Академический Документы
Профессиональный Документы
Культура Документы
Management of Acute Nasal Fractures
Загружено:
Taufiq HidayatОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Management of Acute Nasal Fractures
Загружено:
Taufiq HidayatАвторское право:
Доступные форматы
I
njuries to the nose are relatively com-
mon; in cases of facial trauma, nasal
fractures account for approximately 40
percent of bone injuries.
1
Fights and
sports injuries account for most nasal frac-
tures in adults, followed by falls and vehicle
crashes. Play and sports account for most
nasal fractures in children. Physical abuse
should be considered in children and women,
and should be appropriately ruled out.
2
Nasal fractures may occur in isolation or
in association with other facial injuries. Fur-
thermore, many nasal fractures go undiag-
nosed and untreated because some patients
do not seek medical care.
3
Though seen occa-
sionally in family practice, patients with nasal
fractures are more likely to present to emer-
gency departments or urgent care settings.
Fractures that are more than two days old
will have substantial edema and should be
referred urgently for subspecialty evaluation.
Anatomy
The nose is easily exposed to trauma because
it is the most prominent and anterior feature
of the face. The nose is supported by cartilage
anteriorly and inferiorly, and by bone poste-
riorly and superiorly (Figure 1). The paired
nasal bones, the nasal process of the frontal
bone, and the maxilla form a framework to
support the cartilaginous skeleton. Although
most of the nasal structures are cartilaginous,
the nasal bones usually are fractured in an
injury.
Overlying this framework are soft tissues,
mucous glands, muscles, and nerves respon-
sible for sensation and function of the nose.
By virtue of its natural taper, the supporting
nasal septum becomes increasingly thin and
is therefore subject to fracture toward the tip
of the nose.
The relative ease by which epistaxis can
occur with minor trauma is explained by
the dense and redundant vascular network
that supplies the nose. This plexus, known
as Kiesselbachs area, is responsible for the
vast majority of normal epistaxis.
4
However,
bleeding as a result of nasal fracture usually
originates from other locations within the
nose. For example, profuse anterior bleeding
In cases of facial trauma, nasal fractures account for approximately
40 percent of bone injuries. Treatment in the primary care setting
begins with evaluating the injury, taking an accurate history of the
situation in which the injury occurred, and ascertaining how the face
and nose appeared and functioned before the injury occurred. Serious
injuries should be treated, then nasal inspection and palpation may be
performed to assess for airway patency, mucosal laceration, and sep-
tal deformity. A thorough examination of the nose and surrounding
structures, including the orbits, mandible, and cervical spine, should
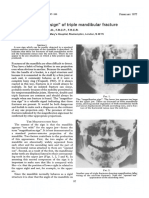
be completed. Imaging studies are necessary for facial or mandibular
fractures. Patients with septal hematomas, cerebrospinal fluid rhi-
norrhea, malocclusion, or extraocular movement defects should be
referred to a subspecialist. Treatment in the primary care setting con-
sists of evaluation, pain and infection management, minimal debride-
ment and, when the physician is appropriately trained, closed reduc-
tion. If an immediate referral is not indicated, close follow-up, possibly
with a subspecialist, should be arranged within three to five days after
the injury. (Am Fam Physician 2004;70:1315-20. Copyright 2004
American Academy of Family Physicians.)
Management of Acute Nasal Fractures
CORRY J. KUCIK, LT, MC, USN, TIMOTHY CLENNEY, CDR, MC, USN, and JAMES PHELAN, CDR, MC, USN
Naval Hospital Jacksonville, Jacksonville, Florida
October 1, 2004
Volume 70, Number 7 www.aafp.org/afp American Family Physician 1315
Downloaded from the American Family Physician Web site at www.aafp.org/afp. Copyright 2004 American Academy of Family Physicians. For the private, noncommercial
use of one individual user of the Web site. All other rights reserved. Contact copyrights@aafp.org for copyright questions and/or permission requests.
1316 American Family Physician www.aafp.org/afp Volume 70, Number 7
October 1, 2004
may originate from the anterior
ethmoid artery (a branch of the
ophthalmic artery), while pos-
terior bleeding is more likely
to arise from a branch of the
sphenopalatine artery. Arterial
ligation may be necessary if packing fails to
control bleeding. In such cases, early consulta-
tion with an otolaryngologist is indicated.
5,6
Assessment
HISTORY
Understanding the mechanism of trauma is
helpful to the physician in determining the
extent of the injury. It is useful to know the
responsible object, the direction from which
it came, and the strength of force sustained by
the nose. For example, a direct frontal blow
can depress the dorsum of the nose, causing
the fractured bones to telescope posteriorly.
Likewise, a laterally directed injury can cause
a depression on the side of the impact, often
with a corresponding outward displacement
on the opposite side of the nose. Traction
and torsion injuries, though rare, also can
cause cartilaginous disruption.
7
The patient should be asked about the
timing and extent of any bleeding associ-
ated with the injury. The history also should
include information regarding previous sur-
geries, injuries, and a subjective assessment
of baseline nasal function and appearance.
Finally, because alcohol use frequently is
associated with such trauma, physicians may
wish to determine whether the patient had
been drinking before the injury. This point
may have implications for selection of pain
medications, potential for repeat injury, and
the ability to assess for mental status changes
associated with head injury.
PHYSICAL EXAMINATION
Most nasal fractures are the result of minor
trauma such as being punched or elbowed.
However, when assessing a patient with an
acute nasal injury, the physician should avoid
focusing solely on the obviously traumatized
nose. This is particularly important if the
patient has experienced a violent traumatic
event such as a motor vehicle crash or an
assault. A substantial direct blow to the
mid-face area can result in cervical spine
injury, and the physician must therefore
exercise clinical judgment in using appropri-
ate precautions until a cervical spine injury is
ruled out. During the initial assessment, the
physician should be certain that the patient
has an adequate airway and is ventilating
appropriately.
A nasal injury may be associated with other
head and neck trauma that could compromise
the patency of the trachea. Furthermore, given
the close proximity of the nose to other facial
structures, the physician must consider the
possibility of an associated facial or mandib-
ular fracture.
3
Therefore, all bony structures
of the face, including the malar eminences,
orbital rims, zygomatic arches, mandible, and
teeth, should be carefully inspected and pal-
pated for irregularity or tenderness. All facial
lacerations, swellings, and deformities should
be noted, and the eyes should be examined
for symmetry and mobility of gaze.
8
If a facial
or mandibular fracture is suspected, radio-
logic assessment with computed tomography
(CT) is indicated.
9
A deformity of the nose usually will be
evident when a nasal fracture has occurred.
However, epistaxis without obvious nasal
deformity may be the only clinical finding
in some nasal fractures. Edema and ecchy-
mosis of the nose and periorbital structures
ordinarily will be present, particularly if
examination is performed more than sev-
eral hours after the injury. Palpation of the
Understanding the mecha-
nism of trauma is helpful to
the physician in determin-
ing the extent of the injury.
Figure 1. Anatomic relationship between the nasal bones, cartilage,
and septum.
Nasal bone
Upper lateral
cartilage
Medial and lateral
crura of lower lateral
cartilage
Fibroareolar
tissue
Frontal process
of maxilla
Septal cartilage
Lateral
crus
Medial crus
I
L
L
U
S
T
R
A
T
I
O
N
S
B
Y
C
H
R
I
S
T
Y
K
R
A
M
E
S
October 1, 2004
Volume 70, Number 7 www.aafp.org/afp American Family Physician 1317
Nasal Fractures
nasal structures should be done to elicit any
crepitus, indentation, or irregularity of the
nasal bone. Uncommon findings such as
a cerebrospinal fluid (CSF) leak posing as
clear rhinorrhea, subcutaneous emphysema,
mental status changes, new malocclusion,
or limited extraocular movement should
prompt immediate subspecialty referral.
3,10
Knowledge of the shape and appearance of
the patients nose before the injury will aid
in comprehending the severity of the nasal
injury. This is best accomplished by view-
ing a good quality photograph of the patient
taken before the injury. If a photograph is
not available, the photo on a drivers license
or identification card also may be used.
Photographs of the injured nose also may be
obtained for legal purposes and to measure
treatment success.
11
External and internal examination may
be difficult following nasal injury because
of ecchymoses, edema, and dried blood,
especially if more than three hours have
passed.
6
If this is the case in a patient with
an uncomplicated acute nasal fracture, it
is appropriate to prescribe pain medication
and release the patient with instructions to
rest, apply ice, and maintain head elevation.
Because no clinical evidence exists to man-
date early fracture reduction,
6,12
follow-up
evaluation and management can be safely
scheduled after the swelling resolves, usu-
ally within three to five days.
7
Reduction
should be accomplished between the fifth
and 10th day after the injury, and before the
nasal bones start to fixate.
5
However, before
releasing a patient with any type of nasal
trauma, it is critical to rule out septal hema-
tomas. These may appear as slightly white
or purple areas of fluctuance lying on one
or both sides of the nasal septum (Figure 2).
Failure to identify and treat a septal hema-
toma can result in a saddle deformity of the
septum, which will require surgical repair.
A thorough internal examination is facili-
tated with good lighting, suction, anesthesia,
and vasoconstrictive nasal sprays. A nasal
speculum and a headlamp will improve
visualization, as will a fiberoptic endoscope,
if available. The initial internal inspection
usually will reveal the presence of large
blood clots, which should be removed with
warm saline irrigation, suction, and cotton-
tipped applicators.
Adequate anesthesia and vasoconstric-
tion should be obtained before the complete
internal examination. This is best achieved
with topical agents administered as sprays,
impregnated cotton-tipped applicators, or
local injections. Cocaine in a 5 or 10 percent
solution, though often difficult to obtain,
is a highly effective single therapy appro-
priate for both vasoconstriction and anal-
gesia. Alternatives for anesthesia include
intranasal topical lidocaine (Xylocaine),
bupivacaine (Marcaine), and
pontocaine (Opticaine) spray.
Topical vasoconstrictors, such
as oxymetazoline (Afrin) and
phenylephrine hydrochloride
(Neo-Synephrine) are useful
adjuncts for controlling bleed-
ing and decreasing intranasal edema.
7,11
Some experts report that a 1:1 mixture of
the topical decongestant oxymetazoline or
phenylephrine and 4 percent topical lido-
caine (liquid) is as effective as cocaine.
During the internal examination, the phy-
sician should assess nasal airway patency
and should determine if ongoing epistaxis
or septal deformities are present. The turbi-
nates and inferior meatus should be visual-
ized bilaterally, and the septum must be
carefully inspected for septal hematomas.
Finally, any mucosal lacerations should be
noted because they may suggest an underly-
ing fracture.
IMAGING STUDIES
When an uncomplicated nasal fracture is
suspected, plain radiography rarely is indi-
cated. In fact, because of poor sensitivity and
Substantial direct injury
to the mid-face can result
in cervical spine injury or
a compromised airway.
Figure 2. Bilateral septal hematomas associ-
ated with a nasal fracture.
1318 American Family Physician www.aafp.org/afp Volume 70, Number 7
October 1, 2004
specificity, plain radiography
may serve only to confuse the
clinical picture.
4
Plain radiogra-
phy will not allow identification
of cartilaginous disruptions,
and physicians may misin-
terpret normal suture lines as
nondisplaced fractures. However, when find-
ings such as CSF rhinorrhea, extraocular
movement abnormalities, or malocclusion
are present, radiologic imaging by CT is
indicated to assess for facial and mandibular
fractures.
9
Management
After ensuring airway patency, adequate ven-
tilation, and overall stability of the patient,
the physician can devote attention to the
nasal fracture itself.
1,3
Treatment begins with management of
external soft tissue injuries. If an open wound
is present and appears to be contaminated
with foreign matter, copious irrigation will
be required. Some debridement also may
be necessary. However, debridement should
be done judiciously because tissue will be
needed to cover any exposed cartilage.
Reduction of acute nasal fractures in the
primary care setting is confined largely to
the closed reduction of mild unilateral frac-
tures. However, on rare occasions, open
reduction in an operating room is necessary.
It is worthwhile for family physicians to
understand how closed reduction of a nasal
fracture is performed, although it is not
considered a standard family medicine pro-
cedure. Physicians who anticipate perform-
ing open or closed reductions should gain
experience and training before attempting
these procedures.
The goal of closed reduction is to realign
cartilaginous and bony structures to their
locations before the injury to decrease dis-
comfort and maximize airway patency.
The aesthetic outcomes of closed reduc-
tion techniques are often less than opti-
mal, and patients should be counseled that
nasal reconstruction might eventually be
necessary.
4
Given the obvious anxiety and
pain associated with reduction, pretreat-
ment with anxiolytic and pain medications
should be considered.
Manual realignment is the easiest method
of closed reduction. A few simple instruments
can vastly improve outcomes in nasal fracture
reduction (Figure 3). Two instruments, the
Asch and the Walsham forceps, are designed
to reduce the displaced septum and impacted
Fracture reduction can be
performed within three to
five days after ecchymoses
and edema resolve.
The Authors
CORRY J. KUCIK, LT, MC, USN, is a flight surgeon and hyperbaric medical officer
with Marine Fighter Attack Squadron 251 at Marine Corps Air Station, Beaufort,
S.C. He received his medical degree from the Uniformed Services University
of the Health Sciences F. Edward Hbert School of Medicine, Bethesda, Md.,
and completed an internship in family medicine at Naval Hospital Jacksonville,
Jacksonville, Fla.
TIMOTHY CLENNEY, CDR, MC, USN, is a staff family physician at Naval Hospital
Jacksonville. He received his medical degree from the University of South Florida
College of Medicine, Tampa, and his master of public health degree from
Emory University, Atlanta. He completed a residency in family medicine at Naval
Hospital Jacksonville.
JAMES PHELAN, CDR, MC, USN, is head of the Department of Otorhinolaryngology
at the Naval Aerospace Medical Institute, Pensacola, Fla., and a flight surgeon in
the U.S. Navy. He received his medical degree from the University of Medicine
and Dentistry of New Jersey, Newark, and completed a residency in otolaryngol-
ogy at Naval Regional Medical Center, Oakland, Calif.
Address correspondence to Timothy Clenney, CDR, MC, USN, 1705 Broad Water
Ct., Orange Park, FL 32003 (e-mail: tclenney@msn.com). Reprints are not avail-
able from the authors.
Figure 3. Reduction instruments. (Left) Asch
forceps, (center) Walsham forceps, and (right)
Boies elevator.
October 1, 2004
Volume 70, Number 7 www.aafp.org/afp American Family Physician 1319
nasal bones, respectively, although these
instruments often are used interchangeably.
An important drawback with these instru-
ments is the possibility of mucosal crushing
injuries and resulting hematomas that may
occur between their tines.
The Boies elevator (Figure 3) offers more
precision than the aforementioned forceps.
When used correctly, the Boies elevator is
inserted into the nostril deeply to an inter-
nally or externally displaced fracture. The
blade of the elevator opposes the physicians
thumb on the outside of the nose. The
physician then gently attempts to raise or
depress the misaligned bones to their origi-
nal configuration. The reduction may be felt
as the fractured bone returns to its proper
alignment.
A septal hematoma is a blood-filled cav-
ity between the cartilage and the support-
ing perichondrium. If left untreated, these
pockets of blood easily become infected.
The resulting necrosis of the underlying
cartilaginous support may result in per-
manent saddle nose deformity.
7
When a
septal hematoma is identified, it should be
aspirated immediately or incised with the
aid of local anesthesia (Figure 4). To prevent
reaccumulation of blood, a sterile drain may
be left in place. However, there is conflict-
ing evidence regarding the benefit of using a
drain.
13
Splints (Figure 5) or sutures may be
applied to both sides of the septum to pro-
vide pressure and support, or anterior nasal
packing also may be used.
1
If improperly
managed, a septal hematoma
may have a disastrous outcome.
Therefore, the treating physi-
cian should consult with an oto-
laryngologist or plastic surgeon
when feasible.
The physician should com-
plete a final external and internal
(endoscopic, if possible) exami-
nation before releasing a patient
who has undergone manipula-
tion and reduction of a nasal fracture. This
examination should ensure alignment of the
nose and the absence of significant epistaxis
or hematomas. When completed, an external
The goal of closed reduc-
tion of an acute nasal
fracture is to realign
cartilaginous and bony
structures to decrease
discomfort and maximize
airway patency.
Figure 4. Management of septal hematoma. (A) Cross-sectional view of a septal hematoma,
showing blood accumulation between the septum and perichondrium. Treatment involves
anesthesia, followed by (B) incision using a hemostat, (C) drainage of the hematoma, and (D)
insertion of sterile gauze to prevent the reaccumulation of blood.
Nasal
septum
Septal
hematoma
Perichondrium
A B
C D
Nasal Fractures
1320 American Family Physician www.aafp.org/afp Volume 70, Number 7
October 1, 2004
splint or cast should be applied to the nasal
dorsum for about one week. If nasal packing
is required, the physician should remember
that nasal packing rarely has been associated
with toxic shock syndrome.
14
Accordingly,
packing material should be impregnated
with an antistaphylococcal ointment.
The tetanus status of all patients should
be determined and managed appropriately;
prophylactic antibiotics may be prescribed
when indicated, such as in a grossly con-
taminated open fracture.
5
Although most family physicians rou-
tinely will not perform closed reduction
of nasal fractures, it is still important to
understand the preliminary assessment and
basic management principles. Furthermore,
because of the uncertainty of functional and
cosmetic outcomes following a nasal frac-
ture reduction,
15
referral to an otolaryngolo-
gist or plastic surgeon within three to five
days post-reduction, while not absolutely
necessary, usually is appropriate. Ideally, the
referral should be arranged before the family
physician releases the patient.
The authors acknowledge the efforts of Bettye
Stilley, who is the medical librarian at Naval Hospital
Jacksonville, Jacksonville, Fla.
This article is one in a series on practical therapeutics
coordinated by the Department of Family Medicine at
Naval Hospital Jacksonville, Jacksonville, Fla. Guest edi-
tor of the series is Anthony J. Viera, LCDR, MC, USNR.
Figures 3 and 5 courtesy of Timothy Clenney, CDR, MC,
USN.
The opinions and assertions contained herein are the
private views of the authors and are not to be construed
as official or as reflecting the views of the U.S. Navy
Medical Corps or the U.S. Navy at large.
The authors indicate that they do not have any conflicts
of interest. Sources of funding: none reported.
REFERENCES
1. Bartkiw TP, Pynn BR, Brown DH. Diagnosis and manage-
ment of nasal fractures. Int J Trauma Nurs 1995;1:11-8.
2. Smith JA. Nasal emergencies and sinusitis. In: Tintinalli
JE, Ruiz E, Krome RL, American College of Emergency
Physicians. Emergency medicine: a comprehensive study
guide. 4th ed. New York: McGraw-Hill, 1996:1087-90.
3. Ellis E III, Scott K. Assessment of patients with facial
fractures. Emerg Med Clin North Am 2000;18:411-48.
4. Hester TO, Campbell JP. Diagnosis and management
of nasal trauma for primary care physicians. J Ky Med
Assoc 1997;95:386-92.
5. Cummings CW, ed. Otolaryngologyhead & neck
surgery. 3d ed. St Louis: Mosby, 1998:871.
6. Bailey BJ, ed. Head and neck surgeryotolaryngology.
Philadelphia: Lippincott, 1993:996.
7. Cox AJ III. Nasal fracturesthe details. Facial Plast Surg
2000;16:87-94.
8. Rodriguez JO, Lavina AM, Agarwal A. Prevention and
treatment of common eye injuries in sports. Am Fam
Physician 2003;67:1481-8.
9. Rhea JT, Rao PM, Novelline RA. Helical CT and three-
dimensional CT of facial and orbital injury. Radiol Clin
North Am 1999;37:489-513.
10. Sargent LA, Rogers GF. Nasoethmoid orbital fractures:
diagnosis and management. J Craniomaxillofac Traum
1999;5:19-27.
11. Rohrich RJ, Adams WP Jr. Nasal fracture management:
minimizing secondary nasal deformities. Plast Reconstr
Surg 2000;106:266-73.
12. Gilpin T, Carley S. Toward evidence based emergency
medicine: best BETs from the Manchester Royal Infir-
mary. Early management of displaced nasal fractures.
J Accid Emerg Med 2000;17:286.
13. Canty PA, Berkowitz, RG. Hematoma and abscess of
the nasal septum in children. Arch Otolaryngol Head
Neck Surg 1996;122:1373-6.
14. Jacobson JA, Kasworm EM. Toxic shock syndrome after
nasal surgery. Case reports and analysis of risk factors.
Arch Otolaryngol Head Neck Surg 1986;112:329-32.
15. Kane AP, Kane LA. Open reduction of nasal fractures.
J Otolaryngol 1978;7:183-6.
Figure 5. External splint providing pressure
and support.
Nasal Fractures
Вам также может понравиться
- Nasal FractureДокумент12 страницNasal Fracturejean_bernardesОценок пока нет
- Evaluation and Reduction of Nasal TraumaДокумент15 страницEvaluation and Reduction of Nasal TraumaAnnisa Priscasari DwiyantiОценок пока нет
- Articulo PDFДокумент9 страницArticulo PDFNayeli Díaz InzunzaОценок пока нет
- Nasal Trauma and The Deviated Nose: SummaryДокумент12 страницNasal Trauma and The Deviated Nose: SummaryAlexandru BadeaОценок пока нет
- Nasal Fracture Reduction: Continuing Education ActivityДокумент11 страницNasal Fracture Reduction: Continuing Education Activityvidro alifОценок пока нет
- An Algorithm For The Initial Management of Nasal Trauma: John F. Hoffmann, MD, FACSДокумент11 страницAn Algorithm For The Initial Management of Nasal Trauma: John F. Hoffmann, MD, FACSDaniel Celestino DiazОценок пока нет
- Maxillofacial Trauma: Child DevelopmentДокумент8 страницMaxillofacial Trauma: Child DevelopmentAchmadArifinОценок пока нет
- Nasal Fracture: Case ReportДокумент8 страницNasal Fracture: Case ReportMas KaryonОценок пока нет
- Facial Fractures 2Документ30 страницFacial Fractures 2chetotskimdОценок пока нет
- Sps 24398Документ12 страницSps 24398ali alenziОценок пока нет
- Nasal and Facial Fractures: DR - Imran Qazi Ent A Tmo KTH PeshawarДокумент42 страницыNasal and Facial Fractures: DR - Imran Qazi Ent A Tmo KTH Peshawarimran qaziОценок пока нет
- Preliminary Management of Maxillofacial Injuries MADE EASYДокумент9 страницPreliminary Management of Maxillofacial Injuries MADE EASYMohammedОценок пока нет
- Lu2017 Nasal FracturesДокумент10 страницLu2017 Nasal FracturesInne CarolineОценок пока нет
- Tbone FX 100331 PDFДокумент7 страницTbone FX 100331 PDFPcrОценок пока нет
- Regional Assessment and Special Diagnostic TestsДокумент2 страницыRegional Assessment and Special Diagnostic TestsBereket temesgenОценок пока нет
- Maxillofacial TraumaДокумент15 страницMaxillofacial TraumadewiswahyuОценок пока нет
- Nasal TraumaДокумент5 страницNasal TraumaRae Marie AquinoОценок пока нет
- Tolley - Pediatric TraumaДокумент8 страницTolley - Pediatric TraumaRicardo GrilloОценок пока нет
- Emergency Assessment and Treatment: Bony Injuries and FracturesДокумент11 страницEmergency Assessment and Treatment: Bony Injuries and FracturesBereket temesgenОценок пока нет
- Emergency Assessment and Treatment: Bony Injuries and FracturesДокумент11 страницEmergency Assessment and Treatment: Bony Injuries and FracturesBereket temesgenОценок пока нет
- Tratamiento Del Paciente TraumatizadoДокумент10 страницTratamiento Del Paciente TraumatizadomariaОценок пока нет
- Brmedj02607 0047Документ2 страницыBrmedj02607 0047Fedi NurrizallОценок пока нет
- CraniomaДокумент7 страницCraniomaSophia BeecherОценок пока нет
- Primary Survey KGD LBM 1Документ9 страницPrimary Survey KGD LBM 1Nur Azizah PermatasariОценок пока нет
- Frontal Sinus FracturesДокумент9 страницFrontal Sinus Fracturesshehla khanОценок пока нет
- Nasolaryngoscopy: Scott E. MoserДокумент5 страницNasolaryngoscopy: Scott E. Moserriski novitaОценок пока нет
- Complications of OtoplastyДокумент10 страницComplications of OtoplastyLaineyОценок пока нет
- Management of Frontal Sinus Fractures: SummaryДокумент17 страницManagement of Frontal Sinus Fractures: SummaryAlexandru BadeaОценок пока нет
- Basics and Emergency Care: Key PointsДокумент10 страницBasics and Emergency Care: Key Pointsنورالهدى حسام عليОценок пока нет
- All Medical Questions and All Medical Questions and Answers AnswersДокумент18 страницAll Medical Questions and All Medical Questions and Answers AnswersazizОценок пока нет
- Nasalseptal Hematoma/abscess: Management and Outcome in A Tertiary Hospital of A Developing CountryДокумент5 страницNasalseptal Hematoma/abscess: Management and Outcome in A Tertiary Hospital of A Developing CountryShabrina Sari MedinaОценок пока нет
- Corneal LacerationДокумент5 страницCorneal LacerationAchmad HariyantoОценок пока нет
- Facial Trauma: Dr. Azher A. Auda Oral and Maxillofacial Surgeon Bds CabsДокумент56 страницFacial Trauma: Dr. Azher A. Auda Oral and Maxillofacial Surgeon Bds CabsHaider F YehyaОценок пока нет
- Ear TraumaДокумент7 страницEar TraumaYogi S. RosadiОценок пока нет
- Panfacial FracturesДокумент35 страницPanfacial FracturesMARISOL GALLEGO DUQUEОценок пока нет
- Contents OcnaДокумент4 страницыContents OcnaGirish SubashОценок пока нет
- Author's Accepted Manuscript: Seminars in Ultrasound, CT, and MRIДокумент29 страницAuthor's Accepted Manuscript: Seminars in Ultrasound, CT, and MRIasfwegereОценок пока нет
- Orbitalfractures: Kris S. Moe,, Andrew H. Murr,, Sara Tullis WesterДокумент15 страницOrbitalfractures: Kris S. Moe,, Andrew H. Murr,, Sara Tullis Westerstoia_sebiОценок пока нет
- Traumatic Optic Neuropathy: Review ArticleДокумент9 страницTraumatic Optic Neuropathy: Review ArticleTiwi QiraОценок пока нет
- Maxillofacial TraumaДокумент56 страницMaxillofacial TraumaErnesto Fer FdezОценок пока нет
- Face and Neck InjuryДокумент20 страницFace and Neck Injurycanjaysfan89Оценок пока нет
- 130-044 EnglishДокумент6 страниц130-044 EnglishMuhammad Syauqie AssegafОценок пока нет
- Klasifikasi Dan Management Deviasi SeptumДокумент8 страницKlasifikasi Dan Management Deviasi SeptummawarmelatiОценок пока нет
- Management of Nasal Fractures.: Author InformationДокумент1 страницаManagement of Nasal Fractures.: Author InformationAnnisa Priscasari DwiyantiОценок пока нет
- Otoplasty For The Protruded EarДокумент8 страницOtoplasty For The Protruded EarroyvillafrancaОценок пока нет
- Cirugía de Senos y Globo OcularДокумент21 страницаCirugía de Senos y Globo Ocularjorge pradaОценок пока нет
- Anestheticconsiderations Fororal, Maxillofacial, and NecktraumaДокумент17 страницAnestheticconsiderations Fororal, Maxillofacial, and NecktraumaDasubabu GantiОценок пока нет
- Ostrower Preauricular Cysts, Pits, and Fissures - Practice Essentials, Epidemiology, EtiologyДокумент8 страницOstrower Preauricular Cysts, Pits, and Fissures - Practice Essentials, Epidemiology, EtiologyAndre HawkОценок пока нет
- Open Fracture Raju3Документ72 страницыOpen Fracture Raju3Chowdhury Iqbal MahmudОценок пока нет
- Maxillofacial Trauma: Dr. Azher A. Auda Bds CabsДокумент17 страницMaxillofacial Trauma: Dr. Azher A. Auda Bds CabsHaider F YehyaОценок пока нет
- Associated Signs Symptoms: Eye and of Head InjuriesДокумент5 страницAssociated Signs Symptoms: Eye and of Head InjuriesSary Ghassan IbrahimОценок пока нет
- History of The Procedure: Mandibular Bone PlatingДокумент7 страницHistory of The Procedure: Mandibular Bone PlatingNiero GalangОценок пока нет
- Diagnosis and Management Crooked Nose EbcrДокумент12 страницDiagnosis and Management Crooked Nose EbcrnewdewiОценок пока нет
- 002-Trauma & BurnsДокумент35 страниц002-Trauma & Burnsmotasem alsharifОценок пока нет
- Atlas of Paranasal Sinus SurgeryДокумент81 страницаAtlas of Paranasal Sinus SurgeryNemer Al-KhtoumОценок пока нет
- Maxillofacial Trauma: Karen Adiel Rances, MD, FPSO-HNSДокумент78 страницMaxillofacial Trauma: Karen Adiel Rances, MD, FPSO-HNSJuan Gabriel SovillaОценок пока нет
- Pediatric and Adult Airway Management of AnesthesiaДокумент141 страницаPediatric and Adult Airway Management of AnesthesiaMulatu MilkiasОценок пока нет
- Orbital Roof Fractures A Clinically Based Classification and Treatment AlgorithmДокумент7 страницOrbital Roof Fractures A Clinically Based Classification and Treatment AlgorithmEl KaranОценок пока нет
- Soft Tissue & Skeletal Injuries of The FaceДокумент20 страницSoft Tissue & Skeletal Injuries of The FaceStevan SaputraОценок пока нет
- Anime VillageДокумент57 страницAnime VillageTaufiq HidayatОценок пока нет
- Y, Z, C-Series and LBG Monitors Spec SheetsДокумент4 страницыY, Z, C-Series and LBG Monitors Spec SheetsTaufiq HidayatОценок пока нет
- E. Cysts: 10. Hidradenoma PapilliferumДокумент4 страницыE. Cysts: 10. Hidradenoma PapilliferumTaufiq HidayatОценок пока нет
- Journal Reading Tonsilitis Akut PDFДокумент6 страницJournal Reading Tonsilitis Akut PDFTaufiq HidayatОценок пока нет
- Nej Me 1114206Документ2 страницыNej Me 1114206Taufiq HidayatОценок пока нет
- CH 29 Patients With Noninfectious Upper Respiratory ProblemsДокумент24 страницыCH 29 Patients With Noninfectious Upper Respiratory Problemsjrflores1284Оценок пока нет
- 2 - Maxillofacial Trauma 18 V2 PDFДокумент28 страниц2 - Maxillofacial Trauma 18 V2 PDFMazen AlwajihОценок пока нет
- Management of Le Fort II Fracture Accompanied With Blowout Fracture of Orbital Base (Case Report)Документ4 страницыManagement of Le Fort II Fracture Accompanied With Blowout Fracture of Orbital Base (Case Report)Anonymous HyPucbHRОценок пока нет
- Lower Limb Injuries Arising From Motorcycle Crashes: Original ArticleДокумент4 страницыLower Limb Injuries Arising From Motorcycle Crashes: Original ArticleSonagnon Sonagnon SonagnonОценок пока нет
- Blueprints - Radiology PDFДокумент134 страницыBlueprints - Radiology PDFBenny KMОценок пока нет
- Basic Management of - Maxillofacial Trauma1Документ26 страницBasic Management of - Maxillofacial Trauma1Pratikshya KothiaОценок пока нет
- Orbital Fracture JournalДокумент11 страницOrbital Fracture JournalPramod KumarОценок пока нет
- Comparison of 3-D Locking Miniplates Versus Conventional Miniplates in Anterior Mandibular FracturesДокумент9 страницComparison of 3-D Locking Miniplates Versus Conventional Miniplates in Anterior Mandibular FracturesInternational Journal of Innovative Science and Research TechnologyОценок пока нет
- Ojanes 2019121113522570 PDFДокумент6 страницOjanes 2019121113522570 PDFArifudin Cipto HusodoОценок пока нет
- Medind - Nic.in Iad t08 s1 Iadt08s1p688Документ11 страницMedind - Nic.in Iad t08 s1 Iadt08s1p688Anonymous S0H8cqgnfiОценок пока нет
- Managing Dental EmergenciesДокумент46 страницManaging Dental EmergenciesBoris AbayevОценок пока нет
- Article 2 - NZMJ Midface FracturesДокумент9 страницArticle 2 - NZMJ Midface FracturesIndra D KristionoОценок пока нет
- Essay Questions For Medipro Offshore Medics Refresher CourseДокумент5 страницEssay Questions For Medipro Offshore Medics Refresher CourseRobert TurnerОценок пока нет
- Journal Analysis of Fractured MandibleДокумент5 страницJournal Analysis of Fractured MandiblePrazna ShafiraОценок пока нет
- Maxillofacial Injuries in The Pediatric PatientДокумент9 страницMaxillofacial Injuries in The Pediatric PatientManena RivoltaОценок пока нет
- Garage Door Injury StatisticsДокумент6 страницGarage Door Injury StatisticsCityNewsTorontoОценок пока нет
- Nasal TraumaДокумент5 страницNasal TraumaRae Marie AquinoОценок пока нет
- Basic Principles in Management of Patients With Maxillofacial InjuriesДокумент11 страницBasic Principles in Management of Patients With Maxillofacial InjuriesVishnu S PattathОценок пока нет
- Signos Radiograficos de Fracturas MandibularesДокумент4 страницыSignos Radiograficos de Fracturas MandibularesFelipe SuárezОценок пока нет
- Risk Factors Contributing To Symptomatic Plate Removal in Orthognathic Surgery PatientsДокумент4 страницыRisk Factors Contributing To Symptomatic Plate Removal in Orthognathic Surgery PatientsAli FaridiОценок пока нет
- Mandibulasr Truma ManagementДокумент18 страницMandibulasr Truma Managementjoal510Оценок пока нет
- 2021 Incidence and Pattern of Mandible Fractures An Urban Tertiary Care Centre ExperienceДокумент5 страниц2021 Incidence and Pattern of Mandible Fractures An Urban Tertiary Care Centre ExperienceSatisha TSОценок пока нет
- Trauma MaksilofacialДокумент69 страницTrauma MaksilofacialgedepambudiОценок пока нет
- Ultimate Surgery MCQДокумент104 страницыUltimate Surgery MCQSivakumar Kathuu KarthikeyanОценок пока нет
- Otter Tail County LawsuitДокумент22 страницыOtter Tail County LawsuitinforumdocsОценок пока нет
- Oral Surgery Part - IДокумент7 страницOral Surgery Part - ISushma Bezwada100% (1)
- Case StudyДокумент15 страницCase StudyMuhamad XalefaОценок пока нет
- Hassan - Pediatric TraumaДокумент12 страницHassan - Pediatric TraumaRicardo GrilloОценок пока нет