Академический Документы
Профессиональный Документы
Культура Документы
Desquamative Gingivitis Treated by An Antioxidant Therapy - A Case Report
Загружено:
inventionjournalsОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Desquamative Gingivitis Treated by An Antioxidant Therapy - A Case Report
Загружено:
inventionjournalsАвторское право:
Доступные форматы
International Journal of Pharmaceutical Science Invention
ISSN (Online): 2319 6718, ISSN (Print): 2319 670X
www.ijpsi.org Volume 5 Issue 4 July 2016 PP.18-22
Desquamative Gingivitis Treated By An Antioxidant Therapy- A
Case Report
Maya Mhaske1, Neha Thakur2, Supriya Bansode3, Poonam Kedar4
1, 2, 3, 4
(C.S.M.S.S. Dental College and Hospital, Aurangabad, Maharashtra, India)
Abstract: Desquamative gingivitis is described as an erythematous, desquamated or eroded gingival lesion.
Various etiologic factors are present for the appearance of such lesions. Despite of considering etiology,
treatment is oftenly provided by systemic or topical corticosteroids. Apart from steroid application, another
optionable treatment is antioxidant therapy which provides rapid healing of the tissue. As antioxidants posses
various advantageous properties, it can be considered as a first treatment option for desquamative gingivitis.
The presented case report of desquamative gingivitis is successfully treated using systemic antioxidants in the
form of commercially available oxitard capsule.
Keywords: Antioxidants, Corticosteroids, Desquamative gingivitis, Oxitard capsule, Systemic
I. Introduction
Desquamative gingivitis is a descriptive term, first introduced by Prinz in 1932 that is synonymous
with the presence of erythema, desquamation, erosion, and blistering of attached and marginal gingiva [1]. It is
seen mainly in adults, especially women, although rare cases have been observed in children [2]. Mucous
membrane pemphigoid, oral lichen planus and pemphigus vulgaris have emerged as the most common causes of
desquamative gingivitis. It may occur due to aging, abnormal response to bacterial plaque, allergy, idiopathic,
chronic infections, autoimmune diseases or idiopathic [1]. Definitive diagnosis of the specific disease or
disorder causing desquamative gingivitis is mainly depend on clinical manifestations, histopathological
examination and direct immunofluorescence testing [2].
There is no standard treatment protocol available for the management of patients with desquamative
gingivitis. The treatment strategies vary according to the preference of the physician, the age of the patient, the
severity of the disease and the site involved [1]. Treatment is most commonly provided in the form of plaque
control and steroid application. Among the various available treatment modalities, antioxidants are also useful to
treat dequamative gingivitis. Though it is more effective, it is less frequently used as a treatment option. Very
few case reports are available in literature which had been treated using antioxidants.
Here the presented case report of desuamative gingivitis was treated using antioxidant therapy.
II. Case Report
A 52-year-old female patient reported to the department of Periodontology, CSMSS dental college &
hospital, Aurangabad, with the chief complaint of burning sensation in upper & lower anterior gingiva since 9
months. Also gave history of aggravation of burning sensation on having spicy & hot beverages.
On examination, red, linear, diffused patches noticed on the buccal /labial marginal gingiva with slight
involvement of attached gingiva. Such reddish patches were present with respect to maxillary teeth
(11,21,22,24,25,26) & madibular teeth (31, 32, 35,41,42,43). Lesions also showed signs of desquamation. (Fig
1, 2)
No significant dental and medical history was given. Patient had habit of tobacco chewing, 3-4 times in
a day since last 10 years but she had quitted her habit, 3 yrs back. Patient also gave history of change of tooth
paste, 1 year back which was continued by her for 3 months and again she shifted to her regular tooth paste. But
the appeared desquamated lesion did not heal even after the discontinuation of changed tooth paste. Exact
etiology for the appearance of desquamated lesions in this patient was not known. But it could be due the
change of tooth paste, past tobacco chewing habit or nutritional deficiency.
After obtaining written consent, an incisional gingival biopsy was taken from maxillary anterior region
for the histopathological examination. The hematoxyline & eosin (H & E) stained tissue showed clefts at the
sub-epithelium. Underlying connective tissue showed bundles of collagen fibers arranged haphazardly along
with fibroblast & small foci of inflammatory cells. (Fig. 3). Clefts in the epithelium were suggestive of
desquamative lesions.
Thorough oral prophylaxis (scaling & polishing) was done. Patient was advised with 0.2%
chlorhexidine mouth rinse, modified bass technique of brushing & also asked to maintain good oral hygiene.
Topical application of steroid (Triamcinolone acetonide) twice in a day for three weeks was prescribed. Lesions
did not show any improvement clinically with topical steroids application in the follow up visits.
www.ijpsi.org
18 | P a g e
Desquamative Gingivitis Treated By An Antioxidant Therapy- A Case Report
Patient was asked to stop topical steroid & shifted to the systemic antioxidant therapy. Commertially
available capsule oxitard (Himalaya drug company), which is a herbal antioxidant was advised to take
systemically B.D. for two months along with reinforcement of oral hygiene maintenance. The patient was kept
under observation upto 6 months. Desquamated lesions started healing and disappeared within 2 months of
treatment. No recurrence was found. (Fig 4, 5)
(Fig 1): Desquamative gingivitis lesion with maxillary anterior teeth at baseline
(Fid 1.2): Desquamative gingivitis lesion with mandibular anterior teeth at baseline
(Fig 3): H & E stained tissue for histopathological examination
www.ijpsi.org
19 | P a g e
Desquamative Gingivitis Treated By An Antioxidant Therapy- A Case Report
(Fig. 4): Disappearance of desquamative gingival lesions in maxillary region after antioxidant therapy
(Fig. 5): Disappearance of desquamative gingival lesions in mandibular region after antioxidant
therapy
III. Discussion
Desquamative gingivitis is a fairly common disorder in which the gingiva is desquamated. Chronic
soreness is commonly seen and intake of spicy foods may further worsen the condition. Erythematous gingiva
with loss of stippling, extending apically from the gingival margins to the alveolar mucosa is a frequent
observation. Severity may range from mild, almost insignificant small patches to widespread erythema with
glazed appearance. Occassionally, such lesions may occur in the absence of bacterial plaque [1]. Differential
diagnosis of multiple oral ulcers may include aphthous ulcers major, erosive lichen planus, mucous membrane
pemphigoid, pemphigus vulgaris, acute necrotizing ulcerative gingivitis, allergies, acute herpetic
gingivostomatitis, and erythema multiforme [3]. Sometimes contact allergic reactions to various oral hygiene
products have also been reported to present as desquamative gingivitis [2]. But oral mucosa is less commonly
prone to contact allergic reactions, when compared to skin, though the latter is exposed to a wide variety of
antigenic stimuli [3].
The therapeutic approaches to desuamative gingivits are based on expert opinion rather than empirical
evidence. Several treatment methods have been reported (Carrozzo & Gandolfo, 1999; Chan et al., 2002; Endo
et al., 2008b; Fatahzadeh et al., 2006; Kirtschig et al., 2003; Lamey et al., 1992; Motta et al., 2009; Nisengard,
1996; Nisengard & Levine, 1995) [2]. Treatmemts are available in the form of systemic or topical steroids,
antimetabolites (cyclophosphamide, azathioprine, mycophenolate mofetil, methotrexate), antibiotics
(tetracyclines), and dapsone intravenous immunoglobulins, plasmapheresis, and Low level laser therapy which
causes pain relief and accelerates regeneration of damaged tissues [1].
Treatment of desquamative gingivitis requires elimination or control of local irritants. Rough
restorations, illfitting dentures, traumatic oral hygiene procedures, and dysfunctional oral habits should be
corrected [4]. In most of the cases, such lesions are successfully managed with topical corticosteroids combined
www.ijpsi.org
20 | P a g e
Desquamative Gingivitis Treated By An Antioxidant Therapy- A Case Report
with effective plaque control [5, 6]. Plaque accumulation acts as a stimulus factor for worsening of
desquamative gingivitis, but the plaque itself does not cause such lesions. It is difficult for patients with
desquamative gingivitis to brush their teeth due to pain and bleeding. Therefore, their oral hygiene is likely to be
ineffective, making it difficult to treat this condition [2]. Lack of correct oral hygiene and the accumulation of
plaque may increase the long-term risk for plaque-induced periodontal diseases along with desquamative
gingivitis [7].
Some of these desuamated lesions are a consequence of oxidative damage, therefore antioxidants can
delay or inhibit oxidation of oxidizable substrate in a chain reaction. Therefore the presented case of
desuamative gingivitis was successfully responded to the antioxidant therapy. The formulation of the oxitard
capsules (Himalaya drug company) contains the extracts of Mangifera indica, Withania somnifera, Daucus
carota, Glycyrrhiza glabra, Vitis vinifera, powders of Emblica officinalis and Yashada bhasma; and oils of
Triticum sativum. Mangifera indica is shown to have antibiotic, anti-asthamatic, antiseptic, antiviral,
hypotensive, anti-emetic properties. Withania somnifera provides overall health and wellness with its anti-stress,
anti-anxiety, anti-inflammatory, anti-convulsive and anti-arthritic properties. Daucus carota acts as a good
antiseptic as it is a rich source of vitamin A. Glycyrrhiza glabra normalizes the hoarseness in voice and has
immunomodulatory and anti-inflammatory properties. Vitis vinifera have anti-inflammatory, astringent and an
effect to curb the burning sensation. Emblica officinalis is a rich source of vitamin C and is a potent antibiotic.
Yashada bhasma contains zinc which plays a significant role in protein synthesis, cell division and wound
healing. Triticum sativum is a rich source of minerals and has an antioxidant property Various ingredients of it
acts as an immunomodulator, stimulator of antioxidant enzymes, free redical scavenger, astringent, source of
vitamin A & C, potent antibiotic, also helps in protein synthesis, cell division, wound healing. Same drug
formulation was successfully used in the treatment of Oral submucous fibrosis because of its antioxidant & antiinflammatory properties [8].
Similarly, antioxidant properties of honey was used in the treatment of various vescicullobullous &
desquamative gingivitis lesions. Pure, unboiled, commertially available honey was topically applied. Excllent
healing noticed in such desquamative gingivitis lesions with no recurrence.8 The mechanism of therapeutic
effects of honey as anti-inflammatory effect might be attributed to reduction in prostaglandin synthesis at the
site of application, elevation of nitric oxide in the lesions, inhibition of leukotriene B4, & to its antioxidant &
anti inflammatory activities [9]. Other antioxidant agents have also been successfully tried for desquamative
gingivitis. Lower concentrations of retinoids combined with other antioxidant agents like lycopene and tocoferol (vitamin E) are known to have synergistic effect in the remission of the lichen planus lesions.
Lycopene, a carotenoid, is a most efficient antioxidizing and immunomodulating agent, and is known to modify
intercellular exchange junctions. It is the most promising candidate in reducing hyperkeratosis of oral mucosa
and can be used effectively in management of oral lichen planus lesions. Alpha-tocoferol (vitamin E) is also an
effective antioxidant at high levels of oxygen, protecting cellular membranes from lipidic peroxidation. It can be
used to reduce the size of lichen planus lesions. Combination of lycopene, vitamin E, and retinoids, was found
to be very effective in the reduction of gingival lesions of lichen planus, along with topical corticosteroids [10].
Various desquamated lesions are usually treated with steroids either topically or systemically. Steroids
have many drawbacks, besides the side effects of long term use, they are not uniformly effective, can damage
collagen, the candidiasis occasionally is a complication of their use. Antioxidants do not produce such effects
even after long term use. So, antioxidants can be added to the traditional treatment modalities of desquamative
gingivitis because it significantly speeds up resolution of inflammation, ulcerative oral lesions, pain sensation &
helps to achieve healthy healing [9].
Further studies using long term follow up and histological examination for tissue changes after using
antioxidants in desquamative gingivitis are required.
IV. Conclusion
The management of desquamative gingivitis is challenging because lesions reoccur after it goes into
remission. The present case was successfully treated using systemic antioxidant therapy along with oral hygiene
maintenance.
Clinical anecdotal evidence supporting the beneficial use of antioxidants for desquamative gingivitis
lesion was found. Therefore antioxidants can be added to the traditional treatment modalities of such lesions &
can be use as a first treatment option as a substitute to the corticosteroids.
References
[1].
[2].
Shamimul Hasan, Desquamative gingivitis - A clinical sign in mucous membrane pemphigoid: Report of a case and review of
literature, Jornal of Pharmacy & Bioallied Sciences, 6(2), 2014, 122126.
Hiroyasu Endo and Terry D. Rees, Diagnosis and Management of Desquamative Gingivitis, Gingival Diseases Their Aetiology,
Prevention and Treatment, www.intecopen.com, 171-188.
www.ijpsi.org
21 | P a g e
Desquamative Gingivitis Treated By An Antioxidant Therapy- A Case Report
[3].
[4].
[5].
[6].
[7].
[8].
[9].
[10].
Baljeet Singh, Alka Sharma, and Avnika Garg, Herbal oral gel induced contact stomatitis along with desquamative gingivitis due to
a coloring agent, Journal of Indian Society of Periodontology, 19(5), 2015, 569572.
Fatahzadeh, M., Radfar L., and Sirois, D.A., Dental care of patients with autoimmune vesiculobullous diseases: case reports and
literature review, Quintessence International, 37(10), 2006 Nov-Dec, 77-87.
Endo H., Rees T D, Kuyama K, Matsue M, and Yamamoto H, Successful treatment using occlusive steroid therapy in patients with
erosive lichen planus: a report on 2 cases, Quintessence International, 39(4), 20008 April, 162-172.
Guiglia R, Di Liberto C, Pizzo G, Picone L, Lo Muzio L and Gallo P D, A combined treatment regimen for et al. gingivitis in
patients with oral lichen planus, Journal of Oral Pathology & Medicine, 36(2), 2007 February, 110-116.
Pradeep A.R , Manojkumar S.T, and Arjun R, Pemphigus vulgaris with significant periodontal findings: a case report, Jornal of the
California Dental Association, 38(5), 2010 May, 343-346.
Santosh Patil, Vishal Halgatti, Sneha Maheshwari, and B S. Santosh, Comparative study of the efficacy of herbal antioxdants
oxitard and aloe vera in the treatment of oral submucous fibrosis, Journal of Clinical & Experimental Dentistry, 6(3), 2014 Jul,
e265e270.
Salley A EI-Haddad, Maysara D AI-Shawaf, Effect of honey for treatment of some common oral lesions: Follow up of 50 cases,
Journal of dentistry & oral hygiene, 5(6), June 2013, 55-61.
Ribeiro AS, Salles PR, da Silva TA, Mesquita RA, A review of the nonsurgical treatment of oral leukoplakia, International Journal
of Dentistry, 2010,18601.
www.ijpsi.org
22 | P a g e
Вам также может понравиться
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (894)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (119)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2219)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Dentistry MCQ With AnswersДокумент34 страницыDentistry MCQ With AnswersAyesha Awan57% (7)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Effects of Online Marketing On The Behaviour of Consumers in Selected Online Companies in Owerri, Imo State - Nigeria.Документ12 страницEffects of Online Marketing On The Behaviour of Consumers in Selected Online Companies in Owerri, Imo State - Nigeria.inventionjournalsОценок пока нет
- Literary Conviviality and Aesthetic Appreciation of Qasa'id Ashriyyah (Decaodes)Документ5 страницLiterary Conviviality and Aesthetic Appreciation of Qasa'id Ashriyyah (Decaodes)inventionjournalsОценок пока нет
- The Effect of Transformational Leadership, Organizational Commitment and Empowerment On Managerial Performance Through Organizational Citizenship Behavior at PT. Cobra Direct Sale IndonesiaДокумент9 страницThe Effect of Transformational Leadership, Organizational Commitment and Empowerment On Managerial Performance Through Organizational Citizenship Behavior at PT. Cobra Direct Sale Indonesiainventionjournals100% (1)
- Effects of Online Marketing On The Behaviour of Consumers in Selected Online Companies in Owerri, Imo State - NigeriaДокумент12 страницEffects of Online Marketing On The Behaviour of Consumers in Selected Online Companies in Owerri, Imo State - Nigeriainventionjournals100% (1)
- A Critical Survey of The MahabhartaДокумент2 страницыA Critical Survey of The MahabhartainventionjournalsОценок пока нет
- The Impact of Leadership On Creativity and InnovationДокумент8 страницThe Impact of Leadership On Creativity and InnovationinventionjournalsОценок пока нет
- A Discourse On Modern Civilization: The Cinema of Hayao Miyazaki and GandhiДокумент6 страницA Discourse On Modern Civilization: The Cinema of Hayao Miyazaki and GandhiinventionjournalsОценок пока нет
- Islamic Insurance in The Global EconomyДокумент3 страницыIslamic Insurance in The Global EconomyinventionjournalsОценок пока нет
- The Network Governance in Kasongan Industrial ClusterДокумент7 страницThe Network Governance in Kasongan Industrial ClusterinventionjournalsОценок пока нет
- The Social Composition of Megaliths in Telangana and Andhra: An Artefactual AnalysisДокумент7 страницThe Social Composition of Megaliths in Telangana and Andhra: An Artefactual AnalysisinventionjournalsОценок пока нет
- Inter-Caste or Inter-Religious Marriages and Honour Related Violence in IndiaДокумент5 страницInter-Caste or Inter-Religious Marriages and Honour Related Violence in IndiainventionjournalsОценок пока нет
- E0606012850 PDFДокумент23 страницыE0606012850 PDFinventionjournalsОценок пока нет
- Negotiated Masculinities in Contemporary American FictionДокумент5 страницNegotiated Masculinities in Contemporary American FictioninventionjournalsОценок пока нет
- An Appraisal of The Current State of Affairs in Nigerian Party PoliticsДокумент7 страницAn Appraisal of The Current State of Affairs in Nigerian Party PoliticsinventionjournalsОценок пока нет
- Student Engagement: A Comparative Analysis of Traditional and Nontradional Students Attending Historically Black Colleges and UniversitiesДокумент12 страницStudent Engagement: A Comparative Analysis of Traditional and Nontradional Students Attending Historically Black Colleges and Universitiesinventionjournals100% (1)
- The Usage and Understanding of Information and Communication Technology On Housewife in Family Welfare Empowerment Organization in Manado CityДокумент10 страницThe Usage and Understanding of Information and Communication Technology On Housewife in Family Welfare Empowerment Organization in Manado CityinventionjournalsОценок пока нет
- H0606016570 PDFДокумент6 страницH0606016570 PDFinventionjournalsОценок пока нет
- Muslims On The Margin: A Study of Muslims OBCs in West BengalДокумент6 страницMuslims On The Margin: A Study of Muslims OBCs in West BengalinventionjournalsОценок пока нет
- D0606012027 PDFДокумент8 страницD0606012027 PDFinventionjournalsОценок пока нет
- C0606011419 PDFДокумент6 страницC0606011419 PDFinventionjournalsОценок пока нет
- Effect of P-Delta Due To Different Eccentricities in Tall StructuresДокумент8 страницEffect of P-Delta Due To Different Eccentricities in Tall StructuresinventionjournalsОценок пока нет
- Non-Linear Analysis of Steel Frames Subjected To Seismic ForceДокумент12 страницNon-Linear Analysis of Steel Frames Subjected To Seismic ForceinventionjournalsОценок пока нет
- F0606015153 PDFДокумент3 страницыF0606015153 PDFinventionjournalsОценок пока нет
- E0606012850 PDFДокумент23 страницыE0606012850 PDFinventionjournalsОценок пока нет
- H0606016570 PDFДокумент6 страницH0606016570 PDFinventionjournalsОценок пока нет
- Non-Linear Analysis of Steel Frames Subjected To Seismic ForceДокумент12 страницNon-Linear Analysis of Steel Frames Subjected To Seismic ForceinventionjournalsОценок пока нет
- F0606015153 PDFДокумент3 страницыF0606015153 PDFinventionjournalsОценок пока нет
- D0606012027 PDFДокумент8 страницD0606012027 PDFinventionjournalsОценок пока нет
- C0606011419 PDFДокумент6 страницC0606011419 PDFinventionjournalsОценок пока нет
- Development of Nighttime Visibility Assessment System For Road Using A Low Light CameraДокумент5 страницDevelopment of Nighttime Visibility Assessment System For Road Using A Low Light CamerainventionjournalsОценок пока нет
- Desquamative GingivitisДокумент6 страницDesquamative Gingivitissidra malikОценок пока нет
- PIIS1875957222000493Документ2 страницыPIIS1875957222000493Ana Clara Maia PalhanoОценок пока нет
- Case Study For Oral Pathology - FinalДокумент4 страницыCase Study For Oral Pathology - Finalapi-330041747Оценок пока нет
- White Sponge NevusДокумент4 страницыWhite Sponge NevusFRANCHEZKA ANGELICA TANIEGRAОценок пока нет
- Lichen Planus: Images in Clinical MedicineДокумент1 страницаLichen Planus: Images in Clinical MedicineMr. LОценок пока нет
- NBDHE Board Review 2013 Oral Pathology TermsДокумент15 страницNBDHE Board Review 2013 Oral Pathology TermsDENTAL REVIEWER ONLY100% (1)
- CME Part IIДокумент14 страницCME Part IIEkkapap UnityОценок пока нет
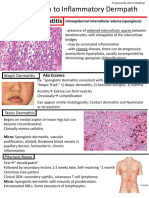
- Spongiotic Dermatitis: Aka EczemaДокумент8 страницSpongiotic Dermatitis: Aka EczemafadoОценок пока нет
- Chapter 15. Nummular Eczema, Lichen Simplex Chronicus, and Prurigo NodularisДокумент11 страницChapter 15. Nummular Eczema, Lichen Simplex Chronicus, and Prurigo NodularisandiОценок пока нет
- Pharmacological Management of Common Soft Tissue Lesions of The Oral CavityДокумент16 страницPharmacological Management of Common Soft Tissue Lesions of The Oral CavityAcisum2Оценок пока нет
- Eritroderma - Bolognia 4th EditionДокумент15 страницEritroderma - Bolognia 4th EditionAisyahОценок пока нет
- Oral Lichen PlanusДокумент7 страницOral Lichen Planusdrgurpal74100% (1)
- 5 - Differential Diagnosis of DermatologyДокумент6 страниц5 - Differential Diagnosis of DermatologyAyaa YousefОценок пока нет
- Levamisole in L.PДокумент5 страницLevamisole in L.PjalalfaizОценок пока нет
- Current Perspectives On Use of Aloe Vera in DentistryДокумент12 страницCurrent Perspectives On Use of Aloe Vera in DentistrysevattapillaiОценок пока нет
- What Is Lichen Planus?Документ8 страницWhat Is Lichen Planus?Asharib AfsarОценок пока нет
- Case Report: Journal of Chitwan Medical College 2020 10 (31) :91-93Документ3 страницыCase Report: Journal of Chitwan Medical College 2020 10 (31) :91-93Yeni PuspitasariОценок пока нет
- Oral Medicine Mcqs - ٠٧٠٠١٨Документ5 страницOral Medicine Mcqs - ٠٧٠٠١٨alshybanyalmz30Оценок пока нет
- Oral Lichenoid Lesions: Clinico-Pathological Mimicry and Its Diagnostic ImplicationsДокумент8 страницOral Lichenoid Lesions: Clinico-Pathological Mimicry and Its Diagnostic Implicationsshehla khanОценок пока нет
- Ashy Dermatosis and Lichen PlanusДокумент27 страницAshy Dermatosis and Lichen PlanusAthenaeum Scientific PublishersОценок пока нет
- KERATOSIS AND RELATED DISORDERS OF ORAL MUCOSA (2) Edited JsmuДокумент126 страницKERATOSIS AND RELATED DISORDERS OF ORAL MUCOSA (2) Edited JsmuMINI DHABAОценок пока нет
- An Overview On Melasma 2376 0427 1000216Документ18 страницAn Overview On Melasma 2376 0427 1000216dhilaidrisОценок пока нет
- Eczema, Psoriasis, Cutaneous Infections, Acne, and Other Common Skin DisordersДокумент6 страницEczema, Psoriasis, Cutaneous Infections, Acne, and Other Common Skin DisordersElrey InocianОценок пока нет
- Dermatology Images (All in One Merged)Документ692 страницыDermatology Images (All in One Merged)Woo Rin Park100% (2)
- Vulvar Ulcer CausesДокумент4 страницыVulvar Ulcer CausesChibiОценок пока нет
- 17 Oral Mucosal LesionsДокумент6 страниц17 Oral Mucosal LesionsninisskyОценок пока нет
- Phototherapy For Dermatologic ConditionsДокумент18 страницPhototherapy For Dermatologic ConditionsSeth MosebyОценок пока нет
- 43. 구진인설질환 - 강의교안Документ72 страницы43. 구진인설질환 - 강의교안John DoeОценок пока нет
- New Thesis Topics in Oral Medicine and RadiologyДокумент6 страницNew Thesis Topics in Oral Medicine and Radiologyoabfziiig100% (2)