Академический Документы
Профессиональный Документы
Культура Документы
Management of Arterial Line
Загружено:
Farcasanu Liana GeorgianaАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Management of Arterial Line
Загружено:
Farcasanu Liana GeorgianaАвторское право:
Доступные форматы
Review date: October 2011
Page 1 of 16
Management of Arterial Lines
TCP 211
GUIDELINES FOR THE MANAGEMENT OF ARTERIAL LINES
TCP 211
CROSS REFERENCE
This Strategy/ Policy should be read in
conjunction with:
TCP 113 Aseptic Non Touch Technique
(ANTT) Protocol
TCP 169 Policy for the Quality
Assessment of Blood Gas Analysers
TCP 185 Guidelines for the Management
of Transduced Central Venous Pressure
(CVP) Lines
Progress and date of approval
(Approved / Under review)
January 2009
Under review
July 2006
Manager Responsible
Principle Lead Consultant for Critical Care
Author
Critical Care Clinical Governance Lead
Date
February 2009
Policy Number
TCP 211
Previous code
N/A
Version number
Approving Committee
Trustwide Clinical Policies
Signed by Chair of the Committee
Review Date
Trustwide Clinical Policies Committee
October 2011
Review date: October 2011
Page 2 of 16
Management of Arterial Lines
TCP 211
Consultation and Ratification Schedule
Name of Committee
Trustwide Clinical Policies
Date of Committee
February 2009
Name of Person / Team
Date
Trustwide Clinical Policies Committee
Review date: October 2011
Page 3 of 16
CONTENTS
1.0 Policy Statement
2.0 Key Principles
3.0 Scope
4.0 Responsibilities
5.0 Monitoring for Effectiveness
6.0 Clinical Indication and Documentation
7.0 Insertion of arterial lines
8.0 Arterial line labelling
9.0 Arterial line fluid prescription
10.0 The transducer
11.0 Setting up the transducer
12.0 Care of the line and transducer
13.0 Arterial blood gas sampling
14.0 Arterial blood gas measurements
15.0 Causes of Inaccurate Readings or Measurements
16.0 Removal of arterial lines
17.0 Bibliography
18.0 Appendix 1
Trustwide Clinical Policies Committee
Management of Arterial Lines
TCP 211
Review date: October 2011
Page 4 of 16
Management of Arterial Lines
TCP 211
1. POLICY STATEMENT
1. 1
Recent Recommendations from the National Patient Safety Agency recommend
the development of guidelines for the management of arterial lines.
2. KEY PRINCIPLES
2.1
Arterial lines are routinely used in critical care areas for monitoring arterial blood
pressure or serial blood gas measurements. This guidance applies to all staff in
critical care, theatres and other areas such as the Emergency Department where
arterial lines are inserted and managed. Patients should not be nursed outside
these areas with arterial lines in order to avoid complications of insertion such as:
Ischaemia
Bleeding
Accidental intra-arterial administration of drugs
Nerve trauma
3. SCOPE
3.1
3.2
This policy applies to all Staff
The policy is applicable within the Trust
4. RESPONSIBILITIES
4.1
Responsibility of the Trust Board
The Trust Board delegates authority for approving this policy to the Trustwide
Clinical Policies Committee
4.2
Responsibilities of Assistant Director, Clinical Governance/Head of
Modern Matrons
To ensure the policy is reviewed
4.3
Responsibilities of Clinical Governance/Audit Lead Clinicians for Critical Care
To ensure the policy is audited annually and undertake further steps to ensure
compliance with the policy
5. MONITORING FOR EFFECTIVENESS OF POLICY
5.1
The use of the guidelines will be audited by the department of critical care.
Compliance with the guidelines will be audited annually in all critical care
areas by medical and nursing staff
This will be feedback to the relevant areas at Trust Clinical governance
meetings
Trustwide Clinical Policies Committee
Review date: October 2011
Page 5 of 16
Management of Arterial Lines
TCP 211
6. DOCUMENTATION OF CLINICAL NEED FOR INSERTION
6.1
Arterial lines and arterial blood gas sampling can be associated with morbidity
and mortality and so the clinical indication for the insertion of an arterial line
should be documented.
6.2
Indications for the insertion of arterial lines include:
6.2.1 Continuous arterial pressure monitoring:
Haemodynamically unstable patients
Patients on vasopressor or vasodilator drugs
Cardiopulmonary bypass
Major vascular, thoracic, abdominal or neurologic surgical procedures
Patients supported on an intra-aortic balloon pump (IABP)
Patients receiving intracranial pressure monitoring
6.2.2 Serial blood gas measurements:
Patients in respiratory failure
Patients being maintained on or being weaned from mechanical ventilatory
support
Patients with severe acid/base abnormalities
Where frequent blood samples are required to measure electrolyte
concentrations.
7. INSERTION OF ARTERIAL LINES
7.1
Suitable sites for the insertion of arterial lines include the radial, brachial, femoral,
dorsalis pedis and axillary arteries.
7.2
The arterial line must be inserted by a doctor or other practitioner competent in
the procedure. If the radial artery is selected the operator may perform an Allen
test to assess peripheral limb perfusion distal to the proposed arterial cannula
site prior to insertion.
Practice
1. Explain and discuss procedure with
patient
2. Doctor and assistant wash hands and
put on gloves and plastic apron. Facial
protection must be worn when there is a
risk of splashing
3. Prepare cannulation site, remove hair if
necessary. Clean skin with 2% alcoholic
chlorhexidine skin cleanser. Place
disposable pad under limb. Aseptic non-
Trustwide Clinical Policies Committee
Rationale
2. Prevents transmission of microorganisms
Review date: October 2011
Page 6 of 16
touch technique must be used at all times
to prevent cross infection and
contamination of site.
4. Infiltrate cannulation site with local
anaesthetic and leave to take effect
5. Nurse may need to immobilise limb.
6. Cannula inserted
7. Apply pressure to cannulated artery
whilst transducer line is securely attached.
8. Secure cannula using Tegaderm
dressing. Secure tubing safely to limb.
9. Remove gloves, apron and if
appropriate facial protections and dispose
of as clinical waste.
10. Decontaminate hands
Management of Arterial Lines
TCP 211
4. Minimise pain during procedure, so
facilitating patient co-operation.
5. Facilitate cannulation.
7. Prevents blood spillage
8. Allow visualisation of insertion site.
9. Prevents transmission of microorganism
8. IDENTIFICATION OF ARTERIAL LINES
8.1
An appropriate red line connection should be used to clearly indicate that the line
is arterial.
8.2
The arterial line must be clearly labelled with a red sticker.
9. ARTERIAL LINE FLUID PRESCRIPTION
9.1
Appropriate fluids must be used. Normal saline +/ - heparin. I unit heparin per ml
of fluid must be used.
9.2
Patients with a current or previous diagnosis of Heparin Induced
Thrombocytopenia should only be prescribed Normal saline as arterial line fluid.
9.3
The arterial line fluid must be prescribed on the patients drug chart or Clinical
Information System (CIS).
9.4
The fluid must be checked by two registered practitioners before it is connected
to the arterial line.
10. THE TRANSDUCER SYSTEM
The measurement of a patients blood pressure with a pressure transducer involves the
arterial cannula being connected to a pressurized line. The pressures in the cannula are
transmitted through fluid filled tubing to the transducer diaphragm.
The movement of the diaphragm is converted to a low voltage electrical signal. The
signal is amplified and converted to a real-time waveform display on the monitor. The
measurements are then digitally displayed in mmHg.
Trustwide Clinical Policies Committee
Review date: October 2011
Page 7 of 16
Management of Arterial Lines
TCP 211
11. SETTING UP THE TRANSDUCER
Practice
1. Before and after handling any
intravenous equipment the hands
should be decontaminated with soap
and water or alcoholic hand rub. Put
on gloves and apron.
2. The transducer should be removed
from its package and the Luer
connections checked for tightness.
3. The extension kits to allow blood
sampling should be as short as
possible.
4. A bag of 0.9% sodium chloride or
heparinised saline should be attached
to the transducer set.
5. The fluid bag label should be
clearly visible through the pressure
bags.
6. Label the system when set up with
date and time.
7. The drip chamber should be
squeezed gently to fill only the bottom
of the chamber.
8. To prime the set pull the small cord
on the plastic transducer.
9. When the set is primed the
pressure bag should be fitted and
inflated to 300mmHg.
Trustwide Clinical Policies Committee
Rationale
1. Significantly reduces the number of
pathogens on the hands (Larson
1995).
2. The connections can be loosely
packed.
3. Long extensions alter the pressure
reading
6. To ensure it is changed as per
protocol.
7. When the bag is pressurized the
drip chamber will fill higher.
9. At this pressure 3 to 4 mls/hr of
0.9% sodium chloride or heparinised
saline will pass through the flush
device to keep the line patent.
Review date: October 2011
Page 8 of 16
10. The pressure lines should be
examined for air bubbles. If found
they can be removed by
flushing or gently tapping the set.
11. All connections should be
swabbed with a 2% PDI wipe for 30
seconds then allow to dry.
12. Connect the line to the arterial
catheter using a non-touch technique.
The line is then labelled with the time
and date.
13.Needle free connectors for
example, red swanlocks are
recommended for the blood sampling
port and should be changed weekly
unless the device is changed
14. The transducer should be fitted
into its holder on the drip stand,
levelled to the patients sternal notch
or foramen magnum (neuro) and the
electrical lead connected to the
monitor by the bedside.
15. The transducer should be opened
to air and zeroed to atmospheric
pressure. Open the port on the
transducer and zero on the monitor
menu at least once per shift prior to
taking a reading
16. The pre-connected bungs on the
zero port of the transducer should be
changed for either the white bungs
provided in the set or red bungs (not
swanlocks).
17. Re-level the transducer each time
the patient changes position or the
bed is raised or lowered.
18. Check that the arterial trace is
satisfactorily displayed on the
monitor.
19.Remove gloves, apron and if
appropriate facial protections and
dispose of as clinical waste.
20. Decontaminate hands
Trustwide Clinical Policies Committee
Management of Arterial Lines
TCP 211
10. All air must be removed to
prevent dampening of the arterial
waveform.
11. Reduces the possibility of
bacterial
contamination.
12. Reduces bacterial contamination
and protection of patient and yourself.
14. To get an accurate reference
point.
16. Air can entrain into the transducer
and alter the pressure reading and/or
water can leak from the hole in the
pre-connected bungs which are
intended for initial zeroing only.
17. To ensure a consistent zero
reference point.
18. This makes sure that the line is
patent and the readings should be
accurate.
Review date: October 2011
Page 9 of 16
Management of Arterial Lines
TCP 211
12. CARE OF THE LINE AND THE TRANSDUCER
Practice
1. Care must be taken to ensure that
the arterial line does not become
disconnected.
2. The waveform should be
continuously displayed
3. The arterial line fluid should be
checked against the prescription once
per nursing shift.
4. Every third day the transducer and
flush bag should be either changed or
taken down if no longer required (see
label for date).
5. The cannula does not need regular
flushing while on a pressure bag
system, but a flush may be required
to gain an arterial trace. The cannula
can be flushed with the manual fast
flush device.
6. The pressurized flush bag should
be maintained at a pressure of
300mmHg.
If the waveform changes check the
pressure.
7. The flush bag should be changed
with the transducer or when empty.
8. Maintain a closed system ensuring
minimal disconnection in the circuit.
9. Handwashing must be performed
and personal protective equipment
applied before cleaning the catheter
site.
10.Chloraprep or Clinnell wipes
MUST be used to clean the catheter
site during dressing changes and
allow to air dry.
11. Prior to securing the line it should
be curled in a U to prevent any
direct pull on the line
12. The site should be secured with a
sterile, moisture permeable, dressing
e.g. Tegaderm
Dressings should only be changed
when soiled or when the line is being
changed
13. If the catheter is not sutured,
Trustwide Clinical Policies Committee
Rationale
1. As the line is in an artery and not a
vein the patient can potentially
exsanguinate.
2. The arterial trace should not be
under or over damped as this will
generate inaccurate readings
3. To ensure it is visible and correct.
4. To reduce the risk of contamination
and infection.
5. Ensuring a patent line and a good
waveform will provide an accurate
arterial pressure reading. A flush can
be used to test for dampness of the
arterial trace.
6. This will ensure that 4mls/hr of
0.9% sodium chloride or heparinised
saline will be delivered through the
cannula, thereby keeping it patent
and will maintain constant pressure
within the system.
7. To avoid contamination.
9. & 10.To reduce risk of infection
11. To reduce the risk of
dislodgement of the line
13. To ensure the cannula is not
Review date: October 2011
Page 10 of 16
renewal of dressings should be
preformed by 2 nurses.
14. The line should be observed for
signs of inflammation/ infection.
Changes should be reported to
medical staff.
Management of Arterial Lines
TCP 211
dislodged during the procedure
13. SAMPLING FROM THE ARTERIAL LINE
13.1
Staff should always ask themselves do I need to take this sample?
Indications include:
Changes in monitored respiratory variables e.g. oxygen saturation or tidal
volume
Monitoring of results of changes in ventilation
Monitoring of electrolytes
Monitoring of bleeding or coagulation tests
Monitoring acid/base abnormalities
13.2
Sampling from arterial lines should only be performed by staff competent in the
technique.
Procedure
1.Wash hands and apply gloves and
apron
2. Use non-touch technique at all times.
Clean port with 2% PDI wipe for 30
seconds; allow to dry prior to any
access. The port should have a RED
needleless valve and should also be
cleaned after use.
3. Mute alarm on monitor.
4. Connect 5 ml syringe to hub, turn port
on to artery, off to transducer. Withdraw
3 ml of blood, or until line is clear of
infusate.
5. Turn 3 way tap diagonally to close off
artery, port and transducer.
6. Connect either heparinised blood gas
syringe or vacutainer equipment and
withdraw blood slowly.
7. Turn 3 way tap off diagonally to
artery, port and transducer prior to
removing syringe/vacutainer.
8. Turn 3 way tap on to transducer and
artery and squeeze flush device
actuator to clear line completely of
blood.
9. Turn 3 way tap on to port and
Trustwide Clinical Policies Committee
Rationale
2. Reduce risk of infection
3. Prevent unnecessary noise
4. Prevent decontamination of blood
with infusate
5. Prevent back flow of blood from
artery and contamination with infusate
6. Prevent haemolysis and inaccurate
results
8. Blood is a rich culture medium and
so reduction of infection risk
Review date: October 2011
Page 11 of 16
Management of Arterial Lines
TCP 211
transducer and flush port clear of blood
into empty syringe packet, or piece of
sterile gauze.
10. Clean port with 2% PDI wipe.
11. Turn 3 way tap on to transducer and
artery.
12. Dispose of waste materials, remove
gloves and apron and wash hands
14. ARTERIAL BLOOD GAS MEASUREMENT
Blood gas analyser should only be used after or under the supervision of
someone suitably trained in its use.
14.1
Any air must be expelled immediately from the blood gas syringe as this will alter
the results
14.2
Blood gas syringes, other than those from critical care must have a clot catcher
attached attached before the blood is analysed
14.3
Results should be recorded either on the patients chart or electronic record
14.4
A brief guide to the interpretation of blood gas results is provided in Appendix 1,
but is no substitute for training and competency assessment.
14.5
Unexpected results should be discussed with the Shift leader or medical staff as
soon as possible and documented in the patients health records. The possibility
of contamination should always be considered.
15. CAUSES OF INACCURATE READINGS OR MEASUREMENTS
15.1
Pressures
System not levelled/zeroed
No fluid/ Pressure in flush bag
Wrong tubing used.
Bubbles in tubing
Limb or patient position
Cannula position
Arrhythmias
Size of cannula
15.2
Sample results
Air in syringe
Inadequate clearance of infusate
Wrong infusate and inadequate clearance
Delay in analysis
Haemolysis due to rapid withdrawal
Trustwide Clinical Policies Committee
Review date: October 2011
Page 12 of 16
Management of Arterial Lines
TCP 211
16.
REMOVAL OF ARTERIAL LINES
16.1
16.2
Arterial lines should be removed when no longer required.
As arterial pressure is greater than venous pressure a longer period of pressure
is required over the cannula site in order to prevent haematoma formation
Pressure must be applied aseptically over the site until there is no further
evidence of bleeding or tissue swelling.
16.3
17.
BIBLIOGRAPHY
Allan, D. 1984 Care of the patient with an arterial catheter. Nurs Times 1984, 80(46), 401
Bernsten AD, Soni N, Oh T E, 2003 Ohs Intensive Care Manual 5th Edition p80-81
Butterworth Heinemann
Brown J D et al. 1997 The potential for catheter microbial contamination from a
needleless connector. Journal of Hospital Infection. 36. 181-189.
Daily, E., & Schroeder, J. 1995. Techniques in bedside hemodynamic monitoring. (5th
ed). St Louis: Mosby
Darovic, G., Vanriper, J., & Vanriper, S. 1995. Arterial pressure monitoring. In Darovic,
G. (Ed.), Hemodynamic Monitoring: Invasive and noninvasive clinical application.
(pp.177-210). Philadelphia: W.B. Saunders Company
Department of Health (DoH), 2008. Clean, Safe Care Reducing Infections and Saving
Lives
EPIC (Evidence based Practice in Infection Control), 2007 National evidence-based
guidelines for preventing Healthcare-associated infections in NHS Hospitals in England,
Journal of Hospital Infection, 65s, S1-S64
Kirchhoff KT, Rebenson-Piano M, Patel MK 1984 Mean arterial pressure readings:
variations with positions and transducer level. Nurs Res. 1984 Nov-Dec; 33(6):343-5.
NPSA. 2008 Problems with infusions and sampling from arterial lines..
http://www.npsa.nhs.uk/nrls/alerts-and-directives/rapidrr/arterial-lines/
Pratt, R.J et al 2007. Epic 2; National Evidence-Based Guidelines for Preventing
Healthcare-Associated Infection in NHS Hospitals in England.
http://www.epic.tvu.ac.uk/PDF%20Files/epic2/epic2-final.pdf
Slogoff S, Keats As, Arlund C. 1983 On the safety of radial artery cannulation.
Anesthesiology 1983; 59:42-7
Trustwide Clinical Policies Committee
Review date: October 2011
Page 13 of 16
Management of Arterial Lines
TCP 211
Traor O, Liotier J, Souweine B. 2005 Prospective study of arterial and central venous
catheter colonization and of arterial- and central venous catheter-related bacteremia in
intensive care units. Crit Care Med. 2005 Jun; 33(6):1276-80
S1134 - UpToDate - Arterial catheterization.htm
Yentis SM, Hirsch NP, Smith GB. 2003 Anaesthesia and Intensive Care A-Z 3rd edition
p44 Butterworth Heinemann
Trustwide Clinical Policies Committee
Review date: October 2011
Page 14 of 16
Trustwide Clinical Policies Committee
Management of Arterial Lines
TCP 211
Review date: October 2011
Page 15 of 16
Management of Arterial Lines
TCP 211
18.0 APPENDIX 1: QUICK GUIDE TO ARTERIAL BLOOD GAS ANALYSIS
DO NOT TAKE THE PATIENT OFF OXYGEN
Look at the Pa02 and Fi02
Note the inspired oxygen % and flow rate and document on blood gas print out.
This allows a more accurate interpretation of the patients oxygen requirements in light of their present
oxygen need. For example a low Pa02 on high flow/percentage oxygen should trigger a senior medical
review for further management.
Look at the pH
< 7.35
> 7.45
ACIDOSIS
ALKALOSIS
Look at the C02 and Bicarbonate
pCO2 >
45 mmHg
or 6.0 kPa
Respiratory Acidosis
HCO3 < 22
Metabolic Acidosis
pCO2 < 35 mmHg
or 4.6 kPa
Respiratory Alkalosis
HCO3 > 22
Metabolic Alkalosis
Look for compensation
HCO3 > 22
Metabolic
compensation
pCO2 < 35 mmHg
or 4.6 kPa
Respiratory compensation
HC03 < 22
Metabolic
compensation
pCO2 > 45 mmHg
or 6.0 kPa
Respiratory compensation
Normal values
pH
Pa02
PaC02
Standard HC03
Base Excess
Lactate
Oxygen Saturations (Sa02)
7.35 7.45
80 100 mmHg or 10.6 13.3 kPa
35 45 mmHg or 4.6 6.0 kPa
22 26 mmol/litre
+2 to -2 mmols/litre
0.5 2.0 mmols/litre
95 100%
Document the ABG and your interpretation/management plan in the patients medical notes.
Further reading
Rhodes A and Cusack R J (2000) Arterial blood gas analysis and lactate. Current Opinion in Critical Care.
6:227-231.
Williams A J (1998) Assessing and interpreting arterial blood gases and acid-base balance. BMJ. Volume
317. Downloaded from bmj.com.
Driscoll P, Brown T, Gwinnutt C & Wardle T. (1997) A Simple Guide to Blood Gas Analysis. BMJ Publishing
Group.
DH/DB Critical Care Outreach Team 08/2008
Review date: October 2011
Page 16 of 16
Management of Arterial Lines
TCP 211
Equality IMPACT ASSESSMENT FORM (EIAF) Race, Gender, Religion/Belief,
Disability, Age and Sexual Orientation
Section One:
Screening / Prioritising for Full Impact Assessment
Name of the Policy Management of Arterial Lines
Is there public
concern that the
function/
policy is being
carried out in a
discriminatory
way?
Which of the 3
parts does it
apply to (if any)
1 Eliminating
discrimination?
2 Promoting
equal
opportunities?
3 Promoting good
community
relations?
Is there
evidence
or reason
to believe
that
some
groups
could be
differently
affected?
Which
groups
are
affected
How much
evidence
do you
have?
No
No
No
No
No
No
0-2 None
or little
3-4 Some
5-6
Substantial
Priority
(add
column
s 3 & 4)
0-2 None or little
3-4 Some
5-6 Substantial
RACE
RELIGION/
BELIEF
DISABILITY
MEN/WOMEN/
TRANSGENDER
AGE
SEXUAL
ORIENTATION
Вам также может понравиться
- Arterial Line Arterial LineДокумент13 страницArterial Line Arterial LineLinamaria Lozano100% (1)
- Tracheostomy Care - An Evidence-Based Guide - American Nurse TodayДокумент4 страницыTracheostomy Care - An Evidence-Based Guide - American Nurse TodayZulaikah Nur IstiqomahОценок пока нет
- A Nurse's Guide to Caring for Cardiac Intervention PatientsОт EverandA Nurse's Guide to Caring for Cardiac Intervention PatientsОценок пока нет
- Manual for Iv Therapy Procedures & Pain Management: Fourth EditionОт EverandManual for Iv Therapy Procedures & Pain Management: Fourth EditionОценок пока нет
- Mechanical Ventilation Practice Guidelines: 1. 2. Initial Settings - ModeДокумент12 страницMechanical Ventilation Practice Guidelines: 1. 2. Initial Settings - ModeGayathri RОценок пока нет
- NIV Pediatric Respiratory SupportДокумент96 страницNIV Pediatric Respiratory SupportbhongskirnОценок пока нет
- Hepatic Encephalopathy and ComaДокумент19 страницHepatic Encephalopathy and ComaJas Castro JoveroОценок пока нет
- Management of The EVDДокумент7 страницManagement of The EVDplethoraldork100% (1)
- Burns Assessment and ManagementДокумент33 страницыBurns Assessment and ManagementErina Erichan Oto100% (1)
- Blood Gas Analysis For Bedside DiagnosisДокумент6 страницBlood Gas Analysis For Bedside DiagnosisMuhamad Wirawan AdityoОценок пока нет
- Assisting Central Venous Catheter (CVC) Insertion (Procedure1)Документ7 страницAssisting Central Venous Catheter (CVC) Insertion (Procedure1)BsBs A7medОценок пока нет
- Liverpool SDL CRRTДокумент62 страницыLiverpool SDL CRRTupul85Оценок пока нет
- Cardiac MonitorДокумент4 страницыCardiac MonitorFahyesha MaulaniОценок пока нет
- Patient Education for Ileal Conduit CareДокумент11 страницPatient Education for Ileal Conduit CareICa MarlinaОценок пока нет
- CPR - Cardiopulmonary ResuscitationДокумент31 страницаCPR - Cardiopulmonary ResuscitationPanji HerlambangОценок пока нет
- Medical Surgical Nursing Suretech College of NursingДокумент18 страницMedical Surgical Nursing Suretech College of NursingSanket TelangОценок пока нет
- ICU TriageДокумент27 страницICU TriageAkmal FahrezzyОценок пока нет
- IV Fluid ChartДокумент2 страницыIV Fluid Charthady920Оценок пока нет
- Airway and VentilationДокумент36 страницAirway and Ventilationmasoom bahaОценок пока нет
- Presus Interactive Lecture Handout - September 2015Документ4 страницыPresus Interactive Lecture Handout - September 2015api-317814049Оценок пока нет
- Arterial Lines in PACU: Presented by Autum Jacobs RN, BSNДокумент34 страницыArterial Lines in PACU: Presented by Autum Jacobs RN, BSNinuko1212Оценок пока нет
- Cardiac CatheterizationДокумент3 страницыCardiac CatheterizationAmir ZiadОценок пока нет
- Necrotizing Otitis 2022Документ20 страницNecrotizing Otitis 2022asmashОценок пока нет
- TXTДокумент356 страницTXTJec AmracОценок пока нет
- DialysisДокумент20 страницDialysisSiwani rai100% (1)
- Med SurgДокумент9 страницMed SurgCharlie Gemarino LumasagОценок пока нет
- Ventilator, Weaning, SuctioningДокумент81 страницаVentilator, Weaning, SuctioningwaqarОценок пока нет
- OxygenationДокумент50 страницOxygenationLulu MushiОценок пока нет
- NIV Fs 9108147 e 1911 1 PDFДокумент4 страницыNIV Fs 9108147 e 1911 1 PDFliuchenshitaoОценок пока нет
- Addis Ababa University Faculty of Medicine Difficult Airway ManagementДокумент54 страницыAddis Ababa University Faculty of Medicine Difficult Airway ManagementagatakassaОценок пока нет
- Central Venous Pressure (CVP)Документ38 страницCentral Venous Pressure (CVP)Kimberly Abella CabreraОценок пока нет
- Infant Radiant WarmerДокумент7 страницInfant Radiant WarmerManish MandaviyaОценок пока нет
- Advanced Airway Care: Intensive Care Unit PerspectiveДокумент42 страницыAdvanced Airway Care: Intensive Care Unit PerspectiveJeffery Samuel100% (1)
- Arterial Puncture and CannulationДокумент19 страницArterial Puncture and CannulationAzizah Rahawarin100% (1)
- Rapid Sequence InductionДокумент8 страницRapid Sequence InductionAngela Mitchelle NyanganОценок пока нет
- Sinus Bradycardia: I. Sinus Dysrhythmias Description ManagementДокумент4 страницыSinus Bradycardia: I. Sinus Dysrhythmias Description ManagementMargueretti Delos ReyesОценок пока нет
- Neurologica L Assessment: Lijo Joseph Msc. Nursing Ist YrДокумент38 страницNeurologica L Assessment: Lijo Joseph Msc. Nursing Ist YrBibi Renu100% (2)
- ps52 2015 Guidelines For Transport of Critically Ill Patients PDFДокумент12 страницps52 2015 Guidelines For Transport of Critically Ill Patients PDFPalwasha MalikОценок пока нет
- ECGДокумент154 страницыECGSandeep BansalОценок пока нет
- Temperature RegulationДокумент23 страницыTemperature Regulationapi-3805717100% (2)
- Basics of Waveform Interpretation: RET 2284 Principles of Mechanical VentilationДокумент66 страницBasics of Waveform Interpretation: RET 2284 Principles of Mechanical VentilationNanda MinndinОценок пока нет
- RSI For Nurses ICUДокумент107 страницRSI For Nurses ICUAshraf HusseinОценок пока нет
- Arterial Line Monitoring GuideДокумент13 страницArterial Line Monitoring GuideberhanubedassaОценок пока нет
- Neonatal Transition: Training of The Trainers Neonatal ResuscitationДокумент36 страницNeonatal Transition: Training of The Trainers Neonatal ResuscitationmitaОценок пока нет
- Medication Administration Via Enteral Tube Feeding GuideДокумент31 страницаMedication Administration Via Enteral Tube Feeding GuideSara Aly YoussefОценок пока нет
- Mechanical Ventilation and Intracranial PressureДокумент30 страницMechanical Ventilation and Intracranial PressureFlavius AnghelОценок пока нет
- Plasmapheresis Procedure Removes Antibodies From BloodstreamДокумент13 страницPlasmapheresis Procedure Removes Antibodies From BloodstreamSampath GoudОценок пока нет
- Intraoperative CareДокумент5 страницIntraoperative CareraffineeОценок пока нет
- Suctioning Artificial Airways - AdultsДокумент27 страницSuctioning Artificial Airways - AdultssdaОценок пока нет
- Mechanical Ventilation For NursingДокумент55 страницMechanical Ventilation For NursingAmira AttyaОценок пока нет
- 2020 Neonata Lcare PDFДокумент20 страниц2020 Neonata Lcare PDFserigne badianeОценок пока нет
- Phlebitis and ThrombophlebitisДокумент27 страницPhlebitis and ThrombophlebitisMaría Fernanda RíosОценок пока нет
- Saudi Nursing Lisencure Examination Applicant GuideДокумент16 страницSaudi Nursing Lisencure Examination Applicant GuideSomaya SiddiqueОценок пока нет
- Central Venous PressureДокумент10 страницCentral Venous PressureAngelo ArquizaОценок пока нет
- Patient SafetyДокумент18 страницPatient SafetySuhatman AhОценок пока нет
- Operating Room Preparation: Philipp Acaso Ralph ArcoДокумент158 страницOperating Room Preparation: Philipp Acaso Ralph ArcoTiffany Luv Adrias100% (1)
- Ebstein Anomaly, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОт EverandEbstein Anomaly, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОценок пока нет
- A Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsОт EverandA Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsОценок пока нет
- Guidelines For Enteral Feeding in Adult Hospital Patients 2Документ12 страницGuidelines For Enteral Feeding in Adult Hospital Patients 2Farcasanu Liana GeorgianaОценок пока нет
- CG3 - Administration of Medicine GuidelinesДокумент7 страницCG3 - Administration of Medicine GuidelinesFarcasanu Liana GeorgianaОценок пока нет
- Arterial Line Blood SamplingДокумент14 страницArterial Line Blood SamplingFarcasanu Liana GeorgianaОценок пока нет
- Admin Blood Components BCSH 05012010 PDFДокумент59 страницAdmin Blood Components BCSH 05012010 PDFFarcasanu Liana GeorgianaОценок пока нет
- Research in Social and Administrative PharmacyДокумент4 страницыResearch in Social and Administrative PharmacyAndrea MendozaОценок пока нет
- Bio Research ProjectДокумент12 страницBio Research Projectapi-428108720Оценок пока нет
- Managing The Health Insurance PortfolioДокумент3 страницыManaging The Health Insurance PortfolioShantanuОценок пока нет
- Aorn Laser SafetyДокумент16 страницAorn Laser SafetyAmanda RapaОценок пока нет
- Alprazolam PoisoningДокумент4 страницыAlprazolam PoisoningRahmat AkmalОценок пока нет
- Non-Disclosure Agreement (Healthcare)Документ2 страницыNon-Disclosure Agreement (Healthcare)Clarebeth Recaña Ramos100% (1)
- Alterations With Infectious, Inflammatory and Immunologic ResponsesДокумент8 страницAlterations With Infectious, Inflammatory and Immunologic ResponsesPATRIZJA YSABEL REYESОценок пока нет
- How To Fill ADR Reporitng Form and Causality AssessmentДокумент38 страницHow To Fill ADR Reporitng Form and Causality AssessmentVishal AryaОценок пока нет
- New Hanover County 2024-28 Five-Year Strategic PlanДокумент2 страницыNew Hanover County 2024-28 Five-Year Strategic PlanJamie BouletОценок пока нет
- Overview of Neuropathic Pain: DR Tay Kwang Hui Dept of Anaesthesia, NUHS 8 Jan 2011Документ37 страницOverview of Neuropathic Pain: DR Tay Kwang Hui Dept of Anaesthesia, NUHS 8 Jan 2011CaioSelaimenОценок пока нет
- Nursing Student Cover LetterДокумент8 страницNursing Student Cover Letterafmrpaxgfqdkor100% (1)
- 2009 HESI Practice - FundamentalsДокумент14 страниц2009 HESI Practice - FundamentalsQueennita100% (1)
- Course Details: Assessment Task SITXINV002 Maintain The Quality of Perishable Items Page 1 of 9Документ9 страницCourse Details: Assessment Task SITXINV002 Maintain The Quality of Perishable Items Page 1 of 9Boban GorgievОценок пока нет
- Eastern Connecticut State University Informed Consent Form: Participant's Printed NameДокумент4 страницыEastern Connecticut State University Informed Consent Form: Participant's Printed NameKisu Hive GamesОценок пока нет
- Pediculosis: Pubis (Pubic Louse)Документ4 страницыPediculosis: Pubis (Pubic Louse)christian quiaoitОценок пока нет
- Food Worksheet Go Grow and Glow Foods Worksheet Grade 1 WAKДокумент2 страницыFood Worksheet Go Grow and Glow Foods Worksheet Grade 1 WAKdawn100% (4)
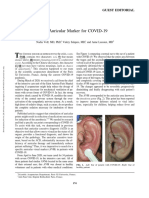
- An Auricular Marker For Covid-19: Nadia Volf, MD, PHD, Valery Salques, MD, and Anne Lassaux, MDДокумент2 страницыAn Auricular Marker For Covid-19: Nadia Volf, MD, PHD, Valery Salques, MD, and Anne Lassaux, MDyan92120Оценок пока нет
- Task+3+ +threadwormsДокумент2 страницыTask+3+ +threadwormsVin MenesesОценок пока нет
- Employee AbsenteeismДокумент13 страницEmployee AbsenteeismManuel KevogoОценок пока нет
- EДокумент375 страницEANA MARIA CRISTIANAОценок пока нет
- 2.11 SEPTIC ABORTION AND SEPTIC SHOCK. M. Botes PDFДокумент4 страницы2.11 SEPTIC ABORTION AND SEPTIC SHOCK. M. Botes PDFteteh_thikeuОценок пока нет
- Scenr Chairman Decision (8) of 2006Документ14 страницScenr Chairman Decision (8) of 2006jerin sam kurianОценок пока нет
- WB CE Act Registration RegulationДокумент42 страницыWB CE Act Registration RegulationDipak Ranjan MukherjeeОценок пока нет
- NephritisДокумент21 страницаNephritisruchikaОценок пока нет
- Plan de Nutritie in HipotiroidismДокумент48 страницPlan de Nutritie in Hipotiroidismalbinuta100% (1)
- PPE Use, Disposal & Recycling SurveyДокумент2 страницыPPE Use, Disposal & Recycling SurveySamantha DomileОценок пока нет
- First Aid: NSTP 002Документ5 страницFirst Aid: NSTP 002Alvin VelasquezОценок пока нет
- Lesson PlanДокумент7 страницLesson PlanMr. khanОценок пока нет
- PEDIATRIC AUDIOLOGY WEEKLY TOPICSДокумент3 страницыPEDIATRIC AUDIOLOGY WEEKLY TOPICSAhiawortor KplorlaОценок пока нет
- Ebola Virus HOMEOPHATYДокумент3 страницыEbola Virus HOMEOPHATYgiopscribdОценок пока нет