Академический Документы
Профессиональный Документы
Культура Документы
Jurnal Mikosis
Загружено:
Rachmi AnnisaОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Jurnal Mikosis
Загружено:
Rachmi AnnisaАвторское право:
Доступные форматы
mycoses
Diagnosis, Therapy and Prophylaxis of Fungal Diseases
Original article
Isolation and identification of Malassezia species from Chinese and
Korean patients with seborrheic dermatitis and in vitro studies on
their bioactivity on sebaceous lipids and IL-8 production
1,
2,
Soo Young Kim, * Se Hyun Kim, * Su Na Kim, Ah-Reum Kim, Yu Ri Kim, Min Jung Kim,
2
2
3
1,4
1,4
Won-Seok Park, John Hwan Lee, Won Hee Jung, Yang Won Lee, Yong Beom Choe and
1,4
Kyu Joong Ahn
1
Department of Dermatology, Konkuk University School of Medicine, Seoul, Korea, 2AMOREPACIFIC Corp. R&D Unit, Yongin, Korea, 3Department of
Systems Biotechnology, Chung-Ang University, Anseong, Korea and 4Research Institute of Medical Science, Konkuk University, Seoul, Korea
Summary
We investigated the distribution of Malassezia yeast in 120 Chinese (20 patients from
each of six cities) and 20 Korean patients with scalp seborrheic dermatitis (SD) and
dandruff (SD/D) using ITS1 and ITS2 polymerase chain reaction-restriction fragment
length polymorphism. Bioactivity was studied by quantifying sebum lipid production
by human primary sebocytes and inflammatory cytokine, interleukin-8 (IL-8) production was studied by exposing HaCaT keratinocytes with extracts of five standard
Malassezia strains; M. globosa, M. restricta, M. sympodialis, M. dermatis and M.
sloof- fiae. M. restricta and M. globosa were the most frequently encountered species
from both Chinese and Korean patients. These two Malassezia species also promoted
neu- tral lipid synthesis although the result was not statistically significant and
induced significant increase in IL-8 production among the five Malassezia species
studied. The study suggests a possible role of these organisms in the pathogenesis of
SD/D.
Key words: dandruff, seborrheic dermatitis, Malassezia yeast, ITS1 and ITS2 PCR-RFLP, neutral lipid synthesis,
IL-8.
Introduction
Seborrheic dermatitis (SD) and dandruff (D) are common diseases of the scalp characterised by flaking and
itching. Both the clinical conditions are believed to be
basically same, but differing in their severity. It is said
that about 13% of the general population suffer from
SD, while more than 50% of them from D.1 For
more than a century, Malassezia yeast have been
Correspondence: Yang Won Lee, MD, PhD, Department of Dermatology,
Konkuk University School of Medicine, 120-1
Neungdong-ro,
Gwangjin-gu, Seoul 143-729, Korea.
Tel.: +82 2 2030 5172. Fax: +82 2 2030 5179.
E-mail: 20050078@kuh.ac.kr
*These authors contributed equally to this work.
Submitted for publication 13 February 2015
Revised 10 November 2015
Accepted for publication 10 December 2015
doi:10.1111/myc.12456
incriminated to be the cause of SD/D and a large number of studies as well as clinical response as well as
reduction in the yeast population following antifungal
therapy support this hypothesis.2,3 Among the 14
Malassezia species identified to date, Malassezia restricta
and M. globosa are considered to be the predominant
species in the pathogenesis of SD/D, although the discrepancies exist between the studies, they can be
attributed to the methodological as well as geographical and ethnic variations in the population studied.46
It is not clear which virulence factor or factors of
Malassezia species initiates the development or exacerbation of SD. Probably, it is the interplay between
Malassezia, keratinocytes and immune mechanism
determines the transformation of a commensal Malassezia into a pathogen.7 Malassezia utilise the sebum
present on the scalp as a source of nutrient.8 Lipases
produced by Malassezia degrade the sebum, releasing
free fatty acids from triglycerides (TGs) and a part of
2016 Blackwell Verlag GmbH
Mycoses, 2016, 59, 274280
Malassezia on the scalp seborrheic dermatitis
the saturated fatty acids are utilised and the remaining
unsaturated fatty acids are responsible inflammation
of the
skin.8
One study
demonstrated that
Malassezia species can
induce
pro-inflammatory
cytokine produc- tion by keratinocytes.9
In this study, we used polymerase chain reactionrestriction fragment length polymorphism (PCR-RFLP)
to identify and to speciate the Malassezia organisms
from scalp of Chinese and Korean patients with SD/D.
In addition, the bioactivities of different Malassezia species on the induction of sebum secretion and interleukin (IL)-8 pro-inflammatory cytokine production by
epidermal cells were studied.
(EDTA), 100 lg ml
RNase A] in a 1.5-ml tube. All
sam- ples were stored at 20 C until used.
Standard strains
Six reference strains of Malassezia species were used to
determine the 26S rDNA PCR-RFLP pattern. Standard
strains were obtained from the Centraalbureau voor
Schimmelcultures (CBS, Utrecht, the Netherlands) Biological Resource Center and from the Japan Collection
of Microorganisms (JCM, Saitama, Japan). These
included M. furfur (CBS 1878), M. restricta (CBS 7877),
M. dermatis (JCM 11348), M. sympodialis (CBS 7222),
M. slooffiae (CBS 7956) and M. globosa (CBS 7966).
Material and methods
Patient population
The subjects comprised of 140 female patients, aged
between 3565 years with readily visible scalp SD,
which included 120 Chinese (20 patients each from the
six cities, namely, Guangzhou, Shanghai, Beijing,
Wuhan, Chengdu and Shenyang), and 20 Korean
patients, all from the city of Seoul. All participants were
instructed to wash their hair on the previous day. Samples were collected from two matched subjects with similar grades of SD. The signs of inflammation and scaling
were measured according to their severity on a six-point
scale (0 = none, 1 = slight, 2 = mild, 3 = moderate,
4 = pronounced, 5 = severe) and only patients with
scores of 35 were retained in the study group. Similarly, subjects having received treatment with antimicrobials in the previous 4 weeks were also excluded
from the study. The study protocol was approved by the
institutional review board of each of the seven hospitals
from where the subjects were enrolled, namely, Shanghai Skin Disease Hospital; West China Hospital, Sichuan
University; The Third Affiliated Hospital Of Sun Yat-Sen
University; Renmin Hospital Of Wuhan University; The
First Hospital Of China Medical University; The General
Hospital Of Air Force; Konkuk University Hospital.
Informed consent for participation was obtained from
each individual prior to enrolment.
Sample collection
Samples were collected by rubbing the scalp with a cotton
swab soaked in detergent solution (0.01% NaH2PO4 2H2O, 1.01% Na2HPO4, 0.1% Triton X-100; pH
7.9). After 30 rubs, the head part of the cotton swab was
cut off and placed into 200 ll resuspension buffer [50
mM Tris- HCl
(pH 8.0),
10
mM
Ethylenediaminetetraacetic acid
2016 Blackwell Verlag GmbH
Mycoses, 2016, 59, 274280
Isolation of genomic DNA
After thawing the samples, 200 ll lysis buffer [10 mM
Tris-HCl (pH 8.0), 1 mM EDTA, 100 mM NaCl, 1%
Sodium dodecyl sulfate (SDS), 2% Triton X-100] was
added. All samples were vortexed for 5 min before
removing the cotton swab. A quantity of 200 ~ 300 ll
of glass beads (Sigma, St. Louis, MO, USA) were added
and vortexed for 20 s, followed by stirring for a further
10 min with 200 ll phenol:chloroform (1 : 1, v/v)
mixture. Samples were kept at 4 C for 3 min and centrifuged at 11 400 g for 10 min. The upper aqueous
phase was transferred into a new tube and an equal volume of isopropanol was added to precipitate the DNA at
20 C for 90 min. The DNA pellet was separated by
centrifuging the samples at 11 400 g for 15 min. After
aspirating the supernatant, the DNA pellet was washed
with 500 ll 70% ethanol and dried at room temperature. The sample pellet was resuspended in 30 ll Tris/
EDTA buffer [10 mM Tris-HCl (pH 8.0), 1 mM EDTA].
ITS1 and ITS2 PCR
The following primers were synthesised to amplify the
ITS1 and ITS2 regions of the Malassezia genomic DNA:
ITS1 forward (50 -AGG TTT CCG TAG GTG AAC CT-30 )
and reverse (50 -TTC GCT GCG TTC TTC ATC GA-30 ),
and ITS2 forward (50 -TCG ATG AAG AAC GCA GCG
AA-30 ) and reverse (50 -TCC TCC GCT TAT TGA TAT
GC-30 ). Using 100 ng of each DNA sample used as
template DNA, ITS1 and ITS2 were amplified using
AccuPower Taq PCR PreMix (Bioneer, Daejeon,
Korea). PCR was performed using the following conditions: 95 C for 14 min (predenaturation); 40 cycles
of 94 C for 45 s (denaturation), 55 C for 45 s
(annealing) and 72 C for 1 min (extension); and
72 C for 7 min (final extension).
19
RFLP analysis
Amplification of 26S rDNA was conducted using the
same PCR conditions as above, except with an annealing temperature of 52 C, 60 cycles of extension, and
the following forward and reverse primers: 50 -TAA
CAA GGA TTC CCC TAG TA-30 and 50 -ATT ACG CCA
GCA TCC TAA G-30 respectively. The final PCR product was purified with an AccuPrep PCR Purification
Kit (Bioneer). After confirming the presence of a 580bp band corresponding to 26S rDNA by electrophoresis
in an agarose gel, the sample was treated with HhaI
and BtsCI (New England Biolabs, Ipswich, MA, USA).
Restriction digests were performed for 5 h with
10 units of enzyme at 37 C with HhaI or 50 C with
BtsCI. DNA fragments were visualised by electrophoresis in a 2% agarose gel.
Human primary sebocyte and HaCaT keratinocyte
cultures
Human primary sebocytes (Celprogen, Torrance, CA,
USA) were maintained in Human Primary Sebocyte
Complete Growth Medium with Serum (Celprogen) at
37 C in a humidified atmosphere containing 5% CO2.
Spontaneously immortalised, non-tumorigenic human
HaCaT keratinocytes were maintained in Dulbeccos
modified Eagles medium (Invitrogen, Waltham, MA,
USA) with low L-glutamine supplemented with 10%
fetal bovine serum (JRH Bioscience, Tokyo, Japan),
100 mg ml 1 penicillin, and 100 mg ml 1
streptomycin (GIBCO, Milan, Italy) at 37 C in a humidified
atmosphere containing 5% CO2.
In vitro model of seborrheic dermatitis
To study the sebum secretion and pro-inflammatory
cytokine expression, we established a co-culture system
wherein, human primary sebocytes and HaCaT keratinocytes were seeded in equal amounts into 24-well
plates and co-cultured in Human Primary Sebocyte
Complete Growth Medium with serum and incubated at
37 C in a humidified chamber containing 5% CO2. On
the following day, a cocktail containing 50 lM linoleic
acid (Sigma), 50 lM arachidonic acid (Sigma) and
10 nM dihydrotestosterone (Sigma), and 2 lg ml 1
Malassezia extracts from M. globosa, M. restricta,
M. sympodialis, M. dermatis and M. slooffiae were added
to the co-cultured cells and were incubated for 48 h.
However, control wells did not receive any cocktail. Cultivation of standard strains: Standard
strains of
Malasse- zia were
cultured
on
Leeming and
Notman agar
incubated at 34 C for 3 days, except for M. restricta,
which was incubated for 5 days. Growth from the cultured plates were harvested and resuspended in 29 volume of Phosphate buffered saline (PBS). After 3 quick
successive freezing and thawing, cells were lysed by sonication. Qualitative analysis of each Malassezia extract
was performed by Bicinchoninic acid assay (BCA) protein assay (Bio-Rad, Hercules, CA, USA). The supernatants were used for inflammatory cytokine assay and
the cells were fixed with 4% paraformaldehyde for
5 min which were subsequently used for assessment of
synthesised neutral lipids.
Assay of inflammatory interleukin-8
Supernatants from co-cultured cells were assayed for
IL-8 using the Human IL-8 BD OptEIA ELISA kit (BD
Biosciences, San Jose, CA, USA). Each sample was
assayed thrice by measuring the absorbance at
450 nm (reference filter of 540 nm) using a Synergy
H2 Multi-Mode Microplate Reader (BioTek, Winooski,
VT, USA).
Assay of neutral lipid
Lipid production by Malassezia species was assayed by
staining with Nile red stain. A stock solution of Nile
red (1 mg ml 1 in acetone) was diluted in phosphatebuffered saline (PBS) to a final concentration of
1 lg ml 1 and 4% paraformaldehyde fixed co-cultured
cells were stained with working solution of Nile red
solution for 10 min, washed with PBS, and then covered with fresh PBS. Fluorescence was measured using
the fluorescence mode of a Synergy H2 Multi-Mode
Microplate Reader (BioTek) with a 530-550 nm bandpass excitation filter. Fluorescence was compared with
that of a control sample.
Statistical analysis
Students t-test was used to compare variables. Analyses were performed using SPSS software (version 21.0
for Windows; SPSS, Chicago, IL, USA). The cut off for
statistical significance was set at P < 0.05.
Results
Identification of Malassezia yeast in scalp SD
The identification rate of Malassezia yeast was 91.4%
in all the subjects. M. restricta and M. globosa were
found predominantly from the scalp of patients with
SD in China (82.8% for each species) and Korea
(100% for each species). The distribution of Malassezia
species varied between the patients from the six cities
in China, but two were still the most common species
at a frequency of 60100%. M. sympodialis was found
in 11.1% of the SD patients from Korea and Guangzhou, Chengdu, but it was not isolated from the
patients from the rest of the four cities in China. There
was no evidence of M. dermatis, M. furfur or M. slooffiae in the scalp specimens from any of the patients in
this study (Table 1).
Synthesis of neutral lipid by individual Malassezia
species
Mean neutral lipid synthesis rates increased by 30.7%
and 29.8% in cells treated with M. globosa and M.
restricta protein extracts, respectively, compared with
the controls (P = 0.10 and P = 0.08 respectively).
Though both increases were not statistically significant, they showed a tendency. Similarly, extracts from
M. sympodialis showed an increase of 13.6%, whereas
extracts from M. dermatis and M. slooffiae showed a
decrease in the lipid synthesis by 16.6% and 5.7%
respectively. However, none of these findings are statistically significant (Fig. 1).
Inflammatory cytokine IL-8 secretion by individual
Malassezia species
IL-8 concentration increased in all co-culture systems
treated with extracts of Malassezia species compared
with controls. Cells treated with M. globosa extract
showed most significant increase followed M. restricta.
With M. globosa, the IL-8 concentration increased by
almost threefold compared with the control. Similarly,
M. restricta induced a 2.77-fold increase. IL-8 production rates induced by M. sympodialis, M. dermatis and
M. slooffiae also significantly increased, by 2.58-fold,
Figure 1 Neutral lipid synthesis in response to extraction of each
Malassezia species. NC, normal control.
2.31-fold and 2.38-fold, respectively, compared with
the controls (Fig. 2).
Discussion
This study revealed that M. restricta and M. globosa
are the two prevalent species on the scalps of Chinese
and Korean patients with SD/D. This is in agreement
46,1014
with the findings of several other studies.
Gemmer et al. [10] and Crespo-Erchiga et al. [11]
reported M. restricta as the most common species in
SD patients, whereas Gupta et al. [12] and Gaitanis
et al. [13] reported M. globosa as the most common. A
recent study from China has shown M. globosa and
M. restricta are almost equally distributed (87.0% and
81.5% respectively).14 The disparity in the prevalence
rates between different studies could be attributed to
the variations in the sampling and identification techniques adopted by the workers as well as geographical
and ethnicity differences in the population.4,6,1014
Several studies have demonstrated that Malassezia
yeast are the normal inhabitants of healthy human
skin and their distribution varies depending on the
12,1519
body sites.
On the scalp and forehead,
Table 1 Isolation of Malassezia species from the scalp of patients with SD in Korea and China (%).
M. restricta
M. globosa
M. sympodialis
M. dermatis
M. furfur
M. slooffiae
Others
None
Korea
China
Guangzhou
Chengdu
Wuhan
Shanghai
Beijing
Shenyang
100.0
100.0
11.1
0.0
0.0
0.0
0.0
0.0
82.8
82.8
3.4
0.0
0.0
0.0
5.2
5.2
100.0
77.8
11.1
0.0
0.0
0.0
0.0
0.0
100.0
100.0
11.1
0.0
0.0
0.0
0.0
0.0
90.0
60.0
0.0
0.0
0.0
0.0
0.0
0.0
60.0
60.0
0.0
0.0
0.0
0.0
0.0
40.0
70.0
100.0
0.0
0.0
0.0
0.0
30.0
0.0
80.0
100.0
0.0
0.0
0.0
0.0
0.0
0.0
Figure 2 IL-8 concentration in response to each Malassezia spe-
cies. NC: normal control. *P < 0.05; **P < 0.005; ***P < 0.001,
as compared to normal control.
M. restricta is the most common, while M. globosa is
the most common species found on the chest and
back.12,1719 The differences are attributed to the variations in the lipid content at different body sites.18
Incidentally, these two species are also the common
species in other related skin diseases such as atopic
dermatitis and pityriasis versicolor.15,16,20,21 M. globosa is predominant in pityriasis versicolor, while
M. restricta is the dominant species in SD/D as well as
the head and neck atopic dermatitis.11,13,15,16
Although, earlier studies indicated M. globosa as the
causative agent of pityriasis versicolor,22 subsequent
studies showed that there is no difference in the distribution of these organism in the healthy as well as on
the diseased skin.23 Similar confusion exists not only
in PV, but also in other Malassezia-associated skin dis24
ease. Now, it is postulated that it is the proliferation
of a particular organism on the involved body site that
may disturb the homeostasis of the skin environment
and induce skin symptoms. Quantitative studies found
that the number of inhabiting Malassezia species was
significantly elevated in SD patients relative to healthy
controls,4,25 which may disrupt skin barriers and
induce inflammation.
It has been proposed that at least three prerequisites
Malassezia yeast, sebaceous lipids and individual susceptibility are essential for the development of SD/
D.26 The specific interactions between Malassezia species and the two other etiological factors of SD/D need
to be investigated in order to understand how Malassezia yeast shift from commensal to pathogenic organisms. The role of sebaceous activity in the aetiology of
SD/D is suggested by the temporal predilection during
infancy (cradle cap) and in adolescence and young
adulthood and in areas where there is high sebaceous
activity.27 Sebum is a source of nutrition for Malassezia organisms, and when degraded, it produces free
fatty acids, inducing irritation and inflammation of the
skin.28 It has been shown that the colonisation of
Malassezia species is threefold greater on the scalp of D
patients than on healthy controls due to high levels of
4
sebum secretion. However, the ability of Malassezia in
inducing sebum secretion by sebaceous glands has not
been investigated till date. In acne, Propionibacterium
acnes itself has been reported to augment lipid droplet
formation and TG synthesis in hamster sebocytes.29
We observed that there was an increase in the neutral
lipid synthesis in the presence of extracts of M. globosa
and M. restricta in the co-culture system that we studied. Although this was not statistically significant, this
finding calls for further studies to elucidate the interaction between the Malassezia yeast and sebaceous gland
activity.
Since lipid metabolites (i.e. free fatty acids such as
oleic acid) induce skin irritation and inflammation,
lipases and phospholipases of Malassezia yeast are currently considered to be strong candidates for the factors influencing the intrinsic virulence of Malassezia
4,2628,30
species.
Genome sequencing of Malassezia species has led to the recognition and detection of relevant genes in the various strains that may have
pathogenetic potential. The high lipase activity of
M. globosa on the scalp of SD patients increases the
significance of this particular species.27 We previously
reported on the gene expressions of several M. restricta
lipases, and found that one particular lipase gene was
strongly expressed on the scalp of patients with SD,
which we named MRE-0242. This gene is suspected
to play a pathogenic role in M. restricta, similar to the
LIP-1 in M. globosa.28,31 The increased secretion of
lipases and phospholipases from Malassezia species on
the skin could produce irritating lipid metabolites,
damage the epidermal barrier and activate the local
9,24
immune response in SD.
Malassezia yeast have been shown to induce
immune reactions.7,27 Keratinocytes produce cytokines
and chemokines and thus play a role in the inflammatory reaction leading to the development of SD/D. In
the study, we observed that IL-8 productions by
human keratinocytes exposed to Malassezia extracts
increased significantly compared to the controls. In
particular, two species, M. globosa and M. restricta
exerted a significant increase in IL-8, and of the two
organisms, M. globosa showed significant effect. It has
been shown that keratinocytes can produce proinflammatory cytokines (IL-1a, IL-6, IL-8, IL-12, and
tumour necrosis factor-a) when exposed to Malassezia
yeast, and that the profile of releasing cytokines in
response to each species were differnt.3235 IL-8 is
involved in the inflammatory process by stimulating
the migration of neutrophils and lymphocytes.32 It
was reported that the level of IL-8 was significantly
increased in the biopsy samples of stratum corneum
34
taken from D relative to non-D subjects at baseline.
The mechanism underlying the regulation of cytokine
production by Malassezia species are not clear. Toll-like
receptor 2 was reported to mediate intracellular signalling in human keratinocytes in response to M. furfur, leading to the expression of human b-defensin 2
and IL-8 mRNA.36 The findings of the study show that
Malassezia, particularly M. globosa and M. restricta,
induce the secretion of IL-8 by keratinocytes further
strengthen the pro-inflammatory role of Malassezia in
the pathogenesis of SD/D.
In conclusion, the present findings implicate
Malassezia yeast in the pathogenesis of SD/D. M. restricta and M. globosa were the two most frequent
Malassezia species on the scalp of SD/D patients in
China and Korea. Their bioactivity, with respect to
the induction of TGs and the pro-inflammatory cytokine IL-8, appears to be the highest in these two
Malassezia species among all of the tested species.
This suggests that M. restricta and M. globosa, which
are major species isolated from SD patients, play
roles in triggering inflammatory responses and modifying sebum secretion. Further studies are needed to
elucidate the role of Malassezia species and the
underlying mechanisms, especially in immune reactions and lipid synthesis.
Acknowledgements
This work was supported by the Basic Science
Research Program through the National Research
Foundation of Korea (NRF), funded by the Ministry
of
Science,
ICT,
Future
Planning
NRF2013R1A1A2007863 and AMOREPACIFIC Corp., and
the grant of Paul-Janssen from Korean Dermatologic
Association (2015).
The authors thank Professor Xuemin Wang at the
Shanghai Skin Disease Hospital, Professor Li Li at the
West China Hospital of Sichuan University, Professor
Wei Lai at The Third Affiliated Hospital of Sun YatSen University, Professor Hong Liang at the Renmin
Hospital of Wuhan University, Professor Xinghua Gao
at The First Hospital of China Medical University, and
Professor Wei Liu at The General Hospital of Air Force
for their clinical support in China.
References
1
2
3
10
11
12
13
14
15
16
17
18
19
20
Batra R, Boekhout T, Gu eho E, Caban~es FJ, Dawson TL Jr,
Gupta
AK. Malassezia Baillon, emerging clinical yeasts. FEMS Yeast Res
2005; 5: 11013.
Faergemann J. Pityrosporum yeastswhats new? Mycoses 1997; 40
(Suppl. 1): 2932.
Skinner RB Jr, Noah PW, Taylor RM et al. Double-blind treatment of
seborrheic dermatitis with 2% ketoconazole cream. J Am Acad Dermatol 1985; 12: 8526.
Hiruma M, Cho O, Hiruma M, Kurakado S, Sugita T, Ikeda S. Genotype analyses of human commensal scalp fungi, Malassezia globosa,
and Malassezia restricta on the scalps of patients with dandruff and
healthy subjects. Mycopathologia 2014; 177: 2639.
Gupta AK, Batra R, Bluhm R, Boekhout T, Dawson TL Jr. Skin diseases associated with Malassezia species. J Am Acad Dermatol 2004;
51: 78598.
Lee YW, Byun HJ, Kim BJ et al. Distribution of Malassezia species on
the scalp in Korean seborrheic dermatitis patients. Ann Dermatol
2011; 23: 15661.
Gaitanis G, Magiatis P, Hantschke M, Bassukas ID, Velegraki A. The
Malassezia genus in skin and systemic diseases. Clin Microbiol Rev
2012; 25: 10641.
Ro BI, Dawson TL. The role of sebaceous gland activity and scalp
microfloral metabolism in the etiology of seborrheic dermatitis and
dandruff. J Investig Dermatol Symp Proc 2005; 10: 1947.
Schwartz JR, Messenger AG, Tosti A et al. A comprehensive pathophysiology of dandruff and seborrheic dermatitistowards a more
precise definition of scalp health. Acta Derm Venereol 2013; 93:
1317.
Gemmer CM, DeAngelis YM, Theelen B, Boekhout T, Dawson JT Jr.
Fast, noninvasive method for molecular detection and differentiation
of Malassezia yeast species on human skin and application of the
method to dandruff microbiology. J Clin Microbiol 2002; 40: 3350
7.
Crespo-Erchiga V, Ojeda Martos A, Vera Casano A, Crespo-Erchiga A,
Sanchez Fajardo F. Isolation and identification of Malassezia spp in
pityriasis versicolor, seborrhoeic dermatitis and healthy skin. Rev
Iberoam Micol 1999; 16: 1621.
Gupta AK, Kohli Y, Summerbell RC, Faergemann J. Quantitative culture of Malassezia species from different body sites of individuals with
or without dermatoses. Med Mycol 2001; 39: 24351.
Gaitanis G, Velegraki A, Alexopoulos EC et al. Distribution of Malassezia species in pityriasis versicolor and seborrheic dermatitis in Greece.
Typing of the major pityriasis versicolor isolate M. globosa. Br J Dermatol 2006; 154: 854859.
Zhang H, Ran Y, Xie Z, Zhang R. Identification of Malassezia species in
patients with seborrheic dermatitis in China. Mycopathologia 2013;
175: 8389.
Tajima M, Sugita T, Nishikawa A, Tsuboi R. Molecular analysis of
Malassezia microflora in seborrheic dermatitis patients: comparison
with other diseases and healthy subjects. J Invest Dermatol 2008;
128: 34551.
Zhang E, Tanaka T, Tajima M, Tsuboi R, Nishikawa A, Sugita T.
Characterization of the skin fungal microbiota in patients with atopic
dermatitis and in healthy subjects. Microbiol Immunol 2011; 55:
62532.
Jang SJ, Lim SH, Ko JH et al. The Investigation on the distribution of
Malassezia yeasts on the normal Korean skin by 26S rDNA PCRRFLP. Ann Dermatol 2009; 21: 1826.
Lee YW, Yim SM, Lim SH, Choe YB, Ahn KJ. Quantitative investigation on the distribution of Malassezia species on healthy human skin
in Korea. Mycoses 2006; 49: 40510.
Kim SC, Kim HU. The distribution of Malasseiza species on the normal human skin according to body region. Korean J Med Mycol
2000; 5: 1208.
Morishita N, Sei Y, Sugita T. Molecular analysis of Malassezia microflora from patients with pityriasis versicolor. Mycopathologia 2006;
161: 6165.
21
22
23
24
25
26
27
28
Takahata Y, Sugita T, Kato H, Nishikawa A, Hiruma M, Muto M.
Cutaneous Malassezia flora in atopic dermatitis differs between adults
and children. Br J Dermatol 2007; 157: 117882.
Crespo Erchiga V, Ojeda Martos A, Vera Casano A, Crespo Erchiga
A, Sanchez Fajardo F. Malassezia globosa as the causative agent of
pityriasis versicolor. Br J Dermatol 2000; 143: 799803.
Oh BH, Lee YW, Choe YB, Ahn KJ. Epidemiologic study of
Malassezia yeasts in seborrheic dermatitis patients by the analysis of
26S rDNA PCR-RFLP. Ann Dermatol 2010; 22: 14955.
Gaitanis G, Velegraki A, Mayser P, Bassukas ID. Skin diseases associated with Malassezia yeasts: facts and controversies. Clin Dermatol
2013; 31: 45563.
McGinley KJ, Leyden JJ, Marples RR, Kligman AM. Quantitative
microbiology of the scalp in non-dandruff, dandruff, and seborrheic
dermatitis. J Invest Dermatol 1975; 64: 4015.
DeAngelis YM, Gemmer CM, Kaczvinsky JR, Kenneally DC, Schwartz
JR, Dawson TL Jr. Three etiologic facets of dandruff and seborrheic
dermatitis: Malassezia fungi, sebaceous lipids, and individual sensitivity. J Investig Dermatol Symp Proc 2005; 10: 2957.
Dawson TL Jr. Malassezia globosa and restricta: breakthrough understanding of the etiology and treatment of dandruff and seborrheic
dermatitis through whole-genome analysis. J Investig Dermatol Symp
Proc 2007; 12: 1519.
Lee YW, Lee SY, Lee Y, Jung WH. Evaluation of expression of lipases
and phospholipases of Malassezia restricta in patients with seborrheic
dermatitis. Ann Dermatol 2013; 2: 31014.
29
30
31
32
33
34
35
36
Iinuma K, Sato T, Akimoto N et al. Involvement of Propionibacterium
acnes in the augmentation of lipogenesis in hamster sebaceous glands
in vivo and in vitro. J Invest Dermatol 2009; 129: 211319.
Patin~o-Uzca tegui A, Amado Y, Cepero de Garc a M et al.
Virulence gene expression in Malassezia spp. from individuals with
seborrheic dermatitis. J Invest Dermatol 2011; 131: 21346.
DeAngelis YM, Saunders CW, Johnstone KR et al. Isolation and
expression of a Malassezia globosa lipase gene, LIP1. J Invest Dermatol
2007; 127: 213846.
Ishibashi Y, Sugita T, Nishikawa A. Cytokine secretion profile of
human keratinocytes exposed to Malassezia yeasts. FEMS Immunol
Med Microbiol 2006; 48: 4009.
Watanabe S, Kano R, Sato H, Nakamura Y, Hasegawa A. The effects
of Malassezia yeasts on cytokine production by human keratinocytes.
J Invest Dermatol 2001; 116: 76973.
Kerr K, Darcy T, Henry J et al. Epidermal changes associated with
symptomatic resolution of dandruff: biomarkers of scalp health. Int J
Dermatol 2011; 50: 10213.
Thomas DS, Ingham E, Bojar RA, Holland KT. In vitro modulation of
human keratinocyte pro- and anti-inflammatory cytokine production
by the capsule of Malassezia species. FEMS Immunol Med Microbiol
2008; 54: 20314.
Baroni A, Orlando M, Donnarumma G et al. Toll like receptor 2
(TLR2) mediates intracellular signaling in human keratinocytes in
response to Malassezia furfur. Arch Dermatol Res 2006; 297: 2808.
Вам также может понравиться
- Normal Size of Thoracic Aortic Segments.: Foto PaДокумент2 страницыNormal Size of Thoracic Aortic Segments.: Foto PaRachmi AnnisaОценок пока нет
- Wolff. K, Johnson. R.A, Suurmond. D - 2007. Fitzpatrick's, The Color Atlas andДокумент1 страницаWolff. K, Johnson. R.A, Suurmond. D - 2007. Fitzpatrick's, The Color Atlas andRachmi AnnisaОценок пока нет
- Skizofrenia Paranoid: Bed Site TeachingДокумент2 страницыSkizofrenia Paranoid: Bed Site TeachingRachmi AnnisaОценок пока нет
- Obat Anti-Inflamasi Nonsteroid (AINS) : ReferatДокумент1 страницаObat Anti-Inflamasi Nonsteroid (AINS) : ReferatRachmi AnnisaОценок пока нет
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Integumentary System - NUR1019 - 20sept2022Документ33 страницыIntegumentary System - NUR1019 - 20sept2022琪琪Оценок пока нет
- Principles of Equine Dentistry, Klugh, 2010Документ241 страницаPrinciples of Equine Dentistry, Klugh, 2010alicata123100% (1)
- Mechanisms of Action of AntibioticsДокумент4 страницыMechanisms of Action of AntibioticsClarissa Marie LimmangОценок пока нет
- Polymorphic Phases in Locusts Antomonology Final YearДокумент29 страницPolymorphic Phases in Locusts Antomonology Final YearMohammad SalmanОценок пока нет
- Septic Peritonitis in DogsДокумент7 страницSeptic Peritonitis in DogsTactvisОценок пока нет
- PAPER (ENG) - Pseudodysphagia Due To Omohyoid Muscle SyndromeДокумент6 страницPAPER (ENG) - Pseudodysphagia Due To Omohyoid Muscle SyndromeAldo Hip NaranjoОценок пока нет
- Polyvagal TheoryДокумент24 страницыPolyvagal Theorymkrnhr100% (7)
- Clinical Laboratory Hematology 3rd Edition Mckenzie Test BankДокумент35 страницClinical Laboratory Hematology 3rd Edition Mckenzie Test Bankgeincupola.06zi100% (28)
- Vomiting: Compendium (Yardley, PA) February 2009Документ10 страницVomiting: Compendium (Yardley, PA) February 2009Vini SasmitaОценок пока нет
- Behaviours Learned Through Classical ConditioningДокумент6 страницBehaviours Learned Through Classical Conditioningapi-314561050Оценок пока нет
- Pathophysiology, Bone CancerДокумент7 страницPathophysiology, Bone CancerMaria Grace Raquel Ormeneta100% (1)
- Pineapple Smoothie DNA Isolation Laboratory ReportДокумент4 страницыPineapple Smoothie DNA Isolation Laboratory ReportKrizelle Ann HugoОценок пока нет
- A Uri Culo TherapyДокумент322 страницыA Uri Culo Therapyserafim67100% (1)
- Marfan Does Not Mean Martian - 0Документ28 страницMarfan Does Not Mean Martian - 0Anonymous S5bG7pОценок пока нет
- Answer Key Simulated Pre Board Set 4 NagaДокумент11 страницAnswer Key Simulated Pre Board Set 4 NagaRaymark MoralesОценок пока нет
- Jim Nursing Essay - Chronic Obstructive Pulmonary Disease (COPD) .Документ8 страницJim Nursing Essay - Chronic Obstructive Pulmonary Disease (COPD) .SarahJaneОценок пока нет
- 10578200Документ90 страниц10578200Bradda Derru Nesta MarleyОценок пока нет
- USMLE Step 1 High Yield TopicsДокумент13 страницUSMLE Step 1 High Yield TopicsNixon GoyalОценок пока нет
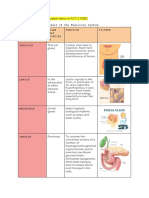
- Endocrine System ChartДокумент2 страницыEndocrine System ChartValeria Guadalupe Ramírez Moctezuma100% (2)
- 1111111111111111111111111111111Документ7 страниц1111111111111111111111111111111Andrei Jose V. LayeseОценок пока нет
- Blood ClottingДокумент3 страницыBlood Clottingridwan100% (9)
- Medicinski Engleski - SkriptaДокумент12 страницMedicinski Engleski - SkriptaNikola Kudoić100% (1)
- CHEM 151 (Chapter 3)Документ4 страницыCHEM 151 (Chapter 3)Chantel AceveroОценок пока нет
- AIDA+MEDICAL+STATEMENT+v2 2+june+2019Документ2 страницыAIDA+MEDICAL+STATEMENT+v2 2+june+2019AB OutОценок пока нет
- PubertyДокумент5 страницPubertyalok nayakОценок пока нет
- Hyperpituitarism Group e Bsn3Документ17 страницHyperpituitarism Group e Bsn3Mari IllustriousОценок пока нет
- Reviwer 29Документ3 страницыReviwer 29chaSephОценок пока нет
- Effect of Music Therapy On A Brainwave For Stress RecognitionДокумент3 страницыEffect of Music Therapy On A Brainwave For Stress RecognitionIJIERT-International Journal of Innovations in Engineering Research and TechnologyОценок пока нет
- Night Shifts Can Also Be TiringДокумент2 страницыNight Shifts Can Also Be TiringMariccon Celestial PalmaОценок пока нет
- Don Tolman - FDR3 - WholeFoodMedicines PDFДокумент176 страницDon Tolman - FDR3 - WholeFoodMedicines PDFLerere Allala100% (4)