Академический Документы
Профессиональный Документы
Культура Документы
2005 EXEC 136 FocusSummer05
Загружено:
Nur Camelia PragnandaАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
2005 EXEC 136 FocusSummer05
Загружено:
Nur Camelia PragnandaАвторское право:
Доступные форматы
Focus Summer 2005
2/6/05
2:56 pm
Page 2
FOCUS
ISSUE THIRTY FOUR: SUMMER 2005
O C C A S I O N A L U P D AT E F R O M T H E R O YA L C O L L E G E O F O P H T H A L M O L O G I S T S
Removal of the Eye
he prospect of ocular excision fills most patients (and
many ophthalmologists) with horror. Patients fear loss
of visual function and the cosmetic implications of a
glass eye. We may inadvertently reinforce these
negative perceptions when we talk about losing the eye. In fact
the loss of a healthy eye has already occurred. In addition,
some patients may have suffered pain and poor cosmesis for a
long time. We should therefore regard removal of a diseased eye
in a more positive light and concentrate on providing the patient
with an ideal anophthalmic socket. The features of the ideal
socket are comfort, normal lid positions and contours, prosthetic
motility, and the ability to blink and close the lids normally.
Pre-operative care
Pre-operative counselling is vital and should be tailored
according to the patients circumstances. Patients with a blind,
painful eye who request surgery tend not to require as much
counselling as those with newly diagnosed intraocular
malignancy in a seeing eye. Many of the patients anxieties may
be allayed by explaining what he/she should expect during
their stay in hospital; the fact that they may still legally drive, (if
visual function in the remaining eye is normal), and that a
bespoke prosthesis will be fitted which will look like their eye
and have some degree of movement.
Selection of Procedure
Evisceration is usually performed for a blind, painful eye. It is
contraindicated in the presence of intraocular malignancy and
remains controversial where sympathetic ophthalmia is
considered a risk. B-scan ultrasonography should be performed
pre-operatively to exclude an intraocular tumour if clinical
examination cannot.
Enucleation is most commonly performed for intraocular
malignancy, a blind, painful eye, and to prevent sympathetic
ophthalmia following severe trauma.1
Exenteration is a disfiguring procedure reserved mainly for
control of aggressive malignancies (e.g. sebaceous cell
carcinoma, melanoma) or advanced squamous or basal cell
carcinomas with orbital involvement. It may rarely be
performed for pain or disfigurement in benign orbital disease.2
Surgical considerations
Every precaution should be taken to ensure the correct eye is
removed. This should include examination on the operating
table, following draping, with indirect ophthalmoscopy if the
pathology is located in the posterior segment.
Evisceration involves removal of ocular contents, preserving
the sclera, and leaving the extraocular muscles and optic nerve
intact. In order to replace as much volume as possible and
reduce the risk of forward extrusion, superior and inferior flaps
may be created by division of the sclera at the 1 and 7 o'clock
positions, extending posteriorly to the optic nerve. The nerve is
then excised on a small islandof sclera. The implant is inserted
posterior to the flaps, thereby reducing the risk of forward
extrusion, and allowing placement of a larger implant than
otherwise possible. Advantages of evisceration over enucleation
are reduced anatomical disruption, greater motility and often
improved cosmesis as a result.
Enucleation involves removal of the globe from the orbit,
preserving the adnexal tissues except for a stump of anterior
optic nerve. Intraoperative haemorrhage may be reduced by
using a retrobulbar injection of 5 ml of long-acting local
anaesthetic (e.g. chirocaine 7.5%) with adrenaline 1:100,000 after
induction of general anaesthesia. It also reduces the need for
early post-operative analgesia.3 Following removal of the globe,
the orbital implant is inserted into the intraconal space using a
specialised inserter or sterile sheath to avoid dragging of
anterior tissues posteriorly. The extra-ocular muscles may be
sutured together in a cruciate fashion anterior to, or to the
surface of the implant/wrapping (depending on implant type
and use of wrapping material). The posterior Tenons, anterior
Tenons and conjunctiva should be closed with absorbable
sutures in separate layers to discourage implant extrusion. A
plastic conformer and pressure bandaging should be applied for
a minimum of two days.
Exenteration is a highly invasive technique, usually
performed in large, specialist centres and involving a
multidisciplinary team of ophthalmologists, maxillofacial and
neurosurgeons. Further surgical detail is beyond the scope of
this article.
Orbital Implants
There is no consensus on which implant type is optimal,
although it is now widely recognised that failure to replace
orbital volume results in poor motility and cosmesis,
characterised by the Post-Enucleation Socket Syndrome (PESSalso an acronym for its features, Ptosis, Enophthalmos and
Superior Sulcus).
Both integrated (e.g. hydroxyapatite, porous polyethylene)
and non-integrated implants (e.g. acrylic, silicone) are ideally
implanted at the time of enucleation or evisceration, in the
absence of infection.4
As a general rule, the largest implant which may be
accommodated should be implanted such that the volume of the
prosthesis does not exceed 2ml in order to avoid PESS.5 Most
Focus Summer 2005
2/6/05
2:56 pm
Page 1
F O C U S O N : R E M O VA L O F T H E E Y E
adults will accommodate a 22mm for enucleations6, 20mm for
eviscerations.
Wrapping materials are used by some surgeons. Donor sclera
is now rarely employed in the United Kingdom (due to the
theoretical risk of transmissible encephalopathy). Other
materials may be autologous (e.g. sclera from the enucleated
eye, fascia lata) or synthetic (e.g. polyglactin mesh).
Integrated implants have the facility to retain a coupling peg,
which articulates with the prosthesis to increase prosthetic
excursions. Complications such as infection, chronic discharge,
and audible click are common, (37.5% in one series7), and
therefore enthusiasm for pegging has waned in recent years. The
considerable cost of intergrated implants leads some authorities
to argue that an inexpensive non-integrated implant should be
selected if a peg is not planned.
Complications of Implantation
Improper placement of the implant, particularly below inferior
rectus obliterates the inferior fornix and may preclude retention
of a prosthesis. Implants may also migrate or rotate within the
orbit over a number of years, particularly if undersized.
Exposure, following erosion through the superficial layers
occurs most commonly with hydroxyapatite implants due to
their rough surface.1 Vaulting of the prosthesis to relieve friction
over the exposure may be helpful. Burring down of the exposed
convexity of the implant, or patching with materials such as
hard palate or temporalis fascia may be necessary in refractory
cases.
Infection, characterised by chronic discharge and recurrent
pyogenic granulomata may occur in the absence of visible
exposure, and is a serious problem. Sockets where postoperative
inflammation and discharge fails to settle may have been
contaminated at the time of implantation. Integrated implants in
particular allow sequestration of bacteria beyond the reach of
systemic antibiotics and explantation may be necessary.
Extrusion tends to occur with the smooth, non-integrated
implants. It is usually possible to perform secondary
implantation in these instances.
Rehabilitation
The ocularist plays a key role in the postoperative rehabilitation
of the patient. In addition to fitting and maintaining the
prosthesis he/she will offer support and advice long after the
patient has been discharged from the ophthalmology clinic.
However, as the patients first visit to the artificial eye clinic is
not until six weeks postoperatively, good prosthetic handling
technique should be taught prior to discharge from hospital,
preferably with diagramatic or written instructions.
To insert; the prosthesis should be lubricated and slid high
into the superior fornix; a small downward movement will then
place the lower edge inside the inferior fornix. For removal;
gentle, posterior pressure on the lower lid will allow the
prosthesis to prolapse over the lid. Dragging down of the lower
lid during insertion and removal should be discouraged, as
should direct digital contact with the mucous socket lining. The
prosthesis should be worn at all times to discourage socket
shrinkage, and should not be manipulated excessively as this
will cause irritation and increase mucous discharge.
Post-Enucleation Socket Syndrome
The enucleated socket undergoes a number of anatomical soft
tissue changes postoperatively, which are particularly
pronounced if volume replacement is inadequate. These include
backward tilt of the superior fornix, with deepening of the
superior sulcus; shallowing and forward displacement of the
inferior fornix and lower lid stretching. In advanced cases,
contraction of the socket may lead to incomplete closure of the
lids over the prosthesis, upper and lower lid entropion, and
instability or inability to retain a prosthesis.
Correction of PESS involves orbital volume augmentation
(with secondary orbital or subperiosteal implants); increasing
the socket surface area (buccal mucosa or dermis fat graft)
correction of lid malposition and/or laxity (levator aponeurosis
advancement, lateral tarsal strip) or a combination of these.
Some highly motivated patients may be keen to undergo
multiple procedures in order to achieve the best cosmesis
possible. Others may only wish to retain a stable prosthesis.
Clear communication between the patient, surgeon and
ocularist is essential to determine the appropriate measures for
each individual patient.
Conclusion
Ocular excision should be considered primary orbital
reconstructive surgery. Sensitive counselling of patients; careful
consideration in choice of procedure and good surgical
technique minimises psychological trauma and provides the
patient with comfort, good cosmesis and a rapid return to
normal activities.
Julia Sen, Adnexal Fellow
Acknowledgements: Miss Jane Dickinson and Professor Bertil Damato
References:
1. Moshfeghi DM, Moshfeghi AA, Finger PT. Enucleation. Survey of Ophthalmology. 2000;44(4)277-301
2. Rose GE, Wright JE. Exenteration for benign orbital disease. Br J Ophthalmol. 1994 Jan;78(1):14-8
3. Yeatts RP, Doneyhue W, Scuderi PA, Brasington CR, James R Effect of preemptive retrobulbar analgersia on perioperative haemodynamics and
Postoperative pain after enucleation. Ophthal Plast Reconstr Surg. 2004:226-31
4. Smit TJ, Koornneef L, Wonneveld FW, Groet E, Otto AJ. Primary and secondary implants in the anophthalmic orbit. Preoperative and postoperative computed
tomographic appearance. Ophthalmology 1991;98(1):106-10
5. Kaltreider SA, Jacobs JL, Hughes MO. Predicting the ideal implant size before Enucleation. Ophthal Plast Reconstr Surg Jan;15(1):37-43
6. Adenis JP, Robert PY, Boncoeu-Martel MP. Abnormalities of orbital volume. Eur J Ophthalmol 2002 Sep-Oct;12(5):345-50.
7. Jordan DR, Cahn S, Mawn L, et al. Complications associated with pegging Hydroxyapatite orbital implants. Ophthalmology.1999 Mar;106(3):505-12
FOCUS
PUBLISHED BY THE ROYAL COLLEGE OF OPHTHALMOLOGISTS
17 CORNWALL TERRACE LONDON NW1 4QW TEL: 020 7935 0702 FAX: 020 7935 9838
Вам также может понравиться
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Research Article Investigation of Effects of Terpene Skin Penetration Enhancers On Stability and Biological Activity of LysozymeДокумент7 страницResearch Article Investigation of Effects of Terpene Skin Penetration Enhancers On Stability and Biological Activity of LysozymeNur Camelia PragnandaОценок пока нет
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- 10 1080@14764172 2017 1368666Документ30 страниц10 1080@14764172 2017 1368666Nur Camelia PragnandaОценок пока нет
- Long Term Outcome of Secondary Glaucoma Following Vitreoretinal SurgeryДокумент3 страницыLong Term Outcome of Secondary Glaucoma Following Vitreoretinal SurgeryNur Camelia PragnandaОценок пока нет
- Effect of Head and Body Position On Intraocular PressureДокумент5 страницEffect of Head and Body Position On Intraocular PressureNur Camelia PragnandaОценок пока нет
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Jurnal - Paliatif - Rama-SuryaДокумент4 страницыJurnal - Paliatif - Rama-SuryaRama Mikril JulyanaОценок пока нет
- Via Zis 1991Документ2 страницыVia Zis 1991drvivek reddyОценок пока нет
- Housekeeping ManualДокумент22 страницыHousekeeping ManualWe Care Facility Management ServicesОценок пока нет
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Principles of Continuous Renal Replacement Therapy For AkiДокумент43 страницыPrinciples of Continuous Renal Replacement Therapy For AkiFelicia Risca RyandiniОценок пока нет
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Florocol - SPC PDFДокумент2 страницыFlorocol - SPC PDFReal_Bartman0% (1)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- CEIR Registration Form FrontДокумент2 страницыCEIR Registration Form Frontjhon villafuerteОценок пока нет
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Neral Information Title: Venue: Date: Participants:: Project ProposalДокумент2 страницыNeral Information Title: Venue: Date: Participants:: Project ProposalAida Potacag Buasen100% (1)
- Pre Test Health Assessment and The NurseДокумент4 страницыPre Test Health Assessment and The NurseAileen A. MonaresОценок пока нет
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Signs, Symptoms and Health Problems: Etty Komariah S, S.Kp.,M.KepДокумент14 страницSigns, Symptoms and Health Problems: Etty Komariah S, S.Kp.,M.KepHimatul AliyahОценок пока нет
- EAU Guidelines On Urological Infections 2021Документ74 страницыEAU Guidelines On Urological Infections 2021ioana teodorescuОценок пока нет
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- Family Health Nursing PlanДокумент2 страницыFamily Health Nursing PlanGuezil Joy R. DelfinОценок пока нет
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- Medical Helminthology Introduction PDFДокумент13 страницMedical Helminthology Introduction PDFfaiz0% (1)
- Srishti Software Corporate PPT v1 For EmailerДокумент37 страницSrishti Software Corporate PPT v1 For EmailerRafikul RahemanОценок пока нет
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- (For MGH Patients Only) : IV SolutionДокумент1 страница(For MGH Patients Only) : IV SolutionampalОценок пока нет
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Handouts Comminicable Disease by DR SalvadorДокумент24 страницыHandouts Comminicable Disease by DR SalvadorrachaelОценок пока нет
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Section 9 - Students WorksheetДокумент6 страницSection 9 - Students WorksheetEsraa AhmedОценок пока нет
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
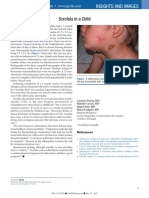
- Scrofula in A Child: Insights and ImagesДокумент1 страницаScrofula in A Child: Insights and Imagesmawarni siahaanОценок пока нет
- Dna BHP AllInOne 2021-04 ENДокумент1 страницаDna BHP AllInOne 2021-04 ENKevin Patrick PalmerОценок пока нет
- Lebanon - Congenital Anomalies Prevalence and Risk FactorsДокумент7 страницLebanon - Congenital Anomalies Prevalence and Risk FactorsAbdelrhman WagdyОценок пока нет
- FAQs KCRKITДокумент2 страницыFAQs KCRKITRohith RohanОценок пока нет
- Chronic Kidney Disease (PSN) 03Документ28 страницChronic Kidney Disease (PSN) 03Logia LegisОценок пока нет
- Practice Parameters For The Management of Hemorrhoids PDFДокумент6 страницPractice Parameters For The Management of Hemorrhoids PDFIoanaОценок пока нет
- Reporting in Nursing: By: ImavikeДокумент16 страницReporting in Nursing: By: ImavikererenrahmawatiОценок пока нет
- Ways Radiation Is Used in Medicine - Cobalt 60 Radiotherapy MachineДокумент22 страницыWays Radiation Is Used in Medicine - Cobalt 60 Radiotherapy MachineKavidu KeshanОценок пока нет
- Chinese-Medical Terminology 13021Документ5 страницChinese-Medical Terminology 13021YS NateОценок пока нет
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Medical Lay TermsДокумент35 страницMedical Lay TermsXuMengОценок пока нет
- Network Lists in UAE - Mar 2015Документ93 страницыNetwork Lists in UAE - Mar 2015Kamran KhanОценок пока нет
- Who BG PDFДокумент21 страницаWho BG PDFAastha AroraОценок пока нет
- EFS-SLB-SRA-002 Risk Assessment For Carpet Cleaning Vacuum & ShampooДокумент4 страницыEFS-SLB-SRA-002 Risk Assessment For Carpet Cleaning Vacuum & Shampoomohammed ayazОценок пока нет
- Community Health Survey: College of NursingДокумент3 страницыCommunity Health Survey: College of NursingMaria Pina Barbado PonceОценок пока нет