Академический Документы
Профессиональный Документы
Культура Документы
HP Sep04 Gangrene PDF
Загружено:
Della FerginaИсходное описание:
Оригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
HP Sep04 Gangrene PDF
Загружено:
Della FerginaАвторское право:
Доступные форматы
Case Report
Fourniers Gangrene
Zsolt T. Stockinger, MD, FACS
ourniers gangrene (Meleneys synergistic gangrene,1,2 perineal necrotizing fasciitis3,4) is a fulminant necrotizing infection of the perineum and
genitalia that constitutes a surgical emergency
and can rapidly progress to sepsis and death. Physicians
unfamiliar with this infection will likely misdiagnose it,
and those who have seen it will never forget it. Although
it has been recently dramatized in the lay press as a disease caused by flesh-eating bacteria,5 Fourniers gangrene has been known since biblical times.3 All physicians who work in the acute care setting should be aware
of this virulent infection, which is frequently misdiagnosed as cellulitis with potentially devastating results.
This article presents the case of a man with Fourniers
gangrene that was initially diagnosed as cellulitis.
CASE PRESENTATION
Initial Presentation
A 51-year-old man presented to the emergency department with a 2-day history of scrotal swelling. He
denied fever, chills, malaise, and other symptoms except for mild scrotal and left buttock pain. His medical
history was negative for drug abuse, steroid use, diabetes, and other medical conditions except for hypertension, but heavy alcohol use was suspected. Edema of
the scrotum and cellulitis of the perineum were noted
during physical examination. The erythema extended
onto the left buttock, where an extremely indurated
area with skin sloughing was noted medially. No perianal or perirectal abscess was found. The results of urinalysis were negative, and the leukocyte count was within normal limits. The urologist on call admitted the
patient to the hospital with a diagnosis of scrotal cellulitis. Treatment with levofloxacin was then initiated.
Diagnosis and Subsequent Management
By the following day, the patients physical condition had deteriorated. He exhibited signs of sepsis,
with fever, tachycardia, and leukocytosis with left shift.
The severity of the scrotal edema and the skin sloughing on the left buttock had worsened, and the area of
induration had increased (Figure 1). Consultation was
requested with the general surgeon on call, who noted
a patch of green-black, necrotic skin 1- to 2-cm in size
www.turner-white.com
on the patients medial left buttock, pneumoscrotum
(crepitation of the scrotal skin), and a foul odor. The
surgeon correctly diagnosed the infection as Fourniers gangrene, and the patient underwent immediate
surgery.
Rigid sigmoidoscopy did not reveal an anorectal
source of infection. The frankly necrotic skin was excised, and necrotic, green-grey, gelatinous, subcutaneous fat was revealed (Figure 2). Malodorous dishwatery fluid drained from along the gluteal fascial planes.
Wide excision and dbridement of all devitalized tissue
from the medial buttock into the base of the scrotum
was performed (Figure 3). The subcutaneous necrosis
was much more extensive than the cutaneous necrosis.
After having undergone this procedure, the patient
was treated with triple antibiotic therapy (ampicillin,
gentamycin and clindamycin) to cover gram-positive,
gram-negative, and anaerobic bacteria. By the next day,
the leukocytosis, edema, and cellulitis had begun to
resolve. Examination under anesthesia revealed no
need for additional dbridement. Antibiotic treatment
was continued, and whirlpool therapy was initiated.
Gram stain of tissue obtained during the surgical procedure revealed numerous gram-positive and gramnegative bacteria, including Staphylococcus aureus and
Escherichia coli.
Case Resolution
By postoperative day 22, the edema had resolved,
the wound was healing well, and no sign of surrounding infection was detected (Figure 4). In the operating
room, the wound underwent primary closure over a
Penrose drain to prevent abscess. The drain was removed in 5 days. At the final follow-up evaluation
Dr. Stockinger is a staff surgeon in the Department of General Surgery,
Naval Medical Center, Portsmouth, VA.
DISCLAIMER: This article was written by CDR Zsolt T. Stockinger, MC,
USNR, during his fellowship training in trauma surgery and surgical critical care at Tulane University School of Medicine in New Orleans,
Louisiana. The views expressed in this article are those of the author and do
not reflect the official policy or position of the US Department of the Navy,
the US Department of Defense, or the government of the United States.
Hospital Physician September 2004
37
Stockinger : Fourniers Gangrene : pp. 37 40
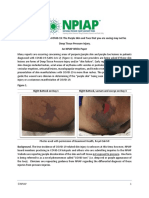
Figure 1. Scrotal edema with skin bronzing and sloughing on
the left medial buttock. The characteristic green-black spot is
indicated by the arrow.
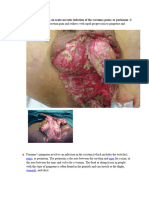
Figure 3. Completed dbridement. The involved area is
much greater than that suggested by skin necrosis.
Figure 2. Excision of necrotic skin reveals extensive liquefaction necrosis of the underlying subcutaneous fat.
several weeks later, the patient was well and a good cosmetic and functional result had been achieved.
DISCUSSION
Fourniers gangrene is a fulminant soft tissue infection that spreads through the subcutaneous tissue
planes and can rapidly cause death from sepsis, acute
renal failure, diabetic ketoacidosis, or multiple organ
failure.2 4 It occurs with a male-to-female predominance of 10:1.3 The mean age of patients ranges from
46 to 56 years,2,4,6,7 although Fourniers gangrene has
been reported in children.2 4 Mortality rates range
38 Hospital Physician September 2004
Figure 4. Twenty-two days after dbridement. The wound
is much smaller after the resolution of edema. Note the flaccidity of the scrotal skin in comparison with its appearance
before the first dbridement (Figure 1).
from 3% to 45%,3,4,6,8 and more than 1700 cases from
5 continents have been reported in the literature.3
www.turner-white.com
Stockinger : Fourniers Gangrene : pp. 37 40
Pathogenesis
Fourniers gangrene is a polymicrobial infection,3 the
source of which is anorectal in 13% to 50% of cases,3,7,8
genitourinary in 17% to 87%,3,7,8 and cutaneous in 21%
to 24%.2,3 It develops after urologic and anorectal procedures, including vasectomy.3,4 Thus, it is not surprising
that the most common etiologic pathogens are commensal genitourinary or anorectal bacteria. In decreasing incidence, these are E. coli; Proteus, Klebsiella, and
Bacteroides species; streptococci; and staphylococci.2 4
Anaerobes are rarely recovered from tissue culture,
probably because of inadequate sample collection or the
improper handling of samples.4 The reasons for which
organisms of normally low virulence produce such an
aggressive infection are unclear. However, the frequent
comorbid conditions associated with Fourniers gangrene, which include diabetes mellitus (21%79% of
cases),3,4,6 8 immunodeficiency,3,4,7 alcoholism (25%
66% of cases),3,4,7,8 intravenous or subcutaneous drug
abuse,6 and malnutrition,2,4 may contribute to the rapid
progression of the infection.
A more typical superficial cellulitis is characterized
by spreading erythema with edema but without cellular
necrosis. In Fourniers gangrene, infection leads to
obliterative endarteritis and thrombosis of the subcutaneous vessels.3,4 That thrombosis in turn causes ischemic necrosis of the overlying skin, the appearance
of which fails to indicate the extent of infection. The
localized tissue hypoxia then promotes the growth of
the anaerobic bacteria usually identified in cases of
Fourniers gangrene. Liquefaction necrosis of the subcutaneous fat may be caused by toxic bacterial products, such as hyaluronidases and collagenases from
staphylococci and streptococci, coagulases from hemolytic streptococci, heparinases from some anaerobic bacteria, and lipopolysaccharides from gram-negative
bacteria.2,8 Infection spreads along the subcutaneous and
fascial planes, although myonecrosis is rare.3
Although Jean Alfred Fourniers original description of the disease that bears his name included only
scrotal involvement,3 Fourniers gangrene can also involve the penis, labia, abdominal wall, thighs, and buttocks. Because Colles fascia attaches to the perineal
body posteriorly and to the pubic rami laterally, the
spread of infection is most likely to occur anteriorly
along Scarpas or Campers fascia to the abdominal
wall and to the scrotum if the source is perianal.2,4,8
The testes are usually uninvolved because their blood
supply arises separately from the intraabdominal aorta,
but the blood supply of the scrotum arises from
branches of the femoral artery.3,8 However, orchiectomy rates of 10% to 30% have been reported.2,4
www.turner-white.com
Diagnosis
The classic signs of Fourniers gangrene are pain,
swelling, and erythema of the scrotum in addition to
fever.2,4,8 Patients usually present after 2 to 7 days of
symptoms.2,4 As the infection progresses, cyanosis, blistering, and bronzing of the skin2,4,8 evolve into the formation of black or green plaques of frank dermal necrosis in up to 100% of cases (Figure 1).9 These plaques
are perhaps the hallmark diagnostic finding of the
infection on physical examination. Pain may diminish
after skin necrosis has occurred.2 Pneumoscrotum has
been reported in 18% to 62% of cases.4,8 That finding
can lead to misdiagnosis as gas gangrene, even though
Clostridium perfringens is infrequently isolated from tissue
cultures.3 Septic symptoms may be disproportionate to
the appearance of the scrotal skin.4,8
Urinalysis, cystoscopy, anoscopy, or rigid sigmoidoscopy may be indicated because a genitourinary or
anorectal source of infection is often identified.3,8 A
search for the previously mentioned comorbid conditions frequently associated with Fourniers gangrene is
also warranted.2,4 Fourniers gangrene has also been
reported as the initial presentation of HIV infection4
and of diabetes mellitus.2,3
Fourniers gangrene is most frequently misdiagnosed as strangulated hernia, scrotal cellulitis, or other
intrascrotal pathology (eg, torsion, abscess).2,4 However, pyoderma gangrenosum and dry (noninfectious)
gangrene caused by vasculitis are occasionally misdiagnosed as Fourniers gangrene.2 Cellulitis that does not
respond appropriately to antibiotic treatment is highly
suggestive of Fourniers gangrene8 and should prompt
early surgical consultation. A high index of suspicion is
required for accurate, early diagnosis, which minimizes
tissue loss and mortality.
Although imaging studies such as plain radiographs, computed tomography, and ultrasonography
can reveal tissue gas or edema, those evaluations usually are not necessary in the diagnosis of this infection.2,4
Ultrasonography is probably most useful to rule out
other acute scrotal pathologies in questionable cases.2,8
Treatment
At diagnosis, treatment with broad-spectrum parenteral antibiotics effective against gram-positive, gramnegative, and anaerobic bacteria should be initiated.3 An
appropriate empiric antibiotic regimen could include
ampicillin or penicillin G to cover gram-positive bacteria,
an aminoglycoside or third-generation cephalosporin to
cover gram-negative and coliform organisms, and clindamycin or metronidazole to cover anaerobic bacteria.6,8
However, the primary treatment remains surgical; in fact,
Hospital Physician September 2004
39
Stockinger : Fourniers Gangrene : pp. 37 40
the removal of devitalized tissue can alleviate systemic
toxicity.3
Delay in surgical treatment is a key factor in mortality.6 Definitive treatment requires prompt, aggressive surgical dbridement and removal of all nonviable tissue,
which may require multiple surgical procedures.2 4
According to Yaghan et al, Under no circumstance
should the surgeon worry about the amount of tissue
excised [sic] needed to reach viable margins.4 Because
the spread of infection is subcutaneous, the dbrided
area is usually greater than that suggested by necrotic
skin2 (Figures 2 and 3). If the dbridement involves the
perianal region, colostomy for fecal diversion may be
required to facilitate wound care.2,3 Urinary diversion
by Foley catheter is usually sufficient,4 and dbridement
of muscle and deep fascia is not usually required.2
Occasionally, the removal of all scrotal skin will leave
the testes hanging on their spermatic cords like the
clappers of a bell,3 or the penis may need to be degloved. In such cases, creative reconstruction is required at a later date, but the testes must be protected
from desiccation in the interim. This can be accomplished by creating a temporary or permanent thigh or
abdominal wall pouch that is superficial enough to
allow the lower temperatures required for spermatogenesis; alternatively, wet-to-dry dressings can be used.2,8
Fertility is rarely compromised.3
Regardless of the results of Gram stain or tissue culture, Fourniers gangrene is assumed to be a polymicrobial infection, and broad-spectrum antibiotic coverage should be continued postoperatively.3,8 Treatment
to eradicate anaerobic bacteria, which frequently fail to
grow in culture, is mandatory. Hyperbaric oxygen has
been proposed for the treatment of Fourniers gangrene,7 possibly because scrotal crepitation erroneously
suggests clostridial gangrene.3 However, that treatment
has not been uniformly advocated,3,4 and under no circumstance should its use delay surgical dbridement.2,4
Although extensive dbridement of affected areas is
required, the apparent degree of tissue loss decreases
as edema resolves (Figures 3 and 4), and wounds are
often left to heal by secondary intention.2,4 In spite of
this, skin grafting or flap reconstruction is frequently
required,2 4,8 and lengthy hospitalizations for wound
care and reconstruction are common. Wound care
after the completion of dbridement should follow the
usual surgical principles8 and may involve the use of
wet-to-dry dressings, hydrotherapy, or enzymatic dbridement.4 Maintenance of positive nitrogen balance,
preferably by enteral feeding, is necessary.3
CONCLUSION
Fourniers gangrene is an aggressive necrotizing
infection of the perineum and genitalia that can rapidly
progress to sepsis and death. Unfamiliarity with this disease results in misdiagnosis and a delay in treatment,
which contribute greatly to morbidity and mortality.
Fourniers gangrene is often misdiagnosed as scrotal cellulitis, strangulated hernia, or other intrascrotal pathology and should be suspected in patients with cellulitis that
does not respond appropriately to antibiotic treatment.
A green or black patch of necrotic skin is the classic sign
of this infection. Fourniers gangrene spreads subcutaneously, and as a result, visible signs of the disease fail to
indicate the extent of tissue destruction.
Fourniers gangrene is associated with a mortality rate
of 3% to 45%. Because the infection is usually polymicrobial, treatment with broad-spectrum antibiotics is required to eliminate gram-positive, gram-negative, and
anaerobic bacteria. Operative dbridement remains the
definitive treatment, and surgical consultation should be
obtained early to ensure the best possible outcome. HP
REFERENCES
1. Meleney FL. Hemolytic streptococcus gangrene. Arch
Surg 1924;9:31731.
2. Smith GL, Bunker CB, Dinneen MD. Fourniers gangrene. Br J Urol 1998;81:34755.
3. Eke N. Fourniers gangrene: a review of 1726 cases. Br J
Surg 2000;87:71828.
4. Yaghan RJ, Al-Jaberi TM, Bani-Hani I. Fourniers gangrene: changing face of the disease. Dis Colon Rectum
2000;43:13008.
5. Moses AE. Necrotizing fasciitis: flesh-eating microbes
[editorial]. Isr J Med Sci 1996;32:7814.
6. Bosshardt TL, Henderson VJ, Organ CH Jr. Necrotizing
soft-tissue infections. Arch Surg 1996;131:84654.
7. Dahm P, Roland FH, Vaslef SN, et al. Outcome analysis
in patients with primary necrotizing fasciitis of the male
genitalia. Urology 2000;56:316.
8. Vick R, Carson CC 3rd. Fourniers disease. Urol Clin
North Am 1999;26:8419.
9. Benizri E, Fabiani P, Migliori G, et al. Gangrene of the
perineum. Urology 1996;47:9359.
Copyright 2004 by Turner White Communications Inc., Wayne, PA. All rights reserved.
40 Hospital Physician September 2004
www.turner-white.com
Вам также может понравиться
- PCCN PrepДокумент133 страницыPCCN Prepdaniel100% (2)
- TB of The TestesДокумент2 страницыTB of The Testesntambik21Оценок пока нет
- Ectopic PregnancyДокумент26 страницEctopic PregnancyCHryz TinОценок пока нет
- Nursing Care Plan (Post Op Exlap)Документ2 страницыNursing Care Plan (Post Op Exlap)Kay D. BeredoОценок пока нет
- Fournier's Gangrene EmergencyДокумент4 страницыFournier's Gangrene EmergencyLalo ZaraloОценок пока нет
- Gangrena de FourniereДокумент11 страницGangrena de FourniereSebas MuñozОценок пока нет
- Chen 2018Документ5 страницChen 2018Teja Laksana NukanaОценок пока нет
- Surgical Management of Fourniers Gangrene A Seven Year Experience at The Philippine General HospitalДокумент6 страницSurgical Management of Fourniers Gangrene A Seven Year Experience at The Philippine General HospitalGian PagadduОценок пока нет
- Management of Fournier GangrenДокумент4 страницыManagement of Fournier GangrenArby ShafaraОценок пока нет
- Fournier S GangreneДокумент8 страницFournier S GangreneabhishekbmcОценок пока нет
- Necrotizing Cellulitis of The Perineum Complicating A Surgical Cure For Bartholinitis: A Case ReportДокумент6 страницNecrotizing Cellulitis of The Perineum Complicating A Surgical Cure For Bartholinitis: A Case ReportIJAR JOURNALОценок пока нет
- Chronic Meningococcemia in A 16-Year-Old Boy: A Case ReportДокумент3 страницыChronic Meningococcemia in A 16-Year-Old Boy: A Case ReportUjean Santos SagaralОценок пока нет
- Fournier Gangrene-A Flesh Eating DiseaseДокумент35 страницFournier Gangrene-A Flesh Eating DiseaseDr Diana EnachescuОценок пока нет
- Fournier's Gangrene: Literature Review and Clinical CasesДокумент8 страницFournier's Gangrene: Literature Review and Clinical CasesDaniel RusieОценок пока нет
- NEJM 347 p0340Документ7 страницNEJM 347 p0340Nantini GopalОценок пока нет
- Pi Is 0278239103007407Документ5 страницPi Is 0278239103007407tengoplatita2008Оценок пока нет
- Fournier Gangrene Pictorial ReviewДокумент11 страницFournier Gangrene Pictorial ReviewKristell PérezОценок пока нет
- Diagnosis BandingДокумент7 страницDiagnosis BandingSyafar SmОценок пока нет
- Fournier'S Gangrene: Rajah Amina SuleimanДокумент27 страницFournier'S Gangrene: Rajah Amina SuleimanAmina RajahОценок пока нет
- Necrotizing FascitisДокумент3 страницыNecrotizing FascitisSanchai RabinoОценок пока нет
- Fournier's Gangrene: An Experience in Tertiary Care HospitalДокумент9 страницFournier's Gangrene: An Experience in Tertiary Care HospitalKriti KumariОценок пока нет
- MMH - Infections of The Upper LimbsДокумент50 страницMMH - Infections of The Upper LimbsHugo de la RosaОценок пока нет
- Fourniers Gangrene and Its Management A Prospective StudyДокумент12 страницFourniers Gangrene and Its Management A Prospective StudyAthenaeum Scientific PublishersОценок пока нет
- Sexually Transmitted Infections (Sti) Ii: Return To SyllabusДокумент15 страницSexually Transmitted Infections (Sti) Ii: Return To SyllabusANGGITA LARASATI PURBANINGRUMОценок пока нет
- 13 - 266fourniers Gangrene PDFДокумент5 страниц13 - 266fourniers Gangrene PDFMochamad RizalОценок пока нет
- Anthrax of The Gastrointestinal Tract: Thira Sirisanthana and Arthur E. BrownДокумент3 страницыAnthrax of The Gastrointestinal Tract: Thira Sirisanthana and Arthur E. BrownJuli SatriaОценок пока нет
- 832-Article Text-2516-3-2-20220920Документ6 страниц832-Article Text-2516-3-2-20220920halimfathoniiОценок пока нет
- Septic Arthritis Characterized byДокумент55 страницSeptic Arthritis Characterized byNdor BariboloОценок пока нет
- Necrotizing FasciitisДокумент45 страницNecrotizing FasciitisKuchai BaruОценок пока нет
- 1 PBДокумент8 страниц1 PBrahmah.hayya00Оценок пока нет
- FournierДокумент3 страницыFournierjkfloresОценок пока нет
- The History Holds The Key in This Gardener With A Skin InfectionДокумент4 страницыThe History Holds The Key in This Gardener With A Skin InfectionPercy Ureta SierraОценок пока нет
- ORF Nodule Complicated by Erythema Multiforme About 2 CasesДокумент3 страницыORF Nodule Complicated by Erythema Multiforme About 2 CasesAthenaeum Scientific PublishersОценок пока нет
- Necrotizingsofttissue Infections: Dennis L. Stevens,, Amy E. Bryant,, Ellie Jc. GoldsteinДокумент21 страницаNecrotizingsofttissue Infections: Dennis L. Stevens,, Amy E. Bryant,, Ellie Jc. GoldsteinHen RyОценок пока нет
- Jurding Mata EndophthalamitisДокумент24 страницыJurding Mata EndophthalamitisBenk Setsuna F. SeieiОценок пока нет
- Ceju 73 0060Документ6 страницCeju 73 0060Jefferson RuizОценок пока нет
- Jurnal MenagementДокумент5 страницJurnal Menagementelsy oktaviaОценок пока нет
- 1 s2.0 S0302283822026252 MainДокумент6 страниц1 s2.0 S0302283822026252 MainjuanmisqjОценок пока нет
- Phlegmon: Signs and SymptomДокумент4 страницыPhlegmon: Signs and SymptomFadly RizkyОценок пока нет
- Staphylococcal Scalded Skin Syndrome in Child A CAДокумент6 страницStaphylococcal Scalded Skin Syndrome in Child A CAsalshabilaОценок пока нет
- Reporte de CasoДокумент2 страницыReporte de CasoEdgarОценок пока нет
- Necrotizing FasciitisДокумент11 страницNecrotizing FasciitisElvira Rodriguez EstebanОценок пока нет
- Acc 3121Документ8 страницAcc 3121adadanОценок пока нет
- Sindrome Duh Genital GOДокумент9 страницSindrome Duh Genital GOIntan PermataОценок пока нет
- ©npiap 1Документ6 страниц©npiap 1Carolina RodriguezОценок пока нет
- Necrotizing Fasciitis: David Hough MSIII Penn State College of MedicineДокумент33 страницыNecrotizing Fasciitis: David Hough MSIII Penn State College of Medicineaaz220Оценок пока нет
- Case Summary 14 - Necrotizing FasciitisДокумент12 страницCase Summary 14 - Necrotizing FasciitisIndra Purwanto AkbarОценок пока нет
- Mus III Assignment 1Документ3 страницыMus III Assignment 1zacialyОценок пока нет
- 51 Uysal EtalДокумент4 страницы51 Uysal EtaleditorijmrhsОценок пока нет
- Sudema 2019 EditedДокумент1 страницаSudema 2019 EditedAditya Riadi SyafeiОценок пока нет
- Case Report: Mucormycosis of Mandible With Unfavorable OutcomeДокумент5 страницCase Report: Mucormycosis of Mandible With Unfavorable OutcomeDr.Sudarsan SenОценок пока нет
- A Case of Mucormycosis of ThighДокумент3 страницыA Case of Mucormycosis of ThighHAMMADОценок пока нет
- Fistula-In-Ano Extending To The ThighДокумент5 страницFistula-In-Ano Extending To The Thightarmohamed.muradОценок пока нет
- Fournier GangreneДокумент4 страницыFournier GangreneMwana MahmoudОценок пока нет
- Necrotizing Soft Tissue Infections: A Primary Care ReviewДокумент6 страницNecrotizing Soft Tissue Infections: A Primary Care ReviewYeni PuspitasariОценок пока нет
- Benedictmitnick2019 PDFДокумент9 страницBenedictmitnick2019 PDFArthur TeixeiraОценок пока нет
- Hand Foot and Mouth DiseaseДокумент14 страницHand Foot and Mouth DiseaseE=MC2Оценок пока нет
- Jurnal P.acnesДокумент4 страницыJurnal P.acnesFazlicha SyaradilaОценок пока нет
- Scrofuloderma: A Common Type of Cutaneous Tuberculosis. A Case ReportДокумент5 страницScrofuloderma: A Common Type of Cutaneous Tuberculosis. A Case ReportIndah IndrianiОценок пока нет
- 2028-Article Text-6551-1-10-20230128Документ5 страниц2028-Article Text-6551-1-10-20230128hellowqueenyОценок пока нет
- Fast Facts: Complex Perianal Fistulas in Crohn's Disease: A multidisciplinary approach to a clinical challengeОт EverandFast Facts: Complex Perianal Fistulas in Crohn's Disease: A multidisciplinary approach to a clinical challengeОценок пока нет
- Clinical Management of Bowel Endometriosis: From Diagnosis to TreatmentОт EverandClinical Management of Bowel Endometriosis: From Diagnosis to TreatmentSimone FerreroОценок пока нет
- Cough PBLДокумент3 страницыCough PBLDella FerginaОценок пока нет
- Modul Sooca Mata Refraksi TranslateДокумент3 страницыModul Sooca Mata Refraksi TranslateDella FerginaОценок пока нет
- Nama/umur/jenis Kelamin Follow Up Hari Ini Terapi: Hasil LaboratoriumДокумент3 страницыNama/umur/jenis Kelamin Follow Up Hari Ini Terapi: Hasil LaboratoriumDella FerginaОценок пока нет
- Daftar Pasien Kardiologi KJS Atas 27 Februari 2015Документ1 страницаDaftar Pasien Kardiologi KJS Atas 27 Februari 2015Della FerginaОценок пока нет
- Nama/umur/jenis Kelamin Follow Up Hari Ini Terapi: Hasil LaboratoriumДокумент3 страницыNama/umur/jenis Kelamin Follow Up Hari Ini Terapi: Hasil LaboratoriumDella FerginaОценок пока нет
- Bladder Stones and Kidney Stones: Common ConditionsДокумент2 страницыBladder Stones and Kidney Stones: Common ConditionsDella FerginaОценок пока нет
- Bladder Stone: Images in Clinical MedicineДокумент1 страницаBladder Stone: Images in Clinical MedicineDella FerginaОценок пока нет
- Crigler Najjar SyndromeДокумент3 страницыCrigler Najjar SyndromeDella FerginaОценок пока нет
- Pulmonary Embolism: DefinitionДокумент1 страницаPulmonary Embolism: DefinitionDella FerginaОценок пока нет
- Stones Renal PDFДокумент2 страницыStones Renal PDFDella FerginaОценок пока нет
- Absorption of A Substance by The Intestine Signifies Its Passage Through The Intestinal Epithelium andДокумент3 страницыAbsorption of A Substance by The Intestine Signifies Its Passage Through The Intestinal Epithelium andDella FerginaОценок пока нет
- Risk Factors: Inherited Genetic SyndromesДокумент2 страницыRisk Factors: Inherited Genetic SyndromesDella FerginaОценок пока нет
- New England Journal Medicine: The ofДокумент8 страницNew England Journal Medicine: The ofHarli FeryadiОценок пока нет
- Theories of The Treatment of Narcissistic PersonalitiesДокумент8 страницTheories of The Treatment of Narcissistic PersonalitiesDella FerginaОценок пока нет
- Theories of The Treatment of Narcissistic PersonalitiesДокумент8 страницTheories of The Treatment of Narcissistic PersonalitiesDella FerginaОценок пока нет
- Narcissistic Personality DisorderДокумент2 страницыNarcissistic Personality DisorderDella FerginaОценок пока нет
- How To DiagnoseДокумент2 страницыHow To DiagnoseDella FerginaОценок пока нет
- Carl Rogers and Humanistic EducationДокумент48 страницCarl Rogers and Humanistic EducationMd Tanweer100% (1)
- Healing With Happiness Free PDFДокумент229 страницHealing With Happiness Free PDFBill Gee88% (8)
- Angelina Jolie - NotesДокумент8 страницAngelina Jolie - NotesJan DalawampuОценок пока нет
- Case Study Questions HIVДокумент2 страницыCase Study Questions HIVJill Arciaga0% (5)
- BursitisДокумент8 страницBursitisAgeededin HartОценок пока нет
- The 5 Dysfunctions of A TeamДокумент6 страницThe 5 Dysfunctions of A TeamZie1970Оценок пока нет
- The Use of Hypnosis and Systematic Desensitisation in The Management of Dental Phobia A Case ReportДокумент6 страницThe Use of Hypnosis and Systematic Desensitisation in The Management of Dental Phobia A Case ReportAnissa Citra UtamiОценок пока нет
- Andrew Eastman Resume 3Документ2 страницыAndrew Eastman Resume 3api-281509868Оценок пока нет
- Functional Classification of Ventilator ModesДокумент53 страницыFunctional Classification of Ventilator ModesNasrullah KhanОценок пока нет
- Quick Rubric - 1Документ2 страницыQuick Rubric - 1api-356824125Оценок пока нет
- BFR - Blood Flow Restriction Training - Gain More Muscle While Lifting Light Weight (Re-Edited)Документ39 страницBFR - Blood Flow Restriction Training - Gain More Muscle While Lifting Light Weight (Re-Edited)DanCurtis67% (3)
- Final ReferencesДокумент29 страницFinal ReferencesUday KapoorОценок пока нет
- Glustitch PDFДокумент1 страницаGlustitch PDFRossnani Juaing100% (1)
- APA - DSM5 - Severity Measure For Specific Phobia Adult PDFДокумент3 страницыAPA - DSM5 - Severity Measure For Specific Phobia Adult PDFaasdfjlkОценок пока нет
- Anticholinergic CardДокумент1 страницаAnticholinergic CardSupalerk KowinthanaphatОценок пока нет
- Emdr Client HandoutДокумент6 страницEmdr Client HandoutNeeraj MishraОценок пока нет
- Oral Rehydration TherapyДокумент12 страницOral Rehydration TherapypasambalyrradjohndarОценок пока нет
- Pocket MedicineДокумент10 страницPocket Medicinecrazyballerman8080% (3)
- 3 Kuliah GERDДокумент40 страниц3 Kuliah GERDAnonymous vUEDx8Оценок пока нет
- Diagnosis and Management of ShockДокумент31 страницаDiagnosis and Management of ShockAmeliaОценок пока нет
- Example TF CBT Treatment PlanДокумент5 страницExample TF CBT Treatment PlanSean ThomasОценок пока нет
- Fistula PerianalДокумент25 страницFistula PerianalHafiizh Dwi PramuditoОценок пока нет
- Chapter 5 GuidelinesДокумент4 страницыChapter 5 GuidelinesDennis RossОценок пока нет
- Eclampsia From MedscapeДокумент11 страницEclampsia From Medscapevicky v. p. wardenaar100% (1)
- Bismillah Daftar Pustaka IbdДокумент3 страницыBismillah Daftar Pustaka IbdvennaОценок пока нет
- 3D-19001205-Adlyn Firdaus Sopyan-Kodifikasi-Tugas 2Документ3 страницы3D-19001205-Adlyn Firdaus Sopyan-Kodifikasi-Tugas 2Anis KhoirunisaОценок пока нет
- Doctor LLLLL 4Документ54 страницыDoctor LLLLL 4loveОценок пока нет