Академический Документы
Профессиональный Документы
Культура Документы
(OS 213) LEC 15 Pneumonia (B) - 1
Загружено:
Yavuz DanisОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
(OS 213) LEC 15 Pneumonia (B) - 1
Загружено:
Yavuz DanisАвторское право:
Доступные форматы
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
LEC 15: PNEUMONIA
Exam 2 | Dr. Regina Pascua-Berba| August 16, 2012
OUTLINE
I. Introduction
IV.
II. Pathophysiology
A.
Route of Infection
B.
Risk Factors
V.
C.
Etiology
D. Different Syndromes of
Pneumonia
III. Clinical Presentation of
VI.
Pneumonia
VII.
A. Commone Presentations
VIII.
B. Chest Examinations
IX.
Diagnostic Tools
A. Chest X-ray
B. Other Diagnostic Tests
Management
A.
Decisions
on
Management
B.
Empiric Treatment
Prevention
Cases
Important Lecture Points
Appendix
Objectives
o To understand the pathophysiology of pneumonia
o To differentiate the different syndromes, etiology, and
presentations of pneumonia
o To discuss the recommended diagnostic and treatment
management for CAP
Suggested readings
o Harrisons Principles of Internal Medicine
o Philippine CPG for CAP in Immunocompetent Adults 2010
(PSMID- Philippine Society for Microbiology and Infectious
Diseases has the guidelines)
o Infectious Diseases Society of America (IDSA) Guidelines
for Community-acquired Pneumonia 2007
Fig. 1. Economic Consequences: Disability
Adjusted Life Years
This trans is not complete because Dr. Berba has not
sent us the slides yet! Boo! But dont you worry! Thisi s
already meaty; well be serving the side dishes for higher
learning (aka additional stuff on CAP and HAP, figures of
radiologic pathologic findings, management accdg. to specific
age group, and cheat sheet on Initial Empirical Antibiotic
Therapy) through an appendix once we receive the slides.
Anyways, for the exam, Dr. Berba said to focus on risk
stratification (check out the Megatable and Summary).
I. INTRODUCTION
Pneumonia
Abnormal inflammatory condition of the lung
Lower respiratory tract infection
An infection of pulmonary parenchyma and alveolar
compartment
May be caused by various organisms
o Bacteria 70%
o Virus 10-20%
o Rarely parasites and fungi
Usually patients are ill enough to require immediate
attention
Not a single disease; not self-limiting: patients are
required to come in and be treated
Group of specific infections based on:
o Epidemiology
o Pathogenesis
o Clinical Presentation and Course
Identification of etiology is IMPORTANT!
Diagnosis directs therapy; from empiric to specific
anti-microbial regimen
Who are at Risk?
Different people can get pneumonia at various points
in their life (babies, elderly people, and even med
students! :S)
Those who are immunocompromised- leukemia, postchemotherapy, etc
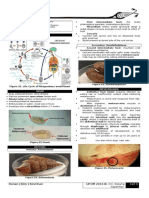
II. PATHOPHYSIOLOGY
A. Route of Infection
Microbes enter the lungs by:
1. Hematogenous spread (Least common: ~2%)
from an extrapulmonary site (distal to the lungs,
ex. Carbuncle)
Ex. Staphylococcus aureus in endocarditis
2. Spread from a contiguous focus of infection
(anything close to the lung parenchyma)
Spread of infection from mediastinum
Stab wound to the chest
Necrotic cancer in chest wall or lungs
3. Inhalation of aerosolized particles
Common pathway
Large particles more than 10 micrometer: dust,
most bacteria
Small airborne droplets less than 10 micrometer:
TB, virus (like Influenza), Histoplasma, and
Legionella
Efficient: one particle can be lodged onto alveoli
and initiate infection
4. Aspiration of oropharyngeal secretions
most common mechanism
Healthy individuals may carry some organisms in
their mouth, teeth, and gingival
Increase
w/
hospitalization,
worsening
disabilities, advanced age, alcoholism, and DM
Aspiration
during
sleep,
unconsciousness,
seizure, NGT
Impairment
in
fibronectin,
cough
reflex,
mucociliary function
Microbes travel down to lower respiratory tract
(alveolar sacs and parenchyma) deposition of
fibrinous material and pyrogenic cells, initiating
inflammatory response interruption in gas
exchange difficulty in breathing and increase in
secretions
Bacterial infection: neutrophils predominate
Viral infection: lymphocytes predominate
Burden of Illness
Major cause of hospitalization worldwide
Has significant health and economic consequences
In the Philippines:
o 3rd leading cause of morbidity (2001)
o 3rd leading cause of mortality (1998)
Worldwide, lung infection is the leading cause of
DALYs lost (2002)
Bobbie, Camille, Ginnie
UPCM 2016 B: XVI, Walang
Kapantay!
1 of 7
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
LEC 15: PNEUMONIA
Exam 2 | Dr. Regina Pascua-Berba| August 16, 2012
Fig. 2. Alveoli in Pneumonia. Normally, alveoli are
thin-walled. But here, there is thickened alveolar lining
with fibrinous materials, heavyily laden with
polymorphonuclear
cells
and
purulent
materials/exudates.
B. Risk Factors
The normal airway and lungs are equipped with
mechanisms to protect against infections. But there
may be events that could lead to the impairment of
these defense mechanisms.
Risk Factors:
o Structural disease of orophraynx
o Impaired cough reflexes (i.e. alcoholics)
o Impaired mucociliary transport (i.e. smokers)
o Immunocompromised states
Other Risk factors:
o Age > 65 yrs old
o Alcoholism- risk for aspiration, alcohol is generally
bad for the immune system
o Smoking- destroys the cough reflex mechanism
o Asplenia- lacks antibodies
o Malnutrition
o COPD
o Previous episode of pneumonia
o Chronic bronchitis*
o Bronchiectasis*
o Cystic fibrosis*
o Diabetes
o Immotile cilia syndrome*
o Anatomic obstruction of bronchus*
o AIDS
*Anatomic changes in respiratory system- will
accumulate secretions and tend to be directed towards
the evolution of pneumonia
C. Etiology
Determining etiology is important
empiric treatment
in
choosing
Table 1. Important Pathogens Causing
Pneumonia
Young
adult
healthy
Elderly
Streptococcus
pneumoniae,
Mycoplasma pneumoniae, virus,
TB
S. pneumoniae, Influenza
TB
Debilitated
S. pneumoniae, influenza, oral
flora, TB, Gram-negative bacilli
Hospitalized
Oral
flora,
Staphylococcus
aureus, Gram negative bacilli
Immunocompr
omised
Oral flora, Gram negative bacilli
*As patient becomes more and more immunocompromised,
the prominence of Gram-negative bacteria as etiology
increases
The severity of the disease (and therefore, the site of
care, see Table 2) would be dictated by the specific
organism that caused the pneumonia
Table 2. Microbial Causes of Community-Acquired
Pneumonia, by site of care (Hospitalized
Patients)
Outpatients
Non-ICU
ICU
Streptococcus
S. pneumoniae
S.
pneumoniae
M. pneumoniae
pneumonia
Mycoplasma
C. pneumoniae
e
pneumoniae
H. influenza
S. aureus
Haemophilus
Legionella spp.
Legionella
influzena
Respiratory
spp.
Chlamydia
Viruses
Gram(-)
pneumoniae
bacilli
Respiratory Viruses
H. influenza
*consider the characteristics of your patient and the agent
D. Different Syndromes of Pneumonia
Community-acquired VS Hospital-acquired
Involves different spectrum of etiologic agents
Requires different empiric therapy; dictates initial
management
Community-acquired Pneumonia (CAP)
o Acute infection of the pulmonary parenchyma that
is associated with at least some symptoms of
acute infection accompanied by the presence of an
acute infiltrate on a chest radiograph, or
auscultatory findings consistent with
pneumonia, in a patient not hospitalized or
residing in a long term care facility for >14 days
before onset of symptoms.
o Examples:
med student working in a hospital who gets
pneumonia is still considered as CAP since he/she
does not reside in the healthcare facility.
patient admitted for cardiac problems (heart
attack) in ICU
o Chest pain is because of inflammation that extends
to pleura
o Lots of fibrinous secretions that go up
o PE: decreased breath sounds, increased vocal
fremitus, dullness on percussion, crackles/rales
(can help localize the area affected), increased
whispered pectoriloquy, decrease movement on
tactile fremitus
Hospital-acquired Pneumonia
o aka Nosocomial pneumonia
o aka Healthcare-associated pneumonia
o caused by endemic flora of the hospital; usually
Gram (-) bacteria but depends on the type of
hospital
o 48 hours after admission (if before admission:
community-acquired, if after: hospital-acquired);
and not incubating at the time of admission
o VCAP-pneumonia which arises more than 48-72
hours after endotracheal incubation (V is for
ventilatory?)
o HCAP-pneumonia within 90 days after receiving
any form of health care
Chronic VS Acute
Acute Pneumonia
Bobbie, Camille, Ginnie
UPCM 2016 B: XVI, Walang
Kapantay!
2 of 7
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
LEC 15: PNEUMONIA
Exam 2 | Dr. Regina Pascua-Berba| August 16, 2012
Chronic Pneumonia- if >2 weeks
Typical VS Atypical
These are old terms
Pneumonia might present in different/atypical ways
Table 3. Typical vs. Atypical Pneumonia (A very
important table!)
Typical
Atypical
Sudden onset of fever
Gradual
onset
of
symptoms, often mild
Cough
with
purulent Dry cough
sputum- doesnt matter
what color
Shortness of breath
Shortness of breath
Pleuritic chest pain
Extrapulmonary
symptoms:
headache,
mylagia, fatigue, sore
throat, nausea, vomiting,
diarrhea
PE with consolidation Systemic response of
(dullness,
increased body
not
really
fremitus,
egophony, understood until now
decreased
bronchial Minimal signs on PE
breath sounds, rales)
Usually
caused
by Usually attributed to:
bacteria (Memorize!):
- Mycoplasma
- S. pneumoniae
pneumoniae
- H. influenza
- Chlamydophila
pneumoniae
- Moraxella catarrhalis
- Legionella spp.
III. CLINICAL PRESENTATION OF PNEUMONIA
A. Common (Typical) Presentations of Pneumonia
1.Cough: natural reflex to try to expel secretions
2.Fever: part of the inflammatory response
o Caused by interleukins
3.Chills: Kasabay po ba ng lagnat ay may panlalamig?
o Usually denotes bacterial or viral etiology
4.Chest Pain: caused by pleuritic pain
5.Difficulty in Breathing
o fluid-filled alveolar sacs inefficient for gas
exchange
o Indicative of the severity of pneumonia
o Can be measured by respiratory rate
6. Malaise
B. Chest Examination
Early on in disease a fine crepitant rales over the
involved portion of the lung(s)
Progression to lobar consolidation results in:
o Dullness to percussion due to secretions and fluid
in alveoli within the specific region in the lungs
being percussed
o Vocal fremitus
o Whispered pectoriloquy
o Bronchial breathing
Table 4. Different Ways to Diagnose Pneumonia
Decision
Basis
Physicians
Clinical
Judgment
Heckerlings
Score
(threshold 2)
Variable
s
History
PE
Temp > 37.8
Pulse >100
Rales
Bobbie, Camille, Ginnie
Gennis
Rule
(threshold
1)
Temp> 37.8
RR> 20
Accuracy
to Predict
Pneumon
ia
60-80%
Decreased BS
Absence of
asthma
68%
76%
IV. DIAGNOSTIC TOOLS
A. Chest Radiograph
Value of Chest Radiograph
For diagnostic certainty
Assess severity of disease and prognostication
Suggest possible etiology of pneumonia
Help differentiate pneumonia from other conditions:
Correct CXR
The following have to be considered to avoid
misinterpretations
o Rotation- centered/ equidistant based on trachea;
equal distance between medial end of clavicle and
midline of the chest X-ray
o Penetration affected by technique of radiology;
results might be mistaken for something else
o Inspiration/Expiration
o Remember your anatomy: (RUL, RML, RLL, LUL,
LLL)
Fig. 3. Normal Chest Radiograph. Clear lung
fields, normal shadow of pulmonary vascular
markings and cardiac silhouette
Radiographic Findings
Air Bronchogram- pathognomonic of pneumonia
o bronchial markings filled with gases, usually seen
to penetrate dense infiltrates (as seen in CXR), or
consolidation which indicates pneumonic process
(as see in CT)
o
in pneumonia w/o fluid, only inflammatory
response = fremitus is increased, sounds are
resonant, w/ crackles
Meniscus Sign
o When no air bronchograms are seen, this suggests
that lung is filled with fluid which forms a convexity
Hilar mass lesion
o No obvious infiltrates, but presents with fever and
cough
o Can already start treatment if clinically present
with pneumonia
o Use CT scan to rule out malignancy
Multiple masses
o Fungal pneumonia can present as multiple nodules
o work out if this is pneumonia or malignancy
RUL collapse
UPCM 2016 B: XVI, Walang
Kapantay!
3 of 7
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
LEC 15: PNEUMONIA
Exam 2 | Dr. Regina Pascua-Berba| August 16, 2012
o
o
o
o
Clearly defined margin showing that the right lung
is being pulled down
Other observations: no air bronchograms, traction
of midline structures
Due to atelectasis, brought about by blockage of
airway
decreased lung sounds, decreased fremitus
Cavitating lesion
o abscess/ TB cavity
o pneumonia can look initially as the usual infiltrates
and then necrotize and form a cavity
Millet seed - miliary TB (usually severe)miliary
shadowing
Conditions Mimicking Pneumonia on X-ray
Asthma or COPD
Congestive heart failure (could present with crackles)
Malignancy (primary lung or metastatic)
Collagen vascular disorders (e.g. SLE, scleroderma)
Pulmonary embolism
Sarcoidosis
Interstitial pneumonitis
Pyelonephritis
B. Other Diagnostic Tests
Sputum Gram strain and culture important!
Sputum AFB (Acid Fast Bacilli)
Induced sputum for PCP (Pneumocystis carinii)
Serology for other atypical pathogens
o Mycoplasma pneumoniae
o Chlamydophilapneumoniae
o Legionella pneumophila
Sputum Examination
Mainstay of evaluation of pneumonia
Can identify etiology in only 50-60% of cases
Good non-contaminated sputum
o Predominantly pus cells: PMN > 25/lpf (low power
field)
o Proportionately less epithelial cells: Epithelial cells
< 10/lpf
o With bacterial pathogens
o Observed in ~15 of cases studies
Inadequate sample usually contain only saliva (with
lots of epithelial cells > 25/lpf and no PMN)
It is important fo us to INSTRUCT the patient on how
to obtain appropriate sputum samples
o Hingang malalim 2 beses, umubo hanggang
makapagbigay ng magandang halak
Order gram stain and culture (Sputum GS/CS)
More invasive tests as needed
Important causative agent of community-acquired:
Streptococcus pneumonia (if
immunocompromised, Aspergillus and Candida)
Fig. 4.Streptococcus with many PMNs
(polymorphonuclear cells)
Table 5. Clinical indications for more extensive
diagnostic testing
Pneumoco
Othe
Indicati
Bloo
Sput
Legion
ccal
rs
on
d CS
um
ella
Antigen
CS
Antige
n
ICU
X
X
X
X
X
Failure of
X
X
X
OPD Rx
Cavitary
Infiltrates
Leukopen
ia
Active
Alcohol
Abuse
Chronic
severe
liver
disease
Severe
Structura
l
lung
disease
Asplenia
Recent
travel
(w/in
2
weeks)
Pleural
Effusion
X
X
X
X
X
X
V. MANAGEMENT
Cant always rely on culture results to be readily
available it takes 48 hours and unavailable in some
areas
NOTE: Decisions on Management and Empiric
Management based on risk stratification were
merged in one mega table! See last page
A. Decisions on Management
According to risk stratification (check Megatable!),
would have different mortality rates and site of care:
o CAP low risk
o CAP moderate risk
o CAP high risk
o HAP
o Other etiologies
Etiologic agents vary for different age groups
Scoring systems such as PORT and CURB-65 gave been
developed for the recommendation of site of care;
these are not usually used in the Philippines
Table 6. Pneumonia PORT Severity Index (PSI)
Patient Characteristic
Demographic factors
Age
Male (no. yrs)
Female (no. yrs. 10)
Nursing home resident
Comorbid Illness
Neoplastic disease
Liver disease
Congestive heart failure
Cerebrovascular disease
Renal disease
Physical examination findings
Altered mental status
Respiratory rate 30 breath/min
Bobbie, Camille, Ginnie
Points
Assigned
+10
+30
+20
+10
+10
+10
+20
+20
UPCM 2016 B: XVI, Walang
Kapantay!
4 of 7
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
LEC 15: PNEUMONIA
Exam 2 | Dr. Regina Pascua-Berba| August 16, 2012
Systolic blood pressure < 90 mm Hg
Temperature < 35 C
Pulse > 125 beats/min
Laboratory and/or radiographic
findings
Arterial pH < 7.35
Blood urea nitrogen 30mg/dL
Sodium < 130 mmol/L
Glucose > 250 mg/dL
Heamtocrit< 30%
Hypoxemia by O2 Saturation;
< 90% by pulse oximetry,
< 60 mm Hg by arterial blood gas
Pleural effusion on baseline
radiograph
B. Empirical Management
According to risk stratification and likely etiology
(check Megatable!)
+20
+15
+10
+30
+20
+20
+10
+10
Penicillin and/or drug resistant Streptococcus
pneumoniae
+10
+10
Table 7. Pneumonia PORT Severity Index (PSI)
Interpretations
Total Point Score (points for each applicable patient
characteristic)
Recommen
PSI
ded
Risk
Characteristic Points
Site of
Class
Care
I
Age < 50 yrs + no comorbid
Outpatient
conditions normal range vital
signs, normal mental status
II
70
Outpatient
III
71-90
Outpatient/
Brief
IV
91-130
Inpatient
V
>130
Inpatient
Inpatient
Age > 65
Beta-lactam therapy within the previous three
months
Alcoholism
Immune suppressive illness (including use of
corticosteroids)
Multiple medical comorbidities
Exposure to child in day care
True for US but in the Philippines, penicillin is still
effective (our S. pneumoniae is still sensitive to
penicillin, yey!)
Enteric gram-negatives
Moderate to severe types
Residents in nursing homes
Underlying cardiopulmonary disease
Multiple medical comorbidities
Recent antibiotic use
Pseudomonas aeruginosa
One of the deadliest, signifies bad prognosis
Difficult to treat (takes >2 weeks IV to completely
eradicate)
Table 8.CURB 65 Severity Scores for CAP
Clinical Factors
Confusion
BUN < 19 mg/dL
Respiratory rate >/= 30 breaths/min
Systolic BP < 90 mmHg or Diastolic BP > 60
mmHg
Age > 65 years
Total
Point
s
1
1
1
1
1
5
Table 9. CURB 65 Severity Scores for CAP
Interpretation
CURB
Score
0
1
2
Death
s (%)
0.6
2.7
6.3
3
4 or 5
14.0
27.8
Recommendations
Low risk; consider home treatment
Low risk; consider home treatment
Short
inpatient
hospitalization
or
closely
supervised
outpatient
treatment
Moderate risk; inpatient care
Severe pneumonia; consider intensive
care
Criteria for Severe Community-Acquired
Pneumonia
Minor Criteria (abnormal values for tests)
o Respiratory rate > or = 30 breaths per min
o PaO2/FiO2 < 250
o Multilobar infiltrates
o Confusion, disorientation
o Uremia (BUN level > 20 mg/dl)
o Leukopenia (WBC count < 4,000 cells/mm)
o Thrombocytopenia (platelet count < 100,000
cells/mm2)
o Hypothermia (core temperature < 36 C)
o Hypotension requiring aggressive fluid
resuscitation
Major Criteria
o Invasive mechanical ventilation
o Septic shock with the need for vasopressin
Bobbie, Camille, Ginnie
Who are at risk for Pseudomonas? (EXAM
QUESTION)
o History of prolonged antibiotic use (> 7 days)
Broad-spectrum antibiotics (>7 days w/in last
month)
o Chronic lung disease
COPD, bronchiecstasis, cystic fibrosis
o Malnutrition
o Use of steroids
Corticosteriod therapy (>10 mg Prednisone
daily)
VI. PREVENTION
1. Smoking cessation
2. Pneumococcal vaccine
o For > 60 years old in the Philippines
o Once every five years
o Those with certain chronic illnesses
Diabetes, Congestive Heart Failure, Chronic
Liver Disease, COPD, Chronic Renal Disease,
asplenia (reduction in antibodies)
o Those with immunocompromised states
o Residents of nursing homes and other long term
facilities
o Smokers and asthmatic persons 19-64 years old
o The pneumonia shot protects against 23
serotypes of pneumococcus (there are 100
serotype)
o Not 100% effective in prevention but decreases
chances of mortality
3. Influenza vaccine
o For > 50 years
o Yearly, even if not viral pneumonia, since
pneumonia can be superimposed on flu
o Those with chronic illnesses and
immunocompromised states
o Pregnant in 2nd and 3rd trimester
o Residents of nursing homes
UPCM 2016 B: XVI, Walang
Kapantay!
5 of 7
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
LEC 15: PNEUMONIA
Exam 2 | Dr. Regina Pascua-Berba| August 16, 2012
o Healthcare workers
o Household contacts and caregivers of persons w/
medical conditions and children <5 years or
adults >50 years
o Basically, EVERYONE
4.
Infection Control prevents transmission of
pneumonia
o Hand hygiene/handwashing
o Isolation of sick patients
o Proper suctioning
o Wearing of masks more cost effective if patients
will be the ones to wear masks
o Respiratory etiquette
VII. CASES
Case 1: y/o male, SM employee, non-smoker
Chief complaint: cough and fever
PE: crackles at Right base, decreased breath sounds
2 day history of high fever with chills and yellow
phlegm
Vital signs: 120/70, 39.8, RR 36, HR 110
Diagnosis: Low to Moderate risk CAP (right
middle lobe)
Management: Admit to ward, IV with penicillinase, 2nd
generation cephalosporin/ cefuroxime
Case 2: 68/M
Chief complaint: fever and cough
Greenish phlegm, 30 pack-years
Diagnosis: High Risk pneumonia (Strep, Varicella
catarrhalis, pseudomonas)
Expected PE: rales, crakles, whispered pectoriloquy,
lag (tactile fremitus), consolidation (which would
increase fremitus) or if liquid, decrease fremitus),
diffuse wheezing (smoker)
Management: admit to ward
Case 3: 40/M unresponsive, smells of mixed
alcohol and vomitus
Diagnosis: possible aspiration, high risk CAP
(hemodynamic compromise), Pseudomonas
Management: intubate/ ICU
Intubate because multilobar, almost all lung fields
Case 4: 28/F pregnant 32 weeks AOG, required
intubation
Reticular patterns, diffused crackles, incessant
coughs
Viral (otherwise young)
Diagnosis: high risk CAP
Management: ICU, Pseudomonas antibiotics, AVOID
using quinolones (teratogenic)
Sputum G/S, nasopharyngeal swab
This is a case where the patient missed her influenza
shot before the pregnancy; bacterial pneumonia was
superimposed on top of influenza
Case 5: 28/M
Chief complaint: fever, shortness of breath
Discharged 3 weeks for moderate CAP with
Cefuroxime
Bobbie, Camille, Ginnie
PE: clear lungs, tachycardic, chest XRay normal, CBC
normal
What tests to order (and their resuts)?
o Sputum (normal)
o ABG (slightly decreased)
o But Pneumocystis was identified
Diagnosis: PCP
Management: get ABG: hypoxemic (pO2: Normal=
80-100)
In PCP, patients could be very ill yet with atypical
manifestations.
VIII. IMPORTANT LECTURE POINTS
Pneumonia is a frequently seen illness and all
physicians must be familiar with its diagnosis and
management
Diagnosis by good history and PE, chest X-ray, and
sputum test
Risk stratification will guide management
Prevention for those at risk
Different etiologies depending on risk stratification so
empiric therapy/drug of choice at presentation also
varies
Table 10. Drug of choice for CAP type
Clinical situation
Drug of choice
Low risk CAP
Amoxicillin
No comorbidities
Low risk CAP
Extended macrolides
Suspecting
atypical
pathogens
Low risk CAP
Amoxicillin
clavulanic
Stable comorbidities
acid
(ex.
Controlled
DM, Amoxicillin sulbactam
asthmatic but with no Sultamicillin
attack in the last 10 years, Cefaclor
etc)
Cefuroxime
+/- extended macrolide
Moderate risk CAP
Beta-lactam
Cephalosporin
Ertapenem
+
macrolide
or
respiratory quinolone
High risk CAP
Ceftriaxone
or
No Pseudodomonas risk
Ertapenem
+
Macrolide
or
Respiratory quinolone
High risk CAP
Piperacillin-tazo
With Pseudomonas risk
Ceftazidime
Carbapenem
END
Bobbie: Hello Millie and
Ginnie! Hello to all Block B
people! Im excited for
sembreak! And Christmas!!!
Camille: I love this week!
Ginnie: Delikado magka long
weekend. NAKAKATAMAD. Manood kayo ng Once Upon
A Time! Hihi. Hello TritiPwidi! Maligayang Buwan ng
Wika! Hi Millie and Bobbie! Hi Phil, just because. :P
Hello sa mga kalaro kong guess the movie! Haha.
UPCM 2016 B: XVI, Walang
Kapantay!
6 of 7
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
LEC 15: PNEUMONIA
Exam 2 | Dr. Regina Pascua-Berba| August 16, 2012
o
o
o
o
o
o
o
o
o
o
o
o
o
o
Bobbie, Camille, Ginnie
UPCM 2016 B: XVI, Walang
Kapantay!
7 of 7
Вам также может понравиться
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5795)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- USMLE Step 3 CCS NotesДокумент20 страницUSMLE Step 3 CCS Notesaustinhitz96% (26)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Infectious Disease Essentials HandbookДокумент157 страницInfectious Disease Essentials HandbookCalin Popa100% (3)
- Gyane MCQS 6, 7, 9 Chapter Irfan Masood PDFДокумент16 страницGyane MCQS 6, 7, 9 Chapter Irfan Masood PDFJansher Ali Chohan100% (1)
- IARC Coffee Carcinogenic StudyДокумент512 страницIARC Coffee Carcinogenic StudyEater100% (1)
- Reiki Level Two ManualДокумент34 страницыReiki Level Two ManualSoumya PandeyОценок пока нет
- Radiology 1Документ4 страницыRadiology 1sha100% (3)
- Rubrics For Children in MurphyДокумент18 страницRubrics For Children in MurphyVirag PatilОценок пока нет
- Clinical Trials and BiostatisticsДокумент16 страницClinical Trials and BiostatisticsArumugam RamasamyОценок пока нет
- ResearchДокумент26 страницResearchJhen de Vera83% (12)
- Skippers United Pacific, Inc. vs. Lagne DigestДокумент4 страницыSkippers United Pacific, Inc. vs. Lagne DigestEmir MendozaОценок пока нет
- A Durable Ultrasound Phantom For Trainees Using Common MaterialsДокумент7 страницA Durable Ultrasound Phantom For Trainees Using Common MaterialsYavuz DanisОценок пока нет
- 2016 May - NCДокумент36 страниц2016 May - NCYavuz DanisОценок пока нет
- Radio 25 E1 Lec 10 MSK RadiologyДокумент3 страницыRadio 25 E1 Lec 10 MSK RadiologyYavuz DanisОценок пока нет
- 5 Medicine OSCE Collection: By: Fatimah Al-IbrahimДокумент69 страниц5 Medicine OSCE Collection: By: Fatimah Al-IbrahimJim JordenОценок пока нет
- (OS 213) LEC 03 Drugs Acting On The Respiratory System (1) - 1Документ16 страниц(OS 213) LEC 03 Drugs Acting On The Respiratory System (1) - 1Yavuz DanisОценок пока нет
- (OS 213) LAB 03 Paragonimus Westermani (A)Документ3 страницы(OS 213) LAB 03 Paragonimus Westermani (A)Yavuz DanisОценок пока нет
- (OS 213) LEC36 CVS Course SummaryДокумент12 страниц(OS 213) LEC36 CVS Course SummaryYavuz DanisОценок пока нет
- (Os 213) Pictotrans Ws 02 - Ecg Skills Enhancement (A)Документ16 страниц(Os 213) Pictotrans Ws 02 - Ecg Skills Enhancement (A)Yavuz DanisОценок пока нет
- Cutaneous Adverse Drug ReactionsДокумент5 страницCutaneous Adverse Drug ReactionsEpi PanjaitanОценок пока нет
- Essential Oils Phytochemicals Used For Treatment MRSA Diabetic Foot TBДокумент23 страницыEssential Oils Phytochemicals Used For Treatment MRSA Diabetic Foot TBSurgicalgownОценок пока нет
- Professional Nursing OrganizationsДокумент6 страницProfessional Nursing OrganizationsJohn Askof NyabutiОценок пока нет
- Maternal and Child Health Nursing, 8 Edition.: LESSON PREVIEW/REVIEW (5 Minutes)Документ7 страницMaternal and Child Health Nursing, 8 Edition.: LESSON PREVIEW/REVIEW (5 Minutes)raker boiОценок пока нет
- Chapter 09Документ66 страницChapter 09moeОценок пока нет
- Sarcoma Surveillance A Review of Current Evidence.2Документ12 страницSarcoma Surveillance A Review of Current Evidence.2Fernanda Lorena AcevesОценок пока нет
- Hepatitis BДокумент23 страницыHepatitis BAbraham RumayaraОценок пока нет
- NASC 4 Fact or BluffДокумент33 страницыNASC 4 Fact or BluffJona MangabanОценок пока нет
- Soal Bahasa InggrisДокумент23 страницыSoal Bahasa InggrisAnonymous C4tZ8wОценок пока нет
- Matary Appendix Summary01Документ4 страницыMatary Appendix Summary01Muhammad GoharОценок пока нет
- State of Health in The EU Cycle, OECD PublishingДокумент204 страницыState of Health in The EU Cycle, OECD PublishingJasmin Džaja DurmiševićОценок пока нет
- PHD ProposalДокумент21 страницаPHD ProposalHAIMANOTОценок пока нет
- Cold Agglutinin DiseaseДокумент8 страницCold Agglutinin Diseasehtunnm@gmail.comОценок пока нет
- Monitoring and Evaluation of Health Services: Dr. Rasha SalamaДокумент52 страницыMonitoring and Evaluation of Health Services: Dr. Rasha SalamaLibyaFlowerОценок пока нет
- Doctor Jarir Nakouzi Has Researched Clinical Oncology As A Doctor Procedure of Illness For Over 25 YearsДокумент2 страницыDoctor Jarir Nakouzi Has Researched Clinical Oncology As A Doctor Procedure of Illness For Over 25 Yearsgrowth0roomОценок пока нет
- Imaging and RadiologyДокумент7 страницImaging and RadiologyOdyОценок пока нет
- Prophylactic MastectomyДокумент5 страницProphylactic MastectomyMuhammad Darussalam DarwisОценок пока нет
- GRP2Документ87 страницGRP2Veronica ChanОценок пока нет
- Handout 2 1522436248 PDFДокумент82 страницыHandout 2 1522436248 PDFHarnadi WonogiriОценок пока нет
- Visual Inspection With Acetic Acid (VIA) : Evidence To DateДокумент16 страницVisual Inspection With Acetic Acid (VIA) : Evidence To DateruntunОценок пока нет