Академический Документы
Профессиональный Документы
Культура Документы
Nej MR A 1202392
Загружено:
Kamila JasmineОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Nej MR A 1202392
Загружено:
Kamila JasmineАвторское право:
Доступные форматы
The
n e w e ng l a n d j o u r na l
of
m e dic i n e
anniversary article
Two Hundred Years of Surgery
Atul Gawande, M.D., M.P.H.
From the Department of Surgery, Brigham
and Womens Hospital; and the Department of Health Policy and Management,
Harvard School of Public Health both
in Boston. Address reprint requests to Dr.
Gawande at the Department of Health
Policy and Management, Harvard School
of Public Health, 677 Huntington Ave.,
Boston, MA 02115.
This article (10.1056/NEJMra1202392) was
updated on August 9, 2012, at NEJM.org.
N Engl J Med 2012;366:1716-23.
Copyright 2012 Massachusetts Medical Society.
A timeline is
available at
NEJM.org
urgery is a profession defined by its authority to cure by means
of bodily invasion. The brutality and risks of opening a living persons body
have long been apparent, the benefits only slowly and haltingly worked out.
Nonetheless, over the past two centuries, surgery has become radically more effective, and its violence substantially reduced changes that have proved central to
the development of mankinds abilities to heal the sick.
Surger y befor e the A dv en t of A ne s the si a
The first volume of the New England Journal of Medicine and Surgery, and the Collateral
Branches of Science, published in 1812, gives a sense of the constraints faced by surgeons,
and the mettle required of patients, in the era before anesthesia and antisepsis. In
the April issue for that year, John Collins Warren, surgeon at the Massachusetts
General Hospital and son of one of the founders of Harvard Medical School, published a case report describing a new approach to the treatment of cataracts.1 Until
that time, the prevalent method of cataract treatment was couching, a procedure
that involved inserting a curved needle into the orbit and using it to push the clouded
lens back and out of the line of sight.2 Warrens patient had undergone six such attempts without lasting success and was now blind. Warren undertook a more radical and invasive procedure actual removal of the left cataract. He described the
operation, performed before the students of Harvard Medical School, as follows:
The eye-lids were separated by the thumb and finger of the left hand, and then,
a broad cornea knife was pushed through the cornea at the outer angle of the
eye, till its point approached the opposite side of the cornea. The knife was
then withdrawn, and the aqueous humour being discharged, was immediately followed by a protrusion of the iris.
Into the collapsed orbit of this unanesthetized man, Warren inserted forceps he
had made especially for the event. However, he encountered difficulties that necessitated improvisation:
The opaque body eluding the grasp of the forceps, a fine hook was passed
through the pupil, and fixed in the thickened capsule, which was immediately drawn out entire. This substance was quite firm, about half a line in
thickness, a line in diameter, and had a pearly whiteness.
A bandage was applied, instructions on cleansing the eye were given, and the
gentleman was sent home. Two months later, Warren noted, inflammation required
two or three bleedings, but the patient is now well, and sees to distinguish every
object with the left eye.
The implicit encouragement in Warrens article, and in others like it, was to be
daring, even pitiless, in attacking problems of an anatomical nature. As the 18th-
1716
n engl j med 366;18 nejm.org may 3, 2012
The New England Journal of Medicine
Downloaded from nejm.org on December 2, 2014. For personal use only. No other uses without permission.
Copyright 2012 Massachusetts Medical Society. All rights reserved.
Two Hundred Years of Surgery
century surgeon William Hunter had told his students, Anatomy is the Basis of Surgery, it informs
the Head, guides the hand, and familiarizes the
heart to a kind of necessary inhumanity.3 That
first volume of the Journal provided descriptions
of a remarkable range of surgical techniques, including those for removing kidney, bladder, and
urethral stones; dilating the male urethra when
strictured by the passage of stones; tying off aneurysms of the iliac artery and infrarenal aorta; treating burns; and using leeches for bloodletting.
There were articles on the problem of the ulcerated uterus and on the management of gunshot
and cannonball wounds, not to mention a spirited
debate on whether the wind of a passing cannonball alone was sufficient to cause serious softtissue injury.
Surgery, nonetheless, remained a limited profession. Pain and the always looming problem of
infection restricted the extent of a surgeons reach.
Entering the abdomen, for instance, was regarded
with reproach attempts had proved almost
uniformly fatal.4 The chest and joints were also
out of reach. The primary remit of surgery was
therefore the management of external conditions,
and medicine dealt with the internal ones (hence
the term internal medicine, which persists to
this day). Even for those conditions that appeared
to be externally accessible, surgical accounts often
spoke of failure more than derring-do. For example, in an article on spina bifida that appeared in
the January 1812 issue of the Journal, a surgeon
noted the uniform fatality of the condition and
recounted an effort to repeatedly lance, drain, and
bandage an infants meningocele, which proved
to be utterly futile.5 The skin had become thickened, and as inelastic...as the upper leather of
a shoe; it also ulcerated, the author wrote. Pus
was formed in the sac, and the infant died. Such
reports often maintained an almost defiant optimism. (We have no doubt, this surgeon concluded, that if performed with due caution, a
technique of draining meningoceles will be engineered and the disease of Spina Bifida may
cease to be an opprobrium of medicine.) Nonetheless, breakthrough surgical successes were, for
a long time, few and far between.
They were also often illusory. In 1831, for instance, a Mr. Preston reported in the Journal his
treatment of a man with an acute stroke that had
resulted in left hemiparesis and speech difficulties.6 He did not use the usual, ineffective method
of bloodletting and applying leeches but instead
decided to take the curious approach of ligating
the patients right common carotid artery. Preston conjectured that by diminishing the supply of
blood to the affected side of the brain, the treatment would reduce congestion and inflammation.
By luck, the man survived. He was discharged
1 month later, walking with the aid of a stick and
speaking normally, leading Preston to propose that
surgeons might consider tying both carotids in
future cases. Fortunately, his case notwithstanding, the procedure failed to catch on.
The crucial spark of transformation the moment that changed not just the future of surgery
but of medicine as a whole was the publication
on November 18, 1846, of Henry Jacob Bigelows
groundbreaking report, Insensibility during Surgical Operations Produced by Inhalation7 (Fig. 1).
The opening sentences crisply summarized the
achievement: It has long been an important problem in medical science to devise some method of
mitigating the pain of surgical operations. An efficient agent for this purpose has at length been
discovered. Bigelow described how William Morton, a Boston dentist, had administered to his own
patients, and then to several more who had undergone surgery at the Massachusetts General
Hospital, a gas he called Letheon, which successfully rendered them insensible to pain. Morton had
patented the composition of the gas and kept it a
secret even from the surgeons. Bigelow revealed,
however, that he could smell ether in it. The news
burst across the world. The Letters to the Editor
pages were occupied for months with charges and
countercharges over Bigelows defense of Mortons
secrecy and credit for the discovery. Meanwhile,
ether anesthesia rapidly revolutionized surgery
how it was practiced, what could be attempted
with its use, and even what it sounded like.
Consider, for instance, amputation of the leg.
The procedure had long been recognized as lifesaving, in particular for compound fractures and
other wounds prone to sepsis, and at the same
time horrific. Before the discovery of anesthesia,
orderlies pinned the patient down while an assistant exerted pressure on the femoral artery or
applied a tourniquet on the upper thigh (Fig. 2A,
upper drawing). Surgeons using the circular method proceeded through the limb in layers, taking a
long curved knife in a circle through the skin first,
then, a few inches higher up, through the muscle,
and finally, with the assistant retracting the muscle to expose the bone a few inches higher still,
taking an amputation saw smoothly through the
n engl j med 366;18 nejm.org may 3, 2012
The New England Journal of Medicine
Downloaded from nejm.org on December 2, 2014. For personal use only. No other uses without permission.
Copyright 2012 Massachusetts Medical Society. All rights reserved.
1717
The
n e w e ng l a n d j o u r na l
Figure 1. Operation Being Performed with the Use of
Ether Anesthesia.
This daguerreotype was taken in the spring of 1847 by
Josiah Hawes in the Operating Room (now known as
the Ether Dome) of the Massachusetts General Hospital. The first public demonstration of surgical anesthesia occurred in the same room on October 16, 1846,
presided over by the surgeon John Collins Warren,
seen here touching the patient. Although it is believed
that a photographer was present during the first event
as well, he took no pictures because the sight of blood
made him nauseated.8 Courtesy of the Massachusetts
General Hospital, Archives and Special Collections.
bone so as not to leave splintered protrusions (Fig.
2A, lower drawing). Surgeons using the flap
method, popularized by the British surgeon Robert Liston, stabbed through the skin and muscle
close to the bone and cut swiftly through at an
oblique angle on one side so as to leave a flap
covering the stump (Fig. 2B).
The limits of patients tolerance for pain forced
surgeons to choose slashing speed over precision.
With either the flap method or the circular method, amputation could be accomplished in less than
a minute, though the subsequent ligation of the
severed blood vessels and suturing of the muscle
and skin over the stump sometimes required 20 or
30 minutes when performed by less experienced
surgeons.9 No matter how swiftly the amputation
was performed, however, the suffering that patients experienced was terrible. Few were able to
put it into words. Among those who did was
Professor George Wilson. In 1843, he underwent
a Syme amputation ankle disarticulation
performed by the great surgeon James Syme himself. Four years later, when opponents of anesthetic agents attempted to dismiss them as
needless luxuries, Wilson felt obliged to pen a
description of his experience11:
1718
n engl j med 366;18
of
m e dic i n e
The horror of great darkness, and the sense
of desertion by God and man, bordering
close on despair, which swept through my
mind and overwhelmed my heart, I can
never forget, however gladly I would do so.
During the operation, in spite of the pain
it occasioned, my senses were preternaturally acute, as I have been told they generally are in patients in such circumstances.
I still recall with unwelcome vividness the
spreading out of the instruments: the twisting of the tourniquet: the first incision: the
fingering of the sawed bone: the sponge
pressed on the flap: the tying of the bloodvessels: the stitching of the skin: the bloody
dismembered limb lying on the floor.
Before anesthesia, the sounds of patients
thrashing and screaming filled operating rooms.
So, from the first use of surgical anesthesia, observers were struck by the stillness and silence. In
London, Liston called ether anesthesia a Yankee
dodge having seen fads such as hypnotism
come and go but he tried it nonetheless, performing the first amputation with the use of anesthesia, in a 36-year-old butler with a septic knee,
2 months after the publication of Bigelows report.10 As the historian Richard Hollingham recounts, from the case records, a rubber tube was
connected to a flask of ether gas, and the patient
was told to breathe through it for 2 or 3 minutes.12
He became motionless and quiet. Throughout the
procedure, he did not make a sound or even grimace. When are you going to begin? asked the
patient a few moments later. He had felt nothing.
This Yankee dodge beats mesmerism hollow,
Liston exclaimed.
It would take a little while for surgeons to discover that the use of anesthesia allowed them time
to be meticulous. Despite the advantages of anesthesia, Liston, like many other surgeons, proceeded in his usual lightning-quick and bloody
way. Spectators in the operating-theater gallery
would still get out their pocket watches to time
him. The butlers operation, for instance, took an
astonishing 25 seconds from incision to wound
closure. (Liston operated so fast that he once accidentally amputated an assistants fingers along
with a patients leg, according to Hollingham. The
patient and the assistant both died of sepsis, and
a spectator reportedly died of shock, resulting in
the only known procedure with a 300% mortality.)
nejm.org
may 3, 2012
The New England Journal of Medicine
Downloaded from nejm.org on December 2, 2014. For personal use only. No other uses without permission.
Copyright 2012 Massachusetts Medical Society. All rights reserved.
Two Hundred Years of Surgery
A Ne w Er a of A ne s the si a
a nd A n t isepsis
Surgeons soon found, however, that anesthesia allowed them to perform more complex, invasive,
and precise maneuvers than they had dared to attempt before. Within a decade, for instance, the
first successful hysterectomy and bilateral ovariotomy removal of massive ovarian cysts weighing several pounds13,14 proved that the abdomen
could be safely penetrated. Further experiments
revealed other effective anesthetics: nitrous oxide,
chloroform, and eventually halothane and other
nonvolatile agents. Narcotics such as laudanum
were found to relieve postoperative suffering. Suddenly, pain was no longer a barrier to surgical
capability.
A second major barrier persisted, however: sepsis. The mortality associated with ovariotomy and
other types of major abdominal surgery, repair of
open fractures, and limb amputation commonly
remained at 50% or higher owing to infection.15
One therefore might have thought that the news
of Joseph Listers landmark series of articles in
The Lancet in 186716 describing the effectiveness of
his new system of antisepsis with the use of carbolic acid would be received with the same fanfare as the report on ether anesthesia had been
(Fig. 3). Instead, it was regarded with overwhelming skepticism. The Journal first mentions Listers
breakthrough as a method that was neither original nor beneficial.17 Nearly a decade later, a surgeon writing in the Journal on the dressing of
wounds could still insist that there is good reason to believe that the theory of M. Pasteur, upon
which Lister bases his treatment, is unsound.18
Ignaz Semmelweiss, the Viennese obstetrician who
in 1847 had found that hand washing by birth
attendants eliminated puerperal sepsis, the leading cause of maternal death,19 was not even mentioned in the Journal until the end of the 19th
century. J.M.T. Finney recalled his experience as a
house officer at the Massachusetts General Hospital in the 1880s: The operating surgeon was
usually garbed in a black Prince Albert coat, kept
hanging in a closet for the occasion and showing
numerous evidences of previous operations in the
way of dried blood, wound secretions, etc.20 For
decades, hand washing and skin cleansing remained routinely perfunctory.
Some surgeons, however, especially younger
ones, began accepting the diligence required for
n engl j med 366;18
Figure 2. Methods of Amputation in the Early 19th
Century.
Panel A is a drawing by Charles Bell from 1821 showing the circular method of amputation.9 Panel B shows
the flap method of amputation being used in 1837,
with an assistant retracting the tissue flap to allow the
surgeon to saw through the femur.10
aseptic and antiseptic practice. Such practice,
along with effective anesthesia, led them to hitherto unimagined treatments and discoveries. In
1868, for instance, John Stough Bobbs reported
on a 30-year-old woman with a large, painful right
abdominal mass presumed to be an ovarian cyst.21
Chloroform allowed him to explore her abdomen
through a 4-in. incision. Sweeping the omental
adhesions aside with a finger, he encountered a
5-in.wide, smooth-walled, oval tumor. When he
cut through the wall of the tumor, a perfectly
limpid fluid escaped, propelling, with considerable force, several solid bodies about the size of
ordinary rifle bullets. He drained the sac of its
fluid, extracted some 50 concretions that ranged
in size from that of a mustard seed to that of a
bullet, and then closed the incision, uncertain
what the concretions were. The patient recovered
uneventfully with the help of laudanum and lemnejm.org
may 3, 2012
The New England Journal of Medicine
Downloaded from nejm.org on December 2, 2014. For personal use only. No other uses without permission.
Copyright 2012 Massachusetts Medical Society. All rights reserved.
1719
The
n e w e ng l a n d j o u r na l
Figure 3. Introduction of Carbolic Acid for Antisepsis.
In the late 19th century, Joseph Lister introduced antisepsis, using carbolic acid for hand washing, for dressings, and as a spray over the operative field to prevent
infection in the surgical wound.8 Drawing by William
Watson Cheyne, courtesy of Wellcome Library, London.
onade. Only later, when he carefully examined the
smooth, mahogany-colored, irregularly spherical
objects that he had extracted, did Bobbs understand what he had encountered. They were gallstones. The absence of greenyellow bile in the sac
had confused him the clear, mucoid fluid
would come to be known as white bile but he
had, in fact, performed the worlds first successful gallbladder operation.
A slew of firsts rapidly followed, each more
daring than the last. In 1880, Tait performed the
first transabdominal resection of a gangrenous
appendix,22 and Rehn performed the first subtotal thyroidectomy for Graves disease.23 In 1884,
Bennett and Godlee reported the first successful
removal of a brain tumor.24 Methods for suprapubic prostatectomy, total gastrectomy, chest surgery, and joint repair were worked out.15,25 Alexis
Carrel devised methods for suturing blood vessels
and performing surgical grafts that became the
foundation for the field of vascular surgery and
won him a Nobel Prize in 1912.26 Surgeons developed such skill and confidence that they began
performing exploratory laparotomies simply for
the purpose of diagnosis. Indeed, articles raising
concern that there were perhaps too many laparotomies began to appear by the turn of the century.27 The key barriers to surgical knowledge and
imagination were gone.
Until this time, surgical discoveries had provided only halting contributions to the capabilities
of the medical community. In the early part of the
1720
n engl j med 366;18
of
m e dic i n e
19th century, just one fifth of the Journals scientific articles were surgical in nature (if one takes
as a guide the review and classification of each
article in the first volume for each decade, beginning with 1812) (Fig. 4). Surgery had been, one
might politely say, a modest contributor to medical progress. Between the mid-1800s and the
1920s, however, the coverage of surgical advances
took up half the Journal. Physicians in the Victorian era had few effective drugs, but surgeons began reporting new treatments almost monthly,
and the breakneck pace of innovation continued
for nearly a century. Surgery became a dominant
force in medical advancement.
Profe ssiona l i z at ion,
Minimi z at ion, a nd
Rou t ini z at ion
Surgery also began to progress through an increasingly important process of refinement and
professionalization. William Halsted introduced
and popularized the use of rubber gloves to help
prevent infection. Care of burns and other wounds
was made radically simpler and less traumatizing.
Anesthetic techniques and apparatus were being
made more reliable and sophisticated. And in
1917, the American College of Surgeons founded
the Hospital Standardization Program (later renamed the Joint Commission for the Accreditation
of Hospitals) to shift the role of hospitals from
serving primarily as a place for the convalescence
of the sick poor to providing safe and effective
care for patients undergoing surgery.
Specialization was likewise an important force.
Historians continue to debate whether the growth
in knowledge drove specialization or specialization led to the growth in knowledge. (There are
numerous examples of each.) Nonetheless, in
1905, the Long Island Society of Anesthetists
was formed, which would evolve into the American Society of Anesthesiologists.28 After World
War I, national associations were formed for neurologic surgeons, orthopedic surgeons, urologists,
and other specialists, and dedicated training programs were established. Surgery the invasion
of peoples bodies for cure was becoming normalized.
Much of the story appeared only obliquely in
the Journal. But that too reflected the changing
nature of progress. The milestone reports of the
new era often seemed obscure when they first apnejm.org
may 3, 2012
The New England Journal of Medicine
Downloaded from nejm.org on December 2, 2014. For personal use only. No other uses without permission.
Copyright 2012 Massachusetts Medical Society. All rights reserved.
Two Hundred Years of Surgery
60
Percentage of Articles on Surgery
peared. Werner Forssmann, a 25-year-old surgical
intern in Eberswalde, Germany, published his report on successful catheterization of the heart in
a German medical journal in 1929.29 Forbidden
by his professors from attempting the experiment
on either animals or patients (they thought the
idea preposterous and dangerous), he performed
it on himself (Fig. 5). His investigation would eventually lead to the creation of the field of cardiology
and win Forssmann the Nobel Prize in Medicine.
Yet it was more than a decade before anyone recognized the significance of his report. Likewise,
anesthesia resident David Massas ingenious creation of the plastic intravenous catheter probably
seemed a minor innovation to many at the time.
A description of his device appeared in 1950 in
the Proceedings of the Staff Meetings of the Mayo Clinic
under the modest title A Plastic Needle, and it
was not until the 1960s that this type of catheter
became well known.30 Eventually, however, it
transformed the approach to patient resuscitation.
The field of surgery, with its ethos of radical
action and perfectionist refinement, defined
much of medical culture in the early 20th century. By midcentury, however, surgerys outsize
role and influence began to subside. Whereas its
discoveries had taken up half the space in the
Journal in 1922, the proportion fell to one third
during the next decade. By the 1950s, reports of
new diagnostic tests, vaccines, antibiotics, and
other innovations from the wet laboratory dominated the pages of the Journal. Scientists had
found an even more prolific source of discovery
than the operating room: the laboratory bench.
With the advent of chemotherapeutics, molecular medicine, and other technologies, surgery
was no longer the driving force behind medical
breakthroughs. Since 1972, just a tenth of the
Journals articles have been devoted to surgical
advances.
To be sure, the field of surgery continued to
register a steady stream of seminal breakthroughs. This was the era in which the heart
was conquered, after all. In 1948, Dwight Harken and colleagues published an astonishing
report describing the successful surgical treatment of mitral-valve disease31; in 1945, Blalock
and Taussig designed their shunt operation for
blue babies32; Robert Gross and colleagues
reported in 1952 on open-heart surgery to close
atrial septal defects in children33; and the development of cardiopulmonary-bypass technology
1862
1892
1922
50
40
1872
1842
30
20
1822
1882
1902
1942
1912
1952
1932
1852
1962
1812
2002
10
1972
1832
0
1800
1850
1900
1992
1982
1950
2000
2011
2050
Year
Figure 4. Changes in the Proportion of Articles on Surgery Published
in the Journal since 1812.
The percentages shown are based on a review of the scientific articles in the
first volume of issues published by the Journal for each decade since 1812.
allowed open-heart procedures to be carried out.
Similarly, transplantation of organs between human beings first kidneys, then livers, then
hearts and lungs, and most recently, even faces
altered basic concepts about ourselves and led
us to redefine death. Implantation of organs engineered in the laboratory from a persons own
cells is now being reported.34 Surgeons are still
traversing remarkable frontiers.
But the most striking story of surgery in recent decades is how firmly it has become established as an essential tool for helping people live
long and healthy lives. Virtually no one escapes
having a condition for which effective treatment
requires surgery a serious orthopedic injury,
a cataract, a tumor, obstructed labor, joint failure,
severe cardiac disease. Today, surgeons have in
their arsenal more than 2500 different procedures.
Thus, the focus of recent advances in the field has
been less on adding to the arsenal than on ensuring the successes of the treatments we have.
Minimization of the invasiveness of surgical
procedures is an advance that is arguably as significant as the discovery of anesthesia. In recent
decades, the advent of laparoscopy and thoracoscopy reduced the debilitating, half-meter-long abdominal and chest incisions to a half centimeter.
The subsequent introduction of endoscopic and
percutaneous techniques has turned incisions into
mere puncture wounds. Gallbladder surgery, resection of colonic polyps and ovarian tumors, and
n engl j med 366;18 nejm.org may 3, 2012
The New England Journal of Medicine
Downloaded from nejm.org on December 2, 2014. For personal use only. No other uses without permission.
Copyright 2012 Massachusetts Medical Society. All rights reserved.
1721
The
n e w e ng l a n d j o u r na l
Figure 5. Radiograph of the Heart Self-Catheterized
by a Surgical Intern in 1929.
The radiograph shows successful self-catheterization of
the heart, performed by Werner Forssmann, at the time
a 25-year-old surgical intern in Eberswalde, Germany.29
lung biopsies have become outpatient procedures.
We are now in an era in which a teenage boy can
undergo reoperation for repair of a severe coarctation of his thoracic aorta percutaneously on a
Thursday and be well enough to sprain his ankle
playing sports the following Saturday (as my son
did not long ago). The technological refinement
of our abilities to manipulate the human body has
been nothing short of miraculous.
The increased safety and ease of surgery have
produced an explosion in the volume of operations
being performed to at least 50 million annually in the United States alone. At the present rate,
the average American can expect to undergo seven
operations during his or her lifetime.35 This profound evolution has brought new societal con-
of
m e dic i n e
cerns, including how to ensure the quality and
appropriateness of the procedures performed, how
to make certain that patients have access to needed surgical care nationally and internationally, and
how to manage the immense costs. As early as
the 1970s, researchers began documenting substantial rates of fatal errors in surgical care, wide
differences in outcomes among institutions, and
large disparities in access to care both within the
United States and between countries. The science
of effectively routinizing surgery for mass populations is still in its infancy, as it is for all areas
of medicine. The Journal is entering its third century of publication, yet we are still unsure how to
measure surgical care and its results. Experiments
in the delivery of care will probably provide the
next major advancement in the field of surgery.
Meanwhile, the practice of surgery itself will
continue to change. Prognostication is a hazardous enterprise. But if the past quarter century has
brought minimally invasive procedures, the next
may bring the elimination of invasion. One feels
foolish using terms like nanotechnology I
havent the slightest idea what it really means or
can do but scientists are already experimenting with techniques for combining noninvasive
ways of seeing into the body through the manipulation of small-scale devices that can be injected
or swallowed. Surgical work will probably even
become fully automated.
The possibilities are tantalizing. A century into
the future, a surgeon will tell the tale that is,
if the world still makes such people.
Disclosure forms provided by the author are available with the
full text of this article at NEJM.org.
I thank Ami Karlage for assistance with the historical research.
References
1. Warren JC. Case of operation for sec-
ondary cataract. N Engl J Med Surg 1812;1:
194-5.
2. Chan CC. Couching for cataract in
China. Surv Ophthalmol 2010;55:393-8.
3. Hunter W. A lecture, introductory to a
course on anatomy, delivered by Dr. William Hunter, October 1775. Lancet 1829;
12:769-73.
4. Richardson RG. The story of surgery:
an historical commentary. Shrewsbury,
United Kingdom: Quiller Press, 2004.
5. Anonymous. Spina bifida. N Engl J
Med Surg 1812;1:98-102.
6. Preston. Ligature of the carotid artery
for hemiplegia, with a case in illustration.
Boston Med Surg J 1831;5:92-5.
1722
Bigelow HJ. Insensibility during surgical operations produced by inhalation.
Boston Med Surg J 1846;35:309-17.
8. Rutkow IM. Surgery: an illustrated
history. St. Louis: Mosby, 1993:333.
9. Stanley P. For fear of pain: British surgery, 1790-1850. Amsterdam: Rodopi, 2003.
10. Liston R. Practical surgery. London:
John Churchill, 1837.
11. Robertson HR. Without benefit of anesthesia: George Wilsons amputation
and Fanny Burneys mastectomy. Ann R
Coll Physicians Surg Can 1989;22:28.
12. Hollingham R. Blood and guts: a history of surgery. London: BBC Books, 2008.
13. Peaslee ER. Case of double ovarian
dropsy both ovaries successfully re7.
n engl j med 366;18
nejm.org
moved by the large peritoneal section.
Boston Med Surg J 1851;44:429-37.
14. Kimball G. Successful case of extirpation of the uterus. Boston Med Surg J
1855;52:249-55.
15. Wangensteen OH, Wangensteen SD.
The rise of surgery: from empiric craft to
scientific discipline. Minneapolis: University of Minnesota Press, 1978.
16. Lister J. On a new method of treating
compound fracture, abscess, etc., with
observations on the conditions of suppuration. Lancet 1867;89:326-329, 357-359,
507-509, 90:95-6.
17. Simpson JY. Carbolic acid and its
compounds in surgery. Boston Med Surg J
1867;77:390-2.
may 3, 2012
The New England Journal of Medicine
Downloaded from nejm.org on December 2, 2014. For personal use only. No other uses without permission.
Copyright 2012 Massachusetts Medical Society. All rights reserved.
Two Hundred Years of Surgery
18. Goss FW. The dressing of wounds.
Boston Med Surg J 1874;91:73-80.
19. Nuland SB. The doctors plague:
germs, childbed fever, and the strange
story of Ignc Semmelweis. New York:
W.W. Norton, 2003.
20. Finney JMT. Changing conditions in
surgery since the time of Henry Jacob Bigelow. N Engl J Med 1932;206:263-76.
21. Bobbs JS. Case of lithotomy of the
gallbladder. Trans Indiana State Med Soc
1868;18:68-73.
22. Tait RL. The surgical treatment of
typhlitis. Birm Med Rev 1890;27:26-34,
76-89.
23. Rehn L. Ueber die Extirpation des
Kropfs bei Morbus basedowii. Berl Klin
Wochenschr 1884;21:163-6.
24. Bennett AH, Godlee RJ. Hospital for
epilepsy and paralysis, Regents Park: excision of a tumor from the brain. Lancet
1884;2:1090-1.
25. Watson FS. Suprapubic prostatectomy
in a patient aged sixty-nine years, the
subject of profuse haematuria from an
unusual source: recovery. Boston Med Surg
J 1889;120:237-8.
26. Nobelprize.org. The Nobel Prize in
Physiology or Medicine 1912: Alexis Carrel: biography. Nobel lectures, physiology
or medicine 1901-1921 (http://www.nobel
prize.org/nobel_prizes/medicine/laureates/
1912/carrel-bio.html).
27. Munro JC. Needless laparotomies,
with a report of eight cases. N Engl J Med
1902;146:58-60.
28. Caton D. The history of anaesthesia.
In: Encyclopedia of life sciences. New York:
Wiley, 2011 (http://www.els.net/WileyCDA/
ElsArticle/refId-a0003621.html).
29. Forssmann W. Die Sondierung des
rechten Herzens. (Probing the right heart.)
Klin Wochenschr 1929;8:2085-7. (In German.)
30. Massa DJ, Lundy JS, Faulconer A Jr,
Ridley RW. A plastic needle. Proc Staff
Meet Mayo Clin 1950;25:413-5.
31. Harken DE, Ellis LB, Ware PF, Nor-
man LR. The surgical treatment of mitral
stenosis: valvuloplasty. N Engl J Med 1948;
239:801-9.
32. Blalock A, Taussig HB. The surgical
treatment of malformations of the heart
in which there is pulmonary stenosis or
pulmonary atresia. JAMA 1945;128:189202.
33. Gross RE, Pomeranz AA, Watkins E
Jr, Goldsmith EI. Surgical closure of defects of the interauricular septum by use
of an atrial well. N Engl J Med 1952;
247:455-60.
34. Macchiarini P, Jungebluth P, Go P, et
al. Clinical transplantation of a tissueengineered airway. Lancet 2008;372:202330.
35. Lee PHU, Gawande AA. The number
of surgical procedures in an American
lifetime in 3 states. J Am Coll Surg 2008;
207:Suppl 1:S75. abstract.
Copyright 2012 Massachusetts Medical Society.
an nejm app for iphone
The NEJM Image Challenge app brings a popular online feature to the smartphone.
Optimized for viewing on the iPhone and iPod Touch, the Image Challenge app lets
you test your diagnostic skills anytime, anywhere. The Image Challenge app
randomly selects from 300 challenging clinical photos published in NEJM,
with a new image added each week. View an image, choose your answer,
get immediate feedback, and see how others answered.
The Image Challenge app is available at the iTunes App Store.
n engl j med 366;18 nejm.org may 3, 2012
The New England Journal of Medicine
Downloaded from nejm.org on December 2, 2014. For personal use only. No other uses without permission.
Copyright 2012 Massachusetts Medical Society. All rights reserved.
1723
Вам также может понравиться
- The Butchering Art: Joseph Lister's Quest to Transform the Grisly World of Victorian MedicineОт EverandThe Butchering Art: Joseph Lister's Quest to Transform the Grisly World of Victorian MedicineРейтинг: 4 из 5 звезд4/5 (210)
- Victory Over PainДокумент366 страницVictory Over PainadimantoОценок пока нет
- Sketchy GynaecologyДокумент28 страницSketchy GynaecologyHuawei100% (4)
- Bad Medicine Doctors Doing Harm Since HippocratesДокумент273 страницыBad Medicine Doctors Doing Harm Since HippocratesYezdi Solaina100% (1)
- Anesthesia For Oral and Maxillofacial SurgeryДокумент347 страницAnesthesia For Oral and Maxillofacial SurgeryMaryol BallesterosОценок пока нет
- Ventilator Waveform AnalysisДокумент96 страницVentilator Waveform AnalysisVeerapong Vattanavanit100% (11)
- ChoeДокумент116 страницChoeJihad AnadОценок пока нет
- ResumenowДокумент6 страницResumenowRyan GarciaОценок пока нет
- History of CancerДокумент17 страницHistory of CancercheaussieОценок пока нет
- Understanding Surgery: A Comprehensive Guide for Every FamilyОт EverandUnderstanding Surgery: A Comprehensive Guide for Every FamilyОценок пока нет
- Introduction To SurgeryДокумент43 страницыIntroduction To Surgerylexscribis100% (2)
- Hydatidosis: A Mystery Box at Various SitesДокумент7 страницHydatidosis: A Mystery Box at Various SitesIJAR JOURNALОценок пока нет
- Sejarah Dan Perkembangan Ilmu Bedah September 2017Документ18 страницSejarah Dan Perkembangan Ilmu Bedah September 2017Arief Fakhrizal100% (1)
- Dr. Folkman's War: Angiogenesis and the Struggle to Defeat CancerОт EverandDr. Folkman's War: Angiogenesis and the Struggle to Defeat CancerРейтинг: 4.5 из 5 звезд4.5/5 (8)
- Getting BetterДокумент18 страницGetting BetterSonia AceresОценок пока нет
- History of neurosurgery from antiquityДокумент14 страницHistory of neurosurgery from antiquityNaimОценок пока нет
- HistoryДокумент4 страницыHistoryAnghel MadalinaОценок пока нет
- Gifted Hands: Journal of Clinical Investigation June 2010Документ2 страницыGifted Hands: Journal of Clinical Investigation June 2010opoboОценок пока нет
- Dr. A.K. Srivastava's Background in NeurosurgeryДокумент63 страницыDr. A.K. Srivastava's Background in NeurosurgeryphaniОценок пока нет
- John Holter's Shunt HistoryДокумент7 страницJohn Holter's Shunt Historyedupr76Оценок пока нет
- S 2400 Id 1378648Документ602 страницыS 2400 Id 1378648Branko NikolicОценок пока нет
- Arie History of SurgeryДокумент20 страницArie History of SurgeryArie RezaОценок пока нет
- Gifted HandsДокумент2 страницыGifted Handsabelmasresha12Оценок пока нет
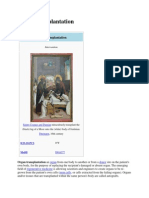
- Organ Transplantatio1Документ26 страницOrgan Transplantatio1Bindashboy0Оценок пока нет
- Treatment of Smallpox by IodineДокумент2 страницыTreatment of Smallpox by IodinefrankОценок пока нет
- RДокумент140 страницRmessam110Оценок пока нет
- Injection Treatment For Hernia - Its InefficacyДокумент56 страницInjection Treatment For Hernia - Its Inefficacyseng li chewОценок пока нет
- Get Curious Final DraftДокумент11 страницGet Curious Final Draftapi-334568771Оценок пока нет
- Electrosurgery: History, Principles, and Current and Future UsesДокумент12 страницElectrosurgery: History, Principles, and Current and Future Usesyacine tarikОценок пока нет
- History of SurgeryДокумент5 страницHistory of SurgeryjbahalkehОценок пока нет
- SEJARAH DAN PERKEMBANGAN ILMU BEDAH September 2017Документ18 страницSEJARAH DAN PERKEMBANGAN ILMU BEDAH September 2017Dipo Mas Suyudi100% (2)
- Ian's Update Newsletter: Ultrasound Procedures-Time To Start Respecting The Guide-Lines?Документ10 страницIan's Update Newsletter: Ultrasound Procedures-Time To Start Respecting The Guide-Lines?salsa0479Оценок пока нет
- General Surgery Final Exam ReviewДокумент215 страницGeneral Surgery Final Exam ReviewSara Abdul Rahman0% (1)
- The Birth of Cardiology: The Golden Decade: Braunwald's CornerДокумент2 страницыThe Birth of Cardiology: The Golden Decade: Braunwald's CornerBhageerath AttheОценок пока нет
- Download Anesthesiology 3Rd Edition David Longnecker Et Al full chapterДокумент67 страницDownload Anesthesiology 3Rd Edition David Longnecker Et Al full chapterteri.sanborn876100% (2)
- Ps 1009154 ElectrocauteryДокумент12 страницPs 1009154 ElectrocauteryWicara PutraОценок пока нет
- The History of CancerДокумент34 страницыThe History of CancerGermánОценок пока нет
- 2022 Article 1648-2Документ6 страниц2022 Article 1648-2solxmar tmОценок пока нет
- Greenblatt, S. H. (2003) - Harvey Cushing's Paradigmatic Contribution To Neurosurgery and The Evolution of His Thoughts About Specialization.Документ35 страницGreenblatt, S. H. (2003) - Harvey Cushing's Paradigmatic Contribution To Neurosurgery and The Evolution of His Thoughts About Specialization.MARIA MONTSERRAT SOMOZA MONCADAОценок пока нет
- Nej M CPC 1314240Документ11 страницNej M CPC 1314240bi3uuОценок пока нет
- Osler VS JanewayДокумент7 страницOsler VS JanewaytanjxОценок пока нет
- Simultaneously.: Ligature The ExternalДокумент12 страницSimultaneously.: Ligature The ExternalSaurabh SatheОценок пока нет
- Charity's Children: The Long Days and Nights of the Iron MenОт EverandCharity's Children: The Long Days and Nights of the Iron MenОценок пока нет
- Invasion of the Body: Revolutions in SurgeryОт EverandInvasion of the Body: Revolutions in SurgeryРейтинг: 3 из 5 звезд3/5 (4)
- Costar I No 2005Документ23 страницыCostar I No 2005DavidChandraОценок пока нет
- 3.Does Luck Exist in MedicineДокумент2 страницы3.Does Luck Exist in Medicineunknownsince1986Оценок пока нет
- Annotated BibliographyДокумент8 страницAnnotated BibliographyPayton WilliamsОценок пока нет
- Barker ClinicalLectureOperations 1879Документ4 страницыBarker ClinicalLectureOperations 1879zia malikОценок пока нет
- Healing by Manipulation - (Bone-Setting) - Jones, J. Henry - 1926 - London - Watts - Anna's ArchiveДокумент92 страницыHealing by Manipulation - (Bone-Setting) - Jones, J. Henry - 1926 - London - Watts - Anna's Archivedarksilver.wasfoundbynewtОценок пока нет
- Canmedaj01017 0045a PDFДокумент1 страницаCanmedaj01017 0045a PDFamoet_122Оценок пока нет
- A Modification of The Swenson Operation For Congenital MegacolonДокумент8 страницA Modification of The Swenson Operation For Congenital MegacolonGunduz AgaОценок пока нет
- Biomedical Instrumentation: A Historical PerspectiveДокумент26 страницBiomedical Instrumentation: A Historical PerspectiveSandhya NatarajanОценок пока нет
- 9 Be 8Документ86 страниц9 Be 8Ghea Jovita SinagaОценок пока нет
- 1 s2.0 S2090536X15000283 MainДокумент5 страниц1 s2.0 S2090536X15000283 MainDr K. Mamatha Prof & Hod FMTОценок пока нет
- Slow Ideas - The New YorkerДокумент23 страницыSlow Ideas - The New YorkerxfallingstarОценок пока нет
- WesterneuropemedДокумент2 страницыWesterneuropemedapi-305871964Оценок пока нет
- Great Doctors of The World 1. Edward JennerДокумент10 страницGreat Doctors of The World 1. Edward JennerNeethu ChandranОценок пока нет
- A History of AnesthesiaДокумент13 страницA History of AnesthesiaDiana NiculaeОценок пока нет
- History of Hemostasis in Neurosurgery Paulo Et Al 2018Документ14 страницHistory of Hemostasis in Neurosurgery Paulo Et Al 2018AlexОценок пока нет
- Download ebook Anesthesiology Pdf full chapter pdfДокумент67 страницDownload ebook Anesthesiology Pdf full chapter pdfwendy.johnson850100% (22)
- Organtransplantation 130429210618 Phpapp02Документ36 страницOrgantransplantation 130429210618 Phpapp02ayan_tokОценок пока нет
- Medicine During The Age of IndustrializationДокумент3 страницыMedicine During The Age of IndustrializationJuliah Elyz Alforja TanОценок пока нет
- The History of CancerДокумент35 страницThe History of CancerAnjum RizviОценок пока нет
- The History of SuturesДокумент11 страницThe History of SuturesamokraneОценок пока нет
- Structural and Dynamic Bases of Hand Surgery by Eduardo Zancolli 1969Документ1 страницаStructural and Dynamic Bases of Hand Surgery by Eduardo Zancolli 1969khoxОценок пока нет
- Fluids Balance: Tanto HДокумент31 страницаFluids Balance: Tanto HKamila JasmineОценок пока нет
- Fluids Balance: Tanto HДокумент31 страницаFluids Balance: Tanto HKamila JasmineОценок пока нет
- EndocrineДокумент20 страницEndocrineKamila JasmineОценок пока нет
- Fluids Balance: Tanto HДокумент31 страницаFluids Balance: Tanto HKamila JasmineОценок пока нет
- Tugas Matakuliah Bahasa Inggris Naskah Role PlayДокумент4 страницыTugas Matakuliah Bahasa Inggris Naskah Role PlayKamila JasmineОценок пока нет
- SmokingДокумент14 страницSmokingKamila JasmineОценок пока нет
- Anfis EndokrinДокумент68 страницAnfis EndokrinKamila JasmineОценок пока нет
- How Can Nurses Help Patients Quit SmokingДокумент2 страницыHow Can Nurses Help Patients Quit SmokingKamila JasmineОценок пока нет
- Tugas Matakuliah Bahasa Inggris Naskah Role PlayДокумент4 страницыTugas Matakuliah Bahasa Inggris Naskah Role PlayKamila JasmineОценок пока нет
- How Can Nurses Help Patients Quit SmokingДокумент2 страницыHow Can Nurses Help Patients Quit SmokingKamila JasmineОценок пока нет
- Tugas Matakuliah Bahasa Inggris Naskah Role PlayДокумент4 страницыTugas Matakuliah Bahasa Inggris Naskah Role PlayKamila JasmineОценок пока нет
- Tugas Matakuliah Bahasa Inggris Naskah Role PlayДокумент4 страницыTugas Matakuliah Bahasa Inggris Naskah Role PlayKamila JasmineОценок пока нет
- Nej MR A 1202392Документ8 страницNej MR A 1202392Kamila JasmineОценок пока нет
- Hipertensi 2Документ11 страницHipertensi 2Kamila JasmineОценок пока нет
- G Proteins - The Disease Spectrum Expands: Allen M. Spiegel, M.DДокумент2 страницыG Proteins - The Disease Spectrum Expands: Allen M. Spiegel, M.DKamila JasmineОценок пока нет
- Blood Pressure in Early Autosomal Dominant Polycystic Kidney DiseaseДокумент12 страницBlood Pressure in Early Autosomal Dominant Polycystic Kidney DiseaseKamila JasmineОценок пока нет
- 226 - Pengaruh Senam Diabetik Terhadap Penurunan Resiko Ulkus Kaki Diabetik Pada Pasien DM Tipe 2 Di Perkumpulan DiabetikДокумент7 страниц226 - Pengaruh Senam Diabetik Terhadap Penurunan Resiko Ulkus Kaki Diabetik Pada Pasien DM Tipe 2 Di Perkumpulan DiabetikYadhie Funkjazz AgmОценок пока нет
- Generan Anaesthesia For DentistryДокумент13 страницGeneran Anaesthesia For DentistrynissadhaniaОценок пока нет
- Renal EmergenciesДокумент93 страницыRenal EmergenciesShubham gaurОценок пока нет
- Surgery - PPT'sДокумент172 страницыSurgery - PPT'sShreya KulkarniОценок пока нет
- Endoscopic Telovelar Approach To The Fourth Ventricle - Anatomic StudyДокумент9 страницEndoscopic Telovelar Approach To The Fourth Ventricle - Anatomic StudyfrancsicovillegaslopezОценок пока нет
- Clinical Research: The Surgical Learning Curve For Modified Lapidus Procedure For Hallux Valgus DeformityДокумент5 страницClinical Research: The Surgical Learning Curve For Modified Lapidus Procedure For Hallux Valgus DeformityGeraldine Alvarez AОценок пока нет
- Neurosurgery For NeurologistsДокумент44 страницыNeurosurgery For NeurologistsDilip Kumar MОценок пока нет
- Group 2B Case Study On Ectopic PregnancyДокумент36 страницGroup 2B Case Study On Ectopic PregnancyANGEL GADOОценок пока нет
- EXSA - Gold Award Recipients 2006Документ15 страницEXSA - Gold Award Recipients 2006applebarrel100% (1)
- Batchala 2021Документ6 страницBatchala 2021qrscentralОценок пока нет
- Histology of The Digestive SystemДокумент70 страницHistology of The Digestive Systemiananicole.b30Оценок пока нет
- ObsNGyn - Urogynecology and Mics Topics AtfДокумент17 страницObsNGyn - Urogynecology and Mics Topics AtfarongeremewОценок пока нет
- Recognized Ho So ListДокумент64 страницыRecognized Ho So ListGuru MogaralaОценок пока нет
- Prevention and Management of Airway FireДокумент19 страницPrevention and Management of Airway Fireacegi135Оценок пока нет
- Public Assessment Report Decentralised Procedure: Procedure Number: DE/H/3730/001/DCДокумент12 страницPublic Assessment Report Decentralised Procedure: Procedure Number: DE/H/3730/001/DCafiОценок пока нет
- Cardiac AnatomyДокумент75 страницCardiac AnatomythetlwinagОценок пока нет
- AMC College Return Demonstration VideosДокумент3 страницыAMC College Return Demonstration VideosDoneva Lyn MedinaОценок пока нет
- Hernia protrusion organ tissue openingДокумент1 страницаHernia protrusion organ tissue openingK.P. MOHITHRAJОценок пока нет
- Robodoc Surgical Robot Sucess StoryДокумент3 страницыRobodoc Surgical Robot Sucess StoryPintilie MihaelaОценок пока нет
- Robotic Surgery Techniques and ApplicationsДокумент28 страницRobotic Surgery Techniques and ApplicationsAashi Anand100% (1)
- E023721 FullДокумент9 страницE023721 Fulljimmy xanzОценок пока нет
- Alex Chernov CompletoДокумент4 страницыAlex Chernov CompletolaparovetОценок пока нет
- Varicose Veins Treatment and Prognosis in Ayurveda Ascompared To ModernДокумент3 страницыVaricose Veins Treatment and Prognosis in Ayurveda Ascompared To ModernEditor IJTSRDОценок пока нет
- Figo Consensus Guidelines On Intrapartum Fetal Monitoring: Intermittent AuscultationДокумент7 страницFigo Consensus Guidelines On Intrapartum Fetal Monitoring: Intermittent AuscultationWilliam WongОценок пока нет
- S 0038 1631878Документ11 страницS 0038 1631878Izo ZronОценок пока нет