Академический Документы
Профессиональный Документы
Культура Документы
Renal Vulnerability To Drug Toxicity: In-Depth Review
Загружено:
Eric GibsonОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Renal Vulnerability To Drug Toxicity: In-Depth Review
Загружено:
Eric GibsonАвторское право:
Доступные форматы
In-Depth Review
Renal Vulnerability to Drug Toxicity
Mark A. Perazella
Section of Nephrology, Department of Medicine, Yale University, New Haven, Connecticut
Drug-induced kidney disease occurs primarily in patients with underlying risk factors. A number of factors enhance the
vulnerability of the kidney to the nephrotoxic effects of drugs and toxins. They are broadly categorized as patient-specific,
kidney-related, and drug-related factors. One, two, or all three of the factor categories can act to promote various forms of renal
injury. Importantly, all compartments of the kidney can be affected and result in one or more classic clinical renal syndromes.
These include acute kidney injury, various tubulopathies, proteinuric renal disease, and chronic kidney disease. Recognizing
risk factors that increase renal vulnerability to drug-induced kidney disease is the first step in reducing the renal complications of drugs and toxins.
Clin J Am Soc Nephrol 4: 12751283, 2009. doi: 10.2215/CJN.02050309
he kidney performs a number of essential functions in
the body. Most important are the clearance of endogenous waste products, control of volume status, maintenance of electrolyte and acid-base balance, and endocrine
function. Metabolism and excretion of exogenously administered therapeutic and diagnostic agents as well as environmental exposures are other major functions. In its role as the primary eliminator of exogenous drugs and toxins, the kidney is
vulnerable to develop various forms of injury. This paper will
review the important nephrotoxins that the kidney is exposed
to, the factors that increase vulnerability of the kidney to potential toxins, the renal compartments afflicted by toxins, and
the clinical renal syndromes promoted by these agents.
Potential Nephrotoxins
The first step in the development of nephrotoxicity requires
adequate exposure to the offending agent. Humans are exposed
to a variety of potential nephrotoxic substances on a rather
frequent basis (Table 1). Several therapeutic agents have known
nephrotoxic potential; classic examples include anti-microbial
agents, chemotherapeutic agents, analgesics, and immunosuppressive agents (1 8). While most are prescribed, many others
are available to the general population over-the-counter. Numerous new drugs with unknown toxic potential are constantly
being released for use into clinical practice. Diagnostic agents,
in particular iodinated radiocontrast and high dose intra-arterial gadolinium, are another source of nephrotoxin exposure
(9,10).
An important and unregulated source of potentially nephrotoxic substances is the alternative/complementary products,
which include herbal remedies, natural products, and nutritional supplements that are widely available at most health
Published online ahead of print. Publication date available at www.cjasn.org.
Correspondence: Mark A. Perazella, Associate Professor of Medicine, Section of
Nephrology, Department of Medicine, Yale University, 330 Cedar Street, New
Haven, Connecticut 06520-8029. Phone: 203-785-4184; Fax: 203-785-7068; E-mail:
mark.perazella@yale.edu
Copyright 2009 by the American Society of Nephrology
food stores (11,12). More concerning is the harmful contaminants and chemicals contained in the products that are not
listed on the label (11,12). Interaction of herbal products with
conventional drugs is also a potential source of toxicity. Examples of nephrotoxic alternative products include aristolochic
acid, Ephedra species and Glycyrrhiza species (11,12). Adulteration of herbal products with dichromate, cadmium, and phenylbutazone also causes significant renal injury (11,12). A recent example of adulteration is worth mentioning. To falsely
elevate protein content, melamine was added to baby formula.
This is an example of contamination with a substance that
causes acute kidney injury (AKI) and nephrolithiasis in neonates (13).
Finally, environmental exposure to various nephrotoxins remains a problem (14 16). Included are toxins such as lead,
cadmium, mercury, copper, uranium, and bismuth, to name a
few. An increasing nephrotoxic concern is lead exposure, even
at levels that are considered safe and acceptable to governmental agencies. Low-level lead exposure appears to exacerbate
underlying chronic kidney disease (CKD), leading to more
rapid progression to advanced stages of CKD and dialysisrequiring end-stage renal disease (ESRD) (14 16).
Risk Factors for Nephrotoxicity
A simplified approach to understanding the renal vulnerability to nephrotoxins entails the classification of risk factors
into three major categories (Table 2). Each category or specific
risk factor contributes to the enhanced development of kidney
injury. In general, more than one of the risk factors is acting to
promote renal injury. Most often, at least two or all three
conspire to cause various forms of clinical kidney disease. It is
these factors that explain the variability and heterogeneity seen
with drug or toxin-induced kidney disease.
Patient-Specific Characteristics
Underlying patient-specific characteristics comprise the first
risk factor category (Table 2). The patient exposed to drugs and
other substances is predisposed to develop nephrotoxicity
ISSN: 1555-9041/4071275
1276
Clinical Journal of the American Society of Nephrology
Clin J Am Soc Nephrol 4: 12751283, 2009
Table 1. Commonly encountered nephrotoxic agents and exposuresa
Therapeutic Agents
Antimicrobial
Aminoglycosides
Antiviral agents
Amphotericin B
Colistin
Sulfadiazine
Ciprofloxacin
Chemotherapy
Platins
Ifosfamide
Mitomycin
Gemcitabine
Methotrexate
Pentostatin
Interleukin-2
Anti-angiogenesis agents
Alternative Products
Herbal remedies
Aristolochic acid
Ephedra sp.
Glycyrrhiza sp.
Datura sp.
Taxus celebica
Uno degatta
Cape aloes
Adulterants
Mefenamic acid
Dichromate
Cadmium
Phenylbutazone
Melamine
Diagnostic Agents
Radiocontrast
High osmolar
Low osmolar
Iso-osmolar
Other agents
Gadolinium (in high dose)
Oral NaP solution
(colonoscopy prep)
Environmental
Exposures
Heavy metals
Lead
Mercury
Cadmium
Uranium
Copper
Bismuth
Solvents
Hydrocarbons
Other toxins
Silicon
Germanium
Analgesics
NSAIDs
Selective COX-2 inhibitors
Phenacetin
Analgesic combinations
Immunosuppressives
Sirolimus
Calcineurin inhibitors
Other
ACE inhibitors/ARBs
Methoxyflurane
Sucrose, Hydroxyethyl starch, Mannitol
Pamidronate, Zolendronate
Topiramate, Zonisamide
Orlistat
Statins
Mesalamine
a
NaP, sodium phosphate; NSAIDs, nonsteroidal anti-inflammatory drugs; ARBs, angiotensin-receptor blockers; ACE,
angiotensin-converting enzyme.
when certain underlying risk factors are present. Many of these
factors are nonmodifiable, such as older age and female gender.
Risk in the elderly and females occurs through the following: 1)
changes in total body water, which is reduced in setting of
decreased lean body mass and leads to drug overdose; 2)
unrecognized lower GFR despite normal serum creatinine concentration; and 3) reduced drug binding to proteins due to
hypoalbuminemia, which results in increased free drug concentrations (1720). The elderly also have increased propensity to
vasoconstriction from excessive angiotensin II and endothelin
and have higher levels of oxidatively modified biomarkers (17).
These factors combine to expose the patient to excess drug
concentration and risk of nephrotoxicity. Along these same
lines, both underlying AKI and CKD are important risk factors
for increasing vulnerability to nephrotoxic injury (18 20). Excessive drug dosing, exposure of a reduced number of functioning nephrons to toxins, ischemia preconditioned tubular
cells, and more robust renal oxidative injury response to toxins
are all contributors in these settings.
Nephrotic syndrome and cirrhosis raise risk through multiple mechanisms that include altered renal perfusion from reduced effective circulating blood volume, hypoalbuminemia
with increased free circulating drug, and unrecognized renal
impairment (18 21). The last point is a particular problem as
Clin J Am Soc Nephrol 4: 12751283, 2009
Table 2. Risk factors that increase renal vulnerability to
nephrotoxinsa
Patient-Specific Factors
Female sex
Old age (65 yr)
Nephrotic syndrome
Cirrhosis/obstructive jaundice
Acute/Chronic kidney disease
True or effective volume depletion
Decreased glomerular filtration rate
Enhanced proximal tubular toxin reabsorption
Sluggish distal tubular urine flow rates
Metabolic perturbations
Hypokalemia, hypomagnesemia, hypercalcemia
Alkaline or acid urine pH
Immune response genes
Pharmacogenetics favoring drug toxicity
Gene mutations in hepatic and renal P450 system
Gene mutations in renal transporters and
transport proteins
Kidney-Specific Factors
High rate of blood delivery (20-25% of cardiac
output)
Increased toxin concentration in renal medulla &
interstitium
Biotransformation of substances to reactive
oxygen species
High metabolic rate of tubular cells (loop of Henle)
Proximal tubular uptake of toxins
Apical uptake via endocytosis/pinocytosis
Basolateral transport via OAT and OCT
Drug-Specific Factors
Prolonged dosing periods and toxin exposure
Potent direct nephrotoxic effects of the drug or
compound
Combinations of toxins/drugs promoting
enhanced nephrotoxicity
Competition between endogenous and
exogenous toxins for transporters, increasing
toxin accumulation within the tubular cell
Insoluble parent compound and metabolite with
intratubular crystal precipitation
a
OAT, organic anion transporters; OCT, organic cation
transporters.
serum creatinine is often low or normal in these patients. Obstructive jaundice also enhances toxicity to certain drugs, such
as the aminoglycosides through altered hemodynamics (decreased renal blood flow) and direct effects of bile salts on
tubular epithelia (22). Both true (vomiting, diarrhea, diuretics)
and effective volume depletion (congestive heart failure, ascites, sepsis) increase renal vulnerability to various agents.
Through induction of renal hypoperfusion and prerenal
azotemia, these underlying processes enhance nephrotoxicity
of many drugs and substances. In particular, renal hypoperfu-
Drug Nephrotoxicity
1277
sion increases nephrotoxicity in drugs excreted primarily by the
kidney (excessive drug dosing), in those reabsorbed in the
proximal tubule (increased intracellular concentration), and in
those that tend to be insoluble in the urine where crystal
precipitation occurs within distal tubular lumens with sluggish
flow (18 21,23).
Metabolic disturbances also increase renal vulnerability to
certain drugs and potential toxins. Hypokalemia, hypomagnesemia, and hypocalcemia are electrolyte and divalent ion
disorders that increase renal toxicity associated with aminoglycosides (18 20). Severe hypercalcemia induces afferent arteriolar vasoconstriction and renal sodium/water wasting, leading
to prerenal physiology, which enhances nephrotoxic drug injury. Patients with metabolic disorders that alter urine pH are at
risk to develop intratubular crystal deposition when certain
drugs and substances precipitate within tubular lumens in the
distal nephron (23,24). Systemic metabolic acidosis or alkalosis
may decrease or increase urine pH, while proximal and distal
renal tubular acidoses are associated with alkaline urine due to
impaired renal ability to excrete H ion. Acidic urinary pH (
5.5) increases crystal deposition with drugs such as sulfadiazine, methotrexate, and triamterene that are insoluble in a low
pH environment (23,24). Alkaline urine (pH 6.0) increases
crystal precipitation within tubular lumens from drugs such as
indinavir, oral sodium phosphate solution, and ciprofloxacin
(2325). In addition, drugs such as topiramate, zonisamide, and
acetazolamide alkalinize the urine through inhibition of carbonic anhydrase and promote precipitation of calcium phosphate within tubules, thereby enhancing renal stone formation
(26,27).
The underlying genetic makeup of the host can also enhance
renal vulnerability to potential nephrotoxins (28 30). The drug
or its metabolite form adducts that modify their physical structure, making them more immunogenic. There is, however, significant heterogeneity in the response of patients to drugs and
exogenous exposures. One obvious example is the heightened
allergic response of some individuals as compared with others.
Differences in innate host immune response genes can predispose certain patients to develop an allergic response to a substance. The variability of immune responses has been demonstrated in patients who develop drug-induced interstitial
nephritis, which appears to be a T cell driven process (31). This
translates into enhanced vulnerability to an allergic response in
the kidney and development of an acute interstitial nephritis.
An area of intense interest is the role of pharmacogenetics as
an explanation for the heterogeneous response of patients to
drugs as it relates to efficacy and toxicity (28 30). The hepatic
cytochrome P450 (CYP450) enzyme system has been well studied, and several CYP450 enzyme gene polymorphisms are associated with reduced metabolism and subsequent end organ
toxicity. The kidney also possesses CYP450 enzymes that participate in drug metabolism (28 30). One would expect that
gene polymorphisms favoring reduced metabolism could increase nephrotoxic risk as well. Polymorphisms of genes encoding proteins involved in the metabolism and subsequent
renal elimination of drugs have been described and are correlated with various levels of drug sensitivity. Specific to the
1278
Clinical Journal of the American Society of Nephrology
discussion of nephrotoxicity, loss-of-function mutations in apical secretory transporters (reduce cell drug efflux into the
urine), and mutations in kinases that regulate drug carrier
proteins can impair drug elimination and promote toxicity by
elevating intracellular toxin concentrations (29). In the future,
more information regarding how patients differ in the function
and regulation of channels, transporters, and carriers that regulate elimination of drugs and other compounds cleared by the
kidney will be brought to light. An elegant example of this is
seen with tenofovir-induced Fanconi syndrome (32). In patients
exposed to tenofovir who developed Fanconi syndrome, a single nucleotide polymorphism (1249 G3 A SNP) was present in
the gene coding the multidrug-resistant protein-2 (MRP2) efflux transporter, which transports tenofovir out of the cell.
Tenofovir-exposed patients who did not develop Fanconi syndrome did not have the polymorphism.
Kidney-Specific Factors
The next category of risk relates to the mechanism by which
the kidney metabolizes and excretes various drugs and toxins
(Figure 1). Significant renal exposure to potential nephrotoxins
occurs due to the high rate of drug and toxin delivery to the
kidney, a result of the high blood flow to the kidney, which
approaches 25% of cardiac output. Many renal cells, particularly those in the loop of Henle, exist in a relatively hypoxic
environment due to the high metabolic rates required to actively transport many solutes via Na-K-ATPase driven trans-
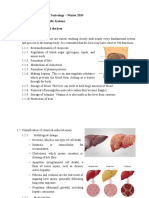
Figure 1. Kidney specific factors that enhance nephrotoxic risk
are noted. First, high RBF increases drug delivery to the kidney.
High metabolic rates of cells increase risk for nephrotoxicity
with certain drugs. Renal biotransformation of drugs to toxic
metabolites and ROS overwhelms local anti-oxidants. Increased
concentration of drugs in the medulla and interstitium causes
nephrotoxicity. Finally, apical uptake of certain drugs (aminoglycosides, sucrose) and basolateral transport of drugs through
the OAT (tenofovir) and OCT (cisplatin) transporters increases
renal toxicity. Abbreviations: RBF, renal blood flow; OAT, organic anion transporter; OCT, organic cation transporter; ROS,
reactive oxygen species.
Clin J Am Soc Nephrol 4: 12751283, 2009
port. This excess cellular workload and hypoxic environment
promotes increased sensitivity to injury when exposure to potentially nephrotoxic substances occurs (33,34). Another factor
that enhances renal nephrotoxicity is the high concentration of
parent compounds and their metabolites that develop in the
renal medulla and interstitium from the enormous concentrating ability of the kidney (33,34). Elevated tissue concentration
of these toxins promotes injury through both direct toxicity and
ischemic damage (reduced prostaglandins, increased thromboxane).
Biotransformation of drugs, xenobiotics, and other substances by multiple renal enzyme systems, including CYP450
and flavin-containing monooxygenases, favors the formation of
toxic metabolites and reactive oxygen species (3335). The presence of these byproducts of metabolism tilts the balance in
favor of oxidative stress, which outstrips natural antioxidants
and increases renal injury via nucleic acid alkylation or oxidation, protein damage, lipid peroxidation, and DNA strand
breaks (3335).
Enhanced toxicity in proximal tubular cells occurs due to the
extensive cellular uptake of potential toxins and drugs by both
apical and basolateral transport systems. Apical uptake of substances occurs via endocytosis and other transport pathways
(36 40). Examples include the polycationic aminoglycosides
(Figure 2), heavy metals, and various complex sugars and
starches. Following endocytosis of aminoglycosides, which involves the endocytic receptor (megalin) for cationic ligands,
these drugs are translocated into the lysosomal compartment
where they accumulate and subsequently form myeloid bodies
(33,34,36). These bodies are membrane fragments and damaged
Figure 2. Apical membrane handling of substances, in this example aminoglycosides, by proximal tubular cells. Aminoglycosides interact with anionic phospholipids/megalin on the
apical surface where they are endocytosed and enter the cell.
The drug is then translocated into lysosomes, where it is associated with various forms of cellular injury. Abbreviations: AG
(), aminoglycoside; (-) PL, anionic phospholipids; M, megalin;
Lys, lysosome; Na, sodium; K, potassium.
Clin J Am Soc Nephrol 4: 12751283, 2009
organelles formed as a consequence of aminoglycoside inhibition of lysosomal enzymes. This apical pathway of uptake leads
to accumulation of a critical concentration of aminoglycoside
within cells, which triggers an injury cascade leading to cell
injury and death. Another pathway of proximal tubular cell
toxin exposure occurs via basolateral delivery of endogenous
and exogenous organic ions (anions and cations) by peritubular
capillaries (39,40). Toxicant delivery via peritubular capillaries
is followed by uptake into proximal tubular cells via a family of
transporters, including human organic anion (HOAT) and cation (HOCT) transporters (39,40). As classic examples, acyclic
nucleotide phosphonates are transported via HOAT (39),
whereas cisplatin is transported via HOCT. Transport of toxicants into cells, followed by movement through the intracellular space via various regulated carrier proteins, and subsequent
exit from the cells via apical transport proteins enhances toxicity in proximal tubular cells (40). Loss of function mutations in
and competition for apical secretory transporters (41), which
reduces toxin efflux from cell into urine, may promote accumulation of toxic substances within proximal tubular cell and
cause cellular injury via apoptosis or necrosis (Figure 3). This
extensive trafficking of substances increases renal tubular exposure and risk for elevated concentration of toxin when other
risk factors supervene.
Drug-Specific Factors
The underlying characteristics of the offending agent also
play an important role in the development of nephrotoxicity.
Figure 3. Basolateral handling of substances, in this example
tenofovir, by proximal tubular cells. Tenofovir (TDF) is delivered to the basolateral membrane, transported into the cell via
the organic anion transporter-1 (OAT-1), and excreted by various apical transporters into the urinary space. In this example,
transport by the multidrug-resistance protein (MRP2) transporter is inhibited or dysfunctional, causing intracellular accumulation of drug and nephrotoxicity. Abbreviations: Pgp, Pglycoprotein; PEPT1/2, peptide transporters; OA, organic
anions; OC, organic cations; OAT, organic anion transporter,
OCT, organic cation transporter; Na, sodium; K, potassium.
Drug Nephrotoxicity
1279
From a practical standpoint, prolonged therapy at high doses
with toxic substances enhances renal injury based on excessive
renal exposure in the absence of other risks. Exogenous substances and their metabolites that are insoluble in human urine
may cause renal injury. In addition to unique characteristics of
the offending agent that induce insolubility, factors such as
urine pH, sluggish tubular urine flow rates, and rapid parenteral or excessive dosing (high peak serum and urine concentrations) enhance risk for precipitation and crystal formation in
distal nephron tubular lumens (19 21). Commonly used medications such as acyclovir, methotrexate, sulfadiazine, indinavir, atazanavir, and oral sodium phosphate solution are examples. Aminoglycosides with more positive charge are more
likely to cause nephrotoxicity, perhaps due to enhanced interactions with negatively charged membrane phospholipids and
megalin (7,36). This is reflected by the greater nephrotoxicity of
the neomycin as compared with amikacin. Drug combinations
also raise risk of nephrotoxicity. Combinations such as aminoglycosides and cephalothin, nonsteroidal anti-inflammatory
drugs (NSAIDs) and radiocontrast, and cisplatin and aminoglycosides are a few examples of enhanced nephrotoxic risk
with concurrent drug administration (18 21). As mentioned
previously, various drugs and endogenously produced molecules can compete for transport proteins in the proximal tubular cells, thereby reducing renal elimination and increasing
intracellular drug/toxin concentration (1,3,5,23). This favors
development of nephrotoxicity.
Several drugs and toxins are more highly nephrotoxic and
can promote renal injury, even with brief or low-level exposure.
Examples include the aminoglycosides (in particular neomycin), amphotericin B, the polymyxins, zolendronate, and the
antiviral agents adefovir and cidofovir (1,3,57,42 44). Aminoglycosides are a classic nephrotoxin. Accumulation of high
concentrations within lysosomes and release into the cell cytoplasm promotes phospholipid membrane interruption, oxidative stress, and mitochondrial injury that cause proximal tubular cell apoptosis and necrosis, leading to clinical AKI.
Amphotericin B, and the lipid/liposomal formulations to a
lesser degree, disrupt cellular membranes and increase permeability to cations, resulting in tubular dysfunction due to cell
swelling and lysis (42). Colistin and polymyxin B are polymixin
antimicrobials that are extremely nephrotoxic with a very narrow therapeutic window. Their toxicity appears to be due to the
D-amino content and fatty acid component, which increase
membrane permeability and influx of cations (43). As seen with
amphotericin B, cell swelling and lysis results. The acyclic
nucleotide phosphonates enter the cell via basolateral HOAT-1
and promote cellular injury through multiple mechanisms. Mitochondrial injury, as manifested by mitochondrial enlargement, clumped cristae, and convoluted contours, occurs with
adefovir through inhibition of DNA polymerase gamma, which
is the sole DNA polymerase in mitochondria (3,5). Cidofovir,
which forms cidofovir-phosphocholine (analog of cytidine
5-diphosphocholine) within cells, interferes with synthesis
and/or degradation of membrane phospholipids, resulting in
proximal tubular injury (3,5). Tenofovir also impairs cellular
energetics through mitochondrial disruption and other intra-
1280
Clinical Journal of the American Society of Nephrology
Clin J Am Soc Nephrol 4: 12751283, 2009
Nephrotoxic substances produce disease in all compartments
of the kidney. The entire nephron and collecting duct system
are capable of being injured by various nephrotoxins. For ease
of classification, they can be divided into the following renal
compartments and the associated disease components: 1) Hemodynamic (prerenal disease); 2) Renal parenchyma (intrinsic
renal disease); and 3) Collecting system (postrenal disease).
tration), formation of reactive oxygen species with injurious
oxidative stress, and osmolar effects with loss of normal cellcell contact and tubular luminal occlusion (23,33).
In the loop of Henle, ischemic injury from reduced medullary
oxygen delivery (shunting blood to the cortex) and enhanced
tubular cell metabolic rate can occur with radiocontrast, especially in combination with NSAIDs (1,5,23,33). Rhabdomyolysis
with myoglobinuria can develop following therapy with certain drugs or toxins. It causes renal injury via hemodynamic
effects, tubular toxicity from direct toxicity of ferrihemate, and
tubular obstruction from myoglobin casts (1,23,33). In the cortical and medullary collecting ducts, tubular injury develops
from precipitation of insoluble crystals within tubular lumens
with or without an interstitial reaction (1,3,5,23,25). Exogenous
drugs or toxins promote this type of kidney disease.
Finally, disease within the interstitial compartment develops
from either an acute process such as acute interstitial nephritis
(AIN) or chronic insult such as chronic tubulointerstitial nephritis (CTIN). AIN represents an exuberant host immune response to an exogenously administered medication or toxin
(1,5,23). CTIN develops from persistent, untreated inflammation associated with AIN or chronic ischemia/toxicity from
certain analgesic combinations, mesalamine, heavy metals, or
nephrotoxic alternative/herbal medications (1,2,23,49).
Hemodynamic
Collecting System
Hemodynamic disturbances induced by certain medications
may produce a prerenal form of kidney injury in patients at
risk. Increased afferent arteriolar tone from direct or indirect
vasoconstrictors and reduced efferent arteriolar tone from ACE
inhibitors and ARBs in patients with true or effective volume
depletion or underlying kidney disease alter renal hemodynamics (1,5,6). They do so by reducing intrarenal perfusion and
lowering intracapillary hydraulic pressure, thereby reducing
the filtration fraction and ultimately the GFR.
Disease of the collecting system (postrenal disease) represents the last compartment of kidney injury that occurs from
certain medications or toxins. Both AKI and CKD result from
obstructive renal disease (1,23). Many drugs and toxins cause
either intrinsic or extrinsic urinary obstruction, from structural
problems such as stone formation (sulfadiazine, indinavir,
atazanavir, melamine) and retroperitoneal disease (methysergide, pergolide) or functional disturbances from bladder dysfunction (anticholinergics, opioids, -1 receptor agaonists, benzodiazepines) with urinary retention (1,23,50).
cellular processes (3,5,23). A unique and newly recognized
form of nephrotoxicity has been described with anti-angiogenesis therapy (45,46). Vascular endothelial growth factor (VEGF),
produced by adjacent podocytes, is required to maintain normal fenestrated endothelial function and is particularly important for normal functioning of the glomerular basement membrane (47). Reduction in VEGF or its effects by the various
anti-angiogenic drugs leads to loss of the healthy fenestrated
endothelial phenotype and promotes microvascular injury and
thrombotic microangiopathy, causing proteinuria and kidney
disease. Also, reduced nephrin expression in the slit diaphragms from these drugs may also contribute to proteinuria.
While these drugs cause a number of renal lesions, endothelial
injury and thrombotic microangiopathy are the most commonly noted (46,48).
Renal Compartments and Nephrotoxin Injury
Renal Parenchyma
Intrinsic kidney disease due to exogenous nephrotoxins may
occur in several compartments. Medium and small vessel vascular disease may result from toxin or drug-induced thrombotic microangiopathy (TMA) from endothelial injury or antibody formation against VWF cleaving protease or induction of
a hypercoaguable state. Glomerular disease with decreased
GFR and proteinuria develops from a wide array of toxins and
drugs (1,5,23). Injury occurs via damage to glomerular endothelial cells, visceral epithelial cells, microthrombi within glomerular capillaries, or immune complex deposition within glomerular capillary basement membranes from a drug antigen
inducing antibody formation (1,5,23).
Tubular disease, particularly in the proximal tubule, is a
common complication of prescribed nephrotoxins and environmental exposures. As was previously reviewed, the mechanism
by which the proximal tubule handles substances contributes to
enhanced nephrotoxicity in this nephron segment. Proximal
cell tubular toxicity develops due to direct nephrotoxic effects
(mitochondrial dysfunction, lysosomal hydrolase inhibition,
phospholipid damage, increased intracellular calcium concen-
Clinical Syndromes of Nephrotoxicity
To illustrate the various injuries that may occur along most
nephron segments and the collecting duct system and the clinical syndromes that may result from toxic substances, examples
of common forms of renal injury will be briefly reviewed. They
are divided into four major categories (Table 3) and some of the
common offenders are reviewed below.
Acute Kidney Injury
Many forms of nephrotoxicity result in AKI. Hemodynamic
kidney disease is caused by NSAIDs (including selective COX-2
inhibitors), several vasoconstrictors, and ACE inhibitors/ARBs
in at-risk patients (CKD, true or effective volume depletion).
The proximal tubule is commonly injured by multiple exogenous toxins, causing the syndrome of acute tubular necrosis
(ATN). A classic example of ATN in the proximal tubule is
aminoglycoside nephrotoxicity (7), while other nephrotoxins
that affect this segment include ifosfamide, cisplatin, zolendronate, and radiocontrast (9,34 36,41 43,45). Acyclic nucleotide
phosphonates promote ATN (3,5,23). Heavy metal intoxication
Clin J Am Soc Nephrol 4: 12751283, 2009
Table 3. Clinical renal syndromes caused by
nephrotoxinsa
Tubulopathies
Renal Tubular Acidosis/Fanconi Syndrome
Sodium Wasting
Potassium Wasting
Nephrogenic Diabetes Insipidus
Nephrotic Syndrome/Proteinuria
Glomerular Disease
Minimal Change Glomerulonephritis
Focal Segmental Glomerulosclerosis
Membranous Glomerulonephritis
Other
Thrombotic Microangiopathy
HUS/TTP
Acute Kidney Injury
Hemodynamic Disturbances
Parenchymal Kidney Disease
Collecting System Disease
Chronic Kidney Disease
Analgesic Nephropathy
Chronic Tubulointerstitial Nephritis
Secondary Progression of Toxin-induced
Kidney Disease
a
HUS, hemolytic uremic syndrome; TTP, thrombotic
thrombocytopenic purpura.
with lead, cadmium, and mercury cause proximal tubular injury and ATN (15,16). Osmotic proximal tubular injury occurs
with various sugars (sucrose, dextran, mannitol) and starches
(hydroxyethyl starch) (23).
Acute interstitial nephritis from prescribed and over-thecounter drugs is another relatively common cause of AKI.
While B-Lactams and sulfa-based drugs are widely recognized
etiologies, any drug maintains potential such as the NSAIDs,
selective COX-2 inhibitors, quinolones, H2-blockers, and proton
pump inhibitors, to name a few (1,5,23). Due to their widespread use, proton pump inhibitors are now the leading cause
of drug-induced AIN (51). Crystal nephropathy develops following administration of indinavir, acyclovir, sulfadiazine,
methotrexate, and oral sodium phosphate solution (purgative)
in host with at-risk physiology (1,3,5,23,48). Obstructive nephropathy occurs with complete urinary tract obstruction from
drug-related nephrolithiasis, induction of retroperitoneal fibrosis from methysergide and other drug or toxin exposures
(1,5,49). Urinary retention from a host of drugs also may promote AKI from complete obstruction.
Nephrotic Syndrome/Proteinuria
Several drugs and a few exposures cause glomerular disease
with associated proteinuria, which can be nephrotic range. Minimal change disease develops from NSAIDs, selective COX-2 inhibitors, and IFN-alpha, while focal segmental glomerulosclerosis
(FSGS) occurs following exposure to pamidronate, contaminated
heroin, and lithium (1,5,23). Sirolimus, particularly high serum
Drug Nephrotoxicity
1281
levels, also is associated with FSGS in transplant recipients (52).
Membranous glomerulopathy, an immune complex disease, is
associated with gold, penicillamine, NSAIDs/COX-2 inhibitors,
and captopril among others (1,5,23). Thrombotic microangiopathy
develops with gemcitabine, mitomycin-C, cisplatin, quinine, radiation therapy, and many other agents (1,5). Anti-angiogenesis
therapy with bevacizumab, sorafenib, and sunitinib have been
associated with development of proteinuria and TMA (46,48).
Multiple glomerular patterns of injury are described, with TMA
being the most common (46,48).
Tubulopathies
Briefly, a number of tubular dysfunction syndromes can occur
following toxin exposure. In the proximal tubule, a proximal renal
tubular acidosis or full blown Fanconi syndrome may follow
therapy with acyclic nucleotide phosphonates, aminoglycosides,
ifosfamide, or exposure to heavy metals and herbs such as Aristolochic acid and Akebia species (1,3,11,23). Salt wasting from loop
or distal nephron tubular injury is seen with cisplatin and aminoglycosides (acquired Bartter syndrome) (1,4,31,33). Nephrogenic
diabetes insipidus occurs with lithium, acyclic nucleotide phosphonates, and heavy metals such as cadmium (1,3).
Chronic Kidney Disease (CKD)
Most forms of parenchymal kidney injury can progress to
CKD. Focusing on chronic tubulointerstitial nephritis, several
agents are more commonly associated with CKD, including
combination analgesics (phenacetin, NSAIDS, caffeine), 5-aminosalicylic acid (mesalamine), aristolochic acid-containing
herbal remedies, and other natural/complementary product
adulterants (2,11,43). Heavy metal exposure, in particular lead,
can cause CTIN and CKD (14 16). Phosphate nephropathy also
causes CKD in a significant number of patients (23).
Conclusion
The kidney is vulnerable to injury from a variety of substances
with nephrotoxic potential. Numerous known and potential nephrotoxins are prescribed to patients, while many are available without prescription at health food and other stores, and present in the
environment. Recognizing that these substances maintain nephrotoxic potential is the first step in avoiding or reducing renal
injury. Awareness of the factors that enhance nephrotoxic risk is
important. These include specific patient characteristics, renal handling of the offending agents, and the nephrotoxicity of the substance itself. Importantly, all compartments of the kidney are
subject to injury by these substances. Injury by these nephrotoxins
results in recognizable clinical renal syndromes, including AKI,
nephrotic syndrome and proteinuric renal disease, tubular dysfunction syndromes, and CKD. Putting these data together allows
one to predict potential for nephrotoxicity and reduce development of kidney impairment.
Disclosures
None.
1282
Clinical Journal of the American Society of Nephrology
Clin J Am Soc Nephrol 4: 12751283, 2009
References
1. Schetz M, Dasta J, Goldstein S, Golper T: Drug-induced
acute kidney injury. Curr Opin Crit Care 11: 555565, 2005
2. Elseviers MM, DeBroe ME: Analgesic nephropathy: Is it
caused by multi-analgesic abuse or single substance use?
Drug Saf 20: 1524, 1999
3. Izzedine H, Launay-Vacher V, Deray G: Antiviral druginduced nephrotoxicity. Am J Kidney Dis 45: 804 817, 2005
4. Kintzel PE: Anticancer drug-induced kidney disorders.
Drug Saf 24: 19 38, 2001
5. Perazella MA: Drug-induced nephropathy: An update. Expert Opin Drug Saf 4: 689 706, 2005
6. Gambaro G, Perazella MA: Adverse renal effects of antiinflammatory agents: Evaluation of selective and nonselective cyclooxygenase inhibitors. J Intern Med 253: 643 652,
2003
7. Rougier F, Ducher M, Maurin M, Corvaisier S, Claude D,
Jeliffe R, Maire P: Aminoglycoside dosages and nephrotoxicity. Clin Pharmacokinet 42: 493500, 2003
8. Lamieire NH, Flombaum CD, Moreau D, Ronco C: Acute
renal failure in cancer patients. Ann of Med 37: 1325, 2005
9. Briguori C, Colombo A, Airoldi F, Morici N, Sangiorgi GM,
Violante A, Foraccio A, Montorfano M, Carlino M, Condorelli G, Ricciardelli B: Nephrotoxicity of low-osmolality
versus iso-osmolality contrast agents: Impact of N-acetylcysteine. Kidney Int 68: 2250 2255, 2005
10. Ergun I, Kenan K, Uruc I, Ekmekci Y, Canbakan B, Erden
I, Karatan O: The safety of gadolinium in patients with
stage 3 and 4 renal failure. Nephrol Dial Transplant 21:
697700, 2006
11. Isnard Bagnis C, Deray G, Baumelou A, Le Quintrec M,
Vanherweghem JL: Herbs and the kidney. Am J Kidney Dis
44(1): 111, 2004
12. Blowey DL: Nephrotoxicity of over-the-counter analgesics,
natural medicines, and illicit drugs. Adolesc Med Clin 16:
31 43, 2005
13. Wang IJ, Chen PC, Hwang KC: Melamine and nephrolithiasis in children in Taiwan. N Engl J Med 12; 360(11): 1157
1158, 2009
14. Van Vleet TR, Schnellmann RG: Toxic nephropathy: Environmental chemicals. Semin Nephrol 23: 500 508, 2003
15. Brewster UC, Perazella MA: A review of chronic lead
intoxication: An unrecognized cause of chronic kidney disease. Am J Med Sci 327(6): 341347, 2004
16. Yu CC, Lin JL, Lin-Tan DT: Environmental exposure to
lead and progression of chronic renal diseases: A four-year
prospective longitudinal study. J Am Soc Nephrol 15(4):
1016 1022, 2004
17. Jerkic M, Vojvodic S, Lopez-Novoa JM: The mechanism of
increased renal susceptibility to toxic substances in the
elderly. Part I. The role of increased vasoconstriction. Int
Urol Nephrol 32(4): 539 547, 2001
18. Evenepoel P: Acute toxic renal failure. Best Prac & Res Clin
Anaesthesiol 18: 3752, 2004
19. Singh NP, Ganguli A, Prakash A: Drug-induced kidney
diseases. JAPI 51: 970 979, 2003
20. Guo X, Nzerue C: How to prevent, recognize, and treat
drug-induced nephropathy. Cleve Clin J Med 69(4): 289
297, 2002
21. Wyatt CM, Arons RR, Klotman PE, Klotman ME: Acute renal
22.
23.
24.
25.
26.
27.
28.
29.
30.
31.
32.
33.
34.
35.
36.
37.
38.
failure in hospitalized patients with HIV: Risk factors and
impact on in-hospital mortality. AIDS 20: 561565, 2006
Lucena MI, Andrade RJ, Cabello MR, Hidalgo R, GonzalezCorrea JA, Sanchez de la Cuesta F: Aminoglycoside-associated nephrotoxicity in extrahepatic obstructive jaundice.
J Hepatol 22(2): 189 196, 1995
Markowitz GS, Perazella MA: Drug-induced renal failure:
A focus on tubulointerstitial disease. Clin Chimica Acta 351:
31 47, 2005
Perazella MA, Brown E: Electrolyte and acid-base disorders associated with AIDS: An etiologic review. J Gen
Intern Med 9(4): 232236, 1994
Stratta P, Lazzarich E, Canavese C, Bozzola C, Monga G:
Ciprofloxacin crystal nephropathy. Am J Kidney Dis 50(2):
330 335, 2007
Vega D, Maalouf NM, Sakhaee K: Increased propensity for
calcium phosphate kidney stones with topiramate use. Expert Opin Drug Saf 6(5): 547557, 2007
Wroe S: Zonisamide and renal calculi in patients with
epilepsy: How big an issue? Curr Med Res Opin 23(8):
17651773, 2007
Harty L, Johnson K, Power A: Race and ethnicity in the era
of emerging pharmacogenomics. J Clin Pharmacol 46: 405
407, 2006
Ciarimboli G, Koepsell H, Iordanova M, Gorboulev V,
Durner B, Lang D, Edemir B, Schroter R, Van Le T,
Schlatter E: Individual PKC-phosphorylation sites in organic cation transporter 1 determine substrate selectivity
and transport regulation. J Am Soc Nephrol 16:15621570,
2005
Ulrich CM, Bigler J, Potter JD: Non-steroidal anti-inflammatory drugs for cancer prevention: promise, perils and
pharmacogenetics. Nature Reviews 6: 130 140, 2006
Spanou Z, Keller M, Britschgi M, Yawalkar N, Fehr T,
Neuweiler J, Gugger M, Mohaupt M, Pichler WJ.: Involvement of drug-specific T cells in acute drug-induced
interstitial nephritis. J Am Soc Nephrol 17: 2919 2927,
2006
Izzedine H, Hulot JS, Villard E, Goyenvalle C, Dominguez
S, Ghosn J, Valantin MA, Lechat P, Deray AG: Association
between ABCC2 gene haplotypes and tenofovir-induced
proximal tubulopathy. J Infect Dis 194(11): 14811491, 2006
Cummings BS, Schnellmann RG: Pathophysiology of
nephrotoxic cell injury. In Diseases of the Kidney and Urogenital Tract, edited by Schrier RW, Philadelphia PA, Lippincott Williams & Wilkinson, 2001, pp 10711136
Kaloyanides GJ, Bosmans J-L, DeBroe ME: Antibiotic and
Immunosuppression-related renal failure. In Schrier RW
(ed): Diseases of the Kidney and Urogenital Tract, edited by
Schrier RW, Philadelphia PA, Lippincott Williams &
Wilkinson, 2001, pp 11371174
Aleksa K, Matsell D, Krausz K, Gelboin H, Ito S, Koren G:
Cytochrome P450 3A and 2B6 in the developing kidney:
Implications for ifosfamide nephrotoxicity. Pediatr Nephrol
20: 872 885, 2005
Nagai J, Takano M: Molecular aspects of renal handling of
aminoglycosides and strategies for preventing the nephrotoxicity. Drug Metab Pharmacokin 19: 59 70, 2004
Fanos V, Cataldi L: Renal transport of antibiotics and nephrotoxicity: A review. J Chemother 13: 461 472, 2001
Orbach H, Tishler M, Shoenfeld Y: Intravenous immuno-
Clin J Am Soc Nephrol 4: 12751283, 2009
39.
40.
41.
42.
43.
44.
45.
globulin and the kidneyA two-edged sword. Semin Arthritis Rheum 34: 593 601, 2004
Enomoto A, Endou H: Roles of organic anion transporters (OATS) and urate transporter (URAT1) in the pathophysiology of human disease. Clin Exp Nephrol 9: 195
205, 2005
Ciarimboli G, Ludwig T, Lang D, Pavenstadt H, Koepsell
H, Piechota HJ, Haier J, Jaehde U, Zisowsky J, Schlatter E:
Cisplatin nephrotoxicity is critically medicated via the human organic cation transporter 2. Am J Pathol 167: 1477
1484, 2005
Lang F: Regulating renal drug elimination. J Am Soc Nephrol 16: 15351536, 2005
Alexander BD, Wingard JR: Study of renal safety in amphotericin B lipid complex-treated patients. Clin Infect Dis.
40 Suppl 6: S414 S421, 2005
Falagas ME, Kasiakou SF: Nephrotoxicity of intravenous
colistin: A prospective evaluation. Crit Care 10:R27 113,
2006
Markowitz GS, Fine PL, Stack JI, Kunis CL, Radhaksrishnan, Palecki W, Park J, Nasr SH, Hoh S, Siegel DS, DAgati
VD: Toxic acute tubular necrosis following treatment with
zoledronate (Zometa). Kidney Int 64: 281289, 2003
Yang JC, Hayworth L, Sherry RM, Hwu P, Schwartzentruber DJ, Topalian SL, Steinberg SM, Chen HX, Rosenberg
SA: A randomized trial of bevacizumab, an anti-vascular
Drug Nephrotoxicity
46.
47.
48.
49.
50.
51.
52.
1283
endothelial growth factor antibody, for metastatic renal
cancer. N Engl J Med 349: 427 434, 2003
Eremina V, Jefferson JA, Kowalewska J, Hochster H, Haas
M, Weisstuch J, Richardson C, Kopp JB, Kabir MG, Backx
PH, Gerber HP, Ferrara N, Barisoni L, Alpers CE, Quaggin
SE: VEGF inhibition and renal thrombotic microangiopathy. N Engl J Med 358(11): 1129 1136, 2008
Sugimoto H, Hamano Y, Charytan D, Cosgrove D, Kieran
M, Sudhakar A, Kalluri R: Neutralization of circulating
vascular endothelial growth factor (VEGF) by anti-VEGF
antibodies and soluble receptor 1 (sFlt-1) induces proteinuria. J Biol Chem 278: 1260512608, 2003
Gurevich F, Perazella MA: Renal effects of anti-angiogenesis therapy: Update for the Internist Am J Med. 122:
322328, 2009
Bennett WM, Henrich WL, Stoff JS: The renal effects of nonsteroidal anti-inflammatory drugs: Summary and recommendations. Am J Kidney Dis 28(1 Suppl 1): S56 S62, 1996
Verhamme KM, Sturkenboom MC, Stricker BH, Bosch R:
Drug-induced urinary retention: Incidence, management
and prevention. Drug Saf 31: 373388, 2008
Brewster UC, Perazella MA: Proton pump inhibitors and
the kidney: Critical review. Clin Nephrol 68(2): 6572, 2007
Letavernier E, Bruneval B, Mandet C, Van Huyen JPD,
Peraldi MN, Helal I, Noel LH, Legendre C: High sirolimus
levels may induce focal segmental glomerulosclerosis De
Novo. Clin J Am Soc Nephrol 2: 326 333, 2007
Вам также может понравиться
- Condimente Home MadeДокумент22 страницыCondimente Home MadeCodruța Gabriela NedeleaОценок пока нет
- Urine Test Strips and Microscopy: Compendium of UrinalysisДокумент180 страницUrine Test Strips and Microscopy: Compendium of UrinalysisLory LaneОценок пока нет
- Nutrition Therapy For Chronic Kidney Disease-CRC Press (2012)Документ304 страницыNutrition Therapy For Chronic Kidney Disease-CRC Press (2012)Johnny Atman100% (2)
- Diabetes Complication LectureДокумент63 страницыDiabetes Complication LectureDoni MarthenОценок пока нет
- HBN 07-01 FinalДокумент34 страницыHBN 07-01 FinalYahya Hammoudeh100% (1)
- 2020 International Society of Hypertension Global Hypertension Practice GuidelinesДокумент48 страниц2020 International Society of Hypertension Global Hypertension Practice GuidelinesNicoleta Popa-FoteaОценок пока нет
- TBI Report To Congress Epi and Rehab-AДокумент72 страницыTBI Report To Congress Epi and Rehab-AEric GibsonОценок пока нет
- Brand Name Generic Name Indication and Contraindication Nursing Consideration Action of The Drug Dose and Administration Side EffectsДокумент2 страницыBrand Name Generic Name Indication and Contraindication Nursing Consideration Action of The Drug Dose and Administration Side EffectsCarla Dana GozumОценок пока нет
- Histopathology of Preclinical Toxicity Studies: Interpretation and Relevance in Drug Safety EvaluationОт EverandHistopathology of Preclinical Toxicity Studies: Interpretation and Relevance in Drug Safety EvaluationОценок пока нет
- Drug-Induced Liver Disease.Документ16 страницDrug-Induced Liver Disease.Dr. Ammar Khalil100% (1)
- MS Compre 2015A Ans KeyДокумент8 страницMS Compre 2015A Ans KeyPaul Lexus Gomez LorenzoОценок пока нет
- DialysisДокумент20 страницDialysisSiwani rai100% (1)
- For The Clinician: Pharmacology Behind Common Drug NephrotoxicitiesДокумент12 страницFor The Clinician: Pharmacology Behind Common Drug NephrotoxicitiesKarla HernándezОценок пока нет
- Drug Induced LiverДокумент8 страницDrug Induced LiverDita IndahОценок пока нет
- Medicinal Plants in The Protection and Treatment of Liver DiseasesДокумент16 страницMedicinal Plants in The Protection and Treatment of Liver DiseasesrocioОценок пока нет
- Neutrosec PPT BriefДокумент6 страницNeutrosec PPT BriefBenОценок пока нет
- Review: Hepatocellular Damage From Non-Steroidal Anti-Inflammatory DrugsДокумент5 страницReview: Hepatocellular Damage From Non-Steroidal Anti-Inflammatory Drugsshessy-jolycia-kerrora-3047Оценок пока нет
- Faught Et Al-2015-British Journal of Clinical PharmacologyДокумент9 страницFaught Et Al-2015-British Journal of Clinical PharmacologyHendra Wana Nur'aminОценок пока нет
- Chapter One AnuriДокумент16 страницChapter One AnuriIbitamuno SimeonОценок пока нет
- Pi Is 0272638623009320Документ18 страницPi Is 0272638623009320Sa7arОценок пока нет
- Hepatotoxicity Related To Anti-Tuberculosis Drugs: Mechanisms and ManagementДокумент13 страницHepatotoxicity Related To Anti-Tuberculosis Drugs: Mechanisms and ManagementkhacthuanprovipОценок пока нет
- We Are Intechopen, The World'S Leading Publisher of Open Access Books Built by Scientists, For ScientistsДокумент17 страницWe Are Intechopen, The World'S Leading Publisher of Open Access Books Built by Scientists, For ScientistsBipashwi Nath UpretyОценок пока нет
- Drugs and Kidney Dec 28 2012Документ43 страницыDrugs and Kidney Dec 28 2012Vin BitzОценок пока нет
- Drug Induced Tubular InjuryДокумент8 страницDrug Induced Tubular InjuryRania T. SabriОценок пока нет
- ChoiДокумент19 страницChoiLuciana RafaelОценок пока нет
- AKI DrugsДокумент4 страницыAKI DrugsPIH SHTОценок пока нет
- Drug-Induced Liver Toxicity and Prevention by Herbal Antioxidants: An OverviewДокумент18 страницDrug-Induced Liver Toxicity and Prevention by Herbal Antioxidants: An OverviewWarenda May LatifahОценок пока нет
- Effects of polyphenols on endothelial gene expressionДокумент6 страницEffects of polyphenols on endothelial gene expressionVivi GaviriaОценок пока нет
- Drug-Induced Liver DiseaseДокумент20 страницDrug-Induced Liver DiseaseNoreen ArshadОценок пока нет
- 2008 - Antituberculosis Drug-Induced Hepatotoxicity Concise Up-To-Date ReviewДокумент12 страниц2008 - Antituberculosis Drug-Induced Hepatotoxicity Concise Up-To-Date ReviewCarlos LuqueОценок пока нет
- Pathogenesis of Renal Failure in Multiple Myeloma: Any Role of Contrast Media?Документ10 страницPathogenesis of Renal Failure in Multiple Myeloma: Any Role of Contrast Media?Link BuiОценок пока нет
- Meyer 2010Документ24 страницыMeyer 2010deltanueveОценок пока нет
- Clin Infect Dis. 2004 Kaplowitz S44 8Документ5 страницClin Infect Dis. 2004 Kaplowitz S44 8Indra GunawanОценок пока нет
- International Journal of Basic & Clinical Pharmacology: IjbcpДокумент7 страницInternational Journal of Basic & Clinical Pharmacology: IjbcpDiego GomezОценок пока нет
- Antioxidants May Protect Kidneys by Reducing Oxidative StressДокумент3 страницыAntioxidants May Protect Kidneys by Reducing Oxidative StressZaid AhmadОценок пока нет
- Drug-Induced Nephrotoxicity: Cynthia A. Naughton, Pharmd, BCPS, North Dakota State University College of PharmacyДокумент8 страницDrug-Induced Nephrotoxicity: Cynthia A. Naughton, Pharmd, BCPS, North Dakota State University College of PharmacyAbdur Rachman Ba'abdullahОценок пока нет
- Drugs and The Liver - Metabolism and Mechanisms of Injury - UpToDate 2Документ17 страницDrugs and The Liver - Metabolism and Mechanisms of Injury - UpToDate 2hugo roblesОценок пока нет
- Drug-Induced Nephrotoxicity: A Review of Risk Factors and BiomarkersДокумент9 страницDrug-Induced Nephrotoxicity: A Review of Risk Factors and BiomarkersCecep Darwis MuttaqinОценок пока нет
- 24 OctДокумент38 страниц24 OctVenkatesh JaiswalОценок пока нет
- ATT Induced Hepatotoxicity: Dr. K. K. SharmaДокумент36 страницATT Induced Hepatotoxicity: Dr. K. K. SharmaSucharita Ray100% (1)
- Antituberculosis Treatment Hepatotoxicity MechanismsДокумент6 страницAntituberculosis Treatment Hepatotoxicity Mechanismsadilah fazliОценок пока нет
- Drug Induced Liver Toxicity (DILD)Документ39 страницDrug Induced Liver Toxicity (DILD)Surya Pratama100% (1)
- A Case Report On Adult Onset of Nephrotic Syndrome: Research ArticleДокумент2 страницыA Case Report On Adult Onset of Nephrotic Syndrome: Research ArticleTTОценок пока нет
- Drug-Induced Damage To Liver Cell StructureДокумент8 страницDrug-Induced Damage To Liver Cell StructureCentral Asian StudiesОценок пока нет
- Drug-Induced Hepatotoxicity: BackgroundДокумент13 страницDrug-Induced Hepatotoxicity: BackgroundrianiОценок пока нет
- Drug Induced Hepatitis With Anti-Tubercular Chemotherapy: Challenges and Difficulties in TreatmentДокумент5 страницDrug Induced Hepatitis With Anti-Tubercular Chemotherapy: Challenges and Difficulties in Treatmentmufqifitra160491Оценок пока нет
- Drug Induced Liver Diseases in The Elderly: Chandy GM, Chandy RGДокумент4 страницыDrug Induced Liver Diseases in The Elderly: Chandy GM, Chandy RGkazekiraОценок пока нет
- SAAM-6636-001: Industrial Toxicology - Winter 2019 Class 11: Toxicology of Specific Systems 1. Occupational Toxicology of The LiverДокумент10 страницSAAM-6636-001: Industrial Toxicology - Winter 2019 Class 11: Toxicology of Specific Systems 1. Occupational Toxicology of The Liverkriz0812Оценок пока нет
- Patfis DiliДокумент8 страницPatfis DiliHanum IndriОценок пока нет
- Nephrotoxic DrugsДокумент8 страницNephrotoxic DrugsAhmad Radhya DionandaОценок пока нет
- AIM2 Inflammasome Target for Kidney Disease TreatmentДокумент3 страницыAIM2 Inflammasome Target for Kidney Disease TreatmentSamana ZaynabОценок пока нет
- Drug Induce Hepatotoxicity 2014Документ14 страницDrug Induce Hepatotoxicity 2014Shinichi Conan HaibaraОценок пока нет
- Drug Induced LupusДокумент4 страницыDrug Induced LupusRohaniОценок пока нет
- Sindroma NefrotikДокумент36 страницSindroma NefrotikjustrudinОценок пока нет
- Antituberculosis: Drug-Induced Hepatiti: Risk Factors PR Ntion and ManagementДокумент7 страницAntituberculosis: Drug-Induced Hepatiti: Risk Factors PR Ntion and Managementmufqifitra160491Оценок пока нет
- Drug Induced NephrotoxicityДокумент13 страницDrug Induced NephrotoxicityAgnes BastonОценок пока нет
- First do no harmДокумент21 страницаFirst do no harmPHARMACY 2021Оценок пока нет
- 10 13040@ijpsr 0975-8232 53 690-02Документ14 страниц10 13040@ijpsr 0975-8232 53 690-02Luluil MunirohОценок пока нет
- Prescribing in Liver Disease Issue 2 Volume 32 Australian PrescriberДокумент6 страницPrescribing in Liver Disease Issue 2 Volume 32 Australian PrescriberAnonymous 9dVZCnTXSОценок пока нет
- (RENAL) Dental Management in Renal Failure Patients On DialysisДокумент8 страниц(RENAL) Dental Management in Renal Failure Patients On DialysisAna Emilia Holanda RolimОценок пока нет
- 122 134 Dili 2017Документ13 страниц122 134 Dili 2017Nico MancanegaraОценок пока нет
- Anticonvulsivantes Mecanismos de AccionДокумент23 страницыAnticonvulsivantes Mecanismos de Accionmondragon_cortesОценок пока нет
- Review Article: Treatment of Nonalcoholic Steatohepatitis in Adults: Present and FutureДокумент15 страницReview Article: Treatment of Nonalcoholic Steatohepatitis in Adults: Present and FutureEsha TwinkleОценок пока нет
- 1 Vol. 10 Issue 1 Jan 2019 IJPSR RE 2667Документ11 страниц1 Vol. 10 Issue 1 Jan 2019 IJPSR RE 2667Armando GemeОценок пока нет
- ATT Induced Liver Injury: Dr. Zubair Sarkar JR2, Deptt. of Medicine J.N.M.C.H., Aligarh Muslim UniversityДокумент61 страницаATT Induced Liver Injury: Dr. Zubair Sarkar JR2, Deptt. of Medicine J.N.M.C.H., Aligarh Muslim UniversityFahadKamalОценок пока нет
- Voican Et Al 2014 Antidepressant Induced Liver Injury A Review For CliniciansДокумент12 страницVoican Et Al 2014 Antidepressant Induced Liver Injury A Review For Cliniciansxiaonguyen02Оценок пока нет
- Which Psychotropic Medications Induce He PDFДокумент9 страницWhich Psychotropic Medications Induce He PDFnisastОценок пока нет
- Organophosphorus Insecticide Induced Hemorrhagic Pancreatitis - A Case ReportДокумент3 страницыOrganophosphorus Insecticide Induced Hemorrhagic Pancreatitis - A Case ReportIOSRjournalОценок пока нет
- Clin Pharmacy ADRДокумент36 страницClin Pharmacy ADRAnonymous DgPsK0oQОценок пока нет
- Diagnosis, Treatment, and Prevention of Typhoid Fever (WHO)Документ48 страницDiagnosis, Treatment, and Prevention of Typhoid Fever (WHO)Nina KharimaОценок пока нет
- Jurnal - PPT Total Hip ReplacementsДокумент11 страницJurnal - PPT Total Hip ReplacementsEric GibsonОценок пока нет
- 2015 ESC Guidelines for Infective Endocarditis ManagementДокумент54 страницы2015 ESC Guidelines for Infective Endocarditis ManagementEric GibsonОценок пока нет
- Tuberkulosis PDPI 2006Документ22 страницыTuberkulosis PDPI 2006Nuciana Siti AndriantiОценок пока нет
- Head Injury ManagementДокумент2 страницыHead Injury ManagementWaiwit ChotchawjaruОценок пока нет
- Hypoglycemic and Hepatoprotective Effects of Processed Aloe Vera Gel 2155 6156.1000303Документ6 страницHypoglycemic and Hepatoprotective Effects of Processed Aloe Vera Gel 2155 6156.1000303Eric GibsonОценок пока нет
- Tutorial 4 Facial NerveДокумент7 страницTutorial 4 Facial NerveAnimeAngelОценок пока нет
- A Comparision of The Effects of Aloe Barbadensis and Allium Albino RatsДокумент4 страницыA Comparision of The Effects of Aloe Barbadensis and Allium Albino RatsEric GibsonОценок пока нет
- Orthopaedic Journal - 4 Dan 5Документ5 страницOrthopaedic Journal - 4 Dan 5Eric GibsonОценок пока нет
- EAU Pocket Guidelines 215 Edn.Документ369 страницEAU Pocket Guidelines 215 Edn.Mohammed HusseinОценок пока нет
- EAU Pocket Guidelines 2012Документ405 страницEAU Pocket Guidelines 2012josephmhaasОценок пока нет
- Jurnal - PPT Total Hip ReplacementsДокумент11 страницJurnal - PPT Total Hip ReplacementsEric GibsonОценок пока нет
- Tumor Urogenital: Dr. Alvarino SPB SpuДокумент41 страницаTumor Urogenital: Dr. Alvarino SPB SpuDita Azzahra SupraptoОценок пока нет
- Ran TraumaДокумент11 страницRan TraumaAnnisa RahimОценок пока нет
- The Current State of Head and Neck Injuries in Extreme SportsДокумент6 страницThe Current State of Head and Neck Injuries in Extreme SportsEric GibsonОценок пока нет
- EAU Pocket Guidelines 2012Документ405 страницEAU Pocket Guidelines 2012josephmhaasОценок пока нет
- Clinical Review Frozen ShoulderДокумент4 страницыClinical Review Frozen ShoulderEric GibsonОценок пока нет
- Scale 0510Документ1 страницаScale 0510Eric GibsonОценок пока нет
- Head Injury A5Документ36 страницHead Injury A5Eric GibsonОценок пока нет
- Riu005004 0227Документ5 страницRiu005004 0227Eric GibsonОценок пока нет
- Trigeminal NeuralgiaДокумент6 страницTrigeminal NeuralgiaputrisarahОценок пока нет
- Effect of Flavonoids On Glutathione Level, Lipid Peroxidation and Cytochrome P450 CYP1A1 Expression in Human Laryngeal Carcinoma Cell LinesДокумент11 страницEffect of Flavonoids On Glutathione Level, Lipid Peroxidation and Cytochrome P450 CYP1A1 Expression in Human Laryngeal Carcinoma Cell LinesEric GibsonОценок пока нет
- Screening Dec 09Документ6 страницScreening Dec 09Eric GibsonОценок пока нет
- EFEKTIFITAS Sterilisasi Dan Efisiensi Media TanamДокумент14 страницEFEKTIFITAS Sterilisasi Dan Efisiensi Media TanamEric GibsonОценок пока нет
- ErlindaДокумент9 страницErlindaEric GibsonОценок пока нет
- Hepatoprotective Activity of Silybum Marianum and Cichorium Intybus Against Thioacetamide in RatДокумент5 страницHepatoprotective Activity of Silybum Marianum and Cichorium Intybus Against Thioacetamide in RatyigalbyОценок пока нет
- 1.beneficial Effects of Aloe Vera Leaf Gel Extract On Lipid Profile Status in Rats With Streptozotocin DiabetesДокумент9 страниц1.beneficial Effects of Aloe Vera Leaf Gel Extract On Lipid Profile Status in Rats With Streptozotocin DiabetesEric GibsonОценок пока нет
- Cystatin C As A Marker of GFR-History, Indications, and Future ResearchДокумент8 страницCystatin C As A Marker of GFR-History, Indications, and Future ResearchMaya RustamОценок пока нет
- Acidity Theory of AtherosclerosisДокумент46 страницAcidity Theory of Atherosclerosissecretary6609Оценок пока нет
- Chapter 12 Biochemistry and Clinical Pathology Complete Notes by Noteskarts Acc To ER20Документ6 страницChapter 12 Biochemistry and Clinical Pathology Complete Notes by Noteskarts Acc To ER20prat.medbooksОценок пока нет
- Health Pack For Chronic Renal FailureДокумент6 страницHealth Pack For Chronic Renal Failurekishore JoshiОценок пока нет
- Jurnal CKDДокумент5 страницJurnal CKDramadhaniDLОценок пока нет
- G1 Acute Glomerulonephritis Case AnalysisДокумент38 страницG1 Acute Glomerulonephritis Case AnalysisMELANIE GALEDOОценок пока нет
- Adeera Levin Ckd-Cv-Lipid-Sharp Web HandoutsДокумент12 страницAdeera Levin Ckd-Cv-Lipid-Sharp Web Handoutsmariatul fithriasariОценок пока нет
- Renal Learning OutcomesДокумент11 страницRenal Learning OutcomesBhuwan TandonОценок пока нет
- Approach To A Case of Chronic Kidney Disease: DR - Tanmay Tiwari MD, PDCC, Mnams Associate Professor KgmuДокумент43 страницыApproach To A Case of Chronic Kidney Disease: DR - Tanmay Tiwari MD, PDCC, Mnams Associate Professor KgmuMilind KothiyalОценок пока нет
- JNC 8 Hypertension Guideline AlgorithmДокумент2 страницыJNC 8 Hypertension Guideline Algorithmnaila inayatiОценок пока нет
- Total Summerized EMPA STUDIES 2Документ51 страницаTotal Summerized EMPA STUDIES 2EslamОценок пока нет
- Immune Dysfunction and Risk of Infection in CKD - 2019Документ8 страницImmune Dysfunction and Risk of Infection in CKD - 2019Lú VillalobosОценок пока нет
- CinacalcetДокумент4 страницыCinacalcetSorina HermanОценок пока нет
- Effectiveness and Outcomes of H-Isdn in Addition To Conventional Therapy in Acute Heart Failure Patients With Renal ImpairmentДокумент10 страницEffectiveness and Outcomes of H-Isdn in Addition To Conventional Therapy in Acute Heart Failure Patients With Renal ImpairmentIJAR JOURNALОценок пока нет
- Maharashtra University of Health Sciences Dissertation TopicsДокумент45 страницMaharashtra University of Health Sciences Dissertation TopicsAnil Subhash RathodОценок пока нет
- IgA Nephropathy: Autoimmune Kidney Disease ExplainedДокумент11 страницIgA Nephropathy: Autoimmune Kidney Disease Explainedsky.blueОценок пока нет
- Ada 2014Документ159 страницAda 2014Leito CzBf AlvaradoОценок пока нет
- Nephrotic Syndrome in ChildrenДокумент36 страницNephrotic Syndrome in ChildrenMalueth AnguiОценок пока нет
- RRT in ElderlyДокумент8 страницRRT in ElderlySupandy HasanОценок пока нет
- Deteksi Dini KomplikasiДокумент70 страницDeteksi Dini KomplikasiWiwik Puji LestariОценок пока нет
- Ada 2023Документ294 страницыAda 2023Ahmed Ashab FerdousОценок пока нет