Академический Документы
Профессиональный Документы
Культура Документы
Cardio CFD
Загружено:
aeroacademicАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Cardio CFD
Загружено:
aeroacademicАвторское право:
Доступные форматы
REVIEW
Print ISSN 1738-5520 / On-line ISSN 1738-5555
Copyright 2011 The Korean Society of Cardiology
http://dx.doi.org/10.4070/kcj.2011.41.8.423
Open Access
Computational Fluid Dynamics in Cardiovascular Disease
Byoung-Kwon Lee, MD
Division of Cardiology, Department of Internal Medicine, Gangnam Severance Hospital, Yonsei University College of Medicine, Seoul, Korea
ABSTRACT
Computational fluid dynamics (CFD) is a mechanical engineering field for analyzing fluid flow, heat transfer, and associated
phenomena, using computer-based simulation. CFD is a widely adopted methodology for solving complex problems in
many modern engineering fields. The merit of CFD is developing new and improved devices and system designs, and optimization is conducted on existing equipment through computational simulations, resulting in enhanced efficiency and lower operating costs. However, in the biomedical field, CFD is still emerging. The main reason why CFD in the biomedical field
has lagged behind is the tremendous complexity of human body fluid behavior. Recently, CFD biomedical research is more
accessible, because high performance hardware and software are easily available with advances in computer science. All CFD
processes contain three main components to provide useful information, such as pre-processing, solving mathematical equations, and post-processing. Initial accurate geometric modeling and boundary conditions are essential to achieve adequate results. Medical imaging, such as ultrasound imaging, computed tomography, and magnetic resonance imaging can be used
for modeling, and Doppler ultrasound, pressure wire, and non-invasive pressure measurements are used for flow velocity and
pressure as a boundary condition. Many simulations and clinical results have been used to study congenital heart disease,
heart failure, ventricle function, aortic disease, and carotid and intra-cranial cerebrovascular diseases. With decreasing hardware costs and rapid computing times, researchers and medical scientists may increasingly use this reliable CFD tool to deliver accurate results. A realistic, multidisciplinary approach is essential to accomplish these tasks. Indefinite collaborations
between mechanical engineers and clinical and medical scientists are essential. CFD may be an important methodology to
understand the pathophysiology of the development and progression of disease and for establishing and creating treatment
modalities in the cardiovascular field. (Korean Circ J 2011;41:423-430)
KEY WORDS: Hydrodynamics; Viscosity; Cardiovascular diseases.
What is Computational Fluid Dynamics?
it is a widely adopted methodology for solving complex problems in many modern engineering fields. CFD is becoming
a vital component in the design of industrial products and
systems. Examples are aerodynamics and hydrodynamics of
vehicles, power plants including turbines, electronic engineering, chemical engineering, external and internal environmental architectural design, marine and environmental engineering, hydrology, meteorology, and biomedical engineering.1)2)
The merit of CFD is developing new and improved devices
and system designs, and optimization is conducted on existing equipment through computational simulations resulting
in enhanced efficiency and lower operating costs. However,
CFD is still emerging in the biomedical field. The main reason why CFD in the biomedical field has lagged behind is the
tremendous complexity of human anatomy and human body
fluid behavior. Recently, biomedical research with CFD is
more accessible because high performance hardware and software are easily available with advances in computer science.1)
Computational fluid dynamics (CFD) is a mechanical engineering field for comprehensively analyzing fluid flow,
heat transfer, and associated phenomena with the use of computer-based simulation. The technique is very powerful and
spans a wide range of areas. In the beginning, CFD was primarily limited to high-technology engineering areas-, but now
Correspondence: Byoung-Kwon Lee, MD, Division of Cardiology, Department of Internal Medicine, Gangnam Severance Hospital, Yonsei
University College of Medicine, 211 Eonju-ro, Gangnam-gu, Seoul 135720, Korea
Tel: 82-2-2019-3307, Fax: 82-2-3463-3882
E-mail: cardiobk@yuhs.ac
The author has no financial conflicts of interest.
cc This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
423
Computational Fluid Dynamics in CV Disease
The study of fluid mechanics includes the study of fluids
either in motion (fluid in dynamic mode) or at rest (fluid in
stationary mode). CFD is usually dedicated to fluids that are
in motion, and how the fluid flow behavior influences processes. Additionally, the physical characteristics of fluid motion
can usually be described through fundamental mathematical equations, usually in partial differential form, which govern the process of interest and are often called governing equations. These mathematical equations are solved by being
converted by computer scientists using high-level computer
programming languages. The computations reflect the study
of fluid flow through numerical simulations, which involves
employing programs performed on high-speed digital computers to attain numerical solutions.2)
Using CFD, medical researchers can gain an increased knowledge of how body fluids and system components are expected to perform, to make the required improvements for
bio-fluid physiology studies, and to develop medical devices.
CFD offers chances for simulation before a real commitment
is undertaken to execute any medical design alteration and
may provide the correct direction to develop medical interventions.
Computational Fluid
Dynamics Components
Computational fluid dynamics is usually performed with
use of commercial CFD codes. CFD codes are structured by
numerical algorithms that consider fluid-flow problems. All
CFD codes must contain three main components to provide
useful information; 1) a pre-processor, 2) a solver, and 3) a
post-processor.1)
Pre-processor
Pre-processing consists of inputting a fluid flow problem
into a CFD program. This includes defining the geometry of
the region of interest, grid or mesh generation, selection of the
physical and chemical phenomena that need to be modeled,
a definition of fluid properties, and specification of appropriate boundary conditions at the inlet and outlet. The larger the
number of cell grids the better the solution accuracy. The accuracy of a solution and the required time for computational
problem solving are dependent on grid fineness. Most of the
time spent is devoted to this process. In cardiovascular systems, computational imaging tools may confer the grid generation information, but limitations are that the resolution
of current imaging tools is still low and geometry varies according to the cardiac cycle. Blood acts as a non-Newtonian
fluid, because blood has varying viscosities according to its
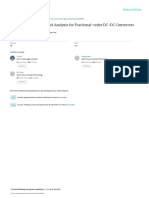
shear rate. Fig. 1 shows the correlation between blood viscosity and shear rate.3-5) Thus, the correct viscosity model using a mathematical equation should be selected according to
Viscosity
424
Newtonian fluid
Non-newtonian fluid
Shear rate
Fig. 1. Viscosity of Newtonian and non-Newtonian fluids according to shear rate.
the range of shear rates. The energy conservation law of fluid
motion is an important consideration for basic concepts. Boundary conditions, such as blood pressure, blood flow velocity, and temperature are readily available from invasive and
non-invasive measurements based on the region of interest.
Another essential consideration is that these boundary conditions also vary according to the cardiac cycle and the unique conditions of coronary circulation. Fig. 2 shows a sample
of these pressure and velocity profiles during cardiac cycles
for modeling and CFD.6)
Solver
Numerical solution techniques are available such as finite
difference, finite element, finite volume, and spectral methods.
Each has a distinct numerical technique, but the basis of the
solver is to perform an approximation of unknown flow variables by means of simple functions, discretisation by substitution of the approximations into the governing flow, and an
algebraic solution. If the user uses a solution technique, the
time spent depends upon the calculating capacity of the computer. Usually, the finite volume method is adopted for cardiovascular systems.
Post-processor
The object of this process is to visualize the computational
results. Many visualization tools have been developed, including domain geometry and grid display, vector plots, line and
shaded contour plots, two-dimensional and three-dimensional surface plots, particle tracking, and color postscript outputs. After this process, the researcher can easily understand
the simulation results. For example, the changes in blood
flow profiles, pressure distribution, wall shear stress (WSS),
oscillating shear index (OSI), and shear rate can be visual-
Byoung-Kwon Lee
425
Abdominal
Aorta
Fig. 2. Pressure and velocity of the coronary artery and aorta as a boundary condition in the bifurcation model (Lee et al.). A: left coronary
artery. B: abdominal aorta.
ized using color rendering techniques. Furthermore, a cyclic
motion view can be obtained during cardiac cycles.
Applications in the Cardiovascular
System
Recently, medical researchers have used simulation tools
to assist in predicting the behavior of circulatory blood flow
inside the human body. Computational simulations provide
invaluable information that is extremely difficult to obtain
experimentally and is one of the many CFD sample applications in the biomedical area in which blood flow through an
abnormal artery can be predicted. CFD analysis is increasingly performed to study fluid phenomena inside the human
vascular system. Medical simulations of circulatory function
offer many benefits. They can lower the chances of postoperative complications, assist in developing better surgical procedures, and deliver a good understanding of biological processes, as well as more efficient and less destructive medical
equipment such as blood pumps. Furthermore, medical applications using CFD have expanded not only into the diseased clinical situation, but also into health life supportives,
such as sport medicine and rehabilitation. Several examples
are discussed as follows.
Coronary artery disease: atherosclerosis
Although many systemic risk factors predispose development of atherosclerosis, it preferentially affects certain regions
of circulation, suggesting that lesion-prone areas may at least
in part be due to biomechanically related factors. Furthermore, luminal hemodynamics, such as flow velocity, pressure changes, and WSS have been suggested as other risk
factors for developing coronary atherosclerosis.7-9)
Information regarding the spatial distribution of intraluminal hemodynamics of the coronary vascular tree are available using CFD.10-14) Fig. 3 shows an example of performing
CFD from pre-processing to post-processing. At first, a mesh
or grid of region of interest is generated from the coronary
extract images of computerized tomogram. The researchers
might use any three dimensional medical images. The Digital
Imaging and Communications in Medicine (DICOM) files
should be converted into a file which can be used in a soft ware
analyzing three dimensional vector information. All the digitalized data, such as velocity and pressure information according as cardiac cycle as a boundary condition were selected to put into an appropriate algebraic solution. And, the
next step is mathematic solving process by the computer. At
this process, mechanical engineers and medical scientists should discuss about all the clinical situations for selecting an
appropriate viscosity models due to non-Newtonian fluid
analysis, governing equations. Final step is visualization process for user. There are so many representative processing
results, such as pressure profiles, velocity profiles, particle
tracing, time-averaged wall shear stress (TAWSS), OSI, etc.
This figure shows high TAWSS, OSI at bifurcation. TAWSS
shows higher at bifurcation apex, but OSI shows higher at
lateral side of side branch.
Fig. 4 shows an final example of flow velocity and WSS profiles in a artificial coronary artery model.9) Low WSS and
low flow velocity are formed at the outer wall of a curved artery at the bifurcation with the inner wall. Spatial fluctuations in flow-velocity and recirculation occur at the curved
outer wall of the left anterior descending coronary artery
and are due to differences in flow-velocity and shear stress,
particularly during the declaration phase of pulsatile flow.
These results suggest that hemorheologic properties may be
a part of the atherogenic process in the bifurcated and
curved areas.
This kind of study might be applied to a modified coronary artery geometry model or varying viscosity models.13)14)
Furthermore, the effect of percutaneous coronary intervention15)16) and coronary bypass grafts17)18) can be simulated and
suggest the best method of intervention. CFD may be useful
to understand the biomechanical pathophysiology of atherosclerosis and its complications.
426
Computational Fluid Dynamics in CV Disease
1. Preprocessing
2. Soving with an appropriate algebraic solution with computer; an example.
Carreau model of following equation for relationship between shear rate and viscosity
The following continuity equation and Navier-Stokes equation were used as governing equations for the numerical analysis, where , u, p,
and i, j were the density, velocity vector, pressure, apparent viscosity, and tensor indexes, respectively.
3. Post-processing; time averaged wall shear stress and oscillating shear index
Fig. 3. An example of CFD in left coronary artery. Finite volume method, adapting Rhie-Chow algorithm, computed with ANSYS CFX package program (Anflux, Seoul, Korea) in SUN SPARC station 20 (Sun Korea Co., Seoul, Korea) were used. At first, a mesh or grid of region of
interest is generated from the coronary extract images of computerized tomogram. All the digitalized data velocity, pressure information according as cardiac cycle as a boundary condition was selected to put into an appropriate algebraic solution. And, the next step is mathematic solving process by the computer. At this process, mechanical engineers and medical scientists should discuss about all the clinical
situations for selecting an appropriate algebraic solution. Final step is visualization process for user. There are so many representative processing results, such as pressure profiles, velocity profiles, particle tracing, time-averaged wall shear stress (TAWSS), oscillating shear index (OSI), etc. This figure shows high TAWSS, OSI at bifurcation.
Congenital heart disease; Fontan circulation
Fontan circulation, first described by Fontan and Baudet,19)
is characterized by the absence of a right ventricle and functions under unique hemodynamics. The key targets of geometric correction of Fontan procedure are the separation of
systemic and pulmonary venous return and establishing the
pathway of a passive, direct, and unobstructed connection between the systemic venous return and the pulmonary artery
(PA) for treating single ventricle physiology, as one example
of congenital heart disease.
While the Fontan procedure is a classic treatment procedure for a functional single ventricle in patients with congenital heart diseases, it has a potentially harmful effect for normal circulation. The absence of a right ventricle induces a pressure elevation in the venous system. The basic pathophysiological mechanisms originate from increased central venous
pressure and the superior vena cava (SVC) and inferior vena
cava (IVC).
Byoung-Kwon Lee
(a) Acceleration period
427
(b) Deceleration period
Fig. 4. The velocity vectors (upper) and distribution of wall shear stress (lower) in the coronary artery model. Prominent abrupt changes in
velocity and wall shear stress at the outer wall around the branched site are noted during the deceleration period.
Elevated central venous pressure is poorly tolerated over
time, particularly in the IVC, and has deleterious effects on
liver and splanchnic circulation. Protein-losing enteropathy
and plastic bronchitis20) characterize the worst outcomes. At
the liver level, elevated central venous pressure may induce
complex liver dysfunction and stimulate angiogenesis factors21) favoring a venovenous anastomosis, pulmonary venous fistula, and, potentially, aortopulmonary collateral anastomoses. At the lung level, the upper PA branches are poorly or not perfused, and the lymphatic circulation is globally
impaired.22) The single ventricle faces a significant increase
in total systemic resistance because it needs to push against
not only the usual systemic resistance but also lung resistance.
As a consequence, the systemic ventricle becomes hypertrophied, with elevated end-diastolic pressure, which diminishes
diastolic performance.23)24) Several studies have focused on
solving these problems.25-29)
Computational fluid dynamics was performed after artificially modeling the Fontan circulation using medical information. Fig. 5 shows the velocity profiles at maximal flow
among cardiac cycle time periods. Significantly increased
flows were driven from the SVC, particularly during inspiration, indicating that unmixed blood flow to the PA and blood
flow in the IVC may be more congested during inspiration
than during expiration. During standing and inspiration, blood flow profiles aggravate the stagnation of systemic venous
Fig. 5. Maximal velocity profile at inspiration (A) and expiration (B)
in the supine position and inspiration (C) and expiration (D) in the
standing position at an model of Fontan circulation. Tube structures
represent cross-shaped reconstructed model of superior vena
cava, inferior vena cava, right pulmonary artery, and left pulmonary
artery at upper, lower, left and right tube.
blood flow return and failure of the blood mixing function,
suggesting that an artificial pumping device is essential for
correcting Fontan circulation failure.
428
Computational Fluid Dynamics in CV Disease
C1: Proximal compliance
L: Inertia of blood
C2: Distal compliance
Rs: Peripheral resistance
160
150
Aorta
LV
P1: Proximal blood pressure
Qin
P1
Q1
Qin-Q1
Flow rate (mL/s)
Hypothetical arterial system
P2: Distal blood pressure
P2
Q2
eq1
Q1-Q2
eq3
C2
130
120
110
100
eq2
C1
140
Rs
90
0.1
0.2
0.3
0.4
0.5
0.6
0.7
0.8
Time (s)
Fig. 7. Proximal (Q1) and distal (Q2) flow rates in the left ventricle
calculated with the Herschel-Bulkley equation.
Fig. 6. Modified Windkessel model for the human arterial system
(Qin, Q1, and Q1 are defined as the flow rate exiting from the left
ventricle during systole, the flow rate passing through the peripheral system, and the flow rate passing through the distal system,
respectively. Similarly, p1 and p2 are the pressures measured at
the proximal and distal locations, respectively. C1 and C2 are proximal and distal compliances where L corresponds to the inertia of
blood.
Work of the heart
This is another example of using CFD as a diagnositic tool
for evaluating heart function.
Work of the heart (WHO) is calculated using a pressurevolume curve. Some new indirect diagnostic tools are available to evaluate the WOH. The modified Windkessel model
was used with blood viscosity models to develop a mathematical model for estimating WOH utilizing the pulse waves between two points of a vessel. The human arterial system is a
network of vessels that converts intermittent flow of the heart into steady flow through the capillaries and venous system.
The modified Windkessel model is a type of lumped parameter model that allows simulation of blood flow in the entire
circulatory system as an electrical circuit (Fig. 6).
In this figure, Qin, Q1, and Q1 are defined as the flow rate
exiting from the left ventricle during systole, the flow rate passing through the peripheral system, and the flow rate passing
through the distal system, respectively. Similarly, p1 and p2 are
the pressures measured at the proximal and distal locations,
representatives of central and peripheral blood pressure, respectively. Moreover, C1 and C2 are proximal and distal
compliances, where L corresponds to the inertia of blood (L=
0.017 mmHgs2/mL). Flow rate in the left ventricle can be calculated with the mathematical fluid analysis shown in Fig. 7
by measuring blood pressure curves at two points in the peripheral arteries (brachial and radial arteries).30) The blood
viscosity model is essential to solve the problem of an increased burden of work on the heart, so further study will be needed to verify which viscosity model results are similar compared to in vivo results. However, this type of study might
suggest the possibility of developing non-invasive devices
for measuring WHO.31)32)
Other cardiovascular systems
Physiology and diseases of the aorta, carotid, and cerebral
arteries are also studied with CFD. CFD is being increasingly employed to understand carotid stenosis and its biological
properties according to geometric risks,33-36) or via virtual prototyping to recommend the best design for surgical reconstruction during a carotid endarterectomy,37) and conjunctional research magnetic resonance images.37-42) Furthermore,
CFD is being used to better understand blood flow through
an aneurysm in the abdominal artery, and the development
and progression of aortic dissection.43-47) In intracranial cerebral artery disease, CFD is also used to identify the geometric
and hemodynamic risks for rupture of a cerebral aneurysm
and for stent design for a cerebral aneurysm.48-52)
Computational Fluid Dynamics
Advantages and Limitations
There are many advantages when considering CFD. Theoretical development in the computational sciences focuses on
the construction and solution of governing equations and the
study of various approximations to these equations. CFD complements experimental and analytical approaches by providing an alternative cost-effective means of simulating real fluid
flow, particularly in human body fluids. CFD has the capacity to simulate flow conditions that are not reproducible during experimental tests found in geophysical and biological
fluid dynamics, such as scenarios that are too huge, too remote, or too small to be simulated experimentally. Furthermore, CFD provides rather detailed visual and comprehensive information when compared to analytical and experimental fluid dynamics.
Although CFD is advantageous, it cannot easily replace experimental testing as a method to gather information for
Byoung-Kwon Lee
design purposes. Despite its many advantages, the researcher must consider the inherent limitations of applying CFD.
Numerical errors occur during computations; therefore, there
will be differences between the computed results and reality.
Visualizing numerical solutions using vectors, contours, or
animated movies of unsteady flow are the most effective ways
to interpret the huge amount of data generated from numerical calculations. Wonderfully bright color pictures may provide a sense of realism to the actual fluid mechanics inside a
flow system, but they are worthless if they are not quantitatively correct. Thus, numerical results must always be thoroughly examined before they are believed; therefore, a CFD
user needs to learn how to properly analyze and make critical judgments about the computed results.
Another important comment is collaboration between mechanical engineers and medical scientists. Not any one department can deliver a result. Each discipline should provide
feedback on the results at each step.
Final Remarks
Rapid advances of many industrial applications in computer science are outstanding, which requires changes in CFD.
This changing situation is partly attributed to the rapid evolution of CFD techniques and models. Excellent creative models for simulating complex fluid mechanics problems in the
human body and therapeutic models are now being progressively applied, particularly with the availability of commercial
CFD computer programs. The increasing use of these programs in medicine might reveal how demanding the practical problems analyzed by CFD are. With decreasing hardware
costs and rapid computing times, researchers and medical scientists may be relying increasingly on this reliable CFD tool
to deliver accurate results. However, a realistic multidisciplinary approach is essential to accomplish these tasks. Indefinite collaborations between mechanical engineers and clinical and medical scientists are essential. CFD may be an important methodology for understanding the pathophysiology of developing and progressing cardiovascular disease
and for establishing creative treatment modalities in the cardiovascular field.
REFERENCES
1) Versteeg HK, Malalasekera W. Introduction To Computational Fluid
Dynamics. The Finite Volume Method. 1st ed. New York: Longman
Scientific & Technical;1995.
2) Tu J, Yeoh GH, Liu C. Computational Fluid dynamics. A Practical Approach. 1st ed. Oxford: Elesevier;2008.
3) Fung YC. Biomechanics. New York: Springer-Verlag;1981.
4) Cho YI, Cho DJ. Hemorheology and microvascular disorders. Korean
Circ J 2011;41:287-95.
5) Nichols WW, ORouke MF. McDonalds Blood Flow in Arteries
Theoretical, Experimental and Clinical Principles. 5th ed. London:
Hodder Arnold;2005.
429
6) Lee BK, Kwon HM, Hong BK, et al. Hemodynamic effects on atherosclerosis-prone coronary artery: wall shear stress/rate distribution and
impedance phase angle in coronary and aortic circulation. Yonsei Med
J 2001;42:375-83.
7) Freidman MH, Deter OJ, Mar FF, Bargeron CB, Hutchins GM. Arterial
geometry affects hemodynamics: a potential risk factor for atherosclerosis. Atherosclerosis 1983;46:225-31.
8) Fuster V, Badimon L, Badimon J, Chesebro JH. The pathogenesis of
coronary artery disease and acute coronary syndromes. N Engl J Med
1992;326:242-50.
9) Lee BK, Kwon HM, Kim DS, et al. Computed numerical analysis of
the biomechanical effects on coronary atherogenesis using human hemodynamic and dimensional variables. Yonsei Med J 1998;39:16674.
10) Qiu Y, Tarbell JM. Numerical simulation of pulsatile flow in a compliant curved tube model of a coronary artery. J Biomech Eng 2000;
122:77-85.
11) Ramaswamy SD, Vigmostad SC, Wahle A, et al. Fluid dynamic analysis in a human left anterior descending coronary artery with arterial motion. Ann Biomed Eng 2004;32:1628-41.
12) Giannoglou GD, Soulis JV, Farmakis TM, Giannakoulas GA, Parcharidis GE, Louridas GE. Wall pressure gradient in normal left coronary
artery tree. Med Eng Phys 2005;27:455-64.
13) LaDisa JF Jr, Olson LE, Douglas HA, Warltier DO, Kersten JR, Pagel
PS. Alterations in regional vascular geometry produced by theoretical stent implantation influence distributions of wall shear stress: analysis of a curved coronary artery using 3D computational fluid dynamics modeling. Biomed Eng Online 2006;16:40.
14) Papafaklis MI, Bourantas CV, Theodorakis PE, Katsouras CS, Fotiadis DI, Michalis LK. Association of endothelial shear stress with
plaque thickness in a real three-dimensional left main coronary artery
bifurcation model. Int J Cardiol 2007;115:276-8.
15) Lee BK, Lee JY, Hong BK, et al. Hemodynamic analysis of coronary
circulation in angulated coronary stenosis following stenting. Yonsei
Med J 2002;43:590-600.
16) Ramaswamy SD, Vigmostad SC, Wahle A, et al. Comparison of left
anterior descending coronary artery hemodynamics before and after
angioplasty. J Biomech Eng 2006;128:40-8.
17) Sankaranarayanan M, Chua LP, Ghista DN, Tan YS. Computational
model of blood flow in the aorto-coronary bypass graft. Biomed Eng
Online 2005;4:14.
18) Freshwater IJ, Morsi YS, Lai T. The effect of angle on wall shear
stresses in a LIMA to LAD anastomosis: numerical modelling of pulsatile flow. Proc Inst Mech Eng H 2006;220:743-57.
19) Fontan F, Baudet E. Surgical repair of tricuspid atresia. Thorax
1971;26:240-8.
20) Feldt RH, Driscoll DJ, Offord KP, et al. Protein-losing enteropathy
after the Fontan operation. J Thorac Cardiovasc Surg 1996;112:67280.
21) Starnes SL, Duncan BW, Kneebone JM, et al. Angiogenic proteins in
the lungs of children after cavopulmonary anastomosis. J Thorac Cardiovasc Surg 2001;122:518 -23.
22) Matthews IL, Fredriksen PM, Bjrnstad PG, Thaulow E, Gronn M.
Reduced pulmonary function in children with the Fontan circulation
affects their exercise capacity. Cardiol Young 2006;16:261-7.
23) Gewillig M. The Fontan circulation. Heart 2005;91:839-46.
24) Cheung YF, Penny DJ, Redington AN. Serial assessment of left ventricular diastolic function after Fontan procedure. Heart 2000;83:
420-4.
25) Gerdes A, Kunze J, Pfister G, et al. Addition of a small curvature reduces power losses across total cavopulmonary connections. Ann Thorac Surg 1999;67:1760-4.
26) Myers CD, Boyd JH, Presson RG Jr, et al. Neonatal cavopulmonary
assist: pulsatile versus steady-flow pulmonary perfusion. Ann Thorac
Surg 2006;81:257-63.
27) Hager A, Fratz S, Schwaiger M, Lange R, Hess J, Stern H. Pulmonary blood flow patterns in patients with Fontan circulation. Ann Tho-
430
Computational Fluid Dynamics in CV Disease
rac Surg 2008;85:186-91.
28) Bove EL, de Leval MR, Magliavacca F, Guadagni G, Dubini G.
Computational fluid dynamics in the evaluation of hemodynamic performance of cavopulmonary connections after the Norwood procedure
for hypoplastic left heart syndrome. J Thorac Cardiovasc Surg 2003;
126:1040-7.
29) de Zelicourt DA, Pekkan K, Parks J, Kanter K, Fogel M, Yoganathan
AP. Flow study of an extracardiac connection with persistent left superior vena cava. J Thorac Cardiovasc Surg 2006;131:785-91.
30) Suh SH, Kaptan Y, Roh HW, et al. Estimation of Heart work by
means of modified Windkessel model and different whole blood viscosity models. Proceedings of 7th International Conference on Computational Heat and Mass Transfer, Istanbul;2011.
31) Westerhof N, Lankhaar JW, Westerhof BE. The arterial Windkessel.
Med Biol Eng Comput 2009;47:131-41.
32) Ylmaz Y, Gndodu MY. A critical review on blood flow in large arteries: relevance to blood rheology, viscosity models and physiologic
conditions. Korea-Aust Rheol J 2008;20:197-211.
33) Milner JS, Moore JA, Rutt BK, Steinman DA. Hemodynamics of human carotid artery bifurcations: computational studies with models reconstructed from magnetic resonance imaging of normal subjects. J
Vasc Surg 1998;28:143-56.
34) Lee SW, Antiga L, Spence JD, Steinman DA. Geometry of the carotid
bifurcation predicts its exposure to disturbed flow. Stroke 2008;39:
2341-7.
35) Lee SE, Lee SW, Fischer PF, Bassiouny HS, Loth F. Direct numerical simulation of transitional flow in a stenosed carotid bifurcation. J
Biomech 2008;41:2551-61.
36) Martin D, Zaman A, Hacker J, Mendelow D, Birchall D. Analysis of
haemodynamic factors involved in carotid atherosclerosis using computational fluid dynamics. Br J Radiol 2009;82:S33-8.
37) Hayase H, Tokunaga K, Nakayama T, et al. Computational fluid dynamics of carotid arteries after carotid endarterectomy or carotid artery stenting based on postoperative patient-specific computed tomography angiography and ultrasound flow data. Neurosurgery 2011;
68:1096-101; discussion 1101.
38) Xue YJ, Gao PY, Duan Q, et al. Preliminary study of hemodynamic
distribution in patient-specific stenotic carotid bifurcation by imagebased computational fluid dynamics. Acta Radiol 2008;49:558-65.
39) Hammer S, Jeays A, Allan PL, et al. Acquisition of 3-D arterial geometries and integration with computational fluid dynamics. Ultrasound
Med Biol 2009;35:2069-83.
40) LaDisa JF Jr, Bowers M, Harmann L, et al. Time-efficient patient-
specific quantification of regional carotid artery fluid dynamics and
spatial correlation with plaque burden. Med Phys 2010;37:784-92.
41) Marshall I. Computational simulations and experimental studies of
3D phase-contrast imaging of fluid flow in carotid bifurcation geometries. J Magn Reson Imaging 2010;31:928-34.
42) Groen HC, Simons L, van den Bouwhuijsen QJ, et al. MRI-based quantification of outflow boundary conditions for computational fluid
dynamics of stenosed human carotid arteries. J Biomech 2010;43:
2332-8.
43) Frauenfelder T, Lotfey M, Boehm T, Wildermuth S. Computational fluid dynamics: hemodynamic changes in abdominal aortic aneurysm
after stent-graft implantation. Cardiovasc Intervent Radiol 2006;29:
613-23. Erratum in: Cardiovasc Intervent Radiol 2006;29:724.
44) ORourke MJ, McCullough JP. A comparison of the measured and predicted flowfield in a patient-specific model of an abdominal aortic aneurysm. Proc Inst Mech Eng H 2008;222:737-50.
45) Suh GY, Les AS, Tenforde AS, et al. Quantification of particle residence time in abdominal aortic aneurysms using magnetic resonance
imaging and computational fluid dynamics. Ann Biomed Eng 2011;
39:864-83.
46) Filipovic N, Ivanovic M, Krstajic D, Kojic M. Hemodynamic flow modeling through an abdominal aorta aneurysm using data mining tools.
IEEE Trans Inf Technol Biomed 2011;15:189-94.
47) Karmonik C, Bismuth J, Davies MG, Shah DJ, Younes HK, Lumsden
AB. A computational fluid dynamics study pre- and post-stent graft
placement in an acute type B aortic dissection. Vasc Endovascular Surg
2011;45:157-64.
48) Tremmel M, Xiang J, Natarajan SK, et al. Alteration of intra-aneurysmal hemodynamics for flow diversion using enterprise and vision
stents. World Neurosurg 2010;74:306-15.
49) Radaelli AG, Augsburger L, Cebral JR, et al. Reproducibility of haemodynamical simulations in a subject-specific stented aneurysm model: a report on the Virtual Intracranial Stenting Challenge 2007. J
Biomech 2008;41:2069-81.
50) Cebral JR, Mut F, Weir J, Putman C. Quantitative characterization
of the hemodynamic environment in ruptured and unruptured brain aneurysms. AJNR Am J Neuroradiol 2011;32:145-51.
51) Sforza DM, Lhner R, Putman C, Cebral J. Hemodynamic Analysis
of intracranial aneurysms with moving parent arteries: basilar tip
aneurysms. Int J Numer Methods Biomed Eng 2010;26:1219-27.
52) Cebral JR, Mut F, Weir J, Putman CM. Association of hemodynamic
characteristics and cerebral aneurysm rupture. AJNR Am J Neuroradiol 2011;32:264-70.
Вам также может понравиться
- Computer Simulations of Blood Flow With Mass Transport Through The Carotid Artery BifurcationДокумент33 страницыComputer Simulations of Blood Flow With Mass Transport Through The Carotid Artery BifurcationinodanaОценок пока нет
- Physics Driven Real-Time Blood Flow Simulations: SciencedirectДокумент17 страницPhysics Driven Real-Time Blood Flow Simulations: SciencedirectTim LeeОценок пока нет
- Computational Fluid Dynamics in Coronary and Intra-Cardiac Flow SimulationДокумент8 страницComputational Fluid Dynamics in Coronary and Intra-Cardiac Flow SimulationIJRASETPublicationsОценок пока нет
- Untitled 2Документ4 страницыUntitled 2agneswingetОценок пока нет
- Computational Fluid DynamicsДокумент4 страницыComputational Fluid DynamicsSujith NakkaОценок пока нет
- 18 FullДокумент11 страниц18 FullTemple MaduomaОценок пока нет
- CFD Validations With FDA Benchmarks of Medical Devices FlowsДокумент9 страницCFD Validations With FDA Benchmarks of Medical Devices FlowsVijay KadliОценок пока нет
- Genetic Algorithm Techniques For Calibrating Network ModelsДокумент44 страницыGenetic Algorithm Techniques For Calibrating Network ModelsAde YahyaОценок пока нет
- Kissas 2020Документ28 страницKissas 2020chethan mahadevОценок пока нет
- Ijecet: International Journal of Electronics and Communication Engineering & Technology (Ijecet)Документ10 страницIjecet: International Journal of Electronics and Communication Engineering & Technology (Ijecet)IAEME PublicationОценок пока нет
- Biomedical Fluid Mechanics UPCДокумент16 страницBiomedical Fluid Mechanics UPCMasterAlbus3dОценок пока нет
- High-Level Synthesis of Digital Microfluidic BiochipsДокумент32 страницыHigh-Level Synthesis of Digital Microfluidic BiochipsTeferiОценок пока нет
- Specialized Finite Element Analysis Computer Software For Modeling Hemodynamics in Abdominal Aortic and Carotid Artery Bifurcation AneurysmsДокумент8 страницSpecialized Finite Element Analysis Computer Software For Modeling Hemodynamics in Abdominal Aortic and Carotid Artery Bifurcation AneurysmsKanesan MuthusamyОценок пока нет
- Definition of CFDДокумент2 страницыDefinition of CFDKabir ShafayatОценок пока нет
- CFD Presentation - Aditya PatilДокумент14 страницCFD Presentation - Aditya PatiladityaОценок пока нет
- Aerospace Marine Systems Communication Systems Transportation and Vehicles Bio MedicalДокумент12 страницAerospace Marine Systems Communication Systems Transportation and Vehicles Bio MedicalUmair IqbalОценок пока нет
- Sketch-Based Dynamic Illustration of Fluid Systems: Online Submission ID: 0260Документ8 страницSketch-Based Dynamic Illustration of Fluid Systems: Online Submission ID: 0260VicshannОценок пока нет
- Computational Uid Dynamics Modelling in Cardiovascular MedicineДокумент12 страницComputational Uid Dynamics Modelling in Cardiovascular MedicineMasterAlbus3dОценок пока нет
- pvc1Документ18 страницpvc1Feni FardilaОценок пока нет
- CFD Blood Flow PDFДокумент4 страницыCFD Blood Flow PDFmadhsudan senapatiОценок пока нет
- Presentation On CFD 2Документ17 страницPresentation On CFD 220MVB325 Md Abdur RahimОценок пока нет
- High Performance Deformable Image Registration Algorithms for Manycore ProcessorsОт EverandHigh Performance Deformable Image Registration Algorithms for Manycore ProcessorsОценок пока нет
- CFD IntroductionДокумент1 страницаCFD IntroductionbennyОценок пока нет
- Melka2018 Article MultiphaseSimulationOfBloodFloДокумент9 страницMelka2018 Article MultiphaseSimulationOfBloodFlonitesh_n2840Оценок пока нет
- Applied Sciences: A Hybrid Degradation Modeling and Prognostic Method For The Multi-Modal SystemДокумент21 страницаApplied Sciences: A Hybrid Degradation Modeling and Prognostic Method For The Multi-Modal SystemsdfsdghОценок пока нет
- Loosely Coupled MethodДокумент18 страницLoosely Coupled MethodMadhu Kiran Reddy MuliОценок пока нет
- Experimentacion RapidasДокумент10 страницExperimentacion RapidasOscar Choque JaqquehuaОценок пока нет
- 3D Reconstruction of Coronary Arteries From Angiographic Images: A SurveyДокумент6 страниц3D Reconstruction of Coronary Arteries From Angiographic Images: A SurveyijcsnОценок пока нет
- Ao - 36 - 359Документ9 страницAo - 36 - 359xikun WОценок пока нет
- 1 s2.0 S0020740321003842 Main PDFДокумент13 страниц1 s2.0 S0020740321003842 Main PDFKhalla InesОценок пока нет
- Odenthal 2010 Tundish CFDДокумент11 страницOdenthal 2010 Tundish CFDGreg BurgreenОценок пока нет
- Fluid AssignmentДокумент23 страницыFluid AssignmentYush KumarОценок пока нет
- Simulating Radial Pressure Waveforms With A Mock Circulatory Flow Loop To Characterize Hemodynamic Monitoring SystemsДокумент12 страницSimulating Radial Pressure Waveforms With A Mock Circulatory Flow Loop To Characterize Hemodynamic Monitoring Systemsyue jiangОценок пока нет
- Fru Chard 2014Документ10 страницFru Chard 2014mezianeОценок пока нет
- CFD Report (Introduction To CFD)Документ10 страницCFD Report (Introduction To CFD)Israel Torres100% (1)
- A Modeling and Analysis Method For Fractional-Order DCDC ConvertersДокумент12 страницA Modeling and Analysis Method For Fractional-Order DCDC ConvertersHoussem GrachaОценок пока нет
- Module 1 CFD RssДокумент24 страницыModule 1 CFD Rssruikar manojОценок пока нет
- Fluent Workshop Lecture NotesДокумент206 страницFluent Workshop Lecture NoteszubbbuОценок пока нет
- Three-Dimensional Computational Fluid Dynamics Simulation of Valve-Induced Water HammerДокумент12 страницThree-Dimensional Computational Fluid Dynamics Simulation of Valve-Induced Water HammerDario Andres Serrano FlorezОценок пока нет
- Physical Problem: General Introduction: Historical Background and Spectrum of ApplicationsДокумент6 страницPhysical Problem: General Introduction: Historical Background and Spectrum of ApplicationshetanshuОценок пока нет
- Jimmy Finaly Year ProjectДокумент56 страницJimmy Finaly Year Projectßélå Åß MélÉssêОценок пока нет
- Into To CFDДокумент57 страницInto To CFDRohit ThakranОценок пока нет
- CDC by Ajaysimha - VlsiДокумент14 страницCDC by Ajaysimha - VlsiPriyanka GollapallyОценок пока нет
- Numer Methods Biomed Eng - 2018 - Finsberg - Efficient Estimation of Personalized Biventricular Mechanical FunctionДокумент20 страницNumer Methods Biomed Eng - 2018 - Finsberg - Efficient Estimation of Personalized Biventricular Mechanical FunctionLiubovОценок пока нет
- Applied Computational Fluid Dynamics I ToДокумент353 страницыApplied Computational Fluid Dynamics I ToIvan Hernández100% (4)
- Research On Prediction Method of Gear PumpДокумент21 страницаResearch On Prediction Method of Gear PumpDamigo DiegoОценок пока нет
- Scale-Up of Micro and Milli ReactorsДокумент75 страницScale-Up of Micro and Milli ReactorsBessalah MohammedОценок пока нет
- Dirkes 2024Документ19 страницDirkes 2024xlv10525Оценок пока нет
- Computational Fluid Mechanics Simulation and Computation With Gambit and FluentДокумент69 страницComputational Fluid Mechanics Simulation and Computation With Gambit and FluentYush KumarОценок пока нет
- Wang 2009Документ11 страницWang 2009Tuan PhanОценок пока нет
- Detected Pulses From The Motion of The Head To Estimate Heartbeat RateДокумент5 страницDetected Pulses From The Motion of The Head To Estimate Heartbeat RateMai Anh ThưОценок пока нет
- Computerized Medical Imaging and Graphics: Zhonghua Sun, Lei XuДокумент13 страницComputerized Medical Imaging and Graphics: Zhonghua Sun, Lei XuKain SmithОценок пока нет
- Applied Computational Fluid DynamicsДокумент354 страницыApplied Computational Fluid Dynamicstriantosd100% (1)
- A Comprehensive Review On Accuracy in USM Using Reconfigurable Systems and Deep Learning ApproachesДокумент16 страницA Comprehensive Review On Accuracy in USM Using Reconfigurable Systems and Deep Learning ApproachesВіталій РоманОценок пока нет
- Bio Med PaperДокумент13 страницBio Med PaperironmanjrpОценок пока нет
- Special Issue On Healthcare Mechatronics: Chinese Journal of Mechanical EngineeringДокумент2 страницыSpecial Issue On Healthcare Mechatronics: Chinese Journal of Mechanical Engineeringalamin khondakerОценок пока нет
- Heart Blood Flow Simulation: A Perspective Review: Biomedical Engineering OnlineДокумент28 страницHeart Blood Flow Simulation: A Perspective Review: Biomedical Engineering Onlinemartin.dureux888Оценок пока нет
- Journal of Computational PhysicsДокумент17 страницJournal of Computational PhysicsKain SmithОценок пока нет
- Design of Embedded Microcontroller For Controlling and Monitoring Blood PumpДокумент8 страницDesign of Embedded Microcontroller For Controlling and Monitoring Blood PumpGEORGE MYLONASОценок пока нет
- Personalized Computational Hemodynamics: Models, Methods, and Applications for Vascular Surgery and Antitumor TherapyОт EverandPersonalized Computational Hemodynamics: Models, Methods, and Applications for Vascular Surgery and Antitumor TherapyОценок пока нет
- Prop RelationsДокумент5 страницProp RelationsaeroacademicОценок пока нет
- Noc19-Ae10 Assignment Week 02Документ3 страницыNoc19-Ae10 Assignment Week 02aeroacademicОценок пока нет
- Assignment 11: Unit 12 - Week 11Документ3 страницыAssignment 11: Unit 12 - Week 11aeroacademicОценок пока нет
- Assignment 10: Unit 11 - Week 10Документ3 страницыAssignment 10: Unit 11 - Week 10aeroacademicОценок пока нет
- Assignment 12: Unit 13 - Week 12Документ3 страницыAssignment 12: Unit 13 - Week 12aeroacademicОценок пока нет
- Assignment 03: Unit 4 - Week 3Документ5 страницAssignment 03: Unit 4 - Week 3aeroacademicОценок пока нет
- Noc19-Ae10 Assignment Week 09Документ3 страницыNoc19-Ae10 Assignment Week 09aeroacademicОценок пока нет
- Assignment 06: Unit 7 - Week 6Документ4 страницыAssignment 06: Unit 7 - Week 6aeroacademicОценок пока нет
- Assignment 05: Unit 6 - Week 5Документ3 страницыAssignment 05: Unit 6 - Week 5aeroacademicОценок пока нет
- Assignment 07: Unit 8 - Week 7Документ3 страницыAssignment 07: Unit 8 - Week 7aeroacademicОценок пока нет
- Suresh C Khandai - 1Документ9 страницSuresh C Khandai - 1aeroacademicОценок пока нет
- Free/Libre and Open Source Software (FLOSS) Resources For Online CoursesДокумент4 страницыFree/Libre and Open Source Software (FLOSS) Resources For Online CoursesaeroacademicОценок пока нет
- Washington1993 CurvatureДокумент9 страницWashington1993 CurvatureaeroacademicОценок пока нет
- The Research Analysis of Aerodynamic Numerical Simulation of Grid FinДокумент6 страницThe Research Analysis of Aerodynamic Numerical Simulation of Grid FinaeroacademicОценок пока нет
- Tamil Guide For PrintДокумент238 страницTamil Guide For PrintaeroacademicОценок пока нет
- Numerical Study On Drag Reduction For Grid-Fin ConfigurationsДокумент10 страницNumerical Study On Drag Reduction For Grid-Fin ConfigurationsaeroacademicОценок пока нет
- Grid Fins New Concept Missile Stability and Control: Alaa A ForДокумент12 страницGrid Fins New Concept Missile Stability and Control: Alaa A ForaeroacademicОценок пока нет
- Sizing of A Turboprop Unmanned Air Vehicle and Its Propulsion SystemДокумент10 страницSizing of A Turboprop Unmanned Air Vehicle and Its Propulsion SystemaeroacademicОценок пока нет
- Suresh C Khandai - 2Документ9 страницSuresh C Khandai - 2aeroacademicОценок пока нет
- Development of Flight Controller Using STM Microcontroller BoardДокумент5 страницDevelopment of Flight Controller Using STM Microcontroller BoardaeroacademicОценок пока нет
- B BPP Prog Guide-EДокумент29 страницB BPP Prog Guide-EaeroacademicОценок пока нет
- Answers: Exercise 1.1Документ22 страницыAnswers: Exercise 1.1aeroacademicОценок пока нет
- Smart MatrlsДокумент13 страницSmart MatrlsaeroacademicОценок пока нет
- BelieverДокумент1 страницаBelieveraeroacademicОценок пока нет
- ANSYS CFD-Post Users GuideДокумент376 страницANSYS CFD-Post Users GuideAvuluri Sreenivasa RaoОценок пока нет
- Tense FormsДокумент1 страницаTense FormsaeroacademicОценок пока нет
- Status and Future Trends: W. H. AveryДокумент8 страницStatus and Future Trends: W. H. AveryaeroacademicОценок пока нет
- Atrial Fibrillation - Annals of Internal Medicine (2023)Документ18 страницAtrial Fibrillation - Annals of Internal Medicine (2023)silvermist100% (2)
- College of Nursing: Pharmacological ManagementДокумент4 страницыCollege of Nursing: Pharmacological ManagementBianca Mikaela DosdosОценок пока нет
- CVS, PVS and LymphДокумент27 страницCVS, PVS and Lymphjjmojica99Оценок пока нет
- Human Resource Management - AMRI MKPДокумент123 страницыHuman Resource Management - AMRI MKPSayantan MandalОценок пока нет
- Kayak AlpaДокумент16 страницKayak AlpaR_Aranganathan100% (2)
- Medical Terms in Lay Language2Документ7 страницMedical Terms in Lay Language2Mavra zОценок пока нет
- Vijay ShreeДокумент98 страницVijay ShreeRafi SungkarОценок пока нет
- Science QPДокумент67 страницScience QPVENKATESH YОценок пока нет
- Emergency Surgical Interventions in Patients With Pericardial EffusionДокумент7 страницEmergency Surgical Interventions in Patients With Pericardial Effusionnatalia figueroaОценок пока нет
- Ñ-û-Ç-â-Ç - Û-Ç-+-+ - +-Ç-+-Ä-Û-+-ÎДокумент34 страницыÑ-û-Ç-â-Ç - Û-Ç-+-+ - +-Ç-+-Ä-Û-+-ÎVidhyanand RamachandranОценок пока нет
- Had Unit I Notes UpdatedДокумент43 страницыHad Unit I Notes UpdatedPoonguzhaliОценок пока нет
- Ob Scan TemplateДокумент1 страницаOb Scan TemplateAmed ClinicОценок пока нет
- UntitledДокумент10 страницUntitledGuia Charish SalvadorОценок пока нет
- Critical Care Nursing Notes 1Документ10 страницCritical Care Nursing Notes 1pauchanmnlОценок пока нет
- Jewish Mafia in Wales Instigates The Murder of A 7-Year-Old-Girl, Isabellaan Battiscombe, in Hospital in Wales, UK.Документ17 страницJewish Mafia in Wales Instigates The Murder of A 7-Year-Old-Girl, Isabellaan Battiscombe, in Hospital in Wales, UK.andrew kaprusiakОценок пока нет
- Pacemakers & AICDДокумент32 страницыPacemakers & AICDqmmmОценок пока нет
- Sample Questions For HAAD Prometric and DHA For NursesДокумент46 страницSample Questions For HAAD Prometric and DHA For NursesJaezelle Ella Sabale100% (4)
- MKSAP 17 Audio Companion 2015 - PDF File - Cardiology PDFДокумент68 страницMKSAP 17 Audio Companion 2015 - PDF File - Cardiology PDFPaul StatoОценок пока нет
- Ecg Basic ConceptsДокумент18 страницEcg Basic ConceptsDaniel SolonyaОценок пока нет
- Meg Roswick ProfileДокумент4 страницыMeg Roswick Profileapi-344976059Оценок пока нет
- Cir 0000000000000899Документ25 страницCir 0000000000000899hanifa ambОценок пока нет
- The Hazards: OF Blood TransfusionДокумент7 страницThe Hazards: OF Blood TransfusionPranjal Kr SahariaОценок пока нет
- Mitral RegurgitationДокумент10 страницMitral RegurgitationWalter Saavedra YarlequeОценок пока нет
- Diploma in KalariPayattu - Final Syllabus - 25 - 7 - 18Документ18 страницDiploma in KalariPayattu - Final Syllabus - 25 - 7 - 18Adhithya KiranОценок пока нет
- Case Study 1Документ3 страницыCase Study 1Da NicaОценок пока нет
- Chest TraumaДокумент47 страницChest Traumafrenee aradanasОценок пока нет
- SyncopeДокумент83 страницыSyncopeReza SatriaОценок пока нет
- Adult Tachycardia (With Pulse) AlgorithmДокумент1 страницаAdult Tachycardia (With Pulse) AlgorithmJames ChoiОценок пока нет
- AmiodaroneДокумент2 страницыAmiodaroneedemОценок пока нет
- Benefits of Ajwa Dates.Документ1 страницаBenefits of Ajwa Dates.mamun31Оценок пока нет