Академический Документы
Профессиональный Документы
Культура Документы
Predictive Risk Factors in Double-Valve Replacement (AVR and MVR) Compared To Isolated Aortic Valve Replacement
Загружено:
DanteОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Predictive Risk Factors in Double-Valve Replacement (AVR and MVR) Compared To Isolated Aortic Valve Replacement
Загружено:
DanteАвторское право:
Доступные форматы
J.
Litmathe
M. Kurt
P. Feindt
E. Gams
Predictive Risk Factors in Double-Valve
Replacement (AVR and MVR) Compared to
Isolated Aortic Valve Replacement
Background: The operative risk of combined aortic and mitral
surgery is still between 5 and 13 %, whereas isolated AVR normally causes complications in less than 4 % of all patients. Thus,
it was the aim of the study to compare both procedures and to
evaluate risk stratification in our patient cohort. Patients and
Methods: The inhospital mortality and complication rates were
analyzed in both groups over a period of 4 years. There were 396
patients with isolated AVR, and 98 patients with AVR and MVR.
For both groups, we investigated 16 possible risk factors for perioperative death or severe complications, such as low cardiac output syndrome (LCOS). The risk factors were analyzed by univariate analysis, and factors with p < 0.01 were entered into a multivariate analysis. Results: There were 11/396 perioperative deaths
in patients with AVR (2.8 %) compared to 5/98 (5.1 %) in DVR. The
incidence of major complications was 5.3 % in AVR vs. 11.2 % in
DVR. As risk factors (p < 0.05) for death, we found in AVR: former
Introduction
Although many previous reports on simultaneous double-valve
replacement (DVR) have compared the long-term outcome according to the type or combination of the implanted prosthesis,
controversy persists regarding the ideal selection of heart valve
cardiac surgery, aortic stenosis, and pulmonary arterial pressure
> 55 mmHg. In patients with DVR, we additionally found: left atrial pressure (LAP) > 20 mmHg and creatinine > 2 mg/dl. Risk factors for severe complications in AVR were: former cardiac surgery and creatinine > 2 mg/dl, in cases of DVR, additionally: tricuspid valve disease (TVD) and LAP > 20 mmHg. Conclusions:
Our analysis of risk factors shows that in patients with DVR preoperative parameters, which sometimes are estimated to be unimportant, may cause an adverse outcome. The operation should
be carried out before reaching advanced or even end-stage heart
failure, and more attention should be paid to an individual perioperative concept and optimized myocardial protection in such
patients.
Original Cardiovascular
Abstract
Key words
Aortic valve replacement double-valve replacement risk factor
regression analysis
459
prosthesis in DVR [1 3, 5, 8, 9]. Few reports on simultaneous
DVR have been made which examine the influence of not only
the type and combination of valve prosthesis but also of other
preoperative and intraoperative variables that influence early
and late mortality and morbidity [4 10].
Affiliation
Department of Thoracic and Cardiovascular Surgery, Heinrich-Heine-University Hospital,
Dsseldorf, Germany
Dedication
The results of this paper were presented in part during the 34th annual meeting of the
German Society of Thoracic- and Cardiovascular Surgery, February 13th 16th, 2005
in Hamburg/Germany as poster presentation.
Correspondence
M. Kurt Department of Thoracic and Cardiovascular Surgery Moorenstrae 5 40225 Dsseldorf
Germany Phone: + 49 21181183 32 Fax: + 49 2118 1183 33 E-mail: litmathe@med.uni-duesseldorf.de
Received January 20, 2006
Bibliography
Thorac Cardiov Surg 2006; 54: 459 463 Georg Thieme Verlag KG Stuttgart New York
DOI 10.1055/s-2006-924247
ISSN 0171-6425
Downloaded by: World Health Organization ( WHO). Copyrighted material.
U. Boeken
The operative risk of combined aortic and mitral surgery is still
between 5 and 13 %, whereas an isolated AVR normally causes severe complications in less than 4 % of patients [9,10]. It was the
aim of our study to identify the main perioperative risk factors
which may be responsible for this significantly increased incidence of adverse events in simultaneous DVR in 98 patients.
Table 1 Suspected preoperative risk factors
Redo surgery (former cardiac surgery)
Tricuspid valve disease (TVD)
LAP 20 mmHg
Creatinine 2 mg/dl
Patients and Methods
Urgent operation
Age > 70 years
LV-EF 0.35
IDDM
Anemia (Hb 10 g/dl)
Aortic stenosis
Previous neurological events
Cardiogenic shock
Peripheral vascular disease
The mean age of the entire cohort was 63.8 6.8 years, without
significant differences between the groups (AVR: 62.4 6.6 vs.
DVR: 64.1 6.7 years). For both groups, we investigated probable
risk factors for perioperative death or major complications, such
as cardiogenic shock (systolic arterial pressure < 90 mmHg for
more than 30 min, oliguria/anuria, somnolence), low cardiac
output syndrome (LCOS with ejection fraction < 35 % and catecholamine therapy for hemodynamic stabilization), prolonged
stay in the ICU, prolonged ventilation, need of catecholamines,
major neurological complications (stroke), tricuspid valve disease (severe insufficiency) or severe infection (Table 1).
Statistical methods
Our aim was to validate identification factors (predictors) for a
complicated course or an adverse outcome after valve replacement procedures. In particular, the differences between an
isolated aortic valve replacement and a double-valve replacement, including the aortic and mitral valve (DVR), were examined. We used multivariate analysis, limited to variables that
were known prior to operation. The risk factors with p 0.01
were entered into multivariate analysis.
A subsequent analysis was performed with preoperative variables to determine factors associated with perioperative complications, especially the additional risk factors in DVR.
We then used independent predictive variables from regression
analysis to generate a risk score (RS) for death or severe complications in AVR and DVR. We derived the points in the scoring system from the regression coefficient, the odds ratio and the clinical relevance. The patients were stratified from low to high risk
for death or severe complications based on their individual risk
scores. Ninety-five percent confidence intervals were calculated
for each risk interval.
Operative procedure
All operations were performed using a median sternotomy, with
the help of cardiopulmonary bypass (CPB) in moderate hypothermia and cardioplegic arrest using Bretschneiders solution.
The anticoagulation regime in both groups during the postoperative course was maintained using heparin and coumarone immediately after removing the chest tubes, in cases of mechanical
Litmathe J et al. Predictive Risk Factors Thorac Cardiov Surg 2006; 54: 459 463
Coagulopathy
valve replacement or persistent atrial fibrillation. The proportion
of mechanical valves was 65 % in the isolated AVR group and
70.5% in the DVR group.
Altogether, 16 perioperative factors were validated. We did not
compare the results between both groups with regard to intraoperative parameters due to the substantial differences between
the operative procedures. It is obvious that in DVR procedures,
the duration of extracorporeal circulation (ECC) and of myocardial ischemia is normally prolonged compared to AVR. Thus, it
was our aim to find additional parameters that may result in an
adverse outcome, independent from the time of ECC or myocardial ischemia. Table 1 gives a short overview concerning the suspected predictive factors.
Results
Data was completely available for 93 % of patients. Intraoperative
data were as follows: mean duration of the entire operation was
184 17 min, mean ECC time was 84 10 min and mean ischemic
time 55 8 min in the isolated AVR group. In the DVR group, the
times were 239 30 min (duration of entire operation), 128
16 min (ECC time) and 89 11 min (ischemic time).
There were 11 perioperative deaths in patients with isolated AVR
(2.8 %) compared to 5 (5.1 %) in the DVR group. The incidence of
major complications was 5.3 % in the AVR group vs. 11.2 % in patients undergoing DVR (Fig. 1).
Multivariate analysis could identify identify six parameters as
predictors for death in isolated AVR (redo surgery, aortic stenosis,
PAP 55 mmHg, cardiogenic shock, severely reduced left ventricular function and age > 70 years); seven parameters were additionally identified as predictors for severe complications in
isolated AVR (redo surgery, creatinine 2 mg/dl, aortic stenosis,
cardiogenic shock, IDDM, coagulopathy, PAP 55 mmHg). The coefficient, the odds ratio, and the 95 % confidence interval with
the corresponding p value are shown in Tables 2, 3.
Downloaded by: World Health Organization ( WHO). Copyrighted material.
Original Cardiovascular
460
Over a period of 4 years, we investigated 396 patients with isolated aortic valve replacement (AVR) and 98 patients undergoing
aortic and mitral valve replacement (DVR) and performed a retrospective analysis. All elective and emergent procedures as well as
redo operations were included. The study included a total of 302
male and 192 female patients (AVR: 238/158 vs. DVR: 59/39).
Predictor
-coefficient
Odds
ratio
95 % Confidence interval
P value
Table 3 Predictive factors for severe complications in AVR with
corresponding -coefficient, odds ratio, 95% confidence interval, and p value
Predictor
-coefficient
Odds ratio
95% Confidence interval
P value
Redo surgery
1.73
7.1
4.6 12.8
0.01
Aortic stenosis
1.52
5.2
2.0 7.5
0.001
Redo surgery
1.87
7.4
4.4 13.3
0.001
Creatinine
2 mg/dl
1.66
6.9
4.4 12.4
0.01
Aortic
stenosis
1.46
4.5
1.2 7.8
0.003
Cardiogenic
shock
1.45
3.7
2.0 5.8
0.001
IDDM
1.22
4.1
2.7 6.5
0.01
Coagulopathy
1.12
2.2
1.7 2.9
0.004
PAP
55 mmHg
1.01
1.7
0.9 1.9
0.0006
PAP 55 mmHg
1.48
4.8
1.8 7.2
0.02
Cardiogenic shock
1.42
4.8
1.9 6.8
0.001
LV-EF 0.35
1.33
3.3
2.1 5.2
0.003
Age > 70 years
1.08
2.7
1.8 3.8
0.01
For the DVR group multivariate analysis identified redo surgery,
coexisting tricuspid valve disease, LAP 20 mmHg, creatinine
2 mg/dl, PAP 55 mmHg, cardiogenic shock, age > 70 years, severely reduced left ventricular function, IDDM and anemia as predictors for death, whereas cardiogenic shock, coexisting tricuspid
valve disease, LAP 20 mmHg, redo surgery, creatinine > 2 mg/dl,
severely reduced left ventricular function and IDDM could be
identified as predictors for severe complications. The -coefficient, the odds ratio, and the 95 % confidence interval with the
corresponding p value of these factors are shown in Tables 4, 5.
The predictive value and, therefore, the risk score for severe complications or death was calculated for these factors. The highest
scores were calculated for the predictor redo surgery for isolated
AVR and for the predictors cardiogenic shock and tricuspid valve
disease for patients undergoing DVR (Tables 6, 7).
Discussion
Combined aortic and mitral valve surgery has a substantial morbidity and mortality [11 15]. Our analysis of risk factors was
able to show that in patients with DVR preoperative parameters,
which sometimes seem to be unimportant, may cause an adverse
outcome. Carrying out the operation before the patient is in an
advanced stage of heart failure and the use of an optimized myocardial protection seems to be of great importance for such patients.
Our results suggest that combined surgery can be performed
with an acceptable risk but, predictably, this remains higher
compared to isolated aortic valve replacement. In most cases,
sudden death and heart failure are the major causes of death.
The most prominent risk factor for death or severe complications
after double valve replacement in our analysis was concomitant
tricuspid valve disease and perioperative cardiogenic shock. The
prognostic importance of preoperatively increased pulmonary
vascular resistance points to the impact of chronic pressure load
on the right ventricle for the postoperative outcome. Thus, not
Litmathe J et al. Predictive Risk Factors Thorac Cardiov Surg 2006; 54: 459 463
Original Cardiovascular
Table 2 Predictive factors for death in AVR with corresponding coefficient, odds ratio, 95% confidence interval, and p value
461
Downloaded by: World Health Organization ( WHO). Copyrighted material.
Fig. 1 Major complications and mortality in
both groups.
-coefficient
Odds
ratio
95 % Confidence
interval
P value
Redo surgery
1.88
7.2
4.8 18.1
0.001
Tricuspid valve
disease (TVD)
1.53
4.8
1.7 7.3
LAP 20 mmHg
1.51
4.0
Creatinine 2 mg/dl
1.48
3.6
Predictor
Original Cardiovascular
462
PAP 55 mmHg
1.28
2.7
Table 5 Predictive factors for severe complications in DVR with
corresponding -coefficient, odds ratio, 95% confidence interval, and p value
Predictor
-coefficient
Odds
ratio
95% confidence interval
P value
2.14
4.8
2.5 13.0
0.004
0.01
Cardiogenic
shock
6.8
4.3 12.2
0.001
0.02
Tricuspid valve
disease (TVD)
1.98
2.6 7.4
2.2 5.4
0.001
LAP 20 mmHg
1.52
3.0
2.2 10.2
0.01
0.0001
Redo surgery
1.45
2.8
2.4 11.8
0.003
Creatinine
2 mg/dl
1.38
2.8
2.5 10.2
0.001
LV-EF 0.35
1.03
2.2
2.0 3.7
0.02
IDDM
1.01
1.6
0.8 2.0
0.02
1.8 5.9
Cardiogenic shock
0.96
2.1
1.6 3.1
0.004
Age > 70 years
0.84
1.5 3.3
0.01
LV-EF 0.35
0.7
1.7
1.3 2.4
0.04
IDDM
0.5
1.5
1.1 2.7
0.0001
Hb < 10 g/dl
0.45
1.3
1.1 2.4
0.0001
Table 6 Risk score for death and severe complications after AVR
Table 7 Risk score for death and severe complications after DVR
Predictor
Risk score (RS)
Predictor
Risk score (RS)
Redo surgery
Cardiogenic shock
Creatinine 2 mg/dl
Tricuspid valve disease (TVD)
Aortic stenosis
LAP 20 mmHg
Cardiogenic shock
Redo surgery
IDDM
Creatinine 2 mg/dl
Coagulopathy
EF 0.35
PAP 55 mmHg
IDDM
only the actual diseased tricuspid valve but also chronic overload
of the right ventricle with dilation and possibly biventricular failure may complicate the postoperative course. Tricuspid valve repair should be performed when significant hemodynamic regurgitation is present, because such disease does not disappear after
correction of the left side. However, this will lead to an increase
in the duration of the entire operation [16,17].
High left atrial pressure was another prominent predictor for
death or major complications following double-valve replacement. This is yet another reflection of a chronically high preload
and correspondingly impaired cardiac function. It is, therefore,
important to consider prior to the operation what the best conservative compensation strategy could be.
Other groups have already reported that the potential for recovery after successful double-valve replacement is limited when
preoperative systolic function is severely decreased [13,18,19], a
finding which was borne out by our current series, which showed
an ejection fraction below 35 % to be one of the predictors with a
relatively high score.
Litmathe J et al. Predictive Risk Factors Thorac Cardiov Surg 2006; 54: 459 463
Finally, redo surgery and impaired renal function were identified
as risk factors with a moderate score after double-valve replacement, whereas former cardiac surgery was shown to be one of
the most powerful predictors in isolated aortic valve replacement. It is obvious that both surgical adhesions and complete renal failure may worsen the postoperative course.
A possible limitation of the study is its retrospective character.
Additional follow-up may be able to show the current status of
all survivors in the near future.
In summary, biventricular failure and redo surgery were found to
be the most prominent predictors for adverse events after AVR
and/or DVR. However, in contrast to the EuroSCORE or comparable systems which are nonspecific for all cardiac operations [20],
the impact of the individual risk score was specific for each type
of operation. On the basis of such information, we concluded that
stabilization of the hemodynamic situation of a critical patient
prior to surgery and the treatment of concomitant cardiac disease has an important impact on subsequent outcomes.
Downloaded by: World Health Organization ( WHO). Copyrighted material.
Table 4 Predictive factors for death in DVR with corresponding coefficient, odds ratio, 95% confidence interval, and p value
10
12
13
14
15
16
17
18
19
20
Galloway AC, Grossi EA, Baumann FG et al. Multiple valve operation
for advanced valvular heart disease: results and risk factors in 513 patients. J Am Coll Cardiol 1992; 19: 725 732
Edmunds LH, Clark RE, Cohn LH, Grunkemeier GL, Miller C, Weisel RD.
Guidelines for reporting morbidity and mortality after cardiac valvular operations. Ann Thorac Surg 1996; 62: 932 935
Turina J, Stark T, Seifert B, Turina M. Predictors of the long-term outcome after combined aortic and mitral valve surgery. Circul 1999; 100
(Suppl 2): 48 53
Bebatz LF, Ruchat P, Hurni M. St. Jude Medical valve prosthesis: an
analysis of long-term outcome and prognostic factors. J Thorac Cardiovasc Surg 1997; 113: 134 148
Mueller XM, Tevaearai HT, Stumpe F. Long-term results of mitralaortic valve operations. J Thorac Cardiovasc Surg 1998; 115: 1298
1309
Simon R, Oelert H, Borst HG, Lichtlen P. Influence of mitral valve surgery on tricuspid incompetence concomitant with mitral valve disease. Circul 1980; 62: 1152 1157
King RM, Schaff HV, Danielson GK, Gersh BJ, Orszulak TA, Pichler JM,
Puga FJ, Pluth JR. Surgery for tricuspid regurgitation late after mitral
valve replacement. Circul 1984; 70 (Suppl 2): 193 197
Cohn LH, Couper GS, Aranki SF, Rizzo RJ, Kinchla NM, Collins JJ. Longterm results of mitral valve reconstruction for regurgitation of the
myxomatous mitral valve. J Thorac Cardiovasc Surg 1994; 107: 143
151
Turina J, Milinic J, Seifert B, Turina M. Valve replacement in chronic
aortic regurgitation: true predictors of survival after extended follow-up. Circul 1998; 98 (Suppl 2): 100 107
Nashef SA, Roques F, Michel P, Cortina J, Faichney A, Gams E, Harjula A,
Jones MT. Coronary surgery in Europe: comparison of the national
subsets of the european system for cardiac operative risk evaluation
database. Eur J Cardiothorac Surg 2000; 17: 396 399
Original Cardiovascular
Bortolotti U, Milano A, Testolini L, Trusi V, Mazzucco A, Gallucci V. Influence of type of prosthesis on late results after combined mitralaortic valve replacement. Ann Thorac Surg 1995; 59: 1113 1119
Munro AL, Jamieson E, Burr LH, Ling H, Miyagishima RT, Germann E.
Comparison of porcine bioprostheses and mechanical prostheses in
multiple valve replacement operations. Ann Thorac Surg 1995; 60:
459 463
Khan SS, Trento A, DeRobertis M. Twenty-year comparison of tissue
and mechanical valve replacement. J Thorac Cardiovasc Surg 2001;
122: 257 269
Kuwaki K, Tsukamoto M, Komatsu K, Morishita K, Sakata J, Abe T. Simultaneous aortic and mitral valve replacement: predictors of adverse outcome. J Heart Valve Dis 2003; 12: 169 176
Armenti F, Stephenson LW, Edmunds LH. Simultaneous implantation
of St. Jude Medical aortic and mitral prostheses. J Thorac Cardiovasc
Surg 1987; 94: 733 739
Arom KV, Nicoloff DM, Kersten TE, Northrup WF, Lindsay WG, Emery
RW. Ten-year follow-up study of patients who had double valve replacement with the St. Jude Medical prosthesis. J Thorac Cardiovasc
Surg 1989; 98: 1008 1016
Teoh KH, Christakis GT, Weisel RD. The determinants of mortality and
morbidity after multiple-valve operations. Ann Thorac Surg 1987; 43:
353 358
Fiore AC, Swartz MT, Sharp T. Double-valve replacement with Medtronic Hall or St. Jude valve. Ann Thorac Surg 1995; 59: 1113 1119
Brown PS, Roberts CS, McIntosh CL, Swain JA, Clark RE. Relation between choice of prostheses and late outcome in double-valve replacement. Ann Thorac Surg 1993; 66: 631 640
Caus T, Rouviere P, Clooart F, Mouly-Bandini A, Monties JR, Mesana T.
Late results of double-valve replacement with biological or mechanical prostheses. Ann Thorac Surg 2001; 71: 261 263
11
463
Litmathe J et al. Predictive Risk Factors Thorac Cardiov Surg 2006; 54: 459 463
Downloaded by: World Health Organization ( WHO). Copyrighted material.
References
Вам также может понравиться
- The Construction of Optimal Portfolio Using Sharpe's Single Index Model - An Empirical Study On Nifty Metal IndexДокумент9 страницThe Construction of Optimal Portfolio Using Sharpe's Single Index Model - An Empirical Study On Nifty Metal IndexRevanKumarBattuОценок пока нет
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Project ManagementДокумент11 страницProject ManagementBonaventure NzeyimanaОценок пока нет
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- Chapter 1 To 5 For Printing.2Документ86 страницChapter 1 To 5 For Printing.2Senku ishigamiОценок пока нет
- 1.technical Specifications (Piling)Документ15 страниц1.technical Specifications (Piling)Kunal Panchal100% (2)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- C - Amarjit Singh So Bhura SinghДокумент5 страницC - Amarjit Singh So Bhura SinghRohit JindalОценок пока нет
- Lesson PlanДокумент2 страницыLesson Plannicole rigonОценок пока нет
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Career Essay 1Документ2 страницыCareer Essay 1api-572592063Оценок пока нет
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Science7 - q1 - Mod3 - Distinguishing Mixtures From Substances - v5Документ25 страницScience7 - q1 - Mod3 - Distinguishing Mixtures From Substances - v5Bella BalendresОценок пока нет
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- E Flight Journal Aero Special 2018 Small PDFДокумент44 страницыE Flight Journal Aero Special 2018 Small PDFMalburg100% (1)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Thermally Curable Polystyrene Via Click ChemistryДокумент4 страницыThermally Curable Polystyrene Via Click ChemistryDanesh AzОценок пока нет
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Working With Difficult People Online WorksheetДокумент4 страницыWorking With Difficult People Online WorksheetHugh Fox IIIОценок пока нет
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- HirePro Video Proctored Online-Instruction Sheet - Bain IndiaДокумент1 страницаHirePro Video Proctored Online-Instruction Sheet - Bain Indiaapoorv sharmaОценок пока нет
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- Strucure Design and Multi - Objective Optimization of A Novel NPR Bumber SystemДокумент19 страницStrucure Design and Multi - Objective Optimization of A Novel NPR Bumber System施元Оценок пока нет
- SSGC-RSGLEG Draft Study On The Applicability of IAL To Cyber Threats Against Civil AviationДокумент41 страницаSSGC-RSGLEG Draft Study On The Applicability of IAL To Cyber Threats Against Civil AviationPrachita AgrawalОценок пока нет
- of Thesis ProjectДокумент2 страницыof Thesis ProjectmoonОценок пока нет
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
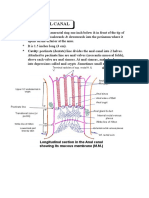
- Anatomy Anal CanalДокумент14 страницAnatomy Anal CanalBela Ronaldoe100% (1)
- CH 1 - Democracy and American PoliticsДокумент9 страницCH 1 - Democracy and American PoliticsAndrew Philip ClarkОценок пока нет
- Soft Ground Improvement Using Electro-Osmosis.Документ6 страницSoft Ground Improvement Using Electro-Osmosis.Vincent Ling M SОценок пока нет
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- ISO 9001 2015 AwarenessДокумент23 страницыISO 9001 2015 AwarenessSeni Oke0% (1)
- Azimuth Steueung - EngДокумент13 страницAzimuth Steueung - EnglacothОценок пока нет
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- Technical Specification For 33KV VCB BoardДокумент7 страницTechnical Specification For 33KV VCB BoardDipankar ChatterjeeОценок пока нет
- Regions of Alaska PresentationДокумент15 страницRegions of Alaska Presentationapi-260890532Оценок пока нет
- CEE Annual Report 2018Документ100 страницCEE Annual Report 2018BusinessTech100% (1)
- CX Programmer Operation ManualДокумент536 страницCX Programmer Operation ManualVefik KaraegeОценок пока нет
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Crown WF-3000 1.2Документ5 страницCrown WF-3000 1.2Qirat KhanОценок пока нет
- B.SC BOTANY Semester 5-6 Syllabus June 2013Документ33 страницыB.SC BOTANY Semester 5-6 Syllabus June 2013Barnali DuttaОценок пока нет
- Hima OPC Server ManualДокумент36 страницHima OPC Server ManualAshkan Khajouie100% (3)
- From Philo To Plotinus AftermanДокумент21 страницаFrom Philo To Plotinus AftermanRaphael888Оценок пока нет
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Technical Bulletin LXL: No. Subject Release DateДокумент8 страницTechnical Bulletin LXL: No. Subject Release DateTrunggana AbdulОценок пока нет
- Introduction-: Microprocessor 68000Документ13 страницIntroduction-: Microprocessor 68000margyaОценок пока нет