Академический Документы
Профессиональный Документы
Культура Документы
Neurology Nursing Study Guide
Загружено:
HayleyLangleyАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Neurology Nursing Study Guide
Загружено:
HayleyLangleyАвторское право:
Доступные форматы
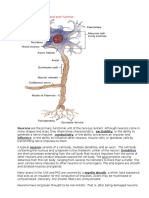
Neuro Study Guide
Disease
Brief
Clinical
pathophysiology manifestation
/Assessment
Diagnostic
tests &
findings
Altered Level
of
Consciousness
(LOC)
Not a disease
process!
At risk for
alterations in
any body
system!!!
3 types
-Neurologic
-Toxic
-Metabolic
Can be caused by
factors such as:
drug overdose
head injury
stroke
alcohol
hepatic/renal
failure
DKA
Increased
Intracranial
Pressure (ICP)
Not a disease
process!
Increased ICP
occurs when one
of the three
factors
(blood,brain,CSF)
increases and the
LOC is a
continuum from
A&O x3 to coma
Restlessness
Anxiety
Slow pupils
Conscious?
Decreased
verbal response
Decreased
motor response
Decreased eye
response
Respiratory
depression
*Earliest signs are
change in LOC,
slowed speech,
delayed response
More signs:
Restlessness
Increased
drowsiness
Confusion
Full
assessment
Neuro exam
Glasgow
coma scale
Medical
management
**Airway is first
priority,
especially if
unconscious
-Find the cause
to find the
treatment
Potential labs:
Blood glucose,
Electrolytes,
Liver function,
BUN, Serum
ammonia,
PT/PTT, Serum
ketone, Blood
alcohol/drug,
ABGs
Diagnostic:
CT, MRI, EEG,
PET/SPECT
**NO lumbar
punctures!!
CT, MRI, PET,
SPECT, cerebral
angiography,
transcranial
doppler,
Evoked
EMERGENCY
Intracranial
monitoring
indicated
Craniotomy,
craniectomy,
Osmotic
Nursing
diagnoses
Interventions
Other notes:
Ineffective Airway
clearance
Risk of injury
Deficient fluid
volume
Impaired oral
mucous
membranes
Risk for impaired
skin integrity
Impaired tissue
integrity of the
cornea
Ineffective
thermo-regulation
Impaired urinary
elimination
Bowel
incontinence
Disturbed sensory
perception
Interrupted family
process
Obtain/ maintain
patent airway
Protect the patient
Maintain fluid balance/
IV fluids as ordered
Tube feedings if
indicated
Mouth care
ROM
Turning/ repositioning
Keep eyes moist and
protected
Heat/cold as necessary
to maintain body
temperature
Bladder scan/ Catheter
Promote bowel
function
Provide sensory
stimulation
Care for the family
SCD hose/ DVT
prevention
Coma:
unconscious,
unrousable,
unresponsive
Locked In
syndrome:
Inability to move
or respond except
for eye movement
(lesion of Pons)
Akinetic Mutism:
Sometimes opens
eyes but makes
not movement or
sound
Persistent
vegetative state:
devoid of
cognitive function
but has sleepwake cycles
Ineffective airway
clearance
Ineffective
breathing pattern
Ineffective
cerebral tissue
perfusion
Deficient fluid
volume
Maintain patent
airway
Monitor respiratory
status
HOB up to 60
Avoid stimuli that
increases ICP
Hourly I/O during
acute phase
CPP: 70-100 mm
Hg
ICP in ventricles is
0-10 mm Hg, with
a max of 15 mm
Hg
Neuro Study Guide
other two cannot
compensate to
maintain normal
ICP
Seizures
Uncontrolled
electrical
discharge in the
brain.
Is either primary
or secondary to
metabolic,
systemic and
other causes.
Weakness on one
side or in one
extremity
Headache
Vomiting
Impaired gag
and/or corneal
reflexes
Progression
towards stupor
and coma
Late signs:
Coma
Fixed pupils
Decortication
Decerebration
Impaired/ absent
respirations
Cushings
response:
Increased BP
Widened pulse
pressure
Cardiac slowing
Cushings triad:
Bradycardia
Hypertension
Bradypnea
Depends on
type of seizure
how they
present- see
note.
During a seizure
documentation:
Circumstance
before the seizure
Aura
potential
studies,
electrophysiologic
monitoring.
Dx:
CBC, CMB, UA,
drug screen,
lumbar
puncture, CT
scan, EEG, skull
xray
Assess:
Patient Hx
Family Hx
diuretics, fluid
restriction, CSF
drainage, fever
control,
maintaining BP
and O2 status,
reducing cerebral
demands, avoid
increases r/t
increased
abdominal
pressure,
straining with
BM, high PEEP.
Usually treated
with medication
though surgical
options do exist
in some cases.
Risk for infection
Impaired skin/
mucous
membrane
integrity
Risk for injury
Fear
Ineffective
individual coping
Strict aseptic
technique with ICP
monitoring
Turn/reposition hygiene
Do not restrain
patient, pad siderails,
place on their side
Adherence to
medications is
important to prevent,
identify triggers and
avoid
***See pages 8-11
on the ch 61-62
notes packet.
Details types of
seizures, etc
**recommend rereading the status
epilepticus section
as well
Neuro Study Guide
Head injury, CVA
are biggest causes
of new onset
seizures
What the patient
does first area
affected and how,
type of
movements,
areas of body
involved, size of
pupils and if eyes
are open,
automatisms,
incontinence,
duration,
unconsciousness,
paralysis, inability
to speak,
cognitive status,
and movements
at the end of
seizure as well as
if the patient
sleeps after.
protect from
injury and do not
touch during
seizure-
Characteristics
of the seizures
Deficient
knowledge
Teaching about
management and
referral to counseling
Ongoing education
and encouragement.
Medic alert bracelet.
Family teaching.
Nurse then
prevents
complications and
allows patient to
rest bedrails up
and padded if
needed
Headache (HA) Migraine:
abnormal
metabolism of
serotonin exact
mechanism
unknown
4 phases of
migraine:
Prodrome
nondescript
symptoms
(depression,
food cravings,
Detailed Hx
Medication Hx
Assessment of
head and neck
Complete
neuro exam
Abortive
medications
Prevention
techniques
(identify triggers,
etc)
Analgesics
Acute pain
Medication and other
nonpharmacological
measures(dark, quiet
room, cold/heat,
massage, elevate HOB
30)
Migraine in
particular can
occur with
hormonal changes
related to
menstruation
Neuro Study Guide
Tension
contraction of
scalp/neck
muscles with
physical or
emotional stress
Cluster dilation
of orbital and
nearby
extracranial
arteries (theory)
feeling cold)
hours-days
before
AuraNot in most
patients, may
have neuro
symptoms
Headache- 4-72
hours
Recovery
exhaustion, may
sleep for
extended
periods
Other
diagnostics not
used unless
biologic, toxic,
oncologic
cause
suspected
Non-medication
therapies
(massage,
heat/cold, etc)
Deficient
knowledge
Help identify triggers
and provide teaching
on lifestyle
modifications to
prevent or reduce
occurrences. Provide
teaching about
medications and to
take triptans and
ergot derivatives at
the first symptoms.
Hx, complete
neuro and
physical exam,
-initial focus is
Thrombolytic
therapy within
less than 3 hours
unless
contraindicated
Impaired physical
mobility
ROM, positioning,
turning q 2,
ambulation
assistance, exercises,
PT consult
Tension:
Band like pain
or like a weight
on the head.
Steady, constant
pressure
Cluster:
unilateral and
come in clusters
of 1-8 in a day.
Excruciating
pain 15min-3hrs
usually in
eye/orbit region
but may radiate
Ischemic
stroke
Separated into 5
catagories based
on location/origin
but basically a
blood clot or
Numbness/wea
kness of
face/arm/leg on
one side
Good health Hx is
a must as well as
good assessment
of the headache
See
questions
on page
1891
Neuro Study Guide
plaque causes
blockage in the
brain causing
tissue death
Confusion/LOC
change
Trouble
speaking or
understanding
speech
Visual
disturbances
Difficulty
walking and
dizziness
Sudden severe
headache
Hemiplegia
Sensory
loss/agnosia
airway
patencyCT asap to
determine if
ischemic or
hemorrhagic,
MRI/MRA,
ECG, carotid
ultrasound, TE
echo, and
SPECT
by INR >1.7,
anticoagulant
use, and recent
intracranial
pathology.
If not candidate
for TPAHeparin not
usually used but
is still an option.
Maintenance of
cerebral
hemodynamics
mannitol, PCO2
between 30-35,
preventing
increase in ICP,
and managing
complications
(UTI,
dysrhythmia, etc)
Acute pain
Self care deficit
Disturbed sensory
perception
Impaired
swallowing
Impaired urinary
elimination
Disturbed thought
processes
Impaired verbal
communication
Risk for impaired
skin integrity
Interrupted family
processes
Sexual
dysfunction
Analgesia,
amitriptyline, lamictal,
lyrica
Assistive devices,
teaching,
encouragement
Approach from
unaffected side and
put objects on that
side
Special diet (thick
liquid and pureed
foods), tube feeding if
needed, swallowing
techniques
Bladder (and bowel)
training, cath if
needed
Reality orientation,
cueing,
interdisciplinary
training program
Emotional support
and understanding,
therapeutic and
facilitating
communication,
speech therapy, social
contact
Patient and family
teaching and inclusion
in plan of care,
realistic approach that
progress may be slow,
emotional care
Communication,
education, counseling,
medication adjust
Neuro Study Guide
Hemorrhagic
stroke
Depends on
cause:
Arteriovenous
malformations,
aneurysm,
intracranial
neoplasms,
subarachnoid
All cause bleeding
into the brain and
increased ICP
which can cause
brain death
Head injury
(HI)
Skull fracture,
Contusion,
laceration and/or
torn blood vessels
due to impact,
accelerationdeceleration
injuries, and
foreign object
penetration.
Increase in ICP
can cause
ischemia
The same as
intracranial
most common
complaint is
severe
headache
Key symptoms:
Vomiting
Seizures
Sudden change
in LOC
Symptoms
relate to the
injury and
affected area
May have
nosebleed,
battle sign,
bleeding from
pharyx or ears,
csf drainage
May have
seizures, coma,
S/S of increased
ICP
CT, MRI,
cerebral
angiography,
lumbar
puncture (only
if ICP not
increased)
Toxicology
screening
Hx, Neuro
exam, xray,
MRI, CT,
cerebral
angiography
If bleeding
caused by
warfarin, Vit K or
FFP given.
Surgical
intervention
when applicable
or endovascular
procedures.
Prevent/treat
rebleeding,
antiseizure meds,
DVT prevention,
Fever,
hyponatremia
and
hyperglycemia
treated, BP
stabilized
Ineffective
cerebral tissue
perfusion
Depends on
injury.
Also depends on
type of injury and
if there is brain
damage present
and/or
neurological
symptoms and
deficits. Managing
ICP is key here so
review (again) the
second topic of
this study guide
May have
surgical
intervention
Maintaining
cerebral
homeostasis is
key
Risk for bleeding
Disturbed sensory
perception
Anxiety
-others depending
on needs of the
patient see
above
Airway is #1
there rest are also
similar to stroke
Avoid increase in ICP,
HOB 15-30, SCD, close
monitoring of VS and
status
(Rebleeding) BP
carefully maintained
and increase in ICP
avoided
r/t aneurysm
precautions, pt is on
strict bedrest with
environment keep as
calm and quiet as
possible, visitors
restricted, etc. keep
patient informed and
family when possible.
Provide reassure and
support
Terms:
Concussion
Contusion
Diffuse Axonal
injury?
Epidural and
subdural
hematoma
Neuro Study Guide
Spinal Cord
injury (SCI)
Traumatic damage
to any level of the
spinal cord. May
have partial or
complete lesions
of either sensory
or motor or both
Dependent on
type and level of
injury.
May have
respiratory
failure, impaired
sensory and/or
motor function,
dependent on
level of injury,
may be unable
to speak,
swallow
Xray, CT,
possibly MRI
Full
neurological
exam
IV corticosteroids
(methylpredniso
ne) first 24-48
hrs, respiratory
therapy
including vent if
necessary O2
given bc
hypoxemia
increased
secondary
damage.
Immobilization
and stability
devices. Surgical
intervention
when indicated
(compression,
fragmented or
unstable
vertebrae,
wound
penetrating cord,
bone frags in
spinal canal,
deterioration of
pt neuro status)
Ineffective
breathing pattern
Ineffective airway
clearance
CAUTIOUS suctioning,
close monitoring of
resp status, assisted
coughing, air
humidification
Impaired bed and
physical mobility
Frequent positioning
and early ambulation,
ROM
Disturbed sensory
perception
Risk for impaired
skin integrity
Impaired urinary
elimination
Constipation
Acute pain
Long term
anticoagulation
Provide prism glasses,
coping strategies,
provide emotional
support, music, touch
Turn q2, frequent
assessment, kinetic
bed, hygiene and
skin/peri care
Intermittent cath,
teach pt and family
and encourage
participation, teach to
record I/O and
monitor void status
Stool softeners, high
fiber diet, bowel
program institution
Provide comfort
measures, analgesia
Most common in
young males
MVAs, falls,
violence, sports
Respiratory
affected T1-T11
Diaphragm
controlled by C4
Review chart 63-7
on pg 1935 &
table 63-3 on pg
1936
Autonomic
Dysreflexia
know it, know its
signs and
symptoms. Know
that can be
caused by ANY
stimulus below
level of injury
Spinal and
Neurogenic shock
not well
described in book,
google for better
idea
Also- this study
guide doesnt
cover long term
management pgs
1943-46
Neuro Study Guide
Multiple
Sclerosis (MS)
Immune
mediated,
progressive
demyelinating
disease. Theory
virus triggers
autoimmune
response. T cells
allow infiltrates in
that cause
demyelination.
Areas- optic
nerves chiasm and
tracts, the
cerebrum, brain
stem, cerebellum
and spinal cord.
Most patients
have relapse
and remission
deficits may
occur and
accumulate over
time. 50% of
RR progress to
secondary
progressive
course with
increase in
deficits and rare
plateaus
Primary
progressive:
Quadriparesis
Cognitive
dysfunction
Visual loss
Brain stem
syndromes
Specific
symptoms
depend on area
of brain affected
MRI,
electrophoresis
of CSF, Evoked
potential
studies,
urodynamic
studies, neuropsychological
testing
Sexual Hx
Pt may have:
Diplopia, pain,
fatigue,
numbness,
weakness,
blurry vision,
patchy and
total blindness,
depression,
coordination
difficulties
No Cure
Individualized
treatment based
on symptoms
Nerve blocks
Possible meds:
Rebif, Betaseron,
Avonex,
Copaxone- cause
flu like
symptoms-treat
with nsaids
May take 6
months for
improvement
Baclofen, valium
for spasticity
Symmetrel,
Cylert and Prozac
for fatigue
Inderal,
Neurontin, and
Klonopin for
Ataxia
Bowel and
bladder meds
Impaired bed and
physical mobility
Risk for injury
Impaired urinary
and bowel
elimination
Impaired verbal
communication
Impaired
swallowing
Disturbed thought
processes
Ineffective
individual coping
Impaired home
maintenance
management
Potential for
sexual dysfunction
Myasthenia
Gravis (MG)
Auto-immune
disease that
targets
Initial:
Diplopia and
ptosis,
Acetycholinest
erase inhibitor
test.
Aimed at
improving
function and
Myasthenic Crisis:
Exercises, walking,
minimize spasticity
and contracture,
stretching
Gait training, assistive
devices, monitor for
pressure ulcers
Void schedule,
bowel/bladder
training, self-cath
teaching, adequate
fluids and diet
including fiber
Diet modifications if
needed, speech
consult, alternate
communication
methods teaching
Pt and family
teaching, set realistic
goals, structured
environment
Support, home care,
service referrals,
assistive devices, offer
resources
Home modifications
for independence,
assistive devices,
temperature control
Identification of the
problem, Referral to
sex counselor,
alternative methods
Education and
medication
Onset ages 20-40
Terms:
Spasticity
Ataxia
During
Myasthenic crisis
ABGs,
Neuro Study Guide
acetycholine and
impairs
transmission of
impulses across
the myoneural
junction.
Causes weakness
of the voluntary
muscles.
80% also have
thymic
hyperplasia or
thymic tumor.
Guillain-Barre
syndrome
Autoimmune
Attack on the
peripheral nerve
myelin. The result
is acute rapid
demyelination of
peripheral nerves
and some cranial
nerves producing
ascending
weakness with
dyskinesia,
hyporeflexia and
paresthesias.
weakness of
face and throat
muscles.
Dysphonia and
generalized
weakness.
-tensilon given
IV to diagnose.
-face weakness
and ptosis
resolve for 5
minutes
MRI, EMG
Begins with
muscle
weakness and
diminished
reflexes of
lower
extremities and
may progress to
tetraplegia,
Neuromuscular
respiratory
failure, bulbar
weakness,
blindness,
Patient
presents with
symmetric
weakness,
diminished
reflexes and
ascending
motor
weakness.
Hx of viral
illness.
Lab tests not
useful.
CSF evaluation.
targeting
antibodies
No Cure
Anticholinesteras
e mediation,
pyridostigmine,
corticosteroids,
imurian, IVIG
*No Novocaine
Plasmapheresis
Thymectomy
** Medical
Emergencies **
Requires ICU
management.
Assessment of
muscle strength
and respiratory
function.
Intubation.
Plasmapheresis
and IVIG
continuous ECG
monitoring
Respiratory
Distress
Dysphagia
Dysarthria
Ptosis
Diplopia
Prominent Muscle
Weakness
*Airway is priority
Nursing Diagnoses
depend on
symptoms and
course of disease.
Aimed at
preventing and
managing
complications
Ineffective
breathing pattern
Impaired bed and
physical mobility
Imbalanced
nutrition, less
than body
requirements.
management
important.
Conservation of
energy.
Minimize aspiration
by timing meals at
peak effect of
anticholinesterase
medications.
Supplemental
feedings may be
needed for adequate
nutrition.
Eye care important for
prevention of corneal
damage.
Avoidance of
triggering factors and
infections.
Close Monitoring and
potential mechanical
ventilation which
should be discussed
on admission.
ROM, SCD, Position
Changes,
Anticoagulation.
IV fluids and
Parenteral nutrition,
gastrostomy
management
electrolytes, i/o
and daily weight
are monitored.
NG tube if
impaired
swallowing.
Sedatives and
tranquilizers
avoided.
Neuro Study Guide
Caused by
antecedent event
most often viral
infection. The
myelin damage
results from the
inability to
distinguish
between two
proteins.
Bells Palsy
Meningitis
Paralysis of the
face caused by
unilateral
inflammation of
cranial nerve VII.
Exact cause
unknown,
theories include
vascular ischemia,
viral disease,
autoimmune
disease or a
combination.
May be a type of
pressure paralysis.
Septic=bacterial
infection.
Aseptic=viral
infection.
Can be blood
stream or direct
inability to
swallow or clear
secretions and
autonomic
dysfunction.
Evoked
potential
studies.
Increased
lacrimation,
painful
sensation in the
face behind the
ear and in the
eye, speech
difficulties,
unable to eat on
affected side.
No Diagnostics
Nuchal
rigidity=early
sign. +kernigs
sign.
+brudzinskis
sign.
photophobia
CT, MRI, CSF
studies may
demonstrate
low
glucose/high
WBC/high
protein.
Hypotension
managed with
fluid.
Impaired verbal
communication
Fear and anxiety.
Treatment aimed
at maintaining
muscle tone and
preventing or
minimizing
denervation.
Corticosteroids,
analgesics,
surgical
exploration if
tumor suspected
or to decompress
nerve if doesnt
resolve.
Acute pain
Antibiotics for
bacterial (vanco,
cephalosporins).
Decadron,
dexamethasone,
dehydration and
shock are treated
Hypovolemia.
Actual infection.
Risk for injury r/t
seizures.
Impaired gas
exchange.
Risk for Corneal
injury
Picture Cards, Eye
blink system, speech
consult.
Encourage family
participation in care,
increase patient sense
of control, provide
information about the
condition, teach
relaxation and
distraction,
diversional activities,
encourage visitors,
listening to music,
reading, TV.
Analgesic and facial
massage when
tolerated.
Eye patch, eye
ointment,
moisturizing drops,
eye shield and use of
wrap around glasses
during the day to
minimize moisture
loss.
ABGs and PO2 to
identify need for
support if increasing
ICP compromises
brain stem. Possible
trach. Possible
mechanical
Most patients are
younger than 45.
Protect patient
from further
injury and
infection.
Neuro Study Guide
introduction
through trauma.
CreutzfeldtJakob disease
Caused by a prion.
It causes
spongiform
changes in the
brain
(degeneration of
brain tissue).
Trigeminal
Neuralgia
As the brain ages
a loop of cerebral
artery or vein may
compress the
nerve root entry
point.
Peripheral
neuropathy
Most commonly
caused by
diabetes and poor
glycemic control.
with fluids.
Phenytoin for
seizures.
ventilations. Monitor
BP. Rapid fluid
replacement but take
care to prevent
overload. Fever
reduction.
Offer support to the
patient and family.
Palliative care. Offer
emotional support.
Muscle spasms,
rigidity,
dysarthria,
incoordination,
cognitive
impairment.
Mental
deterioration,
memory loss,
paralysis.
Pain ends as
abruptly as it
starts and is
usually
unilateral and
described as
shooting or
stabbing.
MRI, EEG, CSF,
brain biopsy
No effective
treatment. Death
is inevitable.
Palliative care
Ineffective coping
Grief
Progression of the
disease occurs
quickly after the
onset of specific
neurologic
symptoms.
Survival is an
average of
22months.
MRI, assessing
trigger points
Acute pain.
Risk for injury.
Educating on
preventative
strategies such as
avoiding too hot or
too cold foods, drinks,
water. The nurse
needs to assist with
the care of the
anxiety, depression,
and insomnia that
often accompanies
the chronic pain.
Occurs most often
before the age of
35 and is more
common in
women and
people with MS
compared to the
general
population.
Loss of
sensation and
muscle atrophy
and weakness.
Diminished
reflexes.
Physical
assessment
and findings.
Pain and
sensation
Pharm:
antizeisure
agents,
gabapentic,
baclofen
Surg:
decompression
of the nerve,
radiofrequency
thermal
coagulation,
percutaneous
balloon
microcompressio
ns.
Gabapentin,
lyrica,
Chronic pain.
Risk for injury/fall
Diabetes education
and management.
Depression and
anxiety are common
side effects and
It is important
that it is
prevented b/c
there is no cure.
Educating
diabetics on the
Neuro Study Guide
Parasthesia and
pain.
Huntingtons
Disease
Degenerative
Disc Disease
Cervical
Herniation
Premature death
of cells in the
striatum of the
basal ganglia. Cells
are also lost in the
cortex (the region
associated with
thinking, memory,
perception,
judgment) and in
the cerebellum
(the region
responsible for
coordinated
voluntary muscle
movement)
Herniation of the
intervertebral disc
with subsequent
compression it is
preceded by
degenerative
changes that
occur with aging.
The same at DDD
but with the risk
of lesions forming
on the spinal cord.
testing of
extremities.
support for these are
important.
importance of
blood sugar
management is
key.
If there is a family
history, people
can be tested for
the genetic
marker before
symptoms occur.
Positive family
history.
Presence of
genetic
markers.
No cure just treat
the symptoms.
Dopamine
receptor
blockers.
Antiparkinsons
medications for
rigidity.
Risk for injury.
Focus on the
palliative and
coping
Look beyond the
disease and focus on
the patients needs
and capabilities. End
of life care will be a
priority. Teach
strategies to manage
symptoms. Increased
risk for aspiration
pneumonia.
C/M depends on
the location in
the spine.
Health HX.
Physical exam.
MRI, CT
Neurologic
exam.
Pain.
Infection risk if
surgery is
undertaken.
Pain management and
support.
Often prescribed
many pain
medications and
can have chronic
narcotic use
resulting in
increased need for
pain medications.
Typically occurs
at the C5-C7
interspaces.
Pain and
stiffness of the
neck.
Parasthesia.
MRI of the Cspine.
Bedrest and pain
medications for
cervical and
lumbar disks.
Surgical excision
of the herniated
disc.,
laminectomy,
fusion.
Pain medications
and rest of the
surgical spine to
allow the C spine
to heal and
reduce
inflammation.
Surgical excision
Pain. Infection risk
if surgery.
Skin integrity is at
risk d/t bedrest.
May be flat bedrest
after surgery. Watch
for excruciating pain
after surgery. Could
mean a need for
further surgery. Neck
should be kept
Hospital stay is
likely to be short.
Self care must be
promoted and
taught.
Abnormal
involuntary
movement
(chorea),
intellectual
decline,
emotional
disturbance,
constant
writhing,
motions are
devoid of
rhythm or
purpose.
Neuro Study Guide
Brain Abscess
Collection of
infectious
material within
the tissue of the
brain.
Can be caused by:
-intracranial
surgery,
penetrating head
injury, of tongue
piercing.
-Headache,
usually worse in
the morning
-fever
-vomiting
-focal
neurologic
deficits
-Decrease LOC
-seizure
-MRI or CT scan
-blood cultures
-Chest x-ray
-EKG
Alzheimers
A chronic,
progressive, and
degenerative
brain disorder
that is
accompanied by
profound effects
on memory,
cognition, and
ability for self-care
-loss of memory
and cognition
that disturbs
daily life
-Trouble
understanding
visual images
and spatial
relationships
-Problems with
words or
speaking
-Misplacing
things and
losing the ability
to retrace steps
-Poor judgment
-withdrawn
from activities
-Medical
history
including
family history
-Mental status
testing
-physical and
neurological
exam
-Blood test to
rule out other
causes
-MRI & CT
usually used to
rule out other
causes
of the herniated
disk may be
necessary.
-Control ICP
-drain abscess
-Antimicrobial
therapy
-high dose
antibiotics
-Corticosteroids
-Antiseizure
meds
-goal is to
manage
symptoms
-assessing for
underlying
depression
-pharm to treat
symptoms but
does not stop the
progression.
-behavioral and
psychosocial
therapies
midline and in a
neutral position.
-Acute confusion
-fear
-Grieving
-Decreased
intracranial
adaptive capacity
-Acute pain
-Vision loss
-Risk for injury
-Vision loss
-Prevention such as
promptly treating
otitis media,
mastoiditis,
rhinosinusitis, dental
infections, and
systemic infections.
-monitor neuro status
-admin meds
-assess response to
treatment
-supportive care
-monitoring safety
-educate patient and
family
-Wandering
-Promoting patient
-impaired memory function and
-impaired physical independence.
mobility
-promoting safety
-self-neglect
-reducing anxiety and
-risk of loneness
agitation
-caregiver role
-providing
strain
socialization
-chronic confusion -adequate nutrition
-hopelessness
-supporting and
-powerlessness
education patient and
family
-Seizures are
common.
-definitive
diagnosis can be
made only at
autopsy
Neuro Study Guide
-Change in
mood or
personality
Parkinsons
Cerebral
metastases
-Slowly
progressing
neurologic
movement
disorder that
eventually leads
to disability.
-decresed level of
dopamine
resulting from
destruction of
pigmented
neuronal cells in
the substatia nigra
in the basal
ganglia region of
the brain. The loss
of dopamine
results in more
excitatory
neurotrasmitters
than inhibitory
neurotransmitters
, leading to an
imbalance that
affects voluntary
movement.
-cancer that has
metastasized
(spread) to the
brain from
another location
in the body
Gradual onset
and symptoms
progress slowly.
-Cardinal
manifestations:
-Tremors
-Rigidity
-Bradykinesia
-Postural
instability
-PET & SPECT
scans
-diagnosed
clinically from
the patients
history and the
presence of
two of the four
cardinal
manifestations
Focuses on
controlling
symptoms and
maintaining
functional
independence
-Pharm therapy:
antiparkinsonian
meds (ex.
levodopa)
-stereotactic
procedures
-neural
transplantation
-Deep brain
stimulation
-Impaired physical
mobility
-Self-care deficits
-Constipation
related to
medication and
reduced activity
-imbalanced
nutrition
-impaired verbal
communication
ineffective coping
-Improving mobility
-Enhancing self-care
activities
-Improving bowel
elimination
-Improved nutrition
-enhancing swallowing
-encouraging the use
of assistive devices
-Improving
communication
-supporting coping
abilities
-promoting home and
community-based
care
-neurologic
exam
-Headache
-gait
disturbances
-MRI along
with S/S
-palliative and
involves
eliminating of
reducing serious
symptoms.
-Self-care deficit
-Imbalanced
nutrition
-Anxiety
-Interrupted
family processes
-Pain management
-improve nutrition
-compensation for
self-care deficits
-relieving anxiety
-survival time:
*no treatment for
brain metastases:
1 month
Neuro Study Guide
Spinal tumors
Tumor within the
spine. Classified
by anatomic
relation to the
spinal cord.
-intramedullary
lesions: within the
spinal cord
-extramedullaryintradural lesions:
within or under
the spinal dura
-extramedullaryextradural lesions:
outside the dural
membrane
ALS
Unknown cause,
there is a loss of
motor neurons in
the anterior horns
of the spinal cord
and the lower
-visual
impairment
-personality
changes
-altered
mentation
(memory loss
and confusion)
-focal weakness
-paralysis
-aphasia
-seizures
-localized or
shooting pains
and weakness
and loss of
reflexes above
the tumor level
-neurologic
examiniation:
assess pain, loss
of refexes, loss
of sensation or
motor function,
and the
presence of
weakness and
paralysis
-pain longer
than 1 month
-depends on
location of the
affected motor
neuron
-fatigue
-Radiation
therapy
-surgery
-Chemotherapy
-Corticosteriods
-Osmotic
diuretics
-Antiseizure
agents
-enhancing family
processes
-promoting home and
community-based
care.
-MRI scans:
most common
used.
-x-ray
-radionuclide
bone scan
-CT scans
-biopsy
-Surgical
interventions:
primary
treatment
-partial removal
of the tumor
-decompression
of the spinal cord
-chemotherapy
-radiation
therapy
-Provide per and postoperative care
-Managing pain
-monitoring for
complications
-Patient and family
teaching.
-compensation for
self-care deficits
Diagnosed on
the basis of the
signs and
symptoms, no
clinical or
laboratory test
NO specific
therapy exists for
ALS. The main
focus of medical
and nursing
management is
on interventions
-ineffective
breathing pattern
-impaired verbal
communication
-decisional conflict
-Chronic sorrow
-Monitor for
aspiration may in
enteral feeds
-maintain or improve
function, well-being,
and quality of life
*corticosteroid
treatment alone:
2 months
*Radiation
therapy: 3-6
months.
-The average
survival time is 3-5
years with death
due, most
commonly to
respiratory
insufficiency.
Neuro Study Guide
Muscular
Dystrophies
Post-Polio
nuclei of the
lower brain stem.
-progressive
muscle
weakness,
-cramps,
-facial twitching
-loss of
coordination
are specific for
this disease.
-Electromyography and
muscle biopsy
may be done
-MRI
-Neuropsychological
testing
Incurable muscle
disorders
characterized by
progressive
weakening and
wasting of the
skeletal or
voluntary
muscles.
Unknown prior
polio infection
-Muscle wasting
and weakness
-abnormal
elevation in
serum levels of
muscle
enzymes.
-elevated
muscle
enzymes.
Post-Polio
symptoms:
NO diagnostic
test for this**
-Progressive
muscle and joint
weakness and
pain
-General fatigue
and exhaustion
with minimal
activity
-Muscle atrophy
-Breathing or
swallowing
problems
-Sleep-related
breathing
Hx, physical
exam and
exclusion of
other medical
conditions
to maintain or
improve
function, wellbeing, and
quality of life.
-riluzole (Rilutek),
a glutamate
antagonist, is the
only med
approved for the
treatment of ALS.
-focuses on
supportive care
and prevention
of complications
-individualized
therapeutic
exercise program
-spinal fusion
-Impaired
swallowing
-Risk for
aspiration
-anxiety
No specific
treatment
focus on
symptoms
Activity
intolerance
-intense therapy to
keep the muscles
active and functioning
normally
-night splints
-teaching patient selfcare
Chronic pain
Risk for ineffective
breathing pattern
Plan activities to
conserve energy,
schedule rest periods,
use assistive devices
Heat/Cold, cautious
use of medications
Pulmonary hygiene,
adequate fluid intake,
CPAP if applicable
Provide teaching and
resources for diet and
safe exercise
Imbalanced
nutrition: more
than
requirements
Disturbed sleep
Limit caffeine, assess
pattern
for nocturia
Risk for injury/falls Use of assistive
devices, fall
-Most of these
disorders are
inherited.
-spinal deformity
is a severe
problem.
Neuro Study Guide
Primary Brain
tumors
Glioma:
most common
type, with the
most common
type of glioma
being an
astrocytoma
which is also
graded
Note: I
recommend
re-reading this
section: brief
synopsis only
included here
+ the following
sections on
pre/post
surgical care
Description:
Intracranial
Craniotomy
Surgery
opening the skull
to gain access to
structures (Used
for: removal of
tumor or clot,
control
hemorrhage,
reduce pressure)
Craniectomyremoving a piece
of the skull
(usually for
pressure relief,
but can be used
for access of
specific site)
disorders (as
sleep apnea)
-Decreased
tolerance of
cold temps
Meningioma:
Common,
benign and slow
growing.
Manifestations
are result of
pressure.
Surgery is
preferred
treatment
Pre-Op:
Depends on
reason for
surgery. May
not be coherent
due to increased
ICP or
alterations in
LOC.
Hair will be
shaved on the
access site.
Post-Op:
Large head
dressing until
surgeon
removal
prevention, and
osteoporosis
(common with postpolio) management
Acoustic
neuroma:
8th cranial
nerve tumortinnitus,
hearing loss,
vertigo,
stagger- most
benign and
managed
conservatively
Pituitary
adenoma:
Either cause
pressure effects
or hormonalusually prolactin,
growth hormone
and ATCH- also
rarely TSH, FSH
and LH.
Angioma:
Abnormal clusters
of blood vessels
cause
hemorrhagic
stroke in <40 yo
Pre-Op:
CT, MRI,
cerebral
angiography,
transcranial
doppler.
Pre-Op:
Prophylactic
antibiotics and
phenytoin,
corticosteroids
(dexamethasone)
Mannitol/Lasix,
Anxiolytics
Pre-Op:
Depends on
patient disease
process and
functioning.
Neuro
evaluation,
assessment of
LOC, visual
assessment,
M/S strength,
bowel and
bladder
function
Post-Op:
Knowledge deficit
Anxiety
Fear
Post-Op:
Same as above
Post-Op:
Nursing diagnoses and
interventions will be
varied based on the
type of tumor. All are
at risk for increased
intracranial pressure
and varying forms of
neurologic
presentation.
Med surg book
Pg 1978 figure 651: common
locations of
tumors
Pre-Op:
***Deficient
knowledge of
Post-Op
expectations/care
needs to be
addressed BEFORE
surgery
Provide teaching
about Post Op
including hair
removal, catheter,
possible mechanical
ventilation, central
and ART lines, large
head dressing until
surgeon Oks smaller
one, limited vision if
periorbital swelling is
present, how to
communicate on the
vent
Post Op:
Location is
everything with
tumors where it
grows defines
what it affects
Neuro Study Guide
Burr holes: either
to facilitate a
craniotomy OR as
a means of
pressure relief
(also usually for
pressure relief,
but can be used
for access of
specific site)
Likely ET tube.
Assess:
Respiration
and
oxygenation
status, VS, LOC,
bleeding/CSF
leakage,
seizure, I/O
ICP monitoring
ABGs
CBC/CMB
BUN/
Creatinine,
blood glucose,
phenytoin
levels (10-20
mcg/mL)
Ineffective
cerebral tissue
perfusion
Risk of
imbalanced body
temperature
Potential for
impaired gas
exchange
Disturbed sensory
perception
Body image
disturbance
Impaired
communication
Risk for impaired
skin integrity
Risk for infection
Risk for fluid and
electrolyte
imbalance
Q15-60min VS/Neuro
assessment, HOB flat
or 30 degrees, control
cerebral edema and
ICP
Cover pt
appropriately, treat
hyperthermia
aggressively
Deep breathing/
Incentive spirometer,
Cautiously suction/
help pt cough,
humidify air
Announce presence,
cool compresses and
HOB elevation (30) to
decrease periorbital
edema
Verbalization,
interaction, grooming,
cover head with
turban (later, a wig)
Use of communication
boards, signals
Turning q 2 hours,
hygiene care
Aseptic technique
with ICP monitoring
Monitor I/O,
electrolyes, and urine
specific gravity, fluid
restriction, IV
fluids/diuretics as
ordered
Neuro Study Guide
Transsphenoidal
surgery
Description:
Access to the
brain (usually the
pituitary gland)
through the
mouth and
sinuses
Also used for
ablation of the
pituitary with
disseminated
breast or prostate
cancer
Pre-Op:
Depends on
reason for
surgery. May
have increased
ICP and altered
LOC
Post-Op:
Swollen/
bruised face
Nasal packing
cannot remove
blood around
until packing
removed!
Pre-Op:
Endocrine
workup
Rhinologic
evaluation
Nasopharyngea
l culture
(surgery
contraindicate
d with sinus
infection)
Visual
evaluation
Neuroradiologic
studies
Post-Op:
Urine specific
gravity after
EACH urination
to monitor for
diabetes
insipidus and
SIADH
ICP monitoring
CMB
CBC
Pre-Op:
May have
corticosteroids,
phenytoin,
and/or
prophylactic
antibiotics
prescribed
before surgery
Pre-Op: Same as
above
Pre-Op: Same as
above
Post-Op: Same as
above
Post-Op: Same as
above
Impaired oral and
nasal mucous
membranes
Mouth rinses every 4
hours no brushing
until incision heals
Petrolatum for lips
Use of air humidifier
Post-Op:
Antibiotics
Corticosteroids
Analgesics
-medication for
diabetes
insipidus if
indicated
(Desmopressin)
**Disturbed
sensory
perception r/t
proximity to optic
chiasm
Monitor visual fields
and acuity frequently
-decreasing acuity
suggests expanding
hematoma
***Deficient
knowledge of
Post-Op
expectations/care
needs to be
addressed BEFORE
surgery
HOB at 60 for at
least 2 weeks to
promote venous
drainage from site
Teaching:
Post Op
expectations,
potential
complications,
cares, Deep
breathing,
avoidance of
increasing ICP
(coughing,
sneezing etc)
Вам также может понравиться
- Neuro DisordersДокумент13 страницNeuro DisordersMicz Celiz100% (3)
- COMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideОт EverandCOMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideОценок пока нет
- Medical Surgical Nursing Review NotesДокумент78 страницMedical Surgical Nursing Review NotesLouie ParillaОценок пока нет
- Chicago Review Press NCLEX-PN Practice Test and ReviewОт EverandChicago Review Press NCLEX-PN Practice Test and ReviewРейтинг: 4 из 5 звезд4/5 (4)
- Shock Study Guide NursingДокумент4 страницыShock Study Guide NursingKory Christina100% (2)
- Medication Work Sheet For MedSurgДокумент5 страницMedication Work Sheet For MedSurgRyanMitchell100% (2)
- Med-Surg Nusing BulletsДокумент65 страницMed-Surg Nusing BulletsHarley C. Tan100% (1)
- MedSurg NeuroДокумент8 страницMedSurg NeuroZachary T Hall100% (1)
- Neuro Study GuideДокумент7 страницNeuro Study GuideNursingSchoolNotes100% (2)
- Fluid and Electrolytes for Nursing StudentsОт EverandFluid and Electrolytes for Nursing StudentsРейтинг: 5 из 5 звезд5/5 (12)
- Exam 2 - Neurological Study GuideДокумент10 страницExam 2 - Neurological Study GuideStephanieОценок пока нет
- Nursing Fluids and ElectrolytesДокумент14 страницNursing Fluids and Electrolytesaga1028100% (18)
- Head To Toe AssessmentДокумент3 страницыHead To Toe AssessmentCatherine Drew Sims100% (6)
- Chart of Neuro DisordersДокумент1 страницаChart of Neuro DisordersNursingSchoolNotes100% (2)
- Fluid and Electrolytes Study GuideДокумент16 страницFluid and Electrolytes Study GuideDianaNursing96% (28)
- STUDENT-Eating - Disorder-F&E-UNFOLDING ReasoningДокумент14 страницSTUDENT-Eating - Disorder-F&E-UNFOLDING ReasoningPeggy100% (12)
- Lab Values Cheat SheetДокумент8 страницLab Values Cheat SheetJamie Lebon100% (4)
- Neuro Study GuideДокумент11 страницNeuro Study GuideEllen Hennings100% (1)
- Endocrine NursingДокумент8 страницEndocrine NursingBunny Bonny100% (5)
- Cardiac DrugsДокумент10 страницCardiac Drugssurviving nursing school100% (3)
- Med Surg A Neuro PPT 120515134413541 5Документ93 страницыMed Surg A Neuro PPT 120515134413541 5Sapiah RamanОценок пока нет
- Nurses Note DONEДокумент1 страницаNurses Note DONEjhenssineОценок пока нет
- Neuro NursingДокумент22 страницыNeuro Nursingheiyu100% (6)
- Chapter 14 Fluid and Electrolytes ChartsДокумент7 страницChapter 14 Fluid and Electrolytes ChartsBNA_RN100% (3)
- Basic Drug CardsДокумент13 страницBasic Drug Cardsnene lewis100% (2)
- Neuro Nursing-Seizure DisorderДокумент8 страницNeuro Nursing-Seizure DisorderBell Jose50% (4)
- Shock With Hemodynamic ChangesДокумент2 страницыShock With Hemodynamic ChangesBNA_RN100% (1)
- ATI NotesДокумент16 страницATI NotesMei Sarte100% (1)
- STUDENT-Sickle - Cell-FUNDAMENTAL ReasoningДокумент7 страницSTUDENT-Sickle - Cell-FUNDAMENTAL ReasoningSharon Tanveer0% (1)
- HA-RLE-WS # 10 Assessing Nutritional StatusДокумент4 страницыHA-RLE-WS # 10 Assessing Nutritional StatusJULIE ANNE CORTEZОценок пока нет
- Med Surge 2 Mod 3 Study GuideДокумент19 страницMed Surge 2 Mod 3 Study GuideDirk Buckner100% (4)
- Medical Surgical Nursing Review NotesДокумент75 страницMedical Surgical Nursing Review NotesMary Ann Comia RañolaОценок пока нет
- GI NursingДокумент14 страницGI NursingKarl Bayonito100% (5)
- The 12-Lead Electrocardiogram for Nurses and Allied ProfessionalsОт EverandThe 12-Lead Electrocardiogram for Nurses and Allied ProfessionalsОценок пока нет
- Nursing Pharmacology Drug Study GuideДокумент15 страницNursing Pharmacology Drug Study GuideChelsea SmithОценок пока нет
- Head Eyes: Head To Toe AssessmentДокумент2 страницыHead Eyes: Head To Toe AssessmentVijungco88% (8)
- PrioritizationДокумент20 страницPrioritizationPascal St Peter Nwaorgu100% (1)
- CardioДокумент10 страницCardioMar OrdanzaОценок пока нет
- Quick Nursing Student Notes 2Документ1 страницаQuick Nursing Student Notes 2Frank KimОценок пока нет
- Med Surg Cheat Sheet 1Документ1 страницаMed Surg Cheat Sheet 1Figmentum FigmentumОценок пока нет
- CRITICAL THINKING IN CLINICAL NURSING PRACTICE (RN): Passbooks Study GuideОт EverandCRITICAL THINKING IN CLINICAL NURSING PRACTICE (RN): Passbooks Study GuideОценок пока нет
- RN Notes Med SurgДокумент15 страницRN Notes Med Surgiamdarn100% (3)
- Neurologic NursingДокумент10 страницNeurologic NursingAllisson Beckers100% (1)
- Med Surg Study GuideДокумент24 страницыMed Surg Study Guidekylie100% (4)
- 2510 - A-07 Nursing Physical AssessmentДокумент1 страница2510 - A-07 Nursing Physical AssessmentJenОценок пока нет
- A Handbook for Student Nurses, second edition: Introducing Key Issues Relevant for PracticeОт EverandA Handbook for Student Nurses, second edition: Introducing Key Issues Relevant for PracticeОценок пока нет
- Endocrine Disorders (Study Notes)Документ11 страницEndocrine Disorders (Study Notes)Danelle Harrison, RN90% (10)
- Med Surg CardsДокумент54 страницыMed Surg CardsIanne Merh100% (3)
- Surviving the ICU: A Toolkit for the Critical Care NurseОт EverandSurviving the ICU: A Toolkit for the Critical Care NurseОценок пока нет
- Gastrointestinal NursingДокумент8 страницGastrointestinal Nursingohsnapitslei90% (10)
- A Handbook for Student Nurses, 201819 edition: Introducing key issues relevant for practiceОт EverandA Handbook for Student Nurses, 201819 edition: Introducing key issues relevant for practiceОценок пока нет
- Pediatric Nursing: Immediate Care For Newborn (OLD)Документ8 страницPediatric Nursing: Immediate Care For Newborn (OLD)KristaRicaAbayabayОценок пока нет
- SEPTEMBER 6, 2021 Hematology Assessment: Characteristic FeaturesДокумент23 страницыSEPTEMBER 6, 2021 Hematology Assessment: Characteristic FeaturesChristian John V. CamorahanОценок пока нет
- Lab Report 3Документ18 страницLab Report 3api-273323485Оценок пока нет
- Enzymes NPДокумент25 страницEnzymes NPBharatShethОценок пока нет
- MODUL Praktikum Anatomi Dan HistologiДокумент20 страницMODUL Praktikum Anatomi Dan HistologiandikaОценок пока нет
- 1 PediatricsДокумент21 страница1 PediatricsHannah Lei100% (1)
- TEAM MEDIC DRILLS v4Документ11 страницTEAM MEDIC DRILLS v4Jimmy JamesОценок пока нет
- 5090 w10 Ms 61Документ3 страницы5090 w10 Ms 61mstudy123456Оценок пока нет
- Unlocking The BrainДокумент3 страницыUnlocking The BrainPsychedelicBaronОценок пока нет
- ANS & CVS Response To Exercise v2Документ18 страницANS & CVS Response To Exercise v2chow wing yin amandaОценок пока нет
- DMLT I IiДокумент11 страницDMLT I IisyedzahidshabirОценок пока нет
- 12 Bio-Chemic SALTSДокумент17 страниц12 Bio-Chemic SALTSfakhanОценок пока нет
- Sri Lankan Biology Olympiad 2008Документ5 страницSri Lankan Biology Olympiad 2008Science Olympiad BlogОценок пока нет
- Background Results: DR Aditya Bhat, DR, Amit Misri Department of Paediatric Cardiology, Medanta-The Medicity, GurgaonДокумент1 страницаBackground Results: DR Aditya Bhat, DR, Amit Misri Department of Paediatric Cardiology, Medanta-The Medicity, GurgaonADОценок пока нет
- Toxic A History of Nerve Agents From Nazi Germany To Putins Russia 1St Edition Edition Dan Kaszeta Download 2024 Full ChapterДокумент23 страницыToxic A History of Nerve Agents From Nazi Germany To Putins Russia 1St Edition Edition Dan Kaszeta Download 2024 Full Chaptermari.artrip178100% (9)
- LeafanatomyДокумент18 страницLeafanatomyTeach FrezОценок пока нет
- 41 - Type of Shock PDFДокумент2 страницы41 - Type of Shock PDFjamesОценок пока нет
- The Endocrine System: Year 9 Biological ScienceДокумент20 страницThe Endocrine System: Year 9 Biological ScienceSasha VoleskyОценок пока нет
- COVID ProlongadoДокумент22 страницыCOVID ProlongadoSMIBA MedicinaОценок пока нет
- URRAДокумент3 страницыURRAMubashir RafiqueОценок пока нет
- EOT2 BiologyДокумент21 страницаEOT2 BiologyKasumi SatoОценок пока нет
- SaucerizationДокумент12 страницSaucerizationSaran NuiОценок пока нет
- Jaw RelationДокумент48 страницJaw RelationBharanija100% (1)
- Pelvic Floor MuscleДокумент11 страницPelvic Floor MuscleSonia guptaОценок пока нет
- Wingate Anaerobic Test PercentileДокумент10 страницWingate Anaerobic Test PercentileFernando Rojas LopezОценок пока нет
- NCPsДокумент13 страницNCPsRocel DevillesОценок пока нет
- June 2017 QP - Paper 2 Edexcel Biology (A) A-Level PDFДокумент32 страницыJune 2017 QP - Paper 2 Edexcel Biology (A) A-Level PDFIrrationaities324Оценок пока нет
- Qbank FormatДокумент5 страницQbank FormatpashaОценок пока нет
- DwsДокумент27 страницDwsKunni MardhiyahОценок пока нет
- The Heart: Test I: Read and Understand The Question Circle The Best AnswerДокумент2 страницыThe Heart: Test I: Read and Understand The Question Circle The Best AnswerHolly May MontejoОценок пока нет
- Breathing Exercises 0Документ2 страницыBreathing Exercises 0Julyhathul Kuraishi100% (1)