Академический Документы
Профессиональный Документы
Культура Документы
Br. J. Anaesth. 2002 Van Der Vyver 459 65
Загружено:
Annisa AuliaАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Br. J. Anaesth. 2002 Van Der Vyver 459 65
Загружено:
Annisa AuliaАвторское право:
Доступные форматы
British Journal of Anaesthesia 89 (3): 459-65 (2002)
Patient-controlled epidural analgesia versus continuous infusion
for labour analgesia: a meta-analysis
M. van der Vyver1, S. Halpern2* and G. Joseph2
Department of Anaesthesia, University of Stellenbosch and Tygerberg Academic Hospital Private Bag 3,
Tygervallei 7505, Western Cape, South Africa. 2Department of Anaesthesia, University of Toronto and
Sunnybrook and Women's Health Sciences Centre, Women's College Campus, 76 Grenville Street, Toronto,
Ontario, M5S 1B2 Canada
^Corresponding author
Background. Patient-controlled epidural analgesia (PCEA) is a relatively new method of maintaining labour analgesia. There have been many studies performed that have compared the efficacy of PCEA with continuous epidural infusion (CEI). The purpose of this systematic review is
to compare the efficacy and safety of PCEA and CEI.
Results. Nine studies comprised of 640 patients were found. There were fewer anaesthetic
interventions in the PCEA group (RD, 27%; 95% Cl, 18-36%; P<0.0000l). This group also
received less local anaesthetic (WMD, -3.92; 95% Cl, -5.38 to -2.42; P<0000l) and less motor
block (RD, 18%; 95% Cl, 6-3 I %; P=0.003). Both methods were safe for mother and newborn.
Conclusion. Patients who receive PCEA are less likely to require anaesthetic interventions,
require lower doses of local anaesthetic and have less motor block than those who receive
CEI. Future research should be directed at determining differences in maternal satisfaction and
obstetric outcome.
BrJ Anaesth 2002; 89: 459-65
Keywords: analgesia, obstetric; analgesia, patient-controlled; analgesic techniques, epidural;
safety, techniques
Accepted for publication: April 11, 2002
Epidural analgesia is the most effective way of providing
pain relief in labour.! A number of techniques have evolved
to maintain the level of analgesia throughout labour,
Historically, intermittent bolus dosing of local anaesthetic
by the clinician (anaesthetist, nurse or midwife) was used,
However, this technique had a number of drawbacks
including inconsistent analgesia, potential toxicity, and
concerns about sterility each time the clinician opened the
system to administer a bolus.
Continuous epidural infusion (CEI) of local anaesthetics
was introduced into common clinical practice in the 1980s,
While the technique has circumvented a number of
difficulties,2 it is not ideal. Many patients still required
clinician-initiated top-ups and experienced unacceptably
dense motor block in the lower extremities. Although many
combinations of infusion rates and various concentrations of
local anaesthetics and additives have been investigated,
these problems persist.
Patient-controlled epidural analgesia (PCEA) for relief of
labour pain was first described by Gambling in 1988.3 This
technique allowed the patient to control the dose of epidural
medication as labour and pain patterns changed. It also
The Board of Management and Trustees of the British Journal of Anaesthesia 2002
Downloaded from http://bja.oxfordjournals.org/ by guest on January 10, 2016
Methods. All randomized controlled trials that compared PCEA, without background infusion,
with CEI were sought from the literature. These were rated for quality using a validated, fivepoint scale. The primary outcome was the number of patients who received anaesthetic interventions. Secondary outcomes included the dose of local anaesthetic, incidence of motor
block, quality of analgesia, obstetric and safety outcomes. Where feasible, the data were combined using meta-analytical techniques. For dichotomous data, the risk difference (RD) and 95%
confidence intervals (Cl) were calculated. For continuous data, the weighted mean differences
(WMD) were calculated. The differences were statistically significant when the 95% Cl
excluded 0.
van der Vyver et al.
Table 1 PCEA vs CEI study characteristics. B=bupivacaine; R=ropivacaine; epi=epinephrine; F=fentanyl; S=sufentanil; PCEA=patient-controlled epidural
analgesia; CEI=continuous epidural infusion; UA=umbilical artery; UV=umbilical vein
Reference Quality Patients
score
number
(year)
PCEA
group
treatment
CEI group
treatment
Population
Outcomes measured
Significantly different
outcomes
0.1% R; F 2
\ig ml"1;
bolus 5 ml;
lockout 10
min; max
25 ml h"1
0.125% B;
bolus 6 ml;
lockout 20
min; no max
0.125% B; F
2.5 (ig ml"1;
E 1:400000;
bolus 2-6 ml;
lockout
10-30 min
0.125% B; F
2 ng ml"1;
bolus 3 ml;
lockout 10
min; no max
0.125% B;
F2|agmr1;
bolus 3 ml;
lockout 10
min, no max
0.1% R; F 2
M-g m r ' ;1
8 ml h"
Nulliparous
R/F ml h , midwife top-ups, VAS
every 15-30 min, motor weakness
(ambulation), obstetric outcomes,
hypotension and 1 and 5 min Apgar
scores.
None
0.125% B;
10 ml h"1
Mixed parity Analgesia, patient satisfaction, motor
block, sensory level, B mg h"1, number
of top-ups, duration of labour, mode of
delivery and hypotension.
Nulliparous Analgesia, patient satisfaction, motor
block, numbers of patients requiring
clinician-interventions, mean B mg h"1
and F jj.g h"1, mode of delivery,
hypotension and Apgar scores.
in PCEA/
n CEI)
5
27/29
11 (1994)
30/30
14 (1993)
55/13
12 (1991)
20/20
13 (1994)
15/15
9 (1999)
48/50
0.125% B; S
0.5 ng ml"1;
bolus 5 ml;
lockout 10
min; max 50
ml 4b."1
10 (1999)
44/46
7 (1992)
75/84
0.1% B; F 2
0.1% B; F 2 u.g
(ig ml"1;
ml"1; 10 ml h"1
bolus 10 ml;
lockout 30
min; no max
0.25% B; bolus 0.125% B
3 ml; lockout
10 ml h"1
5 min; max
4 boluses h~'
8 (1994)
15 (1999)
20/20
0.2% R;
bolus 5 ml;
lockout 15
min; max
15 ml h"1
0.125% B;
F 2.5 \lg
ml"1; E
1:400000
8 ml h"1
0.125% B; F 2
|ig ml"1;
12 ml h"1
0.125% B;
F 2 \ig ml"
12 ml h"1
0.125% B;
S 0.5 |ig mF1
at 8-14 ml h"
Mean B mg h ', patient
satisfaction and number
of top-ups: favouring PCEA.
Mean B mg IT1 and
F |^g h ', and
spontaneous deliveries:
all favouring PCEA.
Mixed parity Analgesia, motor block, sensory level,
B mg h"\ F |a.g h"1, number of clinician
top-ups, duration of labour (1st and 2nd
stage), mode of delivery, hypotension,
pruritus and Apgar scores.
Mixed parity Analgesia, motor block, sensory level,
B mg h"1, number of clinician top-ups,
duration of labour (1st and 2nd stage),
mode of delivery, hypotension and
Apgar scores.
Hourly B mg h
(/><0.0002) and F ug h"
(P<0.0002): lower in
PCEA.
Mixed parity Analgesia, patient satisfaction, motor
block, sensory level, total and hourly
dose of B, number of patients, requiring
clinician top-ups, total duration of
labour, mode of delivery, hypotension,
pruritus and Apgar scores.
B mg h"1 less in
PCEA
(P<0.05); smaller
number of patients
requiring top-ups
in treatment group
(P<0.05).
Motor and block, B dose
If1: in favour of PCEA.
Nulliparous
Nulliparous
0.2% R 8 ml h"1 Nulliparous
allowed for individualization of drug dosage by the patient,
allowing her to trade off therapeutic effects (e.g. complete
pain relief) and side-effects (e.g. motor block). However,
the equipment needed for PCEA may be more expensive
than CEI. Also, more time is required to educate both the
patient and staff about the appropriate use of the medication
and equipment.
Many studies have been performed comparing PCEA
with CEI. The purpose of this systematic review is to
Analgesia, patient satisfaction, motor
block, B mg h"1, F jig h"1, number of
patients., requiring top-ups, total
duration of labour, mode of delivery,
Apgar scores >UA and UV pH.
Analgesia, patient satisfaction, motor
block, mean total B mg, number of
anaesthetist interventions, duration
of second stage, mode of delivery
and hypotension.
Analgesia, motor block, sensory level,
R mg h"1, number of clinician top-ups,
duration of second stage, mode of
delivery, hypotension, shivering,
nausea and Apgar scores.
B mg h"1 less in
treatment group
(P<0.0002); number of
spontaneous vaginal
deliveries less in CEI
Motor block less in
PCEA group (P<0.01);
number of anaesthetist
interventions less in
PCEA groups.
R mg h"1 dose lower in
PCEA group (P<0.05);
motor block less in
PCEA group (P<0.05).
compare the efficacy and safety of PCEA with that of CEI
for maintenance of labour analgesia.
Methods
We sought randomized controlled trials (RCTs) that compared PCEA with CEI. Reports were identified by electronically searching Medline (January 1980 to September 2001),
EMBase (January 1980 to September 2001), Science
460
Downloaded from http://bja.oxfordjournals.org/ by guest on January 10, 2016
16 (2001)
PCEA vs continuous infusion epidural for labour
sensitivity analysis on the primary outcome on the basis of
the quality score (0-2 vs 3 or more).
Results
We identified a total of 12 RCTs. Two manuscripts were not
available through the University of Toronto Library system
and were excluded.5 6 The outcome of one of the studies was
reported in two manuscripts.7 8 Therefore, nine studies (in
ten manuscripts) described a total of 641 patients of whom
545 patients received bupivacaine7"14 and 96 patients
received ropivacaine.15 16 The range of numbers of patients
included in the studies was 30-159. The median quality
score was 3. Five studies had quality scores of three or
greater.11"1416
Table 1 details the quality score, the obstetric population
studied, the number of patients involved in each group and
drugs used for maintenance in PCEA and CEI groups. None
of the studies reported the incidence of induced and
spontaneous labour. All measured outcomes, as well as
those that were significantly different, are shown.
Unscheduled anaesthetic interventions
In five of the studies, clinician top-up of the epidural for
inadequate analgesia was reported as a separate
outcome.9~n 14 In one study, this outcome and catheter
manipulation or replacement were considered together.
Figure 1 shows the combined data for the number of patients
who needed no unscheduled anaesthetic interventions.
Significantly fewer patients needed clinician top-ups in the
PCEA group compared with CEI (RD, 27%; 95% CI,
18-36%; P<0.00001). This observation was also true when
only studies with a quality score of three or greater were
considered (RD, 35%; 95% CI, 19-51%; P<0.0001).
Although four of the studies included patients of mixed
parity, 911 " 13 there was no evidence of heterogeneity
(P=0.36) among the studies for this outcome.
Three studies reported the number of anaesthetic interventions in a manner that could not be combined in the
meta-analysis above. One did not report the number of topups but noted the volume of local anaesthetic given per
hour. In this study, the midwives administered less
ropivacaine in the PCEA group compared with the CEI
(5.4 vs 6.9 ml hf1; ns).16 Two studies did not measure the
number of patients who required interventions, rather they
reported the amount of bupivacaine used in each group.12 13
One of these studies reported that 'similar numbers' of
patients required top-ups in each group.12 The other
reported an increased bupivacaine requirement in the
PCEA group compared with CEI related to clinician topups.13 This was statistically significant for first stage but not
for the second stage or the total length of labour.
In addition to reporting the number of patients who
required no interventions, three studies reported the total
number of clinician top-ups in the CEI group compared with
461
Downloaded from http://bja.oxfordjournals.org/ by guest on January 10, 2016
Citation index (1993-2001) and the Cochrane Library (June
2000, Issue 3).
We used the following search terms as key words and text
words: 'Patient-controlled', 'labour analgesia', 'anaesthesia' (excluding anaesthesia for Caesarean section) and
'pregnancy'. Alternative spellings of the search terms were
also used. No language restriction was applied. The last
search was done on the September 20, 2001. Additional
reports were identified from reference lists of retrieved
reports and review articles.
We included published RCTs in healthy parturients that
used the same local anaesthetic and additives for both the
study and control group. Furthermore, we only included
RCTs that had no continuous background infusion in the
PCEA group. We excluded abstracts of scientific meetings,
unpublished observations and correspondence.
Each report meeting the inclusion criteria, was read
independently by each of the authors and assigned a quality
score according to a previously published, validated scale.4
This scale consists of three items and has a maximum
possible score of five. When the report was described as
randomized, one point was given. If the randomization
process was appropriate an extra point was given. The
original point for randomization was lost if randomization
was inappropriate (e.g. if it was based on date of birth). One
point was given when a study was described as blinded. If
blinding was inappropriate this point was lost, but an extra
point was gained if blinding was appropriate. If all patients
randomized were fully accounted for another point was
given. The final quality score for each article was reached by
the authors by means of consensus.
The primary outcome of the study was the number of
patients who received anaesthetic interventions during the
maintenance of labour analgesia. Secondary outcomes
included the dose of local anaesthetic, the incidence of
motor block, the quality of analgesia and maternal satisfaction. Obstetric and neonatal outcomes included the length of
labour, rate of Caesarean section, the rate of instrumental
deliveries and the incidence of low Apgar scores at 1 and 5
min. Other outcomes included the incidence of hypotension,
high block, nausea, pruritus and shivering.
Data were recorded independently by two of the authors
(M.V. and G.J.) and discrepancies resolved by reinspection
of the original articles. The data were entered into the
statistical program (S.H.H) and rechecked (M.V.).
Where feasible, meta-analytical techniques, using a
random effects model were used (Metaview software,
Revman 4.1, Cochrane Library, Oxford, UK). For dichotomous data, the risk difference (RD) and 95% confidence
intervals (95% CI) were calculated. For continuous data, the
weighted mean difference and 95% CI were calculated. We
considered the results statistically significant if the 95% CI
excluded 0. The %2 test was used to calculate heterogeneity
and a P-value of <0.05 was regarded as significant. Where
meta-analysis was not appropriate, the results of the
individual studies were reported. We also performed a
van der Vyver et al.
Study
(first author)
PCEA
(n/W)
Infusion
(n/N)
Risk difference
(95% confidence
interval)
Sia
17/20
16/20
-H i
Butros
42/48
34/50
-m-
Gambling
34/55
5/13
Purdie
38/75
16/84
Collis
27/44
12/46
Curry
29/30
17/30
Total (95% Cl)
187/272
100/243
study assessed motor power by asking the patient to sit up
and then walk. However, the time at which this outcome was
measured is not clear. The authors noted that all their
patients, in both groups, could walk at some time during
labour.16
Tan and colleagues8 reported that patients receiving
PCEA were more likely to have 'no motor weakness'
compared with those having CEI, based on repeated
assessments of each patient (P<0.01). The incidence of
complete immobility of the lower extremities was not
different between groups (4.5 vs 2.9%; ns). Two other
studies found no difference between groups in 'dense motor
block' as defined by Bromage scores of 2 or 3. 12 13
""
-1.0-0.5 0 0.5 1.0
Favours Favours
infusion
PCEA
Analgesia
Drug dose
Patient satisfaction
1
The dose (mg h" ) of local anaesthetic administered to
patients receiving CEI was significantly greater than those
in the PCEA group (Table 2). All studies that measured this
outcome reported the same result regardless of whether
bupivacaine or ropivacaine was used. The addition of opioid
to the maintenance solution (either fentanyl or sufentanil)
did not make a difference to this outcome. Because different
regimen were used, this outcome is heterogeneous
(P<0.0001) even though all studies favoured the PCEA
group (Fig. 2).
Overall patient satisfaction with the method of analgesia,
using a VAS score, was reported in five studies.9"11 14 15 The
data from four of these could be combined (Table 2). One
study reported maternal satisfaction using a VAS scale at
various times during labour and reported the data in
graphical form, but did not report an overall score.14 One
study reported 'patient satisfaction with analgesia'.7 These
studies did not show a difference in maternal satisfaction
between groups.
Obstetric and neonatal outcomes
Motor weakness
Motor power was measured in a number of different ways in
each of the studies. Two studies reported 'no motor
weakness' throughout the labour.9 14 Two additional studies
described no or minimal weakness at 2-h intervals over
time. 1015 We used the 2-h incidence of 'no weakness' in
these studies for our analysis and found that this side-effect
was significantly reduced in the PCEA group (Table 2). One
The total length of labour (in minutes) was reported in three
studies9"11 and there was no difference between the groups.
Similarly there was no difference in the duration of first
stage of labour12 13 or second one.7 12 13 15 None of the
studies reported a difference in the incidence of Caesarean
section or instrumental delivery between groups. The
incidence of low Apgar scores at 1 and 5 min after birth
was low and similar in each group (Table 2).
462
Downloaded from http://bja.oxfordjournals.org/ by guest on January 10, 2016
PCEA. Tan and colleagues found a significantly higher
number in the CEI group than in the PCEA group (120 topups in 84 women compared with 49 in 75 women,
respectively). Curry and colleagues11 reported 27 top-ups
in 30 patients who received CEI compared with only two
top-ups in 30 patients who received PCEA CP<0.001). Sia
and colleagues15 reported six top-ups in 20 patients in the
CEI group compared with three top-ups in 20 patients in the
PCEA group during the first stage of labour (P=0.4).
Labour analgesia was measured at intervals using a visual or
verbal analogue score (VAS) in seven studies,9"15 and the
number of distressing pain episodes in one.7 These results
were either displayed in graphic form or described qualitatively. The VAS scores were not different between groups
in any of the studies. The numbers of distressing pain
episodes were also similar. Finally, pain scores, when
classified as mild, moderate or severe, were the same in both
groups.10
One study specifically reported VAS scores for pain in the
second stage of labour and found no difference between
groups.10 A second study reported that complete or good
analgesia was also not significantly different between
groups.7 However, in this study 16.9% of women suffered
'unacceptable' pain in the PCEA group compared with
2.8% in the CEI group (P=0.01).
Fig 1 The number of patients who required no unscheduled interventions
by the clinician. The RD and 95% CI for each study and the pooled
estimates are shown. The size of the box represents the relative weight of
each study, the lines represent the 95% CI. The midpoint of the diamond
is the pooled estimate of the RD. The diamond extends over the 95% CI
of the pooled estimate.
PCEA vs continuous infusion epidural for labour
Table 2 Summary of study outcomes. PCEA=patient-controlled epidural analgesia; CEI=continuous epidural infusion; WMD=weighted mean difference;
RD=risk difference, CI=confidence interval
Outcome
9-16
9, 10, 14, 15
7
9-11, 15
11
10
7
7
PCEA
(n or n/N)
CEI
(n or n/N)
WMD or RD
and 95% CI
P-Value
257
221
151/167
65/75
103/129
73/84
139
30
40
144
30
44
WMD: -3.92 (-5.38, -2.42)
RD: 18% (6%, 31%)
RD: 0% (-11%, 10%)
WMD: 3.86 (-2.15, 9.88)
WMD: -7.20 (-19.16, 4.76)
WMD: 3.00 (3.00, -0.80, 6.80)
RD: 2% (-17%, 13%)
RD: 16% (2%, 31%)
RD: 5% (-8%, 18%)
WMD: 20.00 (7.44, 32.56)
RD: 4% (-8%, 1%)
RD: 1% (-6%, 7%)
WMD: 7.68 (-65.75, 81.10)
WMD: 21.00 (-37.72, 79.71)
WMD:-10.33 (-21.59, 0.93)
WMD: 0.01 (-0.02, 0.05)
WMD: 0.00 (-0.07, 0.07)
RD: - 1 % (-3%, 2%)
RD: 1% (-5%, 6%)
RD: 5% (-21%, 31%)
RD: 5% (-8%, 18%)
RD: 3% (-15%, 21%)
<0.00001
0.003
1
0.2
0.2
0.14
0.8
0.03
0.5
0.02
0.12
0.9
0.8
0.5
0.07
0.5
1
0.6
0.9
0.7
0.4
0.8
47/75
55/75
62/95
54/84
48/84
62/104
10
41
44
7, 9-16
7, 9-16
9-11
12, 13
7, 12, 13, 15
9, 10, 12-15
9, 10, 12-15
9, 10, 12, 14-16
7, 9, 11
41/333
19/333
51/307
98/307
7, 15
122
35
130
4/201
23/201
4/275
9/153
5/20
1/20
11/68
15
15
9, 12
Other outcomes
There was no difference between groups in the incidence of
hypotension or high block (as described by any of the
authors). The incidence of pruritus, shivering and nausea
were similar in each group (Table 2).
Discussion
This systematic review shows that PCEA in labour consistently results in fewer clinician interventions when compared
with CEI. This result was achieved using a lower dose of
local anaesthetic but without any measurable change in pain
relief or patient satisfaction. In addition, patients in most
studies had better mobility in the PCEA group.
The need for unscheduled clinician interventions is an
important outcome for a number of reasons, apart from
simple convenience. Additional drug doses require opening
the 'closed system' and may increase the risk of infection.
Furthermore, it is usual for the clinician to use an increased
drug dose compared with that available to the patient. If this
dose is misplaced (either in the intravascular or intrathecal
space), toxicity might result. Finally, because of the
increased drug dose, motor block of the lower extremities
may be more evident.
The use of less local anaesthetic is also an important
advantage of PCEA. While this review did not show a
difference in operative delivery between patients who
received PCEA and those who received CEI, there is
some evidence that drug dose may affect labour outcome.
Recently, the COMET group17 in the United Kingdom have
shown that there is an increased incidence of operative
126
35
139
1/164
12/164
7/246
8/164
4/20
0/20
7/70
vaginal delivery when conventional doses of local anaesthetic (0.25% bupivacaine) are used in labour compared
with low dose techniques. Furthermore, cumulative doses of
opioids, which are often combined with local anaesthetics in
the infusions, may result in mild neonatal depression.17
While none of the studies we have reviewed reported results
from 'high' doses of local anaesthetics, it may still be an
advantage to use less of the drugs.
The differences in patient mobility were also consistent
between groups when this outcome was measured. This
consistency was present despite the numerous ways in
which motor weakness of the lower extremities was
reported and was likely to have been a result of the
observed increase in local anaesthetic dosage in the CEI
group. Of note, in one study that used 0.1% ropivacaine and
fentanyl 2 jig ml"1, all patients could walk. It is possible that
by reducing the concentration of local anaesthetic sufficiently, the difference in motor block between PCEA and
CEI may become insignificant.
Of interest, although many of the studies reported
measures of maternal satisfaction, there was no consistent
difference between PCEA and CEI. This may be due to a
number of reasons. First, satisfaction with both forms of
analgesia appeared to be extremely high. Therefore, even by
combining the results of all studies, the sample size may be
insufficient to demonstrate a difference. This is particularly
true because of the numerous different methods used to
measure satisfaction and the different times (during labour
or the next day) at which the question was asked. Second, it
is very difficult to accurately measure maternal satisfaction.
Often satisfaction with a particular technique is confused
463
Downloaded from http://bja.oxfordjournals.org/ by guest on January 10, 2016
Mean dose of local anaesthetic
Motor block: patients with no motor weakness
Maternal satisfaction: patients satisfied with technique
Maternal satisfaction: VAS scores
Pain relief: global pain assessment (VAS)
Pain relief: pain of labour first stage (VAS)
Pain relief: excellent analgesia first stage
Pain relief: no distressing pain in first stage
Pain relief: complete or good analgesia in second stage
Pain relief: pain assessment second stage (VAS)
Mode of delivery: Caesarean section
Mode of delivery: instrumental deliveries
Total length of labour
Length of first stage
Length of second stage
Low Apgar score at 5 min
Low Apgar score at 1 min
Hypotension
High sensory block
Shivering
Nausea
Pruritus
Studies included
(reference number)
van der Vyver et al.
Study (first
author (yr))
PCEA
(n)
Mean (SD) Infusion Mean (SD)
(n)
Ferrante(1991)
20
9(4)
20
16(4)
Ferrante (1994)
15
9(4)
15
17(4)
Curry
30
8(3)
30
14(4)
Gambling
55
5(2)
13
9(3)
Sia
20
18(3)
20
21(5)
Collis
44
9(2)
46
12(3)
Butros
48
13(4)
50
15(4)
Smedvig
25
8(5)
27
8(0.4)
Total (95% Cl)
257
Weighted mean difference
(95% confidence interval)
221
-10-5
Favours
infusion
5 10
Favours
PCEA
with satisfaction with pain relief. However, satisfaction is
multidimensional and other factors such as patient expectations, communication skills of the health care team and the
obstetric outcome are far more important than analgesia per
se.ls One study attempted to measure multiple aspects of
satisfaction but still did not find any difference between
groups.10
In this review, we found no difference between groups in
the incidence of Caesarean section or instrumental vaginal
delivery. Furthermore, there was no difference in the
duration of either the first or second stages of labour.
However, the studies were small and the total number of
patients enrolled may have been insufficient. In addition, the
combination of nulliparous and multiparous parturients in
some of the studies would reduce the power to detect these
outcomes. A single, large study with standardized obstetric
management would be more likely to find a difference if it
exists.
Both CEI and PCEA appear to be safe for the mother and
neonate. The incidence of maternal side-effects and neonatal depression was extremely low in the studies that
measured these outcomes. Maternal hypotension occurred
in less than 3% of cases and a low 5 min Apgar score
occurred in under 2% (Table 2). An extremely large series
of patients would be required to determine if the two groups
were different with respect to these outcomes.
In summary, PCEA for labour pain has several advantages when compared with CEI. These include a reduction
in the number of unscheduled clinician top-ups, a reduction
in the amount of drug used and a reduction in the amount of
motor block of the lower extremities. Both methods are safe
for the mother and newborn. More information is needed to
determine which method of analgesia maintenance leads to
a reduced need for obstetric intervention and better patient
satisfaction.
Acknowledgement
We would like to thank Dr Barbara Leighton, Professor of Clinical
Anesthesiology, Weill Medical College of Cornell University, New York,
USA for her editorial assistance.
References
464
1 Glosten B. Epidural and spinal analgesia/anesthesia. In: Chestnut
DH, ed. Obstetric Anesthesia: Principles and practice, 2nd edition. St
Louis: Mosby, 1999; 360-86
2 Taylor HJ. Clinical experience with continuous epidural infusion
of bupivacaine at 6 ml per hour in obstetrics. Can Anaesth SocJ
1983; 30: 277-85
3 Gambling DR, Yu P, Cole C, McMorland GH, Palmer L A
comparative study of patient controlled epidural analgesia
(PCEA) and continuous infusion epidural analgesia (CIEA)
during labour. Can J Anaesth 1988; 35: 249-54
4 Jadad AR, Moore RA, Carroll D, et al. Assessing the quality of
reports of randomized clinical trials: is blinding necessary? Control
Clin Trials 1996; 17: 1-12
5 Turhanoglu S, Ozyilmaz MA, Olmez G, Tok D, Bayhan N.
Comparison of continuous epidural infusion and patientcontrolled epidural analgesia in labour. Agri 1999; I I: 23-8
6 Uckunkaya N, Bilgin H, Sahin S, Ozarac O. Comparison of
continuous infusion and patient-controlled epidural analgesia
during labor. Turk Anesteziyoloji Ve Reanimasyon 1996; 24:
19-23
7 Purdie J, Reid J, Thorburn J, Asbury AJ. Continuous extradural
analgesia: Comparison of midwife top-ups, continuous infusions
and patient controlled administration. Br J Anaesth 1992; 68:
580-4
8 Tan S, Reid J, Thorburn J. Extradural analgesia in labour:
complications of three techniques of administration. 8r J
Anaesth 1994; 73: 619-23
Downloaded from http://bja.oxfordjournals.org/ by guest on January 10, 2016
Fig 2 Dose of local anaesthetic. The weighted mean difference and 95% CI and pooled estimates are shown. The size of the box represents the
relative weight of each study, the lines represent the 95% CI. The midpoint of the diamond is the pooled estimate of the weighted mean difference.
The diamond extends over the 95% CI of the pooled estimate.
PCEA vs continuous infusion epidural for labour
9 Boutros A, Blary S, Bronchard R, Bonnet F. Comparison of
intermittent epidural bolus, continuous epidural infusion and
patient controlled-epidural analgesia during labor. Int J Obstet
Anesth 1999; 8 : 2 3 6 ^ 1
10 Collis RE, Plaat FS, Morgan BM. Comparison of midwife topups, continuous infusion and patient-controlled epidural
analgesia for maintaining mobility after a low-dose combined
spinal-epidural. Br J Anaesth 1999; 82: 233-6
I I Curry PD, Pacsoo C, Heap DG. Patient-controlled epidural
analgesia in obstetric anaesthetic practice. Pain 1994; 57:
125-7
12 Ferrante FM, Lu L, Jamison SB, Datta S. Patient-controlled
epidural analgesia: demand dosing. Anesth Analg 1991; 73:
547-552
13 Ferrante FM, Rosinia FA, Gordon C, Datta S. The role of
continuous background infusions in patient-controlled epidural
analgesia for labor and delivery. Anesth Analg 1994; 79: 804
14 Gambling DR, Huber CJ, Berkowitz J, et al. Patient-controlled
15
16
17
18
epidural analgesia in labour: varying bolus dose and lockout
interval. Can J Anaesth 1993; 40: 211-7
Sia AT, Chong JL Epidural 0.2% ropivacaine for labour analgesia:
parturient-controlled or continuous infusion? Anaesth Intensive
Care 1999; 27: 154-8
Smedvig JP, Soreide E, Gjessing L Ropivacaine I mg/ml, plus
fentanyl 2 microg/ml for epidural analgesia during labour. Is
mode of administration important? Ada Anasthesiol Scand 2001;
45: 595-9
Comparative Obstetric Mobile Epidural Trial (COMET) Study
Group UK. Effect of low dose mobile versus traditional epidural
techniques on mode of delivery: a randomized controlled trial.
Lancet 2001; 358: 19-23
Drew N, Salmon P, Webb L Mothers', midwives' and
obstetricians' views on the features of obstetric care which
influence satisfaction with childbirth. Br J Obstet Gynaecol 1989;
96: 1084-8
Downloaded from http://bja.oxfordjournals.org/ by guest on January 10, 2016
465
Вам также может понравиться
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- Tetanus ProtocolДокумент6 страницTetanus ProtocolRebecca BlackburnОценок пока нет
- Preconception Care Policy BriefДокумент8 страницPreconception Care Policy BriefAnnisa AuliaОценок пока нет
- AmiodaroneДокумент2 страницыAmiodaroneSri PurwantiОценок пока нет
- 2018 OAT GuideДокумент32 страницы2018 OAT GuideAnnisa AuliaОценок пока нет
- Bod CerebrovasculardiseasestrokeДокумент67 страницBod CerebrovasculardiseasestrokeErlin IrawatiОценок пока нет
- Manajemen Sepsis - SSCДокумент8 страницManajemen Sepsis - SSCDeborah Bravian TairasОценок пока нет
- Bevacizumab For GlaucomaДокумент10 страницBevacizumab For GlaucomaAnnisa AuliaОценок пока нет
- PCEAДокумент2 страницыPCEAAnnisa AuliaОценок пока нет
- Wound Dressing in Skin InfectionДокумент17 страницWound Dressing in Skin InfectionAnnisa Aulia100% (1)
- Piis0002939416301945 PDFДокумент9 страницPiis0002939416301945 PDFAnnisa AuliaОценок пока нет
- Comparison of Outcomes of Resident-Performed Ahmed Valve Implantation Vs TrabeculectomyДокумент8 страницComparison of Outcomes of Resident-Performed Ahmed Valve Implantation Vs TrabeculectomyAnnisa AuliaОценок пока нет
- Comparison of Outcomes of Resident-Performed Ahmed Valve Implantation Vs TrabeculectomyДокумент8 страницComparison of Outcomes of Resident-Performed Ahmed Valve Implantation Vs TrabeculectomyAnnisa AuliaОценок пока нет
- Vallecular Cyst Airway Challenge and Options of Management 2161 119X.1000158 PDFДокумент3 страницыVallecular Cyst Airway Challenge and Options of Management 2161 119X.1000158 PDFAnnisa AuliaОценок пока нет
- Comparison of Outcomes of Resident-Performed Ahmed Valve Implantation Vs Trabeculectomy PDFДокумент8 страницComparison of Outcomes of Resident-Performed Ahmed Valve Implantation Vs Trabeculectomy PDFAnnisa AuliaОценок пока нет
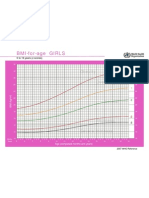
- Z Score BMI 5-19yearsold Label GirlДокумент1 страницаZ Score BMI 5-19yearsold Label GirlVienny Widhyanti RosaryaОценок пока нет
- Guideline For The Diagnosis and Management of Hypertension in Adults - 2016Документ84 страницыGuideline For The Diagnosis and Management of Hypertension in Adults - 2016Are Pee Etc100% (1)
- JNC8Документ14 страницJNC8Syukron FadillahОценок пока нет
- Comparison of Outcomes of Resident-Performed Ahmed Valve Implantation Vs TrabeculectomyДокумент8 страницComparison of Outcomes of Resident-Performed Ahmed Valve Implantation Vs TrabeculectomyAnnisa AuliaОценок пока нет
- Vallecular Cyst Airway Challenge and Options of Management 2161 119X.1000158Документ3 страницыVallecular Cyst Airway Challenge and Options of Management 2161 119X.1000158Annisa AuliaОценок пока нет
- Efficacy of Latanoprostene Bunod 0.024% Compared With Timolol 0.5% in Lowering Intraocular Pressure Over 24 HoursДокумент9 страницEfficacy of Latanoprostene Bunod 0.024% Compared With Timolol 0.5% in Lowering Intraocular Pressure Over 24 HoursAnnisa AuliaОценок пока нет
- Comparison of Outcomes of Resident-Performed Ahmed Valve Implantation Vs TrabeculectomyДокумент8 страницComparison of Outcomes of Resident-Performed Ahmed Valve Implantation Vs TrabeculectomyAnnisa AuliaОценок пока нет
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (399)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (120)
- AtelectasisДокумент21 страницаAtelectasisshilpaОценок пока нет
- Good Knight 420 GPatien ManualДокумент30 страницGood Knight 420 GPatien ManualJose Antonio AlcazarОценок пока нет
- Foods SiddhasДокумент4 страницыFoods SiddhasSanjay JayaratneОценок пока нет
- RSPCA Shuts Down Another Animal SanctuaryДокумент10 страницRSPCA Shuts Down Another Animal SanctuaryGlynne SutcliffeОценок пока нет
- Essay 25.01.2021Документ2 страницыEssay 25.01.2021Uyen TranОценок пока нет
- Tre Mad OdesДокумент31 страницаTre Mad OdesmoosОценок пока нет
- Nurse - Resignation LetterДокумент1 страницаNurse - Resignation LetterphoenixdashОценок пока нет
- MfA Leadership ExperienceДокумент49 страницMfA Leadership ExperienceAlex MoralesОценок пока нет
- Philippine Science and Technology InnovationДокумент7 страницPhilippine Science and Technology Innovationgabosara298Оценок пока нет
- ACSM - 2007 SpringДокумент7 страницACSM - 2007 SpringTeo SuciuОценок пока нет
- Hand in Hand For A Healthier World: Logiq V5 ExpertДокумент4 страницыHand in Hand For A Healthier World: Logiq V5 ExpertPablo RamirezОценок пока нет
- Book StickerДокумент4 страницыBook Stickerilanabiela90Оценок пока нет
- ID Faktor Faktor Yang Berhubungan Dengan Perilaku Berisiko Remaja Di Kota MakassarДокумент11 страницID Faktor Faktor Yang Berhubungan Dengan Perilaku Berisiko Remaja Di Kota MakassarEva VidiaОценок пока нет
- 7 DR BookletДокумент13 страниц7 DR BookletDebraОценок пока нет
- Laboratory Result Report: Requested Test Result Units Reference Value Method ImmunologyДокумент1 страницаLaboratory Result Report: Requested Test Result Units Reference Value Method ImmunologyYaya ZakariaОценок пока нет
- Construction of Magic Soak Pit With Locally Available Materials and Economical DesignДокумент4 страницыConstruction of Magic Soak Pit With Locally Available Materials and Economical DesignInternational Journal of Innovative Science and Research TechnologyОценок пока нет
- Formularium 2018 AДокумент213 страницFormularium 2018 Asupril anshariОценок пока нет
- BDSM Checklist: General InformationДокумент6 страницBDSM Checklist: General Informationmiri100% (1)
- Care of The Hospitalized ChildДокумент60 страницCare of The Hospitalized ChildJSeasharkОценок пока нет
- Blood TypingДокумент11 страницBlood Typingprakash gusainОценок пока нет
- Villegas Lucero 1Документ8 страницVillegas Lucero 1api-213921706Оценок пока нет
- Letter To ProfessorДокумент3 страницыLetter To ProfessorAlannaОценок пока нет
- FA Form No2-Visa Application FormДокумент1 страницаFA Form No2-Visa Application FormacademydonutОценок пока нет
- Job Application LetterДокумент12 страницJob Application LetterIcha Aisah100% (3)
- Endo Gia Curved Tip Reload With Tri StapleДокумент4 страницыEndo Gia Curved Tip Reload With Tri StapleAntiGeekОценок пока нет
- Health 10: 3 Quarter Week 7Документ10 страницHealth 10: 3 Quarter Week 7Maria Rose Tariga Aquino50% (2)
- Mental Health Awareness SpeechДокумент2 страницыMental Health Awareness SpeechThea Angela Longino95% (20)
- Intr On: State LifeДокумент27 страницIntr On: State LifeSarfraz AliОценок пока нет
- MBA Students Habit Toward ToothpasteДокумент29 страницMBA Students Habit Toward ToothpasteSunil Kumar MistriОценок пока нет
- Bed Making LectureДокумент13 страницBed Making LectureYnaffit Alteza Untal67% (3)