Академический Документы
Профессиональный Документы
Культура Документы
Placental Weight and Excess Postpartum Haemorrhage: A Population Study of 308 717 Pregnancies
Загружено:
Gladstone AsadОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Placental Weight and Excess Postpartum Haemorrhage: A Population Study of 308 717 Pregnancies
Загружено:
Gladstone AsadАвторское право:
Доступные форматы
Epidemiology
DOI: 10.1111/j.1471-0528.2011.02954.x
www.bjog.org
Placental weight and excess postpartum
haemorrhage: a population study of 308 717
pregnancies
A Eskild,a,b LJ Vattenc
a
Medical Faculty Division, Department of Obstetrics and Gynaecology, Akershus University Hospital, Lrenskog b Division of Mental Health,
Norwegian Institute of Public Health, Oslo c Department of Public Health, Norwegian University of Science and Technology, Trondheim,
Norway
Correspondence: Prof A Eskild, Department of Obstetrics and Gynaecology, Akershus University Hospital, 1478 Lrenskog, Norway.
Email anne.eskild@medisin.uio.no
Accepted 15 February 2011. Published Online 18 May 2011.
Objective To investigate whether placental weight may be
positively associated with the prevalence of excess postpartum
haemorrhage because large placentas have large surface areas.
Design Registry-based cross-sectional study.
Setting Population study.
Population All singleton deliveries after 21 weeks of gestation in
Norway during 19992004 (n = 308 717).
Methods Data were obtained from the Medical Birth Registry of
Norway, which is based on compulsory notification of births by
the midwife or doctor in charge of the delivery.
Main outcome measure Excess postpartum haemorrhage was
defined as bleeding of 500 ml or more within 2 hours of delivery.
Results There was a gradual increase in the prevalence of excess
for trend, P < 0.05). Having a placenta of 1100 g or more was
associated with 2.5 times (odds ratio 2.54, 95% CI 2.312.79)
higher prevalence than having a placenta of 300499 g,
after adjustment for offspring birthweight, parity, caesarean
section and placenta-related and delivery-related
complications. A large placenta relative to birthweight was also
associated with higher prevalence of excess postpartum
haemorrhage.
Conclusion The size of the placental surface may explain
the positive association of placental weight with the
prevalence of postpartum haemorrhage. In pregnancies with a
large placenta relative to offspring birthweight, other factors that
enhance bleeding may also play a role.
Keywords Birthweight, placental weight, postpartum haemorrhage,
risk factors.
postpartum haemorrhage with increasing placental weight (test
Please cite this paper as: Eskild A, Vatten L. Placental weight and excess postpartum haemorrhage: a population study of 308 717 pregnancies.
BJOG 2011;118:11201125.
Introduction
Excess postpartum haemorrhage is a serious complication
of delivery and a major cause of maternal morbidity and
mortality worldwide.1 To prevent the condition from
occurring, and to provide prompt and accurate treatment,
knowledge of risk factors for excess postpartum haemorrhage is essential.2,3 Previous research suggests that parity,
high offspring birthweight, labour dystocia and caesarean
section are factors that may increase the risk of excess
haemorrhage.49 In addition, complications that are closely
linked to the placenta, including placenta praevia, placental
abruption, as well as a retained placenta and pre-eclampsia,
have been related to excess postpartum haemorrhage.3,610
1120
A large placenta will typically have a large surface area
attached to the uterine wall, and it is therefore conceivable that large placental size is associated with increased
risk of excess postpartum haemorrhage. Such an association may partly explain why women who deliver large
babies are at higher risk of postpartum haemorrhage5
because birthweight and placental weight are strongly correlated.11
We hypothesised that placental weight is positively associated with excess postpartum haemorrhage also after
adjustment for offspring birth size and other risk factors of
excess postpartum haemorrhage. We also studied whether a
large placenta relative to offspring birthweight is associated with excess postpartum haemorrhage. Our study
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
Placental weight and postpartum haemorrhage
Methods
Study population
In Norway, a total of 332 705 deliveries occurred after
16 weeks of gestation from 1999 through 2004. We
restricted the analyses to singleton deliveries occurring after
21 weeks of gestation, leaving 308 717 deliveries eligible for
the study. Data were obtained from the Medical Birth Registry of Norway, which has been in operation since 1967.12
Deliveries after 16 weeks of gestation are compulsorily notified to the registry on standardised forms that are filled in
by the midwife or doctor in charge of the delivery. Since
1999, placental weight has been included in the registration
to the Medical Birth Registry. A large proportion of pregnancies with delivery between 16 and 21 weeks of gestation
had no information available on placental weight. Therefore, we only included pregnancies with delivery after the
21 weeks of gestation.
Study factors
Excess postpartum haemorrhage at delivery is recorded in
the Medical Birth Registry in two separate categories, as
either 500 ml, or as 1500 ml, within 2 hours after delivery. The blood volume is visually estimated by the midwife
or doctor in charge of the delivery. In this study, we defined
500 ml as excess postpartum haemorrhage. However, we
also present the crude prevalence of postpartum haemorrhage 1500 ml related to placental weight. Placental weight
is recorded in grams, and divided into six categories in the
analyses: <300, 300499, 500699, 700899, 9001099 and
1100 g or higher, using the group of 300499 g as the reference. We also constructed a ratio of placental weight and
birthweight by dividing placental weight (g) by birthweight
(g). In the analyses, the ratio was divided into six categories:
<0.14, 0.150.19, 0.200.24, 0.250.29, 0.300.34, or 0.35.
Hence, a relatively high ratio will indicate a large placenta
relative to offspring birthweight.
We also studied the associations of placental weight and
placental/birthweight ratio with postpartum haemorrhage
after adjustment for pregnancy complications that are
strongly related to the placenta and to excess postpartum
haemorrhage. Hence, information on placenta praevia, placental abruption and retained placenta (manual/operative
delivery of the placenta) were included in the analyses as
potentially confounding factors. Other variables that were
taken into account, included parity (coded: 1, 2 or 3 previous deliveries), caesarean section (yes or no), pre-eclampsia (blood pressure >140/90 mmHg and proteinuria, yes or
no), labour dystocia (duration of labour >12 hours after a
cervix opening of 4 cm, yes or no), perineal rupture (yes
or no) and offspring birthweight (coded: <1500, 1500
2999, 30004499, or 4500 g).
Statistical analyses
We estimated the prevalence of excess postpartum haemorrhage (500 and 1500 ml) according to categories of placental weight, and we also estimated the prevalence of
postpartum haemorrhage (>500 ml) according to categories
of the placental weight to birthweight ratio. We used logistic
regression analysis to estimate odds ratios of excess postpartum haemorrhage (500 ml) according to placental weight
and the placental weight to birthweight ratio, and used 95%
CI to indicate precision of the estimates. We estimated both
crude and adjusted odds ratios, where adjustments were
made for birthweight in addition to placenta-related complications and complications related to delivery, as specified
above. The statistical analyses were performed by applying
SPSS version 17.0 (Chicago, IL, USA).
Ethics
The study was approved by the internal review board of
the Medical Birth Registry of Norway, and by the Norwegian Directorate of Health. All data in the study were
anonymous.
Results
Of all women in our study, 13.9% (42 813/308 717) had
postpartum haemorrhage 500 ml, and 1.4% (4306/
308 717) had postpartum haemorrhage 1500 ml. There
was a gradual increase in the prevalence of excess postpartum haemorrhage (500 and 1500 ml) with increasing
placental weight, except for the lowest category of placental
weight (Figure 1). On average, 28.5% of women with placental weight 1100 g had postpartum haemorrhage
500 ml, compared with 11.5% among women with
placental weight between 300 and 499 g (reference). From
the reference category, the prevalence displayed a gradual
30
>500 ml
25
Percent
population included all women with a singleton delivery in
Norway during the 6-year period 19992004.
>1500 ml
20
15
10
5
0
<300
300 to
<500
500 to
<700
700 to
<900
900 to
<1100
>1100
Placental weight (g)
Figure 1. Proportions of women with excess postpartum haemorrhage
according to placental weight.
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
1121
Eskild, Vatten
increase with increasing placental weight (test for trend,
P < 0.05). A similar association was present for postpartum
haemorrhage 1500 ml; 3.2% of the women with placental
weight 1100 g, compared with 1.6% in the reference
group (300499 g), had postpartum haemorrhage 1500 ml
(Figure 1).
For placental weights 1100 g, the crude odds ratio of
excess postpartum haemorrhage (500 ml) was 3.05
(95% CI 2.803.32), compared with the reference weight
(300499 g) (Table 1). After adjustment for placental complications (placenta praevia, placental abruption, retained
placenta, pre-eclampsia), parity, caesarean section, labour
dystocia, perineal rupture and offspring birthweight, the
association was attenuated from 3.05 to 2.54 (95% CI 2.31
2.79). Among women in the lowest category of placental
weight (<300 g), 18.6% had postpartum haemorrhage
500 ml (crude odds ratio, 1.75), but after adjustment for
the potentially confounding factors indicated above, the
association was fully attenuated (adjusted odds ratio 0.95,
95% CI 0.771.09). Additional adjustment for maternal age
did not alter the estimated association of placental weight
with postpartum haemorrhage. In a separate analysis of
deliveries before 37 weeks of pregnancy (17 145 pregnancies, 5.5% of total) the adjusted association of placental
weight with postpartum haemorrhage >500 ml showed estimates that were almost identical to the estimates for the
sample as a whole, except for deliveries with placental
weight >1100 g (odds ratio 1.64, 95% CI 0.952.78).
Other placental factors were also associated with the
prevalence of excess postpartum haemorrhage. Women
with placenta praevia had eight-fold higher odds of excess
haemorrhage, but after adjustment for the other variables
in Table 1, the association was attenuated by nearly 50%
(adjusted odds ratio 4.64, 95% CI 4.005.39). Placental
abruption and retained placenta were also associated with a
high prevalence of excess postpartum haemorrhage, and
the associations were attenuated in multivariable analyses
(Table 1).
The factors related to delivery; caesarean section, labour
dystocia and perineal rupture, were all associated with a
Table 1. Crude and adjusted odd ratios (OR) with 95% confidence intervals (95% CI) for postpartum haemorrhage of more than 500 ml,
according to placental weight and other selected pregnancy factors
Women with PPH/Total (%)
Total
Placental weight (g)
<300
300499
500699
700799
8001099
1100
Placental complications
Placenta praevia*
Placental abruption*
Retained placenta*
Parity
0
1
2
3
Caesarean section*
Pre-eclampsia*
Labour dystocia*
Perineal rupture*
Birthweight (g)
<1500
15002999
30004499
4500
Crude OR
95% CI
Adjusted OR
95% CI
1.75
1.0 Ref
0.96
1.44
2.19
3. 05
1.522.01
0.771.09
0.941.02
1.391.50
2.092.30
2.803.32
0.95
1.0 Ref
1.14
1.59
2.10
2.54
1.091.20
1.511.67
1.982.23
2.312.79
8.41
6.18
8.66
7.309.69
5.546.89
8.239.12
4.64
3.69
6.71
4.005.39
3.284.15
6.357.09
(16.4)
(12.3)
(11.3)
(11.1)
1.0 ref
0.72
0.65
0.64
0.700.74
0.630.67
0.616.75
1.0 ref
0.77
0.69
0.67
0.750.79
0.660.71
0.640.71
002
386
859
769
(32.6)
(21.7)
(28.7)
(22.7)
3.98
1.76
2.75
1.87
3.894.07
1.691.84
2.662.85
1.791.96
3.19
1.33
1.64
2.02
3.113.27
1.271.40
1.581.70
1.922.12
538/2407
4479/37 103
34 110/254 424
3686/14 783
(22.4)
(12.1)
(13.4)
(24.9)
1.0 ref
0.48
0.54
1.15
0.430.53
0.490.59
1.041.28
1.0 ref
0.74
0.92
1.37
0.650.85
0.801.05
1.191.58
42 813/308 717 (13.9)
263/1417
2950/25544
17 042/150 852
16 715/105 596
4876/21 912
967/3396
(18.6%)
(11.5)
(11.3)
(15.8)
(22.3)
(28.5)
452/789 (57.3)
644/1300 (49.5)
3516/6234 (56.4)
22 096/135 093
13 442/108 850
5464/48 517
1811/16 257
14 021/29
2682/12
5989/20
2444/10
All singleton pregnancies in Norway from 1999 through 2004 (n = 308 717).
*Compared to women without the condition.
PPH, postpartum haemorrhage.
1122
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
Placental weight and postpartum haemorrhage
higher prevalence of excess postpartum haemorrhage. After
multivariable adjustment, these associations were also
attenuated, but to a lesser degree than the effects of the
placenta-related complications referred to above.
Nulliparous women had a higher prevalence of excess
postpartum haemorrhage than other women, but there was
no substantial difference between second-time mothers and
women with higher parity. In relation to birthweight, there
was a U-shaped pattern, with higher prevalence of excess
postpartum haemorrhage at both ends of the distribution.
Hence, deliveries of a small (<1500 g) or a large (4500 g)
offspring were both associated with relatively higher prevalence of excess postpartum haemorrhage.
Only 1.4% of the women had postpartum blood loss
1500 ml. Although the statistical power was limited, we
found similar associations with placental weight as those
reported for a postpartum haemorrhage of 500 ml or
higher. Hence, the odds ratio of placental weight >1100 g
was 1.93 (95% CI 1.732.08) compared with the reference
(300499 g). Also the other risk factors displayed similar
patterns. The strongest association was estimated for
retained placenta (odds ratio 10.26, 95% CI 9.4411.17).
In a separate analysis, we assessed the placental weight to
birthweight ratio related to excess postpartum haemorrhage. For the higher ratios (0.2 and above), the prevalence
of excess postpartum haemorrhage was higher in both
crude and adjusted analyses (Table 2), suggesting that a
large placenta relative to birth weight, and not only placental weight in itself, is associated with a relatively higher
prevalence of excess postpartum haemorrhage.
Discussion
In this large population study, there was a positive association
of placental weight with excess postpartum haemorrhage.
The strength of the association was moderately attenuated
after adjustment for parity, offspring birthweight, placenta-related complications and complications related to
delivery, but the gradual increase in excess postpartum
haemorrhage with increasing placental weight persisted
after adjustment for these potentially confounding factors.
We also found that a large placenta relative to the offsprings birthweight was associated with excess postpartum
haemorrhage.
This study was based on information from almost all
singleton deliveries in Norway from 1999 to 2004. Therefore, a skewed selection of the study sample is unlikely.
The measurements of postpartum haemorrhage are based
on visual estimations and therefore rather crude.13,14
Despite the inherent imprecision of the measurements, the
discrepancy between the true and the reported blood loss is
likely to be proportional.13 In addition, there is little reason
to suspect that the reported blood loss depended on the
size of the placenta. Any misclassification of blood loss
across the categories we have used in our study will generally decrease rather than increase the estimated associations.
We had information on placenta-related complications that
were taken into account in the analyses. After adjustment
for these pregnancy complications, the strong association
of placental weight with the prevalence of excess postpartum haemorrhage was partly attenuated, but remained and
showed a gradual increase in excess haemorrhage with
increasing placental weight.
We are only aware of one previous study that assessed
the association of placental weight with the prevalence of
excess postpartum haemorrhage.15 That study also reported
a positive association. However, the study included
524 women and was aimed at studying delivery outcomes
according to methods of labour induction. Previously,
high birthweight has been associated with higher risk of
Table 2. Crude and adjusted odds ratios (OR) with 95% confidence intervals (95% CI) for postpartum haemorrhage of more than 500 ml
according to the ratio of placental weight and birth weight (in grams). A high ratio indicates a large placental weigh relative to birth weight.
All singleton pregnancies in Norway from 1999 through 2004 (n = 308 717)
Placental weight/birthweight
Total
<0.15
0.15 to
0.20 to
0.25 to
0.30 to
0.35
<0.20
<0.25
<0.30
<0.35
Women with PPB/Total (%)
42 813/308 717
3814/30 272
22 469/179 236
13 414/84 608
2461/11 765
395/1706
260/1130
(13.9)
(12.6)
(12.5)
(15.9)
(20.9)
(23.2)
(23.0)
Crude OR
95% CI
Adjusted OR*
95% CI
1.0 ref
0.99
1.31
1.84
2.09
2.07
0.951.03
1.261.36
1.741.94
1.852.35
1.802.39
1.0 ref
1.00
1.18
1.45
1.32
1.40
0.961.04
1.141.23
1.361.53
1.171.50
1.201.63
*Adjustment was made for placenta praevia, placental abruption, retained placenta, parity, caesarean section, pre-eclampsia, labour dystocia and
perineal rupture.
PPH, postpartum haemorrhage.
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
1123
Eskild, Vatten
postpartum haemorrhage.35,8,15 We also found a positive
association of high birthweight, but after adjustment for
placental weight, the association of birthweight was
strongly attenuated. It has been suggested that impaired
uterine contractions may occur more often after deliveries
of large babies, and one consequence of this could be a
longstanding postpartum haemorrhage. Also in pregnancies
with labour dystocia, uterine contractions after delivery
may be impaired.6,15 Our study included most obstetric
factors that have been associated with excess postpartum
haemorrhage, and the independent effect of each of these
factors is presented. The placenta-related factors, placental
abruption, retained placenta and placenta praevia, were
most strongly associated with excess postpartum haemorrhage, also after mutual adjustment for the other risk factors. We found a relatively higher prevalence of excess
postpartum haemorrhage in first-time mothers, also after
adjustment for pregnancy complications that are associated
with both parity and postpartum haemorrhage (preeclampsia, caesarean delivery and perineal rupture). One
explanation for the higher prevalence of postpartum haemorrhage in first-time mothers may be a tendency for a prolonged third stage of labour in these deliveries.7
Large placentas have a relatively large surface area
attached to the uterine wall. For this reason, detachment of
a large placenta may reflect a larger potential for excess
bleeding compared with the detachment of a small placenta. The higher blood loss associated with a large placenta could also be explained by impaired uterine
contractions after delivery. If pregnancies with a large placenta have impaired contractions, placental detachment
may be delayed, and increased bleeding may be more likely
to occur, both from the uterine wall and from the placenta
itself. Unfortunately, there was no available information on
the timing of placental delivery in relation to the delivery
of the infant.
We also found that a high placental weight relative to
birthweight was associated with excess postpartum haemorrhage, but the interpretation of this finding is not obvious.
Nonetheless, it is possible that maternal conditions, not
necessarily related to pregnancy, may enhance the risk of
bleeding in these pregnancies. For instance, the mother
may have an underlying bleeding disorder that will increase
her risk of excess postpartum haemorrhage16 and simultaneously cause a disproportional placental weight to birthweight ratio. It is also possible that certain pregnancy
complications may initiate enlargement of the placenta relative to the fetus, and simultaneously deactivate the maternal clotting system. Hence, placental enlargement and
reduced blood clotting could represent mechanisms that
will increase placental blood flow to secure survival of a
threatened fetus. Similar reasoning could be applied to the
increased risk of postpartum haemorrhage in pregnancies
1124
involving pre-eclampsia.10 For example, the anti-angiogenic
factor sFlt1-1, which has been closely linked to pre-eclampsia and small-for-gestational-age offspring,1719 has also
been associated with excess postpartum haemorrhage.20
The high prevalence of postpartum haemorrhage after
delivery of very small infants (birthweight <1500 g), independent of placental weight, suggests that factors associated
with a pathological pregnancy may increase the risk of
postpartum haemorrhage. Hence, our findings may be
important for better understanding the underlying causes
of postpartum haemorrhage than in predicting risk. There
may be yet unknown factors that are associated with
increased risk of postpartum haemorrhage in pregnancies
with a large placenta relative to birthweight.
In conclusion, our results suggest that women with a
large placenta have a higher prevalence of excess postpartum haemorrhage than other women. Having a large placenta relative to offspring birthweight was also associated
with a higher prevalence of postpartum haemorrhage.
In the clinical setting, these findings may be useful when
caring for women after delivery.
Disclosure of interest
There is no conflict of interest related to this work.
Contribution to authorship
AE conceived the idea, analysed and interpreted the data
and wrote the paper. LJV interpreted the data and wrote
the paper.
Details of ethics approval
The Medical Birth Registry of Norway is approved by the
Parliament of Norway. We used anonymous data.
Funding
The study was financially supported by Akershus University
Hospital and by the Norwegian University of Science and
Technology.
Acknowledgements
We are indebted to the women who provided the information that enabled this study. j
References
1 Potts M, Hemmerling A. The worldwide burden of postpartum
haemorrhage. Policy development where inaction is lethal. Int J
Gynaecol Obstet 2006;94 (Suppl 2):S11621.
2 Carroli G, Cuesta C, Abalos E, Gulmezoglu AM. Epidemiology of
postpartum haemorrhage: a systematic review. Best Pract Res Clin
Obstet Gynaecol 2008;22:9991012.
3 Lu MC, Korst LM, Fridman M, Muthengi E, Gregory KD. Identifying
women most likely to benefit from prevention strategies for postpartum hemorrhage. J Perinatol 2009;29:4227.
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
Placental weight and postpartum haemorrhage
4 Sosa CG, Althabe F, Belizan JM, Buekens P. Risk factors for postpartum hemorrhage in vaginal deliveries in a Latin-American population. Obstet Gynecol 2009;113:13139.
5 Siggelkow W, Boehm D, Skala C, Grosslercher M, Schmidt M,
Koelbl H. The influence of macrosomia on the duration of labor, the
mode of delivery and intrapartum complications. Arch Gynecol
Obstet 2008;278:54753.
6 Allen VM, Baskett TE, OConnell CM, McKeen D, Allen AC. Maternal and perinatal outcomes with increasing duration of the second
stage of labour. Obstet Gynecol 2009;113:124858.
7 Combs CA, Murphy EL, Laros RK Jr. Factors associated with postpartum hemorrhage with vaginal birth. Obstet Gynecol 1991;77:6976.
8 Al-Zirgi I, Vangen S, Forsen L, Stray-Pedersen B. Prevalence and risk
factors of severe obstetric haemorrhage. BJOG 2008;115:126572.
9 Naef RW, Chauhan SP, Chevalier SP, Roberts WE, Meydrech EF,
Morrison JC. Prediction of hemorrhage at cesarean delivery. Obstet
Gynecol 1994;83:9236.
10 Eskild A, Vatten LJ. Abnormal bleeding associated with preeclampsia: a population study of 315,085 pregnancies. Acta Obstet Gynecol Scand 2009;88:1548.
11 Eskild A, Vatten LJ. Do pregnancies with preeclampisa have larger
placentas? BJOG 2010;117:15216.
12 Irgens LM. The Medical Birth Registry of Norway. Epidemiological
research and surveillance throughout 30 years. Acta Obstet Gynecol
Scand 2000;79:4359.
13 Duthie SJ, Ven D, Yung GL, Guang DZ, Chan SY, Ma HK. Discrepancy between laboratory determination and visual estimation of
14
15
16
17
18
19
20
blood loss during normal delivery. Eur J Obstet Gynecol Reprod Biol
1991;38:11924.
Zhang WH, Deneux-Tharaux C, Brocklehurst P, Juszczak E, Joslin M,
Alexander S, et al. Effect of a collector bag for measurement of
postpartum blood loss after vaginal delivery: cluster randomised trial
in 13 European countries. BMJ 2010;340:c293.
Phillip H, Fletcher H, Reid M. The impact of induced labour on postpartum blood loss. J Obstet Gynaecol 2004;24:125.
Chauleur C, Cochery-Nouvellon E, Mercier E, Ava G, Fabbro-Peray P,
Mismetti P, et al. Some hemostasis variables at the end of the population distributions are risk factors for severe postpartum hemorrhages. J Thromb Haemost 2008;6:206774.
Levine RJ, Maynard SE, Qian C, Lim KH, England LJ, Yu KF, et al.
Circulating angiogenic factors and the risk of preeclampsia. N Engl J
Med 2004;350:67283.
Vatten LJ, Eskild A, Nilsen TI, Jeansson S, Jenum PA, Staff AC.
Changes in circulating level of angiogenic factors from the first to
second trimester as predictors of preeclampsia. Am J Obstet Gynecol
2007;196:23945.
Asvold BO, Vatten LJ, Romundstad PR, Jenum PA, Karumanchi SA,
Eskild A. Angiogenic factors in maternal circulation and the risk of
severe fetal growth restriction. Am J Epidemiol 2011;173:6309.
Eskild A, Jeansson S, Jenum PA, Staff AC, Thadhani R, Karumanchi
A, et al. Levels of angiogenic factors in pregnancy and postpartum
bleeding. Acta Obstet Gynecol Scand 2008;87:10813.
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
1125
Вам также может понравиться
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- KadДокумент25 страницKadraisaОценок пока нет
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Syok KardiogenikДокумент31 страницаSyok KardiogenikcantikarevieraОценок пока нет
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- P Knowlesi PDFДокумент3 страницыP Knowlesi PDFNurbieber Saiianklylavrilavigne BieberОценок пока нет
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (399)
- Osteoporosis F DHДокумент39 страницOsteoporosis F DH95kodok85Оценок пока нет
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- Telmisartan AmlodipineДокумент10 страницTelmisartan AmlodipineDeby Tri Widia LestariОценок пока нет
- HonkДокумент11 страницHonkYozhanОценок пока нет
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Disease of Adrenal Gland: Dr. Fatimah Eliana, SPPD, KemdДокумент57 страницDisease of Adrenal Gland: Dr. Fatimah Eliana, SPPD, KemdDeby Tri Widia LestariОценок пока нет
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- GPQ 20 Jun08 PDFДокумент4 страницыGPQ 20 Jun08 PDFDeby Tri Widia LestariОценок пока нет
- Kuliah Obat Esensial Dan FormulariumДокумент12 страницKuliah Obat Esensial Dan FormulariumNita RahmatunnisaОценок пока нет
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Japan Earthquake HighlightedДокумент3 страницыJapan Earthquake HighlightedDeby Tri Widia LestariОценок пока нет
- 0704 06Документ4 страницы0704 06Deby Tri Widia LestariОценок пока нет
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Konsumsi Makanan Dan Kejadian Anemia Pada Siswi Salah Satu SMP Di Kota MakassarДокумент4 страницыKonsumsi Makanan Dan Kejadian Anemia Pada Siswi Salah Satu SMP Di Kota MakassarTegoeh RizkiОценок пока нет
- Sexual Violence Sept 2014 152Документ6 страницSexual Violence Sept 2014 152Deby Tri Widia LestariОценок пока нет
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- Headache QuestionnaireДокумент10 страницHeadache QuestionnairePerisha VeeraОценок пока нет
- 15Документ5 страниц15Deby Tri Widia LestariОценок пока нет
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
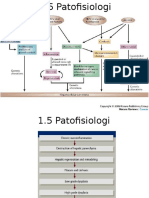
- 1.5 Patofisiologi Karsinoma HepatoselulerДокумент2 страницы1.5 Patofisiologi Karsinoma HepatoselulerDeby Tri Widia LestariОценок пока нет
- NAP For Web - Headache Diagnosis TestingДокумент38 страницNAP For Web - Headache Diagnosis TestingDeby Tri Widia LestariОценок пока нет
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- VaksinasiДокумент9 страницVaksinasiDeby Tri Widia LestariОценок пока нет
- Migraine Prevalence, Alexithymia, and Post-Traumatic StressДокумент9 страницMigraine Prevalence, Alexithymia, and Post-Traumatic StressDeby Tri Widia LestariОценок пока нет
- IndianJMedSci6611-3703196 101711Документ12 страницIndianJMedSci6611-3703196 10171195kodok85Оценок пока нет
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Life Stress TestДокумент2 страницыLife Stress Test95kodok85Оценок пока нет
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Stress Dan AnxietasДокумент4 страницыStress Dan AnxietasIhsan Rasyid YuldiОценок пока нет
- Prevalence of Stress Among Medical Students in Jizan University Kingdom of Saudi ArabiaДокумент7 страницPrevalence of Stress Among Medical Students in Jizan University Kingdom of Saudi ArabiaDeby Tri Widia LestariОценок пока нет
- Epidemiological Investigation of A Temporal Increase in Atonic Postpartum Haemorrhage A Population-Based Retrospective Cohort StudyДокумент10 страницEpidemiological Investigation of A Temporal Increase in Atonic Postpartum Haemorrhage A Population-Based Retrospective Cohort StudyDeby Tri Widia LestariОценок пока нет
- Maternal Near Miss in Rural Hospital SudanДокумент4 страницыMaternal Near Miss in Rural Hospital SudanVikas LonikarОценок пока нет
- Konsumsi Makanan Dan Kejadian Anemia Pada Siswi Salah Satu SMP Di Kota MakassarДокумент4 страницыKonsumsi Makanan Dan Kejadian Anemia Pada Siswi Salah Satu SMP Di Kota MakassarTegoeh RizkiОценок пока нет
- Prevalence of Anemia Risk Factors in Pregnant Women in Kerman, IranДокумент4 страницыPrevalence of Anemia Risk Factors in Pregnant Women in Kerman, IranDeby Tri Widia LestariОценок пока нет
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Exsanguinated Uterus After Massive Atonic Postpartum HaemorrhageДокумент4 страницыExsanguinated Uterus After Massive Atonic Postpartum HaemorrhageDeby Tri Widia LestariОценок пока нет
- Postpartum Haemorrhage in Midwifery Care in The Netherlands Validation of Quality Indicators For Midwifery GuidelinesДокумент6 страницPostpartum Haemorrhage in Midwifery Care in The Netherlands Validation of Quality Indicators For Midwifery GuidelinesDeby Tri Widia LestariОценок пока нет