Академический Документы
Профессиональный Документы
Культура Документы
Total External Ophthalmoplegia Induced by Phenytoin A Case
Загружено:
Gheavita Chandra DewiОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Total External Ophthalmoplegia Induced by Phenytoin A Case
Загружено:
Gheavita Chandra DewiАвторское право:
Доступные форматы
Short Reports
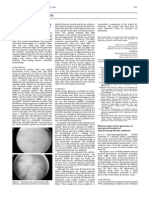
tive reaction for Synaptophysin and Chromogranin. The picture was
consistent with desmoplastic infantile ganglioglioma.
Discussion
Desmoplastic supratentorial neuroepithelial tumors of infancy form a rare but distinctive group of tumors occurring in
children less than 2 years of age. Vanden Berg et al1 (1987),
named these tumors as desmoplastic cerebral astrocytoma of
infancy and desmoplastic infantile ganglioglioma (DIG), on
the basis of immunohistochemistry and electron microscopy.
Both these groups of tumors occur in children less than 2
years of age. They have identical clinical and radiological features and both have favorable outcome following successful
excision. Subsequently, these groups of tumors have been included as a distinctive group, in the revised World Health
Organization (WHO) classification of brain tumors (Kleihues
et al21993).
Less than 50 cases of desmoplastic infantile ganglioglioma
(DIG) have been reported in the literature. Several authors
have reported single case reports and small series of cases of
DIG.3,4 The youngest patient has been 4 months of age. All
these children presented with macrocephaly, seizures, psychomotor delay, either in isolation or in combination. All these
patients have similar Computerized Tomographic scan (CT)
and Magnetic Resonance Imaging (MRI) characteristics (Martin et al 1991, Tenreiro-Picon et al5,6 1995). The tumors commonly occur in frontal or parietal lobes, with a solid component closely attached to the dura, which intensely enhances
with contrast, surrounded by a parenchymal cystic component and mass effect. Most of these tumors are amenable to
surgical excision because of their surface location and distinct
firmness with clear demarcation from the surrounding normal brain. No adjuvant therapy is recommended after total
excision, despite the fact that the lesion has a low malignant
potential. Long-term prognosis after total surgical excision
has been excellent in all the reported series.
Histologically, these tumors have intense desmoplasia, with
neoplastic astrocytes with occasional neuronal elements.
Desmoplastic cerebral astrocytoma of infancy and DIG are
difficult to differentiate under light microscopy. Immunohistochemistry plays a very important role in the diagnosis of
DIG. In DIG, the tumor shows intense positivity for Glial
Fibrillary Acidic Protein (GFAP) which is a glial marker, with
areas positive for synaptophysin or neurofilament
immunostain, which are neuronal markers. In desmoplastic1,4,7
cerebral astrocytoma, there is positivity for GFAP only.
References
1.
2.
3.
4.
5.
6.
7.
Vanden Berg SR, May EE, Rubeinstein LJ, et al. Desmoplastic supratentorial
neuroepithelial tumors of infancy with divergent differentiation potential
(desmoplastic infantile gangliogliomas). J Neurosurg 1987;66:58-71.
Kleihues P, Burger PC, Scheithauer BW. The new WHO classification of brain
tumors. Brain Pathol 1993;3:255-68.
Duffner PK, Burger PC, Cohen ME, et al. Desmoplastic infantile
gangliogliomas: An approach to therapy. Neurosurg 1994;34:583-9.
Sperner J, Gottschalk J, Neumann K, et al. Clinical, radiological and histological findings in desmoplastic infantile ganglioglioma. Childs Nerv Syst
1994;10:458-63.
Martin DS, Levy B, Awwad EE, et al. Desmoplastic infantile ganglioglioma:
CT and MR features. Am J Neuroradiol. 1991;12:1195-7.
Tenreiro-Picon OR, Kamath SV, Knorr JR, et al. Desmoplastic infantile
ganglioglioma: CT and MRI features. Pediatr Radiol 1995;25:540-3.
VandenBerg SR. Desmoplastic infantile ganglioglioma and desmoplastic cerebral astrocytoma of infancy. Brain Pathol 1993;3:275-81.
Accepted on 11.11.2003.
Total external ophthalmoplegia induced by phenytoin: A case
report and review of literature
Vinod Puri, Neera Chaudhry
Department of Neurology, G. B. Pant Hospital, New Delhi - 110002, India.
A 28-year-old male developed total external ophthalmoplegia following oral administration of phenytoin. The case is
reported and its significance is discussed.
Key Words: External ophtalmoplegia, Phenytoin induced
ophtalmoplegia, phenytoin toxicity.
Introduction
There have been innumerable reports concerning phenytoin
toxicity, but few have mentioned its effects on eye movements
other than nystagmus.1 Ophthalmoplegia has been reported
with administration of large doses of Phenytoin,2,3 Phenobar-
Vinod Puri
16, Type 5, MAMC Campus, New Delhi - 110002, India. E-mail: vpuri@bol.net.in
386
386 CMYK
Neurology India September 2004 Vol 52 Issue 3
Short Reports
bitone, Primodone, Carbamazepine and Amitriptyline. Spector
et al2 reported that phenytoin could induce total external ophthalmoplegia irrespective of oral or intravenous administration. Incomplete4 as well as complete ophthalmoplegia5 has
been reported with phenytoin even within therapeutic range.
We present a patient with phenytoin intoxication who developed disturbances in the ocular movements.
Case Report
A 28-year-old mentally retarded male, with IQ-55, had generalized tonic-clonic epilepsy for two years. He was placed on
carbamazepine (Tegretol) 800mg per day. However, due to financial
reasons, he was irregular with his treatment. Subsequently, he was
placed on Diphenyl hydantoin (300mg per day). After about two
weeks of the change in the drug treatment he reported inability to
move his eyes. He denied excessive ingestion of the drug. The pupils
were 5mm in diameter, round, equal and reacting well to light. The
gaze was fixed directly forward. The patient did not move his eyes on
command and could not follow the light. The eyes could not be moved
by head turning or neck bending or by irrigation of the ears with ice
water. Fundi were normal. The rest of the neurological examination
was normal. The cerebrospinal fluid examination was normal. The
CT of the head was normal. The phenytoin drug level was 22 microgm
per ml. The phenytoin was withdrawn and he was given loading dose
of phenobarbitone, followed by its maintenance dose. On the fifth
day, he could move his eyes about 100 in horizontal direction (laterally and medially) but was unable to move them in the vertical direction. On the seventh day, the horizontal movements had improved
and he could move the eyes slightly downward but not upward. Irrigation of the left ear with ice cold water produced no movements of
the eyes but irrigation of right ear produced occasional nystagmus
with fast component to the left. On the eleventh day his eye movements were normal. He was seizure-free on 120 mgm of phenobarbitone per day.
rigation may occur even when the blood phenytoin level is
within the accepted therapeutic range.
GABA mediates the inhibition of oculomotor neurons produced by the vestibular system. Phenytoin increases the postsynaptic potentials produced by GABA in the cerebral cortex7
and the spinal cord. Spector et al2 attributed the unresponsive cold caloric irrigation with phenytoin to an increased effectiveness of GABA-induced inhibition at the synapses of the
vestibulo-oculomotor system. The lag in the recovery of the
oculovestibular response in the present case could be explained
with the above said hypothesis.
The cerebellum has an inhibitory role over the vestibular
ocular reflex through Purkinje cells. Phenytoin increases the
rate of Purkinje cell discharge.8 Whether this phenytoin-augmented Purkinje cell firing would act in a manner analogous
to electric stimulation of the cerebellar cortex and result in
the depression of transmission through the vestibular nucleus
and affect the normal function of the vestibulo-ocular apparatus is unclear. The majority of the reported cases of phenytoin-induced ophthalmoplegia recovered completely over a
variable period with normalization of the phenytoin level.
The present case is unique; in spite of the drug toxicity the
patient was alert and had bilateral external ophthalmoplegia
with loss of oculocephalic and oculovestibular reflexes. The
recognition of this entity is important to avoid unnecessary
investigations in a patient on phenytoin.
References
1.
2.
3.
Discussion
Phenytoin is a vestibular depressant.6 Spector et al2 observed
that the return of vestibulo-ocular response in their patients
with phenytoin intoxication lagged behind the return of consciousness and other reflex activities and attributed it to its
depressant effect on the vestibulo-oculomotor system which
may be out of proportion to its actions on other levels of the
neuraxis. The oculomotor unresponsiveness to cold caloric ir-
4.
5.
6.
7.
8.
Remler BF, Leigh RJ, Osorio I, Tomsak RL. The characteristics and mechanisms of visual disturbance associated with anticonvulsant therapy. Neurology
1990;40:791-6.
Spector RH, Davidoff RA, Schwartzman RJ. Phenytoin-induced ophthalmoplegia. Neurology 1976;26:1031-4.
Fredericks CA, Giannotta SL, Sadun AA. Dilantin-induced long-term bilateral
total external ophthalmoplegia. Clin Neuro ophthalmol 1986;6:22-6.
Manlapaz JS: Abducens nerve palsy in Dilatin intoxication. J Pediatr
1959;55:73-4.
Sandyk R. Total external ophthalmoplegia induced by phenytoin. A case report. S Afr Med J 1984;28;65:141-2.
Posner JB, Plum F: Diagnostic significance of vestibulo-ocular responses. Neurol
Neurosurg Psychiatry 1975;38:727-8.
Davidoff RA: Dipenylhydantoin increases spinal presynaptic inhibition. Trans
Am Neurol Assoc 1972;97:193-5.
Halpern LM, Julien RM: Augmentation of cerebellar Purkinje cell discharge
rate after diphenylhydantoin. Epilepsia 1972,13:377-85.
Accepted on 12.06.2003.
Calvarial malignant fibrous histiocytoma
R. Chhabra, S. K. Gupta, K. S. Manjunath Prasad, D. Gupta*, R. K. Vasishta*, R. K. Sharma**,
V. K. Khosla
Departments of Neurosurgery, *Pathology and **Plastic Surgery , PGIMER, Chandigarh, India.
S. K. Gupta
Additional Professor, Department of Neurosurgery, PGIMER, Chandigarh - 160012, India. E-mail: sktulika@yahoo.com
Neurology India September 2004 Vol 52 Issue 3
387
CMYK 387
Вам также может понравиться
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5795)
- TranslateДокумент3 страницыTranslateGheavita Chandra DewiОценок пока нет
- Gleeson 1993Документ2 страницыGleeson 1993Gheavita Chandra DewiОценок пока нет
- Maternal Obesity, Gestational Hypertension, and Preterm DeliveryДокумент8 страницMaternal Obesity, Gestational Hypertension, and Preterm DeliveryGheavita Chandra DewiОценок пока нет
- Doppler Ultrasound in The Assessment of Suspected Intra-Uterine Growth RestrictionДокумент10 страницDoppler Ultrasound in The Assessment of Suspected Intra-Uterine Growth RestrictionGheavita Chandra DewiОценок пока нет
- Vitamin E in Preeclampsia: Lucilla Poston, Maarten Raijmakers, and Frank KellyДокумент7 страницVitamin E in Preeclampsia: Lucilla Poston, Maarten Raijmakers, and Frank KellyGheavita Chandra DewiОценок пока нет
- Plasma, Urinary, and Salivary 8-Epi-Prostaglandin F Levels in Normotensive and Preeclamptic PregnanciesДокумент4 страницыPlasma, Urinary, and Salivary 8-Epi-Prostaglandin F Levels in Normotensive and Preeclamptic PregnanciesGheavita Chandra DewiОценок пока нет
- Assessment of Gestational Age in The First Trimester of Pregnancy by Maximum Fetal DiameterДокумент4 страницыAssessment of Gestational Age in The First Trimester of Pregnancy by Maximum Fetal DiameterGheavita Chandra DewiОценок пока нет
- OsteoporosisДокумент3 страницыOsteoporosisGheavita Chandra DewiОценок пока нет
- OsteoporosisДокумент6 страницOsteoporosisGheavita Chandra DewiОценок пока нет
- Rheumathoid ArthritisДокумент5 страницRheumathoid ArthritisGheavita Chandra DewiОценок пока нет
- Ankyloblepharon Filiforme Adnatum: A Case ReportДокумент4 страницыAnkyloblepharon Filiforme Adnatum: A Case ReportGheavita Chandra DewiОценок пока нет
- Embryology-Nervous System DevelopmentДокумент157 страницEmbryology-Nervous System DevelopmentGheavita Chandra DewiОценок пока нет
- OsteoporosisДокумент8 страницOsteoporosisGheavita Chandra DewiОценок пока нет
- Research: Lateral Wedge Insoles For Medial Knee Osteoarthritis: 12 Month Randomised Controlled TrialДокумент9 страницResearch: Lateral Wedge Insoles For Medial Knee Osteoarthritis: 12 Month Randomised Controlled TrialGheavita Chandra DewiОценок пока нет
- DafputДокумент1 страницаDafputGheavita Chandra DewiОценок пока нет
- Letters To The EditorДокумент8 страницLetters To The EditorGheavita Chandra DewiОценок пока нет
- JPMA (Journal of Pakistan Medical Association) Vol 53, No.2, Feb. 2003Документ10 страницJPMA (Journal of Pakistan Medical Association) Vol 53, No.2, Feb. 2003Gheavita Chandra DewiОценок пока нет
- Daftar PustakaДокумент1 страницаDaftar PustakaGheavita Chandra DewiОценок пока нет
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- User Manual: VT5230 VentilatorДокумент183 страницыUser Manual: VT5230 VentilatorArtur FloriánОценок пока нет
- Acute Lymphoblastic LeukemiaДокумент5 страницAcute Lymphoblastic LeukemiaernitaОценок пока нет
- Febrile Seizure: Dr. Masdar Muid, Sp. A (K)Документ18 страницFebrile Seizure: Dr. Masdar Muid, Sp. A (K)Kani0% (1)
- Fcps IMMДокумент22 страницыFcps IMMHaseeb Rasool0% (1)
- Foundations of QigongДокумент7 страницFoundations of QigongAudrygodwynОценок пока нет
- CHAPTER 7: Mood Disorders and SuicideДокумент13 страницCHAPTER 7: Mood Disorders and SuicideDana Mikaella CervaОценок пока нет
- Firefly Product BrochureДокумент20 страницFirefly Product BrochureKidz to Adultz ExhibitionsОценок пока нет
- Platelet Counting Fordirect Indirect MethodДокумент30 страницPlatelet Counting Fordirect Indirect MethodShana Flame Haze100% (2)
- Appendix XVI D. Microbiological Quality of Non-Sterile Pharmaceutical Preparations and Substances For Pharmaceutical UseДокумент2 страницыAppendix XVI D. Microbiological Quality of Non-Sterile Pharmaceutical Preparations and Substances For Pharmaceutical UseJagdish ChanderОценок пока нет
- Uveitis and IritisДокумент5 страницUveitis and IritisHester Marie SimpiaОценок пока нет
- Cam4 6 1861Документ10 страницCam4 6 1861Ćatke TkećaОценок пока нет
- Psychology Presentation Chapter 10 - Life Span DevelopmentДокумент15 страницPsychology Presentation Chapter 10 - Life Span DevelopmentEduardo VillanuevaОценок пока нет
- Eating DisordersДокумент238 страницEating DisordersIldikó Márton100% (5)
- The Doctor Will Sue You NowДокумент11 страницThe Doctor Will Sue You NowMateja MijačevićОценок пока нет
- Character Styles Introduction PDFДокумент4 страницыCharacter Styles Introduction PDFKOSTAS BOUYOUОценок пока нет
- Bumetanide MIMSДокумент2 страницыBumetanide MIMSIndri WahyuniОценок пока нет
- Case Solutions For Personality Theories Workbook 6th Edition by AshcraftДокумент7 страницCase Solutions For Personality Theories Workbook 6th Edition by AshcraftMonikaОценок пока нет
- Hayes, Villatte, Levin, Hildebrandt ARCP 2011Документ30 страницHayes, Villatte, Levin, Hildebrandt ARCP 2011JohnОценок пока нет
- Safety of Magnesium Sulfate For Management of Severe Pre-Eclampsia and Eclampsia: A Practical Review of Research FindingsДокумент15 страницSafety of Magnesium Sulfate For Management of Severe Pre-Eclampsia and Eclampsia: A Practical Review of Research FindingsJhpiegoОценок пока нет
- The Aetiology of Gingival RecessionДокумент4 страницыThe Aetiology of Gingival RecessionshahidibrarОценок пока нет
- Activity 2Документ3 страницыActivity 2Neliza SalcedoОценок пока нет
- Austin Journal of Nuclear Medicine and RadiotherapyДокумент5 страницAustin Journal of Nuclear Medicine and RadiotherapyAustin Publishing GroupОценок пока нет
- American Board of Family Medicine: TTT SAMPLE TTTДокумент72 страницыAmerican Board of Family Medicine: TTT SAMPLE TTTSalah Elbadawy100% (1)
- Design of Facilities For The Mentally RetardedДокумент55 страницDesign of Facilities For The Mentally RetardedNevin NicksonОценок пока нет
- Pengaruh Massage Kaki Terhadap Penurunan Insomnia Pada Lansia Di Banjar Temesi Desa Temesi Kabupaten GianyarДокумент12 страницPengaruh Massage Kaki Terhadap Penurunan Insomnia Pada Lansia Di Banjar Temesi Desa Temesi Kabupaten Gianyar119 CIKOKOLОценок пока нет
- Program and Proceedings - 4th Caribbean Biomedical Research Days CBRD-2017, Jan 16-18, 2017, Rodney Bay, St. LuciaДокумент18 страницProgram and Proceedings - 4th Caribbean Biomedical Research Days CBRD-2017, Jan 16-18, 2017, Rodney Bay, St. LuciaISBS_SocietyОценок пока нет
- Myoskeletal Injuries in The Podiatric ProfessionДокумент10 страницMyoskeletal Injuries in The Podiatric ProfessionelproedrosОценок пока нет
- Psychodynamic Theories of Schizophrenia - Revisited: 6 Review PaperДокумент10 страницPsychodynamic Theories of Schizophrenia - Revisited: 6 Review PaperJuan Carlos SaguyodОценок пока нет
- Diabetes Mellitus Drug ChartДокумент3 страницыDiabetes Mellitus Drug Chartlui.stephanie1751100% (1)
- NHS Highland Wound Management Guidelines and FormularyДокумент91 страницаNHS Highland Wound Management Guidelines and FormularyAnton NopiarОценок пока нет