Академический Документы
Профессиональный Документы
Культура Документы
Evaluation of Gallbladder Content Spillage in Laparoscopic Cholecystectomy
Загружено:
IOSRjournalАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Evaluation of Gallbladder Content Spillage in Laparoscopic Cholecystectomy
Загружено:
IOSRjournalАвторское право:
Доступные форматы
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS)
e-ISSN: 2279-0853, p-ISSN: 2279-0861.Volume 14, Issue 8 Ver. VI (Aug. 2015), PP 105-122
www.iosrjournals.org
Evaluation of Gallbladder Content Spillage in Laparoscopic
Cholecystectomy
Dr. Keval Sansiya1, Dr. Hardik Dodia2, Dr. Dimple Patel3, Dr. Neel Patel4
1
(General Surgery department, B.J. Medical College/ Gujarat University,India)
(General Surgery department, B.J. Medical College/ Gujarat University,India)
1
(General Surgery department, B.J. Medical College/ Gujarat University,India)
1
(General Surgery department, B.J. Medical College/ Gujarat University,India)
21
Abstract:With increasing number of laparoscopic cholecystectomy performed worldwide, there has been
increasing cases of complications related to it. One of which is gallbladder content spillage and its
complications. Here I present study of 25 such cases randomly selected during my period of surgical residency
from july 2012 to november 2014, I have tried to evaluate factors affecting it, its age/sex incidence, incidence
according to gall bladder status, post operative complications in form of Surgical site infection, Peritonitis,
Increased hospital stay, etc
Keywords:Bile spillage in laparoscopic cholecystectomy, Gall bladder perforation during laparoscopic
cholecystectomy, post operative complication in bile spillage, Factors causing bile spillage in laparoscopic
cholecystectomy
I.
Introduction
Gallstones are present in about 10% to 15% of the adult population & 3-6 % of adult Indian
population 19. Between 1% and 4% become symptomatic in a year requiring cholecystectomy, making
cholecystectomy one of the most common operations performed by general surgeons. Before 20 years open
cholecystectomy was operation of choice for cholecystitis. It is since last 20 years that laparoscopic
cholecystectomy is established as gold standard surgery for the cholelithiasis. laparoscopic cholecystectomy has
clear cut advantages over open cholecystectomy so much so as to establish laparoscopic approach as the
treatment of choice. However, with the increase in the number of laparoscopic operations performed, there has
also been a noticeable increase in the number of complications specific to these procedures. Gallstones can be
spilled during an open cholecystectomy, but these stones are eliminated usually through direct removal, copious
irrigation and mopping with laparotomy sponges. In laparoscopic procedures, these techniques are more difficult
or unavailable and so stones can disappear from view and can become "lost". Studies show that the incidence of
spilled gallstones during laparoscopic cholecystectomy accounts for 6 to 40% of procedures performed, while
incidence of stone loss is unknown 5. Complications from stones that are left within the peritoneal cavity can
cause unusual but significant morbidity. So I want to evaluate the cases in which gallbladder perforation and
spillage occurred in laparoscopic cholecystectomy to evaluate the postoperative outcome and the risk factors for
spillage as well.
Index
1) Table of contents
2) Aims and objectives of study
3) Materials and methods / Data Collection
4) Review of literature
5) Observation and Discussion
6) Summary
7) Conclusion
8) References
Acknowledgements
2) Aims of Study
1. To study and evaluate the predisposing risk factors for gallbladder spillage during laparoscopic
cholecystectomy.
2. To study and evaluate all possible postoperative outcomes that occur during laparoscopic cholecystectomy
with gallbladder perforation and spillage.
3. To study and evaluate the predisposing risk factors for developing complications in a patient with
gallbladder spillage during laparoscopic cholecystectomy.
DOI: 10.9790/0853-1486105122
www.iosrjournals.org
105 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
II.
Material And Method
Hospital Setting
The study was conducted at the surgical unit of civil hospital, Ahmedabad, a publicly funded tertiary
care institution, which serves as the major referral centre for other public and private hospitals within Gujarat
state and surrounding states particularly Rajasthan and Madhya Pradesh. Hospital has also 24 hours emergency
care service with ICU care.
Data collection
A total of 25 patients, with a diagnosis of chronic calculus cholecystitisthat underwent laparoscopic
cholecystectomy with intra operative Gallbladder spillage from July 2012 to December 2014, were collected.
Patients were interviewed according to the proforma. Data was obtained from surgical records to complete
proforma and summarize events. Data collected included clinical features, past history, laboratory
investigations, imaging, intraoperative or postoperative complications and duration of hospital stay.
Inclusion criteria
Patients with cholelithiasis proven by ultrasonography with atleast one attack of upper abdominal pain and
considered fit for cholecystectomy were included in the study.
Exclusion criteria
The patients having history or investigation suggestive of common bile duct stone were excluded from the
study.
Patient with acute cholecytitis were excluded.
Review of Literature
HISTORY:(3)
1420: The first account of gallstones was given by a Florentine pathologist Antonio Benevieni, in an
autopsy of a woman who died with abdominal pain.
1687: Stal Pert Von Der Wiel, while operating a patient with purulent peritonitis accidentally found
gallstones.
1733: Jean-Louis Petit, the founder of gall bladder surgery suggested removal of gallstone and drainage of
the gall bladder, thus creating fistula in patients with empyema, which he successfully performed in 1743.
1859: J.L.W Thudichum proposed a two-stage elective cholecystostomy. In the first stage, the inflamed gall
bladder was sewed to the anterior abdominal wall through a small incision, which served as a route for the
removal of gall stone at a later date.
1867: Dr John StoughBobbs from Indianopolis, Indiana while operating on a patient with suspected ovarian
cyst found an inflamed and adhered sac containing several solid ordinary rifle bullet like structures. He
opened the sac, which incidentally happened to be the gall bladder packed with multiple gallstones. He
removed the gallstones and left the gall bladder in the abdomen after closing the defect in the gall bladder
(cholecystostomy).
1878: Marion Simms performed first cholecystostomy on a 45-year-old woman with obstructive jaundice.
Though the patient died on the eighth postoperative day due to massive internal haemorrhage, it paved the
way for Theodor Kocher to perform the first successful cholecystostomy in June 1878.
1882: Carl Johann August Langenbuch who observed that these measures were only temporary and rallied
to find a definite solution for the disease. He developed the technique of cholecystectomy through cadeveric
dissection and he successfully removed the gall bladder of a 43-year-old man who was suffering from the
disease for 16 years. Langenbuch found two gallstones and a chronically inflamed and thickened gall
bladder. The patient was discharged uneventfully from the hospital after six weeks.
By the turn of the century it was established that cholecystectomy could guarantee permanent relief from
pain whereas cholecystostomy gave a permanent fistula and not a pain-free state.
1987: Mouret from France performed the first human laparoscopic cholecystectomy. On that day as he was
completing a gynaecologic laparoscopy on a woman also suffering from symptomatic gallstones, he shifted
his laparoscope to the subhepatic area. Upon finding a comparatively free and supple gall bladder he
decided to remove it laparoscopically instead of opening up. He performed the procedure successfully and
the patient recovered without complications.
1992: Within two years, in the USA, the procedure was being adopted and because of the massive demand
from the patients, standard traditional stages of scientific evaluation were bypassed. Finally, in September
1992 a NIH consensus conference held in Bethesda concluded that laparoscopic cholecystectomy was the
treatment of choice for cholelithiasis.
DOI: 10.9790/0853-1486105122
www.iosrjournals.org
106 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
Actually Prof Dr Med Erich Mhe of Bblingen, Germany, performed the first laparoscopic
cholecystectomy on September 12, 1985. The German Surgical Society rejected Mhe in 1986 after he
reported that he had performed the first laparoscopic cholecystectomy, yet in 1992 he received their highest
award, the German Surgical Society Anniversary Award.
Perissat, Berci, Cuschieri, Dubois, and Mouret were recognized by SAGES for performing early
laparoscopic cholecystectomies, but Mhe was not. However, in 1999 he was recognized by SAGES for
having performed the first laparoscopic cholecystectomySAGES invited Mhe to present the Storz
Lecture.
In Mhes presentation, titled The First Laparoscopic Cholecystectomy, which he gave in March1999 in
San Antonio, Texas, he described the first procedure.
Finally, Mhe had received the worldwide acclaim that he deserved for his pioneering work.
Complications of laparoscopic cholecystectomy(6)
Haemorrhage
Bile duct injury
Bile leak
Gallstone spillage
Pancreatitis
Wound infection
Incisional hernia
Pneumoperitoneum related: CO2 embolism, vasovagal reflex, hypercarbic acidosis, cardiac arrhythmias
Trocar related: abdominal wall bleeding, hematoma, visceral injury, vascular injury
Wound infection and/or abscess
Deep vein thrombosis
Conversion to open procedure
Laparoscopic cholecystectomy has its own new complications other than of open cholecystectomy.
These are mainly trocar related complications and spillage from gallbladder perforation. Spillage of bile and
stone leads to some short term and long term complications but in a very low rate.
Studies on Gallbladder Spillage
A number of animal studies have been undertaken to determine the potential consequences of spilled
gallstones in the abdominal cavity. Welch et al. 20 investigated the effects of unretrieved gallstones in a rabbit
model. These researchers placed unwashed human gallstones (cholesterol, pigmented and mixed) retrieved from
Laparoscopic cholecystectomy in the peritoneal cavity of rabbits within 6 hours of collection. Wound infection
did not develop in any of the animals, and at autopsy no intra-abdominal sepsis or marked adhesions were
discovered.
Furthermore, a 25% decrease in the size of pigmented stones was noticed after 2 months, raising the
possibility of spontaneous absorption by the peritoneum. Welch et al.20 concluded that free intraperitoneal
gallstones are harmless and thus do not warrant exploratory laparotomy.
However, a larger animal study by Johnston et al. 21 using rats found that leakage of bile in combination
with gallstones was associated with a significant risk of postoperative adhesion formation and possible
intraabdominal abscesses in contradiction to the aforementioned study. These authors, however, did not endorse
the policy of routine laparotomy, except when a large number of stones were unretrievable during Laparoscopic
cholecystectomy.
Leland and Dawson 22 conducted an experimental study using Sprague Dawley rats as a model to
determine the incidence of intra-abdominal adhesions 88 days after sterile artificial cholesterol stones were
placed in the peritoneal cavity. They noted formations ranging from thin and flimsy membranes to thick and
well-developed stalks in 27% of their animals. However, they did not observe any major complication or
absorption of these stones. These authors suggested that intraperitoneal stones could lead to an even higher
incidence of adhesion formation in association with contaminated bile. They observed, furthermore, that other
minerals present in the naturally occurring human gallstones could result in a much stronger inflammatory
response in humans. Leland and Dawson therefore concluded that unretrieved gallstones are not benign and
should be aggressively removed to decrease long-term complications.
Cline et al.23, using Sprague-Dawley rats, reported the effects of various numbers of gallstones lost in the
peritoneal cavity. The authors placed no gallstones, one gallstone, and five gallstones in the peritoneal cavity of
these rats. They killed these animals after 2, 4, and 8 weeks and looked for adhesions, fistulae, perforations, or
obstructions. Except for a trend toward more stones becoming fixed within the abdomen over time, no other
DOI: 10.9790/0853-1486105122
www.iosrjournals.org
107 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
complications were noted in any of these groups. These authors concluded that spilled gallstones do not increase
morbidity after Laparoscopic cholecystectomy.
One of the definitive studies from the Mayo clinic24 addressed the long-term consequences of
intraoperative spillage of bile and gallstones during Laparoscopic cholecystectomy. This study analyzed
prospectively data from 1,059 consecutive Laparoscopic cholecystectomies performed over a 3-year period. The
iatrogenic gallbladder perforation was 29%. The factors associated with higher incidence of gallbladder
perforation included male gender, increasing age, body weight, and the presence of omental adhesions.
The Mayo study demonstrated that spillage of gallbladder content is associated with statistically
significant incidences of intra-abdominal abscesses compared with intact Laparoscopic cholecystectomy.
However, the overall risk of serious complications is very low. The authors emphasized the need for removal of
as many calculi as possible laparoscopically. However, they advised conversion to an open procedure in patients
for whom it is not possible to retrieve the majority of the gallstones laparoscopically, especially when
bacteriobilia is suspected or confirmed by Gram stain of the bile. They noticed that percutaneous drainage of
intra-abdominal abscesses in most of their patients was ineffective if the inciting gallstones were not removed.
In retrospective study from Switzerland25, which analyzed 10,174 Laparoscopic cholecystectomies
performed at 82 surgical institutions over a 3-year period, the incidence of iatrogenic gallbladder perforation
was only 6%, and serious postoperative complications occurred very rarely (0.08%). This study concluded that
elderly patients who have acute cholecystitis with infected bile and spilled stones may experience an increased
risk of intra-abdominal abscess formation. Therefore, perforation of the gallbladder should be prevented
whenever possible. They also emphasized the need to retrieve spilled gallstones and irrigate the abdominal
cavity to dilute the infected bile and spilled stones. They reiterated the message of previous studies that the
laparoscopic procedure should not be converted to an open one just for the retrieval of stones because the
incidence and the mortality rate of serious complications are extremely low.
Risk of Gallbladder Perforation
Certain situations lead to higher risk of gallbladder perforation during laparoscopic cholecystectomy.
Patients with acutely inflamed gallbladders have friable tissue which is susceptible to tear. Dense adhesions
around the gallbladder make dissection potentially more difficult, and a tense, distended gallbladder that has not
been decompressed is at risk of perforation8. This usually occurs when the gallbladder is manipulated by
laparoscopic instruments or when it is dissected from the liver bed or during gallbladder extraction. Spilled
stones are also caused by the slipping of the cystic duct clip or the tearing of the gallbladder while it is retrieved
from the port site9.
There is also a well recognised learning curve for performing laparoscopic cholecystectomies, and the
risk of perforation is high early in a surgeon's laparoscopic career 8.
Risk of Complications from Spillage
Although lost gallstones were initially considered innocuous, it is now recognised that they can be a
small but significant source of postoperative morbidity (0.1 to 6%) 11. The presentation of complications will
vary from patient to patient. Recognised symptoms include abdominal pain, fever, abdominal masses, bowel
obstruction and the presence of a sinus infection or fistula9, 10. In most instances, the diagnosis is made
retrospectively, or after visualisation of the stones on imaging and revisiting the patient's surgical history.
Most complications occur within the first few months, but presentations up to ten years after the
procedure have also been documented13. Zehetner et al.10 looked into all documented complications from lost
gallstones and these ranged from the most common like intra-abdominal and subcutaneous abscesses and
fistulas, to the less common, such as liver abscess, staphylococcus bacteraemia, broncholithiasis and
expectoration, empyema, granulomas, bowel obstruction and incarceration within a hernial sac.
Studies also show risk factors for complications after spilled stones, such as the presence of infected
bile, spillage of pigmented gallstones, multiple stones (>15), stone size (>1.5 cm) and old age10.
Complications from Gallbladder Spillage (27)
1. Intraabdominal abscesses
Subphrenic abscess
Subhepatic abscess
Retroperitoneal abscess
Pouch of douglas abscess
Cutaneous Complications
Port site wound infection
Port site sinus tract formation
Cutaneous fistula
DOI: 10.9790/0853-1486105122
www.iosrjournals.org
108 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
Anterior abdominal wall abscess
Gastrointestinal
Acute pancreatitis
Small bowel obstruction
Sigmoid colon erosion
Partial necrosis and perforation of small bowel
Respiratory
Pleural effusion
Empyema
Pleurolithiasis
Hemoptysis
Cholelithoptysis
Miscellaneous
Incarceration within hernia sac
Cholelithiasis of ovary
Peritoneal granuloma
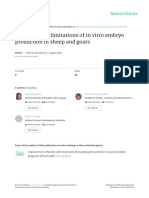
Fig.1 Single Gall bladder perforation during callots triangle dissection.
DOI: 10.9790/0853-1486105122
www.iosrjournals.org
109 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
Fig.2 Single gall bladder perforation at body region
Fig.3Single gall bladder perforation during dissection of Gallbladder fossa
DOI: 10.9790/0853-1486105122
www.iosrjournals.org
110 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
Fig.4 Dissected specimen showing perforation at infundibulum
Fig.5 Spilled stone retrieved by laparotomy
Prevention and Management of Sppillage
The best way to avoid complications from spillage is to have awareness of the situations where
perforation is likely, perform precise dissection, meticulously handle tissue and use devices such as endobags to
retrieve dissected gallbladders through the port sites. Perforation usually occurs when dissecting the gallbladder
from the hepatic fossa, and care taken at this stage of the operation can save many minutes attempting to retrieve
stones from within the peritoneum11.
Despite all precautionary measures, it is unavoidable that gallbladder perforation and stone spillage still
occur in some patients. In these cases, it is crucial to minimize the number of stones spilled, attempt to retrieve
all stones and to copiously irrigate the peritoneal cavity9. This serves the purpose of diluting any infected bile
and may allow the stones to be washed up into the suction system. Some surgeons advocate the use of clips or
an endoloop to close the hole in the gallbladder, while others will introduce a retrieval bag and 'park' it on the
liver to receive all spilled stones14. In some situations it may be necessary to use an extra port adjusted to a 30DOI: 10.9790/0853-1486105122
www.iosrjournals.org
111 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
or 45-degree scope or use a fan liver retractor to improve visualisation 11.
Use of antibiotics has been suggested for patients who undergo laparoscopic cholecystectomy to treat acute
cholecystitis, have visibly infected bile, or have a high amount of spillage.
Possibly the most important aspect in the management of perforated gallbladders and potential stone spillage is
documentation. Diagnosis of complications related to lost stones is often done only after the identification of
gallstones on radiological imaging. If the documentation is clear and the patient is aware of the perforation, then
clinicians may be alerted early to the possibility of a stone complication in order to expedite treatment.
Thus recommended steps during laparoscopic cholecystectomy in case of spillage are:
Informed consent from patient and family preoperatively and mentioning that dropped stones are common
depending on the size of stones and condition of the gallbladder wall and liver bed.
Every effort should be made to retrieve the gallstones and the peritoneum should be irrigated with copious
saline, in case of spillage.
There is routinely no need for converting the laparoscopic procedure to a laparotomy for spilled stones, but
it should be essential to document spilled stones in the operation notes and if laparoscopic stone removal is
not possible, conversion to laparotomy should be done if stones are multiple and/or very large in size
All possible but unlikely consequences of the spillage should be informed to the patient.
The surgeon should have long term follow up of these patients unlike other routine cholecystectomy, as
there is possibility of delayed complications.
In view of confusing delayed clinical presentation during post-op period, surgeon should be alert to rule out
possible complications due to spillage and manage them accordingly.
Management of Complications
Investigations
The imaging method of choice is usually ultrasound, as stones are usually visualised well using this
method. Visualization, however, depends on the location of the lost stones. CT and magnetic resonance imaging
(MRI) can also be used to obtain adjunct images depending on the biochemical composition of the stone. Radioopaque calcified stones, such as pigmented stones, can be seen clearly on CT with unenhanced pictures. On
MRI most stones are hypo-intense on T2-weighted images and iso-intense to hyperintense on T1-weighted
images. These are best seen without fat suppression as this allows for the contrasting features of the stone to be
seen against the fat. Sometimes the radiological findings mimic unusual diagnoses such as actinomycosis,
hydatid disease or even malignancy, so diagnosis can be difficult.
Treatment
Treatment of complications basically depends on the type and site of the complication.
Abdominal wall abscess from stones caught at the port site can be dealt with by local drainage and
evacuation of the stones. Stones which are the foci of infection in these abscesses and sinuses should be
completely removed for a cure.13, 14
Intra-abdominal abscesses can be dealt with percutaneously by minimally invasive technique and
laparotomy where this technique fails15, 17. The percutaneous procedure has the advantage of being less invasive,
having a short hospital stay and minimal discomfort, and is ideally suited for old patients. 18 Computed
tomography guided drainage of the pus is first done with a pigtail catheter. A few weeks later the tract is dilated
with a dilator system and a nephroscope is passed through it and stones are removed.16 Treatment is not
complete until all the stones that are present in the abscess are removed. The size of the stone is an important
determinant. Smaller stones usually less than 1 cm can often be removed through the nephroscope and using a
basket. Larger ones need fragmentation by mechanical means or lithotripsy before attempting removal. 16
Ultrasonic lithotripsy requires a rigid endoscope and keeps stone fragments to a minimum, thereby minimising
the risk of breaking an infected stone into tiny fragments, which may serve as a nidus for further infection. In
dealing with a deep seated abscess with a tortuous tract electrohydraulic lithotripsy in association with
choledochoscopy is a good alternative. 16A completion contrast study (abscessogram) is recommended to check
for the intactness of the cavity and for any retained stones.
Gall stones found at distant sites, have been an incidental finding and can be found in a hernial sac, in
urine, or in sputum. Gall stones causing vesical granulomas resulting in haematuria have been dealt with by
cystoscopic excision of the granulomas. 16
III.
Observation & Discussion
A total of 25 patients, with a diagnosis of chronic calculus cholecystitiswho underwent laparoscopic
cholecystectomy with intra operative Gallbladder spillage from July 2012 to November 2014, were collected.
Following parameters were observed and analyzed. Information data was represented as charts. Data was also
DOI: 10.9790/0853-1486105122
www.iosrjournals.org
112 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
compared with similar studies in the past.
Table 1: Age distribution
Age group
20-29
30-39
40-49
50-59
60-69
No. of patients(n=25)
5
4
10
4
2
Percentage
20%
16%
40%
16%
8%
Table 2: Gender distribution
Sex
Female
Male
Present study(n=25)
No. of patients
Percentage
19
76%
6
24%
DOI: 10.9790/0853-1486105122
Jasim et al(n=73)
No. of patients Percentage
62
84%
11
16%
Rice et al(n=306)
No. of patients
Percentage
174
57%
132
43%
www.iosrjournals.org
113 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
Table 3:Meanage
Study
Rice et al
Jasim et al
Present study
Mean age(yr)
52
36.6
41.48
In present study there were 25 patients with mean age 41.48 ranging from 23 to 61 years. Female group
accounts for 76% and male group for 24% of study.
In the study done by jasimet al.26 mean age was 38.6 and female group accounts for 84% while male
group was 16%.Another study done by rice et al.24 mean age was 52 years, female group was 57% and male
group was 43%.
Gallstone diseases are more common in females than males. Results found similar to present study.
Table 4: Symptoms
Symptoms
Abdominal pain
Nausea
Vomiting
Belching
Bloating
Flatulence
DOI: 10.9790/0853-1486105122
Present study(n=25)
No. of patients
Percentage
25
100%
4
16%
1
4%
12
48%
10
40%
7
28%
Memon MA et al(n=165)
No. of patients Percentage
165
100%
30
18%
6
4%
72
44%
60
36%
42
25%
www.iosrjournals.org
114 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
In the present study symptomatology distribution of patients shows abdominal pain as a most common
symptom followed by belching and bloating. While nausea, vomiting and flatulence are other minor symptoms.
In other study by Memon MA et al.27 all patients had abdominal pain, 44% had belching, 36% had
bloating, 25% had flatulence, 18% had nausea and 4% had vomiting.
So the symptoms can be comparable to present study.
Table 5: USG (single/multiple stones)
USG: GB stone
Single stone
Multiple stones
Present study(n=25)
No. of patients
Percentage
3
12%
22
88%
Memon MA et al(n=165)
No. of patients
Percentage
32
19%
133
81%
Table 6: USG (Gallbladder)
USG gallbladder
Contracted
Distended
Wall normal
Wall thickened
Peri GB collection
DOI: 10.9790/0853-1486105122
Present study(n=25)
No. of patients
Percentage
17
68%
8
32%
23
92%
2
8%
0
0
Memon MA et al(n=165)
No. of patients
Percentage
108
65%
57
35%
144
89%
21
11%
-
www.iosrjournals.org
115 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
In present study 88% patients have multiple GB stones while 12% patients have single GB stone.32%
patients have distended gallbladder and 68% patients have contracted gallbladder. Out of these, 92%
patientshave normal GB wall with 8% have thickened GB wall.None of these have peri GB collection.
In a study by Memon MA et al.27 81% had multiple GB stones with 35% had distended gallbladder
while 65% had contracted gallbladder. 89% had normal GB wall and 11% had thickened wall.
Ultrasonography findings are not more important in a relation with GB perforation and spillage. It is
rather intraoperative GB status which is more important for occurance of gallbladder perforation and spillage.
Table 7: Intraoperative GB finding
Intra operative GB
Chronically inflamed
Mucocele
Pyocele
Present study(n=25)
No. of patients
Percentage
25
100%
1
4%
1
4%
Memon MA et al(n=165)
No. of patients
Percentage
157
95%
4%
4%
-
Table 8: Intraoperative peri GB adhesions and difficult dissection
Peri GB adhesions &
difficult dissection
Yes
No
Present study(n=25)
No. of patients
16
9
DOI: 10.9790/0853-1486105122
Percentage
64%
36%
Memon et al(n=165)
No. of patients
94
71
Percentage
57%
43%
www.iosrjournals.org
Rice et al(n=306)
No. of patients
127
179
Percentage
42%
58%
116 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
Intra operative GB status
Chronically inflammed
Mucocele
Pyocele
Peri GB adhesions
Present study(n=25)
100%
4%
4%
64%
Memon MA et al(n=165)
95%
57%
Rice et al(n=306)
89%
42%
In present study, Intraoperative 100% GB were chronically inflammed out of which 4% turned into
mucocele and 4% into pyocele. There was peri GB adhesions and difficult dissection in 64% of patients while
36% had no peri GB adhesions.
In other study by Memon MA et al.27 95% had chronically inflammed GB while other 5% had acutely
inflammed gallbladder and 57% had peri GB omental adhesions.
Another study done by rice et al.25 at mayo clinic, 89% patients had chronically inflammed gallbladder
and 42% had peri GB omental adhesions.
Chronically inflammed gallbladder has thickened, variegated and friable wall so increasing chances of
GB perforation and spillage.
Omental adhesions makes dissection difficult and increses the chances of gallbladder perforation and
spillage.
Table 9: Bile and Stone spillage
Spillage
Bile
Mucus
Pus
Stone
DOI: 10.9790/0853-1486105122
No. of patients(n=25)
23
1
1
7
Percentage
92%
4%
4%
28%
www.iosrjournals.org
117 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
Spillage
Bile
Mucus
Pus
Stone
Present study(n=25)
92%
4%
4%
28%
Jasim et al(n=73)
97%
3%
47%
Rice et al(n=306)
62%
38%
In present study out of 25 GB spillage, 92% patients had bile spillage, 4% had pus spillage and 4% had
mucus spillage. 7 (28%) patients had stone spillage. 16(64%) patients had only bile spillage while 7 (28%)
patients had bile/mucus/pus with stone spillage.A study by Jasimet al. 26 bile spillage was present in 97% of
patients and gallstone spillage was 47% and 3% had pus spillage.Another study by rice et al 24 bile spillage was
present in 62% of patients and gallstone spillage was 38%.
So in present study occurrence of stone spillage is lower than above mentioned studies. Though there is
significant difference in stone spillage between two studies, there is no significant difference in terms of
complications between two studies. It is retained stones in peritoneal cavity which might be left after saline
wash and irrigation, are more important for developing complications rather than occurance of stone spillage.
Table 10: Postoperative complications
Complications
Port site wound infection
Port site sinus tract
Intraabdominal abscess
Conversion to laparotomy
No complications
DOI: 10.9790/0853-1486105122
No. of patients(25)
3
1
1
1
19
Percentage
12%
4%
4%
4%
76%
www.iosrjournals.org
118 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
Table 11: Comparison of complications
Complications
Port site wound infection
Port site sinus tract
Intraabdominal abscess
Persistant abdominal pain
Conversion to laparotomy
Present study(n=25)
No. of patients
Percentage
3
12%
1
4%
1
4%
1
4%
Jasim et al(n=34)
No. of patients
Percentage
3
8.8%
1
2.94%
3
8.8%
1
2.94%
-
Table 12: Relation between gallbladder spillage and complications
Bile only
Bile/mucus/pus+stone
Total
Complications developed
1
5
6
No complications
17
2
9
Total
18
7
25
In present study no complications occurred in 76% cases. 6 patients (24%) developed complications of
which 3 patients had port site wound infection, 1 had intraabdominal abscess, 1 had sinus tract formation and 1
was converted to open cholecystectomy
20% complicated cases had both stone and bile/pus spillage while 4% had only bile spillage.
In other study by Jasimet al26 complication rate was 23.53%. In that study, out of 34 patients 3
patients(8.8%) developed intaabdominal abscess,3 patients(8.8%) developed port site wound infection, 1
patient(2.94%) developed port site sinus tract formation and other 1 patient(2.94%) developed persistant
abdominal pain due to retained gallstone in peritoneal cavity.
So wound infection and intraabdominal abscess are common complications occurred after gallbladder
spillage.
The p value of table 11 is 0.000535 (p<0.05) which is significant. So chances of postoperative
complications are more in case of bile and stone spillage rather than only bile spillage.
Table 12: postoperative drain removal day
Postoperative day of drain removal
1
2
3
4
5
6
Study
Memon MA at el
Present study
No. of patients(25)
4
17
2
1
0
1
Percentage
16%
68%
8%
4%
0
4%
Mean postoperative drain removal day
2.5 days
2.16
Days
In present study postoperative drain removed on 1st day in 16% of cases, 2nd day in 68% of cases, on 3rd
day in 8% of cases, on 4th day in 4% of cases and on 6th day in 4% of cases.
Mean postoperative drain removal day was 2.16.
In a study by Memon MA et al27 mean postoperative drain removal day was 2.5.
Table 13: Relation between complications and postoperative drain removal day
Drain removal day<=2
Drain removal day >2
Total
Complications developed
4
2
6
No complications
17
2
19
Total
21
4
25
The p value of above table is 0.184 (p=0.184) which is not significant. Therefore postoperative
complications are not related to early or late drain removal.
DOI: 10.9790/0853-1486105122
www.iosrjournals.org
119 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
Table 11: Postoperative hospital stay
Day of postoperative hospital stay
1
2
3
4
5
15
Study
Rice et al
Jasim et al
Present study
No. of patients(25)
1
9
11
2
1
1
Percentage
4%
36%
44%
8%
4%
4%
Mean postoperative hospital stay
2.1 days
2 days
3.2 days
In present study 44% patients discharged on 3rd postoperative day while 36% were discharged on 2nd
postoperative day. Mean postoperative stay was 3.2 ranging from 1 to 15.In a study by Jasimet al 26 mean
postoperative hospital stay was 2 days.Another study by rice et al. 25 mean postoperative hospital stay was 2.1
days.So In this study mean postoperative hospital stay is 1 day longer than above studies. This difference may
be due to different protocols for discharging the patient.
Summary
In this study we have considered randomly selected 25 cases of gallbladder spillage during laparoscopic
cholecystectomy according to inclusion and exclusion criteria.
Study was conducted during period of 30 months (July 2012 to november 2014).
After filling details in proforma, master chart was prepared. A detailed analysis was done and various
observations were derived, discussed and concluded.
The gallbladder spillage is more common in age group 41-50 years (n=10, 40%) with female predominance
DOI: 10.9790/0853-1486105122
www.iosrjournals.org
120 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
(F:M:19:6)as gallstone disease itself is more common in females with 41-50 age group.
All patients (n=25, 100%) presented with abdominal pain with 12(48%) patients had belching, 10(40%)
patients had bloating, 7(28%) patients had flatulence, 4(16%) patients had nausea and 1(4%) patient had
vomiting. Abdominal pain, belching and bloating are common clinical features associated with gallstone
disease.
In ultrasonography, 17(68%) patients had contracted gallbladder and 8(32%) patients had distended
gallbladder. 23(92%) patients had normal gallbladder wall and 2(8%) patients had thickened gallbladder
wall. None of them had peri GB collection. 22(88%) patients had multiple GB stones while 3(12%) patients
had single GB stone.
Intraoperative, all patients (100%) had chronically inflammed gallbladder with 1(4%) patient had mucocele
and 1(4%) had pyocele. Out of them, 16(64%) patients had peri GB omental adhesions with difficult
dissection.
Bile spillage was present in 23(92%) patients. 1(4%) patient had pus spillage and 1(4%) patient had mucus
spillage. 7(28%) patients had stone spillage as well. So 16(64%) patients had only bile spillage and 7(28%)
patients had both bile/pus/mucus and stone spillage.
Postoperative complication rate was 24% (n=6). 3(12%) patients developed port site wound infection,
1(4%) patient had intraabdominal abscess formation, 1(4%) patient had port site sinus tract formation and
1(4%) case was converted to laparotomy. Out of these 6 patients, 5(20%) patients had bile/pus with stone
spillage while 1(4%) patient had only bile spillage.
Postoperative, in 17(68%) patients drain was removed on 2nd postoperative day, in 4(16%) patients drain
was removed on 1st day while in 4(16%) patients drain was removed after 2 days.
In 11(44%) patients postoperative hospital stay was 3 days, in 9(36%) patients it was 2 days and 1(4%)
patient discharged on 1st postoperative day. In 4(16%) patients postoperative hospital stay was more than 3
days.
IV.
Conclusion
Laparoscopic cholecystectomy is the gold standard for gallstone disease.
Gallbladder perforation occurs as a result of intraoperative retraction, dissection and extraction of
gallbladder especially when gallbladder is acutely inflammed and fragile and there is peri GB omental
adhesions.
Gallbladder content spillage is an uncommon occurrence in most of the cases but when it occurs, main goal
of all surgeons should be to manage these complications with minimal harm to the patients and to minimize
unwanted consequences of these complications.
Surgeon should take utmost care and attempt to remove all visible stones and should irrigate abdominal
cavity to dilute infected bile.
If spillage occurs it should be recorded and such patients should be kept under close follow up to aid in
early diagnosis of late complications.
There is no indication for routine conversion to open surgery just for sake of removal of spilled gallstones.
Though complications arises from spillage of gallbladder during laparoscopic cholecystectomy are rare,
they can present months to years later after surgery with septic complications.
Complications are more common after spillage of both bile and stones rather than bile only.
Most of the complications of spillage can be managed by minimal invasive techniques like percutaneous
drainage of abscess. However laparotomy may be needed to address large abscess formation with mass
within it.
Gallbladder spillage during laparoscopic cholecystectomy can be a source of morbidity. So every attempt
should be made to prevent it rather than managing it afterwards.
Acknowledgement
I express my sincere gratitude, indebtedness and respect to Dr. G.H.Rathod Professor and Head of
department, Department of Surgery, B.J Medical college and Civil Hospital, Ahmedabad who by his
constant encouragement and concern, inspired and guided me from the very first step of preparation of this
dissertation. His depth of knowledge and insight into the subject of surgery has helped me to study this
topic. His kindness, compassion, perfection, and loving approach to the patients as well as his students has
left a deep impact on my life which will remain throughout my career.
I am also thankful to Dr. H.R. Chauhan, Associate professor Sola Civil Ahmedabad, Dr. R.A Makwana,
Assistant Professor, Dr R.P Gadani, Assistant Profesor and Dr. R.K. Patel, Assistant Professor Department
of Surgery, B.J.Medical College and for their support and invaluable guidance.
I am also thankful to Dr. M.M. Prabhakar, Medical Superintendent, Civil Hospital, for allowing me to carry
out my study in Civil Hospital, Ahmedabad, and for allowing me to use all the invaluable resources.
DOI: 10.9790/0853-1486105122
www.iosrjournals.org
121 | Page
Evaluation Of Gallbladder Content Spillage In Laparoscopic Cholecystectomy
I am grateful to my parents who have always inspired me in every sphere of my life.
Last but not the least, I am thankful to all my patients and my colleagues and juniors for their cooperation
which helped to complete my study.
References
[1].
[2].
[3].
[4].
[5].
[6].
[7].
[8].
[9].
[10].
[11].
[12].
[13].
[14].
[15].
[16].
[17].
[18].
[19].
[20].
[21].
[22].
[23].
[24].
[25].
[26].
[27].
Bailey and Love short practice of surgery 25th Edition chapter 63
Laparoscopic cholecystectomy an evidence based guide by ferdinandoagresta, 1st edition, page no. 23,24.
Evolution of cholecystectomy: A tribute to Carl August Langenbuch. Indian Journal of Surgery 2004;66:97-100.
Grays anatomy, 39th edition, page no. 243-245.
Laparoscopic surgery of the abdomen By Bruce V. MacFadyen, 1st edition, chapter 15, page no.127
Maingots abdominal operations 11th edition
Mastery of surgery, 5th edition, chapter 97
Frola C, Cannici F, Cantoni S, et al.: Peritoneal abscess formation as a late complication of gallstones spilled during lapar oscopic
cholecystectomy. British Journal of surgery 1999, 72:201-203.
Hand AH, Self ML, Dunn E: Abdominal wall abscess formation two years after laparoscopic cholecystectomy. Journal of surgical
endoscopy 2006, 10:105-107.
Zehetner J, Shamiyeh A, Wayand W: Lost gallstones in laparoscopic cholecystectomy: all possible complications. American
Journal of Surgery 2007, 193:73-78.
Chowbey PK, Bagchi N, sharma A, et al.: Abdominal Wall Sinus: An unusual presentation of spilled gallstone. Journal of
Laparoscopic and endoscopic Surgery Tech A 2006, 16:613-615.
Patterson EJ, Nagy AG: Don't cry over spilled stones? Complications of gallstones spilled during laparoscopic cholecystectomy:
case report and literature review. Canadian Journal of Surgery 1997, 40:300-304.
Cacdac RG, Lakra YP. Abdominal wall sinus tract secondary to gall stones. A complication of laparoscopic cholecystectomy.
Journal of Laparoscopic and endoscopic Surgery 1993; 3: 50911.
Yao CC, Wong HH, Yang CC, et al. Abdominal wall abscess secondary to spilled gallstones: late complication of laparoscopic
cholecystectomy and preventive measures. Journal of laparoscopic and endoscopic surgery 2001;11:4751.
Albrecht RM, Eghtestad B, Gibel L, et al. Percutaneous removal of spilled gallstones in a subhepatic abscess. American journal of
Surgery2002;68:1935
Brueggemeyer MT, Saba AK, Thibodeaux LC. Abscess formation following spilled gallstones during laparascopic
cholecystectomy. Journal of the Society of the Laparoscopic and endoscopic surgery1997;1:14552.
Zamir G, Lyass S, Pertsemlidis D, et al. The fate of dropped gallstones during cholecystectomy. Journal of Surgical
endoscopy1999;13:6870.
Campbell WB, McGarity WC. An unusual complication of laparoscopic cholecystectomy. American journal of surgery
1992;58:64142.
Singh V, Trikha B, Nain CK, Singh K, Bose SM. Epidemiology of gallstone disease in india: A community-based study. Journal of
Gastroenterology 2001; 16: 560-563.
Welch N, Hinder RA, Fitzgibbons RJ Jr, Rouse JW (1991) Gallstones in the peritoneal cavity: a clinical and experimental study.
Journal of Laparoscopic and Endoscopic surgery 1: 246247
Johnston S, OMalley K, McEntee G, Grace P, Smyth E, Bouchier Hayes D (1994) The need to retrieve the dropped stone during
laparoscopic cholecystectomy. American Journal of Surgery 167: 608610
Leland DG, Dawson DL (1993) Adhesions and experimental intraperitoneal gallstones. International journal of Contemporary
Surgery 42: 27327
Cline RW, Poulos E, Clifford EJ (1994) An assessment of potential complications caused by intraperitoneal gallstones. American
journal of Surgery 60: 303-305
Rice DC, Jamison RL, et al (1997) Long-term consequences of intraoperative spillage of bile and gallstones during laparoscopic
cholecystectomy. Journal of Gastrointestinal Surgery 1: 8591
Schafer M, Suter C, Klaiber CH, Wehrli H, Frei E, Krahenbuhl L(1998) Spilled gallstones after laparoscopic cholecystectomy: a
relevant problem? A retrospective analysis of 10,174 laparoscopic cholecystectomies. Journal of Surgical Endoscopy 12: 305309
Jasim D Saud, MazinA Abdulla &Mushtaq Ch. Abu-Alhail spilled gallstones during laparoscopic cholecystectomy: a prospective
study. (2011) basrah journal of surgery 2: 123-127
M. A. Memon, R. K. Deeik, T. R. Maffi, R. J. Fitzgibbons The outcome
of unretrieved gallstones in the peritoneal cavity
during laparoscopic cholecystectomy: A prospective analysis Journal of Surgical Endoscopy (1999) 13: 848857
DOI: 10.9790/0853-1486105122
www.iosrjournals.org
122 | Page
Вам также может понравиться
- Kinesics, Haptics and Proxemics: Aspects of Non - Verbal CommunicationДокумент6 страницKinesics, Haptics and Proxemics: Aspects of Non - Verbal CommunicationInternational Organization of Scientific Research (IOSR)Оценок пока нет
- CholecystectomyДокумент5 страницCholecystectomyRachelle Maderazo CartinОценок пока нет
- Human Rights and Dalits: Different Strands in The DiscourseДокумент5 страницHuman Rights and Dalits: Different Strands in The DiscourseInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Basic Principles of Cross-Examination: Claire F. RushДокумент14 страницBasic Principles of Cross-Examination: Claire F. RushSellappan RathinamОценок пока нет
- The Impact of Technologies On Society: A ReviewДокумент5 страницThe Impact of Technologies On Society: A ReviewInternational Organization of Scientific Research (IOSR)100% (1)
- Sspc-Ab 2Документ3 страницыSspc-Ab 2HafidzManafОценок пока нет
- Project Name: Proposed Icomc & BMC Building Complex Phe Design ReportДокумент19 страницProject Name: Proposed Icomc & BMC Building Complex Phe Design ReportAmit Kumar MishraОценок пока нет
- Safe CholecystectomyДокумент60 страницSafe CholecystectomyCarlos Reyes100% (1)
- Open CholecystectomyДокумент35 страницOpen CholecystectomywqОценок пока нет
- 1 s2.0 S0022480423002895 MainДокумент7 страниц1 s2.0 S0022480423002895 Mainlucabarbato23Оценок пока нет
- Original Research ArticleДокумент9 страницOriginal Research ArticleAnand ShanmugaiahОценок пока нет
- Management strategies for intestinal obstruction and pseudo-obstructionДокумент13 страницManagement strategies for intestinal obstruction and pseudo-obstructionJeimy CarvajalОценок пока нет
- Capsula EndoscopicaДокумент4 страницыCapsula EndoscopicaYuu DenkiОценок пока нет
- Rouvieres Sulcus and Critical View of Safety A Guide To Prevent Bile Duct Injury During Laparoscopic CholecystectomyДокумент4 страницыRouvieres Sulcus and Critical View of Safety A Guide To Prevent Bile Duct Injury During Laparoscopic CholecystectomyeviltohuntОценок пока нет
- Iatrogenic Injury To The Common Bile Duct: Case ReportДокумент3 страницыIatrogenic Injury To The Common Bile Duct: Case ReportGianfranco MuntoniОценок пока нет
- Jurnal AppendicitisДокумент10 страницJurnal AppendicitisEwoJatmikoОценок пока нет
- B - Bile Duct Injuries in The Era of Laparoscopic Cholecystectomies - 2010Документ16 страницB - Bile Duct Injuries in The Era of Laparoscopic Cholecystectomies - 2010Battousaih1Оценок пока нет
- Case Report of Recurrent Acute Appendicitis in AДокумент2 страницыCase Report of Recurrent Acute Appendicitis in AGarryОценок пока нет
- Cutaneous Needle Aspirations in Liver DiseaseДокумент6 страницCutaneous Needle Aspirations in Liver DiseaseRhian BrimbleОценок пока нет
- Cholelithiasis With Choledocholithiasis: Epidemiological, Clinical ProfileДокумент3 страницыCholelithiasis With Choledocholithiasis: Epidemiological, Clinical ProfileShashank KumarОценок пока нет
- Case Report: Cholecystomegaly: A Case Report and Review of The LiteratureДокумент5 страницCase Report: Cholecystomegaly: A Case Report and Review of The LiteratureAnti TjahyaОценок пока нет
- Ogilvie Syndrome After Emergency Cesarean Section: A Case ReportДокумент4 страницыOgilvie Syndrome After Emergency Cesarean Section: A Case ReportIJAR JOURNALОценок пока нет
- Anatomy. Eight Edition. Saint Louis: Mosby.: Ped PDFДокумент10 страницAnatomy. Eight Edition. Saint Louis: Mosby.: Ped PDFannisa ussalihahОценок пока нет
- 1-s2.0-S2667008923000253-mainДокумент4 страницы1-s2.0-S2667008923000253-mainal malikОценок пока нет
- Notes Clinicalreview PDFДокумент8 страницNotes Clinicalreview PDFLuthie SinghОценок пока нет
- 1 s2.0 S0016510711024308 MainДокумент6 страниц1 s2.0 S0016510711024308 Mainpainkiller78Оценок пока нет
- Case Report of Recurrent Acute Appendicitis in AДокумент2 страницыCase Report of Recurrent Acute Appendicitis in Anita alisyahbanaОценок пока нет
- Todani IVДокумент3 страницыTodani IVJoshua Patrick MuljadiОценок пока нет
- Review StrikturДокумент13 страницReview StrikturFryda 'buona' YantiОценок пока нет
- Laparoscopy in The Acute AbdomenДокумент15 страницLaparoscopy in The Acute AbdomenDragoiu AlexandraОценок пока нет
- 2015 Laparoscopic Surgery in Abdominal Trauma A Single Center Review of A 7-Year ExperienceДокумент7 страниц2015 Laparoscopic Surgery in Abdominal Trauma A Single Center Review of A 7-Year ExperiencejohnnhekoОценок пока нет
- Role of Open Surgical Drainage or Aspiration in Management of Amoebic Liver AbscessДокумент9 страницRole of Open Surgical Drainage or Aspiration in Management of Amoebic Liver AbscessIJAR JOURNALОценок пока нет
- Minimally Invasive SurgeryДокумент6 страницMinimally Invasive SurgerycarmenОценок пока нет
- 9 Management of Common Bile-Duct Stones and Associated Gallbladder Stones: Surgical AspectsДокумент14 страниц9 Management of Common Bile-Duct Stones and Associated Gallbladder Stones: Surgical AspectsekoОценок пока нет
- Ostomia Intestinal PDFДокумент7 страницOstomia Intestinal PDFDaniela Pérez LópezОценок пока нет
- Gall Bladder Stones Surgical Treatment by Dr. Mohan SVSДокумент5 страницGall Bladder Stones Surgical Treatment by Dr. Mohan SVSFikri AlfarisyiОценок пока нет
- Laparoscopic Appendectomy For Complicated Appendicitis - An Evaluation of Postoperative Factors.Документ5 страницLaparoscopic Appendectomy For Complicated Appendicitis - An Evaluation of Postoperative Factors.Juan Carlos SantamariaОценок пока нет
- TMP CD3Документ4 страницыTMP CD3FrontiersОценок пока нет
- Surgical ArticleДокумент8 страницSurgical ArticleKevin Leo Lucero AragonesОценок пока нет
- Postoperative Fistula PancreaticДокумент7 страницPostoperative Fistula PancreaticstonmanОценок пока нет
- Laparoscopic Appendectomy PostoperativeДокумент6 страницLaparoscopic Appendectomy PostoperativeDamal An NasherОценок пока нет
- Risk factors for carcinogenesis in choledochal cyst patientsF/491Gender/AgeTodanitypeTable 1. Clinical characteristics of 15 patients with malignant tumors arising from choledochal cystsДокумент8 страницRisk factors for carcinogenesis in choledochal cyst patientsF/491Gender/AgeTodanitypeTable 1. Clinical characteristics of 15 patients with malignant tumors arising from choledochal cystsDaphne Ongbit JaritoОценок пока нет
- Hepatic Subcapsular BIloma A Rare Complication of Laparoscopic CholecystectomyДокумент4 страницыHepatic Subcapsular BIloma A Rare Complication of Laparoscopic CholecystectomyIndra PrimaОценок пока нет
- Pattern of Acute Intestinal Obstruction: Is There A Change in The Underlying Etiology?Документ4 страницыPattern of Acute Intestinal Obstruction: Is There A Change in The Underlying Etiology?neildamiОценок пока нет
- IMU Learning Outcome: Psychomotor SkillsДокумент11 страницIMU Learning Outcome: Psychomotor SkillsRameshОценок пока нет
- Infected Meckels Diverticulum Masquerading As Spontaneous Rupture of Umbilical Granuloma - A Case Report in One Month Old InfantДокумент4 страницыInfected Meckels Diverticulum Masquerading As Spontaneous Rupture of Umbilical Granuloma - A Case Report in One Month Old InfantIJAR JOURNALОценок пока нет
- Jurnal 3Документ3 страницыJurnal 3Ega Gumilang SugiartoОценок пока нет
- Tube IleostomyДокумент5 страницTube IleostomyabhishekbmcОценок пока нет
- Laparoscopic Appendicectomy in Appendicular LumpДокумент2 страницыLaparoscopic Appendicectomy in Appendicular LumpinventionjournalsОценок пока нет
- An Unusual Cystic Pancreatic MassДокумент7 страницAn Unusual Cystic Pancreatic MassIJAR JOURNALОценок пока нет
- 10.1007@s11605 018 04090 ZДокумент11 страниц10.1007@s11605 018 04090 ZGabriel RangelОценок пока нет
- Capsule Endoscopy GuideДокумент25 страницCapsule Endoscopy GuideAnonymous Z3sU48Оценок пока нет
- Complicationsoflapmyomectomy ANZ 2010Документ7 страницComplicationsoflapmyomectomy ANZ 2010Nadila 01Оценок пока нет
- Repair of Bowel Perforation Endoscopic State of The ArtДокумент6 страницRepair of Bowel Perforation Endoscopic State of The ArtAthenaeum Scientific PublishersОценок пока нет
- Gastritis 2014 HistopathologyДокумент11 страницGastritis 2014 HistopathologyMerly Espinoza RivasОценок пока нет
- Management of Iatrogenic Colorectal Perforation: From Surgery To EndosДокумент6 страницManagement of Iatrogenic Colorectal Perforation: From Surgery To EndosDiego CadenaОценок пока нет
- Article 1615981002 PDFДокумент3 страницыArticle 1615981002 PDFMaria Lyn Ocariza ArandiaОценок пока нет
- JMinAccessSurg114223-7427737 203757Документ8 страницJMinAccessSurg114223-7427737 203757Jonas De Oliveira MenescalОценок пока нет
- Emerging Endoscopic Treatments For Nonvariceal Upper Gastrointestinal HemorrhageДокумент14 страницEmerging Endoscopic Treatments For Nonvariceal Upper Gastrointestinal HemorrhageIsais NОценок пока нет
- Clinical Spotlight Review - Intraoperative Cholangiography - A SAGES PublicationДокумент19 страницClinical Spotlight Review - Intraoperative Cholangiography - A SAGES PublicationMu TelaОценок пока нет
- Chronic Empyaema Gall BladderДокумент2 страницыChronic Empyaema Gall BladderSuresh Kalyanasundar (Professor)Оценок пока нет
- Laparoscopic Cholecystectomy:An Experience of 200 Cases: Original ArticleДокумент4 страницыLaparoscopic Cholecystectomy:An Experience of 200 Cases: Original ArticleAndrei GheorghitaОценок пока нет
- Surgical Endoscopy Apr1998Документ95 страницSurgical Endoscopy Apr1998Saibo BoldsaikhanОценок пока нет
- Post-cholecystectomy Bile Duct InjuryОт EverandPost-cholecystectomy Bile Duct InjuryVinay K. KapoorОценок пока нет
- Colitis: A Practical Approach to Colon and Ileum Biopsy InterpretationОт EverandColitis: A Practical Approach to Colon and Ileum Biopsy InterpretationAnne Jouret-MourinОценок пока нет
- Attitude and Perceptions of University Students in Zimbabwe Towards HomosexualityДокумент5 страницAttitude and Perceptions of University Students in Zimbabwe Towards HomosexualityInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Topic: Using Wiki To Improve Students' Academic Writing in English Collaboratively: A Case Study On Undergraduate Students in BangladeshДокумент7 страницTopic: Using Wiki To Improve Students' Academic Writing in English Collaboratively: A Case Study On Undergraduate Students in BangladeshInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Socio-Ethical Impact of Turkish Dramas On Educated Females of Gujranwala-PakistanДокумент7 страницSocio-Ethical Impact of Turkish Dramas On Educated Females of Gujranwala-PakistanInternational Organization of Scientific Research (IOSR)Оценок пока нет
- "I Am Not Gay Says A Gay Christian." A Qualitative Study On Beliefs and Prejudices of Christians Towards Homosexuality in ZimbabweДокумент5 страниц"I Am Not Gay Says A Gay Christian." A Qualitative Study On Beliefs and Prejudices of Christians Towards Homosexuality in ZimbabweInternational Organization of Scientific Research (IOSR)Оценок пока нет
- The Lute Against Doping in SportДокумент5 страницThe Lute Against Doping in SportInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Comparative Visual Analysis of Symbolic and Illegible Indus Valley Script With Other LanguagesДокумент7 страницComparative Visual Analysis of Symbolic and Illegible Indus Valley Script With Other LanguagesInternational Organization of Scientific Research (IOSR)Оценок пока нет
- A Proposed Framework On Working With Parents of Children With Special Needs in SingaporeДокумент7 страницA Proposed Framework On Working With Parents of Children With Special Needs in SingaporeInternational Organization of Scientific Research (IOSR)Оценок пока нет
- The Role of Extrovert and Introvert Personality in Second Language AcquisitionДокумент6 страницThe Role of Extrovert and Introvert Personality in Second Language AcquisitionInternational Organization of Scientific Research (IOSR)Оценок пока нет
- A Review of Rural Local Government System in Zimbabwe From 1980 To 2014Документ15 страницA Review of Rural Local Government System in Zimbabwe From 1980 To 2014International Organization of Scientific Research (IOSR)Оценок пока нет
- An Evaluation of Lowell's Poem "The Quaker Graveyard in Nantucket" As A Pastoral ElegyДокумент14 страницAn Evaluation of Lowell's Poem "The Quaker Graveyard in Nantucket" As A Pastoral ElegyInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Assessment of The Implementation of Federal Character in Nigeria.Документ5 страницAssessment of The Implementation of Federal Character in Nigeria.International Organization of Scientific Research (IOSR)Оценок пока нет
- Investigation of Unbelief and Faith in The Islam According To The Statement, Mr. Ahmed MoftizadehДокумент4 страницыInvestigation of Unbelief and Faith in The Islam According To The Statement, Mr. Ahmed MoftizadehInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Edward Albee and His Mother Characters: An Analysis of Selected PlaysДокумент5 страницEdward Albee and His Mother Characters: An Analysis of Selected PlaysInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Relationship Between Social Support and Self-Esteem of Adolescent GirlsДокумент5 страницRelationship Between Social Support and Self-Esteem of Adolescent GirlsInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Transforming People's Livelihoods Through Land Reform in A1 Resettlement Areas in Goromonzi District in ZimbabweДокумент9 страницTransforming People's Livelihoods Through Land Reform in A1 Resettlement Areas in Goromonzi District in ZimbabweInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Importance of Mass Media in Communicating Health Messages: An AnalysisДокумент6 страницImportance of Mass Media in Communicating Health Messages: An AnalysisInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Substance Use and Abuse Among Offenders Under Probation Supervision in Limuru Probation Station, KenyaДокумент11 страницSubstance Use and Abuse Among Offenders Under Probation Supervision in Limuru Probation Station, KenyaInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Women Empowerment Through Open and Distance Learning in ZimbabweДокумент8 страницWomen Empowerment Through Open and Distance Learning in ZimbabweInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Role of Madarsa Education in Empowerment of Muslims in IndiaДокумент6 страницRole of Madarsa Education in Empowerment of Muslims in IndiaInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Beowulf: A Folktale and History of Anglo-Saxon Life and CivilizationДокумент3 страницыBeowulf: A Folktale and History of Anglo-Saxon Life and CivilizationInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Classical Malay's Anthropomorphemic Metaphors in Essay of Hikajat AbdullahДокумент9 страницClassical Malay's Anthropomorphemic Metaphors in Essay of Hikajat AbdullahInternational Organization of Scientific Research (IOSR)Оценок пока нет
- An Exploration On The Relationship Among Learners' Autonomy, Language Learning Strategies and Big-Five Personality TraitsДокумент6 страницAn Exploration On The Relationship Among Learners' Autonomy, Language Learning Strategies and Big-Five Personality TraitsInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Designing of Indo-Western Garments Influenced From Different Indian Classical Dance CostumesДокумент5 страницDesigning of Indo-Western Garments Influenced From Different Indian Classical Dance CostumesIOSRjournalОценок пока нет
- Motivational Factors Influencing Littering in Harare's Central Business District (CBD), ZimbabweДокумент8 страницMotivational Factors Influencing Littering in Harare's Central Business District (CBD), ZimbabweInternational Organization of Scientific Research (IOSR)Оценок пока нет
- A Study On The Television Programmes Popularity Among Chennai Urban WomenДокумент7 страницA Study On The Television Programmes Popularity Among Chennai Urban WomenInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Micro Finance and Women - A Case Study of Villages Around Alibaug, District-Raigad, Maharashtra, IndiaДокумент3 страницыMicro Finance and Women - A Case Study of Villages Around Alibaug, District-Raigad, Maharashtra, IndiaInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Design Management, A Business Tools' Package of Corporate Organizations: Bangladesh ContextДокумент6 страницDesign Management, A Business Tools' Package of Corporate Organizations: Bangladesh ContextInternational Organization of Scientific Research (IOSR)Оценок пока нет
- ResearchSTEM 12Документ77 страницResearchSTEM 12JhanelОценок пока нет
- Drug in PregnancyДокумент5 страницDrug in PregnancyjokosudibyoОценок пока нет
- Graphic Health QuestionnaireДокумент5 страницGraphic Health QuestionnaireVincentОценок пока нет
- Multicontrol Level 2: Cat. No. Pack Name Packaging (Content)Документ2 страницыMulticontrol Level 2: Cat. No. Pack Name Packaging (Content)NonameОценок пока нет
- From Solidarity To Subsidiarity: The Nonprofit Sector in PolandДокумент43 страницыFrom Solidarity To Subsidiarity: The Nonprofit Sector in PolandKarimMonoОценок пока нет
- Atwwi "Virtual" Trading Room Reference Document November 2, 2020Документ4 страницыAtwwi "Virtual" Trading Room Reference Document November 2, 2020amisamiam2Оценок пока нет
- 116 Draft OilsДокумент233 страницы116 Draft OilsMarcela Paz Gutierrez UrbinaОценок пока нет
- EpididymitisДокумент8 страницEpididymitisShafira WidiaОценок пока нет
- Diabetes and Hearing Loss (Pamela Parker MD)Документ2 страницыDiabetes and Hearing Loss (Pamela Parker MD)Sartika Rizky HapsariОценок пока нет
- Functional Electrical StimulationДокумент11 страницFunctional Electrical StimulationMohd Khairul Ikhwan AhmadОценок пока нет
- Climate Change and National Security - Shakeel RamayДокумент43 страницыClimate Change and National Security - Shakeel RamayBashir AhmedОценок пока нет
- Nursing Audit ScheduleДокумент2 страницыNursing Audit ScheduleArvinjohn Gacutan0% (1)
- Sabrina Nelson Winters Op Ed - BHM 2024Документ2 страницыSabrina Nelson Winters Op Ed - BHM 2024Andrew WilsonОценок пока нет
- Moosa Amandio PDFДокумент12 страницMoosa Amandio PDFMussa AmândioОценок пока нет
- Saudi Board Exam - Surgery Questions from 2009 Exam (192/200Документ47 страницSaudi Board Exam - Surgery Questions from 2009 Exam (192/200Rahmah Shah Bahai100% (2)
- Advances and Limitations of in Vitro Embryo Production in Sheep and Goats, Menchaca Et Al., 2016Документ7 страницAdvances and Limitations of in Vitro Embryo Production in Sheep and Goats, Menchaca Et Al., 2016González Mendoza DamielОценок пока нет
- Herbal Toothpaste FactsДокумент26 страницHerbal Toothpaste Factsmahek_dhootОценок пока нет
- The Premier University in Zamboanga Del Norte: Jose Rizal Memorial State UniversityДокумент1 страницаThe Premier University in Zamboanga Del Norte: Jose Rizal Memorial State UniversityCHARLEES BRAVOОценок пока нет
- Statistics: Dr. Ebtisam El - HamalawyДокумент20 страницStatistics: Dr. Ebtisam El - Hamalawydruzair007Оценок пока нет
- Nurse Licensure Examination Review Center for Allied Professions (RCAPДокумент15 страницNurse Licensure Examination Review Center for Allied Professions (RCAPnikko0427Оценок пока нет
- From MaureenДокумент1 страницаFrom MaureenWKYC.comОценок пока нет
- Legal Aid ProjectДокумент5 страницLegal Aid ProjectUday singh cheemaОценок пока нет
- Neonatal LupusДокумент19 страницNeonatal Lupusyogeshraval368Оценок пока нет
- Sop Cleaning Rev 06 - 2018 Rev Baru (Repaired)Документ20 страницSop Cleaning Rev 06 - 2018 Rev Baru (Repaired)FajarRachmadiОценок пока нет
- Stok Benang Kamar OperasiДокумент5 страницStok Benang Kamar OperasirendyОценок пока нет
- Acyanotic Congenital Heart Disease: Pediatric Cardiology Division University of Sumatera UtaraДокумент40 страницAcyanotic Congenital Heart Disease: Pediatric Cardiology Division University of Sumatera UtaraHanda YaniОценок пока нет
- 1 s2.0 S2214785321052202 MainДокумент4 страницы1 s2.0 S2214785321052202 MainTusher Kumar SahaОценок пока нет