Академический Документы
Профессиональный Документы
Культура Документы
Treatmen For Cronic Constipation
Загружено:
Gembong Van BeethovenИсходное описание:
Оригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Treatmen For Cronic Constipation
Загружено:
Gembong Van BeethovenАвторское право:
Доступные форматы
S962 Vol.
6 (10B) November 2006
ABSTRACT
Commonly used first-line treatments for chronic
constipation are simple: dietary fiber, fluids, exer-
cise, and allocating time for defecation. Often,
the patient will most likely have tried the first 3
treatments on their own. It is important to docu-
ment what has been tried and the results. This
article describes the recommended treatments for
chronic constipation once the patient presents to
a healthcare provider for this problem.
Frequently recommended treatments include
medicinal fiber supplements, bulking agents,
stool softeners, and laxatives. Two prescription
treatments, tegaserod and lubiprostone, are
available. Study results have proven that these
treatments have shown good efficacy and tolera-
bility. A brief review of those study results is
included in this article, in addition to a discussion
of when to refer a patient to the gastroenterolo-
gist and the management of pelvic dyssynergia.
(Adv Stud Med. 2006;6(10B):S962-S967)
P
atients suffering from chronic constipation
a re often willing to try almost anything to
re l i e vetheir pain and discomfort. Howe ve r,
first-line treatments for constipation are, in
fact, simple: increased dietary fiber, fluids,
e xe rcise, and allocating time to have a bowel move-
ment. The patient will most likely have tried the first 3
t reatments on their own. As Julia Pallentino, MSN, JD,
ARNP-BC, notes in this monograph, it is important to
document what has been tried and the results. On the
other hand, allocating sufficient time for a bowel move-
ment is often not considered, but is a common re m e d y
for chronic constipation. The best time for a bowe l
m ovement is in the morning, after breakfast, when
d i g e s t i vestimuli prompt the urge to evacuate the bow-
els. If that urge is ignored, it tends to diminish ove r
time. Scientific evidence showing that these simple
t reatments (other than increased dietary fiber) are effec-
t i ve is lacking, but this has not diminished their popu-
larity or usefulness.
Fiber consists of the long-chain polysaccharides
and several other plant components, such as cellulose,
lignin, and waxes, which are not digested in the
human stomach or small intestine. If the patient is not
consuming sufficient fiber (>20 g daily), he should
begin with lower doses (46 g daily) of dietary fiber
(eg, bran), or medicinal fiber (eg, psyllium), and
increase it gradually to avoid bloating and flatulence.
The digestive tract needs time to adjust to the increase
in fiber intake. There are many types of medicinal fiber
supplements available: psyllium, methylcellulose, cal-
cium polycarbophil, and guar gum. The total recom-
mended daily intake of fiber (diet + supplementation)
is 20 to 25 grams, but could be increased to 30 grams,
if necessary.
1
Several Web sites provide the fiber con-
tent for different foods (Table 1); this information is
also available on the nutrition labeling of products.
Bulking agents are poorly absorbed agents that act
PROCEEDINGS
NEW TREATMENTS FOR AN OLD PROBLEM:
CHRONIC CONSTIPATION*
Lawrence R. Schiller, MD, FACP, FACG
*Based on a presentation at a symposium held at the
2006 National Conference of the American Academy of
Nurse Practitioners, Grapevine, Texas, on June 21, 2006.
G a s t ro e n t e rology Department, Baylor University
Medical Center, Dallas, Texas.
Address correspondence to: Lawrence R. Schiller, MD,
FA C P, FACG, Gastro e n t e rology Department, Baylor
University Medical Center, 3500 Gaston Avenue, Dallas, TX
75246. E-mail: lrsmd@aol.com.
Johns Hopkins Advanced Studies in Medicine S963
PROCEEDINGS
by absorbing liquids in the intestines. The ingested
bolus then swells to form a soft, bulky stool, which
prompts a bowel movement. Psyllium and most other
fiber supplements are bulking agents; they improve
bowel frequency and consistency. Several studies have
shown the efficacy of bulking agents for relieving
chronic constipation. Unfortunately, the studies were
not ideally designed, so the American College of
Gastroenterology (ACG) Task Force gave psyllium
only a Grade B recommendation.
2
Stool softeners are often the second treatment
patients try after bulking agents. Stool softeners are
minor laxative agents that modestly reduce fluid
absorption and thereby prevent dry, hard stools from
forming. These products decrease the need for strain-
ing and facilitate the ability to evacuate the bowel.
However, they may not be as effective as psyllium for
increasing stool frequency. Although scientific studies
show only minimal effects on stool frequency, many
patients have had great success with stool softeners.
2
There are several types of laxatives. Osmotic laxa-
tives promote retention of water within the bowel
lumen, softening the stool and increasing bowe l
actions. Saline laxatives, nonabsorbable sugars or sugar
alcohols, and certain polymers constitute the 3 types
of osmotic laxatives. Examples of saline laxative s
include magnesium hydroxide (milk of magnesia),
magnesium citrate, and sodium phosphate. Of note,
although there is insufficient scientific evidence to
s u p p o rt a recommendation for using magnesium
hydroxide for chronic constipation, many patients try
it because it is promoted as a more gentle treatment
that works overnight. The taste of milk of magnesia is
an issue for many patients and some claim that it stops
working after a while, although it is not clear why this
occurs. Other patients prefer poorly absorbable sugar
and sugar alcohol laxatives (eg, lactulose, sorbitol,
mannitol, and lactitol). Even though these agents
increase stool frequency and consistency, excessive fla-
tus produced by bacterial metabolism of these fer-
mentable substrates in the colon limits their
acceptance. The most widely prescribed osmotic laxa-
tive is the polymer laxative, polyethylene glycol, which
is effective for the relief of constipation (Grade A rec-
ommendation).
2
Any osmotic laxative can create fluid
or electrolyte abnormalities if used inappropriately and
may cause hypovolemia or diarrhea.
2,3
Stimulant (irritant) laxatives act on the intestinal
wall, stimulating secretion of water and salt by the
mucosa, in addition to increasing muscle contractions
to move the stool. As a result, these products may
induce cramping and discomfort associated with
bowel movement and occasionally cause electrolyte
imbalances. Allergic reactions complicate the use of
some of the plant-based products. Therefore, they
should be used for short-term relief, rather than as a
long-term solution to a chronic problem.
2,3
The only lubricant laxative is mineral oil, which
coats the bowel and is incorporated into the stool
mass, keeping it soft and easing passage through the
digestive tract. It is sometimes used as an acute treat-
ment for children, less so with adults. Aspiration of
mineral oil may lead to a lipoid pneumonia that may
be difficult to treat.
In general, regular intake of currently available lax-
atives is considered unlikely to be harmful to the colon
and data do not support a potential for addiction.
2
However, although laxative preparations are effective
for short-term relief, they tend to cause unpleasant
side effects that preclude their long-term use.
2,3
The
ACG Task Force specifically recommended psyllium,
stool softeners, polyethylene glycol, and lactulose for
use as laxatives, citing insufficient data to make rec-
ommendations for any other laxative treatments.
2
Table 1. Web Sites Listing the Fiber Content of
Common Foods
American Dietetic Association, Fiber Facts
http://www.eatright.org/cps/rde/xchg/ada/hs.xsl/nutrition_5440_E
NU_HTML.htm
Continuum Health Partners, Dietary Fiber Chart
http://www.wehealnewyork.org/healthinfo/dietaryfiber/fibercon-
tentchart.html
Harvard University Health Services, Nutrition Know How
http://huhs.harvard.edu/PDF/FiberContentNutritiionFall2004a.pdf
The Mayo Clinic
http://www.mayoclinic.com/health/fiber/NU00033
University of Arizona, College of Agriculture and Life Sciences
http://cals.arizona.edu/pubs/health/az1127.html
S964 Vol. 6 (10B) November 2006
PROCEEDINGS
NEWER TREATMENTS FOR CONSTIPATION
TEGASEROD
Tegaserod was approved by the US Food and Drug
Administration (FDA) in 2002, initially for irritable
bowel syndrome (IBS) with constipation in women
and then for chronic constipation in both men and
women under age 65. Tegaserod acts by enhancing the
peristaltic reflex (and thus moving the fecal bolus
through the gastrointestinal tract) by mimicking sero-
tonin. Tegaserod also may decrease visceral sensitivity,
thus decreasing the amount of pain associated with
IBS with constipation.
4-6
There are 2 published large clinical trials showing
the efficacy of tegaserod in chronic constipation.
Tegaserod was significantly more effective than place-
bo in the percentage of subjects who met a difficult
primary endpoint: increasing the number of complete
spontaneous bowel movements per week by at least 1
over the first 4 weeks of treatment (Figure 1).
7,8
In both studies, patients were treated for 12
weeks and tegaserod produced a statistically sig-
nificant improvement over placebo for the full
12 weeks of treatment (secondary endpoint) as
well.
7,8
On the basis of these studies, tegaserod
was approved by the US FDA for treatment of
c h ronic constipation in men and women
younger than 65 years of age. Because the data
were strong, the ACG Task Force gave tegaserod
a Grade A recommendation for the treatment of
chronic constipation.
2
Nonetheless, patients with chronic constipa-
tion typically have symptoms for more than 12
weeks; therefore, it is important to note how
tegaserod works over a longer period of time.
Shetzline et al recently presented the results of a
long-term study of tegaserod in 111 patients
who responded to tegaserod during the first 4
weeks of a 12-week study. During 13 additional
months of treatment, symptom improvement
was maintained in those who continued the
medication.
9
It has been shown that tegaserod is well tol-
erated. During the 12-week studies, there was
no rebound effect when tegaserod was discon-
tinued over a 4-week withdrawal period.
7,8
The
most frequent side effect is diarrhea that typical-
ly lasts from 1 to 2 days when first starting the
medication. In clinical trials, diarrhea occurred
more frequently in the tegaserod-treated patients than
the placebo-treated patients (6%7% vs 2%4%,
respectively). It is helpful to warn patients about the
possibility of an initial episode of diarrhea (which the
patient may not mind after suffering from constipa-
tion). There are no clinically relevant drug-drug inter-
actions with tegaserod, and no prolongation of QT
intervals on electrocardiography.
7-9
There is a precau-
tion noted in the labeling for tegaserod regarding
recently re p o rted cases of ischemic colitis with
tegaserod use: [tegaserod] should be discontinued
immediately in patients who develop symptoms of
ischemic colitis, such as rectal bleeding, bloody diar-
rhea, or new or worsening abdominal pain.
10
However, a causal association has not been established,
and the occurrence of ischemic colitis may be no high-
er with the drug than with the underlying condition
alone.
F i g u re 1 . Responder Rates During the First 4 Weeks of
1 2 - Week Studies of Te g a s e rod vs Placebo
*P <.0001;
P <.01. BID = twice a day.
Responders had an increase of more than1 spontaneous complete bowel movement per
week and completed more than 7 days of treatment. Responder rates were significantly high-
er than placebo for the primary study endpoint (weeks 14) and the secondary endpoint
(weeks 112, not shown).
Adapted with permission from Johanson et al
7
; Kamm et al.
8
LUBIPROSTONE
Lu b i p rostone is indicated for the treatment of chro n-
ic idiopathic constipation in adults.
11
It is a bicyclic func-
tional fatty acid that selectively activates a specific subset
of chloride channels on the cells lining the gastro i n t e s t i-
nal tract (ClC-2 channels).
12,13
It works locally from the
intestinal lumen and does not have detectable systemic
absorption. Im p o rt a n t l y, it is not a prostaglandin and
does not activate prostaglandin receptors. The activa t i o n
of chloride channels by lubiprostone enhances fluid
s e c retion into the intestine, which promotes sponta-
neous bowel movements, softens the stool, and re d u c e s
abdominal discomfort/pain and bloating.
14,15
Lubiprostone has been studied in 2 large clini-
cal trials. Patients taking 24 mg of lubiprostone
twice a day with meals had significantly more
spontaneous bowel movements per week than
those receiving placebo, starting at week 1 and
continuing through week 4 (Fi g u res 2A and 2B).
15-
17
Lubiprostone is equally effective in men and
women and, importantly, is effective in elderly
patients, based on pooled study results from the 2
studies.
18,19
Elderly patients receiving lubiprostone
24 mg twice a day showed significant improve-
ment in the number of spontaneous bowel move-
ments during each of 4 weeks of tre a t m e n t
compared with those receiving placebo and they
tolerated the drug well.
18
The most common side effects with lubipro s-
tone noted during clinical studies we re nausea, diar-
rhea, and headache.
15,20-24
Ap p roximately 30% of
patients experienced nausea with lubiprostone com-
p a red with approximately 5% of placebo patients.
Nausea can be minimized by taking lubipro s t o n e
with food or by reducing the dose. Most study sub-
jects tolerated the nausea in order to re l i e ve their
constipation; howe ve r, approximately 10% of
patients discontinued lubiprostone because of nau-
sea. Headache occurred twice as often in the
l u b i p rostone patients compared with the placebo
patients (13% vs 6.6%), and dizziness was more
common as well (4% vs 1.3%).
11
Lu b i p rostone does
not cause any electrolyte imbalances or renal dys-
function, and systemic dru g - d rug interactions have
not been a pro b l e m .
25
Fi n a l l y, the prescribing infor-
mation suggests that lubiprostone be used only in
women who are not pregnant (verified by a negative
p regnancy test) because of the potential for fetal loss
o b s e rved in guinea pigs that re c e i ved lubipro s t o n e .
11
WHEN TO REFER TO A GASTROENTEROLOGIST
An accurate history, careful physical examination,
and appropriate specialized investigations are essential
for the diagnosis and selection of appropriate tre a t m e n t
for chronic constipation. If patients do not respond to
t reatment for chronic constipation, they must be
re f e r red to a gastro e n t e rologist. Patients should also be
re f e r red if they present with new-onset constipation
with any alarm symptoms, which are described in this
monograph by Ms Pallentino in New T h o u g h t s
About an Old Problem: The Impact and Diagnosis of
Johns Hopkins Advanced Studies in Medicine S965
PROCEEDINGS
Figures 2A and 2B. Efficacy of Lubiprostone vs Placebo in
4-Week Studies
SBM = spontaneous bowel movement; LUB = lubiprostone; PL = placebo.
*P <.05 vs placebo;
P <.007 vs placebo;
P .0004 vs placebo.
In these studies, 237 patients (A) or 242 patients (B) received oral lubiprostone 24g or
placebo twice a day for 4 weeks, preceded by a 2-week, drug-free washout period.
Reprinted with permission from McKeage et al. Drugs. 2006;66:873-879.
15
C h ronic Constipation. Ad d i t i o n a l l y, if patients
re q u i rehigh doses of medication to adequately treat the
constipation or if constipation is not alleviated with
any of the recommended treatments, they should be
re f e r red to a gastro e n t e rologist. Lastly, patients should
be re f e r red if they are thought to have pelvic floor
dyssynergia, also known as functional outlet obstru c-
tion or anismus. In this condition, the pelvic floor con-
tracts during attempted defecation, pre venting opening
of the rectal outlet.
When patients are referred, the gastroenterologist
may perform a colonoscopy to exclude causes of sec-
ondary constipation, such as obstructing lesions, or
any of several tests to discern the pathophysiology of
constipation. In clinical practice, the most useful
pathophysiologic tests are anorectal manometry, bal-
loon expulsion, defecography, and the colonic marker
transit study.
3,26
Anorectal manometry assesses several aspects of
internal and external anal sphincter function, in addi-
tion to providing clues to the movements of the pelvic
floor and the function of associated nerves. Anorectal
manometry provides important information regarding
the pressures generated by the anal sphincters at rest
and during maximum voluntary contraction, the pres-
ence or absence of internal sphincter relaxation during
balloon distention, rectal sensation, and the ability to
relax the anal sphincter during straining.
3
In patients
with constipation, this test is especially useful to look
for pelvic floor dyssynergia.
The balloon expulsion test involves placing and
inflating a balloon inside the patients rectum, usually
to a volume of 50 mL. The patient is then asked to
expel the balloon as if defecating. Most normal indi-
viduals can expel the balloon voluntarily within 60
seconds. This is a simple, office-based screening test to
detect a problem with defecation.
3
Defecography detects structural abnormalities of
the rectum and provides clues to the presence of pelvic
floor dyssynergia. It involves placing barium into the
rectum, having the patient sit on a radiolucent com-
mode, and using a fluoroscope to make a videotape
from the lateral position as the patient is asked to hold
stool, bear down while holding, and then release stool
from the rectum. Observations include the patients
ability to completely evacuate their bowels, measuring
the anorectal angle, and detecting any stru c t u r a l
abnormalities (eg, a rectocele). This test is useful when
the radiologist is experienced in its performance and
interpretation, but is subject to performance anxiety
by the patient and misinterpretation by less experi-
enced observers.
3
Colonic marker transit studies are used to evaluate
colonic transit time and are essential for the diagnosis
of slow-transit constipation. For this study, patients
ingest radio-opaque markers in a gelatin capsule; laxa-
tives or enemas are prohibited and abdominal radiog-
raphy is performed 120 hours later. If any of the
markers remain in the intestine, slow-transit constipa-
tion is likely. This test should always be performed
before considering surgery for chronic constipation.
3
Patients with pelvic floor dyssynergia often benefit
from biofeedback training. This approach emphasizes
appropriate coordination of the muscles during defe-
cation. A balloon is inserted into the rectum and
inflated to simulate enough stool that would prompt
the urge to evacuate the bowels. Patients are then asked
to note how this feels and to relax the sphincter mus-
cles and pelvic floor while contracting the diaphragm
and abdominal wall muscles to increase intra-abdomi-
nal pressure. Relaxation and contraction are moni-
tored by electromyography and the display is shown to
the patient so that they can see what they are doing.
Correct relaxation and contraction are reinforced by
the therapist; thus, rapport with the therapist is critical
to success of this treatment.
3
Studies show that approx-
imately 70% of patients with dyssynergic defecation
have complete resolution of constipation with this
treatment (P = .001) and the effects appear to be long
lasting (up to 1 year).
27,28
Of note, biofeedback only is
effective in patients with pelvic floor dyssynergia, not
in patients with slow-transit disorders.
28
Unfortunately,
there are only approximately 12 major motility centers
in the United States that can perform this treatment
effectively, so availability is limited.
CONCLUSIONS
Although chronic constipation can be an uncom-
fortable and embarrassing problem for the patient,
there are many treatment alternatives. The healthcare
provider can work with patients to counsel them about
their treatment options and allay fears of more serious
concerns (eg, cancer) once the appropriate diagnostic
tests have been performed. Although patients often
have tried many of their own treatment strategies by
the time they enter the doctors office, it is important
to document exactly what treatments have been tried
S966 Vol. 6 (10B) November 2006
PROCEEDINGS
and the results. Initial recommendations invo l ve
increased dietary fiber, adequate fluid intake, exercise,
and a dedicated time for bowel movements. Even
when the patient maintains that they have tried
n u m e rous strategies, these treatments should be
reviewed first. In addition to laxatives, there are 2 pre-
scription treatments that offer significant improve-
ment in constipation symptoms for numero u s
patients. Therefore, patients need not feel a sense of
hopelessness or anxiety over this symptom.
REFERENCES
1. Marlett JA, McBurney MI, Slavin JL, American Dietetic
Association. Position of the American Dietetic Association:
health implications of dietary fiber. J Am Diet Assoc.
2002;102:993-1000.
2. Brandt LJ, Prather CM, Quigley EM, et al. Systematic
review on the management of chronic constipation in North
America. Am J Gastroenterol. 2005;100(suppl 1):S5-S21.
3. Lembo A, Camilleri M. Chronic constipation. N Engl J
Med. 2003;349:1360-1368.
4. Prather CM, Camilleri M, Zinsmeister AR, et al. Tegaserod
accelerates orocecal transit in patients with constipation-pre-
dominant irritable bowel syndrome. Gastroenterology.
2000;118:463-468.
5. Coffin B, Farmachidi JP, Rueegg P, et al. Tegaserod, a 5-
HT4 receptor partial agonist, decreases sensitivity to rectal
distension in healthy subjects. Aliment Pharmacol Ther.
2003;17:577-585.
6. Naliboff BD, Chang L, Crowell MD, et al. Tegaserod
increases sigmoid accommodation in female irritable bowel
syndrome (IBS) patients [abstract]. Gastroenterology.
2004;126(suppl 2):A-101.
7. Johanson JF, Wald A, Tougas G, et al. Effect on tegaserod
in chronic constipation: a randomized, double-blind, con-
trolled trial. Clin Gastroenterol Hepatol. 2004;2:796-805.
8. Kamm MA, Muller-Lissner S, Talley NJ, et al. Tegaserod for
the treatment of chronic constipation: a randomized, dou-
ble-blind, placebo-controlled multinational study. Am J
Gastroenterol. 2005;100:362-372.
9. Shetzline M, Dolker M, Bottoli I, Cohard-Radice M. Patients
with chronic constipation who respond to tegaserod after 4
weeks maintain symptom improvement for over 13 months.
Am J Gastroenterol. 2005;100(suppl 9):S339-S340.
Abstract 927.
10. Novartis. Tegaserod prescribing information. Available at:
http://www.pharma.us.novartis.com/product/pi/pdf/zel-
norm.pdf. Accessed August 2006.
11. Sucampo Pharmaceuticals, Inc. Lubiprostone prescribing
information. Available at:
http://www.amitiza.com/resources/pi.pdf. Accessed
August 2006.
12. Moeser A, Engelke K, Perentesis GP, et al. Recovery of
mucosal barrier function in ischemic porcine ileum and
colon is stimulated by a novel antagonist of the Clc-2 chlo-
ride channel, Spi-0211. Gastroenterology.
2005;128(suppl 2):A539. Abstract T1734.
13. Cuppoletti J, Malinowska DH, Tewari KP, et al. SPI-0211
activates T84 cell chloride transport and recombinant
human CIC-2 chloride currents. Am J Physiol Cell Physiol.
2004;287:C1173-C1183.
14. Basavappa S, Vulapalli SR, Zhang H, et al. Chloride chan-
nels in the small intestinal cell line IEC-18. J Cell Physiol.
2005;202:21-31.
15. McKeage K, Plosker GL, Siddiqui MA. Lubiprostone. Drugs.
2006;66:873-879.
16. Johanson JF, Gargano MA, Holland PC, et al. Phase III
study of lubiprostone, a chloride channel-2 (ClC-2) activator
for the treatment of constipation: safety and primary effica-
cy. Am J Gastroenterol. 2005;100(suppl 9):s328-s329.
Abstract 896.
17. Johanson JF, Gargano MA, Holland PC, et al. Phase III effi-
cacy and safety of RU-0211, a novel chloride channel acti-
vator, for the treatment of constipation. Gastroenterology.
2003;124(suppl 1):A48. Abstract 372.
18. Joswick TR, Ueno R, Wahle A, et al. Efficacy and safety of
lubiprostone for the treatment of chronic constipation in
elderly vs non-elderly subjects. Gastroenterology.
2006;130(suppl 2):A189. Abstract S1262.
19. Joswick TR, Ueno R, Wahle A, et al. Efficacy and safety of
lubiprostone for the treatment of chronic constipation in
male vs female subjects. Gastroenterology.
2006;130(suppl 2):A322. Abstract M1195.
20. Johanson JF, Gargano MA, Holland PC, et al. Initial and
sustained effects of lubiprostone, a chloride channel-2 (ClC-
2) activator for the treatment of constipation: data from a 4-
week phase III study. Am J Gastroenterol. 2005;100(suppl
9):s324-s325. Abstract 884.
21. Johanson JF, Gargano MA, Holland PC, et al. Multicenter
open-label study of oral lubiprostone for the treatment of
chronic constipation. Am J Gastroenterol. 2005;100(suppl
9):s331. Abstract 903.
22. Johanson JF, Gargano MA, Holland PC, et al. Phase III
patient assessments of the effects of lubiprostone, a chloride
channel-2 (ClC-2) activator, for the treatment of constipa-
tion. Am J Gastroenterol. 2005;100(suppl 9):s329-s330.
Abstract 899.
23. Johanson JF, Gargano MA, Holland PC, et al. Phase III, ran-
domized withdrawal study of RU-0211, a novel chloride
channel activator for the treatment of constipation [abstract].
G a s t ro e n t e ro l o g y. 2004;126(suppl 2):A100. Abstract 749.
24. Johanson JF, Gargano MA, Patchen ML, et al. Efficacy and
safety of a novel compound, RU-0211, for the treatment of
constipation. Gastroenterology. 2002;122(suppl 1):A315.
Abstract M1511.
25. Ueno R, Osama H, Habe T, et al. Oral SPI-0211 incre a s e s
intestinal fluid secretion and chloride concentration without
altering serum electrolyte levels. G a s t ro e n t e ro l o g y.
2004;126(suppl 2):A298. Abstract M1109.
26. Rao SS, Ozturk R, Laine L. Clinical utility of diagnostic tests
for constipation in adults: a systematic review. Am J
Gastroenterol. 2005;100:1605-1615.
27. Rao SS, Kinkade KJ, Miller MJ, et al. Randomized con-
trolled trial of long-term outcome of biofeedback therapy for
dyssynergic defecation. Am J Gastroenterol.
2005;100(suppl 9):S150. Abstract 386.
28. Chiarioni G, Salandini L, Whitehead WE. Biofeedback
benefits only patients with outlet dysfunction, not patients
with isolated slow transit constipation. Gastroenterology.
2005;129:86-97.
Johns Hopkins Advanced Studies in Medicine S967
PROCEEDINGS
Вам также может понравиться
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Diabetic Foot CareДокумент50 страницDiabetic Foot CareaswiniОценок пока нет
- The Book of BulkДокумент16 страницThe Book of BulkpopeyeballinaОценок пока нет
- User's Manual: M200A Syringe PumpДокумент44 страницыUser's Manual: M200A Syringe PumpGandavaa Enkhee50% (4)
- VACCP Template Checklist - SafetyCultureДокумент7 страницVACCP Template Checklist - SafetyCulturepattysaborio520Оценок пока нет
- Barangay Anti-Drug Abuse Council (Badac) Training: Activity DesignДокумент3 страницыBarangay Anti-Drug Abuse Council (Badac) Training: Activity DesignMaria Fiona Duran Merquita100% (2)
- Pilferage Control in HospitalsДокумент4 страницыPilferage Control in HospitalsDr. Rakshit Solanki100% (3)
- POCSOДокумент15 страницPOCSOThakur Avnish Singh100% (1)
- Nursing Care Plan 2 Knowledge DeficitДокумент7 страницNursing Care Plan 2 Knowledge Deficitdbryant0101100% (3)
- Mmda V Concerned Citizens of Manila Bay (GR No 171947) DigestДокумент2 страницыMmda V Concerned Citizens of Manila Bay (GR No 171947) DigestJose Ramon Ampil83% (6)
- Gaint Cell Lesions UPLOADДокумент176 страницGaint Cell Lesions UPLOADAkshayОценок пока нет
- ABC of Intensive CareДокумент49 страницABC of Intensive CareCurro MirallesОценок пока нет
- Product PlanДокумент19 страницProduct Planlily30109150% (2)
- Tri Gunadi Healthcare Ecosystem SolutionДокумент21 страницаTri Gunadi Healthcare Ecosystem SolutionGembong Van BeethovenОценок пока нет
- Standar Obat AalДокумент15 страницStandar Obat AalGembong Van BeethovenОценок пока нет
- OIYRGBДокумент4 страницыOIYRGBGembong Van BeethovenОценок пока нет
- Wuwse6 2Документ1 страницаWuwse6 2Gembong Van BeethovenОценок пока нет
- Sterilization by FiltrationДокумент13 страницSterilization by FiltrationGembong Van BeethovenОценок пока нет
- Lion Air Eticket Itinerary / ReceiptДокумент2 страницыLion Air Eticket Itinerary / ReceiptGembong Van BeethovenОценок пока нет
- Determination and Validation of Uv Spectrophotometric Method For Estimation of Bicalutamide TabletДокумент5 страницDetermination and Validation of Uv Spectrophotometric Method For Estimation of Bicalutamide TabletGembong Van BeethovenОценок пока нет
- Gout N AlkoholДокумент0 страницGout N AlkoholGembong Van BeethovenОценок пока нет
- 2005-4137S1 04 ShahДокумент31 страница2005-4137S1 04 ShahGembong Van BeethovenОценок пока нет
- Factsheet CodeineДокумент2 страницыFactsheet CodeineGembong Van BeethovenОценок пока нет
- DCMA Sampling GuidanceДокумент4 страницыDCMA Sampling GuidanceGembong Van BeethovenОценок пока нет
- Q4B Annex4B R1 Step4Документ8 страницQ4B Annex4B R1 Step4Udayabhaskar BandarupalliОценок пока нет
- Presentation Title: My Name Contact Information or Project DescriptionДокумент2 страницыPresentation Title: My Name Contact Information or Project DescriptionGembong Van BeethovenОценок пока нет
- Presentation Title: My Name Contact Information or Project DescriptionДокумент2 страницыPresentation Title: My Name Contact Information or Project DescriptionGembong Van BeethovenОценок пока нет
- Filmstrip Countdown: Please Note The Countdown Timer Will Only Work On The Latest Versions of Powerpoint (2003 and Later)Документ16 страницFilmstrip Countdown: Please Note The Countdown Timer Will Only Work On The Latest Versions of Powerpoint (2003 and Later)Gembong Van BeethovenОценок пока нет
- 00217Документ24 страницы00217oumhineaОценок пока нет
- 00214Документ8 страниц00214Hekmatyar Aslamthu HaqОценок пока нет
- Back To School Powerpoint Template 3Документ4 страницыBack To School Powerpoint Template 3Gembong Van BeethovenОценок пока нет
- 00217Документ24 страницы00217Gembong Van BeethovenОценок пока нет
- Back To School Powerpoint Template 3Документ4 страницыBack To School Powerpoint Template 3Gembong Van BeethovenОценок пока нет
- Back To School Powerpoint Template 3Документ4 страницыBack To School Powerpoint Template 3Gembong Van BeethovenОценок пока нет
- PCNE Classification V5.01Документ9 страницPCNE Classification V5.01Alfredo DiasОценок пока нет
- A Stability Program For The Distribution of Drug ProductsДокумент5 страницA Stability Program For The Distribution of Drug ProductsGembong Van BeethovenОценок пока нет
- Sustained-Release Matrix Tablets of Metformin Hydrochloride in Combination With Triacetyl-B-CyclodextrinДокумент7 страницSustained-Release Matrix Tablets of Metformin Hydrochloride in Combination With Triacetyl-B-CyclodextrinGembong Van BeethovenОценок пока нет
- A Stability Program For The Distribution of Drug ProductsДокумент5 страницA Stability Program For The Distribution of Drug ProductsGembong Van BeethovenОценок пока нет
- SmadaДокумент6 страницSmadaGembong Van BeethovenОценок пока нет
- Blue Green Yellow Modern English Intrapersonal Communication Educational Presentation - 20231109 - FixДокумент12 страницBlue Green Yellow Modern English Intrapersonal Communication Educational Presentation - 20231109 - FixmhailvandalzОценок пока нет
- Tinnitus Today September 1986 Vol 11, No 3Документ8 страницTinnitus Today September 1986 Vol 11, No 3American Tinnitus AssociationОценок пока нет
- Exam Table For Shoulder and ElbowДокумент17 страницExam Table For Shoulder and ElbowLouie OkayОценок пока нет
- Antibiotic Use in Food Animals Worldwide, With A Focus On Africa - Pluses and MinusesДокумент8 страницAntibiotic Use in Food Animals Worldwide, With A Focus On Africa - Pluses and MinusesxubicctОценок пока нет
- ROICAM7 BookletДокумент99 страницROICAM7 BookletPopy HalifahОценок пока нет
- Aspiracion Destornillador Implanto Roa-V1-Id1018Документ3 страницыAspiracion Destornillador Implanto Roa-V1-Id1018CesarAmorotoОценок пока нет
- Development of Road Header Roof Bolting ModuleДокумент7 страницDevelopment of Road Header Roof Bolting ModuleCraig ThomasОценок пока нет
- Medical Examiner'S Confidential ReportДокумент2 страницыMedical Examiner'S Confidential ReportParesh BorboruahОценок пока нет
- Survey QuestionnaireДокумент3 страницыSurvey Questionnairebintot882Оценок пока нет
- K4health-The Mhealth Planning Guide Key Considerations For Integrating Mobile Technology Into Health Programs-2015!04!06Документ49 страницK4health-The Mhealth Planning Guide Key Considerations For Integrating Mobile Technology Into Health Programs-2015!04!06DitaMaryaniОценок пока нет
- Headache Management Guideline For Adults Version 10Документ6 страницHeadache Management Guideline For Adults Version 10TomiОценок пока нет
- A Review On Water Used in Pharma Industry: European Journal of Pharmaceutical and Medical ResearchДокумент11 страницA Review On Water Used in Pharma Industry: European Journal of Pharmaceutical and Medical ResearchDinesh babuОценок пока нет
- Root Caries: A Periodontal Perspective: Review ArticleДокумент21 страницаRoot Caries: A Periodontal Perspective: Review ArticleIlmia AmaliaОценок пока нет
- RULE 1142. Marine Tank Vessel OperationsДокумент8 страницRULE 1142. Marine Tank Vessel OperationsksalvaradoОценок пока нет
- BAYBAY AwardsДокумент63 страницыBAYBAY AwardsClennil Palmes SustraidoОценок пока нет
- AOE - Hiral Labs LTD Company Brochure 20180416170521Документ20 страницAOE - Hiral Labs LTD Company Brochure 20180416170521Dr VENKAT1 LUОценок пока нет
- How To Build Your Creative Confidence PDFДокумент2 страницыHow To Build Your Creative Confidence PDFSteph GonzagaОценок пока нет
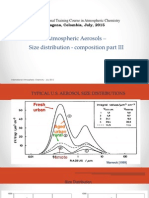
- Cartagena Part3 Aerosols CompositionДокумент62 страницыCartagena Part3 Aerosols CompositionEDWARDОценок пока нет
- Microbial Content and Diversity Inseveral Tempe From Bogor AreasДокумент9 страницMicrobial Content and Diversity Inseveral Tempe From Bogor AreasCendra KammiОценок пока нет
- NDEPДокумент5 страницNDEPjoeОценок пока нет