Академический Документы
Профессиональный Документы
Культура Документы
Desquamative Gingiva
Загружено:
Dewi FOrtyuna0 оценок0% нашли этот документ полезным (0 голосов)
18 просмотров5 страницTidak hanya proses destruksi oleh S.mutans dan produksi membran abses saja yang terjadi pada peristiwa pembentukan abses ini, tapi juga ada pembentukan pus oleh bakteri pembuat pus (pyogenik), salah satunya juga adalah S.aureus. jadi, rongga yang terbentuk oleh sinergi dua kelompok bakteri tadi, tidak kosong, melainkan terisi oleh pus yang konsistensinya terdiri dari leukosit yang mati (oleh karena itu pus terlihat putih kekuningan), jaringan nekrotik, dan bakteri dalam jumlah besar.
Оригинальное название
desquamative gingiva
Авторское право
© © All Rights Reserved
Доступные форматы
PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документTidak hanya proses destruksi oleh S.mutans dan produksi membran abses saja yang terjadi pada peristiwa pembentukan abses ini, tapi juga ada pembentukan pus oleh bakteri pembuat pus (pyogenik), salah satunya juga adalah S.aureus. jadi, rongga yang terbentuk oleh sinergi dua kelompok bakteri tadi, tidak kosong, melainkan terisi oleh pus yang konsistensinya terdiri dari leukosit yang mati (oleh karena itu pus terlihat putih kekuningan), jaringan nekrotik, dan bakteri dalam jumlah besar.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
18 просмотров5 страницDesquamative Gingiva
Загружено:
Dewi FOrtyunaTidak hanya proses destruksi oleh S.mutans dan produksi membran abses saja yang terjadi pada peristiwa pembentukan abses ini, tapi juga ada pembentukan pus oleh bakteri pembuat pus (pyogenik), salah satunya juga adalah S.aureus. jadi, rongga yang terbentuk oleh sinergi dua kelompok bakteri tadi, tidak kosong, melainkan terisi oleh pus yang konsistensinya terdiri dari leukosit yang mati (oleh karena itu pus terlihat putih kekuningan), jaringan nekrotik, dan bakteri dalam jumlah besar.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 5
Periodontics
Desquamative gingivitis: A clinical, histopathoiogic, and
immunologie study
A- K.. Markopoulos*/D. Antoniades*/P. Papanayotou*/G. Trigonidis*
Abstract
Desquamative gingivitis is believed to be a clinical sign of certain mucocutaneous
diseases rather than a distinct pathologic entity. The prevalence of desquamative
gingivitis was studied in a group of patients with the most common mucocutaneous
diseases. Of 414 patients with pemphigus vulgaris. mucous membrane
pemphigoid, or oral lichen planus. 49 (1.8%) exhibited gingival lesions in the
form of desquamative gingivitis. Desquamative gingivitis was most prevalent in the
patients with mucous membrane pemphigoid (41.6%) followed by those with
pemphigus vulgaris (9.1%). Other elinieal characteristics, as well as histo-
pathoiogic and imtnunohistochemical findings, that aid in early diagnosis are
presented. (Quintessence Int 996:27:763-767.')
Clinical relevance
Desquamative gingivitis, in most cases, represents a
manifestation of systemic diseases. Because it has no
specific clinical pathognomonic features, laboratory
aids, such as histopathoiogic and immunohistochem-
ical examination, should be used to unmask the
underlying disease so that the appropriate treatment
can be provided.
Introduction
Desquamative gingivitis (DG) is characterized by
erythematous and desquamative lesions of the free and
attached gingiva. The condition was first described by
Tomes and Tomes' in 1894 and was further defined
several years later by Prinz^ and Merrit,^ who pro-
posed the term chronic diffuse desquamative gingivitis.
UsuaUy the changes are confined to the labial
gingival mueosa, which varies from bright to dark red
and is edematous. Tbe epithelium is quite friable and
can be removed easily from the underlying connective
tissue, leaving a red surface that bleeds readily after
minimal trauma. Other gingival sites, such as palatal
and lingual surfaces, are rarely involved,"*
The etiology of DG remains obscure. Early investi-
gators believed that there was a single cause. McCarthy
et al^ were among the first who proposed that DG is a
nonspecific reaction pattern that can be associated
with any one of several diseases or conditions. This
group suggested that dermatologie diseases, hormonal
factors, aging, metabolic disturbances, irdtational
factors, and chronic infections could cause DG,
However, in recent years, it has been shown that the
great majority (approximateiy 75%) of cases of DG are
manifestations of mucocutaneous diseases, primarily
mucous membrane pemphigoid (MMP), oral lichen
planus (OLP), and pemphigus vulgaris (PV).'''^"'''
In the present investigation, the prevalence of DG
was retrospectively studied in a large group of patients
with these mucocutaneous diseases. Furthermore the
clinical, histopathoiogic, and immunologie features in
each disease group were analyzed.
' Department of Oral Medicine and Pathology, Aristotle University of
Thessaloniki, School of Dentistry, Thessaloniki, Greece.
Reprint requests: Dr A. K. Markopoulos, Department of Oral Medicine
and Pathology, Aristotle University ofThessaloniki, School of Dentistry,
Thessaloniki 54006, Greece.
Method and materials
The records of all patients with PV, MMP, and OLP
who were seen during the period from Januari' 1983 to
Quintessence Intemalional Volume 27, Number 11/1996 763
Markopoulos et al
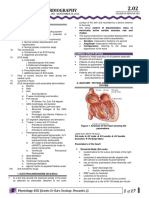
Fig 1 Desquamalive gingivitis in a palien! with pemphigus.
Areas o erosion are seen.
Fig 2 Desquamalive gingivitis in a patient with mucous
membrane pemphigoid.
Fig 3 Desquamalive gingivitis in a patient wiih oral lichen
planus.
January 1993 in the Oral Medicine Clinic were
retrieved from the files ofthe Oral Pathology Depart-
ment. A total of 414 cases were studied. Each file was
examined carefully for documentation of DG, The
final diagnosis was established on the basis of clinical,
histopathologic, and immunohistochemical criteria.
From the clinical point of view, only t>pical patients
with severe lesions were included in the study. Typical
patients were considered to be those presenting with
bright to dark red, edematous, and friable gingival
mucosa, Tlie patients were subjected to careflii phy-
sical examination, including slit-lamp examination,
laryngoscopy, and examination of the ear canal,
anogenital area, and skin.
The histologie slides were stained with hematoxylin
and eosin. The major criteria for the histopathologic
diagnosis of each mucocutaneous disease category
were acantholysis and intraepithelial ciefting forma-
tion for PV; subepithelial bulla formation for MMP;
and hydropic degeneration of the basal layer of the
epithelium with bandiike lymphocytic infiltration of
the upper lamina propria for OLP.
The immunohistochemical slides had been stained
with a streptavidin-biotin immunoperoxidase tech-
nique using polycional antibodies for the demonstra-
tion of immunoglobulin G (IgG), immunoglobulin A
(IgA), immunoglobulin M (IgM). and complement
(C3) on paraffin-embedded tissues (Immunostain
Diagnostic Products, Lianbaris), Direct immuno-
fluorescence had also been performed on fresh tissues
for the demonstration of fibrin-fibrinogen. The major
immunologie criteria that we used were the following;
intercellular deposition of IgG and IgA at the epithe-
lial surface for PV; deposition of IgG and IgA in the
linear basement membrane for MMP; nonspecific
immunohistochemical staining of IgG and IgA for
OLP; and deposition of IgM and fibrin-fibrinogen for
OLP.
Results
An interim clinical diagnosis ofthe underlying disease
in DG patients was based on the presence of erythema-
tous and friable gingival mucosa or on the occasional
presence of accompanying clinical matufestations of
each disease in other sites of the oral mucosa; the
presence of vesiculoerosive lesions and Nikolsky's
sign, which are indicative of PV and MMP, or the
presence of laceiike white lesions combined with
erosions or atrophie mucosa, which are suggestive of
erosive or atrophie OLP.
764
Quintessence International Volume 27, Number 11/1996
Markopoulos et al
Table ! Prevalence of desquamative gingivitis ( DG) in 414 patients with mucosal disease
Underlying
disease
Pemphigus vulgaris
Mucous membrane
pemphigoid
Oral lichen
plan us
Idiopathic
Total
No. of
patients
33
53
326
2
414
Patients
witb DG
No.
3
22
22
2
49
(%)
( 9.1)
( 41.6)
{ 6.8)
(100,0)
( 11.8)
Male
No,
1
4
6
1
11
(%)
(33.3)
(18.2)
(27.3)
(50,0)
(23.4)
Female
No.
2
18
16
1
36
(%)
(66.7)
(81,8)
(72,7)
(50.0)
(76.6)
Mean age of
patients with
DG
37.7 y
55,1 y
50,0 y
45.4 y
47.1 y
No. of patients
with mucosal
lesions in other
oral sites
1
8
12
0
21
Tabie 2 Immunohistochemical findings in biopsy specimens taken from patients with desquamative gingivitis
Und e dying
disease
Pemphigus vulgaris
Mucous membrane
pemphigoid
Oral lichen
planus
Idiopathic
' Nol performed.
No. of
patients
3
22
22
2
Streptavidin-biotin immunoperoxidase
staining
Positive
IgG IgA
3 3
17 16
IgM
1
4
10
C3
3
16
IgG
5
22
2
Nei
IgA
6
22
2
native
IgM
2
18
12
2
C3
6
22
2
Direct immunouorescence
for fibrinogen
Positive Negative
19 3
The DG lesions were confined to the labial gingiva,
which appeared bright to dark red and edematous
(Figs 1 to 3). Accompanying lesions were found
mainly in patients with OLP (12 of 22) (Table 1).
Thorough physical examination oft he patients did not
reveal any extraora! manifestations. Pain was a pre-
dominant symptom in many patients, while the pre-
sence of local factors, such as plaque or dental
calculus, was evident in the majority of patients in each
group.
On the basis of histopathologic and immunohisto-
chemical examination the 49 DG patients were
divided into four categories; P y MMP. OLP, and
idiopathic cases. Histopathologicaily. 47 patients ful-
filled the classic criteria for PV, MMP, or OLP (Table
2). Two parients did not manifest specific microscopi-
cally pathognomonic features, and therefore their
cases were considered idiopathic. All the patients with
PV were positive for IgG and IgA. while parients with
MMP were found positive for IgG and IgA to a lesser
extent (17 of 22 patients). In contrast all patients with
OLP were negative for IgG and IgA. and some were
posirive for IgM and fibrin-fibrinogen. The idiopathic
cases were negative in all the immunohistochemical
stainings that were performed. The immunohistochem-
ical findings are illustrated in Figs 4 to 6.
Table 1 reveals that the majority of parients with DG
have MMP (41.6%). while 9.1% and 6,8% have PVand
OLP, respectively. The great majority oft he patients in
all disease groups were female.
Discussion
The clinical appearance of DG is not pathognomonic.
Therefore, supplementary procedures, such as histo-
pathologic examination and immunohistochemical
tests of gingival biopsy specimens, are necessary for a
definitive diagnosis. In the present study, one of the
Quintessence Intemational Volume 27, Number 11/1996
765
Markopouios et ai
Fig 4 Desquamative gingivitis m pemphigus. Intercellular
deposition ol igG is apparent (Streptavidin-biotin staining,
originai magnification x480.1
Fig 5 Desquamative gingivifis in mucous membrane pem-
phigoid. The linear basemenf membrane exhibifs deposits
of IgG (Sfreptavidin-biotin sfaining; originai magnificafion
Fig 6 Desquamative gingivitis in orai lichen pianus. Direct
immunofluorescence discloses the presence of fibrinogen
along the basemenf membrane zone. (Original magnifica-
fion x120.)
few clinical characteristics beyond the erythematous
atid friable gingiva was the occasional presence of
accompanying lesions in other sites ofthe oral mucosa.
These lesions were more frequently observed in
patients with OLP. Twelve of 22 patients manifested
lacelike white formations combined with erosive or
atrophie lesions in other sites of their oral mucosa.
The highest prevalence of DG (41.6%) was ob-
served in patients with MMP. Eight of 22 of these
patients had vesiculoerosive lesions in other sites of
the oral mucosa.
A lower prevalence of DG (9.1%) was observed in
patients with PV One ofthe three DG patients in this
group had vesiculoerosive lesions in other sites of his
oral mucosa. Nikolsky's sign (ie, the detachment of
epithelium after mild rubbing with a cotton tip) was
positive in these lesions.
The lowest prevalence of DG( 6.8%) was counted in
the OLP group. Erosive or atrophie lesions accom-
panied the gingivai desquamation in 12 of 22 patients,
suggesting that erosive and atrophie forms are the most
common forms of OLP to be the underlying disease in
DG, Similar findings have been repotied by Daniels
and Quadra-White'^ and Jadinski and Shklar.'^
No underlying disease was detected in two patients,
and therefore their cases were considered idiopathic.
Microscopic examination ofthe oral biopsy speci-
mens revealed the classic histopathologic changes for
MMP, Py and OLP, The two idiopathic cases mani-
fested nonspecific histopathologic changes (nonspe-
cific inflammatory reaction).
The results of the immnnohistochemical tests that
were performed on the gingival biopsy specimens of
the patients with PV were in all cases positive, showing
intercellular deposits of IgG, IgA, and complement at
the spindle cell layer ofthe epithelium. Ofthe gingival
specimens from patients with MMP, 77% were positive
for IgG, while approxittiately 72% showed deposition
of IgA and complement in the basement membrane.
These findings are reasonable, because PV and MMP
are autoimmune diseases in which the antigenic target
of autoimmunity is believed to be located between the
spindle cells of the epithehum and in the basement
membrane, respectively. Similar immunohistochemi-
cal findings have been reported by other investi-
gators.''"^^
Results were negative in all patients with OLP for
IgG and IgA; results were positive in some instances
for IgM, Positive staitiing results were also seen under
766
Quintessence International Vciume 27, Number 11/1996
Mariopoulos et al
the direct immunofluorescence for ftbrin-fibrinogen in
the patients with OLP. It has been proposed that
positive staining of IgM and fibrin-ftbrinogen are
suggestive of OLP.-'
The evaluation of the files of patients with muco-
cutaneous diseases demonstrated that desquamative
gingival lesions are not rare; they were found in 11.8%
ofthe individuals in the present study. However, the
prevalence of DG in patients with mucocutaneotjs
diseases varies in the literature.'^*----^
Desquamative gingivitis is seen in both sexes but is
more prevalent in women.-'' The present results
corroborate this assumption.
Before the final diagnosis of DG is made, difier-
ential diagnosis should be made, especially at the
hi sto patho logic level, from plasma cell gingivitis. Tlie
prominent histopathologic feature of plasma cell
gingivitis is the dense infiltration of lamina propria
with plasma cells.
Treatment of DG is symptomatic.^^ Systemic admin-
istration of prednisolone may be a treatment for DG
patients with PV.-'' Systemic or topical corticosteroid
treatment, in the form of fluocinonitie, may be effective
for DG patients with MMR-" Topical therapy with
ttocinonide is also recommended for the alleviation
of gingival lesions in patients with OLP.^^ Local
irritating factors must always be removed. This thera-
peutic measure is especiaUy recommended in patients
with DG who exhibit no detectable underlying disease
(idiopathic cases).
Desquamative gingivitis usually represents a mani-
festation of MMP, Py or OLP. Special laboratory
techniques are needed to reach the correct diagnosis so
that the appropriate therapy is provided.
References
1. TomesJ. Tomes G. Dental Surger>',ed 4. London: Chjrchitl. 1894.
2. Prinz H. Chronic diffuse desqiiamative gingivitis. Dent Cosmos
3. Meiiit AH, Chronic desquamatiye gingivitis. J Periodontol 1933;
430-34.
4. Wood NK, Goaz PW. Differential Diagnosis of Oral Lesions, ed 4, St
Louis: Mosby. 199t:93-95.97.
5. McCarthy FP, McCarthy PL. Shklar G. Chronic desquamative
gingivitis, A reconsideration. Oral Surg Oral Med Oral Pathol
t96O;t3:130O-13t3,
6, Shktar G. Meyer t, Lacarian S, Oral tesions in buJtous pemphigoid.
Arch Dertnatol t99:99:663-67O.
7. Shklar G. McCarthy PL. Oral lesions of miicoii membrane
pemphigoid. A study of 85 eases. Arch Otolaryngot t971i93:354-
364,
8. Qles RD. Chronic desquamative gingivitis, J Periodontol 967i
38:485-490.
9, Shklar G. McCarthy PL. The Oral Manifestations of Systemic
Disease. London; Butterworths. 1976:136.
10. Laskaris G, Varettzidis A. Capetanakis J. A ctirucal study of
pemphigus; observations on t28 patients. Mater Med Greca
197S;6r627-630.
11. Carranza FA Jr. Giiekman's Clinical PeriodunLuiogy. Philadeiphia;
Saunders. t979:155-t92.
12. McCanhy PL. Shktar G. Diseases ofthe Oral Mueosa. Phitadelphia;
Lea & Febiger. t980.
t3. Nisengard RJ. Neiders M. Desquamative gingivitis. J Periodontol
19S1:52:500-50.
t4, Sktavounou A. Laskaris G. Frequency of desquamative gingivitis in
skin disease. Oral Surg Orat Med Oral Pathol 1983:56:141-144.
15. Daniels TE, Quadra White C. Direct inimunofluorescence in oral
mucosal disease; A diagnostic anaiysis of 30 cases. Orat Surg Oral
Med Orai Pathol 1981;5t;38-47,
t6. Jadinsfci JJ, Shktar G. Lichen planus of the gingiva. J Periodontol
1976:47:724-733,
t7. Williams DM. Vesicutobullous mucocutaneous disease: Pemphigus
vulgaris. J Oral Pathol Med 1989;t8:544-553.
18, Bean SF. Cicatricial pemphigoid. Arch Dermatol t974;lt0:552-
555.
19, Peng T. Nisengard RJ. Levine MJ. Gingivai basement membrane
antigens in desquamative lesions of the gingiva. Oral Surg Orat Med
OralPathut 1986;6t:584-589.
20, Lamey PJ, Bimjje WH, Ranking KV Mucous membrane pemphi-
goid. Treatment experience at two institutions. Oral Surg Oral Med
Oral Pathol 1992;74:50-53.
21. Baart de al Faille-Kyper EH, Baart de ta Faille H. An immuno-
fluorescent study of tichen pianus. Br J Demiatot 1974;90;365-371.
22. Rogers RS, Sheridan PJ, Jordon RE. Desquamative gingivitis:
Clinical, histopathotogic and immunologie investigation. Orat Surg
Oral Med Oral Pathol l976;42:3l6-327.
23, Laskaris G. Dimitriou N, Angelopoulos A. Immunofluorescent
studies in desquamatjve gingivitis. J Oral Pathol 198i;10:39S-407,
24, Ghckman 1, Smulow JB, Chronic desquamative gingivitis: Its nature
and treatment, J Penodontol 1964;35:397-4O5.
25. Nisengard RJ, Rogers RS, The treatment of desquamative gingival
lesions. J Periodontol 1987:58:167-172.
26. KormanN. Pemphigus. J Am Acad Dermatol 1988;18:1219-1238.
27. Scully C, Mason DK. Therapeutic measures in oral medicine. In:
Jones JH. Mason DK. (eds). Oral Manifestations of Systemic
Disease. London- Satinders. l9S0:30-542. D
Quintessence International Volutne 27, Number 11/1996 767
Вам также может понравиться
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- PNF PatternsДокумент19 страницPNF PatternsDany VirgilОценок пока нет
- 10 1016@j Lungcan 2016 10 008Документ2 страницы10 1016@j Lungcan 2016 10 008restu anindityaОценок пока нет
- The Nursing Diagnosis Body Image Disturbance Is Most Likely To Be Written For Which of The Following PersonsДокумент3 страницыThe Nursing Diagnosis Body Image Disturbance Is Most Likely To Be Written For Which of The Following PersonsenzoОценок пока нет
- 4.-Rapid Sequence Intubation in Adults - Uptodate PDFДокумент14 страниц4.-Rapid Sequence Intubation in Adults - Uptodate PDFkendramura100% (1)
- Methanol Information 2 PDFДокумент5 страницMethanol Information 2 PDFPark RangerОценок пока нет
- Acute Respiratory Failure: Part 1. Failure in OxygenationДокумент6 страницAcute Respiratory Failure: Part 1. Failure in OxygenationnytenurseОценок пока нет
- Understanding Laryngopharyngeal Reflux DiseaseДокумент30 страницUnderstanding Laryngopharyngeal Reflux Diseaseamitkulkarni83100% (1)
- Rebt Vs CT Vs Med in DepressionДокумент19 страницRebt Vs CT Vs Med in DepressionPaula StroianОценок пока нет
- Arthrogryposis Multiplex Congenita of The Upper Limb: Linical RticleДокумент6 страницArthrogryposis Multiplex Congenita of The Upper Limb: Linical RticleBlajiu BeatriceОценок пока нет
- 2 02-Electrocardiography PDFДокумент17 страниц2 02-Electrocardiography PDFMiguel DomingoОценок пока нет
- Clinical - Bilirubin TestДокумент9 страницClinical - Bilirubin Testbarbie.monster89100% (3)
- Preventing Infant Abduction in The Hospital.17-2Документ2 страницыPreventing Infant Abduction in The Hospital.17-2Andrés HerrónОценок пока нет
- Photodynamic TherapyДокумент5 страницPhotodynamic TherapyPranav UpadhyayaОценок пока нет
- Procedure Checklist With Rating Form Donning and Removing Sterile GlovesДокумент4 страницыProcedure Checklist With Rating Form Donning and Removing Sterile GlovesRachel VillanuevaОценок пока нет
- Acute Pancreatitis: Aguirre, Lucas Galligani, Guido Gorostiaga, Marcos Kreutzer, GustavoДокумент20 страницAcute Pancreatitis: Aguirre, Lucas Galligani, Guido Gorostiaga, Marcos Kreutzer, GustavoGüids GalliganiОценок пока нет
- What Did Freud Get RightДокумент3 страницыWhat Did Freud Get RightGustavo AvendañoОценок пока нет
- Group C Report FinalДокумент57 страницGroup C Report FinalRI NAОценок пока нет
- Case Study: Carpal Tunnel SyndromeДокумент30 страницCase Study: Carpal Tunnel SyndromeMuslihah Mohd Razali0% (1)
- 06 Senior Citizen PolicyДокумент26 страниц06 Senior Citizen PolicyJaimson FrancisОценок пока нет
- 46.5. Professional Services, Inc. v. CA (2008)Документ10 страниц46.5. Professional Services, Inc. v. CA (2008)Iñigo Mathay RojasОценок пока нет
- Nursing InformaticsДокумент16 страницNursing InformaticsSherina W. Edding100% (2)
- Inpatient Pre Authorization FormДокумент1 страницаInpatient Pre Authorization FormSemeeeJuniorОценок пока нет
- Multiple Choice Question (MCQ) Exam: 15 Sample QuestionsДокумент4 страницыMultiple Choice Question (MCQ) Exam: 15 Sample QuestionsAnkita AgarwallОценок пока нет
- ERAS - Personal StatementДокумент1 страницаERAS - Personal StatementfewОценок пока нет
- Class II MalocclusionДокумент67 страницClass II Malocclusionsonal agarwal100% (1)
- Cerebral Palsy Revalida FormatДокумент10 страницCerebral Palsy Revalida FormatChelsea CalanoОценок пока нет
- Ivig GAMMARAS - FullДокумент13 страницIvig GAMMARAS - FullNisa UcilОценок пока нет
- Swan Ganz CathetersДокумент27 страницSwan Ganz CatheterschadchimaОценок пока нет
- G. Psychosocial Profile (Gordon's Functional Pattern)Документ7 страницG. Psychosocial Profile (Gordon's Functional Pattern)ampalОценок пока нет
- Estimating Glomerular Filtration RateДокумент7 страницEstimating Glomerular Filtration RateShirin SyailandiraОценок пока нет