Академический Документы
Профессиональный Документы
Культура Документы
Jurnal Periodontik Gilut
Загружено:
Sylvia Surya Dewi0 оценок0% нашли этот документ полезным (0 голосов)
22 просмотров4 страницыThis paper reports the treatment of multiple gingival recessions associated with shallow root caries. The success of the surgical approach was confirmed by the absence of tooth sensitivity and presence of gingival tissue with normal colour, texture and contour. After 12 months of follow-up, the clinical conditions were stable with satisfactory root coverage and periodontal health.
Исходное описание:
Оригинальное название
JURNAL PERIODONTIK GILUT
Авторское право
© © All Rights Reserved
Доступные форматы
PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документThis paper reports the treatment of multiple gingival recessions associated with shallow root caries. The success of the surgical approach was confirmed by the absence of tooth sensitivity and presence of gingival tissue with normal colour, texture and contour. After 12 months of follow-up, the clinical conditions were stable with satisfactory root coverage and periodontal health.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
22 просмотров4 страницыJurnal Periodontik Gilut
Загружено:
Sylvia Surya DewiThis paper reports the treatment of multiple gingival recessions associated with shallow root caries. The success of the surgical approach was confirmed by the absence of tooth sensitivity and presence of gingival tissue with normal colour, texture and contour. After 12 months of follow-up, the clinical conditions were stable with satisfactory root coverage and periodontal health.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 4
C a s e R e p o r t
Journal of Kathmandu Medical College, Vol. 1, No. 1, Issue 1, Jul.-Sep., 2012
29
Vol. 1 No. 1 Issue 1 Jul.-Sep. 2012 Journal of Kathmandu Medical College
Address for correspondence
Dr. Rita Singh
Oracare Periodontal Clinic
114, SamaMarg, Kamalpokhari,
Kathmandu
E-mail: s.rita2000@gmail.com
Treatment of gingival recession with coronally advanced
Flap - A case report
Singh R
1
1
Associate Professor, KMC BDS Programme, Kathmandu Medical College Teaching Hospital, Kathmandu, Nepal
Abstract
Extensive gingival recession associated with cervical abrasions is common. Several different surgical and/or restorative
therapies have been proposed to correct these lesions. This paper reports the treatment of multiple gingival recessions
associated with shallow root caries. The procedure involved utilization of coronally advanced ap. At the postoperative
follow-up visits, the success of the surgical approach was conrmed by the absence of tooth sensitivity and presence of
gingival tissue with normal colour, texture and contour. After 12 months of follow-up, the clinical conditions were stable
with satisfactory root coverage and periodontal health. An excellent aesthetical outcome was achieved and the patient
was satised with the outcome.
Key words: Coronally Advanced Flap, Gingival Recession, Root coverage
Introduction
G
ingival recession is dened as the displacement
of the soft tissue margin apical to the cemento
enamel junction
1
and is a frequent clinical feature in
populations with both good
2,3
and poor
4
standards
of oral hygiene. Toothbrush trauma is considered the
most common precipitating factor in initiation and
progression of non-inammatory, localized gingival
recession, and is associated with several variables
found to be erroneous and traumatic: tooth brushing
frequency
5
, use of hard bristle brushes
6
and brushing
technique
7
. Another important risk factor for gingival
recession is progressive plaque accumulation, which can
induce periodontal destruction. This normally causes
initial attachment loss as periodontal pockets, but can
also appear as initial gingival recession
8,9
.
Gingival recession can render patients aesthetically
conscious. Besides, it can cause tooth sensitivity, cervical
abrasion, and increased susceptibility to root caries and
leads to poor oral hygiene. This necessitates alleviation
of gingival recession in a predictable manner. Clinicians
are challenged to achieve outcomes that meet these
exacting standards, and therefore need a sound, clinically
oriented and scientically supported decision-making
process to plan the therapeutic approach, to predict
the outcome and, nally, to achieve it. The functional
aspects of root coverage may be controversial, but the
cosmetic aspect and satisfaction is not debatable.
Evidence shows that a coronally advanced ap alone
in many instances results in complete root coverage
and is stable over time
10
. A coronally advanced ap is
less invasive for the patient, requires less chair-time
and probably less surgical skill. It would therefore be
desirable to use a coronally advanced ap approach
when indicated. It has been hypothesized that a
coronally advanced ap approach alone could be
successfully applied when the residual gingiva is thick
11
and wide
12
, although existing evidence does not support
this hypothesis in full. It can be used in treating single or
multiple recession defects.
Case Report
A 35-year-old female was referred to periodontics
specialist complaining of the unaesthetic appearance
and tooth sensitivity of her maxillary front teeth. During
the clinical examination, it was noted that there were
multiple Millers class I
13
gingival recessions in teeth
numbers 11 and 21. Gingival recessions were associated
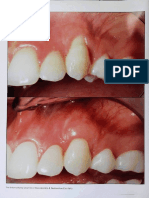
with cervical abrasions and root caries (Figures 1 and
2). The teeth presented shallow probing depth with
bleeding on probing.
30
Vol. 1 No. 1 Issue 1 Jul.-Sep. 2012 Journal of Kathmandu Medical College
Singh R
The patient was rst submitted to initial preparation
comprising scaling, root planing and oral hygiene
instructions. After 10 days, she was scheduled for root
coverage procedure with coronally advanced ap.
This was the technique chosen as she demonstrated
more than 3 mm of attached gingiva and thick gingival
biotype.
After antisepsis and anaesthesia, an intrasulcular
incision was made with a surgical blade on the buccal
aspect of the involved teeth. Two oblique vertical
releasing incisions were made lateral to the recession
defects starting at a point apical to the interdental
papillae extending into the alveolar mucosa. The
distance between the coronal extension of the vertical
incision and the crest of the interdental papillae
was approximately equal to the anticipated coronal
displacement of the ap, to minimize tissue overlapping
in the interdental area. A trapezoidal mucoperiosteal
ap was raised 1 to 2 mm apical to the crest of the
bone to expose the dehiscence. Then a partial thickness
dissection was carried out apically from this level leaving
the underlying periosteum in place. A mesiodistal and
apical dissection parallel to the vestibular lining mucosa
was performed to release residual muscle tension and
facilitate the passive coronal displacement of the ap.
The papillae were de-epithelialized and the ap then
displaced at least 1 mm coronal to the cemento-enamel
junction. The root caries were excavated using a spoon
excavator (gure 3).
Suturing of oblique releasing incision was performed
with 4-0 silk sutures as described by Allen and Miller
14
in
an apico-coronal direction before suturing the papillae.
This allowed for positioning of the gingiva without
tension. Additional interrupted sutures were placed
to close the oblique releasing incisions in the alveolar
mucosa. The coronal, mesial and distal extremities ties
of the ap were secured with two single sutures placed
in the interdental areas (Fig 4). Tin foil and periodontal
dressing were placed over the sites.
After surgery, the patient received pain relieving
medication (Ibuprofen 400mg every 6 hours) when
needed, antibiotic (Amoxicillin 500 mg every 8 hours for 7
days) and chemical plaque control (0.12% Chlorhexidine
gluconate rinse - every 12 hours for 14 days). The pack
and sutures were removed after 10 days. Three weeks
after surgery, she was instructed to resume mechanical
tooth cleaning using a soft toothbrush and a careful roll-
technique. She was called for follow up weekly for four
weeks, once a month for 3 months and once every 3
months up to 12 months.
Complete root coverage was obtained and the results
were maintained. The patient reported to be completely
satised with the aesthetical outcome. Her tooth
sensitivity was also totally abolished. At 6 (g 5) and
12 months (Fig 6) after the procedure, the periodontal
tissues presented normal colour, texture and contouring.
Discussion
The amount and thickness of keratinized tissue is
generally thought to inuence the outcome of root
coverage: thick tissues and large amounts of residual
keratinized tissue are perceived as favourable. Many
clinicians select a coronally advanced ap or a sliding ap
when the residual keratinized tissue is well represented,
or place a graft under the ap when keratinized tissue is
insufcient in thickness and width
15
. However, there is
limited evidence to support this approach.
A clinical study
11
tested the inuence of ap thickness
following coronally advanced ap procedures. The results
indicate that ap thickness is signicantly (P < 0.0001)
associated with root coverage. A ap thickness of
Fig. 1 and 2: Gingival recessions on maxillary central incisors associated with root abrasions and caries.
31
Vol. 1 No. 1 Issue 1 Jul.-Sep. 2012 Journal of Kathmandu Medical College
Treatment of gingival recession with coronally advanced Flap - A case report
>0.8 mm was associated with complete root coverage,
while a ap thickness of <0.8 mm was associated with
partial root coverage. In addition, linear regression
analysis showed that with each increase in thickness
of 0.1 mm, recession was reduced by approximately
0.2 mm in all treated sites. Therefore, 0.8 mm can be
considered as the critical ap thickness above which
the expected clinical outcome should be complete root
coverage when using a coronally advanced ap alone.
Another study
12
evaluated the relationship between
root coverage and baseline amount of keratinized
tissue in laterally positioned and coronally advanced
aps. Multiple logistic regression analysis showed a
statistically signicant relationship between complete
root coverage and the amount of keratinized tissue
lateral to the gingival defects: the greater the amount
of keratinized tissue, the greater the percentage of root
coverage.
Many studies and recent systematic reviews showed the
importance of baseline recession depth in the treatment
outcome. The results of the meta-analyses of controlled
and randomized clinical trials published by Roccuzzo
et al.
16
and Clauser et al.
17
showed a relationship between
the initial recession depth and the nal outcome of the
surgical procedure, reporting that greater baseline
recession depths were always associated with decreased
complete root coverage.
Following coronally advanced ap therapy of single
recession defects, Pini Prato et al.
18
reported that the
gingival margin, sutured, on average, 1 mm coronal to
the cementoenamel junction, remained stable at week
1, but shifted apically from weeks 2 to 4, uncovering
the cementoenamel junction in 60% of the sites with
an average shift of 1.5 0.6 mm. From week 4 to week
12 after the procedure, the gingival margin remained
stable.
Coronally advanced ap can be utilized when indicated.
Unfortunately, the key information to be able to
forecast when coronally advanced ap will be successful
is still missing. Many experts support the hypothesis
Fig. 3: Flap reected and root caries excavated
Fig. 4: Coronally advanced ap on gingival recessions. The
trapezoidal ap has been sutured coronally to the
cementoenamel junction.
Fig 5: The 6 months clinical outcome. Fig. 6: The 12 months clinical outcome.
32
Vol. 1 No. 1 Issue 1 Jul.-Sep. 2012 Journal of Kathmandu Medical College
Singh R
that therapy with coronally advanced ap alone can be
successfully applied when the residual gingiva is thick
and wide. Accordingly, the adjunctive use of a graft
could be restricted to sites with thin and narrow residual
gingiva. A potential alternative is the use of enamel
matrix derivative.
Conclusions
This case report indicates that teeth with multiple
gingival recessions, associated with shallow root caries
can be successfully treated by the coronally advanced
ap. When used in indicated cases, this root coverage
technique is less invasive for the patient, requires less
chair-time and less surgical skill.
References
1. American Academy of Periodontology. Glossary of
periodontal terms. 3rd ed. Chicago: The American
Academy of Periodontology; 1992.
2. Le H, Anerud A, Boysen H. The natural history of
periodontal disease in man: prevalence, severity,
and extent of gingival recession. J Periodontol.
1992;63:48995.
3. Serino G, Wennstrm JL, Lindhe J, Eneroth L. The
prevalence and distribution of gingival recession in
subjects with a high standard of oral hygiene. J Clin
Periodontol.1994;21:5763.
4. Baelum V, Fejerskov O, Karring T. Oral hygiene,
gingivitis and periodontal breakdown in adult
Tanzanians. J Periodontal Res. 1986;21:22132.
5. Vehkalahti M. Occurrence of gingival recession in
adults. J Periodontol. 1989;60:599603.
6. Khocht A, Simon G, Person P, Denepitiya JL. Gingival
recession in relation to history of hard toothbrush
use. J Periodontol.1993;64:9005.
7. Checchi L, Daprile G, Gatto MR,Pelliccioni GA.
Gingival recession and toothbrushing in an
Italian school of dentistry: a pilot study. J Clin
Periodontol.1999;26:27680.
8. Yoneyama T, Okamoto H, Lindhe J, Socransky
SS, Haffajee AD. Probing depth, attachment
loss and gingival recession:ndings from a
clinical examination in Ushiku, Japan. J Clin
Periodontol.1988;15:58191.
9. Heitz-Mayeld LJA, Schtzle M, Le H, Brgin W,
Anerud A, Boysen H, Lang NP. Clinical course of
chronic periodontitis II. Incidence, characteristics
and time of occurrence of the initial periodontal
lesion. J Clin Periodontol. 2003;30:9028.
10. Cairo F, Pagliaro U, Nieri M.Treatment of gingival
recession with coronally advanced ap procedures: a
systematic review. J Clin Periodontol. 2008;35:136-62.
11. Baldi C, Pini Prato GP, Pagliaro U, Nieri M, Saletta
D, Muzzi L, Cortellini P. Coronally advanced ap
procedure for root coverage. Is ap thickness a
relevant predictor to achieve root coverage? A 19-
case series. J Periodontol. 1999;70:107784.
12. Zucchelli G, Cesari C, Amore C, Montebugnoli L, De
Sanctis M. Laterally moved, coronally advanced ap:
a modied surgical approach for isolated recession-
type defects. J Periodontol. 2004:75:173441.
13. Miller PD Jr. A classication of marginal tissue
recession. Int J Periodontotics Restorative Dent.
1985;5:813.
14. Allen EP, Miller PD. Coronal positioning of existing
gingiva: short term results in the treatment of
shallow marginal tissue recession. J Periodontol.
1989:60:3169.
15. Wennstrm JL, Zucchelli G. Increased gingival
dimensions. A signicant factor for successful
outcome of root coverage procedures? A 2-year
prospective clinical study. J Clin Periodontol.
1996;23:7707.
16. Roccuzzo M, Bunino M, Needleman I, Sanz M.
Periodontal plastic surgery for treatment of localized
gingival recessions: a systematic review. J Clin
Periodontol. 2002;29:17894.
17. Clauser C, Nieri M, Franceschi D, Pagliaro U, Pini
Prato GP. Evidence-based mucogingival therapy.
Part 2: Ordinary and individual patient data meta-
analyses of surgical treatment of recession using
complete root coverage as the outcome variable. J
Periodontol. 2003;74:74156.
18. Pini Prato GP, Baldi C, Pagliaro U, Nieri M, Saletta
D, Rotundo R, Cortellini P. Coronally advanced ap
procedure for root coverage. Treatment of root
surface: root planing versus polishing. J Periodontol.
1999;70:106476.
Вам также может понравиться
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Essential Quick Review PERIODONTICSДокумент258 страницEssential Quick Review PERIODONTICSJude Aldo Paul100% (2)
- INBDEBooster Periodontics NotesДокумент28 страницINBDEBooster Periodontics NotesShawqi A100% (1)
- Adult Orthodontics SeminarДокумент52 страницыAdult Orthodontics Seminaravanthika krishnaraj100% (2)
- Failures in FPDДокумент45 страницFailures in FPDdr rolly agarwal100% (1)
- Essentials of Dentistry Quik Review and Examination Preparation PDFДокумент327 страницEssentials of Dentistry Quik Review and Examination Preparation PDFpatriciatarauОценок пока нет
- Incisions and FlapsДокумент22 страницыIncisions and FlapsDrDevyani100% (1)
- Ceramic Laminate Veneers: Clinical Procedures With A Multidisciplinary ApproachДокумент23 страницыCeramic Laminate Veneers: Clinical Procedures With A Multidisciplinary ApproachBenjiОценок пока нет
- Oet Listening and Reading GuideДокумент182 страницыOet Listening and Reading Guide121456985% (53)
- Banding in OrthodonticsДокумент22 страницыBanding in OrthodonticsJessamine de Jesus0% (1)
- Crown Lengthening Procedures - A Review ArticleДокумент11 страницCrown Lengthening Procedures - A Review ArticleIOSRjournalОценок пока нет
- Recurrent Gingival Cyst of Adult: A Rare Case Report With Review of LiteratureДокумент5 страницRecurrent Gingival Cyst of Adult: A Rare Case Report With Review of Literaturesayantan karmakarОценок пока нет
- Bruxism in ChildrenДокумент6 страницBruxism in ChildrenMuhammad Shakeel KhawajaОценок пока нет
- Avulsi Gigi AnkДокумент4 страницыAvulsi Gigi AnkSylvia Surya DewiОценок пока нет
- 528 4099 1 PBДокумент3 страницы528 4099 1 PBSylvia Surya DewiОценок пока нет
- 1 PBДокумент3 страницы1 PBSylvia Surya DewiОценок пока нет
- Neonatal CystДокумент4 страницыNeonatal CystSylvia Surya DewiОценок пока нет
- Target Mds Aiims Mock PDFДокумент22 страницыTarget Mds Aiims Mock PDFReddyОценок пока нет
- ImplantsДокумент132 страницыImplantsDr Fahad and Associates Medical and dental clinicОценок пока нет
- 5Документ86 страниц5Georgi GugicevОценок пока нет
- Nterior Estorations: Choose A Job You Love and You Will Never Have To Work A Day in Your LifeДокумент20 страницNterior Estorations: Choose A Job You Love and You Will Never Have To Work A Day in Your LifeABОценок пока нет
- Apostilaem InglesДокумент6 страницApostilaem InglesricardoОценок пока нет
- Care Plan Template CompleteДокумент6 страницCare Plan Template Completeapi-643737824Оценок пока нет
- Dentonic: Product DescriptionДокумент8 страницDentonic: Product DescriptionSameer ShafqatОценок пока нет
- Nutrition and DiseaseДокумент3 страницыNutrition and DiseaseAhmad SyahrirОценок пока нет
- Medical Vocabulary HospitalДокумент27 страницMedical Vocabulary HospitalTeodor PopОценок пока нет
- (13C) The Role of Dental Calculus and Other Local Predisposing FactorsДокумент9 страниц(13C) The Role of Dental Calculus and Other Local Predisposing FactorsNegrus StefanОценок пока нет
- Comma Incision For Impacted Mandibular Third MolarsДокумент4 страницыComma Incision For Impacted Mandibular Third MolarsSukhvinder Singh RanaОценок пока нет
- Andrew 1994Документ15 страницAndrew 1994Néia CostaОценок пока нет
- Archive of SID: Bluish Discoloration of Periodontal TissueДокумент3 страницыArchive of SID: Bluish Discoloration of Periodontal TissueApurava SinghОценок пока нет
- Paramjit Kaur - Oral Cavity of NeonatesДокумент27 страницParamjit Kaur - Oral Cavity of Neonatesdr parveen bathlaОценок пока нет
- Assessing Periodontal DiseaseДокумент4 страницыAssessing Periodontal Diseaseمؤمل رياض سعد كاظمОценок пока нет
- Fibroma FibrosarkomaДокумент24 страницыFibroma FibrosarkomanadaprahastiwiОценок пока нет
- PPD July Top Tip - Cervical MatrixДокумент2 страницыPPD July Top Tip - Cervical MatrixCarolyn WilkinsonОценок пока нет
- Clinical Evaluation of Removable Partial Dentures On The Periodontal Health of Abutment Teeth: A Retrospective StudyДокумент8 страницClinical Evaluation of Removable Partial Dentures On The Periodontal Health of Abutment Teeth: A Retrospective StudyEduard Gabriel GavrilăОценок пока нет
- ASSESSING MOUTH, THROAT, NOSE and SINUSESДокумент13 страницASSESSING MOUTH, THROAT, NOSE and SINUSESKenneth Andre Batuyog TecsonОценок пока нет