Академический Документы
Профессиональный Документы
Культура Документы
PAthos Exam 3 Disorders of The Abd.
Загружено:
simonedarling0 оценок0% нашли этот документ полезным (0 голосов)
132 просмотров9 страницAlimentary tract Functions Ingestion of food Propulsion of food and wastes Secretion of mucus, water, and enzymes to break down food Mouth Tongue surface has chemoreceptors (taste buds) Chemical messengers, relay to brain - salty, sweet, sour, etc. 32 permanent teeth (adult mouth) Starts breakdown of food, mastication.
Исходное описание:
Оригинальное название
PAthos exam 3 disorders of the abd.
Авторское право
© Attribution Non-Commercial (BY-NC)
Доступные форматы
DOCX, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документAlimentary tract Functions Ingestion of food Propulsion of food and wastes Secretion of mucus, water, and enzymes to break down food Mouth Tongue surface has chemoreceptors (taste buds) Chemical messengers, relay to brain - salty, sweet, sour, etc. 32 permanent teeth (adult mouth) Starts breakdown of food, mastication.
Авторское право:
Attribution Non-Commercial (BY-NC)
Доступные форматы
Скачайте в формате DOCX, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
132 просмотров9 страницPAthos Exam 3 Disorders of The Abd.
Загружено:
simonedarlingAlimentary tract Functions Ingestion of food Propulsion of food and wastes Secretion of mucus, water, and enzymes to break down food Mouth Tongue surface has chemoreceptors (taste buds) Chemical messengers, relay to brain - salty, sweet, sour, etc. 32 permanent teeth (adult mouth) Starts breakdown of food, mastication.
Авторское право:
Attribution Non-Commercial (BY-NC)
Доступные форматы
Скачайте в формате DOCX, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 9
Disorders of the Abdomen
Julie Mann, ACNP
HSCI 302
• Structure of the Digestive System
○ One big hollow tube from mouth to rectum.
• Alimentary Tract Functions
○ Ingestion of food
○ Propulsion of food and wastes
○ Secretion of mucus, water, & enzymes to break down food
○ Mechanical digestion of food particles
○ Chemical digestion of food particles
○ Absorption of digested food
○ Elimination of waste products by defecation
• Mouth
○ Tongue surface has chemoreceptors (taste buds)
• Chemical messengers, relay to brain - salty, sweet, sour,
etc.
○ 32 permanent teeth (adult mouth)
• Starts breakdown of food, mastication.
○ Salivary Glands
Lubricate food, break down food (particularly CHO)
• Submandibular Glands - floor of mouth
• Sublingual Glands - under tongue
• Parotid Glands - upper part of mandible, secrete through
stenson ducts.
• Esophagus
○ Conducts food from oropharnyx to stomach
○ Peristalsis
• Sequential relaxation and contraction.
○ Upper and
• Keeps air from entering stomach during inspiration.
○ Lower Esophageal Sphincter (cardiac sphincter)
• Prevents food from regurgitating back up from stomach
into esophagus.
• Swallowing
○ Oropharyngeal Phase (take 1 second)
i. Food made into bolus by tongue, pushed to back of
pharnyx
i. Superior constrictor muscle of pharnyx contracts
i. Respiration is inhibited, epiglottis slides down
○ Esophageal Phase (5-10sec)
i. Bolus enters the esophagus
i. Wave of relaxation travels over esophagus
i. Peristalsis to the lower esophageal sphincter
i. Bolus enters the stomach, sphincter returns to resting tone
• GI wall Structure (4 layers) inner to out
1. Mucosa
i. Lining of epithelial tissues and underlying tissue, and
smooth muscles.
i. Secrete mucus to protect from acid.
i. Enzymes released to break down food products.
i. Helps protect body against foreign antigens/pathogens.
1. Submucosa
i. Dense CT
i. Contains blood vessels and nervous tissue.
i. Layer that secretes digestive enzymes.
1. Muscularis
i. Longitudinal muscles, circular muscles, help propel food
through digestive tract.
1. Adventitia (serosal layer)
Squamous epithelium and some CT.
• Peritoneum
Double layered tissue with space in middle (potential
space) with fluid (peritoneal fluid)
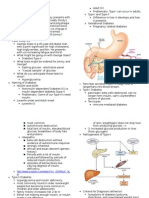
• Stomach
○ Food enters through lower esophageal sphincter, enzymes
secreted, food moved down through pylorus into duodenum.
○ Blood supply is abundant, therefore problematic when ulcers
occur.
• Gastric Motility
○ Peristaltic contractions influenced by neural and hormonal
activity
• Neural - vegas nerve
• Hormonal - Gastrin, modolin, etc. help control peristaltic
contractions.
○ Mixing and emptying of food (chyme) from stomach takes
several hours
○ Rate of Gastric emptying depends on:
• Volume
Larger volume increases rate of gastric emptying.
• Osmotic Pressure
Non-isotonic food decreases rate of emptying.
• Chemical Composition of Gastric Contents
Fat takes longer to empty.
• Gastric Secretion
○ Mucus
• protects gastric mucosa from acid
○ Acid-formed in the parietal cells, secretion is stimulated by
acetylcholine, gastrin, and histamine and inhibited by
somatostatin
• Decrease rate when exposed to unpleasant odors.
• Dissolves food fibers
• Acts as bacteriocide against swallowed organisms
• Chronic situation increases acid secretion
○ Pepsin- secreted from chief cells proteolytic enzyme.
• Breaks down protein (all in stomach, so if pushed out too
rapidly it won't digest properly in small intestine)
• Inactivated in duodenum (alkaline environment).
• G.I. Hormones
○ Stomach
• Gastrin
Secreted from G-cells, located in antum of stomach
Increase gastric acid secretion into stomach.
• Ghrelin
Polypeptide hormone, produced by endocrine cells
inside of fundus of stomach.
Stimulates body to intake food and reduces energy
expenditure at time of ingestion of food.
○ Intestine
• Secretin
Secreted by S-Cells
Inhibits secretion of gastrin --> less acids.
• Cholecystokinin (CCK)
Secreted by I-Cells in mucosa of small intestine
Downregulates action of secretin. Increase gastric
secretion.
○ GLP-1 (not covered)
○ GIP (not covered)
• Small Intestine
○ Duodenum, jejunum, & ileumIleocecal valve
○ Microvilli & brush border
• Microvilli - folds that create a huge surface area where
electrolytes and fluids can be absorbed during digestive
process.
• Length gives time for food to digest (CHO further broken
down, protein, fats)
○ Digestion aided by pancreatic enzymes, intestinal enzymes,
and bile salts
• Intestinal Motility (Small Intestine)
○ Enteric Nervous System Innervation
• myenteric (Auerbach) plexus
Nervous tissue sits between longitudinal and circular
muscles in small intestine.
Controls movement of bolus.
• submucosal (Meissner) plexus
Sits between mucosal layer and circular layer
Controls mixing movement.
Controls local blood flow.
○ ANS Innervation
• Mainly Parasympathetic- vagus nerve
Stimulate both plexuses to increase intestinal motility
• Sympathetic
Inhibits intestinal motility.
○ Intestinal Smooth Muscle
• slow wave activity
Muscle cells within small intestinal wall with generate
rhythmic waves, 12 waves/min.
• How own intrinsic rate for firing.
• Large Intestine
○ Cecum, appendix (no function, possibly immune), colon,
rectum, and anal canal
○ Colon
• Ascending, Transverse, Descending, & Sigmoid
○ Ileocecal valve to cecum, O’Briene sphincter (from descending
to sigmoid), Internal (unconscious control) and External
(conscious control) anal sphincters (defecation)
• Colonic Motility
○ Two types of movement
• Haustrations
Water absorbed from chyme by mixing it around.
• propulsive mass movements
Move forward to anal canal.
○ Defecation
• initiated by mass movements
• controlled by internal and external sphincters (poop!)
• Anorexia: loss of appetite
○ Any loss of appetite, forerunner to nausea.
• Nausea: subjective sensation
• Retching: rhythmic spasmodic movements
○ but not expelling, vs. vomiting.
• Vomiting: sudden forceful oral expulsion of the contents of the
stomach
○ Activation of vomiting center of brain.
○ Chemoreceptors that send the message.
• Dysphasia
○ Difficulty of swallowing.
○ Problems with Cranial nerves 5,9,10.
○ Narrowing of esophagus.
○ Stroke
• Hiatal Hernia
○ Herniation of stomach up through diaphragm (see pics in book)
○ Sliding
• Bell shaped protrusion through stomach.
• Pouch slides up and back down
• Gastric acid can come back up through esophagus
○ Paraesophageal
• Whole separate portion of stomach comes up through
diaphragm opening.
• Gastroesophageal Reflux
○ LES relaxes 1-2 hours after eating
○ Can cause inflammatory response called reflux esophagitis
• GERD
○ Persistant reflux of gastric contents
○ Assoc. with weak LES and delayed gastric emptying (chyme
and acids)
○ Tell pt. to sit up so that chyme doesn't flow back up over LES.
○ Symptoms: heartburn
○ Reflux esophagitis: mucosal injury, hyperemia (increase of
blood to area), inflammation.
• More of a problem when chronic
○ Complications:
• Strictures
Narrowing within esophagus
• Barrett esophagus
Form of metaplasia, cells change over esophagus,
when untreated --> increased risk towards esophageal
cancer.
• Peptic Ulcer Disease
○ Any break, or ulceration, in the protective mucosal lining of the
lower esophagus, stomach, or duodenum
○ Acute/Chronic, Superficial/Deep
• Chronic - Decrease mucosal secretion, ie smokers.
• Superficial inner lining, vs deep through to the muscles.
• Acid kills/desolves cells in stomach
○ Risk Factors?
• Smoking, advance age, habitual use of anti-inflammatories
(aspirin), chronic alcohol, emphysema, RA, exposure to h.
pylori.
○ Clinical Manifestations
• Discomfort/pain in between meals, eat - pain goes away
• Muscle guarding - tense stomach muscles when try to
touch abd.
• Can have exacerbations then remissions.
○ Complications: hemorrhage, perforation (hole through tissue),
and penetration (into surrounding tissues)
• Irritable Bowel Syndrome
○ persistent or recurrent sympt. of abd pain, altered bowel
function, and flatulence, bloating, nausea, anorexia,
constipation, diarrhea, anxiety, and depression to varying
degrees.
○ Dysfunction in regulation of the intestinal motor and sensory
fuctions
○ Stress exacerbates issue, physiological and psychological.
○ More common in women than men, usually during
premenstrual time period (hormonal trigger?).
○ diagnosis made by signs and symptoms
○ Treatment
• Treat stress (trigger).
• Inflammatory Bowel Disease
○ Ulcerative Colitis
• Chronic inflammatory disease causes ulceration (erosion of
tissue) of the mucosa of the colon
Bleed into colon, cramping pain, strong urge to
defecate.
• Age 20 – 40 years
• Risk Factors
Family history, Jewish descent, Caucasian.
• Cause is unknown, start with inflammatory process
primarily in rectum and sigmoid colon.
• Frequent exacerbations and remissions, watery diarrhea, a
lot of blood (will be redder cause lower in GI tract).
When GI bleed Higher up in GI tract will be blacker.
• Clinical Manifestations
Lesion begins with inflammation, usually in rectum
and sigmoid colon causing mucosal destruction
• Complications
Anal fissures, hemorrhoids, abcesses form around
rectal area, increased risk for colon cancer.
• Treatment - surgically fix colon/rectum. Anti-inflammatory.
○ Crohn’s Disease
• Inflammatory disorder of the small and large intestines
(not as often in Sigmoid or rectum), cause fissures in the
colon
• Nonspecific irritable bowel symptoms for many years,
bloody diarrhea, weight loss.
• Problems depend on area which is destroyed, which
nutrients are no longer absorbed.
• Rectum is rarely involved
• Risk Factors/causes
Jewish descent, caucasian, family history.
• Ascending and transverse colon most affected
Skipped lesions, areas of inflammation, then ok, then
inflamed, etc.
• Clinical Manifestations
• Complications
Intestinal obstructions (narrowing), fistulas (opening
between 2 areas of body where there shouldn't be.
• Treatments - surgically remove damaged sections, Anti-
inflammatory.
• Diverticular Disease
○ Saclike outpouchings of mucosa through the muscle layer-
usually sigmoid colon
○ Diverticulosis
• Having the pouch
○ Diverticulitis
• Pouch gets infected/inflamed
○ Common in elderly, or if diet high in refined foods (the
American diet) because bolus does not require a lot of muscle
to push through, therefore fiber eaters triumph again!
○ Symptoms
• When eat something with little parts that get stuck in
outpouchings, diverticulitis can set in --> cramping of abd,
distension, flatulant, diarrhea or constipation, obstruction,
infection (fever, inc WBCs, pain)
• When severe, can rupture, get peritonitis (inflammation of
peritoneal area)
Вам также может понравиться
- Student Evaluation of Clinical Setting 3-29-10 JSBДокумент1 страницаStudent Evaluation of Clinical Setting 3-29-10 JSBsimonedarlingОценок пока нет
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- Children With Special Needs and Ethical DilemmasДокумент45 страницChildren With Special Needs and Ethical DilemmassimonedarlingОценок пока нет
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- UCSF PRDG Purchasing Letter 9-1.2010 1Документ1 страницаUCSF PRDG Purchasing Letter 9-1.2010 1simonedarlingОценок пока нет
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Community Health Work LogДокумент1 страницаCommunity Health Work LogsimonedarlingОценок пока нет
- Pediatric Nursing AssessmentДокумент1 страницаPediatric Nursing AssessmentsimonedarlingОценок пока нет
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Asthma That Disappears Between Ages 6-8 - Bronchioles Grew & Resolved The AsthmaДокумент27 страницAsthma That Disappears Between Ages 6-8 - Bronchioles Grew & Resolved The Asthmasimonedarling100% (1)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Growth and Development Nature vs. NurtureДокумент6 страницGrowth and Development Nature vs. NurturesimonedarlingОценок пока нет
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Fluid and Electrolytes: Acids and Bases: Tuesday, July 14, 2009 9:42 PMДокумент11 страницFluid and Electrolytes: Acids and Bases: Tuesday, July 14, 2009 9:42 PMsimonedarling67% (3)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- Cancers Sum 2009Документ34 страницыCancers Sum 2009simonedarlingОценок пока нет
- Head To Toe AssessmentДокумент2 страницыHead To Toe Assessmentsimonedarling100% (4)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Endocrine Disorders Julie Mann, NP - Case StudyДокумент10 страницEndocrine Disorders Julie Mann, NP - Case Studysimonedarling75% (4)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Tuesday, July 28, 2009 9:25 PMДокумент8 страницTuesday, July 28, 2009 9:25 PMsimonedarlingОценок пока нет
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Musculoskeletal SystemДокумент6 страницMusculoskeletal SystemsimonedarlingОценок пока нет
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- Cardiovascular 1Документ7 страницCardiovascular 1simonedarling100% (2)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- Cardiac+Conditions 1Документ14 страницCardiac+Conditions 1simonedarling100% (2)
- Cardiovascular 1Документ7 страницCardiovascular 1simonedarling100% (2)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Cardiovascular 1Документ7 страницCardiovascular 1simonedarling100% (2)
- Cardiac+Conditions 1Документ14 страницCardiac+Conditions 1simonedarling100% (2)
- Pathophysiology of RHDДокумент4 страницыPathophysiology of RHDshmily_0810Оценок пока нет
- Urinary Tract Infection and Bacteriuria in PregnancyДокумент14 страницUrinary Tract Infection and Bacteriuria in PregnancyAbby QCОценок пока нет
- FIT HW - Module 2Документ34 страницыFIT HW - Module 2Ivan Louis C. ARNOBITОценок пока нет
- Case Presentation On Parkinson'S Disease: Presented By: T.Avinash Vith Pharm D Y13PHD0721Документ21 страницаCase Presentation On Parkinson'S Disease: Presented By: T.Avinash Vith Pharm D Y13PHD0721AVINASH TALAPALA100% (1)
- Lesson 3 - The Circulatory and Respiratory SystemsДокумент26 страницLesson 3 - The Circulatory and Respiratory SystemsEmieleah Lorenzo PauigОценок пока нет
- Tension Pneumothorax: Modifiable FactorsДокумент3 страницыTension Pneumothorax: Modifiable FactorsJustin MaverickОценок пока нет
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Management of Acne Scarring, Part II: A Comparative Review of Non-Laser-Based, Minimally Invasive ApproachesДокумент10 страницManagement of Acne Scarring, Part II: A Comparative Review of Non-Laser-Based, Minimally Invasive ApproachesShintaОценок пока нет
- Case Reports in The Use of Vitamin C Based Regimen in Prophylaxis and Management of COVID-19 Among NigeriansДокумент5 страницCase Reports in The Use of Vitamin C Based Regimen in Prophylaxis and Management of COVID-19 Among NigeriansAndi.Thafida KhalisaОценок пока нет
- Glaucoma and Diabetes - Is There An Association? Jain Shashi, Lakhtakia Sujata, Tirkey Eva Rani, Jain Sheel ChandraДокумент5 страницGlaucoma and Diabetes - Is There An Association? Jain Shashi, Lakhtakia Sujata, Tirkey Eva Rani, Jain Sheel ChandranjmdrОценок пока нет
- Rabbit Analgesia: Standard Operating Procedure #102Документ5 страницRabbit Analgesia: Standard Operating Procedure #102Malu Verruck TortolaОценок пока нет
- Adrenal Gland: Bardelosa, Jesse Gale M. Barretto, Alyssa Nicole 3MT1Документ88 страницAdrenal Gland: Bardelosa, Jesse Gale M. Barretto, Alyssa Nicole 3MT1Alyssa Nicole BarrettoОценок пока нет
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- List of Philhealth Accredited Level 3 Hospital As of October 31, 2019Документ35 страницList of Philhealth Accredited Level 3 Hospital As of October 31, 2019Lex CatОценок пока нет
- The Human Microbiome and Infectious Diseases: Beyond KochДокумент151 страницаThe Human Microbiome and Infectious Diseases: Beyond KochRamesh ShahОценок пока нет
- Maternal and Early-Life Nutrition and HealthДокумент4 страницыMaternal and Early-Life Nutrition and HealthTiffani_Vanessa01Оценок пока нет
- PATHFit I Chapter 4Документ6 страницPATHFit I Chapter 4bamboogabrieltaclaОценок пока нет
- Nguyen 2021Документ8 страницNguyen 2021Yaseen MohamnadОценок пока нет
- Geriatric Medicine and Gerontology: Prevention of Frailty in The Elderly Through Physical Activity and NutritionДокумент8 страницGeriatric Medicine and Gerontology: Prevention of Frailty in The Elderly Through Physical Activity and NutritionSARAH AZIZAH 2015Оценок пока нет
- Diabetic NephropathyДокумент10 страницDiabetic NephropathySindi Nabila PutriОценок пока нет
- Additional RRLДокумент3 страницыAdditional RRLManuel Jaro ValdezОценок пока нет
- BetulaДокумент22 страницыBetulaDenise TirsaОценок пока нет
- 30613167: Management of Osteitis Pubis in Athletes Rehabilitation and Return To Training - A Review of The Most Recent Literature PDFДокумент10 страниц30613167: Management of Osteitis Pubis in Athletes Rehabilitation and Return To Training - A Review of The Most Recent Literature PDFRicovially DavyaОценок пока нет
- NCP 1activity Intolerance N C P BY BHERU LALДокумент1 страницаNCP 1activity Intolerance N C P BY BHERU LALBheru LalОценок пока нет
- Thorn Eh and OutДокумент24 страницыThorn Eh and OutNick MaxОценок пока нет
- Îeéuwûéaéié Uréékéï: (Diseases of Tongue)Документ87 страницÎeéuwûéaéié Uréékéï: (Diseases of Tongue)Pranit Patil100% (1)
- Management of Severe Hyperkalemia PDFДокумент6 страницManagement of Severe Hyperkalemia PDFCarlos Navarro YslaОценок пока нет
- Health Assessment Made Incredibly Visual Incredibly Easy Series 2nd Edition PDFDrive 9 18Документ10 страницHealth Assessment Made Incredibly Visual Incredibly Easy Series 2nd Edition PDFDrive 9 18mianpenarandaОценок пока нет
- Speech Language Pathology (SLP)Документ6 страницSpeech Language Pathology (SLP)Shariq MОценок пока нет
- Ipd - Kelas Ac - Kad Dan Hhs - DR - DR.K Heri Nugroho HS, SP - PD, K-EmdДокумент51 страницаIpd - Kelas Ac - Kad Dan Hhs - DR - DR.K Heri Nugroho HS, SP - PD, K-EmdTeresia MaharaniОценок пока нет
- Sample Internal Medicine Admission NoteДокумент4 страницыSample Internal Medicine Admission NoteMayer Rosenberg100% (8)
- Module 7 Taking Vital SignsДокумент7 страницModule 7 Taking Vital SignsMary Joy CejalboОценок пока нет
- Secrets From the Eating Lab: The Science of Weight Loss, the Myth of Willpower, and Why You Should Never Diet AgainОт EverandSecrets From the Eating Lab: The Science of Weight Loss, the Myth of Willpower, and Why You Should Never Diet AgainРейтинг: 3.5 из 5 звезд3.5/5 (38)