Академический Документы
Профессиональный Документы
Культура Документы
07-Clerici Amputaion Adolescent
Загружено:
esbat07Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
07-Clerici Amputaion Adolescent
Загружено:
esbat07Авторское право:
Доступные форматы
See
discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/8206241
Clinical experience with psychological aspects
in pediatric patients amputated for
malignancies
ARTICLE in TUMORI JULY 2004
Impact Factor: 1.27 Source: PubMed
CITATIONS
READS
120
12 AUTHORS, INCLUDING:
Carlo Alfredo Clerici
Maura Massimino
Fondazione IRCCS Istituto Nazionale dei T
Fondazione IRCCS Istituto Nazionale dei T
66 PUBLICATIONS 247 CITATIONS
235 PUBLICATIONS 2,706 CITATIONS
SEE PROFILE
SEE PROFILE
Monica Terenziani
Filippo Spreafico
Fondazione IRCCS Istituto Nazionale dei T
Fondazione IRCCS Istituto Nazionale dei T
121 PUBLICATIONS 2,533 CITATIONS
132 PUBLICATIONS 1,535 CITATIONS
SEE PROFILE
SEE PROFILE
Available from: Filippo Spreafico
Retrieved on: 07 February 2016
Tumori, 90: 399-404, 2004
CLINICAL EXPERIENCE WITH PSYCHOLOGICAL ASPECTS
IN PEDIATRIC PATIENTS AMPUTATED FOR MALIGNANCIES
Carlo Alfredo Clerici1,2, Andrea Ferrari1, Roberto Luksch1, Michela Casanova1, Maura Massimino1,
Graziella Cefalo1, Monica Terenziani1, Filippo Spreafico1, Daniela Polastri1, Sergio Mapelli3, Primo Daolio3,
and Franca Fossati Bellani1
1
Pediatric Oncology Unit, Istituto Nazionale dei Tumori, Milan; 2Department of Psychology, University of Milan-Bicocca, Milan;
Cancer Surgery, Istituto Gaetano Pini, Milan, Italy
3Orthopedic
Aims and background: Amputation surgery in pediatric patients
suffering from malignant tumors is less common than in the
past, but has a great emotional impact on patients and their
families as well as on the medical team. Studies addressing
the psychological aspects of limb amputation in childhood
cancer are still relatively limited, and the results have sometimes been contradictory.
Methods: At the Pediatric Oncology Unit of the Istituto
Nazionale Tumori of Milan psychological support was provided to candidates for amputation and their families, involving
medical oncologists, a clinical psychologist, and social assis-
tants. Twenty-two patients were analyzed and 16 underwent
mutilating surgery.
Results: Different emotional reactions were observed. Surgery
proved to be easier to accept when the tumor caused pain
and functional loss. Specialist medical psychological support
was needed in case of defense mechanisms (eg, splitting and
projection) and depressive reactions evolving into isolation or
intolerance.
Conclusions: The reported experience could be helpful in providing adequate support to children with tumors requiring
mutilating surgery.
Key words: amputation, childhood cancer, psychosocial adjustment, quality of life.
Introduction
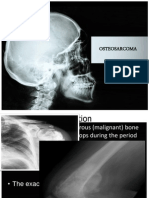
Various malignant childhood tumors (eg, osteosarcoma, Ewings sarcoma and, less frequently, soft tissue
sarcomas of the extremities) may make limb amputation
necessary as part of the treatment. The systematic use of
multidisciplinary integrated treatment in the last 20
years and the use of preoperative chemotherapy in
particular has reduced the number of patients undergoing amputation or dysarticulation: nowadays 5-20%
of the patients with osteosarcoma are submitted to amputation. However, when mutilating surgery is needed,
it induces considerable stress in patients and their families. The better chances of long-term survival for these
patients poses the problem of adapting to permanent
disability and its social and psychological consequences
in future adult life.
The aims of this study were to review the literature
on the psychological problems related to amputation in
pediatric oncology and on the type of support provided,
and to report on the psychological support provided at
the Pediatric Oncology Unit of the Istituto Nazionale
Tumori in Milan.
were observed. Suitable psychological support was provided for patients and their families.
In recent years, due to the increased request of evidence-based protocols, the necessity has arisen to
clearly define the techniques of intervention also in the
psychosocial setting. However, we believe it is very difficult to standardize into a protocol the procedures related to the support needed by these patients. Therefore, a
descriptive rather than a quantitative clinical method
was adopted. Nevertheless, some simple guidelines
were followed in our individually tailored approach to
the talks with patients and parents.
Support was given on two different levels:
Material and methods
1) The medical psychology level: this involved the
medical team (medical oncologists and nursing
staff), social assistants and teachers. In addition to
technical information, this first approach offered a
first line of emotional support and a restraint on the
anguish associated with cancer and the prospect of
amputation.
2) The clinical psychology level: provided by a physician specializing in clinical psychology, a member
of the medical team; this involved clinical talks and
psychotherapy sessions.
From January 1998 to June 2003 22 patients who
were candidates for limb amputation or disarticulation
It is essential to underline that the foundations of optimal communication with the family and the patient
Acknowledgments: This research was partly funded by the Associazione Bianca Garavaglia, which supported the medical psychological
assistance provided at the Pediatric Unit of the Istituto Nazionale Tumori of Milan.
Correspondence to: Carlo Clerici, MD, Pediatric Oncology Unit, Istituto Nazionale Tumori, Via G. Venezian 1, 20133 Milan, Italy.
Tel +39-02-23902588; fax +39-02-2665642; e-mail carlo.clerici@fastwebnet.it.
Received December 9, 2003; accepted March 30, 2004
400
should be laid from the very beginning of treatment, before the need for amputation is mentioned. During
every talk it is important that the physician test the degree of understanding of the previous information received by patients and parents.
Although a protocol seems unfeasible, adequate rules
concerning the setting, the time available and the organization of the talks are needed. Particular attention
should be paid to choosing a suitable setting where participants will not be disturbed; interruption by phone
calls, for example, should be avoided. In addition,
enough time should be taken for the talks, with the possibility of further talks, if necessary, to provide additional information. During the talks with parents and
patients it is important that alternative treatment options
and relative risks and benefits are presented to allow
adequate informed consent but in particular to make
sure that participants correctly understand all the details
of the situation. Talks with parents and with patients
need to be planned and performed separately.
The parents should be informed first about the need
for surgery and possibly be supported by psychological
interventions. When the parents have given their consent
to the proposed amputation, the patient must be informed and prepared for the surgical procedure. This is
done using different, individually tailored strategies depending on the patients age and maturity: the aim of
these talks is to help patients understand and convince
themselves of the need for this type of treatment.
Through talks with relatives, the specialist seeks to identify the patients personality traits, self-esteem and cognitive, social and physical abilities, the defense mechanisms they have used in previous situations, their present
coping skills and their need for specialist support after
surgery. In younger patients it is best to avoid mentioning the need for mutilating surgery too soon, since it
may cause unnecessary anguish and become intolerable.
It is brought up only a few days before surgery (usually,
2-3 days). This can be quite different for adolescents,
who might need more time to come to terms with the
clinical situation and the necessity of the mutilation.
Results
Twenty-two young patients were candidates for limb
amputation or disarticulation during the study period.
Table 1 shows the characteristics of the patients. Sixteen
underwent mutilating surgery consisting of lower limb
amputation above the knee in eight cases, below the
knee in five cases, coxofemoral disarticulation in one
case, interscapular-humeral disarticulation in one case,
and hemipelvectomy in one case. One patient did not
undergo the scheduled surgery due to unexpected disease progression detected at the preoperative workup.
Five adolescents (four girls, one boy; four osteosarcomas, one Ewings sarcoma) refused amputation. One
of them underwent conservative surgical treatment
(considered inadequate by our surgeons) elsewhere and
was lost to follow-up. The other four received radio-
CA CLERICI, A FERRARI, R LUKSCH ET AL
therapy as the only local treatment. At the time of writing, one patient was alive in complete remission (26
months from diagnosis), one was alive with stable disease (21 months from diagnosis), one relapsed locally at
20 months from diagnosis while on second-line treatment, and the last patient developed pulmonary metastases 24 months from diagnosis and died.
Below we describe a number of particular case reports.
Case 1
V. was a 15-year old girl from Sicily with an osteosarcoma of the right tibia. She helped out in a hairdressers shop and was very anxious about her physical
appearance. During the first hospital stay she worried
more about the side effects of treatment such as hair
loss and the risk of scarring than about the prognosis of
her disease. On clinical reconsideration following the
first cycles of chemotherapy, amputation was recommended. The patient defined the amputation as absolutely unacceptable. Despite several talks with
physicians, in agreement with her mother she decided to
consult various other clinical centers. Most of these
confirmed the choice of amputation; however, she eventually found a center that proposed conservative surgery
(considered inadequate by our surgeons).
In this case, excessive denial prevented the patient
from accepting the prospect of amputation, which
would probably have caused an identity crisis beyond
the patients emotional resources.
Case 2
When she was 12 years old, A. was treated with
chemotherapy and complete excision of an osteosarcoma of the left tibia. At age 15 she had local recurrence of
the disease requiring amputation. From the first talks
Table 1 - Characteristics of the patients
Candidates for amputation or disarticulation
22
Gender
12
Male
Female
10
Age
6-21 years (median, 15 years)
Histology
Primary osteosarcoma
18
1
Ewings sarcoma
1
Post-irradiation sarcoma
Rhabdomyosarcoma
1
Synovial sarcoma
1
Tumor site
Femur
11
Tibia
5
2
Pelvis
Humerus
1
1
Calcaneus
1
Soft tissue of calf
Soft tissue of foot
1
Patients who underwent mutilating surgery
16
Type of surgery
Lower limb amputation above the knee
8
5
Lower limb amputation below the knee
1
Coxofemoral disarticulation
Interscapular-humeral disarticulation
1
Hemipelvectomy
1
401
PSYCHOLOGICAL ASPECTS IN AMPUTATED PEDIATRIC PATIENTS
about surgery she surprised the physicians because she
appeared extremely relaxed about the idea of amputation. When her mother despaired and asked for psychological support, the patient invited her to calm down.
She underwent amputation and, surprisingly, adamantly
refused the planned chemotherapy, stating that it would
not add anything to what had already been done. She refused hospitalization and would not even talk to the doctors. Psychological counseling, suggested by managing
physicians and parents, initially took place at a hospital
fire exit. The patients maturity was assessed and the
conclusion was that she was capable of understanding
the risks associated with incomplete compliance with the
scheduled treatment. At a talk two weeks later she confirmed her decision; the medical team accepted it and A.
agreed to join a periodic follow-up program.
In this case the adolescent patient dramatically expressed the need to regain some degree of control over
her own life, opposing decisions made by others. Three
years later she was still disease-free, adapting very well
to her prosthesis.
Case 3
C. was a 12-year-old boy with an osteosarcoma of
the left leg. He was very fond of soccer, playing in a
team coached by his dad, and dreamed of becoming a
professional when he grew up. When amputation of the
leg below the knee was suggested, the patients reactions were dramatic. He accepted surgery only after numerous difficult talks. After surgery, he was depressed
for several months. Reorganization of existential planning took place only after the conclusion of postoperative chemotherapy: the patient quickly started rehabilitation and used a prosthesis. During a talk he enthusiastically reported, My dad bought me a radio-controlled
car. Its wonderful! I can take it apart and reassemble it
in no time. Im not that fond of soccer anymoreId
like to become a mechanic when I grow up.
This is a case of a process of adapting to amputation
that included a depressive phase followed by restructuring of the patients identity and a new investment for
the future. Unfortunately, the patient developed
metastatic pulmonary disease six months later; he underwent various chemotherapy regimens, but eventually
died of the disease.
Case 4
O. was a 17-year-old girl from Southern Italy. She
had a relapsing rhabdomyosarcoma of the left leg. The
disease developed when she was 14 and since then she
had been treated with numerous cycles of chemotherapy
and radiotherapy. She had left school several years before and she drew great comfort from her friends, particularly those of a folk group, with whom she danced
and sang. She paid a lot of attention to her physical appearance. The disease had progressed extensively, however, so much so that vast areas of muscle had been lost,
exposing the underlying bone and smelling putrid. The
diseased leg was kept well bandaged and hidden from
the patient beneath a sheet. When amputation was suggested the parents were very worried about how O.
would react and thought she would probably refuse
surgery. During her talks with the doctors, she appeared
greatly anguished and she refused to give her consent.
Further consultation at a different orthopedic oncology
center confirmed the need for amputation. In the meantime, she frequently asked the staff for details about the
disease and wanted to know what the amputation would
be like. A turning point was reached when O., in tears,
asked, How do you accept living without a leg? How
did the other patients make it?. In subsequent talks
with the medical staff O. was told about the experience
of other patients. She agreed to pick a date for surgery,
providing she could change her mind at any time. The
anguish of the first days was replaced by severe anxiety
prompted by the prospect of having to make a decision.
She was virtually unable to sleep and dwelt constantly
on what was ahead of her. The last night before surgery,
in the early hours of the morning, she wrote a farewell
letter to her leg and after that managed to get some
sleep without help. The next morning she gave her
consent and underwent the amputation. The postoperative course was satisfactory and the patient proudly exhibited the leg that is no longer there. She wanted her
letter to be read by the doctors and thought her experience might be useful to other patients.
In this patient, an excessively rigid denial developed
into the acceptance of her new situation only through a
certain degree of idealization.
Case 5
R. was a 13-year-old girl originally from Sicily with
an osteosarcoma of the right ankle. The disease required
amputation of the right foot. The patient suffered intense pain and functional loss. Talks between the patient
and the physicians were calm; the doctor emphasized
the advantages of surgery, ie, remission of pain and the
ability to walk again without the aid of a prosthesis. The
girl was also introduced to a young male patient who
had undergone the same amputation a few months earlier. The boy told her about his experience and removed
his prosthesis to show her how it worked: surgery was
seen as a possibility to be considered without untoward
anguish. Following surgery the patient rapidly adapted
to the prosthesis and experienced good functional recovery.
Discussion
This study describes our experience with children
and adolescents who require amputation, focusing on
the psychological aspects and the support provided by a
multidisciplinary team composed of medical oncologists, nurses, social assistants, teachers, and a medical
psychologist. Twenty-two consecutive patients were included in the study.
Our experience confirmed that talks were generally
followed by strong emotional reactions, associated with
402
a sense of impotence at being faced with a decision already taken by others and the feeling of being attacked.
First of all, the support measures aimed to ease these
painful feelings.
The proposed surgery seemed easier to accept when
the tumor caused significant pain and, more importantly, involved the functional loss of a limb. The sharing
of the decision might in this case be based on the perception of a clinical and physical improvement; the patient would be freed of the pain and of a useless
limb and might realistically see the prospects of
prompt rehabilitation and the possibility of functional
improvement.
Amputation was more difficult to accept if it was proposed after the patient had received preoperative
chemotherapy that had reduced the pain. The immediate
resistance to the idea of amputation was generally associated with a rejection of the efficacy of surgery (Even
cutting away the leg will be of no use), or an overestimation of the effects of initial treatment (What do you
mean? Amputating the leg is pointless, the therapy is effective, I feel much less pain and the swelling has gone
down.) hiding the anguish induced by the idea of severe
physical disability and its consequences in future life.
In our patients, specialist medical psychological support was needed when excessively rigid defence mechanisms, particularly denial, interfered with the patients
adaptation to reality and ability to express genuine consent or opposition to the surgical procedure. Coping
with amputation was generally a long-term process,
partly because the physical and psychological changes
were associated with a disruption of the patients family
and social structure.
From a psychodynamic point of view, we observed
the activation of defense mechanisms, such as splitting
and projection, with variable degrees of adaptation.
When splitting led to the diseased limb being invested
with all the persons positive and vital aspects, depressive reactions ensued (Without the leg I feel dead. Life
is not worth living in this state), evolving into social
isolation.
When the affected limb was associated with negative
aspects, an idealization process developed, followed by
reactions of omnipotence that might lead to underestimation of the functional loss (What was the use of
keeping the diseased leg? I feel much better now. Actually, I feel a lot stronger). It was important to make
sure that this did not evolve into a distorted sense of reality, with a diminished risk perception and inability to
ask for help.
Furious reactions sometimes develop, with an intolerance of healthy people, which may compromise family, social and emotional relationships. The body might
be felt as an object of curiosity. The uneasiness might
be aggravated by the patient projecting his intolerance
of the disability on others (They give me strange looks
because Im disabled; theres no respect for people who
suffer).
For patients adopting dysfunctional psychological
CA CLERICI, A FERRARI, R LUKSCH ET AL
defense mechanisms despite effective disease control,
the quality of life and social adaptability remain poor
and specialist psychotherapy might be needed.
The defense mechanisms adopted by patients may also influence future rehabilitation and prosthetic options.
If idealization prevails, the prosthesis is integrated into
the body image, facilitating omnipotence (With the artificial limb I can do everything, just like before, or better
still). Conversely, the prosthesis might be refused and
experienced as an obstacle to self-esteem, with the patient offering practical explanations, such as, I prefer
not to use the prosthesis ... Im used to getting along
with crutches. It takes me less time to get into the car.
Using the prosthesis makes me feel I have to depend on
something artificial from the outside to be able to walk
Our experience should be compared with similar
findings reported in the literature. It is of note that there
is an abundance of literature on the psychosocial aspects of adult patients undergoing traumatic (mainly
wartime) or vascular amputation, but such studies are
only marginally useful in understanding the psychological aspects associated with mutilating surgery in pediatric oncology. In adult trauma, surgery is usually performed in an emergency setting associated with intense
pain and involves subjects with a fully developed body
image. In childhood cancer, on the other hand, amputation is generally performed as elective surgery. It involves limbs with residual functional utility and symptom relief may have been achieved by neoadjuvant
chemotherapy. In addition, the body image is still incomplete in children and adolescents.
The first studies on the psychological aspects of mutilating cancer surgery date back roughly 30 years,
when childhood cancer began to receive specific treatment. Since then, psychological support for patients and
analyses of their quality of life have been instituted, involving staff with very different professional backgrounds (oncologists, psychiatrists, clinical or medical
psychologists, childhood neuropsychiatrists, professional nurses)1.
Notwithstanding the numerous possible approaches,
there are at least three common research areas: quality
of life, coping with the amputation, and the emotional
aspects of the disability.
The first area of research, concerning quality of life,
aims to address the effects of mutilating surgery on the
patients physical performance and subjective perception of well-being. Quantitative statistical methods have
been used to determine the incidence of psychopathological conditions and the resulting difficulties in social
adaptation factors that have greater affinity with biological studies than with psychological considerations.
The term quality of life has become popular in recent
years; it includes heterogeneous aspects, eg the normality of the subjects physiological parameters and
ability to perform daily activities, the presence of physical or psychopathological symptoms, and adaptation in
the social, school and family settings2.
Interest in the problems of patients and families cop-
403
PSYCHOLOGICAL ASPECTS IN AMPUTATED PEDIATRIC PATIENTS
ing with amputation stems mainly from cognitive-behavioral research. Since the 1960s various psychosocial
studies have been performed in pediatric oncology evaluating the aspects of coping with cancer. The greatest
difficulties arise from the lack of an unequivocal definition of this concept: Folkman describes coping as the
constantly changing cognitive and behavioral effort to
manage specific external or internal demands3. However, clinical experience generally suggests a continuity
in the same individual between the defense mechanisms
adopted in daily life and the coping skills used in lifethreatening situations.
Research into the emotional and affective aspects of
amputation is psychodynamic in origin and has generally used the case method. This has led to the development of intervention theories and methods dealing with
patients and families faced with amputation.
The general impression from our literature analysis is
that the studies on the psychological aspects of patients
undergoing amputation for childhood cancer are inadequate and their findings often contradictory. For example, there is no consensus on the psychological advantages of conservative surgery resulting in partial loss of
function compared with amputation4-6. A different line
of research investigated the role of psychological aspects in protracted phantom limb syndrome, discussing
how it could be influenced by emotional factors7-9. Various studies have focused on quality of life assessment
and psychosocial unrest in these patients5,10,11. Other
fields of mainly cognitive-behavioral research have attempted to define predictive factors in coping with amputation, including the severity of the disability, its perception by the patient and family, the presence of pain,
the patients gender and degree of intelligence5,12,13. The
association between the patients age at surgery and
their ability to cope with amputation is still controversial: various authors agree that younger patients run a
greater risk of interference with their personal evolution, others described prompt and satisfactory coping in
young amputated patients14,15. The time it takes to adapt
to amputation may vary; anxiety and depression may
persist long after surgery16. Few studies have investigated the dynamics of emotional adaptation in amputated
patients. The condition has been compared with mourning, marked by a succession of adaptive phases8.
Our experience has taught us that patients may adopt
different defense mechanisms, such as regression to a
previous phase of development or behavior designed to
elicit care and attract attention17. Denial is common,
particularly in the early stages, demanding an exhausting effort to cope with an inevitable reality and sometimes prompting a sense of anger. Carers therefore have
to deal with a substantial degree of aggressiveness,
which is sometimes self-inflicted, resulting in depression. Support aims partly at easing the anguish associated with the sense of helplessness and facilitating the
process of reorganizing future projects. Adolescents react dramatically to changes in their body image and to
having to depend more on others.
With regard to the psychological support required by
patients, it is of note that few studies have described
theoretical and practical models of psychological support for young patients undergoing amputation for cancer, partially due to the limited number of cases generally seen at a given cancer center. Interventional models
therefore stem from the results of psychodynamic clinical trials and research in the field of general pediatric
psycho-oncology. One of the main models is the emotional containment postulated by the psychoanalyst W
Bion18. Cancer and any related disability are true life
events that induce a strong sense of anguish in patients19; without a chance to share the experience, dwell
on it and use it to evolve further, the mind is invaded by
paralyzing anguish, confusion (beta elements) and the
onset of defense mechanisms, eg splitting, projection
and denial. Support measures aim to reduce the patients isolation, making them realize that anguish and
aggressiveness can be accepted and restrained in a relationship, and that these emotions are less dangerous
than pity and empathy. Various case reports describe
psychological support for amputated patients based on
this model, without it being expressly quoted.
After completing medical treatment, the patient faces
a change of perspective from curing a tumor to coping
with a disability. An identity crisis may develop, with
the need to formulate new projects for the future and
new life investments. During this phase, a condition defined by Schneider as the chronic patient triad may develop20,21 with dependence, regression and passivity if
the patient converts the chronic illness into a condition
that guarantees tangible primary benefits and secondary
psychological benefits, such as regaining a certain
amount of control within the family and care and attention that is mistakenly thought to arise from the presence of disease.
A commonly described aspect is the fear of disease
progression or relapse, partly because the mutilation is a
constant reminder of the original disease. Worry may
sometimes evolve into the so-called Damocles syndrome, unless adaptive defense mechanisms are triggered22.
Conclusions
The apparent contradictions and shortcomings of the
literature emphasize the well-known problems involved
in merging clinical and psychological knowledge23. Attempts to integrate the psychological sciences with
medical practice to produce quantitative observations
and statistically significant objective data may divert
our attention from know-how deriving from the tradition of clinical methodology.
It is an apparently obvious observation that any body
mutilation damages a patients integrity. Although difficult to define with scales and questionnaires, this must
always be borne in mind, both when recommending
surgery and during the patients rehabilitation and coping with the disability. The identity crisis may occur on
404
an intrapsychological level, revealing little on a behavioral level.
The patient-clinician relationship may help in the
stages immediately after suggesting surgery and in the
initial restructuring of the patients identity, essential to
the integration of the amputation experience into their
life history.
We feel that our experience could be useful for those
studying childhood cancer that involves mutilating
surgery. Psychological support must be provided at various stages and on different levels, by the whole treatment team and also by staff with specific psychological
competence. Its aims are to provide emotional containment for the anguish associated with the prospect of
amputation, to evaluate defense mechanisms adopted by
CA CLERICI, A FERRARI, R LUKSCH ET AL
the patient, and to treat maladaptive conditions, with the
final purpose of integrating the experience of disease
and amputation in a tolerable perspective of life. The
quality of life of amputated patients may vary greatly
in relation to their ability to develop and maintain an investment in life and their future prospects.
We cannot claim to propose a protocol but we do
want to suggest the need for a multidisciplinary approach at all centers dealing with pediatric patients with
diseases potentially requiring mutilating surgery. In our
experience the aid of staff with specific psychological
training is useful, although the leading part is played by
the oncologist, who must learn to develop proper communication skills. Such skills, however, are not easily
adaptable to a rigid framework or study protocol.
References
1. Van Dongen-Melman JE, Sanders Woudstra JAR: Psychosocial aspects of childhood cancer: a review of the literature.
J Child Psychol Psychiatr, 27: 145-180, 1986.
2. Leplge A, Hunt S: The problem of quality of life in medicine. JAMA, 278: 47-50, 1997.
3. Folkman S: Personal control and stress and coping processes:
a theoretical analysis. J Pers Soc Psychol, 46: 839-852, 1984.
4. Sugarbaker PH, Barofsky I, Rosenberg SA, Gianola FJ:
Quality of life assessment of patients in extremity sarcoma
clinical trials. Surgery, 91: 17-23, 1982.
5. Weddington WW Jr, Blindt Segraves K, Simon MA: Psychological outcome of extremity sarcoma survivors undergoing
amputation or limb salvage. J Clin Oncol, 10: 1393-1399, 1985.
6. Postma A, Kingma A, De Ruiter JH, Schraffordt Koops H,
Veth RP, Goeken LN, Kamps WA: Quality of life in bone tumor patients comparing limb salvage and amputation of the
lower extremity. J Surg Oncol, 51: 47-51, 1992.
7. Parkes CM: Reaction to the loss of a limb. Nurs Mirror Midwives J, 140: 36-40, 1975.
8. Parkes CM: Psycho-social transitions: comparison between
reactions to loss of a limb and loss of a spouse. Br J Psychiatry, 127: 204-210, 1975.
9. Fisher K, Hanspal RS: Phantom pain, anxiety, depression,
and their relation in consecutive patients with amputated
limbs: case reports. BMJ, 7135: 903-904, 1998.
10. Boyle M, Tebbi CK, Mindell ER, Mettlin CJ: Adolescent adjustment to amputation. Med Pediatr Oncol, 10: 301-312, 1982.
11. Tebbi CK, Petrilli AS, Richards ME: Adjustment to amputation among adolescent oncology patients. Am J Pediatr
Hematol Oncol, 11: 276-280, 1989.
12. Casari EF, Puncuh E: Amputare un arto: problemi psicologici
nellosteosarcoma delladolescente. In: Argomenti di psicooncologia, Comazzi AM, Morselli R (Eds), pp 98-106, CNR,
Milano, 1988.
13. Tebbi CK: Psychological effects of amputation in osteosarcoma. In: Osteosarcoma in adolescents and young adults: new
developments and controversies, Bennett Humphrey G,
Schraffordt Koops H, Molenaar WM (Eds), pp 39-44, Kluwer Academic Publishers, Boston, 1993.
14. Frantz CH: The child with an amputation. In: The child with
a handicap, Martmer EE (Ed), pp 56-61, Thomas, Springfield, 1959.
15. Vote PA, Burgers JM, van Putten WJ, van Dobbenburgh
OA: Amputations in children. Clinical indications and psychological implications. Arch Chir Neerl, 25: 427-433,
1973.
16. Simon JI: Emotional aspects of physical disability. Am J Occup Ther, 25: 408-410, 1971.
17. Siller J: Psychological concomitants of amputation in children. Child Develop, 31: 109-120, 1960.
18. Bion WR: Apprendere dallesperienza. Armando, Roma,
1972.
19. Di Cagno L, Gandione M, Massaglia P: Il contenimento delle
angosce come momento terapeutico nel lavoro con i genitori
di bambini con patologia organica grave. In: Dalle cure
materne allinterpretazione, Fava Vizziello G, Stern DN
(Eds), pp 115-142, Cortina, Milano, 1992.
20. Schneider PB: La psychologie du malade chronique. Folia
Psychopractica, pp 112-119, Hoffmann La Roche SA,
Basilea, 1978.
21. Comazzi AM: Riabilitazione psicologica sino alla fine. Acta
Biomedica de lAteneo Parmense, 63: 461-468, 1992.
22. Koocher GP, OMalley JE: The Damocles syndrome: psychosocial consequences of surviving childhood cancer. McGraw Hill, New York, 1981.
23. Sala G: La necessit di unopzione clinica per la ricerca psicologica in ambito medico. In: Ricerche di psicologia, CesaBianchi M, Bosio AC (Eds), Franco Angeli, 1996-1997.
Вам также может понравиться
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- I Support Palliative Care For A Better Quality of Life: Rizal Medical CenterДокумент1 страницаI Support Palliative Care For A Better Quality of Life: Rizal Medical Centeresbat07Оценок пока нет
- Enteral Nutrition in The Critically Ill Child: Science Supporting Better NutritionДокумент27 страницEnteral Nutrition in The Critically Ill Child: Science Supporting Better Nutritionesbat07Оценок пока нет
- Treating Alcoholism As A Chronic Disease: Approaches To Long Term Continuing CareДокумент15 страницTreating Alcoholism As A Chronic Disease: Approaches To Long Term Continuing Careesbat07Оценок пока нет
- Coronary SyndromeДокумент15 страницCoronary Syndromeesbat07Оценок пока нет
- Final NUHRA 2017-2022 PDFДокумент32 страницыFinal NUHRA 2017-2022 PDFesbat07Оценок пока нет
- Morphine, Oxygen, Nitrates, and Mortality Reducing Pharmacological Treatment For Acute Coronary Syndrome: An Evidence-Based ReviewДокумент13 страницMorphine, Oxygen, Nitrates, and Mortality Reducing Pharmacological Treatment For Acute Coronary Syndrome: An Evidence-Based Reviewesbat07Оценок пока нет
- Health 2013082314512668 PDFДокумент4 страницыHealth 2013082314512668 PDFesbat07Оценок пока нет
- Checklist of Requirements For Acupuncture Certification For Filipino Applicants - 06302015Документ2 страницыChecklist of Requirements For Acupuncture Certification For Filipino Applicants - 06302015esbat07Оценок пока нет
- Apgar Description 1Документ2 страницыApgar Description 1esbat07Оценок пока нет
- Capgar Description 1Документ4 страницыCapgar Description 1esbat07100% (1)
- Quick Reference - Requirements For NEW and RENEWAL S2Документ1 страницаQuick Reference - Requirements For NEW and RENEWAL S2esbat07100% (1)
- Youth Outcome QuestionnaireДокумент2 страницыYouth Outcome Questionnaireesbat07Оценок пока нет
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Review of Histological Grading SystemsДокумент20 страницReview of Histological Grading SystemsEzequiel Davi Dos SantosОценок пока нет
- Bone Tumors: Department of Pathology Anatomy Universitas PadjadjaranДокумент28 страницBone Tumors: Department of Pathology Anatomy Universitas PadjadjaranSabrina Indri WardaniОценок пока нет
- KONDROSARKOMAДокумент18 страницKONDROSARKOMAMangGun-gunGunawanОценок пока нет
- DR LI VS SOLIMANДокумент9 страницDR LI VS SOLIMANShiena Lou B. Amodia-RabacalОценок пока нет
- Bone TumorsДокумент62 страницыBone TumorsChinta Nur SilmiОценок пока нет
- S RL 31072018 Desmoplastic FibromaДокумент23 страницыS RL 31072018 Desmoplastic FibromaAnonymous bE4VegCcОценок пока нет
- Cartilage Forming Tumors Cartilage Forming TumorsДокумент53 страницыCartilage Forming Tumors Cartilage Forming TumorsFerryzal OkviandaОценок пока нет
- OsteosarcomaДокумент3 страницыOsteosarcomaStephen Jao Ayala UjanoОценок пока нет
- Case of OsteosarcomaДокумент25 страницCase of Osteosarcomadocs2009100% (3)
- OSTEOSARCOMAДокумент20 страницOSTEOSARCOMAAngel Gaoiran MolinaОценок пока нет
- Musawi 23Документ22 страницыMusawi 23Full MarksОценок пока нет
- Novel p53 Splicing Site Mutation in Li-Fraumeni-like Syndrome With OsteosarcomaДокумент5 страницNovel p53 Splicing Site Mutation in Li-Fraumeni-like Syndrome With OsteosarcomaMissy MishaОценок пока нет
- OsteosarcomaДокумент87 страницOsteosarcomaCob CornОценок пока нет
- Pediatric Solid TumorsДокумент43 страницыPediatric Solid Tumorsririliberti100% (1)
- Rubi Li Vs Sps. SolimanДокумент16 страницRubi Li Vs Sps. SolimanNicole SantosОценок пока нет
- Tumor OITE - 2012 2013 2014Документ254 страницыTumor OITE - 2012 2013 2014ICH Khuy100% (1)
- Kyle LiДокумент12 страницKyle Liapi-407846283Оценок пока нет
- F.09 BONE RADIOLOGY - Dr. GalangДокумент11 страницF.09 BONE RADIOLOGY - Dr. GalangDasha VeeОценок пока нет
- Pediatric Blood Cancer - 2023 - AbstractsДокумент600 страницPediatric Blood Cancer - 2023 - AbstractsAlonso GamirОценок пока нет
- OsteosarcomaДокумент25 страницOsteosarcomaDimas PrasetyoОценок пока нет
- MCQ 20Документ19 страницMCQ 20Old driverОценок пока нет
- Osteosarcoma 1Документ9 страницOsteosarcoma 1Md Ahsanuzzaman PinkuОценок пока нет
- Uk Guidelines SarcomaДокумент21 страницаUk Guidelines Sarcomachu_chiang_3Оценок пока нет
- 08 Pathology Orthobullets2017 PDFДокумент189 страниц08 Pathology Orthobullets2017 PDFdr_shafiq100% (1)
- Non-Odontogenic Tumors - Osteosarcoma, Ewing's Sarcoma, ChondrosarcomaДокумент38 страницNon-Odontogenic Tumors - Osteosarcoma, Ewing's Sarcoma, ChondrosarcomaDeepika barathi MОценок пока нет
- Final Examination in Radiology2015Документ13 страницFinal Examination in Radiology2015Ndor BariboloОценок пока нет
- SCFHS Diagnostic Radiology ExamsДокумент123 страницыSCFHS Diagnostic Radiology ExamsDr-Khaled Shaaban100% (1)
- Gaint Cell Lesions UPLOADДокумент176 страницGaint Cell Lesions UPLOADAkshayОценок пока нет
- Li v. Soliman-DigestДокумент3 страницыLi v. Soliman-DigestEloisa SalitreroОценок пока нет
- Official NBME 21Документ200 страницOfficial NBME 21Ily LagoniyaОценок пока нет