Академический Документы
Профессиональный Документы
Культура Документы
Dialysis Notes 1
Загружено:
Kavidu KeshanОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Dialysis Notes 1
Загружено:
Kavidu KeshanАвторское право:
Доступные форматы
DIALYSIS NOTES:
Dialysis is primarily used to provide an artificial replacement for lost kidney function (renal
replacement therapy) due to renal failure
Dialysis works on the principles of diffusion of solute through a semipermeable membrane that
separates two solutions.
Direction of diffusion depends on concentration of solute in each solution.
Rate and efficiency depend on concentration gradient, temperature of solution, pore size of
membrane, and molecular size.
Indications
The decision to initiate dialysis or hemofiltration in patients with renal failure depends on several factors.
These can be divided into acute or chronic indications.
ndications for dialysis in the patient with acute kidney in!ury are"
#etabolic acidosis in situations where correction with sodium bicarbonate is impractical
or may result in fluid overload.
$lectrolyte abnormality, such as severe hyperkalemia, especially when combined with
%&.
nto'ication, that is, acute poisoning with a dialysable drug, such as lithium, or aspirin.
(luid overload not e'pected to respond to treatment with diuretics.
)omplications of uremia, such as pericarditis or encephalopathy.
)hronic indications for dialysis"
*ymptomatic renal failure
+ow glomerular filtration rate (,(R) (RRT often recommended to commence at a ,(R of
less than -./-0 mls1min1-.23m
4
). n diabetics dialysis is started earlier.
Difficulty in medically controlling fluid overload, serum potassium, and1or serum
phosphorus when the ,(R is very low
Goals
Reduce level of nitrogenous waste.
)orrect acidosis, reverse electrolyte imbalances, remove e'cess fluid.
Two main types of dialysis
A. Hemodialysis
5emodialysis removes wastes and water by circulating blood outside the body through an
e'ternal filter, called a dialyzer, that contains a semipermeable membrane
n hemodialysis, the patient6s blood is pumped through the blood compartment of a dialyzer,
e'posing it to a partially permeable membrane.
The dialyzer is composed of thousands of tiny synthetic hollow fibers.
The fiber wall acts as the semipermeable membrane. 7lood flows through the fibers, dialysis
solution flows around the outside the fibers, and water and wastes move between these two solutions.
The cleansed blood is then returned via the circuit back to the body.
8ltrafiltration occurs by increasing the hydrostatic pressure across the dialyzer membrane.
This usually is done by applying a negative pressure to the dialysate compartment of the dialyzer.
This pressure gradient causes water and dissolved solutes to move from blood to dialysate, and
allows the removal of several litres of e'cess fluid during a typical 3 to 0 hour treatment.
*tudies have demonstrated the clinical benefits of dialyzing 0 to 2 times a week, for 9 to : hours.
These fre;uent long treatments are often done at home, while sleeping but home dialysis is a
fle'ible modality and schedules can be changed day to day, week to week.
Types of venos access fo! "emodialysis
-. $'ternal shunt
)annula is placed in a large vein and a large artery that appro'imate each other.
$'ternal shunts, which provide easy and painless access to bloodstream, are prone to
infection and clotting and causes erosion of the skin a round the insertion area.
4. %rteriovenous fistulas or graft
+arge artery and vein are sewn together (anastomosed) below the surface of the skin
(fistula) or subcutaneous graft using the salphenous vein, synthetic prosthesis, or bovine 'enograft
to connect artery and vein.
<urpose is to create one blood vessel for withdrawing and returning blood.
%dvantage is greater activity range than %= shunt and no protective asepsis.
Disadvantage is necessity of two venipunctures with each dialysis.
3. =ein catheterization
(emoral or subclavian vein access is immediate
#ay be short or long term duration.
#omplications d!in$ "emodialysis
-. Dyse;uilibrium syndrome
Rapid removal of urea from blood.
Reverse osmosis, with water moving into brain cells.
)erebral edema
<ossible headache, nausea, vomiting, confusion, and convulsions> usually occurs with
initial dialysis treatments
*horter dialysis time and slower rate minimizes.
4. 5ypotension
Results from e'cessive ultrafiltration or e'cessive antihypertensive medications.
3. 5ypertension
Results from fluid volume overload (water and1or sodium), causing dise;uilibrium
syndrome or an'iety.
?. %rrhythmias
Due to hypotension and rapid removal of potassium.
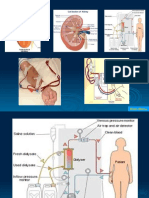
%. &e!itoneal dialysis
&e!itoneal dialysis is a treatment for patients with severe chronic kidney failure
@astes and water are removed from the blood inside the body using the peritoneal membrane as
a natural semipermeable membrane.
@astes and e'cess water move from the blood, across the peritoneal membrane, and into a
special dialysis solution, called dialysate, in the abdominal cavity which has a composition similar to
the fluid portion of blood.
n peritoneal dialysis, a sterile solution containing minerals and glucose is run through a tube into
the peritoneal cavity, the abdominal body cavity around the intestine, where the peritoneal membrane
acts as a semipermeable membrane.
The peritoneal membrane or peritoneum is a layer of tissue containing blood vessels that lines
and surrounds the peritoneal, or abdominal, cavity and the internal abdominal organs (stomach,
spleen, liver, and intestines).
The dialysate is left there for a period of time to absorb waste products, and then it is drained out
through the tube and discarded. This cycle or Ae'changeB is normally repeated ?/0 times during the
day, (sometimes more often overnight with an automated system).
8ltrafiltration occurs via osmosis> the dialysis solution used contains a high concentration of
glucose, and the resulting osmotic pressure causes fluid to move from the blood into the dialysate. %s
a result, more fluid is drained than was instilled.
<eritoneal dialysis is less efficient than hemodialysis, but because it is carried out for a longer
period of time the net effect in terms of removal of waste products and of salt and water are similar to
hemodialysis.
<eritoneal dialysis is carried out at home by the patient.
#omplications of &e!itoneal Dialysis
-. $'cessive loss of fluid can result in hypovolemic shock or hypotension while e'cessive fluid
retention can result in hypertension and edema.
The volume of dialysate removed and weight of the patient are normally monitored> if
more than 0..ml of fluid are retained or a litre of fluid is lost across three consecutive treatments,
the patient6s physician is generally notified.
4. %lso monitored is the color of the fluid removed" normally it is pink/tinged for the initial four cycles
and clear or pale yellow afterwards. The presence of pink or bloody effluent suggests bleeding inside
the abdomen while feces indicates a .
3. The patient may also e'perience pain or discomfort if the dialysate is too acidic, too cold or
introduced too ;uickly, while diffuse pain with cloudy discharge may indicate an infection. *evere pain
in the rectum or perinium can be the result of an improperly placed catheter. The dwell can also
increase pressure on the diaphragm causing impaired breathing, and constipation can interfere with
the ability of fluid to flow through the catheter.
GETTING YO'( )AS#'LA( A##ESS (EADY
Cne important step before starting hemodialysis is preparing a vascular access, a site on your body from
which your blood is removed and returned. % vascular access should be prepared weeks or months
before you start dialysis. t will allow easier and more efficient removal and replacement of your blood with
fewer complications. (or more information about the different kinds of vascular accesses and how to care
for them, see the Dational nstitute of Diabetes and Digestive and &idney Diseases (DDD&) fact
sheet =ascular %ccess for 5emodialysis.
Вам также может понравиться
- Swollen Kidney, (Hydronephrosis) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОт EverandSwollen Kidney, (Hydronephrosis) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОценок пока нет
- TypesДокумент3 страницыTypesProser Faith TabaculdeОценок пока нет
- Dialysis PresentationДокумент21 страницаDialysis PresentationRon Anderson100% (1)
- Hepatorenal Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОт EverandHepatorenal Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОценок пока нет
- Dialysis CompactДокумент16 страницDialysis CompactTue100% (1)
- Hemodialysis 1Документ25 страницHemodialysis 1Jasmine KaurОценок пока нет
- Dialysis PrescriptionДокумент23 страницыDialysis PrescriptionMercy Juliana Jacqualine100% (1)
- Renal Nursing 4 April 2021Документ30 страницRenal Nursing 4 April 2021Benard Were100% (1)
- DIALYSISДокумент7 страницDIALYSISIvy E. LantapeОценок пока нет
- DIALYSIS ProcedureДокумент8 страницDIALYSIS ProcedureRaman SamraoОценок пока нет
- Dialysis DocumentДокумент3 страницыDialysis DocumentLucelle ArellanoОценок пока нет
- Hemodialysi S: Ariane Jake C. Fernandez, RN, MSNДокумент37 страницHemodialysi S: Ariane Jake C. Fernandez, RN, MSNMicah Alexis Candelario100% (3)
- Renal Replacement TherapyДокумент50 страницRenal Replacement TherapyMalueth Angui100% (1)
- DIALYSIS ReportingДокумент10 страницDIALYSIS ReportingGlenelyn Grace InfanteОценок пока нет
- Peritoneal DialysisДокумент23 страницыPeritoneal Dialysismakyofrancis20Оценок пока нет
- Hemodialysis, Phosphorus and Calcium, Peritoneal DialysisДокумент29 страницHemodialysis, Phosphorus and Calcium, Peritoneal DialysisTrizha MaeОценок пока нет
- Dialysis: Notes MS Vol. 2 Krizza Myrrh Gomera Balcita, RNДокумент52 страницыDialysis: Notes MS Vol. 2 Krizza Myrrh Gomera Balcita, RNWhimsey CipresОценок пока нет
- Myths of DialysisДокумент26 страницMyths of DialysisSijo Muthukad M100% (1)
- Complications of DialysisДокумент7 страницComplications of DialysisDilessandro PieroОценок пока нет
- How Does Hemodialysis WorkДокумент19 страницHow Does Hemodialysis WorkMaxence KouessiОценок пока нет
- Dialysis: Dr. Frank EdwinДокумент50 страницDialysis: Dr. Frank EdwinASHRAFQOTMOSH100% (2)
- Dialysis: Edna Co RN ManДокумент37 страницDialysis: Edna Co RN ManMary Shine GonidaОценок пока нет
- Dialysis: Acute Dialysis Is Indicated When There Is A High and Rising Level of SerumДокумент19 страницDialysis: Acute Dialysis Is Indicated When There Is A High and Rising Level of SerumMJ Amarillo100% (1)
- HemodialysisДокумент120 страницHemodialysissigmundmaharajanОценок пока нет
- Peritoneal DialysisДокумент3 страницыPeritoneal DialysisRovefrances ErpeluaОценок пока нет
- Dialysis TermsДокумент2 страницыDialysis TermsmagillaniОценок пока нет
- Peritoneal DialysisДокумент37 страницPeritoneal DialysisEm CastilloОценок пока нет
- Acute Glomerulonep Hritis: By: Edelrose D. Lapitan BSN Iii-CДокумент29 страницAcute Glomerulonep Hritis: By: Edelrose D. Lapitan BSN Iii-CEdelrose Lapitan100% (1)
- Peritoneal DialysisДокумент56 страницPeritoneal DialysisVanet100% (1)
- Peritoneal DialysisДокумент5 страницPeritoneal DialysisJulienne Sanchez-SalazarОценок пока нет
- Hemodialysis Catheter InfectionДокумент38 страницHemodialysis Catheter InfectionKavidu KeshanОценок пока нет
- Principles Dialysis 12-09-3Документ35 страницPrinciples Dialysis 12-09-3cystanarisaОценок пока нет
- Renal Failure PresentationДокумент110 страницRenal Failure PresentationMusa yohana100% (1)
- Fundamentals of DialysisДокумент38 страницFundamentals of DialysisGede Purnawinadi100% (1)
- DIALYSISДокумент30 страницDIALYSISHecel Olita75% (4)
- DialysisДокумент19 страницDialysisSachin Singh100% (2)
- Hemodialysis in ChildrenДокумент28 страницHemodialysis in ChildrenKarna Yuli sitanggangОценок пока нет
- DialyzerДокумент10 страницDialyzerfatima rasheedОценок пока нет
- Hemodialysis: NURSING DIAGNOSIS: Injury, Risk For (Loss of Vascular Access) Risk Factors May IncludeДокумент10 страницHemodialysis: NURSING DIAGNOSIS: Injury, Risk For (Loss of Vascular Access) Risk Factors May IncludeChevelle Valenciano-GaanОценок пока нет
- KDOQI Clinical Practice Guideline Hemodialysis Update - Public Review Draft FINAL - 20150204 PDFДокумент78 страницKDOQI Clinical Practice Guideline Hemodialysis Update - Public Review Draft FINAL - 20150204 PDFศักดิ์ชัย พูนศรีเจริญกุลОценок пока нет
- Dialysis: Duaa Farooq Khan 11634 Amina Bashir 11283 Syed Uzair Iftikhar 13608 Qamar Ud Din 13071Документ11 страницDialysis: Duaa Farooq Khan 11634 Amina Bashir 11283 Syed Uzair Iftikhar 13608 Qamar Ud Din 13071Aimal SafdarОценок пока нет
- Kidney DialysisДокумент80 страницKidney DialysisAhmad Tafish100% (1)
- Peritoneal DialysisДокумент31 страницаPeritoneal Dialysisapi-372245489% (9)
- DialysisДокумент6 страницDialysissakuraleeshaoranОценок пока нет
- How Does Haemodialysis WorkДокумент19 страницHow Does Haemodialysis Workhello_khay100% (1)
- Hemodialysis Adequacy DwiДокумент27 страницHemodialysis Adequacy Dwiryo_ninukОценок пока нет
- Diabetic NephropathyДокумент21 страницаDiabetic NephropathyNugroho HarsonoОценок пока нет
- Dialysis: Cresencio C. Cajigal, Jr. RN, ManДокумент32 страницыDialysis: Cresencio C. Cajigal, Jr. RN, ManMary Jane Avila Bacquial100% (7)
- Haemodialysis in ChildrenДокумент38 страницHaemodialysis in ChildrenValliammalShanmugam75% (8)
- Adequacy of HemodialysisДокумент42 страницыAdequacy of Hemodialysiswael abodiabОценок пока нет
- Complications of DialysisДокумент26 страницComplications of DialysisrlinaoОценок пока нет
- CRRT ProtocolДокумент21 страницаCRRT ProtocolBejo UtomoОценок пока нет
- Renal Failure PresentationДокумент65 страницRenal Failure PresentationBhawna JoshiОценок пока нет
- Ks Module 12Документ29 страницKs Module 12jerinthomasrajanОценок пока нет
- PD (Peritoneal Dialysis) Exit Site CareДокумент35 страницPD (Peritoneal Dialysis) Exit Site CareMarc Pipoy100% (1)
- Anticoagulation in Hemodialysis: Arlene S. Munoz MD, FPCP, FPSNДокумент51 страницаAnticoagulation in Hemodialysis: Arlene S. Munoz MD, FPCP, FPSNBryant MunozОценок пока нет
- DialysisДокумент34 страницыDialysisAntonio Junior CastroОценок пока нет
- What You Should Know About Dialyzer Reuse: A Guide For Hemodialysis Patients and Their FamiliesДокумент8 страницWhat You Should Know About Dialyzer Reuse: A Guide For Hemodialysis Patients and Their FamiliesDewiyanti TodingОценок пока нет
- Dialysis: Hemodialysis (HD) Peritoneal Dialysis (PD)Документ66 страницDialysis: Hemodialysis (HD) Peritoneal Dialysis (PD)joms_pasanoОценок пока нет
- Network11 Cannulation ReportДокумент3 страницыNetwork11 Cannulation ReportKavidu KeshanОценок пока нет
- RTD 025 Rev 5092Документ2 страницыRTD 025 Rev 5092Kavidu KeshanОценок пока нет
- FF ChangeДокумент3 страницыFF ChangeKavidu KeshanОценок пока нет
- Oral Medication and Self-Management in Hemodialysis PatientsДокумент14 страницOral Medication and Self-Management in Hemodialysis PatientsKavidu KeshanОценок пока нет
- Hemodialysis: By: Liana Lee SenciónДокумент14 страницHemodialysis: By: Liana Lee SenciónKavidu KeshanОценок пока нет
- Buttonhole Cannulation of AV Fistulas: Vascular Access GuidelineДокумент14 страницButtonhole Cannulation of AV Fistulas: Vascular Access GuidelineKavidu KeshanОценок пока нет
- Hemodialysis Catheter InfectionДокумент38 страницHemodialysis Catheter InfectionKavidu KeshanОценок пока нет
- Essentials of Anticoagulation in Hemodialysis: Core CurriculumДокумент12 страницEssentials of Anticoagulation in Hemodialysis: Core CurriculumKavidu KeshanОценок пока нет
- Cannulation TrainingGuideДокумент28 страницCannulation TrainingGuideKavidu Keshan100% (1)
- Care of Needling Sites Post Hemodialysis For Fistulas & Grafts (Hemostasis)Документ7 страницCare of Needling Sites Post Hemodialysis For Fistulas & Grafts (Hemostasis)Kavidu KeshanОценок пока нет
- Hemodialysis SOMДокумент6 страницHemodialysis SOMKavidu KeshanОценок пока нет
- Understanding Your Hemodialysis Options EngДокумент16 страницUnderstanding Your Hemodialysis Options EngKavidu KeshanОценок пока нет
- Peritoneal Dialysis: Infections. The Most Common Problem For People Receiving PeritonealДокумент6 страницPeritoneal Dialysis: Infections. The Most Common Problem For People Receiving PeritonealKavidu KeshanОценок пока нет
- DR ShihДокумент3 страницыDR ShihKavidu KeshanОценок пока нет
- AL06136 HemodialysisДокумент2 страницыAL06136 HemodialysisKavidu KeshanОценок пока нет
- Hemodialysis For End-Stage Renal Disease (ESRD) : When Your Kidneys FailДокумент5 страницHemodialysis For End-Stage Renal Disease (ESRD) : When Your Kidneys FailKavidu KeshanОценок пока нет
- Ways Radiation Is Used in Medicine - Cobalt 60 Radiotherapy MachineДокумент22 страницыWays Radiation Is Used in Medicine - Cobalt 60 Radiotherapy MachineKavidu KeshanОценок пока нет
- RUHS Pre PG 2014 MBBS Section I Question Paper and Answer KeyДокумент18 страницRUHS Pre PG 2014 MBBS Section I Question Paper and Answer KeyAnweshaBoseОценок пока нет
- Nursing Case Study (Final) - ArchieДокумент23 страницыNursing Case Study (Final) - ArchieArchie Astorga100% (2)
- NCLEX Review Question 101-200Документ14 страницNCLEX Review Question 101-200Felimon BugtongОценок пока нет
- Important Question of PhysiologyДокумент8 страницImportant Question of PhysiologyRahul Yadav100% (2)
- 2018 Year 11 Human Biology ATAR Course OutlineДокумент21 страница2018 Year 11 Human Biology ATAR Course OutlineNessrynОценок пока нет
- Renal and Genitourinary ConditionsДокумент139 страницRenal and Genitourinary ConditionsjustinahorroОценок пока нет
- Justification For MonetizationДокумент3 страницыJustification For MonetizationCharina Balunso100% (1)
- CRF Fluid Volume Excess NCPДокумент3 страницыCRF Fluid Volume Excess NCPchubbielitaОценок пока нет
- Rarwrrmicroscopic Examination of Urine: RCF 1.118 X 10 XR CMXRPMДокумент13 страницRarwrrmicroscopic Examination of Urine: RCF 1.118 X 10 XR CMXRPMpixiedustОценок пока нет
- Ilocos Kidney Plus Dialysis Center Supply and Medicine Flow ChartДокумент1 страницаIlocos Kidney Plus Dialysis Center Supply and Medicine Flow ChartWyn AgustinОценок пока нет
- Oldage CareДокумент6 страницOldage CareDickson DanielrajОценок пока нет
- Kidney Yang DeficiencyДокумент4 страницыKidney Yang DeficiencynpapadokostasОценок пока нет
- Formulas and DripsДокумент6 страницFormulas and DripsJsohna BelinaОценок пока нет
- Lapsus Dr. DodyДокумент36 страницLapsus Dr. DodyPriscilla Christina NatanОценок пока нет
- Evaluation and Management of HematuriaДокумент12 страницEvaluation and Management of HematuriaCarlos Daniel CruzОценок пока нет
- Wilm's Tumor Pa Tho PhysiologyДокумент1 страницаWilm's Tumor Pa Tho Physiologya_yeLОценок пока нет
- Erc PDFДокумент16 страницErc PDFJosé Luis Conde SalazarОценок пока нет
- Assessment of Renal and Urinary Tract FunctionДокумент19 страницAssessment of Renal and Urinary Tract FunctionokaciaОценок пока нет
- RENALMCQДокумент5 страницRENALMCQkrishnadoctor1Оценок пока нет
- End Stage Renal Disease 2o Hypertensive NephrosclerosisДокумент63 страницыEnd Stage Renal Disease 2o Hypertensive NephrosclerosisGregory LitangОценок пока нет
- 1st Term s3 BiologyДокумент35 страниц1st Term s3 BiologyAdio Babatunde Abiodun CabaxОценок пока нет
- Contoh Soal KMB Ujikom 1Документ34 страницыContoh Soal KMB Ujikom 1RobbyОценок пока нет
- Renal Calculi (Nephrolithiasis) Notes By:Justin Sir: EtiologyДокумент8 страницRenal Calculi (Nephrolithiasis) Notes By:Justin Sir: Etiologygeorgejhon1949Оценок пока нет
- Hamer Conflict DiseaseДокумент2 страницыHamer Conflict DiseasemoninistorОценок пока нет
- Questions For ApmcДокумент15 страницQuestions For ApmcAde AlcarazОценок пока нет
- SCFHS NEPHRO MCQs DR. RANA ZAHID HAFEEZДокумент52 страницыSCFHS NEPHRO MCQs DR. RANA ZAHID HAFEEZranazahidhafeez100% (1)
- Estimated Glomerular Filtration RateДокумент5 страницEstimated Glomerular Filtration Rateseno adi pОценок пока нет
- Acute Kidney Injury: Sarah Abigail C. Ong Siu Second Year ResidentДокумент41 страницаAcute Kidney Injury: Sarah Abigail C. Ong Siu Second Year ResidentSarah Ong SiuОценок пока нет
- Renap Update Pre-Kt - MDJДокумент46 страницRenap Update Pre-Kt - MDJRenalNursesPhОценок пока нет
- Science Workbook (Bones and Muscles)Документ83 страницыScience Workbook (Bones and Muscles)Reinhart LogronioОценок пока нет
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDОт EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDРейтинг: 5 из 5 звезд5/5 (3)
- The Age of Magical Overthinking: Notes on Modern IrrationalityОт EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityРейтинг: 4 из 5 звезд4/5 (30)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeОт EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeРейтинг: 2 из 5 звезд2/5 (1)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)От EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Рейтинг: 3 из 5 звезд3/5 (1)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionОт EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionРейтинг: 4 из 5 звезд4/5 (404)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsОт EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsРейтинг: 4 из 5 звезд4/5 (4)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisОт EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisРейтинг: 4.5 из 5 звезд4.5/5 (42)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsОт EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsРейтинг: 5 из 5 звезд5/5 (1)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsОт EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsОценок пока нет
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedОт EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedРейтинг: 5 из 5 звезд5/5 (81)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsОт EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsРейтинг: 4.5 из 5 звезд4.5/5 (170)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaОт EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.От EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Рейтинг: 4.5 из 5 звезд4.5/5 (110)
- Why We Die: The New Science of Aging and the Quest for ImmortalityОт EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityРейтинг: 4 из 5 звезд4/5 (5)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisОт EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisРейтинг: 5 из 5 звезд5/5 (8)
- Empath: The Survival Guide For Highly Sensitive People: Protect Yourself From Narcissists & Toxic Relationships. Discover How to Stop Absorbing Other People's PainОт EverandEmpath: The Survival Guide For Highly Sensitive People: Protect Yourself From Narcissists & Toxic Relationships. Discover How to Stop Absorbing Other People's PainРейтинг: 4 из 5 звезд4/5 (95)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeОт EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeРейтинг: 4.5 из 5 звезд4.5/5 (253)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessОт EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessРейтинг: 4.5 из 5 звезд4.5/5 (328)
- Summary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedОт EverandSummary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedРейтинг: 4 из 5 звезд4/5 (61)
- The Obesity Code: Unlocking the Secrets of Weight LossОт EverandThe Obesity Code: Unlocking the Secrets of Weight LossРейтинг: 4 из 5 звезд4/5 (6)
- The Marshmallow Test: Mastering Self-ControlОт EverandThe Marshmallow Test: Mastering Self-ControlРейтинг: 4.5 из 5 звезд4.5/5 (60)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesОт EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesРейтинг: 4.5 из 5 звезд4.5/5 (1412)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryОт EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryРейтинг: 4 из 5 звезд4/5 (45)