Академический Документы
Профессиональный Документы
Культура Документы
Peripheral Giant Cell Granuloma: A Case Report and Review of Literature
Загружено:
Alfonsius Jeri0 оценок0% нашли этот документ полезным (0 голосов)
11 просмотров5 страницA case of peripheral giant cell granuloma arising at the left maxillary premolar region in a 18 year old boy is being reported here. The lesion was completely excised upto the periosteum level; there was no residual or recurrence of swelling or bony defect apparent in the area of biopsy after a follow-up period of 1 year.
Исходное описание:
Оригинальное название
pjsr2013v6n2p55
Авторское право
© © All Rights Reserved
Доступные форматы
PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документA case of peripheral giant cell granuloma arising at the left maxillary premolar region in a 18 year old boy is being reported here. The lesion was completely excised upto the periosteum level; there was no residual or recurrence of swelling or bony defect apparent in the area of biopsy after a follow-up period of 1 year.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
11 просмотров5 страницPeripheral Giant Cell Granuloma: A Case Report and Review of Literature
Загружено:
Alfonsius JeriA case of peripheral giant cell granuloma arising at the left maxillary premolar region in a 18 year old boy is being reported here. The lesion was completely excised upto the periosteum level; there was no residual or recurrence of swelling or bony defect apparent in the area of biopsy after a follow-up period of 1 year.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 5
55 Peoples Journal of Scientific Research Vol.
6(2), July 2013
Peripheral Giant Cell Granuloma: A Case Report and Review of Literature
S. Moghe, M.K. Gupta, A. Pillai, A. Maheswari
Department of Oral & Maxillofacial Surgery, Peoples Dental Academy, Peoples University, Bhopal - 462037
(Received January, 2013) (Accepted June, 2013)
Abstract:
Peripheral Giant Cell Granuloma or so called Giant cell epulis is the most common oral giant cell lesion.It usually
presents as a purplish-red soft tissue nodule consisting of multinucleated giant cells in a background of mononuclear
stromal cells and extravasated red blood cells. This lesion probably does not represent a true neoplasm but it may be a
reactive in nature which is believed to be stimulated by local irritation or trauma, but the cause is not known with certainty.
A case of peripheral giant cell granuloma arising at the left maxillary premolar region in a 18 year old boy is being reported
here. The lesion was completely excised upto the periosteum level; there was no residual or recurrence of swelling or bony
defect apparent in the area of biopsy after a follow-up period of 1 year.
Key Words: Peripheral giant cell Granuloma, Epulis.
Introduction:
Peripheral giant cell granuloma (PGCG) is the
most common oral giant cell lesion as a soft tissue
extra-osseous purplish-red nodule. This lesion is
probably not a true neoplasm but could be a reactive in
nature. The initiating stimulus is believed to be due to
local irritation or trauma but the cause is not known
with certainity. It has also been termed as a peripheral
giant cell reparative granuloma; but whether it is in
fact reparative, has not been established and their
osteoclastic activity appears doubtful. Their membrane
receptors for calcitonin, demonstrated by immuno
-histochemistry and their osteoclastic activity when
cultured in vitro are evidence that they are osteoclasts
(Bonetti et al, 1990; Lim & Gibbins 1995; Mighell et al,
1996), whereas other authors have suggested that the
lesion is formed by cells of the mononuclear phagocyte
system(Carvalho et al, 1995). The PGCG bears a close
microscopic resemblance to the central giant cell
granuloma, and hence some pathologists believe that it
may represent a soft tissue counterpart of the central
bony lesion (Katsikeris et al, 1988).
The lesion can be sessile or pedunculated,
penetrating through periodontal membrane and may or
may not be ulcerated. Occasionally lesions arise from
the periosteum overlying edentulous area. Secondary
ulceration due to trauma may give the lesions a focal
yellow zone caused by the formation of fibrin clot over
the ulcer.
---------------------------------------------------------------
Corresponding Author: Dr. Swapnil Moghe, Sr. Lecturer,
Department of Oral & Maxillofacial Surgery, Peoples Dental
Academy, Peoples University, Bhopal - 462037
Phone No. : 07314004613, 918959566485
E-mail : swap2112@gmail.com
Case Report
Lesions can become large, sometimes attaining
a size upto 2 cm. The clinical appearance is similar to
the more common pyogenic granuloma, although the
PGCG is often more bluish-purple as compared with
the bright-red colour of a typical pyogenic granuloma.
Recently, the PGCG associated with dental implants
has been reported (Hirshberg et al, 2003). Although
the PGCG develops within soft tissue, superficial
resorption of the underlying alveolar bony crest is
sometimes seen. On occasion, it may be difficult to
determine whether the mass arose as a peripheral
lesion or a central giant cell granuloma eroding through
the cortical plate into the gingival soft tissues (Chadwick
et al, 1989; Giansanti & Waldrom, 1969).
Rarely a giant cell epulis may be due to
hyperparathyroidism, representing the so-called
osteoclastic brown tumours associated with this
endocrine disorder (Smith et al, 1988; Burkes & White,
1989) and is then likely to be associated with other
lesions in bones and changes in the blood chemistry.
The extra-osseous lesions of cherubism involving the
gingiva appear very similar to giant cell epulide.
However, the other distinctive clinical and radiological
features of cherubism indicate the correct diagnosis
(Odell & Morgan, 1998). Histologically, PGCG is
composed of nodules of multinucleated giant cells in a
background of plump ovoid and spindle-shaped
mesenchymal cells and extravasated red blood cells.
The giant cells may contain only a few nuclei or up to
several dozen. Some of them are large, vesicular nuclei;
others are small, pyknotic nuclei. The origin of the giant
cell is unknown.
56 Peoples Journal of Scientific Research Vol. 6(2), July 2013
Case Report
A 18 year old boy was referred to the
Department of Oral & Maxillofacial Surgery, Peoples
Dental Academy, Bhopal for an non-tender exophytic
lesion in the left maxillary premolar region since May,
2010 (Fig. I). Since then the lesion had gradually
increased in size. It bled from time to time but the patient
did not seek any treatment. The patient had no
significant medical history. The clinical differential
diagnoses included PGCG, pyogenic granuloma and
haemangioma. The excisional biopsy was undertaken
upto the periosteum level under local anaesthesia, and
haemostasis was achieved by electrocautery and
Surgicel. The irritational factor was seen during
exploration of lesion (Fig. III).To prevent recurrence
of tumour, denuded bone was treated with Carnoys
solution. Chlorhexidine mouth rinse was prescribed
post-operatively twice a day for 7 days.
On gross examination, the excised nodule was
red in colour and measured 30 x 20 x 35mm in maximum
dimension. There was periodontal bone loss in the
maxillary left canine region (Fig. II). Due to the
extensive nature of lesion, there was displacement of
maxillary left canine.
Histologically, the overlying epithelium was
composed of aggregates of multinucleated giant cells
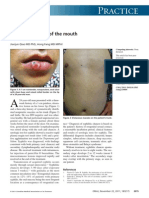
Fig. I: A red exophytic, non-painful lesion arising in the maxillary
left premolar area
Fig. II: Bone loss associated with the lesion, as seen on the occlusal
view.
Fig. I II: Irritational factor as seen during exploration of lesion.
Fig. IV. Photomicrograph showing aggregates of multinucleated giant
cells in a background of mononuclear stromal cells, extravasated
erythrocytes and deposits of haemosiderin (H & E Stain, 100X).
Peripheral Giant Cell Granuloma: A Case Report and Review of Literature ------- S. Moghe, M. K. Gupta, A. Pillai, & A. Maheswari
57 Peoples Journal of Scientific Research Vol. 6(2), July 2013
in a background of mononuclear stromal cells,
extravasated red blood cells and deposits of
haemosiderin (Fig. IV). After a period of 6 months, no
residual or recurrence of swelling or bony defect was
seen. The patient was then referred to the Department
of Prosthodontics and the Department of Periodontics
for a new partial denture and periodontal treatment.
Discussion:
The etiology and nature of PGCG (giant cell
epulide) still remains undecided. In the past, several
hypotheses had been proposed to explain the nature of
multinucleated giant cells, one of them is that they are
osteoclasts left from physiological resorption of teeth
or reaction to injury to periosteum. Now there is a
strong evidence that these cells are osteoclasts as they
have been shown to possess receptors for calcitonin
and were able to excavate bone in vitro (Flanagan et
al 1988).
The study of Lim & Gibbins (1995) confirmed
that the multinucleated giant cells reacted strongly for
a monoclonal antibody (MB1) which reacts with
lymphocytes and a proportion of T cells and monocytes.
The MB1 antibody has previously been shown to be
expressed by osteoclasts in fetal bone. Interestingly,
the re-expression of the blood vessels in the lesion for
the widely used endothelial cell marker factor VIII
related antigen had failed to demonstrate the presence
of blood vessels other than on the periphery of the
lesion although these lesions appear to be extremely
vascular in nature.
There is also a growing body of opinion that
giant cells may simply represent a reactionary
component of the lesion and are derived via blood
stream from bone marrow mononuclear cells and may
be present only in response to an yet unknown stimulus
from the stroma. This concept is based on the results
of some more recent studies using cell culture and
transplantation (el Mofty & Osdoby, 1985; Cohen et
al, 1988) in which the giant cells have been found to be
short lived and to disappear early in culture in contrast
to the active proliferation of the stromal cells.
A study by Wulling et al (2001) revealed that
the stromal cells secrete a variety of cytokines and
differentiation factors, including Monocyte chemo-
attractant protein-1 (MCP1), Osteoclast differentiation
factor (ODF), and Macrophage-colony stimulating
factor (M-CSF). These molecules are monocyte
chemo-attractants and are essential for osteoclast
differentiation, this suggest that the stromal cell
stimulates blood monocyte immigration into tumour
tissue and enhances their fusion into osteoclast like
multinucleated giant cells. Further more, the recently
identified membrane-bound protein family a disintegrin
and metalloprotease (ADAM) is considered to play a
role in the multinucleation of osteoclasts and
macrophage derived giant cells from mononuclear
precursor cells (Abe et al, 1999).
In a recent study by Liu et al (2003), in situ
hybridization was carried out to detect the mRNA
expression of the receptor activator of NF-kappaB
ligand (RANKL), that is shown to be essential in the
osteoclastogenesis, its receptor RANKL and its decoy
receptor osteopritegrin (OPG). They concluded that
RANKL and OPG expressed in these lesions may play
on important role in the formation of multinucleated
giant cells.
There are no pathognomonic clinical features
whereby these lesions can be differentiated from other
forms of gingival enlargement including pyogenic
granuloma, fibrous epulis, peripheral ossifying fibroma,
inflammatory fibrous hyperplasia, peripheral
odontogenic fibroma, hemangiomacaverosum and
papilloma. Microscopic examination is required for the
definitive diagnosis(Carranza & Hogan, 2012;
Chaparro-Avendano et al, 2005).
Generally, this lesion is clinically indistingui-
shable from a pyogenic granuloma, although a PGCG
is more likely to cause bone resorption than pyogenic
granuloma, the differences are otherwise minimal
(Regezi et al, 2008). Microscopically, the lesion arises
from, or is at least attached to the periodontal ligament
or mucoperiosteum. The most characteristic
histological features include a non-encapsulated highly
cellular mass with abundant giant cells, inflammation,
interstitial hemorrhage, hemosiderin deposits and
mature bone or osteoid.
Fibroblasts are the basic element of peripheral
giant cell granulomas. Scattered among the plump,
young fibroblasts are numerous multinucleated giant
cells with abundant eosinophilic cytoplasm which
appear to be non-functional in the usual sense of
phagocytosis and bone resorption(Regezi et al, 2008).
Two types of giant cells are mainly found, one
representing metabolically active cells (Type I) and
the other representing dying cells (Type II). The origin
of these cells has not been defined yet. However, a
striking similarity between these cells and osteoclasts
does exist (Katsikeris et al, 1988). Both the type of
Peripheral Giant Cell Granuloma: A Case Report and Review of Literature ------- S. Moghe, M. K. Gupta, A. Pillai, & A. Maheswari
58 Peoples Journal of Scientific Research Vol. 6(2), July 2013
cells consists of multiple, large, ovoid, vesicular,
somewhat translucent nuclei with prominent nucleoli
and the nuclear chromatin was located peripherally
on distinct nuclear membrane. Type I cells vary in
size, often exceeding 100 in diameter.The type II
cells are fewer in number, have smaller and more
irregular nuclei than type I. The nucleoli are not easily
seen and the cytoplasm stains deeply eosinophilic and
granular than the type I cells (Bhaskar et al, 1971).
Despite ultrastructural studies, the true nature
of the giant cells in PGCG remains debatable (Bonetti
et al, 1990).Inflammation is a constant finding but is
varied not only in degree but also in location. The
inflammatory cells consist primarily of lymphocytes,
plasma cells, histiocytes and occasional
polymorphonuclear cells. Rarely, ulceration was an
associated feature (Bhaskar et al, 1971).
Vascular proliferation, especially capillary, was
found in a study of Peralles et al (2006). Calcified tissue
which is found in some of the lesions varying from
small amorphous foci to well developed trabeculae
(Bhaskar et al, 1971). The woven bone or lamellar bone
is thought to be produced by mononuclear stromal cells,
which resemble latent proliferative osteoblasts or
osteoprogenitor cells. Thus, it is not surprising that
woven bone and lamellar bone are formed in PGCG
(Dayan et al, 1990). No correlation was found between
amount of bone with location or reported duration of
the lesion (Giansanti & Waldron, 1969). The histologic
appearance is similar to that of a giant cell granuloma
of the jaw, but for the fact that the epulis has a covering
of stratified squamous epithelium (Regezi et al, 2008).
In rare instances, both a soft tissue and intraosseous
lesion can co-exist. The overlying mucosal surface is
ulcerated in about 50% cases. A clear zone of dense
fibrous connective tissue usually separates the giant
cell proliferation from the mucosal surface (Neville et
al, 2009).
Treatment consists of local surgical excision
down to the underlying bone, for extensive clearing of
the base (Neville et al, 2009).Removal of local factors
or irritants is also required(Regezi et al, 2008). If
resection is only superficial, the growth may recur.
Exposure of all bony walls following thorough surgical
resection responds satisfactorily most of the times.
Recurrence rate of 5.0-70.6% (average 9.9%) has
been reported in various epidemiologic studies (Mighell
et al, 1996).
A recurrence rate of 5% has been reported
by Giansanti & Waldron (1969). Recurrence is believed
to be related to lack of inclusion of the periosteum or
periodontal ligament in the excised specimen (Regezi
et al, 2008). A re-excision must be performed for these
cases (Neville et al, 2009). Aggressive tendencies or
malignant transformation of these lesions has never
been reported (Katsikeris et al, 1988). The treatment
rendered in this case was surgical excision to the bone,
chemical cauterization and curettage followed by oral
prophylaxis.The 1 year follow-up has shown no
recurrence indicating that the given treatment along
with maintenance of a good oral hygiene is sufficient
to treat PGCG.
References:
1. Abe E, Mocharla H, Yamate T, Taguchi Y. Monolages
SC: Meltrin-alpha, a fusion protein involved in
multinucleated giant cell and osteoclast formation.
Calcified Tissue International, 1999;64(6): 508-515.
2. Bhaskar SN, Cutright DE, Beasley JD, Perez B: Giant cell
reparative granuloma (peripheral): report of 50 cases.
Journal of Oral Surgery, 1971;29(2):110-115.
3. Bonetti F, Pelosi G, Martignoni G, Mombello A, Zamboni
G, Pea M, Scarpa A, Chilosi M: Peripheral giant cell
granuloma: evidence for osteoclastic differentiation.
Oral Surgery, Oral Medicine & Oral Pathology,
1990;70(4): 471-475.
4. Burkes EJ (J r.), White RP (Jr.): A peripheral giant-cell
granuloma manifestation of primary hyperpara-
thyroidism: report of case. Journal of the American
Dental Association, 1989;118(1): 62-64.
5. Carranza FA, Hogan EL: Peridontal Pathology-Gingival
Enlargements. In: Carranzas Clinical Periodontology.
MG Newman, H Takei, PR Klokkevold, RA Rarranga
(Eds.); 10
th
Edn.; Elsevier Saunders, St Louis; 2012.pp.84-
95.
6. Carvalho YR, Loyola AM, Gomez RS, Araujo VC:
Peripheral giant cell granuloma. An immuno-
histochemical and ultrastructural study. Oral Diseases,
1995;(1)1: 20-25.
7. Chadwick BL, Crawford PJ , Aldred MJ: Massive giant
cell epulis in a child with familial cyclic neutropenia.
British Dental Journal, 1989;16(8):279-281.
8. Chaparro-Avendano AV, Berini-Ayts L, Gay-Escoda C:
Peripheral giant cell granuloma. A report of five cases
and review of literature. Medicina Oral, Patologia, Oral
& Cirugia Buccal, 2005;10(1): 48-52.
9. Cohen MA, Grossman ES, Thompson SH: Features of
central giant cell granuloma of the jaws xenografted in
nude mice. Oral Surgery, Oral Medicine & Oral
Pathology, 1988;66(2): 209-217.
10. Dayan D, Buchner A, Spirer S: Bone formation in
Peripheral giant cell granuloma. Journal of
Periodontology, 1990; 61(7): 444-446.
Peripheral Giant Cell Granuloma: A Case Report and Review of Literature ------- S. Moghe, M. K. Gupta, A. Pillai, & A. Maheswari
59 Peoples Journal of Scientific Research Vol. 6(2), July 2013
Source of Support : Nil.
Conflict of Interest: None declared.
11. Eversole LR, Rovin S: Reactive lesions of the gingiva.
Journal of Oral Pathology, 1972;1(1):30-38.
12. el-Mofty SK, Osdoby P: Growth behavior and lineage of
isolated and cultured cells derived from giant cell
granuloma of the mandible. Journal of Oral Pathology,
1985;14(7):539-552.
13. Flanagan AM, Nui B, Tinkler SM, Horton MA, Williams
MD, Chambers DJ : The multinucleated giant cell
granulomas of the jaws are osteoclasts. Cancer,
1988;62(6):1139-1145.
14. Giansanti J S, Waldron CA: Peripheral giant cell
granuloma: review of 720 cases. Journal of Oral Surgery,
1969;17(10):787-791.
15. Hirshberg A, Kozlovsky A, Schwartz-Arad D, Mardinger
O, Kaplan I: Peripheral giant cell granuloma associated
with dental implants. Journal of Periodontology,
2003;74(9):1381-1384.
16. Katsikeris N, Kakarantza-Angelopoulou E, Angelopoulos
AP: Peripheral giant cell granuloma. Clinicopathologic
study of 224 new cases and review of 956 reported cases.
International Journal of Oral Maxillofacial Surgery,
1988;17(2):94-99.
17. Lim L, Gibbins JR: Immunohistochemical and ultra
structural evidence of a modified microvasculature in
the giant cell granuloma of the jaws. Oral Surgery, Oral
Medi ci ne, Oral Pathology, Oral Radi ology &
Endodontics, 1995;79(2):190-198.
18. Liu B, Yu SF, Li TJ: Multinucleated giant cells in various
forms of giant cell containing lesions of the jaws express
features of osteoclasts. Journal of Oral Pathology &
Medicine, 2003; 32(6):367-375.
19. Mighell AJ, Robinson PA, Hume WJ: PCNA and Ki-67
immunoreactivity in multinucleated cells of giant cell
fibroma and peripheral giant cell granuloma. Journal of
Oral Pathology & Medicine, 1996; 25(5):193-199.
20. Neville B, Allen CM, Damm DD, Bouquot JE: Soft Tissue
Tumors. In: Oral and Maxillofacial Pathology. 3
rd
Edn.;
Elsevier Saunders, St. Louis; 2009.pp.507-563.
21. Odell EW, Morgan PR: Biopsy Pathology of the Oral
Tissues (Biopsy pathology series 22). Chapman & Hall
Medical, London, 1998.pp. 486.
22. Peralles PG, Viana APB, Azevedo ALR, Pires FR: Gingival
and alveolar hyperplastic reactive lesions:
clinicopathological study of 90 cases. Brazilian Journal
of Oral Sciences, 2006; 5(18):1085-1089.
23. Regezi J A, Sciubba J J , Jordan RCK. Red-Blue lesions:
In: Oral Pathology: Clinical Pathologic Correlations. 5
th
Edn.; Elsevier Saunders, St. Louis; 2008.pp.107-125.
24. Smith BR, Fowler CB, Svane TJ : Primary
hyperparathyroidism presenting as a peripheral giant
cell granuloma. Journal of Oral & Maxillofacial Surgery,
1988;46(1): 65-69.
25. Wulling M, Engels C, Jesse N, Werner M, Delling G, Kaiser
E: The nature of giant cell tumor of bone. Journal of
Cancer Research & Clinical Oncology, 2001;127(8): 467-
474.
Peripheral Giant Cell Granuloma: A Case Report and Review of Literature ------- S. Moghe, M. K. Gupta, A. Pillai, & A. Maheswari
Вам также может понравиться
- Perawatan Ortodonti Dengan Menggunakan Sistem Damon: (Orthodontic Treatment With Damon System)Документ1 страницаPerawatan Ortodonti Dengan Menggunakan Sistem Damon: (Orthodontic Treatment With Damon System)Alfonsius JeriОценок пока нет
- Dentj 38 2 02Документ4 страницыDentj 38 2 02Alfonsius JeriОценок пока нет
- Jurnal-4-Naskah 5 JURNAL PDGI Vol 59 No 3Документ5 страницJurnal-4-Naskah 5 JURNAL PDGI Vol 59 No 3Alfonsius JeriОценок пока нет
- Restoring Proximal Caries Lesions Conservatively With Tunnel RestorationsДокумент8 страницRestoring Proximal Caries Lesions Conservatively With Tunnel RestorationsAlfonsius JeriОценок пока нет
- Case Report: DiscussionДокумент2 страницыCase Report: DiscussionAlfonsius JeriОценок пока нет
- Third Molar ControversyДокумент8 страницThird Molar ControversyAlfonsius JeriОценок пока нет
- Practice: Syphilitic Chancre of The MouthДокумент1 страницаPractice: Syphilitic Chancre of The MouthAlfonsius JeriОценок пока нет
- EAPD Guidelines For The Use of Pit and Fissure Sealants: R. Welbury, M. Raadal, N.A. LygidakisДокумент6 страницEAPD Guidelines For The Use of Pit and Fissure Sealants: R. Welbury, M. Raadal, N.A. LygidakisAlfonsius JeriОценок пока нет
- Fissure SealantДокумент2 страницыFissure SealantAlfonsius JeriОценок пока нет
- GTSL Akrilik GTKL: Basis Konektor Retainer Sadel Anasir GTДокумент1 страницаGTSL Akrilik GTKL: Basis Konektor Retainer Sadel Anasir GTAlfonsius JeriОценок пока нет
- Oral Candidiasis:: Clinical Manifestations, Diagnosis, and TreatmentДокумент0 страницOral Candidiasis:: Clinical Manifestations, Diagnosis, and TreatmenttristiarinaОценок пока нет
- Pen TingДокумент32 страницыPen TingAlfonsius JeriОценок пока нет
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5795)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Tmod Vignette CurrentДокумент33 страницыTmod Vignette CurrentIsabelle MoscardiniОценок пока нет
- Immunology & Serology: Safety and Specimen PreparationДокумент25 страницImmunology & Serology: Safety and Specimen PreparationChristian John V. CamorahanОценок пока нет
- Connective TissueДокумент26 страницConnective TissueooiszehuiОценок пока нет
- Biomaterials in OrthepadicsДокумент455 страницBiomaterials in OrthepadicsDeva Raj100% (2)
- In Ammation and Tumor Progression: Signaling Pathways and Targeted InterventionДокумент46 страницIn Ammation and Tumor Progression: Signaling Pathways and Targeted Interventionenkiyna archОценок пока нет
- Granulation Tissue 13102015Документ33 страницыGranulation Tissue 13102015Widi Widurai100% (1)
- Blood: Types of Blood Cells and Their Average NumberДокумент32 страницыBlood: Types of Blood Cells and Their Average NumberSumayya KabeerОценок пока нет
- DEngue FlowchartДокумент2 страницыDEngue FlowchartJelly Cruz100% (3)
- KRV, PLAZMA, HEMATOPOEZAДокумент35 страницKRV, PLAZMA, HEMATOPOEZASinisa RisticОценок пока нет
- Acute Coronary SyndromesДокумент879 страницAcute Coronary SyndromesDiana PepineОценок пока нет
- Inform Consent HIVДокумент465 страницInform Consent HIVHartini100% (2)
- Chemical Mediators of Acute Inflammation 2Документ41 страницаChemical Mediators of Acute Inflammation 2Sashika Tharindu100% (1)
- Inflammation Questions: Dr. Abdullah Al-Samawi Professor of PathologyДокумент147 страницInflammation Questions: Dr. Abdullah Al-Samawi Professor of PathologyAhmed AzeezОценок пока нет
- Macrofagos Asociados A TumoresДокумент9 страницMacrofagos Asociados A Tumoresjuan ramon zepeda tejedaОценок пока нет
- Innate ImmunityДокумент16 страницInnate ImmunityikhaОценок пока нет
- Microbiology 1st Semeter BSN Mcqs by RCN, Educational PlatformДокумент10 страницMicrobiology 1st Semeter BSN Mcqs by RCN, Educational PlatformPrince Masroor Ali AbroОценок пока нет
- Pathophysio DengueДокумент1 страницаPathophysio DengueDANICA BONBONОценок пока нет
- I - BloodДокумент9 страницI - BloodKim NgọcОценок пока нет
- Gleeson 2011Документ9 страницGleeson 2011Jerônimo CoelhoОценок пока нет
- Vitreoscilla Filiformis Extract For 2021Документ13 страницVitreoscilla Filiformis Extract For 2021kdsmphОценок пока нет
- List of PH.D Thesis at IvriДокумент21 страницаList of PH.D Thesis at IvriMuguo Mouafo BriceОценок пока нет
- Dengue Hemorrhagic Fever Pathophysiology DiagramДокумент4 страницыDengue Hemorrhagic Fever Pathophysiology DiagramAni MarlinaОценок пока нет
- Avian Histophatology, 4th Edition (VetBooks - Ir) PDFДокумент664 страницыAvian Histophatology, 4th Edition (VetBooks - Ir) PDFAnn Tyshkivska100% (4)
- Macrophages: Development and Tissue Specialization: Chen Varol, Alexander Mildner, and Steffen JungДокумент35 страницMacrophages: Development and Tissue Specialization: Chen Varol, Alexander Mildner, and Steffen JungGustavo VilcapazaОценок пока нет
- Clinical Serology and Immunology by StevensДокумент611 страницClinical Serology and Immunology by StevensAlexandr TrotskyОценок пока нет
- Describe The Principles of Blood Cell MaturationДокумент11 страницDescribe The Principles of Blood Cell MaturationnotsoninjaninjaОценок пока нет
- ISCB ProtocolДокумент55 страницISCB ProtocoloffbeОценок пока нет
- Inosine Pranobex: Drug EvaluationДокумент42 страницыInosine Pranobex: Drug EvaluationCarolina GómezОценок пока нет
- Molecular and Cellular Endocrinology: EditorialДокумент2 страницыMolecular and Cellular Endocrinology: EditorialSheila GouveiaОценок пока нет
- Hematopoiesis: Part 2: Erythropoiesis and LeukopoiesisДокумент62 страницыHematopoiesis: Part 2: Erythropoiesis and LeukopoiesisJohn Marie IdavaОценок пока нет