Академический Документы
Профессиональный Документы
Культура Документы
The NATURE and IMPLICATIONS of Support in Graduate Nurse TRansition Programs - An Australian Study
Загружено:
kitsil0 оценок0% нашли этот документ полезным (0 голосов)
67 просмотров8 страницStudy: support is critical to graduate nurse transition from novice to advanced beginner-level practitioner. "Informal teachers" and the graduate nurses themselves are often the best sources of support. A new operational definition of support is proposed and recommendations are made.
Исходное описание:
Авторское право
© © All Rights Reserved
Доступные форматы
PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документStudy: support is critical to graduate nurse transition from novice to advanced beginner-level practitioner. "Informal teachers" and the graduate nurses themselves are often the best sources of support. A new operational definition of support is proposed and recommendations are made.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
67 просмотров8 страницThe NATURE and IMPLICATIONS of Support in Graduate Nurse TRansition Programs - An Australian Study
Загружено:
kitsilStudy: support is critical to graduate nurse transition from novice to advanced beginner-level practitioner. "Informal teachers" and the graduate nurses themselves are often the best sources of support. A new operational definition of support is proposed and recommendations are made.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 8
THE NATURE AND IMPLICATIONS OF
SUPPORT IN GRADUATE NURSE
TRANSITION PROGRAMS: AN
AUSTRALIAN STUDY
MEGAN-JANE JOHNSTONE, PHD, BA, RN, FRCNA,
OLGA KANITSAKI, PHD, MEDSTUD, BAPPSC (ADVNSG), RN, FRCNA, AND
TRACEY CURRIE, MED, GRADCERTHEALTHLAW, BN, RN
It is widely recognized that support is critical to graduate nurse transition from novice to
advanced beginner-level practitioner and to the integration of neophyte practitioners into safe
and effective organizational processes. Just what constitutes support, however, and why (if at all)
support is important, when, ideally, support should be given, by whom, how, and for how long,
have not been systematically investigated. Building on the findings (previously reported) of a
yearlong study that had, as its focus, an exploration and description of processes influencing the
successful integration of new graduate nurses into safe and effective organizational processes and
systems, the findings presented in this article strongly suggest that support is critical to the
process of graduate nurse transition, and that integration into the system is best provided
during the first 4 weeks of a graduate nurse transition program and thereafter at the beginning of
each ward rotation; that informal teachers and the graduate nurses themselves are often the
best sources of support; and that the most potent barriers to support being provided are the
untoward attitudes of staff toward new graduates. Drawing on the overall findings of the study, a
new operational definition of support is proposed and recommendations are made for future
comparative research on the issue. (Index words: Support; Graduate nurse; Transition; Patient
safety and quality care; Nursing management) J Prof Nurs 24:4653, 2008. A 2008 Elsevier Inc.
All rights reserved.
T
HE SUCCESSFUL INTEGRATION of neophyte
graduate nurses into safe and effective organiza-
tional systems and processes is of considerable impor-
tance to the provision and management of safe health
care services. How best to facilitate and achieve this
integration, however, remains the subject of ongoing
debate and inquiry.
There is general agreement in the graduate nurse
transition literature that if theoretical knowledge is to be
transferred successfully into practice, the transfer of
knowledge must take place in a supportive and
nonthreatening environment that well integrates the
neophyte practitioners of nursing into the organization's
systems and processes. In keeping with this view, it is
further held that graduate nurse transition programs
must be framed in such a way that they provide graduate
nurses with the kinds and level of support that is
conducive to the development of their confidence and
competence as neophyte practitioners and, accordingly, a
supportive clinical transition that has, as its focus,
positive patient outcomes and clinical excellence.
While advocating that support should be provided, the
literature stops short of providing an operational defini-
tion of what constitutes support (as would be useful for
the purposes both of comparative research and bench-
marking practice and policy initiatives) or of providing
Professor of Nursing/Director of Research, Division of Nursing and
Midwifery, School of Health Sciences, RMIT University, Melbourne VIC
3083, Australia.
Adjunct Professor, Division of Nursing and Midwifery, RMIT
University, Melbourne VIC 3083, Australia.
Lecturer, Division of Nursing and Midwifery, RMIT University,
Melbourne VIC 3083, Australia.
Address correspondence to Dr. Johnstone: Professor of Nursing/
Director of Research, Division of Nursing and Midwifery, School of
Health Sciences, RMIT UniversityBundoora West Campus, PO Box
71, Melbourne VIC 3083, Australia.
E-mail: megan.johnstone@rmit.edu.au
8755-7223/$ - see front matter
Journal of Professional Nursing, Vol 24, No 1 (JanuaryFebruary), 2008: pp 4653 46
doi:10.1016/j.profnurs.2007.06.003 A 2008 Elsevier Inc. All rights reserved.
research-based accounts of the importance of support to
neophyte graduate nurses, when, ideally, support should
be given (and for how long); who is best situated to
providing support; how support should be given; or the
kinds of barriers that exist to support being given in a
timely and appropriate manner. A key aim of this article is
to redress this oversight.
Literature Review
The term support (from Old French supporter and Latin
supportre, meaning to bring, to carry) is defined in
various English dictionaries as to give aid or courage
and to give strength to. Its pertinence to graduate nurse
transition is discussed below.
It is widely recognized that the process of transition
from student to practitioner, and fromnovice to advanced
beginner-level practitioner, is a difficult and stress-
ful experience for newly qualified nurses (Brown &
Edelmann, 2000; Chang & Daly, 2001a, 2001b;
Chang et al., 2006; Clare, White, Edwards, & van
Loon, 2002a; Duncan, 1997; Gerrish, 2000; Goh &
Watt, 2003; Greenwood, 2000; Levett-Jones & Fitzgerald,
2005; Maben & Mcleod Clark, 1998; Mackin, Macera, &
Jennings, 2006; Piggott, 2001; Roberts & Farrell, 2003;
Stanley, 2003; Theobald & Mitchell, 2002; Thomka,
2001). Reasons for this are many and complex and in-
clude the following:
the often untenable professionalbureaucratic
conflict arising from the differences in the culture
between the school of nursing and the hospital
setting (Gerrish, 2000, p. 474);
lack of appropriate individual support and a
supportive clinical learning environment during
the initial postqualification period (De Bellis,
Longson, Glover, & Hutton 2001; Dearmun,
2000; Hart & Rotem, 1995; Levett-Jones &
Fitzgerald, 2005; Maben & Mcleod Clark, 1998;
Parker, Plank, & Hegney, 2003; Thomka, 2001);
poor working conditions, characterized by such
things as heavy workloads, staffing shortages,
inappropriate skill mix, and high acuity of
patients (De Bellis et al., 2001; Johnstone, 2002);
sudden increases in levels of responsibility and
accountability that come with being a registered
nurse (Chang & Daly, 2001a, 2001b; Clare et al.,
2002a; Gerrish, 2000; Maben & Mcleod Clark,
1998); and
less than helpful attitudes of veteran nurses,
including the following: hostility and stigmatizing
behavior against university-educated graduates,
having a sink or swim mentality toward new
graduates, the marginalization of new graduates,
and a stubborn resistance to change underscored
by a continual longing for a return to the good old
days (De Bellis et al., 2001; Boychuk Duchscher
& Cowin, 2004; Duncan, 1997; Johnstone &
Kanitsaki, 2006a; Johnstone & Kanitsaki, in press;
Maben & Mcleod Clark, 1998; Piggott, 2001).
To address the difficulties and stresses that new
graduates are known to experience upon commencing
their practice as registered nurses, many in the field have
steadfastly argued that new graduates must have both
individual support and a supportive workplace environ-
ment. They go on to contend that unless such support is
provided, it will be extremely difficult for new graduates
to make the transition successfully from novice to
advanced beginner-level practitioner and become inte-
grated into the system as effective members of the team.
Researchers argue that support is crucial to graduate
nurse transition because it helps to decrease job stress;
improve job satisfaction, motivation, and commitment;
and, importantly, develop confidence and competency in
the new graduate nurse (Crooks et al., 2005; Dearmun,
2000; Duncan, 1997; Maben & Mcleod Clark, 1998;
McCloskey, 1990). These outcomes, they suggest, help
improve staff recruitment and retention rates and, ipso
facto, patient safety and quality care (Kurtzman & Kizer,
2005; Needleman, Buerhaus, Mattke, Stewart, & Zele-
vinsky, 2002; Page, 2004).
The failure to provide support during the graduate
nurse transition phase, in contrast, has been implicated in
high levels of stress and poor coping, poor job satisfac-
tion, and burnout among neophyte graduate nurses and,
in some instances, to their marginalization in practice
contexts (Boychuk Duchscher & Cowin, 2004; Brown &
Edelmann, 2000; Chang et al., 2006; De Bellis et al.,
2001). Worryingly, these outcomes have been linked not
only to poor recruitment and retention of graduate nurses
in specific organizations but also to the loss of the new
graduates from the profession altogether. As Parker et al.
(2003) explain:
Lack of professional and collegial support during
this transition phase can seriously affect both short
and long-term performance and, therefore deter-
mine whether or not the new graduate remains in
the workforce (p. 301).
Despite the recognized importance of support to the
successful transition of graduate nurses and their
successful integration into an organization's safe and
effective systems and processes, there has been cur-
iously little research on support per se. A search of
multiple electronic databases (for all years) using the
key words graduate nurse, neophyte nurse, and
support has revealed numerous articles and research
reports (such as those already cited in this article)
underscoring the importance of support to graduate
nurse transition and that new graduates often do not get
the support they need. A limited number of articles also
reported various behaviors that new graduates have
found to be supportive, such as nursing staff being
helpful, being patient, giving praise about care plans,
enabling autonomous neophyte practice, being available
to give assistance, encouraging and answering ques-
tions, providing nonjudgmental guidance, acknowled-
ging how stressful a situation can be, making the new
graduates feel valued, and pairing new graduates with
47 THE NATURE AND IMPLICATIONS OF SUPPORT IN GRADUATE NURSE TRANSITION PROGRAMS
mentors or preceptors to help them become integrated
into unfamiliar workplace environments (Brown &
Edelmann, 2000; De Bellis et al., 2001; Duncan, 1997;
Mackin et al., 2006; Roberts & Farrell, 2003; Smith,
1997; Thomka, 2001).
Various behaviors that new graduates have found to be
unsupportive have also been reported, such as nursing staff
treating them in a rude, resentful, hostile or dismissive
manner; being disrespectful; going behind their backs to
the managers; being overly critical of their work and
telling new graduates you should know more; being
critical of new graduates in front of patients or other staff;
treating the new graduates like a kid; and expecting
new graduates to function in roles above their level of
education and experiencefor example, being put in
charge (De Bellis et al., 2001; Thomka, 2001). None of the
articles located, however, provided a systematic examina-
tion of the nature and implications of support in itself
including when, where, for howlong, and by whomneeded
support should be provided to newgraduate nurses during
their first year of practice. If policy and practice develop-
ments are to be progressed in this area, it is evident that
further support research is required.
Methodology
This project was undertaken using an exploratory
descriptive case study approach, incorporating both
qualitative and quantitative data collection and analysis
strategies (Hamel, 1993; Stake, 1995; Yin, 2003). This
approach was chosen because it is eminently suitable to
advancing an empirical study that seeks to explore and
describe a unique casein this instance, of a graduate
nurse transition program in its real-life context and the
unique experiences of the group of graduate nurses
enrolled in this program during their first year of practice.
The case study approach is also eminently suitable to
answering what and how type of questions such as
those that this study sought to answer (Yin, 2003). Other
components of this study (reported elsewheresee
Johnstone & Kanitsaki, 2006a; Johnstone & Kanitsaki, in
press; Johnstone et al., 2007) had, as their focus, the timely
provision of pertinent information on clinical risk manage-
ment to new graduates and the translation of that
information into practice. This article (which builds on
the previous articles) reports the findings of the study that
relate specifically to the role of support in assisting
neophyte graduate nurses to (a) integrate into safe and
effective organizational systems and processes, (b) develop
their capacity to function effectively as advanced beginner-
level practitioners, and (c) contribute to the organization's
broader patient safety and quality care processes.
Research Purpose and Aims
The key purpose and aims of the component of the
project being reported here were to explore and describe
the following:
nature and implication of support being
provided and/or not being provided to neophyte
graduate nurses during their first year of practice,
development of a supportive environment that
encourages and facilitates a safe environment and
safe practice among neophyte graduate nurses, and
safe transition of the graduate nurse from novice
to advanced beginner-level practitioner.
Design
The project was designed to be conducted over a
12-month period and consisted of five phases: problem
definition, design, data collection, data analysis, and
composing and disseminating the final report (Yin, 2003).
During the course of the project, a total of six survey
questionnaires were distributed to and completed by two
cohorts of neophyte graduate nurses who commenced
their programs 6 weeks apart. The questionnaires sought
descriptive data on the graduate nurses' feelings, attitudes,
and beliefs concerning their general levels of confidence
and competence, particularly in regard to their capacity to
practice safely, practice evidence-based nursing care,
assess and manage for risk in patients, assess and manage
for risk in their own practice, seek advice on patient care
matters, recognize their own limitations as a newgraduate
and seek assistance when necessary, make independent
clinical decisions about nursing care, report an incident,
and understand and practice the principles and practice of
clinical risk management in nursing and health care
contexts. In addition, a total of 35 individual and focus
group interviews were conducted at regular intervals over
the 12-month period.
Research Problem
The successful integration of neophyte graduate nurses
into safe and effective organizational systems and
processes is of considerable importance in the provision
and management of safe health care services. The notion
and operationalization of support as a process critical to
facilitating graduate nurse transition and integration into
a hospital's local systems and processes have not been
fully investigated, however.
Research Questions
The research questions informing this component of the
study were the following:
What constitutes support?
How important is support to improving con-
fidence and competence in new graduates and to
their achieving integration into safe and effective
organizational systems and processes?
Whenshouldsupport be given(andfor howlong)?
How should support be given?
Who is best situated to providing support?
What barriers are there to appropriate support
being provided to new graduates?
Sample
The following three purposeful sample units of analysis
were selected for this study:
1. Neophyte graduated nurses. Two cohorts of
newly graduated nurses (n = 11) undertaking
48 JOHNSTONE ET AL
a 12-month graduate nurse transition program
at a regional health service in the Australian
State of Victoria.
2. Key stakeholders. Thirty-four key stakeholders,
that is, nurse unit managers, clinical teachers,
preceptors, the quality manager, librarian, and
senior nurse administrators employed by the
health service and directly involved with
graduate nurses undertaking the Graduate
Nurse Program during the period under study.
3. Literature. Published studies and discussion
papers addressing key graduate nurse transition
issues, cultural and organizational frameworks
and approaches to patient safety and quality
care, and employee integration into effective
and safe organizational processes and systems.
Data Collection
Data were collected from multiple sources via survey
questionnaires, individual and focus group interviews,
participant observation, field notes, minutes of research
teammeetings, aggregate patient data collected for quality
assurance purposes, and other documents. During the
course of the project, a total of 63 questionnaires were
completed and returned for analysis. As well, a total of 35
focus group and individual interviews were conducted. Of
these, 14 (5 focus group and 9 individual) interviews were
conducted with graduate nurse (GN) participants, and 21
(9 focus group and 12 individual) interviews were
conducted with key stakeholders (KSH).
Ethical Considerations
Approval was obtained from the Human Research
Ethics Committee at RMIT University prior to the
commencement of the study. Approval was also
obtained from the participating health service. Each
participant was given a plain language letter explain-
ing the nature and purpose of the study. They were then
invited to provide written consent to participate. None
refused to participate and none dropped out of the
study. Confidentiality and the anonymity of participants
were maintained by the use of codes on all ques-
tionnaires and transcripts of interviews. The anonymity
of participants was further assured via the aggregate
presentation of the data, from which any identifying
information was removed.
Data Analysis
Quantitative data obtained from the questionnaires were
analyzed using the SPSS cross-tabulation statistical
procedure and organized under the following four
broad themes:
Support of graduate nurses,
Confidence of graduate nurses,
Helpfulness of graduate nurse program, and
Learning needs of the graduate nurses.
Qualitative data, in turn, were analyzed using the
content and thematic analysis strategies commonly used
in naturalistic inquiries (Lincoln & Guba, 1985; Patton,
2002). Initial depictions of the data analyzed were
organized around the research questions and the
categories of participants interviewed. To ensure the
rigor of the research, data were constantly scrutinized
and compared for rival interpretations and depictions.
Where appropriate, quantitative data were used to
triangulate qualitative data and vice versa.
Findings
The Notion of Support
Support was identified by both graduate nurse and key
stakeholder participants as including
availability of clinical teaching staff (always
being there, making time),
approachability of clinical teaching staff (having
the right attitude, friendly faces, right
chemistry),
being enabled to ask questions (not made to feel
a git or an idiot, not being put down),
being prompted to engage in best practice,
benevolent surveillance (being allocated to a part
of the ward that was readily visible so that
experienced staff could keep an eye on them
and ensure that they did not drift to another part
of the ward and get lost),
getting feedback in a timely and constructive man-
ner (not having to wait around for an answer),
being given reassurance (being told you are
doing good),
having backup (even when not encountering
any problems), and
being debriefed (after dealing with a difficult
situation).
Several graduates commented that, upon the com-
mencement of their graduate nurse program and when
first commencing their work on the wards, their confi-
dence was very low. They went on to reveal that what
they most needed at this time was positive feedback:
I would say that what would help would be being
complimented more. All I seem to be getting fed
back is all the things I'm doing wrong, instead of
what things I'm doing good (GN-FG:26:03, p. 7).
Key stakeholder participants agreed, adding that, in
their experience, what the new graduates also needed
when first starting out in their clinical practice was
reassurancenotably, that they were on the right track,
and that it was acceptable to ask questions, to seek advice,
and to seek assistance if and when they were unsure.
Commensurate with the need for reassurance was the
concomitant need to have backup. Having backup, in
this instance, was defined by key stakeholder participants
as having someone to bounce ideas off (e.g., how to
prioritize their tasks and manage their time) and to
know that the backup is there when the proverbial does
actually hit the fan, which it can do quite regularly
(KSH-FG:21:02. p. 7).
49 THE NATURE AND IMPLICATIONS OF SUPPORT IN GRADUATE NURSE TRANSITION PROGRAMS
Importance of Support
Providing support to the graduate nurses in an appro-
priate and timely manner had a direct and positive impact
on their sense of confidence and competence as
beginning practitioners. Being given support was also
perceived as being critical to helping the new graduates to
avoid making mistakes. As one graduate responded:
If you try and do it yourself, you think, well, Is this
how you do it, or is it not? Am I doing it right? You
don't really know if you're doing it correctly and
you don't want to continue doing it if you don't
know whether you're doing it correctly or not. You
don't want to do the wrong thing (GN-FG:12:03,
p. 14).
It was evident from the data that, on account of being
provided appropriate (tailored) support, the graduates
achieved transition from novice to advanced beginner-
level practitioner relatively quickly, with most achieving
that transition within 34 months of commencing their
graduate nurse program. It was further evident that being
supported enabled the new graduates to also quickly
become functional members of the team. As one graduate
reflected with reference to her first ward rotation and the
support she had received from the day she started:
I can't believe we've been here for three weeks. It
feels like I've been here forever. I feel like I'm
actually part of the team (GN-FG:12:03, p. 10).
When, How Much, and For How Long Support
Should Be Given
Analysis of both the graduate nurse and key stakeholder
data revealed that the issue of when support should be
provided and for how long was very much an individual
matter and something that had to be determined on a
case-by-case basis. How much support new graduates
needed, in turn, largely depended on the kind and
number of ward rotations they had. (Most believed that
rotations of between 3 and 4 months' duration were ideal
because these gave the new graduates time to find their
way around, develop their routine, and consolidate their
skills before moving on to the next rotation.) None-
theless, overall, it was evident that support needed to be
given during the early transition and integration phase of
the graduate nurse year (i.e., during the first 4 weeks of
the graduate nurse year) because this was the time that
the graduates most felt the loss of what they described as
the safety net they felt they had as students:
It's really been a big jump when you come from the
safety net of being a student to work (GN-FG:02:03,
p. 19).
After this initial period, support then needed to be
given at the beginning of each new rotation as scheduled
for the remainder of the program.
One unexpected finding under this category was that
the period for which a new graduate needed support was
not necessarily commensurate with the time it took to
achieve transition from novice to experienced practi-
tioner or integration into the hospital's organizational
processes and systems. Most of the graduates felt
confident at the end of a ward rotation and as their
experience increased, although this changed when their
rotation was changed and they had to start again (GN-
FG:26:03, p. 24). Significantly, as their experience
increased, the graduates' need of support became more
a matter of knowing that they had backup (if and
when it was needed it), rather than having someone
always there.
How Support Should Be Given
Both the nurse graduate and key stakeholder participants
strongly believed that one of the most substantive means
of providing support was by providing and sustaining
opportunities to new graduates to gain experience (i.e.,
as opposed to being taught). As one Nurse Unit
Manager explained:
I am trying to give them experience. I'm not really
trying to naturally teach them We try to expose
them to as much experience as possible (KSH-
FG:21:02, pp. 2021).
Prompting best practice (via preceptor-guided prac-
tice, utilizing key cards, or meeting regularly through a
shift to, for instance, identify what needs to be attained
and how to go about attaining it) was also regarded as an
important support mechanism.
Staff Best Suited to Providing Support
There was a strong view among the graduates that:
Who you work with, or who you are preceptored
with, makes all the difference to how confident you
feel (GN-FG:12:3, p. 14).
Graduates emphasized that it was important to
ensure that they and their designated preceptors were
matched appropriately and got along so that they
could have the freedom they needed to develop and
improve their confidence and competence as registered
nurses (GN-FG:26:03, p. 9). They indicated that having
the freedom to ask for help and knowing that help was
there for the asking, getting one's own patients, and
doing one's own thing enabled them to feel like a
nurse and not feel like a student anymore (GN-
FG:12:03, p. 9). It was revealed, however, that,
sometimes, new graduates had been assigned preceptors
who were inexperienced and unqualified for and/or
disinterested in the role, which had a devastating
impact on their confidence and perceived competence
as beginning practitioners.
It was evident from the data that designated
preceptors and clinical teachers were not necessarily
the only ones providing appropriate support to new
graduates or, indeed, the ones best suited to do so.
Often, it was other helpful nurses who functioned as
informal clinical teachers who provided most support
to the new graduates. An example of the kind of
50 JOHNSTONE ET AL
support provided by an informal clinical teacher is
given below:
I had three patients on IV antibiotics all night and
by the end of the night I felt a lot better about it
because sheone of those helpful nursesex-
plained everything about it to me. She could see
that I wasn't really confident with looking after a
patient with it [IV antibiotics] on my own, so she
went through it all with me and helped me with it
and by the end of the night I was doing it
[administering the IV antibiotics] on my own all
the time (GN-FG:12:03, p. 14).
One interesting finding under this category was that
one of the greatest sources of support for a new graduate
was self-support. As one key stakeholder observed:
By and large the new graduates direct their own
graduate experience and their own inquiring minds.
It doesn't matter who is on the shiftthey'll be
asking questions and just making sure they're going
in the right direction (KSH-FG:21:02, p. 8).
Data further revealed that a key way in which new
graduates supported themselves was by actively seeking
out staff whom they thought would most support them.
Supportive staff in this instance tended to be identified
by their manner and whether they made the new
graduate feel comfortable. Ironically, whether new
graduates actually got the support from staff they were
seeking, and how much, often depended on the
graduates' confidence levels and own support-seeking
behaviors. Paradoxically, those who exhibited most
confidence tended to attract more support from staff
than did those who lacked confidence:
Some of it comes down to actual confidence of the
individual. If they are a confident person, they are
willing to take on new cases and assist. The others
who aren't so confident will be hesitant and
therefore will perhaps not be taken on board quite
so much by staff. So they perhaps lose out a little
bit, because the confident one, you take under
your wing and push them a little bit further (KSH-
FG:10:02, p. 2).
Barriers to Appropriate Support Being Given
All participants acknowledged that there were significant
problems associated with and barriers to being able to
provide adequate support to new graduates. Notable
among the problems identified were the following:
a lack of staff,
a lack of consistency in preceptors,
the general realities of the ward, and
inappropriate attitudes or behavior of staff.
Data revealed that due to the large number of part-time
staff employed at the hospital, poor skill mix, and
workload issues, it was sometimes impossible for the new
graduates to receive the level of support they needed as
beginning practitioners. In one case, a new graduate had
12 different preceptors during one 2-month ward
rotation (GN-FG:12:03, p. 7). In another case, the
new graduate reported: I haven't had the same person
two days running (GN-FG:12:03, p. 7). Key stake-
holders identified the realities of the ward as also
posing barriers: Once you are on the wards, the phones
are ringing, bells are ringing, there are people every-
where, doctors doing roundsthe reality of what's
happening on the ward on a day-to-day basis (KSH-
FG:10:02, p. 8).
Arguably, the most potent barrier to graduate nurse
support was staff attitudes that included treating the
graduates in a rude and dismissive manner and as being
naturally incompetent and inferior to others. A
poignant example of this can be found in the way in
which some staff persisted in perceiving and treating the
new graduates as perpetual students. During the focus
group interviews and other meetings with key stake-
holders, for instance, graduates were often referred to
inadvertently as students. In one instance, when
challenged by the researchers that the graduates were,
in fact, fully qualified registered nurses, not students, a
key stakeholder remained adamant, stating, No. I'm
sorry. They are not registered nurses. They are still
students (RMAC-11:04).
Another example of poor staff attitude concerns the
indiscrete manner in which some clinical teachers
approached the new graduates, making it difficult for
the graduates to ask for support if it was needed. An
example is as follows:
What I found was when the clinical teachers came
to see me, not that I had any problems, but if I did
have problems, they actually spoke to me in front of
the staff. So if I had a problem with a staff member
or something, I couldn't tell them. But if I did have a
problem I'd still have to ask the clinical teacher to
go into another room and the staff would probably
think that I'd had something to say about them
(GN-FG:26:03, p. 2).
Not all were hostile to or indiscrete in their dealing
with new graduates, however. Many key stakeholder
participants were acutely aware of the problem of poor
staff attitudes toward the graduates and how damaging
this could beboth to the graduates themselves and to
the organization, especially in terms of staff recruitment
and retention. For them, the solution was simple: Staff
needed to change their attitude and simply be more
friendly toward the new graduates:
We try to be a good friend to the graduates without
smothering them. I think that we're all very patient
and understanding, and we know what it would be
likeprobably because of our age group. Our staff
is older, so we've mostly got daughters or sons who
have been through this situationnot necessarily
nursing, but with some sort of a job. And we know
how daunting that can be and how their whole
51 THE NATURE AND IMPLICATIONS OF SUPPORT IN GRADUATE NURSE TRANSITION PROGRAMS
career can be changed by untoward comments or
actions early in the peace (KSH-FG:27:05, p. 3).
Discussion
The findings of this study strongly suggest that the notion
of support, as applied in contexts of neophyte nursing
practice, is fundamentally a process that aids, encourages,
and strengthens and thereby gives courage and confidence
to a new graduate nurse or a group of new graduates to
practice competently, safely, and effectively in the levels
and areas they have been educationally prepared to work.
The findings of this study further suggest that the core
component of this process is primarily attitudinal, not
material. Although the provision of support is obviously
dependent on the availability of appropriately qualified
staff, it is also manifestly dependent on the appropriate
attitudes of the qualified staff that are available.
Appropriate attitudes and their behavioral expression
have beendescribed inthe context of this study as primarily
involving being benevolent, nonjudgmental, respectful,
constructive, reassuring, patient, polite, friendly, approach-
able, helpful, encouraging, validating, and enabling. In
keeping with the findings of other studies already cited in
this article, this study has likewise found that the
expression of these attitudes (which may now be referred
to by the descriptor support) is of critical importance to
new graduate nurses in terms of their being enabled to
develop their confidence, competence, and capabilities
to practice safely and effectively in the system.
It is evident from the findings of this study that when,
how much, and for how long support should be provided
to a new graduate nurse are very much an individual
matter and one that needs to be decided as much by taking
into account the clinical contexts in which a graduate has
been scheduled to work as by considering his or her
individual character. The data strongly suggest, however,
that although different graduates have different needs,
support must nevertheless be provided at least during the
first 4 weeks of their transition to practice period and
thereafter at the beginning of each new ward rotation for
the duration of the program. Because these timelines have
not been previously identified in the literature, they
remain an issue that would benefit from further research.
In response to the questions of how support should be
given to new graduates and by whom, the findings of this
study underscore the pertinence of the consolidation
model of graduate nurse education (discussed elsewhere)
and providing newgraduates withopportunities to practice
and consolidate (rather than top up) their existing
knowledge and skills (Clare, Longson, Glover, Schubert, &
Hofmeyer, 1996; Clare et al., 2002a, 2002b; Greenwood,
2000). The findings of this study also suggest, ironically,
that informal teachers and the graduate nurses them-
selves may be the ones best suited to providing the support
needed. Given this, organizational strategies need to be
devised to ensure that, paradoxically, these support
processes are themselves supported. As this is an issue
that has been underresearched, it too would benefit from
further inquiry.
Just as the core component of support is attitudinal, so
too is attitude a core component of the barriers to
support. Changing poor attitudes, however, is a perennial
problem and one that may not be easily remedied until
and unless the whole question of support is reframed as
being not just a graduate nurse transition issue (if,
indeed, it has ever been just about graduate nurse
transition) but as a substantive patient safety issue and,
accordingly, something that is everybody's responsibility
(Bagian et al., 2001; Johnstone & Kanitsaki, 2007; Page,
2004; Wachter, 2004).
Conclusion and Recommendations
Support has been defined in the context of this article as a
complex process that aids, encourages, and strengthens
and thereby gives courage and confidence to a nurse or a
group of nurses to practice competently, safely, and
effectively in the levels and areas they have been
educationally prepared to work. Furthermore, it has
been concluded that support is critical to enabling
graduate nurse transition and integration into safe and
effective organizational processes and systems. It is
evident, however, that the nature and implications of
support in the context of graduate nurse transition have
been largely underinvestigated, making it difficult for
comparable research and evidence-based practice and
policy initiatives to be advanced in this area. This lack of
research has also made it difficult to defend, what many
know intuitively to be, the critical relationship that exists
between staff support, the recruitment and retention of
staff, and patient safety outcomes. Accordingly, these
issues stand out as preeminent areas that are ripe for
further research (Johnstone & Kanitsaki, 2006b).
References
Bagian, J., Lee, C., Gosbee, J., DeRosier, J., Stalhandske, E.,
Williams, R., et al. (2001). Developing and deploying a patient
safety program in a large health care delivery system: You can't
fix what you don't know about. Journal of Quality Improvement,
27, 522530.
Boychuk Duchscher, J., & Cowin, L. (2004). The experience
of marginalization in new nursing graduates. Nursing Outlook,
52, 289296.
Brown, H., & Edelmann, R. (2000). Project 2000: A study of
expected and experienced stressors and support reported by
students and qualified nurses. Journal of Advanced Nursing, 31,
857864.
Chang, E., & Daly, J. (2001). Managing the transition from
student to graduate nurse. In Chang E & Daly J, (Eds.),
Transitions in nursing: Preparing for professional practice.
Sydney: MacLennan & Petty.
Chang, E., & Daly, J. (Eds.), Transitions in nursing: Preparing
for professional practice. Sydney: MacLennan & Petty.
Chang, E., Daly, J., Hancock, K., Bidewell, J., Johnson, A.,
Lambert, V., et al. (2006). The relationship among workplace
stressors, coping methods, demographic characteristics, and
health in Australian nurses. Journal of Professional Nursing, 22,
3038.
Clare, J., Longson, D., Glover, P., Schubert, S., & Hofmeyer,
A. (1996). From university student to registered nurse: The
perennial enigma. Contemporary Nurse, 5, 169176.
52 JOHNSTONE ET AL
Clare, J., White, J., Edwards, H., & van Loon, A. (2002).
Curriculum, clinical education, recruitment, transition and
retention in nursing. Final report for the Australian Uni-
versities Teaching Committee (AUTC). Adelaide, SA: School of
Nursing and Midwifery, Flinders University of South
Australia (FUSA).
Clare, J., White, J., Edwards, H., & van Loon, A. (2002).
Learning outcomes and curriculum development in major
disciplines: Nursing. Final report for the Australian Univer-
sities Teaching Committee (AUTC). Adelaide, SA: School of
Nursing and Midwifery, Flinders University of South
Australia (FUSA).
Crooks, D., Carpio, B., Brown, B., Black, M., O'Mara, L., &
Noesgarrd, C. (2005). Development of professional confidence by
post diploma baccalaureate nursing students. Nurse Education in
Practice, 5, 360367.
De Bellis, A., Longson, D., Glover, P., & Hutton, A. (2001).
The enculturation of our nursing graduates. Contemporary
Nurse, 11, 894.
Dearmun, A. (2000). Supporting newly qualified staff nurses:
The lecturer practitioner contribution. Journal of Nursing
Management, 8, 159165.
Duncan, K. (1997). Student pre-entry experience and first
year of employment. Journal of Continuing Education in
Nursing, 28, 223230.
Gerrish, K. (2000). Still fumbling along? A comparative
study of the newly qualified nurse's perception of the
transition from student to qualified nurse. Journal of Advanced
Nursing, 32, 473480.
Goh, K., & Watt, E. (2003). From dependent on to
depended on: The experience of transition from student to
registered nurse in a private hospital graduate nurse program.
Australian Journal of Advanced Nursing, 21, 1420.
Greenwood, J. (2000). Critique of the graduate nurse: An
international perspective. Nurse Education Today, 20, 1723.
Hamel, J. (1993). Case study methods. Newbury Park: Sage
Publications.
Hart, G., & Rotem, A. (1995). The clinical learning
environment: Nurses' perceptions of professional development
in clinical settings. Nurse Education Today, 15, 310.
Johnstone, M. (2002). Poor working conditions and the capa-
city of nurses to provide moral care. Contemporary Nurse, 12,
715.
Johnstone, M., & Kanitsaki, O. (2006a). Processes influen-
cing the development of graduate nurse capabilities in clinical
risk management: An Australian study. Quality Management in
Health Care, 15, 268278.
Johnstone, M., & Kanitsaki, O. (2006b). The moral
imperative of designating patient safety and quality care as a
national nursing research priority. Collegian, 13, 59.
Johnstone, M., & Kanitsaki, O. (2007). Clinical risk
management and patient safety education for nurses: a critique.
Nurse Education Today, 2, 185191.
Johnstone, M., & Kanitsaki, O. (In press). Patient safety,
clinical risk management and the integration of neophyte
graduate nurses into safe organisational processes: An Austra-
lian case study. Quality Management in Health Care [Accepted 4
May, 2007].
Johnstone, M., Kanitsaki, O., Currie, T., Smith, E., &
McGennisken, C. (2007). Designing and delivering clinical
risk management education for graduate nurses: An Australian
study. Nurse Education in Practice, 7, 247257.
Kurtzman, E., & Kizer, K. (2005). Evaluating the perfor-
mance and contribution of nurses to achieve an environment of
safety. Nursing Administration Quarterly, 29, 1423.
Levett-Jones, T., & Fitzgerald, M. (2005). A review of
graduate nurse transition programs in Australia. Australian
Journal of Advanced Nursing, 23, 4045.
Lincoln, Y., & Guba, E. (1985). Naturalistic inquiry. Newbury
Park: Sage Publications.
Maben, J., & Mcleod Clark, J. (1998). Project 2000
diplomates' perceptions of their experiences of transition from
student to staff nurse. Journal of Clinical Nursing, 7, 145153.
Mackin, L., Macera, E., & Jennings, D. (2006). Lessons
learned from a mentored graduate program in gerontological
nursing. Journal of Professional Nursing, 22, 137141.
McCloskey, J. (1990). Two requirements for job content-
ment: Autonomy and social integration. Image: Journal of
Nursing Scholarship, 22, 140143.
Needleman, J., Buerhaus, P., Mattke, S., Stewart, M., &
Zelevinsky, K. (2002). Nurse-staffing levels and the quality of care
in hospitals. NewEngland Journal of Medicine, 346, 17151722.
Page, A. (Ed.). (2004). Keeping patients safe: Transforming the
work environment of nurses. Washington, DC: The National
Academies Press.
Parker, V., Plank, A., & Hegney, D. (2003). Adequacy of
support for new graduates during their transition into the
workplace: A Queensland, Australian study. International
Journal of Nursing Practice, 9, 300305.
Patton, M. (2002). Qualitative research and evaluation
methods. (3rd ed.). Thousand Oaks: Sage Publications.
Piggott, H. (2001). Facing reality: The transition from
student to graduate nurse. Australian Nursing Journal, 8, 2426.
Roberts, K., & Farrell, G. (2003). Expectations and percep-
tions of graduates' performance at the start and at the end of
their graduate year. Collegian, 10, 1318.
Smith, P. (1997). The effectiveness of a preceptorship model
in postgraduate education for rural nurses. Australian Journal of
Rural Health, 5, 147152.
Stake, R. (1995). The art of case study research. Thousand
Oaks: Sage Publications.
Stanley, H. (2003). The journey to becoming a graduate
nurse: A study of the lived experience of part-time post-
registration students. Nurse Education in Practice, 3, 6271.
Theobald, K., & Mitchell, M. (2002). Mentoring: Improving
transition to practice. Australian Journal of Advanced Nursing,
20, 2733.
Thomka, L. (2001). Graduate nurses' experiences of interac-
tions with professional nursing staff during transition to the
professional role. Journal of Continuing Education in Nursing, 32,
1519.
Wachter, R. (2004). The end of the beginning: Patient safety
five years after To err is human. Quality of care, health affairs
web exclusive, November 30, W4-534W4-545.
Yin, R. (2003). Case study research design and methods. (3rd
ed.). Thousand Oaks: Sage Publication.
53 THE NATURE AND IMPLICATIONS OF SUPPORT IN GRADUATE NURSE TRANSITION PROGRAMS
Вам также может понравиться
- HF Network 051612 McKeeДокумент38 страницHF Network 051612 McKeekitsilОценок пока нет
- z812 Role of The BHF Heart Failure Palliative Care Specialist Nurse A Retrospective Evaluation 0111Документ65 страницz812 Role of The BHF Heart Failure Palliative Care Specialist Nurse A Retrospective Evaluation 0111kitsilОценок пока нет
- Managing Chronic Heart FailureДокумент51 страницаManaging Chronic Heart FailurekitsilОценок пока нет
- g235 Heart Failure Nurse Services in England Executive Summary 0908Документ27 страницg235 Heart Failure Nurse Services in England Executive Summary 0908kitsilОценок пока нет
- Disease Management For Heart FailureДокумент84 страницыDisease Management For Heart FailureNational Pharmaceutical Council100% (7)
- GM HFIT Primary Care Heart Failure Project Full ReportДокумент56 страницGM HFIT Primary Care Heart Failure Project Full ReportkitsilОценок пока нет
- Nurse Education in Practice (2004) 4, 100-106Документ7 страницNurse Education in Practice (2004) 4, 100-106kitsilОценок пока нет
- Expectations and Perceptions of Graduates' Performance at The Start and at The End of Their Graduate YearДокумент6 страницExpectations and Perceptions of Graduates' Performance at The Start and at The End of Their Graduate YearkitsilОценок пока нет
- Stresses and Challenges For New Graduates in HospitalsДокумент6 страницStresses and Challenges For New Graduates in HospitalskitsilОценок пока нет
- Enhancing Transition: An Enhanced Model of Clinical Placement For Final Year Nursing StudentsДокумент9 страницEnhancing Transition: An Enhanced Model of Clinical Placement For Final Year Nursing StudentskitsilОценок пока нет
- 1 s2.0 S0099176707004485 MainДокумент6 страниц1 s2.0 S0099176707004485 MainkitsilОценок пока нет
- Transition Within A Graduate Nurse Residency ProgramДокумент10 страницTransition Within A Graduate Nurse Residency ProgramkitsilОценок пока нет
- Successful Strategies For New Graduates: Beth Ulrich, Edd, RN, CheДокумент3 страницыSuccessful Strategies For New Graduates: Beth Ulrich, Edd, RN, ChekitsilОценок пока нет
- 1 s2.0 S0260691707001141 MainДокумент10 страниц1 s2.0 S0260691707001141 MainkitsilОценок пока нет
- The Bridge Program Facilitating The Graduate Nurse's Transition Into The ProfessionДокумент4 страницыThe Bridge Program Facilitating The Graduate Nurse's Transition Into The ProfessionkitsilОценок пока нет
- Experiences and Learning During A Graduate Nurse ProgramДокумент6 страницExperiences and Learning During A Graduate Nurse ProgramkitsilОценок пока нет
- Graduate-Only Pre-Registration Mental Health Nursing ProgrammesДокумент6 страницGraduate-Only Pre-Registration Mental Health Nursing ProgrammeskitsilОценок пока нет
- New Graduate Nurse Transitioning Necessary or NiceДокумент9 страницNew Graduate Nurse Transitioning Necessary or NicekitsilОценок пока нет
- The Transitional Journey Through The Graduate Year A Focus Group StudyДокумент7 страницThe Transitional Journey Through The Graduate Year A Focus Group StudykitsilОценок пока нет
- Facing Registration The Expectations and The Unexpected Original Research ArticleДокумент8 страницFacing Registration The Expectations and The Unexpected Original Research ArticlekitsilОценок пока нет
- New Graduate Nurse Practice Readiness Perspectives On The Context Shaping Our Understanding and ExpectationsДокумент5 страницNew Graduate Nurse Practice Readiness Perspectives On The Context Shaping Our Understanding and ExpectationskitsilОценок пока нет
- The Professional Self-Concept of New Graduate NursesДокумент6 страницThe Professional Self-Concept of New Graduate NurseskitsilОценок пока нет
- The Educational Preparation of Undergraduate Nursing Students in Pharmacology Clinical Nurses' Perceptions and Experiences of Graduate Nurses' Medication KnowledgeДокумент12 страницThe Educational Preparation of Undergraduate Nursing Students in Pharmacology Clinical Nurses' Perceptions and Experiences of Graduate Nurses' Medication KnowledgekitsilОценок пока нет
- 2014new Graduate Nurses' Experiences in Their First Year of PracticeДокумент7 страниц2014new Graduate Nurses' Experiences in Their First Year of PracticekitsilОценок пока нет
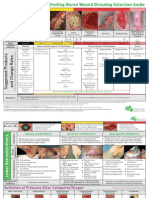
- Wound Dressing GuideДокумент2 страницыWound Dressing Guidekitsil100% (7)
- Best Practice Principles For The Transition From Student To Registered NurseДокумент7 страницBest Practice Principles For The Transition From Student To Registered NursekitsilОценок пока нет
- Fitting in A Pervasive New Graduate Nurse NeedДокумент6 страницFitting in A Pervasive New Graduate Nurse NeedkitsilОценок пока нет
- The Learning Process of Recently Graduated Nurses in Professional Situations - Experiences of An Introduction ProgramДокумент5 страницThe Learning Process of Recently Graduated Nurses in Professional Situations - Experiences of An Introduction ProgramkitsilОценок пока нет
- Graduate Nurse Transition ProgramДокумент5 страницGraduate Nurse Transition ProgramkitsilОценок пока нет
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- 27 ASL For Teacher S BookДокумент28 страниц27 ASL For Teacher S BookNur Syazwani KhamisОценок пока нет
- FY 2022 GAA ProvisionsДокумент2 страницыFY 2022 GAA ProvisionsGamu DILGОценок пока нет
- Healing Elements of Therapeutic ConversationДокумент16 страницHealing Elements of Therapeutic ConversationFERNANDO CABRERA SANTOSОценок пока нет
- Evaluation Tool (Competency Based) - NonescostДокумент35 страницEvaluation Tool (Competency Based) - NonescostFroilan GuilleranОценок пока нет
- Mmda V Concerned Citizens of Manila Bay (GR No 171947) DigestДокумент2 страницыMmda V Concerned Citizens of Manila Bay (GR No 171947) DigestJose Ramon Ampil83% (6)
- Safety Data Sheet: SECTION 1: Identification of The Substance/mixture and of The Company/undertakingДокумент11 страницSafety Data Sheet: SECTION 1: Identification of The Substance/mixture and of The Company/undertakingShahid BhattiОценок пока нет
- C0mponents of A Logic ModelДокумент2 страницыC0mponents of A Logic Modelsameer mohamudallyОценок пока нет
- Brubaker 2001Документ5 страницBrubaker 2001Residencia OftalmologíaОценок пока нет
- Vawc Final ResearchДокумент17 страницVawc Final ResearchWilliam Vincent Soria100% (1)
- Root Caries: A Periodontal Perspective: Review ArticleДокумент21 страницаRoot Caries: A Periodontal Perspective: Review ArticleIlmia AmaliaОценок пока нет
- HSE Assignment 3 FinalДокумент21 страницаHSE Assignment 3 FinalLuqman HakimОценок пока нет
- Environmental Monitoring Incubation Conditions - JustificationДокумент4 страницыEnvironmental Monitoring Incubation Conditions - Justificationveerreddy_157808Оценок пока нет
- Save The ChildrenДокумент12 страницSave The ChildrenBen PalmerОценок пока нет
- Survey QuestionnaireДокумент3 страницыSurvey Questionnairebintot882Оценок пока нет
- Was King Tut Murdered?Документ4 страницыWas King Tut Murdered?mauricio760Оценок пока нет
- A Triumph of Surgery A Triumph of SurgeryДокумент7 страницA Triumph of Surgery A Triumph of SurgeryAmol PagareОценок пока нет
- EMResource - NEDOCS Definitions and Tracking LogДокумент2 страницыEMResource - NEDOCS Definitions and Tracking LogkingdonОценок пока нет
- Baba Farid University of Health Sciences, Faridkot Provisional Merit List of Candidates Applied For Admission To MBBS/BDS Courses Under NEET UG-2021Документ130 страницBaba Farid University of Health Sciences, Faridkot Provisional Merit List of Candidates Applied For Admission To MBBS/BDS Courses Under NEET UG-2021Nitish GargОценок пока нет
- Scientific Point of ViewДокумент2 страницыScientific Point of Viewpavans EnglishОценок пока нет
- Sandy Hill CHC SIS Letter WatsonДокумент3 страницыSandy Hill CHC SIS Letter WatsonJon WillingОценок пока нет
- Reflection PaperДокумент27 страницReflection PaperBon Ryan LeonardoОценок пока нет
- One Compartment Open ModelДокумент81 страницаOne Compartment Open Modelanon_937994778Оценок пока нет
- Aspiracion Destornillador Implanto Roa-V1-Id1018Документ3 страницыAspiracion Destornillador Implanto Roa-V1-Id1018CesarAmorotoОценок пока нет
- Welcome To World of Dream Team For Your SuccessДокумент49 страницWelcome To World of Dream Team For Your SuccessUNKNOWN DREAMERОценок пока нет
- Giant Cell Tumor of Bone - An Overview: Current Concepts ReviewДокумент8 страницGiant Cell Tumor of Bone - An Overview: Current Concepts ReviewDwi fitria nivaОценок пока нет
- ENA - TS - 41-37 - Part - 3 CBДокумент40 страницENA - TS - 41-37 - Part - 3 CBRodolfo DelgadoОценок пока нет
- Understanding and Completing The Reversion (25pp)Документ25 страницUnderstanding and Completing The Reversion (25pp)Tony Lambert100% (3)
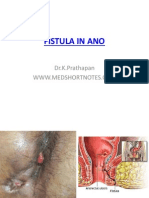
- Fistula in AnoДокумент17 страницFistula in Anoapi-216828341Оценок пока нет
- Ijc Heart & Vasculature: SciencedirectДокумент8 страницIjc Heart & Vasculature: SciencedirectFerdi YuanОценок пока нет
- Spinal Instrumentatio N: Hanif Andhika WДокумент35 страницSpinal Instrumentatio N: Hanif Andhika WHanifОценок пока нет