Академический Документы
Профессиональный Документы
Культура Документы
Research Article: Long-Term Use of A Static Hand-Wrist Orthosis in Chronic Stroke Patients: A Pilot Study
Загружено:
RodrigoJeldres0 оценок0% нашли этот документ полезным (0 голосов)
13 просмотров5 страницLong-term use of a Static Hand-Wrist Orthosis in chronic stroke patients: a pilot Study. A number of stroke patients cannot tolerate a static orthosis over a long-term period because of discomfort. Without appropriate treatment opportunities, these patients will remain at risk of developing a clenched fst.
Исходное описание:
Оригинальное название
SRT2013-546093
Авторское право
© © All Rights Reserved
Доступные форматы
PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документLong-term use of a Static Hand-Wrist Orthosis in chronic stroke patients: a pilot Study. A number of stroke patients cannot tolerate a static orthosis over a long-term period because of discomfort. Without appropriate treatment opportunities, these patients will remain at risk of developing a clenched fst.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
13 просмотров5 страницResearch Article: Long-Term Use of A Static Hand-Wrist Orthosis in Chronic Stroke Patients: A Pilot Study
Загружено:
RodrigoJeldresLong-term use of a Static Hand-Wrist Orthosis in chronic stroke patients: a pilot Study. A number of stroke patients cannot tolerate a static orthosis over a long-term period because of discomfort. Without appropriate treatment opportunities, these patients will remain at risk of developing a clenched fst.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 5
Hindawi Publishing Corporation
Stroke Research and Treatment
Volume 2013, Article ID 546093, 5 pages
http://dx.doi.org/10.1155/2013/546093
Research Article
Long-Term Use of a Static Hand-Wrist Orthosis in
Chronic Stroke Patients: A Pilot Study
Aukje Andringa, Ingrid van de Port, and Jan-Willem Meijer
Revant Rehabilitation Centre Breda, Brabantlaan 1, 4817 JW Breda, Te Netherlands
Correspondence should be addressed to Aukje Andringa; a.andringa@revant.nl
Received 11 December 2012; Revised 31 January 2013; Accepted 31 January 2013
Academic Editor: Valery Feigin
Copyright 2013 Aukje Andringa et al. Tis is an open access article distributed under the Creative Commons Attribution License,
which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Background. Long-termsplinting, using static orthoses to prevent contractures, is widely accepted in stroke patients with paresis of
the upper limb. Anumber of stroke patients complain about increased pain and spasticity, which leads to the nonuse of the orthosis
and a risk of developing a clenched fst. Objectives. Evaluating long-termuse of static hand-wrist orthoses and experienced comfort
in chronic stroke patients. Methods. Eleven stroke patients who were advised to use a static orthosis for at least one year ago were
included. Semistructured telephone interviews were conducted to explore the long-term use and experienced comfort with the
orthosis. Data were analyzed using descriptive statistics. Results. Afer at least one year, seven patients still wore the orthosis for the
prescribed hours per day. Two patients were unable to wear the orthosis 8 hours per day, due to poor comfort. Two patients stopped
using the orthosis because of an increase in spasticity or pain. Conclusions. Tese pilot data suggest that a number of stroke patients
cannot tolerate a static orthosis over a long-termperiod because of discomfort. Without appropriate treatment opportunities, these
patients will remain at risk of developing a clenched fst and will experience problems with daily activities and hygiene maintenance.
1. Introduction
Of all stroke survivors, more than half experience impair-
ments of the upper limb in the chronic phase, including
loss of strength and dexterity, spasticity, muscle contracture,
pain, and edema [13]. Patients with a more severe paresis
have a higher risk of developing spasticity [4] and muscle
contractures of the wrist and fnger fexor muscles [5
7]. Without appropriate spasticity treatment or contracture
prevention, patients are at risk of developing a clenched fst,
a hand which is deformed into a fst by shortening of fexor
muscles of the fngers and sof tissue [8]. Te abnormal
position of the hemiplegic hand and wrist due to spasticity
and muscle contractures may interfere with daily activities
and hygiene maintenance, both negatively infuencing the
quality of life [911].
Diferent approaches are usedto inhibit spasticity, prevent
contractures, reduce pain and edema, or improve hygiene
maintenance of the hand in stroke patients with a nonfunc-
tional spastic upper limb. However, there is no consensus
about the most efective treatment [12]. A commonly used
and widely accepted intervention is prolonged splinting using
static orthoses [1217]. Two reviews on the efect of upper
limb splinting afer stroke have been published [18, 19]. Both
reviews showed no efect of static orthoses on upper limb
function, range of motion, and pain afer an intervention
period less than 13 weeks. However, conclusions should
be interpreted with caution because of the lack of high
quality randomised controlled trials. Tere is a considerable
heterogeneity of included study designs, clinical aims, and
orthosis wearing protocols, materials, and regimes. In addi-
tion, all published studies focused on the short-term efect
of splinting with splinting periods no longer than 13 weeks.
Despite controversies concerning splinting of the hemiplegic
upper limb, static orthoses continue to be advised in clinical
practice.
When used in clinical practice, a considerable amount of
stroke patients complain about increased pain and spasticity
since the use of the static orthosis [20, 21]. Due to discomfort,
the orthosis cannot be worn for the advised 8 hours per day
which leads to nonuse in chronic stroke patients and with
that increases the risk of developing clenched fsts with which
patients may experience problems with daily activities and
hygiene maintenance.
2 Stroke Research and Treatment
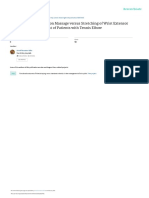
Figure 1: Example of a prefabricated static hand-wrist orthosis.
Given our experiences in clinical practice, the purpose
of this pilot study is to describe the long-term use of
static hand-wrist orthoses and the experienced comfort of
wearing the orthosis in chronic stroke patients in order
to acquire preliminary data to further study the treatment
of this specifc patient population. We hypothesize that, in
a number of the chronic stroke patients with upper limb
impairments, discomfortincreased pain, and spasticity
is the reason for not wearing a static hand-wrist orthosis
for the advised 8 hours per day. Te secondary aim is to
describe the self-reported complaints before and since the use
of the static orthosis to evaluate the efect of the use of the
orthosis in chronic stroke patients. Additionally, the use of
cointerventions for the impaired upper limb is investigated.
2. Methods
In this pilot study, semistructured interviews were used to
explore the long-term use (i.e., more than one year) of the
static orthosis in chronic stroke patients, and the experienced
comfort with the static orthosis in chronic stroke patients
(Figure 1). A selection of stroke patients, who received a
static orthosis from the Orthopaedic Centre OIM Brabant
Breda, Te Netherlands, was taken from the database. All
stroke patients who were advised to use a static orthosis
at least one year ago and were independently living in the
community were included. Patients were excluded when
correct contact details were missing or when patients died
in the study period. If patients were unable to communicate
by telephone, information was obtained from the primary
caregiver. Informed consent was obtained prior to each
interview.
Patients were asked about current use, comfort of the
orthosis, reasons for wearing the orthosis, self-reported
complaints in the hemiplegic upper limb, including spas-
ticity, hygiene maintenance, pain, and edema, and applied
cointerventions. Answers to all twelve questions were scored
categorically except the complaints scores. Complaints scores
were graded from0 (no complaints) to 10 (major complaints).
Te telephone interviews were carried out by a physical
therapist who was not directly involved in the patients
treatment.
Descriptive statistics were used to analyze the results
of the semistructured telephone interviews. Nonparametric
analyses were applied to evaluate self-reported efect of the
orthosis by comparing the data of complaints before and
since the use of the static orthosis using a Wilcoxons signed
rank test. Statistical analysis was performed using SPSS 18.0.
Statistical signifcance was set at the 5% level.
3. Results
3.1. Study Population. A total of 38 patients, diagnosed with
stroke, received a static hand-wrist orthosis at the Ortho-
paedic Centre OIMBrabant Breda, Te Netherlands, between
January 1, 2008 to October 1, 2009. Participants were ret-
rospectively recruited from the database at October 1, 2010.
Nineteen stroke patients matched our inclusion criteria and
were invited for the study. Eight patients could not be
interviewed, since three died between receiving the static
orthosis and data collection, and fve could not be reached by
telephone. Data of eleven patients (7 female, 4 male, median
age 54 years, range 2380 years) was collected. One interview
was conducted with a caregiver. All patients were in chronic
stage afer stroke (median 86 months poststroke, range 27
163 months) and were advised to use the static orthosis for at
least one year ago.
3.2. Long-Term Use of the Orthosis. As shown in Table 1, afer
at least one year from receiving the static orthosis, three
patients still wear the orthosis during night time, with difer-
ent experienced comfort. Four patients wore the orthosis for
at least 8 hours per day, all with good experienced comfort.
Two patients were unable to wear the orthosis prescribed 8
hours per day, due to poor comfort. Two patients stopped
using the orthosis, one because of anincrease of spasticity and
the other because of an increase in pain.
3.3. Self-Reported Complaints in the Hemiplegic Upper Limb.
Te main reasons reported for wearing the orthosis were
reducing spasticity (10/11), improving opening of the hand
(7/11), and improving hygiene maintenance of the hand (5/11)
(see Table 2). None of the patients wore the orthosis to reduce
edema. Te complaints score since the use of the orthosis
showed a decreasing trend; however diferences between
complaints in the hemiplegic upper limb before and since the
use of the orthosis were not signifcant ( < 0.05).
3.4. Cointerventions. Ten patients reported cointerventions
for their upper limb impairments of whom eight were
still using the static orthosis (Table 1). Six patients received
regular physical therapy sessions, six patients performeddaily
home exercises, and two patients used spasticity medication
(Botulinum toxin or Baclofen). Only one patient did not use
any other form of intervention for the impaired upper limb.
4. Discussion
In this pilot study, we investigated the long-term use of
a static hand-wrist orthosis in chronic stroke patients. Of
the 11 interviewed stroke patients, two stopped wearing the
orthosis because of discomfort and two could not endure
the orthosis for the prescribed wearing time of at least 8
Stroke Research and Treatment 3
Table 1: Orthosis wearing time, experienced comfort, and the reported cointerventions in addition to the use of the orthosis.
Patient Wearing time per 24 hours Day/night use Reported comfort Cointervention
1 46 hours Day Poor Handmaster
2 >8 hours Night Poor None
3 0 hours (nonuse) Very poor Medication, home exercises
4 >8 hours Night Poor Physical therapy
5 68 hours Day Very poor Physical therapy, home exercises
6 >8 hours Day Good Physical therapy, home exercises
7 >8 hours Day Good Home exercises
8 0 hours (nonuse) Poor Home exercises
9 >8 hours Day Good Physical therapy
10 >8 hours Day Good Medication, physical therapy, home exercises
11 >8 hours Night Good Physical therapy
Table 2: Self-reported complaints in the hemiplegic upper limb.
Reasons for wearing a static orthosis
Complaints before orthosis use Complaints since use orthosis
Median (range) (010) Median (range) (010)
Spasticity 10/11 8 (510) 7.5 (510)
Hygiene maintenance 5/11 7 (510) 6 (17)
Pain 3/11 8 (710) 7 (09)
Edema 0/11
Opening hand 7/11 8.5 (710) 7.5 (510)
hours per day. Tese fndings support our hypothesis that a
substantial number of patients who are at risk of developing
contractures in the upper limb, that is, four of the eleven,
are not able to endure a static orthosis for the prescribed 8
hours because of discomfort. Concluding that these chronic
stroke patients do not receive the appropriate intervention
to prevent contractures. Of the seven patients who used
the orthosis as prescribed, that is, at least 8 hours, two still
complained of discomfort. Without appropriate contracture
prevention, these patients will develop contractures in the
upper limb which can lead to problems during daily activities
and hygiene maintenance, both negatively infuencing the
quality of life.
Te experienced discomfort can be a result of the static
characteristics of the orthosis. Te position of the orthosis
sets the wrist in a fxed position. However, the level of spastic-
ity varies during daytime resulting indiferent positions of the
wrist. Witha higher level of spasticity of the muscles, the wrist
tends to fex. In contrast, a lower muscle tone can lead to less
fexion, or even extension, of the wrist. Te chosen position of
the static orthosis is seldomadequate to manage these varying
levels of spasticity and changing ranges of wrist mobility.
When spasticity increases, the hand and fngers will try to fex
in the rigid orthosis which causes pain and discomfort. For
stroke patients with varying levels of spasticity in the upper
limb, a static orthosis with a fxed position of the wrist can
lead to problems tolerating the orthosis.
Taking this into account, an orthosis for the prevention
of contractures in the spastic upper limb needs to allow
higher levels of spasticity and fexion of the wrist. A dynamic
orthosis using the low-load and prolonged stretch principle,
with a hinge which allows the wrist to fex during higher
levels of spasticity, might be more appropriate for these stroke
patients.
In our study, most patients use the orthosis because of
spasticity in the upper limb, to prevent contractures or to pre-
serve the ability to open the hand for hygiene maintenance.
Patients in our study did not report a signifcant diference
of the complaints concerning spasticity, contracture, or pain
before and since the use of the static orthosis, although the
complaints tended to decrease inthis small sample size group.
Previous studies on the short-termefect of the static orthosis
indicate that stretch does not have clinically important imme-
diate or short-term efect on joint mobility [22]. Tere is evi-
dence indicating that static orthoses show no efect on upper
limb function, range of motion at the wrist, fngers, or thumb,
nor pain [19, 23]. Despite the lack of studies of long-term
efect, physicians and patients still believe that splinting is an
appropriate intervention for contracture prevention. Because
contractures develop slowly, studies about the efect of splint-
ing need to focus on long-term use of at least six months. All
previous studies focused on an increased joint mobility of the
wrist as an efect of the static orthosis. In our opinion main-
taining the range of motion of the wrist is already a positive
efect of an intervention aiming to prevent contractures.
In conclusion, a static orthosis can be a useful prevention
of contractures for a selection of the stroke patients who
can tolerate this low-cost orthosis. However, there is a group
of chronic stroke patients which is not able to endure a
static orthosis and which needs another intervention for
4 Stroke Research and Treatment
the prevention of contractures in the upper limb. In this
group, stepped care can be used; when static orthoses are not
endured, another intervention has to be applied, for example,
dynamic orthosis.
4.1. Limitations of the Study. Although explorative, this study
ofers insight into the long-term use of a static orthosis in
chronic stroke patients and the patients experiences with it.
Despite the preliminary character of this study, the presented
data are the frst about long-term use of the static orthosis
and experienced comfort. Patients had to recall scores of
complaints before the use of the static orthosis which could
have been infuenced by recall bias. Taking this into account,
in combination with the small sample size, the results about
the self-reported complaints of static splinting should be
handled with care and should be confrmed in larger studies.
4.2. Further Research. Further studies are important to iden-
tify the stroke patients who are able to tolerate the static
orthosis and patients who will need other interventions to
prevent the development of contractures. For these specifc
stroke patients who are not able to tolerate the commonly
used static orthosis, it will be relevant to study the efect of
alternative interventions, for example, dynamic orthoses.
5. Conclusion
Tese pilot data showthat a number of chronic stroke patients
cannot tolerate a static orthosis for at least 8 hours per day
during a long-termperiod of at least one year. Without appro-
priate treatment opportunities, these patients will remain
at risk of developing a clenched fst and will experience
problems with daily activities and hygiene maintenance. It is,
therefore, worthwhile to fnd other interventions which can
be endured by these stroke patients.
Conflict of Interests
Te authors declare that they have no confict of interests.
Acknowledgments
Te authors ofer a special thanks to Daisy van Grinsven and
Ineke Koolhaas for their valuable participation in this study.
Te pilot study was fnancially supported by the Revant
Innovatiefonds.
References
[1] J. G. Broeks, G. J. Lankhorst, K. Rumping, and A. J. H. Prevo,
Te long-term outcome of arm function afer stroke: results of
a follow-up study, Disability and Rehabilitation, vol. 21, no. 8,
pp. 357364, 1999.
[2] H. Nakayama, H. S. Jorgensen, H. O. Raaschou, and T. S. Olsen,
Recovery of upper extremity function in stroke patients: the
Copenhagen Stroke Study, Archives of Physical Medicine and
Rehabilitation, vol. 75, no. 4, pp. 394398, 1994.
[3] H. Nakayama, H. S. Jorgensen, H. O. Raaschou, and T. S. Olsen,
Compensation in recovery of upper extremity function afer
stroke: the Copenhagen stroke study, Archives of Physical
Medicine and Rehabilitation, vol. 75, no. 8, pp. 852857, 1994.
[4] P. P. Urban, T. Wolf, M. Uebele et al., Occurence and clinical
predictors of spasticity afer ischemic stroke, Stroke, vol. 41, no.
9, pp. 20162020, 2010.
[5] K. H. Kong, K. S. G. Chua, and J. Lee, Symptomatic upper limb
spasticity in patients with chronic stroke attending a rehabilita-
tion clinic: frequency, clinical correlates and predictors, Journal
of Rehabilitation Medicine, vol. 42, no. 5, pp. 453457, 2010.
[6] S. Malhotra, A. D. Pandyan, S. Rosewilliam, C. Rofe, and H.
Hermens, Spasticity and contractures at the wrist afer stroke:
time course of development and their association with func-
tional recovery of the upper limb, Clinical Rehabilitation, vol.
25, no. 2, pp. 184191, 2011.
[7] A. D. Pandyan, M. Cameron, J. Powell, D. J. Stott, and M. H.
Granat, Contratures in the post-stroke wrist: a pilot study of
its time course of development and its association with upper
limb recovery, Clinical Rehabilitation, vol. 17, no. 1, pp. 8895,
2003.
[8] I. C. M. Heijnen, R. J. P. Franken, B. J. W. Bevaart, and J. W. G.
Meijer, Long-term outcome of superfcialis-to-profundus ten-
don transfer in patients with clenched fst due to spastic
hemiplegia, Disability and Rehabilitation, vol. 30, no. 9, pp.
675678, 2008.
[9] M. Franceschini, F. La Porta, M. Agosti, and M. Massucci, Is
health-related-quality of life of stroke patients infuenced by
neurological impairments at one year afer stroke? European
Journal of Physical and Rehabilitation Medicine, vol. 46, no. 3,
pp. 389399, 2010.
[10] D. S. Nichols-Larsen, P. C. Clark, A. Zeringue, A. Greenspan,
and S. Blanton, Factors infuencing stroke survivors quality of
life during subacute recovery, Stroke, vol. 36, no. 7, pp. 1480
1484, 2005.
[11] U. Sveen, E. Bautz-Holter, K. M. Sdring, T. B. Wyller, and K.
Laake, Association between impairments, self-care ability and
social activities 1 year afer stroke, Disability and Rehabilitation,
vol. 21, no. 8, pp. 372377, 1999.
[12] S. E. Farmer and M. James, Contractures in orthopaedic and
neurological conditions: a review of causes and treatment,
Disability and Rehabilitation, vol. 23, no. 13, pp. 549558, 2001.
[13] D. B. Cherry, Reviewof physical therapy alternatives for reduc-
ing muscle contracture, Physical Terapy, vol. 60, no. 7, pp. 877
881, 1980.
[14] P. W. Duncan, R. Zorowitz, B. Bates et al., Management of adult
stroke rehabilitation care: a clinical practice guideline, Stroke,
vol. 36, no. 9, pp. e100e143, 2005.
[15] E. L. Miller, L. Murray, L. Richards et al., Comprehensive over-
view of nursing and interdisciplinary rehabilitation care of the
stroke patient: a scientifc statement from the American heart
association, Stroke, vol. 41, no. 10, pp. 24022448, 2010.
[16] R. P. S. Van Peppen, H. J. M. Hendriks, N. L. U. Van Meeteren,
P. J. M. Helders, and G. Kwakkel, Te development of a clinical
practice stroke guideline for physiotherapist in Te Netherland:
a systematic review of available evidence, Disability and Reha-
bilitation, vol. 29, no. 10, pp. 767783, 2007.
[17] E. A. M. Franke, Ed., Commissie CVA-Revalidatie. Rehabilitation
afer a stroke, guidelines and recommendations for health care
professionals, Dutch Heart Foundation, Den Haag, Te Nether-
lands, 2001.
Stroke Research and Treatment 5
[18] N. A. Lannin and R. D. Herbert, Is hand splinting efective for
adults following stroke? A systematic review and methodolog-
ical critique of published research, Clinical Rehabilitation, vol.
17, no. 8, pp. 807816, 2003.
[19] S. F. Tyson and R. M. Kent, Te efect of upper limb orthotics
afer stroke: a systematic review, NeuroRehabilitation, vol. 28,
no. 1, pp. 2936, 2011.
[20] P. A. Feldman, Upper extremity casting and splinting, in Te
Practical Management of Spasticity in Children and Adults, M. B.
Glenn and J. Whyte, Eds., pp. 149166, Lea&Febiger, Philadel-
phia, Pa, USA, 1990.
[21] A. J. Turton and E. Britton, A pilot randomized controlled trial
of a daily muscle stretch regime to prevent contractures in the
arm afer stroke, Clinical Rehabilitation, vol. 19, no. 6, pp. 600
612, 2005.
[22] O. M. Katalinic, L. A. Harvey, R. D. Herbert, A. M. Moseley, N.
A. Lannin, and K. Schurr, Stretch for the treatment and preven-
tion of contractures, Cochrane Database of Systematic Reviews,
vol. 9, Article ID CD007455, 2010.
[23] S. F. Tyson and R. M. Kent, Orthotic devices afer stroke and
other non-progressive brain lesions, Cochrane Database of Sys-
tematic Reviews, no. 1, Article ID CD003694, 2009.
Вам также может понравиться
- The Vojta ConceptДокумент15 страницThe Vojta Conceptaziz012100% (1)
- Ot StrokeДокумент44 страницыOt StrokeDebora Astried F Sipayung100% (1)
- D2.2.-Management of Cerebral Palsy in Children: A Guide For Allied Health Professionals PDFДокумент148 страницD2.2.-Management of Cerebral Palsy in Children: A Guide For Allied Health Professionals PDFZvonkitza CertanecОценок пока нет
- Exercise Guidelines For Cerebral PalsyДокумент4 страницыExercise Guidelines For Cerebral PalsyMarikit20120% (1)
- Rehabilitation of Cerebral Palsy & Motor DelayДокумент49 страницRehabilitation of Cerebral Palsy & Motor DelayasloocltОценок пока нет
- Physical Therapy Clinical Management.9 PDFДокумент24 страницыPhysical Therapy Clinical Management.9 PDFClaudia MicuОценок пока нет
- A.tozeren - Human Body Dynamics - Classical Mechanics and Human MovementДокумент172 страницыA.tozeren - Human Body Dynamics - Classical Mechanics and Human MovementTudor BoarescuОценок пока нет
- Neonatal Neurology 4th Ed - G. Fenichel (Churchill Livingstone, 2007) WW PDFДокумент232 страницыNeonatal Neurology 4th Ed - G. Fenichel (Churchill Livingstone, 2007) WW PDFCampan AlinaОценок пока нет
- Principles and Practice of Emergency Neurology PDFДокумент456 страницPrinciples and Practice of Emergency Neurology PDFZygmunt BaumanОценок пока нет
- Effectiveness of Exercise and Cyriax Physiotherapy in Patients With Tennis Elbow (2012)Документ8 страницEffectiveness of Exercise and Cyriax Physiotherapy in Patients With Tennis Elbow (2012)Sufi Muzahid HussainОценок пока нет
- A Study To Assess The Effectiveness of Hot and Cold Application On Arthritic Pain and Mobility Status Among Clients With Osteoarthritis in Selected Hospitals at Kolar District.Документ31 страницаA Study To Assess The Effectiveness of Hot and Cold Application On Arthritic Pain and Mobility Status Among Clients With Osteoarthritis in Selected Hospitals at Kolar District.Lambert Winston67% (6)
- Evaluation of The Lateral Instability of The Ankle by Inversion Simulation Device and Assessment of The Rehabilitation ProgramДокумент13 страницEvaluation of The Lateral Instability of The Ankle by Inversion Simulation Device and Assessment of The Rehabilitation ProgramZzDel VerdeОценок пока нет
- 1471-2474-13-81 KonsulДокумент7 страниц1471-2474-13-81 KonsulGustan AriadiОценок пока нет
- Arthritis Care Research - 2016 - de Rooij - Efficacy of Tailored Exercise Therapy On Physical Functioning in PatientsДокумент10 страницArthritis Care Research - 2016 - de Rooij - Efficacy of Tailored Exercise Therapy On Physical Functioning in PatientsToli kkakrОценок пока нет
- THA Polyethylene SurvivalДокумент5 страницTHA Polyethylene SurvivalCleff FlowersОценок пока нет
- Clinical Study: Autologous Blood Injection and Wrist Immobilisation For Chronic Lateral EpicondylitisДокумент6 страницClinical Study: Autologous Blood Injection and Wrist Immobilisation For Chronic Lateral EpicondylitistriptykhannaОценок пока нет
- Outcomes of Micro FractureДокумент8 страницOutcomes of Micro FractureTiago SantosОценок пока нет
- Full TextДокумент7 страницFull TextJuan Pablo Casanova AnguloОценок пока нет
- International Journal of Health Sciences and ResearchДокумент8 страницInternational Journal of Health Sciences and Researchrizk86Оценок пока нет
- Clinical ResearcheffectsДокумент7 страницClinical ResearcheffectsJackielyn C. AportaderaОценок пока нет
- Knee Synovial Osteochorndromatosis: Case Report, Saudi ArabiaДокумент4 страницыKnee Synovial Osteochorndromatosis: Case Report, Saudi ArabiaIJAR JOURNALОценок пока нет
- The Journal of Arthroplasty: SciencedirectДокумент12 страницThe Journal of Arthroplasty: SciencedirectAlid AnwarОценок пока нет
- Bagus PDFДокумент4 страницыBagus PDFAditya KrisnaОценок пока нет
- Total Ankle Replacement Surgery (Arthroplasty)Документ12 страницTotal Ankle Replacement Surgery (Arthroplasty)ashut1Оценок пока нет
- Surgical Treatment of Chronic Elbow Dislocation Allowing For Early Range of Motion: Operative Technique and Clinical ResultsДокумент8 страницSurgical Treatment of Chronic Elbow Dislocation Allowing For Early Range of Motion: Operative Technique and Clinical ResultsLuis Carlos HernandezОценок пока нет
- Jurnal RomДокумент8 страницJurnal RomPutri WulandariОценок пока нет
- Tenotomia Percutanea Del BicepsДокумент10 страницTenotomia Percutanea Del BicepsOthoniel RamirezОценок пока нет
- 27 Sankarlingam EtalДокумент4 страницы27 Sankarlingam EtaleditorijmrhsОценок пока нет
- Two Years Outcome of Cemented Austin Moore HemiartДокумент7 страницTwo Years Outcome of Cemented Austin Moore HemiartIkram HussainОценок пока нет
- Comparacion Articulos de Tres Ejercicios para Manguito Rotador en InglesДокумент26 страницComparacion Articulos de Tres Ejercicios para Manguito Rotador en IngleskarolndОценок пока нет
- 129-Article Text-460-5-10-20200513Документ8 страниц129-Article Text-460-5-10-20200513Anushree DatarОценок пока нет
- Acute Hospital Admission For Stroke Is Characterised by InactivityДокумент43 страницыAcute Hospital Admission For Stroke Is Characterised by InactivityZhy CaluzaОценок пока нет
- International Journal of International Journal of International Journal ofДокумент7 страницInternational Journal of International Journal of International Journal ofRipka_uliОценок пока нет
- Effect of Kinesio Taping On Knee Symptoms in Patients With HemophiliaДокумент10 страницEffect of Kinesio Taping On Knee Symptoms in Patients With HemophiliaFrankChenОценок пока нет
- TheEffectofDeepFrictionMassageversus PDFДокумент8 страницTheEffectofDeepFrictionMassageversus PDFRiniaridhaОценок пока нет
- Acta Orthopaedica: Please Scroll Down For ArticleДокумент4 страницыActa Orthopaedica: Please Scroll Down For ArticleRicardo FerreiraОценок пока нет
- Post-Operative Clinical Outcomes in Patients With or Without The Use of Tourniquet in Total Knee Replacement SurgeryДокумент3 страницыPost-Operative Clinical Outcomes in Patients With or Without The Use of Tourniquet in Total Knee Replacement SurgerymunazilatulchasanahОценок пока нет
- Jurnal Sprain AnkleДокумент5 страницJurnal Sprain AnkleMZОценок пока нет
- Full TextДокумент9 страницFull TextdespОценок пока нет
- Approach Sports Health: A MultidisciplinaryДокумент8 страницApproach Sports Health: A MultidisciplinaryLorena WinklerОценок пока нет
- Injections For Chronic Plantas FasciitisДокумент4 страницыInjections For Chronic Plantas FasciitisRainer MujicaОценок пока нет
- Operative Treatment of Terrible Triad of TheДокумент8 страницOperative Treatment of Terrible Triad of TheAndrea OsborneОценок пока нет
- Use of A Static Progressive Stretch Orthosis To Treat Post-Traumatic Ankle StiffnessДокумент5 страницUse of A Static Progressive Stretch Orthosis To Treat Post-Traumatic Ankle StiffnessNararyo anantoОценок пока нет
- LskjjdshiubifsДокумент8 страницLskjjdshiubifsAchmad Luthfi TiflaniОценок пока нет
- Immediate Effects of Two Types of Braces On Pain and Grip Strength in People With Lateral Epicondylalgia: A Randomized Controlled TrialДокумент30 страницImmediate Effects of Two Types of Braces On Pain and Grip Strength in People With Lateral Epicondylalgia: A Randomized Controlled Trialapi-243703329Оценок пока нет
- Research Article: Correlation Between TMD and Cervical Spine Pain and Mobility: Is The Whole Body Balance TMJ Related?Документ8 страницResearch Article: Correlation Between TMD and Cervical Spine Pain and Mobility: Is The Whole Body Balance TMJ Related?gloriagaskОценок пока нет
- Open Patellar Tendon Debridement For Treatment of Recalcitrant Patellar Tendinopathy: Indications, Technique, and Clinical Outcomes After A 2-Year Minimum Follow-UpДокумент5 страницOpen Patellar Tendon Debridement For Treatment of Recalcitrant Patellar Tendinopathy: Indications, Technique, and Clinical Outcomes After A 2-Year Minimum Follow-Upbustyeva77Оценок пока нет
- Heel Pain Plantar Fascitis Hard Vs Sorft Orthotics and Heels PadДокумент11 страницHeel Pain Plantar Fascitis Hard Vs Sorft Orthotics and Heels PadDik 40Оценок пока нет
- Tascioglu Et Al 2010 Short Term Effectiveness of Ultrasound Therapy in Knee OsteoarthritisДокумент10 страницTascioglu Et Al 2010 Short Term Effectiveness of Ultrasound Therapy in Knee Osteoarthritiskrishnamunirajulu1028Оценок пока нет
- Use of Transcutaneous Electrical Nerve Stimulation Device in Early Osteoarthritis of The KneeДокумент7 страницUse of Transcutaneous Electrical Nerve Stimulation Device in Early Osteoarthritis of The KneeAlifah Nisrina Rihadatul AisyОценок пока нет
- Wheeler 2016Документ4 страницыWheeler 2016Alvaro Fabian Córdova WhiteleyОценок пока нет
- Bessire 2014Документ7 страницBessire 2014andrei3cucuОценок пока нет
- Semiconstrained Total Elbow Arthroplasty-1Документ6 страницSemiconstrained Total Elbow Arthroplasty-1Ευαγγελια ΚιμπαρηОценок пока нет
- Quality of Life in Patients Submitted To Arthroplasty Total Hip ResurfacingДокумент9 страницQuality of Life in Patients Submitted To Arthroplasty Total Hip ResurfacingInternational Medical PublisherОценок пока нет
- Prosser 2014Документ7 страницProsser 2014JaumeОценок пока нет
- Intertan Nail Vs PFN AДокумент7 страницIntertan Nail Vs PFN AzubayetarkoОценок пока нет
- Is Extracorporeal Shockwave Therapy Effective Even in The Treatment of Partial Rotator Cuff TearДокумент6 страницIs Extracorporeal Shockwave Therapy Effective Even in The Treatment of Partial Rotator Cuff TearmitchelОценок пока нет
- Nejmoa2108447 ProtocolДокумент41 страницаNejmoa2108447 ProtocolMarcelo Rodrigo TolabaОценок пока нет
- Fraturas Colunas e EAДокумент5 страницFraturas Colunas e EAJayce Layana CallouОценок пока нет
- Immediate and Long Term Outcomes Following Orthopedic Procedures in - 2019 - BLДокумент4 страницыImmediate and Long Term Outcomes Following Orthopedic Procedures in - 2019 - BLMichael John AguilarОценок пока нет
- Heavy-Load Eccentric Calf Muscle Training For The Treatment of Chronic Achilles TendinosisДокумент8 страницHeavy-Load Eccentric Calf Muscle Training For The Treatment of Chronic Achilles TendinosisburgoschileОценок пока нет
- Bed Angels On PainДокумент12 страницBed Angels On PainNiken AninditaОценок пока нет
- The Study To Assess The Effect of Prehabilitation On Postoperative Outcome of The Patients On Total Knee Arthroplasty at Selected HospitalДокумент4 страницыThe Study To Assess The Effect of Prehabilitation On Postoperative Outcome of The Patients On Total Knee Arthroplasty at Selected HospitalEditor IJTSRDОценок пока нет
- J Ppinen Et Al 2016 Musculoskeletal CareДокумент9 страницJ Ppinen Et Al 2016 Musculoskeletal CareMade Fitri DamayantiОценок пока нет
- Compression Stockings Versus Neuromuscular Electrical StimulationДокумент6 страницCompression Stockings Versus Neuromuscular Electrical StimulationrachiddellarОценок пока нет
- Itp Periop1Документ4 страницыItp Periop1Irfan MohammadОценок пока нет
- Sirajrej Leg LockДокумент8 страницSirajrej Leg LockUsman ohorellaОценок пока нет
- A Treatment Schedule of Conventional Physical Therapy Provided To Enhance Upper Limb Sensorimotor Recovery After Stroke Expert Criterion Validity and Intra-Rater ReliabilityДокумент10 страницA Treatment Schedule of Conventional Physical Therapy Provided To Enhance Upper Limb Sensorimotor Recovery After Stroke Expert Criterion Validity and Intra-Rater ReliabilityGeraldo MoraesОценок пока нет
- Tone AbnormalitiesДокумент32 страницыTone AbnormalitiespuchioОценок пока нет
- 24 Hour Positioning Practice GuideДокумент111 страниц24 Hour Positioning Practice GuideIqra AsifОценок пока нет
- Motor Neuron Disease: Amyotrophic Lateral Sclerosis (ALS)Документ2 страницыMotor Neuron Disease: Amyotrophic Lateral Sclerosis (ALS)james cordenОценок пока нет
- Cerebral PalsyДокумент27 страницCerebral PalsyJohn Paul Parungao CrisostomoОценок пока нет
- Tardieu ScaleДокумент1 страницаTardieu ScaleAbhi RokayaОценок пока нет
- 320 PDFДокумент4 страницы320 PDFilona ilincaОценок пока нет
- How Do We Walk?: Sujay Galen PT PHD FheaДокумент52 страницыHow Do We Walk?: Sujay Galen PT PHD FheaColleen JohnsonОценок пока нет
- Pressure SoresДокумент43 страницыPressure SoresArpanpatelОценок пока нет
- Cerebral PalsyДокумент27 страницCerebral PalsyTudor Doncea100% (1)
- Form 115B Student Tandem Medical Advice Form 2016Документ4 страницыForm 115B Student Tandem Medical Advice Form 2016rubana555Оценок пока нет
- Cerebral PalsyДокумент12 страницCerebral PalsyEunice Lan ArdienteОценок пока нет
- Pediatric Endurance and Limb Strengthening For Children With Cerebral PalsyДокумент10 страницPediatric Endurance and Limb Strengthening For Children With Cerebral PalsysudersonОценок пока нет
- Final Expert ReportДокумент29 страницFinal Expert ReportDENNIS N. MUÑOZОценок пока нет
- Butler Darrah 2001Документ13 страницButler Darrah 2001Adnan Faris NaufalОценок пока нет
- Case Report: Stiff Person Syndrome (SPS)Документ2 страницыCase Report: Stiff Person Syndrome (SPS)International Journal of Innovative Science and Research TechnologyОценок пока нет
- The Changing Face of Neurological RehabilitationДокумент10 страницThe Changing Face of Neurological RehabilitationMaria Sri PangestutiОценок пока нет
- Pilot Study of Delayed Versus Immediate Serial Casting After Botulinum Toxin Injection For Partially Reducible Spastic EquinusДокумент4 страницыPilot Study of Delayed Versus Immediate Serial Casting After Botulinum Toxin Injection For Partially Reducible Spastic Equinusyarimar hoyosОценок пока нет
- Filomeno Urbano, Petitioner, vs. Hon. Intermediate Appellate Court and People of The Philippines, RespondentsДокумент7 страницFilomeno Urbano, Petitioner, vs. Hon. Intermediate Appellate Court and People of The Philippines, RespondentsDane DagatanОценок пока нет
- 2012 VCU Engineering Senior Design ProjectsДокумент100 страниц2012 VCU Engineering Senior Design Projects1726giangОценок пока нет
- Motor SysДокумент72 страницыMotor SysLeoОценок пока нет
- 02 Padure, L. Spastic Hip in Cerebral PalsyДокумент4 страницы02 Padure, L. Spastic Hip in Cerebral PalsyminichoixОценок пока нет