Академический Документы
Профессиональный Документы
Культура Документы
Ludwig's Angina
Загружено:
Kenny Jap0 оценок0% нашли этот документ полезным (0 голосов)
43 просмотров7 страницalgoritma diagnosa ludwig's angina
Оригинальное название
ludwig's angina
Авторское право
© © All Rights Reserved
Доступные форматы
PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документalgoritma diagnosa ludwig's angina
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
43 просмотров7 страницLudwig's Angina
Загружено:
Kenny Japalgoritma diagnosa ludwig's angina
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 7
rare disorder, Ludwigs angina is a serious,
potentially life-threatening infection of the
neck and the floor of the mouth (Table 1).
Originally described by Wilhelm Frederick
von Ludwig in 1836,
1
this condition is notorious for its
aggressiveness, rapid progression to air way compro-
mise, and high mortality when not treated promptly.
26
This article discusses the pathophysiology, clinical man-
ifestations, diagnosis, and treatment of this dangerous
condition. Two cases are described to illustrate typical
presentations of the disorder.
I LLUSTRATI VE CASE PRESENTATI ONS
Pat i ent 1
A 39-year -old man with type 1 diabetes mellitus
comes to the emergency department reporting a 3-day
histor y of fever, chills, and facial swelling. He also
reports difficulty swallowing. Examination shows an
acutely ill -appearing man with evident facial edema
but no acute respiratory distress (Figure 1).
Vital signs include an oral temperature of 38.7C
(101.7F), a heart rate of 140 bpm, and a respiratory
rate of 18 breaths/min. Examination of the oral cavity
reveals numerous carious teeth, dry oral mucosae, and
woody, tender edema of the floor of the mouth and
anterior neck. Plain radiographs of the neck show evi-
dence of gas in the soft tissues (Figure 2), a finding
that is confirmed by a computed tomography (CT)
scan (Figure 3). Leukocyte count is 36 10
3
/mm
3
, and
anion gap measurement indicates metabolic acidosis.
After stabilization by administration of intravenous
fluids and antibiotic agents, the patient is transferred
to the operating room, where a formal tracheostomy is
performed. An additional drainage procedure is later
performed because of an infected fluid collection, and
complete dental extraction is also necessary.
Pat i ent 2
A 53-year -old woman with type 1 diabetes mellitus
reports a 2-day history of a worsening sore throat that
has resulted in an inability to swallow her saliva. She
has a productive cough and says that her face has
become swollen from her neck to the lower part of
her ears, bilaterally. The patient sits upright with her
mouth open and her tongue protruding slightly (Fig-
ure 4).
Vital signs include an oral temperature of 37.1C
(98.8F), a pulse of 110 bpm, and a respiratory rate of
24 breaths/min. Physical examination reveals no respira-
tory distress. Oral examination reveals a foul breath
odor, trismus, and a brawny submandibular swelling that
elevates the tongue. Examination of the lungs reveals
ri ght posteri or ral es. Resul ts of l aborator y testi ng
include a leukocyte count of 17,500 10
3
/mm
3
, a serum
glucose level of 285 mg/dL, and a serum bicarbonate
level within normal limits. Radiographs of the soft tissue
of the neck show supraglottic edema (Figure 5), and a
CT scan confirms supraglottitis and soft-tissue gas
(Figure 6). A chest radiograph shows a right-sided infil-
trate, consistent with aspiration pneumonitis (Figure 7).
The patient receives antibiotics, intravenously, and
is transferred to the operating room for fiberoptically
guided orotracheal intubation. However, intubation is
unsuccessful because of airway distortion. A surgical
airway is then established.
PATHOPHYSI OLOGY
Ludwigs angina is a rapidly progressing polymicro-
bial cellulitis of the sublingual and submandibular
spaces that can result in life-threatening airway com-
promise. The bacteriology of Ludwigs angina is poly-
microbial and predominantly involves the oral flora.
The organisms most often isolated in patients with the
disorder are Streptococcus viridans and Staphylococcus
aureus. Anaerobes also are frequently involved, includ-
ing bacteroides, peptostreptococci, and peptococci.
Other gram-positive bacteria that have been isolated
include Fusobacteriumnucleatum, Aerobacter aeruginosa,
spirochetes, and Veillonella, Candida, Eubacteria, and
Clostridiumspecies. Gram-negative organisms that have
been isolated include Neisseria species, Escherichia coli,
Pseudomonas speci es, Haemophilus influenzae, and
Klebsiellaspecies.
A
Dr. Lemonick is a Clinical Instructor, Affiliated Residencyin Emergency
Medicine, University of Pittsburgh; and an Attending Emergency
Physician, TheWestern Pennsylvania Hospital, Pittsburgh, PA.
www.turner-white.com Hospital Physician July 2002 31
Cl i ni cal Revi ew Ar t i cl e
Ludwigs Angina: Diagnosis and Treatment
David M. Lemonick, MD
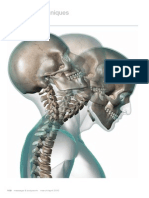
ANATOMY
In order to appreciate the potential of this infection
to spread from the floor of the mouth to the neck and
mediastinal structures, a brief review of the involved
anatomy is helpful (Figure 8). The submandibular space
comprises part of the space above the hyoid bone. The
total space is divided into the sublingual space superiorly
and submandibular space inferiorly. The former, locat-
ed between the geniohyoid and mylohyoid muscles, and
the latter, located between the mylohyoid muscle and
the superficial fascia and skin, communicate around the
free posterior border of the mylohyoid muscle.
Once established in the submandibular space, the
infection can then spread to adjacent structures. Typ-
ically affected structures, in order of most frequent
contamination, are the anterior neck, the pharyngo-
maxillary space, the retropharynx, and the superior
mediastinum.
EPI DEMI OLOGY
Most cases of Ludwigs angina occur in previously
healthy persons. Predisposing conditions include dia-
betes mellitus, neutropenia, alcoholism, aplastic anemia,
glomerulonephritis, dermatomyositis, and systemic
lupus erythematosus (Table 2). Most affected patients
are between age 20 and 60 years, although an age range
from 12 days to 84 years has been reported.
6
There is a
male predominance (3:1 to 4:1)
6
of the disorder.
ETI OLOGY
Ludwigs angina usually originates from an odonto-
genic infection, especially from the second or third
lower molars. These teeth have roots that lie at the
level of the mylohyoid muscle, and abscesses here can
spread to the submandibular space. Other less com-
monly reported causes of Ludwigs angina include
sialadenitis, peritonsillar abscess, open mandibular
fracture, infected thyroglossal duct cyst, epiglottitis,
intravenous injections of drugs into the neck, traumat-
ic bronchoscopy, endotracheal intubation, oral lacera-
tions, tongue piercing, upper respiratory infections,
and trauma to the floor of the mouth.
Ludwigs angina can be thought of as a cellulitis of
the submandibular space that spreads to the structures
of the anterior neck and beyond via connective tissue,
muscle, and fascial planes rather than by the lymphatic
system. For this reason, adenopathy is not associated
with the disorder. Cellulitis, rather than abscess forma-
tion, is the most common early presenting finding. As
the infection progresses, edema of the suprahyoid tis-
sues and supraglottic larynx elevate and posteriorly dis-
place the tongue, resulting in life-threatening airway
narrowing. I n advanced infection, cavernous sinus
thrombosis and brain abscess, in addition to air way
compromise, have been described. Other reported
compl i cati ons of Ludwi gs angi na i ncl ude caroti d
sheath infection and arterial rupture, suppurative
thrombophlebitis of the internal jugular vein, medias-
tinitis, empyema, pericardial and/or pleural effusion,
osteomyelitis of the mandible, subphrenic abscess, and
aspiration pneumonia.
5,710
CLI NI CAL MANI FESTATI ONS
Patients with Ludwigs angina typically have a history
of recent dental extraction or of poor oral hygiene and
dental pain. Clinical findings are consistent with sepsis
and include fever, tachypnea, and tachycardia. Patients
may be anxious, agitated, and confused. Their symptoms
32 Hospital Physician July 2002 www.turner-white.com
L emoni ck : L udwi g s A ngi na : pp. 31 37
Table 1. Clinical Pearls Concerning Ludwigs Angina
Ludwigs angina is rare and sometimes fatal.
Morbidity and mortality primarily result from airway compro-
mise from swelling.
Etiology usually involves an odontogenic infection.
Streptococci and staphylococci are the most common bacte-
ria associated with Ludwigs angina.
Early recognition, prompt airway control, and antibiotic
administration are the keys to optimum outcome.
Early consultation with an anesthesiologist and an ear-nose-
throat surgeon are strongly encouraged.
Figure 1. Appearance of patient 1.
can include swelling and pain in the floor of the mouth
and anterior neck, fever, dysphagia, odynophagia, drool-
ing, trismus, toothache, and fetid breath. Hoarseness,
stridor, respiratory distress, decreased air movement,
cyanosis, and a sniffing position (ie, the characteristic
posture assumed by patients with impending upper air-
way compromise consisting of an upright posture with
the neck thrust forward and the chin elevated) are all
signs of impending air way catastrophe. Patients may
exhibit dysphonia. More specifically, they may have a
muffled tone at higher registers (ie, a hot potato voice)
caused by edema of the vocal apparatus; this finding
should be a warning to clinicians of potentially severe air-
way compromise.
On oral examination, elevation of the tongue, woody,
brawny induration of the floor of the mouth and anteri-
or neck, and nonfluctuant suprahyoid swelling typify the
di sease process. There i s typi cal l y a bi l ateral sub-
mandibular edema, with marked tenderness on palpa-
tion and, occasionally, subcutaneous emphysema. The
swelling of the anterior soft tissues of the neck above the
hyoid bone sometimes leads to the characteristic bulls
neck appearance of affected patients. Adenopathy and
fluctuance are not usually seen in patients with Ludwigs
angina.
DI AGNOSI S
Awareness and recogni ti on of the possi bi l i ty of
Ludwigs angina is the first and most essential step in
the diagnosis and management of this serious condi-
tion. There are 4 cardinal signs of Ludwigs angina:
(1) bilateral involvement of more than a single deep-
tissue space; (2) gangrene with serosanguinous, putrid
infiltration but little or no frank pus; (3) involvement
of connective tissue, fasciae, and muscles but not glan-
dular structures; and (4) spread via fascial space conti-
nuity rather than by the lymphatic system.
6,9
The pres-
ence of brawny induration of the floor of the mouth in
a suggestive clinical presentation should prompt the
clinician to move rapidly toward air way stabilization
first, followed by further diagnostic confirmation. Un-
necessary perturbation of the patient, such as forcing
him or her into a supine position or prematurely at-
tempting endotracheal intubation, might result in
laryngospasm and complete upper airway obstruction
and thus should be avoided.
Plain radiographs of the neck and chest often show
soft-tissue swelling, the presence of gas, and the extent of
airway narrowing. Sonography has been used to identify
fluid collections in the soft tissues, as has gallium citrate
L emoni ck : L udwi g s A ngi na : pp. 31 37
www.turner-white.com Hospital Physician July 2002 33
Figure 3. Computed tomography scan of patient 1.
Figure 2. Soft-tissue radiograph of patient 1 showing the
presence of gas (arrow).
Ga-67 scanning. Panoramic radiographic views of the jaw
may show a dental focus of infection. After the airway
patency is assured, CT scanning is a valuable modality to
show the extent of soft-tissue swelling, the presence of
gas, fluid collection, and airway compromise. Magnetic
resonance imaging is another elegant modality that can
be considered in some patients.
6
The differential diagnosis of Ludwigs angina in-
cludes angioneurotic edema, lingual carcinoma, sub-
lingual hematoma (following anticoagulation), salivary
gland abscess, lymphadenitis, cellulitis, and peritonsil-
lar abscess (Table 3).
MANAGEMENT
A suggested algorithm for the diagnosis and manage-
ment of Ludwigs angina is provided in Figure 9. Be-
cause morbidity and mortality in Ludwigs angina are
primarily related to loss of airway patency, protection of
the airway takes highest priority in the initial manage-
ment of affected patients. Early consultation with an
anesthesiologist and an otolaryngologist is prudent, and
transfer of the patient to the operating room should be
strongly considered before manipulation of the airway
begins. Patients who do not require immediate airway
34 Hospital Physician July 2002 www.turner-white.com
L emoni ck : L udwi g s A ngi na : pp. 31 37
Figure 4. Appearance of patient 2.
Figure 5. Soft-tissue radiograph of patient 2 showing supra-
glottic swelling (arrow).
Figure 6. Computed tomography scan of patient 2, showing
supraglottitis and soft-tissue gas (arrow).
control should receive continuous monitoring for signs
of impending respiratory distress.
For those patients who are in more immediate jeop-
ardy, airway control is ideally achieved in the operating
room, with surgical backup available, for performance
of cricothyroidotomy or formal tracheostomy, if neces-
sary. Endotracheal intubation of these patients can be
difficult, and direct laryngoscopy may even precipitate
the loss of the airway. Awake fiberoptic intubation is an
attractive alternative and should be considered when
the degree of airway narrowing is severe. Blind naso-
tracheal intubation should be avoided because of the
degree of airway distortion and because resulting trau-
ma may further narrow an already tenuous airway or
cause bleeding or rupture of an abscess.
When severe swelling or trismus prevents orotra-
cheal intubation, formal tracheostomy remains the
gold standard for securing the airway. This procedure
is frequently complicated by extensive soft-tissue swel-
ling of the anterior neck, and it risks spreading the
infection to the mediastinum. In the setting of immi-
nent loss of the airway, however, clinicians must not
hesitate to attempt orotracheal intubation or needle or
surgical cricothyroidotomy, even if conditions are sub-
optimal. Administration of nebulized epinephrine has
been suggested as a possible adjunct prior to airway
mani pul ati on, when ti me al l ows, i n an attempt to
reduce mucosal swelling.
Once the airway is secured, aggressive intravenous
admi ni strati on of anti bi oti c agents shoul d begi n
(Table 4). Initial treatment is targeted at gram-positive
organisms and anaerobes in the oral cavity. Adminis-
tration of several antibiotic agents has been proposed,
including high-dose penicillin G plus metronidazole,
L emoni ck : L udwi g s A ngi na : pp. 31 37
www.turner-white.com Hospital Physician July 2002 35
Figure 7. Chest radiograph of patient 2 showing a right-sided
infiltrate.
Table 2. Predisposing Conditions in Cases of Ludwigs
Angina*
Diabetes
Neutropenia
Alcoholism
Aplastic anemia
Glomerulonephritis
Dermatomyositis
Systemic lupus erythematosus
*Entries are listed in order of decreasingfrequency.
Table 3. Differential Diagnosis in Cases of Ludwigs
Angina
Angioneurotic edema
Cellulitis
Lingual carcinoma
Lymphadenitis
Peritonsillar abscess
Salivary gland abscess
Sublingual hematoma
Supramylohyoid
portion of
submandibular
space
Mylohyoid muscle
Inframylohyoid
portion of
submandibular space
Sublingual gland
Tongue
Submandibular
gland
Digastric muscle (anterior belly)
Figure 8. Anatomy of the mandibular space. (Adapted from
Hartmann RW Jr. Ludwigs angina in children. Am Fam
Physician 1999;60:10912. Used with permission of Steve Oh.)
36 Hospital Physician July 2002 www.turner-white.com
L emoni ck : L udwi g s A ngi na : pp. 31 37
Figure 9. A suggested algorithm for the diagnosis and management of Ludwigs angina.
Successful
Unsuccessful
Intensive care unit
Suspicion of Ludwigs angina
(eg, presence of severe pain, neck swelling,
dysphagia, dental pain/extraction)
Rapid airway assessment
Airway loss imminent
(eg, presence of respiratory
distress, anxiety, cyanosis,
stridor, sniffing-position,
retractions)
Establish airway: use sedation-
assisted orotracheal intuba-
tion or fiberoptic intubation
(either oro- or nasotracheal).
Airway compromise
(eg, presence of nuchal rigidi-
ty, drooling, muffled, voice,
trismus, tongue elevation)
No immediate airway threat
(eg, presence of mild swelling,
but no distress)
Cricothyroidotomy
(needle, open procedure),
tracheostomy
Administer antibiotics, intra-
venously (consider giving
corticosteroids).
Imaging studies
(eg, plain radiographs of the
soft tissues of the neck, pano-
ramic radiographs, computed
tomography scans)
Consider the need for surgical
drainage (if fluctuance, gas in
the soft tissues, persistent
sepsis, or a purulent needle
aspirate is present; remove
infected teeth).
Consider nebulized epinephrine.
cl i ndamyci n, cefoxi ti n, pi peraci l l i n -tazobactam,
amoxicillin-clavulanate, and ticarcillin-clavulanate. Al-
though controversial, the use of dexamethasone to
decrease edema and to improve antibiotic penetration
has received some support.
Surgical drainage is indicated when there is suppu-
rative infection, radiologic evidence of fluid collection
or soft-tissue air, clinical fluctuance, crepitus, or a pur-
ulent needle aspirate. Drainage is also indicated when
there is no clinical improvement after an initial course
of antibiotic therapy. Removal of infected teeth is also
essential to complete the drainage process.
The prognosis in Ludwigs angina depends primari-
ly on immediate protection of the airway and then on
prompt antibioticand possibly surgicaltreatment
of the infection. Mortality in the preantibiotic era was
50% but, with the advent of current therapies, has de-
clined to less than 5%.
7,8,10
CONCLUSI ON
Ludwigs angina is a dramatic, life-threatening, soft-
tissue infection of the floor of the mouth and neck. If
vigilant for its clinical presentation and aware of its
potential for rapid compromise of the patients airway,
clinicians can intervene early in order to prevent its
most dire consequences.
Air way control is of paramount importance, and
attention to this consideration, combined with antibiotic
therapy, surgical drainage, and modern intensive care,
have all contributed to a declining mortality. Early and
liberal consultation with otolaryngology and anesthesiol-
ogy services will assure the greatest hope for speedy air-
way control, prompt institution of intravenous antibiotic
therapy, and an uncomplicated recovery from this rare
and dreaded condition. HP
REFERENCES
1. Murphy SC. The person behind the eponym: Wilhelm
Frederick von Ludwig (1790-1865). J Oral Pathol Med
1996;25:5135.
2. Kurien M, Mathew J, Job A, Zachariah N. Ludwigs angi-
na. Clin Otolaryngol 1997;22:2635.
3. Marple BF. Ludwig angina: a review of current airway
management. Arch Otolaryngol Head Neck Surg 1999;
125:5969.
4. Neff SP, Merry AF, Anderson B. Airway management in
Ludwi gs angi na. Anaesth I ntensi ve Care 1999;27:
65961.
5. Barakate MS, Jensen MJ, Heml i JM, Graham AR.
Ludwigs angina: report of a case and review of manage-
ment issues. Ann Otol Rhinol Laryngol 2001;110(5 Pt 1):
4536.
6. Nguyen VD, Potter JL, Hersh-Schick MR. Ludwig angi-
na: an uncommon and potentially lethal neck infection.
AJNR Am J Neuroradiol 1992;13:2159.
7. Moreland LW, Corey J, McKenzie R. Ludwigs angina.
Report of a case and review of the literature. Arch Intern
Med 1988;148:4616.
8. Spitalnic SJ, Sucov A. Ludwigs angina: case report and
review. J Emerg Med 1995;13:499503.
9. Weiss L, Finkelstein JA, Storrow AB. Fever and neck pain.
Ludwigs angina. Acad Emerg Med 1995;2:835,8434.
10. Ferrera PC, Busino LJ, Snyder HS. Uncommon compli-
cations of odontogenic infections. Am J Emerg Med
1996;14:31722.
SUGGESTED READI NG
Blackburn P. Ludwigs angina. I n: Rosen P, Barkin RM,
Hayden SR, et al, editors. The 5-minute emergency medicine
consul t. Phi l adel phi a: Li ppi ncott Wi l l i ams and Wi l ki ns;
1999:6501.
Bramwel l KJ, Davi s DP. Ludwi gs angi na. J Emerg Med
1998;16:481.
Busch RF, Shah D. Ludwigs angina: improved treatment.
Otolaryngol Head Neck Surg 1997;117:S1725.
Furst IM, Ersil P, Caminiti M. A rare complication of tooth
abscessLudwigs angina and mediastinitis. J Can Dent
Assoc 2001;67:3247.
Hartmann RW Jr. Ludwigs angina in children. Am Fam
Physician 1999;60:10912.
Liu RS, Chu YK, Chu LS, et al. Ga-67 scan in the diagnosis and
monitoring of Ludwigs angina. Clin Nucl Med 2001;26:7334.
Pynn BR, Sands T. Ludwigs angina. Ann Emerg Med 1997;
30:713.
L emoni ck : L udwi g s A ngi na : pp. 31 37
www.turner-white.com Hospital Physician July 2002 37
Table 4. Commonly Used Antibiotic Agents in Cases
of Ludwigs Angina
Ampicillin/sulbactam
Cefoxitin
Clindamycin*
Gentamicin
Penicillin G plus metronidazole
Piperacillin/tazobactam
Ticarcillin/clavulanate
*Administer if patient is allergic to penicillin.
Copyright 2002 by Turner White Communications Inc., Wayne, PA. All rights reserved.
Вам также может понравиться
- What Is The Best Way To Treat Tinea Cruris?: Clinical InquiriesДокумент4 страницыWhat Is The Best Way To Treat Tinea Cruris?: Clinical InquiriesKenny JapОценок пока нет
- Laporan PBL 3 Lansia: Universitas Katolik Atma Jaya Fakultas Kedokteran 2010Документ2 страницыLaporan PBL 3 Lansia: Universitas Katolik Atma Jaya Fakultas Kedokteran 2010Kenny JapОценок пока нет
- Acid Base BalanceДокумент44 страницыAcid Base BalanceKenny JapОценок пока нет
- SLE Guidelines For Website 11-03-08Документ105 страницSLE Guidelines For Website 11-03-08Kenny JapОценок пока нет
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5795)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1091)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Imaging For Neuro-Ophthalmic and Orbital Disease - A ReviewДокумент24 страницыImaging For Neuro-Ophthalmic and Orbital Disease - A ReviewMashhoor AlfayezОценок пока нет
- All India Institute of Medical Sciences, Nagpur Result NotificationДокумент4 страницыAll India Institute of Medical Sciences, Nagpur Result NotificationNayan ChaudhariОценок пока нет
- Schizophrenia EssayДокумент6 страницSchizophrenia EssayLaura Jinparn100% (1)
- Assessment Nursing Diagnosis Scientific Explanation Planning Nursing Intervention RationaleДокумент2 страницыAssessment Nursing Diagnosis Scientific Explanation Planning Nursing Intervention Rationalekimglaidyl bontuyanОценок пока нет
- Immunochemistry and BiosensorsДокумент13 страницImmunochemistry and BiosensorsPalak AgarwalОценок пока нет
- VACCINESДокумент8 страницVACCINESzilikajainОценок пока нет
- Seminar On MumpsДокумент40 страницSeminar On Mumpssushmitabiswas052Оценок пока нет
- Adhesive Capsulitis Presentation May 2009Документ29 страницAdhesive Capsulitis Presentation May 2009cm4100% (1)
- Dry Citrasate Part A Acid Concentrate PowderДокумент4 страницыDry Citrasate Part A Acid Concentrate PowderSubhrajit ChattopadhayayОценок пока нет
- Oral Contributions: JACC March 9, 2010 ABSTRACTS: Cardiac Arrhythmias A1Документ217 страницOral Contributions: JACC March 9, 2010 ABSTRACTS: Cardiac Arrhythmias A1Apner Calvin SuОценок пока нет
- Alajar - Act9 - Biol 015Документ3 страницыAlajar - Act9 - Biol 015jarrettrayke14Оценок пока нет
- Bhoomi PatelДокумент9 страницBhoomi PatelPooja PanchalОценок пока нет
- PMDC Full Information PaperДокумент9 страницPMDC Full Information PaperjazzyОценок пока нет
- 2020 Using Sildenafilto Treata Dogwithidiopathic MegaesophagusДокумент7 страниц2020 Using Sildenafilto Treata Dogwithidiopathic MegaesophagusEduardo SantamaríaОценок пока нет
- Cells and Organs of The Immune SystemДокумент53 страницыCells and Organs of The Immune SystemZyma EmaОценок пока нет
- Post Term PregnancyДокумент35 страницPost Term PregnancyNishaThakuri100% (2)
- Somniferous Poisons: DR M. Malleswari Asso. Prof Nri Medical CollegeДокумент58 страницSomniferous Poisons: DR M. Malleswari Asso. Prof Nri Medical CollegeSudheera RachamallaОценок пока нет
- AAST Renal Injury ScaleДокумент11 страницAAST Renal Injury ScaleyuenkeithОценок пока нет
- Pediatric - 18.04.20-Child Guidance ClinicДокумент29 страницPediatric - 18.04.20-Child Guidance ClinicAjeeshОценок пока нет
- Teaching Plan For PidДокумент5 страницTeaching Plan For PidokaciaОценок пока нет
- Working With Whiplash, Part I (Myofascial Techniques)Документ5 страницWorking With Whiplash, Part I (Myofascial Techniques)Advanced-Trainings.com100% (4)
- Pelvix Organ ProlapsДокумент5 страницPelvix Organ ProlapskazugawaОценок пока нет
- ADAT Practice TestДокумент54 страницыADAT Practice TestRyan GrossОценок пока нет
- Burn Mcqs2Документ11 страницBurn Mcqs2Musa yohanaОценок пока нет
- 10.master Rotation Plan M. Sc. Nursing 1st YearДокумент4 страницы10.master Rotation Plan M. Sc. Nursing 1st YearNaresh JeengarОценок пока нет
- Observation On Therapeutic Effects of Cupping Therapy For Allergic RhinitisДокумент2 страницыObservation On Therapeutic Effects of Cupping Therapy For Allergic Rhinitischakir BezzahiОценок пока нет
- Allergy Clinic Policy and ProceduresДокумент4 страницыAllergy Clinic Policy and ProceduresMiselonОценок пока нет
- CVA-Health Teaching PlanДокумент5 страницCVA-Health Teaching PlanAna100% (4)
- GGT enДокумент2 страницыGGT enKaoueche OmarОценок пока нет
- ABO-Rh Blood Typing With Synthetic Blood: Teacher'S Manual and Student GuideДокумент32 страницыABO-Rh Blood Typing With Synthetic Blood: Teacher'S Manual and Student GuideMylan Gaston100% (1)