Академический Документы
Профессиональный Документы
Культура Документы
Lepto and Typhoid
Загружено:
Sigfred Tarnate AoasИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Lepto and Typhoid
Загружено:
Sigfred Tarnate AoasАвторское право:
Доступные форматы
INFECTIONS DUE TO ANAEROBIC ORGANISM
DR. FAJARDO
INFECTIONS DUE TO ANAEROBIC ORGANISM
Definitions
Anaerobic bacteria
o Organisms that require reduced oxygen
tension for growth
o Fail to grow on solid media in 10% CO2 in
air
o Bacteroides fragilis, Prevotella sp.,
Fusobacterium sp.
o Major reservoirs: mouth, colon, skin, female
genital tract
o Commensal anaerobes
Mediators of physiologic,
metabolic, immunologic functions
of the human body host
Interferes colonization of potential
pathogenic bacteria by:
Depletion of oxygen and
nutrients
Production of enzymes
and toxic end products
Modulation of host's
intestinal innate immune
system response
Anaerobic infections
Mucosal barrier/skin - compromised by surgery,
trauma, tumors, ischemia, necrosis
Disruption of anatomic barriers allows penetration
of many organisms leading to mixed infections of
anaerobes + facultative bacteria
*mostly anaerobic + aerobic infection, rarely pure
*Polymicrobial
Anatomic sites and potential pathogens
Anatomic Site
Potential Pathogens
Oral Cavity
Fusobacterium nucleatum
Saliva
Prevotella malanogenica
Tooth surface
Prevotalla oralis group
Gingival crevices
Bacteroides ureolyticus
group
Peptostreptococcus spp.
GIT
Bacteroides spp.
Stomach
Prevotella spp.
Jejunum
Clostridium spp.
Ileum
Peptostreptococcus spp.
Colon
Female Genital Tract
Peptostreptococcus spp.
Bacteroides spp.
Prevotella bivia
Etiology
Infections caused by anaerobes mostly
polymicrobial
Major anaerobic gram positive cocci that produce
disease is Peptostreptococcus sp.
Clostridia spore-forming gram-positive rods most
common isolated organism found in wounds,
abscesses, abdominal infections, blood
Propionibacterium acnes gram positive rod, non
spore forming; involve in formation of acne
Principal anaerobic gram negative bacilli found in
human infections
o B. fragilis group - MC
o Fusobacterium
o Prevotella
o Porphyromonas sp.
Pathogenesis
Disrupted anatomic barrier leads to entry of local
flora in a previously sterile site
Factors that allow organism to penetrate mucosal
barrier are:
o Tissue ischemia
o Trauma
o Surgery
o Perforated viscus (ie. Rupture appendixcolonic contents which is unsterile goes into
peritoneum that is sterile ->peritonitis)
o Shock
o Aspiration oral flora will go to the lungs
creating anaerobic infection
o *all of which provide an environment
conducive for proliferation of anaerobes
Three major factors are involved in the pathogenesis
of anaerobic infections
1. Bacterial synergy
Facultative organisms will create
environment for the anaerobic
organisms to proliferate >
anaerobic organism will produce
enzymes that will help these
facultative organisms thrive to
areas they are not usually seen
Aerobes + anaerobes work hand in
hand to provide a good
environment
Facultative organisms lower the
oxidation-reduction potential
Anaerobic organisms produce
succinic acids and fatty acids
2. Bacterial virulence factors
Confer the ability to evade host
defenses, adhere to cell surfaces,
produce toxins and enzymes/
INFECTIONS DUE TO ANAEROBIC ORGANISM
DR. FAJARDO
display surfaces structures
(capsular polysaccharides, lps)
3. Mechanism of abscess formation
Form a thick wall or cyst
impenetrable to antibiotics
Bacteroides fragilis - most common
in intraabdominlal infections and
bacteremia
Polysaccharide A has the
ability to promote abscess
formation
Approach to the patient: Infections due to mixed anaerobic
organisms
Most of the organism colonizing mucosal sites are
harmless commensals; very few cause disease
For anaerobes to cause tissue infection, they must
spread beyond the normal mucosal barriers
Conditions favoring the propagation of these
bacteria, particularly a lowered oxidation-reduction
potential (esp. areas with necrosis and ischemia)
o Sites of trauma, tissue destruction,
compromised vascular supply, and
complications of pre-existing infection,
which produce necrosis
Anaerobic organism tend to be found in abscess
cavities or in necrotic tissue
Gas is found in many anaerobic infections of deep
tissues (deep tissues or muscles)
Although a putrid-smelling infection site or discharge
develops late in the course and present in 30-50% of
cases
o But even if without putrid smell, anaerobic
infection is still a consideration
Antibiotic therapy combined with debridement and
drainage
o Antibiotics does not work alone, you need
surgical intervention
Severe sepsis and DIC UNUSUAL in patients with
purely anaerobic infection
o Anaerobic infections are only mild to
moderate infections
o ANAEROBE + GRAM NEG OR POS
INFECTION
ANAEROBIC INFECTIONS OF THE MOUTH, HEAD AND NECK
Normal flora of the upper airways - mainly the
Bacteroides oralis group, Prevotella sp, Prevotella
asaccharolytica, Fusobacterium species,
Peptosteptococci and microaerophilic streptococci
Peptostreptoccci and microaerophilic
streptococci: facultative anaerobes
Odontogenic infections - primarily dental caries and
periodontal disease (gingivitis and periodontitis)
Necrotizing Ulcerative Gingivitis
Gingivitis become a necrotizing infection (trench
mouth, Vincent's stomatitis)
o Tender bleeding gums, foul breath and bad
taste
o Gingival mucosa becomes ulcerated and
may be covered by a gray exudate, which is
removable with gentle pressure
o Fever, cervical LAD, and leukocytosis
Acute necrotizing ulcerative mucositis (Cancrum oris, noma)
Ulcerative gingivitis can spread to the buccal
mucosa, teeth and mandible or maxilla leading to a
widespread destruction of bone and soft tissue
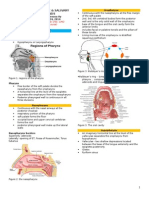
Acute necrotizing infections of the Pharynx
Occur in association with ulcerative gingivitis
Symptoms
o Sore throat, foul breath and a bad taste
o Accompanied by fever and a sensation of
choking due to the swelling of the tonsillar
pillars
o DDx: diphtheria
Tonsillar pillars are swollen, red, ulcerated, and
covered with a grayish membrane that peels easily
LAD and leukocytosis are common in infections of
the oral cavity.
Disease may last for only a few days or, if not
treated, may persist for weeks
Lesions begin unilaterally but may spread to the
other side of the pharynx or the larynx
Aspiration of the infected material by the patient can
result in lung abscesses
Peripharyngeal Space infection (NECK AREA)
Spread of organisms from the upper airways to
potential spaces formed by the fascial planes of the
head and neck
Peritonsillar abscess (quinsy)
o Complication of acute tonsillitis - mixed
flora containing anaerobes and Group A
Streptococcus
Ludwig's angina - submandibular space infection
o 80% caused by infection of the tissues
surrounding the second and third molar
teeth
INFECTIONS DUE TO ANAEROBIC ORGANISM
DR. FAJARDO
Marked local swelling of tissues, with pain,
trismus (locked jaw), and superior and
posterior displacement of the tongue (due
to severe swelling)
Submandibular swelling of the neck can
impair swallowing and cause respiratory
obstruction or aspiration
Tracheotomy may be life-saving
Cervicofacial actinomycosis
o Caused by a branching, gram positive, nonspore-forming, strict/facultative anaerobe
that is a part of the normal oral flora
o Chronic disease - characterized by
abscesses, draining sinus tracts, fistula,
bone destruction, and fibrosis
o It can easily be mistaken for malignancy or
granulomatous disease
o *DDx: TB adenitis or lymphoma d/t the
draining sinus (bone involvement =
Actinomycosis)
Sinusitis and Otitis
Anaerobic bacteria have been implicated in chronic
sinusitis but play little role in acute sinusitis
o Prevotella, Fusobacterium, and
Peptostreptocossus species
Anaerobic bacteria are much more easily implicated
in chronic suppurative otitis media than in acute
otitis media
o Purulent exudate from chronically draining
ears has been found to contain anaerobes
o Bacteroides species, in up to 50% of cases
1. Pharyngitis
2. A tender/swollen neck (d/t
involvement of internal jugular
vein)
3. Noncavitating pulmonary
infiltrates (in Chest X-ray)
CNS INFECTIONS
Complications of Anaerobic Head and Neck Infections
Contiguous cranial spread of these infections
o Osteomyelitis of the skull and mandible
o Intracranial infections such as brain abscess
and subdural empyema
Caudal spread can produce mediastinitis or
pleuropulmonary infection
Hematogenous complications/bacteremia
o Occasionally polymicrobial
o Endocarditis (secondary to anaerobic
infection) or other distant infections
Lemierre's syndrome (which has been uncommon in
the antimicrobial era)
o Acute oropharyngeal infection with
secondary septic thrombophlebitis of the
internal jugular vein (MC structure) and
frequent metastasis, most commonly to the
lung
o Fusobacterium necrophorum is the usual
cause
o Typical clinical triad*
Brain abscess, epidural abscess and subdural
empyema
Anaerobic meningitis is rare, related to
parameningeal collection or shunt infection
As many as 85% of brain abscesses yield anaerobic
bacteria (the rest aerobic)
o Optimal bacteriologic techniques to grow
these organisms
o Usually originate from otorhinolaryngeal
infection
MC chronic suppurative OM
Give empiric treatment because of
the 85% caused by anaerobic
organisms
PLEUROPULMONARY INFECTION
Result from the aspiration of the oropharyngeal
contents
o Altered state of consciousness or
o Absent gag reflex
Four clinical syndromes are associated with
anaerobic pleuropulmonary infection produced by
aspiration:
1. Simple aspiration pneumonia -- simple infiltrate
by CXR
2. Necrotizing pneumonia - cavity formation in
CXR
3. *Lung abscess - accumulation of pus within the
lung parenchyma
4. *Empyema - accumulation of pus within the
pleural cavity, outside the lungs
*different treatment
o Lung abscess does not require surgery
(may cause Atelectasis, instead give
antibiotics for 4-6 weeks)
o Empyema requires surgical drainage
INTRAABDOMINAL INFECTIONS
Mainly peritonitis and abscesses - polymicrobial and
represent the normal intestinal (esp colonic) flora
Breach in the mucosal barrier resulting from
appendicitis, diverticulitis, neoplasm, inflammatory
bowel disease, surgery, or trauma
Predominance of enteric aerobic/facultative gramnegative bacilli, anaerobes and
streptococci/enterococci
INFECTIONS DUE TO ANAEROBIC ORGANISM
DR. FAJARDO
The MC isolates are E. coli (>/=50%) and B. fragilis
(30-50%)
Enterotoxigenic B. fragilis has been associated with
watery diarrhea in a few young children and adults
Neutropenic enterocolitis (Typhlitis) has been
associated with anaerobic infection of the cecum or
the entire bowel
o Patient should be neutropenic
o Usually present with fever, abdominal pain,
tenderness, and distention, and diarrhea
o *Commonly seen in patients undergoing
chemotherapy, leukemia or any
hematologic abnormality
o Bowel wall is edematous with hemorrhage
and necrosis
PELVIC INFECTIONS
The vagina of a healthy woman is major reservoir of
anaerobic and aerobic bacteria
o Anaerobes outnumber aerobes by a ratio
of 10:1
o Anaerobic gram-positive cocci and
Bacteroides species
o Anaerobes are isolated from most women
with genital tract infections that are not
caused by a sexually transmitted pathogen
o
o
Anaerobic bacterial synergistic gangrene
(Meleney's gangrene)*
o Pain, redness and swelling followed by
induration
o Erythema surrounds a central zone of
necrosis, granulating ulcer forms at the
original center as necrosis and erythema
extend outward
o Peptostreptococcus sp and S aureus
o Usual site (POST SURGICAL SITES)
abdominal surgical wound or the area
surrounding an ulcer on an extremity
(superficial fascia)
o Surgical removal of necrotic tissue
(debridement) and antimicrobial
administration
Necrotizing fasciitis
o Rapidly spreading destructive disease of the
fascia usually attributed to a group A
streptococci
o Mixed infection involving anaerobes and
aerobes, usually after surgeries and in
patients with diabetes or peripheral
vascular disease
o Most frequently isolated anaerobes in these
infections are Peptostreptococcus and
Bacteroides species
o Gas may be found in the tissues
o Deeper into the fascia
o Do fasciotomy to release pressure
o Compartment syndrome may be a
complication
Myonecrosis can be associated with mixed
anaerobic infection
Fournier's gangrene
o Cellulitis involving the scrotum, perineum
and anterior abdominal wall
o Mixed anaerobic organism spreading along
deep external fascial planes and causing
extensive loss of skin
B. fragilis, P. bovia, P. disiens, P. melaninogenica,
anaerobic cocci, and Clostridium sp
Bartholin gland abscess, salpingitis, tuboovarian
abscess, septic abortion, pyometra (pus in the
muscles of uterus), endometritis, and postoperative
wound infection (hysterectomy)
Bacterial vaginosis
o MC caused by Gardneralla vaginalis
SKIN AND SOFT TISSUE INFECTIONS
Injury to skin, bone or soft tissue by trauma,
ischemia, or surgery creates a suitable environment
for anaerobic infections
Found in sites prone to contaminated with feces or
with upper airway secretions - eg, wounds
associated with intestinal surgery (contamination
with colonic flora), decubitus ulcers (contamination
with feces is common) or human bites
o Cutaneous abscesses (carbuncle), rectal
abscesses and axillary sweat gland
infections (hidradenitis suppurativa)
Foot ulcers of diabetic patients
o Foul smelling discharge from the foot
(Diabetic foot ulcer)
Bacteroides, peptostreptococcus,
clostridium enterococcus and proteus sp
Associated with a higher frequency of
fever, foul-smelling lesions, gas in the
tissues and visible foot ulcer, necrotizing
fasciitis
DIAGNOSIS
There are three critical steps in the diagnosis of
anaerobic infection:
1. Proper specimen collection
INFECTIONS DUE TO ANAEROBIC ORGANISM
DR. FAJARDO
2. Rapid transport of the specimen to the
microbiology laboratory, preferable in
anaerobic transport media
3. Proper handling of the specifies by the
laboratory
Specimens must be collected by meticulous sampling
of infected sites with avoidance of contamination by
the normal flora
*Aspirate abscess, collect discharge, swabbing is not
recommended
Specimens appropriate for anaerobic culture
o *Sterile body fluids such as
Blood
Pleural fluid
Peritoneal fluid
CSF
Aspirates or biopsies from
normally sterile sites
As a general rule, liquid or tissue specimens are
preferred; swab specimens should be avoided
TREATMENT
Combination of:
o Appropriate antibiotics
o Surgical resection
o Debridement of devitalized tissues
o Drainage of abscesses
Any anatomic breach must be closed promptly,
closed spaces drained, tissue compartments
decompressed, and an adequate blood supply
established
Abscess cavities should be drained as soon as
fluctuation or localization occurs
o Brain abscesses if surgery is dangerous,
prolong antibiotic treatment
ANTIBIOTIC THERAPY:
In many infections, anaerobes are mixed with
coliforms and other facultative organism
The best therapeutic regimens - active against both
aerobic and anaerobic bacteria
1. Metronidazole
o Needs to be given in combination with
aerobic bacterial coverage because it does
not have coverage for gram (+) aerobes
o Below the diaphragm, aerobic gram
negative coverage is needed; add
cephalosporin 3rd or 4th gen
o For infections from an oral source, aerobic
gram positive coverage; add first or second
gen cephalosporins or amoxicillin
2. Carbapenems (imipenem, meropenem,
doripenem)
o Good coverage for aerobic gram (+) and ()
organism and anaerobes
If given initially, esp for GI give as
monotherapy
3. Beta lactam/ -lactamase inhibitor combination
(ampicillin/sulbactam, ticarcillin/clavulanic acid,
piperacillin/tazobactam)
o Coverage: anaerobe, gram + and aerobes
o Some anaerobic coverage
o Ampicillin-Sulbactam for oral infections;
targets anaerobes; may be used as
monotherapy
4. Cephamycins
o Good gram + coverage
o Cefoxitine for anaerobic infections
5. Clindamycin
o Coverage: aerobic gram +
o Can cover for anaerobic organisms
especially for mouth, neck and lung
infections
o Below the diaphragm infections:
DOC: metronidazole
o Above the diaphragm infections:
DOC: clindamycin (anaerobes and
Gram (+) organisms
o
6. Penicillin
o At high doses= gram + anaerobe (e.g.
Peptostreptococcus)
o For streptococcus species
o Given for oropharyngeal infections
o If at very high doses, may have anaerobic
activity
7. Cephalosporins
o 1st and 2nd gen - good coverage for gram +
o 3rd and 4th - gram negative aerobic
o needs to be combined with metro or clinda
8. Vancomycin
o MRSA organisms
o Gram + aerobic
o Has some anaerobic coverage
o If very sever anaerobic, vanco + metro
9. Tigecycline
o New drug
o Has good coverage for MRSA, for gram ()
intraabdominal infections / organism
o Given with metronidazole
o No anaerobic coverage
Worrying about it takes precious time and attention away
from your priorities and increases your feelings of
dissatisfaction about life
MEDICINE 2:
DISEASES CAUSED BY GRAM POSITIVE BACTERIA
DR. FAJARDO
DISEASES CAUSED BY GRAM POSITIVE
BACTERIA
November 6, 2013
Dr. Fajardo
GRAM POSITIVE INFECTIONS
- Pneumococcal infections
- Staphylococcal infections
- Streptococcal and enterococcal infections
- Diphtheria
- Tetanus
- Botulism
- Gas gangrene and other Clostridial
infections
- Infections
caused
by
Listeria
monocytogenes
PNEUMOCOCCAL INFECTIONS
Epidemiology:
- Pneumococcal infections significant
global cause of morbidity and death (even
with the advent of antibiotics)
o Particularly among children and
elderly
- Pneumoccoci are divided into serogroups
or serotypes based on the capsular
polysaccharide
structure
(Quellung
reaction)
- Not all pneumococcal serotypes are
equally likely to cause disease
o Some causes mild diseases, and
o
other causes severe form
Serotype distribution varies with
age, disease syndrome
Strep.
Pneumoniae/Pneumococci
intermittent inhabitants of healthy human
nasopharynx
and
transmitted
by
respiratory droplets (Colonization)
In developing world settings
o Pneumococcal acquisition occurs
within a few days after birth
o Up to age of 5 years 70-90% of
children carry the organism in the
nasopharynx
o Adults > 40%
High rates of colonization
source of transmission
Becomes a source of
transmission
infection later
or
*Colonization is a transient event- org will
not survive in the nasopharynx for a long
time
o When a person is colonized Develops antibodies (IgG)
CLINICAL RISK GROUPS FOR PNEUMOCOCCAL
INFECTION:
- Asplenia or splenic dysfunction
o Spleen:
resposible
for
the
destruction
of
encapsulated
organism
If
no
spleen,
all
encapsulated organisms will
not be cleared by the body
Give vaccinations against strep
pneu, strep meningitidis, HIB
Chronic respiratory disease COPD,
bronchial asthma, cystic fibrosis
Chronic kidney disease
o For
patients
undergoing
hemodialysis
Chronic liver disease
DM
Immunocompromised/immunosuppresionHIV/AIDS,
chemotherapy,
pts
with
malignancy, pts receiving high dose
steroids
Cochlear implants
CSF leaks
o
MISCELLANEOUS
- Infancy and old age
- Prior hospitalization
- Alcoholism
- Cigarette smoking
- Day-care center attendance
- Residence in military training camps
- Prisons
- Homeless shelters
PATHOGENESIS
- From nasopharynx, bacterial spread via:
o Blood stream to distant sites
Brain,
joint,
bones,
peritoneal cavity (sterile
sites)
o Spread locally to mucosal surfaces
causing
otitis
media
or
pneumonia
-
Otitis media, pneumonia, bacteremia and
meningitis
are
the
most
common
pneumococcal infections
Colonization is relatively frequent, yet
disease is rare
o In the nasopharynx, pneumococci
survive in mucus secreted by
epithelial cells; they avoid local
immune factors (leukocytes and
complement)
MEDICINE 2:
DISEASES CAUSED BY GRAM POSITIVE BACTERIA
DR. FAJARDO
Eventually
results
in
the
development of capsule-specific
serum IgG
Play a role in mediating
clearance of bacteria from
the nasopharynx
HOST DEFENSE MECHANISMS:
a. Innate Immunity
- Intact respiratory epithelium and nonspecific or innate immune factors (first
line of defense)
o Examples of non- specific or innate
immune factors : mucus, splenic
function, complement, neutrophils,
and macrophages
- Physical factors cough reflex and
mucociliary escalators > clearance of
bacteria from the lungs
- Immunologic factors activation of
complement system
b. Acquired Immunity
by giving antigen thru vaccines ->
induce production of antibodies
- Induced via contact following colonization
or through cross-reactive antigens
development of serum IgG antibody
specific
for
pneumococcal
capsular
polysaccharide
CLINICAL MANIFESTATIONS:
- Depends on site of infection and duration
of illness
- Clinical syndromes are classified as:
o Noninvasive (otitis media)
Through contiguous spread
form nasopharynx or skin
o
Invasive (bacteremic pneumonia,
meningitis)
Involves infection of a
normally sterile site/body
fluids or follows bacteremia
Organism goes into the
bloodstream (bacteremia)can go to the meninges,
bones and joints , heart
(endocarditis)
PNEUMONIA
- Most common
syndrome
serious
PE
-
Cough evolves from dry cough to non
purulent to productive, sometimes bloodtinged
Pleuritic chest pain- especially if with
pleural effusion
Elderly change in mental status/
confusion or malaise, without fever or
cough; immune system is down regulated
findings:
Tachypnea (>30 bpm), tachycardia
Hypotension in severe cases, fever
Dullness to percussion (consolidation),
crackles on auscultation
Cyanosis hypoxemia
Nonrespiratory findings abdominal pain
(involvement of diaphragmatic pleura),
mental status changes
Differential Diagnosis of Pneumonia:
- Myocardial infarction and heart failure
with atypical pulmonary edema
- Pulmonary conditions atelectasis
- Pneumonia caused by other pathogens
such as viral pathogens, mycoplasmas,
and other bacterial pathogens
Diagnosis:
- Gold standard for etiologic diagnosis
pathologic examination of lung tissue
(biopsy): but it is very invasive so you
dont do it to diagnose, you can do CXR
instead
-
Evidence of an infiltrate on CXR
Blood CS
CBC, elevated LFT, elevated creatinine
o Leukopenia sign of a poorer
prognosis
o Kidneys elevated creatinine, can
lead to acute renal failure
Pneumococcal urinary antigen assays- not
available in our institution
Sputum CS
o Encapsulated
diplococci
presumptive
Picture: X-ray finding consolidation, infiltrates;
*** Some pts who have pneumonia may not
present with crackle/ with normal X-ray findings,
s but when you hydrate them, after hydration
crackles may be heard. Dehydrated pts will not
show any chest/ lung findings.
pneumococcal
Presenting manifestations:
- Abrupt onset of cough and dyspnea, fever
and chills, myalgia
Complications:
Empyema
o MC complication
o Collection of pus outside the lungs,
within pleural cavity
MEDICINE 2:
o
o
Persistent fever and leukocytosis
after 4-5 days of appropriate
antibiotics
Starts as a Parapneumonic effusion
(just a fld in the pleura)
Inflammatory response
self -limiting
Bacteria hematogenously
or by contiguous spread
Treatment:
Chest
tube
thoracostomy
Frank pus, gram (+) diplococci in
Grams staining, fluid pH of < 7.1
treat with aggressive and complete
drainage to avoid shock and sepsis
PNEUMOCOCCAL MENINGITIS
- Presents as a pyogenic condition
- Primary or a complication of other
conditions
o Skull fracture
o Otitis media
o Bacteremia
o Mastoiditis
- Routine Hib vaccine S. pneumoniae and
N. meningitides MC causes of bacterial
meningitis in adults and children ***
Clinical Manifestations:
- Non specific
- Severe,
generalized,
gradual
onset
headache, fever, nausea
- CNS manifestations
o stiff neck, photophobia, seizures,
confusion
- Clinical signs toxic appearance, altered
consciousness, sometimes bradycardia
and hypertension
- Kernigs or Brudzinkis sign or cranial
nerve palsies (3rd and 6th CN)
Definitive diagnosis:
Examination of CSF(Lumbar Tap):
- Evidence of turbidity (visual inspection)
- Elevated CHON level, elevated WBC,
reduced
glucose
concentration
***
(quantitative measurement) bacterial
meningitis
- Specific identification of etiologic agent
(Gram Stain, culture, antigen testing or
PCR)
- Blood culture for S. pneumoniae with
clinical manifestations of meningitis -->
confirmatory
Mortality rate approximately 20%
Acute and chronic complications
o Diffuse brain swelling,
o Subarachnoid hemorrhage,
DISEASES CAUSED BY GRAM POSITIVE BACTERIA
DR. FAJARDO
o
o
o
Hydrocephalus,
Cerebrovascular
complications(arteritis or infarcts),
Hearing loss
OTHER INVASIVE SYNDROMES
- Osteomyelitis- bones
- Septic arthritis- joints
- Endocarditis- heart
- Pericarditis- pericardium
- Peritonitis- abdomen
NON-INVASIVE SYNDROMES : local spread
Sinusitis
Otitis media
Presents initially as URTI facial pain,
congestion, fever, persistent night time
cough
Definitive dx aspiration and culture of
sinus materials
Acute onset of severe pain, fever, deafness,
tinnitus
PE: Red, swollen, bulging tympanic
membrane with reduced movement on
insufflations
Treatment:
Penicillin G
Ampicillin,
cefotaxime,
ceftriaxone and cefuroxime
Macrolides
(azithromycin,
clarithromycin)
and
cephalosporins
Clindamycin,
tetracycline,
TMP-SMZ
Penicillin-resistant
pneumococci
- Drug of choice
susceptible organisms
for
- Alternatives for Penicillin
allergic pts
- Exhibit some activity against
pneumococci
- Alteration in the penicillin
binding protein(PBP) genes**
by
transformation
of
horizontal transfer of DNA
from related streptococcal
species
Meningitis
- Higher dose and longer duration
- First line therapy:
o Vancomycin
+ cefotaxime or
ceftriaxone
Vancomycin + rifampicin
(allergy
to
beta-lactam
agents)
- Glucocorticoids(usually Dexamethasone)
significantly reduce rates of mortality,
severe hearing loss and neurologic
sequelae in adults
- Empiric treatment because result of
culture: 3-5 days to 7 days
MEDICINE 2:
Start
with
vancomycin
cefotaxime or ceftriaxone
DISEASES CAUSED BY GRAM POSITIVE BACTERIA
DR. FAJARDO
For outpatient management
- especially for otitis media, sinusitis; it
depends on the area:
o Amoxicillin
o Levofloxacin/moxifloxacin
o Clindamycin
o Azithromycin/clarithromycin
Prevention
Vaccination vs S. pneumoniae and
influenza viruses ( flu vaccines should
also be given because viral infections are
usually risk factors for the development
of bacterial infections)
2 KINDS OF PNEUMONIA VACCINE:
Capsular
- Recommended for > 65 y/o
Polysaccharide
(elderly)
Vaccine (PPV23)
- In the Philippines, it is given
to those who are 50 y/o and
above
- 2-64 y/o with medical
conditions- asplenic, with
DM, CKD, COPD, Bronchial
asthma
*Give every 5 years
Polysaccharide
- For infants and young
protein
Conjugate
children
Vaccine (PCV)
- In the Philippines, it is
recommended to give at the
age of > 65 y/o
- Efficacy vs IPD (Invasive
Pneumococcal
Disease),
pneumonia, otitis media,
nasopharyngeal colonization
and all-causes of mortality
STAPHYLOCOCCAL INFECTIONS
STAPHYLOCOCCUS AUREUS
- Most virulent, major cause of morbidity &
mortality for all staphylococcal species
- Part of the normal flora
o Anterior nares most frequent site
of colonization
o Vagina,
axilla,
perineum
and
oropharynx
o Reservoir of future S. aureus
infections
- Can invade the bloodstream/ cross the
mucosal barrier
Leading cause of nosocomial infections
surgical site infections, hospital acquired
infection due to S. aureus
PATHOGENESIS OF INVASIVE S. AUREUS
INFECTION:
- Causes infection by:
Inoculation and local colonization of
tissue surfaces brought about by
surface proteins
o Most common surface protein:
MSCRAMMs
(microbial
surface
components recognizing adhesive
matrix molecules)- makes them
adhere to epithelial surfaces
Invasion
o Invade tissues by the production of
serine proteases, hyaluronidases,
thermonuclease and lipases
Evasion of the host response
o By
the
antiphagocytic
polysaccharide microcapsule
Metastatic spread via the bloodstream
HOST RESPONSE:
- Protection: PMNs- first line of defense
against this infection
INCREASED RISK OF INFECTION:
- DM
Neutropenic
chronic granulomatous disease
abnormalities
of
the
skindermatitis
prosthetic devices (prosthetic
valves, catheters)
atopic
heart
TOXIN MEDIATED DISEASES:
3 Types of Toxins:
Cytotoxin
Pyrogenic
superantigens
(endotoxins)
Exfoliative toxins
toxin
Responsible
for
the
formation of Abscesses
Toxic shock syndrome
Food poisoning
Staphylococcal
scalded
skin syndrome (SSSS)
Serotypes ETA, ETB
Serine protease activity
triggers exfoliation
SKIN AND SOFT TISSUE INFECTIONS:
CUTANEOUS INFECTIONS
- Formation of pus-containing blisters
o Begin in hair follicles invade
adjoining tissues
MEDICINE 2:
DISEASES CAUSED BY GRAM POSITIVE BACTERIA
DR. FAJARDO
o
o
o
Septic
-
Folliculitissuperficial
infection with central area
of purulence, induration and
erythema
Furuncles
(boils)more
extensive than foliculitis,
true abscess
Carbuncles collection of
furuncles; most commonly
located in lower neck area,
coalescence
of
smaller
abscess seen deeper in
the skin and subcutaneous
tissue
Mastitis
Impetigo, cellulitis
Hidradenitis
suppurativa
recurrent
follicular
infections
(axilla)
Surgical wound infections
MUSCULOSKELETAL INFECTIONS
S. aureus MC cause of bone infections
Hematogenous
dissemination
or
contiguous spread from a soft tissue site
o Hematogenous osteomyelitis in
children long bones
Adults MC location is vertebra causing
vertebral osteomyelitis, can be secondary
to:
o Endocarditis
(drug
users)
,
undergoing hemodialysis, diabetic
injection drug users
Epidural abscesses
arthritis
Trauma, surgery or hematogenous
Knees, shoulders, hips, phalanges
Joints
previously
damaged
osteoarthritis, Rheumatoid Arthritis
by
Pyomyositis
- Unusual infection of skeletal muscles in
tropical climates
- Usually with history of trauma
RESPIRATORY TRACT INFECTIONS
-
Pneumonia: mc; Shortness of breath,
fever, respiratory failure; course is more
rapid
than
pneumonia
caused
by
pneumococci
CXR pneumatoceles (shaggy, thinwalled cavities)
Pneumothorax, empyema complications
Picture: X-ray with pneumatocele: with
thin cavity as compared to infection by
pneumococci (consolidation)
In selected clinical settings:
- ICU nosocomial pneumonia
- Community acquired
o Postviral infections or as a result of
septic pulmonary emboli
BACTEREMIA, SEPSIS AND IE (endocarditis)
S. aureus bacteremia
Complicated by sepsis, endocarditis,
vasculitis or metastatic seeding
Comorbid conditions: DM, HIV, renal
insufficiency
25-35% of IE cases (usually right sided
IE)
o Concomitant Injection Drug Use,
hemodialysis,
intravascular
prosthetic
device,
immunosuppression
PROSTHETIC DEVICE RELATED INFECTIONS
- Intravascular catheters, prosthetic valves,
orthopedic
devices,
peritoneal/interventricular catheters, and
vascular grafts
- Biofilm formation in the device, pyogenic
collection at the device site -> goes to
bloodstream: bacteremia
- Blood cultures important in the
diagnosis
Abscess cytotoxin
TOXIN-MEDIATED DISEASES:
Toxic Shock Syndrome
- TSST-1 (endotoxin): seen in > 90% in
menstruating women
- Enterotoxins: high in non-menstruating
women
- Begins with a relatively non-specific flulike symptoms
o Menstrual cases 2-3 days after
the onset of menses
Case definition: mostly systemic:
- Fever: > 38.9 C
- Hypotension
- Diffuse macular rash with desquamation in
1-2 wks after onset
- Multisystemic involvement
o Hepatic
o Hematologic
o Renal
o Mucous membranes
o Gastrointestinal
o Muscular
o CNS
- Negative serologic/other test for measles,
lepto, RMSF
MEDICINE 2:
DISEASES CAUSED BY GRAM POSITIVE BACTERIA
DR. FAJARDO
(MRSA)
Food Poisoning
- Secondary to inoculation of toxinproducing S. aureus into food by colonized
food handlers
- Custards, potato salad, processed meats
- Onset of diarrhea 1-6 hrs after ingestion
- n/v, diarrhea, hypotension, dehydration
- symptoms resolve within 8-10 hrs
- self- limiting; just hydrate
Staphylococcal Scalded Skin Syndrome (SSSS)
- most often in newborn and children
o localized
blister
formation
to
exfoliation of much of the skin
surface
o skin- fragile, tender, with thinwalled, fluid-filled bullae/ vesicle
o Nikolskys sign gentle pressure
results in rupture of lesions
denuded underlying skin
o mucous
membranes:
usually
spared
vs Steven Johnsons (skin
lesion,
bullae
formation
involving
the
mucous
membrane)
o fever, irritability with poor feeding
- Pictures: bullae and denuded skin; infant
erythematous with blister like formation
that has already ruptured
COAGULASE
NEGATIVE
STAPHYLOCOCCAL
INFECTIONS
- Less virulent than S. aureus
- MC causes of prosthetic-device infections*
o S.
epidermidis
elaborate
extracellular polysaccharide (slime)
Facilitates formation of a
protective biofilm on the
device surface
General principles of therapy:
- Selection of appropriate antimicrobial
therapy
- Surgical incision and drainage for all
suppurative collections
- Removal of prosthetic devices
- TSS and food poisoning supportive
therapy
Antimicrobial Therapy:
Sensitive to penicillin
Sensitive to methicillin
Resistant
to
Methicillin
Penicillin
Alt:
nafcillin,
oxacillin,
cefazolin
Nafcillin or oxacillin
Alt: cefazolin, vancomycin
Vancomycin
Alt: TMP-SMX, Daptomycin,
Tigecycline, Linezolid
Duration of treatment: IE: 46 weeks IV
Drained Abscess 7-10 days
Prevention
- Hospital
setting:
handwashing
and
appropriate isolation procedures
- Topical antimicrobial agents (mupirocin) -eliminate nasal colonization to prevent
subsequent infection
o Apply at anterior nares every night
for 10 days
o
For
patients
Hemodialysis
and
dialysis
undergoing
peritoneal
Recurrent boils S. aureus
STREPTOCOCCAL INFECTIONS:
Streptococci
Group A Strep (S.
pyogenes)
Group B Strep (S.
agalactiae)
Enterococci
Viridans
Part of normal human flora
Colonizes the respiratory, GI, GUT
Streptococcal
pharyngitis,
Acute
rheumatic fever, GN
Bacterial sepsis and meningitis in
newborn
Endometritis and fever in parturient
UTI,
nosocomial
bacteremia
and
endocarditis
MC bacterial endocarditis (community
acquired)**
GROUP A STREPTOCOCCAL PHARYNGITIS
- MC bacterial infection of childhood 2040% of exudative pharyngitis in children
- Transmission respiratory droplet
- Incubation Period: 1-4 days
- Sore throat, fever, chills, malaise
- Intense erythema and swelling of the
pharyngeal mucosa, purulent exudates
over the posterior pharyngeal wall and
tonsillary pillars
- Enlarged, tender anterior cervical lymph
nodes- a sign that it is casued by Grp A
strep
Treatment
- Symptoms resolve after 3-5 days
- Course is shortened by antibiotics given
to prevent suppurative complications and
rheumatic fever
- Benzathine PCN 1.2 mU IM or
- Penicillin V 250 mg PO TID or 500 mg PO
bid x 10 days ***
MEDICINE 2:
DISEASES CAUSED BY GRAM POSITIVE BACTERIA
DR. FAJARDO
Complications:
- Peritonsillar or retropharyngeal abscesses,
sinusitis,
otitis
media,
meningitis,
bacteremia, endocarditis, pneumonia
- Most Frequent: Acute Rheumatic Fever,
Poststreptococcal Glomerulonephtiris
SCARLET FEVER
- Strep pharyngitis accompanied by a
characteristic rash
- Rash streptococcal pyrogenic exotoxin
A, B, C
o Begins on the 1st or 2nd day of
illness over the upper trunk,
extremities, spares palms and
soles
(vs foot and mouth dse
which involves the palms and
soles)
o Minute papules, sandpaper feel to
the skin
o Associated circumoral cyanosis,
strawberry tongue
o Subsides in 6-9 days, followed by
desquamation of the palms and
soles
- Become less common in recent years
- Picture
o Differentiate from rash of measles,
dengue fever, Chikungunya
SKIN AND SOFT TISSUE
IMPETIGO
- Superficial infection of the skin
- Caused primarily by group A streptococci
- Most often in young children conditions
of poor hygiene
- Usual site face (around nose and
mouth), and the legs
- Red papules, vesicular, pustular lesions;
coalesce to form characteristic honeycomb
crust
Treatment
- Penicillin
- Empiric regimen should cover for both
streptococci and S. aureus
o Dicloxacillin or cefalexin for 10
days
ERYSIPELAS
- Infections
involving
skin
subcutaneous tissue
- Portal of entry traumatic or
wound, insect bite or any break
integrity
o Bright red appearance
involved skin, plateau
and
surgical
in skin
of the
sharply
demarcated
from
surrounding
normal skin
o Warm to touch, tender, appears
shiny and swollen
o Peau
d
orange
texture
involvement
of
superficial
lymphatics
o Malar area of the face and lower
extremities
Treatment: Penicillin
Picture
DEEP SOFT-TISSUE INFECTIONS:
NECROTIZING FASCIITIS
- Aka. Hemolytic Streptococcal Gangrene
- Superficial/deep fascia investing the
muscles of an extremity or trunk
- Usually secondary to Trauma, bowel flora
abdominal surgery, or occult enteric
source diverticular/appendiceal abscess
- Minimal erythema of the overlying skin,
severe pain and tenderness
- Treatment early surgical exploration
o High dose penicillin + clindamycin
STREPTOCOCCAL TOXIC SHOCK SYNDROME
- Isolation of group A strep (S. pyogenes)
- Clinical signs of severity
o Hypotension
o 2 or more of the following signs:
Renal impairment
Coagulopathy
Liver involvement
ARDS, generalized edema,
pleural
or
peritoneal
effusions
with
hypoalbuminemia
Generalized erythematous
macular rash
Soft
tissue
necrosis
necrotizing
fasciitis
or
myositis or gangrene
- Treatment
o Clindamycin more effective in
rapidly
terminating
toxin
production than penicillin
o Penicillin
o IV Ig- adjunctive therapy for
streptococcal TSS
DIPHTHERIA
Corynebacterium diphtheriae
- Aerobic,
nonmotile,
nonsporulating,
irregularly staining, gram-positive rod
- Club-shaped,
arranged
in
clusters
(Chinese letters) or parallel arrays
- Both tox + and tox strain are infectious
MEDICINE 2:
DISEASES CAUSED BY GRAM POSITIVE BACTERIA
DR. FAJARDO
Tox + strains are more likely to
cause pseudomembranes
o Immunization
with
diphtheria
toxoid elicits antibody (antitoxin)
that neutralizes toxin and prevents
diphtheria
Transmission close personal contact,
respiratory
o
Respiratory Diphtheria
- Case definition used by CDC
o Clinical syndrome URTI with sore
throat, low-grade fever and an
adherent membrane of the tonsils,
pharynx and/or nose
o Laboratory criteria isolation of C.
diphtheria from a clinical specimen
or histopathologic diagnosis of
diphtheria
- Complications:
o Obstruction of the respiratory tract
o Myocarditis and polyneuropathy
toxic manifestations of diphtheria
Picture: membrane over the tonsillar area
Treatment
- Diphtheria antitoxin most important
element in the treatment
- Antibiotics little demonstrated effect on
the healing in patient treated with
antitoxin
- Primary goal of antibiotic therapy
eradication and prevention of transmission
from the patient to susceptible contacts
o Erythromycin PO or Pen G IM x 14
days
Prevention
- DTaP children up to 7 y/o
- Td (Tetanus and diphtheria) adult use,
booster immunizaition at 10 years interval
o 0,1,6 tetanus toxoid
- Close contact, household contacts 7-10
days prophylaxis with erythromycin or
penicillin
----end.
MEDICINE 2:
DISEASES CAUSED BY GRAM POSITIVE BACTERIA PART2
DR. FAJARDO
GRAM POSITIVE INFECTIONS PART II
DR. FAJARDO
NOVEMBER 7, 2013
LISTERIA MONOCYTOGENES
Food borne pathogen- serious infection in
pregnant women and
immunocompromised individuals
Infection follows ingestion of
contaminated food- the person should
ingest large or high concentration of the
organism to produce the disease
Entry into cells: mediated by host surface
proteins (internalin)
Internalin-mediated entry and is
important in crossing intestinal, bloodbrain and mucoplacental barrier
Listeriolysin O (LLO)- one of the
determinants which mediates the rupture
of phagosomal membrane following
phagocytosis of the organism
3.
Meningitis
5-10% of all cases of community acquired bacterial
meningitis in adults
Diagnosis is considered in all older and chronically ill
adults
Subacute illness, nuchal rigidity and meningeal signs
less common hence the diagnosis might be missed
o The Subacute course of the illness
differentiates it with meningitis caused by
other etiologic agent
CSF: WBC 100-500/uL, neutrophilic predominance,
low glucose
o WBC count is higher than bacterial yield,
protein is normal
Usually associated with hydrocephalus
4.
Meningoencephalitis and focal CNS infection
Directly invade the brain parenchyma: cerebritis or
focal abscess
Results from bacteremic seeding, often positive
blood culture
Concurrent meningitis may occur: CSF normal
Invasion of the brainstem: rhombencephalitis
o Fever, headache, asymmetrical CN deficits,
+ cerebellar signs, hemiparetic and
hemisensory deficits, respiratory failure
o Waych out for Impending herniation
MRI: ring enhancing lesions are seen (focal
abscesses)
5.
Infection in pregnant women and neonates
Listeriosis in pregnancy- severe, bacterimic
Acute or subacute febrile illness with myalgia,
arthralgia, backache and headache
Preterm delivery is a common complication,
diagnosis may be made only postpartum
70-90% of fetuses from infected women become
infected
Prepartum treatment of bacteremic women:
increases chance of normal infant
Only diagnosed by blood culture
Overall mortality rate for fetuses infected in utero is
50%- very high so always suspect it and include as
differential diagnosis
Among live born neonates treated with antibiotics
20% mortality rate
Granulomatosis infantiseptica: overwhelming
listerial fetal infection with military microabscesses
and granulomas skin, liver and spleen
Late onset neonatal illness; asymptomatic in the 1st
10 days
Groups at risk
Pregnant women, elderly, neonates,
immunocompromised by organ transplants (due to
immunosuppresants), cancer or treatment with TNF
antagonists or glucocorticoids
Chronic medical conditions: alcoholism, diabetes,
renal disease, rheumatologic illness, iron overload
Clinical syndromes
Gastroenteritis
Bacteremia
Meningitis
Meningoencephalitis and focal CNS infection
Infection in pregnant women and neonates
1.
Gastroenteritis
Develops within 48hrs after ingestion of a loarge
inoculums of bacteria in contaminated foods (milk,
delimeates, salads, soft cheeses, hotdogs)
Fever, diarrhea, headache and constitutional
symptoms
Outbreaks
Diagnosis blood culture or stool culture
2.
Bacteremia
Fever, chills, myalgias/arthralgias
o Fever and chills are the usual symptoms
Meningeal symptoms, focal neurologic findings,
mental status changes
Organism is documented in 70-90% of cancer
patients with listeriosis
o We can easily grow this organism
Pregnant women- common presentation is flulike
illness with fever- difficult to differentiate with viral
infection unless blood culture is done
MEDICINE 2:
Treatment
Ampicillin- drug of choice (high dose)
Penicillin also highly effective
Gentamicin + ampicillin - synergistic activity
TMP-SMX alternative for penicillin allergic patients
Cephalosporins are not effective
Neonates: ampicillin + gentamicin- synergistic
activity
Duration of treatment
o Bacteremia-2wks
o Meningitis-3wks
o Endocarditis-4-6wks
o Brain abscess/encephalitis-6-8wks
o Patient must complete the course; if not
completed relapse may occur and is harder
to treatment
TETANUS
2 exotoxins: tetanospasmin (causes the pathology of
spasms) and tetanolysin
Contamination of wound with spores
o Germination and toxin production in
devitalized tissues, foreign bodies, active
infecton
o Toxin binds to peripheral motor neuron
terminalsaxonsnerve cell body in the
brainstem and spinal cord by retrograde
intraneural transport
o Presynaptic terminals- blocks the release of
glycine and GABadinminishes inhibition
rigidity
o Consequent producton of spasms,
increased avtivity of reflexes that limit
spread of impulses
Types
1. Generalized tetanus
Most common form
Increased muscle tone and generalized spasm
Trismus or lockjaw
Dysphagia, stiffness or pain in the neck, shoulder and
back muscles
Rigid abdomen and stiff proximal limb muscles
Risus sardonicus- sustained contraction of facial
muscles
Opisthotonus- contraction of the back muscles
Autonomic dysfucction e.g. hypertensive then
sudden hypotension or tachycardia then sudden
bradycardia, excessive sweating
Neonatal tetanus is under general tetanus
2. Local/cephalic tetanus
Diagnosis
Based entirely on clinical findings- need a very high
suspicion for diagnosis
Wounds should be cultured in suspected cases
DISEASES CAUSED BY GRAM POSITIVE BACTERIA PART2
DR. FAJARDO
Treatment
Goals of therapy
o Eliminate the source of the toxin
o Neutralize unbound toxin
o Prevent muscle spasm
o Provide respiratory support
Spasm of back and abdominal
muscles impair respiratory function
Most common cause of death is
respiratory failure
Admitted to quiet room- ICU
o Cardiopulmonary monitoring
Antibiotic therapy
o Eradicate vegetative cells penicillin
o Metronidazole- drug of choice, preferred
due to the absence of activity antagonistic
to GABA
o Penicillin
o Clindamycin and erythromycin
st
1 thing given is the antitoxin or tetanus
immunoglobulin
o Neutralize circulating toxin and unbound
toxin in the wound
o TIg STAT- may save the patient
o Should be given immediately and within 24
hours it effectively lowers mortality
Control of muscle spasm
o Sedatives
o Diazepam, lorazepam, midazolam
o Barbiturates and chlorpromazine
Respiratory care
o Immediate intubation or tracheostomy with
or without mechanical ventilation
o Give mechanical ventilation if respiration is
impaired
Autonomic dysfunction
o Hypertension and tachycardia or
Sympathetic over reactivity
Labetolol, esmolol, clonidin and
morphine sulfate
o Hypotension and bradycardia
Volume expansion, use of
vasopressors or chronotropic
agents or pacemaker insertion
Vaccine
o Active immunization during recoveryImmunity is not induced by a small amount
of toxin that produces the disease
o Give vaccine during recovery and not on the
active phase of the infection
o If you had tetanus infection in the past it
does not mean you will never have it again
MEDICINE 2:
Prevention
o
Active immunization-Td
All partially immunized and
unimmunized adults should
receive vaccine
Primary series for adults should
receive vaccine
Primary series for adults- 3 doses
(0,1,6-12 mos after 2nd dose)
Booster dose is required every 10years
If a patient is not sure of his
tetanus vaccination, is it ok to
give? YES
Vaccine given during the 1st year of
life- booster dose at ten years old
then another booster at 20 years
old
Proper wound management
BOTULISM
Paralytic disease potent protein neurotoxin
elaborated by C. botulinum
Case classification
o Food borne botulism- from canned goods
that are expired
o Wound botulism
o Intestinal botulism- causes diarrhea
currently less cases of botulism are noted s
Bioterrorism and biological warfare
o Dispersed as an aerosol (inhalational
botulism)
o Contaminant in material to be ingested
(food-borne)
Diagnosis
o Clinically, symmetrical descending paralysis,
afebrile, mentality intact
Differentiate it with CVD or stroke
o Demonstration of toxin in serum by
bioassay-definitive dianosis
GAS GANGRENE AND OTHER CLOSTRIDIAL INFECTIONS
Etiology
Resides in the GI and female genital tract
Anaerobic organism
Do not grow on artificial media in the presence of
oxygen
Produce abundant gas in artificial media and form
subterminal spores
30 species- colonize human
o C. ramrosum- most common
o C. perfringens- gas gangrene
C. perfringens- most common sp isolated from tissue
infections and bacteremias
DISEASES CAUSED BY GRAM POSITIVE BACTERIA PART2
DR. FAJARDO
o
o
C. novyl and septicum
Classified according to lethal toxin
production- types a-e
Type a- food poisoning
Type c- enteritis necroticans
C. difficile- antibiotic associated
colitis
A. GAS GANGRENE (CLOSTRIDIAL MYONECROSIS)
C. perfringens- most common of the clostridial spp
isolated from tissue infections and bacteremias
Rapid and extensive nectrosis of the muscle with gas
formation and systemic toxicity sepsis
Trauma involving deep muscle laceration
o Differentiated from necrotizing fasciitis
because NF only involves fascia but in gas
gangrene it involves deeper tissues like the
muscles
Incubation Period <3 days
Frothy wound exudate tense skin, whiter and cooler
than normal (vascularity in the area is very poor)
o Because of compression of the vascular
structures inside
Symptoms progress rapidly, profuse serous
discharge- peculiar sweetish smell
Treatment
o Surgical debridement of devitalized tissues
with wide excision
o Penicillin +clindamycin
B. TOXIC SHOCK SYNDROME
Clostridial infection of the endometrium C. sordelli
o After gynecological procedures, child birth
and abortions
o very lethal disease but because of aseptic
technique or sterile procedures in gyne, it is
usually not seen anymore
Systemic manifestations- edema, effusions,
profound leukocytosis and hemoconcentrationfollowed by rapid onset of hypotension, multi organ
failure and death
Other infections not gynecologicaly related: IDU,
trauma or surgery
DOC: penicillin + clindamycin
C. CLOSTRIDIUM DIFFICILE INFECTION (CDI/
PSUEDOMEMBRANOUS COLITIS)
Colonic disease that is acquired almost exclusively in
association with prolonged antibiotic use
Disruption of normal colonic flora
Most commonly diagnosed diarrheal illness acquired
in the hospital
CDI results from ingestion of spores that vegetate,
multiply and secrete toxins- diarrhea and
pseudomembranous colitis (PMC)
MEDICINE 2:
Pathogenesis
Spores of toxigenic difficile are ingested- survive
gastric acidity that is why these organisms can go to
the colon
Germinate in the small bowel
Colonize the colon and elaborate 2 toxins
o Toxina a (enterotoxin) and toxin b
(cytotoxin)
o Initiate processes resulting in the disruption
of epithelial cell barrier function, diarrhea
and pseudomembrane formation
Clinical manifestations
Diarrhea- most common manifestation
o Stools almost never grossly bloody, soft to
uniformed, watery to mucoid in consistency
o +/- 20 bowel movements per day high
bowel output
Fever, abdominal pain and leukocytosis
Adynamic ileus results in cessation of stool passage
o Complications: toxic megacolon and sepsis
o Need a high index of suspicion to diagnose
o Eg. Initially a patient had diarrhea for 3 days
but stops on the 4th day due to the
development of adynamic ileusif the
physician does not recognize this it will
progress to sepsis
Treatment
Initially stop the antibiotics
Initial episode
o Mild to moderate- oral metronidazole
o Severe- oral vancomycin
Initial episode, severe, complicated or fulminant
o Vancomycin +metronidazole
o Rectal instillation of vancomycin
st
1 recurrence- same management as initial episode
nd
2 recurrence- vancomycin in tapered/ pulse
regimen
Multiple recurrences
o Repeat vancmoycin taper/pulse
o Vancomycin +saccharomyces bouldardii
o Rifaximin
o Nitazoxanide- not available in the phls
o Fecal transplantation
Rationale: bring back the normal
flora
It can be that feces will be infused
but where will they get the feces?
o IV Immunoglobulin
DISEASES CAUSED BY GRAM POSITIVE BACTERIA PART2
DR. FAJARDO
MEDICINE 2:
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART1
DR. FAJARDO
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA
N. meningitidis
N. gonorrhea
Moraxella catarrhalis
Haemophilus influenzae
Legionella penumophilia
Bordetella
Enterobacteriaceae
A. MENINGOCOCCAL INFECTION
- Neisseria meningitides
o Meningococcal meningitis
o Fulminant meningococcemia
- 13 serogroups according to the antigenicity of the
polysaccharide capsule
o A,B, C, Y, W-135 - >90%of cases
- Humans are the only natural reservoir
- The nasopharynx is the site from which
meningococci are transmitted by aerosol or
secretions
Epidemiology
- Occurs worldwide sporadic cases, outbreaks, large
epidemics
- Largest recorded outbreak of meningococcal disease
in the Philippines started at the end of September
2004-CAR
o Serogroup A, sequence 7
o Over 150 cases, 40 deaths
Pathophysiology
- Outer membrane components associated with
virulence
o Polysaccharide capsule
Major virulence for N.
meningitides
Antiphagocytic and antibactericidal
properties enhance
meningococcal survival in the
bloodstream
o Outer-membrane proteins
Pili outer membrane, proteinbased organelles
Facilitate adhesion
OMP porins Por A and Por B
Creates pores through
which small hydrophilic
solute pass
Opc involved in cell attachment
o
Lipooligosaccharides
Potent endotoxic activity
Mediates the induction of
inflammatory cytokines
Rates of morbidity and mortality
directly correlated with the
amount of circulated endotoxin
Causes the severity of the disease
Host Defense Mechanisms
o Major bactericidal antibodies IgM and IgG
bind to the capsular polysaccharide
o Complement required for bactericidal
activity and efficient opsonophagocytosis
o Infants are protected during the first
months of life passively transferred
maternal IgG antibodies
Clinical Syndromes Associated with Meningococcal Disease
- Respiratory tract infection
o Pneumonia
o Epiglottitis
o Otitis media
- Focal infection
o Conjunctivitis
o Septic arthritis
o Urethritis
o Purulent pericarditis
- Meningococcemia
- Meningitis
Meningococcemia
- Fever, chills, nausea, vomiting, myalgia
- Prostration is common
- Most distinctive feature is rash
o Erythematous macules petechial
purpuric
o Petechiae may coalesce into hemorrhagic
bullae necrosis ulceration
Vs dengue: bigger petechiae than
petechiae in dengue, violaceous
rather than reddish
Concomitant meningitis
10-30% of meningococcemia without clinically
apparent meningitis
Fulminant meningococcemia CSF is normal
o Absence of meningitis poor prognostic
sign
o Rapid multiplication of bacteria in the blood
MEDICINE 2:
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART1
DR. FAJARDO
Chronic meningococcemia
o Rare syndrome of episodic fever, rash,
arthralgia weeks to months
o Maculopapular to petechial rash,
splenomegaly
o Be cautious with giving steroids may
cause meningitis, fulminant
meningococcemia
Waterhouse-Friedrichsen Syndrome
o DIC-induced microthrombosis, hemorrhage
and tissue injury
o Adrenal failure, adrenal hemorrhage
Diagnosis
- Most useful clinical finding petechial, purpuric
rashes
- Definitive diagnosis
o Isolation of bacteria from sterile sites
blood, CSF or synovial fluids
o Mueller-Hinton or chocolate blood agar
Clinical Management in the Hospital Setting
- The clinical management of meningococcal disease
consists of the following
o Diagnostic work up
o Use of antibiotics
o Supportive therapy
o chemoprophylaxis
-
Use of antibiotics
Antibiotic
Benzyl penicillin
Ceftriaxone
Cefotaxime
Chloramphenicol
Treatment
Child 250, 000 u/kg/day,
(Maximum 12 million u/day)
Adult: 1.8 g IV every 4 hours
To be given in 4 divided doses
for 7-10 days
Child: 75-100 mg/kg/day
(maximum 4 gm/day)
Adult: 2 or 4 gm IV
To be given in 1 or 2 doses for
7-10 days
Child: 200 mg/kg/day
(maximum 8 gm/day)
Adult: 2 g IV
To be given IV every 6 hours
for 7 days
Child: 75-100 mg/kg/day
(maximum 2 gm/day)
Adult: 500 mg/dose
To be given IV every 6 hours
for 7-10 days
-
Supportive therapy
o Oxygen, intubation (ARDS)
o IV fluids
D5LRS, D5 0.90 NaCl or plain LRS
Colloids
o Use of steroids remain controversial
Chemoprophylaxis
o Household contact of an index case
o Young daycare center contacts
o Persons who have had significant contact
with the oral/nasal secretion of an index
case
o Health care workers who have had intimate
exposure to nasopharyngeal secretions (e.g.
mouth to mouth resuscitation, intubation)
Recommended chemoprophylaxis Regimens for High-Risk
contacts and people with invasive meningococcal disease
Age of
Infants,
Children and
Adults
Rifampicin
1 mo
Dose
Duration
Cautions
5mg/kg
orally every
12 hour
2 days
<1mo
10mg/kg
(minimum
600mg)
orally every
12 hour
2 days
May interfere
with efficacy of
oral
contraceptives
and some seizure
prevention and
anticoagulant
medications;
may stain soft
contact lenses
Ceftriaxone
15y
125mg IM
SD
>15y
250mg IM
SD
500mg
orally
SD
Ciprofloxacin
18y
To decrease pain
at injection site,
dilutewith 1%
lidocaine
Not
recommended
for people <18
y/o
Prevention
- Meningococcal vaccine
o Available as bivalent (groups A and C) or
tetravalent (groups A,C,Y,W135) vaccines
- Isolation precautions
o Respiratory isolation for the first 24 hours
Transmission is via respiratory
route
MEDICINE 2:
Outbreak control
o Occurrence of 3 or more cases within <3
months in persons who reside in the same
area
o Mass vaccination
o Mass chemoprophylaxis
B. NEISSERIA GONORRHEA
Gonorrhea
- Remains a global public health problem worldwide
- Plays a role in enhancing transmission of HIV
- Transmitted from males to females more efficiently
- Rate of transmission to a woman following a single
unprotected sexual encounter with an infected man
-40-60%
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART1
DR. FAJARDO
Gonococcal Arthritis
- Disseminated Gonococcal infection (DGI)
o Results from gonococcal bacteremia
o DGI strains resists bactericidal action of
human serum
Do not incite inflammation at the
genital sites
Po1A serotype
o Menstruation risk factor, 2/3 of cases are
women
-
Gonococcal Infections in Males
- Acute urethritis most common manifestation
- IP: 2-7 days
o Interval can be longer and some men
remain asymptomatic
- Urethral discharge and dysuria
o Usually without frequency or urgency
o Profuse and purulent
Gonococcal Infections in Females
- Gonococcal cervicitis
o Mucopurulent cervicitis N. gonorrhea, C.
trachomatis, other organisms
o Women usually develop symptom
Scanty discharge from the vagina
and dysuria
Symptoms develop within 10 days
of infection, more acute and
intense than chlamydial cervicitis
In males, amount of
discharge is more but
more number of males
are asymptomatic
o Complications
Dyspareunia and lower abdominal
and back pain
Ascending infection acute
endometritis, acute salpingitis
Tubal scarring - infertility,
increased risk of ectopic pregnancy
Pelvic infection upper abdomen
perihepatitis (Fitz-Hugh Curtis
Syndrome)
-
Gonococcal vaginitis
o Occurs in anestrogenic women (prepubertal
girls and postmenopausal women)
o Vaginal mucosa red and edematous,
abundant purulent discharge
o Inflamed cervical erosions and abscesses
Other clinical manifestations
o Anorectal gonorrhoea anal sex
o Pharyngeal gonorrhoea
o Ocular gonorrhoea in adults
Clinical Manifestations
o Bacteremic stage
Fever and chills
Painful joints, tenosynovitis and
skin lesion (pustules and papules)
Polyarthralgias knees, elbows,
distal joints; axial skeleton spared
o Joint localized stage with suppurative
arthritis
Septic arthritis knees, wrists,
ankles and elbows
Laboratory Diagnosis
- Gram stain of urethral exudates
o Gram negative intracellular monococci or
diplococci - highly selective and sensitive
- Modified Thayer Martin Agar
- DGI - blood and synovial fluid culture
Recommended Treatment for Uncomplicated GC
- Cefixime 400mg PO single dose or Ceftriaxone
125mg SD + Azithromycin 1g PO SD or Doxycycline
100mg PO BID x 7 days
o Gonorrhea is almost always associated with
Chlamydia so give coverage for Chlamydia
Prevention
- A-B-C
o Abstinence
o Be faithful
o Condom
- Spermicidal preparation with diaphragm and cervical
sponges
- All sexual partners should be evaluated and treated
o ping pong effect
C. MORAXELLA CATARRHALIS
- Gram-negative cocci
- Sometimes occurring in pairs kidney bean
configutaion
- Normal flora of upper airways
- Otitis media and sinusitis
MEDICINE 2:
Purulent tracheobronchitis and Pneumonia
o Acute exacerbation of chronic bronchitis
o Fever and leukocytosis
o >50 y/o, history of cigarette smoking and
underlying COPD
o Rarely occurs in otherwise healthy host
Treatment
o Penicillin/clavulanic acid combination
o Penicillin resistance mediated by Blactamases
B-lactam/B-lactamase inhibitor
effective mode of treatment
nd
rd
2 and 3 generation
cephalosporins
Tetracycline, macrolides, ketolides,
TMP-SMX, quinolones,
chloramphenical
o 5 day course respiratory infection
o Longer course in sunisitis (7-14 days)
D. HAEMOPHILUS INFECTIONS
- Gram-negative organism of variable shape
o Pleomorphic coccobacillus
- 2 factors required for growth
o X (hemic) and V (NAD) factors
- 6 serotypes based on distinct polysaccharide capsule
(a-f)
- Type b and nontypable strains most relevant
strains clinically
- 1st free living organism to have its entire genome
sequenced
Transmission
- Airborne droplets or direct contact with secretions
or fomites
- Nontypable strains colonize the upper respiratory
tract of up to of healthy adults
o HiB conjugate vaccine decrease in
nasopharyngeal colonization and incidence
of infection
Pathogenesis
- Hib strains invasion and hematogenous spread to
distant sites such as the meninges, bones and joints
o Type b polysaccharide capsules
Important virulence factor
Avoids opsonisation and cause
systemic disease
*asplenic patients cannot clear
encapsulated organism (S. pneumoniae, N.
meningitides, Hib) should receive
vaccination for these organisms
-
Nontypable strains
o Local invasion of mucosal surfaces
o Otitis media, chronic bronchitis recurrent
lower respiratory tract infection
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART1
DR. FAJARDO
Low incidence of invasive disease
Haemophilus Influenzae Type B (HiB)
- Meningitis
o Most serious manifestation
o Infants <2 y/o
o Subdural effusion most common
complications
o Lower incidence due to advent of HiB
vaccinations
S. pneumoniae and N.
meningitides more common
causes of meningitis at present
- Epiglottitis
o Cellulitis of the epiglottis and supraglottic
area life threatening infection
o 2-7 y/o
Non typable H. influenzae
- Community-acquired pneumonia in adults
o Common among patients with COPD or
AIDS
o Exacerbations of COPD
Increased cough, sputum
production and shortness of
breath
- Childhood otitis media
o With S. pneumoniaand M. catarrhalis
- Less common:
o Puerperal sepsis
o Neonatal bacteremia
o Sinusitis in adults and children
Diagnosis
- Recovery of the organism in culture
- Gram staining- gram negative coccobacilli
Treatment
- Meningitis
o Ceftriaxone or cefotaxime
o Ampicillin + Chloramphenicol
o Glucocorticoids decrease neurologic
sequelae
- Nontypable strains
o 25% produce B lactamase
Resistant to ampicillin
o TMP-SMX, amoxicillin/clavulanic acid,
extended spectrum cephalosporin, newer
macrolides, fluoroquinolones
Prevention
- Hib conjugate vaccine all children
E. HAEMOPHILUS DUCREYI
- Chancroid
o STD genital ulceration and inguinal
adenitis
MEDICINE 2:
o
o
Enhances HIV transmission
Recurring epidemiologic themes have been
apparent in theses outbreaks
Transmission has been
predominantly heterosexual
Males have outnumbered females
by ratios of 3:1 to 25:1
CSW have been important in
transmission of the infection
Chancroid has been strongly
associated with illicit drug use
Clinical Manifestation
o Break in the epithelium during sexual
contact with an infected individual
o Incubation period of 4-7 days
The initial lesion a papule with
surrounding erythema
o Papule evolves into a pustule - ruptures
and form a sharply circumscribed ulcer that
is generally not indurated
o Ulcers are painful and bleed easily
o Develop enlarged, tender inguinal lymph
nodes fluctuant and spontaneously
rupture
o Patients usually seek medical care after 1-3
weeks of painful symptoms
o Clinical picture can be confused with that of
lymphogranuloma venerum
o DDx: primary syphilis, conyloma latum of
secondary symphilis, genital herpes and
donovanosis
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART1
DR. FAJARDO
F. LEGIONELLA INFECTION
- Legionella pneumophila
o Aerobic gram-negative bacilli, do not grow
on routine microbiologic media
o 80-90% of human infections
o Direct fluorescent antibody (DFA) for
diagnosis
Diagnosis
o Clinical diagnosis often inaccurate
o Gram staining of a swab of the lesion may
reveal a predominance of characteristic
gram-negative coccobacilli
o An accurate diagnosis of chancroid relies on
culture of H. ducreyi from the lesion
o Aspiration of culture of suppurative lymph
nodes
Treatment
o Azithromycin 1g SD
o Alternative regimens include
Ceftriaxone 250mg IM SD
Ciprofloxacin 500mgvBID for 3
days
Erythromycin 500mg TID for 7 days
Contact of patients identified and treated
Sexual contact with the patient
during the 10 days preceding
thepatients onset of symptoms
Ecology
Aquatic bodies, lakes and streams
Grow and proliferate in human
constructed aquatic reservoir
Factors known to enhance
colonization
Warm temp, stagnation,
scale and sediment
From microcolonies and biofilms
Transmission
Source - water
Aerosolization, aspiration and
direct instillation in to the lungs
during respiratory tract
manipulation
Aspiration predominant
mode of transmission
Aerosolization by devices
filled with tap water,
including nebulizers and
humidifiers
Legionnaires Disease
o atypical pneumonia
Diarrhea
High fever - >40C
Numerous neutrophils but no
organisms revealed by GS of
respiratory secretions
Hyponatremia
Failure to respond to B-lactams
and aminoglycoside antibiotics
Occurrence of illness in an
environment where water is
contaminated with Legionella
Onset of symptoms 10 days after
discharge from hospital
o
Treatment
Macrolides
MEDICINE 2:
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART1
DR. FAJARDO
Azithromycin
Clarithromycin
Quinolones
Tetracycline
TMP-SMX
*Empiric treatment for CAP B lactam + macrolide or
quinolone
G. PERTUSSIS
- Bordetella pertussis
- Acute infection of the respiratory tract
- whooping cough inspiratory sound made at the
end of an episode of paroxysmal coughing
- Uncommon in infants <6 months and frequently
absent in older children and adults
- Gram negative pleomorphic and aerobic bacilli
- Produces a wide array of toxins and biologically
active products
o Pertussis toxin most important virulence
factor
Epidemiology
- Highly communicable disease
o Attack rate 80-100% among unimmunized
household contacts
o 20% within households in well-immunized
populations
Clinical Manifestations
- Catarrhal phase
o Coryza, lacrimation, mild cough, low-grade
fever, malaise
o Last 1-2 weeks
-
Paroxysmal phase
o Cough becomes more frequent and
spasmodic
o Repetitive bursts of 5-10 coughs within a
single expiration, audible whoop
o Lasts 2-4 weeks
Convalescent phase
o Last from 1-3 months
o Gradual resolution of coughing episodes
o Intercurrent viral infections associated
with recrudescence of paroxysmal cough
Complications
- Subconjunctival haemorrhages, abdominal and
inguinal hernias, pneumothorax, facial and truncal
petechiae
o Increase intrathoracic pressure severe fits
of coughing
Diagnosis
- Classic symptoms of pertussis
Laboratory confirmation
o Lymphocytosis common among young
children
o Gold standard culture of nasopharyngeal
secretions/aspiration
Media: Bordet-Gengou or ReganLowe
Treatment
- Antibiotics
o Eradicate infecting bacteria from the
nasopharynx
Does not alter clinical course
unless given early in the catarrhal
phase
o DOC: Macrolides
TMP-SMX
- Chemoprophylaxis household contacts
o Erythromycin
- Immunization
o Mainstay of pertussis infection
o Lifelong immunity after natural infection
DISEASES CAUSED BY GRAM NEGATIVE ENTERIC BACTERIA
- Enterobacteriaceae
o Escherichia
o Klebsiella
o Proteus
o Enterobacter
o Serratia
o Citrobacter
o Morganella
o Providencia
o Edwardsiella
o Salmonella
o Acinetobacter
o Pseudomonas
A. E. COLI AS AN INTESINAL PATHOGEN
- Pathogenic strains rarely encountered in the fecal
flora of healthy hosts
o Obligate pathogens
- Enteritis, enterocolitis and colitis
- Feco-oral route
- Transmission
o Contaminated food andwater
o Person to person spread
- Commensal strains
o Normal facultative intestinal flora in most
humans
o Lack specialized virulence traits
o May be involved in extraintesinal infections
Presence of aggravating factors
foreign body, functional or
anatomic abnormalities,
immunocompromised states, fecal
contamination of the peritoneum
MEDICINE 2:
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART1
DR. FAJARDO
B.KLEBSIELLA INFECTION
Extraintestinal Pathogenic Strains (EXPEC)
- Infections in the urinary tract, bloodstream, CSF,
respiratory tract, peritoneum
- Surgical and wound infections, osteomyelitis and
myositis
Urinary Tract Infection
- Most frequent site infected by EXPEC
- E. coli single most prevalent pathogen for all UTI
- Most common source of E. coli bacteremia
- Uncomplicated cystitis/urethritis most common
o Dysuria, frequency and suprapubicpain
- Pyelonephritis
o Fever, costovertebral tenderness, nausea
and vomiting
- Abdominal and pelvic infections
o Second most frequent site of extraintestinal
infection due to E.coli
o Acute peritonitis secondary to fecal
contamination, spontaneous bacterial
peritonitis, diverticulitis, appendicitis,
intraperitoneal abscesses, cholangitis
Pneumonia
- E. coli is not a usual pathogen
- Long term care facilities
o GNB common cause of pneumonia
60-70% of hospital acquired
pneumonia
Meningitis
- E. coli one of the 2 leading cause of neonatal
meningitis
o Group B streptococcus
- Strains posses K1 capsular serotype
- Uncommon in older children and adults
o Disruption of meninges due to craniotomy
or trauma, in the presence of cirrhosis
Treatment
- Highly susceptible to antibiotics
- Increasing frequency of ampicillin resistance
o Precludes its empiric use in community
acquired infections
st
- Increasing rates of resistance to 1 generation
cephalosporinsand TMP-SMX
- TMP-SMX DOC for uncomplicated cystitis
- Resistance to B-lactam/BLI: 30-40%
- Rates of resistance to cephalosporins (2nd, 3rd, 4th
gen), quinolones, monobactam, quinolone and
aminoglycosides: <10%
- Acquisition of plasmid containing ESBLs (extendedspectrum beta lactamases)
o DOC: Carbapenem
K. pneumonia most important
o Community acquired, long term care
nosocomial infections
o Colonizes the colon 5-35%, oropharynx
1-5%
K. rhinoscleromatis and K. ozonae tropical climates
o Rhinoscleroma
o Chronic atrophic rhinitis
Clinical syndrome
o Klebsiella causes a variety of clinical
syndromes
Community acquired pneumonia
UTI
Nosocomial infection
Rhinoscleroma and ozena
Colonization
Community Acquired Pneumonia
- Associated with destructive changes in the lungs
- Severe illness with a rapid onset and often-fatal
outcome
- Clinical manifestations
o Acute onset of high fever and chills; flu like
symptoms; and productive cough with an
abundant, thick, tenacious and blood tinged
sputum sometimes called currant jelly
sputum
- Increased tendency for abscess formation,
cavitation, empyema and pleural adhesions
- Community acquired Klebsiella (Friedlander)
pneumonia disease of debilitated middle-aged and
older men with alcoholism
Urinary Tract Infection
- Clinically indistinguishable from UTIs caused by other
common organism
- Clinical manifestations
o Frequency, urgency, dysuria, hesitancy, low
back pain, and suprapubic discomfort
o Systemic symptoms such as fever and chills
are usually indicative of a concomitant
pyelonephritis or prostatitis
- Incidence among healthy adults 1-2%
- Complicated UTIs -5-17%
o Indwelling catheters, diabetics, anatomic
and functional abnormalities
Nosocomial Infections
- Important manifestations in the hospital setting
o UTI, pneumonia, bacteremia, wound
infection, cholecystitis and catheterassociated bacteriuria
Rhinoscleroma
- Chronic granulomatous infection of the upper
respiratory tract
MEDICINE 2:
Present with a purulent nasal discharge
with crusting and nodule formation that
leads to respiratory obstruction
Diagnosis is aided by histology findings and
positive results from blood culture
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART1
DR. FAJARDO
UTI
-
Ozena
- K. ozenae
- Primary atrophic rhinitis that often occurs in elderly
persons
- Common symptoms
o Nasal congestion and a constant nasal bad
smell
o Headache
Treatment
- Severely ill patients
o Third-generation cephalosporins,
carbapenems, aminoglycosides and
quinolones
o Intrinsically resistant to ampicillin and
ticarcillin
- Extended Spectrum Beta Lactamases (ESBL)producing strains DOC: carbapenems
C. PROTEUS INFECTION
- Proteus organisms are implicated as serious causes
of infections in humans
- Normal human intestinal flora
- Multiple environmental habitat, including long term
care facilities and hospitals
o Colonize both the skin and oral mucosa of
both patients and hospital personnel
Proteus mirabilis
- 90% of proteus infections
- Community acquired infection
- Urease production + presence of bacterial motility
and fimrbiae favors the production of upper
urinary tract infections
Risk factors
- Recurrent infections
- Structural abnormalities of the urinary tract
- Urethral instrumentation
Pathophysiology
- Proteus organisms produce urease and able to
alkalinize the urine by hydrolyzing urea to ammonia
o Leads to precipitation of organic and
inorganic compounds struvite stone
formation
Composed of a combination of
magnesium ammonium
phosphate(struvite) and calcium
carbonate - apatite
Urethritis, cystitis, prostatitis or pyelonephrits
Chronic recurrent stones may be an indication of
chronic infection
Women present with dysuria, pyuria and increased
frequency of urination
Presenting symptoms in males are usually mild,
urethral discharge
Prostatitis occurs more acutely than cystitis
o More common as men age
o Fever and chills
o Perianal pain and various symptoms of
urinary obstruction may be present
o Prostate may be tender and diffusely
swollen
Pyelonephritis progression of disease
o Symptoms are more profound
o Sepsis develops quickly elderly patients or
immunocompromised
o Flank pain, nausea and vomiting,
costovertebral tenderness and fever
o Palpable and tender kidney
o Hematuria and pyuria
Other infections
- Pneumonia
- Nosocomial sinusitis
- Intraabdominal abscesses
- Biliary tract infection
- Surgical site infection
- Soft tissue infection (decubitus and diabetic ulcers)
- Osteomyelitis (primarily contiguous)
Treatment
- Uncomplicated UTIs in women
o Oral quinolone for 3 days or
trimethoprim/sulfamethoxazole (TMP/SMZ)
for 3 days (OPD basis)
-
Acute uncomplicated pyelonephritis in women
o Oral quinolones for 7-14 days
o Single dose ceftriaxome or gentamicin IM
followed by TMP/SMZ
o Oral cephalosporin or quinolone for 14 days
For hospitalized patients
o Parenteral ceftriaxone, quinolone,
gentamicin (plus ampicillin), or azteronam
until defervescence
o Oral quinolone, cephalosporin, or TMP/SMZ
for 14 days may be added to complete
treatment
D. ENTEROBACTER INFECTIONS
- Enterobacter cloacae and E. aerogenes
o Important community-acquired and
nosocomial pathogens
MEDICINE 2:
Community-acquired infections
o UTIs, skin and soft tissue infections, and
wound infections
Enterobacter species possess inducible B-lactamases
o ESBL
o Undetectable in vitro but are responsible
for resistance during treatment
Treatment
o Significant antimicrobial resistance exists
o Ampicillin and 1st and 2nd gen
cephalosporins have little or no activity
rd th
o Extensive use of 3 -4 gen cephalosporins,
monobactams, B-lactam/B-lactamase
inhibitor
Production of high levels of betalactamases
o Imipenem, cefepime, , aminoglycosides,
TMP-SMX, Fluoroquinolones
Retained excellent activity (9099%)
E. ACINETOBACTER INFECTIONS
- A. baumannii
- Highly prevalent in the environment
- Increased colonization of the skin, respiratory and
GIT
o Individuals in long-term care facilities and
hospitals
Infectious syndromes
- Respiratory tract (ventilated patients)
- Intravascular devices
- Severe CAP uncommon
o Affects compromised hosts alcoholics
- Infections of catheterized urinary tract, post-op sites,
burn sites, biliary stents and sinuses
Treatment
- Many strains highly resistant to antimicrobial
agents
- Empiric combination
- Ampicillin, aztreonam, 1st-2nd gen cephalosporin
little or no activity
- Resistance rates: 20-50%
o Piperacillin, quinolones, 3rd gen
cephalosporin, gentamicin
- Imipenem most active agent (>95%)
- BL/BLI, cefepime, amikacin
F. SERRATIA INFECTIONS
- S. marcescens - >90% of infections
- Primarily seen in the environment - moist foci
- Healthy humans rarely colonized
- Reservoirs 0 HCW, food, milk in neonatal units, sink,
respiratory and other hospital equipment
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART1
DR. FAJARDO
Serratias sp account for 1-3% of hospital acquired
infections
Infectious syndromes
- Respiratory, genitourinary tracts, intravascular
devices , surgical wounds
- Soft tissue infections (myositis, osteomyelitis),
abdominal and biliary tract
infections(postprocedural), contact lens associated
keratitis, endophthalmitis, septic arthritis, infusion
related bacteremias less common
Treatment
st
- >80% of strains resistant to ampicillin and 1 gen
cephalosporins
- >90% of isolates are susceptible to other GNBappropriate antibiotics
G. CITROBACTER INFECTIONS
- C. freundii and C. koseri majority of human
infections
- Epidemiologically and clinically similar to
Enterobacter and Acinetobacter infections
- Present in water, food, soil and intestinal tract of
animals
- Colonization increasing in long term care facilities
and hospitals
- Citrobacter species account for 1-2% of nosocomial
infections
Infectious Syndromes
- Urinary tract most common site of infection (4050%)
- Less commonly infected sites
o Biliary tree, respiratory tract, surgical site,
soft tissue, peritoneum, intravascular
devices
- Uncommon cause of neonatal meningitis
o C. koseri 90% of cases
Complication brain abscess (5080%)
Treatment
- C. freundii is more resistant to antibiotics than C.
koseri
st
- Poor activity of ampicillin and 1 gen cephalosporin
- >90% of isolates are susceptible to other Gram
negative Bacteria -appropriate antibiotics
H. PSEUDOMONAS INFECTIONS
aerobic, gram negative bacterium of relatively low
virulence
- Ubiquitous with a predilection to moist
environments, primarily as waterborne and
soilborne organisms
- Pseudomonas aeruginosa colonization
>50% of humans
MEDICINE 2:
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART1
DR. FAJARDO
P aeruginosa is the most common
pseudomonal species
Clinically significant and opportunistic pathogen
nosocomial infections
serious and often life-threatening
diseases
exhibit innate resistance to many antibiotics and can
develop new resistance after exposure to
antimicrobial agents
Pseudomonas aeruginosa
Pseudomonal pneumonia
o associated with mortality that occurs 34 days after the first signs or
symptoms of
pulmonary or
extrapulmonary infections
Ventilator-associated pneumonia (VAP) caused by
P. aeruginosa is associated with higher mortality
rates as high as 60% than VAPs caused by other
infectious organisms
Clinical syndromes
AIDS-related infections
Bacteremia and sepsis
Febrile neutropenia*
bone and joint infection
o (e.g. osteochondritis, osteomyelitis,
pyarthrosis)
CNS infection
o ( e.g. brain abscess, meningitis)
Ear infections
o (e.g. otitis media, chronic suppurative otitis
media, otitis externa, malignant external
otitis or swimmers itch*)
Eye infections*
o (e.g. endophthalmitis, keratitis, opthalmia
neonatorum, blepharoconjunctivitis, scleral
abscess, orbital cellulitis)
GI infections
o (e.g. epidemic diarrhea, NEC, typhitis, rectal
abscess, shanghai fever)
Cardiovascular (CV) infections
o (e.g. endocarditis, pericarditis, cardiac
tamponade)
Respiratory infections esp VAP*
o (e.g. primary or nonbacteremic, bactermic,
colonization, and nosocomial pneumonia,
lower respiratory tract infections of CF,
VAP)
Skin and soft tissue infections
o (e.g. burn wound sepsis, dermatitis,
Ecthyma Gangrenosum, pyoderma, surgical
and wound infections, including cellulitis,
hot tub folliculitis, necrotizing fasciitis,
chronic paronychia)
*Cystic fibrosis almost always associated with pseudomonal
infections**
*Ecthyma gangrenosum is a rare but pathognomonic form of
pseudomonal infection
Pseudomonas cepacia
- now known as Burkholderia cepacia
first reported as a human pathogen that caused
endocarditis**
- catheter-associated UTIs, wound infections, and IV catheterassociated bacteremias
Pseudomonas mallei
- now known as Burkholderia mallei
causes glanders (primary equine infection)- a serious
infectious disease of animals, primarily horses
- Transmission direct contact
- Glanders transmission to humans
rare and presumably occurs through inoculation of
broken skin or the nasal mucosa with contaminated
discharges
- manifestation of the glanders in humans
acute localized suppurative infection
acute pulmonary infection
acute septicemic infection to chronic suppurative
infections
fulminant disease with multiple organ system
involvement occurs with septicemic infection
Pseudomonas pseudomallei
- now known as Burkholderia pseudomallei
causes melioidosis (Whitmore disease)
clinically and pathologically resembles glanders but
has an entirely different epidemiologic profile from
B. mallei
- Transmission direct contact
inhalation possible route of acquisition
- Pathogen spreads to humans and animals
direct contact with a contaminated source
- *can cause brain, pulmonary and GI abcesses
- *worse than glanders
- In healthy hosts
disease manifestations range from acute to chronic
local suppurative infections to septicemia with
multiple abscesses in all organs of the body
Treatment
- Antimicrobial agents are needed to treat Pseudomonas
infection
two antipseudomonal drug combination therapy
(e.g. a beta lactam antibiotics with aminoglycoside)
neutropenia, bacteremia, sepsis, severe URIs, or
abscess formation
*antipseudomonal activity cephalosporin- Cefatidime
*4th gen ceph Cefipime (good antipseudomonal activity)
*Aminoglycoside gentamicin, Amikacin
*carbapenems
10
MEDICINE 2:
*betalactam-betalactamase inhibitors Piperacillintazobactam, ticarcillin-clavulanic acid
-B. cepacia
resistant to aminoglycosides, antipseudomonal
penicillins, and most beta lactam agents
variably susceptible to third-generation
cephalosporins, ciprofloxacin, trimethoprimsulfamethoxazole, ampicillin-sulbactam,
chloramphenicol, or meropenem
*quinolones esp Ciprofloxacin = good anti
pseudomonal activity
-B. pseudomallei
DOC: Ceftazidime +/- TMP-SMX or amoxicillin
clavulanate
Sensitive to imipenem, PCN, doxycycline, azlocillin,
ceftazidime, ticarcillin-clavulanic acid, and
ceftriaxone
Initiate treatment early in the course of the disease
The organism is resistant to ciprofloxacin and
aztreonam
3-12 months with the longest duration of therapy
used for chronic extrapulmonary disease
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART1
DR. FAJARDO
11
MEDICINE 2:
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART2
DR. FAJARDO
ENTERIC GRAM NEGATIVE INFECTIONS
-
Organisms that are pathogens of the GIT tract
o We have normal colonic flora, does not
cause disease if does not go out the colon
Organisms that causes diseases/GI infections
o Salmonella
o Shigella
o Campylobacter
o Cholera
SALMONELLA
Based on DNA studies
o 2 species:
a. Salmonella enteric
b. Salmonella gongori
Salmonella typhi and paratyphi- part of salmonella 1
subspecie
o Salmonella enteric 1 subspecie serotype
typhi S. Typhi
o Only these 2 are pathogenic to human
Pathogenesis
- Ingestion of organism via contaminated food and
water
organism invades the GIT tract
- Multiply in the mononuclear phagocytic cells in
Spleen, liver, and Peyers patches in terminal ileum
o Abdominal pain due to Infiltration in the
Peyers patches
Risk factors:
- Decrease stomach acidity
o Age <1 yr old, antacid ingestion, achlorydic
diseases
- Decrease intestinal integrity
o Problem in the GI mucosa
o IBD, prior GI surgery, anitiotic administration
(kill the normal flora)
Clinical Manifestations:
ENTERIC (TYPHOID) FEVER
- Incubation period: 10- 14 days (3 21 days)
- Most prominent symptom: prolonged fever (38.8 C
40.5 C), until for weeks if untreated
-
Prospective study of 669 cases (Nepal)
o Headache (80%)
o Chills (35 45%)
o Cough (30%)
o Sweating, myalgia, malaise, arthralgia
o GI symptoms: anorexia (55%), abdominal
pain (40%), nausea and vomiting, diarrhea,
constipation
Chronic Carrier State
- Have the organism in the body but does not cause
the disease
o Often seen in gallbladder (stones)
Stool carriage is more frequent in people with preexisting biliary abnormality
S. enteric survives in gallstones: greater incidence of
cholecystitis
Greater risk for carcinoma of the gallbladder and
other GI malignancies
Chronic inflammation cause by bacteria
Diagnosis:
- Clinical presentation relatively non-specific
- Considered in any febrile traveler returning from a
developing country
- Gold standard culture positive for S. typhi or S.
paratyphoid
- Blood Culture and sensitivity 90% positive in the
first week of infection, 50% in the 3rd week
- BMA (bone marrow aspiration) remain highly
sensitive (90%) despite >5 days of Antibiotic
treatment
Treatment:
- Empiric treatment: (if still do not know if it is
salmonella or not)
o Ceftriaxone 1-2g/day (7-14 days)
o Azithromycin 1g/day (5 days)
- If fully susceptible
o Ciprofloxacin 500mg bid po, or 400mg every
12 h IV (5 7 days)
o Amoxicillin 1gram tid (14 days)
o Chloramphenicol 25mg/kg tid (14-21 days)
o TMP-SMZ 800mg
- Multi-drug resistant
o Ciprofloxacin 500mg bid po, or 400mg every
12h IV (5-7 days)
o Ceftriaxone 2-3g / day (7-14 days)
o Azithromycin 1g/day (5 days)
- Nalidixic acid resistant
o Same with multidrug resistant
Prevention
- Typhoid vaccines
o Ty 21 day, Oral live attenuated S. typhi
vaccine (given on days 1, 3, 5, 7 with booster
every 5 years)
o Vi CPS, purified Vi polysaccharide from
bacterial capsule (given in 1 dose with
booster of every 2 years)
NON-TYPHOIDAL SALMONELLOSIS (NTS)
- Serotypes: typhi murium, enteritidis
- Minor infections
- Highest rates of morbidity and mortality:
o Elderly
o Infants
o Immunocompromised
-
NTS can b acquired from animal reservoirs
MEDICINE 2:
Transmission associated with animal food products
(eggs, poultry)
Increase antibiotic drug resistant: due to antibiotic
use in animal foods
Clinical Manifestations:
- Gastroenteritis
o Nausea and vomiting, diarrhea occurs in 68 hours
- Bacteremia and endovascular infections
- Localized infections
o Hepatic splenic abscess, UTI, meningitis,
infectons in the bones
Diagnosis
- High index of suspicion - prolonged or recurrent
fever
- Isolation of organism
o Blood, stool, sterile body fluids
- Echocardiography
- CT scan/ MRI
o Intra-abdominal abscess, bone and joint
involvement
Treatment
- Increasingly prevalence of antibiotic resoistance
o Life threatening NTS bacteremia or focal NTS
infection
o 3rd gen. Cephalosporin, Fluoroquinolone
o Given 7 -14 days
- Patient with AIDS and NTS bacteremia
o 1-2 weeks of IV antibiotic followed by 4
weeks of oral therapy Fluoro
o Relapse give long term suppression therapy
of cotrimoxazole or fluoroquinolones
(indefinite time: 3-6 months)
SHIGELLA (SHIGELLOSIS)
Shugella dysenteriae, S. flexneri, S. boydii, S. sonnei
o MC species that cause human infection
Shigella dysenteriae type 1 etiologic agent of
dysentery
o Produces Shiga toxin (cytotoxin)
o Fecal oral route
o Some: water-borne transmission
Pathogenesis
- Resistance to low pH condition allows Shigella to
survive through the gastric barrier
- Small inoculum ( as few as 100 CFU) is sufficient to
cause infection
- Watery diarrhea that precedes the dysenteric
syndrome is attributable to active secretion and
abnormal water reabsorption
o Enterotoxin (SHET-1) and mucosal
inflammation
-
Invasion of the mucosa manifested by bloody and
mucopurulent stools dysenteric syndrome
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART2
DR. FAJARDO
Clinical Manifestation
- Shigellosis typically evolves through 4 phases
o Incubation period (non specific), watery
diarrhea, dysentery,post infectious
a.
Incubation Period
o Last about 1-4 days, but maybe as long as 8
days
o Typically, initial manifestations are transient
fever, limited watery diarrhea, malaise and
anorexia
o S/Sx may change from mild abdominal
discomfort to severe cramp
o Tenesmus
b.
Dysentery follows within hours or days
o Chaaracterized by uninterrupted excretion of
small volume of bloody mucopurulent stools
with increase tenesmus and abdominal
cramp
o Produce acute colitis involving distal colon
and rectum
o Unlike most diarrheal syndrome dysenteric
syndrome rarely present with DHN as major
feature
o Most episodes are Self-limited, result
without treatment within 1 week;
o if with appropriate treatment
resolves/recovery within few days-week
without sequelae
Complications:
o Toxic megacolon and Hemolytic Uremic
Syndrome
o
Toxic megacolon
is a consequence of severe
inflammation extending to the
colonic smooth muscle layer and
causing paralysis and dilatation
The patient present with abdominal
distention and tenderness with or
withput signs of localized or
generalized peritonitis
Predisposing factors:
Hypokalemia
Paralytic ileus
Opiods
Anti-cholinergic
Do not give anti diarrheal
meds
HUS
Is an early complication that most
often develop after several days of
diarrhea
MEDICINE 2:
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART2
DR. FAJARDO
Clinical examination shows pallor,
asthenia and irritability;
in some cases, bleeding of the nose
and gums, oliguria and increasing
edema, increase creatinine
HUS nonimmune (Coombs Test
negative) hemolytic anemia
designed by diagnostic triad
Microangiopathic
hemolytic anemia hgb
level <80g/L
Thrombocytopenia (mild to
moderate)
Acute renal failure due to
thrombosis of glomerular
capillaries (marked
increase of creatinine
levels)
Lab. Dx
- Gold standard for diagnosis of shigella infection
remains the isolation and identification of the
pathogen from fecal material (stool Culture)
- Blood Culture positive in less than 5% of cases
(only done in severe sepsis)
Treatment
- First line
o Ciprofloxacin 500mg 1 cap bid x 3 days
- 2nd line
o Ceftriaxone
o Azithromycin
CAMPYLOBACTER INFECTIONS
Campylobacters are found in the GI tract of many
animals use for food
o Including poultry, cattle, shhep, and swine
o Also seen in household pets (dogs, cats)
Other mode of transmission
o Ingestion of raw (unpasteurized) milk or
untreated water
o Contact with infected household animals
o Travelling to developing countries
Clinical Manifestation
Campylobacter jejuni
- C. jejuni infections may be subclinical
o In host who have had multiple prior
infections and are partially immnune
- Symptomatic infections mostly occur within 2-4
days of exposure (range 1-7 days)
- Site of tissue injury: mostly in jejunum, but can have
infection in ileum and colon
- A prevalence of fever. Headache, myalgia and /or
malaise often occur 12 48 hours before the onset
of diarrheal symptom
The MC s/sx of the intestinal phase are diarrhea,
abdominal pain and fever
o Degree of diarrhea varies from several loose
stools to grossly bloody stools
o Abdominal pain usually consists of cramping
and may be the most prominent symptom
Generalized but may become
localized
C. jejuni infection may cause
pseudoappendicitis (mimic
appendicitis)
o Fever in some, it is the only manifestation
of the disease, can mimic typhoid fever
Campylobacter enteritis
- Is generally self-limited
o But Symptoms may persist for > 1 week
Diagnosis
- Confirmation of diagnosis is based on the
identification of an isolate from culture of stool,
blood, or another site
- Campylobacter specific media should be used to
culture stool
Treatment
- Fluid and Electrolyte is central to the treatment of
diarrheal illness
- Even among patients presenting for medical
attention with campylobacter enteritis, not all will
clearly benefit from specific antibiotics
- Patients that will benefit from antibiotics:
(indications for antibiotics)
o High grade fever
o Bloody diarrhea
o Persistence for more than 1 week
o Worsening symptoms
-
DOC: 5-7 day course of Erythromycin (250mg QID PO
for children, 30- 50 mg/kg/day in divided dose)
Azithromycin ( a 1 or 3 day regimen)
Ciprofloxacin
*antidiarrheal agents: be careful in giving campylobacter
infection may also be associated with toxic megacolon and
HUS
CHOLERA INFECTIONS
Acute diarrheal disease that can result in profound,
rapidly progressing Dehydration and death
Cholera gravis severe form
o Caused by Vibrio cholera serogroup O1 or
O139
Toxin-mediated disease
o In small intestine: toxin-coregulated pilus its synthesis is regulated in parallel with that
of cholera toxin
MEDICINE 2:
Pathogenesis
- Cholera is a toxin mediated disease
- The watery diarrhea characteristic of cholera is due
to action of cholera toxin
o Potent protein enterotoxin elaborated by the
organism in the SI
o In small intestine: toxin-coregulated pilus its synthesis is regulated in parallel with that
of cholera toxin also enable the organism
to survive in the SI
Clinical Manifestations:
- Asymptomatic or have only mild diarrhea
- Sudden onset of explosive and life-threatening
diarrhea (cholera gravis)
- After a 24 48 hours incubation period begins with
sudden onset of painless watery diarrhea that may
quickly become voluminous
- Patient often vomits
- The stool has a characteristic appearance
o nonbilious, gray, slightly cloudy, fluid with
flecks of mucoid, no blood and somewhat
fishy, inoffensive odor
- Clinical symptoms parallel volume contraction:
o At losses of <5% of normal body weight,
thirst develops;
o at 510%, postural hypotension, weakness,
tachycardia, and decreased skin turgor are
documented; and
o at >10%, oliguria, weak or absent pulses,
sunken eyes (and, in infants, sunken
fontanelles), wrinkled ("washerwoman")
skin, somnolence, and coma are
characteristic.
- Complications derive exclusively from the effects of
volume and electrolyte depletion and include renal
failure due to acute tubular necrosis.
- if the patient is adequately treated with fluid and
electrolytes, complications are averted and the
process is self-limited, resolving in a few days.
Diagnosis
- The clinical suspicion of cholera can be confirmed by
the identification of V. cholerae in stool
- Laboratory isolation of the organism requires the use
of a selective medium such as taurocholate-telluritegelatin (TTG) agar or thiosulfatecitratebile salts
sucrose (TCBS) agar
- If a delay in sample processing is expected, CareyBlair transport medium and/or alkaline-peptone
water-enrichment medium may be used
- Standard microbiologic biochemical testing for
Enterobacteriaceae will suffice for identification of
V. cholerae. All vibrios are oxidase-positive.
Treatment
- Death from cholera is due to hypovolemic shock;
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART2
DR. FAJARDO
first and foremost requires fluid resuscitation
and management
level of dehydration, the patient's age and weight euvolemia should first be rapidly restored, and
adequate hydration should then be maintained to
replace ongoing fluid losses
Administration of oral rehydration solution (ORS)
takes advantage of the hexose-Na+ co-transport
mechanism to move Na+ across the gut mucosa
together with an actively transported molecule such
as glucose (or galactose).
Cl and water follow.
This transport mechanism remains intact even when
cholera toxin is active.
o
ORS may be made by adding safe water to
prepackaged sachets containing salts and sugar; or
0.5 teaspoon of table salt (NaCl; 3.5 g) and 4
tablespoons of table sugar (glucose; 40 g) to 1 L of
suspension
ORS can be administered via a nasogastric tube to
individuals who cannot ingest fluid
total fluid deficit in severely dehydrated patients
(>10% of body weight)
o replaced safely within the first 36 h of
therapy, half within the first hour.
Transient muscle cramps and tetany are common.
oral therapy can usually be initiated, with the goal of
maintaining fluid intake equal to fluid output
Antibiotics
- use of antibiotics diminishes the duration and
volume of fluid loss and hastens clearance of the
organism from the stool
- WHO recommends administration of antibiotics to
cholera patients only if they are severely
dehydrated,
- Doxycycline (a single dose of 300 mg) or
- tetracycline (12.5 mg/kg four times a day for 3 days)
may be effective in adults but is not recommended
for children <8 years of age because of possible
deposition in bone and developing teeth.
For nonpregnant adults with cholera in areas where
tetracycline resistance is prevalent
o ciprofloxacin [either in a single dose (30
mg/kg, not to exceed a total dose of 1 g) or
in a short course (15 mg/kg bid for 3 days,
not to exceed a total daily dose of 1 g)],
o erythromycin (4050 mg/kg daily in three
divided doses for 3 days),
o azithromycin (a single 1-g dose) may be a
clinically effective substitute.
- Pregnant women and children are usually treated
with erythromycin or azithromycin (10 mg/kg in
children).
MEDICINE 2:
DISEASES CAUSED BY GRAM NEGATIVE BACTERIA PART2
DR. FAJARDO
Prevention
- Provision of safe water and facilities for sanitary
disposal of feces, improved nutrition, and attention
to food preparation and storage in the household
can significantly reduce the incidence of cholera
- Oral cholera vaccines
NON-CHOLERA VIBRIOSES
NONCHOLERA VIBRIOSES
ORGANISM
VEHICLE
OR
ACTIVITY
V.
Shellfish,
parahaemolyti seawater
cus
seawater
Non- O1/O139
V. cholerae
V. vulnificus
V. alginolyticus
HOST AT RISK
SYNDROME
Normal
Gastroenteri
tis
Normal
Wound
infection
Gastroenteri
tis
Wound
infection,
otitis media
Sepsis,
secondary
cellulitis
Wound
infection,
cellulitis
Wound
infection,
cellulitis,
otitis media
sepsis
Shellfish,
travel
Seawate
r
Normal
shellfish
immunosuppre
ssed
seawater
Normal,
immunosuppre
ssed
Normal
seawater
seawater
Normal
Burned, other
immunosuppre
ssed
Вам также может понравиться
- 911 Pigeon Disease & Treatment Protocols!От Everand911 Pigeon Disease & Treatment Protocols!Рейтинг: 4 из 5 звезд4/5 (1)
- 5 Mikrobiologi (Dr. Enny S, M.kes)Документ115 страниц5 Mikrobiologi (Dr. Enny S, M.kes)fitkaОценок пока нет
- Medical Mnemonic Sketches : Pulmonary DiseasesОт EverandMedical Mnemonic Sketches : Pulmonary DiseasesОценок пока нет
- Anesthesia For Tonsillectomy: Aau-Chs School of AnesthesiaДокумент54 страницыAnesthesia For Tonsillectomy: Aau-Chs School of AnesthesiaagatakassaОценок пока нет
- Infection of Nose, Sinus and EarДокумент18 страницInfection of Nose, Sinus and EarMuhammad FadlilahОценок пока нет
- Pulmonary PathologyДокумент134 страницыPulmonary PathologyFor ChristОценок пока нет
- Pathophysiology of Respiratory SystemДокумент9 страницPathophysiology of Respiratory SystemArumi HamasakiОценок пока нет
- Maxillofacial - Infection - Dari KikiDrДокумент20 страницMaxillofacial - Infection - Dari KikiDrmashitadyahОценок пока нет
- Otitis ExternaДокумент19 страницOtitis ExternaEren YooОценок пока нет
- Bacterial Causes of URIДокумент28 страницBacterial Causes of URIOmar MohammedОценок пока нет
- Bacteria Infection of The Respiratory TractДокумент8 страницBacteria Infection of The Respiratory TractChidi EmmanuelОценок пока нет
- Clinical Microbiology (17 - 11)Документ8 страницClinical Microbiology (17 - 11)Arthur YanezОценок пока нет
- Adenotonsillar Diseases DrbugnahДокумент37 страницAdenotonsillar Diseases DrbugnahDr.Sherif Bugnah100% (8)
- Abscess of The Lung Current Therapeutic OptionsДокумент9 страницAbscess of The Lung Current Therapeutic OptionsTalat AksuОценок пока нет
- Normal FloraДокумент28 страницNormal FloraMuhammad KashifОценок пока нет
- Orofacial Infections in Children PedoДокумент40 страницOrofacial Infections in Children PedoFourthMolar.comОценок пока нет
- Airborne Transmission: Nurul Aqmar Mohd Nor Hazalin Phc454 - Pharmaceutical MicrobiologyДокумент27 страницAirborne Transmission: Nurul Aqmar Mohd Nor Hazalin Phc454 - Pharmaceutical MicrobiologySuhaila Abdul RahimОценок пока нет
- IVRSДокумент61 страницаIVRSAndrew ChinchillaОценок пока нет
- Etiology: M Tuberculosis Is A Slow-Growing, Obligate Aerobe and A Facultative, Intracellular Parasite. TheДокумент5 страницEtiology: M Tuberculosis Is A Slow-Growing, Obligate Aerobe and A Facultative, Intracellular Parasite. TheFerdi StefiyanОценок пока нет
- Unit X URTIДокумент37 страницUnit X URTIdiadiaidaОценок пока нет
- Anaerobic BacteriaДокумент52 страницыAnaerobic BacteriazaheerbinzubairОценок пока нет
- Chronic Suppurative Otitis MediaДокумент7 страницChronic Suppurative Otitis MediaMeis MalirmaseleОценок пока нет
- Anaerobic Bacteria: Dept. of Microbiology Medical Faculty, Padjadjaran UniversityДокумент52 страницыAnaerobic Bacteria: Dept. of Microbiology Medical Faculty, Padjadjaran UniversitySabrina Indri WardaniОценок пока нет
- 18 Tonsil, Adenoid Notes Cumming Abd Key Topics (New Moe)Документ7 страниц18 Tonsil, Adenoid Notes Cumming Abd Key Topics (New Moe)osamaeОценок пока нет
- 2 Microbial Disease of The Respiratory SystemДокумент63 страницы2 Microbial Disease of The Respiratory Systemrandom stuffОценок пока нет
- SinusitisДокумент44 страницыSinusitisAmosОценок пока нет
- 1.0 Upper Airway InfectionsДокумент45 страниц1.0 Upper Airway InfectionsMariahОценок пока нет
- Bacterial Infections of The Oral CavityДокумент212 страницBacterial Infections of The Oral CavitydrrakbdsОценок пока нет
- I.T.S Dental College, Greater Noida: Subject: Oral Pathology Lecture: Bacterial Infections:T BДокумент30 страницI.T.S Dental College, Greater Noida: Subject: Oral Pathology Lecture: Bacterial Infections:T BAMIT GUPTAОценок пока нет
- 2.oral Manifestation of Bacterial InfectionДокумент18 страниц2.oral Manifestation of Bacterial Infectionhesti_margarethaОценок пока нет
- Respiratory System DisordersДокумент9 страницRespiratory System Disordersasop06Оценок пока нет
- Normal Flora in Respiratory SystemДокумент2 страницыNormal Flora in Respiratory SystemJames Villanueva CalardeОценок пока нет
- Chronic Suppurative Otitis Media (CSOM)Документ31 страницаChronic Suppurative Otitis Media (CSOM)Mimo HemadОценок пока нет
- ENT Pathology: Assistan Professor Dr. Sazan Abdulwahab MirzaДокумент66 страницENT Pathology: Assistan Professor Dr. Sazan Abdulwahab MirzaMariam QaisОценок пока нет
- World's Largest Science, Technology & Medicine Open Access Book PublisherДокумент21 страницаWorld's Largest Science, Technology & Medicine Open Access Book PublisherStefana NanuОценок пока нет
- Mycotic InfectionДокумент22 страницыMycotic InfectionDevanshi Kulkarni100% (1)
- Pap0242 LabirinitisДокумент13 страницPap0242 LabirinitisPutri Andhini IzhmaОценок пока нет
- Mycotic Infectios of The Oral CavityДокумент45 страницMycotic Infectios of The Oral CavityoladunniОценок пока нет
- Lnfecciones Del Aparato Respiratorio SuperiorДокумент23 страницыLnfecciones Del Aparato Respiratorio Superiormonterrubio_jl2909Оценок пока нет
- Sinusitis 2000Документ7 страницSinusitis 2000GenaroMallquiОценок пока нет
- Matthew E. Levison: PneumoniaДокумент30 страницMatthew E. Levison: PneumoniaWira AisyaОценок пока нет
- Case Presentation - Acute Otits MediaДокумент31 страницаCase Presentation - Acute Otits MediaJean nicole Garibay0% (1)
- Rabbit DiseasesДокумент315 страницRabbit DiseasesABOHEMEED ALY100% (1)
- Upper Respiratory Tract Infections: DR John Egbagba FmcpathДокумент37 страницUpper Respiratory Tract Infections: DR John Egbagba FmcpathPrincewill SeiyefaОценок пока нет
- Online Learning ModuleДокумент38 страницOnline Learning ModuleMani SainiОценок пока нет
- Nugroho - A Rare Case of Primary Pulmonary Amoebiasis Without Gastrointestinal InvolvementДокумент5 страницNugroho - A Rare Case of Primary Pulmonary Amoebiasis Without Gastrointestinal InvolvementbernadinchynthiaОценок пока нет
- Laura A Goguen, MD Daniel G Deschler, MD, FACS Morven S Edwards, MD Howard Libman, MD Contributor Disclosures Peer Review ProcessДокумент4 страницыLaura A Goguen, MD Daniel G Deschler, MD, FACS Morven S Edwards, MD Howard Libman, MD Contributor Disclosures Peer Review ProcessDaniela Chavez DiazОценок пока нет
- Acute Suppurative Otitis MediaДокумент41 страницаAcute Suppurative Otitis Mediarani suwadjiОценок пока нет
- 9acutegingivalinfections Pdabscess 160503154630Документ141 страница9acutegingivalinfections Pdabscess 160503154630kishore KumarОценок пока нет
- The Pathology of Lung Diseases: I. Restrictive Lung Diseas ESДокумент65 страницThe Pathology of Lung Diseases: I. Restrictive Lung Diseas ESLiana Ika SuwandyОценок пока нет
- Sken 3 HoarseДокумент9 страницSken 3 HoarsearyaОценок пока нет
- Abses SubmandibularДокумент17 страницAbses Submandibularhoney_hannieОценок пока нет
- Drugs and Substance AbuseДокумент75 страницDrugs and Substance Abuseseline sherylОценок пока нет
- The Pathology of DiphtheriaДокумент5 страницThe Pathology of DiphtheriaKang KikiОценок пока нет
- Son OdtДокумент8 страницSon OdtAnonymous sV7PyHXbW5Оценок пока нет
- The Pharynx and Salivary GlandsДокумент21 страницаThe Pharynx and Salivary GlandsAce Ashley BaronОценок пока нет
- AdenotonsilitisДокумент42 страницыAdenotonsilitisELIA RICHARDОценок пока нет
- Principles of Management and Prevention of Odontogenic InfectionsДокумент167 страницPrinciples of Management and Prevention of Odontogenic InfectionsNur IbrahimОценок пока нет
- Otitis MediaДокумент31 страницаOtitis MediaManish AdhikariОценок пока нет
- CPD Act WordДокумент61 страницаCPD Act WordSigfred Tarnate Aoas100% (1)
- Exercise 6: Malarial Parasites: Parasitology LaboratoryДокумент2 страницыExercise 6: Malarial Parasites: Parasitology LaboratorySigfred Tarnate AoasОценок пока нет
- AutismДокумент3 страницыAutismSigfred Tarnate AoasОценок пока нет
- AutismДокумент3 страницыAutismSigfred Tarnate AoasОценок пока нет
- Banana Oil LabДокумент5 страницBanana Oil LabjbernayОценок пока нет
- Harry Potter and The Prisoner of Azkaban: Chapter 3-1 Owl PostДокумент20 страницHarry Potter and The Prisoner of Azkaban: Chapter 3-1 Owl PostodfasdОценок пока нет
- RPS Spare CatalogДокумент25 страницRPS Spare Catalogसुरेश चंद Suresh ChandОценок пока нет
- CWWДокумент2 страницыCWWmary joy martinОценок пока нет
- Partnership Liquidation May 13 C PDFДокумент3 страницыPartnership Liquidation May 13 C PDFElla AlmazanОценок пока нет
- KNOLL and HIERY, The German Colonial Experience - IntroДокумент6 страницKNOLL and HIERY, The German Colonial Experience - IntroGloria MUОценок пока нет
- Form A HypothesisДокумент2 страницыForm A Hypothesismrshong5bОценок пока нет
- Jacksonville's Taste 2012Документ100 страницJacksonville's Taste 2012Ali KhanОценок пока нет
- 00664-Hepting Excerpts of RecordДокумент240 страниц00664-Hepting Excerpts of RecordlegalmattersОценок пока нет
- All About Me - RubricДокумент3 страницыAll About Me - Rubricapi-314921155Оценок пока нет
- The Sacred Bee: Ancient Egypt: by Planet Bee FoundationДокумент4 страницыThe Sacred Bee: Ancient Egypt: by Planet Bee Foundationsoha elmahdyОценок пока нет
- EpitheliumДокумент48 страницEpitheliumdrpankaj28100% (1)
- Rehabilitation Major Repair of Permanent Bridges Bariis Br.Документ2 страницыRehabilitation Major Repair of Permanent Bridges Bariis Br.John Rheynor MayoОценок пока нет
- KodalyДокумент11 страницKodalySally Di Martino100% (3)
- Social Legislation Cases On Kasambahay LawДокумент12 страницSocial Legislation Cases On Kasambahay LawLiee Raine100% (1)
- Grade12 Rigel Group4 Assesing The Solid Waste Management Off Small Foos Store in Gingoog CityДокумент31 страницаGrade12 Rigel Group4 Assesing The Solid Waste Management Off Small Foos Store in Gingoog CityMa. Joan ApolinarОценок пока нет
- 2016 Biology CheckpointДокумент14 страниц2016 Biology CheckpointNicholas Leong100% (1)
- D2-S1 C Harmony in The Human Being July 23Документ20 страницD2-S1 C Harmony in The Human Being July 23padmaОценок пока нет
- Short-Term Memory and Working MemoryДокумент32 страницыShort-Term Memory and Working Memorysiempreviva84Оценок пока нет
- Resonant Excitation of Coherent Cerenkov Radiation in Dielectric Lined WaveguidesДокумент3 страницыResonant Excitation of Coherent Cerenkov Radiation in Dielectric Lined WaveguidesParticle Beam Physics LabОценок пока нет
- Syllabus Spring 2021Документ17 страницSyllabus Spring 2021Eden ParkОценок пока нет
- Rule 110 CasesДокумент102 страницыRule 110 Casesアブドゥルカリム エミールОценок пока нет
- Communique Supply Teacher (Oriental Languages) (Primary) 2021-2022Документ4 страницыCommunique Supply Teacher (Oriental Languages) (Primary) 2021-2022nishiОценок пока нет
- Exception Aggregation in Sap Bi PDFДокумент2 страницыException Aggregation in Sap Bi PDFPamela0% (1)
- 2202 Infantilization Essay - Quinn WilsonДокумент11 страниц2202 Infantilization Essay - Quinn Wilsonapi-283151250Оценок пока нет
- Frontpage: Don'T Befriend Brutal DictatorsДокумент16 страницFrontpage: Don'T Befriend Brutal DictatorsFrontPageAfricaОценок пока нет
- Term Coalition Has Been Derived From The Latin Word 'Coalitio' Which Means To Grow Up TogetherДокумент2 страницыTerm Coalition Has Been Derived From The Latin Word 'Coalitio' Which Means To Grow Up TogetherShree MishraОценок пока нет
- WLP Math Week 4 Q4Документ4 страницыWLP Math Week 4 Q4JUDELYN O. DOMINGOОценок пока нет
- Principle of ManagementsДокумент77 страницPrinciple of ManagementsJayson LucenaОценок пока нет
- Article WritingДокумент10 страницArticle WritingmutabargaybullayevnaОценок пока нет