Академический Документы
Профессиональный Документы
Культура Документы
Hemodialysis
Загружено:
Jon Adam Bermudez SamatraИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Hemodialysis
Загружено:
Jon Adam Bermudez SamatraАвторское право:
Доступные форматы
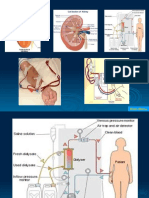
hemodialysis (HD), blood is shunted through an artificial kidney (dialyzer) for removal of toxins/excess fluid and then returned
to the venous circulation. Hemodialysis is a fast and efficient method for removing urea and other toxic products and correcting fluid and electrolyte imbalances but requires permanent arteriovenous access. Procedure is usually performed three times per week for 4 hrs.Hemodialysis may be done in the hospital, outpatient dialysis center, or at home.
Nursing Care Plans
Learn more about hemodialysis with these 3 Hemodialysis Nursing Care Plan (NCP).
Risk for Injury
NURSING DIAGNOSIS: Injury, risk for [loss of vascular access] Risk factors may include Clotting; hemorrhage related to accidental disconnection; infection Possibly evidenced by [Not applicable; presence of signs and symptoms establishes an actual diagnosis.] Hemodialysis Nursing Care Plans Desired Outcomes Maintain patent vascular access. Be free of infection.
Nursing Interventions Monitor internal AV shunt patency at frequent intervals:Palpate for distal thrill;Auscultate for a bruit; Note color of blood and/or obvious separation of cells and serum; Rationale Thrill is caused by turbulence of high-pressure arterial blood flow entering low-pressure venous system and should be palpable above venous exit site.Bruit is the sound caused by the turbulence of arterial blood entering venous system and should be audible by stethoscope, although may be very faint.Change of color from uniform medium red to dark purplish red suggests sluggish blood flow/early clotting. Separation in tubing is indicative of clotting. Very dark reddish-black blood next to clear yellow fluid indicates full clot formation.Diminished blood flow results in coolness of shunt. Rapid intervention may save access; however, declotting must be done by experienced personnel.
Palpate skin around shunt for warmth.
Notify physician and/or initiate declotting procedure if there is evidence of loss of shunt patency. Evaluate reports of pain, numbness/tingling; note extremity swelling distal to access. Avoid trauma to shunt; e.g., handle tubing gently, maintain cannula alignment. Limit activity of extremity. Avoid taking BP or drawing blood samples in shunt extremity. Instruct patient not to sleep on side with shunt or carry packages, books, purse on affected extremity. Attach two cannula clamps to shunt dressing. Have tourniquet available. If cannulas separate, clamp the arterial cannula first, then the venous. If tubing comes out of vessel, clamp cannula that is still in place and apply direct pressure to bleeding site. Place tourniquet above site or inflate BP cuff
May indicate inadequate blood supply.
Decreases risk of clotting/disconnection.
Prevents massive blood loss while awaiting medical assistance if cannula separates or shunt is dislodged.
to pressure just above patients systolic BP. Assess skin around vascular access, noting redness, swelling, local warmth, exudate, tenderness. Avoid contamination of access site. Use aseptic technique and masks when giving shunt care, applying/changing dressings, and when starting/completing dialysis process. Monitor temperature. Note presence of fever, chills, hypotension. Culture the site/obtain blood samples as indicated. Monitor PT, activated partial thromboplastin time (aPTT) as appropriate. Administer medications as indicated, e.g.:Heparin (low-dose);Antibiotics (systemic and/or topical). Signs of local infection, which can progress to sepsis if untreated.
Prevents introduction of organisms that can cause infection.
Signs of infection/sepsis requiring prompt medical intervention. Determines presence of pathogens.
Provides information about coagulation status, identifies treatment needs, and evaluates effectiveness. Infused on arterial side of filter to prevent clotting in the filter without systemic side effects.Prompt treatment of infection may save access, prevent sepsis.
Deficient Fluid Volume
Deficient Fluid Volume Hemodialysis Nursing Care Plans NURSING DIAGNOSIS: Fluid Volume, risk for deficient Risk factors may include Ultrafiltration Fluid restrictions; actual blood loss (systemic heparinization or disconnection of the shunt) Possibly evidenced by [Not applicable; presence of signs and symptoms establishes an actual diagnosis.] DESIRED OUTCOMES/EVALUATION CRITERIAPATIENT WILL: Hydration (NOC) Maintain fluid balance as evidenced by stable/appropriate weight and vital signs, good skin turgor, moist mucous membranes, absence of bleeding.
Nursing Interventions Measure all sources of I&O. Have patient keep diary. Rationale Aids in evaluating fluid status, especially when compared with weight. Note: Urine output is an inaccurate evaluation of renal function in dialysis patients. Some individuals have water output with little renal clearance of toxins, whereas others have oliguria or anuria. Weight loss over precisely measured time is a measure of ultrafiltration and fluid removal. Hypotension, tachycardia, falling hemodynamic pressures suggest volume depletion.
Weigh daily before/after dialysis run.
Monitor BP, pulse, and hemodynamic pressures if available during dialysis. Note/ascertain whether diuretics and/or antihypertensives are to be withheld.
Dialysis potentiates hypotensive effects if these drugs have been administered.
Verify continuity of shunt/access catheter. Apply external shunt dressing. Permit no puncture of shunt. Place patient in a supine/Trendelenburgs position as necessary. Assess for oozing or frank bleeding at access site or mucous membranes, incisions/wounds. Hematest/guaiac stools, gastric drainage. Monitor laboratory studies as indicated:Hb/Hct;Serum electrolytes and pH; Clotting times, e.g., PT/aPTT, and platelet count. Administer IV solutions (e.g., normal saline [NS])/volume expanders (e.g., albumin) during dialysis as indicated;Blood/PRCs if needed.
Disconnected shunt/open access permits exsanguination.
Minimizes stress on cannula insertion site to reduce inadvertent dislodgement and bleeding from site. Maximizes venous return if hypotension occurs.
Systemic heparinization during dialysis increases clotting times and places patient at risk for bleeding, especially during the first 4 hr after procedure.
May be reduced because of anemia, hemodilution, or actual blood loss.Imbalances may require changes in the dialysate solution or supplemental replacement to achieve balance.Use of heparin to prevent clotting in blood lines and hemofilter alters coagulation and potentiates active bleeding. Saline/dextrose solutions, electrolytes, and NaHCO3 may be infused in the venous side of continuous arteriovenous (CAV) hemofilter when high ultrafiltration rates are used for removal of extracellular fluid and toxic solutes. Volume expanders may be required during/following hemodialysis if sudden/marked hypotension occurs.Destruction of RBCs (hemolysis) by mechanical dialysis, hemorrhagic losses, decreased RBC production may result in profound/progressive anemia requiring corrective action. Reduces the amount of water being removed and may correct hypotension/hypovolemia. May be needed to return clotting times to normal or if heparin rebound occurs (up to 16 hr after hemodialysis).
Reduce rate of ultrafiltration during dialysis as indicated Administer protamine sulfate as appropriate.
Excess Fluid Volume
NURSING DIAGNOSIS: Fluid Volume, risk for excess Risk factors may include Rapid/excessive fluid intake: IV, blood, plasma expanders, saline given to support BP during dialysis Possibly evidenced by [Not applicable; presence of signs and symptoms establishes an actual diagnosis.] DESIRED OUTCOMES/EVALUATION CRITERIAPATIENT WILL: Fluid Balance (NOC) Maintain dry weight within patients normal range; be free of edema; have clear breath sounds and serum sodium levels within normal limits.
Nursing Interventions Measure all sources of I&O. Weigh routinely. Rationale Aids in evaluating fluid status, especially when compared with weight. Weight gain between treatments should not exceed 0.5 kg/day.
Monitor BP, pulse.
Hypertension and tachycardia between hemodialysis runs may result from fluid overload and/or HF. Fluid volume excess due to inefficient dialysis or repeated hypervolemia between dialysis treatments may cause/exacerbate HF, as indicated by signs/symptoms of respiratory and/or systemic venous congestion. Fluid overload/hypervolemia may potentiate cerebral edema (disequilibrium syndrome). High sodium levels are associated with fluid overload, edema, hypertension, and cardiac complications. The intermittent nature of hemodialysis results in fluid retention/overload between procedures and may require fluid restriction. Spacing fluids helps reduce thirst.
Note presence of peripheral/sacral edema, respiratory rales, dyspnea, orthopnea, distended neck veins, ECG changes indicative of ventricular hypertrophy. Note changes in mentation.
Monitor serum sodium levels. Restrict sodium intake as indicated. Restrict PO/IV fluid intake as indicated, spacing allowed fluids throughout a 24-hr period.
anuria ncp, nursing care plan for hemodialysis, rationale for hemodialysis, nursing care plan for motor vehicular accident, nursing care plan for open wounds, nursing care plan patient on dialysis, nursing care plans for haemodialysis
Вам также может понравиться
- Risk For Bleeding - Cirrhosis NCPДокумент2 страницыRisk For Bleeding - Cirrhosis NCPPaula AbadОценок пока нет
- COMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideОт EverandCOMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideОценок пока нет
- Nursing Care Plan For "HEMODIALYSIS"Документ5 страницNursing Care Plan For "HEMODIALYSIS"jhonroks100% (6)
- 3 Hemodialysis Nursing Care Plans - NurseslabsДокумент7 страниц3 Hemodialysis Nursing Care Plans - NurseslabsAshleyОценок пока нет
- Case: Liver Cirrhosis Assessment:: Nursing InferenceДокумент7 страницCase: Liver Cirrhosis Assessment:: Nursing InferenceLovelyn GanirОценок пока нет
- NCP Liver CirrhosisДокумент7 страницNCP Liver CirrhosisIris Jimenez-BuanОценок пока нет
- Gastrectomy Post OpДокумент5 страницGastrectomy Post Opfeirri100% (4)
- Nursing Care Plan Renal FailureДокумент18 страницNursing Care Plan Renal FailureKundan KumarОценок пока нет
- TypesДокумент3 страницыTypesProser Faith TabaculdeОценок пока нет
- Nursing Care Plan For "DYSRHYTHMIAS"Документ12 страницNursing Care Plan For "DYSRHYTHMIAS"jhonroks79% (14)
- Nursing Care Plan of CataractДокумент3 страницыNursing Care Plan of CataractDimzmonyo100% (1)
- 8 Sample Care Plans For ACDFДокумент11 страниц8 Sample Care Plans For ACDFacasulla98Оценок пока нет
- Week 10 Drug Card - Hydrochlorothiazide (HCTZ)Документ2 страницыWeek 10 Drug Card - Hydrochlorothiazide (HCTZ)RCurry09Оценок пока нет
- Septic Shock Student Case StudyДокумент6 страницSeptic Shock Student Case StudyJenn GallowayОценок пока нет
- Patho NCP DrugsДокумент8 страницPatho NCP DrugsMyco Reyes GarcesОценок пока нет
- Impaired Gas ExchangeДокумент1 страницаImpaired Gas ExchangeLyka Mae Imbat - PacnisОценок пока нет
- Drugstudy and NCP of HemodialysisДокумент5 страницDrugstudy and NCP of HemodialysisJM Nelson100% (1)
- NCP-Case Presentation (CHF)Документ4 страницыNCP-Case Presentation (CHF)Jessamine EnriquezОценок пока нет
- CystoclysisДокумент2 страницыCystoclysisRaymond BasiloniaОценок пока нет
- Anatomy and Physiology-Liver CirrhosisДокумент2 страницыAnatomy and Physiology-Liver CirrhosisHilmi Ramos100% (3)
- Impaired Tissue IntegrityДокумент2 страницыImpaired Tissue IntegrityJacoJone11100% (1)
- Ncp-Ineffective Airway ClearanceДокумент3 страницыNcp-Ineffective Airway Clearancelouanne0550% (2)
- Hyperosmolar Hyperglycemic Nonketotic Syndrome (HHNS)Документ8 страницHyperosmolar Hyperglycemic Nonketotic Syndrome (HHNS)amiraОценок пока нет
- CNN Practice QuestionsДокумент5 страницCNN Practice QuestionsUri Perez MontedeRamosОценок пока нет
- Hepatic EncephalopathyДокумент10 страницHepatic Encephalopathymiss RN100% (1)
- Nursing Care Plan: Congestive Heart Failure-Deep Vein ThrombosisДокумент19 страницNursing Care Plan: Congestive Heart Failure-Deep Vein ThrombosisRiza Angela BarazanОценок пока нет
- SIADH (Syndrome of Inapproperiate Antidiuretic Hormone Secretion)Документ11 страницSIADH (Syndrome of Inapproperiate Antidiuretic Hormone Secretion)itsmesubu100% (2)
- Care of Clients With Problems in Cellular Aberrations Key TermsДокумент2 страницыCare of Clients With Problems in Cellular Aberrations Key Termsjoyrena ochondraОценок пока нет
- Dialysis Disequilibrium SyndromeДокумент2 страницыDialysis Disequilibrium SyndromeKayla AbadОценок пока нет
- Colon Rectal CancerДокумент6 страницColon Rectal Cancerbryantmaroney811Оценок пока нет
- Case Study Pleural EffusionДокумент4 страницыCase Study Pleural EffusionKhristine Anne FabayОценок пока нет
- Case Study On Fluid OverloadДокумент37 страницCase Study On Fluid OverloadradicalmpОценок пока нет
- Congestive Heart FailureДокумент18 страницCongestive Heart FailureAisha Rashed100% (1)
- Hypoglycemia: Presented by Farse GhabayenДокумент11 страницHypoglycemia: Presented by Farse GhabayenFares G. Ghabayen100% (2)
- Case StudyДокумент34 страницыCase StudyBSNNursing101Оценок пока нет
- HaemodialysisДокумент98 страницHaemodialysisKo Zin100% (1)
- Cast CareДокумент1 страницаCast CareCarmelita SaltОценок пока нет
- Anatomy and Physiology BPH!Документ1 страницаAnatomy and Physiology BPH!Christian BuenaОценок пока нет
- Caring For Patients With Chest TubesДокумент10 страницCaring For Patients With Chest Tubesphoenix180100% (1)
- Nursing Care PlansДокумент5 страницNursing Care PlansMa Liezel M Camba100% (1)
- Nursing Care Plan Impaired Gas ExchangeДокумент1 страницаNursing Care Plan Impaired Gas ExchangeKarylle PetilОценок пока нет
- NCP and DStudyДокумент8 страницNCP and DStudyJessica Rosan Hewald ManapatОценок пока нет
- Drug StudyДокумент7 страницDrug Studykymsh_kimОценок пока нет
- Preoperative and Post Liver Transplant Nursing Care Plan, Nursing ProcessДокумент2 страницыPreoperative and Post Liver Transplant Nursing Care Plan, Nursing ProcessOctoober100% (3)
- SimvastatinДокумент1 страницаSimvastatinLyka Mae Imbat - PacnisОценок пока нет
- 1 Acute Pain NCPДокумент2 страницы1 Acute Pain NCPFilipinas BelzaОценок пока нет
- Hemodialysis: Carina Joane Villareal-Barroso, R.N.,M.NДокумент108 страницHemodialysis: Carina Joane Villareal-Barroso, R.N.,M.NJune BarsОценок пока нет
- Bone Tumor 2011 Nursing StudentsДокумент40 страницBone Tumor 2011 Nursing StudentsRaveenmayi94% (16)
- Nursing Care Plan: Fluid Volume Deficit R/T Active Fluid Loss (Increased Urine Output)Документ9 страницNursing Care Plan: Fluid Volume Deficit R/T Active Fluid Loss (Increased Urine Output)Gayu Patel0% (1)
- Nursing Care Plan Priorities: Risk For InjuryДокумент6 страницNursing Care Plan Priorities: Risk For InjuryPauling FrezОценок пока нет
- Hemodialysis: NURSING DIAGNOSIS: Injury, Risk For (Loss of Vascular Access) Risk Factors May IncludeДокумент10 страницHemodialysis: NURSING DIAGNOSIS: Injury, Risk For (Loss of Vascular Access) Risk Factors May IncludeChevelle Valenciano-GaanОценок пока нет
- Demonstration ON Haemodialysis: Submitted ToДокумент46 страницDemonstration ON Haemodialysis: Submitted ToAbirajanОценок пока нет
- Fluid Imbalance (NCP)Документ9 страницFluid Imbalance (NCP)Putry RainismОценок пока нет
- Excess Fluid Volume HypervolemiaДокумент7 страницExcess Fluid Volume HypervolemiaLuthfiy IrfanasruddinОценок пока нет
- Acute Renal Failure Nursing Care PlanДокумент15 страницAcute Renal Failure Nursing Care PlanRanusha AnushaОценок пока нет
- HemodialysisДокумент4 страницыHemodialysisQueen Factor VedraОценок пока нет
- Renal Dialysis PeritonealДокумент7 страницRenal Dialysis Peritonealmardsz100% (2)
- Renal Nursing 4 April 2021Документ30 страницRenal Nursing 4 April 2021Benard Were100% (1)
- Excess Fluid Volume - Nursing Diagnosis & Care Plan - NurseslabsДокумент8 страницExcess Fluid Volume - Nursing Diagnosis & Care Plan - NurseslabsEricsonMitraОценок пока нет
- Introduction To Nursing PharmacologyДокумент5 страницIntroduction To Nursing PharmacologyJon Adam Bermudez SamatraОценок пока нет
- Akapulko or Acapulco in English Is A Shrub Found Throughout The PhilippinesДокумент6 страницAkapulko or Acapulco in English Is A Shrub Found Throughout The PhilippinesJon Adam Bermudez SamatraОценок пока нет
- EthicsДокумент7 страницEthicsJon Adam Bermudez SamatraОценок пока нет
- Assessment Procedure Methods Actual Findings Normal Status Interpretati On SkinДокумент8 страницAssessment Procedure Methods Actual Findings Normal Status Interpretati On SkinJon Adam Bermudez SamatraОценок пока нет
- CNS: GI: Assessment & Drug Effects: Generic Name Brand Name Indications Action Side Effects Nursing ResponsibilitiesДокумент4 страницыCNS: GI: Assessment & Drug Effects: Generic Name Brand Name Indications Action Side Effects Nursing ResponsibilitiesJon Adam Bermudez SamatraОценок пока нет
- Assessment Nursing Diagnosis Scientific Explanation Planning Intervention Rationale EvaluationДокумент1 страницаAssessment Nursing Diagnosis Scientific Explanation Planning Intervention Rationale EvaluationJon Adam Bermudez SamatraОценок пока нет
- Generic Name Brand Name Indications Action Side Effects Nursing ResponsibilitiesДокумент1 страницаGeneric Name Brand Name Indications Action Side Effects Nursing ResponsibilitiesJon Adam Bermudez SamatraОценок пока нет
- Generic Name Drug Class Action Indication Contraindication Side Effect Nursing InterventionДокумент2 страницыGeneric Name Drug Class Action Indication Contraindication Side Effect Nursing InterventionJon Adam Bermudez SamatraОценок пока нет
- Nursing InformaticsДокумент11 страницNursing InformaticsJon Adam Bermudez SamatraОценок пока нет
- Omran WalidДокумент196 страницOmran WalidDébora AmougouОценок пока нет
- Heuristic Cheat Sheet Clickable LinksДокумент2 страницыHeuristic Cheat Sheet Clickable Linksemily100% (1)
- Os Unit-1Документ33 страницыOs Unit-1yoichiisagi09Оценок пока нет
- Qdoc - Tips Sinister-TarotzДокумент92 страницыQdoc - Tips Sinister-TarotzAleister DahmerОценок пока нет
- 1st Quarter 2016 Lesson 5 Powerpoint With Tagalog NotesДокумент25 страниц1st Quarter 2016 Lesson 5 Powerpoint With Tagalog NotesRitchie FamarinОценок пока нет
- HRIRДокумент23 страницыHRIRPhuong HoОценок пока нет
- Manual en TC1 TD4 Curr 2018-07-16Документ39 страницManual en TC1 TD4 Curr 2018-07-16Daniel Peña100% (1)
- Erp FinalДокумент33 страницыErp FinaltenetchatОценок пока нет
- Apache Nifi Tutorial - What Is - Architecture - InstallationДокумент5 страницApache Nifi Tutorial - What Is - Architecture - InstallationMario SoaresОценок пока нет
- Restoring PH Balance in The BodyДокумент6 страницRestoring PH Balance in The Bodycinefil70Оценок пока нет
- Annex A2 - CS Form 100 - Revised 2023 - CSESP - A1 - Edited - A1Документ2 страницыAnnex A2 - CS Form 100 - Revised 2023 - CSESP - A1 - Edited - A1obs.obando2022Оценок пока нет
- Tasha Giles: WebsiteДокумент1 страницаTasha Giles: Websiteapi-395325861Оценок пока нет
- Paper 3 FrinqДокумент4 страницыPaper 3 Frinqapi-301975170Оценок пока нет
- D2165151-003 Preliminary SGRE ON SG 6.0-170 Site Roads and HardstandsДокумент46 страницD2165151-003 Preliminary SGRE ON SG 6.0-170 Site Roads and HardstandsMarcelo Gonçalves100% (1)
- EASA Part-66 Module 17 QBДокумент53 страницыEASA Part-66 Module 17 QBFaisal Ahmed Newon80% (5)
- CSMP77: en Es FRДокумент38 страницCSMP77: en Es FRGerson FelipeОценок пока нет
- Assignment Brief - Starting A Business and Fundamental of MarketingДокумент7 страницAssignment Brief - Starting A Business and Fundamental of Marketingmd rahimОценок пока нет
- Circuit Breaker - Ground & Test Device Type VR Electrically OperatedДокумент24 страницыCircuit Breaker - Ground & Test Device Type VR Electrically OperatedcadtilОценок пока нет
- SolBridge Application 2012Документ14 страницSolBridge Application 2012Corissa WandmacherОценок пока нет
- Useful C Library FunctionДокумент31 страницаUseful C Library FunctionraviОценок пока нет
- Steve Talbott Getting Over The Code DelusionДокумент57 страницSteve Talbott Getting Over The Code DelusionAlexandra DaleОценок пока нет
- User Manual ManoScanДокумент58 страницUser Manual ManoScanNurul FathiaОценок пока нет
- GE Elec 7 UNIT-3 NoДокумент22 страницыGE Elec 7 UNIT-3 NoLyleОценок пока нет
- DIFFERENCE BETWEEN Intrior Design and DecorationДокумент13 страницDIFFERENCE BETWEEN Intrior Design and DecorationSadaf khanОценок пока нет
- Watt AC-DC Converters: FeaturesДокумент3 страницыWatt AC-DC Converters: FeatureskofidОценок пока нет
- Syncretism and SeparationДокумент15 страницSyncretism and SeparationdairingprincessОценок пока нет
- PMP Exam Questions and Answers PDFДокумент12 страницPMP Exam Questions and Answers PDFAshwin Raghav SankarОценок пока нет
- Characteristics of Victorian BritainДокумент3 страницыCharacteristics of Victorian BritainmwaqasenggОценок пока нет
- JIS-G3455 - Carbon Steel Pipes For High Pressure ServiceДокумент27 страницJIS-G3455 - Carbon Steel Pipes For High Pressure ServiceHoang Tan100% (1)
- KITZ - Cast Iron - 125FCL&125FCYДокумент2 страницыKITZ - Cast Iron - 125FCL&125FCYdanang hadi saputroОценок пока нет
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionОт EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionРейтинг: 4 из 5 звезд4/5 (404)
- The Age of Magical Overthinking: Notes on Modern IrrationalityОт EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityРейтинг: 4 из 5 звезд4/5 (34)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDОт EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDРейтинг: 5 из 5 звезд5/5 (3)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)От EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Рейтинг: 3 из 5 звезд3/5 (1)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsОт EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsРейтинг: 4 из 5 звезд4/5 (4)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedОт EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedРейтинг: 4.5 из 5 звезд4.5/5 (82)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeОт EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeРейтинг: 4.5 из 5 звезд4.5/5 (254)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsОт EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsРейтинг: 4.5 из 5 звезд4.5/5 (170)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsОт EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsОценок пока нет
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeОт EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeРейтинг: 2 из 5 звезд2/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisОт EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisРейтинг: 4.5 из 5 звезд4.5/5 (44)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsОт EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsРейтинг: 5 из 5 звезд5/5 (1)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaОт EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesОт EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesРейтинг: 4.5 из 5 звезд4.5/5 (1412)
- The Twentysomething Treatment: A Revolutionary Remedy for an Uncertain AgeОт EverandThe Twentysomething Treatment: A Revolutionary Remedy for an Uncertain AgeРейтинг: 4.5 из 5 звезд4.5/5 (2)
- The Obesity Code: Unlocking the Secrets of Weight LossОт EverandThe Obesity Code: Unlocking the Secrets of Weight LossРейтинг: 4 из 5 звезд4/5 (6)
- To Explain the World: The Discovery of Modern ScienceОт EverandTo Explain the World: The Discovery of Modern ScienceРейтинг: 3.5 из 5 звезд3.5/5 (51)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.От EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Рейтинг: 4.5 из 5 звезд4.5/5 (110)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisОт EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisРейтинг: 3.5 из 5 звезд3.5/5 (2)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsОт EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsОценок пока нет
- Hearts of Darkness: Serial Killers, The Behavioral Science Unit, and My Life as a Woman in the FBIОт EverandHearts of Darkness: Serial Killers, The Behavioral Science Unit, and My Life as a Woman in the FBIРейтинг: 4 из 5 звезд4/5 (20)
- Why We Die: The New Science of Aging and the Quest for ImmortalityОт EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityРейтинг: 4.5 из 5 звезд4.5/5 (6)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryОт EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryРейтинг: 4 из 5 звезд4/5 (46)