Академический Документы
Профессиональный Документы
Культура Документы
Retroperit. Pelvis & Perineum - PPT - Compatibility Mode
Загружено:
Mignot AnileyИсходное описание:
Оригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Retroperit. Pelvis & Perineum - PPT - Compatibility Mode
Загружено:
Mignot AnileyАвторское право:
Доступные форматы
1/8/2011
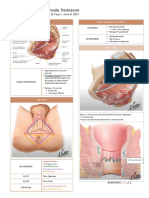
RETROPERITONEUM AND PELVIS-PERINEUM
THE PELVIC WALL
Pelvis lies inferoposterior to the abdomen Connects the trunk to the lower limb Pelvis is anatomically bounded by bony girdle The bony pelvis is formed by 4 bones 1. two hip bones (coxal bones) 2. one sacral bones 3. one coccygeal bone The bones are connected by 4 joints - two sacroiliac joints - one pubic symphysis - one sacrococcygeal joint Femur & vertebral bones are connected to this bony ring 2
1/8/2011
Cont.
Pelvic girdle gives the following functions: 1. bear weight of upper body when sitting & standing 2. transfer weight from axial to lower appendicular skeleton 3. provide attachment for muscle 4. contain & protect the pelvic viscera 5. provide attachment for erectile bodies of external genitalia The pelvis is divided into two parts by superior pelvic aperture
1. Upper part (Greater or False) pelvis
- expanded part of pelvis above pelvic brim - lie superior to the pelvic inlet - spreading wing of ilium forms its lateral wall - contains more of abdominal 4viscera
1/8/2011
Cont.
- boundaries of greater pelvis ! laterally:- wings of ilium ! posteriorly:- upper part of sacrum ! anteriorly:- lower abdominal wall 2. Lower part (Lesser or True) pelvis - inferior & posterior to the pelvic brim - formed by part of ilium, pubis, ischium, sacrum & coccyx - contains the pelvic viscera - lie b/n pelvic inlet & pelvic outlet
5
1/8/2011
Cont.
Pelvic inlet (sup. pelvic aperture or pelvic brim) is bounded by - posteriorly:- sacral promontory & ala of sacrum - laterally:- arcuate line of ilium & iliopectine eminence - anteriorly:- pectineal line, pubic crest & upper border of symphysis pubis Terminal line is extending from sacral promontory to upper border of symphysis pubis Pelvic cavity lie b/n the two apertures
7
Cont.
Pelvic outlet (inferior pelvic aperture) is closed by pelvic floor consisting of pelvic and urogenital diaphragms Lesser pelvis has inlet, cavity & outlet Boundaries of pelvic outlet include: ! posteriorly:- coccyx ! laterally:- ischial tuberosity
! anteriorly:- pubic arch & symphysis
8
1/8/2011
Pelvic Wall
Wall of pelvis has three planes or layers: external, intermediate & internal External plane or layer is formed by gluteal muscles Intermediate plane is composed of: - bones (hipbone, sacrum & coccyx) - ligaments (sacrotuberous & sacrospinous ligaments) - membranes (obturator membrane) Internal plane is formed by:
- muscles & fascia attached to intermediate plane by the peritoneum - blood vessels, lymphatic vessels & nerves - structures b/n peritoneum & fascial coverings of muscles
10
1/8/2011
1. Anterior wall ! formed by: - body & rami of the pubic bones 2. Lateral wall ! formed by: - right & left hip bone
- obturator membrane - obturator & pelvic fascia - pubic symphysis
Pelvic cavity has anterior, lateral, posterior walls & floor
3. Posterior wall
! formed by:- sacrum & coccyx - associated joints & ligaments - piriformis & coccygeus muscles & their fascia
4. Floor:- formed by peritoneum & pelvic diaphragm
- support abdominal & pelvic viscera
11
12
1/8/2011
" Composed of three separate bones in infants & children
Hip (Pelvic) Bone
" The three bones are separated by Y-shaped cartilage at the acetabulum called triradiate cartilage " After puberty the separating cartilage is ossified " B/n ischium & pubis, there is large opening called obturator foramen
" Obturator foramen is covered by obturator membrane except upper part with small opening (obturator canal) for the passage of obturator vessels & nerves " The lateral cup-like part of hip bone that articulates with the head of femur is called acetabulum 13
14
1/8/2011
Acetabulum
Cup or socket for the head of femur Formed by bodies of ilium & ischium & superior pubic ramus Acetabulum has two parts: 1. lunate area:- smooth half moon shaped articular area - covered by articular hyaline cartilage 2. acetabular fossa:- nonarticular depression Surrounded by prominent bony margin called limbus acetabuli except inferior 1/3rd margin Inferiorly it has a notch called acetabular notch The notch is bridged by transverse acetabular ligament This notch is traversed by vessels supplying the joint the ligament is continuous with acetabular labrum
15
16
1/8/2011
Ilium
# Superior fan-shaped part of the hip bone # The ala or wing of ilium represents the spread of the fan # The body is the handle of the fan # Has two principal parts: 1. Body:- participate in the formation of superior acetabulum - medially separated from ala by curved ridge called arcuate line 2. Wing (ala):- form major upper expanded part of hip bone # Ilium has three surfaces: 1. Gluteal or lateral surface:- marked by three curved gluteal lines radiating from margin of greater sciatic notch - three lines are: posterior, anterior & inferior gluteal lines
17
Cont.
2. Pelvic (medial) surface - contains iliac fossa & arcuate line - iliac fossa is a depression on the medial surface of ala - arcuate line is iliac part of terminal line and ends at the iliopubic eminence 3. Sacral surface - has two parts: i. Auricular part:- flat surface articulating with sacrum ii. Preauricular sulcus:- located anterior & below articular surface - found only in females
18
1/8/2011
19
Iliac crest
Superior free border of ilium The highest point reaches up to L4 spinous process On its anterior 2/3rd part, it has the following parts: 1. Outer lip:- posterior 1/3rd serve as origin of latissmus dorsi - anterior for insertion of external oblique ms. 2. Inner lip:- serve as origin of transverse abdominis muscle 3. Intermediate line:- serve as origin of internal oblique Has the following projections on the crest a. tubercle of iliac crest:- projection on outer lip behind anterior superior iliac spine b. anterior superior iliac spine - lie on anterior border of iliac crest 20 - sartorius, tensor fascia lata & inguinal lig. attach on it
10
1/8/2011
Cont.
c. posterior superior iliac spine - projection at the posterior end of the iliac crest d. iliac tubercle - expanded rough surface behind posterior sup. iliac spine - iliolumbar & sacroiliac ligaments are attached Has the following projections below the crest i. Anterior inferior iliac spine - serve as origin of rectus femoris muscle ii. Posterior inferior iliac spine - lie above the greater sciatic notch
21
22
11
1/8/2011
# Has two major parts: 1. Body:- forms posteroinferior part of acetabulum - has ischial spine for attachment of sacrospinous lig. - has ischial tuberosity for origin of hamstring muscles 2. Ramus:- inferior curved part # Has lesser sciatic notch b/n ischial spine & ischial tuberosity
23
Ischium
- continuous with inferior ramus of the pubic bone
Pubis
" Angulated bone & has three parts: 1. Body:- found b/n superior & inferior rami - body of rt & lt parts join at the symphysis pubis - superior border forms proximal ridge called pubic crest - pubic crest extend laterally & end at pubic tubercle
24
12
1/8/2011
Cont.
2. Superior ramus - lie lateral to the tubercle - extend to form part of acetabulum - at the junction with ilium it forms iliopubic eminence - lateral part of superior ramus has oblique ridge called the pecten pubis (pectineal line) - pectineal line serve as origin of pectineus muscle - anterior border forms obturator crest 3. Inferior ramus - attached to body medially & to ischial ramus laterally to form ischiopubic ramus - bounds the inferomedial margin of obturator foramen - form pubic arch (subpubic angle)
25
26
13
1/8/2011
Differences b/n Male & Female Hipbones
Bony pelvis General structure Greater pelvis Lesser pelvis Pelvic outlet Pubic arch Males Thick & heavy Deep Narrow, deep, tapering Comparatively small Narrow (< 700) Females Thin & lighter Shallow Wide, shallow, cylindrical Comparatively large Wide (> 800) Oval Small Almost 900 Less Less curved inward
27 Infront of auricular surface
Obturator foramen Round Acetabulum Large Great sciatic notch Narrow (~ (~700) DA vs AA-SP Ischial spine Preauricular sulci Equal Highly curved inward absent
28
14
1/8/2011
29
A. Female pelvis B. Male pelvis
30
15
1/8/2011
Joints & Ligaments of the Pelvis
1. Pubic Symphysis
Secondary cartilagenous joint Has a fibrocartilagenous interpubic disc At the center of the disc there is fluid filled symphyseal cavity The interpubic disc is wider in females Has two ligaments to hold bones together i. Superior pubic ligament - connect superior aspect of pubic bodies & interpubic disc - extend laterally up to the pubic tubercles ii. Inferior (arcuate) pubic ligament - extend b/n inferior rami 31 of right & left pubic bone
32
16
1/8/2011
Cont.
2. Sacroiliac Joints
Strong weight-bearing synovial joint Formed by auricular surface of sacrum & ilium Has limited mobility Has the following ligaments i. Iliolumbar ligament:- lie b/n costarius process of 4th & 5th lumbar vertebrae & ilium ii. Anterior sacroiliac ligament - occur b/n pelvic surface of sacrum & ilium iii. Posterior sacroiliac ligament - lie b/n dorsal surface of sacrum & ilium
33
34
17
1/8/2011
Cont.
iv. Interosseous sacroiliac ligament - b/n tuberosities of sacrum & ilium v. Sacrospinal ligament - extend from lateral sacrum & coccyx to ischial spine - subdivide large sciatic foramen into greater & lesser sciatic foramina vi. Sacrotuberous ligament - pass from posterior ilium, lateral sacrum and coccyx to ischial tuberosity - cross over the sacrospinal ligament - serve as origin of gluteus maximus muscle - transform sciatic notch of hipbone to large sciatic foramen 35
36
18
1/8/2011
37
Pelvimetry
#It is measurement of pelvic diameter #Important in gynaecology & obstetrics for delivery #Measurable diameters could be internal & external
1. Internal Pelvic Measurements
! could be measured at the pelvic inlet, outlet & pelvic cavity A. Pelvic Inlet Measurements 1. Conjugate (anteroposterior) diameter - it is about 11cm long - d/nce b/n sacral promontory & symphysis pubis 2. Transverse diameter:- about 13.5cm long - longest diameter of the pelvic inlet 3. Oblique diameter:- about 12.5cm long - extend from sacroiliac joint to opposite iliopubic emenence
38
19
1/8/2011
39
B. Pelvic Cavity Measurements 1. Anteroposterior diameter:- about 12cm long - from lower border of symphysis pubis to S4 vertebra 2. Transverse (Interspinous) diameter:- about 10.5cm long - the difference b/n two ischial spines - it is the shortest diameter in the pelvis C. Pelvic Outlet Measurements 1. Transverse diameter:- about 11cm long - d/nce b/n two ischial tuberosities 2. Diameter recta:- about 9cm long
- extend from lower border of symphysis pubis to tip of coccyx - this diameter can increase b/c of mobility of coccyx - it can reach up to 11cm during delivery
40
20
1/8/2011
41
2. External Pelvic Measurements
a. Interspinal distance - it is about 24-26cm long - d/nce b/n right & left anterior superior iliac spines b. Intertrochanteric distance - about 31-32cm long - d/nce b/n right & left greater trochanters of femur c. External conjugate diameter - about 18-21cm long on the outer part
- lie b/n upper border of symphysis pubis & spinous process of L4
d. Intercristal distance - it is about 28-29cm long - it is the longest distance b/n the iliac crests
42
21
1/8/2011
# According to Caldwell and Moloy, there are 4 types female pelvis 1. Gynecoid pelvis: - found in 41-44% of females - typical female pelvis - transeverse diameter > anteroposterior diameter - subpubic arch ~ 900 2. Android pelvis:- male like pelvis - found in 23-32% of the females - funnel-shaped pelvis - the pelvic inlet is heart-shaped - has smaller pelvic cavity - subpubic arch ~ 700
43
Types of Pelvis
44
22
1/8/2011
Cont.
3. Antropoid pelvis: - ape like pelvis - found in 23-28% of the females - long, narrow & oval in shape - pelvic inlet has long anteroposterior diameter & short transverse diameter 4. Platypelloid (flat) pelvis - found in about 2-5% of the females - wide pelvis, flattened at pelvic inlet - has short anteroposterior diameter - has wide subpubic arch - delivery is difficult in this type of pelvis 45
46
23
1/8/2011
# According to Greulich & Thoms, female pelvis can be classified into 4 types as: i. Dolicopellic (long) pelvis:
Cont.
- anteroposterior diameter is greater than transverse diameter ii. Mesatipellic (round) pelvis:- transverse diameter is greater than the anteroposterior diameter (by 0-1cm) iii. Brachypellic (oval) pelvis:- transverse diameter is greater than anteroposterior diameter by 1-3cm iv. Platypellic (flat) pelvis:- transverse diameter is greater than anteoposterior diameter by 3cm or more
47
$ Retroperitoneal Space $ Pelvic Cavity $ Perineum
48
24
1/8/2011
" A pair of endocrine glands " Situated on the posterior abdominal wall " Lie superior to kidneys behind the peritoneum " Yellowish brown in color b/c of lipoid substance " Each gland lies in front of crus of the diaphragm " Size - height 30 to 50 mm - breadth 30 mm - thickness 10 mm " Shape - Rt gland is pyramidal or in shape - Lt gland is semi-lunar in shape
49
THE SUPRARENAL GLANDS
50
25
1/8/2011
" Weight is about 5 g, medulla forms 1/10th of the gland " Each gland consist of two parts: 1. Cortex:- mesodermal in origin
Cont.
" B/n the two glands, the following structures are situated - crura of diaphragm - aorta (abdominal part) - celiac trunk - celiac plexus - inferior vena cava
51
2. Medulla:- developed from neural crest
Relations of Suprarenal Gland
Right Suprarenal Gland Posteromedially:- diaphragm Anteromedially:- IVC Anteriorly:- Rt lobe of liver Inferiolaterally:- Rt kidney Superiorly:- bare area of the liver Left Suprarenal Gland Posteriorly:- diaphragm Anteriorly:- stomach with - lesser sac & pancreas - splenic artery Inferiolaterally:- Lt kidney
52
26
1/8/2011
Structure of the Suprarenal Glands
Each gland is enclosed by tough connective tissue capsule Fresh glands show two distinct regions: 1. external cortex:- major part, secrete steroid hormones 2. internal medulla:- secrete adrenalin & noradrenalin These regions are also distinct: - embryologically - structurally - functionally Each gland is enclosed in renal fascia but separated from the kidneys by fibrous tissue
53
54
27
1/8/2011
Arterial supply of the suprarenal glands 1. Superior suprarenal arteries:- from inferior phrenic aa 2. Middle :- from abdominal aorta 3. Inferior :- from renal arteries Venous drainage of the suprarenal glands % Rt suprarenal vein:- drain into IVC % Lt :- drain into the left renal vein Lymphatic drainage of the suprarenal glands %drain into lateral aortic (superior lumbar) lymph nodes Innervation of the suprarenal glands & celiac plexus & greater splanchnic nerves
55
Clinical Conditions
Addisons disease:- muscular weakness, low BP, anemia, Cushings syndrome:- obesity, excess hairiness of face & In women, musculinization (virilism) may occur due to excessive androgenic hormones electrolyte imbalance etc
trunk, diabetes mellitus, impotence etc
Children may show precocious body growth & devt of external genital organs with early menstruation in girls In female fetus may lead to pseudohermaphroditism (excess of androgen interferes & leads to large clitoris (resemble mens penis)
56
28
1/8/2011
# A pair of excretory organs # Lie one on each side of the vertebral column # Retroperitoneal organ # Extend from T12 to L3 or L1 to L4 in erect position # Rt kidney is slightly lower in position b/c of the liver # Function: 1. remove excess water & salt 2. excrete products of protein metabolism 3. maintain the pH of the blood # The transpyloric plane passes through: - the upper part of hilum of rt kidney - the lower part of hilum of lt kidney
57
THE KIDNEYS (RENES)
58
29
1/8/2011
# Each kidney lies in a mass of perirenal (perinephric) fat # Each kidney has two poles: ! superior pole:- nearer to the median plane ! inferior pole:- pointed part # Each kidney has two surfaces: ! anterior surface ! posterior surface # Each kidney has two borders: ! lateral border:- convex in shape
59
Cont.
! medial border:- convex at both ends & concave at hilum
# The renal sinuses are located in the hilum of the kidney # The human fetal kidney has up to 21 lobes
Cont.
# The human adult kidney usually lacks external lobation # Adult fresh kidneys are reddish-brown in color # The upper end of the kidney is slightly thicker # Each kidney measures: ! 11 cm in length ! 6 cm in width
# The lower end is about 1 inch above the iliac crest
! 3 cm in thickness
60
30
1/8/2011
#On average each kidney weighs: ! 150 g in adult males ! 135 g in adult females
Cont.
#The left kidney is often slightly longer than the right one #Nephrectomy:- surgical removal of kidney #Redundance:- enlargement of one kidney due to functional overload
61
#The structures at the hilum are arranged as follows:
1. renal vein:- anterior 2. renal artery:- intermediate 3. pelvis of the kidney:- posterior How to Identify each Side of the Kidney 1. hilum is medial in position 2. renal vessels are anterior to the pelvis 3. ureter is directed inferiorly
62
Cont.
31
1/8/2011
63
Functions of the Kidney
1. Excretion of metabolic waste products & excess water 2. Maintain fluid & electrolyte balance in the tissue fluid 3. Maintain the pH of blood 4. Endocrine function: formation
! production of erythropoietin that influence RBC
! formation of renin to regulate BP through control of
! formation of 1,25-hydroxycholecalciferol (Ca++
fluid & electrolyte
regulation by modification of action of parathormone)
64
32
1/8/2011
Occupies the renal sinus
Pelvis of the Ureter
Divided into 2-3 major calyces
Each major calyx is divided into 7-14 minor calyces Each minor calyx terminates by nipple like indentation called renal papilla This perforated area is called area cribrosa
65
Renal papilla is perforated by papillary ducts
66
33
1/8/2011
67
" Each kidney is closely invested by strong fibrous capsule " Capsule is embedded in the substantial mass of perirenal fat " Perirenal fat & capsule constitutes a fatty renal capsule ! there is less fatty tissue anteriorly
Renal Fascia and Renal Fat
" The fatty renal capsule is in turn covered by fibroareolar tissue called the renal fascia
68
! the amount of this fat varies with the individuals
34
1/8/2011
" Renal fascia encloses: ! kidney
Cont.
! surrounding fibrous & fatty capsules " The coverings help kidneys to be maintained in position ! suprarenal gland
69
" The renal fascia is continuous:
Cont.
! Superiorly:- with diaphragmatic fascia
! Medially:- left & right sides blend with each other anterior to the abdominal aorta & IVC " The extraperitoneal fat outside the renal fascia (pararenal fat) is located b/n the peritoneum of the posterior abdominal wall and the renal fascia
70
! Posteriorly:- fuses with psoas major fascia
35
1/8/2011
Relations of the Kidney
Posterior Relations
1. Diaphragm 2. Quadratus lumborum 3. Poas major 4. Transversus abdominis 5. Subcostal vessels 6. Subcostal nerve 7. Iliohypogastric nerve 8. Ilioinguinal nerve 9. 12th rib (right kidney) 11th & 12th ribs (left kidney)
71
Posterior relations of kidneys
72
36
1/8/2011
Anterior Relations
Right Kidney
1. Right suprarenal gland 2. 2nd part of the duodenum 3. Right lobe of the liver 4. Right colic flexure 5. Coils of small intestine (jejunum)
73
Left Kidney
1. Left suprarenal gland 2. Spleen 3. Stomach 4. Pancreas (body) 5. Descending colon 6. Left colic flexure 7. Coils of jejunum 8. Splenc vessels (artery)
Anterior Relations of Kidneys
74
37
1/8/2011
Each kidney has two parts: outer (cortex) & inner (medulla) Renal medulla consists of 10-18 conical or pyramidal structures called the medullary pyramids From the base of each pyramids, parallel arrays of tubules called medullary rays penetrate the cortex Each medullary ray consists of one or more collecting tubules together with straight portions of several nephrons Mass of cortical tissue surrounding each medullary pyramid is a renal lobe Each medullary ray forms the center of a conical renal lobule The area b/n two pyramids is 75 called renal column of Bertin
Microscopic Structures of the Kidney
76
38
1/8/2011
Blood Circulation of the Kidney
Renal artery Segmental artery Lobar artery
Interlobular artery
Arcuate artery
Interlobar artery
Afferent arteriole
Glomerulus (capp)
Efferent arteriole
Arcuate vein Interlobar vein
Interlobular vein Renal vein 77
Peritubular capp + vasa recta
78
39
1/8/2011
Lymphatic Drainage of the Kidney
lymph vessels of the kidney follow the renal vein & drain into the lumbar (lateral aortic) lymph nodes
Innervation of the Kidneys
Nerve to the kidneys come from the renal plexus
Consist of sympathetic and parasympathetic fibers
This plexus is supplied by fibers from the lesser and lowest splanchnic nerves
79
Rapid excessive distention of the ureter causes severe rhythmic pain called ureteric colic (frequently the pain results from a kidney stone) It is known as ureteric calculus Calculi may be located in the calices, renal pelvis, ureter or urinary bladder Ureteric colic is a sharp pain following the course of the ureter Kidney stones can be removed in three ways: 1. open surgery 2. precutaneous surgery:- by the help of nephroscope 3. lithotripsy 80
Clinical Correlations
40
1/8/2011
THE URETER
Narrow, thick walled muscular tube Convey urine from the kidney to the urinary bladder Retroperitoneal organ through out its length Begins within the renal sinus as a renal pelvis, which gradually narrow to become ureter As urine passes, peristaltic waves occur in their walls Each ureter is a tubular organ, 25 cm long & 5 mm wide Half of the ureter length lies in the abdominal part thickest portion is near the entrance of urinary bladder ~ 10 mm 81
82
41
1/8/2011
Relations of the Ureter
Right Ureter
Anteriorly:- renal vessels - 2nd & 3rd part of duodenum - peritoneum - rt colic vessels, ileocolic vessels, gonadal vessels - root of mesentry Posteriorly:- psoas major muscle - tips of transverse processes - genitofemoral nerve Medially:- IVC
83
84
42
1/8/2011
Left Ureter
Anteriorly:- renal vessels - peritoneum - pancreas & jejunum - lt colic vessels & lt gonadal vessels - sigmoid colon & sigmoid mesocolon Posteriorly:- psoas major muscle - tips of transverse processes - genitofemoral nerve Medially:- lt gonadal veins - inferior mesenteric vein
85
Arterial Supply of the Ureters
Abdominal part
- renal arteries - gonadal arteries - aorta - iliac arteries (common & internal iliac)
Pelvic part
- vesical arteries (superior & inferior) - middle rectal arteries - uterine arteries
86
43
1/8/2011
Venous Drainage of the Ureters
! Testicular veins ! Ovarian veins
Lymphatic Drainage of the Ureters
! Middle part:
! Superior part:- drain into lumbar (lateral aortic) LN ! Inferior part: common iliac LN common iliac, external or
internal iliac LN
Innervation of the Ureters
! Renal plexus:- consist of symp. & parasymp. fibers
' Ovarian or inferior hypogastric plexus
87
Normal Constrictions of the Ureter
1. At the pelvi-ureteric junction 2. At the brim of the lesser pelvis 3. At its passage through the bladder wall
88
44
1/8/2011
Microscopic Structures of the Ureter
The wall of the ureter consists of three layers: 1. mucosa 2. muscularis 3. adventitia Mucosa:- consist of transitional epithelium - cells produce mucus with a protective film Muscularis:- consist of inner (longitudinal) & outer (circular) layer of smooth muscles - proximal 1/3rd of ureter contain another longitudinal layer externally - produce peristaltic movt of urine Adventitia: - composed of loose fibrous CT 89 ureter in place - help to anchor
90
45
1/8/2011
91
THE URINARY BLADDER
! a muscular reservoir of urine ! in adults the empty bladder lies in the pelvic minor ! lies posterior to symphysis pubis & anterior to the rectum ! in females it is in contact with the uterus & vagina ! in males prostate gland is located below it ! the shape is determined by the volume of urine ! empty bladder is pyramidal in shape ! it has the following parts: 1. apex 2. base or fundus 92 3. neck
46
1/8/2011
93
! Apex:- is directed anteriorly ligament (fibers of embryonic urachus) ! Base (fundus) - lie posteriorly - in females, related to uterine cervix & vagina - in males, upper part separated from rectum by ' lower part related to seminal vesicle & vas deferens
94
Cont.
- connected to the umbilicus by median umbilical
retrovesical pouch (containing coils of intestine)
47
1/8/2011
Cont. ! Neck - lie 3-4cm behind lower part of symphysis pubis - pierced by the internal urethral orifice - in males it rests on the base of prostate - in females, it is related to pelvic fascia
95
96
48
1/8/2011
Surfaces of the Urinary Bladder
( In living persons, the bladder always contains urine and is usually more or less rounded ( When bladder is filled it holds maximum of 500 cc of urine ( Mean vesical capacity varies 120-320 cc (micturition mostly occurs at 280 cc) ( Empty bladder has four surfaces:
1. Superior surface:- the only part covered by peritoneum 2. Inferiolateral surfaces:- related to retropubic fat 3. Posterior surface
97
( The area of mucus membrane covering the internal surface of the base of bladder is called trigone
Cont.
( Mucus membrane in trigone is always smooth even when empty b/c it is firmly adherent to the underlying muscular coat (it lacks rugae)
98
49
1/8/2011
99
( The trigone is limited above by a muscular ridge which runs from the opening of one ureter to the ( That ridge is known as the interureteric ridge immediately behind the urethral orifice lobe of the prostate gland
100
Cont.
other
( The uvula vesicae is a small elevation situated ( The uvula is produced by the underlying median
50
1/8/2011
101
102
51
1/8/2011
Arterial Supply of the Urinary Bladder
! Superior vesical artery ! Obturator artery ! Inferior vesical artery (in males) ! Inferior gluteal artery
! Uterine & vaginal arteries (in females)
Venous Drainage of the Urinary Bladder
iliac veins
103
! Vesicular venous plexus empties into the internal
Lymphatic Drainage of the Urinary Bladder
External iliac LN:- from superior part Internal iliac LN:- from inferior part Sacral or common iliac LN
Innervation of the Urinary Bladder
Parasympathetic fibers:- from pelvic splanchnic nn (S2,S3 S4) - motor to detrusor muscle - inhibitory to the internal sphincter - when the fibers are stimulated the bladder will contract, the sphincter relax & urine flow into the urethra Sympathetic fibers:- derived from T11, T12, L1 & L2 nerves - inhibitory to the bladder Vesical nerve plexus continues to inferior hypogastric plexus
104
52
1/8/2011
Newborn urinary bladder
Adults urinary bladder
105
The wall of the urinary bladder consists of four layers: 1. Mucosa:- composed of transitional epithelium - further distention is permitted by folds of mucosa called rugae - fleshy flaps of mucosa help to prevent back flow of urine 2. Submucosa:- supports mucosa 3. Musculars:- consist of three interlaced smooth muscle layers & is referred as detrusor muscle - at the neck the muscle forms internal sphincter - three layers: inner & outer (long.), middle (circ) 4. Adventitia:- continuation of a peritoneum - appear only on106 the superior surface
Microscopic Structures of the Urinary Bladder
53
1/8/2011
Transverse section of urinary bladder Massons trichome stain
107
108
54
1/8/2011
Ligaments of the Urinary Bladder
Pubovesical ligaments: of the pubic bone the umbilicus
Median umbilical ligament:- attach apex of bladder to
- extend from the bladder neck to the inferior aspect - the two pubovesical ligaments lie one on each side of the median plane - constitute the upper extensions of the: ! puboprostatic ligaments in males
109
! pubourethral ligaments in females or
Clinical Correlations
A urinary bladder infection is called cystitis Cystitis is more common in females because womens urethra is much shorter than males An infection that involves the renal pelvis is called pyelitis
If the infection continues to the nephron, it is known as pyelonephritis
110
55
1/8/2011
URETHRA
MALE URETHRA
Long muscular tube Measures 15 to 20 cm long Extends from internal orifice to external opening Conveys urine & semen to the outside of the body Has a double curve while the penis is in its flaccid state Has preprostatic part, approximately 1 cm long Divided into three basic parts: 1. prostatic urethra 2. membraneous urethra 3. spongy or penile urethra 111
112
56
1/8/2011
113
" First part of urethra, about 3 cm long " Start at the apex of the trigone
1. The Prostatic Urethra
" Begins around the internal urethral orifice " Passes through the prostate gland
" The widest & dilatable part of urethra
" The mucosa on the posterior wall presents a median ridge known as the urethral crest
" The lumen is narrower superiorly & inferiorly than in the middle
" On each side of the urethral crest, there is a groove called prostatic sinus
114
57
1/8/2011
" Most of the prostatic ductules open into prostatic sinuses
Cont.
" About middle of the gland, urethral crest forms rounded elevation known as colliculus seminalis (verumontanum) " Collicular opening lead to blind ended pouch called prostatic utricle (about 5 mm)
" Prostatic utricle is homologous with uterus or vagina of females " On each side of the orifice of the prostatic utricle is the minute opening of an ejaculatory duct " Prostatic utricle is vestigial remnant of uterovaginal canal 115
( Second part of urethra (about 1.5 to 2 cm)
2. Membranous Urethra
( The shortest, thinnest & narrowest portion of urethra
( Begins at the apex of prostate & ends at the bulb of penis ( Pierces the perineal membrane 2.5 cm below & behind pubic symphysis ( Surrounded by sphincter urethra muscle ( Skeletal muscles form external urethral sphincter
( Posterolateral to the membraneous urethra, on each side is the bulbourethral glands ( Lie between two membranes (pelvic fascia & perineal membrane) 116
58
1/8/2011
3. The Spongy Urethra
!The longest part of urethra (15 to 16 cm long) !Passes through bulb of the penis & corpus spongiosum !Ends at external urethral orifice (extreme narrowest part) !Lumen is about 5mm in diameter but has two expansions: 1. In the bulb of a penis to form intrabulbar fossa (fossa terminalis) 2. In the glans penis to form the navicular fossa !On each side in the proximal part, duct of bulbourethral gland (Cowper s gland) opens
! There are small duct openings of mucus secreting ureth. glds ' any instrument that pass through external urethral 117the bladder orifice can easily reach to
118
59
1/8/2011
Arterial Supply of the Male Urethra
! Arteries of the prostate:- prostatic part ! Arteries of bulb & urethral arteries:- supply distal part
Venous Drainage of the Male Urethra
! follow the arteries & have similar names
Innervation of the Male Urethra
! branches of pudendal nerve ! most afferent fibers from urethra run to pelvic splanchnic nn ! nerves from prostatic plexus, arise from inf. hypogastric plexus are distributed to all parts of urethra ! sacral, internal iliac & inguinal lymph nodes 119
Lymphatic Drainage of the Male Urethra
Microscopic Structures of Male Urethra
The prostatic urethra is lined by transitional epithelium Membranous urethra is lined by stratified or pseudostratified columnar epithelium Surrounding this part is sphincter urethra by straited muscles Bulbous & pendulous parts of urethra are located in the corpus spongiosum Epithelium of penile urethra is pseudostratified columnar with stratified & squamous areas Littres glands are mucous glands found along the entire length of urethra 120
60
1/8/2011
Pseudostratified epithelium from male urethra; H & E stain
121
FEMALE URETHRA
Short muscular tube Measures about 4 to 5 cm long & 6 mm in diameter Superior half corresponds to prostatic urethra & inferior half to membranous urethra in males Wider & more dilatable than the male urethra Mid-part is surrounded by an external straited voluntary sphincter Begins at the internal urethral orifice at the neck of the bladder & descends downward & forward
122
61
1/8/2011
Cont.
Traverses the deep & superficial perineal pouches Open into the vestibule in front of the vaginal orifice Urethral glands are found in the superior part These group of glands on each side called paraurethral glands (of Skene) are homologous to the prostate Paraurethral glands have a common paraurethral duct
123
Microscopic Structures of Female Urethra
(Epithelium lined with stratified squamous epithelium and areas of pseudostratified columnar epithelium (Wall of female urethra comprises outer muscle coat & inner mucous membrane (The muscle coat contains outer sleeve of straited muscle (external urethral sphincter) together with an inner coat of smooth muscles
124
62
1/8/2011
Congenital Malformations of the urinary System
1. Renal agenesis:- unilateral absence of kidney 2. Renal ectopia:-one or both kidneys are in abnormal position 3. Horseshoe kidney:- fusion of kidneys across the midline 4. Unilateral double kidney 5. Pelvic kidney 6. Rosette kidney 7. Aberrant renal artery:- causing urinary obstruction 8. Polycystic kidney 9. Duplication of ureters 10.Exstrophy of bladder:- protrusion of posterior bladder wall 11.Hypospadias 12.Epispadias 13.Accessory kidneys:- more than two kidneys 14.Lobated kidneys 125
Symptoms and Diagnosis of Urinary Disorders
( Dysuria:- painful urination ( Hematuria:- blood in the urine ( Pyuria:- pus in the urine
( Bacteriuria:- bacteria in the urine ( Oligouria:- scanty output of urine
( Polyuria:- excessive output of urine accumulates in the blood
126
( Uremia:- substances ordinarily excreted in the urine ( Enuresis or incontinence:- inability to control micturation
63
1/8/2011
GENITAL ORGANS
127
MALE GENITAL ORGANS
# Primary sex organs include:- testes which produce:- gametes (spermatozoa) - sex hormones # Secondary sex organs include:- epididymes - ductus deferentia - ejaculatory ducts - penis (urethra) - accessory glands:- which in turn includes:! prostate gland ! bulbourethral gland ! seminal vesicles - scrotum:- pouch of skin 128
64
1/8/2011
" Paired ovoid organs " Have elastic consistency " Suspended in the scrotum by spermatic fascia " Whitish organs that produce spermatozoa & sex hormones " Each testis is about 4cm long, 25g weight & 2.5cm in diameter " Left testis is usually lie in the lower position " Left testis is the first to descend " Right testis is heavier than the left " Each testis has: - superior and inferior ends - flattened medial and lateral surfaces - anterior and 129 posterior borders
The Testis
130
65
1/8/2011
Coverings of the Testis
1. Scrotum:- external covering of skin with no fat but rich in sebaceous glands 2. Tunica dartos:- smooth muscle containing subcutaneous tissue 3. External spermatic fascia:- covers the cremaster muscle - extension of superficial fascia of abdominal muscles 4. Cremaster muscle:- continuation of internal oblique and transversus abdominis muscle
131
5. Internal spermatic fascia:- continuation of transversalis fascia 6. Tunica vaginalis: - peritoneal fold entered during testis descent - has two layers 1. outer parietal layer forms periorchium 2. inner visceral layer forms epiorchium
Cont.
Between the two layers of tunica vaginalis is the scrotal cavity which contains a serous fluid
If there is excess fluid accumulation we call it hydrocele
132
66
1/8/2011
133
Cont.
Right & left testes are separated by scrotal septum (CT) The scrotal raphe (septum) is visible on the skin
Appendix testis
- remnant of Mullerian duct (paramesonephric duct) - found on the upper pole - homologous to fimbriae of oviduct
Appendix epididymidis
- remnant of mesonephric duct (Wolffian) duct - lie on the head of epididymis
134
67
1/8/2011
135
136
68
1/8/2011
Arterial Supply of the Testes
! Testicular arteries ! Inferior vesical artery
Venous Drainage of the Testes
- Rt testicular vein:- drain to IVC
! Testicular vein:- from pampiniform plexus of veins - Lt testicular vein:- drain to left renal vein
' If testicular valves are insufficient it causes dilation of the venous plexus which results varicocoele (this occurs most on the left side about 80%)
137
Lymphatic Drainage of the Testes
! Lumbar (para-aortic) lymph nodes ! Aortic lymph nodes
Innervation of the Testes
! Genitofemoral nerve ! Testicular plexus
! Posterior scrotal nerve (This is vasomotor)
! Sympathetic fibers from T10
138
69
1/8/2011
Microscopic Structures of the Testis
( Testis is surrounded by thick capsule called tunica albuginea ( Under tunica albuginea there is loose layer of CT rich in blood vessels called the tunica vasculosa. ( The tunica albuginea is thickened on the posterior surface to form the mediastenum testis.
( Fibrous septa penetrates the gland and divide into 250 pyramidal compartments called testicular lobules
( Testicular lobules are triangular in shape (apex directed to the mediastinum)
139
( Each lobule consist of 2-4 coiled tubules called seminiferous tubules ( Seminiferous tubules:
Cont.
- have 30-70cm length; 150-250 m in diameter - produce male reproductive cells - at the termination the lumen narrows and continuous as a short segment called straight tubules (tubuli recti)
140
70
1/8/2011
141
( Tubuli recti connect seminiferous tub. to rete testis
Cont.
( The rete present in the CT of mediastinum is connected to the cephalic portion of epididymis by ductuli efferents ( Ductuli efferents are 10-20 in number & 20cm length
( Efferent ductuli after leaving mediastinum take tortuous course & surrounded by CT fiber to form the conus vasculosus of head of epididymis
142
71
1/8/2011
( Seminiferous tubules have: - a tunic of fibrous CT - well defined basal lamina
Cont.
( An outer capsule (tunica propria):- consist of several ( Basal lamina consist of flattened myoid cells ( The epithelium consist of two types of cells: 1. sertoli or supporting cells 2. spermatogenic cells
143
- a complex germinal or seminiferous epithelium
layers of fibroblasts
Tall columnar cells Extend from basal lamina to the lumen of a tubule Function:-
Sertoli or Supporting Cells
! support sperm cells ! nourish sperm cells ! form blood-sperm barrier ! phagocytosis of degenerated sperm cells ! conversion of hormones (testestrone to dehydrotestest.) ! regulate spermatogenesis ! secretion (androgen binding protein) called inhibin which suppresses FSH
144
72
1/8/2011
Spermatogenic Cells
Cells stacked in 4-8 layers Occupy space between basal lamina & lumen
Leydigs Cells (Interstitial Cells of Leydig)
Differentiate several times & produce spermatozoa Glandular cells of testis Produce male hormone (testosterone) Found within the lobules in the interstices Start function in 4 months of fetal life After birth their function interrupted up to puberty Stimulated by pituitary hormone (ICSH)
145
146
73
1/8/2011
147
148
74
1/8/2011
" Comma shaped structure " Lie to the superior & posteriolateral surfaces of the testis " Ducts of epididymis is highly coiled & contains millions of spermatozoa " If epididymis was uncoiled it measures about 5-6 meters " It consist of three parts:
Epididymis
1. Head
- upper expanded portion - composed of lobules of epididymis - coiled ends of efferent ductules (transmit sperm from testis to epididymis) - efferent ductules open into ductus epididymis (single) 149
Cont. 2. Body
- consist of convoluted duct of epididymis - found behind the testis - sinus of epididymis separates it from lateral surfaces
3. Tail
- found behind lower part of testis - lowest and smallest part " Epididymis is attached to the tunica albuginea by the ligament of epididymis
150
- continuous with the ductus deferens
75
1/8/2011
" Blood supply, lymphatics & innervation is almost similar with the testis " The innervation has also hypogastric plexus contribution " Help to store spermatozoa until full maturation " Epithelial lining has two types of cells: - columnar cells " Columnar cells contain non-motile cilia called stereocilia " The wall contains few smooth muscles
151
Cont.
- basal cells
152
76
1/8/2011
153
Ductus Deferens (Vas Deferens)
Fibromuscular tube about 45cm long & 2.5mm thick Continuation of ductus epididymis Conveys spermatozoa from epididymis to ejaculatory duct Has narrow lumen & thick layer of smooth muscle Forms part of the spermatic cord Ends by joining the duct of seminal vesicles (to form ejaculatory duct) Crosses ureter at the posteriolateral angle of the bladder Enlarged part (ampulla) is the terminal portion that joins ejaculatory duct
154
77
1/8/2011
155
156
78
1/8/2011
157
Accessory Glands of Male Genital System
$ Seminal Vesicles $ Prostate Gland $ Bulbourethral Glands
158
79
1/8/2011
Seminal Vesicles
Paired accessory male sex organs Each vesicle is thin walled pear shaped structure About 5cm long & 1-2cm in diameter Lies b/n the base of the bladder and the rectum Its broad blunt end is directed upward & laterally Each consist of a single coiled tube; 10-15cm long and 3-4mm in diameter Do not store sperms Secrete sticky, slightly alkaline yellowish substance Secretions serve as medium of spermatozoa movt and longevity
159
Contents of seminal secretion - fructose - monosaccharides - citric acid - coagulation proteins - prostaglandins - fibrinogen
160
80
1/8/2011
Cont.
Discharge from seminal vesicles make up about 60% of the volume of semen The duct of each seminal vesicle joins the ductus deferens to form the ejaculatory duct Have extensively coiled mucosal layer, breaking lumen into several intercommunicating spaces Mucosa is lined by pseudostratified columnar & cuboidal secretary epithelia Muscular coat contains inner (circular) & outer (longitudinal) layers Adventitia has numerous elastic fibers
161
162
81
1/8/2011
163
Arterial Supply of Seminal Vesicles
! inferior vesical artery ! middle rectal artery
Venous Drainage of Seminal Vesicles
! accompanies the arteries with similar names ! internal iliac lymph nodes
Lymphatic Drainage of Seminal Vesicles Innervation of Seminal Vesicles
! sympathetic fibers arise from superior lumbar nerves
' sympathetic stimulation releases contents to ejaculatory duct 164
! parasympathetic fibers arise from pelvic splanchnic nerves
82
1/8/2011
Ejaculatory Duct
Formed by union of duct of seminal vesicle and ductus deferens It is slender like tube It is about 2.5cm long Formed near and behind the bladder neck Begins at the base of prostate, pass down wards & forward through the substance of prostate gland Passes b/n the median lobe medially and right or left lobe laterally
165
Cont.
It goes on the sides of the prostatic utricle and opens on the colliculus seminalis close to the opening of the utricle Mucosa has columnar epithelium Contain thin outer (circular) & inner (longitudinal) strata of smooth muscles It has also thin outer fibrous layer
166
83
1/8/2011
167
The Prostate Gland
Largest accessory gland of the male reproductive system Partly glandular and partly fibromuscular organ It surrounds the prostatic urethra Conical in shape Has the following parts: - apex:- directed downwards; 1.5cm below the margin of symphysis pubis - base:- continuous with bladder neck - surfaces:- anterior, posterior & 2 inferiolateral surfaces
168
84
1/8/2011
169
Cont.
Situated in the lesser pelvis, below neck of bladder, behind lower part of pubic symphysis & in front of rectal ampulla Dimensions of the prostate gland are: - Anterioposterior:- 2cm - Vertical:- 3cm - Transverse:- 4cm Surgical routes of prostate gland - transvesical - retropubic (suprapubic) - perineal - urethral
170
85
1/8/2011
171
172
86
1/8/2011
Produce milky secretions
Functions of the Prostate Gland
Their secretion has the following advantages 1. assist motility of spermatozoa 2. help to nourish the spermatozoa 3. makes the semen more liquefied 4. its alkalinity protects sperm as it passes through the acidic vagina Clinically important since in the old ages the median lobe enlarged & projected to the bladder to impede urination
173
5. makes from 20 - 40% of volume of the semen
174
87
1/8/2011
175
Arterial Supply of Prostate Gland
! inferior vesical artery ! middle rectal artery
Venous Drainage of Prostate Gland
! prostatic venous plexus ! internal iliac LN to internal iliac vein
Lymphatic Drainage of Prostate Gland
! sacral LN ! external iliac LN
Innervation of Prostate Gland
! parasympathetic from pelvic splanchnic nerves () secretion) ! sympathetic from inferior hypogastric plexus 176
88
1/8/2011
Bulbourethral Glands (Cowpers Glands)
Two pea-shaped yellowish glands Lie posteriolateral to the membranous urethra Superior to the bulb of the penis Each gland is about 1cm in diameter Relatively long duct 2.5 to 3cm drain into urethra (end by opening into spongy urethra) Secrete mucoid substances that: - coats the lining of the urethra - neutralize the pH of urine residue - lubricates the tip of the penis Blood supply comes from the 177 arteries to the bulb of penis
178
89
1/8/2011
" External male genital organ " Common outlet for urine and semen " Copulatory organ of the male reproductive system " Has very thick skin; dark in color " Skin is loosely connected with fascial sheath of penis " The skin at the neck is folded to form prepuce " Median fold of skin on under surface is called frenulum of prepuce " The potential space between the glans & prepuce is called prepusial sac " Size of flaccid penis is variable (average 9.5cm); these 179erect state variation is less apparent in
The Penis
" Smegma:- is sebaceous material secreted by sebaceous glands on the corona glandis & neck of penis - these glands that secrete smegma are called prepusial glands
Cont.
180
90
1/8/2011
Parts of the Penis
1. The Root
- attached portion of the penis - located in the superficial perineal space - consist of crura, bulb & bulbospongiosus muscle - the bulb is situated in the midline - crura is attached to pubic rami and covered by ischiocavernosus muscle
181
Cont. 2. The Body (shaft)
- free pendulous part - has no muscle - consist of two corpora cavernosa (dorsal) & one corpus spongiosum (ventral) - corpora cavernosa are continuation of the crura and corpus spongiosum is also a continuation of the bulb - three cylinders of erectile tissue are enclosed in a sheath - spongy urethra is within corpus spongiosum - distally corpus spongiosum expands to form conical glans penis
182
91
1/8/2011
183
Cont.
3. The Glans
- separated from the body by neck - the prominent margin is corona glandis - has external urethral orifice - covered by skin called prepuce (double layer of skin) - frenulum of the prepuce run from deep layer of prepuce to external urethral orifice - has higher concentration of sensory nerve endings - sensitive to physical stimulation
184
92
1/8/2011
185
186
93
1/8/2011
# The root , body and glans of penis feel spongy because they are composed of cavernous erectile tissue, which # Most of penile urethra is lined by pseudostratified columnar epithelium but in the glans penis consists of interlacing & intercommunicating spaces
Cont.
# The epithelium becomes stratified squamous epithelium # Mucus secreting glands of Littre are found throughout the length of the penile urethra
187
188
94
1/8/2011
189
The penis is supported by two types of ligaments 1. Fundiform ligament: - arise from the lower part of linea alba - split to enclose the penis below - inferiorly fuses with the septum of the scrotum 2. Suspensory ligament: - arise from the symphysis pubis - lie deep to the fundiform ligament - it is triangular elastic band - blends with the deep fascia on each side of the penis
190
Supports of the Body of the Penis
95
1/8/2011
191
Arterial Supply of the Penis
Dorsal arteries:- run on each side of deep dorsal veins Deep arteries:- run within the corpora cavernosa Arteries of the bulb:- run in the corpus spongiosum along it Superficial external pudendal artery
- branch of femoral artery - supply skin and fascia of penis ' the above arteries arise from internal pudendal artery
# Deep arteries supply cavernous spaces (erectile tissue)
- involved in erection - give numerous branches open onto the space directly - when penis is flaccid, these arteries become coiled & called helicine arteries 192
96
1/8/2011
Venous Drainage of the Penis
! Superficial dorsal vein:- drain into superficial external ! Deep dorsal vein:- drain into prostatic venous plexus pudendal vein
Lymphatic Drainage of the Penis
! Deep inguinal LN:- from glans penis
! Superficial inguinal LN:- from skin & prepuce ! External iliac & internal iliac LN:- from the rest parts
193
Innervation of the Penis
! Dorsal nerve of the penis - branch of pudendal nerve - lie lateral to the arteries - supply both the skin & glans penis ! Cavernous nerves - from inferior hypogastric plexus - supply the erectile tissue ! Ilioinguinal nerve - supply skin covering the root of penis ! Deep perineal branches - supply the bulb & corpus spongiosum 194
97
1/8/2011
195
When the male is stimulated erotically cavernous nerves (parasympathetic system) carry out: % helicine arteries relax % the arteries straighten & lumen enlarged % allow more blood into cavernous spaces % blood engorges & dilates these spaces % bulbospongiosus & ischiocavernousus muscles compress venous plexus % this empedes the return of venous blood % as a result the three corpora becomes enlarged & rigid % all these lead the penis to erect
196
Erection of Penis
98
1/8/2011
& Controlled by sympathetic impulses from pelvic & Movement of sperm from epididymis to ejaculatory ducts & Caused by rhythmic contraction of the smooth muscles of epididymis, ductus deferentia, ejaculatory ducts, seminal & Contraction of the internal vesical sphincter prevents reflux of semen into the bladder
197
Emission
(lumbar) plexus
& secretions of accessory glands to ejaculatory duct
vesicles & prostate
* immediately follows the emission phase
Ejaculation
* accompanied by orgasm (climax of sexual act) * occurs in a series of spurts of semen from the urethra to out
* PS impulse through pudendal nerve stimulate contraction of bulbosongiosus muscle at the base of penis & cause them to contract rhythmically
* Sympathetic stimulation cause urethral wall smooth muscles to contract; this helps semen to eject
198
99
1/8/2011
#Due to the above two stimulations ejaculation is completed
Cont.
#Sexual function in male requires the synergistic action of parasympathetic & sympathetic divisions of the ANS #Sympathetic impulse causes the body activities return to normal (e.g. cardiac output, blood flow etc)
#Following ejaculation, another erection & ejaculation cannot be triggered for 10 to 30 minutes or longer
199
Semen
Consist of spermatozoa & additives from accessory reproductive glands 1.5 to 5 ml of semen is ejected during ejaculation Come from seminal vesicle (~ 60%), from prostate (~ 40%) Spermatozoa contribute < 1% of the volume of ejaculate There are 60 to 150 million sperms per ml of ejaculate Male ejaculates fewer than 10 million per ml (oligospermia) is likely to have fertility problems
200
100
1/8/2011
Some Related Terms
Epispadia:-urethra opens in the dorsum of penis Hypospadia:- under surface the penis Phimosis:- non retractable tightly fitted prepuceover the glans penis Paraphimosis (capistration):- painful constriction of the glans penis by phimotic foreskin
Cont.
Detumescence:- return of penis to flaccid state after orgasm because of sympathetic stimulation Micropenis:- boys born with small penis (<2cm) but rare Circumcision:- surgical removal of the prepuce Impotence:- failure of erection because of psychic, hormonal or neural problems Priapism:- abnormal painful erection of penis for long time because of spinal cord lesions
202
101
1/8/2011
FEMALE GENITAL ORGANS
Functions of the Female Reproductive System
1. Produce ova 2. Secrete sex hormones 3. Transport the ova of zygote 4. Receive spermatozoa from males during coitus 5. Provide sites for fertilization & implantation 6. Facilitate delivery of the baby 7. Provide nourishment for the baby
203
Components of the Female Genital Organs
Primary sex organs include: - ovaries which produce:- ova (gametes) or eggs - sex hormones Secondary sex organs include: - uterus (womb) - uterine tube (fallopian tube) - vagina - mammary glands - external genital organs:- which consist of: ! mons pubis ! bulb of vestibule ! labia majora & minora ! clitoris ! vestibule of vagina 204 ! Bartholins gland
102
1/8/2011
205
The Ovaries
Paired primary sex organs Intraperitoneal organ Homologous to the testes Oval-shaped pinkish-white glands Each ovary is 3cm long, 1.5cm wide & 1cm thick Each ovary weighs about 10-15 grams Has variable size but smaller at menopause Produce estrogen & progesterone for:a. regulation of menstrual cycle b. secondary sex organ to appear c. maturation of primary 206 sex organs
103
1/8/2011
Cont.
Color & texture of ovaries vary according to:- age - reproductive stage of females Ovaries of young girl are smooth & pinkish After puberty ovaries become pinkish gray & rough b/c of scarring caused by ovulation In the nulliparous woman the ovary has: - two surfaces:- medial & lateral - two ends:- upper (tubal) & lower (uterine) - two borders:- free & mesovarian (attached)
207
Cont.
On the medial portion is the hilum, for entrance of ovarian vessels & nerves Lateral portion is near the open end of the uterine tube Ovaries are located to the lateral wall of pelvis minor in a recess called ovarian fossa Ovarian fossa is bounded: - anteriorly by medial umbilical ligament - posteriorly by the ureter & internal iliac artery The ovary is attached to the upper (posterior) layer of broad ligament by short fold of peritoneum called mesovarium 208
104
1/8/2011
209
Attachments of the Ovary
1. Suspensory Ligament - attach to the lateral wall of the pelvis - contain ovarian vessels & nerves - fibers are connected to psoas sheath 2. Ovarian Ligament - attach uterine end to tubal angle on the uterus - contain ovarian branch of uterine artery 3. Mesovarium - specialized posterior extension of broad ligament
210
105
1/8/2011
211
Arterial Supply of the Ovaries
! Ovarian arteries ! Ovarian branches of uterine arteries
Venous Drainage of the Ovaries
! From ovarian plexus two veins arise: 1. right ovarian vein:- drain into IVC 2. left ovarian vein:- drain into the left renal vein
Lymphatic Drainage of the Ovaries Innervation of the Ovaries
! Ovarian plexus
212
! Follow the arteries & drain into lumbar (aortic) LN
106
1/8/2011
213
Each ovary consist of four layers: 1. Superficial Epithelium - thin outer most layer
Microscopic Structures of the Ovaries
- composed of cuboidal epithelial cells (simple squamous) - also called germinal epithelium 2. Tunica Albuginea - lie under germinal epithelium - dense collagenous connective tissue layer - give whitish color for the ovaries
214
107
1/8/2011
Cont.
3. Ovarian Cortex - ovarian follicles containing the oocyte predominate - compact layer & rich in stroma cells - also contain glandular structures & corpora lutea - broad outer part interrupted at the hilum 4. Ovarian Medulla (zona vasculosa) - inner vascular layer - composed of loose connective tissue (elastic fibers) - rich in blood vessels, nerves & lymphatic vessels - also contain smooth muscle fibers near the hilum N.B. The boundary b/n cortex and medulla is not clear
215
216
108
1/8/2011
217
Ovarian Follicles
Embedded in the stroma of the cortex Follicle consisting of oocyte is surrounded by one or more layers of follicular cells, the granulosa cells Total follicle number in both ovaries in youngs ~ 400,000 Most follicles disappear through atresia during reprod. years Follicular regression begins before birth & continues over reproductive life After menopause only small number of follicles remain Only one ovum is liberated in each menstrual cycle Reproductive life of a woman lasts about 30-40 years Totally only about 450 ova are liberated in ones life time All other follicles with oocytes become atretic & degenerate
218
109
1/8/2011
A. Primordial Follicles
Most numerous before birth squamous follicular cells The oocyte in these follicles is spherical approximately The squamous follicular cells are joined by desmosomes Basal lamina marks the boundary b/n the avascular follicle and the surrounding stroma
219
Each consist of primary oocyte enveloped by simple
around 25m in diameter
220
110
1/8/2011
B. Growing Follicles
Involves follicular cell growth, primary oocytes & stroma Oocyte growth is most rapid Oocyte reaches maximum diameter of 125-150m Nucleus enlarges & is called germinal vesicle Organelles increase in size & number Follicular cells form single layer of cuboidal cells called unilaminar primary follicle Follicular cells proliferate by mitosis & form stratified follicular epithelium or granulosa layer Zona pellucida surrounds the oocyte
221
' the follicle is then called multilaminar primary follicle
Primary follicle with zona pellucida & single layer of follicular cells
222
111
1/8/2011
Cont.
Both oocyte & follicular cells contribute to form zona pellucida The stroma around the follicle differentiates to form the theca follicle Theca follicle differentiate into theca interna & theca externa - theca interna:- highly vascularized - theca externa:- consist of mainly CT As follicles grow, granulosa cells increase in size & number; follicular fluid (liquor folliculi) accumulates b/n the cells 223
224
112
1/8/2011
Secondary follicle with 20 oocyte in cumulus oophorus & liquor folliculi surrounded by thin membrana granulosa
225
Cont.
Cavities that contain this fluid forms larger cavity, antrum Follicles are then called secondary (vesicular) follicles Follicular fluid contains transudates of plasma and products secreted by follicular cells such as: - GAGs - proteins - steroids etc . Granulosa layer forms small hillock of cells, the cumulus oophorus, which contains the oocytes Cumulus oophorus protrudes toward the interior of antrum
226
113
1/8/2011
C. Mature Follicles (Graafian follicle)
About 2mm in diameter Occupies the whole thickness of the cortex Follicular cavity increases in size Oocyte adheres to the wall of the follicle through a pedicle formed by granulosa cells Zona pellucida forms corona radiata which accompanies the ovum Corona radiata is still present when spermatozoa fertilizes the ovum Oocyte with corona radiata forms conical projection called stigma
227
228
114
1/8/2011
Cont.
Ovum with corona radiata & cumulus oophorus cells and follicular fluid are discharged into the uterine tube ' called ovulation Ovum usually fertilizes within 24 hours Fertilization usually takes place in the ampulla of oviduct After ovulation corpus luteum (yellow body) serve as temporary endocrine gland If no fertilization, corpus luteum attain maximum size about one week after ovulation Later degenerate & transformed to whitish scar called corpus albicans If ovum is fertilized it )es in size until replaced by placenta
229
230
115
1/8/2011
231
232
116
1/8/2011
The Uterine Tube
Paired organs extend laterally from cornu of uterus Also known as fallopian tube or oviduct Occasionally termed as salpinx Situated in the free upper margin of broad ligament of uterus Lie b/n the folds of broad ligament Each uterine tube is about 10 to 12cm long Has a diameter of: - 3mm at the abdominal ostium - 4mm at the ampulla - 2mm at the isthmus - 1mm at the intramural 233 part
Each tube opens into two ends: 1. proximal end:- to cornu or horn of uterus 2. distal end:- to peritoneal cavity near the ovary Function - carry oocytes from ovary to site of fertilization - transport sperm from uterus to - communicate peritoneal cavity to exterior of the body - move zygote to site of implantation Has four parts: 1. Infundibulum 2. Ampulla 3. Isthmus 4. Intramural (uterine) part 234
117
1/8/2011
Isthmus Ampulla Infundibulum
Intramural part
235
# An ovum takes 3 to 5 days to reach the uterus by: 1. Ciliary action of the epithelia 2. Peristaltic action of the muscular coat
Cont.
# If implantation occurs outside the normal site we call it ectopic pregnancy # Tubal ectopic pregnancy leads to the swelling of the oviduct & later cause rupture of the tube
# Lamina propria reacts like the endometrium forming numerous decidual cells # Abdominal ectopic pregnancy occur due to tubal abortion & secondarily implanted in the abdominal cavity 236
118
1/8/2011
Arterial Supply of the Uterine Tube
! Uterine arteries ! Ovarian arteries
237
Venous Drainage of the Uterine Tube
! Uterine veins ! Ovarian veins
Lymphatic Drainage of the Uterine Tube
! From ovarian to lateral aortic & aortic LNs ! From uterine end by round ligament of uterus to the superficial inguinal LNs ! Ovarian plexus ! Uterine plexus ! Inferior hypogastric plexus ! Afferent fibers from tubes are contained in T11, T12 & L1 nerves 238
Innervation of the Uterine Tube
119
1/8/2011
The Uterus
Also known as womb or hystera Hollow thick walled muscular organ Pear shaped organ located between the bladder & rectum Fertilized ovum is embedded, grows & nourished until birth by this organ Uterus varies in shape, size & position based on: - age - pregnancy - state of rectum & urinary bladder It projects superoanteriorly over the urinary bladder
239
Uterus doesnt lie in the midline rather inclinded to the right Cervix & upper part of vagina are slightly tilted to the left Dimensions of the uterus in non-gravid woman is: - length 7 to 10cm - transverse diameter 5 to 7cm at the fundus 2 to 2.5cm at the cervix - anteroposterior diameter 2 to 3cm thick - weighs about 50g
240
Cont.
120
1/8/2011
Cont. Uterus usually bent anteriorly (anteflexed) b/n cervix & body with about 1700 The entire uterus is inclinded anteriorly (anteverted) from the vagina with 900 Uterus has the following parts: 1. fundus 2. body 3. isthmus 4. cervix
241
242
121
1/8/2011
Parts of the Uterus
1. Fundus
! convex in all directions ! lie above the opening of the uterine tube
! uterine tube enter the uterus through the cornua (horns) ! covered by peritoneum ! related to coils of ileum
! uterine tube joins uterus at the junction of fundus & body
243
2. Body
! forms the upper two-third of the uterus ! narrows from the fundus to the cervix ! the junction with the cervix is called isthmus
! body is covered by the peritoneum on both surfaces i. Right border ! has two surfaces: ii. Left border
! has two borders related to the respective broad ligaments
i. Anterior surface ii. Posterior surface
244
122
1/8/2011
# Anterior (vesical) surface - flattened
Cont.
- related to the upper surface of the urinary bladder # Posterior (intestinal) surface - convex shaped - separated from sigmoid & rectum by rectouterine pouch (of Douglas); this pouch also called cul-desac which contain some part of ileum
245
- separated from the bladder by uterovesical pouch
3. Isthmus
! it measures about 1cm long
! constricted portion at the junction of body & cervix ! constriction is clearly seen in nulliparous woman ! the cavity forms internal ostium (Lathin, door) ! it is a site of anteflexion
4. Cervix
! about 2.5cm long
! lie b/n the isthmus & vaginal opening of the uterus
! has a canal called cervical canal
246
! cervical canal is wider in the middle than the two ends
123
1/8/2011
! has two portions as cervix projects down to the vagina a. Supravaginal portion
- anteriorly has no peritoneum & related to base bladder - posteriorly covered by peritoneum & related coils of intestine - laterally attach to broad ligament & related to the uterine vessels & ureter
b. Vaginal portion
- project through the anterior wall of the vagina - surrounded by vaginal fornices - open into the vagina by external ostium (os) - opening is small & rounded in nulliparous woman & transverse slit in woman who 247 have borne children
Cont. $Cervix does not participate in menstruation but alter its secretions during d/t stages of menstrual cycle $Cervix has simple columnar epithelium except inferior portion covered by stratified squamous epithelium
248
124
1/8/2011
249
250
125
1/8/2011
251
Ligaments (Attachments) of Uterus
1. Broad Ligament
- double layered fold of peritoneum - attach uterus to the lateral wall of the pelvis - has free anterior and attached posterior borders - parts of the broad ligament include: i. Mesosalpinx:- lie b/n uterine tube & mesovarium - upper part of broad ligament ii. Mesometrium:- lie b/n pelvic floor, ligament of ovary & body of uterus situated inferiorly iii. Mesovarium:- suspend ovary from broad ligament - attached to the hilum of ovary posteriorly 252
126
1/8/2011
253
254
127
1/8/2011
2. Round Ligament of the Uterus
- fibromuscular band attached to vesical surface of uterus - follow similar route like ductus deferens - extends from lateral wall of uterus to the labia majora - raises a ridge on the lower surface of broad ligament - before entering inguinal canal it crosses: " umbilical artery " external iliac vessels
" vesical & obturator vessels &
" hooks on inferior epigastric artery - round ligament & ovarian ligament corresponds together to the gubernaculum of the testes in males 255
3. Ligaments of the Ovary
- attach uterus to the ovaries - fibromuscular band - raises a ridge on the upper surface of broad ligament
4. Lateral (Transverse) Cervical or Cardinal Ligament
- thick vesical pelvic fascia - extend laterally from cervix & vagina - contains some smooth muscles, vessels & nerves
5. Rectouterine & Uterosacral Ligaments
- part of thickened visceral fascia - attach uterus to the sacrum N.B. Uterus is inferiorly supported by the pelvic diaphragm
256
128
1/8/2011
Conditions Affecting Size, Shape & Position of Uterus
1. During Fetal Life - uterus is higher in position - projects above the place of pelvic brim - cervix is larger than the body 2. At Puberty - uterus is just below the plane of pelvic brim - the shape becomes pear-like 3. During Pregnancy - uterus is greatly enlarged - devt of muscle fiber is prominent - the wall becomes thinner 257 as pregnancy advances
4. After Labour - uterus differ from the virgin state a) cavity becomes larger b) vessels are highly tortuous c) wall becomes thicker d) external os becomes slit-like 5. After Menopause - uterus undergoes involution
258
Cont.
- uterus gradually diminishes to its original size
129
1/8/2011
Arterial Supply of the Uterus
! uterine arteries:- from internal iliac
! small part from ovarian and vaginal arteries
Venous Drainage of the Uterus
! uterine plexus + uterine vein + internal iliac vein
Lymphatic Drainage of the Uterus
! from fundus:- to aortic LNs - some to external iliac LNs - some to superficial inguinal LNs
! from body:- to external iliac LNs ! from cervix:- to internal iliac LNs - sacral LNs
259
260
130
1/8/2011
Innervation of the Uterus
! From inferior hypogastric plexus by uterovaginal plexus ! Parasympathetic from pelvic splanchnic nerves (S2, S3 & S4)
Microscopic Structures of the Uterus
! the wall is relatively thick 1. serosa (perimetrium) 2. muscularis (myometrium) 3. mucosa (endometrium)
261
! the wall is formed of three layers
1. Perimetrium (Serosa)
Outer peritoneal cover of uterus Lateral portion is continuous with broad ligament Pouches are formed as this peritoneum is reflected over the rectum & urinary bladder
2. Myometrium (Muscularis)
Thickest tunic of uterus Forms most of the uterine wall About 15mm in thickness Composed of bundles of smooth muscle fibers Have loose connective tissue
262
131
1/8/2011
263
264
132
1/8/2011
265
Endometrium (Mucosa)
Contains: - epithelium - lamina propria The epithelium is simple columnar with ciliated & nonciliated cells Endometrial (uterine) glands are lined by columnar epithelium No submucosa in the uterine wall i. the functionalis ii. the basalis
266
- simple tubular glands
The endometrial layer can be divided into two zones:
133
1/8/2011
Cont. The functionalis
- constitutes the portions sloughed off at menstruation - replaced during each menstrual cycle - thin superficial layer with straight glands is called compacta - deep layer with bulk of functionalis is called spongiosa
The basalis
- portion retained after menstruation - proliferate & provide a new epith. & lamina propria - endometrium is renewed (re-epithelized) by this zone
267
134
1/8/2011
Cont. Related Terms with Uterus
" Hysterectomy:- surgical removal of uterus " Retroversion:- whole uterus inclind posteriorly in old woman " Retroflexion:- posterior curvature of body of uterus alone opening " Prolaps of uterus:- protrusion of uterus through the vaginal
269
270
135
1/8/2011
# Female organ of copulation # Musculomembraneous tube 7- 9cm long # Length:- anterior wall 7.5cm - posterior wall 9cm # Extends upward & backward from the vulva # Connects cervix of the uterus to the vestibule # Forms 90O with the uterus in empty bladder & rectum # Width about 4cm but can be distended & elongate # Highly dilatable organ # When it is empty the cavity has H-like shape on cross section
271
The Vagina
272
136
1/8/2011
#The recesses b/n vaginal part of cervix & vagina is called fornix
Cont.
#There are four fornices (1 anterior, 1 posterior & 2 lateral)
#Aspiration (taking) of fluid from posterior fornix is called cul de centesis #Walls of vagina are in contact with each other #As the vagina descends it traverses the superficial & deep perineal pouches
273
#Relations
- Posteriorly:- to rectum & anal canal
Cont.
- Anteriorly:- to urinary bladder & urethra i.e. - upper 1/4th with peritoneum of rectum - middle 2/4th with rectum - lower 1/4th with anal canal - Laterally:- to levator ani & pelvic fascia
274
137
1/8/2011
# Circumscribed by skeletal muscle at its external orifice # Sphincters of the vagina includes 3 muscles: i. Pubovaginalis muscle ii. Urogenital diaphragm # Exterior opening of the vagina is called vaginal orifice # Vaginal orifice is partially covered by thin fold of mucous membrane called hymen
275
Cont.
iii. Bulbospongiosus muscle
# Vagina orifice is located posterior to the urethral orifice
Hymen
Horizontal fold of mucous membrane Structurally similar with the vaginal mucosa Annular or crescentric in shape Its existence shows no coitus & delivery before (virginity) Can be torn with strong exercises After rupture small rounded elevation at attached margin is called carunculae hymenalis Types include: - single orificed (annular) - cribriformed (perforated) - bifurcated (setptate) - imperforate 276
138
1/8/2011
277
Arterial Supply of the Vagina
! vaginal branch of uterine artery ! vaginal branch of internal iliac artery ! vaginal branch of middle rectal artery ! internal pudendal artery
Venous Drainage of the Vagina
Vaginal venous plexus ! Vaginal veins ! Uterine or vesical venous plexus ! Internal iliac veins
278
139
1/8/2011
Lymphatic Drainage of the Vagina
1. Superior part along with uterine artery drains in to internal & external iliac LNs 2. Middle part along vaginal artery drains into internal iliac LNs 3. Inferior (vestibular) part drains into sacral, common iliac & superficial inguinal LNs
Innervation of the Vagina
! Uterovaginal plexus:- most parts ! Branches from pudendal nerve:- lower part nerves
! Also from inferior hypogastric plexus & pelvic splanchnic
279
Microscopic Structure of the Vagina
Wall of vagina is devoid of glands except cervical end
The mucus found in the lumen of vagina comes from the glands of uterine cervix The wall consist of three layers:
1. Mucosa
, epithelium is non-keratinized stratified squamous , vaginal rugae provides
, forms series of transverse folds called vaginal rugae a. distention for penetration of erect penis b. friction ridges for stimulation of the erect penis
280
140
1/8/2011
, The mucosa synthesize & accumulate glycogen + for + this keeps pH of vagina low + retards microbial growth lymphocytes bacteria to metabolize + into lactic acid
, Acidic mucus comes from cervix glands
Cont.
, Lamina propria is rich in elastic fibers & infiltrated by , Mucosa devoid of sensory nerve endings except pain fibers on the lower part
281
Cont.
2. Muscularis - outer longitudinal smooth muscles at large - innermost some circular smooth muscles - skeletal muscles near the vaginal orifice 3. Adventitia:- composed of dense regular CT - rich in thick elastic fibers & connect it - unite the vagina with the surrounding tissues
282
141
1/8/2011
Mucosa of vagina showing non-keratinized stratified squamous epithelium and the lamina propria beneath
283
284
142
1/8/2011
Female External Genitalia
Collectively known as vulva Structures of the vagina surround the vaginal orifice Includes the following structures:
1. The Mons Pubis
! rounded fatty elevation anterior to the pubic symphysis ! consist of mainly pad of fat under the skin ! amount of fat )es at puberty & -es after menopause ! skin is covered by pubic hairs after puberty ! pubic hair pattern is almost triangular
285
! helps to cushion symphysis pubis & vulva during coitus
2. The Labia Majora
! two thick symmetrical longitudinal folds f skin ! homologous to the scrotum of the males ! continuous anteriorly with mons pubis ! contain loose fibrous CT, adipose tissue & smooth ms. ! lie on each side of the pudendal (urogenital) cleft ! protects the urethral and vaginal orifices hairs ! its skin has sebaceous & sweat glands & covered by ! the two labia majora fuse anteriorly to form anterior labial commissure
286
143
1/8/2011
! two labia majora dont fuse posteriorly but a transverse bridge skin called posterior labial commissure passes ! round ligament of uterus enters the labia majora 3. The Labia Minora ! pair of thin skin folds b/n labia majora sebaceous glands & elastic fibers b/n them
Cont.
! its skin is fat free, hairless but rich in blood vessels, ! has many sensory nerve endings
287
! in nulliparous L. minora is concealed by L. majora
! L. minora encloses the vestibule of the vagina
Cont.
! sebaceous & sweat glands open on both of their surfaces ! in youngs, the two lips unite posteriorly by small fold of skin called frenulum of labia minora (fourchette) ! the depression b/n frenulum of labia minora & vaginal orifice is called vestibular fossa ! Anteriorly each lip of L. minora is divided into two parts: 1. lateral part 2. medial part
288
144
1/8/2011
% Lateral part:- fuse anterior to the clitoris & forms % Medial part:- fuse behind the clitoris & form frenulum of clitoris N.B. Episiotomy:- incision on external female genitalia - done to facilitate delivery - could be median or mediolateral - both majora & minora are incised the prepuce of clitoris
Cont.
289
290
145
1/8/2011
4. Vestibule of the Vagina
! the space b/n the labia minora ! contains opening of urethra & vagina, greater & lesser vestibular glands ! median aperture located 2 or 3cm posterior to clitoris ! lie immediately anterior to the vaginal orifice ! on each side opening of ducts of paraurethral glands (Skenes glands) ! large opening posterior to urethral opening ! narrowed by the hymen 291
5. External Urethral Orifice
6. Vaginal Orifice
292
146
1/8/2011
7. Greater Vestibular (Bartholins) Glands
Two large rounded bodies on each side of the vestibule Lie posteriolateral to the vaginal orifice Homologous to bulbourethral glands in males Their duct opens b/n labia minora & vaginal hymen Secrete lubricating mucus into vestibule during sexual arousal
8. Lesser Vestibular Glands
small numerous glands on each side of vestibule opens b/n the urethral & vaginal orifices secrete mucus into vestibule to moisten it resemble the glands of Littre in the male 293
294
147
1/8/2011
9. Skenes (Urethral) Glands
Numerous glands in the wall of female urethra Secrete mucus to the urethra
10. Bulb of the Vestibule
Two masses of erectile tissue on each side of vaginal opening Covered by bulbospongiosus muscle Homologous to the bulb of penis in males
295
296
148
1/8/2011
11. Clitoris
Homologous to the penis of males About 2-3cm long & 0.5cm in diameter Has crura, body & glans Unlike penis, urethra doesnt pass through it i.e. no corpus spongiosum Hidden by the labia when flaccid Erection of clitoris is like the penis by engorgement of blood Has two corpora cavernosa Important (sensitive) for sexual arousal of females Attached to symphysis pubis by suspensory ligament Main part removed during circumcision
297
298
149
1/8/2011
Arterial Supply of Female External Genitalia
! External pudendal artery:- from femoral ! Internal pudendal artery:- from internal iliac
! Anterior labial artery:- from external pudendal
! Posterior labial artery:- from internal pudendal
Venous Drainage of Female External Genitalia
! Labial veins:- drain into internal pudendal veins ! Some veins drain to external pudendal veins ! Some drains to the uterine plexus
299
! Most of the veins follow the arteries
Lymphatics of Female External Genitalia
! Superficial inguinal LNs ! Deep inguinal LNs
Innervation of Female External Genitalia
! Ilioinguinal nerves ! Pudendal nerve ! Genital branch of genitofemoral nerve ! Perineal branch of femoral cutaneous nerve of thigh ! Uterovaginal plexus
300
150
1/8/2011
Mechanism of Erection & Orgasm
Vision, hearing, smell, touch & other psychic stimuli gradually build up the intensity of sexual excitement During sexual excitement, hypothalamus sends parasympathetic nerve impulses through sacral segments Upper part of vagina is sensitive to stretch only but labia minora & clitoris are extremely sensitive to touch Dilation of arteries to clitoris & vestibular bulbs
301
)ed flow of blood cause erectile tissues to swell enlarged Vagina expands & elongates
Cont.
Erectile tissues in the areola of breasts also become
Parasympathetic impulses cause vestibular glands to secrete mucus Mucus continues to be secreted during coitus so that genitalia do not become irritated
302
151
1/8/2011
Cont.
Position of the sensitive clitoris usually allows it to be stimulated during coitus If stimulation is sufficient, woman will experience a culmination of pleasurable psychological & physiological release called orgasm Associated with orgasm is a rhythmic contraction of the muscles of the perineum & muscular wall of uterus & oviduct. This aid movt of spermatozoa Following orgasm, sympathetic impulses cause reduction in arterial flow to erectile tissues & their size diminishes to normal
303
Homologous Reproductive Organs & their Devt
Indifferent stage
Gonads Urogenital groove Genital tubercle Urethral folds Labioscrotal fold
Male
Testes Membranous urethra Glans penis Spongy urethra Bulbourethral gland & Scrotum
Female
Ovaries Vaginal vestibule Clitoris Labia minora Labia majora vestibular gland
304
152
1/8/2011
# Pelvic wall has three layer:-
WALLS OF THE PELVIS
1. External layer:- formed of gluteal muscles 2. Intermediate layer:- contains bones and ligaments
# The pelvis has two part by plane of pelvic inlet:1. upper part:- greater (false) pelvis # Plane of pelvic inlet passes from sacral promontory to upper margin of symphysis pubis
305
3. Internal layer:- has muscles & fascia
2. lower part:- lesser (true) pelvis
306
153
1/8/2011
forms lower boundary of pelvis divided into two parts by a line through ischial tuberosities 1.urogenital triangle 2.anal triangle the above triangles are formed of muscles & fascia
The Pelvic Floor
Urogenital diaphragm
- lie between pubic rami & ischial tuberosities
- has perineal membrane & muscles - muscles includes:-sphincter urethra muscle - superficial & deep transverse muscles - ischiocavernosus - bulbospongiosus 307
Cont.
- Urogenital diaphragm has glands: i. bulbourethral (in males) ii. vestibular glands (in females) - Innervated by perineal nerve which is a branch of pudendal nerve - Action of urogenital diaphragm i. voluntary constriction of urethra & vagina ii. Support pelvic viscera
308
154
1/8/2011
Pelvic Diaphragm
Gutter-shaped sheet muscle Consist of levator ani and coccygeus muscles Also contain fascia that covers upper & lower surfaces Separates pelvic cavity from perineum Pierced by urethra, anal canal & vagina
Supports pelvic viscera & resist )ed intraabdominal pressure
1. Levator ani Muscle
Action: 1. support pelvic viscera 2. resist )ed intraabdominal pressure 3. assist abdominal wall muscles 4. help to control micturation
309
Cont.
- Nerve supply of levator ani muscle: ! S3 and S4 ventral rami, ! inferior rectal nerve - Has three parts i. Iliococcygues origin:- pelvic part of ischial spine & obturator fascia Insertion:- side of coccyx & anococcygeal ligament 310 ! perineal branch of pudendal nerve
155
1/8/2011
311
ii. Pubococcygeus main part of levator ani muscle origin:- back of body of pubis
Cont.
insertion:- coccyx, perineal body & anal canal
anterior fibers surround prostate or vagina & form levator prostate & pubovaginalis muscle iii. Puborectalis forms mucular sling behind anorectal junction origin:- lateral part of body of pubis
312
insertion:- loop around anorectal junction
156
1/8/2011
Cont. 2. Coccygeus Muscles
- lie posterior to iliococcygeus muscle - origin:- pelvic surface ischial spine & sacrospinous ligament - insertion:- side of coccyx & S5 vertebra - innervation:- branch of S4 & S5 nerves - action: " assist levator ani muscle " support pelvic viscera " elevate pelvic floor
313
314
157
1/8/2011
Perineal Body
Central tendon of perineum Fibromuscular node situated in the median plane Lie 1.25cm in front of anal margin Has both skeletal & smooth muscles Also composed of elastic & collagen fibers Nine muscles converge & interlace in this site Three unpaired muscles
i. external anal sphincter ii. bulbospongiosus iii. long. ms. coat of rectal ampulla & anal canal
Three paired muscles
i. superficial transverse perinei ii. deep transverse perinei 315 iii. levator ani
316
158
1/8/2011
317
The Pelvic Fascia
1. Visceral Pelvic Fascia (Endopelvic Fascia)
- binds pelvic viscera together - envelops viscera by forming false capsule - has variable smooth muscles to support pelvic floor - in females this fascia laterally thickened to form uterosacral & transverse cervical ligaments - it also forms lateral ligament of rectum & bladder
318
159
1/8/2011
2. Parietal Pelvic Fascia
- lines the pelvic cavity
Cont.
- attached to periosteum of ilium around the brim - extends onto the superior surface of the pelvic diaphragm - then pass to pelvic viscera where it is continuous with visceral pelvic fascia - parietal pelvic fascia also encloses great vessels of pelvis - superiorly continuous with transversalis fascia - helps to support the pelvic viscera 319
Cont.
- it covers the pelvic surface of: " obturator internus muscle (obturator fascia) " piriformis muscle " sphincter urethra " levator ani " coccygeus muscle
- levator ani muscle attach to a thickening of obturator fascia called tendinous arch stretches b/n body of pubis & ischial spine - it also forms rectovesical & rectovaginal septa
320
160
1/8/2011
Cont.
$ Superior fascia of the pelvic diaphragm - in females attached to: ! posterior aspect of body of pubis ! the neck of urinary bladder ! the vagina & ! the rectum - fascia of pelvic diaphragm covers both its superior & inferior surfaces, & named with corresponding surfaces
- in males attaches to: ! the prostate ! the rectum
321
Cont.
- the superior fascia is thickened at the neck of urinary bladder to form two cord like bands called: ! pubovesical ligaments in females ! puboprostatic ligament in males
$Inferior fascia of the pelvic diaphragm - covers inferior surface of levator ani muscle - forms medial wall of ischioanal fossae
322
161
1/8/2011
Diamond shaped space found below the pelvic diaphragm Corresponds to the outlet of pelvis Has a ridge called perineal raphe run from anus to scrotum & penis The roof is formed by pelvic diaphragm Boundaries: " Anteriorly:- upper part of pubic arch - arcuate (inferior) pubic ligament " Posteriorly:- tip of coccyx " On each side:- ischiopubic ramus - ischial tuberosity 323 - sacrotuberous ligament
Perineum
Perineum is divided into two triangles:
1. Anal Triangle: - posteriorly located - ischiorectal fossa is found on each side 2. Urogenital Triangle: - located anteriorly - contains external urogenital organs
Cont.
- has superficial & deep perineal spaces (pouches)
324
162
1/8/2011
Cont. A. Superficial perineal space (pouch)
- lie b/n deep perineal fascia & perineal membrane - boundaries: " superficial:- Colles fascia " deep:- perineal membrane " on each side:- ischiopubic ramus
" anteriorly:- pouch is open & continuous with penis, scrotum & anterior abdominal wall " posteriorly:- pouch is closed by union of perineal membrane & Colles fascia
325
Contents of superficial perineal pouch
" root of penis (two crura & one bulb) " bulb of the vestibule " crura of the clitoris " muscles:- superficial transverse perinei - ischiocavenosus - bulbospongiosus " arteries:- posterior scrotal artery - transverse perineal artery - artery of penis " nerves:- posterior scrotal nerve - nerve to bulb - muscular branch of perineal nerve " glands & ducts:- greater vestibular gland in females - duct of326 bulbourethral gland in males
163
1/8/2011
Cont. B. Deep Perineal Space (pouch)
# Deep space of urogenital triangle # Boundaries: # Lie deep to the perineal membrane " superficial:- perineal membrane " on each side:- ischiopubic rami pelvic fascia
" deep:- pelvic fascia (inferior fascia of pelvic diaph.) " anteriorly:- closed by union of perineal membrane & " posteriorly:- closed by union of perineal membrane & pelvic fascia
327
#Contents of the deep perineal pouch
- membranous urethra - muscles:- sphincter urethra - deep transverse perinei - vessels:- internal pudendal vessels - vessels of the bulb - nerves:- dorsal nerve of penis - dorsal nerve of clitoris - glands:- bulbourethral glands in males
328
Cont.
164
1/8/2011
Pudendal Canal (Alcocks Canal)
. Extends from lesser sciatic notch to posterior border of perineal membrane . Fibrous funnel formed by splitting of obturator fascia . The contents are:- internal pudendal artery - internal pudendal vein . Pudendal nerve in the canal gives - inferior rectal nerve - dorsal nerve of penis - perineal nerve
329
- pudendal nerve
Cont.
Inferior rectal nerve is also accompanied by inferior rectal vessels Branches of internal pudendal artery 1. Muscular branches 2. Inferior rectal artery 3. Perineal artery 4. Artery of bulb of penis 5. Urethral artery 6. Deep artery of penis 7. Dorsal artery of penis
330
165
1/8/2011
. Lie posterior to urogenital triangle
Anal Triangle
. Large part on each side is hold by ischiorectal fossa
. Ischiorectal fossa (Ischioanal fossa)
- appear triangular in cross section - its base is directed down wards - the apex lies upward - base is formed by skin
- wedge shaped space below pelvic diaphragm
- apex:-fusion of obturator fascia with inferior fascia of pelvic diaphragm 331
166
1/8/2011
. Ischioanal fossa is bounded:
membrane
Cont.
- anteriorly:- limited by post. border of perineal - posteriorly:- lower border of gluteus maximums and sacrotuberous ligament - lateral wall:- obturator internus muscle and fascia; medial surface of ischial tuberosity - medial wall:- external anal sphincter levator ani muscle and anal fascia
333
. Ischioanal fossa is a site of abscess formation
Cont.
- communicate with the rectum and anal canal
. Contents of ischioanal fossa
- ischiorectal pad of fat
- right and left sides communicate behind anal canal
- inferior rectal nerves and vessels - posterior scrotal or labial nerves and vessels - perineal branch of s4 nerve - posterior femoral cutaneous nerve - perforating cutaneous branches of s2 & S3 nerves - pudendal canal
334
167
1/8/2011
Cont.
. Nerve Supply of the Pelvis
- lumbar spinal nerves - sacral spinal nerves - coccygeal spinal nerves
! The above three nerves form autonomic nervous
system
335
Lymphatic Drainage of the Pelvis
- Sacral LNs - Internal iliac LNs - External iliac LNs - Lumbar or aortic LNs - Subaortic LNs - Inferior gluteal LNs - Deep inguinal LNs - Superficial inguinal LNs
336
168
1/8/2011
337
338
169
1/8/2011
Blood Vessels of Abdomen & Pelvic Cavity
Abdominal Aorta
Continuation of thoracic aorta Slightly inclinded to the left of median plane Has relations:
A. Anteriorly:- celiac trunk & its branches
- pancreas & splenic vein - left renal vein - 3rd part of duodenum - superior mesenteric vessels - root of mesentery
339
Cont. B. Posteriorly:
- body of upper four lumbar vertebra - intervertebral discs - anterior longitudinal ligament - 2nd to 3rd left lumbar veins
C. On the Right Side
- cisterna chyli & thoracic duct - azygos vein - right crus of diaphragm - inferior vena cava
340
170
1/8/2011
Cont. D. On the Left Side
- Left crus of diaphragm - Duodeno-jejunal flexure - 4th part of doudenum - Inferior mesenteric vessels - Sympathetic trunk
341
Branches of Abdominal Aorta
I. Single branches
Celiac trunk Superior mesenteric artery Inferior mesenteric artery Median sacral artery Inferior phrenic arteries Middle suprarenal arteries Renal arteries Testicular or ovarian arteries Lumbar arteries Common iliac arteries 342
II. Paired branches
171
1/8/2011
343
344
172
1/8/2011
345
Common Iliac Arteries
Formed at the fourth lumbar vertebra Divided into two arteries 1. External iliac artery - larger of the two branches - branches:- inferior epigastric artery - deep circumflex iliac artery - twigs to external iliac LNs - twigs to the psoas major muscle 2. Internal iliac artery - Major supply of the pelvis - Gives parietal and visceral branches 346
173
1/8/2011
Cont. Parietal branches of internal iliac artery include:Iliolumbar artery Lateral sacral artery Obturator artery Superior gluteal artery Inferior gluteal artery Internal pudendal artery
347
348
174
1/8/2011
349
Cont. Visceral branches of internal iliac artery include:Umbilical artery Superior vesical artery Uterine artery Artery of ductus deferens Inferior vesical artery Vaginal artery Middle rectal artery
350
175
1/8/2011
351
Inferior Vena Cava
Formed at the level of L5 vertebra from two common iliac veins Inclinded a bit to the right of median plane Lie behind the right common iliac artery Enter the thorax through vena caval opening Widest vein of the body Relation of the inferior vena cava: A. Anteriorly: - peritoneum in the lower part - 3rd part of duodenum - head of pancreas - lesser sac - liver 352
176
1/8/2011
Cont.
B. Posteriorly: - vertebral column - anterior longitudinal ligament - right sympathetic trunk - right crus of diaphragm - right renal artery - right middle suprarenal artery - right inferior phrenic artery - right suprarenal artery
353
Cont.
C. On the Left side - lower part:- abdominal aorta - upper part:- right crus of diaphragm - caudate lobe of the liver D. On the Right side - lower part:- right ureter - upper part:- right lobe of the liver
354
177
1/8/2011
Tributaries of the Inferior Vena Cava
Common iliac veins Lumbar veins Median sacral veins Renal veins
Right testicular (ovarian) vein Right suprarenal vein Hepatic veins
Inferior phrenic veins
355
356
178
1/8/2011
Cont. Common iliac veins drain blood from:1. external iliac vein 2. internal iliac vein 3. iliolumbar vein 4. lateral sacral vein (some times) 5. median sacral vein (some times to left common iliac vein)
357
Drains blood from pelvic wall & cavity The tributaries include: - superior gluteal vein - inferior gluteal vein - obturator vein - vesical vein - middle rectal vein - uterine vein - internal pudendal vein - lateral sacral vein (some times) - inferior vesical vein (in males)
358
Internal Iliac Veins
179
1/8/2011
Lumbar Plexus
- Formed by ventral rami of (L1 to L4) nerves - Lie within the psoas major muscle - The nerves are connected to the lumbar sympathetic trunk by communicating rami - Formed by L1-L3 and upper part of L4 nerves - Lower part of L4 & whole of L5 together with sacral nerves form lumbosacral plexus
359
Branches of the Lumbar Plexus
1. Iliohypogastric nerve (L1) 2. Ilioinguinal nerve (L1) 3. Genitofemoral nerve (L1,2) 4. Lateral femoral cutaneous nerve (L2,3 posterior division) 5. Femoral nerve (L2,3,4 posterior division) 6. Obturator nerve (L2,3,4 ventral division)
360
180
1/8/2011
Cont.
7. Accessory obturator nerve (L3,4 ventral division):- formed only in 10% of individuals 8. Lumbosacral trunk (L4,5 ventral division) 9. Muscular branches: Quadratus lumborum (T12, L1-4) Psoas minor (L1) Psoas major (L2,3,4) Iliacus (L2,3)
361
362
181
1/8/2011
Sacral Plexus
- Formed by:- lumbosacral trunk (L4,5) & - ventral rami of S1,2,3 & part of S4 - Lies in front of piriformis muscle deep to pelvic fascia - Each ventral ramus receives a grey ramus communicans from sympathetic chains
Branches of the Sacral Plexus
A. From the root of the Plexus 1. Muscular Branches to: Piriformis (S1,2) Levator ani (S4) Coccygeus (S4) Sphincter ani externus (S4) 363
2. Pelvic Splanchnic nerves Arise from S2,3,4 ; small branches Unite with sympathetic pelvic plexus Fibers are preganglionic & relay in ganglia situated in the walls or close to the wall of viscera Represent parasympathetic sacral outflow & supply a. motor to left third of transeverse colon, descending & sigmoid colon & rectum b. Motor fibers to the urinary bladder c. Inhibitory fibers to uterus & uterine tubes d. Vasodilator fibers to erectile tissue of penis & clitoris, testes, ovaries, uterus & uterine tubes
364
Cont.
182
1/8/2011
Cont.
B. From the Ventral Surface of the Plexus i. Nerve to quadratus femoris (L4,5 & S1) ii. Nerve to obturator internus (L5,S1,2) C. From both dorsal & ventral surfaces of the Plexus i. Superior gluteal nerve (L4,5 & S1) ii. Inferior gluteal nerve (L5 & S1,2) iii. Perforating cutaneous nerve (S2,3) iv. Posterior cutaneous nerve of the thigh (S1,2,3)
365
Cont.
E. Terminal Branches
# Sciatic nerve (L4,5 S1,2,3) - Tibial nerve (L4,5 S1,2,3 ventral division) # Pudendal nerve (S2,3,4) - Common peroneal nerve (L4,5 S1,2 dorsal division)
- leave pelvis through greater sciatic foramen - enters the pudendal canal through lesser sciatic foramen
366
183
1/8/2011
367
. Formed by lower part of ventral ramus of S4, S5 & coccygeal nerves
Coccygeal Plexus
. S5 & coccygeal ventral rami come out through the sacral hiatus . Nerves unite in front of coccygeus muscles to form small plexus . Plexus gives anococcygeal nerves which supply: - coccygeus - levator ani - skin on the back of coccyx
368
184
1/8/2011
Celiac Plexus
Has network nerve fibers around celiac trunk Contains two ganglia laterally It is the largest plexus Also called cerebrum of the abdomen Receive fibers from sympathetic trunk, vagus, splanchnic nerves & phrenic nerves Continues caudally as abdominal aortic plexus Give a number of secondary plexus that goes along arteries: 1. Phrenic plexus " to suprarenal gland 2. Hepatic " to liver, gall bladder & bile duct 369
3. Left gastric plexus " to stomach 4. Splenic plexus " to spleen
Cont.
5. Suprarenal plexus " to chromaffin cells of suprarenal 6. Renal plexus " to kidney & upper part of ureter gland
7. Testicular plexus " to testis, epididymis & vas deferens 8. Superior mesenteric plexus " to territory of superior mesenteric artery 9. Abdominal aortic plexus
370
185
Вам также может понравиться
- Demographic Health Ststistic Ethiopia.Документ452 страницыDemographic Health Ststistic Ethiopia.Eshetu EwuОценок пока нет
- P - 3 - Gender Based Violence (GBV) - 2013Документ14 страницP - 3 - Gender Based Violence (GBV) - 2013Mignot AnileyОценок пока нет
- P - 4 - Women Friendly Care - 2013Документ14 страницP - 4 - Women Friendly Care - 2013Mignot AnileyОценок пока нет
- P - 2 - Current Aproaches - 2013Документ40 страницP - 2 - Current Aproaches - 2013Mignot AnileyОценок пока нет
- P - 1 - Aproach To CB Training - 2013Документ24 страницыP - 1 - Aproach To CB Training - 2013Mignot AnileyОценок пока нет
- Worku Antomy and Physiology of Reproductive OrganДокумент206 страницWorku Antomy and Physiology of Reproductive OrganMignot AnileyОценок пока нет
- Anatomy of The Female Pelvis FinalДокумент209 страницAnatomy of The Female Pelvis FinalMignot Aniley86% (14)
- GonddiДокумент49 страницGonddiMignot AnileyОценок пока нет
- Anatomy of The Female PelvisДокумент60 страницAnatomy of The Female PelvisMignot AnileyОценок пока нет
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- CH 15 Excretory-SystemДокумент94 страницыCH 15 Excretory-SystemAntonio Calleja II100% (1)
- Penile CaДокумент76 страницPenile CaUsmle GuyОценок пока нет
- Retrograde Urethrogram - RUGДокумент2 страницыRetrograde Urethrogram - RUGJALIL UR REHMANОценок пока нет
- Sebutkan Anatomi Dari Sistem Perkemihan Menurut Gambar Dibawah IniДокумент19 страницSebutkan Anatomi Dari Sistem Perkemihan Menurut Gambar Dibawah IniAisyia MuktisariОценок пока нет
- MUSCULAR SYSTEM Written ReportДокумент34 страницыMUSCULAR SYSTEM Written Reportpauline cabualОценок пока нет
- كتاب اسئلة جميلДокумент401 страницаكتاب اسئلة جميلMohammadSAL-Rawashdeh100% (1)
- Class Presentation ON BPH: Presented By: Ruchika Kaushal M.Sc. Nursing 1 YearДокумент31 страницаClass Presentation ON BPH: Presented By: Ruchika Kaushal M.Sc. Nursing 1 YearRuchika KaushalОценок пока нет
- MicturitionДокумент7 страницMicturitionOsama MohamedОценок пока нет
- UrethrocystographyДокумент9 страницUrethrocystographyyinyangdongОценок пока нет
- Urological EmergencyДокумент83 страницыUrological EmergencyAlfred LiОценок пока нет
- Types of CathetersДокумент2 страницыTypes of CathetersLorie Fadol100% (1)
- GHSB Lec - Perineum CorrectedДокумент8 страницGHSB Lec - Perineum CorrectedVee ManahanОценок пока нет
- Parts of The Male Reproductive SystemДокумент2 страницыParts of The Male Reproductive SystemEris MolenoОценок пока нет
- Reproductivesystem g10Документ88 страницReproductivesystem g10Mernie Grace DionesioОценок пока нет
- Urinary Bladder & Ureters: DR W Mushiwokufa MBCHB, Mmedsci (Anatomy) Department of Anatomy Msu Faculty of MedicineДокумент27 страницUrinary Bladder & Ureters: DR W Mushiwokufa MBCHB, Mmedsci (Anatomy) Department of Anatomy Msu Faculty of MedicineLeona Tinotenda ManjeruОценок пока нет
- UrinaryДокумент87 страницUrinaryJohn Paolo Dalida SalazarОценок пока нет
- A&P - 2. Functional Anatomy of The Urinary System (9p)Документ9 страницA&P - 2. Functional Anatomy of The Urinary System (9p)Kris GulleyОценок пока нет
- Difference Between Male and Female UrethraДокумент12 страницDifference Between Male and Female Urethradr mezbahemchОценок пока нет
- Male Urethritis With or Without Discharge A ClinicДокумент5 страницMale Urethritis With or Without Discharge A ClinicDian FitriОценок пока нет
- Histologi Saluran KemihДокумент34 страницыHistologi Saluran KemihArif SyahОценок пока нет
- Baileys Table (Important!!!!)Документ8 страницBaileys Table (Important!!!!)shaun lisonОценок пока нет
- Case Study - Urinary Tract InfectionДокумент10 страницCase Study - Urinary Tract InfectionJiffy198867% (3)
- TOPIC# 1 Maternal AnatomyДокумент26 страницTOPIC# 1 Maternal AnatomyRachel CayangaoОценок пока нет
- Bacterial Infections To Humans Chapter 12.3Документ24 страницыBacterial Infections To Humans Chapter 12.3Berdeng ArawОценок пока нет
- MNT in Diseases of Kidney and UrinaryДокумент38 страницMNT in Diseases of Kidney and UrinaryJosephine A. Bertulfo100% (1)
- Background KarunkelДокумент2 страницыBackground KarunkeldatascribdyesОценок пока нет
- PERINEUM and Urogenital Triangle (Lect 18-11)Документ29 страницPERINEUM and Urogenital Triangle (Lect 18-11)Farahh ArshadОценок пока нет
- BPHДокумент34 страницыBPHBryan DorosanОценок пока нет
- Cystoscopy - Mayo ClinicДокумент7 страницCystoscopy - Mayo ClinicSAIFUL ISLAMОценок пока нет
- Anatomy of MicturictionДокумент19 страницAnatomy of MicturictionsalomonmarinaОценок пока нет