Академический Документы
Профессиональный Документы
Культура Документы
Review of Systems
Загружено:
Joevet T. TadlasИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Review of Systems
Загружено:
Joevet T. TadlasАвторское право:
Доступные форматы
Review of General Health Status
System
s The patient is 42 years old, male, and is married, and had 4 children. The patient is wearing a blue
and white striped hospital gown on the first visit. The patient weighed 60 kgs(Feb. 2 ,2010) and on
Feb. 3,2010 58kgs, upon admission 63kgs, ascites present with the abdominal girth of 39 on the 1st
day and 38 on the 2nd day. Height is 5’5. He also had bipedal pitting edema grade 2, has icteric
sclerae and is jaundice all over. He is conversant and witty, is alert and oriented to time, place and
person. Is experiencing weight loss. He had no mobility problems but he needs assistance upon
dressing because of the IV line, he can consume a cup of rice,1 serving of any kind of viand and a
cup of water every meal. He considers his health not in good condition because of his illness.
Areas/Syste ROS Physical Assessment/Examination
ms
Inspection Palpation Percussion Auscultation
Skin:
Integument The patient had no • jaundice, • CRT- 3 sec.
ary skin diseases • caput medusa • Poor skin
present such turgor
• Cracked red
as rashes,
lips
sores, ulcers,
warts, or • Scaly
moles. There Nails:
are no skin • Pale,
tumors, (-)clubbing
masses, and Temperature:
bruises. Hairs Feb. 2,2010
are evenly 10 pm-37.9
distributed. 2 am-37.8
Bathed daily 6 am-37.5
with special Feb. 3, 2010
skin care 10 pm- 38.4
preparation 2 am- 37.5
(applying of 6 am-37.3
lotion). Nails
are clean and
well trimmed.
Head The pt experiences Head:
hangover after • Symmetrical • No lumps and
drinking spree • Can move up tenderness
with his and down, left noted
companions. to right • Scalp freely
Two years ago without pain movable
had experience Face: without
collapse for 10 • Jaundice lesions or
minutes tenderness
because prior • Can do
at night they different facial
had drinking expressions
session with
• Evenly
his friends.
distributed
Hadn’t
hair
experience stiff
neck or head
trauma.
Eyes The patient is • Eyelashes and
already unable Eyebrows are
to read small well
letters. He distributed
does not wear • Icteric Sclerae
any eyeglasses • No lesions or
and did not go inflammation
for a check-up of eyelids
with an • Pupils equally
ophthalmologis reactive to
t. light
Ears The patient had no External Ear:
history of • Auricles are • No
hearing aligned with tenderness
disturbances. eyebrows. noted
Had not • No pain upon
experience any movement of
discharges or auricle and
pain. tragus
• No discharges
noted
External Canal:
• No redness,
swelling,and
discharges
noted
Nose and Experience colds if • No
Sinuses exposed to rain • Nasal cavities tenderness
sometimes are patent noted
Mouth and He had history of • Red, dry,
Pharynx alcoholism;eve cracked lips.
ry 15 days he • Dry buccal
always buy 1 mucosa,
long neck of intact, no
tanduay rhum prescence of
a day for 3-4 lesion.
days. He is • Gums appear
fond of eating very red but
meat as well as there are no
salty and fatty signs of
food. bleeding.
Neck No history of lumps • Freely moves • (-)pain
or swelling. -chin to chest • (-)masses
Had not -bends head • (-)enlargemen
experience stiff forward t of thyroid
neck and any and backward gland
limitation of -side to side
motion.
No history of lung • SOB when • chest • diaphrag • clear
Thorax and diseases, chest lying excursion matic breath
pain with Respiratory System =15 cm excursion sounds
Lungs/ breathing and Feb. 1, 2010 • vocal = 5cm on all
Respiratory wheezing or 2 am-26 cpm ( tactile) lung
noisy breathing. 6 am-31 cpm fremitus fields
Feb. 2, 2010 bilaterally
10 pm-30 cpm equal
2 am-34 cpm • no lumps
6am-30 cpm and
Feb. 3, 2010 masses
10 pm- 29 cpm noted
2 am- 30 cpm
No history of • JVD =3cm @ • PR : • BP
Cardiovascul cardiovascular 45 degrees Feb. 2, 2010 Feb. 2
diseases, no 2am=84 10pm=100/8
ar history of bpm 0
hypertension, 6am=93 2am=110/80
had normal BP bpm 6am=100/60
range 100/70- Feb. 3, 2010 Feb. 3
120/80 mmHg 10pm=98bp 10pm=110/7
since. m 0
2am=96bpm 2am=110/70
6am-90bpm 6am=100/70
Can consume • Veins are • (+) • Bowel
Abdomen four spoon full’s visible in shifting sounds
of rice and viand both right dullness cannot be
every meal and left • (+) fluid appreciat
before, and on upper wave test ed
admission can quadrant
consume 1 cup • Abdominal
of rice and 1 girth
serving of viand Feb 2, 2010
every meal. Had - Cm
experienced Feb 3, 2010
abdominal - Cm
pain(epigastric
area) 2 weeks
prior to
admission.
Defecates 2
times a day. 2
weeks prior to
admission the
client has stated
that he had
noticed that his
Вам также может понравиться
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- RadionicsДокумент178 страницRadionicsNisha Joshi82% (22)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
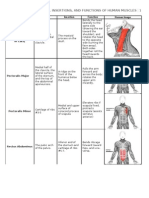
- Origins, Insertions, and Functions of Human MusclesДокумент5 страницOrigins, Insertions, and Functions of Human MusclesNikhil Narang100% (1)
- Positioning ChecklistДокумент2 страницыPositioning ChecklistMark Terence Padua AbrenicaОценок пока нет
- Gummy Smile017Документ55 страницGummy Smile017Shathra'a HamzaОценок пока нет
- Electrotherapy 1 Viva QuestionsДокумент9 страницElectrotherapy 1 Viva QuestionsAmaan Shafique100% (2)
- Block 1 Eccentric Below 80 Triphasic Training Single Legs SpeedДокумент2 страницыBlock 1 Eccentric Below 80 Triphasic Training Single Legs SpeedTj NewsomОценок пока нет
- Ch22 HeartДокумент65 страницCh22 HeartC Bala Diwakesh100% (4)
- Anatomy of External and Middle Ear by Dr. Faisal RahmanДокумент87 страницAnatomy of External and Middle Ear by Dr. Faisal RahmanFAISAL RAHMANОценок пока нет
- DactylographyДокумент14 страницDactylographyniraj_sdОценок пока нет
- 2 Day Action Plan: Adolescent and Youth Health and Development Program (AYHDP)Документ3 страницы2 Day Action Plan: Adolescent and Youth Health and Development Program (AYHDP)Joevet T. Tadlas100% (1)
- Ier and GilesДокумент6 страницIer and GilesVanessa Mae MapanaoОценок пока нет
- Review of SystemsДокумент7 страницReview of SystemsJoevet T. TadlasОценок пока нет
- Case Study On Pre EclampsiaДокумент28 страницCase Study On Pre EclampsiaVianca Louriele Lavarro100% (3)
- Routine Immunization Schedule For InfantsДокумент2 страницыRoutine Immunization Schedule For InfantsanreilegardeОценок пока нет
- Pa Tho 3Документ1 страницаPa Tho 3Joevet T. TadlasОценок пока нет
- Diabetes MellitusДокумент66 страницDiabetes MellitusJoevet T. TadlasОценок пока нет
- Patch AssessmentДокумент5 страницPatch AssessmentJoevet T. Tadlas0% (1)
- HepatocellularДокумент1 страницаHepatocellularJoevet T. TadlasОценок пока нет
- Descriptives (A) Statistic 4.60 Lower Bound Upper BoundДокумент8 страницDescriptives (A) Statistic 4.60 Lower Bound Upper BoundJoevet T. TadlasОценок пока нет
- Characteristics BenignДокумент4 страницыCharacteristics BenignJoevet T. TadlasОценок пока нет
- Definition of TermsДокумент6 страницDefinition of TermsJoevet T. TadlasОценок пока нет
- Prevalence of LC and CДокумент2 страницыPrevalence of LC and CJoevet T. TadlasОценок пока нет
- Community Action PlanДокумент4 страницыCommunity Action Planroren100% (1)
- Test Bank For Anatomy and Physiology The Unity of Form and Function 5th Edition SaladinДокумент52 страницыTest Bank For Anatomy and Physiology The Unity of Form and Function 5th Edition Saladinronaldoruby3i9100% (25)
- Mouth Throat Nose and Sinuses Assessment FindingsДокумент5 страницMouth Throat Nose and Sinuses Assessment FindingsChris SmithОценок пока нет
- Chapter 5 The Integumentary SystemДокумент25 страницChapter 5 The Integumentary Systemlolasparkle100% (2)
- Solution Manual For Holes Human Anatomy Physiology 16th Edition Charles Welsh Cynthia Prentice CraverДокумент36 страницSolution Manual For Holes Human Anatomy Physiology 16th Edition Charles Welsh Cynthia Prentice Cravertroul.cubit.nwjkgf100% (41)
- Module 1.nerve and Humoral RegulationДокумент65 страницModule 1.nerve and Humoral RegulationParamveer SinhОценок пока нет
- Removable Partial Denture OcclusionДокумент17 страницRemovable Partial Denture OcclusionJhuselle Patrice de MesaОценок пока нет
- Anatomy AdhyapakДокумент50 страницAnatomy AdhyapakChief Nike - Clash RoyaleОценок пока нет
- Heart Dissection Lab Report Guide2Документ7 страницHeart Dissection Lab Report Guide2Dylan FernandezОценок пока нет
- Anatomi-EXTREMITAS INFERIORДокумент78 страницAnatomi-EXTREMITAS INFERIORMuhammad Ilham Arif D3 FisioterapiОценок пока нет
- Lab - Nerve ReflexesДокумент6 страницLab - Nerve Reflexesirfan100% (1)
- Otorhinolaryngology: Inferior Turbinectomy: What Is The Best Technique?Документ2 страницыOtorhinolaryngology: Inferior Turbinectomy: What Is The Best Technique?Ramya KamathОценок пока нет
- EmtДокумент9 страницEmtNiki CheeruОценок пока нет
- Reviewer ANPH111 CandyДокумент21 страницаReviewer ANPH111 CandyRein TopacioОценок пока нет
- 37 Posture Yang Short FormДокумент3 страницы37 Posture Yang Short Formschorleworle100% (1)
- #0、aneurysmДокумент39 страниц#0、aneurysmMargaret ThatcherОценок пока нет
- Fierce 5 SpreadsheetДокумент14 страницFierce 5 SpreadsheetMamalo YazoОценок пока нет
- Biomechanical CanineДокумент8 страницBiomechanical CanineSANTIAGO NICOLAS CUERVO MALDONADOОценок пока нет
- Insanity Workout Excel WorksheetДокумент3 страницыInsanity Workout Excel WorksheetClinton D'CostaОценок пока нет
- Cleft Lip and Palate - Claniofacial Clefts BookДокумент137 страницCleft Lip and Palate - Claniofacial Clefts BookAbdulaziz HassenОценок пока нет