Junc Tissue can take over control of the heart rate & rhythm
Alfrina Hany,S.Kp/Brawijaya University
Basic Principles of ECG Booklet
Fundamentals of ECG
EKG Machine
(Ginger & Melvin Och, 1997)
An EKG machine is a highly sensitive voltmeter that measures voltage difference between two points on the body surface The voltage difference comes from depolarization and repolarization of cardiac muscle cells An EKG machine has a positive and a negative terminal Single, Multi Channel
Fundamentals of ECG
Electrophysiology
(Ginger & Melvin Och, 1997) Normal electrical activity of the heart Polarization the phase of readiness. The muscles is relaxed and the cardiac cells are ready to receive an electrical impulse Depolarization the phase of contraction. The cardiac cells have transmitted an electrical impulse, causing the cardiac muscle to contract. Repolarization the recovery phase. The muscles are returning to a relaxed state. ** The cardiac muscle cells have K inside and Na outside the cells. When polarized cell is stimulated by an electrical impulse, K moves outside the cell and Na moves inside.
Alfrina Hany,S.Kp/Brawijaya University
Basic Principles of ECG Booklet
Fundamentals of ECG
.1 mv
paper
Voltage
.5 mv .04 seconds
Time
.20 seconds
Paper speed = 25mm / second
1 small box = 0.040 sec 5 small boxes = 0.20 sec 15 small boxes = 3 sec 30 small boxes = 6 sec 300 small boxes = 1 min
1 mm = 1mV
Fundamentals of ECG
ECG Waveform Analysis
Consist of : 1. Isoelectric Line 2. ECG Waves * P * QRS *T *U 3. ECG Intervals * P-R * QRS 4. ST Segment 5. J Point Picture 1 Picture 1 & 2
Picture 1 & 2 Picture 2 Picture 2
Alfrina Hany,S.Kp/Brawijaya University
Basic Principles of ECG Booklet
Fundamentals of ECG
Picture1
Picture 2
Fundamentals of ECG
EKG Intervals
QRS Complex
P-R Interval = A-V Conduction Time Q-T Interval = Ventricular Contraction Time R-R Interval = Cardiac Cycle Time Heart Rate = 1/R-R Interval
One Cardiac Cycle
P wave T wave Q-T Interval P wave
P-R Interval
Alfrina Hany,S.Kp/Brawijaya University
Basic Principles of ECG Booklet
Fundamentals of ECG
P Wave represents the electrical activity of the original impulse from the SA node and its subsequent spread to the atria. If the P wave is absent or abnormal in shape, it means the impulse originates from outside of the SA node. Normal duration is 0.04 to 0.11 second (maximum about 3 small squares) PR Intervals is measured from the beginning of the P wave to the beginning of the QRS complex. It represents the time taken for the impulse to travel from the SA node to the AV node and the ventricles. Normal duration is 0.12 to 0.20 second (3 to 5 small squares)
Emergency Nursing Chapter, 2001
Fundamentals of ECG
QRS Complex represents the time taken for the impulse to travel from the Bundle of His to the Purkinje fibres, wich results in the contraction of the ventricles. Duration is less than 0.12 second (3 small squares). The complex consists of an initial downward deflection Q wave, an upward deflection R wave and second downward deflection S wave. The configuration of the QRS complex varies from lead to lead and there are several patterns. ST Segment begins at the end of the S wave and terminates at the upstroke of the T wave. The J point (junction point) marks where the S wave ends the ST segment begins. The segment is elevated in acute injury of AMI and depressed in ischemic states Emergency Nursing Chapter, 2001
Alfrina Hany,S.Kp/Brawijaya University
Basic Principles of ECG Booklet
Fundamentals of ECG
T Wave represents the recovery phase after ventricular contraction. Tall, peaked or tented T waves indicate myocardial injury or hyperkalemia. Inverted T waves may mean myocardial ischemia.
QT Interval represents the depolarization& repolarization of the ventricles. Abnormal duration indicates myocardial problems
U Wave represents the recovery period of the Purkinje fibres. It is not present on all ECG waveforms. A prominent u wave may indicated hypercalemia, hypokalemia or digoxin overdose. Emergency Nurses Chapter, 2001
Fundamentals of ECG
Characteristics of a Normal Sinus Rhythm
Regular rhythm Heart rate 60 to 100 per minute P wave precedes every QRS complex. All P waves are similar in shape and size All QRS complexes are similar in shape and size Normal PR interval T waves are after the QRS complexes All waves and interval are normal in duration and position
An Arrhytmia is an abnormal rhythm I.e. either the rate or the contour/position of any individual wave is abnormal
Alfrina Hany,S.Kp/Brawijaya University
10
Basic Principles of ECG Booklet
Obtaining 12 Lead EKG
About 12-Lead EKG Recording 12-Lead EKG Troubleshooting (Problems & Solution) Care & Cleaning
Obtaining 12-lead ECG
12-Lead ECG
The 12 EKG leads measure the electrical activity of the heart from 12 different directions Bipolar Leads (augmented vector): Lead I, Lead II, Lead III Unipolar Leads: aVR, aVL, aVF Precordial Leads: V1, V2, V3, V4, V5, V6
Alfrina Hany,S.Kp/Brawijaya University
11
Basic Principles of ECG Booklet
Obtaining 12-lead ECG
Alfrina Hany,S.Kp/Brawijaya University
12
Basic Principles of ECG Booklet
Alfrina Hany,S.Kp/Brawijaya University
13
Basic Principles of ECG Booklet
Alfrina Hany,S.Kp/Brawijaya University
14
Basic Principles of ECG Booklet
Obtaining 12-lead ECG
Recording the 12-Leads ECG
(Emergency Nurses Chapter, 2001)
Explanation
Tell the patient that the doctor has ordered an ECG and explain the procedure Emphasize that the test takes about a few minutes and that its a safe and painless way to evaluate cardiac function Answer the patients question, and offer reassurance. Preparing him well helps alleviate and promote co-operation
Obtaining 12-lead ECG
Prepping the Patient
Ask the patient to lie supine in the center of the bed with his arms at his sides If he cant tolerate lying flat, raise the head of the bed to semi-Fowlers position Ensure privacy, and expose the patients arms, legs, and chest
Selection of the Electrode Sites
Choose spots that are flat and fleshy, not muscular or bony Clean excess oil or ather substances from the skin to enhance electrode contact. Remember the better
the electrode contact, the better the recording
Alfrina Hany,S.Kp/Brawijaya University
15
Basic Principles of ECG Booklet
Obtaining 12-lead ECG
Steps in recording the ECG
Know your machine Set the ECG paper speed selector to 25mm/second. If necessary, enter the patients identification data. Then calibrate or standardize the machine according to the manufacturers instructions. Plug the cord of the ECG machine into a grounded outlet. If the machine operates on a charged battery, it may not need to be plugged in. Place one or all of the electrodes on the patients chest, based on the type of machine youre using. Make sure all the leads are securely attached, and then turn on the machine.
Obtaining 12-lead ECG Instruct
the patient to relax, lie still, and breathe normally. Ask him not to talk during the recording to prevent distortion of the ECG tracing.
Press
the AUTO button and record the ECG. If youre performing a right chest lead ECG, select the approriate button for recording.
Observe Remove
the quality of the tracing. When the machine finishes the recording, turn it off. the electrodes and clean the patients skin.
Alfrina Hany,S.Kp/Brawijaya University
16
Basic Principles of ECG Booklet
Obtaining 12-lead ECG
Documentation
Date Time Doctors name Nurses name Special circumstances : vital sign, clients condition
Obtaining 12-lead ECG
Troubleshooting
Problem Power line AC interference Cause Poor electrode contact. Dry or dirty electrodes Solution Abrade skin. Use new electrodes. Reapply electrodes.
Power line AC interference
Lead wires may be picking Route lead wires along limbs and away up interference from from other equipment. Fix or move poorly poorly grounded grounded equipment equipment near the patient Patient cable is too Move cardiograph away from the close to the cardiograph patient. Unplug the cardiograph and or other power cords operate on battery only. Move other equipment away from the patient
Power line AC interference
Alfrina Hany,S.Kp/Brawijaya University
17
Basic Principles of ECG Booklet
Problem
Wandering baseline
Cause
Electrode movement. Poor electrode contact and skin preparation Patient movement Respiratory interference
Solution
Be sure that the lead wires are not pulling on the electrodes. Reapply electrodes. Press the filterkey Reassure and relax the patient Move lead wires away from areas with the greatest respiratory motion
Obtaining 12-lead ECG
Obtaining 12-lead ECG
Problem
Tremor or muscle artifact
Cause
Poor electrode placement. Poor electrode contact. Patient is cold
Solution
Clean the electrode site. Be sure the limb electrodes are placed on flat, nonmuscular areas. Warm the patient Reassure and relax the patient. Press the filterkey Attach the limb electrodes near the trunk. Pressthe filterkey
Tense, uncomfortable patient Tremors
Alfrina Hany,S.Kp/Brawijaya University
18
Basic Principles of ECG Booklet
Obtaining 12-lead ECG
Problem
Intermittent or jittery waveform
Cause
Poor electrode contact. Dry electrodes
Solution
Clean the electrode site. Reapply electrodes
Faulty lead wires
Poor print quality Dirty printhead or ink has finished
Replace faulty patient cable
Clean printhead or change the ECG stylus
Emergency Nurses Chapter, 2001
Interpreting Basic ECG
5 Steps of Arrhythmia Interpretation Classification of Arrythmias Recognition & Treatment Acute Myocard Infarct
Alfrina Hany,S.Kp/Brawijaya University
19
Basic Principles of ECG Booklet
Interpreting Basic ECG
5 Steps of Arrhythmia Interpretation
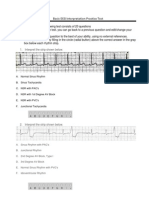
Step 1 : Calculate the Heart Rate
Using the two simplest methods :
10-times / 20-times method
= Number of R-waves in a 6 second strip multiply by 10 = Number of R waves in 3 second strip multiply by 20 = 1500 divided by the number of small boxes between consecutive R-waves
Dividing Methods
Use only if the rhythm is regular. Divide 300 with the big boxes between 2 R waves. If there are also small boxes, add the small boxes to the big boxes. Divide 300 with the combination
Interpreting Basic ECG
Step 2 : Measure the regularity of the R waves
Using methods :
Pen/pencil and paper method Caliper method
Step 3 : Examine the P waves
Present before all QRS Normal configuration Similar size & shape
Alfrina Hany,S.Kp/Brawijaya University
20
Basic Principles of ECG Booklet
Interpreting Basic ECG
Step 4 : Measure the PR interval
Number of small squares between the start of P wave and the beginning of QRS complex not more than 5.
Step 5 : Evaluate the QRS complex
Number of small squares from the beginning to the end of the complex not more than 3. Conclusion
Interpreting Basic ECG
Classification of Arrhythmia
Emergency Nursing Chapter, 2001
According to :
Site of arrhythmia Mechanism of disorder Seriousness of the arrhythmia
Alfrina Hany,S.Kp/Brawijaya University
21
Basic Principles of ECG Booklet
Interpreting Basic ECG
Major Sites
Sinus arrhythmia Atrial arrhythmia AV node arrhythmia Ventricular arrhythmia Tachycardia (HR > 100 beats per minute) Bradycardia (HR < 60 beats per minute) Premature beats Flutter Fibrilation Defects in conduction e.g. heart block
Major Mechanisms
Interpreting Basic ECG
Recognition & Treatment
Ginger & Melvin Och, 1997 Thaler, 2000
Normal Sinus Rhythm Sinus Arrhythmias Atrial Arrhythmias Heart Blocks Ventricular Arrhythmias
Alfrina Hany,S.Kp/Brawijaya University
22
Basic Principles of ECG Booklet
Interpreting Basic ECG
Normal Sinus Rhythm (NSR)
Description This is the normal heart rhythm. It originates in the SA node and follows the appropriate conduction pathways. The rate is normal, and the rhythm is regular. Every beat has a P wave, and every P wave is followed by a ventricular response. EKG Criteria Rate: 60-100 bpm. Rhythm: Regular. A normal variant called Sinus Arrythmia changes rhythm in response to respiration. This is seen most often in young healthy people. Pacemaker: Each beat originates in the SA node. P wave: look the same, all originate from the same locus (SA node) PRI: 120-200 msec QRS: 80-120 msec, narrow unless effected by underlying anomoly
Interpreting Basic ECG
SINUS BRADYCARDIA
Description Sinus bradycardia originates in the SA node. It has reduced rate generally from a reduction in sympathetic input, or excessive vagal (parasympathetic) tone. This rhythm may accompany inferior MI's, hypoxia, hypothermia, or drug reactions. At moderately slow rates, the patient may be asymptomatic. At slower rates, they may become hypotensive and present with symptoms consistant with decreased perfusion: dizziness, syncope, shock like signs and symptoms. Treatment is aimed at increasing the heart rate. Therapies include atropine, transcutaneous and transvenous pacing, epinephrine, dopamine, isoproterenol. EKG Criteria Rate: <60 bpm. Rhythm: Regular generally. Pacemaker: SA node P wave: Present, all originating from SA node, all look the same. PRI: <200 msec, and constant. QRS: Normal, 80-120 msec.
Alfrina Hany,S.Kp/Brawijaya University
23
Basic Principles of ECG Booklet
Interpreting Basic ECG
SINUS TACHYCARDIA
Description This arrythmia originates from the SA node. It is defined as a sinus rhythm exceeding 100 bpm. Sinus tach is a normal rhythm which occurs in response to increased oxygen demand. This occurs with exercise, infection, hypovolemia, hypoxia, myocardial infarct, and in response to stimulant drugs, The rate usually has a gradual onset and elimination. Treatment is not usually needed, but is aimed at treating the underlying condition. EKG Criteria Rate: >100 bpm. Rhythm: Regular, generally. Pacemaker: SA node. P wave: Present and normal, may be buried in T waves in rapid tracings. PRI: 120-200 msec., generally closer to 120 msec. QRS: Normal.
Interpreting Basic ECG
PREMATURE ATRIAL COMPLEXES(PAC)
Description These complexes originate in the atria. They often originate from ectopic pacemaker sites within the atria which results in an abnormal P wave. The complex occurs before the normal beat is expected, hence the prematurity. It is followed by a pause. There are many causes including: increased sympathetic input, exogenous stimulants, drug interactions, AMI, cardiac ischemia, idiopathic. These complexes can indicate increased automaticity. They may lead to re-entry rhythms. EKG Criteria Rate: Underlying rhythm. Rhythm: Irregular with PACs. Pacemaker: Ectopic atrial pacemaker outside SA node. P wave: Ectopic P wave present, generally different than normal SA P wave. PRI: Generall normal range 120-200 msec, but differ from underlying rhythm. QRS: Same as underlying rhythm.
Alfrina Hany,S.Kp/Brawijaya University
24
Basic Principles of ECG Booklet
Interpreting Basic ECG
SUPRAVENTRICULAR TACHYCARDIA (SVT)
Description There are several different types of SVT depending on the site of reentry (accessory pathway, atrioventricular node or atrium). This rapid rhythm starts and stops suddenly. Treatment includes vagal maneuvers, antiarrhythmia medication, radio-frequency ablation or surgical modification of site of reentry. EKG Criteria Rate: 140 - 220 bpm Rhythm: Regular Pacemaker: Reentry circuit Accessory pathway: Normal or short (if down accessory pathway) A-V nodal reentry: Hidden in or at end of QRS PRI: Depends on location of circuit QRS: Normal if accessory pathway used - prolonged (>120 msec) with delta wave
Interpreting Basic ECG
ATRIAL FLUTTER
Description Atrial flutter is characterized by "sawtooth" atrial activity and a conduction ratio to the ventricles of 2:1 to 8:1. It is caused by a reentrant circuit located in the right atrium. It may occur when the atria are enlar ged in chronic obstructive lung disease, mitral or tricuspid disease, pericarditis or post-operatively. Definitive treatment is direct-current cardioversion, surgical or catheter ablation. EKG Criteria Rate: 250 - 350 bpm (atrium) Rhythm: Atrial rate regular, ventricular conduction 2:1 to 8:1 Pacemaker: Reentrant circuit rhythm located in the right atrium P wave: Saw-tooth or picket fence PRI: Constant onset
Alfrina Hany,S.Kp/Brawijaya University
25
Basic Principles of ECG Booklet
Interpreting Basic ECG
ATRIAL FIBRILLATION
Description This is the most common sustained cardiac arrhythmia. It is characterized by an undulating baseline replacing P waves and an irregularly irregular ventricular response. This arrhythmia occurs with hypertension, ischemic, mitral, myocardial and pericardi al disease, thyrotoxicosis, aging and sometimes occurs in normals. Treatment includes anticoagulation, drugs to slow ventricular conduction and/or cardioversion EKG Criteria Undulating baseline replaces P waves Rhythm: Irregularly irregular
Interpreting Basic ECG
FIRST DEGREE AV BLOCK
Description Conduction disturbances are characterized as first degree, second degree Mobitz 1, second degree Mobitz II and complete heart block. The normal P-R interval is 120 - 200 msec. First degree AV block is a constant and prolonged PR interval. Possible etiologies include insult to AV node, hypoxemia, myocardial infarction, digitalis toxicity, ischemia of the conduction system and increased vagal tone but is also seen in normals.
EKG Criteria Rhythm: Regular PRI: >200 msec
Alfrina Hany,S.Kp/Brawijaya University
26
Basic Principles of ECG Booklet
Interpreting Basic ECG
SECOND DEGREE AV BLOCK MOBITZ I (WENKEBACH)
Description Wenkebach is characterized by progressive delay at the AV node until the impulse is completely blocked. Etiologies are the same as cause first degree AV block and is also seen in normals. This conduction abnormality does usually not progress to higher degree heart blocks. EKG Criteria Rhythm: Irregular PRI: Progressive lengthening of PRI until dropped beat. A clue to Wenckebach is that the QRS's appear to occur in groups.
Interpreting Basic ECG
SECOND DEGREE AV BLOCK MOBITZ II
Description This is a higher degree of conduction block then Mobitz I and may progress to complete AV block. AV conduction appears normal until suddenly there is no AV conduction following one P wave. This may occur in a pattern (every 2nd, 3rd or 4th complex) or may occur randomly. This is intermittent block at the AV node and may progress to complete heart block.
EKG Criteria PRI: Constant on conducted complexes until a sudden block of AV conduction. That is, a P wave is abruptly not followed by a QRS
Alfrina Hany,S.Kp/Brawijaya University
27
Basic Principles of ECG Booklet
PREMATURE VENTRICULAR CONTRACTIONS (PVC)
Description A PVC is a depolarization that arises in either ventricle before the next expected sinus beat. The normal sequence of depolarization is altered because the impulse originates in the ventricle. The two ventricules depolarize sequentially insteat of simultaneously. Conduction moves more slowely than through the specialized conduction pathways, this results in a widened QRS complex (greater than 0.12 sec). PVCs may occur as isolated complexes or may occur in pairs, triplets, or in a repeating sequence with normal QRS complexes. Three or more PVCs in a row is considered a run of Ventricular Tachycardia. If it lasts for more than 30 seconds it is designated sustained VT. Treatment: Rarely treated unless symptomatic. PVCs may indicate acute mycardial ischemia requiring rapid intervention including oxygen, NTG, morphine, thrombolytic. Treating with lidocaine will cease the PVC, but won't address the ischemic cause. EKG Criteria Rhythm: Irregular QRS: Is not normal looking. Broadened, greater than 0.12 seconds. P waves are usually obscured by the QRS, ST segment, or T wave of the OVC. The P wave may sometimes be seen as notching during the ST segment or T wave.
Interpreting Basic ECG
BIGEMINY PVCs
Description PVC's may occur in patterns. When each normal complex is followed by a PVC forming groups of 2, the term "ventricular bigeminy" is used.
EKG Criteria QRS: Normal QRS complex followed by premature wide bizarre complex (PVC) in patterns of 2
Alfrina Hany,S.Kp/Brawijaya University
28
Basic Principles of ECG Booklet
Interpreting Basic ECG
VENTRICULAR TACHYCARDIA
Description Ventricular Tachycardia (VT) is defined as three or more beats of ventricular origin in succession at a rate greater than 100 beats per minute. There are no normal (narrow) looking QRS complexes. Consequences of VT depend on accompanying myocardial dysfunction. It may be well tolerated or associated with life-threatening hemodynamic compromise. Treatment: If patient is stable, they are initially treated with lidocaine, procainamide, or bretylium tosylate. Hemodynamically unstable VT (with a pulse) is cardioverted at 200J, 300J, 360J as needed. VT without a pulse is treated like VF and defibrillated. EKG Criteria No normal looking QRS complexes, often bizzare with notching. Width of QRS>0.12 sec. ST segment and T wave are opposite polarity to the QRS. Sinus node may be depolarizing normally. There is usually complete AV dissociation. P waves are sometimes seen between QRS complexes. They have no impact on the QRS complexes. Rate: Generally 100 to 220 bpm Rhythm: Generally regular, on occassion can be modestly irregular.
Interpreting Basic ECG
VENTRICULAR FIBRILLATION
Description
Ventricular Fibrillation is a rhythm in which multiple areas within the ventricles display marked variation in depolarization and repolarization. There is no organized depolarization, therefore the ventricles do not contract as a unit. The myocardium is quivering when visualized grossly. There is no cardiac output. This is the most common arrythmia seen in cardiac arrest from ischemia or infarction. The rhythm is described as coarse or fine VF. Coarse VF indicates recent onset of VF. Prolonged delay without defibrillation results in fine VF and eventually asysyole. Resuscitation becomes more difficult as VF becomes finer. Treatment is always immediate unsynchronized defibrillation at 200J, 300J, 360J for adult patients.
EKG Criteria
Rate: Very rapid, too disorganized to count. Rhythm: Irregular, waveform varies in size and shape No normal QRS complexes. Absent ST segments, P waves, T waves.
Alfrina Hany,S.Kp/Brawijaya University
29
Basic Principles of ECG Booklet
Interpreting Basic ECG
ASYSTOLE
Description Asystole represents the total absence of ventricular electrical activity. Since depolarization does not occur, there is no ventricular contraction. This may occur as a primary event in cardiac arrest, or it may follow VF or pulseless electrical activity (PEA). Ventricular asystole can occur also in patients with complete heart block in whom there is no excape pacemaker. VF may masquerade as asystole; it is best always to check two leads perpendicular to each other to make sure that asystole is not VF. Treatment for each arrythmia is very different. Fine VF which may mimic asystole should be treated with defibrillation. But defibrillating asystole is potentially harmful. Treatment: Epinephrine and Atropine are administered. Consider causes: pulmonary embolism, acidosis, tension pneumothorax, cardiac tamponade, hyperkalemia, hypokalemia, hypoxia, hypothermia, overdose, myocardial infarction. EKG Criteria Complete absence of ventricular electrical activity. Occasional P waves or erratic ventricular beats may be seen. These patients will be pulseless. Treatment must be immediate if the patient is to have any chance at resusctiation. Rate: None Rhythm: None
Interpreting Basic ECG
Myocardial Infarction
ECG will reflect the three pathologic changes of a MI : Ischaemia Injury Infarction/Necrotic
Alfrina Hany,S.Kp/Brawijaya University
30
Basic Principles of ECG Booklet
Interpreting Basic ECG
Zone of Infarction / Necrotic
Area of myocardial necrosis may develop within an hour of an infarct / a few days later. Irreversibel & permanent Pathologic Q wave (1/3 R wave)
Interpreting Basic ECG
Zone of Injury Marked by an elevated ST-segment Result from prolonged lack of blood supply
Alfrina Hany,S.Kp/Brawijaya University
31
Basic Principles of ECG Booklet
Interpreting Basic ECG
Zone of ischaemia Results from an interrupted blood supply Represented by T-wave inversion or J-point depression
Alfrina Hany,S.Kp/Brawijaya University
32
Basic Principles of ECG Booklet
EVOLUTION OF AMI
Assessing AMI
Alfrina Hany,S.Kp/Brawijaya University
33
Basic Principles of ECG Booklet
Conclusion
It is important for nurses not only to record the patients ECG but also interpret it to give the best treatment for their patient based on his/her problem
Alfrina Hany,S.Kp/Brawijaya University
34
Basic Principles of ECG Booklet
Alfrina Hany,S.Kp/Brawijaya University
35
Вам также может понравиться
- Med Surg BulletsДокумент15 страницMed Surg BulletsCin DyОценок пока нет
- Clinical Examination of CVSДокумент33 страницыClinical Examination of CVSmahnoorОценок пока нет
- ECG Study GuideДокумент7 страницECG Study GuideannaОценок пока нет
- Electrocardiography ECGДокумент60 страницElectrocardiography ECGSalman KhanОценок пока нет
- Supraventricular Tachycardia - Life in The Fast Lane ECG LibraryДокумент29 страницSupraventricular Tachycardia - Life in The Fast Lane ECG LibraryYehuda Agus SantosoОценок пока нет
- 106 Prefi Critical Care Nclex ReviewДокумент10 страниц106 Prefi Critical Care Nclex ReviewraigeneОценок пока нет
- Arrhythmia Recognition Part 1 and 2 DOC1178264 Rev2Документ2 страницыArrhythmia Recognition Part 1 and 2 DOC1178264 Rev2Nico Angelo CopoОценок пока нет
- How To Calculate Drug Dosage AccuratelyДокумент7 страницHow To Calculate Drug Dosage AccuratelyAiramCeszDelaCruzОценок пока нет
- Basic EcgДокумент17 страницBasic EcgJohn Vincent DerlaОценок пока нет
- Mechanical Ventilation For NursingДокумент55 страницMechanical Ventilation For NursingAmira AttyaОценок пока нет
- Cardiology Teaching PackageДокумент9 страницCardiology Teaching PackageRicy SaiteОценок пока нет
- Basic EKG Interpretation ExamДокумент13 страницBasic EKG Interpretation Examtwdroppoint100% (1)
- Chapter 47 EKG WorksheetДокумент4 страницыChapter 47 EKG WorksheetChris CamarilloОценок пока нет
- A Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsОт EverandA Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsОценок пока нет
- Arrhythmias Teacher GuideДокумент12 страницArrhythmias Teacher GuideMayer Rosenberg100% (3)
- Jesse Felts PGY2, Not A CardiologistДокумент43 страницыJesse Felts PGY2, Not A Cardiologistイオン天国Оценок пока нет
- Nursing TerminologyДокумент48 страницNursing Terminologyyuhuma_qyu68410% (1)
- Heart BlockДокумент26 страницHeart BlockMihir Patel88% (8)
- Cardiovascular System: By: Marc Anthony Liao RNДокумент59 страницCardiovascular System: By: Marc Anthony Liao RNloveseeker06Оценок пока нет
- Mnemonics PDFДокумент15 страницMnemonics PDFbeingfiredОценок пока нет
- Basic ECG Interpretation Practice Test: DIRECTIONS: The Following Test Consists of 20 QuestionsДокумент10 страницBasic ECG Interpretation Practice Test: DIRECTIONS: The Following Test Consists of 20 Questionsmihaela_bondocОценок пока нет
- Passmedicine 2021 Key Notes MRCP IIДокумент79 страницPassmedicine 2021 Key Notes MRCP IIzehra khowajaОценок пока нет
- Nursing Student Guide TantocksengДокумент0 страницNursing Student Guide TantocksengUmiaziente SuchiОценок пока нет
- Approach To Ventricular ArrhythmiasДокумент18 страницApproach To Ventricular ArrhythmiasDavid CruzОценок пока нет
- Hematologic System2Документ70 страницHematologic System2Jesus Mario LopezОценок пока нет
- DYSRHYTHMIAS (A.k.a. Arrhythmias) Disorders in TheДокумент3 страницыDYSRHYTHMIAS (A.k.a. Arrhythmias) Disorders in TheDarell M. Book100% (1)
- ECG Lead PlacementДокумент3 страницыECG Lead PlacementLord Pozak MillerОценок пока нет
- Practice StripsДокумент9 страницPractice StripsErica Yamamoto50% (4)
- Pharma - Week 3 (Drug Calculations)Документ5 страницPharma - Week 3 (Drug Calculations)MIKAELA DAVIDОценок пока нет
- A Simplified ECG GuideДокумент4 страницыA Simplified ECG GuidecherryОценок пока нет
- Ecg Practice TestДокумент1 страницаEcg Practice TestSoySauceОценок пока нет
- ACLS Algorithms (2011)Документ6 страницACLS Algorithms (2011)senbonsakuraОценок пока нет
- Ch. 1, Lesson 1: What Is The Next Gen NCLEXДокумент4 страницыCh. 1, Lesson 1: What Is The Next Gen NCLEXChantelОценок пока нет
- Schiller Argus LCM - Service Manual PDFДокумент144 страницыSchiller Argus LCM - Service Manual PDFDalvin Amarante100% (2)
- Care of Clients With Problems in OxygenationДокумент5 страницCare of Clients With Problems in OxygenationSkyla FiestaОценок пока нет
- Or ExamДокумент21 страницаOr Examlouie roderosОценок пока нет
- NCLEX ReviewersДокумент19 страницNCLEX ReviewersPaolo Canonizado MilladoОценок пока нет
- Medical-Surgical Nursing Review Flashcards - QuizletДокумент14 страницMedical-Surgical Nursing Review Flashcards - QuizletNursyNurse100% (1)
- Evaluation Checklist Case 7 Bronchial AsthmaДокумент7 страницEvaluation Checklist Case 7 Bronchial AsthmaChristian MendiolaОценок пока нет
- AH2 Hesi ReviewДокумент46 страницAH2 Hesi ReviewJamie Antonini Grant100% (1)
- (K29) Electrocardiogram CVSДокумент43 страницы(K29) Electrocardiogram CVSXeniel AlastairОценок пока нет
- Cardiovascular Anatomy Physiology PDFДокумент22 страницыCardiovascular Anatomy Physiology PDFMahesh ChendakeОценок пока нет
- Tara's Anatomy and Physiology - Aehlert ECGs Made EasyДокумент16 страницTara's Anatomy and Physiology - Aehlert ECGs Made EasyTara McNeillОценок пока нет
- Nurs 1300 Case Studies and Lab WorkДокумент11 страницNurs 1300 Case Studies and Lab WorkNancy Cummings0% (1)
- Dosage & CalculationsДокумент20 страницDosage & CalculationsKnight-Zussette VillarОценок пока нет
- Cardiovascular Disorders Proper 1232011849539043 1Документ111 страницCardiovascular Disorders Proper 1232011849539043 1api-19824701Оценок пока нет
- IV Lab Practice Problems Answers SP 2013 PALДокумент2 страницыIV Lab Practice Problems Answers SP 2013 PALjmraczynskiОценок пока нет
- Medical Surgical Nursing Critical Thinking in Patient Care Single Volume 4th Edition Lemone Test BankДокумент4 страницыMedical Surgical Nursing Critical Thinking in Patient Care Single Volume 4th Edition Lemone Test BankRebeccaGilliamОценок пока нет
- Jennifer Portillo Health Assessment VocabularyДокумент9 страницJennifer Portillo Health Assessment VocabularyJennifer PortilloОценок пока нет
- Pharmacology Pretest XДокумент7 страницPharmacology Pretest Xapi-258903855Оценок пока нет
- Chest TubesДокумент12 страницChest TubesMark Hammerschmidt100% (4)
- Tracheostomy Care SkillsДокумент8 страницTracheostomy Care Skillshoangt2002Оценок пока нет
- Maternal Ob NotesДокумент103 страницыMaternal Ob NotesBoris OrbetaОценок пока нет
- Sinus Bradycardia: I. Sinus Dysrhythmias Description ManagementДокумент4 страницыSinus Bradycardia: I. Sinus Dysrhythmias Description ManagementMargueretti Delos ReyesОценок пока нет
- Physiology of Excitation and Conduction System of Heart by Dr. Mudassar Ali RoomiДокумент17 страницPhysiology of Excitation and Conduction System of Heart by Dr. Mudassar Ali RoomiMudassar Roomi100% (1)
- Safe and Effective Care EnvironmentДокумент8 страницSafe and Effective Care Environmentgretch_carreonОценок пока нет
- Robinson Mejia Preceptor Evaluation of StudentДокумент1 страницаRobinson Mejia Preceptor Evaluation of Studentapi-418543464Оценок пока нет
- Lab ValuesДокумент14 страницLab Valuessylwiasajna100% (2)
- 11 Test Taking Tips & Strategies For Nurses 101Документ5 страниц11 Test Taking Tips & Strategies For Nurses 101xaileenxОценок пока нет
- Qrs Complexes: Fast & Easy Ecgs - A Self-Paced Learning ProgramДокумент49 страницQrs Complexes: Fast & Easy Ecgs - A Self-Paced Learning ProgramMuhammad Hatta HamzahОценок пока нет
- 5 ECG Interpretation With AnswersДокумент48 страниц5 ECG Interpretation With AnswersQusai Ibraheem100% (1)
- Burn 2Документ4 страницыBurn 2lyn_aiОценок пока нет
- ABC Dictionary of Urinary SystemДокумент26 страницABC Dictionary of Urinary Systemaby_romero9750% (2)
- Nervous System AlterationsДокумент45 страницNervous System AlterationsMajesty ParkerОценок пока нет
- Cardiovascular System (Report)Документ2 страницыCardiovascular System (Report)Arlan AbraganОценок пока нет
- NURSING CARE OF ADULTS II: Passbooks Study GuideОт EverandNURSING CARE OF ADULTS II: Passbooks Study GuideОценок пока нет
- Medication ManagementДокумент52 страницыMedication Managementyuhuma_qyu6841100% (1)
- Kebersihan DiriДокумент46 страницKebersihan Diriyuhuma_qyu6841Оценок пока нет
- Perspective of Pediatric NursingДокумент41 страницаPerspective of Pediatric Nursingyuhuma_qyu6841Оценок пока нет
- Tata Laksana Sindroma Koroner Akut: Cholid Tri TjahjonoДокумент96 страницTata Laksana Sindroma Koroner Akut: Cholid Tri TjahjonoAhmad Riva'iОценок пока нет
- Blood PressureДокумент25 страницBlood Pressureyuhuma_qyu6841Оценок пока нет
- All About CHFДокумент180 страницAll About CHFyuhuma_qyu6841Оценок пока нет
- Proses CHN Ns - KumboДокумент27 страницProses CHN Ns - Kumboyuhuma_qyu6841Оценок пока нет
- Cardiovascular Physiology: Heart and CirculationДокумент25 страницCardiovascular Physiology: Heart and Circulationyuhuma_qyu6841Оценок пока нет
- Fluid & Electrolytes ManagementДокумент54 страницыFluid & Electrolytes ManagementasriplОценок пока нет
- The Community Health Nursing Process: Program Evaluation: Presented By: KumboyonoДокумент12 страницThe Community Health Nursing Process: Program Evaluation: Presented By: Kumboyonoyuhuma_qyu6841Оценок пока нет
- Oleh: Septi Dewi Rachmawati: Jurusan Keperawatan Fakultas Kedokteran Universitas BrawijayaДокумент28 страницOleh: Septi Dewi Rachmawati: Jurusan Keperawatan Fakultas Kedokteran Universitas Brawijayayuhuma_qyu6841Оценок пока нет
- ECG Taking Checklist-Ez VersionДокумент2 страницыECG Taking Checklist-Ez VersionKeisha Bartolata100% (1)
- 10 1016@j Amjcard 2018 03 369Документ21 страница10 1016@j Amjcard 2018 03 369Martin De Santiago ValenzuelaОценок пока нет
- H-6801-20-50941 BeneView T6 使用说明书(英文)-25.0Документ472 страницыH-6801-20-50941 BeneView T6 使用说明书(英文)-25.0omar valdiviaОценок пока нет
- How To Read An Electrocardiogram (ECG) - Part One: Basic Principles of The ECG. The Normal ECGДокумент84 страницыHow To Read An Electrocardiogram (ECG) - Part One: Basic Principles of The ECG. The Normal ECGshaine htetОценок пока нет
- Nellcor Khoury Clinical SummaryДокумент2 страницыNellcor Khoury Clinical SummaryjematheuОценок пока нет
- The Mechanism Isorhythmic: of Synchronization A-VДокумент11 страницThe Mechanism Isorhythmic: of Synchronization A-VSheila AdiwinataОценок пока нет
- Dr. Firman Leksmono SP - JP Basic ECG Interpretation For StudentДокумент54 страницыDr. Firman Leksmono SP - JP Basic ECG Interpretation For Studentacha kyungsooОценок пока нет
- 2016ps79 Iot ProjectДокумент50 страниц2016ps79 Iot ProjectpumaОценок пока нет
- WARDEN Presentation July 2017 FinalДокумент9 страницWARDEN Presentation July 2017 FinalrickylimaperuОценок пока нет
- SR AIIMS Supe-60 MT-6 - (27-12-2022) - Key & Solution - FinalДокумент15 страницSR AIIMS Supe-60 MT-6 - (27-12-2022) - Key & Solution - FinalAdithya BharadwajОценок пока нет
- Tif30Документ49 страницTif30HCX dghhqОценок пока нет
- 11-1.InBody S10 ManualДокумент64 страницы11-1.InBody S10 ManualMina Magdy FahmyОценок пока нет
- Spek MX 450 STDRДокумент2 страницыSpek MX 450 STDRubaОценок пока нет
- Risk Stratification of The J Wave SyndromeДокумент11 страницRisk Stratification of The J Wave SyndromepuchioОценок пока нет
- Campugan Jay Patho AssignmentДокумент27 страницCampugan Jay Patho AssignmentJAY M. CAMPUGANОценок пока нет
- Catalogo Fluke Biomedical 2019Документ37 страницCatalogo Fluke Biomedical 2019Fabricio AlmeidaОценок пока нет
- Irjet V4i5119 PDFДокумент7 страницIrjet V4i5119 PDFAnonymous plQ7aHUОценок пока нет
- Esaote Ecg p80 Operting ElementsДокумент28 страницEsaote Ecg p80 Operting ElementsDerkis MarcanoОценок пока нет
- Axcent CMS EN 052020Документ1 страницаAxcent CMS EN 052020Shaif ZahrahОценок пока нет
- Emotion Recognition Based On Wireless, Physiological and Audiovisual Signals: A Comprehensive SurveyДокумент18 страницEmotion Recognition Based On Wireless, Physiological and Audiovisual Signals: A Comprehensive SurveyOliver GuidettiОценок пока нет
- The Electrocardiogram: Ecg: by Gaurishi Agarwal, 32Документ17 страницThe Electrocardiogram: Ecg: by Gaurishi Agarwal, 32Gaurishi AgarwalОценок пока нет
- QRS-Card Stress ECG System: HighlightsДокумент2 страницыQRS-Card Stress ECG System: HighlightsJhancarlos JuanmacalderonОценок пока нет