Академический Документы
Профессиональный Документы
Культура Документы
The Roche AMPLICOR® HPV Test As A Primary Screen For HPV in Cervical Specimens Collected in ThinPrep® and SurePath™ Liquid Cytology Media
Загружено:
Alberto0 оценок0% нашли этот документ полезным (0 голосов)
388 просмотров1 страницаProgram-based screening using conventional cytology is
reducing cervical cancer mortality, but has limitations:
— Each individual Pap smear has low sensitivity
— Identification of abnormal cytology is subjective and
highly labor-intensive
● Persistent human papillomavirus (HPV) infection is a
necessary cause of cervical carcinoma; testing for HPV
has become an important component of screening
● Roche PCR-based testing offers an alternative to the
Digene Hybrid Capture® 2 (hc2) test
● The rapid and sensitive nature of amplification-based
technology (PCR), together with reduced specimen
requirements, provide an attractive method for HPV
testing for liquid cytology media
Оригинальное название
The Roche AMPLICOR® HPV Test as a primary screen for HPV in cervical specimens collected in ThinPrep® and SurePath™ liquid cytology media
Авторское право
© Attribution Non-Commercial (BY-NC)
Доступные форматы
PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документProgram-based screening using conventional cytology is
reducing cervical cancer mortality, but has limitations:
— Each individual Pap smear has low sensitivity
— Identification of abnormal cytology is subjective and
highly labor-intensive
● Persistent human papillomavirus (HPV) infection is a
necessary cause of cervical carcinoma; testing for HPV
has become an important component of screening
● Roche PCR-based testing offers an alternative to the
Digene Hybrid Capture® 2 (hc2) test
● The rapid and sensitive nature of amplification-based
technology (PCR), together with reduced specimen
requirements, provide an attractive method for HPV
testing for liquid cytology media
Авторское право:
Attribution Non-Commercial (BY-NC)
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
388 просмотров1 страницаThe Roche AMPLICOR® HPV Test As A Primary Screen For HPV in Cervical Specimens Collected in ThinPrep® and SurePath™ Liquid Cytology Media
Загружено:
AlbertoProgram-based screening using conventional cytology is
reducing cervical cancer mortality, but has limitations:
— Each individual Pap smear has low sensitivity
— Identification of abnormal cytology is subjective and
highly labor-intensive
● Persistent human papillomavirus (HPV) infection is a
necessary cause of cervical carcinoma; testing for HPV
has become an important component of screening
● Roche PCR-based testing offers an alternative to the
Digene Hybrid Capture® 2 (hc2) test
● The rapid and sensitive nature of amplification-based
technology (PCR), together with reduced specimen
requirements, provide an attractive method for HPV
testing for liquid cytology media
Авторское право:
Attribution Non-Commercial (BY-NC)
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 1
The Roche AMPLICOR® HPV Test as a primary screen for HPV
in cervical specimens collected in ThinPrep® and SurePath™
liquid cytology media
Jane Gibson, David Vinson, David Flynn, Rebecca Garcia, Dayanara Jacquin, Mark Kohler,
Mike Kratz, Michelle Moss, Rebecca Sneed, Dennis Anderson, Audrey Roberts
Department of Clinical Molecular Genetics, AmeriPath Center for Advanced Diagnostics, Orlando, Florida, USA
Introduction A Table 2. Genotypes identified in AMPLICOR-negative, hc2-
positive samples
HPV L1 gene
● Program-based screening using conventional cytology is
AMPLICOR-negative, hc2-positive
reducing cervical cancer mortality, but has limitations: PVUP/PVDN
x5 x7 (Genotypes detected in 20 samples)
— Each individual Pap smear has low sensitivity AMPLICOR
165 bp amplicon Type n
HPV Test
— Identification of abnormal cytology is subjective and
B 53 5
highly labor-intensive
HPV L1 gene
54 2
● Persistent human papillomavirus (HPV) infection is a 64 1
necessary cause of cervical carcinoma; testing for HPV PGMY 66 3
x5 x 13
has become an important component of screening 67 2
Roche LBA 450 bp amplicon 70 2
● Roche PCR-based testing offers an alternative to the 82 1
Digene Hybrid Capture® 2 (hc2) test 53 and 54 1
Figure 2. PCR primer positions and amplicon sizes for the
● The rapid and sensitive nature of amplification-based AMPLICOR HPV Test (A) and the Roche LBA (B) 53 and 62 1
technology (PCR), together with reduced specimen 53 and 70 1
66 and 70 1
requirements, provide an attractive method for HPV Results
testing for liquid cytology media
● Overall, HPV-positivity was 15.1% with the AMPLICOR
HPV Test and 9.3% with the hc2 test Discussion
Objectives ● 1650/2000 samples (83%) were AMPLICOR and hc2 ● HR HPV was detected by the Roche LBA in 45/138 (33%)
● To use the Roche AMPLICOR® HPV Test (Figure 1) as a concordant negative AMPLICOR-positive/hc2-negative specimens
primary screen for HPV in a cohort of 2000 randomly ● 151/2000 samples (8%) were concordant positive ● Roche LBA-negative samples are being analyzed by E7
selected cervical specimens collected in ThinPrep® and ● 199/2000 samples (9.9%) were discrepant: type-specific PCR to resolve discrepants further
SurePath™ media — 138 were AMPLICOR-positive, hc2-negative: ● All 34 AMPLICOR-negative/hc2-positive specimens
● 93 were Roche LBA-negative or low-risk (LR)- tested by the Roche LBA yielded either negative results
● To compare the results with those obtained using the hc2 (14/34 [41%]), or contained HPV types not intended to
positive (Table 1 shows Roche LBA results of the
test HR genotypes) be detected with the hc2 test (20/34 [59%])
— 34 were AMPLICOR-negative, hc2-positive: ● All 27 hc2-indeterminate samples were resolved using the
Native HPV
UNG Denature and ● 14 of these were Roche LBA-negative, and all AMPLICOR HPV Test or Roche LBA genotype analysis
genome hybridize
digestion
other genotypes were non-target types (Table 2)
None of these types is included in the probe spectra
Conclusions
Wash, add
avidin-HRP ●
PCR conjugate
Biotinylated
primers of the AMPLICOR HPV Test or the hc2 test
— 27 were hc2-indeterminate: ● These data suggest that the AMPLICOR HPV
HPV Test is a more sensitive method, compared
probe 12 of these were AMPLICOR-positive samples:
●
with hc2, for the detection of HR HPV in
Hybridization
— The Roche LBA identified 11 as HR-positive
cervical specimens collected in ThinPrep® and
Oxidized Oxidized
TMB TMB
(types 16 [n=4], 18 [n=3], 31 [n=1], 35 [n=1], SurePath™ liquid cytology media
59 [n=1] and 68 [n=1], and one as LR-positive
Add stop solution,
TMB TMB
● The presence of HR HPV was confirmed in
read absorbance (types 66 and 89 [CP6108])
33% of AMPLICOR-positive/hc2-negative
HRP produces color upon
addition of TMB substrate
Immobilized hybrids react
with avidin-HRP
● 15 were AMPLICOR-negative samples: specimens; negative findings in the remaining
— The Roche LBA was negative in all three cases
93 specimens may be due to the increased
HPV: Human papillomavirus; UNG: Uracil-N-glycosylase; PCR: Polymerase chain reaction; HRP: Horseradish peroxidase;
TMB: 3,3',5,5'-tetramethylbenzidene
tested; 12 additional AMPLICOR-negative sensitivity of the AMPLICOR HPV Test, relative
samples were not analyzed by the Roche LBA to the Roche LBA
Figure 1. AMPLICOR HPV Test Table 1. Genotypes identified in AMPLICOR-positive, hc2- ● E7 type-specific PCR testing is underway to
negative samples characterize these specimens further
No target HR HPV genotypes for the
Materials and methods AMPLICOR-positive, hc2-negative
(HR genotypes detected in 45 samples)
●
AMPLICOR HPV Test and the hc2 test were
● A total of 2000 randomly selected cervical cell specimens found in any of the 34 AMPLICOR-
Type n
in ThinPrep® or SurePath™ liquid cytology media (49% negative/hc2-positive specimens, suggesting
vs 51%, respectively) were included in the study: 16 4 false-positive hc2 results
18 7 ● Understanding and defining the clinical
— 79% of women were ≥ 30 years of age applications of a more sensitive HR HPV
31 2
— 94% had normal cytology 35 1 screening test will be an important component
of future HPV testing and cervical cancer
39 2
● Samples were analyzed in batches of approximately 250 screening
45 3
alternating ThinPrep® or SurePath™ stored samples ● A more sensitive HR HPV test, such as the
52 4
● HPV testing was performed using the FDA-updated hc2 AMPLICOR HPV Test, will contribute to our
56 2
test procedure and, following DNA extraction using overall understanding of the etiology of HPV
58 1
the QIAGEN QIAamp MinElute™ system, by the infections
59 2
AMPLICOR HPV Test; both of these assays detect 68 3
13 high-risk (HR) HPV genotypes Mixed: > 1 HR HPV; no LR 3 References
● DNA samples from discrepant specimens were genotyped Mixed: > 1 HR HPV; 2
with LR type(s) present 1. Gravitt PE, Peyton CL, Alessi TQ et al. J Clin Microbiol 2000;
using the Roche prototype line blot assay (LBA)1,2 38:357–61
Mixed: 1 HR HPV; with LR present 9 2. Gravitt PE, Peyton CL, Apple RJ et al. J Clin Microbiol 1998;
● The smaller size of the AMPLICOR HPV Test amplicon, 36:3020–7
High-risk (HR) types:3 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 68
compared with that in the Roche LBA, lends itself to Possible high-risk types:3 23, 53, 66, 73, 82 3. Munoz M, Bosch FX, de Sanjose S et al. N Engl J Med 2003;
increased sensitivity (Figure 2) Low-risk (LR) types:3 6, 11, 40, 42, 43, 44, 54, 61, 70, 72, 81 348:518–27
Вам также может понравиться
- The Roche LINEAR ARRAY® HPV Test : Improved Performance Over Previous Research PrototypesДокумент1 страницаThe Roche LINEAR ARRAY® HPV Test : Improved Performance Over Previous Research PrototypesAlbertoОценок пока нет
- Hemo Aptima HPV Aug 2021Документ28 страницHemo Aptima HPV Aug 2021shahdadpuri.gauravОценок пока нет
- Abbott HPV RealTime AssayДокумент2 страницыAbbott HPV RealTime AssayIbrehimaОценок пока нет
- Stability of Human Papillomavirus (HPV) DNA in PreservCyt® at 4ºC and Room Temperature, As Detected by The Roche AMPLICOR® HPV TestДокумент1 страницаStability of Human Papillomavirus (HPV) DNA in PreservCyt® at 4ºC and Room Temperature, As Detected by The Roche AMPLICOR® HPV TestAlbertoОценок пока нет
- 21 HPV GenoArray Diagnostic KitДокумент8 страниц21 HPV GenoArray Diagnostic KitYosinee PatrungsiОценок пока нет
- Huang 2009Документ5 страницHuang 2009ilham wildanОценок пока нет
- Please Note: This File Contains Two Layouts of The Same Package InsertДокумент44 страницыPlease Note: This File Contains Two Layouts of The Same Package Insertassem_2222Оценок пока нет
- CACMID 2022 Hamilton Poster CARBA5Документ1 страницаCACMID 2022 Hamilton Poster CARBA5Jessica Toribio AriasОценок пока нет
- DNA Flow Technology - 2016Документ2 страницыDNA Flow Technology - 2016Uswatun hasanah harifuddinОценок пока нет
- IFU Check-Direct - CPO - BD - MAXДокумент26 страницIFU Check-Direct - CPO - BD - MAXRickettsia ProwazekiiОценок пока нет
- Rapide Test PDFДокумент6 страницRapide Test PDFMusa abidinОценок пока нет
- Available Online Through: ISSN 2321 - 6328Документ4 страницыAvailable Online Through: ISSN 2321 - 6328Himanshu ThukralОценок пока нет
- Chapter 12: Human Papillomavirus Technologies: Thomas Iftner, Luisa Lina VillaДокумент9 страницChapter 12: Human Papillomavirus Technologies: Thomas Iftner, Luisa Lina VillaAlbertoОценок пока нет
- Seegene HPV28 Manual en InglésДокумент43 страницыSeegene HPV28 Manual en InglésPort0% (1)
- HPV Genotypes 14 Real-TM Quant: HandbookДокумент19 страницHPV Genotypes 14 Real-TM Quant: HandbookHarun GanićОценок пока нет
- Xpert HPV: Reliable Detection of High-Risk HPV DNA With Genotyping of HPV 16 and 18/45Документ4 страницыXpert HPV: Reliable Detection of High-Risk HPV DNA With Genotyping of HPV 16 and 18/45rhoderickОценок пока нет
- Bauer 1991Документ6 страницBauer 1991Flavio AlvesОценок пока нет
- Evaluating NG-Test CARBA 5 Multiplex Immunochromatographic and Cepheid Xpert CARBA-R Assays Among Carbapenem-Resistant Enterobacterales Isolates Associated With Bloodstream Infection - PubMedДокумент2 страницыEvaluating NG-Test CARBA 5 Multiplex Immunochromatographic and Cepheid Xpert CARBA-R Assays Among Carbapenem-Resistant Enterobacterales Isolates Associated With Bloodstream Infection - PubMedyogesh kumarОценок пока нет
- DNJDKCD, XLPLДокумент1 страницаDNJDKCD, XLPLzell_leonheartОценок пока нет
- 2018 KSU Shrimp Workshop - DharДокумент31 страница2018 KSU Shrimp Workshop - DharRaju RamaiahОценок пока нет
- Evaluation of The RESIST-4 O.K.N.V Immunochromatographic Lateral Flow Assay For The Rapid Detection of OXA-48, KPC, NDM and VIM Carbapenemases From Cultured Isolates - PubMedДокумент2 страницыEvaluation of The RESIST-4 O.K.N.V Immunochromatographic Lateral Flow Assay For The Rapid Detection of OXA-48, KPC, NDM and VIM Carbapenemases From Cultured Isolates - PubMedyogesh kumarОценок пока нет
- Detection of Carbapenemase Producing Enterobacterales and BD Phoenix CPO Detect PanelДокумент19 страницDetection of Carbapenemase Producing Enterobacterales and BD Phoenix CPO Detect PanelLucila MurdochОценок пока нет
- PCR & Cell Culture WorksheetДокумент2 страницыPCR & Cell Culture WorksheetJ Pao Bayro - LacanilaoОценок пока нет
- NG-Test Carba 5: Rapid AccurateДокумент2 страницыNG-Test Carba 5: Rapid AccurateDavidSargFolgarОценок пока нет
- Adamianis Papiloma Virusi (HPV) - Sasvilosnos Yelis Kibos Axali Skrining-SinjiДокумент4 страницыAdamianis Papiloma Virusi (HPV) - Sasvilosnos Yelis Kibos Axali Skrining-SinjiNino KarkashadzeОценок пока нет
- In Vitro Generation Of: Immortalized CD34+Документ3 страницыIn Vitro Generation Of: Immortalized CD34+Mind NiramindОценок пока нет
- CINtec PLUS Cytology Package Insert USДокумент24 страницыCINtec PLUS Cytology Package Insert USrkccharanОценок пока нет
- Cervical Screening Care Pathway: Gov - UkДокумент13 страницCervical Screening Care Pathway: Gov - Ukbm5q2h9xbhОценок пока нет
- Evaluación de Test Rápidos y Diseño de Una Estrategia para La Detección y Caracterización de Carbapenemasas en Cepas de Bacilos GramnegativosДокумент7 страницEvaluación de Test Rápidos y Diseño de Una Estrategia para La Detección y Caracterización de Carbapenemasas en Cepas de Bacilos GramnegativosAndresSalasОценок пока нет
- Expression Ready YFP Retroviral ParticlesДокумент2 страницыExpression Ready YFP Retroviral ParticlesAlleleBiotechОценок пока нет
- RDM6yIjTXmQzOsiI 15mg - Current Methods To Identify Pharmacogenomics VariantsДокумент9 страницRDM6yIjTXmQzOsiI 15mg - Current Methods To Identify Pharmacogenomics VariantsSalman khanОценок пока нет
- Sanchooli2020 Article ProductionOfHumanPapillomaviruДокумент7 страницSanchooli2020 Article ProductionOfHumanPapillomaviruHandiОценок пока нет
- Target Validation II: Michael Bromley, Paul Carr, Sandra Howsley, Sarah Kaye, Danny Tuckwell and Jason OliverДокумент1 страницаTarget Validation II: Michael Bromley, Paul Carr, Sandra Howsley, Sarah Kaye, Danny Tuckwell and Jason OliverTasaduq AzizОценок пока нет
- Rapid and Easy Detection of Carbapenemases in Enterobacterales in The Routine Laboratory Using The New Genepoc Carba/Revogene Carba C AssayДокумент2 страницыRapid and Easy Detection of Carbapenemases in Enterobacterales in The Routine Laboratory Using The New Genepoc Carba/Revogene Carba C Assayyogesh kumarОценок пока нет
- Meningitis ValuesДокумент1 страницаMeningitis ValuesYukta ThackerОценок пока нет
- Comprehensive Genomic Profiling at IlluminaДокумент23 страницыComprehensive Genomic Profiling at IlluminaSaulius BarauskasОценок пока нет
- ACog-natural History of HPVДокумент9 страницACog-natural History of HPVAtit PoudelОценок пока нет
- Elecsys® Anti-HAV IgM Immunoassay For The Qualitative Detection of IgM Antibodies Against HAVДокумент4 страницыElecsys® Anti-HAV IgM Immunoassay For The Qualitative Detection of IgM Antibodies Against HAVLAMA LAMAОценок пока нет
- 5th Rotation - IsBB (Tour)Документ2 страницы5th Rotation - IsBB (Tour)loona oneОценок пока нет
- 28 Lubag, Angela Louisse HernandezДокумент1 страница28 Lubag, Angela Louisse HernandezAngela LubagОценок пока нет
- MBGV STDДокумент10 страницMBGV STDDivergenteОценок пока нет
- Chip-Based Real Time Duplex PCR Test For Human Papillomavirus High Risk Types 16, 31 and 18, 45Документ4 страницыChip-Based Real Time Duplex PCR Test For Human Papillomavirus High Risk Types 16, 31 and 18, 45vivicon2004Оценок пока нет
- Hubers MayoClinProc 2019 SuppДокумент1 страницаHubers MayoClinProc 2019 SuppDaniel LupuОценок пока нет
- 249 FullДокумент3 страницы249 Fullrustyryan77Оценок пока нет
- pCHAC MwasabiДокумент1 страницаpCHAC MwasabiAlleleBiotechОценок пока нет
- Malaria Laboratory Testing AlgorithmДокумент1 страницаMalaria Laboratory Testing AlgorithmAlan FrostОценок пока нет
- Farmacos y Anticuerpos Neutralizantes - CompressedДокумент36 страницFarmacos y Anticuerpos Neutralizantes - CompressedRaisa Paredes PОценок пока нет
- HPV QUANT-21 - Form D3 - IFUДокумент24 страницыHPV QUANT-21 - Form D3 - IFULAB PCRОценок пока нет
- Laboratory Testing For COVID-19 - Dr. Trilis Yulianti, M.kesДокумент20 страницLaboratory Testing For COVID-19 - Dr. Trilis Yulianti, M.kesYayax RakhmanОценок пока нет
- AJCP / Special Article: BackgroundДокумент27 страницAJCP / Special Article: BackgroundnuvitaОценок пока нет
- Detection of MicroorganismsДокумент26 страницDetection of Microorganismsrajprasath20gmailcomОценок пока нет
- High-Resolution Human Papillomavirus Genotyping by MALDI-TOF Mass SpectrometryДокумент9 страницHigh-Resolution Human Papillomavirus Genotyping by MALDI-TOF Mass SpectrometryДенис КрахоткинОценок пока нет
- Aplikasi Pemeriksaan RT-PCR Sars Cov 2: Basti AndriyokoДокумент25 страницAplikasi Pemeriksaan RT-PCR Sars Cov 2: Basti AndriyokoAlif Adiyudha PratamaОценок пока нет
- CD Rom 8 Optional Molecular QCДокумент9 страницCD Rom 8 Optional Molecular QCDr Prutha RathodОценок пока нет
- Read It!Документ4 страницыRead It!Ajeng DiajengОценок пока нет
- Lee 2011Документ12 страницLee 2011Денис КрахоткинОценок пока нет
- 9317802-007-GB-C HHV6 R-GeneДокумент2 страницы9317802-007-GB-C HHV6 R-GeneSachinОценок пока нет
- Saluja Arti Amit ReportsДокумент1 страницаSaluja Arti Amit ReportsDwayne PereiraОценок пока нет
- Ensuring QPCR Data Reliability - Controlling For ContaminationДокумент10 страницEnsuring QPCR Data Reliability - Controlling For ContaminationSyarifHidayatОценок пока нет
- Novel p53 Splicing Site Mutation in Li-Fraumeni-like Syndrome With OsteosarcomaДокумент5 страницNovel p53 Splicing Site Mutation in Li-Fraumeni-like Syndrome With OsteosarcomaMissy MishaОценок пока нет
- The Chemical Composition and Pharmaceutical Effect of Celosia Cristata A Review On Nutritional AspectДокумент6 страницThe Chemical Composition and Pharmaceutical Effect of Celosia Cristata A Review On Nutritional AspectInternational Journal of Innovative Science and Research TechnologyОценок пока нет
- Urban Inequities Survey ManualДокумент364 страницыUrban Inequities Survey ManualAashishTripathiBaluaОценок пока нет
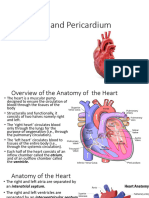
- The Heart and PericardiumДокумент40 страницThe Heart and PericardiumMartha Orendu Oche AttahОценок пока нет
- Aberdeenvaricoseveinsquestionnaire PDFДокумент4 страницыAberdeenvaricoseveinsquestionnaire PDFdesyislamiatiОценок пока нет
- 09 Marijuana Facts For TeensДокумент24 страницы09 Marijuana Facts For Teensapi-309082881Оценок пока нет
- RITM LeprosyДокумент3 страницыRITM LeprosyDanielle Vince CapunoОценок пока нет
- Melborne University OSCE Exam SampleДокумент6 страницMelborne University OSCE Exam Sampleextraxen3690Оценок пока нет
- Study of The Causes of Mortality in Acute Aluminium Phosphide PoisoningДокумент11 страницStudy of The Causes of Mortality in Acute Aluminium Phosphide PoisoningHany TawfikОценок пока нет
- Journal Homepage: - : IntroductionДокумент8 страницJournal Homepage: - : IntroductionIJAR JOURNALОценок пока нет
- Jrsocmed00158 0011 PDFДокумент6 страницJrsocmed00158 0011 PDFWahyu SutrisnaОценок пока нет
- LVS Chronic Pain WsДокумент49 страницLVS Chronic Pain WsdtncorreoОценок пока нет
- Msds PG LyondellДокумент9 страницMsds PG LyondellGia Minh Tieu TuОценок пока нет
- Slide IBSДокумент34 страницыSlide IBSRamadhian Galih PratamaОценок пока нет
- Top 10 Differential Diagnoses in Family Medicine - CoughДокумент2 страницыTop 10 Differential Diagnoses in Family Medicine - CoughTiza OyonОценок пока нет
- Topnotch Practice Exam 1 For MARCH 2020 and SEPT 2020 BatchesДокумент104 страницыTopnotch Practice Exam 1 For MARCH 2020 and SEPT 2020 BatchesJerome AndresОценок пока нет
- Acne Herbal TreatmentДокумент7 страницAcne Herbal TreatmentPriyanka Bundhoo100% (1)
- Giannopoulos PC - AlДокумент54 страницыGiannopoulos PC - AlNikosОценок пока нет
- Journal Pone 0208697 PDFДокумент14 страницJournal Pone 0208697 PDFRenzo Flores CuadraОценок пока нет
- Lesson Plan Additives in FoodДокумент21 страницаLesson Plan Additives in FoodZahra AlkhansaОценок пока нет
- GASTROPATHY NSAIDsДокумент23 страницыGASTROPATHY NSAIDsAyu Yunita Jaury HRОценок пока нет
- Clinical Teaching 4PEUPERAL SEPSISДокумент5 страницClinical Teaching 4PEUPERAL SEPSISAjit M Prasad Prasad100% (1)
- Tinjauan Ekonomi Politik Dan Keamanan Terhadap PenДокумент14 страницTinjauan Ekonomi Politik Dan Keamanan Terhadap PenAnna Yulianti SitumeangОценок пока нет
- 017 Pathology MCQ ACEM Primary GITДокумент3 страницы017 Pathology MCQ ACEM Primary GITRebeenMustafaОценок пока нет
- Vaccine Covid-19: Dr. Annisa Maloveny, SPPDДокумент22 страницыVaccine Covid-19: Dr. Annisa Maloveny, SPPDMagnolia HealОценок пока нет
- Sore ThroatДокумент10 страницSore Throatapi-551073862Оценок пока нет
- Fetal Biophysical ProfileДокумент17 страницFetal Biophysical ProfileBangun PurwakaОценок пока нет
- Clinical Study: Overjet and Overbite Influence On Cyclic Masticatory Movements: A CT StudyДокумент7 страницClinical Study: Overjet and Overbite Influence On Cyclic Masticatory Movements: A CT Studyarya091193Оценок пока нет
- Ethical Judgments Limit The Methods Available in The Production of Knowledge in Both The Arts and The Natural SciencesДокумент5 страницEthical Judgments Limit The Methods Available in The Production of Knowledge in Both The Arts and The Natural SciencesMilena ŁachОценок пока нет