Академический Документы
Профессиональный Документы
Культура Документы
Answers Rationale 81-102
Загружено:
Marisol Jane Jomaya0 оценок0% нашли этот документ полезным (0 голосов)
25 просмотров5 страницquestions and answers on medical surgical nursing
Авторское право
© © All Rights Reserved
Доступные форматы
DOCX, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документquestions and answers on medical surgical nursing
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате DOCX, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
25 просмотров5 страницAnswers Rationale 81-102
Загружено:
Marisol Jane Jomayaquestions and answers on medical surgical nursing
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате DOCX, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 5
81.
2. Because hypotension is a complication
associated with peritoneal dialysis, the nurse
records intake and output, monitors vital signs,
and observes the clients behavior. The nurse also
encourages visiting and other diversional activities.
A client on peritoneal dialysis does not need to be
placed in a bed with padded side rails or kept on
NPO status.
CN: Reduction of risk potential;
CL: Synthesize
82.
1, 2, 4, 5. Broad-spectrum antibiotics may be
administered to prevent infection when a peritoneal
catheter is inserted for peritoneal dialysis. If peritonitis
is present, antibiotics may be added to the
dialysate. Aseptic technique is imperative. Peritonitis,
the most common and serious complication
of peritoneal dialysis, is characterized by cloudy
dialysate drainage, diffuse abdominal pain, and
rebound tenderness.
CN: Safety and infection control;
CL: Synthesize
83.
2. Weight loss is expected because of the
removal of fl uid. The clients weight before and
after dialysis is one measure of the effectiveness of
treatment. Blood pressure usually decreases because
of the removal of fl uid. Hematuria would not occur
after completion of peritoneal dialysis. Dialysis only
minimally affects the damaged kidneys ability to
manufacture urine.
CN: Reduction of risk potential;
CL: Evaluate
84.
3. A client in renal failure develops hyperphosphatemia
that causes a corresponding excretion
of the bodys calcium stores, leading to renal
osteodystrophy. To decrease this loss, aluminum
hydroxide gel is prescribed to bind phosphates in
the intestine and facilitate their excretion. Gastric
hyperacidity is not necessarily a problem associated
with chronic renal failure. Antacids will not prevent
Curlings stress ulcers and do not affect metabolic
acidosis.
CN: Pharmacological and parenteral
therapies; CL: Evaluate
85.
4. Aluminum hydroxide gel (Amphojel) is
administered to bind the phosphates in ingested
foods and must be given with or immediately after
meals and snacks. There is no need for the client
to take it on a 24-hour schedule. It is not administered
to treat hyperacidity in clients with chronic
renal failure and therefore is not prescribed between
meals.
CN: Pharmacological and parenteral
therapies; CL: Evaluate
86.
1. Magnesium is normally excreted by the
kidneys. When the kidneys fail, magnesium can
accumulate and cause severe neurologic problems.
Milk of magnesia is harsher than Metamucil, but
magnesium toxicity is a more serious problem. A
client may fi nd both milk of magnesia and Metamucil
unpalatable. Milk of magnesia is not high in
sodium.
CN: Pharmacological and parenteral
therapies; CL: Apply
87.
2. Uremia can cause decreased alertness, so
the nurse needs to validate the clients comprehension
frequently. Because the clients ability to concentrate
is limited, short lessons are most effective.
If family members are present at the sessions, they
can reinforce the material. Written materials that the
client can review are superior to videotapes because
clients may not be able to maintain alertness during
the viewing of the videotape.
CN: Physiological adaptation;
CL: Synthesize
88.
3. Dietary management for clients with
chronic renal failure is usually designed to restrict
protein, sodium, and potassium intake. Protein
intake is reduced because the kidney can no longer
excrete the byproducts of protein metabolism. The
degree of dietary restriction depends on the degree
of renal impairment. The client should also receive
a high-carbohydrate diet along with appropriate
vitamin and mineral supplements. Calcium requirements
remain 1,000 to 2,000 mg/day.
CN: Basic care and comfort;
CL: Synthesize
89.
2. Altered sexual functioning commonly
occurs in chronic renal failure and can stress marriages
and relationships. Altered sexual functioning
can be caused by decreased hormone levels,
anemia, peripheral neuropathy, or medication. The
client should not decrease or avoid sexual activity
but instead should modify it. The client should rest
before sexual activity.
CN: Psychosocial adaptation;
CL: Synthesize
90.
2. The major benefi t of CAPD is that it
frees the client from daily dependence on dialysis
centers, health care personnel, and machines for
life-sustaining treatment. This independence is a
valuable outcome for some people. CAPD is costly
and must be done daily. Adverse effects and complications
are similar to those of standard peritoneal
dialysis. Peritoneal dialysis usually takes less time
but cannot be done at home.
CN: Reduction of risk potential;
CL: Apply
91.
3. Dietary restrictions with CAPD are fewer
than those with standard peritoneal dialysis because
dialysis is constant, not intermittent. The constant
slow diffusion of CAPD helps prevent accumulation
of toxins and allows for a more liberal diet. CAPD
does not work more quickly, but more consistently.
Both types of peritoneal dialysis are effective.
CN: Basic care and comfort;
CL: Synthesize
92.
1. Cloudy drainage indicates bacterial activity
in the peritoneum. Other signs and symptoms of
infection are fever, hyperactive bowel sounds, and
abdominal pain. Swollen legs may indicate heart
failure. Poor drainage of dialysate fl uid is probably
the result of a kinked catheter. Redness at the insertion
site indicates local infection, not peritonitis.
However, a local infection that is left untreated can
progress to the peritoneum.
CN: Reduction of risk potential;
CL: Analyze
The Client with Urinary Incontinence
93.
1, 2. Laughing may be a part of ones socialization,
so it should not be discouraged. In non-restricted
clients, a fl uid intake of at least 2 to 3 L/day
is encouraged; clients with stress incontinence may
reduce their fl uid intake to avoid incontinence at
the risk of developing dehydration and urinary tract
infections. Establishing a voiding schedule would
be more effective in the prevention of stress incontinence
rather than carrying incontinence pads.
Dietary irritants and natural diuretics, such as caffeine
and alcoholic beverages, may increase stress
incontinence. Kegel exercises strengthen the sphincter
and structural supports of the bladder.
CN: Health promotion and maintenance;
CL: Synthesize
94.
2. The history of three pregnancies is most
likely the cause of the clients current episodes of
stress incontinence. The clients fl uid intake, age, or
history of swimming would not create an increase in
intra-abdominal pressure.
CN: Reduction of risk potential;
CL: Analyze
95.
4. The primary goal of nursing care is to
decrease the number of incontinence episodes
and the amount of urine expressed in an episode.
Behavioral interventions (e.g., diet and exercise)
and medications are the nonsurgical management
methods used to treat stress incontinence. Without
surgical intervention, it may not be possible to
eliminate all episodes of incontinence. Helping the
client adjust to the incontinence is not treating the
problem. Clients with stress incontinence are not
prone to the development of urinary tract infection.
CN: Physiological adaptation;
CL: Synthesize
96.
2. Clients with stress incontinence are
encouraged to avoid substances, such as caffeine
and alcohol, that are bladder irritants. Emotional
stressors do not cause stress incontinence. It is most
commonly caused by relaxed pelvic musculature.
Wearing girdles is not contraindicated. Although
clients may want to limit physical exertion to avoid
incontinence episodes, they should be encouraged
to seek treatment instead of limiting their activities.
CN: Reduction of risk potential;
CL: Create
97.
3. A characteristic of urge incontinence is
involuntary urination with little or no warning. The
inability to empty the bladder is urine retention.
Loss of urine when coughing occurs with stress
incontinence. Frequent dribbling of urine is common
in male clients after some types of prostate surgery
or may occur in women after the development
of a vesicovaginal or urethrovaginal fi stula.
CN: Physiological adaptation;
CL: Analyze
98.
1. Instructing the client to void at regularly
scheduled intervals can help decrease the frequency
of incontinence episodes. Providing a bedside commode
does not decrease the number of incontinence
episodes and does not help the client who leads an
active lifestyle. Infections are not a common cause
of urge incontinence, so antibiotics are not an appropriate
treatment. Intermittent self-catheterization is
appropriate for overfl ow or refl ux incontinence, but
not urge incontinence, because it does not treat the
underlying cause.
CN: Physiological adaptation;
CL: Synthesize
Managing Care Quality and Safety
99.
4. Sensitivity to shellfi sh or iodine may cause
an anaphylactic reaction to the contrast material,
which contains iodine. Administering a cathartic
or antifl atulent will not prevent an anaphylactic
reaction to the contrast material. Keeping a client on
NPO status for 8 hours before the procedure is part
of the usual preparation for such a procedure to prevent
aspiration of food or fl uids if the client vomits
when lying on the X-ray table.
100.
1. The appropriate action would be to discard
the specimen and obtain a new one. Urine that is
allowed to stand at room temperature will become
alkaline, with multiplying bacteria. The specimen
should be examined within 1 hour after urination.
CN: Reduction of risk potential;
CL: Synthesize
101.
1, 2, 3, 4, 6. Before ordering and administering
packed RBCs, the nurse should assess the I.V.
site to make sure it has an 18G to 20G Angiocath.
The nurse should also ensure that normal saline
solution is used to prime the tubing to prevent
RBCs from adhering to the tubing. The client must
indicate informed consent for the procedure by
signing the consent form. The clients blood must
be typed to determine ABO blood typing and Rh
factor and ensure that the client receives compatible
blood. Cross-matching is done to detect the presence
of recipient antibodies to the donors minor
antigens. Vital signs provide a baseline reference for
continuous monitoring throughout the transfusion.
An identifi cation bracelet and red blood band are
essential for client identifi cation per facility policy.
Two nurses must double check the clients identifi
cation with the client listed on the unit of RBCs.
The transfusion should be started within 30 minutes
of the time that the RBC unit is checked out of the
blood bank. Thus, no blood should be kept in the
medication room before transfusion.
CN: Safety and infection control;
CL: Synthesize
102.
3. The correct technique for a clean-catch
urine culture specimen is to have the female client
clean the labia from front to back, void into the toilet,
and then void into the cup. The client does not
need to fully empty her bladder into the cup. It is
not necessary to catheterize the client to obtain the
specimen. The fi rst voided specimen of the day has
the highest bacterial counts.
CN: Basic care and comfort;
CL: Evaluate
Вам также может понравиться
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Essentials of Physical Medicine and Rehabilitation 2nd Ed. - W. Frontera, Et. Al., (Saunders, 2008) WW PDFДокумент847 страницEssentials of Physical Medicine and Rehabilitation 2nd Ed. - W. Frontera, Et. Al., (Saunders, 2008) WW PDFRecuperare100% (9)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Basic Theories of Traditional Chinese Medicine PDFДокумент194 страницыBasic Theories of Traditional Chinese Medicine PDFElanghovan Arumugam100% (31)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Liver CirrhosisДокумент31 страницаLiver CirrhosisMarisol Jane Jomaya50% (2)
- Pharmacology EssayДокумент6 страницPharmacology EssayMarisol Jane JomayaОценок пока нет
- Ayurveda FitoterapiaДокумент112 страницAyurveda FitoterapiaKerol Bomfim100% (2)
- Report CapsicumДокумент105 страницReport CapsicumRina WijayantiОценок пока нет
- Cancer Facts - Philippine Cancer SocietyДокумент79 страницCancer Facts - Philippine Cancer SocietyMarisol Jane JomayaОценок пока нет
- Guidance To Understanding Implications of IRMERДокумент52 страницыGuidance To Understanding Implications of IRMERrochimОценок пока нет
- Nursing Leadership and Management ExamsДокумент4 страницыNursing Leadership and Management ExamsMarisol Jane Jomaya67% (9)
- Free Dive Training Schedules - Land and Pool Based Training SessionsДокумент10 страницFree Dive Training Schedules - Land and Pool Based Training Sessionssjf540100% (1)
- Typhoid FeverДокумент46 страницTyphoid Feverdeskichinta50% (2)
- The Client With Renal CalculiДокумент3 страницыThe Client With Renal CalculiMarisol Jane JomayaОценок пока нет
- Nutrition Lec Syllabus Obe FormatДокумент42 страницыNutrition Lec Syllabus Obe FormatMarisol Jane Jomaya100% (2)
- College of Nursing Carlatan, San Fernando City Nursing Informatics AssignmentДокумент1 страницаCollege of Nursing Carlatan, San Fernando City Nursing Informatics AssignmentMarisol Jane JomayaОценок пока нет
- The Client With Urinary Tract InfectionДокумент4 страницыThe Client With Urinary Tract InfectionMarisol Jane JomayaОценок пока нет
- The Client With Acute Renal FailureДокумент3 страницыThe Client With Acute Renal FailureMarisol Jane Jomaya100% (1)
- The Client With Chronic Renal FailureДокумент4 страницыThe Client With Chronic Renal FailureMarisol Jane JomayaОценок пока нет
- Carpe Diem Spearheads Buwan NG WikaДокумент1 страницаCarpe Diem Spearheads Buwan NG WikaMarisol Jane JomayaОценок пока нет
- The Client With PyelonephritisДокумент2 страницыThe Client With PyelonephritisMarisol Jane JomayaОценок пока нет
- Oman NurseДокумент9 страницOman NurseMarisol Jane JomayaОценок пока нет
- Continuing Improvement DepedДокумент2 страницыContinuing Improvement DepedMarisol Jane JomayaОценок пока нет
- Value of Practice: Conversation Starters 01Документ2 страницыValue of Practice: Conversation Starters 01Marisol Jane JomayaОценок пока нет
- Lipat Lapit at LapatДокумент42 страницыLipat Lapit at LapatMarisol Jane Jomaya100% (1)
- Bautista Tops The RT Licensure ExamДокумент2 страницыBautista Tops The RT Licensure ExamMarisol Jane JomayaОценок пока нет
- Eteeap - NCM 106 Page 1Документ5 страницEteeap - NCM 106 Page 1Marisol Jane JomayaОценок пока нет
- Gastroenterology MEDTRANS SAMPLEДокумент1 страницаGastroenterology MEDTRANS SAMPLEMarisol Jane JomayaОценок пока нет
- Cardio Medical Record Transcription Part 2Документ2 страницыCardio Medical Record Transcription Part 2Marisol Jane Jomaya0% (1)
- NCM 106 - Case Analysis - Nursing Care Plan of Heart FailureДокумент2 страницыNCM 106 - Case Analysis - Nursing Care Plan of Heart FailureMarisol Jane JomayaОценок пока нет
- Gastroenterology Medical Records SampleДокумент1 страницаGastroenterology Medical Records SampleMarisol Jane JomayaОценок пока нет
- Endocrine Medical Transcription SampleДокумент2 страницыEndocrine Medical Transcription SampleMarisol Jane JomayaОценок пока нет
- Dermatology Medical Transcription SampleДокумент1 страницаDermatology Medical Transcription SampleMarisol Jane JomayaОценок пока нет
- Mwalya Wambua Final ProjectДокумент49 страницMwalya Wambua Final ProjectWILSON MACHARIAОценок пока нет
- Cryotech IVF Media Products and Services For Reproductive, Infertility ProfessionalsДокумент9 страницCryotech IVF Media Products and Services For Reproductive, Infertility ProfessionalsCryoTech IndiaОценок пока нет
- Elias On 1983Документ3 страницыElias On 1983JesusCordoba100% (2)
- The Amsterdam Preoperative Anxiety and Information.2Документ7 страницThe Amsterdam Preoperative Anxiety and Information.2Jose Rafael Villafan BernalОценок пока нет
- Arixtra: (Fondaparinux Sodium) InjectionДокумент26 страницArixtra: (Fondaparinux Sodium) InjectionTri Purma SariОценок пока нет
- 766ue 2019-01Документ101 страница766ue 2019-01Angelita Kstro D SilvaОценок пока нет
- Changes in The Body: What Is Puberty?Документ4 страницыChanges in The Body: What Is Puberty?Mitch MarananОценок пока нет
- Twin Block Appliance ThesisДокумент6 страницTwin Block Appliance Thesisjessicahillnewyork100% (2)
- Hospital Network in IndiaДокумент200 страницHospital Network in IndiaAlex GiDeonОценок пока нет
- 080 - Hospital Information Document For New StaffДокумент2 страницы080 - Hospital Information Document For New StaffleicesterbugОценок пока нет
- Ethnobotany and EthnopharmacologyДокумент29 страницEthnobotany and EthnopharmacologyJohn CaretakerОценок пока нет
- OPD Schedule (November 2021)Документ32 страницыOPD Schedule (November 2021)Ajay DherwaniОценок пока нет
- Seizure Updated ILAE ClassificationДокумент12 страницSeizure Updated ILAE ClassificationNasheei RadjaОценок пока нет
- Surving Sepsis Campaign ResultДокумент8 страницSurving Sepsis Campaign Resultmaria arenas de itaОценок пока нет
- Auriculotherapy Manual: Chinese and Western Systems of Ear AcupunctureДокумент2 страницыAuriculotherapy Manual: Chinese and Western Systems of Ear AcupunctureYh KooОценок пока нет
- Blood Culture Recomendation in PicuДокумент11 страницBlood Culture Recomendation in PicuJack Eugene LiowОценок пока нет
- U.p.diary 2020 (English) PDFДокумент431 страницаU.p.diary 2020 (English) PDFAbhayОценок пока нет
- V.Bontilao Sr. Integrated School Summative Test in English 7Документ6 страницV.Bontilao Sr. Integrated School Summative Test in English 7Nevaeh CarinaОценок пока нет
- Vol 2, Issue 1Документ56 страницVol 2, Issue 1Asfandyar Sheikh100% (1)
- Anaesthetic Management of Obstetric: HaemorrhageДокумент52 страницыAnaesthetic Management of Obstetric: Haemorrhagerevathidadam55555Оценок пока нет
- Final Letter To NLM Re - IJOEH Nov 2017Документ35 страницFinal Letter To NLM Re - IJOEH Nov 2017Celeste MonfortonОценок пока нет
- Renal Cell Carcinoma - Nursing Considerations With The Use of Targeted TherapyДокумент50 страницRenal Cell Carcinoma - Nursing Considerations With The Use of Targeted TherapyMarivic DianoОценок пока нет
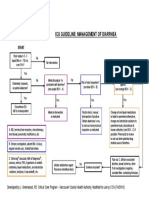
- Icu Guideline: Management of Diarrhea: StartДокумент1 страницаIcu Guideline: Management of Diarrhea: StartGracia VionaОценок пока нет