Академический Документы
Профессиональный Документы
Культура Документы
Congestive Heart Failure
Загружено:
yvasparksАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Congestive Heart Failure
Загружено:
yvasparksАвторское право:
Доступные форматы
Congestive Heart Failure
Disease/Disor
der
Congestive Heart
Failure
*20 million people
affected wordlwide
*30-40% die w/in 1
year of diagnosis
Etiology/Pathogenesis
Heart cant maintain circulator needs
of the body (can be inherited or
genetic)
2 Major Types/Categories (50/50)
1.HF w/ reduced/depressed EF
(systolic failure/<40-50%)
2.HF w/ preserved EF (diastolic
failure)
Considerable Overlap
*CAD (60-70%)
*HTN (75%)
*DM
*Idiopathic (20-30% diastolic
failure)post viral, alcohol, genetic
defects (mostly autosomal dominant)
Pathogenesis
*index event kicks things off: hearts
pumping capacity declines (either
muscle damaged b/c myocytes arent
functioning/force or contraction issues
from diseases/ heriditary/EtOH)
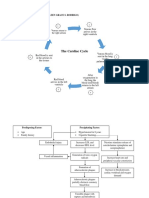
Restore CV
function short
term, thus causing
pts to be
asymptomatic for
years
Heart Compensates by activating:
1.RAAS System (reninangiontension-aldosterone-system):
2.adrenergic nervous system
**RAAS & Adrenergic NS are
responsible for maintaining CO by
increased retention NA and H2O +
increased contractility
3. cytokine system (IL-6)
**activation of vasodilatory
molecules which decrease peripheral
vasoconstriction (atrial & brain
Pathology
*Most asymptomatic for prolonged periods of time (compensatory mechanisms)
*Eventually heart cant compensatesymptomatic HF occurs & is accompanied by increasing activation of
neurohormonal, adrenergic, & cytokine systemscause adaptive change in heart muscle (AKA LV
remodeling)
**a lot known about how CFH & depressed EF/systolic failure work
**little known about CHF & preserved/diastolic failure (increased vascular stiffness, impaired renal function,
& diastolic dysfunction-factors)
Biologic Stimuli: neurohormones (Norephinephrine, & angiotensin II, inflammatory cytokines (TNF), &
other peptides and growing factors (endothelin) & reactive O2 species (superoxide)overexpressed &
contribute to HF by deleterious/harmful effects they have on heart and circulation (important b/c forms
clinical rationale for using pharmacologic antagonizing agents (ACE & BB)
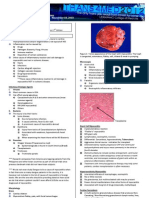
Systolic Dysfunction:
LV remodeling (factors that lead to symptomatic HF) develops in a series of complex events (occur in cellular
& molecular levels)
1.myocute hypertrophy
2.alterations in contractile properties of myoctes
3.progressive loss of myocytes (via necrosis, apoptosis, & autophagic cell death)
4.B-adrenergic desensitization
5. abnormal myocardial energetics & metabolism
6. reorg of extracellular matrix (organized collagen structural weave dissolvesreplaced by interstitial/fibrotic
collagen that doesnt provide support)
*sustained neurohormonal activation and mechanical overload result in trasnscriptional & posttranscriptional
changes in genes & proteins that regulate excitation-contraction coupling & cross bridge interaction (changes
include: decreased function of sarcoplasmic reticulum Ca2+ adenosine triphosphatase-SERCA2A, lower Ca2+
uptake in SR, hyperphosphorylation of ryanodine reception causing leakage of Ca2+ from SR)
*cross-bridge changes include decreased a-myosin increased b-myosin, myocytolysis, + disruption of
cystoskeletal links b/w sarcomeres and extracellular matrix = poor contractility
Diastolic Dysfunction (can occur alone or w/systolic dysfunction):
Background: myocardial relaxation/diastole is an adenosine triphosphate dependent process (ATP) thats
regulated by uptake of Ca2+ into SR by SERCA2A and release/exit of Ca2+ by sarcolemmal pumps
*reductions in ATP, which occurs in ischemia, impairs relaxation
*hypertrophy/fibrosis= reduced compliance= causes filling to be delayedelevated LV pressures at end
Congestive Heart Failure
naturetic peptides, prostaglandins,
NO)
NYHA functional class is a predictor
of prognosis
Class I: asymptomatic
Class II: slight limitation in physical
activity(5-10% annual mortality)
Class III: comfortable at rest, less than
ordinary activity causes fatigue
Class IV: cant do any physical
activity w/out discomfort (30-70%
mortality)
diastole
*HR increases causing shorted diastolic filling time (could lead to elevated LV filling pressures (particularly
non-compliant ventricles)leads to increase in pulmonary capillary pressures)
HR shortens diastolic fill time LV filing pressure capillary pressuresdyspnea
LV Remodeling
*changes in LV mass, volume, shape, & composition of heart after cardiac injury or abnormal hemodynamic
condition
*can contribute independently to progression of HF (mechanical burdens by changes in shape of heart)
-LV wall thinning occurs from LV dilationafterload mismatchfurther decrease in stroke volume
-high end-diastolic wall stress may lead to 1. Hypofusion of subendocardium (worsening of LV function)
2. increased oxidative stressactivates genes/families that are sensitive to free radical generation (TNF,
IL) 3. Sustained activation of stretch activated genes (angiotensin II, endothelin, and TNF) and/or
Activation of hypertrophic signaling pathwaysLV dilation/tethering of papillary muscles
Incompetence of mitral valve and mitral regurgitation further hemodynamic overloading
Congestive Heart Failure
Investigation & Findings
Symptoms
Cardinal Symptoms
Fatigue & dyspnea
Fatigue: low CO output + skeletal muscle abnormalities + noncardiac comorbities
(anemia)
Dysnpea: progresses as CHF gets worse
**most important mechanism is pulmonary congestion w/ accumulation of interstitial
or intra-alveolar fluidactivates juxtacapillary J receptorsstimulate rapid, shallow
breathing (Stage III)
*pulmonary compliance, increased airway resistance, respiratory muscle and/or
diaphragm fatigue, and anemia play a role as well
**can become less frequent w/ onset of RV failure & tricuspid regurgitation
Orthopnea: trouble breathing lying down
*usually later manifestation
*fluid redistributes from the splanchnic circulation (gastric, small intestinal, colonic,
pancreatic, hepatic, & splenic circulations) & lower extremities into central circulation
when lying down/recumbent pulmonary capillary pressure *nocturnal cough
*normally indication of HF but can be present with ascites/pulmonary disease = people
who favor upright position
General Appearance & Vitals
*mild to moderate HF-appears in no distress at rest except for uncomfortable when lying flat for
more than a fever minutes
*severe HF-must sit upright, labored breathing, sometimes cant finish sentence bc breath shortness
*Systolic BP- normal or high in early HFlow in late HF (LV dysfunction)
Jugular Veins
*examination of JVs provides estimation of atrial pressurebest when lying flat head at 45 degree
*normal is 8-10cm
*early stag
es normal at rest may be abnormally elevated w/ sustained pressure on abdomen
Pulmonary Exam
*pulmonary crackles (rales or crepitations) result from the transudation of fluid from the
intravascular space into alveoli
*rales frequently absent in pts with chronic HF because of increased lymphatic drainage of
alveolar fluid
*pleural effusions result from elevation of elevation of pleural capillaries pressure + transudation
of fluid into the pleural cavities
*since pleural veins drain into both system & pulmonary veins, pleural effusions occur mostly in
biventricular failure
Paroxysmal Nocturnal Dyspnea: acture episodes of shortness of breath & coughing
(generally occur at night after 1-3 hours of sleep)NOT RELIEVED SITTING UP
*increased pressure in bronchial arteriesairway compression + interstitial pulmonary
edema
*Cardiac asthma closely related to PBDwheezing occurs secondary to
bronchospasms
Cardiac Exam
*usually doesnt provide useful info
*point of maximal impulse (PMI) usually displaced below 5th intercostal space and/or lateral to
midclavicular line if cardiomegaly is presentenlarged and sustained
*Severity of LV hypertrophy leads to sustained PMI
* S3 (protodiastolic gallop) is audible and palpable at apex ; commonly present in pts w/ volume
overload + tachypnea and tachycardia
* S4 not specific indicator of HF but present in pts w/ diastolic dysfunction
*murmurs of tricuspid and mitral valves frequently present in advanced HF
Cheyne Stokes Respiration (aka periodic or cyclic respiration): abnormal pattern of
Abdomen & Extremities
Congestive Heart Failure
breathing characterized by progressively deeper and sometimes faster breathing,
followed by a gradual decrease that results in a temporary stop in breathing (apnea )
*caused by decreased sensitivity of respiratory center to arterial PCO2
*present in 40% pts w/ advanced HF
*Hepatomegaly important sign in patients with HRfrequently tender may pulsate during systole
(ascites-late sign-increased pressure on hepatic veins & drainage, jaundice also late sign
*Peripheral Edema: cardinal manifestation but absent w/ diuretic useprominent in ankles and
pretibial regions- in bedridden pts can be found in presacral and scrotal region
Diagnosis
Cardiac Cachexia
OthertoSymptoms:
*Key
making diagnosis is to have high index of suspicion, particularly w/ high risk patients-
*vomiting due to congestive hepatomegaly & abdominal fullness, nausea, anorexia
*GI, anorexia, nausea, eat minimal have abdominal pain
*elevation of resting metabolic rate
Blood
Work
*edema
of bowel and/or congestive liverstretching/congestion of liver may lead to
*elevation of concentrations of cytokines & TNF
*CBC,
panel of electrolytes, BUN, SCr, Hepatic Enzymes, & urinalysis (some should have dyslipidemia (cholesterol), fasting serum glucose or oral glucose (DM), and thyroid stimulating
RUQ pain
*impairment of intestinal absorption due to congestion of intestinal veins
hormone levels (thyroid abnormalities)
*cerebral symptoms: confusion, disorientation, sleep and mood disturbances PM peeing *POOR PROGNOSIS WHEN PRESENT
ECG
*assess rate/rhythm to determine presence of LV hypertrophy or prior MI (presence/absence of Q wave)
*look at QRS width to see if resynchronization therapy would help
Chest X-Ray
*provides useful info about size and shape & state of pulmonary vasculature
Treatment
*acute pts may have interstitial pulmonary edema
HF continuum
has 4 do
interrelated
stages
*chronic usually
not (increased
capacity of lymphatics to remove interstitial and/or pulmonary fluid)
Stage A: Pts high risk, but do not have HF (DM, HTN)
Assessment of LV
Stage B: Pts have structural heart disease but no symptoms of HF (previous MI, assymptomatic
LVFunction
dysfunction) Stage 1 NYHA- slow disease progression by blocking neurohormonal
*2-D
echo/doppler
essential
for
diagnosis,
evaluation,
and
management
of
HF
systems that lead to cardiac remodeling (treat w/ ACEI & BBs)
*provides
semiquantitative
assessment
size & function
Stage C:
Pts have
structural heart
disease of
& LV
symptoms
(previous MI, dyspnea, fatigue) Stage 2-4 NYHA Primary goal to alleviate fluid retention, lessen disability, & reduce risk of further
*assess LV wall motion abnormalities (valvular or regionalboth indicative of past MI)
disease progression (combo of diuretics & neurohormonal transmitters)
*presence of LAE, LVH, and diastolic abnormalities in regards to EF
Stage D: Pts w/ refractory HF requiring heart transplant (if 85, send to hospice) every effort should be made to treat preventable causes (HTN) and/or w/ drugs (ACEI & BBs)
*invaluable in assessing RV size & pulmonary pressures (critical to management of cor pulmonale)
MRI assesses LV structure, mass, volume & determining cause of HF (amyloidosis, ischemic cardiomyopathy, hemochromatosis)
Management
of useful
HF w/index
Depressed
EF (<40%)
*EF: most
of LV function
is EF (stroke volume/end diastolic volume)
Treat comorbidities:
HTN,
CAD, DM,since
anemia,
limit EtOH,
smoking,
sleep &apnea
*isnt a true measure
of contractility
it is influenced
by stop
alterations
in preload
afterload- but is good
*AVOID
NSAIDS,
cyclooxygenase
inhibitors
(riskwhen
renalEF
failure
retain fluid),
ANABOLIC
STERIODS (volume retention), & DIETARY SUPPLMENTS (unproven)
* EF
normal 50-70%,
and systolic2 usually
normal;
is low&
<30-40%
contractility
usually depressed
*should get influenza & pneumococcal vaccines- influenza & pneumovax (prevent respiratory infection)
Biomarkers
*Educate
families in HR
*Beta
Naturetic
Peptide(60%
(BNP)max
& N-terminal
pro-BNP
areexercise
released (stationary
from failing bike,
heart, walking)
and are relatively
sensitive
markers
for 1.presence of
& depressed
EF 2.
pts w/ preserved
3.
*Activity: nothing
strenuous
HR), modest
aerobic
beneficial
for class
1-IIIimproves
HFHR
symptoms,
QOL
& HF
increases
exercise EF
capacity
Important
to
know
natriuretic
peptide
levels
increase
w/
age
and
renal
impairment
(moreso
in
women)
&
can
be
elevated
in
right
HF
from
any
cause
**serial
measurement
not
recommended
*Diet: Na restriction (2-3 g/day)- further restriction for severe HF, fluid restriction unnecessary unless hypernatremia present (RAAS excessively excreting ADH or loss of salt)- usually class
troponin T & I, CrP, TNF, uric acid provide good prognostic data
IV *Note: if hyponatremic, and sodium restriction + diuretics not working, vasopressin antagonists helpful
*Increase caloric intake for patients with advanced HF or unintentional weight loss
Exercise Testing
*Not advocated for acute HF MAY BE HELPFUL IN CHRONIC HF TO ASSESS FOR TRANSPLANT
Diuretics (start w/ low dose, titrate upgoal is attempt to obtains pts dry weight--can be administered via IV (beneficial to relieve congestion accurately)
*only pharmalogical
agent that can control fluid retention in advanced HF & should be used to restore fluid in pts w/ congestive symptoms (dyspnea, orthopnea, edema)
Differential Diagnosis
*Loop HF
diuretics
torsemide,
bumetanide)
act on Loop
of Henle
by reversibly
absorption
of Na,2.K,
& cardiac
Cl in thick
ascending
limbedema
of Henles
(fractional
excretion of
should (furosemide,
be distinguished
from 1. Circulatory
congestions
secondary
to abnormal
salt and inhibiting
water retention
(renal failure)
Non
causes
of pulmonary
(acuteloop
respiratory
distress
NA 20-25%)
usually
usedsecondary
to restore
volume
in difficult
pts **watch
for hypokalemia
syndrome)
dyspnea
to normal
pulmonary
edemastatus
may be
to differentiate
(echo, BNP, pulmonary function testing helpful) 3. Ankle edema may arise secondary to varicose veins,
obesity, renal disease, or gravitational effects
Congestive Heart Failure
*Thiasizes & metolazone reduce reabsorption of Na and Cl in 1st of distal convoluted tubule (thiazide fractional excretion of NA 5-10%- tend to lose their effectiveness in pts w/ moderate
or severe renal insufficiency- creatinine >2.5 mg/dL) **watch for hypokalemia
*Potassium- sparing diuretics are aldosterone antagonists (spironolactone) act at level of collecting ductuse in class III and IV if needed **watch for hyperkalemia
*all increase sodium excretion & urinary volume= potency differs
*refractoriness (unruly/resistant) to diuretic therapy can be pt nonadherance, if not, use thiazides or metolazone (usually more potent and longer acting in this setting) 1 or 2 times a day w/
loop diureticIF THAT FAILS ULTRAFILTRATION & DIALYSIS ARE USED
Adverse Effects
*Electrolyte & volume depletion + worsening azotemia (high levels of N containing compounds urea/creatinine) can lead to worsening HF & more neurohormonal activity
* Most important adverse consequences is imbalance of K homeostatsiscan lead to life-threatening arrhythmias
ACE Inhibitors (initiated at low doses, increase dose until dose is similar to those shown to be effective in clinical trials)
*stop enzyme responsible for conversion of Angiotensin 1 to 2
* also inhibit kinase II, which may lead to further up regulation of bradykinin further enhances effects of angiotensin suppression
*stabilizes LV remodeling, improves symptoms, reduces hospitalizations, & prolong life
* diuretic can slow effects of ACE, so better to start diuretic before the ACE (may be necessary to reduce dose of diuretic during ACE initiation to prevent HTN)
Adverse Effects
*majority related to suppression of RAAS systemdecrease BP, mild azotemia, hyperkalemia, Angioedema
* if hypotension is accompanied w/ dizzy & poor renal function, reduce dose
Treatment Continued
ARB: used in ACE intolerant symptomatic/asymptomatic patients w/ an EF of <40% & who are intolerant for reasons other than hyperkalemia
*use for pts intolerant of ACE (cough, skin rash, angioedema)
*ARBs block the effects of angiotensin II on the angiotensin type I receptor
Adverse Effects
*majority related to suppression of RAAS systemdecrease BP, hypotensive, & hyperkalemia
B-Adrenergic Receptor Blocker: indicated for PTs w/ symptomatic or asymptomatic HF & a decreased EF of 40%-- start w/ low doses, titrate up (SLOWLY-2 week intervals- bcv
more chance of fluid retention) (carvedilol 25-50mg bid or metroprolol 200mg/day) + diuretic
*Antagonize B1, B2, and A2 receptors- B1 most potent
*when given with an ACE, beta blockers reverse LV remodeling, improve pt symptoms, prevent hospitalization & prolong life
*If fluid retention does occur w/in 3-5 days- more HF damage is occurring (may have to reduce dose like ACE)
*Comorbid issues (DM, COLD, and PVD) are tolerated well among majority- 10-15% dont tolerate well
Adverse Effects
*generally occur bc of concomitant medications taken w/ BBs
*not recommended for pts w/ asthma w/ active bronchospasm
Congestive Heart Failure
*bradycardia and heart blocks can be present
Aldosterone Antagonists: recommended w/ class III-IV HR w/ EF less than 35% (spironolactone-25-50mg/day & eplerenon-50 mg/day)
*potassium sparing diuretics that block the effects of aldosterone which have beneficial effects on sodium balance
*titrate up recommended dose
Adverse Effects
*life threatening hyperkalemia is the biggest issue (renal insufficient pts most at risk(
*not recommended when SCr is >2.5mg/dL or when serum potassium is >5mmol/L
*painful gynecomastia (big boobs) can develop- try switching from spironolactone to eplerenone
*for class II-IV African American pts, use hydralazine & isosorbide dinitrate in addition to ACE and BB
PTs Still Symptomatic
*Digoxin recommended for pts w/ symptomatic LV systolic dysfunction who have concomitant a-fib should also be considered for pts resistant to therapy who are in normal sinus rhythm
Anticoagulation (Wafarin) & Antiplatelet Therapy (Aspirin)
*depressed LV function is believed to promote relative stasis of blood in dilated cardiac chambers w/ increased risk of thrombus formation
*treatement w/ warfarin is recommended for pts w/ HF & chronic or pulmonary emboli, stoke or TIA (INR goal 2-3)
*pts w/ recent large anterior MI or recent MI w/ left ventricular thrombus- keep on Wafarin for 2-3 months
*aspirin is recommended in HF patients w/ ischemic heart attack disease for prevention of MI & death- lower doses usually preferably (81mg)
Antiarrythmic Therapy: Amiodarone preferred dofetilide backup
*A-fib occurs in 15-30% of pts w/ HF- which is worse for heart
* amiodarone has few or no negative inotropic and/or proarrythmic effects and is most effective againt supraventricular arrhythmiasincreases level of phenytoin & digoxin, which prolongs
INR in pts w/ warfarin, maintain/restores sinus rhythm & may improve electrical success for cardioconversion
Congestive Heart Failure
Implantable Cardiac Device: recommended for pts in sinus rhytm w/ an EF <35% and a QRS >120 ms + symptomatic pts (class III-IV) despite optial drug therapy
*1/3 of pts w/ depressed EF and symptomatic HD (class III-IV) manifest a QRS duration >120 ms.
* mechanical consequences of ventricular dyssynchronous ventricular contraction include: poor ventricular filling, reduction in LV contractility, prolonged duration of mitral regurg, and
paradoxical & septal wall motion
*benefits of CRT in PTs w/ a-fib HAVE NOT been established
Implantable Cardiac Defibrillator (ICD): Indicated in PTs at risk for sudden cardiac death w/ ischemic/nonischemic cardiomyopathy
*can also be considered for PTs in class II-III w/ EF <35% who have had optimal therapy up to this point and are still resistant
Management of HF w/ Preserved EF (>40-50%)- NONE proven, focus on underlying disease process (HTN, Ischemia, Dyspnea from diuretics/nitrates)
Acute Decomposition HF (ADHF): 2 primary hemodynamic determinants of ADHF 1. Elevated filling pressures 2. Depressed CO
Design Appropriate Therapeutic Strategy
1. Stabilize hemodynamic derangements that provoked symptoms
2. ID & treat reversible factors that caused decline/decompensation
3. Reestablish effective outpatient medical regimen
4 Hemodynamic Profiles- therapeutic approach should be tailored to reflect pts hemodynamic presentation
Congestive Heart Failure
A- Normal LV filling pressure w/ normal perfusion (not congested (dry) & have normal tissue perfusion(warm)) Sx usually not due to HF, but hepatic disease, PE, or TIA)
B- Elevated LV filling pressure w/normal perfusion (congested (wet) and normal tissue perfusion (warm) ) treat w/ vasodilators & diuretics
C- Elevated LV filling pressure w/decreased perfusion (congested (wet) and reduced CO and elevated SVR (cold) treat w/ IV inotropes- dobutamine, low-dose dopamine,
milrinone
L- Normal of low filling pressure w/ decreased tissue perfusion (not congested (dry) and reduced CO and elevated SVR (cold) CAREFUL EVAL VIA HEART CATH, IF
FILLING PRESSURES LOW (WEDGE PRESSURE <12 mmHG, TRIAL FLUID REPLACEMENT
Intravenous Vasodilator 2nd most useful med for acute HF (diuretic #1) nitroglycerin, nitroprusside, and nesirtide
*Stimulate guanylyl cyclase w/in smooth muscle cellsdilates arteries and veins lowering LV filling pressure (preload), lower mitral regurg, improves CO (afterload) w/ increase HR or
causing arrhythmias
*Goal:reduce symptoms, reduce LV filling pressure, avoid hypotension
Intravenous Inotropic Agents- improve CO and decrease LV filling pressure- dobutamine, milirone
*produce direct hemodynamic effects by stimulating cardiac contractility as well as by producing peripheral vasodilation
*dobutamine- most common- stimulates B1 and B2 receptors (little effect on A1 receptors)-vasodilates & increases CO- given as continuous effusion; higher doses needed for hypofusion
*milirone- phosphodiesterase III inhibitorincreases cAMP by inhibiting its breakdown- has greater increase on CO & more effective vasodilator than dobutamine but higher risk of
hypotension
*good short term use + hemodynamic benefits: agents prone to cause tachyarrythmias
Vasoconstrictors: support systemic BP in pts w/ HF (dopamine- 1st choice--epinephrine, & phenylephrine are potent- AVOID long use)
*dopamine: endogenous catecholamine stimulates A1 & B1 receptors & dopaminergic receptors (DA1/DA2)- effects dose dependent- low dose increase CO, high dose increase vasoconstrict
Vasopressin Antagonists: Tolvaptan (oral)_& Conivaptan (IV) approved for hyponatremia not for HF
Congestive Heart Failure
*reduce body weight, edema, & normalize associated improved outcomes
Cor Pulmonale (aka pulmonary heart disease)
*dilation and hypertrophy of R ventricle in response to disease of the pulmonary vasculature
*Etiology: develops in response to acute/chronic changes in vasculature sufficient to cause pulmonary HTN
*prognosis of pts with cor pulmonale + HF worsens prognosis (chronic bronchitis, COLD, cystic fibrosis, chronic hypoventilation-fat, neuromuscular disease, chest wall abnormality-living
at high altitude)s
*most common mechanisms that lead to pulmonary HTN, including vasoconstriction, activation of clotting cascade, & obliteration of pulmonary arterial vessels
Congestive Heart Failure
Mnemonics
CHF: causes of exacerbation A SMITH PEAR:
Anemia
Salt/ Stress/ Stopping meds
MI
Infection/ Ischemia
Thyroid (high/low)
HTN
Pericarditis
Endocarditis (valve disease)
Arrhythmia
Rx (beta blocker, etc)
Heart failure: signs TAPED TORCH:
Tachycardia
Ascites
Pulsus alternans
Elevated jugular venous pressure
Displaced apex beat
Third heart sound
Oedema
Right ventricular heave
Crepitations or wheeze
Hepatomegaly (tender)
CHF: Left-sided systolic failure signs and symptoms "Left Systolic Failure Can Have Dialated Heart Cause Of Pulmpnary Backflow":
Loss of hair on legs
Skin cold and clammy
Fatigue
Crackles
Congestive Heart Failure
High heart rate
Dyspnea
HTN
Cyanosis
Orthopnea
Pink Sputum
Acute LVF management LMNOP:
Lasex (frusemide)
Morphine (diamorphine)
Nitrates
Oxygen (sit patient up)
Pulmonary ventilation (if doing badly)
Heart compensatory mechanisms that 'save' organ blood flow during shock "Heart SAVER":
Symphatoadrenal system
Atrial natriuretic factor
Vasopressin
Endogenous digitalis-like factor
Renin-angiotensin-aldosterone system
In all 5, system is activated/factor is released
> Heart failure: causes HEART FAILED:
Hypertension
Endocrine
Anemia
Rheumatic heart disease
Toxins
Failure to take meds
Arrythmia
Infection
Lung (PE, pneumonia)
Congestive Heart Failure
Electrolytes
Diet
Вам также может понравиться
- Psychiatry For Medical Students and ResidentsДокумент80 страницPsychiatry For Medical Students and ResidentsNabeel Kouka, MD, DO, MBA, MPH100% (4)
- Congestive Heart Failure LectureДокумент102 страницыCongestive Heart Failure Lectureluke100% (1)
- North American Indians - A Very Short IntroductionДокумент147 страницNorth American Indians - A Very Short IntroductionsiesmannОценок пока нет
- Heart Failure: Low Output HF High Output HFДокумент7 страницHeart Failure: Low Output HF High Output HFJake BurrОценок пока нет
- Congestive Heart Failure Guide: Causes, Symptoms, TreatmentsДокумент64 страницыCongestive Heart Failure Guide: Causes, Symptoms, TreatmentsBentoys StreetОценок пока нет
- Pathogenesis of Micro and Macrovascular Complications of DiabetesДокумент4 страницыPathogenesis of Micro and Macrovascular Complications of DiabetesFrancesca LiОценок пока нет
- Systolic Dysfunction:: Types of Heart FailureДокумент13 страницSystolic Dysfunction:: Types of Heart FailureElisabeth F. OjhaОценок пока нет
- Cardiovascular & Hematologic SystemДокумент309 страницCardiovascular & Hematologic Systemnursereview100% (3)
- CC Concept MapДокумент11 страницCC Concept Mapapi-546355187Оценок пока нет
- Case Study On Alcoholic Liver DiseaseДокумент20 страницCase Study On Alcoholic Liver DiseaseHomework PingОценок пока нет
- Ebstein Anomaly, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОт EverandEbstein Anomaly, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОценок пока нет
- Hemorrhagic Cerebro Vascular DiseaseДокумент37 страницHemorrhagic Cerebro Vascular Diseasejbvaldez100% (1)
- The Pathophysiology and Pharmacotherapy of Myocardial InfarctionОт EverandThe Pathophysiology and Pharmacotherapy of Myocardial InfarctionNabil El-SherifОценок пока нет
- Chronic Kidney DiseaseДокумент33 страницыChronic Kidney DiseasesexiiimammaОценок пока нет
- Nicolas-Lewis vs. ComelecДокумент3 страницыNicolas-Lewis vs. ComelecJessamine OrioqueОценок пока нет
- A Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsОт EverandA Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsОценок пока нет
- Learning Objectives:: Pathophysiology & Therapeutics, I (MSPR 521) Lecture No. 14Документ9 страницLearning Objectives:: Pathophysiology & Therapeutics, I (MSPR 521) Lecture No. 14adzhangОценок пока нет
- Care of Adults 25 Cardiovascular ManagementДокумент39 страницCare of Adults 25 Cardiovascular ManagementGaras AnnaBerniceОценок пока нет
- A Simple Guide to Circulatory Shock, Diagnosis, Treatment and Related ConditionsОт EverandA Simple Guide to Circulatory Shock, Diagnosis, Treatment and Related ConditionsОценок пока нет
- Stroke and Cerebrovascular DiseaseДокумент14 страницStroke and Cerebrovascular DiseaseMarwan M.Оценок пока нет
- Music 146 SyllabusДокумент4 страницыMusic 146 SyllabusNatОценок пока нет
- Heart Failure Guide for NursesДокумент54 страницыHeart Failure Guide for NursesKacelyn QuibanОценок пока нет
- Portal HypertensionДокумент65 страницPortal HypertensionVenu MadhavОценок пока нет
- Upper GIT BleedingДокумент69 страницUpper GIT BleedingSoleh Ramly100% (1)
- Valvular Heart DiseaseДокумент10 страницValvular Heart DiseaseEzyan SyaminОценок пока нет
- Medscape Hypovolemic ShockДокумент14 страницMedscape Hypovolemic ShockSarah Ovinitha100% (1)
- Peptic Ulcer DiseaseДокумент20 страницPeptic Ulcer Diseasedr_IstiqlalMiftahulJannahОценок пока нет
- Diagnosing Chest Pain CausesДокумент8 страницDiagnosing Chest Pain CausesMedisina101Оценок пока нет
- Dynamics of Bases F 00 BarkДокумент476 страницDynamics of Bases F 00 BarkMoaz MoazОценок пока нет
- Acute Coronary Syndromes-PresentationДокумент86 страницAcute Coronary Syndromes-Presentationpatange jayaprakash rahul100% (4)
- Congestive Heart FailureДокумент12 страницCongestive Heart FailureyvasparksОценок пока нет
- 10 CardiomyopathyДокумент71 страница10 CardiomyopathyAnonymous vUEDx8100% (4)
- Congestive Heart Failure PathophysiologyДокумент7 страницCongestive Heart Failure PathophysiologyAileen Grace RodrigoОценок пока нет
- Cardiogenic ShockДокумент20 страницCardiogenic Shockanimesh pandaОценок пока нет
- Congenital Heart DiseaseДокумент45 страницCongenital Heart DiseaseBrandedlovers OnlineshopОценок пока нет
- Course Syllabus (NGCM 112)Документ29 страницCourse Syllabus (NGCM 112)Marie Ashley Casia100% (1)
- Congestive Cardiac FailureДокумент38 страницCongestive Cardiac FailureSalman KhanОценок пока нет
- Congestive Heart FailureДокумент19 страницCongestive Heart FailureIlavenil PanduranganОценок пока нет
- UrosepsisДокумент22 страницыUrosepsisWita Ferani KartikaОценок пока нет
- Ganzon Vs CAДокумент3 страницыGanzon Vs CARaymond RoqueОценок пока нет
- Acute Coronary SyndromeДокумент5 страницAcute Coronary SyndromeLuis OportoОценок пока нет
- The Discrimination ModelДокумент16 страницThe Discrimination ModelSiti MuslihaОценок пока нет
- AnovaДокумент26 страницAnovaMuhammad NasimОценок пока нет
- Limitations For The Study: Celebrity ViewsДокумент3 страницыLimitations For The Study: Celebrity ViewsPakaya100% (2)
- Ashforth & Mael 1989 Social Identity Theory and The OrganizationДокумент21 страницаAshforth & Mael 1989 Social Identity Theory and The Organizationhoorie100% (1)
- Congestive Heart FailureДокумент14 страницCongestive Heart FailureBella Trix PagdangananОценок пока нет
- Evaluation of Chest Pain: Ruling Out Life ThreatsДокумент16 страницEvaluation of Chest Pain: Ruling Out Life ThreatsAbhinit RiddhiОценок пока нет
- CARDIOVASCULAR DISEASES: SIGNS, SYMPTOMS AND TREATMENT OF HEART FAILUREДокумент27 страницCARDIOVASCULAR DISEASES: SIGNS, SYMPTOMS AND TREATMENT OF HEART FAILURESanthoshi Sadhanaa SankarОценок пока нет
- Left-Sided Congestive Heart Failure Case PresentationДокумент64 страницыLeft-Sided Congestive Heart Failure Case PresentationNicole Villanueva, BSN - Level 3AОценок пока нет
- Acute Hypertension-Hypertensive Urgency and Hypertensive EmergencyДокумент13 страницAcute Hypertension-Hypertensive Urgency and Hypertensive EmergencyAmitKumarОценок пока нет
- Management of Severe Hypertension, Hypertension in Special ConditionДокумент43 страницыManagement of Severe Hypertension, Hypertension in Special Conditionabhandlung100% (3)
- Congestive Heart FailureДокумент28 страницCongestive Heart Failuresarguss1480% (5)
- Cardiovascular DiseaseДокумент6 страницCardiovascular DiseaseDominique Excelsis J. DegamoОценок пока нет
- Capstone Case Study Final - CHFДокумент3 страницыCapstone Case Study Final - CHFapi-351999622Оценок пока нет
- Cardiomyopathy and MyocarditisДокумент8 страницCardiomyopathy and Myocarditisoddone_out100% (1)
- Case Study: Congestive Heart FailureДокумент7 страницCase Study: Congestive Heart FailureXI-E / 21 / MARY TRIANAОценок пока нет
- Congestive Heart Failure OverviewДокумент12 страницCongestive Heart Failure OverviewkazelleОценок пока нет
- Pa Tho Physiology of Congestive Heart FailureДокумент3 страницыPa Tho Physiology of Congestive Heart FailureErin MarieОценок пока нет
- ConceptMap AMLДокумент1 страницаConceptMap AMLnursing concept mapsОценок пока нет
- Cardiovascular ExaminationДокумент2 страницыCardiovascular ExaminationasimОценок пока нет
- Case Study PPT Patho NLNGДокумент36 страницCase Study PPT Patho NLNGKate ChavezОценок пока нет
- 1 LiverДокумент10 страниц1 LiverAlbino Fulgencio Santos III100% (1)
- Hypertensive Cardiovascular DiseaseДокумент16 страницHypertensive Cardiovascular DiseaseTintin Ponciano100% (1)
- Valvular Heart Disease 2Документ46 страницValvular Heart Disease 2Topea BogdanОценок пока нет
- PericarditisДокумент11 страницPericarditisrbarcellonaОценок пока нет
- CHF PathophysiologyДокумент4 страницыCHF PathophysiologyVirtudazo JessaОценок пока нет
- Congestive Heart Failure (CHF) PDFДокумент2 страницыCongestive Heart Failure (CHF) PDFZazulizer Are BackОценок пока нет
- Esophageal Varices Week 4 T2T3Документ37 страницEsophageal Varices Week 4 T2T3liewhuilianОценок пока нет
- Problem-based Approach to Gastroenterology and HepatologyОт EverandProblem-based Approach to Gastroenterology and HepatologyJohn N. PlevrisОценок пока нет
- A Simple Guide to Abdominal Aortic Aneurysm, Diagnosis, Treatment and Related ConditionsОт EverandA Simple Guide to Abdominal Aortic Aneurysm, Diagnosis, Treatment and Related ConditionsОценок пока нет
- 3 - Heart Failure (Modified)Документ17 страниц3 - Heart Failure (Modified)Ali Al-QudsiОценок пока нет
- Valvular Disease HeartДокумент12 страницValvular Disease HeartyvasparksОценок пока нет
- CardiomyopathiesДокумент4 страницыCardiomyopathiesyvasparksОценок пока нет
- Congenital Heart DefectsДокумент2 страницыCongenital Heart DefectsyvasparksОценок пока нет
- CardiomyopathiesДокумент1 страницаCardiomyopathiesyvasparksОценок пока нет
- Musculoskeletal Exam Skills Self-studyДокумент87 страницMusculoskeletal Exam Skills Self-studyGilberto Solares0% (1)
- My Testament On The Fabiana Arejola M...Документ17 страницMy Testament On The Fabiana Arejola M...Jaime G. Arejola100% (1)
- Opinions and ThoughtsДокумент2 страницыOpinions and Thoughtsfikri alfaroqОценок пока нет
- Absolute TowersДокумент11 страницAbsolute TowersSandi Harlan100% (1)
- Corneal Ulcers: What Is The Cornea?Документ1 страницаCorneal Ulcers: What Is The Cornea?me2_howardОценок пока нет
- As 3778.6.3-1992 Measurement of Water Flow in Open Channels Measuring Devices Instruments and Equipment - CalДокумент7 страницAs 3778.6.3-1992 Measurement of Water Flow in Open Channels Measuring Devices Instruments and Equipment - CalSAI Global - APACОценок пока нет
- GUIA REPASO 8° BÁSICO INGLÉS (Unidades 1-2)Документ4 страницыGUIA REPASO 8° BÁSICO INGLÉS (Unidades 1-2)Anonymous lBA5lD100% (1)
- Republic v. EncelanДокумент2 страницыRepublic v. EncelanKyla ReyesОценок пока нет
- Signal WordsДокумент2 страницыSignal WordsJaol1976Оценок пока нет
- Social Media Marketing - AssignmentДокумент8 страницSocial Media Marketing - AssignmentAllen RodaОценок пока нет
- Academic Transcript Of:: Issued To StudentДокумент3 страницыAcademic Transcript Of:: Issued To Studentjrex209Оценок пока нет
- Larry Dossey - HealingBeyondtheBodyДокумент2 страницыLarry Dossey - HealingBeyondtheBodypaulxeОценок пока нет
- Wound Healing (BOOK 71P)Документ71 страницаWound Healing (BOOK 71P)Ahmed KhairyОценок пока нет
- Notes On Statement AssumptionДокумент5 страницNotes On Statement Assumptionsangamesh mbОценок пока нет
- Ghana Constitution 1996Документ155 страницGhana Constitution 1996manyin1Оценок пока нет
- Mpeg-1 11172-1Документ46 страницMpeg-1 11172-1Hana HoubaОценок пока нет
- SMAW Product DevelopmentДокумент9 страницSMAW Product Developmenttibo bursioОценок пока нет
- Jaimini Astrology - Calculation of Mandook Dasha With A Case StudyДокумент6 страницJaimini Astrology - Calculation of Mandook Dasha With A Case StudyANTHONY WRITER100% (3)
- Letter of Recommendation SamplesДокумент3 страницыLetter of Recommendation SamplesLahori MundaОценок пока нет
- 1 CH - 7 - WKSHTДокумент8 страниц1 CH - 7 - WKSHTJohnОценок пока нет