Академический Документы
Профессиональный Документы
Культура Документы
BBA Clinical
Загружено:
Ayus diningsihОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
BBA Clinical
Загружено:
Ayus diningsihАвторское право:
Доступные форматы
BBA Clinical 4 (2015) 3541
Contents lists available at ScienceDirect
BBA Clinical
journal homepage: http://www.journals.elsevier.com/bba-clinical/
Heart-type fatty acid binding protein and high-sensitivity troponin T are
myocardial damage markers that could predict adverse clinical outcomes
in patients with peripheral artery disease
Yoichiro Otaki, Hiroki Takahashi, Tetsu Watanabe , Gensai Yamaura, Akira Funayama, Takanori Arimoto,
Tetsuro Shishido, Takuya Miyamoto, Isao Kubota
Department of Cardiology, Pulmonology, and Nephrology, Yamagata University School of Medicine, Yamagata, Japan
a r t i c l e
i n f o
Article history:
Received 21 May 2015
Accepted 16 June 2015
Available online 18 June 2015
Keywords:
Heart-type fatty acid binding protein
High-sensitivity troponin T
Peripheral artery disease
Major adverse cardiovascular and
cerebrovascular events
a b s t r a c t
Background: Despite many recent advances in endovascular therapy (EVT), peripheral artery disease (PAD) is an
increasing health problem with high mortality. Heart-type fatty acid-binding protein (H-FABP) and highsensitivity troponin T (hsTnT) are markers of ongoing myocardial damage and have been reported to be useful
indicators of future cardiovascular events. However, it remains to be determined whether H-FABP and hsTnT
can predict adverse clinical outcomes in patients with PAD.
Methods and results: We enrolled 208 de novo PAD patients who underwent EVT. Serum H-FABP and hsTnT were
measured in all patients before EVT. During the median follow-up period of 694 days, there were 40 major adverse cardiovascular and cerebrovascular events (MACCEs) including all-cause deaths, and re-hospitalizations
due to cardiovascular and cerebrovascular diseases and amputations. H-FABP and hsTnT were found to be higher
in patients with critical limb ischemia (CLI) compared to those without this condition. Multivariate Cox proportional hazard regression analysis revealed that both H-FABP and hsTnT were independent predictors of MACCEs
after adjustment for confounding factors. KaplanMeier analysis demonstrated that patients in the highest tertile
according to H-FABP levels, as well as those in the highest hsTnT tertile, were at greatest risk for MACCEs. The net
reclassication index was signicantly improved by the addition of H-FABP as well as the addition of hsTnT to
traditional risk factors.
Conclusion: The myocardial damage markers H-FABP and hsTnT were increased in PAD patients with CLI and
could predict MACCEs in PAD patients.
2015 The Authors. Published by Elsevier B.V. This is an open access article under the CC BY-NC-ND license
(http://creativecommons.org/licenses/by-nc-nd/4.0/).
1. Introduction
Peripheral artery disease (PAD) is an athero-occlusive disease of the
lower limb arteries resulting in impaired mortality. The presence of PAD
is an independent predictor of cardiovascular events [1]. Despite medical advances, patients with PAD have three times higher risk of all-cause
mortality in general and of cardiovascular mortality in particular compared to those without PAD [2]. Although reduced lower extremity performance was reported to be a prognostic marker for mortality, little is
known about useful biomarkers for identifying PAD patients at high risk.
Cardiac biomarkers have been reported to be useful in predicting an
increased risk of death, not only in patients with heart disease, but also
for subjects in the general population [35]. Heart-type fatty acidbinding protein (H-FABP) is a low molecular weight protein in the cytosol of cardiomyocytes, and is rapidly released into the circulation from
damaged myocardial tissue [6]. Therefore, H-FABP is a marker for myocardial damage. Cardiac troponin T, which is a myobrillar component
of cardiomyocytes, is an established marker for myocardial damage
[7]. Myocardial damage markers can be used to risk stratify patients
with various types of heart disease [811]. However, the prognostic
value of these myocardial damage markers has not yet been elucidated
in patients with PAD.
The purpose of the present study was to determine whether
myocardial damage, assessed by measuring the concentrations of
H-FABP and high-sensitivity troponin T (hsTnT) in the bloodstream,
can predict major adverse cardiovascular and cerebrovascular events
(MACCEs) and risk stratify patients with PAD.
2. Methods
2.1. Study population
Corresponding author at: Department of Cardiology, Pulmonology, and Nephrology,
Yamagata University School of Medicine, 2-2-2 Iida-Nishi, Yamagata 990-9585, Japan.
E-mail address: tewatana@med.id.yamagata-u.ac.jp (T. Watanabe).
We carried out a prospective study of 208 de novo patients who
were admitted to our hospital for the treatment of PAD. A diagnosis
http://dx.doi.org/10.1016/j.bbacli.2015.06.003
2214-6474/ 2015 The Authors. Published by Elsevier B.V. This is an open access article under the CC BY-NC-ND license
(http://creativecommons.org/licenses/by-nc-nd/4.0/).
36
Y. Otaki et al. / BBA Clinical 4 (2015) 3541
was made by two physicians according to the ankle brachial index (ABI)
and computed tomographic angiography. Endovascular therapy (EVT)
was performed by experienced cardiologists who followed the TransAtlantic Inter-society Consensus II (TASC II) guideline recommendation.
The physicians were blinded to the results of the biochemical analyses,
and medical therapy was independently administered to optimize improvement of symptoms. The exclusion criteria of the present study
were acute coronary syndrome within the 3 months preceding admission, estimated glomerular ltration rate less than 30 mL/min/1.72 m2,
and malignant disease. Blood samples were obtained in the early morning 1 or 2 days before the rst EVT. Demographic and clinical data
including age, gender, ABI, and Fontaine class were collected from
interviews with the patients, as well as from their medical records.
Medications and ABI at discharge were recorded from the hospital
medical records.
2.2. Ethics statement
The Institutional Ethics Committee of the Yamagata University School
of Medicine approved the study, and all participants provided written informed consent. The procedures were performed in accordance with the
Helsinki Declaration.
2.3. Measurements
Hypertension was dened as systolic blood pressure (BP) 140 mm Hg
or diastolic BP 90 mm Hg or antihypertensive medication use. Diabetes mellitus was dened as glycosylated hemoglobin A1c 6.5%
(National Glyco-hemoglobin Standardization Program), or antidiabetic medication use. Hyperlipidemia was dened as total cholesterol 220 mg/dL or triglyceride 150 mg/dL or anti-hyperlipidemic
drug use. Chronic kidney disease (CKD) was dened as a reduced
glomerular ltration rate (b 60 mL/min/1.73 m2 ) according to the
Kidney Disease Outcomes Quality Initiative clinical guideline [12,13].
2.4. Biochemical markers
Blood samples for measurements of serum H-FABP concentrations were drawn and centrifuged at 2500 g for 15 min at 4 C within
30 min of collection, and the obtained serum was stored at 70 C
until analysis. H-FABP levels were measured using a two-step sandwich enzyme-linked immunosorbent assay (ELISA) kit (MARKIT-M
H-FABP, Dainippon Pharmaceutical Co. Ltd., Tokyo, Japan), as previously
described [14]. Concentrations of high-sensitivity troponin T were
measured by using a fourth-generation electrochemiluminescence immunoassay on an Elecsys 2010 automatic analyzer (Elecsystroponin-T,
Roche Diagnostics, Tokyo, Japan) [15]. Blood samples were also
obtained for measuring the concentrations of brain natriuretic
peptide (BNP). These samples were transferred to chilled tubes containing 4.5 mg ethylenediaminetetraacetic acid disodium salt and
aprotinin (500 U/mL), and centrifuged at 1000 g for 15 min at 4 C.
The claried plasma samples were frozen, stored at 70 C, and
thawed just before the assay was performed. BNP concentrations
were measured using a commercially available radioimmunoassay
specic for human BNP (Shiono RIA BNP Assay Kit, Shionogi Co.
Ltd., Tokyo, Japan) [16,17].
2.5. Endpoint and follow-up
All subjects were prospectively followed for a median period
of 694 days (interquartile range, 3491070 days). Patients were
followed up by telephone or medical records twice a year for
1500 days. The endpoint was MACCEs including all-cause death
and rehospitalization due to cardiovascular and cerebrovascular diseases such as stroke, ischemic heart disease, heart failure, abdominal
aortic aneurysm, and the development of critical limb ischemia (CLI)
and amputation.
2.6. Statistical analysis
Normality of continuous variables was checked by a Shapiro
Wilk test. Since the concentrations of H-FABP, hsTnT, and BNP were
not normally distributed, we used loge [H-FABP], log10 [hsTnT], and
log10 [BNP] for all analyses. All values are expressed as the mean
standard deviation. Continuous and categorical variables were compared with t-tests and chi-square tests, respectively. A Cox proportional hazard analysis was performed to determine independent
predictors for MACCEs and signicant predictors selected in the univariate analysis were entered into a multivariate analysis. Survival
curves were constructed with the KaplanMeier method and compared using log-rank tests. The receiver operating characteristics
(ROC) curves for MACCEs were constructed and used as a measure
of the predictive accuracy of H-FABP and hsTnT on MACCEs. The
area under the ROC curve was calculated by using the trapezoidal
rule [18]. In addition, we calculated the net reclassication index
(NRI) and the integrated discrimination index (IDI) to measure the
quality of improvement for the correct reclassication according to
the addition of H-FABP or hsTnT to the model. A value of P b 0.05
was considered statistically signicant. All statistical analyses were
performed with a standard program package (JMP version 8; SAS
Table 1
Comparison of clinical characteristics between patients with and without MACCEs.
Variables
All patients
n = 208
Event free
n = 168
MACCE
n = 40
P value
Age (years old)
Men/women
Hypertension, n (%)
Diabetes mellitus, n (%)
Hyperlipidemia, n (%)
Previous IHD, n (%)
Previous cerebrovascular
disease
Fontaine II/III/IV
CLI, n (%)
CKD, n (%)
74 8
175/33
172 (83%)
98 (47%)
134 (64%)
65 (31%)
38 (18%)
73 8
140/28
140 (84%)
77 (46%)
111 (66%)
42 (25%)
26 (15%)
77 6
35/5
32 (80%)
21 (53%)
23 (58%)
23 (58%)
12 (30%)
0.0022
0.5168
0.6165
0.5350
0.3088
b0.0001
0.0326
157/27/24
24 (10%)
81 (39%)
137/20/11
11 (7%)
60 (35%)
20/7/13
13 (28%)
21 (53%)
b0.0001
0.0004
0.0384
Endovascular therapy data
Iliac artery, n (%)
Femoropopliteal artery, n (%)
Tibial or peroneal artery, n (%)
Stent, n (%)
Pre ABI
Post ABI
142 (68%)
123 (59%)
29 (14%)
175 (90%)
0.58 0.18
0.89 0.19
120 (71%)
96 (57%)
18 (11%)
140 (90%)
0.58 0.18
0.90 0.18
22 (55%)
27 (68%)
11 (28%)
35 (88%)
0.58 0.16
0.84 0.25
Blood examination
Log10 BNP (pg/mL)
Loge H-FABP (ng/mL)
Log10 hsTnT (pg/mL)
Crea (mg/dL)
1.62 0.51
1.50 0.57
1.07 0.37
0.86 0.27
1.52 0.46
1.4 0.49
1.00 0.33
0.83 0.24
1.99 0.51 b0.0001
1.87 0.68 b0.0001
1.25 0.46
0.0002
0.97 0.36
0.0031
146 (70%)
117 (57%)
69 (33%)
44 (21%)
132 (63%)
118 (57%)
117 (70%)
96 (57%)
53 (33%)
34 (20%)
106 (63%)
99 (59%)
29 (73%)
21 (53%)
16 (40%)
10 (25%)
26 (65%)
19 (48%)
0.7226
0.5947
0.3075
0.5075
0.8221
0.1898
103 (50%)
85 (57%)
18 (45%)
0.5247
Medication
Aspirin, n (%)
Clopidogrel, n (%)
Cilostazol, n (%)
Other antiplatelet drug, n (%)
ACEIs and/or ARBs, n (%)
Calcium channel blockers,
n (%)
Statin, n (%)
0.0448
0.2311
0.0059
0.5999
0.9609
0.1811
Data are expressed as mean SD, number (percentage).
ACEIs, angiotensin-converting enzyme inhibitors; ARBs, angiotensin II receptor blockers;
BNP, brain natriuretic peptide; CKD, chronic kidney disease; CLI, critical limb ischemia;
H-FABP, heart-type fatty acid binding protein; hsTnT, high-sensitivity troponin T; MACCEs,
major adverse cardiovascular and cerebrovascular events.
Y. Otaki et al. / BBA Clinical 4 (2015) 3541
Institute Inc., Cary, NC, USA and R 3.0.2 with additional packages including Rcmdr, Epi, pROC, and PredictABEL).
37
The baseline characteristics of the patients are shown in Table 1.
There were 175 men and 33 women. The mean loge [H-FABP] and
log10 [hsTnT] were 1.50 ng/mL and 1.07 pg/mL, respectively. Patients
with MACCEs during the course of the study were older and had higher
prevalence rates of CLI, previous ischemic heart disease (IHD), previous
cerebrovascular disease, and CKD than those without MACCEs. The patients with MACCEs also had higher levels of BNP, H-FABP, hsTnT, and
creatinine compared to those without it. There was no signicant difference in EVT data excluding occlusion of tibial or peroneal artery and
medications at discharge between patients with and without MACCEs.
To determine the risk factors for MACCEs, we performed univariate
and multivariate Cox proportional hazard regression analyses. In the
univariate analysis, H-FABP and hsTnT were signicantly associated
with MACCEs (Table 2). Age, previous cerebrovascular disease, previous
IHD, CLI, CKD, and BNP were also related to MACCEs. Signicant predictors in univariate analysis were entered into multivariate Cox proportional hazard regression analysis in a stepwise manner. Both H-FABP
and hsTnT were found to be independent predictors of MACCEs in patients with PAD after adjustment of previous IHD and BNP (H-FABP,
hazard ratio, 2.61; 95% condence interval, 1.813.76; P b 0.0001 and
hsTnT, hazard ratio, 1.77; 95% condence interval, 1.122.69; P =
0.0083; Fig. 3A). Since myocardial damage markers were affected by
CLI, CKD, and previous IHD, we entered these risk factors into the multivariate Cox proportional hazard regression analysis. Both H-FABP
and hsTnT were found to be independent predictors of MACCEs after
adjusting for CLI, previous IHD, and CKD (H-FABP, hazard ratio, 2.75;
95% condence interval, 1.943.87; P b 0.0001 and hsTnT, hazard
ratio, 2.14; 95% condence interval, 1.423.23; P = 0.0003; Fig. 3B).
3.2. Myocardial damage marker levels in CLI, IHD, and CKD settings
3.4. Risk stratication
As shown in Fig. 1, patients with CLI as well as those with CKD had
higher levels of H-FABP compared to those without either of these conditions. There was, however, no signicant difference in H-FABP levels
between patients with and without previous IHD. hsTnT levels were
also higher in patients with CLI as well as those with CKD compared to
those without either of these conditions, but in contrast to the case of
H-FABP, hsTnT levels were also higher in patients with previous IHD
than in those without IHD (Fig. 2).
All subjects were divided into tertiles according to their H-FABP levels:
rst tertile (b1.28 ng/mL, n = 69), second tertile (1.281.65 ng/mL, n =
69), and third tertile (N 1.65 ng/mL, n = 70). A KaplanMeier analysis
demonstrated that the ratio of MACCEs was highest in the 3rd tertile
of H-FABP than in the other two groups (Fig. 4A). All subjects were also
divided into tertiles according to their hsTnT levels: rst tertile
(b 0.90 pg/mL, n = 69), second tertile (0.901.23 ng/mL, n = 69), and
third tertile (N1.23 ng/mL, n = 70). As was found for H-FABP, the
KaplanMeier analysis of the hsTnT tertiles also demonstrated that the
ratio of MACCEs was highest in the 3rd tertile (Fig. 4B).
3. Results
3.1. Comparison of clinical characteristics between patients with and
without MACCEs
3.3. Myocardial damage and MACCEs in patients with PAD
During the follow-up period, there were 40 MACCEs including 9 allcause deaths, 25 re-hospitalizations due to cardiovascular and cerebrovascular events, and 6 re-hospitalizations due to the development of CLI
and amputation.
To compare the prognostic capacity of H-FABP with that of hsTnT, an
ROC analysis was performed. AUC of H-FABP, sensitivity, and specicity
(B)
3.0
2.5
2.0
1.5
1.0
0.5
0
P<0.0001
CLI (-)
n = 184
CLI (+)
n = 24
Loge H-FABP (ng/mL)
Loge H-FABP (ng/mL)
(A)
3.5. Comparison of the prognostic values of H-FABP and hsTnT
3.0
2.5
2.0
1.5
1.0
0.5
0
P<0.0001
CKD (-)
n = 127
CKD (+)
n = 81
Loge H-FABP (ng/mL)
(C)
3.0
2.5
2.0
1.5
1.0
0.5
0
P=0.4018
IHD (-)
n = 143
IHD (+)
n = 65
Fig. 1. H-FABP levels in patients with and without CLI, CKD and previous IHD. (A) H-FABP levels were higher in patients with CLI than those without CLI. (B) H-FABP levels were higher in
patients with CKD than those without CKD. (C) There was no signicant difference in H-FABP levels between patients with and without IHD. H-FABP, heart-type fatty acid binding protein;
CLI, critical limb ischemia; CKD, chronic kidney disease and IHD, ischemic heart disease.
38
Y. Otaki et al. / BBA Clinical 4 (2015) 3541
(B)
2.0
P<0.0001
Log10 hsTnT (ng/mL)
Log10 hsTnT (ng/mL)
(A)
1.5
1.0
0.5
0
CLI (-)
n = 184
2.0
P=0.010
1.5
1.0
0.5
0
CKD (-)
n = 127
CLI (+)
n = 24
CKD (+)
n = 81
Log10 hsTnT (ng/mL)
(C)
2.0
P=0.0348
1.5
1.0
0.5
0
IHD (-)
n = 143
IHD (+)
n = 65
Fig. 2. hsTnT levels in patients with and without CLI, CKD and previous IHD. (A) hsTnT levels were higher in patients with CLI than those without CLI. (B) hsTnT levels were higher in patients with CKD than those without CKD. (C) hsTnT levels were higher in patients with IHD than those without IHD. hsTnT, high-sensitivity troponin T; CLI, critical limb ischemia; CKD,
chronic kidney disease and IHD, ischemic heart disease.
were found to be 0.746, 88%, and 62%, respectively. The cut-off value of
loge [H-FABP] was 1.46 ng/mL. AUC of hsTnT, sensitivity, and specicity
were 0.681, 65%, and 71%, respectively. The cut-off value of log10 [hsTnT]
was 1.2 pg/mL. AUC of H-FABP was thus signicantly greater than that
of hsTnT (P = 0.0223).
by the addition of H-FABP. NRI was also signicantly improved by the
addition of hsTnT to the basic predictors, but the addition of hsTnT did
not yield any signicant difference in IDI.
3.6. Improving reclassication by addition of H-FABP or hsTnT to predict
MACCEs
The results of this study revealed ve novel ndings: 1) patients
with MACCEs had higher levels of H-FABP and hsTnT compared to
those without MACCE; 2) patients with CLI had higher levels of HFABP and hsTnT than those without CLI; 3) multivariate Cox proportional hazard regression analysis revealed that both H-FABP and hsTnT
levels independently predicted the occurrence of MACCEs; 4) the
KaplanMeier analysis demonstrated that the prevalence of MACCEs
was greatest in patients in the highest H-FABP tertile and in the highest
hsTnT tertile; and 5) a model including H-FABP as well as one including
hsTnT showed signicantly improved abilities to predict MACCEs in patients with PAD.
To determine whether model t and discrimination improve with
addition of H-FABP or of hsTnT to the basic predictors such as age,
previous IHD, CKD, and CLI, we evaluated the improvement of NRI and
IDI. As shown in Table 3, both NRI and IDI were signicantly improved
Table 2
Univariate and multivariate Cox proportional hazard analysis of predicting MACCEs in patients with peripheral artery disease.
Variables
Univariate analysis
Age (years old)
Men/women
Hypertension
Diabetes mellitus
Hyperlipidemia)
Previous IHD
Previous cerebrovascular disease
CLI
CKD
Stent, n (%)
Pre ABI
Post ABI
Log10 BNP
Loge H-FABP
Log10 hsTnT
Abbreviation as in Table 1.
Hazard
ratio
95% condence
interval
P value
1.07
1.01
1.44
1.22
1.36
3.57
2.44
4.08
1.97
2.87
0.98
0.24
2.44
2.48
2.54
1.021.12
0.392.59
0.663.14
0.652.27
0.722.58
1.926.66
1.234.83
2.038.19
1.063.68
0.6712.17
0.137.69
0.041.50
1.753.42
1.863.28
1.783.65
0.0034
0.9815
0.3568
0.5368
0.3461
b0.0001
0.0108
b0.0001
0.0324
0.1522
0.9836
0.1278
b0.0001
b0.0001
b0.0001
4. Discussion
4.1. Myocardial damage in PAD
Previously, troponin leakage detected by a highly sensitive assay kit
(hsTnT N0.003 ng/mL) was reported to occur in 2025% of the general
population and 60% of elderly adults [1921]. In the present study,
troponin leakage was observed in 85% of PAD patients. On the other
hand, H-FABP was detected in all PAD patients examined, with a
mean loge [H-FABP] of 1.50 ng/mL. We previously reported a mean
loge [H-FABP] level of 1.25 ng/mL in the general population [5]. These
ndings suggest that the patients with PAD in our study had a greater
level of myocardial damage than that of the general population. HFABP was reported to be more sensitive than TnT for detection of latent
myocardial damage in patients with CHF [17]. Since, in contrast to troponin, H-FABP is a low molecular weight protein, cytosolic H-FABP is
easily released into the circulation through the porous membranes of
damaged myocardial cells in the absence of cardiomyocyte necrosis
Y. Otaki et al. / BBA Clinical 4 (2015) 3541
39
Hazard ratio
95%CI
P value
H-FABP
2.61
1.81-3.76
<0.0001
hsTnT
1.77
1.12-2.69
0.0083
Hazard ratio
95%CI
P value
H-FABP
2.75
1.94-3.87
<0.0001
hsTnT
2.14
1.42-3.23
0.0003
(A)
(B)
Fig. 3. Multivariate Cox proportional hazard regression analysis for predicting MACCEs in patients with PAD. (A) Hazard ratio after adjustment for IHD and BNP. (B) Hazard ratio after adjustment for CLI, CKD, and IHD. BNP, brain natriuretic peptide; CLI, critical limb ischemia; CKD, chronic kidney disease; IHD, ischemic heart disease and MACCEs, major adverse cardiovascular and cerebrovascular events.
[22,23]. In this way, measuring H-FABP, but not troponin, appears to
have detected latent myocardial damage in all patients with PAD in
the present study.
In accordance with previous reports [19,24], the presence of CKD
and IHD was associated with myocardial damage in patients with
PAD. Troponin levels were reported to be elevated in PAD patients
with CLI [25,26]. In the present study, we showed that patients with
CLI had higher levels of H-FABP and hsTnT compared to those without
CLI. Although the precise mechanism is unclear, these ndings suggest
an association of CLI with myocardial damage.
4.2. Clinical outcomes related to myocardial damage in patients with PAD
Previous studies have not fully determined whether biochemical
markers could be useful for identication and risk stratication of
these high-risk PAD patients, although BNP was reported to be useful
for the diagnosis of PAD in patients with diabetes mellitus and to
(A)
(B)
H-FABP
2nd tertile
n = 69
80
60
40
H-FABP
3rd tertile
n = 70
20
0
Log rank test, P<0.0001
0
250
500
750 1000 1250 1500
Follow up period (days)
hsTnT
1st tertile
n = 69
100
Event free rate (%)
H-FABP
1st tertile
n = 69
100
Event free rate (%)
predict MACCEs in patients with PAD [27,28]. Our results showed,
for the rst time, that H-FABP and hsTnT, diagnostic markers of
myocardial infarction [22], are the feasible markers for MACCEs in
patients with PAD.
Linnemann et al. reported that troponin leakage, detected with a
conventional cardiac TnT assay kit (N0.01 ng/mL), occurred in 21.3% of
PAD patients that were studied, and was signicantly associated with
MACCEs [26]. We also showed that troponin leakage, detected by
high-sensitivity cardiac TnT, can predict MACCEs in patients with PAD.
The abnormal cut-off value of 1.2 pg/mL (0.016 ng/mL) for log10
[hsTnT] in the present study indicates that it is possible that troponin
leakage detected by both high-sensitivity cardiac TnT and conventional
TnT could identify PAD patients at high risk.
We also showed the clinical usefulness of H-FABP in patients with
PAD. The abnormal cut-off value of 1.46 ng/mL (4.3 ng/mL) for loge
[H-FABP] in the present study is equal to that shown to predict cardiac
events in patients with CHF and implantable cardioverter debrillators
80
hsTnT
2nd tertile
n = 69
60
40
hsTnT
3rd tertile
n = 70
20
0
Log rank test, P<0.0001
0
250
500
750 1000 1250 1500
Follow up period (days)
Fig. 4. (A) KaplanMeier analysis of MACCEs among patients in all H-FABP tertiles. (B) KaplanMeier analysis of MACCEs among patients in all hsTnT tertiles. H-FABP, heart-type fatty acid
binding protein; hsTnT, high-sensitivity troponin T and MACCEs, major adverse cardiovascular and cerebrovascular events.
40
Y. Otaki et al. / BBA Clinical 4 (2015) 3541
Table 3
Statistics for model t and improvement with the addition of H-FABP or hsTnT on the prediction of MACCE.
Age+CLI+IHD+CKD
+H-FABP
+hsTnT
AUC (P value)
NRI (95% CI, P value)
IDI (95% CI, P value)
0.811
0.837
(P = 0.1834)
0.812
(P = 0.9184)
Reference
0.5032
(0.16510.8413, P = 0.0035)
0.3929
(0.05450.7312, P = 0.0228)
Reference
0.0549
(0.00470.1051, P = 0.0321)
0.0152
(0.00740.0378, P = 0.1882)
AUC, area under the curve; 95% CI, 95% condence interval; NRI, net reclassication index; IDI, integrated discrimination index; CLI, critical limb ischemia; CKD, chronic kidney disease;
IHD, ischemic heart disease; H-FABP, heart-type fatty acid binding protein and hsTnT, high-sensitivity troponin T.
[8,16]. Latent myocardial damage detected by H-FABP, in particular at
concentrations greater than 4.3 ng/mL, could provide additional clinical
information about MACCEs in patients with PAD.
Myocardial damage is associated with the development of heart failure, ischemic heart disease, and cerebrovascular disease [22,2931]. In
addition, myocardial damage is associated with CLI, which is a risk for
mortality and amputation in patients with PAD [32]. Therefore, the
myocardial damage markers H-FABP and hsTnT could be useful for
predicting MACCEs including amputations in patients with PAD.
4.3. Limitations
First, this study collected baseline information at a single time point.
Subsequent medical interventions may have affected serum H-FABP
and hsTnT levels. Second, since H-FABP levels in patients with CKD
are elevated due to impaired elimination of H-FABP, we could not
completely remove the effect of kidney dysfunction on H-FABP levels.
Third, although acute coronary syndrome was excluded in the present
study, hsTnT levels were higher in patients with IHD than in those without IHD. We could not completely eliminate the impact of IHD on hsTnT
levels. Finally, the study population was relatively small in the present
investigation. A further study with a larger population is needed to
determine precisely what constitutes abnormal levels of H-FABP and
hsTnT in patients with PAD.
5. Conclusions
Latent myocardial damage detected by H-FABP and hsTnT is increased in PAD patients with CLI. Notably, both H-FABP and hsTnT
could predict MACCEs in patients with PAD, suggesting that they are
promising markers for early identication of PAD patients at high risk.
Transparency document
The Transparency document associated with this article can be
found in the online version.
Acknowledgement
This study was supported, in part, by a grant-in-aid for Scientic
Research (No. 26893025 and No. 25860580) from the Ministry of
Education Culture, Sport, Science and Technology and a grant-in-aid
from the Global Century Center of Excellence (COE) program of the
Japan Society for the Promotion of Science.
References
[1] F.G. Fowkes, G.D. Murray, I. Butcher, C.L. Heald, R.J. Lee, L.E. Chambless, et al., Ankle
brachial index combined with Framingham Risk Score to predict cardiovascular
events and mortality: a meta-analysis, JAMA 300 (2008) 197208.
[2] C. Diehm, J.R. Allenberg, D. Pittrow, M. Mahn, G. Tepohl, R.L. Haberl, et al., Mortality
and vascular morbidity in older adults with asymptomatic versus symptomatic
peripheral artery disease, Circulation 120 (2009) 20532061.
[3] K.M. Eggers, P. Venge, B. Lindahl, L. Lind, Cardiac troponin I levels measured with a
high-sensitive assay increase over time and are strong predictors of mortality in an
elderly population, J. Am. Coll. Cardiol. 61 (2013) 19061913.
[4] D.M. Leistner, J. Klotsche, L. Pieper, G.K. Stalla, H. Lehnert, S. Silber, et al., Circulating
troponin as measured by a sensitive assay for cardiovascular risk assessment in
primary prevention, Clin. Chem. 58 (2012) 200208.
[5] Y. Otaki, T. Watanabe, H. Takahashi, A. Hirayama, T. Narumi, S. Kadowaki, et al., Association of heart-type fatty acid-binding protein with cardiovascular risk factors
and all-cause mortality in the general population: the Takahata study, PLoS One 9
(2014) e94834.
[6] J.F. Glatz, R.J. Paulussen, J.H. Veerkamp, Fatty acid binding proteins from heart,
Chem. Phys. Lipids 38 (1985) 115129.
[7] Y. Sato, T. Yamada, R. Taniguchi, K. Nagai, T. Makiyama, H. Okada, et al., Persistently
increased serum concentrations of cardiac troponin t in patients with idiopathic
dilated cardiomyopathy are predictive of adverse outcomes, Circulation 103
(2001) 369374.
[8] H. Daidoji, T. Arimoto, J. Nitobe, H. Tamura, D. Kutsuzawa, D. Ishigaki, et al., Circulating heart-type fatty acid binding protein levels predict the occurrence of appropriate
shocks and cardiac death in patients with implantable cardioverterdebrillators, J.
Card. Fail. 18 (2012) 556563.
[9] S. Matsumoto, D. Nakatani, Y. Sakata, S. Suna, M. Shimizu, M. Usami, et al., Elevated
serum heart-type fatty acid-binding protein in the convalescent stage predicts longterm outcome in patients surviving acute myocardial infarction, Circ. J. (2012).
[10] T. Arimoto, Y. Takeishi, R. Shiga, A. Fukui, H. Tachibana, N. Nozaki, et al., Prognostic
value of elevated circulating heart-type fatty acid binding protein in patients with
congestive heart failure, J. Card. Fail. 11 (2005) 5660.
[11] Y. Otaki, T. Arimoto, H. Takahashi, S. Kadowaki, D. Ishigaki, T. Narumi, et al., Prognostic value of myocardial damage markers in patients with chronic heart failure with
atrial brillation, Intern. Med. 53 (2014) 661668.
[12] K.U. Eckardt, J.S. Berns, M.V. Rocco, B.L. Kasiske, Denition and classication of CKD:
the debate should be about patient prognosisa position statement from KDOQI
and KDIGO, Am. J. Kidney Dis. 53 (2009) 915920.
[13] K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classication, and stratication, Am. J. Kidney Dis. 39 (2002) S1266.
[14] T. Arimoto, Y. Takeishi, T. Niizeki, N. Nozaki, O. Hirono, T. Watanabe, et al., Cardiac
sympathetic denervation and ongoing myocardial damage for prognosis in early
stages of heart failure, J. Card. Fail. 13 (2007) 3441.
[15] E. Giannitsis, K. Kurz, K. Hallermayer, J. Jarausch, A.S. Jaffe, H.A. Katus, Analytical
validation of a high-sensitivity cardiac troponin T assay, Clin. Chem. 56 (2010)
254261.
[16] T. Niizeki, Y. Takeishi, T. Arimoto, T. Takahashi, H. Okuyama, N. Takabatake, et al.,
Combination of heart-type fatty acid binding protein and brain natriuretic peptide
can reliably risk stratify patients hospitalized for chronic heart failure, Circ. J. 69
(2005) 922927.
[17] T. Niizeki, Y. Takeishi, T. Arimoto, N. Takabatake, N. Nozaki, O. Hirono, et al., Hearttype fatty acid-binding protein is more sensitive than troponin T to detect the ongoing myocardial damage in chronic heart failure patients, J. Card. Fail. 13 (2007)
120127.
[18] J.A. Hanley, B.J. McNeil, The meaning and use of the area under a receiver operating
characteristic (ROC) curve, Radiology 143 (1982) 2936.
[19] K.M. Eggers, L. Lind, H. Ahlstrom, T. Bjerner, C. Ebeling Barbier, A. Larsson, et al.,
Prevalence and pathophysiological mechanisms of elevated cardiac troponin I levels
in a population-based sample of elderly subjects, Eur. Heart J. 29 (2008) 22522258.
[20] J.A. de Lemos, M.H. Drazner, T. Omland, C.R. Ayers, A. Khera, A. Rohatgi, et al., Association of troponin T detected with a highly sensitive assay and cardiac structure
and mortality risk in the general population, JAMA 304 (2010) 25032512.
[21] C.R. deFilippi, J.A. de Lemos, R.H. Christenson, J.S. Gottdiener, W.J. Kop, M. Zhan,
et al., Association of serial measures of cardiac troponin T using a sensitive assay
with incident heart failure and cardiovascular mortality in older adults, JAMA 304
(2010) 24942502.
[22] K. Viswanathan, N. Kilcullen, C. Morrell, S.J. Thistlethwaite, M.U. Sivananthan, T.B.
Hassan, et al., Heart-type fatty acid-binding protein predicts long-term mortality
and re-infarction in consecutive patients with suspected acute coronary syndrome
who are troponin-negative, J. Am. Coll. Cardiol. 55 (2010) 25902598.
[23] X. Meng, M. Ming, E. Wang, Heart fatty acid binding protein as a marker for postmortem detection of early myocardial damage, Forensic Sci. Int. 160 (2006) 1116.
[24] J. Mann, M.J. Davies, Mechanisms of progression in native coronary artery disease:
role of healed plaque disruption, Heart 82 (1999) 265268.
[25] D. Rittoo, M. Stahnke, C. Lindesay, E. Grocott, N. Hickey, R. Downing, Prognostic
signicance of raised cardiac troponin T in patients presenting with acute limb
ischaemia, Eur. J. Vasc. Endovasc. Surg. 32 (2006) 500503.
[26] B. Linnemann, T. Sutter, E. Herrmann, S. Sixt, A. Rastan, U. Schwarzwaelder, et al.,
Elevated cardiac troponin T is associated with higher mortality and amputation
rates in patients with peripheral arterial disease, J. Am. Coll. Cardiol. 63 (2014)
15291538.
Y. Otaki et al. / BBA Clinical 4 (2015) 3541
[27] Q.H. Jin, W.L. Ye, H.H. Chen, X.J. He, T.L. Li, Q. Liu, et al., Levels of brain natriuretic
peptide are associated with peripheral arterial disease in subjects with type-2
diabetes mellitus, BMC Endocr. Disord. 14 (2014) 27.
[28] P.A. Stone, H. Schlarb, J.E. Campbell, D. Williams, S.N. Thompson, M. John, et al.,
C-reactive protein and brain natriuretic peptide as predictors of adverse events
after lower extremity endovascular revascularization, J. Vasc. Surg. 60 (2014)
652660.
[29] I. Beaulieu-Boire, N. Leblanc, L. Berger, J.M. Boulanger, Troponin elevation predicts
atrial brillation in patients with stroke or transient ischemic attack, J. Stroke
Cerebrovasc. Dis. 22 (2013) 978983.
41
[30] J.K. Jensen, T. Ueland, P. Aukrust, L. Antonsen, S.R. Kristensen, J.L. Januzzi, et al., Highly sensitive troponin T in patients with acute ischemic stroke, Eur. Neurol. 68 (2012)
287293.
[31] J.T. Saunders, V. Nambi, J.A. de Lemos, L.E. Chambless, S.S. Virani, E. Boerwinkle, et al.,
Cardiac troponin T measured by a highly sensitive assay predicts coronary heart
disease, heart failure, and mortality in the Atherosclerosis Risk in Communities
Study, Circulation 123 (2011) 13671376.
[32] C.M. Bailey, S. Saha, T.R. Magee, R.B. Galland, A 1 year prospective study of management and outcome of patients presenting with critical lower limb ischaemia, Eur. J.
Vasc. Endovasc. Surg. 25 (2003) 131134.
Вам также может понравиться
- Select Event Venue and SiteДокумент11 страницSelect Event Venue and SiteLloyd Arnold Catabona100% (1)
- 2AG2 TRegulatoryLymphocytesДокумент8 страниц2AG2 TRegulatoryLymphocytesPatricia Elena ManaliliОценок пока нет
- The Predictive Values of Beta - Adrenergic and M Muscarinic Receptor Autoantibodies For Sudden Cardiac Death in Patients With Chronic Heart FailureДокумент9 страницThe Predictive Values of Beta - Adrenergic and M Muscarinic Receptor Autoantibodies For Sudden Cardiac Death in Patients With Chronic Heart Failurejustin_saneОценок пока нет
- HFN 031Документ8 страницHFN 031Isti RismaОценок пока нет
- Interferencia Hemólisis y Biotina en CTNT (Saenger)Документ8 страницInterferencia Hemólisis y Biotina en CTNT (Saenger)MiguelОценок пока нет
- tmpCB0B TMPДокумент8 страницtmpCB0B TMPFrontiersОценок пока нет
- 9 - Efficacy, Safety, Tolerate, ApheresisДокумент9 страниц9 - Efficacy, Safety, Tolerate, Apheresisjef5525Оценок пока нет
- Estudo CompletoДокумент16 страницEstudo CompletoRitaIvoОценок пока нет
- Rendina 2016Документ9 страницRendina 2016Sarital BoronОценок пока нет
- 2022 Studies Collection Complete Book V1-2Документ79 страниц2022 Studies Collection Complete Book V1-2txori78Оценок пока нет
- Ehu 090Документ9 страницEhu 090Tatiana CumbicosОценок пока нет
- Heart Failure in The Last Year: Progress and Perspective: Journal ReadingДокумент31 страницаHeart Failure in The Last Year: Progress and Perspective: Journal ReadingIkmah FauzanОценок пока нет
- Amlodipine Valsartan 2Документ8 страницAmlodipine Valsartan 2Anggun Nurul FitriaОценок пока нет
- Clinical Cardiology - 2022 - Liang - Prognostic Value of RDW Alone and in Combination With NT proBNP in Patients With HeartДокумент13 страницClinical Cardiology - 2022 - Liang - Prognostic Value of RDW Alone and in Combination With NT proBNP in Patients With Heartrizkiyah prabawantiОценок пока нет
- Biomarkers in Heart FailureДокумент6 страницBiomarkers in Heart Failurekevin ortegaОценок пока нет
- HipertensiДокумент37 страницHipertensiValentina PujiОценок пока нет
- Risk Factors For Nonadherence To Antihypertensive Treatment: Original ArticleДокумент11 страницRisk Factors For Nonadherence To Antihypertensive Treatment: Original Articlebram AyuОценок пока нет
- ECG Scoring For The Evaluation of Therapy Naive Cancer Patients To Predict CardiotoxicityДокумент11 страницECG Scoring For The Evaluation of Therapy Naive Cancer Patients To Predict CardiotoxicityjuanpbagurОценок пока нет
- Elevated Triglycerides To High-Density Lipoprotein Cholesterol (TG/HDL-C) Ratio Predicts Long-Term Mortality in High-Risk PatientsДокумент8 страницElevated Triglycerides To High-Density Lipoprotein Cholesterol (TG/HDL-C) Ratio Predicts Long-Term Mortality in High-Risk PatientsIrwinОценок пока нет
- Yeshwant 2018Документ16 страницYeshwant 2018StevenSteveIIIОценок пока нет
- Research Article: ECG Markers of Hemodynamic Improvement in Patients With Pulmonary HypertensionДокумент11 страницResearch Article: ECG Markers of Hemodynamic Improvement in Patients With Pulmonary HypertensionFaradilla NovaОценок пока нет
- Prevalence and Clinical Correlates of QT Prolongation in Patients With Hypertrophic CardiomyopathyДокумент7 страницPrevalence and Clinical Correlates of QT Prolongation in Patients With Hypertrophic CardiomyopathyNITACORDEIROОценок пока нет
- Jurnal Kardio 2Документ6 страницJurnal Kardio 2Gaby YosephineОценок пока нет
- Cardiac Troponin T Is Not Increased in PatientsДокумент5 страницCardiac Troponin T Is Not Increased in PatientsAnanda Putri ImsezОценок пока нет
- Introduction and Aims of The ThesisДокумент12 страницIntroduction and Aims of The ThesisRitendra TalapatraОценок пока нет
- Diastolic Function Is A Strong Predictor of Mortality in Patients With Chronic Kidney DiseaseДокумент6 страницDiastolic Function Is A Strong Predictor of Mortality in Patients With Chronic Kidney DiseasehanifahrafaОценок пока нет
- Oxford Medicine Online: Biomarkers in Acute Heart FailureДокумент33 страницыOxford Medicine Online: Biomarkers in Acute Heart Failuremarie saulОценок пока нет
- Evaluation Study of Congestive Heart Failure and Pulmonary Artery Catheterization EffectivenessДокумент9 страницEvaluation Study of Congestive Heart Failure and Pulmonary Artery Catheterization EffectivenessMelisa AnaОценок пока нет
- Serum Concentrations of Adiponectin and Risk of Type 2 Diabetes Mellitus and Coronary Heart Disease in Apparently Healthy Middle-Aged MenДокумент15 страницSerum Concentrations of Adiponectin and Risk of Type 2 Diabetes Mellitus and Coronary Heart Disease in Apparently Healthy Middle-Aged MenEcha MagungОценок пока нет
- Atm 09 20 1587Документ14 страницAtm 09 20 1587Wina Pertiwi 2003113414Оценок пока нет
- Oup Accepted Manuscript 2020Документ11 страницOup Accepted Manuscript 2020Luis Bonino SanchezОценок пока нет
- 6 - Aphresis, + StatinДокумент7 страниц6 - Aphresis, + Statinjef5525Оценок пока нет
- 67 Ej20-0159Документ9 страниц67 Ej20-0159desconocido 123 ambticonОценок пока нет
- The Type of The Functional Cardiovascular Response To Upright Posture Is Associated With Arterial Stiffness: A Cross-Sectional Study in 470 VolunteersДокумент12 страницThe Type of The Functional Cardiovascular Response To Upright Posture Is Associated With Arterial Stiffness: A Cross-Sectional Study in 470 VolunteersVeОценок пока нет
- Kimia2Q PDFДокумент7 страницKimia2Q PDFrezqiОценок пока нет
- hr2008109 PDFДокумент10 страницhr2008109 PDFKumarsai DurusojuОценок пока нет
- Ni Hmsdasads 34581Документ11 страницNi Hmsdasads 34581Joe AjaОценок пока нет
- ESCAPE Study - JAMA 2005Документ9 страницESCAPE Study - JAMA 2005MICHAEL AMARILLO CORREAОценок пока нет
- 1 s2.0 S000287032200093X MainДокумент11 страниц1 s2.0 S000287032200093X Mainwoldekidansamuel299Оценок пока нет
- Acs 34 059Документ7 страницAcs 34 059Mutiara RobbaniiОценок пока нет
- Comparative Study of Serum and Biliary Lipid Profile in Libyan Gallstone PatientsДокумент54 страницыComparative Study of Serum and Biliary Lipid Profile in Libyan Gallstone PatientsJagannadha Rao PeelaОценок пока нет
- A Randomized Controlled Trial CCMДокумент10 страницA Randomized Controlled Trial CCMAnonymous NeRC5JYiSОценок пока нет
- Literature Critical Appraisal-1Документ7 страницLiterature Critical Appraisal-1gizework alemnewОценок пока нет
- Do Angiotensin Converting Enzyme Inhibitors or Angiotensin Receptor Blockers Prevent Diabetes Mellitus? A Meta-AnalysisДокумент9 страницDo Angiotensin Converting Enzyme Inhibitors or Angiotensin Receptor Blockers Prevent Diabetes Mellitus? A Meta-AnalysisURSULA LAZOОценок пока нет
- Debabrata JTM 2013Документ13 страницDebabrata JTM 2013Tarak Nath KhatuaОценок пока нет
- Advpub - CJ 15 0702 PDFДокумент9 страницAdvpub - CJ 15 0702 PDFNefri ArshintaОценок пока нет
- Byrd 2019Документ22 страницыByrd 2019Miriam TorresОценок пока нет
- Prognostic Value of Increased Soluble Thrornbornodulin and Increased Soluble E-Selectin in Ischaernic Heart DiseaseДокумент6 страницPrognostic Value of Increased Soluble Thrornbornodulin and Increased Soluble E-Selectin in Ischaernic Heart DiseaseIoanna Bianca HОценок пока нет
- Hta (G4)Документ9 страницHta (G4)Juan LeonОценок пока нет
- 1 s2.0 S0167527313007894 MainДокумент7 страниц1 s2.0 S0167527313007894 MainGodeliva AdrianiОценок пока нет
- Cardiovascular Revascularization MedicineДокумент6 страницCardiovascular Revascularization MedicineAndrea DonosoОценок пока нет
- An Update On Biomarkers of Heart Failure in Hypertensive PatientsДокумент9 страницAn Update On Biomarkers of Heart Failure in Hypertensive Patientsfotea_nicoleta816Оценок пока нет
- 129 Full PDFДокумент7 страниц129 Full PDFHerlina ApriliaОценок пока нет
- Use of Circulating Micrornas To Diagnose Acute Myocardial InfarctionДокумент9 страницUse of Circulating Micrornas To Diagnose Acute Myocardial InfarctionGheavita Chandra DewiОценок пока нет
- Postdialysis Hypertension: Associated Factors, Patient Profiles, and Cardiovascular MortalityДокумент6 страницPostdialysis Hypertension: Associated Factors, Patient Profiles, and Cardiovascular MortalityLaura PutriОценок пока нет
- Content ServerДокумент7 страницContent ServerRachtipatPitiwararomОценок пока нет
- Wikstrand Et Al-2014-Journal of Internal MedicineДокумент10 страницWikstrand Et Al-2014-Journal of Internal MedicineOrion JohnОценок пока нет
- Value of Epicardial Adipose Tissue Assessment by Cardiac Computerized Tomography in Heart Failure Patients With Preserved Ejection FractionДокумент6 страницValue of Epicardial Adipose Tissue Assessment by Cardiac Computerized Tomography in Heart Failure Patients With Preserved Ejection FractionIJAR JOURNALОценок пока нет
- Predictive Value of High-Sensitivity Troponin-I For Future Adverse Cardiovascular Outcome in Stable Patients With Type 2 Diabetes MellitusДокумент8 страницPredictive Value of High-Sensitivity Troponin-I For Future Adverse Cardiovascular Outcome in Stable Patients With Type 2 Diabetes MellitusRooban SivakumarОценок пока нет
- For Hand Grip Strength: NormsДокумент7 страницFor Hand Grip Strength: NormsPraneethaОценок пока нет
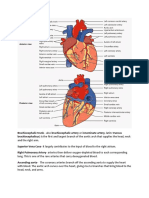
- Reference Document GOIДокумент2 страницыReference Document GOIPranav BadrakiaОценок пока нет
- Brachiocephalic TrunkДокумент3 страницыBrachiocephalic TrunkstephОценок пока нет
- Ineffective Breastfeeding - NCPДокумент10 страницIneffective Breastfeeding - NCPJullian PloyaОценок пока нет
- Snap Bore Ring PDFДокумент8 страницSnap Bore Ring PDFlaaliОценок пока нет
- AcquaculturaДокумент145 страницAcquaculturamidi64100% (1)
- Global Warmin G and Green House Effect: Submit Ted To:-Mr - Kaush Ik SirДокумент24 страницыGlobal Warmin G and Green House Effect: Submit Ted To:-Mr - Kaush Ik SirinderpreetОценок пока нет
- Microbial Communities From Arid Environments On A Global Scale. A Systematic ReviewДокумент12 страницMicrobial Communities From Arid Environments On A Global Scale. A Systematic ReviewAnnaОценок пока нет
- Quarterly Progress Report FormatДокумент7 страницQuarterly Progress Report FormatDegnesh AssefaОценок пока нет
- Hasil Pemeriksaan Laboratorium: Laboratory Test ResultДокумент1 страницаHasil Pemeriksaan Laboratorium: Laboratory Test ResultsandraОценок пока нет
- C 1 WorkbookДокумент101 страницаC 1 WorkbookGeraldineОценок пока нет
- Photoperiodism Powerpoint EduДокумент12 страницPhotoperiodism Powerpoint EduAlabi FauziatBulalaОценок пока нет
- Power of AttorneyДокумент10 страницPower of AttorneyRocketLawyer82% (17)
- Corn Fact Book 2010Документ28 страницCorn Fact Book 2010National Corn Growers AssociationОценок пока нет
- Vicat Apparatus PrimoДокумент10 страницVicat Apparatus PrimoMoreno, Leanne B.Оценок пока нет
- Bakery Ind HygieneДокумент104 страницыBakery Ind Hygienelabie100% (1)
- Analyzing Activity and Injury: Lessons Learned From The Acute:Chronic Workload RatioДокумент12 страницAnalyzing Activity and Injury: Lessons Learned From The Acute:Chronic Workload RatioLukas ArenasОценок пока нет
- PowderCoatingResins ProductGuide 0Документ20 страницPowderCoatingResins ProductGuide 0zizitroОценок пока нет
- UIP ResumeДокумент1 страницаUIP ResumeannabellauwinezaОценок пока нет
- Gintex DSДокумент1 страницаGintex DSRaihanulKabirОценок пока нет
- CPhI Japan InformationДокумент22 страницыCPhI Japan InformationctyvteОценок пока нет
- Athletes Who Made Amazing Comebacks After Career-Threatening InjuriesДокумент11 страницAthletes Who Made Amazing Comebacks After Career-Threatening InjuriesანაОценок пока нет
- Summary Scholten's GroupsДокумент8 страницSummary Scholten's GroupsLily Samardzic-Rafik100% (4)
- Human Rights Law - Yasin vs. Hon. Judge Sharia CourtДокумент7 страницHuman Rights Law - Yasin vs. Hon. Judge Sharia CourtElixirLanganlanganОценок пока нет
- LWT - Food Science and Technology: A A B AДокумент6 страницLWT - Food Science and Technology: A A B ACarlos BispoОценок пока нет
- Capacitor BanksДокумент49 страницCapacitor BanksAmal P RaviОценок пока нет
- Api 579-2 - 4.4Документ22 страницыApi 579-2 - 4.4Robiansah Tri AchbarОценок пока нет
- Cranial Electrotherapy Stimulator (C.E.S.) Earlobe Stimulator, Pocket-Transportable, 9VДокумент1 страницаCranial Electrotherapy Stimulator (C.E.S.) Earlobe Stimulator, Pocket-Transportable, 9VemiroОценок пока нет
- Senographe Crystal: The Choice Is Crystal ClearДокумент7 страницSenographe Crystal: The Choice Is Crystal ClearmuhammadyassirОценок пока нет