Академический Документы
Профессиональный Документы
Культура Документы
Neurofibromatosis 5
Загружено:
caliptra36Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Neurofibromatosis 5
Загружено:
caliptra36Авторское право:
Доступные форматы
Case A Case of Intrathoracic Giant Malignant Peripheral
Report Nerve Sheath Tumor in Neurofibromatosis Type I
(von Recklinghausen’s Disease)
Junzo Shimizu, MD,1 Yoshihiko Arano, MD,1 Tomomi Murata, MD,1
Norihiko Ishikawa, MD,1 Tsuyoshi Yachi, MD,1 Tomo Nomura, MD,2 and
Hiroshi Minato, MD3
The patient was a 32-year-old woman with neurofibromatosis I (von Recklinghausen’s disease),
with chief complaints of shortness of breath and back pain. CT and MRI revealed a giant mass
occupying the right thoracic cavity almost completely. The mass compressed the mediastinal
structure to the left and the liver downwards. She underwent surgery to alleviate respiratory
and circulatory disorders caused by compression of the right lung and inferior vena cava due to
the giant tumor. Intraoperatively, the tumor was found to have originated from the 5th intercos-
tal nerve. The resected tumor was 20×17×15 cm in size and 2,300 g in weight. It was histologi-
cally diagnosed as a malignant peripheral nerve sheath tumor. Her postoperative course was
uneventful. All indicators of respiratory function improved, and edema of the lower half of the
body disappeared, accompanied by disappearance of shortness of breath. She was discharged
21 days after surgery. Seven months after surgery, however, a recurrent tumor was found in the
right thoracic cavity. She died of rapid growth of recurrent tumor 3 months thereafter. This
tumor often complicates neurofibromatosis I and has a high frequency of local recurrence and
distant metastasis, resulting in poor prognosis. Neither an optimal extent of resection needed for
complete resection of this tumor nor an optimal regimen of chemotherapy, radiotherapy, or
other therapy for the tumor has yet been established. It is desirable to establish them in the near
future. (Ann Thorac Cardiovasc Surg 2008; 14: 42–47)
Key words: malignant peripheral nerve sheath tumor, neurofibromatosis I, intrathoracic giant tumor
Introduction On the other hand, the incidence of complication by
MPNST is relatively low (2–13%) among patients with
Malignant peripheral nerve sheath tumor (MPNST) ac- NF-1, and MPNST often affects the extremities in these
counts for 5–10% of all malignant soft tissue tumors. Of cases and it rarely develops in the thoracic cavity.1) We
all cases of this tumor, 30–50% are accompanied by neu- recently encountered a case of giant MPNST of the right
rofibromatosis I (NF-1) (von Recklinghausen’s disease). thoracic cavity which complicated NF-1, who was treated
surgically. This paper will present this case, with refer-
From 1Department of Surgery, KKR Hokuriku Hospital; 2Department of ence to the literature.
Internal Medicine, Kanazawa Redcross Hospital; and 3Department
of Clinical Pathology, Kanazawa Medical University, Kanazawa,
Japan Case Report
Received January 15, 2007; accepted for publication March 20, The patient was a 32-year-old woman with NF-1. In De-
2007 cember 2005, she began to complain of shortness of breath
Address reprint requests to Junzo Shimizu, MD: Department of
Surgery, KKR Hokuriku Hospital, 2–13–43 Izumigaoka, Kanazawa, and back pain. A detailed examination at a nearby clinic
Ishikawa 921–8035, Japan. allowed a diagnosis of massive hydrothorax on the right
42 Ann Thorac Cardiovasc Surg Vol. 14, No. 1 (2008)
Intrathoracic Malignant Peripheral Nerve Sheath Tumor
side. She underwent thoracic drainage but adequate elimi-
nation of the thoracic fluid was not achieved. For this
reason, she was referred and admitted to our department
to receive a detailed examination and treatment.
The largest subcutaneous mass (3 cm in diameter) was
found in the left axillary area, accompanied by many soft
subcutaneous masses (below 1 cm in diameter) in the ex-
tremities and countless café au lait spots on systemic skin.
Marked edema was noted in the lower half of her body.
In auscultation, the right respiratory sound was weak and
intense shortness of breath was noted, allowing a rating
of degree V according to the Hugh-Jones classification.
On admission, C reactive protein (CRP) was as high
as 15.46 mg/dL, and elevation of leukocyte count (11,300/
µL) was also noted. Of the tumor markers tested, only
neuron-specific enolase (NSE) was elevated (64 ng/mL).
Arterial blood gas analysis following oxygen inhalation
at a rate of 3 L/min yielded the following results: pH 7.461,
arterial pressure of carbon dioxide (PCO2) 37.6 mmHg,
arterial pressure of oxygen (PO2) 77.6 mmHg, O2 satura- Fig. 1. Chest X-ray revealed no air in the right thoracic cavity and
tion 95.8% and base excess (BE) 3.1 mmol/L (Table. 1). the mediastinal deviation to the left.
Chest X-ray (Fig. 1) revealed no air in the right thoracic
cavity and the mediastinal deviation to the left, while vi-
sualizing the thoracic drain inserted at a nearby clinic. bility of subcutaneous metastasis of the intrathoracic gi-
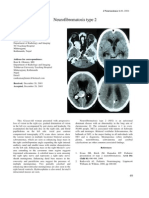
Chest computed tomography (CT) scans disclosed a gi- ant tumor, we first carried out biopsy of the subcutane-
ant mass occupying the right thoracic cavity almost com- ous tumor of the left axillary area (about 3 cm in size).
pletely. The area inside the mass showed an The tumor was pathologically rated as benign neurofi-
unhomogeneous contrast enhancement on contrast-en- broma without mitosis. Thus, a definite diagnosis of in-
hanced CT (Fig. 2). The mass intensely compressed the trathoracic giant tumor was not possible preoperatively.
mediastinal structure (involving the heart, large vessels, However, the intrathoracic tumor seemed to be malig-
trachea, esophagus, etc.) to the left, and the right lung nant in nature, judging from its clinical course and size.
was free of air. Chest magnetic resonance imaging (MRI) She underwent surgery on January 30, 2006, to alleviate
revealed a large mass (19×17×14 cm) in the right tho- respiratory and circulatory disorders caused by compres-
racic cavity. A homogeneously high density was seen sion of the right lung and inferior vena cava (IVC) due to
within the mass already in the early phase of the dynamic the giant tumor. The ideal surgical procedure for cases
study. The mass intensely compressed the mediastinal like this would be to resect only the tumor, while leaving
structure to the left and the liver downwards, but the mass the lung as intact as possible. However, when beginning
was well-demarcated, suggesting the absence of tumor surgery for this case, we made ourselves ready to per-
invasion of the mediastinum or liver (Fig. 3). The feeding form pleuropneumonectomy, against the possibility that,
artery for this tumor seemed to be an intercostals artery, during surgery, we might find extensive tumor invasion
internal thoracic artery, inferior phrenic artery or some- of the lung.
thing of the sort. However, because the CT and MRI find- The chest was opened at the level of the 6th intercostals
ings suggested that the tumor in this case was not very space by means of a long S-shaped skin incision (extend-
invasive, we concluded that it would be relatively easy to ing the standard posterolateral incision forwards and then
deal with the feeding artery. This is why we did not make below the costal arch), as shown in Fig. 4. When we con-
further efforts to identify the feeding artery preoperatively. duct surgery on a giant intrathoracic tumor like the one
On the basis of these findings, she was strongly suspected seen in the present case, we usually adopt a posterolat-
of having an intrathoracic giant malignant neurogenic tu- eral subcostal approach, which involves a larger incision
mor which had complicated NF-1. In view of the possi- than the ordinary posterolateral approach. Our practice is
Ann Thorac Cardiovasc Surg Vol. 14, No. 1 (2008) 43
Shimizu et al.
Fig. 2. Chest CT scan disclosed a giant mass occupying the right Fig. 3. Chest MRI revealed a large mass (19×17×14 cm) in the
thoracic cavity almost completely. The area inside the mass right thoracic cavity. A homogeneously high density was seen
showed an unhomogeneous contrast enhancement on contrast- within the mass already in the early phase of the dynamic study.
enhanced CT. The mass intensely compressed the mediastinal structure to the
left and the liver downwards.
based on the view that an approach allowing safer and
more reliable surgical manipulations in a sufficiently wide
visual field is essential for dealing with this kind of tu-
mor. We adopted this approach for the present case be-
cause the tumor was very large, making it difficult to in-
duce dislocation of the lesion and lung and thus elevating
the risk of major bleeding from a site that was not di-
rectly visible. The tumor occupied the right thoracic cav-
ity, while compressing the entire right lung upwards and
the mediastinum to the left. The tumor had been covered
with a capsule but had not invaded the diaphragm or the
pericardium. Because dislocation of the tumor was not
possible, we were unable to determine whether or not
tumor invasion of the IVC was present. However, tumor Fig. 4. The chest was opened by means of a long S-shaped skin
invasion of the middle and lower lobes of the right lung incision (extending the standard posterolateral incision forwards
was noted. For this reason, partial resection of these lobes and then below the costal arch).
was additionally performed. The border of the mass from
the anterior aspect of the chest wall was not clear, sug-
gesting that the tumor had originated from this area (the side was not broad enough, even using the posterolateral
5th intercostal nerve). To allow an adequate surgical mar- subcostal approach we had adopted (an approach involv-
gin, the 5th costal cartilage, intercostal muscles, inter- ing a larger than ordinary incision), it was not possible to
costal nerves, intercostal arteries and veins were addi- resect the tumor en bloc. It was resected completely after
tionally resected. Since the tumor was large (20 cm in having being divided into two pieces. After tumor resec-
diameter) and because the visual field on the mediastinal tion, expansion of the right lung was resumed, but its ex-
44 Ann Thorac Cardiovasc Surg Vol. 14, No. 1 (2008)
Intrathoracic Malignant Peripheral Nerve Sheath Tumor
pansion was not large enough to completely fill the dead Table 1. Changes of pulmonary function tests
space created by tumor resection. Two thoracic drains Pre Post
were kept inserted and the operation was completed. Spirometry
Her postoperative course was uneventful. All indica- VC(L) 0.84 1.61
%VC 28.7 54.9
tors of respiratory function improved (Table. 1), and
FEV1.0 (L) 0.87 1.70
edema of the lower half of the body disappeared, accom- FEV1.0 (%) 100 100
panied by disappearance of shortness of breath, allowing Blood gas analysis
a rating of degree II according to the Hugh-Jones classi- pH 7.461 7.427
fication. She was discharged 21 days after surgery, re- PaCO2 (mmHg) 37.6 38.9
PaO2 (mmHg) 77.3 84.4
quiring no assistance to walk. Seven months after sur- SaO2 (%) 95.8 96.4
gery, however, a recurrent tumor was found in the right BE (mmol/L) 3.1 1.4
thoracic cavity. She died of tumor 3 months thereafter. Hugh-Jones V° II°
The resected specimen consisted of a huge mass,
Pre, values before surgery under oxygen inhalation at a rate
20×17×15 cm in size, 2,300 g in weight (Fig. 5). It had a
of 3 L/min; Post, values 3 weeks after surgery under room
fleshy appearance with elastic firm and partially muci- air; VC, vital capacity; FEV1.0, forced expiratory volume in
nous consistency. Cut surface was yellow-white to green- 1.0 s; PaCO2, arterial pressure of carbon dioxide; PaO2, ar-
ish-yellow with foci of hemorrhage and necrosis. Histo- terial pressure of oxygen; SaO2, degree of arterial oxygen
logically, the tumor had a spindle-celled fascicular ap- saturation; BE, base excess.
pearance with alternating cellular and less cellular
fibromyxoid areas. Many of the tumor cells had pale,
poorly defined cytoplasm and hyperchromatic nuclei with
a narrow, tapering outline, often with a wavy configura-
tion (Fig. 6). In some cellular areas pleomorphic cells
with clear or eosinophilic cytoplasm, and prominent
nucleoli proliferated intersectingly. Mitoses including
atypical ones were easily found. Perivascular accentua-
tion and infiltration of vessel walls were frequently seen.
The tumor infiltrated focally into the lung parenchyma
which was resected together with the primary lesion.
Immnohistochemically, many tumor cells expressed
CD56, and focally expressed neuron specific enolase
(NSE). The tumor did not express S100 protein, glial
fibrillary acid protein (GFAP), α-smooth muscle actin
Fig. 5. The resected specimen consisted of a huge mass, 20×17×15
(SMA), desmin, myogenin, CD34, and cytokeratin. Based cm in size, 2,300 g in weight It had a fleshy appearance with
on these morphological, immunohistochemical, and clini- elastic firm and partially mucinous consistency.
cal findings, the tumor was diagnosed as MPNST associ-
ated with NF-1.
Discussion neurogenic malignant tumor has also been reported, al-
though in a small number of cases. To put it concretely,
NF-1 was classically called “von Recklinghausen’s dis- Reports have been published concerning cases of NF-1
ease.” It is a genetic disease transmitted via the autoso- complicated by non-neurogenic malignant tumors such
mal dominant trait and involves neurofibroma of skin, as gastric cancer, leiomyosarcoma, lung cancer and gas-
brain, spinal cord and nervous systems, café au lait spots, troenteric cancer.2)
bone lesions, and so on. This disease was named in 1882 Neurogenic malignant tumors are composed of cells
by von Recklinghausen. It has been reported that malig- which constitute the peripheral nerve sheath (schwann
nant nerve sheath tumor, which can determine the prog- cells, perineural cells, etc.) and account for 5–10% of all
nosis, complicates von Recklinghausen’s disease in about malignant soft tissue tumors. In a majority of cases, this
10% of all cases. Complication of this disease by non- type of tumor is accompanied by NF-1. In the past, neu-
Ann Thorac Cardiovasc Surg Vol. 14, No. 1 (2008) 45
Shimizu et al.
The only means of radical treatment for this tumor is
complete surgical resection and the prognosis of patients
with MPNST is significantly determined by whether or
not complete resection has been achieved.7,8) We cannot
rule out that the separated resection served as one of the
factors responsible for the post-surgical recurrence. How-
ever, we chose the separated resection out of consider-
ation that major bleeding due to injury of the IVC could
develop if the operation were performed without adequate
determination of orientation. Resection of about half of
the giant tumor made it possible for us to induce disloca-
tion of the tumor. This is probably the reason that we
succeeded in safely resecting the tumor while viewing
Fig. 6. Histologically, the tumor showed a spindle-shaped fas-
the IVC directly, without causing bleeding. Regarding the
cicular and intersecting appearance with pale or eosinophilic
operative procedure we selected, we now reflect that we
cytoplasm. The nuclei were hyperchromatic with a tapering out-
line and a wavy configuration. Large atypical cells with promi- should have adopted pleuropneumonectomy, accompa-
nent nucleoli were frequently seen (HE stain, original magnifi- nied by resection of the diaphragm and pericardium, to
cation, ×400). achieve a safety margin. However, regarding post-surgi-
cal recurrence of MPNST, we think that its recurrence is
primarily associated with the biological malignancy level
rogenic malignant tumors were classified into malignant of MPNST.
schwannoma, neurofibrosarcoma, neurogenic sarcoma On the other hand, the extent of resection needed for
and so on. However, the third edition of the General Rules complete resection of this tumor has not been established,
for Surgical and Pathological Studies on Malignant Soft and quite high postoperative recurrence rates have been
Tissue Tumors, prepared in July 2002,3) combined these reported, i.e., 45.0% (28/62) by Ducatman et al.,9) 43.1%
tumors into a single disease entity “malignant peripheral (85/197) by Taniguchi et al.7) and 46.4% (13/28) by
nerve sheath tumor (MPNST).” MPNST is defined as tu- Wanebo et al.10) As a means of reducing the local recur-
mors satisfying at least one of the following four require- rence rate of this tumor, Kunisada et al.11) recommended
ments: (i) malignant tumors arising from peripheral nerves resection with an at least a 3 cm safety margin, and
or continuous to nerves, (ii) benign neurogenic tumors Angelov et al.12) reported better prognosis following re-
(e.g., neurofibroma) having been converted into malig- section with a 5 cm or more margin. In the present case,
nant tumors; (iii) malignant tumors developing in NF-1 it was difficult to take a 5 cm or more safety margin be-
cases, and (iv) tumors having histological features simi- cause the tumor was located close to the lung, IVC,
lar to those of the above-mentioned three types, accom- esophagus, diaphragma and liver.
panied by evident immunohistological or electron-micro- According to many reports, chemotherapy and radio-
scopic signs of differentiation into the nerve sheath. therapy are often ineffective against this tumor. However,
MPNST primarily affects extremities, but it can de- cases responding well to high-dose chemotherapy with
velop in other various sites including the trunk, head/neck ifosfamide, vincristine, doxorubicin or cyclophospha-
region and so on. However, its onset in the thoracic cav- mide13) and cases making remarkable responses to post-
ity, as seen in the present case, is very rare.4–6) A typical operative high-dose radiation14) have recently been re-
clinical sign of MPNST having developed on the body ported. An appropriate next step would seem to be to
surface is a rapidly growing hard red mass palpable on evaluate the efficacy of these methods of treatment.
the skin surface. However, if MPNST originates from the Regarding distant metastasis of MPNST, the incidence
nerves of deep tissue, like in the present case, direct ob- of distant metastasis (primarily to the lungs) has been
servation of the tumor is not possible, and early diagno- reported to be 39.0% by Ducatman et al.9) and 17.9% by
sis is difficult. Because of difficulty in early diagnosis, Wanebo et al.10) Distant metastasis of this tumor assumes
MPNST is often detected as a tumor with large diameter, the form of blood-borne metastasis in most cases, and
showing invasion along the nerves. For this reason, sur- metastasis to lymph nodes is rare.9,10)
gical resection tends to be incomplete. The 5-year survival rate of patients with this tumor
46 Ann Thorac Cardiovasc Surg Vol. 14, No. 1 (2008)
Intrathoracic Malignant Peripheral Nerve Sheath Tumor
has been reported to be 12.8% by Taniguchi et al.7) and (in Jpse.)
16.0% by Ducatman et al.9) Thus, the prognosis of pa- 4. Inoue M, Mitsudomi T, Osaki T, Oyama T, Haratake J,
et al. Malignant transformation of an intrathoracic neu-
tients with this tumor is poor. Factors possibly respon-
rofibroma in von Recklinghausen’s disease. Scand
sible for the poor prognosis are: (i) tumor onset at a rela- Cardiovasc J 1998; 32: 173–5.
tively low age, (ii) difficulty in early diagnosis if located 5. Park JH, Choi KH, Lee HB, Rhee YK, Lee YC, et al.
in deep tissue, and (iii) high incidence of death from dis- Intrathoracic malignant peripheral nerve sheath tumor
tant metastasis due to likelihood for repeated local recur- in von Recklinghausen’s disease. Korean J Intern Med
rence following surgical resection because the extent of 2001; 16: 201–4.
6. Kim JG, Sung WJ, Kim DH, Kim YH, Sohn SK, et al.
resection needed for complete tumor resection has not Malignant peripheral nerve sheath tumor in neurofi-
been established. In the present case, local recurrence was bromatosis type I: unusual presentation of intraab-
seen 7 months after surgery, resulting in rapid growth of dominal or intrathoracic mass. Korean J Intern Med
the recurrent tumor and death from tumor. 2005; 20: 100–4.
7. Taniguchi A, Nogawa A, Takada M, Hashimoto T,
Kimura S, et al. Malignant schwannoma in von
Conclusion Recklinghausen’s disease. Report of two cases and sta-
tistical analysis of Japanese reports. Skin Cancer 1992;
A case of MPNST, having developed in the thoracic cav- 7: 78–83. (in Jpse.)
ity, was presented. This tumor often complicates NF-1 8. Asai K, Suzuki K, Shimota H, Takahashi T, Yamashita
and has a high frequency of local recurrence and distant K, et al. Malignant peripheral nerve sheath tumor of
the mediastinum: a temporary aortic transection ap-
metastasis, resulting in poor prognosis. Neither an opti-
proach. J Thorac Cardiovasc Surg 2004; 128: 615–7.
mal extent of resection needed for complete resection of 9. Ducatman BS, Scheithauer BW, Piepgras DG, Reiman
this tumor nor an optimal regimen of chemotherapy, ra- HM, Ilstrup DM. Malignant peripheral nerve sheath
diotherapy or other therapy for the tumor has yet been tumors. A clinicopathologic study of 120 cases. Can-
established. It is desirable to establish them in the near cer 1986; 57: 2006–21.
future. 10. Wanebo JE, Malik JM, VandenBerg SR, Wanebo HJ,
Driesen N, et al. Malignant peripheral nerve sheath
tumors. A clinicopathologic study of 28 cases. Cancer
References 1993; 71: 1247–53.
11. Kunisada T, Kawai A, Ozaki T, Sugihara S, Taguchi K,
1. Asavamongkolkul A, Jiranantakan T, Waikakul S, et al. A clinical analysis of malignant schwannoma.
Phompitaksa K, Muangsomboon S. Malignant periph- Acta Med Okayama 1997; 51: 87–92.
eral nerve sheath tumor with neurofibromatosis type 12. Angelov L, Davis A, O’Sullivan B, Bell R, Guha A.
1: a 2-case report and review of the literature. J Med Neurogenic sarcomas: experience at the University of
Assoc Thai 2001; 84: 285–93. Toronto. Neurosurgery 1998; 43: 56–65.
2. Morikawa M, Hayashi H, Hosokawa O, Kaizaki Y, 13. Masui F, Yokoyama R, Soshi S, Beppu Y, Asanuma K,
Doden K, et al. A case of collision tumor in the papilla et al. A malignant peripheral nerve-sheath tumor re-
of Vater for quintuple cancer associated with von sponding to chemotherapy. J Bone Joint Surg Br 2004;
Recklinghausen’s disease. Gastroenterol Endosco 86: 113–5.
2006; 48: 1437–41. (in Jpse. with Engl. Abstr.) 14. Yone K, Ijiri K, Hayashi K, Yokouchi M, Takenouchi
3. The Orthopedics Surgical Society. General rules for T, et al. Primary malignant peripheral nerve sheath tu-
clinical and pathological studies on malignant soft tis- mor of the cauda equina in a child case report. Spinal
sue tumors. 3rd ed. Tokyo: Kanehara, 2002; pp150–8. Cord 2004; 42: 199–203.
Ann Thorac Cardiovasc Surg Vol. 14, No. 1 (2008) 47
Вам также может понравиться
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5795)
- Neurofibromatosis 28Документ2 страницыNeurofibromatosis 28caliptra36100% (1)
- Facing Neurofibromatosis: A Guide For TeensДокумент10 страницFacing Neurofibromatosis: A Guide For Teenscaliptra36Оценок пока нет
- Neurofibromatosis 21Документ1 страницаNeurofibromatosis 21caliptra36Оценок пока нет
- Neurofibromatosis 12Документ1 страницаNeurofibromatosis 12caliptra36Оценок пока нет
- Testosterone Deficiency Syndrome 3Документ2 страницыTestosterone Deficiency Syndrome 3caliptra36Оценок пока нет
- Hernia Repair 3Документ38 страницHernia Repair 3caliptra36Оценок пока нет
- Hernia Repair 2Документ8 страницHernia Repair 2caliptra36Оценок пока нет
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Of Gods, Glyphs and KingsДокумент24 страницыOf Gods, Glyphs and KingsBraulioОценок пока нет
- Bcos 186Документ3 страницыBcos 186Shiv KumarОценок пока нет
- CPP CheatsheetДокумент10 страницCPP CheatsheetPrakash GavelОценок пока нет
- Brochure Bucket SolutionsДокумент20 страницBrochure Bucket Solutionsmuhammad febri faizinОценок пока нет
- EXERCISE 1-Passive FormДокумент5 страницEXERCISE 1-Passive FormMichele LangОценок пока нет
- A Feasibility/Project Study OnДокумент14 страницA Feasibility/Project Study OnWilson Domingo LazarteОценок пока нет
- CREW Whitaker Recusal Letter DOJ 11-8-2018Документ9 страницCREW Whitaker Recusal Letter DOJ 11-8-2018Beverly TranОценок пока нет
- 1 SAP HCM Overview - IntroductionДокумент32 страницы1 SAP HCM Overview - IntroductionashwiniОценок пока нет
- Hindu Succession-Male & FemaleДокумент14 страницHindu Succession-Male & FemaleKumar MangalamОценок пока нет
- Convention Concerning The Protection of The WorldДокумент41 страницаConvention Concerning The Protection of The WorldMonica Ardeleanu100% (1)
- Internship Proposal FormДокумент3 страницыInternship Proposal FormMuhammad FidaОценок пока нет
- Sen Çal KapımıДокумент9 страницSen Çal KapımıMa Gabriela Ojeda CasellaОценок пока нет
- Bang Thong Ke Phep NamДокумент16 страницBang Thong Ke Phep NamTiến Tươi TỉnhОценок пока нет
- Lesson Plan 4Документ6 страницLesson Plan 4Lilay Barambangan100% (3)
- NMC CBT Sample Q&a Part 3 AcДокумент14 страницNMC CBT Sample Q&a Part 3 AcJoane FranciscoОценок пока нет
- Part D - Disclosure and TransparencyДокумент21 страницаPart D - Disclosure and TransparencyMuhammadYudithEddwinaОценок пока нет
- RLB Procuring For Value 18 July PDFДокумент56 страницRLB Procuring For Value 18 July PDFDaniel LixandruОценок пока нет
- My Kindergarten BookДокумент48 страницMy Kindergarten BookfranciscoОценок пока нет
- Markets and Commodity Figures: Total Market Turnover StatisticsДокумент6 страницMarkets and Commodity Figures: Total Market Turnover StatisticsTiso Blackstar GroupОценок пока нет
- Errors Affecting The Trial BalanceДокумент3 страницыErrors Affecting The Trial BalanceDarwin Lopez100% (1)
- UNIX Introduction 1Документ18 страницUNIX Introduction 1Akash SavaliyaОценок пока нет
- Soal Materi 1 KLS X IntroductionДокумент2 страницыSoal Materi 1 KLS X IntroductionFira AnandaОценок пока нет
- Alcatel 9400 PDFДокумент4 страницыAlcatel 9400 PDFNdambuki DicksonОценок пока нет
- Optical CamouflageДокумент27 страницOptical CamouflageAlliluddin ShaikОценок пока нет
- Maulana Azad Library, Aligarh Muslim UniversityДокумент38 страницMaulana Azad Library, Aligarh Muslim Universitybijesh babuОценок пока нет
- The Brain in Your Pocket Evidence - That - SДокумент8 страницThe Brain in Your Pocket Evidence - That - Sanwaarft123Оценок пока нет
- Nabard Working CapitalДокумент12 страницNabard Working CapitalJaspreet SinghОценок пока нет
- Floline Size eДокумент4 страницыFloline Size eNikesh ShahОценок пока нет
- West Bengal State University Department of EnglishДокумент33 страницыWest Bengal State University Department of Englishnandan yadavОценок пока нет
- STD 12 Accountancy1Документ264 страницыSTD 12 Accountancy1Chetan KhonaОценок пока нет