Академический Документы
Профессиональный Документы
Культура Документы
Optimizing Treatment Approaches in Seborrheic Dermatitis
Загружено:
Shinta Restyana Widya0 оценок0% нашли этот документ полезным (0 голосов)
75 просмотров17 страницaaaaaaaaaa
Авторское право
© © All Rights Reserved
Доступные форматы
DOC, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документaaaaaaaaaa
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате DOC, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
75 просмотров17 страницOptimizing Treatment Approaches in Seborrheic Dermatitis
Загружено:
Shinta Restyana Widyaaaaaaaaaaa
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате DOC, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 17
The Journal of Clinical and Aesthetic Dermatology
Matrix Medical Communications
Optimizing Treatment Approaches in Seborrheic Dermatitis
Goldenberg Gary, MD
Additional article information
Abstract
Seborrheic dermatitis is a chronic, recurring, cutaneous condition that causes
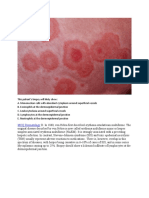
erythema and flaking, sometimes appearing as macules or plaues !ith dry !hite or
moist oily scales" #n adults, it commonly occurs in areas !ith high concentrations of
sebaceous glands" The face and scalp are the most freuently affected areas, and
in$ol$ement of multiple sites is common" Dandruff is regarded as a mild
noninflammatory form of seborrheic dermatitis" There is a high incidence of
seborrheic dermatitis among persons !ith human immunodeficiency $irus infection
or %arkinson&s disease" The cause of seborrheic dermatitis is not !ell understood,
but appears to be related to the composition of the sebaceous gland secretions, the
proliferation of Malessezia yeasts, and the host immune response" Treatment
options for nonscalp and scalp seborrheic dermatitis include topical agents and
shampoos containing antifungal agents, anti'inflammatory agents, keratolytic agents,
and calcineurin inhibitors" (ecause multiple body sites are usually in$ol$ed, the
physician should examine all commonly affected areas" %atients should be made
a!are that seborrheic dermatitis is a chronic condition that !ill probably recur e$en
after successful treatment"
1
Seborrheic dermatitis )SD*, a chronic, recurrent, inflammatory condition
characteri+ed by erythema and skin flaking, may be resistant to treatment and often
has a substantial negati$e impact on uality of life",-. #t affects approximately six
million people in the /nited States and is associated !ith direct and indirect medical
costs of approximately 01.2 million per year"3
Although the causes of SD are not completely understood, progress has been made
in this area, and se$eral effecti$e treatment options are a$ailable" This article !ill
re$ie! the clinical presentation of SD and the current understanding of its etiology
and discuss currently a$ailable treatment options"
2
CLINICAL PRESENTATION
Seborrheic dermatitis may appear as macules or thin plaues !ith a reddish or
yello! appearance and dry !hite or moist oily scales"4 #n adults, it most often occurs
in areas !ith a high concentration of sebaceous glands, including the face, scalp,
ears, chest, and body folds"4 #t usually affects multiple body areas, occurring on the
face in 55 percent of patients, the scalp in 62 percent, the chest in 16 percent, and
the arms or legs in , to 1 percent". #n more than half of patients !ith facial SD, the
scalp is affected as !ell". 7n the face, SD commonly occurs in the nasolabial folds,
eyebro!s, anterior hairline, and glabella",,8 7n the scalp, the lesions may range
from mild desuamation to bro!nish crusts affixed to the skin and hair"4 9esions on
the central chest may ha$e a petaloid appearance"6 Some patients report pruritus,
particularly if the scalp is affected"1,4,8 #t generally is not accompanied by papules or
pustules"1Secondary bacterial infection may occur, aggra$ating erythema and
exudate and causing local discomfort"4
#n adults, SD is a chronic, recurrent condition marked by periods of exacerbation
occurring at $ariable inter$als"8 %atients may report that outbreaks are triggered by
emotional stress, depression, fatigue, exposure to air conditioning or damp or dry
conditions in the !orkplace, systemic infections, use of certain medications, or other
factors".
The infantile form of SD is a self'limited condition generally resol$ing by age three or
four months"8 The adult form usually appears first around the time of puberty, !hen
sebaceous glands become more acti$e, sometimes lasting until young
3
adulthood", The condition increases again in pre$alence after age 42", #t affects
approximately , to 4 percent of immunocompetent adults and as many as 12 to 5.
percent of human immunodeficiency $irus ):#;*'positi$e indi$iduals"4,8 7ther
populations at risk include persons !ith %arkinson&s disease or other neurological
disorders, mood disorders, significant life stress, or lo! exposure to sunlight"1 More
men than !omen ha$e SD, but it sho!s no preference for any racial or ethnic
group"8 #t may occur in association !ith atopic dermatitis or other skin disorders,
complicating its diagnosis"5
Some contro$ersy has surrounded the relationship bet!een SD and dandruff" Most
authors no! agree that dandruff is a mild, noninflammatory form of
SD"1,8,< Dandruff is extremely common, !ith a pre$alence as high as 42 percent of
the population"1
CAUSES OF SEBORREIC DER!ATITIS
Although the causes of SD are not completely understood, it appears to result from a
combination of the follo!ing three factors= sebaceous gland secretion, presence
ofMalassezia yeast, and the host immune response"8
Sebum is an important component of skin surface lipids and contains high amounts
of sualene, !ax esters, and triglycerides",2 %ersons !ith SD do not necessarily
ha$e excess sebaceous gland acti$ity, but the composition of their skin surface lipid
may be altered, creating a more supporti$e en$ironment for gro!th of lipid'
dependent micro'organisms",2
4
The role of Malassezia yeasts in SD is some!hat contro$ersial, although most
researchers belie$e they play an important role"< Malassezia yeasts are normally
commensal species found primarily in follicular infundibula and commonly isolated
from sebum'rich areas of the body, such as the face, scalp, trunk, and back",, They
produce abundant lipases that hydroly+e triglycerides and free saturated fatty acids
on !hich the yeast is dependent",1 These fatty acids may ha$e irritant effects that
induce scaling or may cause release of arachidonic acid, !hich promotes
inflammation in skin"< There are se$en primary species= M. globosa, M. restricta, M.
obtusa, M. sloojjiae, M. sympodialis, M. jurjur, and M. pachydermatis )the last occurs
only on animals*"< M. globosa and M. restricta are thought to be the species most
commonly associated !ith SD, although M. jurjur and other species ha$e also been
implicated"<,,.,,3 Some studies ha$e found high numbers of Malassezia yeasts on
the scalp of persons !ith SD, but others ha$e found no difference in the density of
these yeasts bet!een the skin of persons !ith SD and that of persons !ithout
it", Differing sampling methods may contribute to these contradictory
findings" Malassezia exist not only on the skin surface, but also !ithin the layers of
the stratum corneum, and a true count !ould reuire examining the full thickness of
the skin suama", Support for the role of Malassezia in SD comes from studies
demonstrating that use of $arious antifungal treatments results in reduction
of Malassezia, !hich is accompanied by impro$ement in symptoms"8,<
The role of the host immune response in the pathogenesis of SD is uncertain" Some
researchers ha$e reported increased numbers of natural killer cells, CD,8 cells, and
5
inflammatory interleukins and acti$ation of complement in the lesional skin of
patients !ith SD compared !ith their o!n nonlesional skin or the skin of healthy
controls"8 >e$ertheless, total antibody le$els are no higher in SD patients than in
controls and a host response specific to Malassezia yeasts has not been
identified"<The pre$alence of SD in persons infected !ith :#; suggests that the
condition is mediated by the immune system? ho!e$er, the response of SD to
successful retro$iral therapy is $ariable"4
Thus, a definiti$e understanding of the pathophysiology of SD a!aits further
research, but the role of Malassezia yeasts as causati$e or contributing agents
appears to be !ell established"
DIA"NOSIS
The differential diagnosis of SD should include psoriasis,
rosacea, Demodex dermatitis, atopic ec+ema, pityriasis $ersicolor, contact
dermatitis, and tinea infections"1 SD may also resemble 9angerhans cell
histiocytosis or secondary syphilis"1,4 The diagnosis is usually clinical, but
candidiasis, tinea infection, and Demodex dermatitis may be ruled out !ith a
negati$e potassium hydroxide test"1 #t should be kept in mind that SD may be
accompanied by other dermatological disorders"
Care should be taken to differentiate SD from psoriasis $ulgaris",4 @arly SD has a
spongiform appearance that distinguishes it from psoriasis, but in later stages these
conditions are more difficult to tell apart" Some patients present !ith sebopsoriasis,
6
!hich includes features of both disease states"1 9esions on the elbo!s or knees and
nail pitting suggest psoriasis, !hich may spare the face",4
TREAT!ENT
The primary goals of therapy for SD are to clear the $isible signs of disease and
reduce bothersome symptoms, especially pruritus"8 (ecause the face and scalp are
the most commonly affected areas, itching or redness on the scalp in a patient !ith
facial SD indicates the need for treatment at both sites". %atients should be informed
that SD is a chronic, relapsing condition and that they should anticipate future
outbreaks",8 %atients should also be ad$ised to a$oid triggers of SD symptoms to
the extent possible and not to irritate the lesions by excessi$e scratching or use of
potent keratolytic preparations",8,,6
NONSCALP SEBORREIC DER!ATITIS
Antifungal agents, anti'inflammatory agents, and keratolytic agents are a$ailable in a
$ariety of formulations for treatment of SD on areas other than the scalp" Table , lists
commonly used treatments for nonscalp SD and indicates the le$el of e$idence that
supports their use"
TA(9@ ,
Treatments for nonscalp seborrheic dermatitis
7
Antifungal agents. Aith the understanding of the role of Malassezia in SD,
antifungal agents ha$e taken on an important role in its treatment" Betocona+ole 1C
cream applied t!ice daily for four !eeks has been sho!n to be as effecti$e as
hydrocortisone ,C cream in treatment of SD at multiple body sites",5 #n a
randomi+ed, double'blind trial of 34< patients !ith SD treated !ith ketocona+ole 1C
gel or $ehicle once daily for ,3 days, there !as a significantly higher rate of
successful treatment )14".C $s" ,."<C,PD2"22,3* and significantly greater
reductions in erythema, pruritus, and scaling in ketocona+ole'treated patients",< A
1C foam formulation of ketocona+ole has been sho!n to be significantly more
effecti$e than $ehicle for treatment of SD on the face, scalp, and body, and eually
as effecti$e as ketocona+ole 1C cream"12
Ciclopiroxolamine ,C cream, t!ice daily for 15 days follo!ed by once daily for 15
days, !as compared !ith $ehicle for the treatment of SD in a randomi+ed,
doubleblind trial that enrolled ,1< patients"1, At the end of the maintenance phase,
complete disappearance of erythema and scaling !as found in 8. percent of the
ciclopiroxolamine'treated group and .3 percent of the $ehicle'treated group
)PE2"226*"1,
#n an open'label study of sertacona+ole nitrate 1C cream, 4< percent of 12 subFects
!ith mild'to'se$ere SD !ere successfully treated, !ith impro$ements in scaling,
erythema, induration, and pruritus"11
8
A randomi+ed, double'blind study demonstrated that metronida+ole 2"64C gel is as
effecti$e as ketocona+ole 1C cream in treatment of facial SD, !ith a similar side
effect profile"1.
Gor patients !ith persistent SD resistant to topical agents, oral antifungals may be an
option" 7ral itracona+ole gi$en in a dose of 122mgHday for one !eek, follo!ed by a
maintenance dose, resulted in clinical impro$ement of SD symptoms in t!o open'
label trials"13,14
Corticosteroids. :ydrocortisone and a !ide $ariety of other lo!' to mid'potency
corticosteroids ha$e been used successfully in the treatment of SD" A double'blind
study that compared hydrocortisone ,C cream !ith ketocona+ole 1C cream in 61
patients !ith mild'to'moderate SD found that the t!o agents produced similar rates
of response and similar reductions in scaling, redness, itching, and papules"18 #n a
,1'!eek, single'blind, randomi+ed, comparati$e trial, hydrocortisone ,C ointment
!as found to be eually as effecti$e as tacrolimus 2",C ointment in reducing the
symptoms of facial SD by physician assessment, although tacrolimus !as superior
by patient assessment"16
Combination antifungal/anti-inflammatory. %romisebI Topical Cream )%romius
%harma, 99C, (ridge!ater, >e! Jersey* is a nonsteroidal prescription medical
de$ice !ith anti'inflammatory and antifungal acti$ity appro$ed for treatment of
SD"15 #n an in$estigator'blind, parallel'group study, 66 patients !ith mild or
moderate SD of the face !ere randomi+ed to combination antifungalHanti'
inflammatory cream or desonide 2"24C cream t!ice daily for up to 15
9
days"1< Se$erity of symptoms declined significantly from baseline to Day ,3 and
Day 15 in both groups"1< Treatment !as successful )clear or almost clear* in 54
percent of patients using combination antifungalHanti'inflammatory cream and <1
percent of patients using desonide cream )PDnot significant* and the t!o products
had similar safety profiles"1<
Calcineurin inhibitors. Topical calcineurin inhibitors ha$e immunomodulatory and
anti'inflammatory properties that make them useful in the treatment of SD"16
Tacrolimus 2",C ointment !as found to be as effecti$e as hydrocortisone ,C
ointment in the treatment of SD, reuired fe!er applications during the ,1'!eek
study period because of clearing of symptoms, and !as rated more fa$orably by
patients"16
#n a randomi+ed, open'label trial, pimecrolimus ,C cream !as compared !ith
betamethasone 2",C cream in 12 patients !ith SD !ho !ere instructed to
discontinue treatment !hen symptoms cleared".2 (y Day <, all patients had
discontinued treatment".2 The t!o drugs !ere eually effecti$e at reducing
symptoms of erythema, scaling, and pruritus, but symptom relief !as sustained
longer in the pimecrolimus group".2 #n comparati$e trials, pimecrolimus ,C cream
has been sho!n to be as effecti$e as hydrocortisone ,C cream and ketocona+ole
1C cream in the treatment of SD, !ith higher rates of ad$erse
effects".,,.1 %imecrolimus ,C cream !as found to be significantly more effecti$e for
treatment of facial SD than methylprednisolone 2",C cream or metronida+ole 2"64C
10
gel !hen applied t!ice daily for eight !eeks, !ith fe!er ad$erse effects and a lo!er
rate of recurrence than metronida+ole"..
SCALP SEBORREIC DER!ATITIS
Seborrheic dermatitis of the scalp is most con$eniently treated !ith shampoos
containing antifungal agents, corticosteroids, or keratolytic agents? products are also
a$ailable that combine drugs from these different classes" Table 1 lists commonly
used treatments for SD of the scalp and indicates the le$el of e$idence that supports
their use"
TA(9@ 1
Treatments for seborrheic dermatitis of the scalp
Antifungal shampoos. Betocona+ole 1C shampoo !as compared !ith selenium
sulfide 1"4C shampoo in a four'!eek, randomi+ed, double'blind trial of patients !ith
moderate'to'se$ere dandruff".3 T!ice'!eekly use of either shampoo !as superior to
placebo, but not significantly different from each other".3 There !as a significantly
higher incidence of ad$erse effects among patients using selenium sulfide
shampoo".3
Ciclopirox ,C shampoo used once or t!ice !eekly for four !eeks !as sho!n to be
superior to $ehicle for treatment of SD in a randomi+ed, double'blind, controlled
11
study that recruited <3< patients".4 Subseuent prophylactic use of ciclopirox
shampoo once !eekly or once e$ery t!o !eeks reduced the relapse rate".4
Ciclopirox shampoo and ketocona+ole shampoo !ere compared in a double'blind
study of .42 patients !ith SD".8 The t!o treatments !ere eually effecti$e and both
better than placebo, although patients rated the ciclopirox shampoo more
fa$orably".8
Corticosteroid shampoos. #n a randomi+ed, single'blind study of .18 subFects !ith
moderate'to'se$ere scalp SD, clobetasol propionate 2"24C shampoo t!ice !eekly
for four !eeks produced a significantly greater reduction in symptoms than
ketocona+ole 1C shampoo".6 Alternating use of clobetasol shampoo and
ketocona+ole shampoo !as also superior to ketocona+ole shampoo alone".6
Combination products. %romisebI %lus Scalp Aash )%romius %harma, 99C*
contains surfactants and skin conditioning agents, !hich remo$e excess sebum as
!ell as lactoferrin and piroctone olamine, !hich may reduce the proliferation
ofMalassezia".5 #n an open'label trial, 14 subFects !ith SD used this proprietary
!ash an a$erage of t!ice !eekly for t!o !eeks".5 All 14 had a positi$e response
and more than <2 percent reported impro$ement in seborrhea, dandruff, pruritus,
and redness".5
#n a single'blind study, a shampoo containing ciclopiroxolamine ,"4C and salicylic
acid .C !as sho!n to ha$e efficacy similar to that of ketocona+ole 1C shampoo for
12
the treatment of dandruffHSD".< Gor both groups, impro$ement !as sustained for ,3
days after treatment ended".<
A shampoo containing ciclopiroxolamine ,"4C and +inc pyrithione ,C !as found to
be as effecti$e as ketocona+ole 1C foaming gel in a single'blind study of ,5<
patients !ith scalp SD, !ith a greater reduction in pruritus during the early treatment
phase and more fa$orable ratings from patients"32
Keratolytic products. A randomi+ed, double'blind study compared a shampoo
containing lipohydroxy acid 2",C and salicylic acid ,".C !ith a shampoo containing
ciclopiroxolamine ,"4C and salicylic acid .C in ,22 subFects !ith scalp SD"3, After
four !eeks of treatment, the tolerance, global efficacy, and cosmetic effects of the
lipohydroxy acid shampoo !ere significantly superior to those of the
ciclopiroxolamine shampoo"3,
A topical solution of urea, propylene glycol, and lactic acid, applied daily for four
!eeks then three times per !eek for four !eeks, !as compared !ith placebo for
treatment of mild'to'se$ere SD of the scalp"31 @rythema and desuamation !ere
impro$ed at Aeeks 1 and 3, but the impro$ements !ere not maintained at eight
!eeks"31
CONCLUSION
Seborrheic dermatitis is a common, chronic, inflammatory cutaneous condition
characteri+ed by erythema and skin flaking that tends to recur e$en after successful
treatment and has a significant negati$e impact on uality of life" #ts occurrence
13
appears to be related to the proliferation of commensal Malassezia species"
7ccurrence at multiple body sites is common? the face and scalp are the most
freuently affected areas" >umerous antifungal, anti'inflammatory, keratolytic, and
immunomodulatory agents ha$e been sho!n to be effecti$e in the treatment of SD,
but patients should be informed that recurrence is common and that ongoing
treatment may be necessary"
Footnotes
DISCLOSURE: Dr# "o$%enberg reports no re$e&ant con'$icts o' interest# !an(script %e&e$opment )as
s(pporte% b* Promi(s Pharma+ LLC#
Artic$e in'ormation
, C$in Aesthet Dermato$# Feb -./01 23-45 66768#
P!CID5 P!C09:86;;
"o$%enberg "ar*+ !D
!o(nt Sinai Schoo$ o' !e%icine+ Department o' Dermato$og*+ Ne) <or=+ Ne) <or=
Correspon%ing a(thor#
ADDRESS CORRESPONDENCE TO: "ar* "o$%enberg+ !D+ 9 East 8;th St+ Bo> /.6;+ Ne) <or=+ N<
/..-81 E?mai$5 "ar*go$%enbergm%@at@gmai$#com
Cop*right notice
Artic$es 'rom The ,o(rna$ o' C$inica$ an% Aesthetic Dermato$og* are pro&i%e% here co(rtes* o' Matrix
Medical Communications
REFERENCES
," (iko!ski J" Gacial seborrheic dermatitis= a report on current status and therapeutic
hori+ons" J Drugs Dermatol" 122<?5)1*=,14-,.." J%ubMedK
1" Gupta AB, (luhm L, Cooper @A, et al" Seborrheic dermatitis" Dermatol
Clin"122.?1,=32,-,,1" J%ubMedK
." %eyri J, 9leonart M" and the Spanish Group of the S@(D@LM 11" Study" Clinical
and therapeutic profile and uality of life of patients !ith seborrheic dermatitis" Actas
Dermosifiliogr" 1226?<5=368-51" J%ubMedK
3" (ickers DL, 9im :A, Margolis D, et al" The burden of skin diseases= 1223" J Am
Acad Dermatol" 1228?44=3<2-422" J%ubMedK
4" Sampaio A9, Mameri AC, ;argas TJ, et al" Seborrheic dermatitis" An (ras
Dermatol"12,,?58=,28,-,263" J%ubMedK
14
8" Del Losso JM" Adult seborrheic dermatitis" A status report on practical topical
management" J Clin Aesthet Dermatol" 12,,?3)4*=.1-.5" J%MC free articleK J%ubMedK
6" Leider >, Gritsch %7" Seborrheic dermatitis" #n= (olognia J9, Jori++o J9, Schaffer
J;, editors" Dermatology" .rd ed" %hiladelphia= %enn= @lse$ier? 12,1"
5" Del Losso JM, Bim GB" Seborrheic dermatitis and Malassezia species= ho! are
they relatedN J Clin Aesthet Dermatol" 122<?1),,*=,3-,6" J%MC free
articleK J%ubMedK
<" Gupta AB, (atra L, (luhm L, et al" Skin diseases associated !ith Malasse+ia
species" J Am Acad Dermatol" 1223?4,=654-6<5" J%ubMedK
,2" De 9uca C, ;alacchi G" Surface lipids as multifunctional mediators of skin
responses to en$ironmental stimuli" Mediators #nflamm" 12,2?12,2=.1,3<3" J%MC
free articleKJ%ubMedK
,," :ay LJ" Malassezia, dandruff and seborrhoeic dermatitis= an o$er$ie!" (r J
Dermatol"12,,?,84)Suppl 1*=1-5" J%ubMedK
,1" Da!son T9", Jr" Malassezia globosa and restrica: breakthrough understanding of
the etiology and treatment of dandruff and seborrheic dermatitis through !hole'
genome analysis" J #n$est Dermatol Symp %roc" 1226?,1=,4-,<" J%ubMedK
,." 9ee OA, (yun :J, Bim (J, et al" Distribution of Malassezia species on the scalp
in Borean seborrheic dermatitis patients" Ann Dermatol" 12,,?1.)1*=,48-,8,"J%MC
free articleK J%ubMedK
,3" >akabayashi A, Sei O, Guillot J" #dentification of Malasse+ia species isolated from
patients !ith seborrheic dermatitis, atopic dermatitis, pityriasis $ersicolor and normal
subFects" Med Mycol" 1222?.5=..6-.3," J%ubMedK
,4" :abif T%" %soriasis and other papulosuamous diseases" #n= :abif T%,
editor" Clinical Dermatology= A Color Guide to Diagnosis and Therapy" 4th ed"
%hiladelphia= %enn= @lse$ier? 12,2"
,8" Gaergemann J" Management of seborrheic dermatitis and pityriasis
$ersicolor" Am J Clin Dermatol" 1222?,)1*=64-52" J%ubMedK
,6" Stefanaki #, Batsambasa A" Therapeutic update on seborrheic dermatitis" Skin
Therapy 9ett" 12,2?,4)4*=,-3" J%ubMedK
,5" Batsambas A, Antoniou C:, Grangouli @, et al" A double'blind trial of treatment of
seborrheic dermatitis !ith 1C ketocona+ole cream compared !ith ,C
hydrocortisone cream" (r J Dermatol" ,<5<?,1,=.4.-.46" J%ubMedK
,<" @le!ski (, 9ing ML, %hillips TJ" @fficacy and safety of a ne! once'daily topical
ketocona+ole 1C gel in the treatment of seborrheic dermatitis= a phase ### trial" J
Drugs Dermatol" 1228?4)6*=838-842" J%ubMedK
12" @le!ski (@, Abramo$its A, Bempers S, et al" A no$el foam formulation of
ketocona+ole 1C for the treatment of seborrheic dermatitis on multiple body
regions" J Drugs Dermatol" 1226?8),2*=,22,-,225" J%ubMedK
15
1," Dupuy %, Maurette C, Amoric JC, et al" Landomi+ed, placebo'controlled, double'
blind study on clinical efficacy of ciclopiroxolamine ,C cream in facial seborrhoeic
dermatitis" (r J Dermatol" 122,?,33=,2..-,2.6" J%ubMedK
11" @le!ski (@, Cantrell AC" An open'label study of the safety and efficacy of
sertacona+ole nitrate in the treatment of seborrheic dermatitis" J Drugs
Dermatol"12,,?,2)5*=5<4-5<<" J%ubMedK
1." Seckin D, Gurbu+ 7, Akin 7" Metronida+ole 2"64C gel $s" ketocona+ole 1C
cream in the treatment of facial seborrheic dermatitis= a randomi+ed, double'blind
study" J @ur Acad Dermatol ;enereol" 1226?1,=.34-.42" J%ubMedK
13" Shemer A, Baplan (, >athansohn >, et al" Treatment of moderate to se$ere
facial seborrheic dermatitis !ith itracona+ole= an open non'comparati$e study" #sr
Med Assoc J"1225?,2=3,6-,,5" J%ubMedK
14" Bose 7, @rbil :, Gur AL" 7ral itracona+ole for the treatment of seborrhoeic
dermatitis= an open, noncomparati$e trial" J @ur Acad Dermatol
;enereol" 1224?,<=,61-,64"J%ubMedK
18" Stratigos JD, Antoniou C, Batsambas A, et al" Betocona+ole 1C cream $ersus
hydrocortisone ,C cream in the treatment of seborrheic dermatitis" A double'blind
comparati$e study" J Am Acad Dermatol" ,<55?,<=542-54." J%ubMedK
16" %app BA, %app A, Dahmer (, Clark CS" Single'blind, randomi+ed controlled trial
e$aluating the treatment of facial seborrheic dermatitis !ith hydrocortisone ,C
ointment compared !ith tacrolimus 2",C ointment in adults" J Am Acad
Dermatol" 12,1?86=e,,-e,4" J%ubMedK
15" Bircik 9" An open'label, single'center pilot study to determine the antifungal
acti$ity of a ne! nonsteroidal cream )%romiseb Topical Cream* after 6 days of use in
healthy $olunteers" Clin Dermatol" 122<?16)Suppl*=S33-S36" J%ubMedK
1<" @le!ski (" An in$estigator'blind, randomi+ed, 3'!eek, parallel'group, multicenter
pilot study to compare the safety and efficacy of a nonsteroidal cream )%romiseb
Topical Cream* and desonide cream 2"24C in the t!ice'daily treatment of mild to
moderate seborrheic dermatitis of the face" Clin Dermatol" 122<?16)Suppl*=S35-
S4." J%ubMedK
.2" Ligopoulos D, #oannides D, Balogeromitros D, et al" %imecrolimus cream ,C $s"
betamethasone ,6'$alerate 2",C cream in the treatment of seborrhoeic dermatitis" A
randomi+ed open'label clinical trial" (r J Dermatol" 1223?,4,=,26,-,264" J%ubMedK
.," Giroo+ A, Solhpour A, Gorouhi G, et al" %imecrolimus cream, ,C, $s"
hydrocortisone acetate cream, ,C, in the treatment of facial seborrheic dermatitis= a
randomi+ed, in$estigator'blind, clinical trial" Arch Dermatol" 1228?,31)5*=,284-
,258" J%ubMedK
.1" Boc @, Arca @, Bose 7, Akar A" An open, randomi+ed, prospecti$e, comparati$e
study of topical pimecrolimus ,C cream and topical ketocona+ole 1C cream in the
treatment of seborrheic dermatitis" J Dermatol Treat" 122<?12),*=3-<" J%ubMedK
16
.." Cicek D, Bandi (, (akar S, Turgut D" %imecrolimus ,C cream,
methylprednisolone aceponate 2",C cream and metronida+ole 2"64C gel in the
treatment of seborrheic dermatitis= a randomi+ed clinical study" J Dermatol
Treat" 122<?12=.33-.3<" J%ubMedK
.3" Danby GA, Maddin AS, Margesson 9J, Losenthal D" A randomi+ed, double'
blind, placebo'controlled trial of ketocona+ole 1C shampoo $ersus selenium sulfide
1"4C shampoo in the treatment of moderate to se$ere dandruff" J Am Acad
Dermatol",<<.?1<=,225-,2,1" J%ubMedK
.4" Shuster S, Meynadier J, Berl :, >olting S" Treatment and prophylaxis of
seborrheic dermatitis of the scalp !ith antipityrosporal ,C ciclopirox shampoo" Arch
Dermatol"1224?,3,=36-41" J%ubMedK
.8" Latna$el LC, Suire LA, (oorman GC" Clinical efficacies of shampoos
containing ciclopirox olamine ),"4C* and ketocona+ole )1"2C* in the treatment of
seborrhoeic dermatitis" J Dermatol Treat" 1226?,5=55-<8" J%ubMedK
.6" 7rtonne J'%, >ikkels AG, Leich B, et al" @fficacious and safe management of
moderate to se$ere scalp seborrhoeic dermatitis using clobetasol propionate
shampoo 2"24C combined !ith ketocona+ole shampoo 1C= a randomi+ed,
controlled study" (r J Dermatol"12,,?,84=,6,-,68" J%ubMedK
.5" Bircik 9" SubFect e$aluation of the treatment of seborrheic dermatitis of the scalp
!ith a non'steroidal scalp !ash" %oster presented at= 12,1 Ainter Clinical
Dermatology Conference? January ,3',<, 12,1? Baanapali, :a!aii"
.<" Suire LA, Goode B" A randomised, single'blind, single'centre clinical trial to
e$aluate comparati$e clinical efficacy of shampoos containing ciclopirox olamine
),"4C* and salicylic acid ).C*, or ketocona+ole )1C, >i+oralI* for the treatment of
dandruffHseborrhoeic dermatitis" J Dermatol Treat" 1221?,.=4,-82" J%ubMedK
32" 9orette G, @rmosilla ;" Study #n$estigators Group" Clinical efficacy of a ne!
ciclopiroxolamineH+inc pyrithione shampoo in scalp seborrheic dermatitis
treatment" @ur J Dermatol" 1228?,8)4*=445-483" J%ubMedK
3," Seite S, Lougier A, Talarico S" Landomi+ed study comparing the efficacy and
tolerance of a llipohydroxy acid shampoo to a ciclopiroxolamine shampoo in the
treatment of scalp seborrheic dermatitis" J Cosmet Dermatol" 122<?5=13<-
14." J%ubMedK
31" @mtestam 9, S$ensson A, Lensfeldt B" Treatment of seborrheic dermatitis of the
scalp !ith a topical solution of urea, lactic acid, and propylene glycol )B.2,*= results
of t!o double'blind, randomised, placebo'controlled
studies" Mycoses" 12,1?44)4*=.<.-32."J%ubMedK
17
Вам также может понравиться
- Optimizing Treatment Approaches in Seborrheic Dermatitis: (Literature Review)Документ6 страницOptimizing Treatment Approaches in Seborrheic Dermatitis: (Literature Review)Andika Anjani AgustinОценок пока нет
- Seborrheic Dermatitis in Adolescents and AdultsДокумент51 страницаSeborrheic Dermatitis in Adolescents and AdultsCosmina GeorgianaОценок пока нет
- Clear Skin at Any Age: A Guide for Mature Women: Glowing Skin Solutions, #1От EverandClear Skin at Any Age: A Guide for Mature Women: Glowing Skin Solutions, #1Оценок пока нет
- Diagnosisandmanagementof Psoriasisinchildren: Megha M. TollefsonДокумент17 страницDiagnosisandmanagementof Psoriasisinchildren: Megha M. TollefsonMasithaОценок пока нет
- Adalsteinsson2020 Inmunologia de La Dermatitis SeborreicaДокумент9 страницAdalsteinsson2020 Inmunologia de La Dermatitis SeborreicaLaura GarciaОценок пока нет
- Seborrheic Dermatitis of The Scalp Etiology and TreatmentДокумент9 страницSeborrheic Dermatitis of The Scalp Etiology and TreatmentAndi WahyuniОценок пока нет
- Jurnal Dermatitis Seboroik 3 (Easti)Документ8 страницJurnal Dermatitis Seboroik 3 (Easti)Easti vishiara amdelyОценок пока нет
- 3 PDFДокумент6 страниц3 PDFsandra magdalenaОценок пока нет
- Chapter IIДокумент12 страницChapter IIellyzaherbolingo0Оценок пока нет
- Psoriasis A Case StudyДокумент14 страницPsoriasis A Case StudyYayin PestañoОценок пока нет
- Psoriasis: PathophysiologyДокумент23 страницыPsoriasis: PathophysiologyImran KhanОценок пока нет
- Final OutputДокумент12 страницFinal Outputellyzaherbolingo0Оценок пока нет
- Dermatitis Seboroik PDFДокумент7 страницDermatitis Seboroik PDFscaindrianie2903Оценок пока нет
- Diagnosa Dan Terapi SSSS PDFДокумент6 страницDiagnosa Dan Terapi SSSS PDFni putu.comsurya dianaОценок пока нет
- Background: National Rosacea SocietyДокумент18 страницBackground: National Rosacea SocietyPanda OnlineShopОценок пока нет
- Research Paper On EczemaДокумент7 страницResearch Paper On Eczemauziianwgf100% (1)
- Diagnosis and Treatment of Rosacea: Aaron F. Cohen, MD, and Jeffrey D. Tiemstra, MDДокумент4 страницыDiagnosis and Treatment of Rosacea: Aaron F. Cohen, MD, and Jeffrey D. Tiemstra, MDbookaholic7Оценок пока нет
- Chapter 26:: Seborrheic Dermatitis:: Dae Hun Suh: Clinical FeaturesДокумент10 страницChapter 26:: Seborrheic Dermatitis:: Dae Hun Suh: Clinical FeaturesmyztОценок пока нет
- Jadotte Pityriasis AlbaДокумент8 страницJadotte Pityriasis Albapene asoyОценок пока нет
- 887 1445 1 SM PDFДокумент7 страниц887 1445 1 SM PDFazrinaОценок пока нет
- Jurnal Reading DAДокумент18 страницJurnal Reading DAWinendy Deo HaryantoОценок пока нет
- Glacial RXДокумент15 страницGlacial RXcarloshgmedeirosОценок пока нет
- Oral Lupus ErythematosusДокумент9 страницOral Lupus ErythematosusputriОценок пока нет
- Seborrehic DermatitisДокумент25 страницSeborrehic DermatitisHallidayОценок пока нет
- Rosacea: Clinical PracticeДокумент11 страницRosacea: Clinical PracticeLusy Dwitama LeryОценок пока нет
- DamevskamelasmasjdvДокумент15 страницDamevskamelasmasjdvlaithuyduong007Оценок пока нет
- Isi RefreshingДокумент73 страницыIsi RefreshingKarina Sandra AmiliaОценок пока нет
- Scalp Seborrheic Dermatitis: What We Know So Far: Skin Appendage DisordersДокумент5 страницScalp Seborrheic Dermatitis: What We Know So Far: Skin Appendage DisordersSergio Revuelta HernándezОценок пока нет
- 4 203567156179239592 PDFДокумент47 страниц4 203567156179239592 PDFGg KОценок пока нет
- Plaque Psoriasis: Understanding Risk Factors of This Inflammatory Skin PathologyДокумент14 страницPlaque Psoriasis: Understanding Risk Factors of This Inflammatory Skin PathologyOktavianti Prisilia SoumokilОценок пока нет
- Psoriasis Related Medindia Resources1119scribdДокумент2 страницыPsoriasis Related Medindia Resources1119scribdNicole BensonОценок пока нет
- Pityriasis Capitis: Causes, Pathophysiology, Current ModalitiesДокумент13 страницPityriasis Capitis: Causes, Pathophysiology, Current ModalitiesShashikant DrShashikant BagadeОценок пока нет
- Dissertation On EczemaДокумент7 страницDissertation On EczemaDoMyPapersUK100% (1)
- Articulo Ingles 2 GinaДокумент8 страницArticulo Ingles 2 GinassariedmartinezОценок пока нет
- Pics MCQSДокумент22 страницыPics MCQStania100% (1)
- Clinical Presentation, Risk Factors and Outcomes of Demographic Analysis of Blepharitis in Adults Presenting at Multiple Healthcare CentresДокумент4 страницыClinical Presentation, Risk Factors and Outcomes of Demographic Analysis of Blepharitis in Adults Presenting at Multiple Healthcare CentresNydia OngaliaОценок пока нет
- (Serbian Journal of Dermatology and Venereology) National Guidelines For The Treatment of Atopic DermatitisДокумент25 страниц(Serbian Journal of Dermatology and Venereology) National Guidelines For The Treatment of Atopic DermatitisFebtri IRnawitaОценок пока нет
- Approach To The Patient With Facial Erythema PDFДокумент38 страницApproach To The Patient With Facial Erythema PDFFilipa FigueiredoОценок пока нет
- Dermatitis Atopik PDFДокумент11 страницDermatitis Atopik PDFmlengseОценок пока нет
- Pityriasis RoseaДокумент13 страницPityriasis Roseagagauzne196950% (2)
- 2545-Article Text-7661-1-10-20190414 PDFДокумент6 страниц2545-Article Text-7661-1-10-20190414 PDFClariza ZulyanОценок пока нет
- Psoriasis Research PaperДокумент4 страницыPsoriasis Research Papervvjrpsbnd100% (1)
- The Story Behind Flaky Scalp Presentation For HandoutsДокумент58 страницThe Story Behind Flaky Scalp Presentation For Handoutspriskilas911Оценок пока нет
- Systemic Scleroderma: Genetics Home ReferenceДокумент6 страницSystemic Scleroderma: Genetics Home ReferenceNarendraswari Mendina KusumawardhaniОценок пока нет
- Psoriasis: A Comprehensive Review: Nternational Ournal OF Harmacy & IFE CiencesДокумент21 страницаPsoriasis: A Comprehensive Review: Nternational Ournal OF Harmacy & IFE Ciences24hintheghettoworkoutОценок пока нет
- Diagnosis and Treatment of Allergic Skin Disorders in The ElderlyДокумент9 страницDiagnosis and Treatment of Allergic Skin Disorders in The ElderlyfelipetheОценок пока нет
- Psoriasis - StatPearls - NCBI BookshelfДокумент8 страницPsoriasis - StatPearls - NCBI BookshelfMehmet TaşçıОценок пока нет
- Jurnal Dermatitis SeboroikДокумент10 страницJurnal Dermatitis Seboroikseptsepta1609Оценок пока нет
- Seborrheic Dermatitis From JurnalДокумент6 страницSeborrheic Dermatitis From JurnalindciwОценок пока нет
- Atopic Dermatitis: Review Open AccessДокумент7 страницAtopic Dermatitis: Review Open AccessaraaritonangОценок пока нет
- Stevens-Johnson Syndrome CASEДокумент38 страницStevens-Johnson Syndrome CASEChristy Rose AgrisОценок пока нет
- Manila Central UniversityДокумент5 страницManila Central UniversityRajan ChaudharyОценок пока нет
- Derm Online Resource Pack PDFДокумент81 страницаDerm Online Resource Pack PDFOlaОценок пока нет
- Melasma: An Up-to-Date Comprehensive Review: Oluwatobi A. Ogbechie-Godec Nada ElbulukДокумент14 страницMelasma: An Up-to-Date Comprehensive Review: Oluwatobi A. Ogbechie-Godec Nada ElbulukDra Natalia Maria ZuluagaОценок пока нет
- Fluconazole and Its Place in The Treatment of Seborrheic DermatitisДокумент4 страницыFluconazole and Its Place in The Treatment of Seborrheic DermatitisurusetiaОценок пока нет
- 5: Allergy and The Skin: Eczema and Chronic Urticaria: Mja Practice Essentials - AllergyДокумент6 страниц5: Allergy and The Skin: Eczema and Chronic Urticaria: Mja Practice Essentials - AllergyDavid PattersonОценок пока нет
- Dermodex, Estudo CientificoДокумент10 страницDermodex, Estudo CientificoSantinno JrОценок пока нет
- DermatitisДокумент2 страницыDermatitisRonyRizkОценок пока нет
- Bruce Lyon - Occult CosmologyДокумент55 страницBruce Lyon - Occult Cosmologyeponymos100% (1)
- Food and Beverages Sample Script For NCAДокумент11 страницFood and Beverages Sample Script For NCAHONEY ROSE NAKILAОценок пока нет
- Criteria For Decorative Cosmetics PDFДокумент3 страницыCriteria For Decorative Cosmetics PDFsamudra540Оценок пока нет
- Class 12 Psychology PDFДокумент209 страницClass 12 Psychology PDFSoumyashis Bhattacharya0% (1)
- GalvInfoNote 1 4Документ4 страницыGalvInfoNote 1 4rplata63Оценок пока нет
- TM 55 1520 236 23P 1Документ843 страницыTM 55 1520 236 23P 1Tod A. Wulff100% (1)
- STAT 713 Mathematical Statistics Ii: Lecture NotesДокумент152 страницыSTAT 713 Mathematical Statistics Ii: Lecture NotesLiban Ali MohamudОценок пока нет
- Chapter 8 - Nervous ReviewerДокумент18 страницChapter 8 - Nervous Reviewerchristian anchetaОценок пока нет
- A. Questions: Conversation Activities - TravelДокумент11 страницA. Questions: Conversation Activities - TravelkicsirekaОценок пока нет
- Lesson Plan 3Документ3 страницыLesson Plan 3api-547884261Оценок пока нет
- Discussion 2 Module 2 - Paronda PDFДокумент1 страницаDiscussion 2 Module 2 - Paronda PDFAlvanna ParondaОценок пока нет
- 2 2 1 1 5b Equipmend Data Sheets CommДокумент40 страниц2 2 1 1 5b Equipmend Data Sheets CommMilic MilicevicОценок пока нет
- 1 An Introduction Basin AnalysisДокумент29 страниц1 An Introduction Basin AnalysisMuhamadKamilAzharОценок пока нет
- Chapter 34 Area MethodДокумент14 страницChapter 34 Area Methodthorgod941500% (1)
- Capsicums - Innovative Uses of An Ancient CropДокумент11 страницCapsicums - Innovative Uses of An Ancient CropMaarioОценок пока нет
- Fisher N551 ESVДокумент2 страницыFisher N551 ESVWynn ChoОценок пока нет
- RediFlex Hoses Data SheetДокумент2 страницыRediFlex Hoses Data SheetNordson Adhesive Dispensing SystemsОценок пока нет
- CHAPTER 48 - Skin Integrity & Wound CareДокумент3 страницыCHAPTER 48 - Skin Integrity & Wound CareAОценок пока нет
- 3rd Quarter PHYSICAL SCIENCE ExamДокумент19 страниц3rd Quarter PHYSICAL SCIENCE ExamZhering RodulfoОценок пока нет
- Pid 14 MT23 160412Документ20 страницPid 14 MT23 160412Amol ChavanОценок пока нет
- Project Sanjay YadavДокумент51 страницаProject Sanjay YadavriyacomputerОценок пока нет
- Module 1 - AE4 - Review of Basic Mathematical Concepts (For Discussion)Документ36 страницModule 1 - AE4 - Review of Basic Mathematical Concepts (For Discussion)Kimberly Jean LautrizoОценок пока нет
- Aakash Zoology Study Package 3 SolutionsssssssДокумент104 страницыAakash Zoology Study Package 3 SolutionsssssssRishika PaulОценок пока нет
- Edc Contractors Basic Safety Training: "New Normal" EditionДокумент8 страницEdc Contractors Basic Safety Training: "New Normal" EditionCharles Rommel TadoОценок пока нет
- CO Q1 TLE EPAS 7 8 Module 4 Preparing Technical DrawingsДокумент47 страницCO Q1 TLE EPAS 7 8 Module 4 Preparing Technical DrawingsNicky John Doroca Dela MercedОценок пока нет
- Weekly Reminder August 18, 2014Документ4 страницыWeekly Reminder August 18, 2014PauldingProgressОценок пока нет
- Practice 4Документ11 страницPractice 4Justine Rs Dela TorreОценок пока нет
- Carbon Steel Fittings DimensionsДокумент3 страницыCarbon Steel Fittings DimensionsgiorselОценок пока нет
- PDF 1sz Fe Workshop Manual - CompressДокумент2 страницыPDF 1sz Fe Workshop Manual - CompressJose Luis Apaza Machaca75% (4)
- April262019 Airline Economic Analysis 2018-2019vfwebДокумент62 страницыApril262019 Airline Economic Analysis 2018-2019vfwebapi-548139140Оценок пока нет
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)От EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Рейтинг: 3 из 5 звезд3/5 (1)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionОт EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionРейтинг: 4 из 5 звезд4/5 (404)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsОт EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsОценок пока нет
- The Age of Magical Overthinking: Notes on Modern IrrationalityОт EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityРейтинг: 4 из 5 звезд4/5 (32)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisОт EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisРейтинг: 4.5 из 5 звезд4.5/5 (42)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDОт EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDРейтинг: 5 из 5 звезд5/5 (3)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeОт EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeРейтинг: 2 из 5 звезд2/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedОт EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedРейтинг: 4.5 из 5 звезд4.5/5 (82)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryОт EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryРейтинг: 4 из 5 звезд4/5 (46)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaОт EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsОт EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsРейтинг: 4 из 5 звезд4/5 (4)
- The Obesity Code: Unlocking the Secrets of Weight LossОт EverandThe Obesity Code: Unlocking the Secrets of Weight LossРейтинг: 4 из 5 звезд4/5 (6)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesОт EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesРейтинг: 4.5 из 5 звезд4.5/5 (1412)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsОт EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsРейтинг: 5 из 5 звезд5/5 (1)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.От EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Рейтинг: 4.5 из 5 звезд4.5/5 (110)
- Why We Die: The New Science of Aging and the Quest for ImmortalityОт EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityРейтинг: 4 из 5 звезд4/5 (5)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsОт EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsРейтинг: 4.5 из 5 звезд4.5/5 (170)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisОт EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisРейтинг: 5 из 5 звезд5/5 (8)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisОт EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisРейтинг: 3.5 из 5 звезд3.5/5 (2)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessОт EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessРейтинг: 4.5 из 5 звезд4.5/5 (328)
- Troubled: A Memoir of Foster Care, Family, and Social ClassОт EverandTroubled: A Memoir of Foster Care, Family, and Social ClassРейтинг: 4.5 из 5 звезд4.5/5 (27)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingОт EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingРейтинг: 4 из 5 звезд4/5 (1138)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeОт EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeРейтинг: 4.5 из 5 звезд4.5/5 (254)