Академический Документы
Профессиональный Документы
Культура Документы
Kiss of Death PDF
Загружено:
Flavia ElenaОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Kiss of Death PDF
Загружено:
Flavia ElenaАвторское право:
Доступные форматы
The
n e w e ng l a n d j o u r na l
of
m e dic i n e
clinical problem-solving
Kiss of Death
Brian B. Graham, M.D., Daniel R. Kaul, M.D., Sanjay Saint, M.D., M.P.H.,
and William J. Janssen, M.D.
In this Journal feature, information about a real patient is presented in stages (boldface type)
to an expert clinician, who responds to the information, sharing his or her reasoning with
the reader (regular type). The authors commentary follows.
From the Department of Medicine, Division of Pulmonary Sciences and Critical
Care Medicine, University of Colorado
Health Sciences Center, Denver (B.B.G.,
W.J.J.); the Division of Infectious Disease
(D.R.K.), Department of Internal Medicine (S.S.), and Department of Veterans
Affairs Health Services Research and Development Center of Excellence and Department of Medicine (S.S.) all at the
University of Michigan, Ann Arbor; and
the Department of Medicine, National Jewish Medical and Research Center, Denver
(W.J.J.). Address reprint requests to Dr.
Graham at the University of Colorado
Health Sciences Center, 4200 E. 9th Ave.,
Box C-272, Denver, CO, 80262, or at brian.
graham@uchsc.edu.
N Engl J Med 2009;360:2564-8.
Copyright 2009 Massachusetts Medical Society.
A 23-year-old South African man presented to an emergency department with a 2-day
history of fever, mild dyspnea, headache, nausea, and myalgias. His symptoms had
begun 5 days after he had traveled to Colorado to ski with friends. He was thought to
have a viral illness, was treated with intravenous fluids, and was discharged with a
prescription for acetaminophenhydrocodone. After 2 days, his symptoms worsened
and he returned to the emergency department. A chest radiograph was clear, and he
was treated with intravenous fluids and ibuprofen, again without relief. The following day, he returned to the emergency department with vomiting, dyspnea, and photophobia. He was admitted to the hospital for further evaluation and treatment.
This active young patient presents with nonspecific symptoms that have not improved with treatment. The fever suggests an infectious cause, and the presence of
photophobia raises a concern about meningitis. Bacterial meningitis, however, would
be expected to progress more rapidly. Travelers on crowded airplanes may be exposed to various pathogens (e.g., influenza virus and other viruses), and resulting
infections may not improve rapidly. Pulmonary embolism should be considered,
given the patients recent travel and dyspnea, but this condition would not generally result in photophobia, myalgias, or vomiting. Altitude sickness can cause headaches, nausea, and malaise, but it generally occurs within 24 hours after ascent. At this
point, the patient has undergone three evaluations in the emergency department, and
his condition is worsening. I agree with the decision to admit him to the hospital.
The patient had previously been healthy, took no medications, and had no known
drug allergies. Several of his family members had hypertension. His father had recently recovered from African tick-bite fever. The patient reported that he did not
smoke and did not use recreational drugs. He drank alcohol socially and reported
intermittent binge drinking. He was sexually active and had had more than 15 sexual
partners in his lifetime. The patient was born and lived on the west coast of South
Africa. He worked as a consultant and had traveled extensively the preceding year,
with trips to Mozambique, the United Arab Emirates, Canada, and Japan. He had recently driven across South Africa in an uncovered vehicle.
The patients drive across South Africa, in particular, exposed him to a number of
agents that might lead to a febrile illness. Among vectorborne diseases, malaria may
have an extended incubation period (as long as 3 months for Plasmodium falciparum
malaria) and typically presents as an undifferentiated febrile illness. Rickettsial diseases such as murine typhus and diseases caused by Rickettsia conorii and R. africae
tend to have a shorter incubation period (usually 7 to 14 days) and may be difficult
to distinguish clinically from malaria with the exception that R. conorii and R. africae
2564
n engl j med 360;24 nejm.org june 11, 2009
Downloaded from cme.nejm.org by DR. SIMONA RUTA on June 10, 2009 .
Copyright 2009 Massachusetts Medical Society. All rights reserved.
clinical problem-solving
infections may present with a rash or a black eschar (tache noire) at the bite site. Dengue and tickborne relapsing fever should also be considered,
since the patient may have been infected with a
pathogen just before traveling to the United States.
Typhoid fever, which is not always characterized
by diarrhea, is another possibility. The patients
sexual history mandates testing for the human
immunodeficiency virus (HIV), since acute HIV
infection or later-stage disease complicated by an
opportunistic infection could explain his presentation. Although the patient does not report a sore
throat, acute infection with cytomegalovirus
(CMV) or EpsteinBarr virus (EBV) is common in
young people and should be considered.
liter; aspartate aminotransferase level, 354 U per
liter (normal range, 0 to 47); alanine amino
transferase level, 197 U per liter (normal range,
0 to 47); alkaline phosphatase level, 73 U per liter
(normal range, 39 to 117); and total bilirubin level,
0.7 mg per deciliter (12.0 mol per liter; normal
range, 0.0 to 1.3 mg per deciliter [0.0 to 22.2 mol
per liter]). The international normalized ratio (INR)
was 1.0. A lumbar puncture showed 1 white cell
per cubic millimeter (a lymphocyte) and 2 red cells
per cubic millimeter; the glucose level was 57 mg
per deciliter (3.2 mmol per liter), and the protein
level was 56 mg per deciliter. Blood cultures were
obtained.
The left shift suggests infection. The absence of
reactive lymphocytes makes infection with CMV
or EBV unlikely. The elevated aminotransferase
levels may be caused by a rickettsial infection, a
viral infection, or malaria, although the normal
bilirubin level makes malaria unlikely. The protein level is slightly elevated, but the results of
cerebrospinal fluid analysis are otherwise normal. In this patient, disease acquired in Africa as
well as more routine causes of infection must be
considered. Further testing should include blood
smears to rule out malaria, blood cultures to rule
out Staphylococcus aureus infection and typhoid fever, a nasopharyngeal swab to rule out respiratory viral infections such as influenza, and seroSepsis appears to be likely, although dehydration logic tests for CMV infection, EBV infection,
from fever and vomiting could also explain some rickettsial diseases, and viral hepatitis.
of the patients symptoms. Blood cultures should
be obtained, and broad-spectrum antibiotics The patient was given intravenous fluids and antishould be considered. The absence of nuchal rigid- pyretic agents. The next day, he remained episodiity makes bacterial meningitis unlikely; neverthe- cally febrile, with temperatures as high as 38.9C.
less, it seems reasonable to perform a lumbar punc- The creatinine level decreased to 1.3 mg per deciliture, given the patients photophobia. Although ter (115 mol per liter), but the aspartate amina rash may be absent in some cases of rickettsial otransferase level increased to 701 U per liter and
diseases, an eschar is typically seen at the site of the alanine aminotransferase level increased to
inoculation; the absence of an eschar in this pa- 326 U per liter. The platelet count decreased to
tient makes infection with R. conorii or R. africae 76,000 per cubic millimeter, and the white-cell
unlikely.
count decreased to 3000 per cubic millimeter. The
blood cultures obtained at admission were negaNo previous laboratory-test results were available. tive, and a blood smear was negative for plasmoThe patients white-cell count was 9100 per cubic dium organisms. Empirical antimicrobial therapy
millimeter. A manual differential cell count re- with doxycycline was initiated. Urinary toxicologic
vealed 50% polymorphonuclear cells, 42% bands, screening was negative for alcohol and drugs, and
4% lymphocytes, and 4% monocytes. The hemo- a serum acetaminophen level was undetectable.
globin level was 16.7 g per deciliter, and the plate- Tests for hepatitis C antibody, hepatitis B surface
let count was 123,000 per cubic millimeter. The antigen, hepatitis B core antibody, and hepatitis A
serum creatinine level was 1.4 mg per deciliter antibody were negative, as were tests for antibod(124 mol per liter); albumin level, 3.9 g per deci ies against CMV and HIV types 1 and 2 and seroThe patient appeared ill. He had a temperature of
38.8C, a blood pressure of 96/50 mm Hg, and a
heart rate of 104 beats per minute. The respiratory
rate was 16 breaths per minute, and the oxygen
saturation was 95% while the patient was breathing ambient air. His conjunctiva were injected but
without icterus. There was mild oropharyngeal
erythema, but no oral ulcers or lesions were present. He had no nuchal rigidity. His chest was clear
on auscultation. The abdomen was soft and nontender, without hepatosplenomegaly. No rash or
edema was observed. The remainder of the physical examination was normal.
n engl j med 360;24 nejm.org june 11, 2009
Downloaded from cme.nejm.org by DR. SIMONA RUTA on June 10, 2009 .
Copyright 2009 Massachusetts Medical Society. All rights reserved.
2565
The
n e w e ng l a n d j o u r na l
logic tests for leptospirosis, EBV, Rocky Mountain
spotted fever, typhus, and Q fever.
On day 5 of the patients hospitalization, the
antibiotic regimen was broadened to include levofloxacin, vancomycin, and acyclovir. Liver-function
values continued to increase; on hospital day 6,
the aspartate aminotransferase level was 13,280 U
per liter; the alanine aminotransferase level, 2920
U per liter; the bilirubin level, 4.0 mg per deciliter
(68.4 g per liter); and the INR, 2.4. The patients
mental status declined. He had a generalized tonicclonic seizure that responded to lorazepam.
He underwent orotracheal intubation for airway
protection and was transferred to a tertiary care
hospital for further evaluation and possible liver
transplantation.
The patient appears to have fulminant hepatic
failure. The development of encephalopathy is of
great concern, and coupled with the increasing
INR, it may necessitate urgent liver transplantation. Acute liver failure is most commonly due to
infection (usually hepatitis A or B infection) or
drugs or other toxins (with acetaminophen being
the most common). Less common causes of acute
liver failure include Wilsons disease, autoimmune
hepatitis, and ischemic injury. The hepatitis E virus, which is either waterborne or foodborne,
causes more severe inflammation than the hepatitis A virus, but it is more common in Asia than
in southern Africa. Herpesviruses can also cause
fulminant hepatic failure. The tests for CMV and
EBV are negative, but infection with herpes simplex virus (HSV) or varicellazoster virus (VZV) is
possible. These infections can occur in immuno
competent patients, and skin lesions may be few
or absent. At this point, I would perform serologic tests for hepatitis E virus, HSV, and VZV,
and I would carefully examine the skin for any
lesions suggestive of HSV or VZV infection. A liver
biopsy should be considered, although the short
interval between the development of acute liver
failure and the development of severe coagulopathy can complicate the timing of the procedure.
In VZV and HSV infection, nonspecific necrosis
is often observed; however, inclusion bodies with
positive immunostaining for HSV or VZV antigens
would be diagnostic. It is reasonable to continue
treatment with acyclovir, since HSV is a cause of
fulminant hepatic failure, albeit a rare one.
After the patients transfer to the tertiary care hospital, his renal function deteriorated. Continuous
2566
of
m e dic i n e
renal-replacement therapy was initiated. Computed
tomographic imaging of the brain showed cerebral edema. The coagulopathy and thrombocyto
penia worsened (INR, 3.1; platelet count, 25,000
per cubic milliliter), precluding liver biopsy. Upper
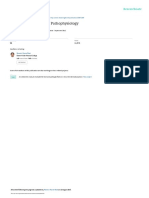
gastrointestinal bleeding and hypotension developed in the patient, and there were chest radiographic findings that were consistent with the
acute respiratory distress syndrome, with diffuse
infiltrates (Fig. 1). The patient required vasopressor support, an increasing fraction of inspired oxygen, and positive end-expiratory pressure. Eval
uation for liver transplantation was initiated.
The patients renal failure and encephalopathy and
the presence of alveolar infiltrates are consistent
with fulminant hepatic failure. The most likely
causes at this point include HSV infection, hepatitis E, or a metabolic or inflammatory disease
such as autoimmune hepatitis. Very rare causes not
yet mentioned include syphilis, adenovirus infection, and hemorrhagic fever (although the short
incubation period makes hemorrhagic fever unlikely).
On the third day after the patients transfer to the
tertiary care hospital, a qualitative polymerasechain-reaction (PCR) assay for HSV type 2 (HSV-2)
from blood obtained on day 5 of the hospitalization was positive, indicating at least 100 viral
copies per milliliter. The next day, an HSV PCR
assay from a bronchial aspirate was also positive.
IgG levels for HSV type 1 (HSV-1) were elevated,
and IgG levels for HSV-2 were negative. HSV IgM
Figure 1. Chest Radiograph Obtained 1 Day after
the Patients Transfer to the Tertiary Care Hospital.
Diffuse alveolar infiltrates are present, a finding that is
Graham
RETAKE
1st
AUTHOR
ICM
consistent
with the acute
respiratory distress
syndrome.
REG F
FIGURE
CASE
TITLE
fig 1
n engl j med 360;24 nejm.org
june 11, 2009
Enon
ARTIST: mleahy
FILL
2nd
3rd
Line
H/T
Combo
4-C
H/T
Revised
SIZE
16p6
Downloaded from cme.nejm.org by DR. SIMONA RUTA on June
10, 2009
. NOTE:
AUTHOR,
PLEASE
Copyright 2009 Massachusetts Medical Society.Figure
All rights
reserved.
has been
redrawn and type has been reset.
Please check carefully.
clinical problem-solving
was not tested. Despite continued treatment with
acyclovir, progressive hepatic failure with coagu
lopathy, lactic acidosis, and hypoglycemia developed in the patient. Superinfection with Candida
albicans in the blood also developed, and he was
treated with caspofungin. After 12 days of multi
organ failure from overwhelming sepsis, the patients family decided to withdraw supportive
care. The patient died shortly thereafter. The family declined an autopsy in order to expedite the return of the patients body to South Africa.
After repeated questioning, the patients friends
revealed that he had left a nightclub with a female
companion several days before he became ill. She
was noted to have a perioral vesicular lesion, which
was consistent with herpes labialis.
This unfortunate young man had a rare but welldescribed complication of what presumably was
primary infection with a very common virus. The
laboratory data suggest an acute infection with
HSV-2 and previous infection with HSV-1. Patients
with fulminant hepatic failure are at high risk for
superinfection, which occurred in this patient.
The decision regarding liver transplantation is difficult in an infected patient with fulminant hepatic failure. Transplantation may be the only lifesaving therapy available, but immunosuppression
after transplantation may exacerbate the infection.
C om men ta r y
Fulminant hepatic failure is most often defined
as the development of acute hepatitis and encephalopathy (within 2 to 8 weeks after initial symptoms) in a person with no history of liver disease.1 A prospective multicenter study in the
United States showed that fulminant hepatic failure in adults was most often caused by an overdose of acetaminophen (in 39% of patients), followed by idiosyncratic drug reactions (13%), acute
hepatitis B virus infection (7%), ischemic liver
injury (6%), hepatitis A (4%), and autoimmune
hepatitis (4%); the cause was unknown in 27% of
patients.2 No cases of HSV were identified. The
incidence of acetaminophen overdosing is lower
in many other countries, perhaps because of differences in the selection of medication or in the
prevalence of alcohol abuse (which lowers the
threshold for acetaminophen overdosing).3
Rapid determination of the cause of fulminant hepatic failure is critical, since prompt initiation of therapy can be lifesaving. Serologic and
antigen tests can be used in the diagnosis of
hepatitis A, B, and E and acute EBV or CMV infection; serologic testing for HSV and VZV is less
helpful because of the high seroprevalence of
these viruses. PCR can detect HSV and VZV DNA
in the serum, but there may be a considerable
delay before the results are available. HSV PCR
assays have excellent specificity (99%) and good
sensitivity (at least 90%), particularly when the
viral load is more than 500 copies per milliliter.4
Liver biopsy can be used to rapidly diagnose HSV
and VZV infection. The histopathological features
of HSV and VZV hepatitis include focal areas of
necrosis with minimal surrounding inflammation. Intranuclear inclusion bodies are often present. Immunohistochemical analysis can be used
to detect viral antigens in tissue sections.
Empirical treatment with antiviral therapy
early in the course of the disease may be indicated in enigmatic cases of fulminant hepatic
failure. Acyclovir is the first choice, since it is
effective against both HSV and VZV infections,
although a response may take several days. The
treatment of other viral infections (e.g., intravenous immune globulin for hepatitis A infection)
is generally not initiated until a specific diagnosis has been made.
HSV is common worldwide but is a rare cause
of fulminant hepatic failure. In the United States,
among people between 14 and 49 years of age,
the estimated seroprevalence of HSV-2 is 17%,
and the estimated seroprevalence of HSV-1 is 62%.5
Most HSV-1 and HSV-2 infections are subclinical. HSV-1 is typically transmitted during childhood by nonsexual contact with oral mucosa;
symptomatic infections are usually limited to the
perioral area. HSV-2 is acquired through sexual
contact and most commonly causes recurrent,
painful anogenital vesicular lesions, but it may
cause oral lesions. HSV is the cause of less than
1% of cases of fulminant hepatic failure,6 resulting in 25 to 50 cases per year in the United
States (40% are caused by HSV-1 and 60% are
caused by HSV-2).7 Fulminant hepatic failure from
HSV occurs primarily in immunosuppressed persons (particularly organ-transplant recipients),
pregnant women, and children (particularly newborns). Pregnant women are at greatest risk during the third trimester, when the virus crosses
the placental membrane and is associated with a
high risk of death for both the mother and the
fetus.8 However, fulminant hepatic failure from
HSV can also occur in immunocompetent per-
n engl j med 360;24 nejm.org june 11, 2009
Downloaded from cme.nejm.org by DR. SIMONA RUTA on June 10, 2009 .
Copyright 2009 Massachusetts Medical Society. All rights reserved.
2567
clinical problem-solving
sons; in one recent series, 24% of patients with
fulminant hepatic failure due to HSV were characterized as being immunocompetent.7
A high index of suspicion is necessary to diagnose fulminant hepatic failure due to HSV, particularly in immunocompetent hosts.9 The physical examination may reveal cutaneous lesions in
the perioral or anogenital regions, but the absence of these lesions does not rule out the diag
nosis.7,10 The interval between primary exposure
and the development of cutaneous lesions ranges
from 3 to 7 days.
Unfortunately, a common theme in the literature is the diagnosis of HSV infection at autopsy.
In one series of patients with fulminant hepatic
failure due to HSV, the correct diagnosis was
made before death in only 23% of patients.11
Fulminant hepatic failure caused by HSV is potentially treatable. The survival rate among patients
who receive acyclovir is higher than the rate
among those who do not receive this drug (88%
vs. 51% in one series),7 and patients who receive it
sooner do better than those who receive delayed
treatment. Unfortunately, because of the delay in
the diagnosis, immunocompetent patients may be
less likely than patients who are not immunocompetent to receive acyclovir initially.10 Liver
transplantation is a potential therapeutic option,
although there is concern that immunosuppression may worsen the infection in the post-transplantation period. Patients with cryptogenic hepatic failure who have undergone transplantation
and in whom HSV infection was diagnosed by
analysis of the explanted organ have been successfully treated with acyclovir during the postoperative period.12 Because of the rapid course of
fulminant hepatic failure, there may be a short
interval between illness that is severe enough to
warrant transplantation and illness that has progressed to the point that the patient would not
survive the operation.
Our patient had a rare complication of a common infection. He probably acquired the infection by oral contact with the woman with whom
he was seen, who was reported to have evidence
of active HSV infection. Why the patient died as
a consequence of this usually benign infection is
unknown, but proposed mechanisms of severe
HSV infection in immunocompetent hosts include
an overwhelming inoculation of virus, latent virus reactivation after reinfection by a second HSV
strain, infection with specific HSV strains with
increased virulence, and defects in host T lymphocytes or macrophages, resulting in an inability to respond to or process unique HSV anti
gens.13,14 Diagnosing HSV infection at the time
of the patients initial presentation would have
been difficult unless a particularly careful history taking had revealed his female acquaintance
with the perioral lesion. Earlier treatment with
acyclovir could have been lifesaving, however,
rendering the presumed kiss less than lethal.
Supported by an Advanced Career Development Award from
the Health Services Research and Development Program of the
Department of Veterans Affairs (to Dr. Saint).
No potential conflict of interest relevant to this article was
reported.
References
1. Trey C, Lipworth L, Chalmers TC, et al.
Fulminant hepatic failure: presumable contribution to halothane. N Engl J Med 1968;
279:798-801.
2. Ostapowicz G, Fontana RJ, Schidt FV,
et al. Results of a prospective study of
acute liver failure at 17 tertiary care centers in the United States. Ann Intern Med
2002;137:947-54.
3. Chan TY. Fulminant hepatic failure due
to acetaminophen poisoning may be less
common in Hong Kong. J Toxicol Clin
Toxicol 2001;39:175-7.
4. Stcher M, Leb V, Bozic M, et al. Parallel detection of five human herpes virus
DNAs by a set of real-time polymerase
chain reactions in a single run. J Clin Virol
2003;26:85-93.
5. Xu F, Sternberg MR, Kottiri BJ, et al.
Trends in herpes simplex virus type 1 and
type 2 seroprevalence in the United States.
JAMA 2006;296:964-73.
2568
6. Schidt FV, Davern TJ, Shakil AO,
McGuire B, Samuel G, Lee WM. Viral
hepatitis-related acute liver failure. Am J
Gastroenterol 2003;98:448-53.
7. Norvell JP, Blei AT, Jovanovic BD, Levit
sky J. Herpes simplex virus hepatitis: an
analysis of the published literature and institutional cases. Liver Transpl 2007;13:
1428-34.
8. Avgil M, Ornoy A. Herpes simplex
virus and Epstein-Barr virus infections in
pregnancy: consequences of neonatal or
intrauterine infection. Reprod Toxicol
2006;21:436-45.
9. Abbo L, Alcaide ML, Pano JR, Robinson PG, Campo RE. Fulminant hepatitis
from herpes simplex virus type 2 in an
immunocompetent adult. Transpl Infect
Dis 2007;9:323-6.
10. Farr RW, Short S, Weissman D. Fulminant hepatitis during herpes simplex virus
infection in apparently immunocompetent
adults: report of two cases and review of the
literature. Clin Infect Dis 1997;24:1191-4.
11. Kaufman B, Gandhi SA, Louie E, Rizzi
R, Illei P. Herpes simplex virus hepatitis:
case report and review. Clin Infect Dis
1997;24:334-8.
12. Montalbano M, Slapak-Green GI, Neff
GW. Fulminant hepatic failure from herpes simplex virus: post liver transplantation acyclovir therapy and literature review.
Transplant Proc 2005;37:4393-6.
13. Miyazaki Y, Akizuki S, Sakaoka H,
Yamamoto S, Terao H. Disseminated infection of herpes simplex virus with fulminant hepatitis in a healthy adult: a case
report. APMIS 1991;99:1001-7.
14. Dix RD, McKendall RR, Baringer JR.
Comparative neurovirulence of herpes simplex virus type 1 strains after peripheral
or intracerebral inoculation of BALB/c
mice. Infect Immun 1983;40:103-12.
Copyright 2009 Massachusetts Medical Society.
n engl j med 360;24 nejm.org june 11, 2009
Downloaded from cme.nejm.org by DR. SIMONA RUTA on June 10, 2009 .
Copyright 2009 Massachusetts Medical Society. All rights reserved.
Вам также может понравиться
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- Tratament Helicobacter PyloriДокумент9 страницTratament Helicobacter PyloriFlavia ElenaОценок пока нет
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (399)
- Scurt Istoric. Gametogeneza. Ovulatie. Fecundatie. Nidatie. PlacentatiaДокумент29 страницScurt Istoric. Gametogeneza. Ovulatie. Fecundatie. Nidatie. PlacentatiaFlavia ElenaОценок пока нет
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- CMV NeonatalДокумент7 страницCMV NeonatalFlavia ElenaОценок пока нет
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (894)
- Pess MeaslesДокумент12 страницPess MeaslescnajesrnasiferfОценок пока нет
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- CCR5 Delta 32 Stem Cells TransplantationДокумент7 страницCCR5 Delta 32 Stem Cells TransplantationcnajesrnasiferfОценок пока нет
- HCV Narcotic DiversionДокумент7 страницHCV Narcotic DiversionJenna MillerОценок пока нет
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Hepatitis C in Narcotic DiversionДокумент10 страницHepatitis C in Narcotic DiversionFlavia ElenaОценок пока нет
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- ANSWER KEY SI Worksheet 14Документ3 страницыANSWER KEY SI Worksheet 14Chandi brunОценок пока нет
- Viruses Verdict 2019Документ9 страницViruses Verdict 2019Klint Rodney Mark LuleОценок пока нет
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (265)
- CHAPTERS 2-4 CROSSWORD #1 SolvedДокумент4 страницыCHAPTERS 2-4 CROSSWORD #1 SolvedYu LucyОценок пока нет
- Protozoan Parasite E. histolytica Life CycleДокумент6 страницProtozoan Parasite E. histolytica Life CyclePrimo GeorgeОценок пока нет
- Histopathology Services GuideДокумент23 страницыHistopathology Services GuidegauravОценок пока нет
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- June 2021Документ90 страницJune 2021SEIYADU IBRAHIM KОценок пока нет
- Cetylpyridinium Chloride Mouthwash Potential Against COVIDДокумент4 страницыCetylpyridinium Chloride Mouthwash Potential Against COVIDNicoll SQОценок пока нет
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- Soal BiomolekulerДокумент3 страницыSoal BiomolekuleralmasyifaОценок пока нет
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Unit 2-Quiz 7Документ14 страницUnit 2-Quiz 7body fayezОценок пока нет
- Doi170066supp1 ProdДокумент47 страницDoi170066supp1 ProdAdniana NareswariОценок пока нет
- Amv - Microbial Contamination Test (MCT)Документ37 страницAmv - Microbial Contamination Test (MCT)vkОценок пока нет
- Vision Ias Science &tech Mains 365 2020Документ93 страницыVision Ias Science &tech Mains 365 2020RakeshОценок пока нет
- LymphomaДокумент78 страницLymphomaastriwahyuni100% (4)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- ANormal Values Saunders 6th, 7th, Uworld 2017 JimirДокумент4 страницыANormal Values Saunders 6th, 7th, Uworld 2017 JimirAce LabosОценок пока нет
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2219)
- The Effects of Sorghum Bicolor Aqueous Leaf Sheaths Extract On Some Selected Biochemical Parameters of Phenylhydrazine-Induced Hemoltyic Anemic Male Wistar RatsДокумент6 страницThe Effects of Sorghum Bicolor Aqueous Leaf Sheaths Extract On Some Selected Biochemical Parameters of Phenylhydrazine-Induced Hemoltyic Anemic Male Wistar RatsInternational Journal of Innovative Science and Research TechnologyОценок пока нет
- Basic Immunology PDFДокумент330 страницBasic Immunology PDFnailul-abrorОценок пока нет
- Schwann CellsДокумент7 страницSchwann CellsVictor Manuel Granada AlvarezОценок пока нет
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Day 1 PNUДокумент250 страницDay 1 PNUM LОценок пока нет
- 1GS Cell PPT 2018Документ73 страницы1GS Cell PPT 2018pixiedustОценок пока нет
- Oxygen in Wound Healing Nutrient, Antibiotic, Signaling Molecule, and Therapeutic Agent PDFДокумент22 страницыOxygen in Wound Healing Nutrient, Antibiotic, Signaling Molecule, and Therapeutic Agent PDFIsabela MagriniОценок пока нет
- Expression of HCV Genotype-4 Core Antigen in Prokaryotic E. Coli System For Diagnosis of HCV Infection in EgyptДокумент9 страницExpression of HCV Genotype-4 Core Antigen in Prokaryotic E. Coli System For Diagnosis of HCV Infection in EgyptLê NgânОценок пока нет
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (119)
- A review of the potential medicinal properties of Cyperus rotundusДокумент17 страницA review of the potential medicinal properties of Cyperus rotundusMuhammad Vaqar HussainОценок пока нет
- Disease Detectives Cheat SheetДокумент2 страницыDisease Detectives Cheat SheetBereket LakiОценок пока нет
- Bio Final ReviewДокумент18 страницBio Final Reviewmarisa corderoОценок пока нет
- Preanalytical Variability Associated With The Procurement and Study of Small Biopsies - 091022dwДокумент19 страницPreanalytical Variability Associated With The Procurement and Study of Small Biopsies - 091022dwkamulegeya RogersОценок пока нет
- Periradicular Repair After Two-Visit Endodontic Treatment Using Two Different Intracanal Medications Compared To Single-Visit Endodontic TreatmentДокумент6 страницPeriradicular Repair After Two-Visit Endodontic Treatment Using Two Different Intracanal Medications Compared To Single-Visit Endodontic TreatmentRodolfo MatosОценок пока нет
- Protozoan Fecal SmearДокумент17 страницProtozoan Fecal SmearLeigh Ann TanpoОценок пока нет
- Leprosy An Overview of PathophysiologyДокумент7 страницLeprosy An Overview of PathophysiologyDurga MadhuriОценок пока нет
- 100 MCQ Questions On DiseaseДокумент31 страница100 MCQ Questions On DiseaseDineshPrakashОценок пока нет
- Antibody Functions and PropertiesДокумент33 страницыAntibody Functions and PropertiesJuan SalenОценок пока нет