Академический Документы
Профессиональный Документы
Культура Документы
Caustic Ingestion Guideline
Загружено:
Moises RiveraИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Caustic Ingestion Guideline
Загружено:
Moises RiveraАвторское право:
Доступные форматы
Clinical Guideline Caustic Ingestion
Toxicology consultation prior to initiation is strongly recommended ** Any signs/symptoms indicative of gastrointestinal perforation warrants resuscitation and immediate surgical consultation. The absence of oropharyngeal injury does not reliably rule out potentially serious caustic injury to the gastrointestinal tract (38% patients with esophageal burns found to have no OP burns) Acids cause immediate coagulative necrosis which tends to self-limit injury. Alkalis cause liquifactive necrosis resulting in deeper penetration and more extensive injury.
1.) Decontamination
Blind nasogastric tube insertion is contraindicated due to risk of accidental perforation. Activated charcoal is contraindicated. Do not attempt to neutralize pH with acid or alkaline lavage, this may cause exothermic reaction and potential for thermal injury. Dilution with milk is only found to be effective if given within minutes of ingestion. Unless the patient must be kept NPO for a clearly indicated endoscopy, it is OK to give water or milk if the patient is able and willing to swallow. In general, there is no need for oral dilution.
2.) Evaluation for Perforation
Any signs/symptoms indicative of gastrointestinal perforation warrants resuscitation and immediate surgical consultation. Plain chest and abdominal x-rays are not sensitive, but may aid in the rapid diagnosis of perforation. Contrast studies may also fail to detect perforations, but extravasation of contrast outside of GI tract is diagnostic. Water-soluble contrast is recommended initially as it is less irritating to tissues in case of perforation. CT scanning may have a role in the evaluation of caustic injury but has not been studied.
2.) Endoscopy
Endoscopy is the standard diagnostic tool for evaluation of caustic injury. Scope should be performed preferentially within the first 12 hours, but no later than 24 hours (wound softening starting on the 2nd day may increase the risk of perforation) Debate exists regarding when endoscopy is indicated in asymptomatic patients after caustic ingestion. Because studies have shown repeatedly that a small percentage of patients will have esophageal and/or gastric injury in the absence of oral burns or dysphagia, some experts advocate endoscopy for all patients regardless of symptoms. It is my opinion that endoscopy is unnecessary for asymptomatic patients after unintentional ingestion (See below). Endoscopy is helpful to diagnose and grade the extent of gastrointestinal injury. A nasogastric tube may be placed under endoscopic guidance should significant injuries be discovered. Grade I = no esophageal stricture risk Grade IIB = 75% will develop stricture Grade III = 100% will develop stricture < Grade IIB = no increased cancer risk > Grade IIB = 1000x risk of cancer (latency 20-40 years) Grade II and III = increased risk of severe complications (stricture, motility problems, TE fistula, erosion into great vessels)
Caustic Ingestion
Un-intentional / Pediatric Ingestion
Intentional / Adult Ingestion
Asymptomatic? Yes
No
GI Medicine Consultation
No Endoscopy
3.) Management issues
A.) Steroids NEJM article of pediatric caustic ingestions showed a possible modest benefit of corticosteroids in patients with grade IIB injury only. In primate studies, corticosteroids significantly increased mortality due to overwhelming sepsis. In the same study, mortality returned to baseline when prophylactic antibiotic coverage was given. Recommendation: I do not feel that the evidence supports corticosteroids for any esophageal burn grade. If you do elect to give corticosteroid for grade IIB injury, give with prophylactic antibiotics. B.) Antibiotics There is no data to support the use of prophylactic antibiotics except (possibly) in conjunction with corticosteroids. C.) Nasogastric tube placement Cases of esophageal perforation associated with blind NGT placement are reported. In high-grade injuries placement of an NGT early may be desirable to allow access to the stomach. Recommendation: NG tube should never be placed blindly. In high grade injuries (grade IIB or III), placement of a feeding tube under endoscopic guidance may be helpful to maintain access to the stomach. D.) Antacids H2 blockers or PPIs are not recommended as these medications may allow for increased gastric bacterial growth.
Special Cases:
A.) Household Bleach (sodium hypochlorite) Grade II and III injuries only occur after large volume ingestions of concentrated bleach. Only patients complaining of pain, high concentration ingestions, or large volume ingestions need endoscopic evaluation. B.) Button Batteries may cause serious corrosive injury possibly related to leakage of contents or local discharge of electrical current. Most injuries occur due to impaction in the esophagus and subsequent perforation. Most cases involve large (25 mm) batteries. If any signs / symptoms of perforation, immediate surgical consultation is indicated. Locations:
Airway or Esophagus emergent endoscopic removal Stomach If symptomatic need emergent removal. If asymptomatic, the batteries usually pass out uneventfully with the stool. Consider giving PEG and rechecking in 2 days. (In rare case of child less than 6 years and battery 25mm, consider endoscopic removal) Beyond pylorus follow with repeat x-ray in 7 days. Consider surgical consultation if not passed. C.) Hydrofluoric Acid extreme systemic toxicity is expected. Immediate toxicology or poison center consultation is indicated.
Last revised: 2/2007
Вам также может понравиться
- Diverticulitis Cure: The Ultimate Diverticulitis Diet: Diverticulitis Recipes: Your Ultimate Diverticulitis CookbookОт EverandDiverticulitis Cure: The Ultimate Diverticulitis Diet: Diverticulitis Recipes: Your Ultimate Diverticulitis CookbookОценок пока нет
- Caustic InjuryДокумент26 страницCaustic InjuryGino FTОценок пока нет
- Post-cholecystectomy Bile Duct InjuryОт EverandPost-cholecystectomy Bile Duct InjuryVinay K. KapoorОценок пока нет
- Standard Treatment Guidelines General Surgery: Ministry of Health & Family Welfare Govt. of IndiaДокумент73 страницыStandard Treatment Guidelines General Surgery: Ministry of Health & Family Welfare Govt. of IndiaiuytrerОценок пока нет
- Colitis: A Practical Approach to Colon and Ileum Biopsy InterpretationОт EverandColitis: A Practical Approach to Colon and Ileum Biopsy InterpretationAnne Jouret-MourinОценок пока нет
- Gastroduodenal PerforationДокумент4 страницыGastroduodenal PerforationMaresp21Оценок пока нет
- Advanced Colonoscopy: Principles and Techniques Beyond Simple PolypectomyОт EverandAdvanced Colonoscopy: Principles and Techniques Beyond Simple PolypectomyToyooki SonodaОценок пока нет
- Caustic Agent RevДокумент32 страницыCaustic Agent RevAziz AndriyantoОценок пока нет
- Caustics & Cholinesterase-Inhibiting Insecticides Seminar (Final Version)Документ27 страницCaustics & Cholinesterase-Inhibiting Insecticides Seminar (Final Version)Laith Al TamimiОценок пока нет
- Corrosive InjuryДокумент6 страницCorrosive InjuryCristian O. Saavedra RodriguezОценок пока нет
- Interventional Approaches Gallbladder DiseaseДокумент9 страницInterventional Approaches Gallbladder DiseaseAntônio GoulartОценок пока нет
- Case Report: Iatrogenic Intraperitoneal Bladder Injury - Presentation & Its ManagementДокумент2 страницыCase Report: Iatrogenic Intraperitoneal Bladder Injury - Presentation & Its ManagementcindyamandaОценок пока нет
- Apgh 3 1Документ2 страницыApgh 3 1Rashmi Ranjan BeheraОценок пока нет
- Intestinal DisordersДокумент11 страницIntestinal DisordersJessica0% (1)
- Corrosive Jabulay SupДокумент5 страницCorrosive Jabulay SupManasi TanwarОценок пока нет
- Endoscopic Retrograde Cholangiopancreatography (ERCP)Документ3 страницыEndoscopic Retrograde Cholangiopancreatography (ERCP)princess0fdeathОценок пока нет
- Surgical ExamДокумент302 страницыSurgical ExamHossam SabriОценок пока нет
- Pan EndosДокумент3 страницыPan EndossilviaОценок пока нет
- Esophageal Disorders: Suazo, Trisha Mae S. 3BSN-AДокумент11 страницEsophageal Disorders: Suazo, Trisha Mae S. 3BSN-AKenneth OpinaОценок пока нет
- Sas 40Документ2 страницыSas 40Sistine Rose LabajoОценок пока нет
- Appendicitis&AppendectomyДокумент5 страницAppendicitis&AppendectomyJestine Joy CustodioОценок пока нет
- Surgical Management of Ulcerative ColitisДокумент56 страницSurgical Management of Ulcerative ColitisMehtab JameelОценок пока нет
- Tubular Ileal Duplication Causing Small Bowel Obstruction in A ChildДокумент5 страницTubular Ileal Duplication Causing Small Bowel Obstruction in A ChildDiego Leonardo Herrera OjedaОценок пока нет
- Abdominal TraumaДокумент29 страницAbdominal TraumaKai XinОценок пока нет
- Clinical Practice Guidelines - Acute AppendicitisДокумент3 страницыClinical Practice Guidelines - Acute AppendicitisJamie Sebastian75% (4)
- Octreotide 2017Документ10 страницOctreotide 2017Issa AbuzeidОценок пока нет
- And Management of Gallstone-Related Diseases in Non-Pregnant Adults - 2019-01-31T04-08-16 PDFДокумент15 страницAnd Management of Gallstone-Related Diseases in Non-Pregnant Adults - 2019-01-31T04-08-16 PDFjuan camilo casadiegoОценок пока нет
- BTK Quick Hits Final PDFДокумент24 страницыBTK Quick Hits Final PDFcusom34Оценок пока нет
- BTK Quick Hits FinalДокумент19 страницBTK Quick Hits FinalMujahed LaswiОценок пока нет
- 2013 WSES (World Society of Emergency Surgery) Guidelines For Management of Intra-Abdominal InfectionsДокумент53 страницы2013 WSES (World Society of Emergency Surgery) Guidelines For Management of Intra-Abdominal InfectionsNyimas NursyarifahОценок пока нет
- Diagnosis and Management of Klatskin Tumor: April 2010Документ6 страницDiagnosis and Management of Klatskin Tumor: April 2010Feby Kurnia PutriОценок пока нет
- Investigations:) - To Diagnose Lesions in The Oesophageal orДокумент4 страницыInvestigations:) - To Diagnose Lesions in The Oesophageal orMarwan M.Оценок пока нет
- General Surgery Board RevieДокумент69 страницGeneral Surgery Board RevieFadi Alkhassawneh88% (8)
- A Patient With Caustic Ingestion Injury: Brinna Anindita Budi WidodoДокумент27 страницA Patient With Caustic Ingestion Injury: Brinna Anindita Budi WidodoBrinna Anindita SatriaОценок пока нет
- Abdominal Injuries Last FormДокумент25 страницAbdominal Injuries Last FormOmar MohammedОценок пока нет
- Principles of Management of Poisoned Patient: 09/09/1440 DR Abdelmonem G. Madboly 1Документ19 страницPrinciples of Management of Poisoned Patient: 09/09/1440 DR Abdelmonem G. Madboly 1JyotiОценок пока нет
- Quiz With AnswersДокумент8 страницQuiz With Answersval284yОценок пока нет
- Z - 2016-03 - Spontaneous Rupture of Pancreatic Pseudocyst - Report of Two CasesДокумент3 страницыZ - 2016-03 - Spontaneous Rupture of Pancreatic Pseudocyst - Report of Two CasesNawzad SulayvaniОценок пока нет
- Billroth I & IIДокумент5 страницBillroth I & IIRoxieparkerОценок пока нет
- Indian AediatricДокумент2 страницыIndian AediatricMuhamad RizauddinОценок пока нет
- Care With Git PTДокумент16 страницCare With Git PTHafidz Ma'rufОценок пока нет
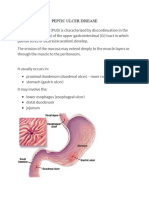
- Peptic Ulcer DiseaseДокумент22 страницыPeptic Ulcer DiseasebhibhiОценок пока нет
- Bowels Open 6 Times Per 24 Hours: Document ControlДокумент7 страницBowels Open 6 Times Per 24 Hours: Document ControlKeith PohlОценок пока нет
- Oncology Nursing Exam and RationaleДокумент9 страницOncology Nursing Exam and RationaleTomzki Cornelio100% (5)
- Management of Iatrogenic Colorectal Perforation: From Surgery To EndosДокумент6 страницManagement of Iatrogenic Colorectal Perforation: From Surgery To EndosDiego CadenaОценок пока нет
- Surgical Bed Side ProceduressДокумент62 страницыSurgical Bed Side Proceduressdrhiwaomer100% (1)
- Caustic Ingestion: Has The Role of The Gastroenterologist Burnt Out?Документ4 страницыCaustic Ingestion: Has The Role of The Gastroenterologist Burnt Out?Ronald VillalobosОценок пока нет
- ERCP Procedure GuideДокумент7 страницERCP Procedure GuideFachrur RodjiОценок пока нет
- Abdominal Stab WoundДокумент5 страницAbdominal Stab WoundHemingmingОценок пока нет
- Diagnosing Gastric Volvulus in Chest X-Ray: Report of Three CasesДокумент4 страницыDiagnosing Gastric Volvulus in Chest X-Ray: Report of Three CasesSuraj KurmiОценок пока нет
- Intestinal Obstruction AditiДокумент67 страницIntestinal Obstruction Aditiaditi BahugunaОценок пока нет
- Integ 4 Answer PDFДокумент12 страницInteg 4 Answer PDFRhasdie MandiОценок пока нет
- Safe CholecystectomyДокумент60 страницSafe CholecystectomyCarlos Reyes100% (1)
- QuizДокумент8 страницQuizJohara Mae De RamaОценок пока нет
- Journal of Pharmaceutical and Scientific Innovation: Case StudyДокумент3 страницыJournal of Pharmaceutical and Scientific Innovation: Case StudyDinoCsbrowОценок пока нет
- Peptic UlserДокумент8 страницPeptic UlserSubhanshu DadwalОценок пока нет
- University of Maryland Medical Center Fluconazole (Diflucan®)Документ6 страницUniversity of Maryland Medical Center Fluconazole (Diflucan®)damondouglasОценок пока нет
- Ultasonographic Detection and Assessment of The Severity of Crohn's Disease Recurrence After Ileal ResectionДокумент12 страницUltasonographic Detection and Assessment of The Severity of Crohn's Disease Recurrence After Ileal ResectionСергей СадовниковОценок пока нет
- M Digestion" Absorption" EliminationДокумент104 страницыM Digestion" Absorption" EliminationChristine Carol FilipinasОценок пока нет
- Patient Preparation For Radiological ProcedureДокумент105 страницPatient Preparation For Radiological ProcedureShidevОценок пока нет
- Gothic Earth GrimoireДокумент8 страницGothic Earth Grimoirejaxnjuva100% (1)
- Safety Data Sheet: 1. Identification of The Material and Supplier Sodium Aluminate SolutionДокумент7 страницSafety Data Sheet: 1. Identification of The Material and Supplier Sodium Aluminate SolutionHeinrich ManaligodОценок пока нет
- Msds HCLДокумент7 страницMsds HCLDachi Diputro NikoОценок пока нет
- Material Safety Data Sheet: Section 1. Chemical Product and Company IdentificationДокумент3 страницыMaterial Safety Data Sheet: Section 1. Chemical Product and Company IdentificationZeckОценок пока нет
- SKF Food Line Y Bearing UnitsДокумент120 страницSKF Food Line Y Bearing UnitsJurun_BidanshiОценок пока нет
- Safety H2so4Документ8 страницSafety H2so4vtpsОценок пока нет
- Instruction Manual MB45 Moisture AnalyzerДокумент70 страницInstruction Manual MB45 Moisture AnalyzerAulia AdimОценок пока нет
- MSDS - Avesta Pickling Gel 122Документ9 страницMSDS - Avesta Pickling Gel 122geoanburajaОценок пока нет
- MegaCleanActive SDSДокумент7 страницMegaCleanActive SDSEdgar Uriel Castillejos DíazОценок пока нет
- 6 Low PH Corrosion During ServiceДокумент13 страниц6 Low PH Corrosion During ServiceWalter RuedaОценок пока нет
- 02-Lab Safety Symbols PDFДокумент19 страниц02-Lab Safety Symbols PDFMark Christian Dimson GalangОценок пока нет
- Pre Lab Electrophilic Aromatic SubstitutionДокумент3 страницыPre Lab Electrophilic Aromatic SubstitutionSana RajpootОценок пока нет
- API 653.docx BrochureДокумент10 страницAPI 653.docx BrochureLily & Ameer لى لى و أميرОценок пока нет
- GDCR - Second RevisedДокумент290 страницGDCR - Second RevisedbhaveshbhoiОценок пока нет
- List of PPEДокумент4 страницыList of PPEBinayОценок пока нет
- SW Management (Regulations 7-10) (EiMAS)Документ100 страницSW Management (Regulations 7-10) (EiMAS)Corona VirusОценок пока нет
- Caustic PermagnateДокумент3 страницыCaustic Permagnateg_sanchetiОценок пока нет
- Emergency and Disaster Response To Chemical Releases: Technician Level TrainingДокумент29 страницEmergency and Disaster Response To Chemical Releases: Technician Level Trainingeduardo burgosОценок пока нет
- Material Safety Data Sheet: 1 IdentificationДокумент6 страницMaterial Safety Data Sheet: 1 IdentificationTaufik TajudinОценок пока нет
- 93c86443-d757-47e5-9b45-b2510e8d861bДокумент1 страница93c86443-d757-47e5-9b45-b2510e8d861bOzi SajaОценок пока нет
- Little Boy Care Chemicals - 14 App 2021 January 11 RM Eng Ver1Документ14 страницLittle Boy Care Chemicals - 14 App 2021 January 11 RM Eng Ver1sadhikbtech_91903923Оценок пока нет
- Material Safety Data Sheet: Hydrochloric Acid, 37% MSDSДокумент7 страницMaterial Safety Data Sheet: Hydrochloric Acid, 37% MSDSFebrianto DimazОценок пока нет
- Material Safety Data Sheet: 1 IdentificationДокумент6 страницMaterial Safety Data Sheet: 1 IdentificationMuhammad Shadab100% (1)
- LY-HY5052 Safety Data SheetДокумент12 страницLY-HY5052 Safety Data SheetAnkit GuptaОценок пока нет
- Potential Hazards in Chemical IndustriesДокумент33 страницыPotential Hazards in Chemical IndustriesAMOL RASTOGI 19BCM0012Оценок пока нет
- Caustic Soda Pels (Axiall) SDSДокумент4 страницыCaustic Soda Pels (Axiall) SDSDeo FactuarОценок пока нет
- Elastomers OverviewДокумент2 страницыElastomers OverviewJobita JMОценок пока нет
- Mercerizing Cellulosic Fibres & Its EffectsДокумент5 страницMercerizing Cellulosic Fibres & Its EffectsMohammed Atiqul Hoque ChowdhuryОценок пока нет
- 2016 Analysis of Copper-Bearing Rocks and Minerals For Their Metal Content Using Visible Spectros PDFДокумент7 страниц2016 Analysis of Copper-Bearing Rocks and Minerals For Their Metal Content Using Visible Spectros PDFRosa PatiñoОценок пока нет
- Inox DMДокумент6 страницInox DMZoran DanilovОценок пока нет
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)От EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Рейтинг: 3 из 5 звезд3/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedОт EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedРейтинг: 4.5 из 5 звезд4.5/5 (82)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDОт EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDРейтинг: 5 из 5 звезд5/5 (3)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionОт EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionРейтинг: 4 из 5 звезд4/5 (404)
- The Age of Magical Overthinking: Notes on Modern IrrationalityОт EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityРейтинг: 4 из 5 звезд4/5 (32)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeОт EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeРейтинг: 2 из 5 звезд2/5 (1)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesОт EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesРейтинг: 4.5 из 5 звезд4.5/5 (1412)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsОт EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsОценок пока нет
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsОт EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsРейтинг: 4 из 5 звезд4/5 (4)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsОт EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsРейтинг: 5 из 5 звезд5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisОт EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisРейтинг: 4.5 из 5 звезд4.5/5 (42)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaОт EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Obesity Code: Unlocking the Secrets of Weight LossОт EverandThe Obesity Code: Unlocking the Secrets of Weight LossРейтинг: 4 из 5 звезд4/5 (6)
- Why We Die: The New Science of Aging and the Quest for ImmortalityОт EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityРейтинг: 4.5 из 5 звезд4.5/5 (6)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisОт EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisРейтинг: 3.5 из 5 звезд3.5/5 (2)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeОт EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeРейтинг: 4.5 из 5 звезд4.5/5 (254)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.От EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Рейтинг: 4.5 из 5 звезд4.5/5 (110)
- To Explain the World: The Discovery of Modern ScienceОт EverandTo Explain the World: The Discovery of Modern ScienceРейтинг: 3.5 из 5 звезд3.5/5 (51)
- Critical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsОт EverandCritical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsРейтинг: 4.5 из 5 звезд4.5/5 (39)
- The Marshmallow Test: Mastering Self-ControlОт EverandThe Marshmallow Test: Mastering Self-ControlРейтинг: 4.5 из 5 звезд4.5/5 (60)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingОт EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingРейтинг: 4 из 5 звезд4/5 (1138)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessОт EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessРейтинг: 4.5 из 5 звезд4.5/5 (328)