Академический Документы
Профессиональный Документы
Культура Документы
Cutaneous Leishmaniasis
Загружено:
RVDАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Cutaneous Leishmaniasis
Загружено:
RVDАвторское право:
Доступные форматы
Cutaneous Leishmaniasis: Recognition and Treatment
WILLIAM H. MARKLE, M.D., and KHALDOUN MAKHOUL, M.D.
University of Pittsburgh Medical Center, McKeesport Hospital, McKeesport, Pennsylvania
Cutaneous leishmaniasis is a parasitic disease occurring throughout the Americas from Texas
to Argentina, and in the Old World, particularly the Middle East and North Africa. It is spread
by the female sandfly. The condition is diagnosed every year in travelers, immigrants, and
military personnel. Physicians in the United States must be alert to the diagnosis of leishmaniasis in travelers returning from endemic areas. Physicians working for short periods in
endemic areas often must make the diagnosis and should be aware of local disease patterns.
When faced with a possible leishmanial skin lesion, a skin scraping with microscopic analysis
is the best test. Punch biopsies with tissue-impression smears also can be diagnostic. Needle
aspiration of tissue fluid from the margin of a lesion can yield fluid for culture to isolate
the organism and identify the species. Immunologic tests are being developed, including a
highly sensitive polymerase chain reaction test. The treatment mainstay is pentavalent antimony (e.g., sodium stibogluconate). Not all patients require treatment; many lesions heal
spontaneously. Antimonials have a high incidence of reversible adverse effects. Other medications used for treatment include amphotericin B, pentamidine isethionate, paromomycin,
and antifungals. This disease must be considered in at-risk patients, and family physicians
should know the basics of diagnosis and where to go for more help. (Am Fam Physician
2004;69:455-60. Copyright 2004 American Academy of Family Physicians.)
See page 1339 for definitions of strength-ofrecommendation labels.
eishmaniasis is endemic in 88
countries throughout Africa, Asia,
Europe, and North and South
America.1 There are an estimated
12 million cases worldwide, with
1.5 to 2 million new cases each year. Although
the incidence of leishmaniasis is greater in the
Old World than in the New World, the U.S.
traveler is most likely to contract this disease
in Latin America. Fifty to 100 cases of New
World cutaneous leishmaniasis are diagnosed
each year in the United States. They are contracted mainly in Peru and Brazil, although
the disease is endemic and can be contracted in
any country from Mexico to Argentina, except
Uruguay and Chile.2 There also is an endemic
focus in Texas. Leishmaniasis is a disease associated with rural areas and poverty, but it has
adapted to the urban environment as well.
In World War II, there was a high incidence
of leishmaniasis and sandfly fever in troops
deployed to the Persian Gulf region. In the Gulf
War (1990 to 1991), approximately 697,000
U.S. troops were deployed in this region. Only
19 cases of cutaneous leishmaniasis and 12
cases of visceral disease were diagnosed in this
group. The improvement came about because
of the use of insecticides and repellents, lower
transmission rates in the summer, and more
time spent in urban areas.3,4 About 150 cases of
leishmaniasis have reportedly been diagnosed
in U.S. soldiers serving in Iraq in 2003, and
more are expected.5 Preliminary data on 22
cases of cutaneous leishmaniasis contracted by
American troops in Afghanistan, Kuwait, and
Iraq and treated at Walter Reed Army Medical
Center between August 2002 and September
2003 were recently released.6 The majority of
these persons were infected with Leishmania
major in urban areas of Iraq after a median
period of deployment of 60 days.
The Leishmania protozoan was first
described in 1903 by Leishman and Donovan,
working separately.2 Since then, this organism
has been found to be a complex grouping of
species, at least 20 of which cause infections
in humans. Some species cause visceral leishmaniasis, some cause cutaneous disease, and
some cause both. Visceral leishmaniasis is
a systemic infection characterized by fever,
weight loss, and hepatosplenomegaly, and it
is usually fatal without treatment. This article
Downloaded from the American Family Physician Web site at www.aafp.org/afp. Copyright 2004 American Academy of Family Physicians. For the private, noncommercial
use of one individual user of the Web site. All other rights reserved. Contact copyrights@aafp.org for copyright questions and/or permission requests.
Cutaneous leishmaniasis begins as an erythematous papule
at the site of a sandfly bite on exposed parts of the body.
focuses on cutaneous leishmaniasis, the more
common form of the disease.
Life Cycle and Vector
The promastigote form of the parasite is a
motile form with an anterior flagellum that
develops in the sandfly, the insect vector. The
promastigote form develops into a metacyclic
infectious form over approximately 10 days.
The parasite enters the human host with the
bite of the sandfly and is pulled into macrophages by ingestion. Leishmania are able to
survive the acidic environment of the lysosome and become amastigote forms. These
forms are obligate, intracellular, nonmotile,
and about 2.5 to 7 microns in diameter. It
is this amastigote form that causes disease in
humans and affects cellular immunity. Eventually, a sandfly will pick up this form while
feeding, and it will develop into the promastigote form again in the insect.
The sandfly vector is a 2-mm long, hairy fly
of the genus Phlebotomus in the Old World
and Lutzomyia in the New World. These
flies are able to pass through the usual netting used for mosquitoes. Sandflies are found
The Authors
WILLIAM H. MARKLE, M.D., is assistant professor of family medicine at the University
of Pittsburgh School of Medicine and family practice residency program director at
the University of Pittsburgh Medical Center (UPMC), McKeesport, Pa. He is a graduate of the Penn State Milton S. Hershey Medical Center, Hershey, Pa., and completed
a residency at Virginia Commonwealth University, Blackstone Family Practice Center,
Blackstone, Va. He received a diploma in tropical medicine and hygiene at Mahidol
University, Bangkok, Thailand.
KHALDOUN MAKHOUL, M.D., is currently in private practice in Easton, Pa. He is a
graduate of the University of Aleppo Faculty of Medicine, Aleppo, Syria, and completed a family practice residency at UPMC McKeesport.
Address correspondence to William H. Markle, M.D., University of Pittsburgh Medical
Center, McKeesport Family Practice Residency, 3518 Fifth Ave., Pittsburgh, PA 15261
(e-mail: marklew@upmc.edu). Reprints are not available from the authors.
1456-AMERICAN FAMILY PHYSICIAN
www.aafp.org/afp
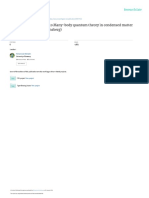
FIGURE 1. Cutaneous leishmaniasis in a young
patient in Honduras.
around human habitations and breed in specific organic wastes such as feces, manure,
rodent burrows, and leaf litter.7
Cutaneous Leishmaniasis
Cutaneous leishmaniasis occurs in the New
World and the Old World. Old World disease
primarily is caused by Leishmania tropica
in urban areas and Leishmania major in dry
desert areas. The two subgenera of interest
in Latin America are Leishmania leishmania
(e.g., Leishmania mexicana, Leishmania amazonensis, Leishmania chagasi) and Leishmania
viannia (e.g., Leishmania panamensis, Leishmania braziliensis, Leishmania guyanensis).
The incubation period is two to eight weeks,
although longer periods have been noted. The
disease begins as an erythematous papule at
the site of the sandfly bite on exposed parts
of the body. The papule increases in size and
becomes a nodule. It eventually ulcerates
and crusts over. The border is usually raised
and distinct. There may be multiple lesions,
especially when the patient has encountered
a nest of sandflies. The ulcer is typically large
but painless unless there is secondary bacterial
or fungal infection.
Old World leishmaniasis and L. mexicana
lesions tend to heal spontaneously in months,
but L. braziliensis may take years to heal.
After healing, a depressed scar remains that
is usually round but can be irregular. Figure
VOLUME 69, NUMBER 6 / MARCH 15, 2004
Cutaneous Leishmaniasis
1 shows a typical leishmaniasis lesion before
treatment. Satellite lesions with a nodular
lymphangitis resembling sporotrichosis have
been described.
Cutaneous leishmaniasis can become disseminated (diffuse cutaneous leishmaniasis),
especially in immunosuppressed persons.
This illness can go on for years and does
not heal spontaneously. Patients with human
immunodeficiency virus (HIV) infection are
particularly susceptible. Other unusual types
of cutaneous disease include leishmaniasis
recidivans, in which small nodules develop
around a healed scar, and postkala-azar dermal leishmaniasis, in which widespread cutaneous lesions arise after a visceral infection.
These conditions occur primarily in the Old
World.
The mucosal form usually occurs after an
initial cutaneous infection. Ninety percent
of cases of mucosal leishmaniasis are found
in Brazil, Bolivia, and Peru, and they usually
begin in the nose or palate.8 Lesions progress
to destruction of mucosa and even cartilage.
They result in scarring and disfigurement and
can cause pulmonary aspiration and death.
Table 1 lists the differential diagnosis for cutaneous and mucosal leishmaniasis.9
Diagnosis
When physicians assess a patient with suspected leishmaniasis in the United States,
the travel and military histories are most
important. Patients who served in the military in the Middle East can return with this
infection. Risk factors for HIV should be
solicited, including sexual encounters, intravenous drug use, and blood transfusions
obtained abroad.
The basic diagnostic tests are summarized
in Table 2. Cutaneous scraping is the simplest
and most common test, but it is only 70 to
75 percent sensitive.2 Proper cleaning and
drying of the site are essential before scraping. Scrapings are made from the center and
the margin of the ulcer. L. mexicana yields
more organisms than L. braziliensis, and older
MARCH 15, 2004 / VOLUME 69, NUMBER 6
When physicians assess a patient with suspected leishmaniasis in the United States, the travel and military service histories are most important.
lesions (more than four months) have fewer
parasites than newer ones.
Multiple slides should be made. They are
fixed with methanol, stained with Giemsa, and
examined under oil immersion. Amastigotes
are seen in monocytes or extracellularly. Slides
must be examined completely before they
can be called negative. It is important to see
the nucleus and the rod-shaped kinetoplast,
a mitochondrial structure containing extranuclear DNA, to diagnose leishmaniasis. The
kinetoplast differentiates Leishmania from
other small organisms such as Histoplasma.
Treatment
Treatment with antimonials will heal lesions
faster and prevent relapse, local dissemination,
TABLE 1
Differential Diagnosis of Leishmaniasis
Cutaneous leishmaniasis
Bacterial skin infections
Blastomycosis
Cutaneous anthrax
Eczema
Fungal skin infections
Leprosy
Mycobacterium marinum
Myiasis
Sarcoidosis
Skin cancer
Sporotrichosis
Syphilis
Tuberculosis
Yaws
Verrucous lesions
Mucosal leishmaniasis
Behets syndrome
Discoid lupus erythematosus
Histoplasmosis
Lethal midline granuloma
Neoplasms
Paracoccidioidomycosis
Rhinoscleroma
Sarcoidosis
Syphilis
Tuberculosis
Wegeners granulomatosis
Yaws
Information from reference 9.
www.aafp.org/afp
AMERICAN FAMILY PHYSICIAN-1457
TABLE 2
Diagnostic Tests for Cutaneous Leishmaniasis
Test
Procedure
Cutaneous scraping
Administer local anesthesia. Clean ulcer of crust, and dry with gauze. Scrape
margin and central area of ulcer, and prepare five slides.
Punch biopsy
Punch 2 to 3 mm along active border; make tissue-impression smears from a biopsy
sample by rolling the cut portion on a slide after blotting excess blood.
Needle aspirate
This test is useful with nodular and papular lesions, using 0.1 mL of preservativefree saline injected into the border through intact skin. Fluid is aspirated while
the needle is moved back and forth under the skin; the fluid is useful for culture
(blood agar Nicolle-Novy-MacNeal media).
Immunologic tests
Antibodies are detected most consistently in mucosal disease. Polymerase chain
reaction test is highly sensitive but not standardized. Test is species specific.
Skin test
Test is no longer available in the United States.
mucosal disease (usually), and transmission.
Not all lesions require treatment. Old World
disease tends to be self-healing, and systemic
treatment seldom is used. New World lesions
more often require systemic treatment. Table
3 gives reasons to consider early treatment.
Pentavalent antimony remains the treatment of choice. It is thought to work by inhibition of adenosine triphosphate synthesis. The
antimonial agent used in the United States
is sodium stibogluconate (Pentostam). This
drug is available from the Centers for Disease
Control and Prevention (CDC), which also
can assist with the investigational new drug
paperwork.
Pentavalent antimonials have a high incidence of side effects, but the latter are reversible. In a military study,10 96 subjects with
leishmaniasis (83 cases were cutaneous) were
treated for 20 to 28 days and followed for one
year. Side effects included aching, arthralgia,
fatigue, gastrointestinal upset, elevation of
amylase, lipase, and liver enzyme levels, leukopenia, anemia, and electrocardiographic
abnormalities.
In general, more adverse reactions are
expected in patients with liver and renal
impairment, cardiac arrhythmias, and pro1458-AMERICAN FAMILY PHYSICIAN
www.aafp.org/afp
longed QT intervals; in small children; in
pregnant and breastfeeding women; and in
obese, elderly, and immunocompromised
patients. There are no known drug interactions, but hepatotoxic drugs, including alcohol, and drugs that prolong the QT interval should be avoided.10 Because pentavalent
antimony is difficult to use, consultation with
an infectious disease specialist and the CDC is
recommended before using it.
After 20 days of treatment with pentavalent
antimonials, there is usually evidence of healing, but lesions may not be re-epithelialized
TABLE 3
Reasons to Treat Cutaneous Leishmaniasis
Cosmetically unacceptable lesions
Chronic lesions
Large lesions
Lesions in immunosuppressed patients
Lesions over joints
Mucosal disease
Multiple lesions
Nodular lymphangitis
Worsening lesions
VOLUME 69, NUMBER 6 / MARCH 15, 2004
Cutaneous Leishmaniasis
completely. They generally go on to heal.
Healing is determined by a healed appearance
at two months, no relapse at 12 months, and
no subsequent mucosal disease. Mucosal disease requires a longer treatment course and is
more difficult to cure.
Trauma can reactivate the disease, so elective surgery is contraindicated for one year,
and pregnancy is inadvisable for one to two
months after treatment. The aching, which
can be debilitating, usually resolves one week
after treatment is finished but can take up to
two months to go away.
Table 4 includes the recommended dosage
of pentavalent antimony and other treatment
options.11-19 A recent randomized, doubleblind, placebo-controlled study of more than
200 patients with cutaneous L. major demonstrated that oral fluconazole (Diflucan) in
a dosage of 200 mg daily for six weeks was
a well-tolerated and effective treatment
option.18 [SOR B, single randomized controlled trial (RCT)].
The CDC is ready to assist with the diagnosis and treatment of leishmaniasis and can be
contacted at 404-488-4050 or 404-639-3670.
Prevention
Vaccine development is under way. The
combination of killed promastigotes plus bacille Calmette-Gurin vaccine is being tested in
Iran, Sudan, and Ecuador.20 Avoiding sandflies is important but difficult, because they
have adapted to urban environments. The use
of insecticides in endemic areas is important
for travelers. House and space spraying have
reduced sandfly populations, and fine-weave
pyrethroid-impregnated bednets have been
used in Burkina Faso, Sudan, and Columbia.
Destruction of rodent reservoirs by pumping insecticides into rodent burrows has had
limited success.7
A recent randomized study in Venezuela evaluated the effectiveness of pyrethroidimpregnated curtains in an urban area with
an incidence of cutaneous leishmaniasis of
4 percent. In 569 homes, 2,913 inhabitants
MARCH 15, 2004 / VOLUME 69, NUMBER 6
Old World leishmaniasis tends to be self-healing, and systemic treatment seldom is used, while New World
lesions more often require systemic treatment.
were included in this study. Use of the curtains
reduced the sandfly population and, 12 months
after the installation of these curtains, the incidence of cutaneous leishmaniasis dropped to
zero.21 [SOR B, single RCT]
Figure 1 provided by Eric J. Sheltra.
The authors indicate that they do not have any
TABLE 4
Treatment of Cutaneous Leishmaniasis
Pentavalent antimony
Meglumine antimoniate (Glucantime) and sodium stibogluconate (Pentostam);
cure rate 94 percent; eliminated by kidneys
Dosage: 20 mg per kg per day for 20 days
Stibogluconate supplied as 100 mg Sb per mL light-sensitive solution
Calculated dose (12 to 20 mL for adults) is diluted in 50 mL of 5 percent
dextrose in distilled water, infused intravenously over 10 to 15 minutes
Amphotericin B (Fungizone)
Reserved for antimony failures
Dosage: 0.5 to 1.0 mg per kg every other day for up to eight weeks;
total dosage is 1.5 to 2 g for the treatment period
Pentamidine isethionate (Pentam 300)
Dosage: 2 mg per kg intramuscularly every other day for seven days
Toxic effects: damage to pancreas, kidney, or bone marrow may be irreversible
May induce diabetes mellitus
Others
Topical paromomycin is effective with L. major and L. mexicana. It can be
combined with antimonials to reduce the number of injections.
Oral antifungals have demonstrated conflicting results, although some good
results have been achieved with L. mexicana19 and L. major.18
Allopurinol (Zyloprim) incorporates into parasite RNA with lethal effect.
Studies are conflicting, and it is not recommended, although there is
synergistic activity with antimonials.11-14
Heat15-16 and cryotherapy17 show good results in uncontrolled trials.
Excision is not recommended because of the high risk of local relapse and
disfiguration.
Information from references 11 through 19.
www.aafp.org/afp
AMERICAN FAMILY PHYSICIAN-1459
Cutaneous Leishmaniasis
conflicts of interest. Sources of funding: none
reported.
REFERENCES
1. Dedet JP, Pratlong F. Leishmaniasis. In: Manson P,
Cook GC, Zumla A, eds. Mansons Tropical diseases. 21st ed. London: Saunders, 2003:1339-64.
2. Herwaldt BL. Leishmaniasis. Lancet 1999;354:
1191-9.
3. Cope SE, Schultz GW, Richards AL, Savage HM,
Smith GC, Mitchell CJ, et al. Assessment of arthropod vectors of infectious diseases in areas of U.S.
troop deployment in the Persian Gulf. Am J Trop
Med Hyg 1996;54:49-53.
4. Hyams KC, Hanson K, Wignall FS, Escamilla J, Oldfield EC 3d. The impact of infectious diseases on
the health of U.S. troops deployed to the Persian
Gulf during operations Desert Shield and Desert
Storm. Clin Infect Dis 1995;20:1497-504.
5. McNeil DG Jr. A region inflamed: medicine; hundreds of U.S. troops infected by parasite borne by
sand flies, Army says. New York Times December
6, 2003:A,8.
6. Centers for Disease Control and Prevention (CDC).
Cutaneous leishmaniasis in U.S. military personnelSouthwest/Central Asia, 2002-2003. MMWR
Morb Mortal Wkly Rep 2003;52:1009-12.
7. Lane RP. Phlebotomine sandflies. In: Manson P,
Cook GC, Zumla A, eds. Mansons Tropical diseases. 21st ed. London: Saunders, 2003:1733-41.
8. WHO fact sheet. The leishmaniases and leishmania/HIV coinfections. Accessed October 16, 2003,
at: http://www.who.int/inf-fs/en/fact116.html.
9. Magill AJ. Leishmaniasis. In: Hunter GW, Strickland
GT, eds. Hunters Tropical medicine and emerging
infectious diseases. 8th ed. Philadelphia: Saunders,
2000:665-87.
10. Aronson NE, Wortmann GW, Johnson SC, Jackson
JE, Gasser RA Jr, Magill AJ, et al. Safety and efficacy
of intravenous sodium stibogluconate in the treatment of leishmaniasis: recent U.S. military experience. Clin Infect Dis 1998;27:1457-64.
11. Martinez S, Marr JJ. Allopurinol in the treatment of
American cutaneous leishmaniasis. N Engl J Med
1460-AMERICAN FAMILY PHYSICIAN
www.aafp.org/afp
1992;326:741-4.
12. Velez I, Agudelo S, Hendrickx E, Puerta J, Grogl
M, Modabber F, et al. Inefficacy of allopurinol as
monotherapy for Colombian cutaneous leishmaniasis. A randomized, controlled trial. Ann Intern
Med 1997;126:232-6.
13. Esfandiarpour I, Alavi A. Evaluating the efficacy of
allopurinol and meglumine antimoniate (Glucantime) in the treatment of cutaneous leishmaniasis.
Int J Dermatol 2002;41:521-4.
14. Llanos-Cuentas A, Echevarria J, Cruz M, La Rosa
A, Campos P, Campos M, et al. Efficacy of sodium
stibogluconate alone and in combination with
allopurinol for treatment of mucocutaneous leishmaniasis. Clin Infect Dis 1997;25:677-84.
15. Navin TR, Arana BA, Arana FE, de Merida AM,
Castillo AL, Pozuelos JL. Placebo-controlled clinical
trial of meglumine antimonate (glucantime) vs.
localized controlled heat in the treatment of cutaneous leishmaniasis in Guatemala. Am J Trop Med
Hyg 1990;42:43-50.
16. Velasco-Castrejon O, Walton BC, Rivas-Sanchez B,
Garcia MF, Lazaro GJ, et al. Treatment of cutaneous leishmaniasis with localized current field (radio
frequency) in Tabasco, Mexico. Am J Trop Med Hyg
1997;57:309-12.
17. Gurei MS, Tatli N, Ozbilge H, Erel O, Seyrek A, Kocyigit A, et al. Efficacy of cryotherapy and intralesional
pentostam in treatment of cutaneous leishmaniasis.
J Egypt Soc Parasitol 2000;30:169-76.
18. Alrajhi AA, Ibrahim EA, De Vol EB, Khairat M, Faris
RM, Maguire JH. Fluconazole for the treatment
of cutaneous leishmaniasis caused by Leishmania
major. N Engl J Med 2002;346:891-5.
19. Davies CR, Kaye P, Croft SL, Sundar S. Leishmaniasis: new approaches to disease control. BMJ 2003;
326:377-82.
20. Sharifi I, FeKri AR, Aflatonian MR, Khamesipour A,
Nadim A, Mousavi MR, et al. Randomised vaccine
trial of single dose of killed Leishmania major plus
BCG against anthroponotic cutaneous leishmaniasis in Bam, Iran. Lancet 1998;351:1540-3.
21. Kroeger A, Avila EV, Morison L. Insecticide impregnated curtains to control domestic transmission
VOLUME 69, NUMBER 6 / MARCH 15, 2004
Вам также может понравиться
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (890)
- Guiffre V MaxwellДокумент40 страницGuiffre V MaxwellTechno Fog91% (32)
- Fuather, That Smid Govern-: Such Time As It May Deem Proper: TeДокумент18 страницFuather, That Smid Govern-: Such Time As It May Deem Proper: Tencwazzy100% (1)
- Gamma World Character SheetДокумент1 страницаGamma World Character SheetDr8chОценок пока нет
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Checklist For Mold RemediationДокумент2 страницыChecklist For Mold Remediation631052Оценок пока нет
- Design Your Loyalty Program in 2 WeeksДокумент53 страницыDesign Your Loyalty Program in 2 WeeksLorena TacuryОценок пока нет
- Talon Star Trek Mod v0.2Документ4 страницыTalon Star Trek Mod v0.2EdmundBlackadderIVОценок пока нет
- Solution of Introduction To Many-Body Quantum Theory in Condensed Matter Physics (H.Bruus & K. Flensberg)Документ54 страницыSolution of Introduction To Many-Body Quantum Theory in Condensed Matter Physics (H.Bruus & K. Flensberg)Calamanciuc Mihai MadalinОценок пока нет
- Siegfried Kracauer - Photography (1927)Документ17 страницSiegfried Kracauer - Photography (1927)Paul NadeauОценок пока нет
- Case Presentation - Bipolar Affective Disorder 2Документ73 страницыCase Presentation - Bipolar Affective Disorder 2Hemant's galaxy All is hereОценок пока нет
- VISCOSITY CLASSIFICATION GUIDE FOR INDUSTRIAL LUBRICANTSДокумент8 страницVISCOSITY CLASSIFICATION GUIDE FOR INDUSTRIAL LUBRICANTSFrancisco TipanОценок пока нет
- Dietary Fiber Intake and Type 2 Diabetes Mellitus An Umbrella ReviewДокумент10 страницDietary Fiber Intake and Type 2 Diabetes Mellitus An Umbrella ReviewRVDОценок пока нет
- CIRCULATIONДокумент2 страницыCIRCULATIONRVDОценок пока нет
- ABC BurdenДокумент1 страницаABC BurdenRVDОценок пока нет
- ABC BurdenДокумент1 страницаABC BurdenRVDОценок пока нет
- 1) PCI Vs CABG Doubt Same Hospitalization? 2) To Study Population Trend Mortality PredictorsДокумент1 страница1) PCI Vs CABG Doubt Same Hospitalization? 2) To Study Population Trend Mortality PredictorsRVDОценок пока нет
- Materials For Step1Документ1 страницаMaterials For Step1RVDОценок пока нет
- Hi Hello Renal System If Glomurulus DZ Important ThanksДокумент1 страницаHi Hello Renal System If Glomurulus DZ Important ThanksRVDОценок пока нет
- USMLEДокумент1 страницаUSMLERVDОценок пока нет
- Genetics Review 2Документ12 страницGenetics Review 2api-19641337Оценок пока нет
- HiiiДокумент1 страницаHiiiRVDОценок пока нет
- Anatomy 1Документ20 страницAnatomy 1RVDОценок пока нет
- PharmacologyДокумент9 страницPharmacologyRVDОценок пока нет
- Case Reports JournalДокумент1 страницаCase Reports JournalRVDОценок пока нет
- Study ScheduleДокумент1 страницаStudy ScheduleRVDОценок пока нет
- Study ScheduleДокумент1 страницаStudy ScheduleRVDОценок пока нет
- Lacatse DefДокумент2 страницыLacatse DefRVDОценок пока нет
- Animal Reservoirs For Visceral LeishmaniasisДокумент10 страницAnimal Reservoirs For Visceral LeishmaniasisRVDОценок пока нет
- Keywords Aortocaval Fistula, Abdominal Aortic Aneurysm, Gore Excluder Stent Graft, Endova Scular Therapy, Physical ExaminationДокумент1 страницаKeywords Aortocaval Fistula, Abdominal Aortic Aneurysm, Gore Excluder Stent Graft, Endova Scular Therapy, Physical ExaminationRVDОценок пока нет
- New DrugДокумент1 страницаNew DrugRVDОценок пока нет
- Activity2 Mba 302Документ2 страницыActivity2 Mba 302Juan PasyalanОценок пока нет
- © 2020 Lippincott Advisor Nursing Care Plans For Medical Diagnoses - Coronavirus Disease 2019 (COVID 19) PDFДокумент7 страниц© 2020 Lippincott Advisor Nursing Care Plans For Medical Diagnoses - Coronavirus Disease 2019 (COVID 19) PDFVette Angelikka Dela CruzОценок пока нет
- Case Study - Help DocumentДокумент2 страницыCase Study - Help DocumentRahОценок пока нет
- FRABA - Absolute - Encoder / PLC - 1 (CPU 314C-2 PN/DP) / Program BlocksДокумент3 страницыFRABA - Absolute - Encoder / PLC - 1 (CPU 314C-2 PN/DP) / Program BlocksAhmed YacoubОценок пока нет
- AIIMS Mental Health Nursing Exam ReviewДокумент28 страницAIIMS Mental Health Nursing Exam ReviewImraan KhanОценок пока нет
- Data Sheet FC SIДокумент2 страницыData Sheet FC SIAndrea AtzeniОценок пока нет
- Module-1 STSДокумент35 страницModule-1 STSMARYLIZA SAEZОценок пока нет
- 6a. ICMR STSДокумент15 страниц6a. ICMR STSVishnu Praba AОценок пока нет
- Hotels Cost ModelДокумент6 страницHotels Cost ModelThilini SumithrarachchiОценок пока нет
- MP & MC Module-4Документ72 страницыMP & MC Module-4jeezОценок пока нет
- Stress Out?: A Study of Trends in Workplace Stress Across The GlobeДокумент14 страницStress Out?: A Study of Trends in Workplace Stress Across The GlobeVishesh Vij100% (1)
- Manuais - 727312 - manuais-Raios-X AXR - 77000001249Документ72 страницыManuais - 727312 - manuais-Raios-X AXR - 77000001249Hosam Ahmed HashimОценок пока нет
- BILL of Entry (O&A) PDFДокумент3 страницыBILL of Entry (O&A) PDFHiJackОценок пока нет
- Heads of Departments - 13102021Документ2 страницыHeads of Departments - 13102021Indian LawyerОценок пока нет
- C++ Programmierung (Benjamin Buch, Wikibooks - Org)Документ257 страницC++ Programmierung (Benjamin Buch, Wikibooks - Org)stefano rossiОценок пока нет
- KCL Thesis PrintingДокумент4 страницыKCL Thesis PrintingMelinda Watson100% (2)
- Questions - TrasportationДокумент13 страницQuestions - TrasportationAbhijeet GholapОценок пока нет
- Culinary Nutrition BasicsДокумент28 страницCulinary Nutrition BasicsLIDYAОценок пока нет
- 7 Equity Futures and Delta OneДокумент65 страниц7 Equity Futures and Delta OneBarry HeОценок пока нет
- CM Template For Flora and FaunaДокумент3 страницыCM Template For Flora and FaunaJonathan Renier Verzosa0% (1)