Академический Документы
Профессиональный Документы
Культура Документы
Diplejia Braquial
Загружено:
Diego Agustin Zarza0 оценок0% нашли этот документ полезным (0 голосов)
44 просмотров7 страницBrachial amyotrophic diplegia is a form of segmental motor neuron disease. This disorder may represent one end of a spectrum of motor neuron diseases. Motor neuron disease associated with human immunodeficiency virus infection was first reported in 1985.
Исходное описание:
Оригинальное название
Diplejia braquial
Авторское право
© © All Rights Reserved
Доступные форматы
PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документBrachial amyotrophic diplegia is a form of segmental motor neuron disease. This disorder may represent one end of a spectrum of motor neuron diseases. Motor neuron disease associated with human immunodeficiency virus infection was first reported in 1985.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
44 просмотров7 страницDiplejia Braquial
Загружено:
Diego Agustin ZarzaBrachial amyotrophic diplegia is a form of segmental motor neuron disease. This disorder may represent one end of a spectrum of motor neuron diseases. Motor neuron disease associated with human immunodeficiency virus infection was first reported in 1985.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 7
OBSERVATION
Brachial Amyotrophic Diplegia in a Patient
With Human Immunodeficiency Virus Infection
Widening the Spectrum of Motor Neuron Diseases Occurring
With the Human Immunodeficiency Virus
Joseph R. Berger, MD; Patricio S. Espinosa, MD, MPH; John Kissel, MD
A
lthough amyotrophic lateral sclerosis and progressive spinal muscular atrophy have
been recognized to occur in association with human immunodeficiency virus infec-
tion, to our knowledge, brachial amyotrophic diplegia, a formof segmental motor neu-
ron disease, has not been previously reported. Brachial amyotrophic diplegia results
in severe lower motor neuron weakness and atrophy of the upper extremities in the absence of
bulbar or lower extremity involvement, pyramidal features, bowel and bladder incontinence, and
sensory loss. We describe a human immunodeficiency virusseropositive man without severe im-
munosuppression or prior AIDS-defining illnesses who had brachial amyotrophic diplegia. This
disorder may represent one end of a spectrum of motor neuron diseases occurring with this ret-
rovirus infection. Arch Neurol. 2005;62:817-823
Motor neuron disease associated with hu-
man immunodeficiency virus (HIV) in-
fection was first reported in 1985,
1
4 years
after the initial description of AIDS. Clini-
cal patterns of HIV-associated motor neu-
ron disease may mirror those of amyotro-
phic lateral sclerosis (ALS)
1-5
or progressive
spinal muscular atrophy (PSMA).
6-11
How-
ever, to our knowledge, a segmental form
of PSMA referred to as brachial amyotro-
phic diplegia (BAD) has not been previ-
ously describedinassociationwithHIVin-
fection. This disorder is a form of
neurogenic man-in-the-barrel syn-
drome in which severe bilateral upper ex-
tremity weakness is unaccompanied by
bulbar lower extremity or pyramidal ab-
normalities.
12
When associated with mo-
tor neuron disease, it has also been re-
ferred to as the flail arm syndrome
13
and
the hanging armsyndrome.
14
BADis clas-
sified as a formof segmental lower motor
neuron disease.
15
While a similar clinical
phenotype of bilateral upper extremity
weakness may occur following cere-
bral,
16-21
brainstem,
22-24
cervical spinal
cord,
25-28
or bilateral brachial plexus in-
sult,
29,30
these may be distinguished from
BAD by clinical presentation and radio-
graphic and electrophysiological stud-
ies.
12
Furthermore, the lack of involve-
ment of bulbar and lower extremity
muscles, the absence of pyramidal signs,
andthe long survival withthis disorder dis-
tinguish it from ALS.
12,15
We describe an
HIV-seropositive manpresenting withpro-
gressive upper extremity weakness that de-
veloped in the absence of a detectable vi-
ral load or any preceding AIDS-related
complications.
REPORT OF A CASE
This 35-year-old man was first aware of a
slowly progressive weakness of the right
shoulder in June 2000 when he noted dif-
ficulty lifting heavy objects above his head
with his right arm. The symptoms in his
right arm progressed, and by June 2001,
a similar weakness had developed in the
left shoulder. Weakness and wasting were
progressive in both upper extremities and
inhis chest muscles inthe ensuing months.
He denied speech or swallowing difficul-
ties, leg weakness, sphincter distur-
Author Affiliations: Departments of Neurology (Drs Berger and Espinosa) and
Internal Medicine (Dr Berger), University of Kentucky College of Medicine,
Lexington; and Department of Neurology, Ohio State University, Columbus
(Dr Kissel).
(REPRINTED) ARCH NEUROL/ VOL 62, MAY 2005 WWW.ARCHNEUROL.COM
817
2005 American Medical Association. All rights reserved.
Downloaded From: http://archneur.jamanetwork.com/ on 08/17/2014
bances, fasciculations, or stiffness. He reported rare mild
cramps in his right medial plantar muscles.
In February 2001, laboratory testing revealed that he
was HIV seropositive by enzyme-linked immunosor-
bent assay and Western blot analysis. At that time, his
CD4 cell count was 244/L and his HIV viral load was
8315 copies per milliliter. He started antiretroviral com-
bination therapy, including zidovudine, lamivudine, and
abacavir succinate (Trizivir) in August 2001, and by Sep-
tember 2001, his CD4 cell count was 377/L and the HIV
viral load was undetectable. His medical history was re-
markable for diabetes mellitus diagnosed at the age of 14
years, which had been complicated by diabetic retinopa-
thy requiring a right eye vitrectomy in 1998, diabetic pe-
ripheral neuropathy, and mild diabetic nephropathy with
nonnephrotic proteinuria. The development of severe
weakness of his upper extremities ultimately precluded
self-injection of insulin, and an insulin pump was in-
serted. There was no family history of neuromuscular dis-
orders.
A physical examination performed in April 2003
showed a slender man, weighing 55.8 kg. His cognition,
language, and speech were normal. The result of a cra-
nial nerve examination was normal. There was dramatic
wasting of the muscles of the shoulder girdle and upper
extremity and to a lesser extent the muscles of the fore-
arms, hands, chest, and thorax (Figure). The scapulae
were winged. Coarse fasciculations were observed in
multiple muscles in the upper extremity and over the
chest. His abdominal muscles were preserved. No spas-
ticity was evident. Upper extremity strength was graded
as trace in both deltoids, 2 of 5 in the right biceps and
brachioradialis, 3 of 5 in the left biceps and brachiora-
dialis, 4 of 5 in both triceps, and 4 of 5 at the wrist
extensors and flexors, although the extensors were
weaker. His interossei and other intrinsic hand muscles
were mildly weak. Wasting in the lower extremities was
confined to both extensor digitorum brevis muscles,
greater on the left, which was associated with weakness
of toe extension. Otherwise, strength in his lower
extremities was preserved. Muscle stretch reflexes were
graded as absent at the right biceps and brachioradialis,
1 at the right triceps, trace at the left biceps and bra-
chioradialis, 1 at the left triceps, 2 at both knee
jerks, and trace at the ankles. There was no Hoffmann
or Babinski sign, and his jaw jerk was normal. His gait
was normal. Pinprick and temperature sensation were
diminished to the lower third of the calves. Vibratory
and position sense was diminished in a stocking distri-
bution in the distal lower extremities, and the Romberg
sign was positive.
The result of magnetic resonance imaging of the cer-
vical spine was normal, with minimal degenerative
changes of the spine. With the exception of a mildly
increased creatine kinase level (3.8610
5
U/L), the
results of hematologic and other laboratory studies,
including erythrocyte sedimentation rate, rheumatoid
factor, antinuclear antibody, tests for hereditary neu-
ropathy with liability to pressure palsies, and antibodies
to GM1 and myelin-associated glycoprotein, were nega-
tive or normal. The complete blood cell count revealed
a hemoglobin level of 12.3 g/dL, a hematocrit of 36%,
and a white blood cell count of 6500/L, with a normal
differential. The vitamin B
12
level was 528 pg/mL (390
pmol/L). Cerebrospinal fluid analysis showed 3/L leu-
kocytes, 0 erythrocytes, a glucose level of 115 mg/dL
(6.38 mmol/L), a protein level of 5.510
2
g/dL, nega-
tive microbiological study results, including those for
the VDRL test and cryptococcal antigen, normal cyto-
logic test results, a normal IgG index, and 7 oligoclonal
bands (attributed to HIV infection). Cerebrospinal fluid
HIV viral assays were not performed. Electrophysiologi-
cal studies performed on February 20, 2001, showed
evidence of active and chronic denervation bilaterally of
muscles innervated by C5 through the middle thoracic
nerve roots by electromyography. The result of needle
electromyography of the lower extremities was normal,
with the exception of the observation of long-duration
large-amplitude motor unit action potentials, fibrilla-
tion potentials, and mildly reduced recruitment in the
muscles supplied by the superficial and deep peroneal
nerves. Nerve conduction studies in the legs revealed
sensory amplitudes all greater than 60% of the lower
limit of normal for our laboratory, with preserved con-
duction velocities. Motor conductions were all greater
than the 90th percentile of the lower limit of normal,
with normal amplitudes. The changes overall were
compatible with a mild to moderate distal sensorimotor
polyneuropathy with predominantly axonal features.
The findings on the nerve conduction study were com-
plex and believed to be most consistent with diabetic
peripheral neuropathy, a right peroneal neuropathy,
and bilateral mild ulnar nerve entrapments at the
elbow.
A trial of intravenous immunoglobulin was initiated
in October 2003 without any improvement. Through
January 2004, there was neither significant progression
of his weakness nor development of any cranial nerve ab-
normalities or weakness, cramps, or fasciculations of the
lower extremities.
COMMENT
Motor neuron disease with HIV infection may appear in
several forms. A summary of previously reported cases
of motor neuron disease complicating HIV infection
and a summary of our patient are included in the
Table. Motor neuron disease with HIV infection may
be indistinguishable from classic ALS, resulting in an
inexorably progressive disorder of upper and lower
Figure. Profound
wasting of the muscles
of the upper extremities
and chest is evident.
(REPRINTED) ARCH NEUROL/ VOL 62, MAY 2005 WWW.ARCHNEUROL.COM
818
2005 American Medical Association. All rights reserved.
Downloaded From: http://archneur.jamanetwork.com/ on 08/17/2014
Table. Summary of Cases of Motor Neuron Disease Heralding HIV Infection
Source
Age, y/
Sex
Clinical
Manifestations
CD4 Cell
Count/L Viral Load at Dx CSF Findings
Opportunistic
Illness Treatment Outcome Survival
Zoccolella et
al,
5
2002
44/M CC: hand weakness,
cramps, and
weight loss. NE:
hypotrophy and
fasciculations
(tongue and
upper and lower
limbs); no
sensory
abnormalities;
Hoffman and
Babinski signs
present.
360 34 000
copies/mL
Leukocytes,
7/L; glucose,
43 mg/dL;
protein,
6.1 10
-2
g/dL; HIV
RNA, 370
copies/mL
None Zidovudine,
lamivudine, and
nevirapine
Bedridden,
respiratory
failure, death
3 y
Nishio et al,
6
2001
42/F CC: dysphagia,
dysarthria, and
dysphonia. NE:
hypotrophy and
fasciculations
(tongue) and
proximal limb
weakness and
atrophy; no
sensory
abnormalities.
107 44 510
copies/mL
Leukocytes,
29/L;
glucose, 46
mg/dL;
protein,
12.6 10
-2
g/dL
None Stavudine,
lamivudine, and
nelfinavir mesylate
Improvement
of the
symptoms
after therapy,
alive
Alive, minimal
neurological
problems?
Verma et al,
9
1990
32/M CC: progressive
lower limb
weakness plus
cramps. NE:
upper and lower
limb proximal
weakness and
fasciculations;
mild atrophy; no
sensory
abnormalities.
NA (T4/T8,
0.73)
NA NA None at Dx NA Successive
opportunistic
infections,
death
2 y
Casado et
al,
4
1997
30/M CC: progressive
upper limb
weakness plus
hypotrophy. NE:
upper and lower
limb distal
weakness and
fasciculations;
mild atrophy; no
sensory
abnormalities.
NA (T4/T8,
0.76)
NA Normal None NA Deterioration of
PSMA Sx,
HIV infection,
stable
Alive at
publication
Galassi et
al,
7
1998
30/M CC: extremity
weakness,
cramps, weight
loss, and fatigue.
NE: proximal limb
asymmetric
weakness; flexor
plantar response;
mild atrophy; no
sensory
abnormalities.
340 (T4/T8,
0.4)
NA Leukocytes,
0/L; glucose,
NA; protein,
17.4 10
-2
g/dL
Skin bacterial
infections
Zidovudine,
zalcitabine, and
methylpredniso-
lone
Progressive
respiratory
failure, death
NA
Sastre-
Garriga et
al,
31
2000
39/F CC: lower limb
weakness and
cramps. NE:
hypotrophy and
fasciculations
(tongue); distal
limb weakness;
no sensory
abnormalities.
540 NA Leukocytes,
0/L; glucose,
60 mg/dL;
protein,
2 10
-2
g/dL
NA NA NA NA
(continued)
(REPRINTED) ARCH NEUROL/ VOL 62, MAY 2005 WWW.ARCHNEUROL.COM
819
2005 American Medical Association. All rights reserved.
Downloaded From: http://archneur.jamanetwork.com/ on 08/17/2014
Table. Summary of Cases of Motor Neuron Disease Heralding HIV Infection (cont)
Source
Age, y/
Sex
Clinical
Manifestations
CD4 Cell
Count/L Viral Load at Dx CSF Findings
Opportunistic
Illness Treatment Outcome Survival
MacGowan
et al,
2
2001
32/F CC: generalized
weakness, weight
loss, and
dysarthria. NE:
tongue
fasciculations and
upper and lower
limb proximal and
more distal
weakness;
Hoffman and
plantar signs
present; no
sensory
abnormalities.
44 77 900
copies/mL
Leukocytes,
14/L;
glucose, NA;
protein,
13.4 10
-2
g/dL
None Zidovudine,
lamivudine, and
nelfinavir
Deterioration;
and after
antiretroviral
treatment, full
recovery
Alive
Goldstein et
al,
32
1993
22/F CC: lower extremity
pain and
weakness. NE:
upper limb P/D,
4/5; distal limb P,
3/5, D 2/5; mild
sensory
abnormalities.
438 (T4/T8,
0.39)
NA Leukocytes,
1/L; glucose,
NA; protein,
7.3 10
-2
g/dL
None Zidovudine, IV
immunoglobulin,
and
methylpredniso-
lone
Deterioration,
relapses,
improvement
NA
38/M CC: facial droop
and upper limb
weakness. NE:
upper and lower
weakness; DTR
absent; no
sensory
abnormalities.
353 (T4/T8,
0.45)
NA Leukocytes,
16/L;
glucose, NA;
protein,
15 10
-2
g/dL
None IV immunoglobulin,
methylpredniso-
lone, and
plasmapheresis
Deterioration,
stabilization
NA
Huang et
al,
10
1993
45/M CC: generalized
weakness,
fasciculations,
weight loss, and
quadriplegia. NE:
tongue atrophy
and
fasciculations;
upper and lower
limb paralysis; no
sensory
abnormalities.
397 (T4/T8,
1.13)
NA Leukocytes,
11/L;
glucose, 60
mg/dL;
protein,
5.7 10
-2
g/dL
None Zidovudine No further
deterioration
NA
Moulignier
et al,
3
2001
27/M CC: right hand
weakness, muscle
wasting, and
dysarthria.
84 NA Leukocytes,
5/L; protein,
4.6 10
-2
g/dL
None Zidovudine Transient
stabilization
6 mo (ADC)
61/M CC: left leg
weakness, muscle
wasting, and
cramps.
44 NA Leukocytes,
8/L; protein,
5.4 10
-2
g/dL
None Zidovudine Full recovery 2 y (OI)
29/M CC: left leg
weakness and
tongue
fasciculations.
2 NA Leukocytes,
3/L; protein,
2.5 10
-2
g/dL
None Zidovudine Partial recovery Unknown
(unavailable
for
follow-up)
22/M CC: bilateral lower
limb weakness,
muscle wasting,
and
fasciculations.
37 3.7 log
10
copies/mL
Leukocytes,
13/L;
protein,
5.2 10
-2
g/dL
None Zidovudine and
didanosine
Partial recovery 3 y (OI)
25/M CC: left arm
weakness, muscle
wasting, and
fasciculations.
123 4.9 log
10
copies/mL
Leukocytes,
2/L; protein,
3.6 10
-2
g/dL
None Zidovudine and
zalcitabine
Partial recovery 4 y (ADC)
40/F CC: left arm
weakness and
mild muscle
atrophy.
227 3.3 log
10
copies/mL
Leukocytes,
1/L; protein,
4.2 10
-2
g/dL
None Zidovudine and
didanosine
Full recovery Alive for 3 y
(continued)
(REPRINTED) ARCH NEUROL/ VOL 62, MAY 2005 WWW.ARCHNEUROL.COM
820
2005 American Medical Association. All rights reserved.
Downloaded From: http://archneur.jamanetwork.com/ on 08/17/2014
motor neurons.
1-5
Alternatively, progressive lower
motor neuron disease affecting bulbar and extremity
muscles may occur in the absence of upper motor neu-
ron findings consistent with PSMA.
6-11
Other disorders
occurring with HIV infection that mimic motor neuron
disease include chronic inflammatory polyradiculoneu-
ropathy,
34
axonal motor polyradiculoneuropathy,
32
and
multifocal motor neuropathy with anti-GM1 antibod-
ies.
33
While progressive lower motor neuron weakness
is seen with these disorders, the slow tempo of our
patients illness would be distinctly unusual for chronic
inflammatory polyradiculoneuropathy and multifocal
motor neuropathy, and its severity and distribution
inconsistent with HIV-associated axonal motor polyra-
diculoneuropathy.
Our patient had focal weakness of the right upper ex-
tremity that progressed to involve the left upper extrem-
ity during the ensuing year. The weakness and wasting
have remained confined to a few myotomes of the cer-
vical and upper thoracic region. There has been neither
involvement of bulbar muscles nor progressive weak-
ness of his lower extremities. The lower extremity find-
ings of distal sensory loss, depressed ankle jerks, and dis-
tal wasting and weakness are the consequence of his
concomitant diabetic peripheral neuropathy and mild en-
trapment neuropathies. Therefore, we believe that pro-
found weakness and wasting of his upper extremities are
consistent with BAD.
Diabetes may result in brachial and lumbosacral
plexopathies, resulting in a disorder referred to as dia-
betic radiculoplexus neuropathy (or diabetic amyotro-
phy) that may mimic the disorder observed in our pa-
tient.
35
This disorder, however, affects the lumbosacral
plexus in most cases, and upper extremity involvement
is uncommon.
36,37
In addition, patients with brachial dia-
betic radiculoplexus neuropathy typically have unilat-
eral weakness that progresses more rapidly than in our
patient with preceding weight loss, severe pain, and sen-
sory andautonomic abnormalities.
35
Because none of these
features was present in our patient, we think this an un-
likely cause of our patients disorder.
Motor neuron disease occurring in association with
HIVinfection has been attributed to direct damage to the
motor neurons by HIV, neurotoxic HIV viral proteins,
cytokines and chemokines arising consequent to HIVin-
fection, and opportunistic viruses that directly attack mo-
tor neurons.
32
The prototypical virally mediated motor
neuron disease is poliomyelitis
36
; however, it is clini-
cally quite distinct fromthe inheritedandidiopathic forms
of motor neuron disease. Flaccid paralysis has been re-
ported with various viruses in the Enterovirus genus.
36
Recently, Frenchinvestigators have foundthe nucleic acid
of enteric cytopathogenic human orphan virus, an en-
terovirus, in the neuronal cell bodies within the gray mat-
ter of the spinal cord of 88% of patients with ALS, sug-
gesting a possible association between this enterovirus
and ALS.
37
However, poliovirus and other enterovi-
ruses, when associated with weakness, are typically char-
acterized by an acute febrile illness followed by a flaccid
paralysis of 1 or more limbs.
36
Whether HIVinfection it-
Table. Summary of Cases of Motor Neuron Disease Heralding HIV Infection (cont)
Source
Age, y/
Sex
Clinical
Manifestations
CD4 Cell
Count/L Viral Load at Dx CSF Findings
Opportunistic
Illness Treatment Outcome Survival
Hoffman et
al,
1
1985
26/M CC: weakness,
atrophy, and
fasciculations of
the left arm.
NA NA NA None NA Progressive 1 y
Sher et al,
8
1988
30/M CC: weakness,
wasting, and
fasciculations.
NA NA NA None NA Partial recovery 3 mo
(pneumonia)
Simpson et
al,
33
1994
45/M CC: asymmetric
limb weakness,
atrophy, and
fasciculations.
560 NA NA None Zidovudine,
prednisone, and IV
immunoglobulin
Stabilization 24 mo
(opportunis-
tic
infections)
Present
case
35/M CC: weakness
(upper
extremities). NE:
atrophy of
shoulder girdle,
upper proximal
extremities, and
pectoral and
thoracic muscles;
mild sensory
abnormalities due
to concomitant
diabetic
neuropathy.
244 Undetectable
viral load
Leukocytes,
3/L; glucose,
115 mg/dL;
protein,
5.5 10
-2
g/dL;
oligoclonal
bands, 7
None Zidovudine,
didanosine,
abacavir succinate,
and IV
immunoglobulin
Stabilization,
no further
deterioration
Alive 46 mo
after onset
Abbreviations: ADC, AIDS dementia complex; CC, chief complaint; CSF, cerebrospinal fluid; D, distal; DTR, deep tendon reflex; Dx, diagnosis; HIV, human
immunodeficiency virus; IV, intravenous; NA, data not available; NE, neurological; OI, osteogenesis imperfecta; P, proximal; PSMA, progressive spinal muscular atrophy;
Sx, symptoms; T4/T8, ratio of CD4 to CD8 lymphocytes.
SI conversion factor: To convert glucose to millimoles per liter, multiply by 0.05551.
(REPRINTED) ARCH NEUROL/ VOL 62, MAY 2005 WWW.ARCHNEUROL.COM
821
2005 American Medical Association. All rights reserved.
Downloaded From: http://archneur.jamanetwork.com/ on 08/17/2014
self or an accompanying, currently unrecognized, op-
portunistic infection is responsible for the motor neu-
ron findings in HIV-infected persons with motor neuron
disease or whether it is unrelated to HIV infection re-
mains to be determined. Findings of reverse transcrip-
tase,
38
antibodies directed to human retroviral anti-
gens,
39
an association of human T-lymphotropic virus I
with clinical and pathological features consistent with
ALS,
40,41
amplification of human T-lymphotropic virus
tax/rex,
39
animal models of retrovirus-induced motor neu-
ron disease,
42,43
and the presence of PSMA and ALS in
HIV infection suggest that HIV infection is causative or
contributory.
While the pathogenesis of ALS remains a conun-
drum, several theories have been proposed. Among the
possible mechanisms that are considered are neuronal
excitation and free radical generation.
44
Both of these
mechanisms have also beenproposedas pathways to brain
neuronal injury in the setting of HIV infection.
45
Mito-
chondria, through several mechanisms, have also been
suggested as instrumental in ALS, as in other neurode-
generative disorders.
46
A critical role of the mitochon-
dria in neuronal apoptosis has been suggested with neu-
rotoxic HIV proteins, gp120,
47
and Tat.
48
Some
investigators have also advanced a role for autoimmu-
nity in ALS.
49,50
Antineuronal antibodies have been dem-
onstrated in HIV infection, and may correlate with the
presence of dementia.
51,52
Therefore, several proposed
pathogenetic mechanisms for ALS may also be opera-
tive in HIV-associated central nervous system disease.
In conclusion, motor neuron disease occurs in asso-
ciation with HIV infection. The spectrum of HIV-
associated motor neuron disease is broad and includes
BAD, PSMA, and ALS. These disorders remain rare, and
their underlying pathogenesis is uncertain.
Accepted for Publication: June 16, 2004.
Correspondence: Joseph R. Berger, MD, Department of
Neurology, University of Kentucky College of Medi-
cine, 740 S Limestone St, Lexington, KY 40536-0284
(jrbneuro@uky.edu).
Author Contributions: Study concept and design: Berger
and Kissel. Acquisition of data: Berger and Kissel. Analy-
sis and interpretation of data: Berger and Espinosa. Draft-
ing of the manuscript: Berger and Espinosa. Critical revi-
sion of the manuscript for important intellectual content:
Berger and Kissel. Administrative, technical, and material
support: Berger and Espinosa. Study supervision: Berger.
REFERENCES
1. Hoffman PM, Festoff BW, Giron LT Jr, Hollenbeck LC, Garruto RM, Ruscetti FW.
Isolation of LAV/HTLV-III from a patient with amyotrophic lateral sclerosis.
N Engl J Med. 1985;313:324-325.
2. MacGowan DJ, Scelsa SN, Waldron M. An ALS-like syndrome with new HIV in-
fection and complete response to antiretroviral therapy. Neurology. 2001;57:
1094-1097.
3. Moulignier A, Moulonguet A, Pialoux G, RozenbaumW. Reversible ALS-like dis-
order in HIV infection. Neurology. 2001;57:995-1001.
4. Casado I, Gomez M, Carmona C, Garcia-Castanon I, Martin C, Sanchez JF. Mo-
tor neuron disease and HIV [in Spanish]. Rev Neurol. 1997;25:552-554.
5. Zoccolella S, Carbonara S, Minerva D, et al. A case of concomitant amyotrophic
lateral sclerosis and HIV infection. Eur J Neurol. 2002;9:180-182.
6. Nishio M, Koizumi K, Moriwaka F, Koike T, Sawada K. Reversal of HIV-
associated motor neuron syndrome after highly active antiretroviral therapy.
J Neurol. 2001;248:233-234.
7. Galassi G, Gentilini M, Ferrari S, et al. Motor neuron disease and HIV-1 infection
ina 30-year-oldHIV-positive heroinabuser: a causal relationship?ClinNeuropathol.
1998;17:131-135.
8. Sher J, Wrzolek M, Shnuter Z. Motor neuron disease with AIDS [abstract]. J Neu-
ropathol Exp Neurol. 1988;47:303.
9. Verma RK, Ziegler DK, Kepes JJ. HIV-related neuromuscular syndrome simu-
lating motor neuron disease. Neurology. 1990;40:544-546.
10. Huang PP, Chin R, Song S, Lasoff S. Lower motor neuron dysfunction associ-
ated with human immunodeficiency virus infection. Arch Neurol. 1993;50:1328-
1330.
11. Pearl D, Noursadeghi M, Manji H, Edwards S, Miller R. Lower motor neuron syn-
drome and HIV infection [letter]. Sex Transm Infect. 2003;79:351.
12. Katz JS, Wolfe GI, Andersson PB, et al. Brachial amyotrophic diplegia: a slowly
progressive motor neuron disorder. Neurology. 1999;53:1071-1076.
13. Hu MT, Ellis CM, Al-Chalabi A, Leigh PN, Shaw CE. Flail arm syndrome: a dis-
tinctive variant of amyotrophic lateral sclerosis. J Neurol Neurosurg Psychiatry.
1998;65:950-951.
14. Mulder DW. The clinical syndrome of amyotrophic lateral sclerosis. Mayo Clin
Proc. 1957;32:427-436.
15. Van Den Berg-Vos RM, Van Den Berg LH, Visser J, de Visser M, Franssen H,
Wokke JH. The spectrum of lower motor neuron syndromes. J Neurol. 2003;
250:1279-1292.
16. Sage JI, Van Uitert RL. Man-in-the-barrel syndrome. Neurology. 1986;36:1102-
1103.
17. Clerget L, Lenfant F, Roy H, Giroud M, Ben Salem D, Freysz M. Man-in-the-
barrel syndrome after hemorrhagic shock. J Trauma. 2003;54:183-186.
18. Crisostomo EA, Suslavich FJ. Man-in-the-barrel syndrome associated with closed
head injury. J Neuroimaging. 1994;4:116-117.
19. Moore AP, Humphrey PR. Man-in-the-barrel syndrome caused by cerebral
metastases. Neurology. 1989;39:1134-1135.
20. Shaw PJ, Tharakaram S, Mandal SK. Brachial diplegia as a sequel to cardio-
respiratory arrest: man-in-the-barrel syndrome [letter]. Postgrad Med J. 1990;
66:788.
21. Hurley JP, Wood AE. Isolated man-in-the-barrel syndrome following cardiac
surgery. Thorac Cardiovasc Surg. 1993;41:252-254.
22. Alberca R, Iriarte LM, Rasero P, Villalobos F. Brachial diplegia in central pontine
myelinolysis. J Neurol. 1985;231:345-346.
23. Georgiadis D, Schulte-Mattler WJ. Cruciate paralysis or man-in-the-barrel syn-
drome? report of a case of brachial diplegia. Acta Neurol Scand. 2002;105:
337-340.
24. Strupp M, Bruckmann H, Hamann GF, Bruning R, Brandt T. Simultaneous bra-
chial diplegia and rotational vertigo due to combined spinal anterior and verte-
brobasilar embolism. Eur Neurol. 2000;43:240-242.
25. Berg D, Mullges W, Koltzenburg M, Bendszus M, Reiners K. Man-in-the-barrel
syndrome caused by cervical spinal cord infarction. Acta Neurol Scand. 1998;
97:417-419.
26. Renard JF, Massardier E, Iasci L, et al. Brachial diplegia caused by cervical spi-
nal cord ischemia: a case [in French]. Rev Neurol (Paris). 1997;153:690-693.
27. Barbizet J, Degos JD, Hurth M, Duval J, Aillerie MA. Brachial diplegia due to is-
chemia of the anterior horns during septicemia caused by Salmonella typhimu-
rium [in French]. Ann Med Interne (Paris). 1974;125:191-194.
28. Fuentes JM, Vlahovitch B, Negre C. Brachial diplegia of traumatic origin as a re-
sult of injuries of the cervical cord [in French]. Neurochirurgie. 1984;30:165-
170.
29. Foncea N, Yurrebaso I, Gomez Beldarrain M, Garcia-Monco JC. Postoperative
bilateral brachial plexopathy mimicking the man-in-the-barrel syndrome [in
Spanish]. Neurologia. 2002;17:388-390.
30. Zuin DR, Neme R, Vera J. Bilateral braquial plexopathy mimicking the man-in-
the-barrel syndrome [in Spanish] [letter]. Neurologia. 2003;18:413.
31. Sastre-Garriga J, Tintore M, Raguer N, Ruiz I, Montalban X, Codina A. Lower
motor neuron disease in a HIV-2 infected woman. J Neurol. 2000;247:718-
719.
32. Goldstein JM, Azizi SA, Booss J, Vollmer TL. Human immunodeficiency virus
associated motor axonal polyradiculoneuropathy. Arch Neurol. 1993;50:1316-
1319.
33. Simpson D, Morgello S, Citak K, Corbo M, Latov N. Motor neuron disease as-
sociated with HIV-1 and antiasialo GM1 antibody [abstract]. Muscle Nerve. 1994;
17:1091.
34. Dalakas MC, Cupler EJ. Neuropathies in HIV infection. Baillieres Clin Neurol. 1996;
5:199-218.
35. Dyck PJ, Windebank AJ. Diabetic and nondiabetic lumbosacral radiculoplexus
neuropathies: new insights into pathophysiology and treatment. Muscle Nerve.
2002;25:477-491.
(REPRINTED) ARCH NEUROL/ VOL 62, MAY 2005 WWW.ARCHNEUROL.COM
822
2005 American Medical Association. All rights reserved.
Downloaded From: http://archneur.jamanetwork.com/ on 08/17/2014
36. Ropka S, Jubelt B. Enteroviruses. In: Berger J, ed. Clinical Neurovirology. New
York, NY: Marcel Dekker Inc; 2003:359-377.
37. Berger MM, Kopp N, Vital C, Redl B, Aymard M, Lina B. Detection and cellular
localization of enterovirus RNA sequences in spinal cord of patients with ALS.
Neurology. 2000;54:20-25.
38. Andrews WD, Tuke PW, Al-Chalabi A, et al. Detection of reverse transcriptase
activity in the serum of patients with motor neurone disease. J Med Virol. 2000;
61:527-532.
39. Westarp ME, Ferrante P, Perron H, Bartmann P, Kornhuber HH. Sporadic ALS/
MND: a global neurodegeneration with retroviral involvement? J Neurol Sci. 1995;
129(suppl):145-147.
40. Kuroda Y, Sugihara H. Autopsy report of HTLV-Iassociated myelopathy pre-
senting with ALS-like manifestations. J Neurol Sci. 1991;106:199-205.
41. Jubelt B. Viruses and motor neuron diseases. Adv Neurol. 1991;56:463-472.
42. Jubelt B. Motor neuron diseases and viruses: poliovirus, retroviruses, and
lymphomas. Curr Opin Neurol Neurosurg. 1992;5:655-658.
43. Gardner MB, Henderson BE, Officer JE, et al. A spontaneous lower motor neu-
ron disease apparently caused by indigenous type-C RNA virus in wild mice.
J Natl Cancer Inst. 1973;51:1243-1254.
44. Bromberg MB. Pathogenesis of amyotrophic lateral sclerosis: a critical review.
Curr Opin Neurol. 1999;12:581-588.
45. Kaul M, Garden GA, Lipton SA. Pathways to neuronal injury and apoptosis in
HIV-associated dementia. Nature. 2001;410:988-994.
46. Manfredi G, Beal MF. The role of mitochondria in the pathogenesis of neurode-
generative diseases. Brain Pathol. 2000;10:462-472.
47. Corasaniti MT, Turano P, Bilotta A, et al. Evidence that increases of mitochon-
drial immunoreactive IL-1 by HIV-1 gp120 implicate in situ cleavage of pro-
IL-1 in the neocortex of rat. J Neurochem. 2001;78:611-618.
48. Kruman II, Nath A, Mattson MP. HIV-1 protein Tat induces apoptosis of hippo-
campal neurons by a mechanism involving caspase activation, calcium over-
load, and oxidative stress. Exp Neurol. 1998;154:276-288.
49. Yi FH, Lautrette C, Vermot-Desroches C, et al. In vitro induction of neuronal apop-
tosis by antiFas antibodycontaining sera from amyotrophic lateral sclerosis
patients. J Neuroimmunol. 2000;109:211-220.
50. Appel SH, Smith RG, Engelhardt JI, Stefani E. Evidence for autoimmunity in amyo-
trophic lateral sclerosis. J Neurol Sci. 1994;124(suppl):14-19.
51. Schutzer SE, Brunner M, Fillit HM, Berger JR. Autoimmune markers in HIV-
associated dementia. J Neuroimmunol. 2003;138:156-161.
52. Kumar M, Resnick L, Loewenstein DA, Berger J, Eisdorfer C. Brain-reactive an-
tibodies and the AIDS dementia complex. J Acquir Immune Defic Syndr. 1989;
2:469-471.
(REPRINTED) ARCH NEUROL/ VOL 62, MAY 2005 WWW.ARCHNEUROL.COM
823
2005 American Medical Association. All rights reserved.
Downloaded From: http://archneur.jamanetwork.com/ on 08/17/2014
Вам также может понравиться
- Neurology Multiple Choice Questions With Explanations: Volume IОт EverandNeurology Multiple Choice Questions With Explanations: Volume IРейтинг: 4 из 5 звезд4/5 (7)
- Guillain-Barre Syndrome Presenting With Sensory Disturbance Following A Herpes Virus Infection: A Case ReportДокумент5 страницGuillain-Barre Syndrome Presenting With Sensory Disturbance Following A Herpes Virus Infection: A Case ReportAsep MetrikaОценок пока нет
- Acquired NeuropathiesДокумент106 страницAcquired NeuropathiesDanny J. BrouillardОценок пока нет
- Progressive Multifocal Leukoencephalopathy - A Case: Ovidiu Rosca, Elena-Cecilia Rosca, Lucian NegrutiuДокумент5 страницProgressive Multifocal Leukoencephalopathy - A Case: Ovidiu Rosca, Elena-Cecilia Rosca, Lucian Negrutiunoorhadi.n10Оценок пока нет
- Case ReportДокумент5 страницCase ReportsyahputriОценок пока нет
- A Rare Presentation of Guillain-Barre Syndrome: Pharyngeal Cervical-Brachial VariantДокумент2 страницыA Rare Presentation of Guillain-Barre Syndrome: Pharyngeal Cervical-Brachial VariantdzakiyahОценок пока нет
- Cranial Nerve Enhancement in The Guillain-Barre Syndrome: DiscussionДокумент3 страницыCranial Nerve Enhancement in The Guillain-Barre Syndrome: DiscussionAdesh KumarОценок пока нет
- Leg Weakness in A 66-Year-Old Woman: A Common Presentation of An Uncommon DiseaseДокумент10 страницLeg Weakness in A 66-Year-Old Woman: A Common Presentation of An Uncommon DiseaseCarlos De Santiago CastilloОценок пока нет
- Ptosis Without Ophthalmoplegia: A Rare Manifestation of Guillain-Barré SyndromeДокумент5 страницPtosis Without Ophthalmoplegia: A Rare Manifestation of Guillain-Barré SyndromeMosОценок пока нет
- Jurnal GBSДокумент26 страницJurnal GBSfajar sugandaОценок пока нет
- Marchiafava-Bignami Disease Literature Review and Case ReportДокумент4 страницыMarchiafava-Bignami Disease Literature Review and Case Reportc5nazs86Оценок пока нет
- Guillain BarréДокумент4 страницыGuillain BarréAlondra CastilloОценок пока нет
- Als LymeДокумент2 страницыAls LymeChristine Anne HellmundОценок пока нет
- GBS Source 1Документ4 страницыGBS Source 1PJHG50% (2)
- Illnesses Presenting As Acute Flaccid Paralysis: Dr. N. Aumeer - PaediatricianДокумент36 страницIllnesses Presenting As Acute Flaccid Paralysis: Dr. N. Aumeer - PaediatricianIqe ChanОценок пока нет
- Fast Facts: Diagnosing Amyotrophic Lateral Sclerosis: Clinical wisdom to facilitate faster diagnosisОт EverandFast Facts: Diagnosing Amyotrophic Lateral Sclerosis: Clinical wisdom to facilitate faster diagnosisОценок пока нет
- Guillain Barre SyndromeДокумент13 страницGuillain Barre SyndromeAdreiTheTripleAОценок пока нет
- BH 010060 ENGДокумент2 страницыBH 010060 ENGCarlosОценок пока нет
- Tuberculous Transverse Myelitis: Case Report and Review of The LiteratureДокумент7 страницTuberculous Transverse Myelitis: Case Report and Review of The LiteraturenoraОценок пока нет
- Diagnosis and Management of Diabetic Amyotrophy: EndocrinologyДокумент3 страницыDiagnosis and Management of Diabetic Amyotrophy: EndocrinologyDavis G. OctaviusОценок пока нет
- AJRM Sept 18-20Документ3 страницыAJRM Sept 18-20Indah RismandasariОценок пока нет
- Subacute Transverse Myelitis Developed Depending On Lyme Disease: A Case ReportДокумент3 страницыSubacute Transverse Myelitis Developed Depending On Lyme Disease: A Case ReportmuthmainnahОценок пока нет
- Exercise-Associated Numbness and Tingling in The Legs: For Editorial Comment See Page 1509Документ4 страницыExercise-Associated Numbness and Tingling in The Legs: For Editorial Comment See Page 1509herpthederpОценок пока нет
- Dampd 5 Manual Del Jugador EspДокумент24 страницыDampd 5 Manual Del Jugador EspClaudio ReichelОценок пока нет
- ChoreaДокумент6 страницChoreamainehoonaОценок пока нет
- Pons LesionДокумент4 страницыPons Lesiontjimen2Оценок пока нет
- A Case of Sporadic Creutzfeldt-JakobДокумент5 страницA Case of Sporadic Creutzfeldt-JakobVlad PopescuОценок пока нет
- Holanda Et Al - J Neurovirol 2022Документ4 страницыHolanda Et Al - J Neurovirol 2022jtd9h2xp5hОценок пока нет
- GB Syndrome, Lancet 2005Документ14 страницGB Syndrome, Lancet 2005Saymin S GlezОценок пока нет
- Neurological Complications of Lyme DiseaseДокумент3 страницыNeurological Complications of Lyme DiseasekumsmmcОценок пока нет
- Guillain Barr Syndrome Occurring Synchronously With Systemic Lupus Erythematosus As Initial Manifestation Treated Successfully With Low DoseДокумент5 страницGuillain Barr Syndrome Occurring Synchronously With Systemic Lupus Erythematosus As Initial Manifestation Treated Successfully With Low DoseTessa CruzОценок пока нет
- Neuro JournalДокумент7 страницNeuro JournalLannydchandraОценок пока нет
- Case Presentation: Prepared &presented by DR - Fatema Al-HamadeДокумент20 страницCase Presentation: Prepared &presented by DR - Fatema Al-HamadeTABEEBAОценок пока нет
- Pn0722 CR MogadДокумент4 страницыPn0722 CR MogadWafae TouchaОценок пока нет
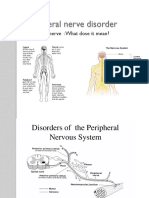
- Peripheral Nerve DisorderДокумент23 страницыPeripheral Nerve DisorderSaman SarKoОценок пока нет
- Guillain-Barré Syndrome in Adults - Clinical Features and DiagnosisДокумент14 страницGuillain-Barré Syndrome in Adults - Clinical Features and DiagnosisElsyAlegríaОценок пока нет
- A Case of Male Sle: An Unusual PresentationДокумент4 страницыA Case of Male Sle: An Unusual PresentationIJAR JOURNALОценок пока нет
- Peripheral Neuropathy in Chronic Liver Disease: Clinical, Electrodiagnostic, and Biopsy FindingsДокумент10 страницPeripheral Neuropathy in Chronic Liver Disease: Clinical, Electrodiagnostic, and Biopsy Findingsrifqi rhОценок пока нет
- The Successful Treatment of DisinhibitioДокумент4 страницыThe Successful Treatment of DisinhibitioVicky NotesОценок пока нет
- Ankylosing Spondylitis: Submitted by Safeer Mohammed S 302 General Medicine Submitted To Dr. Marietta DavidianДокумент20 страницAnkylosing Spondylitis: Submitted by Safeer Mohammed S 302 General Medicine Submitted To Dr. Marietta DavidianSafeer VarkalaОценок пока нет
- Reversible Myelopathy in A 34-Year-Old Man With Vitamin B DeficiencyДокумент4 страницыReversible Myelopathy in A 34-Year-Old Man With Vitamin B DeficiencyT.A.BОценок пока нет
- Case Report Tuberculosis of The Spine (Pott's Disease) Presenting As 'Compression Fractures'Документ5 страницCase Report Tuberculosis of The Spine (Pott's Disease) Presenting As 'Compression Fractures'tari_margonoОценок пока нет
- Medina - Miguel Andrei - SGD 2 - Altered Sensorium 2Документ3 страницыMedina - Miguel Andrei - SGD 2 - Altered Sensorium 2Miguel Andrei MedinaОценок пока нет
- Neuroscience AssignmentДокумент7 страницNeuroscience AssignmentAubrey Unique EvangelistaОценок пока нет
- Case Study: Spinal Cord Injury: Learning ObjectivesДокумент8 страницCase Study: Spinal Cord Injury: Learning ObjectivesMarius Clifford BilledoОценок пока нет
- Uillain Arré Yndrome: L A. M, MDДокумент4 страницыUillain Arré Yndrome: L A. M, MDYuriko AndreОценок пока нет
- Guillain Barré SyndromeДокумент21 страницаGuillain Barré SyndromebagusОценок пока нет
- Amyotrophic Lateral Sclerosis A.: Excellent History But Was This Copy-Pasted?Документ8 страницAmyotrophic Lateral Sclerosis A.: Excellent History But Was This Copy-Pasted?Allan CastroОценок пока нет
- Lambert Eaton SDДокумент6 страницLambert Eaton SDXavier Wong AchiОценок пока нет
- Renal Failure With Multisystem ProblemsДокумент7 страницRenal Failure With Multisystem Problemscammel ramosОценок пока нет
- Sydenham Chorea 2019Документ3 страницыSydenham Chorea 2019Hajrin PajriОценок пока нет
- A 19-Year-Old Man With Sickle Cell Disease Presenting With Spinal Infarction: A Case ReportДокумент6 страницA 19-Year-Old Man With Sickle Cell Disease Presenting With Spinal Infarction: A Case ReportJabber PaudacОценок пока нет
- 1 Neuro A) IIHДокумент3 страницы1 Neuro A) IIHLoren boidОценок пока нет
- Case of Celiac's Disease Mimicking ALSДокумент4 страницыCase of Celiac's Disease Mimicking ALSfakbikОценок пока нет
- P.helliwell@leeds - Ac.uk: AuthorsДокумент10 страницP.helliwell@leeds - Ac.uk: AuthorsWie SeptiaNiОценок пока нет
- Neurosyphilis: The Reemergence of An Historical DiseaseДокумент2 страницыNeurosyphilis: The Reemergence of An Historical DiseaseDrashua AshuaОценок пока нет
- Uremic NeuropathyДокумент10 страницUremic NeuropathyFecky Fihayatul IchsanОценок пока нет
- Pinocchio SyndromeДокумент1 страницаPinocchio SyndromeTakeshi ClairОценок пока нет
- Guillain-Barré SyndromeДокумент21 страницаGuillain-Barré SyndromeZulkarnainBustamamОценок пока нет
- Asbury - Assesment of Current Diagnostic Criteria For GBSДокумент4 страницыAsbury - Assesment of Current Diagnostic Criteria For GBSMarcelo BedoyaОценок пока нет
- Complex Regional Pain Syndrome: Ens Teaching ReviewДокумент8 страницComplex Regional Pain Syndrome: Ens Teaching ReviewDiego Agustin ZarzaОценок пока нет
- ACVKCДокумент9 страницACVKCDiego Agustin ZarzaОценок пока нет
- Distrofia SimpaticaДокумент11 страницDistrofia SimpaticaDiego Agustin ZarzaОценок пока нет
- Causal GiaДокумент7 страницCausal GiaDiego Agustin ZarzaОценок пока нет
- Ni Hms 394608Документ7 страницNi Hms 394608Diego Agustin ZarzaОценок пока нет
- CA ProstataДокумент23 страницыCA ProstataDiego Agustin ZarzaОценок пока нет
- Smoking Induces Oropharyngeal Narrowing and Increases The Severity of Obstructive Sleep Apnea Syndrome.Документ8 страницSmoking Induces Oropharyngeal Narrowing and Increases The Severity of Obstructive Sleep Apnea Syndrome.Diego Agustin ZarzaОценок пока нет
- Autism oДокумент2 страницыAutism oDiego Agustin ZarzaОценок пока нет
- FullRec2010 BMSbooklet enДокумент30 страницFullRec2010 BMSbooklet enDiego Agustin ZarzaОценок пока нет
- J Plast Reconstr Aesthet Surg. 2010 Nov 63 (11) 1761-8.Документ8 страницJ Plast Reconstr Aesthet Surg. 2010 Nov 63 (11) 1761-8.Diego Agustin ZarzaОценок пока нет
- Tarrega, Francisco - ValseДокумент2 страницыTarrega, Francisco - ValseDiego Agustin ZarzaОценок пока нет
- APNEAДокумент14 страницAPNEADiego Agustin ZarzaОценок пока нет
- ParkinsonДокумент36 страницParkinsonDiego Agustin ZarzaОценок пока нет
- ParkinsonДокумент36 страницParkinsonDiego Agustin ZarzaОценок пока нет
- ParkinsonДокумент36 страницParkinsonDiego Agustin ZarzaОценок пока нет
- Task 2 Engineering English (Redho Triwinoko, METO 5B)Документ3 страницыTask 2 Engineering English (Redho Triwinoko, METO 5B)Redho TriwinokoОценок пока нет
- Resmed Astral 150Документ93 страницыResmed Astral 150Lê Văn KhánhОценок пока нет
- Introduction To PsychiatryДокумент153 страницыIntroduction To Psychiatrybelayneh anteneh100% (1)
- Epilepsi 1Документ12 страницEpilepsi 1Ima SoniaОценок пока нет
- Pa Australian Guidelines On Adhd Draft PDFДокумент291 страницаPa Australian Guidelines On Adhd Draft PDFJonОценок пока нет
- Works CitedДокумент5 страницWorks Citedapi-507689477Оценок пока нет
- UnaniДокумент16 страницUnaniRahul Banik888Оценок пока нет
- The Complete CBT Guide For Depression and Low MoodДокумент642 страницыThe Complete CBT Guide For Depression and Low Moodalanbray115Оценок пока нет
- Amicus of ADHSДокумент35 страницAmicus of ADHScronkitenewsОценок пока нет
- Social Perspectives - Unit 10 - Task 1 - Copy 123Документ13 страницSocial Perspectives - Unit 10 - Task 1 - Copy 123zxko24Оценок пока нет
- Case 24-2022: A 31-Year-Old Man With Perianal and Penile Ulcers, Rectal Pain, and RashДокумент10 страницCase 24-2022: A 31-Year-Old Man With Perianal and Penile Ulcers, Rectal Pain, and RashCorina OanaОценок пока нет
- ETS & CapillaryДокумент6 страницETS & CapillaryRoela Marie AlbaniaОценок пока нет
- 2021 重症核心課程CRRT Dose and Prescription-NEW Ver1.0Документ63 страницы2021 重症核心課程CRRT Dose and Prescription-NEW Ver1.0Andy DazОценок пока нет
- Dataset On Child Vaccination in Brazil From 1996 To 2021: Data DescriptorДокумент9 страницDataset On Child Vaccination in Brazil From 1996 To 2021: Data DescriptorlaireneОценок пока нет
- HypertensionДокумент22 страницыHypertensionLubeeha HaselОценок пока нет
- Tuansi-Pa ManuscriptДокумент11 страницTuansi-Pa Manuscriptallkhusairy6tuansiОценок пока нет
- النسخه الثالثه نواف الحارثي ٢٠١٩Документ92 страницыالنسخه الثالثه نواف الحارثي ٢٠١٩Atheer AlsalehОценок пока нет
- Antimicrobial Stewardship Program (Ri)Документ50 страницAntimicrobial Stewardship Program (Ri)Erni Yessyca SimamoraОценок пока нет
- Sacubitril - Valsartan - WikipediaДокумент28 страницSacubitril - Valsartan - WikipediaSUBHADIPОценок пока нет
- Naomi Williams FindingsДокумент58 страницNaomi Williams Findingsscott.faulkner.taylorОценок пока нет
- Comparative Evaluation of Initial Crestal Bone Loss Around Dental Implants Using Flapless or Flap Method: An in Vivo StudyДокумент9 страницComparative Evaluation of Initial Crestal Bone Loss Around Dental Implants Using Flapless or Flap Method: An in Vivo StudyIJAR JOURNALОценок пока нет
- Deep Learning For Cardiovascularmedicine: A Practical PrimerДокумент16 страницDeep Learning For Cardiovascularmedicine: A Practical PrimersilviaОценок пока нет
- Stock Opname 2022Документ9 страницStock Opname 2022laboratorium rsitОценок пока нет
- Patients With Acid, High Fat and Low Protein Diet Have Higher Laryngopharyngeal Reflux Episodes at The Impedance PH MonitoringДокумент10 страницPatients With Acid, High Fat and Low Protein Diet Have Higher Laryngopharyngeal Reflux Episodes at The Impedance PH MonitoringLucien HaОценок пока нет
- Grape Seed Extract: Having A Potential Health BenefitsДокумент11 страницGrape Seed Extract: Having A Potential Health BenefitsGabriel GursenОценок пока нет
- 2019E 14 - Supportive Care and Managment of Side EffectsДокумент82 страницы2019E 14 - Supportive Care and Managment of Side Effectsrusgal8992Оценок пока нет
- Ebook Cohens Pathways of The Pulp 12Th Edition PDF Full Chapter PDFДокумент67 страницEbook Cohens Pathways of The Pulp 12Th Edition PDF Full Chapter PDFchristopher.jenkins207100% (27)
- ISBN Book Abstract ICONMIN 2020Документ91 страницаISBN Book Abstract ICONMIN 2020Lini Anisfatus SholihahОценок пока нет
- RF LatexДокумент1 страницаRF LatexDinesh SreedharanОценок пока нет
- Tle 7 - 8 - FisheryДокумент17 страницTle 7 - 8 - FisheryRey JavierОценок пока нет