Академический Документы
Профессиональный Документы
Культура Документы
Incidence of Cervical Stenosis, Radiographic and Anatomic
Загружено:
Marylin Pilar0 оценок0% нашли этот документ полезным (0 голосов)
48 просмотров6 страницSmall canal diameters have been associated with increased neurologic dysfunction. Some patients with radiographic stenosis may be asymptomatic. A canal diameter of 10 to 13 mm is considered to be relatively stenotic.
Исходное описание:
Оригинальное название
2007. Incidence of Cervical Stenosis, Radiographic and Anatomic
Авторское право
© © All Rights Reserved
Доступные форматы
PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документSmall canal diameters have been associated with increased neurologic dysfunction. Some patients with radiographic stenosis may be asymptomatic. A canal diameter of 10 to 13 mm is considered to be relatively stenotic.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
48 просмотров6 страницIncidence of Cervical Stenosis, Radiographic and Anatomic
Загружено:
Marylin PilarSmall canal diameters have been associated with increased neurologic dysfunction. Some patients with radiographic stenosis may be asymptomatic. A canal diameter of 10 to 13 mm is considered to be relatively stenotic.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 6
Incidence of Cervical
Stenosis: Radiographic and Anatomic
Clayton L. Dean, MD,* Michael J. Lee, MD,
and Ezequiel H. Cassinelli, MD*
Cervical canal size and shape can play a role in the development of myelopathy and/or
radiculopathy. Small canal diameters have been associated with increased neurologic
dysfunction for a variety of conditions. Various radiographic criteria have been used to
better dene sagittal canal dimensions, with variable degrees of accuracy. In addition,
some patients with radiographic stenosis may be asymptomatic, thus making the signi-
cance of radiographic stenosis less clear.
Semin Spine Surg 19:12-17 2007 Elsevier Inc. All rights reserved.
KEYWORDS cervical spine anatomy, stenosis, vertebrae
T
he important role that the size and shape of the cervical
spinal canal plays in the development of symptoms of
myelopathy or radiculopathy has been recognized for some
time. A small sagittal cervical canal diameter has been asso-
ciated with increased risk of neurological injury in traumatic,
degenerative, and inammatory conditions. Lindgren is
credited with rst pointing out the importance of the sagittal
diameter of the cervical canal.
1
Two decades later, additional
investigators corroborated the association of a small canal in
symptomatic cervical spondylosis.
2,3
The average sagittal diameter of the cervical spinal cord
ranges from 5 to 11.5 mm (mean 10 mm) as demonstrated on
computed tomography (CT) and myelography.
4
The average
sagittal diameter of the canal fromC3toC7ranges from15to25
mm(mean, 17 mm). Debate exists regarding the absolute canal
diameter that constitutes cervical stenosis. Absolute stenosis has
been dened as a cervical sagittal canal diameter of less than 10
mm, as seen on a lateral cervical spine radiograph. A canal di-
ameter of 10 to 13 mm is considered to be relatively stenotic.
5
Radiographic Incidence
Plain Radiography
The sagittal distance, as measured from the middle of the
posterior surface of the vertebral body to the closest point on
the spinolaminar line, is known as the developmental seg-
mental sagittal diameter (DSSD).
6
Early attempts to identify
cervical stenosis based on plain radiographs focused on mea-
suring the average sagittal diameter of the spinal canal on
lateral radiography taken at a standardized distance. Countee
and Vijayanathan reported that the normal sagittal diameter
of the spinal canal was between 18.3 and 18.5 mm at C3 and
17.8 mm between C4 and C7 using this method.
7
They re-
ported that males with a canal diameter less than 14 mm had
a higher risk of quadriplegia following cervical trauma. This
denition may be somewhat misleading and an underestima-
tion, however, since the stenosis was measured at the level of
the posterior mid-body, rather than at the superior or inferior
aspect of the posterior body, which is the point of maximum
stenosis in cervical spondylosis.
Edwards and LaRocca described the spondylosis index (SI)
as the difference between the DSSD and the spondylotic seg-
mental sagittal diameter (SSSD). It represents the amount of
canal narrowing due to the spondylotic process
6
(Fig. 1).
Based on their ndings, they predicted that patients with
canal sizes of less than 10 mm were likely to be myelopathic;
those with a 10- to 13-mm canal were premyelopathic; those
with a 13- to 17-mmcanal were less prone to myelopathy but
prone to symptomatic cervical spondylosis, and those with a
canal greater than 17 mm were asymptomatic.
Kang and coworkers analyzed factors involved in fractures
and dislocations of the cervical spine and their relation to the
degree of spinal cord.
8
In reviewing preinjury cervical spine
lms, they found that the mean space available for the cord at
the level of traumatic injury was 10.5 mm in patients who
had a complete injury, 13.1 mmfor those who had an incom-
plete injury, 15.9 mm for those with an isolated nerve root
*Department of Orthopaedic Surgery, Case Medical Center, Cleveland,
Ohio.
Department of Orthopaedic Surgery, Rush University Medical Center, Chi-
cago, Illinois.
Address reprint requests to Ezequiel H. Cassinelli, MD, Department of Or-
thopaedic Surgery, Case Medical Center, 11100 Euclid Avenue, Cleve-
land, OH 44106. E-mail: zekedr@hotmail.com
12 1040-7383/07/$-see front matter 2007 Elsevier Inc. All rights reserved.
doi:10.1053/j.semss.2007.01.003
injury, and 16.7 mmfor those who had no neurologic decit.
Their ndings showed a clear correlation between the space
available for the cord, the sagittal diameter of the spinal canal,
and the severity of spinal cord injury. They concluded that
patients who had a large sagittal canal diameter were less
likely to have severe spinal cord injury following a fracture or
dislocation compared with patients who had a narrow canal.
In this respect, a large spinal canal was considered to be
protective against future spinal cord injury.
In a similar study, Eismont and colleagues investigated the
relationship between cervical spine sagittal canal diameter
and neurologic injury in cases of cervical spine fracture-dis-
location.
9
Their ndings were comparable to those reported
by Kang and coworkers
8
in that small diameter canals were
correlated signicantly with neurologic injury, while large
diameter canals allowed protection fromneurologic injury in
cervical fracture-dislocation.
PavlovTorg Ratio
Pavlov and coworkers introduced a ratio method to identify
levels of stenosis.
10
In their ratio method, the sagittal diame-
ter of the spinal canal is divided by the sagittal diameter of the
corresponding vertebral body (canal diameter/vertebral body
diameter) (Fig. 2). They felt that this method was more reli-
able and reproducible for determining cervical spinal steno-
sis and was independent of technical and magnication vari-
ables. Using this method, a ratio less than 0.82 was thought
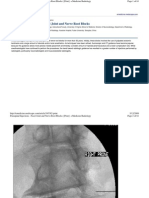
Figure 2 Lateral radiograph depicting the Torg ratio, which is the
sagittal diameter of the spinal canal (A) divided by the sagittal di-
ameter of the corresponding vertebral body (B).
Figure 1 Lateral radiograph depicting the spondylosis index (SI),
which is the difference between the developmental segmental sag-
ittal diameter (A) and the spondylotic segmental sagittal diameter
(B) and represents the amount of narrowing due to the disease
process.
Incidence of cervical stenosis 13
to indicate absolute stenosis. Torg and colleagues later eval-
uated the relationship of developmental narrowing of the
cervical canal to reversible and irreversible injury of the cer-
vical spinal cord in football players.
11
He found that a ratio
of 0.80 or less had a high sensitivity (93%) for transient
cervical neurapraxia. However, its low positive-predictive
value (0.2%) precluded its use as a screening tool for deter-
mining the susceptibility of an athlete to neurapraxia and
therefore for future safe participation in contact sports.
The reliability of the canal/vertebral body ratio for detect-
ing the incidence of cervical stenosis has been studied exten-
sively. Lim and Wong evaluated the variation of this ratio
with gender and ethnicity.
12
They found that the ratio dif-
fered widely not only between different ethnic groups but
also between genders within the same ethnic population. The
sagittal canal diameter was narrowest at C4 in both males and
females, although females had smaller sagittal diameters at all
levels than males. Based on these ndings, they concluded
that the canal/body ratio was not an accurate indicator of the
sagittal canal diameter and therefore could not be used to
reliably identify the presence of cervical canal stenosis.
Hukuda and Kojima also attempted to evaluate the gender
variation in the canal/body ratio method.
13
They found that
the canal/body ratio was signicantly larger in women than in
men and that this difference may help explain the male prev-
alence of cervical myelopathy.
Some studies have also shown that the canal/body ratio is
smaller in patients with cervical spondylotic myelopathy
compared with a nonmyelopathic population. Yue and co-
workers showed that the ratio is signicantly smaller in my-
elopathic patients (mean, 0.72) compared with a group of
control patients (0.95).
14
The authors felt that the ratio
method could be used to predict the likelihood of developing
cervical spondylotic myelopathy. Emery and coworkers, on
the other hand, analyzed the relationship of the canal/body
ratio to cervical myelopathy in a study of 108 patients.
15
Neither the canal/body ratio nor the sagittal diameter of the
canal at its narrowest point were associated with the severity
of preoperative or postoperative myelopathy according to the
Nurick grade.
The study by Kang and coworkers analyzed the relation
between the canal/body ratio and the severity of spinal cord
injury.
8
The mean ratio at the uninjured levels was 0.82 for
the patients who had a complete injury, 0.84 for those with
an incomplete injury, 0.96 for those who had an isolated
nerve root injury, and 0.96 for those who had no neurologic
decit. These ndings supported the predictive value of the
ratio method in determining the possibility and severity of
spinal cord injury. As mentioned previously, these ndings
were further supported by Eismont and colleagues in their
investigation of the relationship between cervical spine sag-
ittal canal diameter and neurologic injury in cases of cervical
fracture-dislocation.
9
Although numerous studies have both supported and re-
futed the validity of using the canal/body ratio in predicting
the likelihood of subsequent spinal cord injury, few have
quantied the actual incidence of cervical spinal stenosis
based on this method. Odor and colleagues studied the inci-
dence of cervical spinal stenosis in professional and rookie
football players.
16
They found that 32% of professional foot-
ball players and 34% of rookies had a canal/body ratio of less
than 0.80 at one or more levels from C3 to C6. This nding
implied that nearly one-third of this cohort of athletes had
cervical spinal stenosis as determined by the ratio method.
This nding suggests that other factors and other imaging
studies must be considered in the evaluation of a patient with
cervical spinal stenosis.
Computed Tomography
The addition of CT, particularly when combined with my-
elography, has several advantages over plain radiography in
the evaluation of cervical spinal stenosis. Bone anatomy is
visualized extremely well, as is intradural and extradural pa-
thology. This is of particular importance in patients with
spondylosis, since the neural foramina, lateral recess, and
spinal canal are often compressed by osteophytes. CT my-
elography helps distinguish soft-tissue neural compression
from bony compression, which may strongly inuence sur-
gical planning. CT enables measurement of both anteropos-
terior (AP) and transverse canal dimensions as well as the
space available for the spinal cord at each spinal level.
The ability of CT to measure the sagittal dimension of the
cervical spinal canal has been evaluated. Blackley and co-
workers correlated lateral radiographs and corresponding CT
scans of 76 patients sustaining trauma to the cervical spine,
whose radiographic examinations were deemed normal.
17
They utilized CT scans to determine the true diameter of the
cervical canal at each level and then compared the canal/body
ratio with the CT canal diameter. They found that the canal/
body ratio was linearly related to the true diameter of the
canal at each vertebral level. However, the correlation coef-
cient for the canal/body ratio compared with the true diam-
eter was found to be relatively low at each level. Based on
these ndings, they felt that the canal/body ratio is of limited
value in the assessment of the true diameter of the cervical
spinal canal.
In their study of 108 patients with cervical spondylotic
myelopathy, Emery and coworkers utilized CT myelography
in 103 of the patients.
15
The cross-sectional area of the spinal
canal at the level of maximum compression was analyzed
with respect to preoperative and postoperative Nurick grade
of myelopathy to determine if it had any predictive value.
They found that the average cross-sectional area of the spinal
canal was 34.6 mm
2
. The cross-sectional area of the spinal
cord was not found to be associated with the preoperative or
postoperative severity of myelopathy. At this time, we are not
aware of any studies to determine the exact incidence of
cervical stenosis based on CT ndings alone.
Signicance of Cervical Spinal Canal Shape
While numerous authors have demonstrated the importance
of the size of the cervical spinal canal on the development of
myelopathy, few have focused on the importance of the
shape of the canal and the effect that this may have on neu-
rologic compromise.
14 C.L. Dean, M.J. Lee, and E.H. Cassinelli
Ogino and coworkers performed a detailed clinicopatho-
logic study of nine patients with cervical spondylotic myelop-
athy.
18
They found a good correlation between the degree of
spinal cord compression and the ratio of the AP (sagittal)
canal diameter to the transverse canal diameter. They desig-
nated this as the AP compression ratio. Their ndings sug-
gested that as the AP compression ratio decreased, the canal
assumed a more elliptical shape and the risk of neurologic
compression and myelopathy increased. In other words, an
elliptical-shaped canal portended a poorer prognosis with
regard to the development of cervical spondylotic myelopa-
thy than did a round canal. They found that developmental
narrowing of the cervical spinal canal was the most signi-
cant factor responsible for a decrease in the AP compression
ratio, with multilevel spondylotic protrusions being less im-
portant. Pathologically, they found that developmental nar-
rowing resulted in extensive demyelination of the posterolat-
eral funiculus and infarction of the gray matter.
Matsuura and colleagues also demonstrated the impor-
tance of the shape of the cervical spinal canal in spinal cord
injured patients.
19
They measured the cross-sectional area
and the sagittal and transverse diameters of the cervical canal
in patients who had a traumatic spinal cord injury and com-
pared these ndings to 100 control subjects. Interestingly,
they observed no difference in the two groups with regard to
cross-sectional area of the spinal canal. However, the sagittal
diameter of the spinal canal of the control group was found to
be signicantly larger than those of the spinal cord injured
group. Conversely, the transverse diameter of the spinal ca-
nal of the spinal cord injured group was signicantly larger
than those of the control group. The difference between their
two groups, based on the ratio of sagittal to transverse diam-
eter, was highly signicant. Because this measure was a ratio,
they concluded that there was no need to evaluate an indi-
vidual on the basis of absolute values alone. These ndings
suggested that certain patients may be predisposed to spinal
Figure 3 Sagittal (A) and axial (B and C) T2-weighted images of a 43-year-old male with a history of mild neck pain
which resolved. MRI reveals multilevel stenosis with myelomalacia and abnormal cord signal. The lack of CSF space
around the spinal cord is indicative of lack of a functional reserve. The patient exhibited no signs or symptoms of
myelopathy despite the degree of stenosis.
Incidence of cervical stenosis 15
cord injury following sufcient trauma and that it may not be
the total volume of space in the spinal canal that was the
critical factor, but rather the shape of the canal.
Magnetic Resonance Imaging (MRI)
MRI has signicantly impacted the diagnosis and treatment
of cervical spondylosis and symptomatic cervical canal ste-
nosis. MRI demonstrates the high contrast between cerebro-
spinal uid and disk/osteophyte material (Fig. 3). It is also
capable of providing multiplanar images and reconstructions
in numerous planes. This imaging modality has become the
standard to evaluate patients with cervical spinal stenosis.
Boden and coworkers prospectively investigated the prev-
alence of abnormal MRI scans of the cervical spine in asymp-
tomatic subjects.
20
They evaluated the MRI scans of asymp-
tomatic volunteers and compared themto scans of a group of
symptomatic patients. The scans demonstrated an abnormal-
ity in 19% of the asymptomatic subjects, including 14% of
those less than 40 years old and 28% of those older than 40.
Of those less than 40, 10% had a herniated disc and 4% had
foraminal stenosis. Of the subjects who were older than 40,
5% had a herniated disc, 3% had bulging of one or more
discs, and 20% had foraminal stenosis. In addition, disc de-
generation or disc narrowing at one or more level was present
in 25% of subjects less than 40 and in nearly 60% of those
older than 40. The authors concluded that the high incidence
of abnormal ndings in asymptomatic subjects was part of
the normal aging process of spinal degeneration. Teresi and
coworkers also studied the incidence of abnormal MRI scans
in 100 asymptomatic subjects.
21
They found spinal cord im-
pingement by MRI in 16% of patients younger than 64 years
and in 26% of patients older than 64 years. These and other
studies emphasize the danger of making operative decisions
based only on diagnostic imaging tests without correlating
such ndings with clinical signs and symptoms (Fig. 3).
Prasad and colleagues correlated cervical MRI measure-
ments with canal/vertebral body ratios.
22
They found that the
correlation between this ratio and the additional space avail-
able for the spinal cord, as shown by the cerebrospinal uid
(CSF) column surrounding the cord, was only moderate,
with the best correlation being at C5. Their study demon-
strated a poor correlation between the canal/body ratio and
the space available for the cord, and they therefore felt that
this ratio alone could not be used to infer conclusions about
actual spinal cord compression.
Other studies have used alternative methods of dening
cervical stenosis based on MRI ndings. Cantu dened cer-
vical canal stenosis as the absence of a functional reserve
(Fig. 3) around the spinal cord.
23
The absence of such a
functional reserve was felt to be a contraindication to further
participation in contact sports following an episode of tran-
sient neurapraxia. Cantu and Mueller reported a 270% re-
duction in permanent spinal cord injury since 1971, from a
peak of 20 per year to only 7.2 per year.
24
Although there are
several possible explanations for this reduction, increased
awareness of preexisting cervical canal stenosis was thought
to be a major factor.
Anatomic Incidence
One method of assessing the cervical spine canal diameter is
by direct measurement of cadaveric spinal canal specimens.
This provides perhaps the most accurate assessment of bony
canal diameter. However, there are several limitations to this
method. Because of variation in radiographic magnication,
anatomic measurements may not directly reect radio-
graphic measurements, which is the most common way to
assess canal diameter. Second, the presence and signicance
of soft-tissue pathology cannot be accounted for by evaluat-
ing only bony cadaveric specimens. Third, measurements of
cadaveric specimens offer no information regarding the pres-
ence or absence of symptoms.
Lee and coworkers reported on the largest series of direct
anatomic measurements to determine the incidence of ana-
tomic cervical stenosis.
25
They analyzed 469 adult cadaveric
cervical spines and correlated these measurements with plain
radiographs. Based on these direct measurements, they
found that the average AP canal diameter for all specimens at
all levels was 14.1 mm. Males had signicantly larger cervical
spinal canals than females at all levels. The C4 level was
found to be the most frequently stenotic level (10.6%). In this
study, stenosis was dened as a sagittal canal diameter of less
than 12 mm. Overall, 21.5% of the population had at least
one stenotic level. Of the specimens older than 50 years of
age, 29.1% had at least one level of stenosis. In specimens
greater than 70 years old, 33.3% were found to have at least
one level of stenosis.
After adjusting for body size and radiographic magnica-
tion, they determined that cervical stenosis would have been
present in 4.9% of the overall adult population, 6.8% of the
population over age 50, and 9.2% of the population over 70
years of age. Allowing for potential errors associated with the
correction for both body size and radiographic magnica-
tion, the authors stated that the true incidence of cervical
stenosis was likely between 4.9 and 21.5% of the general
population. Based on these ndings, an increased incidence
of cervical stenosis occurs with increasing age. Because of the
frequency of cervical spine stenosis, the authors emphasized
that treatment decisions should not be based on radiographic
studies alone, but must be correlated with clinical signs and
symptoms.
Summary
Various methods have been described to determine the inci-
dence of cervical spinal stenosis. Based on MRI studies, up to
19% of asymptomatic individuals may demonstrate radio-
graphic abnormalities.
20
This incidence increases with age,
suggesting that such changes are part of the normal aging
process of spinal degeneration. Similarly, cadaveric studies
using direct canal measurements have suggested that cervical
stenosis is common, affecting approximately 4.9 to 21.5% of
the population. Neither the incidence and prevalence of
asymptomatic nor the symptomatic cervical stenosis has been
accurately determined. Furthermore, the natural history of
asymptomatic stenosis has not been well dened. Future in-
16 C.L. Dean, M.J. Lee, and E.H. Cassinelli
vestigations of these conditions will allow us to better under-
stand the disease process.
References
1. Lindgren E: The importance of the sagittal diameter of the spinal canal
in the cervical region. Nevenartz 10:240, 1937
2. Pallis C, Jones AM, Spillane JD: Cervical spondylosis; incidence and
implications. Brain 77(2):274-289, 1954
3. Payne EE, Spillane JD: The cervical spine. An anatomic pathologic
study of seventy patients. Brain 70:38, 1957
4. Herzog RJ, Weins JJ, Dillingham MF, et al: Normal cervical spine mor-
phometry and cervical spine stenosis in asymptomatic professional
football players. Spine 16:178-186, 1991
5. Murone I: The importance of the sagittal diameters of the cervical canal
in relation to spondylosis and myelopathy. J Bone Joint Surg Br 56:30-
36, 1974
6. Edwards WC, LaRocca H: The developmental segmental sagittal diam-
eter of the cervical spinal canal in patients with cervical spondylosis.
Spine 8(1):20-27, 1983
7. Countee RW, Vijayanathan T: Congenital stenosis of the cervical spine:
diagnosis and management. J Natl Med Assoc 71:257-264, 1979
8. Kang JD, Figgie MP, Bohlman HH: Sagittal measurements of the cervi-
cal spine in subaxial fractures and dislocations. An analysis of two
hundred and eighty-eight patients with and without neurologic de-
cits. J Bone Joint Surg Am 76(11):1617-1628, 1994
9. Eismont FJ, Clifford S, Goldberg M, et al: Cervical sagittal spinal canal
size in spine injury. Spine 9(7):663-666, 1984
10. Pavlov H, Torg JS, Robie B, et al: Cervical spinal stenosis: determination
with vertebral body ratio method. Radiology 164(3):771-775, 1987
11. Torg JS, Naranja RJ Jr, Pavlov H, et al: The relationship of developmen-
tal narrowing of the cervical spinal canal to reversible and irreversible
injury of the cervical spinal cord in football players. J Bone Joint Surg
Am 78(9):1308-1314, 1996
12. Lim JK, Wong HK: Variation of the cervical spinal Torg ratio with
gender and ethnicity. Spine J 4(4):396-401, 2004
13. Hukuda S, Kojima Y: Sex discrepancy in the canal/body ratio of the
cervical spine implicating the prevalence of cervical myelopathy in
men. Spine 27(3):250-253, 2002
14. Yue WM, Tan SB, Tan MH, et al: The Torg-Pavlov ratio in cervical
spondylotic myelopathy. A comparative study between patients with
cervical spondylotic myelopathy and a nonspondylotic, nonmyelo-
pathic population. Spine 26(16):1760-1764, 2001
15. Emery SE, Bohlman HH, Bolesta MJ, et al: Anterior cervical decompres-
sion and arthrodesis for the treatment of cervical spondylotic myelop-
athy. Two to seventeen-year follow-up. J Bone Joint Surg Am 80(7):
941-951, 1998
16. Odor JM, Watkins RG, Dillin WH, et al: Incidence of cervical spinal
stenosis in professional and rookie football players. Am J Sports Med
18(5):507-509, 1990
17. Blackley HR, Plank LD, Robertson PA: Determining the sagittal dimen-
sions of the canal of the cervical spine. The reliability of ratios of
anatomical measurements. J Bone Joint Surg Br 81(1):110-112, 1999
18. Ogino H, Tada K, Okada K, et al: Canal diameter, anteroposterior
compression ratio, and spondylotic myelopathy of the cervical spine.
Spine 8(1):1-15, 1983
19. Matsuura P, Waters RL, Adkins RH, et al: Comparison of computerized
tomography parameters of the cervical spine in normal control subjects
and spinal cord-injured patients. J Bone Joint Surg Am 71(2):183-188,
1989
20. Boden SD, McCowin PR, Davis DO, et al: Abnormal magnetic reso-
nance scans of the cervical spine in asymptomatic subjects. A prospec-
tive investigation. J Bone Joint Surg Am 72(8):1178-1184, 1990
21. Teresi LM, Lufkin RB, Reicher MA, et al: Asymptomatic degenerative
disk disease and spondylosis of the cervical spine. Radiology 164(1):
83-88, 1987
22. Prasad SS, OMalley M, Caplan M, et al: MRI measurements of the
cervical spine and their correlation to Pavlovs ratio. Spine 28(12):
1263-1268, 2003
23. Cantu RC: Functional cervical spinal stenosis: a contraindication to
participation in contact sports. Med Sci Sports Exerc 25(3):316-317,
1993
24. Cantu RC, Mueller FO: Catastrophic spine injuries in American foot-
ball, 1977-2001. Neurosurgery 53(2):362-363, 2003
25. Lee MJ, Cassinelli EH, Riew KD: The prevalence of cervical spine ste-
nosis: an anatomic study of 469 cadaveric specimens. J Bone Joint Surg
Am 2006 (in press)
Incidence of cervical stenosis 17
Вам также может понравиться
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (120)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (399)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- (New Procedures in Spinal Interventional Neuroradiology) Luigi Manfrà (Eds.) - Spinal Canal Stenosis-Springer International PublisДокумент98 страниц(New Procedures in Spinal Interventional Neuroradiology) Luigi Manfrà (Eds.) - Spinal Canal Stenosis-Springer International PublisThuyet Nguyen PhuocОценок пока нет
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Low Back PainДокумент80 страницLow Back PainJagdish AgroyaОценок пока нет
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- DEGENERATIVE SPINE DISEASE and HomeopathyДокумент21 страницаDEGENERATIVE SPINE DISEASE and Homeopathypawajee100% (3)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Lumbar Spinal Stenosis: A Definitive GuideДокумент4 страницыLumbar Spinal Stenosis: A Definitive GuideGuyОценок пока нет
- Low Back PainДокумент20 страницLow Back PainFrancisco CanalesОценок пока нет
- Evidence Based OrthopaedicsДокумент663 страницыEvidence Based Orthopaedicssamabdelaal2000Оценок пока нет
- Lumbar Spine SampleДокумент3 страницыLumbar Spine SampleRizky NoviantoroОценок пока нет
- Tandem Spinal StenosisДокумент4 страницыTandem Spinal StenosisikhwanОценок пока нет
- LaminectomyДокумент5 страницLaminectomyanon_931797817Оценок пока нет
- Computer Aided Diagnosis System For Lumbar Spinal Stenosis Using X-Ray ImagesДокумент45 страницComputer Aided Diagnosis System For Lumbar Spinal Stenosis Using X-Ray Imagesroky100% (1)
- Concept Map FinalДокумент1 страницаConcept Map Finalapi-383763177Оценок пока нет
- Abraham 2016Документ12 страницAbraham 2016w5jctwsq5qОценок пока нет
- Patent Foramen Ovale PFOДокумент3 страницыPatent Foramen Ovale PFOvishwanathОценок пока нет
- Diagnosis and Management of Lumbar Spinal StenosisДокумент12 страницDiagnosis and Management of Lumbar Spinal StenosisMaíra CerqueiraОценок пока нет
- Low Back Pain: Aldy S. RambeДокумент40 страницLow Back Pain: Aldy S. RambeHatta Diana TariganОценок пока нет
- Final - Spinal Stenosis L4, L5 Secondary To Spondylolisthesis L4, L5 Grade II With Hypertrophized Ligament Um and Radiculopathy With Myelopathy Right SidedДокумент66 страницFinal - Spinal Stenosis L4, L5 Secondary To Spondylolisthesis L4, L5 Grade II With Hypertrophized Ligament Um and Radiculopathy With Myelopathy Right SidedJai - Ho100% (1)
- Disorders of The Cauda EquinaДокумент20 страницDisorders of The Cauda EquinaSalvador FigueroaОценок пока нет
- LaminectomyДокумент16 страницLaminectomyNicole John C. BolanteОценок пока нет
- Final - Bme 298 Final Project SkeletonДокумент22 страницыFinal - Bme 298 Final Project Skeletonapi-522861974Оценок пока нет
- Magsaysay v. NLRCДокумент17 страницMagsaysay v. NLRCJohn BernalОценок пока нет
- Low Back Pain-Orthoinfo - AaosДокумент13 страницLow Back Pain-Orthoinfo - AaosBang mantoОценок пока нет
- Daftar Diagnosis Dan Tindakan Orthopaedi Ina CBG Baru Dan PlafonbДокумент17 страницDaftar Diagnosis Dan Tindakan Orthopaedi Ina CBG Baru Dan PlafonbRamco AbtizaОценок пока нет
- Uganda Charitable Spine Surgery Mission 2013 Trip Report Ver 1 Sept 15Документ29 страницUganda Charitable Spine Surgery Mission 2013 Trip Report Ver 1 Sept 15api-197209808Оценок пока нет
- Facet Block TechniqueДокумент61 страницаFacet Block TechniquedrpravinpadalkarОценок пока нет
- Lumbar Laminectomy Surgery For Spinal StenosisДокумент15 страницLumbar Laminectomy Surgery For Spinal StenosisElizabeth Liles MartinezОценок пока нет
- Patofisiologi Lumbal Spinal StenosisДокумент2 страницыPatofisiologi Lumbal Spinal StenosisokkiemsОценок пока нет
- ICD Code ChartДокумент1 страницаICD Code ChartbjpalmerОценок пока нет
- c2Документ37 страницc2LuisAngelPonceTorresОценок пока нет
- Introduction To NeuroimagingДокумент84 страницыIntroduction To NeuroimagingLiezty VioLen'sОценок пока нет