Академический Документы
Профессиональный Документы
Культура Документы
Fractures of Angle of Mandible e A Retrospective Study
Загружено:
dydy_7193Оригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Fractures of Angle of Mandible e A Retrospective Study
Загружено:
dydy_7193Авторское право:
Доступные форматы
Journal of Oral Biology and Craniofacial Research 2012 SeptembereDecember
Volume 2, Number 3; pp. 154e158
Original Article
Fractures of angle of mandible e A retrospective study
Sourav Singha,*, Ramesh R. Fryb, Ajit Joshic, Geeta Sharmac, Smita Singhd
ABSTRACT
Aims: This retrospective study was done to evaluate the efcacy of single miniplate osteosynthesis at superior border
of angle of mandible.
Material and methods: In this study 50 patients were treated by single miniplate osteosynthesis according to
Champys principle. Bite force generated was used as a parameter for judging the efcacy of internal xation. In this
article we present our experience over the years in the management of the fractures of angle of mandible based on
this model.
Results: Most patients were of 21e30 yrs of age with unilateral angle fracture of mandible except one patient who
had isolated bilateral angle fracture. The patients were treated successfully according to Champys principle of
osteosynthesis. There was a progressive improvement in the bite force generated after osteosynthesis.
Conclusions: The angle of the mandible is an anatomically weak and an area susceptible to fracture. The presence
of an impacted or partially erupted third molar tooth further weakens it. Angle of mandible is the most common site for
fracture however, bilateral angle fracture is very rare and uncommon.
Osteosynthesis according to Champys model led to an early functional improvement as demonstrated by the bite
force generated.
Copyright 2012, Craniofacial Research Foundation. All rights reserved.
Keywords: Fracture mandible, Champys principle, Osteosynthesis, Bite force
INTRODUCTION
The mandibular angle is fractured in approximately 25%e
33% of all mandibular fractures1 as is the transition area
between dentate and edentate regions of the mandible. In
fact, according to Moore,2 a change in the direction of the
bone tends to weaken the angle region of the mandible and
increases its susceptibility to fracture. This is observed in
the area where the horizontal body and vertical ascending
ramus meet. Presence of incompletely erupted third molars
is associated with an increased risk of angle fracture.
However, multiple factors inuence fracture patterns in the
mandible, such as presence of soft tissue bulk, direction and
severity of the forces, impact, and biomechanical intrinsic
characteristics of the mandible (e.g., bone density and mass).3
Road trafc accidents4 and assaults5 are the primary
cause of mandibular fractures. Signs and symptoms include
pain and edema, change in occlusion, lower lip paresthesia,
hematoma, ecchymosis, loose teeth, and crepitation on
palpation.6
According to Paza et al,7 displaced angle fractures can
rarely be adequately reduced by maxillomandibular xation
alone. Therefore, an open reduction and internal xation of
these fractures should be performed. However, several
studies have documented high complication rates after rigid
internal xation of the mandibular angle.8 The purpose of
Professor and Head, bProfessor, cSenior Lecturer, Department of Oral and Maxillofacial Surgery, dProfessor and Head, Department of Conservative and Endodontics, Darshan Dental College and Hospital, Ranakpur Road, Udaipur 313001, Rajasthan, India.
*
Corresponding author. Tel.: 91 2942425727, email: udaipurdentalclinic@rediffmail.com
Received: 6.6.2012; Accepted: 5.10.2012
Copyright 2012, Craniofacial Research Foundation. All rights reserved.
http://dx.doi.org/10.1016/j.jobcr.2012.10.001
Fractures of angle of mandible
Original Article
155
this study was to review cases of fractures of the mandibular angle and their associated complications.
PATIENTS AND METHODS
Information was obtained retrospectively from clinical case
sheets, surgical records, and radiographs of 50 patients
treated for fractures of the mandibular angle from 2007
until 2011, in the Department of Oral and Maxillofacial
Surgery at Darshan Dental College And Hospital, Udaipur.
The data recorded included patient age, gender, etiology,
method of surgical treatment, medication, and complications. The radiographs were evaluated with respect to the
condition of the reduction, dislocation, failure of the xation, and fracture union. Success was considered if the fracture xation provided stability, i.e., there was no inter
fragmentary mobility, infection, or nonunion of the bone
fragments. Follow-up of patients was done up to 6-month
post-operatively. Bite force readings were recorded in kilograms, using a locally manufactured bite force recorder.
Bite force recording was done pre-operatively before xing
Erichs arch bar and post-operatively at each follow-up
(7th, 15th, 21st and 90th day). The mean bite force generated in normal young healthy individuals was used for
comparison.
Intermaxillary xation was maintained for 7e14 days
for all patients. Antimicrobial and anti-inammatory drugs
were administered for a week after the surgery. An antiseptic mouthwash, 2.5% povidone iodine, was recommended. Patient was advised functional exercises after
removal of intermaxillary xation for 3 months.
RESULTS
The higher prevalence of trauma was observed in patients
of younger age group. 36% of cases belonged to 11e20
years age and 48% cases between 21 and 30 years. The
majority of fractures in this study were sustained in motor
vehicle accidents (74%), followed by altercation/assault
(14%). Patient demographic data is shown in Table 1.
Fig. 1 Pre-operative intra-oral photograph fracture bilateral
angle of mandible.
Higher prevalence of fracture was on left side, 29 (58%);
right side, 20 (40%); and only 1 bilateral angle fracture
(2%) (Figs. 1 and 2). No relevant medical history affecting
bone healing, notably diabetes, prolonged steroid therapy,
compromised immunity, and associated bony pathology
were noted in any of the patients.
Of the total 50 patients, 46 underwent surgery under
general anesthesia and 4 under local anesthesia. All patients
were treated via intraoral approach, open reduction and
xation (Figs. 3e6), using a 4-hole 2.0-mm stainless steel
miniplate xed on the external oblique ridge (Figs. 7
and 8) as per Champy et al9 Isolated fracture of mandibular
angle accounted for 20 patients, and when associated fractures were detected, the mandibular parasymphyseal fracture was the most prevalent (10 contralateral, 3 ipsilateral)
followed by body fracture (8 contralateral, 2 ipsilateral).
The mandibular third molar was present in 45 cases
(90%). It was extracted in 42 cases where it was involved
in the fracture line. The remaining 3 cases, third molar
was not involved in the fracture line, hence not extracted.
Table 1 Demographic data (N 50).
Category
Gender
Etiology
Males
Females
Road trafc accident
Interpersonal violence
Fall
Accidents at work
N (%)
40
10
37
7
4
2
(80%)
(20%)
(74%)
(14%)
(8%)
(4%)
Fig. 2 Pre-operative OPG fracture bilateral angle of mandible.
156
Journal of Oral Biology and Craniofacial Research 2012 SeptembereDecember; Vol. 2, No. 3
Singh et al.
Fig. 3 Exposure of the fracture site (right).
Fig. 5 Bone plating at the superior border (right).
The bite force measured and calculated was nally found
to be statically highly signicant (Table 2) in both
the regions (incisor and premolar-molar) with the
P value <0.001 respectively.
Fractures of the mandibular angle account for the highest
percentage of mandibular fractures in most of the studies.
Several factors are associated with an increased risk of
angle fracture incidence: site, direction and severity of
force, musculature of the face, architecture of the mandible,
soft tissue bulk, biomechanical intrinsic characteristics of
the mandible, and presence or absence of third molars.
Studies in animals and humans have conrmed that the
presence of third molars is associated with an increased
risk of mandibular angle fractures.1,4,10
Many authors have concluded that the severity of the
force necessary to produce an angle fracture is substantially
less when a third molar is present compared with when
absent.1 According to a theory, the third molars would
weaken the angle by reducing the total available bone
mass in the region. Therefore, the mandibular angle would
become more susceptible to fracture. In other words, the
more deeply impacted are the third molars, the greater
would be the risk for angle fractures. However, this hypothesis was not conrmed by several clinical studies. Instead,
recent studies suggest that the risk of angle fractures is
greater for partially erupted third molars and is decreased
for deeper impactions.1,11
According to Duan and Zhang,10 the impacted mandibular third molars increase the risk of mandibular angle fractures and decrease the risk of mandibular condylar fractures
by moderate trauma force. The partially erupted third
molars disrupt the cortical integrity of the external oblique
ridge which weakens the mandibular angle, thus decreasing
the resistance to angle fractures. Mandibular strength would
be derived from the maintenance of cortical bone integrity.11 Supercially impacted third molars are associated
with an increased risk, whereas deeply impacted molars
are not. In our study, 30 patients had impacted third molars
Fig. 4 Exposure of the fracture site (left).
Fig. 6 Bone plating at the superior border (left).
DISCUSSION
Fractures of angle of mandible
Original Article
157
Table 2 Bite force (in kg).
Pre-operative
90th day post-operative
Control
17.369
0.618
148.90
<0.001a
19.27
0.511
16.77
<0.001a
38.722
0.757
294.19
<0.001a
41.47
0.57
20.51
<0.001a
Incisor region
Mean
1.3162
SD
0.447
T value
P value
Premolar-molar region
Mean
3.2334
SD
0.394
T value
P value
a
Difference is highly signicant.
Fig. 7 Post-operative occlusion.
and 6 patients had them in erupting stage. Thus partially
erupting third molars disrupt the cortical integrity of the
external oblique ridge and increasing the risk of mandibular
angle fracture. Tams et al12 observed negative bending
movements at bite points closer to the fracture angle
thereby leading to tension at the occlusal level. In a retrospective study of 385 patients, Choi et al13 concluded that
the incidence of mandibular angle fracture is greater on
sides with a third molar, whereas the condylar fracture
rate signicantly increased in mandibles lacking a third
molar or without a fully erupted third molar. Thangavelu
et al14 also suggested that removal of mandibular third
molars predisposes to increased incidence of condylar
fractures.
The stability of single miniplate xation of angle fractures was challenged by several biomechanical studies
based on 3D models. Kroon et al15 and Choi et al16
observed bony gaps along the inferior fracture border,
Fig. 8 Post-operative OPG.
and this fracture movement was thought to contribute to
subsequent complications, including infection. A second
plate was suggested to reduce anterior posterior separation
of the fracture line as well as lateral displacement, which is
frequently observed on post-operative radiographs.17 The
resulting clinical studies were inconsistent because an additional miniplate does not cause any change in complications
rates. More recent 3D models have shown that the rotational or torsional forces at the angle are relatively weak.12
All cases in our study were treated via intraoral approach
with a miniplate placed on the external oblique ridge.9 We
preferred intraoral approach to avoid facial scars and facial
nerve injury. Plates were contoured and xed, thus allowing
a stable healing of the fracture. Many surgeons still feel that
miniplate xation does not provide adequate stability and
required intermaxillary xation for additional security. In
a retrospective study of 287 patients with 499 mandible
fractures, Valentino and Marentette18 compared 130
patients who underwent intraoral monocortical plating of
matched fractures and found that the addition of intermaxillary xation did not signicantly alter complication rates.
Seemann et al19 reported a low complication rate with open
reduction and miniplate xation. Prein et al20 noted similar
ndings in a small prospective study of 32 patients,
combining the old AO technique with intermaxillary xation. As miniplates provide semi-rigid xation, intermaxillary xation was done in our study for 7e14 days in all
patients as an additional precaution and to prevent
complications.21
Gerlach and Schwartz22 used bite force measurements
to evaluate the efcacy of Champys tension band principle
in 22 patients. They concluded that up to 31% bite force
was registered at the end of rst week post-operatively
which gradually increased to 58% at the end of 6th
week.22 Our ndings too were consistent with their results
(Table 2).
158
Journal of Oral Biology and Craniofacial Research 2012 SeptembereDecember; Vol. 2, No. 3
CONCLUSIONS
Angle of mandible is the most common site for fracture
however, bilateral angle fracture is very rare and
uncommon. Third molars can be denitively considered
a dominant factor for mandibular angle fractures.
The use of a single miniplate on the superior border of
mandible is simple, reliable, and is the preferred method
of treatment. Osteosynthesis according to Champys model
led to an early functional improvement as demonstrated by
the bite force generated.
CONFLICTS OF INTEREST
All authors have none to declare.
REFERENCES
1. Meisami T, Sojat A, Sndor GK, Lawrence HP, Clokie CM.
Impacted third molars and risk of angle fracture. Int J Oral
Maxillofac Surg. 2002;31:140e144.
2. Moore JR. Principles of Oral Surgery. 2nd ed. Manchester,
UK: Manchester University Press; 1976.
3. Lee JT, Dodson TB. The effect of mandibular third molar
presence and position on the risk of an angle fracture.
J Oral Maxillofac Surg. 2000;58:394e398.
4. Olson RA, Fonseca RJ, Zeitter PL. Fractures of the mandible:
a review of 580 cases. J Oral Maxillofac. 1982;40:23.
5. Greene D, Raven R, Carvalho G, Maas CS. Epidemiology of
facial injury in blunt assault. Determinants of incidence and
outcome in 802 patients. Arch Otolaryngol Head Neck Surg.
1997;123:923e927.
6. Fonseca RJ, Walker RV, Betts NJ. Oral and Maxillofacial
Trauma. 2nd ed., vol. II. Philadelphia: WB Saunders; 1997.
7. Paza AO, Abuabara A, Passeri LA. Analysis of 115 mandibular angle fractures. J Oral Maxillofac Surg. 2008;66:73e76.
8. Peled M, Laufer D, Helman J, Gutman D. Treatment of
mandibular fractures by means of compression osteosynthesis.
J Oral Maxillofac Surg. 1989;47:566e569.
9. Champy M, Wilk A, Schnebelen JM. Treatment of mandibular
fractures by means of osteosynthesis without intermaxillary
immobilisation according to F.X. Michelets technique. Zahn
Mund Kieferheilkd Zentralbl. 1975;63:339e341.
Singh et al.
10. Duan DH, Zhang Y. Does the presence of mandibular third
molars increase the risk of angle fracture and simultaneously
decrease the risk of condylar fracture? Int J Oral Maxillofac
Surg. 2008;37:25e28.
11. Halmos DR, Ellis E, Dodson TB. Mandibular third molars
and angle fractures. J Oral Maxillofac Surg. 2004;62:
1076e1081.
12. Tams J, van Loon JP, Rozema FR, Otten E, Bos RR. A threedimensional study of loads across the fracture for different
fracture sites of the mandible. Br J Oral Maxillofac Surg.
1996;34:400e405.
13. Choi BJ, Park S, Lee DW, Ohe JY, Kwon YD. Effect of lower
third molars on the incidence of mandibular angle and
condylar fractures. J Craniofac Surg. 2011;22(4):1521e1525.
14. Thangavelu A, Yoganandha R, Vaidhyanathan A. Impact of
impacted mandibular third molars in mandibular angle and
condylar fractures. Int J Oral Maxillofac Surg. 2010;39(2):
136e139.
15. Kroon FH, Mathisson M, Cordey JR, Rahn BA. The use of
miniplates in mandibular fractures. An in vitro study.
J Craniomaxillofac Surg. 1991;19:199e204. osteosynthesis.
Otolaryngol Head Neck Surg 1995;112:215.
16. Choi BH, Yoo JH, Kim KN, Kang HS. Stability testing of two
miniplate xation technique for mandibular angle fractures. An
in vitro study. J Craniomaxillofac Surg. 1995;23:123e127.
17. Rudderman RH, Mullen RL. Biomechanics of the facial skeleton. Clin Plast Surg. 1992;19:11.
18. Valentino J, Marentette LJ. Supplemental maxillomandibular
xation with miniplate osteosynthesis. Otolaryngol Head
Neck Surg. 1995;112:215e220.
19. Seemann R, Schicho K, Wutzl A, et al. Complication rates in
the operative treatment of mandibular angle fractures: a 10year retrospective. J Oral Maxillofac Surg. 2010;68(3):
647e650.
20. Prein J, Schilli W, Hammer B. Rigid xation of facial fractures. In: Fonseca RJ, Walker RV, eds. Oral and Maxillofacial
Trauma. Philadelphia: WB Saunders; 1991:1206e1240.
21. Longwe EA, Zola MB, Bonnick A, Rosenberg D. Treatment
of mandibular fractures via transoral 2.0-mm miniplate xation with 2 weeks of maxillomandibular xation: a retrospective study. J Oral Maxillofac Surg. 2010;68(12):2943e2946.
22. Gerlach KL, Schwarz A. Bite forces in patients after treatment
of mandibular angle fractures with miniplate osteosynthesis
according to Champy. Int J Oral Maxillofac Surg. 2002;31:
345e348.
Вам также может понравиться
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5795)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Checklist Manifesto (Chapter-Wise Detail Summary)Документ10 страницThe Checklist Manifesto (Chapter-Wise Detail Summary)Yousuf Zahid67% (3)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- List of Medical Equipment ManufacturerДокумент73 страницыList of Medical Equipment Manufacturerjulee G75% (8)
- Nursing Care PlanДокумент16 страницNursing Care PlanJennifer Post100% (3)
- Engaging Physicians in A Shared Quality Agenda: Innovation Series 2007Документ52 страницыEngaging Physicians in A Shared Quality Agenda: Innovation Series 2007drabhi23Оценок пока нет
- Lab Migrant CasesДокумент33 страницыLab Migrant CasesKalliah Cassandra CruzОценок пока нет
- Surgical InstrumentationДокумент93 страницыSurgical InstrumentationNicole SooОценок пока нет
- Hemiarthroplasty of The HipДокумент10 страницHemiarthroplasty of The HipRusu AdrianОценок пока нет
- How To Read A Postoperative Knee Replacement RadiographДокумент9 страницHow To Read A Postoperative Knee Replacement RadiographNegru TeodorОценок пока нет
- CS Form No. 6 Revised 2020 Application For Leave Fillable 1Документ2 страницыCS Form No. 6 Revised 2020 Application For Leave Fillable 1Leo Artemio PuertosОценок пока нет
- 2016 Article 1849 PDFДокумент8 страниц2016 Article 1849 PDFdydy_7193Оценок пока нет
- PCH 32 s1 033Документ6 страницPCH 32 s1 033dydy_7193Оценок пока нет
- 00 B 4953 B 560 Ccca 872000000Документ9 страниц00 B 4953 B 560 Ccca 872000000dydy_7193Оценок пока нет
- 15 - 1 - 31 (1) - 1Документ6 страниц15 - 1 - 31 (1) - 1dydy_7193Оценок пока нет
- Characteristics of Leprosy Patients in Jakarta: Artikel PenelitianДокумент5 страницCharacteristics of Leprosy Patients in Jakarta: Artikel Penelitiandydy_7193Оценок пока нет
- Characteristics of Leprosy Patients in Jakarta: Artikel PenelitianДокумент5 страницCharacteristics of Leprosy Patients in Jakarta: Artikel Penelitiandydy_7193Оценок пока нет
- Nihms 437493Документ15 страницNihms 437493dydy_7193Оценок пока нет
- Pediatric Mandibular Fractures A ReviewДокумент5 страницPediatric Mandibular Fractures A Reviewdydy_7193Оценок пока нет
- The German Emergency and Disaster Medicine and Management Systemdhistory and PresentДокумент9 страницThe German Emergency and Disaster Medicine and Management Systemdhistory and PresentAhmet DoganОценок пока нет
- Presentation ERAS Digestive TutorialДокумент32 страницыPresentation ERAS Digestive TutorialFebriadi R100% (1)
- Bicontact: Aesculap OrthopaedicsДокумент52 страницыBicontact: Aesculap OrthopaedicsMohamed Swar Eldahab0% (1)
- Diagnosis ListДокумент1 страницаDiagnosis ListSenyorita KHayeОценок пока нет
- Frank 2019Документ15 страницFrank 2019Oliver ArteagaОценок пока нет
- Ledmedics Surgical Lights: Lighting CompetenceДокумент16 страницLedmedics Surgical Lights: Lighting CompetenceMori ArisandyОценок пока нет
- The Use of Hydrogel Coated Latex Versus All SiliconeДокумент4 страницыThe Use of Hydrogel Coated Latex Versus All SiliconeHotОценок пока нет
- Anesthetic Management of Geriatric Patients: Review ArticleДокумент22 страницыAnesthetic Management of Geriatric Patients: Review Articleagita kartika sariОценок пока нет
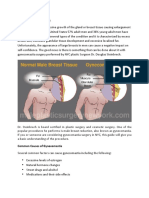
- 7 Types of GynecomastiaДокумент4 страницы7 Types of GynecomastiaSatyajitОценок пока нет
- Geuder Poster Dmek RapidДокумент1 страницаGeuder Poster Dmek Rapidophtho india incОценок пока нет
- Planilha Classificação Qualis 2017-2018.xlsx - MaasДокумент920 страницPlanilha Classificação Qualis 2017-2018.xlsx - MaasGuilherme UchimuraОценок пока нет
- Checklist of Organisation Design Principles by Paul KearnsДокумент4 страницыChecklist of Organisation Design Principles by Paul KearnsaliОценок пока нет
- The Effect of A Platelet-Rich Fibrin Conduit On Neurosensory Recovery Following Inferior Alveolar Nerve Lateralization: A Preliminary Clinical StudyДокумент6 страницThe Effect of A Platelet-Rich Fibrin Conduit On Neurosensory Recovery Following Inferior Alveolar Nerve Lateralization: A Preliminary Clinical Studyr1comfupchОценок пока нет
- Surgery Clerkship ManualДокумент29 страницSurgery Clerkship ManualAndro GalaxОценок пока нет
- Clubfoot A Comprehensive Approach Past Present andДокумент36 страницClubfoot A Comprehensive Approach Past Present andSIVA BHARATHIОценок пока нет
- Osteotomy at Low-Speed Drilling Without Irrigation Versus High-Speed Drilling With Irrigation: An Experimental StudyДокумент6 страницOsteotomy at Low-Speed Drilling Without Irrigation Versus High-Speed Drilling With Irrigation: An Experimental Studyanilsamuel0077418Оценок пока нет
- Anesthetic Management of A Neonate With OEIS ComplДокумент3 страницыAnesthetic Management of A Neonate With OEIS ComplHuzayval AchmadОценок пока нет
- Thesis Recovery After Cataract Surgery: Susanna Porela-TiihonenДокумент40 страницThesis Recovery After Cataract Surgery: Susanna Porela-TiihonenSaskia MediawatiОценок пока нет
- Ethics ProfessionalДокумент47 страницEthics ProfessionalShael ZoletaОценок пока нет
- International Journal of Surgery Case Reports: Unusual Esophageal Foreign Body in Neonates: A Case ReportДокумент4 страницыInternational Journal of Surgery Case Reports: Unusual Esophageal Foreign Body in Neonates: A Case ReportmusdalifahОценок пока нет
- Minor - Surgery UpdateДокумент3 страницыMinor - Surgery UpdateHemkerovner Keresztszegh von Kolowrat-KrakowskyОценок пока нет