Академический Документы
Профессиональный Документы
Культура Документы
OMFS 3 Quizlet
Загружено:
okibreazyАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
OMFS 3 Quizlet
Загружено:
okibreazyАвторское право:
Доступные форматы
Oral Surgery Exam 3
Study online at quizlet.com/_1kh8bz
ATLS primary
survey includes
which five factors?
Airway, Breathing, Circulation,
Disability, Environment (ABCDE)
19.
avulsed teeth
tooth is completely out of the mouth
20.
five factors for
reimplanting
avulsed teeth
no perio ds, socket intact, ortho
contraindications, root development
should be evaluated (open is better), 2
hours in the external envt before its
useless
2.
battle's sign
bruising behind the ear right over the
mastoid, need a CT to rule out back of
skull fracture
3.
Marcus Gunn pupil
during a swinging light test, the affected
side and the contralateral side will dilate
instead of constrict when light is shown
on them
21.
length of time
since avulsion
injury
<20 mins-rinse and reimplant
>20 mins-HBBS for 30mins, then doxy for
5mins then reimplant
>2hrs-do not reimplant
4.
why are septal
hematomas
dangerous?
the nasal cartilage is avascular, so a
hematoma can cause necrosis of the
cartilage along with the normal fullness
symptoms
22.
how long do we
stabilize a wide
apex avulsed
tooth?
2-3weeks with penicillin
5.
abrasion
frictional injury, epithelium but
sometimes deeper layers, minimal
bleeding, painful due to nerve endings
23.
7-10days
6.
contusion
subcutaneous/submucosal
hemorrhage, no soft tissue break, blunt
trauma, no need for antibiotics due to
containment (unless contusion
secondary to dentoalveolar trauma)
how long do we
stabilize an
adult closed
apex avulsed
tooth?
24.
alveolar process
fracture
tear in (sub)epithelial tissue usually
from a sharp object, treat hard tissue
first
reduce segment, splint segment (at least
4wks), if root apices are denuded w/in the
fracture we should do endo within 1-2wks
to prevent resorption
25.
bone healing by
primary
intention
bone segments need to be less than or
equal to 1mm from eachother
26.
bone healing by
secondary
intention
bone segments are greater than 1mm
apart from each other
27.
fibroblastic
stage of bone
healing
osteocellular differentiation, capillary
budding, collageln laid down, fibrous
matrix, callus forms, need
oxygenation/nonmobility (or else cartilage
forms)
28.
remodeling
stage of bone
healing
removal of unnecessary bone and laying
down of new bone, haversian system,
callus shrinks
1.
7.
laceration
where do we put
the first suture on
a full thickness lip
laceration?
at the vermilion border, this way we
know that this part will match, work
form the inside out, three layered
closure
9.
degloving
shearing forces that causes a flap of
tissue
10.
avulsion
tissue ends up missing, animal
bites/blast injury for example
11.
crown crack
limited to the enamel, no treatment
needed except for esthetics, recalls for
pulpal diagnosis
horizontal/vertical
crown fracture
depth is key, pulp checking often
should be done
29.
crown-root
fracture
location of fracture determines
treatment
greenstick
fracture
incomplete fracture, usual children, less
mobility
30.
simple fracture
complete but minimal frature
14.
horizontal root
treatment
the more apical the better the prognosis
(middle-apical third)
31.
comminuted
fracture
multiple segmented fracture
15.
subluxations
intrusion, extrusion
32.
orthodontically erupt it or let it erupt
passively, if primary then extract
fractures that communicate with the
external environment
16.
tx of intrusion
compound
fracture
33.
tx of extrusion
manually seat it back in, splint for a
couple weeks and then endo
muscle function will actually reduce the
fracture, aka reducing the fracture
17.
favorable
mandibular
fracture
18.
displaced teeth
manually reposition tooth and alveolus,
usually a ledge you need to get it over
8.
12.
13.
34.
unfavorable
mandibular fracture
muscle function will actually displace
the fracture
35.
mandibular
fractures usually
come in pairs, where
are the most
common locations?
angle of the mandible and
contralateral subcondylar area
closed reduction
fracture fixation
more favorable, reducing blindly
(casting an arm), in the mandible we
put them into occlusion and wire the
jaws shut, can do this under LA
open reduction
fracture fixation
requires seeing the fracture (incision),
done if mandible is extremely
comminuted or has condition
preventing intermaxillary fixation
(seizures, vomitous)
36.
37.
38.
39.
40.
41.
42.
43.
period of immobility
for closed reduction
of fracture fixation
elderly-5+ weeks
adults-4-6wks
children-2wks
disadvantage to
closed reduction
longer IMF time, patient
noncompliance, altered diet, hygiene,
CI'd in patients with concomitant
conditions (Seizures, sleep apnea, etc)
vestibular approach
for an open
reduction
from symphysis to angle we can incise
through the vestibule, careful of the
mental nerve
submandibular
approach for an
open reduction
parasymphisis to angle of the
mandible, can directly see the
fracture, easier angulation, can
damage the IAN and CNVII, can scar
retromandibular
approach for an
open reduction
angle to subcondyle, direct vision,
easier angulation, difficult dissection,
can damage CNVII or
retromandibular vein
preauricular
approach for an
open reduction
accesses TMJ, condyle, and condylar
neck, best visualization of higher
structures but much higher chance of
dissectiong CNVII
rigid fixation of the
mandible
bone does not move, lag screws (two
screws), two plates, or one large plate,
can be done on unfavorable
fractures
45.
functionally stable
fixation of the
mandible
one miniplate, used for minimal
displacement and put on spots of
tension (usually on top), requires
favorable fractures
46.
vertical stress
bearing areas of the
face
zygomaticomaxillary, nasomaxillary,
pterygomaxillary
44.
47.
horizontal stress
bearing areas of
the face
zygomatic, frontal, maxillary
48.
what fracture
must be present
in order for it to
be a le fort
fracture?
pterygoid plates must be fractured
49.
Le Fort I
least complicated, lateral antral and nasal
walls with lower 1/3 of septum, pterygoid
plates
50.
Le Fort II
nasal and maxillary bone, palatine
bones, lower 2/3 of septum,
dentoalveolus, pterygoid plates
51.
Le Fort III
nasal bones, zygoma, maxilla, plataline,
pterygoid plates, essentially seaparates
face form base of skull
52.
access to Le Fort I
through the maxillary vestibule
53.
access to Le Fort
II
could be vestibular,
transcutaneous/transconjuncitval, or
coronal (for comminuted)
54.
access to Le Fort
III
requires coronal approach
55.
what is the most
common orbital
fracture site?
inferior and medial (medial orbital wall)
56.
emergencies
around the eye
inferior rectus entrapment (can necrose
due to lack of blood, CNV cardiac reflex
(pushing on trigem slows HR) can also
happen), loss of vision, retrobulbar
hematoma
57.
what can happen
from a zygomatic
arch fracture?
trisumus due to coronoid impingement,
approached via Gilles or Keens approach
58.
gilles approach
access to zygomatic arch through
temporal incision
59.
Keens approach
access to zygomatic arch through
intraoral incision
60.
traumatic
telecanthus
drifting apart of the eys due to nasoorbital fracture
61.
what are the two
most common
locations of oral
cancer?
lateral border of the tongue
floor of the mouth
62.
which three
characteristics of
lesions raise the
suspicion of
malignancy?
erythroplakia, leukoplakia, and
leukoerythroplakia
63.
how many
days until we
absolutely
need to
biopsy an
ulcer?
2wks (15days)
76.
two types of
cysts we think
about in the oral
cavity
1) those arising from odontogenic
epithelium
2) those from oral epithelium that is
trapped between fusing processes during
embryogenesis
usually asymptomatic
64.
aspiration
biopsy
needle penetrates lesion and grabs a piece
but no specific diagnosis can be given, can
only show malignancy
77.
enucleation
65.
cytology
biopsy
oral brush or aspirational, no specific
diagnosis can be given, can only show
malignancy
taking the cyst lining out only, attempt to
remove cyst in one piece (without
rupture, shelling out), good for low
recurrence and low chance for anatomical
risk
78.
marsupialization
creating a surgical window on the wall of a
cyst so it can continually drain, only
portion removed is the segment removed
for the window, decreased cystic pressure
and increases shrinkage, enucleation
usually done once its shrunk enough
because the cystic lining will be much
thicker
66.
incisional
biopsy
biopsy of a specimen of the leasion, NOT the
entire lesion, to allow treating doctors to have
something to work with
67.
excisional
biopsy
removal of entire lesion with perimeter of
normal tissue surrounding lesion (2-3mm)
68.
indications
for an
excisional
biopsy
small benign lesions, removability without loss
of function, pigments/small/vascular lesions
79.
indications for
marsupialization
how to
anesthetize a
lesion for
biopsy
do not inject right into the lesion, inject 1cm
surrounding the tissue
too large to remove all in once, extent
could cause pathologic fracture,
anatomical risk, loss of function, simple to
do but we don't get rid of the entire lesion
80.
what syndrome
are OKCs
associated with?
never use
suction
when
performing a
biopsy
so it doesnt get sucked up and you lose the
specimen
Gorlin syndrome (nevoid basal
syndrome)-palmar pits, chest concavity,
multiple basal cells that could turn
cancerous
81.
marginal
resection
removal of tumor without bony disruption
82.
surgical
closure of a
biopsy
undermine the wound margins by at least the
width of the ellipse in each direction, this will
decrease the tension after suturing, obtain
primary closure except for attached mucosal
surfaces (secondary is fine)
segmental
resection
removal of tumor by incising through
uninvolved tissues around it, will
discontinue the bone
83.
composite
resection
resection of tumor with bone adjacent soft
tissues, and lymph node channels
84.
enucleation and
curretage
local removal of tumor by instrumentation
in direct contact with lesion
85.
enucleation and
peripheral
ostectomy
local removal of tumor by instrumentation
in direct contact with lesion in addition to
mechanical removal of at least 2mm of
peripheral bone
86.
autogenous graft
tissue obtained from the same individual,
ideal grafting material due to lack of
immune response, vascularized or nonvascularized
87.
where,
anatomically,
can we get the
most bone?
posterior iliac crest (60-80cc)
88.
when would we
use a rib graft?
mostly in pediatric patients, it will wear
away more in adults
69.
70.
71.
definition of
cyst
closed sac like structures with liquid inside
73.
hamartoma
dysmorphic proliferation of native tissue
which will get to a certain size and then stop
growing
74.
choristoma
dysmorphic proliferatio of NON-native tissue
which will get to a certain size and then stop
growing
75.
difference
between
benign and
malignant
neoplasms
malignancies possess proteins required for
metastasis whereas benign do not
72.
89.
how are maxillary reconstructions for major defects
cured?
a surgical obturator is used with a final prosthesis
90.
why is it important to have a soft tissue bed for a nonvascularized bone graft?
to avoid contamination and have vascularity to the site, incision is done until
healthy soft tissue is encountered
91.
soft tissue reconstruction is indicated when?
primary closure is not feasible, lots of radiation to that area, preparing for
secondary bone grafting
92.
what is a successful reconstruction?
complete return to adequate function with appropriate esthetic results
Вам также может понравиться
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Maxillary Blocks: Block Area Affected Needle Depth Landmark and Orientation ImageДокумент2 страницыMaxillary Blocks: Block Area Affected Needle Depth Landmark and Orientation ImageokibreazyОценок пока нет
- MakingMusic DennisDeSantisДокумент293 страницыMakingMusic DennisDeSantisJulian Trujillo Bonilla0% (1)
- Coco - Remember MeДокумент1 страницаCoco - Remember MeokibreazyОценок пока нет
- Essay PracticeДокумент2 страницыEssay PracticeokibreazyОценок пока нет
- Army Strategic Language List DTD 18 Jan 19Документ5 страницArmy Strategic Language List DTD 18 Jan 19okibreazyОценок пока нет
- Assessment of The Esthetic Smile in Young Japanese Women: Research PaperДокумент9 страницAssessment of The Esthetic Smile in Young Japanese Women: Research PaperokibreazyОценок пока нет
- Moral Theo Paper 1 WordДокумент5 страницMoral Theo Paper 1 WordokibreazyОценок пока нет
- LP6 Guitar Scales SystemДокумент29 страницLP6 Guitar Scales SystemokibreazyОценок пока нет
- Management of Cleft LipДокумент68 страницManagement of Cleft LipokibreazyОценок пока нет
- Jazz Guitar CurriculumДокумент3 страницыJazz Guitar CurriculumokibreazyОценок пока нет
- U.S. Powerboating Class: Saturday & Sunday August 26 & 27 or September 16 & 17Документ4 страницыU.S. Powerboating Class: Saturday & Sunday August 26 & 27 or September 16 & 17okibreazyОценок пока нет
- A Better Affirmative ActionДокумент76 страницA Better Affirmative ActionokibreazyОценок пока нет
- Oral Surgery Final Exam: Study Online atДокумент2 страницыOral Surgery Final Exam: Study Online atokibreazyОценок пока нет
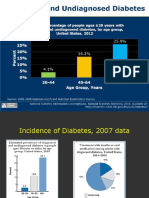
- Diabetes Mellitus in The US:: PrevalenceДокумент48 страницDiabetes Mellitus in The US:: PrevalenceokibreazyОценок пока нет
- A Better Affirmative ActionДокумент76 страницA Better Affirmative ActionokibreazyОценок пока нет
- Analysis of Misty (Errol Garner)Документ4 страницыAnalysis of Misty (Errol Garner)okibreazyОценок пока нет
- Short Haiku Is It Redundant? or Is It Impossible This, A Short HaikuДокумент1 страницаShort Haiku Is It Redundant? or Is It Impossible This, A Short HaikuokibreazyОценок пока нет
- Rules Splendor USДокумент4 страницыRules Splendor USfournies1754100% (1)
- CPR Aha Written ExamДокумент4 страницыCPR Aha Written Examokibreazy100% (3)
- Anticancer DrugsДокумент35 страницAnticancer DrugsokibreazyОценок пока нет
- Pharm Review Class VersionДокумент138 страницPharm Review Class VersionokibreazyОценок пока нет
- ReviewДокумент9 страницReviewokibreazyОценок пока нет
- Jazz Guitar CurriculumДокумент3 страницыJazz Guitar CurriculumokibreazyОценок пока нет
- Stuff To DoДокумент1 страницаStuff To DookibreazyОценок пока нет
- Fender ElectricGuitars ManualДокумент36 страницFender ElectricGuitars ManualokibreazyОценок пока нет
- Pharmacology Crossword PuzzleДокумент3 страницыPharmacology Crossword Puzzleokibreazy100% (2)
- 6th Central Pay Commission Salary CalculatorДокумент15 страниц6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- Guitar Scales PentatonicДокумент1 страницаGuitar Scales PentatonicokibreazyОценок пока нет
- Whitening TraysДокумент68 страницWhitening TraysokibreazyОценок пока нет
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (399)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Revision Notes On FRCRДокумент385 страницRevision Notes On FRCRObaidy Albushaher100% (2)
- Iota PDFДокумент6 страницIota PDFariniОценок пока нет
- Final PPT ProjectДокумент19 страницFinal PPT ProjectGunjan AjmeraОценок пока нет
- An Introduction To Cancer Biology: When Good Cells Go BadДокумент68 страницAn Introduction To Cancer Biology: When Good Cells Go BadSavitaОценок пока нет
- United States Patent: (10) Patent No .: US 10, 105, 389 B1 (45) Date of Patent: Oct - 23, 2018Документ39 страницUnited States Patent: (10) Patent No .: US 10, 105, 389 B1 (45) Date of Patent: Oct - 23, 2018Philipp SellinОценок пока нет
- An Approach To Diagnosis: Neck LumpДокумент36 страницAn Approach To Diagnosis: Neck LumpTracy WheelerОценок пока нет
- 4 2 PDFДокумент9 страниц4 2 PDFMahtab KhalifpourОценок пока нет
- Requisites in Dearmatology - Dermatopathology (PDF) (Tahir99) VRG (Dragged) 12 PDFДокумент1 страницаRequisites in Dearmatology - Dermatopathology (PDF) (Tahir99) VRG (Dragged) 12 PDFJUSASBОценок пока нет
- Oncovet 2008Документ18 страницOncovet 2008Frederico VelascoОценок пока нет
- CAFL EnglishДокумент21 страницаCAFL Englishredtruck99Оценок пока нет
- What Are The Benefits of GarlicДокумент7 страницWhat Are The Benefits of GarlicBellia AyudiaОценок пока нет
- Koss y Honda - Citología Del Tracto Urinario (2012)Документ142 страницыKoss y Honda - Citología Del Tracto Urinario (2012)Lord Verminaard Luis Carreño DuranОценок пока нет
- Master of Internal Medicine Logbook1Документ112 страницMaster of Internal Medicine Logbook1alhusseinaliОценок пока нет
- Jadual Waktu Sem 1 2022.2023 InformmДокумент19 страницJadual Waktu Sem 1 2022.2023 InformmvimalaОценок пока нет
- Benign Breast Disease: Douglas J. Marchant, MDДокумент20 страницBenign Breast Disease: Douglas J. Marchant, MDchristel chadidОценок пока нет
- 2006 89 Canine and Feline Nasal NeoplasiaДокумент6 страниц2006 89 Canine and Feline Nasal NeoplasiaFelipe Guajardo HeitzerОценок пока нет
- 7a. Cellular Aberration With PAIN ConceptДокумент25 страниц7a. Cellular Aberration With PAIN ConceptRENEROSE TORRESОценок пока нет
- Myxofibrosarcoma: Christina L. Roland,, Wei-Lien Wang,, Alexander J. Lazar,, Keila E. TorresДокумент14 страницMyxofibrosarcoma: Christina L. Roland,, Wei-Lien Wang,, Alexander J. Lazar,, Keila E. TorresMarina GorelikОценок пока нет
- Unilateral Tonsil EnlargementДокумент5 страницUnilateral Tonsil EnlargementBryan Albert LimОценок пока нет
- Fordyce GranulesДокумент6 страницFordyce GranuleshanyОценок пока нет
- Salivary Gland CytologyДокумент30 страницSalivary Gland CytologyPatrick BayuОценок пока нет
- Neoplasia 2Документ38 страницNeoplasia 2meutia komalaОценок пока нет
- (Encyclopedia of Pathology) Pieter J. Slootweg (Eds.) - Dental and Oral Pathology-Springer International Publishing (2016)Документ372 страницы(Encyclopedia of Pathology) Pieter J. Slootweg (Eds.) - Dental and Oral Pathology-Springer International Publishing (2016)Maria Mery Garcia VelascoОценок пока нет
- Tan Ah Kau V The Government of Malaysia - (2Документ17 страницTan Ah Kau V The Government of Malaysia - (2Arvin AОценок пока нет
- Single-Cell Map of Diverse Immune Phenotypes in The Breast Tumor MicroenvironmentДокумент53 страницыSingle-Cell Map of Diverse Immune Phenotypes in The Breast Tumor MicroenvironmentRoger FigueiredoОценок пока нет
- Medical Terminology TermsДокумент28 страницMedical Terminology TermsNikka Moreen DagdagОценок пока нет
- Exploring Medical Language A Student Directed Approach 8th Edition Brooks Test BankДокумент16 страницExploring Medical Language A Student Directed Approach 8th Edition Brooks Test BankAnneMuellerqcigf100% (12)
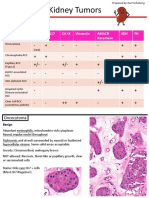
- Kidney Tumors: EosinophilicДокумент11 страницKidney Tumors: EosinophilicPankaj DubeyОценок пока нет
- Zracenje 1Документ22 страницыZracenje 1DejanОценок пока нет
- Warthin's TumorДокумент18 страницWarthin's TumorDoc PrakashОценок пока нет