Академический Документы
Профессиональный Документы
Культура Документы
Best Practice in The Use of Spirometry
Загружено:
Dennis CobbИсходное описание:
Оригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Best Practice in The Use of Spirometry
Загружено:
Dennis CobbАвторское право:
Доступные форматы
art & science respiratory disorders
&
Best practice in the use of spirometry
Booker R (2005) Best practice in the use of spirometry. Nursing Standard. 19, 48, 49-54. Date of acceptance: March 18 2005.
Summary
This article examines spirometry as a method of detecting lung disease, particularly chronic obstructive pulmonary disease (COPD). Methods of producing an accurate assessment and identifying acceptable traces are outlined, and contraindications are discussed.
Definition
A spirometer is a piece of equipment that an individual blows into through a mouthpiece. It is used to measure lung volume and the rate at which air can be exhaled during forced exhalation. There are a variety of spirometers available. The simplest, volumetric spirometers, measure volume directly. Types of volumetric spirometers include: Water-sealed spirometers. Rolling-seal spirometers. Wedge bellow spirometers. Volumetric spirometers tend to be large. A wedge bellow spirometer, for example, is the size of a large microwave and water-sealed and rollingseal spirometers are even larger. Volumetric spirometers are most commonly used in secondary care settings in outpatient clinics and pulmonary function laboratories where they do not need to be moved around. They cost between 1,500 and 3,000, although may cost more. Other spirometers use a variety of technologies to sense airflow and electronically calculate volume from flow. They are smaller and generally more suitable for use by health professionals in primary care and community settings. These include: Pneumotachographs. Anemometers. Turbine spirometers. Ultrasound spirometers. They range from desktop models, which are about the size of a laptop computer, to small hand-held devices. These spirometers range in price from 300500 for a basic hand-held spirometer to 1,0001,500 for a desktop spirometer. Compared with volumetric spirometry, the performance is the same as long as the equipment is used appropriately. The main difference is that the technique is less easy to assess with some electronic flow measuring devices.
Author
Rachel Booker is COPD module leader and head of student support, the National Respiratory Training Centre, Warwick. Email: r.booker@nrtc.org.uk
Keywords
COPD, Lung disorders, Respiratory system and disorders These keywords are based on the subject headings from the British Nursing Index. This article has been subject to double-blind review. For related articles and author guidelines visit our online archive at www.nursing-standard.co.uk and search using the keywords. RESPIRATORY DISEASE is a major cause of morbidity and mortality in the UK. More people die from respiratory disease than coronary heart disease or cancer, and respiratory illness is the most common reason for emergency hospital admission. Almost a third of the population will visit their GP with a respiratory condition at least once a year (British Thoracic Society (BTS) 2000). Objective diagnosis, monitoring and appropriate management of respiratory disease require measurement of lung function. The latest asthma guideline (BTS and Scottish Intercollegiate Guidelines Network (SIGN) 2003) highlights the need for objective diagnosis and recommends spirometry to assist with this. The first national guideline on the management of chronic obstructive pulmonary disease (COPD) (BTS 1997) recommended spirometry for the early and accurate diagnosis of COPD. The recent COPD management guideline from the National Institute for Health and Clinical Excellence (NICE) (National Collaborating Centre for Chronic Conditions (NCCCC) 2004) supports the use of spirometry for diagnosis and monitoring of COPD, and recommends that spirometry be widely available in all healthcare settings. There has been an increase in spirometry use and nurses are more frequently performing the procedure and interpreting results. NURSING STANDARD
Measurement
A spirometer measures accessible lung volume vital capacity. Accessible refers to the fact that august 10 :: vol 19 no 48 :: 2005 49
art & science respiratory disorders
spirometers can only measure the air that is exhaled and inhaled. There is always some air remaining in the lungs at the end of the exhalation that cannot be measured with a spirometer. This is known as the residual volume. The residual volume plus the vital capacity make up the total lung capacity. Accessible lung volume is measured in two ways: Relaxed vital capacity (RVC). A relaxed exhalation from maximal inhalation to maximal exhalation. Forced vital capacity (FVC). A forced exhalation from maximal inhalation to maximal exhalation using maximum effort. The volume of air exhaled in the first second of forced exhalation is also measured: Forced expired volume in one second (FEV1). These lung volumes are expressed as both absolute volumes, in litres, and as a percentage of the predicted reference value for someone of that age, gender, height and ethnic group. Normative values for the UK population are available (Quanjer et al 1993, NCCCC 2004). The FEV1 is also expressed as a percentage of FVC or RVC (if this is greater): FEV1% or FEV1/FVC, FEV1/RVC. FEV1% is the marker of airflow obstruction. Values of less than 70 per cent are diagnostic of obstructive airways disease. Abnormal spirometry, however, cannot confirm a diagnosis. Spirometry must only be interpreted in the light of a good history and other diagnostic tests. RVC, FVC, FEV1 and FEV1% are the most important parameters of lung function. Most electronic spirometers will also produce an array of other measurements, most of which are not essential for simple spirometry. BOX 1 Calculation of forced expired volume in one second as a percentage of forced or relaxed vital capacity (FEV1%) If FVC is greater than RVC: FEV1% = FEV1 x 100 FVC If RVC is greater than FVC: FEV1% = FEV1 x 100 RVC FVC = forced vital capacity; RVC = relaxed vital capacity 50 august 10 :: vol 19 no 48 :: 2005
&
Spirometry results can be presented graphically in two ways: A volume/time graph of volume exhaled in litres (vertical axis) against the time taken in seconds to exhale completely (horizontal axis). A flow/volume graph of flow rate in litres per second (vertical axis) against volume in litres (horizontal axis).
Disease and spirometry measurement
In patients with normal lung function: The FVC should be the same or slightly greater than RVC. The FVC should be greater than 80% of the predicted value for an individual of that age, gender, height and ethnic group. The FEV1 should be greater than 80% of the predicted value for an individual of that age, gender, height and ethnic group. The FEV1% (that is, the FEV1 expressed as a percentage of the FVC or RVC if that is greater) should be between 75 and 85% to be within normal range. The FEV1% is a different measurement from the FEV1 as a percentage of the predicted FEV1. Obstructive lung diseases, such as asthma and COPD, obstruct airflow and will reduce the volume of air exhaled in one second (FEV1), so that it is less than 80% of the predicted value, and reduce FEV1%. An FEV1% that is less than 70% is diagnostic of airflow obstruction. FVC and FEV1 will be less than 80% of the predicted value where lung volumes are restricted, for example, in pulmonary fibrotic diseases such as fibrosing alveolitis, or musculoskeletal disease such as kyphoscoliosis. However, these disorders do not obstruct airflow and FEV1% is unaffected. In restrictive disorders, FEV1% is more than 75% and is often greater than 85%. In severe airflow obstruction, dynamic airway collapse during forced exhalation traps air in the lungs and reduces FVC causing restriction and obstruction. In such cases, RVC will be significantly higher than FVC and will more accurately reflect vital capacity than FVC . Calculation of FEV1 as a percentage of RVC (Box 1) may reveal a reduced FEV1% indicative of airflow obstruction that may otherwise be missed. Table 1 summarises the parameters of lung function affected in various respiratory diseases. The effects of obstructive, severe obstructive and restrictive diseases on volume/time and flow/volume traces are shown in Figures 1 and 2. NURSING STANDARD
Peak expiratory flow
Peak expiratory flow (PEF) is defined as: the maximum flow achieved during an expiration delivered with maximal force starting from maximal lung inflation (American Thoracic Society 1995). Measurement of PEF is easy. PEF meters cost less than 10, are portable and available on prescription. This makes them suitable for patients to use and keep at home, and they are useful for detection and ongoing monitoring of variable airflow obstruction: the hallmark of asthma. PEF is of limited use in other respiratory conditions. PEF measures flow rate in the first tenth of a second of a forced exhalation. PEF measures flow rate and FEV1 is a measure of volume. They are not interchangeable and PEF cannot be predicted from FEV1 or vice versa. Reference predicted PEF values are less robust than spirometric values. PEF is insufficiently sensitive to detect early airflow obstruction in COPD and can seriously underestimate the degree of airflow obstruction in more severe COPD. Therefore, spirometry is more suitable for assisting in the diagnosis of COPD (NCCCC 2004). A further limitation of PEF is TABLE 1 Effect of respiratory disease on spirometry Normal RVC FVC FEV1 Same as or less than FVC More than 80% of predicted More than 80% of predicted Obstruction
that, unlike spirometry, it does not measure lung volumes and cannot be used to detect restrictive lung diseases, such as pulmonary fibrosis.
Criteria for optimal spirometry
The BTS and the Association for Respiratory Technology and Physiology (ARTP) (BTS and ARTP 1994) suggest four optimal criteria for a spirometer (Box 2). Most mid-price range and desktop electronic spirometers fit the above criteria. Hand-held spirometers are relatively cheap, but may not have a visual display. Unless they are linked to a computer, it is not possible to verify adequacy of the technique and hard copies of results may not be produced. Charts of reference values may have to be used to manually calculate and interpret the results, creating the potential for error. Some electronic spirometers have additional mechanisms for checking the adequacy of the patients technique. They will detect errors, such as a slow start to the forced blow, early stoppage, hesitation, and poor effort. An additional feature of some electronic spirometers is the ability to interface with the patients computerised medical record. This allows easy storage and retrieval of
Severe obstruction Greater than FVC Less than 80% of predicted Less than 80% of predicted Less than 70%
Restriction Same as or less than FVC Less than 80% of predicted Less than 80% of predicted 75-85% or higher
Same as or greater than FVC More than 80% of predicted Less than 80% of predicted Less than 70%
FEV1% 75-85%
RVC = relaxed vital capacity; FVC = forced vital capacity; FEV1 = forced expired volume in the first second of exhalation FIGURE 1 Abnormal volume/time traces Obstruction. Flattened trace Restriction. Normal shaped but small trace
Volume in litres Volume in litres
Severe obstruction. Flattened and small trace
Volume in litres
Predicted
FEV1
Predicted
FEV1
Predicted
FEV1
Measured
Measured
Measured
Time in seconds
Time in seconds
Time in seconds
NURSING STANDARD
august 10 :: vol 19 no 48 :: 2005 51
art & science respiratory disorders
results, or emailing of results for quality-control purposes (Box 3).
&
Performance and interpretation
Spirometry, like PEF, is a relatively easy measurement, but it does require effort and coBOX 2 Four optimal criteria for a spirometer A spirometer that produces a hard copy of the results. Print out a hard copy of the volume/time graph that is of sufficient size to enable manual verification of results. A flow/volume graph is an optional extra, but is extremely useful for the detection of early airflow obstruction. It is available with most modern electronic spirometers. Calibration should be checked using a calibration syringe. Some electronic spirometers will allow updating of calibration, others require the spirometer to be sent back to the manufacturer for recalibration. A visual display of the blow, preferably a real-time display of volume/time or flow/volume graphs as the patient is blowing, enables assessment of the patients technique.
(BTS and ARTP 1994)
operation from the patient. It is also essential that the health professional taking the measurements is trained in the technique and is able to recognise technically acceptable results and correct technique errors. It is also vital that whoever interprets the results is trained and competent. Poorly performed and interpreted spirometry is likely to lead to misdiagnosis or missed diagnosis (Woolhouse and OHickey 1999). The NICE COPD guideline recommends that qualitycontrol mechanisms are set up to support primary care spirometry services (NCCCC 2004). In accordance with their Code of Professional Conduct (NMC 2004), nurses responsible for recording or interpreting spirometry must ensure they are appropriately trained.
Contraindications
There are no absolute contraindications to spirometry but common sense should be exercised. Where there are any grounds for concern, assessment at a lung function laboratory may be advisable. Forced expiration using maximum effort raises intracranial, intrathoracic and intraabdominal pressure. Therefore, consider deferring spirometry for about six weeks in patients who have had recent eye, chest or abdominal surgery, or who have recently had a myocardial infarction or cerebrovascular accident (BTS and ARTP 1994). Spirometry can produce bronchospasm, particularly in patients with chest infections and bronchial hyperreactivity. Spirometry readings will progressively worsen with each effort and further attempts should be abandoned. Spirometry should be performed when the patient is clinically stable and free of infection whenever possible.
FIGURE 2 Abnormal flow/volume traces Predicted normal curve Measured Predicted PEF
Flow rate in litres per second
Flow rate in litres per second
Measured
Flow rate in litres per second
Predicted FVC
Volume in litres
Volume in litres
Volume in litres
Restriction. Normal PEF; reduced FVC; narrow, domed trace
Mild obstruction. Scooped, concave trace
Severe obstruction. Markedly scooped out trace; reduced PEF and FVC
PEF = peak expiratory flow; FVC = forced vital capacity 52 august 10 :: vol 19 no 48 :: 2005 NURSING STANDARD
Cross-infection and risk minimisation
Contamination of spirometry equipment and the potential for cross-infection need to be considered. Although there is no study or case report that has demonstrated that spirometry poses a significant risk to patients, common sense and good hygienic practices should be used. Ultrasonic and anemometer spirometers use disposable single-patient-use mouthpieces that prevent cross-infection. The use of one-way mouthpieces with other spirometers can prevent accidental inhalation through the spirometer, and are a minimum requirement to reduce infection risk. If inhalations are required, a bacterial and viral filter will be needed. Patients suspected of having active chest infection, particularly tuberculosis, should not be tested. If spirometry is clinically necessary, patients with chest infection should be tested at the end of the day with equipment that can be disinfected after use. Patients who are immunocompromised should BOX 3 Essential features of a spirometer A good spirometer is one that is: Simple to use. Robust and reliable. Easy to clean and disinfect. Supplied by a company providing reliable technical support and assistance. Suitable for the workplace. Meets the British Thoracic Society and Association for Respiratory Technology and Physiology (1994) criteria.
be tested at the beginning of the day on newly disinfected equipment. Flow sensors, such as pneumotachographs and turbines need to be cleaned and disinfected according to manufacturers instructions. Flow sensors cannot be autoclaved and the use of inappropriate sterilising fluids can damage or destroy them. Disinfection of volumetric spirometers is difficult and costly. Therefore, it is essential that the correct mouthpieces are used and care is taken to protect patients from cross-infection.
Spirometer calibration
Calibration of all spirometers should be regularly checked and a log kept of this procedure. Electronic spirometers should be checked before each session using a calibration syringe. Although current flow sensors are often robust and reliable, it is necessary to check that the equipment is recording accurately.
Technically acceptable and meaningful results
RVC should be recorded as a baseline measurement. It is important to ensure that the patient has taken a maximal inhalation. The mouthpiece is positioned so that the tongue and teeth do not occlude it and the lips are sealed around it to prevent air leaks. A nose clip is used to prevent air leakage down the nose. The patient needs to exhale steadily, in a relaxed manner until he or she is unable to exhale any further. This should be repeated at least twice, or until the two best readings vary by less than 5% and 100ml. A minimum of three forced exhalations needs to be recorded so that the best two readings of FEV1 and FVC vary by less than 5% and 100ml. If necessary, eight exhalations can be undertaken to achieve this level of reproducibility. Vigorous verbal
References
American Thoracic Society (1995) Standardization of spirometry, 1994 update. American Journal of Respiratory and Critical Care Medicine. 152, 3, 1107-1136. British Thoracic Society and the Association for Respiratory Technology and Physiology (1994) Guidelines for the measurement of respiratory function. Respiratory Medicine. 88, 3, 165-194. British Thoracic Society (1997) BTS guidelines for the management of chronic obstructive pulmonary disease. Thorax. 52 (Suppl 5), S1-S28. British Thoracic Society (2000) The Burden of Lung Disease. BTS, London. British Thoracic Society and Scottish Intercollegiate Guidelines Network (2003) British guideline on the management of asthma. Thorax. 58 (Suppl 1), i1-94. Department of Health (2003) Investing in General Practice: The New General Medical Services Contract. www.dh.gov.uk/assetRoot/04/07/19/67/04 071967.pdf (Last accessed: July 29 2005.) Halpin DMG, Rudolph M on behalf of the BTS COPD Consortium (2002) Implementing the BTS COPD Guidelines: how far have we come? European Respiratory Journal. 20 (Suppl 38), 1637. National Collaborating Centre for Chronic Conditions (2004) Chronic obstructive pulmonary disease. National clinical guideline on management of chronic obstructive pulmonary disease in adults in primary and secondary care. Thorax. 59 (Suppl 1), 1-232.
NURSING STANDARD
august 10 :: vol 19 no 48 :: 2005 53
art & science respiratory disorders
FIGURE 3 Acceptable volume/time and flow/volume traces Volume/time. Smooth trace that reaches a plateau Flow/volume. Rapid, almost vertical rise to peak expiratory flow (PEF); trace merges with baseline at forced vital capacity (FVC)
&
FEV1
Flow in litres per second
Volume in litres
FVC
PEF
FVC
Time in seconds
Volume in litres
encouragement to exhale continuously with force will help ensure maximum effort to FVC. The acceptability of the forced exhalations needs to be checked by looking at graphic traces of volume/time and flow/volume. Traces should be smooth and free of irregularity. The volume/time trace should curve smoothly upwards to a plateau and the flow/volume trace should rise almost vertically to a peak and should merge smoothly with the horizontal axis. Inadequate blows must be rejected. Spirometry cannot be interpreted unless acceptability and reproducibility criteria are met. Technically acceptable traces showing normal lung function are shown in Figure 3.
Conclusion
Spirometry was, until recently, only available routinely in secondary care settings. The
publication of disease management guidelines (BTS 1997, BTS and SIGN 2003, NCCCC 2004) has prompted increased spirometry use in primary care (Halpin and Rudolph 2002). The new General Medical Services Contract (Department of Health 2003), which financially rewards general practices for diagnosing and monitoring COPD with spirometry, has prompted the widespread use of spirometers in general practice. There are concerns about the quality of spirometry practice in primary care and the ability of some primary healthcare professionals to interpret results (Woolhouse and OHickey 1999). However, with appropriate training, continued practice and good quality control, respiratory patients in all healthcare settings can have lung function objectively assessed and be diagnosed and treated appropriately (Schermer et al 2003) NS
References continued
Nursing and Midwifery Council (2004) The NMC Code of Professional Conduct: Standards for Conduct, Performance and Ethics. NMC, London. Quanjer PH, Tammeling GJ, Cotes JE, Pedersen OF, Peslin R, Yernault JC (1993) Lung volumes and forced ventilatory flows. Report Working Party Standardization of Lung Function Tests, European Community for Steel and Coal. Official Statement of the European Respiratory Society. European Respiratory Journal Supplement. 16, 5-40. Schermer T, Eaton T, Pauwels R, van Weel C (2003) Spirometry in primary care: is it good enough to face demands like World COPD Day? European Respiratory Journal. 22, 5, 725-727. Woolhouse I, OHickey SP (1999) Accuracy of spirometry measured in general practice compared to a hospital pulmonary function laboratory. European Respiratory Journal. 14 (Suppl 30), 273s. RESOURCES Short course in basic spirometry and interpretation is available from The National Respiratory Training Centre: www.nrtc.org.uk Certification of competence in spirometry and its interpretation is available from The Association for Respiratory Technology and Physiology: www.artp.org.uk British Thoracic Society chronic obstructive pulmonary disease consortium publications: www.brit-thoracic.org.uk/iqs/copd-publications-library.html
54 august 10 :: vol 19 no 48 :: 2005
NURSING STANDARD
Вам также может понравиться
- 1.B.09 Resp TestsДокумент2 страницы1.B.09 Resp Testsalemante100% (1)
- Spirometry (PPT & Words) 1Документ5 страницSpirometry (PPT & Words) 1Fluffyyy BabyyyОценок пока нет
- Spirometry InterpretationДокумент4 страницыSpirometry InterpretationSSОценок пока нет
- Spiro Me Try Cheat Sheet 09Документ2 страницыSpiro Me Try Cheat Sheet 09Yudha Perwira PutraОценок пока нет
- The PFT LexiconДокумент3 страницыThe PFT Lexiconjmel67Оценок пока нет
- Pulmonary Function Tests in Clinical PracticeОт EverandPulmonary Function Tests in Clinical PracticeAli AltalagРейтинг: 5 из 5 звезд5/5 (1)
- Pulmonary Function TestДокумент3 страницыPulmonary Function Testhm3398Оценок пока нет
- lr5 - ILHAASHINI (012021090323) - Lab 5 DoneДокумент7 страницlr5 - ILHAASHINI (012021090323) - Lab 5 DoneIlhaashini krishnanОценок пока нет
- Interpreting Pulmonary Function TestsДокумент10 страницInterpreting Pulmonary Function TestsSuresh Kumar100% (1)
- Resp Yamashita PulmonaryFunctionTests NotesДокумент13 страницResp Yamashita PulmonaryFunctionTests Notes1233211qwerasdОценок пока нет
- Dr. Rowshne Jahan Spirometry Presentation-1Документ40 страницDr. Rowshne Jahan Spirometry Presentation-1Shahadat Hossain BabuОценок пока нет
- Spirometric ValuesДокумент18 страницSpirometric ValuesSensing NonsenseОценок пока нет
- Diagnostic SpirometerДокумент3 страницыDiagnostic SpirometerseventhsensegroupОценок пока нет
- Pulmonary Function TestДокумент7 страницPulmonary Function TestGhada HusseinОценок пока нет
- Lung Asthma Pulmonary Fibrosis Cystic Fibrosis CopdДокумент12 страницLung Asthma Pulmonary Fibrosis Cystic Fibrosis CopdEjnc RuedaОценок пока нет
- Wireless Smartphone-Based SystemДокумент20 страницWireless Smartphone-Based SystemMay Shuen PoonОценок пока нет
- 5-Pulmonary Function TestsДокумент35 страниц5-Pulmonary Function TestsDoha JKОценок пока нет
- Simple Office SpirometryДокумент42 страницыSimple Office SpirometryRoberto Merza III100% (4)
- PBL 1 RSДокумент7 страницPBL 1 RSmarams8bОценок пока нет
- Assessment of Suitability For Lung Resection: Gerard Gould FRCA Adrian Pearce FRCAДокумент4 страницыAssessment of Suitability For Lung Resection: Gerard Gould FRCA Adrian Pearce FRCAsayednourОценок пока нет
- Respiratory Function TestДокумент7 страницRespiratory Function TestMarivic DianoОценок пока нет
- Pulmonary Function Testing in Asthma - UpToDateДокумент17 страницPulmonary Function Testing in Asthma - UpToDateJuan ArangurenОценок пока нет
- Pl1. DM Investigations in Pulmonary Diseases: 1. Tests of Pulmonary VentilationДокумент6 страницPl1. DM Investigations in Pulmonary Diseases: 1. Tests of Pulmonary VentilationVittorio Di PaoloОценок пока нет
- Pulmonary Function TestsДокумент28 страницPulmonary Function TestsHarshit yadavОценок пока нет
- Applsci 09 02842 PDFДокумент13 страницApplsci 09 02842 PDFFelicia SutarliОценок пока нет
- Measurements.: Spirometry Is The Name of The Test, Whilst A Spirometer Is The Device That Is Used To Make TheДокумент7 страницMeasurements.: Spirometry Is The Name of The Test, Whilst A Spirometer Is The Device That Is Used To Make TheDebasis SahooОценок пока нет
- Assessment of Respiratory FunctionДокумент1 страницаAssessment of Respiratory FunctionRoderick AgbuyaОценок пока нет
- Spirometry: DescriptionДокумент7 страницSpirometry: DescriptionJuniar Faiz MОценок пока нет
- BBB 1 - Pulmonary Function Tests InterpretationДокумент14 страницBBB 1 - Pulmonary Function Tests InterpretationArhanОценок пока нет
- (Spondilitis) : SpirometryДокумент4 страницы(Spondilitis) : Spirometrypragna novaОценок пока нет
- COPD - Diagnosis and ManagementДокумент12 страницCOPD - Diagnosis and ManagementfallenczarОценок пока нет
- Onbrez June 2014Документ32 страницыOnbrez June 2014NateStephBarnardОценок пока нет
- Pulmonary Function Pulmonary Function Pulmonary Function Tests TestsДокумент62 страницыPulmonary Function Pulmonary Function Pulmonary Function Tests TestsAaliyah ShaikhОценок пока нет
- Respiration 3... Pulmonary Function TestsДокумент26 страницRespiration 3... Pulmonary Function Testsapi-19641337Оценок пока нет
- Spirometry Testing - What Is A SpirometerДокумент11 страницSpirometry Testing - What Is A SpirometerFatima Sherrisa SaliОценок пока нет
- Penggunaan APEДокумент22 страницыPenggunaan APEdevi efrinaОценок пока нет
- Body Plethysmograph: Department of PhysiologyДокумент9 страницBody Plethysmograph: Department of PhysiologyVeena ShriramОценок пока нет
- Pulmonary Function TestsДокумент13 страницPulmonary Function TestsZazzZaffaОценок пока нет
- Pulmonary Function Test in Pre Anaesthetic EvaluationДокумент10 страницPulmonary Function Test in Pre Anaesthetic EvaluationSuresh KumarОценок пока нет
- Final Project ProposalДокумент7 страницFinal Project Proposalيحيى البشيتيОценок пока нет
- Electronic Spirometer For The Assessment of Lung's FunctionalityДокумент4 страницыElectronic Spirometer For The Assessment of Lung's Functionalitynagarajka100% (2)
- Pulmonary Function TestsДокумент29 страницPulmonary Function TestsOrion JohnОценок пока нет
- 05 j.1532-5415.2007.01332.x EPOC PDFДокумент7 страниц05 j.1532-5415.2007.01332.x EPOC PDFAlejandroОценок пока нет
- PFT Class NotesДокумент7 страницPFT Class NotesFajar AgОценок пока нет
- Spirometry For Diagnosis of CopdДокумент4 страницыSpirometry For Diagnosis of CopdriasaliОценок пока нет
- SpirometryДокумент11 страницSpirometryTrandafirulNegruОценок пока нет
- Imaging in Chronic Obstructive Pulmonary DiseaseДокумент9 страницImaging in Chronic Obstructive Pulmonary DiseaseHarizОценок пока нет
- COPD Dr. Omnia SaeedДокумент23 страницыCOPD Dr. Omnia SaeedOmnia SaeedОценок пока нет
- Pulmonary FuДокумент24 страницыPulmonary FuIrina Luciana DumitriuОценок пока нет
- Spiro& Peak FlowДокумент21 страницаSpiro& Peak FlowMichael BentonОценок пока нет
- "A Study ON Chronic Obstructive Pulmonary Diseases": Ananta Institute of Medical Sciences and ResearchДокумент13 страниц"A Study ON Chronic Obstructive Pulmonary Diseases": Ananta Institute of Medical Sciences and ResearchHamid RazaОценок пока нет
- Why We Investigate Asthma PatientsДокумент5 страницWhy We Investigate Asthma PatientsustaztОценок пока нет
- PFT Demo: Michael J. Markus M.D. Bsom 2011Документ41 страницаPFT Demo: Michael J. Markus M.D. Bsom 2011lovelyc95Оценок пока нет
- Respiratory System & ParametersДокумент35 страницRespiratory System & Parametersrobert robОценок пока нет
- Capnography in DogsДокумент14 страницCapnography in DogswalczakcОценок пока нет
- Monitoring Mechanical Ventilation Using Ventilator WaveformsОт EverandMonitoring Mechanical Ventilation Using Ventilator WaveformsОценок пока нет
- Aerosols and the Lung: Clinical and Experimental AspectsОт EverandAerosols and the Lung: Clinical and Experimental AspectsStewart W. ClarkeОценок пока нет
- Pulmonary Function Measurement in Noninvasive Ventilatory SupportОт EverandPulmonary Function Measurement in Noninvasive Ventilatory SupportОценок пока нет
- Respiratory Monitoring in Mechanical Ventilation: Techniques and ApplicationsОт EverandRespiratory Monitoring in Mechanical Ventilation: Techniques and ApplicationsJian-Xin ZhouОценок пока нет
- Managing Mediastinitis After Cardiac SurgeryДокумент4 страницыManaging Mediastinitis After Cardiac SurgeryDennis CobbОценок пока нет
- User Training AED ProДокумент46 страницUser Training AED ProDennis CobbОценок пока нет
- Arf Post CabgДокумент19 страницArf Post CabgDennis CobbОценок пока нет
- Trend Management Patient of Transposition Great ArteryДокумент3 страницыTrend Management Patient of Transposition Great ArteryDennis CobbОценок пока нет
- Content 8902 PDFДокумент6 страницContent 8902 PDFabdulОценок пока нет
- Tugas Individu Anggun PDFДокумент6 страницTugas Individu Anggun PDFAnggun PermatasariОценок пока нет
- Treatment of Sternal Wound Infections After Open-Heart SurgeryДокумент6 страницTreatment of Sternal Wound Infections After Open-Heart SurgeryDennis CobbОценок пока нет
- Assessment Constipation PDFДокумент6 страницAssessment Constipation PDFDennis CobbОценок пока нет
- Fluid Afterload After CabgДокумент6 страницFluid Afterload After CabgDennis CobbОценок пока нет
- Post Cardiac ComplicationsДокумент6 страницPost Cardiac ComplicationsGull GillОценок пока нет
- Assessment Constipation PDFДокумент6 страницAssessment Constipation PDFDennis CobbОценок пока нет
- APGARДокумент1 страницаAPGARblazegomezОценок пока нет
- Autonomy of Nurse PDFДокумент8 страницAutonomy of Nurse PDFDennis CobbОценок пока нет
- Transient Ischemic PDFДокумент8 страницTransient Ischemic PDFDennis CobbОценок пока нет
- Avian InfluenzaДокумент6 страницAvian InfluenzaDennis CobbОценок пока нет
- Early Postopcare After Cardiac Surgery PDFДокумент23 страницыEarly Postopcare After Cardiac Surgery PDFDennis CobbОценок пока нет
- ArdsДокумент7 страницArdsIpar DayОценок пока нет
- Avian InfluenzaДокумент6 страницAvian InfluenzaDennis CobbОценок пока нет
- Cognitive Impairment PDFДокумент4 страницыCognitive Impairment PDFDennis CobbОценок пока нет
- Liver Cirrhosis PDFДокумент9 страницLiver Cirrhosis PDFDennis CobbОценок пока нет
- Respiration Disorder PDFДокумент14 страницRespiration Disorder PDFDennis CobbОценок пока нет
- Cardiac ArrhythmiaДокумент5 страницCardiac ArrhythmiaDennis CobbОценок пока нет
- Autonomy of Nurse PDFДокумент8 страницAutonomy of Nurse PDFDennis CobbОценок пока нет
- Heart NotesДокумент13 страницHeart NotesDennis CobbОценок пока нет
- CPR Nurse LawДокумент6 страницCPR Nurse LawIpar DayОценок пока нет
- Marfan's Syndrome Signs and Symptoms: EtiologyДокумент3 страницыMarfan's Syndrome Signs and Symptoms: EtiologyDennis CobbОценок пока нет
- Capillary Blood GlucoseДокумент4 страницыCapillary Blood GlucoseDennis CobbОценок пока нет
- Best Practice in The Use of SpirometryДокумент6 страницBest Practice in The Use of SpirometryDennis CobbОценок пока нет
- Atrial FibrilationДокумент10 страницAtrial FibrilationDennis CobbОценок пока нет
- Avian InfluenzaДокумент6 страницAvian InfluenzaDennis CobbОценок пока нет
- EndophthalmitisДокумент2 страницыEndophthalmitisakillerbeast632Оценок пока нет
- Literature Review On Voluntary Blood DonationДокумент7 страницLiterature Review On Voluntary Blood Donationakjnbowgf100% (1)
- Factors Influencing Consumers ' Buying Behaviours Towards Ayurvedic Products: A Case Study of Patanjali ProductsДокумент16 страницFactors Influencing Consumers ' Buying Behaviours Towards Ayurvedic Products: A Case Study of Patanjali ProductsSiladitya MitraОценок пока нет
- Peplu Theory ApplicationДокумент7 страницPeplu Theory ApplicationVarsha Gurung100% (1)
- With Conviction: Moving AheadДокумент155 страницWith Conviction: Moving Aheadkapadia krunalОценок пока нет
- How Human Microbiome Talks To Health and DiseaseДокумент7 страницHow Human Microbiome Talks To Health and DiseaseRafa SotoОценок пока нет
- Reflection Paper - Behavioral Problems and TypesДокумент2 страницыReflection Paper - Behavioral Problems and TypesFirdaus AbdullahОценок пока нет
- Vit and Hormone in Relation To Growth and Development / Orthodontic Courses by Indian Dental AcademyДокумент38 страницVit and Hormone in Relation To Growth and Development / Orthodontic Courses by Indian Dental Academyindian dental academyОценок пока нет
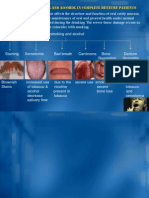
- Effects of Smoking and Alcohol On Complete Denture PatientsДокумент2 страницыEffects of Smoking and Alcohol On Complete Denture PatientsAshwin ThejaswiОценок пока нет
- RCI-CEL-AZA PEME FormA-Rev09-2019 FormB MedCertДокумент8 страницRCI-CEL-AZA PEME FormA-Rev09-2019 FormB MedCertVhal AlbientoОценок пока нет
- ICNCDRS Blindness Registry FormДокумент4 страницыICNCDRS Blindness Registry FormAprilAngeliRobleОценок пока нет
- Aliens & Asteroids - Expansion 02 - More Faces and FactionsДокумент42 страницыAliens & Asteroids - Expansion 02 - More Faces and FactionsJean Dupont100% (1)
- Commercial LawДокумент66 страницCommercial LawBradley MusonzaОценок пока нет
- Benefits of TrekkingДокумент2 страницыBenefits of Trekkinglyka sophia ma-ambongОценок пока нет
- Jurnal GadarДокумент6 страницJurnal GadarLycia Dwi LindiyaniОценок пока нет
- Triamcinolone AcetonideДокумент12 страницTriamcinolone Acetonideawais khanОценок пока нет
- BJGPbookreview Justiceby SandelДокумент2 страницыBJGPbookreview Justiceby SandelEm DeОценок пока нет
- Ammonia SafetyДокумент46 страницAmmonia SafetyMikechal AwacayОценок пока нет
- Safety Plan For Chemical PlantДокумент7 страницSafety Plan For Chemical PlantM Amir Haris100% (1)
- ESICM/ESCMID Task Force On Practical Management of Invasive Candidiasis in Critically Ill PatientsДокумент17 страницESICM/ESCMID Task Force On Practical Management of Invasive Candidiasis in Critically Ill PatientsrennerrsОценок пока нет
- Research Paper FinalДокумент12 страницResearch Paper Finalapi-582867034Оценок пока нет
- Chlamydia SeminarДокумент110 страницChlamydia Seminarsuvarnaramesh2007100% (1)
- Waste ManagementДокумент34 страницыWaste ManagementSivaRamanОценок пока нет
- HSE Covid-19 Doffing CoverallДокумент1 страницаHSE Covid-19 Doffing Coveralliq_dianaОценок пока нет
- Fundamentals of Nursing Part 1Документ8 страницFundamentals of Nursing Part 1Evergreen Verds100% (1)
- MCFP Catalogue 2016Документ33 страницыMCFP Catalogue 2016bader_222_jo50% (2)
- Segmentos Ica 2022 PDFДокумент9 страницSegmentos Ica 2022 PDFRoberto RodríguezОценок пока нет
- MIP17 - HSE - PP - 001 Environment Management Plan (EMP) 2021 REV 3Документ40 страницMIP17 - HSE - PP - 001 Environment Management Plan (EMP) 2021 REV 3AmeerHamzaWarraichОценок пока нет
- Computer Forensics As A Part of A Security Incident Response ProgramДокумент32 страницыComputer Forensics As A Part of A Security Incident Response ProgrammanojОценок пока нет
- BinderДокумент13 страницBinderisabel carreauОценок пока нет