Академический Документы
Профессиональный Документы
Культура Документы
NSAID V Hydrocodone
Загружено:
andrew herringОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
NSAID V Hydrocodone
Загружено:
andrew herringАвторское право:
Доступные форматы
CLINICAL
THERAPEUTICSWOL.
23, NO. 2,200l
Efficacy and Tolerability of Celecoxib Versus
Hydrocodone/Acetaminophen
in the Treatment of Pain
After Ambulatory Orthopedic Surgery in Adults
Joseph S. Gimbel, MD, Andrew Brugger, MD,2 William Zhao, PhD,2
Kenneth M. Verburg, PhD,2 and G. Steven Geis, MD, PhD2
Arizona Research Center LLC, Phoenix, Arizona, and 2Research and Development,
Pharmacia Corporation, Skokie, Illinois
ABSTRACT
Background:
Current outpatient management of postoperative pain includes the use of
oral opioid analgesics or nonsteroidal anti-inflammatory
drugs; however, both types of
medications are associated with side effects that can limit their usefulness in the outpatient setting.
Objective: Two studies with identical protocols assessed the single- and multiple-dose
analgesic efficacy and tolerability of celecoxib, a specific cyclooxygenase-2
inhibitor, in
the treatment of acute pain after orthopedic surgery.
Methods: These were multicenter, randomized, placebo- and active-controlled,
doubleblind, parallel-group trials conducted between January and June 1998. Both consisted of
a single-dose assessment period (SDAP) and a multiple-dose assessment period (MDAP).
In the SDAP, patients who had undergone orthopedic surgery received a single oral dose
of celecoxib 200 mg, hydrocodone 10 mg/acetaminophen
1000 mg, or placebo within 24
hours after the end of anesthesia, with pain assessments conducted over the following 8hour period. In the MDAP, extending from 8 hours after the first dose of study medication up to 5 days, patients who had received 51 dose of rescue medication during the
SDAP continued on study medication (placebo recipients were rerandomized to active
treatment), which could be taken up to 3 times a day as needed.
Results: A total of 418 patients were enrolled in the 2 trials. During the SDAP, 141 patients received celecoxib, 136 received hydrocodone/acetaminophen,
and 141 received
placebo. During the MDAP, 185 patients received celecoxib and 18 1 received hydrocodone/
acetaminophen. When the combined data were analyzed, mean pain intensity difference
(PID) scores generally favored the active treatments over placebo from 1 to 6 hours (with
the exception of 1.5 hours) after dosing (P s 0.016) and favored celecoxib over the other
Accepted
for publication
December 20, 2000.
Printed in the USA. Reproduction
228
in whole or part is not permitted.
0149-2918/01/$19.00
J.S. GIMBEL ET AL.
treatments at 7 and 8 hours after dosing
(P < 0.001). The active treatments demonstrated superior
summed
PID scores
through 8 hours (P c O.OOl), significantly
shorter median times to onset of analgesia
(P < O.OS), and significantly longer median
times to first use of rescue medication
(P < 0.05). During the MDAP, more
hydrocodonelacetaminophen-treated
patients (20%) than celecoxib-treated patients
(12%) required rescue medication (P <
0.05), and the celecoxib group had significantly lower maximum
pain intensity
scores (P < 0.001, days 2-5), required
fewer doses of study medication (P 5 0.01,
days 3-5), and had superior scores on a
modified American Pain Society Patient
Outcome Questionnaire
(P zz 0.013). In
addition, a significantly lower proportion
of celecoxib-treated
patients experienced
adverse events (43%) compared
with
hydrocodone/acetaminophen-treated
patients (89%; P < 0.001).
Conclusions: Over 8 hours, patients
with moderate to severe pain after orthopedic surgery experienced
comparable
analgesia with single doses of celecoxib
and hydrocodonelacetaminophen.
Over a
5-day period, oral doses of celecoxib 200
mg taken 3 times a day demonstrated superior analgesia and tolerability compared
with hydrocodone
10 mg/acetaminophen
1000 mg taken 3 times a day. Most patients required no more than 2 daily doses
of celecoxib 200 mg for the control of
their postorthopedic surgical pain.
Key words: celecoxib, COX-2, opioid
analgesic,
postoperative
pain, clinical
trial. (Clin Thel: 2001;23:228-241)
INTRODUCTION
Outpatient orthopedic procedures are associated with moderate to severe postop-
erative pain, and ambulatory surgery requires effective control of postoperative
pain with oral analgesics after hospital discharge. L2 Current outpatient management
of postoperative pain includes the use of
oral opioid analgesics or nonsteroidal antiinflammatory
drugs (NSAIDs); however,
both types of medications are associated
with side effects that can limit their usefulness in the outpatient setting. Side effects of opioids, such as nausea, vomiting,
constipation,
respiratory depression, and
sedation, can be problematic in some patients.3 Although NSAIDs are effective alternatives to opioid medications for mild
to moderate pain after ambulatory surgical
procedures, they are associated with potentially serious side effects, including gastrointestinal (GI) hemorrhage and ulceration, and alteration of platelet function.4q5
Traditional NSAIDs exert their analgesic and anti-inflammatory
effects through
inhibition of the enzyme cyclooxygenase
(COX). Two isoforms of COX have been
identified-COX1, a constitutive form,
and COX-2, an inducible form that is associated with inflammation
and pain.6
Traditional NSAIDs inhibit both isozymes
by the same mechanism, resulting in nonselective, or concomitant,
inhibition
of
COX-1 and COX-2.6 In contrast, there is
in vitro, in vivo, biochemical, and clinical
evidence that celecoxib* is a specific inhibitor of COX-2. In vitro, celecoxib has
an -375-fold greater affinity for COX-2
than for COX-l.8 Inhibition
of COX-2
without inhibition of COX-1 provides analgesic and anti-inflammatory
activity
without concomitant impairment of normal COX- l-mediated
physiologic functions of the GI tract and platelets.9-13 Re*Trademark: Celebrex@
Skokie, Illinois).
(Pharmacia
Corporation,
229
CLINICAL THERAPEUTICS@
nal tolerability has also been demonstrated
in recent clinical studies. 14,i5
Clinical
trials with celecoxib
have
demonstrated
that it is effective in the
treatment of chronic pain in patients with
rheumatoid
arthritis
and osteoarthritis.16-18 In patients with moderate to severe postsurgical dental pain, celecoxib
dosed at 100 to 400 mg has been shown
to provide clinically significant pain relief
throughout an &hour postdose assessment
period.19 The studies described in this paper assessed the efficacy and tolerability
of celecoxib in the treatment of acute pain
after outpatient orthopedic surgery.
PATIENTS
AND METHODS
Recruitment was conducted between January and June 1998 by 24 investigators at
different sites in the United States. Male
and female patients aged 2 18 years were
eligible for the study if they had undergone
uncomplicated orthopedic surgery that required open manipulation
of bone with
periosteal elevation, including bunionectomy, anterior cruciate ligament repair,
open reduction and internal fixation of
long-bone fractures, laminectomy, or osteotomy for acquired or congenital malformations. Entry requirements also included
a baseline pain intensity score of ~45 mm
on a 100~mm visual analog scale (0 mm =
no pain, 100 mm = worst pain).
Eligible patients had to be in satisfactory
health, as determined by the investigator on
the basis of medical history and physical
examination. Women of childbearing potential were included if they were confirmed
to be using adequate contraception, were
not lactating, and had a negative pregnancy
test result at baseline. Written informed
consent was obtained from all patients before enrollment in the studies.
230
Patients were excluded if they had undergone total hip or knee replacement or
were scheduled for an additional surgical
procedure that might produce greater surgical trauma than the orthopedic procedure alone. Other exclusion criteria included cognitive impairment that would
preclude compliance with the protocol; inability to tolerate oral medication; a diagnosis of or treatment for esophageal, gastric, or duodenal ulceration; a history of
cancer or uncontrolled
chronic disease;
abnormalities
in aspartate transaminase,
alanine transaminase, blood urea nitrogen,
or creatinine levels ~1.5 times the upper
limit of the reference range; or a history of
hypersensitivity
to any NSAID, COX-2specific inhibitor, sulfonamide, opiate, or
analgesic that has cross-sensitivity
with
the medications used in these studies.
Study Design
The 2 randomized, placebo- and activecontrolled, double-blind,
parallel-group,
multicenter trials had identical protocols.
Both studies were divided into 2 assessment periods: the single-dose assessment
period (SDAP), defined as the L&hour period after the first dose of study medication, and the multiple-dose assessment period (MDAP), which began 8 hours after
the first dose of study medication and continued for up to 5 days.
In the SDAP, patients who met the inclusion criteria were randomly assigned to
1 of 3 study arms: celecoxib 200 mg, hydrocodone 10 mg/acetaminophen
1000 mg,
or placebo. Hydrocodone/acetaminophen,
an oral opioid analgesic indicated for the
relief of moderate to severe pain, was chosen as the active comparator to confirm
model sensitivity during the SDAP and to
allow blinding during the MDAI?* The
J.S. GIMBEL ET AL.
dosage of hydrocodone 10 mg/acetaminophen 1000 mg taken 3 times a day as
needed was selected for use during the
MDAP both to reflect the most common
prescribing pattern and to compare effcacy and tolerability with celecoxib 200
mg taken 3 times a day as needed. The 3times-daily dosing of celecoxib for postsurgical pain was in contrast to the onceand twice-daily regimens recommended
for conditions associated with chronic pain.
During the SDAP, patients received a
single dose of study medication within 24
hours after the end of anesthesia. Patients
could request rescue pain medication at
any time during the SDAP However, once
rescue medication was taken, no further
pain assessments were performed during
the SDAP. Patients remained at the treatment facility throughout the SDAP.
Patients who had received 51 dose of
rescue medication during the SDAP continued into the MDAP Those who had received hydrocodoneiacetaminophen
or
celecoxib during the SDAP were continued on the same active treatment in the
MDAP. Placebo was not used in the
MDAP. Those who had received placebo
during the SDAP were rerandomized to 1
of the 2 active treatments in the MDAP.
The MDAP began 8 hours after the initial dose of study medication and continued for up to 5 days. Once it was ascertained that patients were not experiencing
significant side effects and they had received and understood
instructions
for
completing
the pain assessments,
they
were discharged from the clinic. They were
allowed to begin remedication 8 hours after the initial dose of study medication and
repeat the dose as often as once every 8
hours as needed, up to 3 doses per day.
The medication could be taken with or
without food. Patients who required res-
cue medication
at any time during
MDAP were withdrawn immediately.
the
EfJicacy and Tolerability Assessments
The pain model used in these studies
was based on draft documents issued by
the US Food and Drug Administration.22.23 During the SDAP, patients assessed levels of pain intensity and pain
relief at baseline (hour 0) and every 15
minutes for the first hour, at hour 1.5, and
hourly from hours 2 through 8. Pain intensity was reported by patients on a scale
from 0 to 3, with 0 representing no pain
and 3 representing
severe pain; pain relief was reported on a scale from 0 to 4,
with 0 representing no relief and 4 representing complete relief. Time to the onset
of perceptible pain relief and time to the
onset of meaningful pain relief were assessed using 2 stopwatches started at the
time of taking the first study medication.
The patient was instructed to stop the first
stopwatch when pain relief was first perceived and the second stopwatch when
pain relief was first considered
to be
meaningful.
Measures of efficacy for the SDAP included (1) time-specific pain intensity difference (PID), derived by subtracting pain
intensity scores at a specified time point
from the baseline score; (2) summed PID
for the sum of the PID scores of all patients by treatment group through the first
8 hours (SPID-8); (3) time to onset of
analgesia, defined as time to the onset of
perceptible relief in patients who went on
to experience meaningful pain relief; and
(4) time to first use of rescue medication.
During the MDAP, assessments of maximum pain intensity and maximum pain
relief during the preceding 24 hours were
completed at bedtime on each full treat-
231
CLINICAL THERAPEUTICS
ment day for up to 5 days, and just before
taking rescue medication, if used. Patients
used a diary to record the number of doses
taken each day and the time each dose
was taken. A trained observer telephoned
patients each day to ensure compliance
and adequate pain relief.
A modified American
Pain Society
(APS) patient outcome questionnaire,
consisting of 3 relevant measures of pain
and 6 measures of pain interference from
the original questionnaire,24
was completed at the end of the MDAP. All 9 measures are based on a scale from 0 to 10,
with 0 signifying no pain or no interference and 10 signifying worst pain or worst
interference. Pain measures included pain
right now, worst pain in 4 days, and average level of pain in 4 days. Measures of
interference included the amount to which
pain interfered
with general activity,
mood, walking ability, relations with others, sleep, and enjoyment of life.
Measures of efficacy for the MDAP included (1) the proportion of patients who
completed the MDAP; (2) maximum pain
intensity in the past 24 hours for days 2 to
5; and (3) number of doses of study medication taken per day on days 2 to 5. Days
during the MDAP were counted using calendar days.
Tolerability
was assessed during the
SDAP and MDAP by determining the proportion of patients who reported rl adverse event and the overall frequency and
severity of adverse events.
Statistical Analysis
The modified intent-to-treat
(ITT) cohort included all patients in both studies
who took ~1 dose of study medication,
excluding those who dropped out <I hour
after dosing and those for whom 2 con-
232
secutive pain assessments were missing
within the first 2 hours of the study. All
statistical analyses for efficacy during the
SDAP were performed on data from the
modified ITT cohort. All statistical analyses for efficacy during the MDAP were
performed on data from all patients who
entered the MDAP.
Summary statistics for all randomized
patients in both studies were tabulated by
treatment group. Treatment groups were
compared using the chi-square test for categoric variables and 2-way analysis of
variance (ANOVA) with treatment effects
or the Wilcoxon rank sum test, as appropriate, for continuous variables.
Baseline
categoric
variables
were
compared to examine homogeneity
with
regard to surgical procedures and pain
intensity
ratings using the CochranMantel-Haenszel
test stratified by center.
Continuous baseline variables were tested
using 2-way ANOVA.
Time-specific PID and SPID-8 were analyzed by ANOVA, with treatment, center, and pain intensity at baseline (hour 0)
as factors. The Fisher protected leastsignificant-difference
multiple comparisons procedure was applied to the leastsquare treatment means.
Time to onset of analgesia and time to
use of rescue medication were analyzed
using survival analysis methods.25,26 For
time to onset of analgesia, patients were
censored at hour 8 if the second stopwatch
had not been stopped. For time to use of
rescue medication, patients who did not
receive rescue medication were considered censored at 8 hours. Patients who
dropped out and did not receive rescue
medication were censored at the time of
dropout. Patients who took rescue medication were assigned a time by subtracting the time the dose of study medication
J.S. GIMBEL ET AL,
was taken from the time at which rescue
medication was taken.
RESULTS
Single-Dose Assessment Period
Four hundred eighteen patients were
randomized to the SDAP treatment groups
and received rl dose of study medication,
including 141 patients receiving celecoxib
200 mg, 136 patients receiving hydroco-
Table I. Patient characteristics
during the 2 study periods.
Single-dose assessment period
Age (mean k SD), y
Sex, no. (%)*
Female
Male
Surgical procedure, no. (%)*
Bunionectomy
Anterior cruciate ligament repair
Fixation of long-bone fractures
Laminectomy
Osteotomy
Other orthopedic procedure
Other
Baseline pain intensity*
Categoric rating+
Moderate
Severe
Visual analog scale (mean f SD)
Multiple-dose assessment period
Age (mean f SD), y
Sex, no. (%)
Female
Male
NA = not applicable.
*In some categories, percentages
One patient receiving celecoxib
done 10 mg/acetaminophen
1000 mg, and
141 patients receiving placebo. Baseline
characteristics, including age, sex, type of
surgical procedure, and baseline pain intensity, were comparable between groups
(Table I).
More celecoxib patients completed the
SDAP than did hydrocodone/acetaminophen or placebo patients, and fewer celecoxib patients required rescue medication
during the SDAP (P < 0.05). Fifty-five
percent of celecoxib patients completed
Celecoxib
200 mg
(n = 141)
Hydrocodone 10 mg/
Acetaminophen 1000 mg
(n = 136)
Placebo
(n = 141)
47.4 + 15.0
43.9 f 15.2
45.2 + 16.0
84 (60)
57 (40)
85 (63)
51 (38)
84 (60)
57 (40)
19 (13)
19 (14)
13 (10)
28 (20)
7 (5)
9 (6)
93 (66)
0 (0)
12 (9)
0 (0)
11 (8)
81 (60)
12 (9)
0 (0)
13 (9)
3 (2)
7 (5)
78 (55)
88 (62)
52 (37)
65.5 f 16.5
98 (72)
38 (28)
62.8 f 16.5
83 (59)
58 (41)
65.5 k 15.3
46.6 + 15.2
44.4 2 16.1
NA
107 (58)
78 (42)
114 (63)
67 (37)
NA
NA
1 (1)
11 (8)
l(l)
do not total 100 due to rounding error.
bad no baseline pain intensity rating entered on the case report form.
233
CLINICAL THERAPEUTICS
group compared with the hydrocodonel
acetaminophen
and placebo groups (P <
0.001 at 7 and 8 hours). SPID-8 scores for
the active treatments were significantly superior to those for placebo (P < 0.001)
(Figure 2).
the SDAP period, compared
with 48% of
the hydrocodonelacetaminophen
group
and 36% of the placebo group. Two patients were withdrawn from the study during the SDAP because of adverse events,
and the remaining
patients were withdrawn because they received rescue medication. Details of patient disposition are
listed in Table II.
Onset of Analgesia
Compared
with placebo, the active
treatments demonstrated
superiority on
measures of onset of analgesia, including
the percentage
of patients
achieving
analgesia and the median time to onset of
analgesia.
Only 45% of the placebo
group achieved analgesia, compared with
64% and 75% of celecoxib patients and
hydrocodone/acetaminophen
patients, respectively (P < 0.05). The median times
to onset of analgesia in the celecoxib and
hydrocodonelacetaminophen
patients were
significantly shorter (35 and 31 minutes,
Pain Intensity DifSerence
The celecoxib and hydrocodone/acetaminophen treatments were superior to
placebo on most time-specific PID scores
(Figure 1). As early as 1 hour postdose,
mean PID scores significantly
favored
celecoxib and hydrocodonelacetaminophen (P s 0.016 at 2-6 hours, except at
1.5 hours in the celecoxib group). At 7 and
8 hours postdose, mean PID scores were
significantly
superior in the celecoxib
Table II. Patient disposition.
Celecoxib
200 mg
Hydrocodone 10 mg/
Acetaminophen 1000 mg
Placebo
Single-dose assessment period
(SDAP), no. (%)
All randomized SDAP patients
Withdrawal due to adverse event
Patients with ~1 event
Patients requiring 2 1 dose of rescue
medication
Multiple-dose assessment period
(MDAP), no. (%)*
All randomized MDAP patients
Withdrawal due to adverse event
Patients with rl event
Patients requiring 2 1 dose of rescue
medication
Lost to follow-up
Protocol noncompliance
*No patient received placebo during the MDAP.
234
141
136
141
l(1)
16 (11)
l(1)
37 (27)
0 (0)
20 (14)
0.002
62 (44)
70 (51)
90(64)
0.003
185
181
4 (2)
62 (34)
7 (4)
143 (79)
22 (12)
36 (20)
l(1)
l(1)
0 (0)
3 (2)
<O.OOl
0.05
J.S. GIMBEL ET AL.
A Celecoxib 200 mg
A Hydrocodone IO mg/acetaminophen
0 Placebo
01
1000 mg
,,,,I,,IIIIIlIII
0.5
1.5
2.5
3.5
4.5
5.5
6.5
7.5
Time (h)
Figure
1. Mean pain intensity difference (PID) scores over time during the single-dose
assessment period. The visual analog scale ranged from 0 to 3, with 3 representing the worst pain. *P c 0.05,
celecoxib and hydrocodone/acetaminophen
versus placebo; +P < 0.05,
celecoxib versus hydrocodone/acetaminophen
and
placebo.
I_
Celecoxib
200 mg
Hydrocodone 10 mg/
Acetaminophen 1000 mg
Placebo
Figure 2. Summed pain intensity difference scores through 8 hours (SPID-8) during the
single-dose assessment period. The visual analog scale ranged from 0 to 3, with 3
representing the worst pain. *P< 0.001, celecoxib and hydrocodone/acetaminophen
versus placebo.
235
CLINICAL THERAPEUTICS
respectively)
than in the placebo
(>8 hours, P < 0.05).
group
Use of Rescue Medication
The median times to first use of rescue medication
in the celecoxib
and
hydrocodone/acetaminophen
patients were
significantly longer (>8 hours and 7 hours
25 minutes, respectively)
than in the
placebo group (3 hours 52 minutes; P <
0.05).
Fifty-one
percent
of hydrocodonel
acetaminophen
patients
and 64% of
placebo patients required rl dose of rescue medication. In comparison, only 44%
of celecoxib
patients required rescue
medication,
despite the fact that more
celecoxib
patients
than hydrocodone/
acetaminophen
patients experienced severe versus moderate
baseline pain
(P = 0.003 between the 3 groups).
Multiple-Dose
Assessment
Period
Of the 418 patients randomized to the
SDAP, 366 continued to the MDAP. During this period, 185 patients were rerandomized to celecoxib (107 women, 78
men), including
129 who had received
celecoxib during the SDAP and 56 who
had received placebo; 181 patients were
rerandomized to hydrocodone/acetaminophen (114 women, 67 men), including 124
who had received hydrocodonelacetaminophen during the SDAP and 57 who had
received placebo. There were no significant between-group
differences in baseline characteristics, including age and sex
(Table I).
More celecoxib patients than hydrocodone/acetaminophen
patients
completed the MDAP and thus the overall
study, and fewer celecoxib patients required rescue medication
during the
236
(Table II). During this period, 12%
of celecoxib patients, compared with 20%
of the hydrocodonelacetaminophen
patients, required 2 1 dose of rescue medication (P = 0.05).
MDAP
Maximum Pain Intensity
At the end of each day of the MDAP,
the celecoxib group had significantly superior maximum
pain intensity
scores
compared
with the hydrocodone/acetaminophen group (P < 0.001, days 2-5)
(Figure 3).
Number of Daily Doses of Medication
On each day of the MDAP, the celecoxib group required fewer doses of
study medication than did the hydrocodonej
acetaminophen group. Celecoxib patients
required an average of 1.9 doses on day 1
and 1.3 doses on day 5, compared with an
average of 2.1 and 1.7 doses on the same
days in the hydrocodonelacetaminophen
group. The difference between groups was
significant on days 3 through 5 (P s 0.01).
By day 5,41% of patients in the celecoxib
group required no analgesic medication,
compared with 20% of patients in the
hydrocodonelacetaminophen
group.
American Pain Society Outcome
Measures
During the MDAP, 88% of celecoxib
patients
and 93% of hydrocodonel
acetaminophen patients reported that they
had experienced pain over the preceding
4 days. The celecoxib group had statistically superior scores on each of the 9 measures in the modified APS assessment
(P s 0.013) (Figure 4). The composite
pain interference score was significantly
more favorable in the celecoxib patients
(17.8) than in the hydrocodone/acetaminophen patients (24.8; P = 0.001).
J.S. GIMBEL ET AL.
3.0
c!
8 2.5
ul
.z?
g
2 2.0
&
.E
$ 1.5
E
z
3
1.0
5
s
a,
0.5
r
0
n Celecoxib 200 mg
0 Hydrocodone 10 mg/
acetaminophen 1000 mg
I
l
l-7
*
T
1
4
Day
Figure 3. Mean maximum pain intensity scores on days 2 through 5 during the multipledose assessment period. The rating scale ranged from 0 to 3, with 3 representing severe pain. *P < 0.001, celecoxib versus hydrocodone/acetaminophen.
W Celecoxib 200 mg
Pain right now
0 Hydrocodone 10 mg/
acetaminophen 1000 mg
Worst pain in 4 days
Average pain level over 4 days
General activity
Mood
Walking ability
Relations with others
Sleep
Enjoyment
of life
I
0
2
3
American
4
5
6
7
6
9
Pain Society Measure
10
Figure 4. Scores on American Pain Society measures at day 5. For each measure, the rating scale ranged from 0 to 10, with 10 representing worst pain or worst interference. *P 5 0.013, celecoxib versus hydrocodone/acetaminophen.
237
CLINICAL
Table III. Cumulative adverse events in the single- and multiple-dose
randomized patients.*
Adverse Event
Patients with ~1 event
Nausea
Headache
Somnolence
Vomiting
Dizziness
Dyspepsia
Dry mouth
Pruritus
Constipation
assessment periods, all
Celecoxib
200 mg
(n = 195)
Hydrocodone 10 mg/
Acetaminophen 1000 mg
(n = 194)
87 (45)
22 (11)
20 (10)
15 (8)
10 (5)
7 (4)
7 (4)
2 (1)
2 (1)
0 (0)
125 (64)
53 (27)
23 (12)
30 (15)
17 (9)
31 (16)
l(1)
5 (3)
6 (3)
6 (3)
*Totals include all patients who took 21 dose of active drug during either the single-dose
the multiple-dose assessment period.
Tolerability
Adverse events are listed in Table III.
During the SDAP, 1 patient from each of
the active-treatment groups withdrew due
to adverse events. The celecoxib group
had the lowest proportion of patients with
rl adverse event (1 l%), followed by the
placebo group (14%) and the hydrocodone/
acetaminophen
group (27%) (P = 0.002
between groups).
Across the SDAP and MDAP, patients
who had taken ~1 dose of celecoxib had a
significantly lower cumulative proportion of
adverse events than patients who had taken
B 1 dose of hydrocodonelacetaminophen
(43% vs 89%; P < 0.001) (Table III). The
most frequently reported adverse events in
the celecoxib group were nausea (1 l%),
headache (lo%), somnolence (8%), vomiting (5%), dizziness (4%), and dyspepsia
(4%). With the exception of dyspepsia (P =
0.068), all of these events were observed in
a greater proportion
of patients in the
238
THERAPEUTICS
P
<O.OOl
<O.OOl
0.018
<O.OOl
0.015
assessment
period or
hydrocodonelacetaminophen
group. The
most commonly reported adverse events
in the hydrocodonelacetaminophen
group
were nausea (27%; P < O.OOl), somnolence
(15%; P = O.OlS), dizziness (16%; P <
O.OOl), and constipation (3%; P = 0.015).
During the MDAP, 4 patients from the
celecoxib group and 7 patients from the
hydrocodonelacetaminophen
group withdrew because of adverse events. The celecoxib group had a lower proportion of
patients with 21 adverse event (33%) compared with the hydrocodone/acetaminophen group (78%; P < 0.001).
DISCUSSION
The results of these 2 randomized, double-blind, placebo- and active-controlled
trials demonstrate the clinical efficacy and
tolerability of celecoxib, a COX-2-specific
inhibitor, in the treatment of moderate to
severe pain after outpatient orthopedic
surgery. Onset of analgesia
occurred
J.S. GIMBEL ET AL.
within 1 hour of the first dose of celecoxib.
Pain relief was sustained through the 5
days of the study, as demonstrated on several measures of efficacy.
All single-dose analgesic efficacy variables favored a single dose of celecoxib
200 mg compared with placebo. The median onset of analgesia after a single dose
of celecoxib was 35 minutes. The magnitude of analgesic effect over the SDAP was
similar to that with hydrocodone/acetaminophen, and the majority of patients completed this S-hour period without requiring
another dose of analgesic medication.
During the MDAP, measures of efficacy
favored celecoxib over hydrocodone/acetaminophen. Over the 5-day period, 80% to
90% of celecoxib patients experienced satisfactory pain relief while taking an average daily dose of 200 mg twice daily without additional rescue medication. These
data are consistent with the results of clinical trials in osteoarthritis, in which celecoxib 100 and 200 mg twice daily produced significant relief of acute flare pain
from osteoarthritis of the hip* and kneel6
within 1 day of the start of treatment and
demonstrated continuing efficacy for the
remaining 6 days of the assessment.
The present study compared the tolerability profile of celecoxib 200 mg taken 3
times a day as needed with that of a similar
regimen of a mild opiate combination, hydrocodone 10 mg/acetaminophen 1000 mg.
During both assessment periods and cumulatively, celecoxib patients experienced significantly fewer side effects. Cumulatively,
twice as many hydrocodone/acetaminophen
patients reported 81 adverse effect (eg, nausea, somnolence, dizziness, constipation).
Cumulatively,
nausea was reported -2.5
times more frequently and dizziness 4 times
more frequently in patients treated with
hydrocodonelacetaminophen
than with
celecoxib. Approximately
twice as many
hydrocodone/acetaminophen-treated
patients reported vomiting and somnolence.
Constipation was reported by hydrocodone/
acetaminophen-treated
patients but not
celecoxib-treated patients. Opioids such as
hydrocodone are known to have physiologic properties that alter gastric motility.
As a class, they also are known to produce
respiratory depression, alteration in mood,
physical tolerance, and dose-dependent
bradycardia.28
The conditions of the MDAP parallel
actual practice after ambulatory orthopedic
surgery. Specifically, after undergoing a
variety of outpatient procedures, including
laminectomy, arthroscopy, and foot surgery,
patients were discharged home and allowed
to take blinded study medication on an asneeded basis up to 3 times a day. If this
was not sufficient to control their pain, they
were allowed to take rescue medication,
but their participation in the study was discontinued once they did so. A majority of
patients required only 2 daily doses of celecoxib 200 mg to manage acute postoperative pain, and the results suggest that the
majority achieved satisfactory pain control
with few adverse events.
CONCLUSIONS
In this study, celecoxib 200 mg was well
tolerated taken in single oral doses as
needed up to 3 times a day over a 5-day
period. The single dose displayed analgesic efficacy in patients with moderate to
severe pain after outpatient orthopedic
surgery. Taken at a minimum interval of 8
hours over a 5-day period, celecoxib 200
mg displayed analgesic efficacy similar or
superior to that of a similar regimen of
hydrocodonelacetaminophen.
Most patients required only twice-daily doses of
239
CLINICAL THERAPEUTICS
celecoxib 200 mg to control their acute
pain after orthopedic surgery.
ACKNOWLEDGMENTS
The following investigators participated in
this trial: Steven Belknap, MD, Peoria, Illinois; Nelson G. Botwinick, MD, New York,
New York; O.F. Cannon, Jr., MD, Ocala,
Florida; Stephen E. Daniels, DO, Austin,
Texas; Christopher M. Fallows, DO, Inverness, Florida; Joseph S. Gimbel, MD, Glendale, Arizona; Stephen F. Gordon, MD, Atlanta, Georgia; Marc Z. Hammerman, MD,
Hollywood, Florida; Stephen J. Hawes, Jr.,
MD, Charlotte, North Carolina; W. John
Henry III, MD, Greer, South Carolina; Thurman E. Hunt, MD, Newark, New Jersey;
Michael Kentor, MD, Pittsburgh, Pennsylvania; Alan J. Kivitz, MD, Altoona, Pennsylvania; Richard M. Konsens, MD, Orlando, Florida; Leonard I. Kraut, MD,
Lakewood, New Jersey; Paul Lunseth, MD,
Tampa, Florida; Daryl K. MacCarter, MD,
Denver, Colorado; Margaret Michalska,
MD, Chicago, Illinois; Stephen H. Miller,
MD, Las Vegas, Nevada; Robert J. Noveck,
MD, PhD, New Orleans, Louisiana; Jon
Sanchez, MD, Springfield, Montana; Paul
F. Siami, MD, Evansville, Indiana; Randall
R. Stoltz, MD, Evansville, Indiana; and B.
King Tipton, MD, Fort Myers, Florida.
REFERENCES
1. Meridy HW. Criteria for selection of ambulatory surgical patients and guidelines
for anaesthetic management: A retrospective study of 1553 cases. Anesth Analg.
1982;61:921-926.
2. Chung F, Ritchie E, Su J. Postoperative
pain in ambulatory surgery. Anesth Analg.
1997;85:808-8 16.
240
3. Hopkins D, Shipton EA, Potgieter D, et
al. Comparison of tramadol and morphine
via subcutaneous PCA following major
orthopaedic surgery. Can JAnaesth. 1998;
4k435-442.
4. Joris J. Efficacy of nonsteroidal
antiinflammatory drugs in postoperative pain.
Acta Anaesthesiol Belg. 1996;47: 115-123.
5. Borda IT, Koff RS, eds. NSAIDS: A Profile of Adverse Efsects. Philadelphia:
ley & Belfus; 1992.
Han-
6. Vane JR. Inhibition of prostaglandin
synthesis as a mechanism of action for the aspirin-like drugs. Nature. 197 I;23 1:232-
235.
7. Verburg KM, Maziasz TJ, Weiner E, et al.
COX-2 specific inhibitors: Definition of a
new therapeutic concept. Am J Ther. In
press.
8. Penning TD, Talley JJ, Bertenshaw SR, et
al. Synthesis and biological evaluation of
the 1,5-diarylpyrazole class of cyclooxygenase-2 inhibitors: Identification of 4-[5-(4methylphenyl)-3-(trifluoromethyl)-lH-pyrazol-1-yllbenzenesulfonamide
(SC-58635,
celecoxib). J Med Chem. 1997;40: 13471365.
9. Dewitt DL, Meade EA, Smith WL. PGH
synthase isoenzyme selectivity: The potential for safer nonsteroidal antiinflammatory
drugs. Am J Med. 1993;95:40%448.
10. Bensen WG, Zhao SZ, Burke TA, et al.
Upper gastrointestinal tolerability of celecoxib, a COX-2 specific inhibitor, compared to naproxen and placebo. J Rheumatol. 2000;27: 1876-l 883.
11. Goldstein JL, Silverstein FE, Agrawal
NM, et al. Reduced risk of upper gastrointestinal ulcer complications with celecoxib, a novel COX-2 inhibitor. Am J Gastroenterol. 2000;95: 1681-1690.
J.S. GIMBEL ET AL.
12. Leese PT, Hubbard RC, Karim A, et al.
Effects of celecoxib, a novel cyclooxygen-
ase-2 inhibitor, on platelet function in
healthy adults: A randomized, controlled
trial. J Clin Phannacol. 2000;40: 124-l 32.
in non13. Singh G. Recent considerations
steroidal anti-inflammatory drug gastropathy. Am J Med. 3998;105:313-38s.
14. Whelton A, Maurath CJ, Verburg KM,
Geis GS. Renal safety and tolerability of
celecoxib, a novel cyclooxygenase-2
inhibitor. Am J The,: 2000;7:159-175.
15. Whelton A, Schulman G, Wallemark C, et
al. Effects of celecoxib and naproxen on
renal function in the elderly. Arch Intern
Med. 2000;160:1465-1470.
16. Bensen WG, Fiechtner JJ, McMillen JI, et
al. Treatment of osteoarthritis with celecoxib, a cyclooxygenase-2
inhibitor: A
randomized controlled trial. Mayo Clin
Proc. 1999;74:1095-1105.
17. Simon LS, Weaver AL, Graham DY, et al.
Anti-inflammatory
and upper gastrointestinal effects of celecoxib in rheumatoid
arthritis: A randomized controlled trial.
JAMA. 1999;282:1921-1928.
18. Williams GW, Ettlinger RE, Ruderman
EM, et al. Treatment of osteoarthritis with
a once-daily dosing regimen of celecoxib:
A randomized
controlled
trial. J Clin
Rheumatol. 2000;6:65-74.
19. Hubbard RC, Mehlisch DR, Jasper DR, et
al. SC-58635, a highly selective inhibitor
of COX-2, is an effective analgesic in an
acute post-surgical pain model. J Invest
Med. 1996;44;293A. Abstract.
20. VicodinTM (hydrocodone 5 mg/acetaminophen 500 mg) tablets prescribing information. Physicians Desk Reference@.
Montvale, NJ: Medical Economics; 1999:
1366-1367.
21. Physician Drug Diagnosis Audit. Newtown, Pa: Scott-Levin Inc; 1999.
22. Presentation of Eficacy Results of SingleDose Analgesics for Studies Using Acute
Pain Models. FDA Draft Document, June
1997.
23. Guideline for the Clinical Evaluation of
Analgesic Drugs. US Department of Health
and Human Services, US Food and Drug
Administration, Revised December 1992.
24. American Pain Society Quality of Care
Committee. Quality improvement guidelines for the treatment of acute pain and
cancer pain. JAMA. 1995;274:1874-1880.
25. Miller RG. Survival Analysis. New York:
John Wiley & Sons; 1981.
26. Simon R, Lee YJ. Nonparametric contidence limits for survival probabilities and
median survival time. Cancer Treat Rep.
1982;66:3742.
27. Sunshine A, Moskowitz R, Woods E, et al.
Efficacy of celecoxib in treating acute flare
pain in osteoarthritis of the hip. In: Program and abstracts of the 9th World Congress on Pain; August 22-27, 1999; Vienna, Austria. Abstract 248.
28. Ferrante FM. Principles of opioid pharmacotherapy: Practical implications of basic mechanisms. J Pain Symptom Manage.
1996;11:265-273.
Address correspondence to: Joseph S. Gimhel, MD, Medical Director, Arizona Research
Center LLC, 2525 W. Greenway Road, Suite 114, Phoenix, AZ 85023. E-mail: arizrc@aol.com
241
Вам также может понравиться
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Highland Guidelines - LDK 2013-2-15Документ3 страницыHighland Guidelines - LDK 2013-2-15andrew herringОценок пока нет
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- AclsДокумент20 страницAclsqueennita69100% (4)
- K Opiods For Pain BupДокумент2 страницыK Opiods For Pain Bupandrew herringОценок пока нет
- Natural Anxiety CuresДокумент93 страницыNatural Anxiety Curesd_probst5098100% (1)
- Roux 2013Документ7 страницRoux 2013andrew herringОценок пока нет
- Buprenorphine 2016-7-18Документ1 страницаBuprenorphine 2016-7-18andrew herringОценок пока нет
- Original Article: Serratus Plane Block: A Novel Ultrasound-Guided Thoracic Wall Nerve BlockДокумент7 страницOriginal Article: Serratus Plane Block: A Novel Ultrasound-Guided Thoracic Wall Nerve Blockandrew herringОценок пока нет
- Rib Fracture W: PecsДокумент8 страницRib Fracture W: Pecsandrew herring100% (1)
- Rib Fracture SerratusДокумент3 страницыRib Fracture Serratusandrew herring100% (1)
- Ultrasound-Guided Block of TheДокумент6 страницUltrasound-Guided Block of Theandrew herringОценок пока нет
- Intravenous Lidocaine To Treat Postoperative Pain : Lidocaína Intravenosa No Tratamento Da Dor Pós-OperatóriaДокумент6 страницIntravenous Lidocaine To Treat Postoperative Pain : Lidocaína Intravenosa No Tratamento Da Dor Pós-Operatóriaandrew herringОценок пока нет
- Herring ED Intractable Abdominal pain-N+VДокумент1 страницаHerring ED Intractable Abdominal pain-N+Vandrew herringОценок пока нет
- 3.2.16.highland Emergency Medicine Journal Club Methods.2Документ2 страницы3.2.16.highland Emergency Medicine Journal Club Methods.2andrew herringОценок пока нет
- Ketamine As Rescue Treatment FДокумент8 страницKetamine As Rescue Treatment Fandrew herringОценок пока нет
- Dex For Dental Pain & SwellingДокумент7 страницDex For Dental Pain & Swellingandrew herring100% (1)
- Nej MR A 1511480Документ9 страницNej MR A 1511480Tohari Masidi AminОценок пока нет
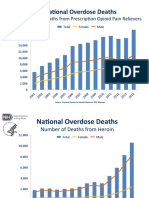
- OPR - Heroin DeathsДокумент2 страницыOPR - Heroin Deathsandrew herringОценок пока нет
- CVS Action Plan v2Документ1 страницаCVS Action Plan v2andrew herringОценок пока нет
- Ultrasound Guided Interventional Procedures In.13Документ14 страницUltrasound Guided Interventional Procedures In.13andrew herring100% (1)
- Ultrasound Guided Interventional Procedures In.4Документ13 страницUltrasound Guided Interventional Procedures In.4andrew herringОценок пока нет
- Special Articles: Awake Intubation Intubation After Induction of General AnesthesiaДокумент1 страницаSpecial Articles: Awake Intubation Intubation After Induction of General AnesthesiaOKE channelОценок пока нет
- CHEMOTHERAPYДокумент28 страницCHEMOTHERAPYDwi CahyaОценок пока нет
- Fast Hugs MaidenДокумент8 страницFast Hugs MaidenPriscila Navarro MedinaОценок пока нет
- MHS 6401Документ5 страницMHS 6401Delelegn EmwodewОценок пока нет
- Does Klonopin (Clonazepam) Work For MigrainesДокумент4 страницыDoes Klonopin (Clonazepam) Work For MigrainesTooba SiddiquiОценок пока нет
- Paediatric Drug DosingДокумент18 страницPaediatric Drug DosingDR JAMAL WARISОценок пока нет
- America Stock Viernes 01-07-2022Документ41 страницаAmerica Stock Viernes 01-07-2022Rosa Irma GaunaОценок пока нет
- Treatment of Schizophrenia and Management of Drug SideДокумент83 страницыTreatment of Schizophrenia and Management of Drug SideAbelОценок пока нет
- Sample NURSING PROCESS IN PHARMACOLOGY PDFДокумент7 страницSample NURSING PROCESS IN PHARMACOLOGY PDFVic Intia PaaОценок пока нет
- 2020 Conference PaperДокумент2 страницы2020 Conference PaperHealthcare Pro LearningОценок пока нет
- Clinical Pharmacology of Antibiotics - PMCДокумент19 страницClinical Pharmacology of Antibiotics - PMCJosette LeyvaОценок пока нет
- Antibiotic Cross-Sensitivity ChartДокумент1 страницаAntibiotic Cross-Sensitivity ChartChing JuОценок пока нет
- IMN1207 McGillActiveProtocolsДокумент11 страницIMN1207 McGillActiveProtocolsapi-3714923Оценок пока нет
- Med GuideДокумент7 страницMed GuideEko YuliantoОценок пока нет
- AclsДокумент2 страницыAclsEman ElzeftawyОценок пока нет
- Pricelist ErelaДокумент1 страницаPricelist ErelaMutia FarmaОценок пока нет
- 11.drug StudyДокумент1 страница11.drug StudyFreisanChenMandumotanОценок пока нет
- Emergency Responder Bag: QTY Unit Item Name Intubation SetДокумент3 страницыEmergency Responder Bag: QTY Unit Item Name Intubation SetferdyОценок пока нет
- Chapter 15 Treatment of Psychological DisordersДокумент52 страницыChapter 15 Treatment of Psychological DisordersChehekОценок пока нет
- HOSPITAL Past PapersДокумент6 страницHOSPITAL Past PapersMr nobodyОценок пока нет
- Az Essential RX ListДокумент141 страницаAz Essential RX ListAbdullah HamdanОценок пока нет
- Rusan Pharma Product ListДокумент4 страницыRusan Pharma Product ListSanjay SharmaОценок пока нет
- Meet 4. Penyiapan Obat SitostatikaДокумент47 страницMeet 4. Penyiapan Obat SitostatikaChoirun NisaОценок пока нет
- One Compartment Open Model IV Bolus: DR Mohammad IssaДокумент79 страницOne Compartment Open Model IV Bolus: DR Mohammad IssaPronoy SahaОценок пока нет
- Alevo Alkem (Ulticare) (Levofloxacin) : Strength Presentation PriceДокумент21 страницаAlevo Alkem (Ulticare) (Levofloxacin) : Strength Presentation Pricepathan mohidОценок пока нет
- MCHДокумент21 страницаMCHmoubarkОценок пока нет
- Strategy Increase SellДокумент7 страницStrategy Increase SellPrashun Shekhar SrivastavaОценок пока нет
- 2018 I.V. Push Administration of Medications Reconstituted With 0.9% NSДокумент2 страницы2018 I.V. Push Administration of Medications Reconstituted With 0.9% NSDaniela MéndezОценок пока нет