Академический Документы
Профессиональный Документы
Культура Документы
Lower Extremity Amputations
Загружено:
alinutza_childАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Lower Extremity Amputations
Загружено:
alinutza_childАвторское право:
Доступные форматы
Volume 7, Number 2
June 2005
Introduction
his issue of Operative Techniques in General Surgery marks
a changing of the editorial guard. As the new editor of
OTIGS and after reviewing the past issues managed and overseen by my predecessors, I recognize the challenge of maintaining the journals quality and relevance that Drs. Van
Heerden and Farley achieved during their tenures. The publishers and I thank them for their excellent past work and the
fine example they have set for our future issues.
OTIGS is first and foremost a practical journal, published
for the operating general surgeon. In this regard, it has an
immediate relevancy for its readership and provides information and techniques that can be applied in a very practical
way. However, general surgery is changing, as are many other
things in health care, and so must this journal. The general
surgeon of today increasingly needs to become more adept
and competent in techniques and procedures that in previous
years were usually delegated to the subspecialist. This is facilitated by the subspecialist who, as he or she concentrates
on evermore esoteric operations, passes the more commonly
performed specialist techniques onto the general surgeon.
OTIGS will play its part in this educational process by presenting, in a measured and practical fashion, subject matter
that reflects this increasing degree of operative sophistication
that is taking place in general surgery. Subspecialists and
surgeons with specialty interests will discuss and illustrate
techniques that are increasingly becoming the responsibility
of the general surgeon.
1524-153X/05/$-see front matter 2005 Elsevier Inc. All rights reserved.
doi:10.1053/j.optechgensurg.2005.08.002
This issue, Lower Extremity Amputations, is an excellent
example of this crossover between specialist and general
surgeon. Despite the association of amputation procedures
with the vascular and orthopedic specialties, many amputations are still done by general surgeons. Besides arterial insufficiency, amputations are used for the treatment of malignancies, trauma, and extremity sepsis, all clearly the bailiwick of the
general surgeon. The methods of amputation that result in the
best possible long term functional and cosmetic outcome are of
critical importance to the patient and paramount concern to the
surgeon, general or otherwise. In this issue, the subtleties involved in choice of amputation, flap construction, soft tissue/
bony prominence cushioning, and wound healing are carefully
explained and illustrated by specialists in vascular and orthopedic surgery. General surgeons can certainly take advantage of
these specialists technical advice to promote improved operative outcomes and patients well being.
Walter A. Koltun, MD
Professor of Surgery,
Peter and Marshia Carlino Professor
of Inflammatory Bowel Disease Chief,
Section of Colon and Rectal Surgery,
Penn State College of Medicine,
Milton S. Hershey Medical Center
Editor-in-Chief
61
Introduction and General Principles
Robert G. Atnip, MD
he feet and toes are surely among the most abused and
least appreciated regions of the human anatomy. There
are few structures in the body, indeed, even fewer man-made
devices or appliances, that are subjected to such intense repetitive, relentless punishment in such an unforgiving environment, yet expected to perform without flaws. Though not
the only animal species capable of mobility on two feet, the
human is, nonetheless, the only species that is exclusively
bipedal and cannot fly. With human girth and mass showing
unprecedented increases of heretofore unimagined demographic proportions, it appears that the human foot will be
tested in the future more than it has ever been tested in the
past.
Only those with bad feet can truly appreciate the bliss of
having good feet. Yet bad feet and good feet alike are seldom
afforded the attention and respect that should be their due.
The good foot is expected to support a mass 200 to 300 times
its own, on a surface area no more than 1% of the body as a
whole, with such assumed performance and durability that
its owner will likely give it no conscious regard. The bad foot
is expected to heal quickly and completely, and preferably
while still in use. The inconvenience of a bad foot is one
which most persons tolerate poorly and with great impatience. But rather than inspiring awe and reverence for the
miracles that the foot routinely performs, such temporary
disabilities more often provoke vexation and resentment at
the unwelcome interruption of mobility. So the host forces
his foot to function while dysfunctional, to heal while unhealthy, and to again withstand the trauma and neglect that
caused the original problem. It is the fate of the feet and toes
to be taken for granted until catastrophe ensues, and even
beyond.
Advances in modern podiatry, plastic surgery, orthopedics, and vascular surgery offer hope and relief for the myriad
problems that beset the modern foot. Most such problems
can either be prevented, or alleviated with orthotic appliances, or corrected with relatively minor surgery. Indeed,
many body parts, including the hips and knees, are ultimately more likely than the foot to fail and require major
surgery. Unlike those structures, however, the foot cannot be
Penn State Hershey Medical Center, College of Medicine of the Pennsylvania
State University, 500 University Drive, Hershey, PA.
Address reprint requests to Dr. Robert G. Atnip, Professor of Surgery and
Radiology, Chief of Vascular Surgery, Penn State Hershey Medical Center, College of Medicine of the Pennsylvania State University, 500 University Drive, Hershey PA 17033-2390. E-mail: ratnip@psu.edu
62
1524-153X/05/$-see front matter 2005 Elsevier Inc. All rights reserved.
doi:10.1053/j.optechgensurg.2005.07.001
replaced. Irreversible disease or injury of the toes and feet
leads to amputation. Amputation surgery itself has advanced
in modern times, though perhaps not as dramatically as the
science of prosthetics. Fortunately, the end result for most
patients is a return to functional ambulation.1,2
The articles and illustrations in this journal present the
essential considerations and techniques for successful lower
extremity amputation, whether of a single toe or of the entire
limb. The methods depicted herein represent standard and
widely employed techniques for amputation surgery. As with
any surgical procedure, individual surgeons will modify their
technique as necessary to achieve optimal outcomes for each
individual patient.
Factors Leading to Amputation
Patients presenting for consideration of toe or partial foot
amputation typically have some combination of injury, ulceration, tissue necrosis, and infection. A variety of conditions
and factors exist that predispose to the occurrence of limbthreatening tissue loss in the foot. In patients with diabetes
mellitus, the processes of infection, ischemia, and neuropathy have been expressed as a combined classic triad of risk
factors, and many similar groupings could be proposed for
diabetics and nondiabetics alike. An alternate and helpful
way of organizing these many influences is to segregate them
into local and systemic categories.
Local Factors
Numerous inherent characteristics of the foot itself are responsible for its vulnerability to injury and infection. The
very purposes of the foot are to bear the weight of the body
and provide mobility, and the design of the foot is specific for
those purposes. The bony architecture provides surfaces that
tolerate high pressures by spreading them over as much area
as possible, while allowing the flexibility needed for all varieties of locomotion. Some loss of that architecture can be
tolerated, but more so on the dorsal surface than the plantar.
Deformities that cause pressure points on the plantar surface
are the cause of much dysfunction, disability, and limb loss.
On the dorsal surface, weight bearing is less of an issue, but
an equally serious problem is the thinness of the skin and soft
tissue and relative lack of protection of the underlying tendons, muscles, and joints. Full-thickness skin loss on the
dorsal surface can result in exposure and dessication of the
underlying fascia and tendons, often with few reconstructive
Introduction and general principles
63
options. Similar problems occur when ulcers develop over
joints on the dorsum of the toes or sides of the foot.
Although well padded on the plantar aspect, the calcaneus
is famously vulnerable on its posterior surface where soft
tissue coverage is much thinner. Decubitus ulcerations in this
area are typically full thickness, often down to the calcaneal
bone itself, and highly resistant to healing unless pressure
relief and optimal perfusion can be achieved.
In many patients, especially diabetics, limb loss is initiated
by seemingly trivial lesions on the toes. Ill-fitting footwear,
nail care accidents, and other minor trauma are the most
common causes, often in the setting of sensory loss and bony
deformity from diabetic polyneuropathy. Chronic fungal and
dermatophyte infections of the toes can act alone or with
other factors to trigger local skin injury and subsequent necrotizing infections.
Patients and their physicians are equally culpable in failing
to recognize minor foot problems, and in failing to treat them
aggressively in the early reversible stages. Though persons
with normally innervated feet are exquisitely sensitive to pain
and pressure, those with neuropathic feet may be completely
unaware of even the worst noxious stimuli unless the injury is
detected visually. Even when blisters, ulcers, lacerations,
paronychiae and other warning signs are noticed and reported, all too many physicians do not recognize these small
lesions for the great havoc that they can wreak, particularly in
the presence of ischemia and systemic disease.
effective treatment options for peripheral arterial disease has
never been greater, but there is much progress to be made in
making treatment available to those with limb-threatening
ischemia in time to prevent major tissue loss.
Other systemic factors that target the foot and toes are
becoming increasingly prevalent. Though not widely discussed in this particular context, obesity cannot be ignored as
a disease whose wide-reaching effects certainly include enormous stress on feet that must support hundreds of pounds of
excess body mass. Obesity leads to increased trauma to the
feet, and promotes lipid disorders, hypertension and diabetes. Obese patients are often physically unable to perform
adequate skin and nail care of the feet, and can develop
substantial edema due to venous or lymphatic insufficiency.
Obese patients pose daunting technical challenges for arterial
reconstructive surgery, but fare even worse with limb loss.
Finally, and in addition to the immunosuppression associated with diabetes, there are numerous pharmacologic
agents that inhibit the immune system and thereby enhance
other processes that lead to skin breakdown and infection in
the feet. Corticosteroids, cyclosporin, methotrexate, plaquenil, and newer immune-targeted drugs not only lower resistance to infection but may also impair tissue integrity, inhibit
healing, and even promote accelerated atherosclerosis.
Systemic Factors
The desired end results of amputation are complete healing,
and restoration of function. An amputation is a reconstructive procedure, and as such requires precise and exacting
technique. For most patients, there will be no second chance
for healing, short of a second higher amputation, an outcome
both physically draining and emotionally devastating. Patients facing limb loss are keenly aware of this possibility, and
often fear it more than the primary procedure itself. Re-amputation can never be entirely prevented or avoided, and its
likelihood can only be minimized by the most rigorous surgical judgment and technique.
Diabetes mellitus is unquestionably the dominant systemic
cause of major limb loss in adults. The risk of limb loss in
patients with this disease is many fold higher than in comparable nondiabetic populations, owing to effects such as immunosuppression, neuropathy, and accelerated vascular disease. Ischemia and neuropathy have a greater incidence in
the lower extremity compared with other anatomic regions,
and clearly act in concert with local factors to promote injury,
infection, and necrosis of the foot and toes. Much remains
unknown regarding specific mechanisms of interaction between this disease and its host, perhaps in part because diabetes is not a single disease entity. Much attention has been
focused on the question of whether complications of diabetes
can be avoided or ameliorated by better glucose control. Yet
even with dramatic progress toward understanding diabetes,
key questions remain unanswered and key misconceptions
persist, especially as concerns the interplay of diabetes and
peripheral vascular disease.
In the classic triad of infection, neuropathy, and ischemia,
the latter entity may well be the least understood. The gaps in
knowledge begin at the level of basic science, but are pervasive in the clinical realm, where the difficulty lies not nearly
so much in a failure to know as in a failure to recognize and
apply that which is known. Although reconstructible atherosclerosis of the named axial arteries of the lower extremity is
the primary cause of ischemia in diabetics and nondiabetics
alike, a well-entrenched fallacy still circulates, even among
experienced clinicians, that nonreconstructible small vessel
disease of the foot is equally prevalent. Such a misperception
underlies a false belief that ischemia is untreatable, which in
turn allows it to go undiagnosed. In fact, the number of
General Principles
of Amputation
The Decision to Amputate
Although generally viewed as the last resort, amputation is,
like all surgical procedures, one that will turn out best for the
patient if it is done for the right patient and the right reason at
the right time. Amputation must never be viewed as a default
procedure that is employed only after all other options have
been explored. Such a perception fails to recognize the reconstructive nature of amputation surgery, and thus results
in grave disservice to the patient. Amputation must be among
the options considered by any clinician, medical and surgical
alike, called to treat the patient with serious infection, ulceration, ischemia, or injury of the lower extremity. In selected
cases, amputation should be the primary procedure. In all
others, the possibility of amputation should be incorporated
early into the physicians thinking, to ensure that the chosen
treatment regimen does not needlessly compromise the
chance of successful amputation should the need arise.
Amputation is generally indicated to control refractory infections, or to treat pathology of the foot that is either irreversible or so far advanced that healing of a functional foot is
R.G. Atnip
64
not feasible. Amputation is usually an elective procedure, but
may become urgent in cases of aggressive local sepsis, especially if accompanied by systemic toxicity. In such cases, the
patient may require open or guillotine amputation to limit
the spread of infection or to avert life-threatening sepsis. The
level and extent of amputation in these circumstances will be
dictated by both local and systemic factors, but must be chosen to ensure swift and effective reversal of the septic process.
Thorough drainage of deep space infections and debridement of wet gangrene are essential to halt propagation of the
infection. Aggressive initial surgery in these patients will usually preserve ultimate limb length and function rather than
compromise them.
In the more typical elective amputation, the surgeons goal
is to select the level of amputation that will optimize both
healing and function, with the recognition that in most cases,
these dual requirements are at cross purposes. In the presence of normal perfusion to the foot, the patient will, as a
rule, obtain optimal function from an amputation that spares
as much length and tissue as is technically possible. Contrariwise, in the face of trauma, ischemia, or any other circumstance that compromises tissue perfusion, the surgeon must
face a fundamental dilemma: the chance of healing and the
chance of function vary inversely with one another. Perfusion
and healing improve with higher amputations, while function will steadily decline. In each such patient, therefore, the
surgeon will need to carefully analyze the arterial flow to the
limb, optimize it however possible, and then essentially prioritize between function and healing. Factors to be considered in this process include a detailed knowledge of the patients psychosocial history, past and current functional
status, general medical condition, rehabilitation potential,
and an objective assessment of the healing potential of the
selected amputation level(s).
Much has been written about choice of amputation level,
but as yet, no specific tool or technology has proven any more
accurate than the combination of physical examination and
bedside Doppler. Basic surgical principles dictate that amputations are not likely to heal if performed through or near
zones of active cellulitis, suppuration, severe ischemia, or
frank necrosis. The severity of all these conditions can typically be determined by careful physical examination. In the
case of ischemia, however, additional useful information can
be obtained with a portable continuous-wave Doppler, supplemented if necessary by simple noninvasive testing, such as
photoplethysmography (PPG) and transcutaneous oximetry
(TCpO2). Other more sophisticated studies such as laser
Doppler velocimetry and Xenon perfusion are much less
widely used, and do not appear to offer any greater accuracy
of prediction.3
Bedside doppler examination includes quantitative (ankle
systolic pressure, ASP) and qualitative (signal quality) information, which both complement and objectify the basic palpation of femoral, popliteal, and pedal pulses. A manual
pulse examination is essential, and can be surprisingly accurate in predicting healing. At any chosen level, the presence
of a palpable pulse at the nearest proximal joint is associated
with healing rates of 90% or higher, whereas those rates drop
significantly if pulses are palpable only at two or more joints
removed from the selected site. Studies have differed as to the
exact relationship between ankle pressure (or ankle-brachial
index, ABI) and the success of healing, but most surgeons
would attempt a toe or partial foot amputation in a nondiabetic
if the ASP were greater than 80 mm Hg, and there were no
other contraindications. As ASP is often inaccurate or not
measurable in diabetics with calcified tibial arteries, the clinician will often find toe systolic pressures or PPGs more
helpful. Toe pressures greater than 40 mm Hg correlate with
improved healing, as do pulsatile PPG tracings. The usefulness of transcutaneous oximetry is debatable, due to a rather
wide range of indeterminate values.
The possibility of limb amputation should enter early into
the thinking of those caring for the patient with a threatened
limb, but should only be enacted after the most thoughtful
and deliberate analysis, a process which must include the
patient and family. Uncertainty of outcome is a given. In that
context, however, the surgeons efforts to ensure healing and
preserve function must be based on as much objective information as possible, and on the exercise of consummate judgment and technical skill.
General Technical Principles
General
Amputation surgery has never been and is not likely to become a popular pursuit among surgeons of any specialty. It is
neither especially challenging nor sophisticated, and does
not require advanced technology. In the era of advanced
endoscopic surgery, complex endovascular intervention,
joint replacement, and nearly miraculous plastic reconstructive surgery, amputation surgery seems to have changed little
since the 19th century. It is no exaggeration to argue that the
persisting stereotype of major limb amputation is that of the
Civil War battlefield.4 Amputation surgery is distasteful and
disturbing to many physicians (and quite a few surgeons),
and is abhorrent for most persons to contemplate. Yet, when
done successfully and well, amputation is not just reconstructive, but also redemptive, capable of transforming recalcitrant suffering and incapacitation into healing and rehabilitation, albeit, at a great and nonrefundable cost. To this
endeavor, the surgeon must apply every skill at his or her
disposal.
In performing an amputation, the surgeon must transect,
ablate, cauterize, and sever, often with large instruments and
bold strokes. But in the same procedure, the surgeon must
debride, smooth, sculpt and re-shape, with movements both
precise and delicate. It is essential not only to possess each set
of skills, but to know when each is needed. Whether a step in
the procedure calls for strength or subtlety, every sequence of
action must be performed with control and clear intention. In
amputations, as in many types of surgery, there is a high price
for haste and carelessness. By long tradition, amputation surgery is often the first procedure performed by novice surgical
trainees, but there is no better time than the beginning for
these young surgeons to learn under close supervision that
amputation requires no less skill and no less attention than
the more advanced procedures they will learn later in training.
Soft Tissue
The single most important technical aspect of amputation (at
any level) is careful handling of tissue. Even the ablative
Introduction and general principles
aspects of the procedure must be done with as little injury to
the transected edges as possible. Virtually all patients who
require amputation have impaired tissue integrity, to which
is added the unavoidable injury of the amputation itself. Yet,
with appropriate technique, the degree and extent of injury
can be controlled. Proper use of the proper tools will enable
the surgeon to divide tissues cleanly, rather than tearing,
breaking, avulsing, or crushing. Particular attention is necessary to protect the skin edges from careless blunt or sharp
injury, which can lead to failure of primary healing. It is
strongly recommended to avoid use of forceps on the skin
edges at any time during an amputation.
One of the more common technical and judgmental errors
in amputation surgery is attempted wound closure under
tension, an error usually culminating in stump breakdown.
Avoiding this error requires forethought from the beginning
of the case, and careful planning throughout. Flaps must be
designed to allow closure without tension. If there is serious
doubt that this can be accomplished, the surgeon should
consider a different method, or even a more proximal amputation. Once committed, however, the surgeon should take
whatever additional time is necessary to sculpt the flaps and
successfully close them. Helpful maneuvers may include further shortening and recessing of bone stumps, and judicious
debulking of soft tissues, as long as blood supply is not compromised.
Bone
The steps of dividing and shaping the bones must be handled
differently in each amputation, but some general concepts
apply. Bones should be transected through the shaft, and
amputations through joints should generally be avoided. Articular cartilage receives its oxygen and nutrient supply from
the synovial fluid, and is at high risk for necrosis if the articular surface is left intact within an amputation wound. Although this particular problem can be averted by removing
the exposed cartilage, an equally significant problem is that
bony articular prominences generally do not make good amputation stumps.
Bones should be methodically stripped of their periosteum, and then transected cleanly with minimal splintering
and fragmentation. Any bone fragements and splinters must
be removed from the wound. Bone edges should be meticulously smoothed, especially in those areas that will lie closest
to the skin. In some cases, beveling of the bone stump is
advisable to avoid sharp edges and pressure points, such as
on the plantar surface of the foot. At every step, the surgeon
must be aware that orthopedic instruments (saws, drills, osteotomes, rongeurs, etc.) have great capacity to damage adjacent soft tissues if used carelessly.
Wound Closure
The meticulous technique employed in the performance of
an amputation must be carried through to placement of the
very last suture. Whether due to trauma, ischemia, local infection and inflammation, age, or other factors, the skin of an
amputation stump is seldom normal and healthy. Yet, the
success of the entire procedure often depends on that skins
ability to heal. Careless and indiscriminate handling of the
65
skin and soft tissues during closure can easily cause an otherwise successful amputation to fail.
The skin is, in fact, often the only tissue layer that can be
readily closed. When a digit or some part of the foot has been
amputated, the surgeon is typically confronted with one or
more bone stumps surrounded by transected joint capsule,
tendons, fascia, muscle, and subcutaneous fat. Depending on
the length of bone stump available, it may be possible to
recess the stump deep enough to allow separate closure of the
fascia or muscle over the bone. The advantages of deep closure coverage of bone and elimination of dead spaceare
substantial. Not infrequently, however, the level of resection
is such that the surgeon must be satisfied with a single layer
skin closure, trusting that the deeper tissues will be coapted
by default.
Specific techniques for closure of the skin vary widely and
are largely the province of personal preference. The author
finds much to recommend in an interrupted nylon, either
simple or vertical mattress, placed without use of forceps and
reinforced by fine Steri-strips. Subcuticular closure or skin
staples are popular in some quarters, although these methods
require more handling of the skin. Whatever method is used,
the goal should be precise alignment and apposition of skin
edges to create the best opportunity for primary healing.
Failure of the skin and subcutaneous tissues to heal primarily
is an ominous development, usually resulting in wound dehiscence and portending greater tissue loss.
The need may occasionally arise to place a wound drain in
an amputation stump, but only if clearly indicated. Standard
measures should be employed to obtain hemostasis, including direct pressure, judicious use of the electrocautery, topical use of local anesthetics containing dilute epinephrine, and
of course ligation of vessels. Even oozing wounds will usually
stop bleeding on re-approximation and closure of the tissues,
particularly if a bulky dressing is applied for added tamponade. If a drain is necessary, it should be inserted through a
separate stab wound, not through the suture line of the
stump; it should be positioned to drain dependently, and
should be removed within 48 hours. Suction drains are preferred to passive drains. A temporary vacuum dressing with
delayed primary closure may be considered in some circumstances.
Dressings
The dressing of amputation stumps is often a matter of religion more than science. Practitioners adopt their favorite
dressings through training and experience, and then adhere
to them fervently. Dressings can be soft or rigid, small or
large, occlusive or open. A good dressing will pad and protect
the stump, inhibit seromas and hematomas, absorb drainage,
immobilize joints, serve as a barrier to contamination, and in
all these ways, generally promote healing. Any given type of
dressing can succeed or fail to accomplish these goals depending on how it is applied. The most common and costly
error in dressing technique is to wrap the dressing too tightly,
resulting in pressure necrosis of the stump or adjacent areas,
which at best will delay healing, and at worst may require
re-amputation. Areas at risk for this complication include the
dorsum of the foot, the malleoli, the heel, and the patella.
Preventive measures include proper technique in applying
R.G. Atnip
66
the dressing, and early frequent dressing changes with skin
inspection, especially if the patient complains of more pain
than expected.
Open amputation stumps are generally handled differently
from closed stumps, with great variation in individual practice. The method chosen may depend on whether the surgeons intention is for early revision, delayed primary closure,
or secondary closure. The use of vacuum-assisted closure
techniques has become increasingly popular.
Postoperative Activity
Postoperative care routines are, again, very surgeon- and amputation-specific. Patient positioning, allowed activity, commencement of physical therapy and weight bearing, use of
antibiotics, and prophylaxis of deep vein thrombosis are all
matters of surgical judgment. A solemn reminder for all caregivers is that patients undergoing limb amputation are
known to be at high risk for eventual loss of the contralateral
limb due to the same factors that caused ipsilateral disease. Of
these factors, one is nosocomial, insidious, and completely
preventable: the calcaneal decubitus ulcer. It is thus imperative that patients who are at bedrest following amputation,
especially those with diabetic neuropathy, must be provided all
available measures to protect their heel(s) from pressure necrosis. Although a panoply of soft mattresses and foot appliances are available to pad the heels, the only fully reliable way
to prevent decubitus ulceration is to avoid all contact and
pressure on the area in question. In the case of the heels, this
can be accomplished by placing pillows under the calf and
ankle such that the heel is not in contact with any surface. In
combination with a well-padded appliance such as the
Rooke boot, and with attentive nursing care, this simple
measure will effectively prevent serious decubitus lesions of
the heel.
References
1. Esquenazi A: Amputation rehabilitation and prosthetic restoration.
From surgery to community reintegration. Disabil Rehabil 26:831-836,
2004
2. Persson B: Lower limb amputation. Part 1: Amputation methodsa 10
year literature review. Prosthet Orthot Int 25:7-13, 2001
3. Smith DG: Amputation. Preoperative assessment and lower extremity
surgical techniques. Foot and Ankle Clinics 6:271-296, 2001
4. Sachs M, Bojunga J, Encke A: Historical evolution of limb amputation.
World J Surg 23:1088-1093, 1999
Toe and Partial Foot Amputations
Robert G. Atnip, MD
ormal ambulation is a complex process made possible
by the architecture of the foot and by the machinery of
the neuromuscular axis. Amputation of any portion of the
foot will alter the process of ambulation in degrees ranging
from trivial to prohibitive, depending not simply on the
amount of tissue removed, but also on the existing health and
functional status of the patient. For any given patient, ambulation will be impaired in direct proportion to the amount of
tissue removed. Further consideration of this concept will be
included in the discussion of each amputation level in the
ensuing paragraphs.
The most commonly employed levels of amputation are
the phalangeal and transmetatarsal, each of which can be
single or multiple, and are sometimes performed in combination. Less common are amputations performed through
the midfoot (Chopart and Lisfranc), and hindfoot (Syme)
(Fig. 1).
to preserving the normal architecture. Multiple ligaments including the large plantar fascia are essential to create and
maintain joint stability.
Sensory innervation is supplied by five nerves: the superficial peroneal for the dorsal surface; the deep peroneal for a
very small area of the first web space; the sural for the posterior and lateral areas; the saphenous for the medial aspect;
and the posterior tibial for the plantar surface. Of these
nerves, only the posterior tibial is crucial for normal function,
as it provides protective sensation on the weight-bearing surface.
Arterial supply derives from the posterior tibial artery, the
dorsalis pedis (a continuation of the anterior tibial), and the
peroneal artery. The latter vessel ends in smaller branches at
the ankle, but the two tibial vessels extend into the foot to
form the plantar arches and directly nourish the forefoot and
toes. Each toe has medial and lateral digital arteries and
nerves.
Anatomy of the Foot and Toes
The complexity of the foot is illustrated by an accounting of
its components: 26 bones, 33 joints, and over 100 muscles,
ligaments, and tendons, in addition to fatty tissue, vessels,
and nerves, and its investing envelope of skin. These structures are somewhat artificially divided into three zones: the
forefoot, including the phalanges, sesamoids, and metatarsals
of the five digits; the midfoot, composed of the five tarsal
bones, and the hindfoot, made up of the talus and calcaneus.
The range of motion of the foot includes plantar flexion,
powered by the posterior compartment muscles (tibialis posterior and flexor digitorum), and innervated by the posterior
tibial nerve. Extension of the foot, also called dorsiflexion, is
enabled by the anterior compartment muscles (tibialis anterior and extensor digitorum), innervated by the anterior tibial
(deep peroneal) nerve. Eversion is performed by the peroneus muscles and is rather limited in range. Inversion derives
from the posterior muscles and is equally limited in range.
The intrinsic muscles of the foot (lumbricals and interossei)
complement the extrinsic forces to maintain balance, allow
for finer movements of the toes, and contribute signficantly
Penn State Hershey Medical Center, College of Medicine of the Pennsylvania
State University, 500 University Drive, Hershey, PA.
Address reprint requests to Dr. Robert G. Atnip, Professor of Surgery and
Radiology, Chief of Vascular Surgery, Penn State Hershey Medical Center, College of Medicine of the Pennsylvania State University, 500 University Drive, Hershey, PA 17033-2390. E-mail: ratnip@psu.edu
1524-153X/05/$-see front matter 2005 Elsevier Inc. All rights reserved.
doi:10.1053/j.optechgensurg.2005.07.002
Phalangeal Amputation
The hallux has two phalanges, and the other four digits have
three, with the distal phalanx being the smallest. Beyond this
simple anatomic difference, the hallux overshadows the
other digits in functional importance by virtue of its roles in
balance of the forefoot and in push-off during ambulation.
Although the second toe can adapt to some extent in the
absence of the great toe, patients who have lost the hallux
invariably notice a substantial difference in the mechanics of
walking, especially after transmetatarsal amputation. Amputations of the great toe should be performed for only the
strictest and most carefully considered indications.
Although amputation of only the distal part of a toe is
technically possible, there is little functional advantage to
having half or two-thirds of a toe, even the great toe. Certainly
in any situation where perfusion is abnormal, digital amputations are best performed through the base of the proximal
phalanx, leaving a relatively short stump with a better likelihood of healing.
Digital amputations are typically performed with a fishmouth technique, which is preferred to a circular incision in
all cases intended for primary closure. Since the vessels
course along the medial and lateral aspects of the toe, it is
sensible to orient the fishmouth in the anterior-posterior
(dorsal-plantar) direction, so that the bases of the flaps are
medial and lateral, including the digital vessels. Nonetheless,
many surgeons obtain equally good results from the use of a
67
R.G. Atnip
68
The ideal flaps will be just long enough to coapt without
tension, but too long is always preferable to too short.
When faced with inadequate soft tissue for closure, the surgeon can use standard plastic techniques to mobilize the flaps
further, or can attempt to shorten the bone, even to the point
of excising the entire base of the phalanx. The options in that
case are to convert to a transmetatarsal amputation (see next
section), or to leave the metatarsal head intact. In the latter
case, it is imperative to remove the articular cartilage to avoid
necrosis and infection of this nonvascular tissue layer.
As described in a previous section, closure of the skin can
be accomplished with the suture method and material of
choice, provided that the technique is as gentle and atraumatic as possible. A minimal number of sutures. combined
with interspersed thin adhesive strips, provide a secure closure with minimal tissue injury.
Transmetatarsal
Amputation (TMA)
This procedure consists of amputation of one or more toes
along with a portion of the corresponding metatarsal bone(s).
The success of the procedure depends heavily on the health
and integrity of the plantar skin and soft tissues that will
provide coverage of the bone stump and ultimately form the
weight bearing surface. Transmetatarsal amputation is a very
useful and effective method for treating ischemic necrosis of
the forefoot, and often represents the patients last hope for
salvage of a functional foot. In cases where the plantar tissues
Figure 1 The skeleton of the foot, showing the level of bony transection for each of the four standard toe or partial foot amputations.
Creation of the soft-tissue flaps for each of these procedures is described in more detail in the text.
medial-lateral fishmouth with anterior and posterior flaps. In
either case, the incisions are arc shaped and symmetric, each
encompassing a hemi-circumference of the toe. It is often
necessary for the apex of the flap to extend rather close to the
margin of necrosis, but the surgeon must visually verify that
the skin margins of the flap are viable and not grossly infected. If the surgeon has any doubt regarding the skin margins, the wound might be better left open temporarily.
The soft tissue of the toes is sparse, consisting of skin,
minimal subcutaneous fat with nerves and vessels, investing
fascia, and tendons within their sheaths. Flaps must therefore
be incised perpendicular to the skin, full thickness down to
the bone, preserving all soft tissue with the flap. The flaps
should initially be generously long (as the distal pathology
permits), with the intent of shortening them to optimal
length for a tension-free closure. After stripping of the periosteum, the bone should be amputated through the midshaft, and then shortened and smoothed with a rongeur
down to the base, taking care not to violate the metatarsophalangeal joint. The large flexor and extensor tendons
should be then be distracted, amputated sharply, and allowed to retract into the deeper soft tissues. Any final debridement of the flaps can then be performed (Fig. 2).
Figure 2 A simple amputation through the proximal phalanx of the
left great toe. Symmetric medial and lateral flaps have been created,
based on the digital arteries. The stump of the phalanx is visible in
the base of the wound, along with the cut ends of the extensor and
flexor tendons.
Toe and partial foot amputations
69
of the forefoot are extensively compromised, however, TMA
is unlikely to be a realistic option.
It is important to note that TMA includes resection of the
metatarsal head. Although sometimes tempting, amputation
of a toe through the metatarso-phalangeal (MTP) joint should
be avoided for several reasons. Leaving the metatarsal head
does not improve function, and instead creates a potential
pressure point that may predispose to recurrent ulceration
and infection. The bulk of the metatarsal head can make skin
closure more difficult. Since articular cartilage depends on
synovial fluid for its nutrient supply, the cartilage may die
once the joint has been disrupted. Removing the cartilage but
leaving the bony head offers no advantage over amputation of
the entire distal metatarsal.
Transmetatarsal amputation is indicated primarily in two
situations: necrosis or ulceration of the toe(s) at or proximal
to the level of the MTP joint; and/or plantar pressure ulceration over the metatarsal heads. The extent of the amputation
is dictated by the extent of necrosis, and can encompass a
single toe, two or three toes, or the entire forefoot. These
variations will be considered separately in the following paragraphs.
Single Outer-Toe TMA
The toe and its metatarsal are sometimes called a ray, and
the corresponding surgery can be called a ray amputation.
The most commonly performed single ray amputations are
those of the first or fifth toes. Each is performed by the use of
a racket-handle incision consisting of an elliptical cut
around the base of the affected toe, and a straight incision
starting at the proximal end of the ellipse and continuing
along the outer edge of the metatarsal shaft (Fig. 3). The exact
contour of the incision must often be modified by the pattern
of ulceration or necrosis of the toe, but must be designed to
preserve as much plantar skin and soft tissue as possible. It is
often convenient to use the elliptical incision to disarticulate
the toe at the MTP joint, and thus remove this ulcerated or
dead tissue from the surgical field before proceeding with the
deeper dissection. This technique has the added advantage
that the metatarsal is easier to visualize and isolate after the
toe itself has been removed (Fig. 4).
After disarticulation of the MTP joint, the joint capsule
must be sharply and completely separated from the metatarsal head. Great care must be taken in avoiding entry into the
MTP joint of the adjacent ray, and in avoiding injury to the
plantar soft tissues abutting the shaft of the metatarsal. (In
these tissues are located the arterial supply to the plantar
flap.) Once the head is free, one then proceeds with stripping
of the periosteum of the metatarsal shaft to the desired level
using a small elevator. The shaft is then divided with a bone
cutter and recessed with a rongeur so that the stump is beveled with the shorter edge on the plantar surface (to avoid a
pressure point) (Fig. 5).
The next step is to excise the remnants of the joint capsule,
which in the case of the first toe, will include the sesamoid
bone. These structures are virtually avascular and heal
poorly. The dissection is best done with a very sharp #15
scalpel blade, taking only the ligamentous and bony components, and sparing the plantar fascia and other soft tissues.
Once the tissue resection has been completed, one must
Figure 3 An example of the racket-handle type of incision used for
transmetatarsal amputation of the great toe. The racket joins the
handle over the medial aspect of the metatarso-phalangeal joint, and
the handle extends along the metatarsal shaft. This incision can be
modified for combined amputations of the first and second toes, and
can also be used for amputation of the fifth toe, or of the fourth and
fifth toes together.
then assess the closure potential of the dorsal and plantar
flaps. If at all possible, any redundancy should be trimmed
from the dorsal flap rather than the plantar, unless the plantar
tissue appears to be of poor quality. In cases where the flaps
will not approximate without tension, the surgeon has the
choices of resecting more bone, debulking the flaps, leaving
part of the wound open, or amputating the adjacent ray to
mobilize more soft tissue. When all is satisfactory, closure is
then performed as described in the preceding section.
Single Inner-Toe TMA
Transmetatarsal amputation of an inner toe (toes 2, 3, or 4)
can be a useful procedure, but requires modifications in technique. Because of the constraints imposed by the adjacent
rays, it is more difficult to perform isolated TMA of an inner
toe, and more difficult to obtain good closure. If the plantar
tissues are relatively normal, the amputation can be done
using the racket-handle technique, with the handle extending from the dorsal end of the ellipse along the dorsal surface
of the metatarsal shaft. Added difficulties occur when the
plantar skin is ulcerated or ischemic, in which case, it is
impossible to avoid an incision on the plantar weight-bearing
surface. In either case, the operation proceeds best by disarticulating and removing the toe at the MTP joint, freeing the
R.G. Atnip
70
Figure 4 Transmetatarsal amputation
of the great toe. The specimen has
been removed after disarticulation of
the metatarso-phalangeal joint. The
sesamoid bone has been carefully excised from the plantar flap. The
transected flexor hallucis longus tendon can be seen posterior to the shaft
of the metatarsal. The plantar flap is
redundant, and will need to be
sculpted and trimmed before closure.
head from the joint capsule (while not entering the adjacent
joints), stripping and resecting the desired length of shaft,
and excising the remnants of joint capsule before closing. The
essentially fixed position of the adjacent metatarsal rays can
make it rather difficult to close an inner-toe TMA without
skin tension. The foot can be wrapped to compress the metatarsals and reduce tension on the suture line, but only if
precautions are taken to avoid pressure ulceration from the
bandage itself.
Figure 5 Transmetatarsal amputation
of the great toe. The metatarsal shaft
has been cut on a posterior bevel, and
the plantar flap has been trimmed of
excess soft tissue. The flexor tendon
has been cut shorter than the bone.
The joint capsule of the adjacent second MTP joint is intact, and has not
been entered or disrupted.
Multiple TMA
Although in theory any combination of toes could be amputated at the TMA level, such a decision should take into
account the relative importance of the various toes in the
stability of the foot and the mechanics of walking. Significant
stability and function are lost with amputation of the great
toe, especially at the TMA level, and the loss is even greater if
the second toe is also taken. To perform TMA of the first three
toes would likely be a disservice to the patient, leaving him/
Toe and partial foot amputations
71
her with a narrow, tapered, and dysfunctional forefoot. Similarly, the more toes removed from the lateral aspect of the
foot, the greater the asymmetry and imbalance of forces on
the remaining rays.
The technique for multiple TMA is a simple modification
of that for first or fifth ray amputation. An ellipitical incision
is created to encompass the base of the affected toes, modified
as needed to incorporate any areas of dorsal or plantar necrosis. The racket handle then extends along the outer aspect of
the metatarsal shaft. Flaps are created in identical fashion to
standard TMA. The MTP joints are disarticulated, the metatarsal shafts amputated, recessed, and beveled appropriately.
The flaps are then sculpted and closed without tension.
Although preservation of the medial toes is more advantageous than saving the lateral toes, it is questionable whether
TMA of more than two adjacent rays should ever be performed. In patients with diabetic or other polyneuropathies,
amputations that create gross asymmetry of the forefoot are
associated with a notoriously high incidence of subsequent
breakdown and re-amputation. As a general rule, balance,
function, and stump integrity will be better with a complete
(full-foot) transmetatarsal amputation.
Full-Foot TMA
Amputation of the entire forefoot at the transmetatarsal level
is one of the most useful procedures in the surgical armamentarium. When properly performed, full-foot TMA results in a
symmetric stump with favorable weight distribution. Although there is no question that patients with TMA must
learn to adapt their balance, gait, and stride after loss of the
forefoot, most patients will be able to walk, either independently or with simple supportive devices. Foot orthoses or
custom shoes can be useful to facilitate walking, but prostheses are not necessary.
If the plantar tissues are intact, the plantar incision for
TMA crosses the foot as close to the base of the toes as possible. The dorsal incision is made across the mid- to distal
level of the metatarsal shafts, as dictated by the pattern of
forefoot necrosis (Fig. 6). The dorsal and plantar incisions are
then connected by axial incisions made along the shafts of the
first and fifth metatarsals. The result will be a plantar flap of
variable length. In developing the plantar flap, the incision
should be carried down to the MTP joints, which should all
then be disarticulated. This allows the surgeon to find the
proper plane along the plantar surface of the metatarsal head
and shaft. From the plantar approach, the metatarsal shafts
angle toward the dorsum of the foot as they traverse proximally, and it is imperative that the surgeon adhere closely to
the shafts to preserve the muscles and vessels of the plantar
flap.
The dorsal incision is carried directly down through the
soft tissues, extensor tendons, and dorsal vessels to the anterior surface of the metatarsal shafts. At the desired level, these
shafts are stripped of periosteum and divided with bone cutter or rongeur. Working simultaneously from the plantar
surface, the interosseus muscles are divided along with any
remaining ligaments and tendons, and the specimen removed. The metatarsal stumps should be recessed and beveled, shorter on the plantar aspect.
Remaining on the plantar flap at this point will be the
Figure 6 Flaps outlined for a full foot transmetatarsal amputation.
The plantar flap is long, and the plantar incision extends along the
base of the toes. The dorsal incision crosses transversely over the
mid- to distal level of the metatarsal shafts. Either the dorsal or
plantar incisions may need to be modified if there is ulceration or
necrosis of the forefoot.
sesamoid bones and portions of the joint capsules, which
should be carefully excised, leaving adjacent muscle and vessels intact. All potentially viable skin and soft tissue of both
dorsal and plantar flaps should be spared until the final stage
of the procedure. Excess tissue can be removed and flaps
trimmed during closure, once it is known how the flaps can
best be re-approximated.
In the presence of ulceration or necrosis on the plantar
surface, the placement of the plantar incision and the creation
of the plantar flap will need to be individualized. In the
common case of a neuropathic ulcer penetrating to the metatarsal head, the ulcer can be excised in elliptical or V-shaped
fashion, which in essence will create two plantar flaps and
hence require a final T-shaped suture line. If the plantar
necrosis is more medial or lateral than central, the remaining
plantar tissue can often be rotated to achieve final closure. In
such situations, some of the metatarsal shafts may need to be
amputated shorter than others to enable closure of the flaps
without tension. It is in these cases that the imagination and
reconstructive skill of the surgeon become especially important.
Like most amputations below the ankle, a full-foot TMA
lends itself to only one layer of closure, the skin. In essence,
the dorsal surface consists of skin, virtually no subcutaneous
fat, and a very thin layer of fascia. If the plantar flap is too
long, it should be shortened to eliminate redundancy and
dead space (and thereby minimize the chance of hematoma).
The optimal length is that which brings the plantar tissues up
72
R.G. Atnip
Figure 7 Closure of the transmetatarsal amputation with simple interrupted sutures. The metatarsal shafts
have been cut with a posterior bevel,
essentially flush with the dorsal incision. The plantar flap has been
sculpted to approximate the dorsal
tissue without tension or redundancy.
to abut and securely cover the bony stumps with minimal
dead space, while allowing the plantar and dorsal skin to be
sutured without tension (Fig. 7).
Given that the success and functionality of forefoot amputation are much superior to that of mid- or hindfoot
amputations, there can be a role for a certain surgical
license in performing modified TMA for patients with
extensive forefoot necrosis. One option is to amputate the
metatarsal shafts very short, provided that the surgeon is
aware of the dangers inherent in violating the tarso-metatarsal joints. Removal of the first and/or fifth metatarsal
bases will result in loss of part of the insertion of the
tibialis posterior and peroneus tendons, respectively. The
ensuing imbalance of forces on the TMA stump leads to
deformity, pressure ulceration, and impaired walking.
Wholesale entry into the tarso-metatarsal joints is tantamount to performing a Lisfranc amputation, which is discussed in the following section.
If the bone and deeper tissues are viable but local coverage
is inadequate, vacuum-assisted closure and/or skin grafting
may allow an open TMA to eventually heal. In rare cases,
the surgeon may wish to consider a free tissue transfer to
salvage the foot, but an almost ideal set of conditions must
pertain to justify such a complex undertaking. The indications, techniques, risks, and outcomes of free-tissue transfer
are beyond the scope of this monograph.
Midfoot Amputations
(Lisfranc and Chopart)
These two surgical procedures were introduced by French
surgeons in the 19th century, and they were supposedly first
employed in America by battlefield surgeons in the Civil
War. They hold out the prospect of saving part of the foot in
patients who fail or are not eligible for TMA, but they are
seldom used in modern amputation surgery. The chief disadvantage of the Lisfranc and Chopart procedures is that they
disrupt the tendinous attachments of the midfoot and predispose to stump deformities associated with dysfunctional ambulation. The loss of foot length and loss of tendon insertions
leaves the plantar flexors almost unopposed, resulting in an
equinus deformity, with a consequent shift of weight bearing
from the calcaneus onto the stump itself. Although technical
modifications have been introduced that partly compensate
for this imbalance of forces, midfoot amputation has still not
gained wide acceptance as an alternative to below-knee amputation. Braces and prostheses are usually required for
walking, and there is a relatively high incidence of conversion
to BKA.
The Lisfranc amputation is essentially a disarticulation of
the tarso-metatarsal joints, using a plantar flap for coverage
with a technique virtually identical to transmetatarsal amputation. The important technical point is to remove as much
articular cartilage as possible from the cuneiform and cuboid
surfaces to circumvent cartilaginous necrosis. Various tendon transfers, reattachments, and tendo-Achilles lengthening
(TAL) have been proposed to prevent equinus deformity, but
results are often suboptimal.
The Chopart amputation shortens the foot even further
by removing the entire mid- and forefoot through the
talo-navicular and calcaneo-cuboid joints. Once again, a
plantar flap is used for coverage, but problems with stump
deformity tend to be even more common than with the
Lisfranc.
Toe and partial foot amputations
Conclusions
Locomotion is a fundamental human activity made possible
by the structure and function of the foot. Most humans consider the potential loss of part or all of the foot as catastrophic,
and view amputation as a disfiguring and destructive procedure. Yet due to either trauma or disease, as many as 150,000
patients per year are confronted with the necessity for amputation surgery, virtually always with no realistic alternative.
For these patients, properly performed amputation surgery is
a reconstructive procedure that rehabilitates and restores quality of life, albeit, a different life than the patient might desire.
Although many patients have such advanced disease that loss
of the entire foot is inevitable, for some the goal of partial foot
salvage is achievable. This chapter has described a variety of
procedures that preserve structure and function of the foot
sufficient to enable ambulation without a limb prosthesis. To
achieve the best results for each patient, the surgeon perform-
73
ing amputations must approach each procedure with the
finest exacting technique and attention to detail worthy of the
craft.
Suggested Reading
Attinger C, Cooper P, Blume P, Bulan E: The safest surgical incisions and
amputations applying the angiosome priciples and using the Doppler to
assess the arterial-arterial connections of the foot and ankle. Foot and
Ankle Clinics 6:745-799, 2001
Crinnion J, Hicks D: Transmetatarsal amputation: an 8-year experience. Ann
R Coll Surg Engl 84:291-295, 2002
Funk C, Young G: Subtotal pedal amputations. Biomechanical and intraoperative considerations. J Am Podiatr Med Assoc 91:6-12, 2001
Pinzur MS, Pinto MA, Schon LC, Smith DG: Controversies in amputation
surgery. Instr Course Lect 52:445-451, 2003
Rumenapf G: Borderline amputations in diabetics open questions and
critical evaluation. Zentralblatt fr Chirurgie 128:726-733, 2003
Sanders LJ: Transmetatarsal and midfoot amputations. Clin Podiatr Med
Surg 14:741-762, 1997
Smith DG: Principles of partial foot amputations in the diabetic. Instr Course
Lect 48:321-329, 1999
The Syme Amputation
Sai Sajja, MD
riginally described in 1843 by James Syme, Professor of
Surgery in Edinburgh, Syme amputation continues to
generate controversy and debate regarding its role in traumatic injuries to the foot, peripheral vascular disease, and
diabetes. Syme reported the successful outcome in a case of
suppurative disease of the tarsus by disarticulation of the foot
at the ankle and removal of the malleoli flush with the lower
articular surface of the tibia.1 It is interesting to note that he
described this procedure twenty-two years before Joseph
Lister, his son-in-law, first embarked on his experiments with
antiseptic surgery.2 The procedure has remained popular
with Canadian and Scottish surgeons, but has found less
favor elsewhere.
The Syme amputation provides an end-bearing stump
with excellent weight bearing characteristics that is covered
with tough and durable skin of the heel flap. From a technical
standpoint, it is one of the most difficult amputations to
perform, and meticulous attention to detail is essential to
ensure a satisfactory outcome.
The primary disadvantages of Syme amputation are its
high failure rate and cosmetically unappealing bulbous
stump. Over the years, various modifications to the original
technique have been introduced to improve the cosmetic
appearance and outcomes in patients with peripheral vascular disease and diabetic foot infections. Wagner popularized a
two-stage technique for use in diabetic patients with an infected or gangrenous foot lesion.3 Sarmiento, in 1972, introduced a modification that consisted of osteotomy of the tibial
and fibular malleoli to narrow the medio-lateral diameter of
the distal end of the stump so that a more cosmetically acceptable prosthesis can be fitted.4
Indications
One of the most important requirements for a positive outcome when performing Syme amputation is patient selection.
The principal indications are congenital deformity of the foot
and traumatic foot injuries in which a viable heel pad remains. It can also be performed in patients with peripheral
vascular disease and diabetic infections of the forefoot. A
Penn State Hershey Medical Center, College of Medicine of the Pennsylvania
State University, 500 University Drive, Hershey, PA.
Address reprint requests to Dr. Sai Sajja, Fellow in Vascular Surgery, Penn
State Hershey Medical Center, College of Medicine of the Pennsylvania
State University, 500 University Drive, Hershey PA 17033-2390. E-mail:
ssajja@psu.edu
74
1524-153X/05/$-see front matter 2005 Elsevier Inc. All rights reserved.
doi:10.1053/j.optechgensurg.2005.07.003
two-stage procedure is recommended in these patients. During the first stage, the ankle joint is disarticulated, followed
six to eight weeks later by osteotomies of the malleoli. A
palpable posterior tibial artery pulse is considered essential
for healing following Syme amputation. In the presence of
vascular insufficiency, patient selection can be further refined
by Doppler studies and transcutaneous PO2 measurements.
An ankle-brachial index of 0.35 to 0.4 or an absolute Doppler
value of 40 to 70 mm of Hg is often quoted as critical to
wound healing.5 An absolute reliance cannot be placed on
these tests, as factors determining the ideal level of amputation in vascular patients are many and complex. Syme amputation should not be performed in the presence of ulceration
involving the heel pad, or when the viability of heel pad is
questionable. Although an insensate stump is generally considered a contraindication, Srinivasan reported good results
in twenty Syme amputations in patients with anesthetic
stumps.6 Gaine and McCreath also reported no problems in
three patients with neuropathic stumps in a review of fortysix cases of Syme amputation.7
Technical Principles
There are several important principles that must be observed
during the procedure to achieve successful outcome. These
were emphasized in the initial report by Syme and later by
Harris.1,2 The posterior tibial artery must be preserved as it
provides the blood supply to the heel flap. It is at risk during
the division of medial ligaments and malleolar transaction.
The heel pad must be dissected subperiosteally from the calcaneum. This ensures that the septae that run from the plantar aponeurosis to the periosteum of the calcaneum remain
intact. These tight compartments contain adipose tissue that
provides resilience and hydraulic resistance to the deforming
forces of weight bearing. If the loculi are opened, the fat is
extruded by pressure because they are no longer closed
spaces. Subperiostal dissection also protects the calcaneal
branches of the posterior tibial artery from injury. The heel
flap lined with periosteum adheres to the cut surface of tibia
more firmly and may allow new bone formation to ensure
firm fixation of the heel flap. The heel flap will contain the
origins of short muscles of the foot. Excessive debridement of
the heel flap should be avoided, as this can lead to damage to
the plantar aponeurosis. Overzealous trimming of the corners of the flap (dog ears) must be avoided, as it may compromise the viability of heel flap. The heel flap must be firmly
secured to the tibia.
The Syme amputation
75
Figure 1 The incision begins at the
distal tip of the lateral malleolus and
passes along the anterior aspect of the
ankle joint at a point one-finger
breadth inferior to the tip of the medial malleolus. It is further extended
across the sole of the foot to the lateral aspect, ending at the lateral starting point.
The tibia must be divided just above the dome of the
articular surface to provide a wide area for optimal weight
bearing. The plane of the tibial osteotomy must be parallel to
the ground to prevent migration of the heel pad over the cut
surface of tibia.
Operative Technique
Single-Stage Syme Amputation
After appropriate preparation and isolation of any forefoot
infective process, the incision is placed as follows. It begins at
the distal tip of the lateral malleolus and passes along the
anterior aspect of the ankle joint at a point one-finger breadth
inferior to the tip of the medial malleolus. The incision is then
extended across the sole of the foot to the lateral aspect,
ending at the lateral starting point (Fig. 1). All the soft tissues
are transected down to the bone.
The foot is then plantar flexed. The tendons crossing the
ankle joint are sharply divided. Anterior tibial artery is ligated
and anterior capsule of the ankle joint is divided (Fig. 2). The
knife is then inserted into the joint space between the medial
malleolus and talus and the deltoid ligament is divided taking
care to avoid injury to posterior tibial artery. The clacaneofibular ligament on the lateral aspect of the joint is sectioned
in a similar maneuver. A bone hook is placed on the posterior
surface of the talus and foot is further plantar flexed. The
posterior capsule of the ankle joint is then divided. This
brings the superior surface of calcaneus into view. Now begins the painstaking subperiostal dissection of calcaneus. The
dissection is continued posteriorly along the superior surface
of the calcaneus (Fig. 3). Tendo-Achilles is identified at this
stage and divided. The skin in this area is densely adherent to
calcaneum and care must be taken to avoid buttonholing.
Using a periosteal elevator or several sharp knives, the soft
tissues are separated from the medial and lateral surfaces of
the calcaneum. The foot is plantar flexed even more and the
dissection is continued along the inferior surface of the calcaneus to the end of the plantar flap. The entire foot with the
exception of heel pad is then removed from the field. The
posterior tibial artery is identified at the distal end of the heel
pad and ligated.
The flap is retracted superiorly and the soft tissues are
separated from the distal ends of tibia and fibula. The periosteum is divided one-half centimeter proximal to the joint
line so that the line of bone division is through the superior
most part of the articular surface of tibia (Fig. 4). This osteotomy should be performed so that the surface will be parallel
to the ground when the patient is standing. (The correct
plane may not necessarily be perpendicular to the long axis of
the tibia.) The sharp edges of the bone are rounded off. Only
minimal debridement of the soft tissues in the heel pad flap is
performed (see preceding section). The wound is irrigated
with antibiotic solution.
A variety of techniques are available to prevent heel pad
migration over the cut surface of the tibia. These include
taping the heel pad with adhesive tape, using a Kirshner wire
to transfix the heel pad to the bone, or drilling holes in the
anterior edge of tibia and fibula and suturing the plantar
fascia to the bone (Fig. 5). A suction drain is recommended
and can be brought out through a separate stab incision in the
distal third of the leg. The skin of the heel pad is then sutured
to the skin of the anterior flap using nonabsorbable sutures.
Redundant corners (dog-ears) are inevitable and should not
be sculpted or debrided. Finally, a padded rigid dressing is
applied to minimize swelling and to prevent heel pad slippage.
Two-Stage Syme Amputation
In the presence of gross infection of the forefoot in patients
who are not candidates for a more distal amputation and have
insufficient vascularity, a two-stage Syme amputation is preferable. Wagner has demonstrated that, in a carefully selected
group of patients, successful healing can be achieved in
ninety-five percent of patients using this approach.3
The first stage consists of disarticulation at the ankle
joint. The incision is placed one cm distal to the incision
described for the one-stage procedure. No attempt is made
to resect the malleoli or the articular surface of the tibia.
S. Sajja
76
Figure 2 The soft tissues are transected down to the bone. Foot is then plantar flexed and the tendons crossing the ankle
joint are sharply divided.
The Syme amputation
Figure 3 Subperiosteal dissection of the calcaneus is the most pain staking part of the procedure. This is best performed
with a sharp knife.
77
S. Sajja
78
Figure 4 The periosteum is divided one-half centimeter proximal to the joint line so that the line of bone division is
through the superior most part of the articular surface of tibia. This osteotomy should be performed so that the cut
surface will be parallel to the ground when the patient is standing.
The Syme amputation
Figure 5 To prevent heel pad migration over the cut surface of the tibia, holes are drilled in the anterior edge of tibia and
fibula and plantar fascia is sutured to the bone. A suction drain is recommended and is brought out through a separate
stab incision in the distal third of the leg. The skin of the heel pad is then sutured to the skin of the anterior flap using
nonabsorbable sutures.
79
80
S. Sajja
Figure 6 Elliptical incisions are
made over each malleolus so as to
excise any redundant skin and the
underlying bone.
Figure 7 The malleoli are dissected
subperiosteally and resected flush
with the articular surface of tibia.
The Syme amputation
Small incisions may need to be made on the sides of the
heel pad to accommodate the malleoli. Suction irrigation
drains may be placed to irrigate the wound with antibiotic
solution in the postoperative period. The skin is loosely
reapproximated, and a soft compressive dressing applied.
A plaster cast can be utilized at the discretion of the surgeon once the signs of infection subside and the drains are
removed.
The second stage or definitive amputation is performed
after six to eight weeks. Elliptical incisions are made
over each malleolus so as to excise any redundancy (Fig.
6). The malleoli are dissected subperiosteally and resected
flush with the articular surface of tibia (Fig. 7). The medial and lateral flares of the tibial metaphysis are resected to decrease the bulk of the stump. Holes are
drilled in the malleoli, and the plantar aponeurosis is sutured to the bones. The skin is closed with nonabsorbable
sutures.
Post-Operative Care and
Prosthetic Considerations
A well-padded rigid dressing is applied in the operating room
to control excessive edema and to enhance the adherence of
the heel flap to the under surface of the tibia. Weight bearing
is delayed until wound healing is assured. As the postoperative swelling decreases, the rigid dressing will need to refashioned to ensure proper stump molding. When weight-bear-
81
ing ambulation is to be instituted, an ambulatory cast should
be constructed by an expert prosthetist.
Conclusion
This chapter has discussed the historical aspects of and indications for Syme amputation. Particular emphasis is placed on the
technical aspects of the one-stage and two-stage Syme amputation. The surgical principles essential for a successful outcome
are outlined. While the role of Syme amputation is well established in congenital foot deformities and traumatic injuries of
the foot, with appropriate patient selection utilizing segmental
limb perfusion pressures and transcutaneous PO2 measurements, satisfactory results can also be obtained in patients with
vascular insufficiency and diabetic foot infections.
References
1. Syme J: Amputation at the ankle joint. Lond Edinb Month J Med Sci
3:93-96, 1873
2. Harris RI: Symes amputation; technical details essential for success.
J Bone Joint Surg [Br] 38:614-632, 1956
3. Wagner FW Jr: Amputations of the foot and ankle: current status. Clin
Orthop 122:62-69, 1977
4. Saramiento A: A modified surgical-prosthetic approach to the Symes
amputation: a follow-up report. Clin Orthop 85:11-15, 1972
5. Burgess EM: Amputations. Surg Clin North Am 63:749-770, 1983
6. Srinivasan H: Symes amputation in insensitive feet: a review of twenty
cases. J Bone Jont Surg [Am] 55-A:558-562, 1973
7. Gaine WJ, McCreath SW: Symes amputation revisited: a review of 46
cases. J Bone Joint Surg [Br] 78-B:461-467, 1996
Below Knee Amputation
Sai Sajja, MD
elow knee amputation (BKA) is the most commonly performed major limb amputation. With proper patient selection, primary healing can be expected in more than 90% of
patients following BKA.1 Similarly, nearly 90% of patients
with BKA have a realistic chance to ambulate with a prosthesis, compared with only 25% of patients with above knee
amputation.2 The advantages of BKA accrue primarily from
the many benefits of preserving the patients own knee joint.
Indications and
Contraindications
BKA is indicated in patients who have infection, gangrene,
nonhealing ulcers, or severe trauma of an extent that precludes salvage of a functional foot by any of the methods
discussed in prior chapters. It is also indicated in patients
with severe peripheral vascular disease who have failed arterial reconstruction or have presented with unreconstructible
disease and intractable rest pain. BKA is also sometimes performed for cure or palliation of neoplastic disease, or for limb
deformities that impair overall functional status.
BKA is the procedure of choice for patients meeting the
above indications and having a good prognosis for healing
and prosthetic ambulation. BKA (rather than AKA) can be
considered in nonambulatory patients if there is a reasonable
expectation that preservation of the knee joint would improve functional status (for example, by providing better balance and ability to transfer). In chronically ill, debilitated,
and/or institutionalized patients, BKA often leads to flexion
contractures of the knee, which in turn impair sitting and
transfer, and predispose to pressure ulceration. Similarly,
BKA should not be performed in patients with preexisting
flexion contracture of the knee exceeding 15. It is also contraindicated in the presence of anything more than minor
ulceration or skin necrosis proximal to the ankle joint. Spastic and rigid lower extremity following a stroke is also a
contraindication for BKA, as muscle spasticity will produce a
fixed flexion deformity.
Penn State Hershey Medical Center, College of Medicine of the Pennsylvania
State University, 500 University Drive, Hershey, PA.
Address reprint requests to Dr. Sai Sajja, Fellow in Vascular Surgery, Penn
State Hershey Medical Center, College of Medicine of the Pennsylvania
State University, 500 University Drive, Hershey, PA 17033-2390. Email: ssajja@psu.edu
82
1524-153X/05/$-see front matter 2005 Elsevier Inc. All rights reserved.
doi:10.1053/j.optechgensurg.2005.07.004
Technical Principles of
Below Knee Amputation
When BKA is performed for nonischemic causes, the ideal
bone length is 12.5 to 17.5 cm, depending on the patient
height. A general guideline is that 2.5 cm of bone length is
needed for each 30 cm of patient height.2 For ischemic limbs,
transection 10 to 12 cm below the joint line is recommended.
At a recommended minimum, three finger-breadths of tibia
distal to the tibial tuberosity should be preserved to enable
prosthetic fit and function. Amputation through the distal
third of the leg is not advisable, as fitting of the prosthesis
becomes more difficult, soft tissue coverage is inadequate,
and the blood supply is tenuous.
A variety of techniques have been described in the construction of BKA skin flaps, including equal anterior and
posterior flaps, long posterior flaps and medial and lateral or
skew flaps.3,4 Whichever the technique employed, care
should be taken not to dissect skin and deep fascia from the
underlying muscle, at risk of compromising flap viability.
While factors such as location of previous incisions influence the choice of flap design, the long posterior flap (posterior myoplasty) and skew flap techniques are the most
widely applicable. The method of equal anterior and posterior flaps can be used in patients with trauma or neoplasm, but is inadvisable in the setting of ischemia or
diabetic foot disease.
The advantages of posterior myoplasty are the superb soft
tissue coverage and the generally good perfusion afforded by
the calf musculature. Disadvantages include the bulbous
shape of the stump in obese or muscular limbs, and the
tendency to have redundant corners (dog ears) that may
lead to delay in rehabilitation. The skew flap technique is an
alternative that provides improved stump contour leading to
earlier prosthetic fitting. In a multicenter randomized control
trial, Ruckley and coworkers found that both techniques are
comparable in terms of healing, prosthetic limb fitting, and
mobility.5 Similar findings were confirmed in a recent Cochrane database systematic review.6 The choice of incision is
usually based on familiarity with a particular technique and
personal preference. The therapeutic goal of all the techniques is to produce a well-healed, pain free, and functional
stump that can be fitted with prosthesis. With the availability
of modern prosthetic techniques, a successful prosthesis can
be fitted to any well-healed BKA stump with a good functional outcome.
Below knee amputation
83
cised to provide a reference for the level of tibial division. The
level of transection of the tibia is further marked with a bone
saw.
The muscles of the anterior compartment are divided
slightly longer than the anticipated tibial stump length. The
superficial peroneal nerve is identified coursing just beneath
the fascia of the lateral compartment and is sharply divided
after gentle traction. The anterior tibial vessels are doubly
ligated and deep peroneal nerve is sharply divided after gentle traction.
The tibia is then divided with a reciprocating saw, and the
fibula is divided 1 to 2 cm shorter, using either a saw, or a
rongeur and bone cutter. Using a bone hook, the distal tibia
is pulled anteriorly and deep posterior compartment muscles
are divided 1 cm distal to the tibial section. The posterior
tibial and peroneal vessels are then identified, doubly ligated
and divided. Posterior tibial nerve is gently retracted and
sharply divided. The gastrocnemeus and soleus muscles are
divided in a tangential fashion to form a myofascial flap long
enough to reach the anterior fascia across the tibia (Fig. 2).
The anterior crest of tibia is beveled 45 to 60. Using a rasp or
pneumatic burr, all the sharp edges of the tibia and fibula are
smoothed. The tourniquet is released and hemostasis is secured. The wound is irrigated with antibiotic solution. A
closed suction drain is placed deep to the muscle flap, and
using absorbable sutures, the deep fascia of the posterior flap
is sutured to the deep fascia and periosteum of the anterior
flap. The skin is closed with interrupted nonabsorbable sutures.
Method of Long Posterior
Flap (Posterior Myoplasty)
Figure 1 Equal anterior and posterior flap method is commonly used
for nonischemic causes. The ideal bone length in this situation is
12.5 to 17.5 cm. The anteroposterior diameter of the leg at this level
is measured and equal anterior and posterior flaps are marked, each
half the diameter of the leg.
Operative Technique
Method of Equal
Anterior and Posterior Flaps
After appropriate anesthesia, the patient is positioned supine
on the operating room table. A pneumatic tourniquet can be
used to minimize blood loss. The desired length of tibia is
measured below the joint line and marked. The anteroposterior diameter of the leg at this level is measured and equal
anterior and posterior flaps are marked, each half the leg
diameter (Fig. 1). The skin and deep fascia are incised along
the marked incisions. As the anterior incision is being carried
over the anteromedial surface of tibia, the periosteum is in-
The operative techniques most commonly used in patients
with ischemic limbs are the long posterior flap method popularized by Burgess and the skew flap technique reported by
Robinson.3,4 The posterior myoplasty method is well established and is based on the principle of superior blood supply
of the posterior tissues.
The patient is placed supine on the operating table. A
tourniquet is typically not used on the ischemia extremity.
The anterior incision is marked at the chosen level (8.5 to
12.5 cm below the joint line, or 6 to 10 cm distal to the
tuberosity), and should encompass the anterior hemi-circumference of the leg. Two methods are available for determining the desired length of the posterior flap: either 2.5 cm
longer than the antero-posterior diameter of the leg at anterior incision line, or one-third the circumference of the leg at
that level (Fig. 3) Once this length has been determined, the
posterior incision is marked along the posterior hemi-circumference. The medial and lateral incisions connect the
anterior and posterior ones.
The skin and deep fascia are incised, and the anterior and
lateral muscles are divided with cautery. The anterior tibial
vessels are ligated and the peroneal nerves divided sharply as
they are encountered. If not already done, the medial, lateral,
and posterior incisions are deepened through the fascia. The
posterior incision should include the tendo-calcaneus. The
tibia is now sectioned with a reciprocating saw, and the fibula
is divided one centimeter shorter.
An individual surgeons preferred method can be used for
S. Sajja
84
Figure 2 After the division of tibia and fibula, the muscles of the deep posterior compartment are divided 1 cm distal to
the tibial division. The gastrocnemeus and soleus muscles are divided in a tangential fashion to form a myofascial flap
long enough to reach the anterior fascia across the tibia.
dividing the soft tissues of the posterior flap. The author
recommends the use of a long very sharp amputation knife.
With the tibia distracted anteriorly with a bone hook, and the
entire specimen on gentle caudal traction, the knife is inserted just along the posterior edge of the fibula. With swift
slicing motions, the path of the knife should follow a gentle
downward curve away from the fibula and toward the posterior incision. The result will be a beveled posterior myofascial
flap, with more muscle thickness proximally and less thickness distally (Fig. 4).
With this technique the posterior tibial and peroneal arteries are transected in uncontrolled fashion, but blood loss
is rarely significant, and the vessels can be promptly compressed once the specimen is removed. The posterior tibial
nerve will be visible on the flap, and should be distracted
distally, crushed proximally to inhibit neuroma, ligated at the
crush site with a 2-0 or 0 ligature, and then divided sharply so
that the stump retracts into the muscle mass posterior to the
tibia. Likewise, the sural nerve is identified along the distal
margin of the flap, distracted gently, ligated, and sharply
divided. The posterior flap is then sculpted to an optimal
shape and thickness.
The anterior edge of the tibia will lie directly beneath the
skin, covered only by subcutaneous fat and anterior fascia. To
avoid erosion and ulceration, the anterior one-fourth to onethird of the tibial circumference should be re-cut with a bevel
of 45 to 60, and the new edge thoroughly smoothed with a
rasp or high-speed pneumatic burr. The posterior flap is then
brought over the tibia and the fascial edges approximated
with a suture of choice. Drains are not usually needed for
amputations in ischemic extremities, but can be employed if
necessary. Skin is closed using interrupted nonabsorbable
sutures.
Skew Flap Method
The skin flaps are of equal length, semicircular, and are based
on a line around the limb at right angles to the long axis. The
circumference of the leg is measured at the chosen level of
tibial division and skin flaps are one fourth this in length. The
anterior starting point of the incision is 2 cm lateral to the
anterior border of the tibia, over the middle of the anterior
compartment. The posterior point is half way around the
circumference. The incision is extended for about 2 cm anteriorly to facilitate beveling of the tibia (Fig. 5). The skin and
deep fascia are divided along the marked incisions. No attempt is made to separate the deep fascia from the underlying
muscle.
Division of the anterior and lateral compartment muscles and neurovascular structures is performed as described previously. Tibia is sectioned at the chosen level
and fibula divided 2 cm proximally. It is beveled as described previously. A bone hook in the medullary cavity
will help retract tibia anteriorly, and the soft tissues are
separated from the tibia and fibula. The length of the gastrocnemeus and soleus muscle flap should be at least equal
to the diameter of the leg. The muscle bulk is thinned and
some of the muscle from the medial and lateral aspects is
removed while leaving the deep fascia intact (Fig 6). After
hemostasis and irrigation, the muscle flap along with the
attached deep fascia is brought anteriorly and sutured to
the deep fascia and periosteum. The skin flaps enclose the
posterior muscle flap and are closed with interrupted nonabsorbable sutures (Fig. 7).
Postoperative Management
Many experienced amputation surgeons employ rigid
dressings, applied in the operating room to help control
postoperative edema, protect the stump and prevent flexion contracture of the knee. Care should be taken to avoid
proximal constriction of the thigh. As the swelling decreases, a new rigid dressing may need to be applied. A
trained therapist should closely supervise prosthetic ambulation. After two to three weeks, elastic stump socks can
be used to further shape the stump before final prosthetic
fitting.
Below knee amputation
Figure 3 The incision is marked 8.5 to 12.5 cm below the joint line, or 6 to 10 cm distal to the tuberosity. It should
encompass the anterior hemi-circumference of the leg. The length of the posterior flap should be 2.5 cm longer than the
antero-posterior diameter of the leg at anterior incision line.
85
S. Sajja
86
Figure 4 To create the posterior flap, the author recommends the use of a long very sharp amputation knife. With the
tibia distracted anteriorly with a bone hook, and the entire specimen on gentle caudal traction, the knife is inserted just
along the posterior edge of the fibula. With swift slicing motions, the path of the knife should follow a gentle downward
curve away from the fibula and toward the posterior incision. The result will be a beveled posterior myofascial flap, with
more muscle thickness proximally and less thickness distally.
Below knee amputation
Figure 5 The incision for skin flaps method is semicircular and is based on a line around the limb at right angles to the
long axis. The circumference of the leg is measured at the chosen level of tibial division and skin flaps are one fourth
this in length. The anterior starting point of the incision is 2 cm lateral to the anterior border of the tibia, over the middle
of the anterior compartment. The posterior point is half way around the circumference. The incision is extended for
about 2 cm anteriorly to facilitate beveling of the tibia.
87
S. Sajja
88
Figure 6 The length of the gastrocnemeus and soleus muscle flap should be at least equal to the diameter of the leg. The
muscle bulk is thinned and some of the muscle from the medial and lateral aspects may need to be removed.
Below knee amputation
89
Figure 7 The muscle flap along with the
attached deep fascia is brought anteriorly and sutured to the deep fascia and
periosteum. A suction drain is placed beneath the muscle layer. The skin flaps
enclose the posterior muscle flap and are
closed with interrupted nonabsorbable
sutures.
Conclusions
References
Below knee amputation is the most frequently performed
major extremity amputation. If loss of the foot is inevitable,
every attempt should be made to preserve the knee joint so
that patients may be afforded the best opportunity to ambulate with prosthesis. In dysvascular extremities, the posterior
myoplasty technique has long been established as a safe and
reliable procedure with excellent functional results. Rigid
stump dressings offer considerable advantages over traditional soft dressings. An aggressive rehabilitation program
should be started early in the postoperative period with the
help of well-trained physical therapists and orthotists to
achieve functional independence.
1. Smith DG: Amputation. Preoperative assessment and lower extremity
surgical techniques. Foot Ankle Clin 6:2, 271-296, 2001
2. Carnesale PG: Amputations of the lower extremity, in Canale ST (ed):
Cambells operative orthopaedics (10th ed). Philadelphia, PA, Mosby,
2003, pp 575-586
3. Burgess EM, Romano, RL et al: Amputations of the leg for peripheral
vascular insufficiency. J Bone Joint Surg Am 53:5, 874-890, 1971
4. Robinson KP, Hoile R, Coddington T: Skew flap myoplastic below-knee
amputation: a preliminary report. Br J Surg 69:9, 554-557, 1982
5. Ruckley CV, Stonebridge PA, Prescott RJ: Skewflap versus long posterior flap in
below-knee amputations: multicenter trial. J Vasc Surg 13:3, 423-427, 1991
6. Tisi PV, Callam MJ: Type of incision for below knee amputation. Cochrane Database Syst Rev 1:CD003749 Review, 2004
Knee Disarticulation and Above-Knee Amputation
Karla M. Anderson, MD
he previous two chapters have described a series of surgical procedures that illustrate priorities in the management of limb-threatening injury and disease. Failing prevention or successful nonoperative management, the surgeon
selects a level of amputation that minimizes tissue loss, enables healing, and preserves as much function as possible.
Walking will almost always still be possible if only the forefoot is lost. The functionality of mid- and hind-foot amputations is highly variable, but may suffice for younger healthier
patients. If no part of the foot can be salvaged, the surgeon
will then typically be faced with a decision that has major
consequences for the patient: whether to attempt salvage of
the knee joint.
As previously emphasized, loss of the knee joint markedly
reduces the chance of community ambulation in all but the
heartiest and most motivated patients. Yet all amputation
surgeons are familiar with the circumstances that render the
leg and knee unsalvageable: severe ischemia, infection, joint
contractures, crush injuries, or other extensive trauma. The
current chapter will address techniques that again give priority to healing and function, even when the knee joint cannot be preserved.
Anatomy of the Knee and Thigh
Knee
The knee joint is the articulation between the femur and the
tibia, more specifically, between the condyles of the femur
and tibia. The knee is a hinge joint, stabilized by the anterior
and posterior cruciate ligaments, the tibial and fibular collateral ligaments, the quadriceps and patellar tendons, the iliotibial tract, and the attachments of the biceps, gastrocnemius, and adductor muscles. The articular surfaces are
cushioned by the medial and lateral mensici, also known as
the semilunar cartilages.
Aside from these musculoskeletal structures, the anatomy
of the knee is notable for the popliteal artery and vein, which
pass in the midline, directly posterior to the intercondylar
notch, along with the tibial nerve. The common peroneal
nerve branches from the sciatic nerve proximal to the knee
Penn State Hershey Medical Center, College of Medicine of the Pennsylvania
State University, 500 University Drive, Hershey, PA.
Address reprint requests to Dr. Karla M. Anderson, Assistant Professor of Surgery
and Radiology, Division of Vascular Surgery, Penn State Hershey Medical Center, College of Medicine of the Pennsylvania State University, 500 University
Drive, Hershey, PA 17033-2390. E-mail: kmanderson@psu.edu
90
1524-153X/05/$-see front matter 2005 Elsevier Inc. All rights reserved.
doi:10.1053/j.optechgensurg.2005.07.005
joint, and courses more laterally behind the knee. The popliteal space consists of the vessels and connective tissue surrounding them, both above and below the knee.
Thigh
Extending from the inguinal crease to the knee, the thigh is
comprised of the femur, vessels and nerves, connective tissue, and three groups of muscles. The anterior group includes the quadriceps femoris and sartorius; the medial
group contains the adductor longus and magnus and the
gracilis; the posterior group is the biceps femoris, semitendinosus, and semimembranosus.
Differences in anatomy at different levels are important for
the surgeon to understand, particularly as regards the vascular anatomy. The common femoral artery and vein are essentially subcutaneous, but both the profunda femoris and (superficial) femoral arteries quickly pass deep to fascia and
muscle as they course distally from the femoral triangle. The
profunda passes medial to but toward the femur, while the
femoral artery parallels the femur until the vessel emerges
from the adductor canal as the popliteal artery and passes
posteriorly into the proximal popliteal space.
The femoral nerve passes deep to the inguinal ligament
and immediately divides into a series of both muscular and
cutaneous sensory branches. The saphenous nerve accompanies the femoral artery through the adductor canal, and then
surfaces to accompany the greater saphenous vein, from behind the sartorius tendon. The sciatic nerve, the largest and
longest peripheral nerve in the body, enters the thigh
through the sciatic notch and courses deep to the biceps
femoris muscle until the nerve divides into the tibial and
common peroneal branches proximal to the knee joint.
Knee Disarticulation
General Considerations
Like the Syme amputation, the knee disarticulation has never
been widely accepted by most amputation surgeons, but retains a loyal following among a minority of surgeons and
prosthetists. Its advantages are numerous. It preserves not
only the length of the limb, but also the function of the thigh
muscles, providing a long and strong lever arm for ambulation. No muscles are cut in performing a knee disarticulation, and the tendons and ligaments around the knee can be
readily reattached to the femur. Because the function of all
thigh muscles is preserved, there is much less likelihood of
Knee disarticulation and above-knee amputation
91
Figure 1 Representative incisions for a knee-disarticulation and for above-knee amputation. Knee-disarticulation
(dashed line below knee): A fish mouth configuration is used, but the anterior flap is typically longer to include the
patella and patellar ligament. The corners are placed at the level of the knee joint, and the anterior flap should extend
about 4 inches distal to the level. The posterior flap is then incised about two or two-and-one-half inches distal to the
knee joint, as depicted. The underlying soft tissues are divided with a gentle bevel corresponding to the flaps themselves. The patellar ligament is divided from its insertion onto the tibial tuberosity. Above-knee amputation (dashed
line above knee): The fish-mouth technique uses equal anterior and posterior flaps, but the length and symmetry of the
flaps can be modified according to the presence of prior incisions, ulcers, or areas of necrosis. The medial and lateral
corners should be at the desired level of bony amputation, and the length of the flaps should be about 3 inches.
contracture of the thigh, compared with AKA. Moreover, the
end of the femur is a more suitable weight bearing surface
than the ischium (for AKA).
Disadvantages of knee disarticulation cannot be ignored,
and account for its lack of popularity. Coverage of the bony
stump requires use of the soft tissues of the upper calf, which
in some cases may be of dubious quality. The stump is somewhat bulky, requiring special considerations in prosthetic
fitting. The prosthetic knee joint is located lower than the
contralateral natural joint, a concern which may or may not
be problematic with walking.
In general, knee disarticulation can be considered in
younger patients, especially children, in whom it preserves
the growth plate of the femur. For young adults, opinions
differ as to whether there is any significant advantage of knee
disarticulation versus distal AKA. Amputation through the
knee should generally be avoided in older patients with vascular disease, who, if they are not suitable for a high BKA, are
not likely to have adequate tissues to heal a knee disarticulation. In selected nonambulatory patients, this type of amputation should be considered to avoid the development of
either knee or hip joint contractures.
Technique
Knee disarticulation is performed with the patient supine,
and with the thigh elevated on a soft roll. A pneumatic tourniquet is preferred by some surgeons, but not mandatory.
Incisions are made and flaps developed by one of several
methods. The classic approach is based on a longer anterior
flap, but the procedure can also be performed with a long
posterior flap, or with equal fishmouth flaps, the latter oriented in either the sagittal or coronal planes. If fishmouth
flaps are used, each should have a length about 2/3 that of the
leg circumference at the site of incision.
Classic Approach
A symmetric anterior curvilinear incision is made from the
level of the joint line, extending to the distal aspect of the
tibial tuberosity (Fig. 1). The incision is taken perpindicular
through the soft tissues down to bone, incising the fascia at
the same length as the skin, which will ensure adequate coverage of the femoral condyles and add durability to the
stump. Periosteum is taken with the flap, which is developed
superiorly, detaching the pes anserinus and patellar ligament
from the tuberosity. The capsule of the knee joint is then
incised anteriorly, medially, and laterally along the margins
of the tibia, exposing the joint itself. Flexion of the knee to
90 aids in exposure of the cruciate ligaments which are then
divided at their tibial insertion site. The posterior capsule is
then located and divided at the tibial attachments (Fig. 2).
At the completion of this sequence of steps, the surgeon
will now be able to visualize the neurovascular bundle within
the popliteal fossa. The veins and artery should be individually exposed, clamped, divided, and doubly ligated (nonabsorbable suture). The tibial nerve should be placed on moderate tension, ligated proximally, then sharply divided and
allowed to retract into the depths of the stump. The neurovascular structures are in some few cases densely adherent to
the posterior capsule and cannot be readily mobilized until
they have been transected. A pneumatic tourniquet is partic-
92
K.M. Anderson
ligament is placed on tension and sutured to the stump of the
cruciate ligaments at the intracondylar notch, thus stabilizing
the quadriceps mechanism and ensuring good muscle function postoperatively (Fig. 3). The remaining biceps tendon
and hamstring tendons are also secured to the cruciate stump
in a similar fashion. Any excess tendon and ligament may be
debrided.
The flaps can now be assessed for length, and carefully
trimmed of redundant or devitalized soft tissues. Once the
flaps are deemed satisfactory, the anterior and posterior fascia
are then closed with interrupted absorbable suture, over a
drain if necessary (see introductory chapter), which is best
brought out through a separate stab wound (Fig. 4). The skin
edges must come together without tension. The surgeons
choice of dressing is then applied.
If appropriate preoperative evaluation has been performed, the flaps will be adequately perfused, with no areas
of infection or necrosis. Should there be major concern during the procedure about the viability or length of the flaps, a
decision will be required to either modify the amputation as
described in the next section, or convert to above-knee amputation. A compression dressing is applied.
Modified Knee Disarticulation
Several modifications of the classical knee disarticulation
have been developed, primarily to equalize the level of the
prosthetic knee to that of the contralateral knee joint. Secondary advantages include a reduction in the bulk of the
Figure 2 A later stage in the knee disarticulation procedure. The flaps
have been developed and the knee joint opened from the front. The
cruciate ligaments, collateral ligaments, and menisci have been
transected. The origins of the gastrocnemius muscles, and the popliteal neurovascular bundle can now be visualized. Stepwise control
and transection of these structures is accomplished. The vessels
should be securely suture ligated. The tibial nerve should be ligated
and divided well behind the femur. Finally, the posterior skin and
fascia are divided to complete the amputation.
ularly useful in such circumstances to avert unexpected
problems with vascular control. The next step is to identify
the biceps tendon as it inserts onto the fibula, and transect it
at that level. The surgeon can then visualize the common
peroneal nerve, which is distracted, ligated and divided in
similar fashion to the tibial nerve.
The amputation is then completed by developing the posterior flap, which in the classic approach has a length about
1/3 less than the anterior flap. The skin incision is again
curvilinear, based at the joint line on each side, and carried
down perpendicular through the fascia. The gastrocnemius
muscle must be bluntly separated from the underlying soleus, and is then divided far enough (several centimeters)
beyond its origin to preserve the superior geniculate arteries.
With this step the specimen is free to be removed from the
field.
If a tourniquet is in use, it can now be deflated. The open
stump should be inspected, and hemostasis obtained. Any
sharp margins of the femoral condyles are smoothed with
ronguer, rasp, file or burr. The femoral articular cartilage may
be left undisturbed.
The patella is left intact within its tendon. The patellar
Figure 3 Closing the completed knee disarticulation. The patellar
tendon is brought down into the intercondylar fossa and sutured to
the stump of the anterior cruciate ligament. The condyles are left
intact in this illustration, but some authors recommend removing
the convex surfaces of the condyles along with the articular cartilage
(see text). Likewise, the patella is typically left intact within its
tendon, but the technique can be modified to excise the patella,
depending on the surgeons preference and the circumstances of the
individual case. The soft tissue flaps consist of relatively thin fascia,
subcutaneous tissue, and skin, and must be carefully closed without
tension.
Knee disarticulation and above-knee amputation
Figure 4 A schematic of the completed and closed knee disarticulation, illustrating the relationship of underlying bony and musculotendinous structures. In this illustration, sutures are visible where
the patella has been (optionally) removed from within its tendon.
stump, and modifications of the flaps that are less problematic for the dysvascular limb. The primary disadvantage of the
modified procedures is a moderate increase in technical difficulty. Similar to the classic approach, each of the modified
techniques can be performed with sagittal or coronal flaps of
variable length.
The four common eponymous modifications are as follows:
1. Gritti-Stokes: removes condyles of femur leaving a beveled anterior femoral edge to which the patella is then
anchored.
2. Burgess: removes patella and portion of condyles.1
3. Youkey: removes patella and completely removes the
condyles.2
4. Nellis/Van De Water: removes the femoral condyles
without bevel, and anchors the patella over the distal
end of the femoral stump.3
Technique
The initial stages of these modified procedures are identical
to the classic technique described above. Most authors
strongly recommend use of the pneumatic tourniquet. All
fascia and tendinous attachments to the tibia and fibula are
divided as distally as possible. Disarticulation of the joint
proceeds through the various ligaments. The neurovascular
structures are divided individually and ligated securely.
The popliteal artery should be ligated distal to the origin of
the superior geniculate branches. Because the posterior tissues have a tendency to retract, the posterior flap should be
cut generously long to include portions of both heads of the
gastrocnemius muscle.
If the patella is to be removed, the resection is done subperiosteally; the resulting defect in the patellar tendon must
be carefully closed with interrupted suture. The different
modifications call for variable lengths of the femoral condyles
to be resected perpendicular to the long axis of the femur,
either with or without beveling. The edges of femur and
93
condyles are smoothed with an instrument of choice. Any
remaining cartilage and the synovium may be left in place.
The patellar ligament (with the patella excised) is placed
on tension, brought down around the femoral stump, and
secured to the stump of the cruciates at the level of the intracondylar notch (nonabsorbable suture). The remaining tendinous ends (biceps and hamstrings) are also brought out
around the bony stump and secured to the sides of the patellar ligament/ tendon or the cruciates. Any excess tissue is
debrided. The remainder of the closure includes interrupted
fascial sutures and skin closure. Temporary (48 hrs) suction drainage is optional, but should be actively considered
with modified knee disarticulation to eliminate dead space
and enhance tissue coaptation.
Although the procedures described in the preceding paragraphs are known as modifications of knee disarticulation,
they could just as accurately be considered as modifications
of trans-femoral (above-knee) amputation with a very long
femoral stump. Except for the specific indications noted
above, mainstream opinion holds that standard AKA is
equivalent or superior to through-the-knee amputation for
patients whose knee joints cannot be preserved.
Above-Knee Amputation
General Considerations
The trans-femoral or above-knee amputation (AKA) is indicated for patients with severe disease, injury, or ischemia of
the leg and foot. Patients selected for AKA are generally those
with some combination of necrosis, infection, injury, neoplasm, or ischemia involving the calf or distal thigh, such that
the musculoskeletal structures of the leg are not usable for
below-knee amputation. A second category of patients includes those who have the potential to heal at the BKA level,
but are nonambulatory and debilitated, with a high risk for
developing flexion contracture of the knee after BKA. In this
latter group of patients the major advantage of preserving
limb length relates to balance and stability in the sitting position, as well as ability to transfer from bed to chair. A well
healed BKA with normal range of motion at the knee joint is
highly advantageous for both balance and transfers, but a
contracted knee joint is a major liability. The possible role
and value of knee disarticulation for such patients has already
been reviewed in the previous section.
It is most commonly the patient with the ischemic limb
that presents the difficult decision whether to spare or sacrifice the knee joint. The surgeon must consider a variety of
factors involving the condition of both the limb and the patient (see the Introduction at the beginning of the Journal).
The many factors must be weighed against each other, and
most are relative rather than absolute. Nonetheless, two specific considerations argue very strongly against an attempt to
save the knee: first, a nonambulatory patient, and second, the
presence of significant nonreconstructible arterial occlusive
disease proximal to the femoral artery (as evidenced by absent ipsilateral femoral pulse). In equivocal or borderline
situations, the patient should be counseled that attempted
salvage of the knee may mean longer hospitalization, slower
healing, a more protracted course, and a significant risk of
re-amputation at the AK level.
K.M. Anderson
94
Figure 5 The open stump prior to fascial closure. The anterior and posterior musculature has been transected in slightly
beveled fashion to match the flaps themselves. Vessels and nerves have been ligated at or proximal to the level of the
femoral stump. The anterior edge of the femur should be smoothed with a rasp or burr to avoid erosion of the overlying
skin. It is imperative to amputate the femur short enough to avoid any tension on the flaps. Standard and accepted
closure is by re-approximation of anterior and posterior fascia using interrupted sutures. The surgeon has the choice to
also perform a myodesis by re-approximating the rectus femoris and biceps over the stump of the femur, prior to closing
the superficial fascia.
Once the decision has been made to perform AKA, the
surgeon then faces a second and sometimes equally difficult
choice: the level of the AKA. Preservation of femoral length
clearly yields better function, but only if the amputation
heals. Differences in functionality of long versus short AKA
are not so dramatic as the difference between BKA and AKA,
but neither can the differences be dismissed. A generally
useful guideline is that the greater the prospect for ambulation, the greater the length of femur that should ideally be
retained.
Technique
The skin incision for AKA is virtually always a fishmouth
configuration with equal anterior and posterior flaps (Fig. 1).
Circular incisions can be used, but are more difficult to close.
Medial and lateral flaps could theoretically be utilized, but
are essentially nonanatomic. The length of the flaps should be
sufficient to provide secure tension-free closure over the femoral stump, without redundant soft tissue or excessive dead
space in the depths of the wound. If myodesis/myoplasty is
planned (fixation of muscle to the femoral stump), the muscle flaps should be fashioned longer.
The incision is made as marked on the skin and carried
sharply through the fascia at the same level. The muscle is
divided at the same level as the skin incision and allowed to
retract. Use of electrocautery for transection of the anterior
musculature will aid with hemostasis, and the electrocautery
is especially useful in distal AKA for division of the patellar
tendon.
The level of amputation will dictate the location of nerves
and vessels. At the more distal levels, the popliteal artery is
located posteromedial to the femur and should be directly
visualized. The artery and accompanying popliteal vein(s)
should be individually isolated and suture ligated, before di-
viding the femur or the posterior flap. In the mid- to proximal
thigh, the (superficial) femoral artery lies deep to the sartorius within the adductor canal, more medial and less posterior than the popliteal artery. Branches of the profunda femoris will also be encountered in proximity to the femur.
After division of the anterior muscles, the periosteum of
the femur is scored circumferentially, and elevated as high as
desired. In the mid- to distal thigh, clearing the femur will
require division of the adductor insertions along the linea
aspera on the posteromedial surface of the bone. The femur
should be divided at least 3 to 5 cm proximal to the line of
skin incision, more if possible, so that the flaps will coapt
easily and cover the femoral stump generously. The correct
tool for cutting the femur is a matter of individual preference,
but power saws are clearly more efficient and probably less
traumatic.
A bone hook placed in the distal femur will now allow
exposure of the posterior muscle groups and facilitate their
division with an amputation knife. The sciatic nerve is identified between the adductor magnus and hamstrings as a large
and often rather vascular structure. It should be placed on
moderate tension, firmly and securely ligated proximally,
sharply divided, and allowed to retract into the proximal
muscle bed. Hemostasis is then obtained by electrocautery
and ligation, taking care to preserve the fascial-cutaneous
flaps both medially and laterally. If myodesis alone is planned
the posterior muscle flaps are left 2 inches longer than the
level of bony transection. If both myodesis and myoplasty are
planned all muscle groups are left long (Fig. 5).
In performing myodesis, a series of small (ex. 7/64 inch)
drill holes are placed in the cortex of the femur about 3/8 inch
from the cut end. Loop mattress sutures of strong braided
polyester suture are placed through the major muscle groups
and drawn thru the drill holes. The knots will be in the
Knee disarticulation and above-knee amputation
medullary cavity of the femur. Only gentle tension is placed
on the suture to avoid necrosis as well as to allow continued
full extension of the hip. If feasible, a long quadriceps flap
with its fascia can be sutured to the posterior fascia and major
muscle groups. This myoplasty technique helps further centralize the femur, a goal that can also be accomplished by
myodesis of the adductor muscle group to the femur. Note
that myodesis and myoplasty are typically not employed in
amputations performed for ischemia.
After hemostasis and irrigation, the length and condition
of the flaps is now evaluated. It is not uncommon to find that
more of the femur needs to be removed to allow for optimal
closure. Once these issues have been addressed, the superficial fascia is closed with interrupted suture (over a drain if
desired), and the skin re-approximated without tension.
Dressings can be most difficult at this level, particularly for
high AKA. An elastic bandage placed in the hip spica configuration is ideal, but usually impractical to apply. A useful
alternative is a bulky gauze dressing held in place with a large
95
self-adhesive drape (such as the Ioban) covering the entire
stump.
References
1. Burgess EM, Malone JM: Major amputations, in Nora PF (ed): Operative
surgery: principles and techniques (3rd ed). Philadelphia, PA, WB Saunders, 1990, Chapter 52, pp 1242-1265
2. Cull D, Youkey JR: A reappraisal of a modified through-knee amputation
in patients with peripheral vascular disease. Am J Surg 182:44-48, 2001
3. Nellis N, Van De Water JM: Through-the-knee amputation: an improved
technique. The American Surgeon 68:466-469, 2002
Suggested Reading
Burgess EM: Disarticulation of the knee. Arch Surg 112:1250-1255, 1977
Malone JM: Lower extremity amputation, in Moore WS (ed): Vascular surgery: A comprehensive review (5th ed). Philadelphia, PA, WB Saunders,
1998, pp 844-884
Persson B: Lower limb amputation: amputation methods. Prosthet Orthot
Int 25:7-13, 2001
Smith DG: Amputation: preoperative assessment and lower extremity surgical techniques. Foot Ankle Clinics 6:271-296, 2001
Hip Disarticulation and Hemi-Pelvectomy
William Parrish, MD
mputations through the hip joint or pelvis are most often
indicated for radical treatment of neoplasia when a primary malignant soft tissue or osseous tumor of the extremity
involves several compartments, the sciatic nerve, or the femoral neurovascular structures. The goal of these procedures
when performed for neoplastic indications is to provide local
disease control. If a primary malignant bone tumor involves
the hip joint or a large portion of the ilium, a hemi-pelvectomy may be indicated. If the tumor involves only a limited
portion of the pelvis but no neurovascular structures, an
internal hemi-pelvectomy may be possible to preserve the
extremity. Amputations through the hip joint or pelvis result
in very similar functional results.
Less often, such amputations may be required in the
setting of vascular catastrophe, such as prosthetic graft
infection or nonhealing of above-knee amputation. Other
indications may include severe trauma with extensive
bone or soft tissue loss and neurovascular injury, or aggressive infectious diseases such as necrotizing fasciitis or
gas gangrene.
Surgical planning for hip disarticulation or hemi-pelvectomy should be based on imaging studies which clearly define the vascular status of the extremity, the anatomic margins of a tumor, or the extent of tissue loss or necrosis from
trauma or an infection. CT scan will provide the best images
to define osseous structures. MRI is most useful for defining
soft tissue extension of a tumor, relationship of a tumor to
neurovascular structures, and extent of marrow involvement.
MRI is also helpful in defining the limits of cellulitis or muscle
necrosis that may occur with aggressive infections. Appropriate vascular studies such a doppler ultrasound, digital subtraction angiography, or venography may be useful when
evaluating the patient with vascular disease.
Hip Disarticulation:
Surgical Technique
Position
As with all surgical procedures, the operating surgeon must
take primary and personal responsibility for correct identifi-
cation of the patient and operative site/side. Before positioning, a regional anesthetic should be introduced and induction of the general anesthetic completed. Epidural anesthetics
with an indwelling catheter provide an excellent means of
postoperative pain control. In addition, a regional anesthetic
can be highly beneficial by reducing the incidence of phantom pain postoperatively.
A Foley catheter is placed while the patient is in the
supine position. The patient is then moved into a lateral
decubitus position and stabilized with the aid of a bean
bag or other similar apparatus (Fig. 1). The operative
(ipsilateral) side will be facing up. An axillary roll is then
placed beneath the chest wall in the contralateral axilla to
avoid pressure on the brachial plexus and neurovascular
structures. The contralateral arm must be carefully and
naturally positioned on an arm board without unusual
angulation of any joint or pressure against the radial and
ulnar nerves. The ipsilateral arm is often best positioned in
an overhead cradle with generous padding. Foam pads or
blankets should also be used to protect the peroneal nerve
of the contralateral leg and ankle.
It is important to perform the skin preparation and draping as widely as possible so that the surgical field is not
compromised. Failure to prep and drape a wide field may
cause great difficulty in placing correct incisions, and increases the risk of contamination of the surgical field. Patient
positioning, skin preparation, and placement of drapes
should be done under the direct supervision of the operating
surgeon or a very trusted associate.
After antiseptic skin preparation, a U-shaped drape is
placed under the operative leg as close to the midline gluteal
cleft as possible (while excluding the anus). The anterior arm
of the drape is brought along the base of the scrotum, extending to the umbilicus and ending at the level of the sternum.
The posterior arm of the U-drape extends along the midline
of the spine to the lower margin of the twelth rib. A second
rectangular drape is then used to complete the surgical field
connecting the two ends of the U-drape along the lower
margin of the rib cage.
Incision
Department of Orthopedics and Rehabilitation, Penn State Hershey Medical
Center, College of Medicine of the Pennsylvania State University, 500
University Drive, Hershey, PA.
Address reprint requests to Dr. William Parrish, Department of Orthopedics
and Rehabilitation, Penn State Hershey Medical Center, College of Medicine of the Pennsylvania State University, 500 University Drive, Hershey, PA 17033. E-mail: wparrish@psu.edu
96
1524-153X/05/$-see front matter 2005 Elsevier Inc. All rights reserved.
doi:10.1053/j.optechgensurg.2005.08.001
See Figs. 1 and 2.
Dissection
The anterior limb of the incision is developed by exposing
the femoral triangle. The femoral triangle is found in the
Hip disarticulation and hemi-pelvectomy
97
Figure 1 Posterior view of patient positioning and placement of incisions for hip disarticulation and hemi-pelvectomy.
The incision for hip disarticulation (dotted line) begins approximately one fingerbreadth inferior and medial to the
anterior superior iliac spine (ASIS) and proceeds caudally toward the greater trochanter. From there, the incision
courses posteriorly within the gluteal crease and then curves anteriorly within the medial thigh crease to reach the pubic
tubercle. Shown in Fig 2 is the anterior component of the incision, extending from the pubic tubercle to the ASIS. For
hemi-pelvectomy (solid line), the incision passes posteriorly from the ASIS along the iliac crest toward the posterior
superior iliac spine (PSIS). At this point, the incision is directed postero-laterally to the tip of the greater trochanter, and
then posteriorly along the gluteal crease to the ischium. The incision then courses within the thigh crease anteriorly
toward the inferior pubic ramus, continuing on to the pubic symphysis. Figure 2 shows the anterior incision extending
from the pubic symphysis, along the inguinal ligament, to the ASIS.
subfascial space of the proximal thigh. The femoral artery,
vein, and nerve pass through this anatomic area as they
exit the pelvis beneath the inguinal ligament and descend
into the leg. The position of the neurovascular structures
in the femoral canal are nerve, artery, vein, and lymphatics
in a lateral to medial progression (NAVL). The femoral
triangle is bounded by the adductor longus muscle medially, the sartorius muscle laterally, and the inguinal ligament superiorly. The iliopsoas and pectineus muscles
form the floor of the femoral triangle (Fig. 2).
The most reliable landmark for identification of the femoral vessels is the inguinal ligament, specifically the inferior
shelving edge, sometimes referred to as Pouparts ligament.
Particularly in patients with previous arterial surgery in the
groin, the inguinal ligament can be the only constant structure. Division of the sartorius muscle at its origin will further
aid in exposing the femoral neurovascular structures in the
femoral triangle. Once exposed, the femoral artery and vein
must be encircled, controlled, and individually suture ligated
with nonabsorbable monofilament suture of 3-0 or larger
size. The femoral nerve is then gently placed under tension,
ligated as it exits beneath the inguinal ligament, divided, and
allowed to retract into the pelvis.
The greater saphenous vein enters the femoral vein very
proximally and may need to be separately ligated. In addition, the obturator, pudendal, and superficial epigastric vessels may require separate ligation. The lateral femoral cutaneous nerve should be identified as it exits the pelvis just
beneath the anterior superior iliac spine. This should be
placed under gentle traction, ligated, and allowed to retract
into the pelvis. The round ligament in a woman or spermatic
cord in a male may be encountered during dissection of the
midline part of the incision. These should be exposed but not
resected with the specimen.
Once these neurovascular structures have been identified and divided, the dissection continues through the soft
tissues toward the hip joint. Proceeding anterior to posteriorly, the iliopsoas muscle is released from its insertion
onto the lesser trochanter of the femur. Circumflex
branches of the femoral vessels may be encountered during the dissection. The pectineus and adductor muscles
are transected at their origins on the bony pelvis. Care
must be taken to ligate the obturator vessels during this
part of the dissection.
As the dissection is carried posteriorly, all the muscles
originating on the ischium are released at their origin. This
will include the gracilis and the hamstring muscles. This part
of the dissection is most easily completed with the leg in a
flexed, abducted, and externally rotated position. The posterior limb of the incision is then developed by dividing the
gluteus maximus muscle and releasing the gluteus medius
and minimus muscles from their insertions on the greater
trochanter. This will provide exposure of the deep posterior
thigh including the sciatic nerve and the short external rotators of the hip. The sciatic nerve should be placed under
gentle traction, securely ligated, divided, and allowed to retract proximally beneath the piriformis muscle. The remaining external rotator muscles are then released from their femoral insertion.
Attention is then redirected to the anterior limb of the
incision. The dissection from the greater trochanter to the
ASIS is completed by dividing the tensor fascia lata and re-
W. Parrish
98
Figure 2 Anterior view of the incisions and deep dissection for hip disarticulation and hemi-pelvectomy. Depicted on
the patients right side are the incisions for the two procedures. Both begin at the anterior superior iliac spine (ASIS) and
course along the inguinal ligament. For hip disarticulation, the incision turns posteriorly at the pubic tubercle; for
hemi-pelvectomy, it extends to the pubic symphysis before curving posterior along the lateral border of the perineum
and into the medial thigh crease. Posteriorly, both incisions pass within the gluteal crease toward the greater trochanter.
The hip disarticulation incision then turns superiorly to course directly back to the ASIS. The hemi-pelvectomy incision
travels from the greater trochanter superiorly, posteriorly, and medially toward the posterior superior iliac spine (PSIS).
The posterior component follows the iliac crest back to the ASIS. These relationships are also shown in Fig 1. The left
side of the patient shows the deep dissection for both hip disarticulation and hemi-pelvectomy, as explained in detail
in the chapter text.
leasing the rectus femoris muscle from its origin on the anterior inferior iliac spine. The hip capsule is the incised around
the lip of the acetabulum, and the hip joint dislocated. The
ligamentum teres is divided by electrocautery, completing
the amputation, and allowing removal of the limb from the
surgical field.
Closure
The surgical field is then thoroughly irrigated and inspected for hemostasis. The short external rotator muscles
and gluteus medius muscles are then approximated with
the obturator externus and iliopsoas muscles to cover the
acetabulum. One or two large drains are then placed in the
surgical bed and the gluteus maximus flap is mobilized
anteriorly with suturing of the gluteus fascia to the inguinal ligament (Fig. 3). Deep dermal sutures are placed and
the skin is closed with interrupted sutures or staples. A
sterile dressing is placed on the wound and may be secured with a long six inch elastic wrap that is secured
around the waist.
Hip disarticulation and hemi-pelvectomy
99
Figure 3 Hip disarticulation before closure with the gluteal flap. The transected and ligated vessels are seen deep in the
wound. Acetabular coverage is obtained by approximating the short external rotator muscles and gluteus medius muscles
with the obturator externus and iliopsoas muscles. One or two large drains can be placed in the surgical bed if desired. The
gluteus maximus flap is then mobilized anteriorly with suturing of the gluteus fascia to the inguinal ligament.
Postoperative Care
The drains should be left in place until output is minimal.
Removal of the drains too quickly will result in the development of a seroma in the large space deep to the gluteal
fascia. The epidural catheter should be left in place for 48
to 72 hours for pain control. Sustained release oral narcotic pain medications should be started while the epi-
dural is in place and should be titrated to the patients pain
requirements as the epidural is weaned. Once the incision
line is completely healed, the patient is referred to prosthetics to initiate fabrication of prosthesis. A preoperative
visit with a prosthetist can be most helpful for the patient
to understand the concept and process of prosthetic fitting.
W. Parrish
100
Hemi-Pelvectomy:
Surgical Technique
Position
Positioning the patient for a hemi-pelvectomy is in many
ways similar to positioning for a hip disarticulation (Fig. 1).
Preoperative preparation for this procedure should include a
mechanical bowel prep on the night before surgery. A betadine-soaked vaginal sponge may be packed into the rectum
to prevent contamination of the surgical field due to manipulation of the retroperitoneum during the surgical procedure. A stent should be placed in the ipsilateral ureter and a
Foley catheter in the urinary bladder while the patient is in
the supine position. This makes it easier to identify the ureter
during surgery and decreases the risk of injury to it.
The patient is moved into a relaxed lateral decubitus position
with placement of an axillary roll and appropriate padding of
pressure points. For a hemi-pelvectomy, the patient is positioned on the OR table so the flexion break in the table is
centered between the lower ribs and the iliac crest. The bed
is then flexed which opens the space between the ribs and
iliac crest, making the exposure of the retroperitoneum easier. The patient is placed into a relaxed lateral position so that
the trunk and pelvis can be moved forward or backward to
facilitate surgical exposure. The arms are positioned and padded as described for hip disarticulation. Skin preparation and
draping is performed in similar fashion. Although these steps
should not be delegated to subordinates, the principles of
positioning and preparation should be familiar to the entire
OR team.
Incision
Posterior flap hemi-pelvectomy is the most common variant
of this procedure. This method utilizes the gluteus maximus
for closure much as was described for a hip disarticulation.
Occasionally, a tumor may involve the posterior aspect of the
pelvis or gluteus maximus, necessitating the use of an anterior flap hemi-pelvectomy. The anterior flap hemi-pelvectomy utilizes an anterior based myocutaneous flap that is
based on the femoral vessels. The incision used will depend
on the type of flap required. This chapter will describe the
posterior flap hemi-pelvectomy. The incisions are outlined
and described in Figs. 1 and 2.
Dissection
The dissection begins at the posterior superior iliac spine and
extends anteriorly along the iliac crest and the inguinal ligament to the pubic symphysis. The retroperitoneal space is
exposed by releasing the insertion of the abdominal muscles
on the iliac crest and inguinal ligament. The peritoneal sac
and contents are retracted medially with the ureter. The common iliac artery and vein are identified as well as the internal
and external iliac vessels. The level of ligation of these vessels
may be determined by the position of the tumor. For a posterior flap hemi-pelvectomy, preservation of the internal iliac
vessel or at least the first branch (the superior gluteal artery)
will result in better flap viability because the superior gluteal
artery supplies the gluteus maximus. Once the level of ligation is determined, the appropriate vessels are suture ligated
with monofilament nonabsorbable suture no smaller than
4-0. Surgeons not familiar with handling of large vessels
should obtain assistance from a vascular surgeon, especially if
the vessels are heavily calcified or aneurysmal. The iliopsoas
muscle is divided near the inguinal ligament. In most cases,
the iliacus will be included in the surgical specimen and the
majority of the psoas muscle preserved. The femoral nerve is
finally identified, ligated, and divided (Fig. 2).
The perineal dissection is then performed. The bladder is
retracted along with the urethra and protected with a broad
malleable retractor. The ischiorectal space is the exposed as
the dissection is extended along the inferior pubic ramus and
the ischium by releasing the muscles of the pelvic floor as
they insert on the boney pelvis. The bladder, urethra, and
spermatic cord should be protected during this part of the
dissection. An osteotome is then used to divide the pubic
symphysis.
The posterior segment of the dissection is then completed
by extending the incision from the PSIS to the greater trochanter, then along the inferior border of the gluteus maximus, connecting to the perineal incision and region of dissection. If possible, the gluteus maximus muscle is preserved
with the posterior flap; however, it may be necessary with
some tumors to sacrifice the gluteus maximus to achieve an
acceptable surgical margin. This myocutaneous or fasciocutaneous flap is then developed in an anterior to posterior
direction.
As the flap is developed posteriorly, the superior gluteal
artery should be preserved in those cases using a myocutaneous gluteus flap. The superior gluteal artery will exit the
pelvis through the greater sciatic notch and is tightly adherent to the bone in this location. Once the posterior flap is
developed, the deep posterior hip musculature and sciatic
nerve will be visible. The piriformis muscle is divided to
reveal the sciatic nerve as it exits the pelvis. The very large
nerve must be firmly ligated, divided, and allowed to retract
into the pelvis. The inferior gluteal artery will exit the pelvis
inferior to the piriformis muscle. This artery should be identified and ligated to avoid bleeding. The thick broad sacrotuberous ligament will then be encountered extending from
the lateral border of the sacrum to the ischial tuberosity, and
must be divided.
Once division of the soft tissues and neurovascular structures are completed, attention is then directed to final step:
sacral osteotomy. The standard hemi-pelvectomy is completed by passing a series of osteotomes through the sacroiliac joint. A blunt ribbon retractor is placed through the
sciatic notch into the pelvis along the anterior margin of the
sacro-iliac joint to protect the anterior structures. The surgeon then directs the osteotomes serially through the joint to
complete the amputation. The amputation specimen is
passed from the surgical field and hemostasis obtained. The
presacral area is highly vascular with great potential for venous bleeding, which must be controlled with suture ligatures or electrocautery.
Closure
The surgical field should then be irrigated with several liters
of fluid and closed over large drains. Closure is accomplished
by bringing the gluteus maximus flap forward and suturing
the gluteus fascia to the external oblique and rectus abdomi-
Hip disarticulation and hemi-pelvectomy
101
nus fasciae of the abdominal wall. Scarpas fascia may be
re-approximated according to the surgeons preference,
along with the desired method of skin closure. The rectal
packing should be removed and a bulky dressing placed on
the wound, secured with a large elastic bandage around the
waist.
sumption of an acceptable quality of life. Aggressive rehabilitation enables most of these patients to ambulate with forearm crutches, which many patients choose in preference to a
large unwieldly prosthesis. Amputation support groups can
be instrumental in helping patients make both emotional and
physical adjustments to their disability.
Conclusion
Suggested Reading
Hip disarticulation and hemi-pelvectomy procedures result
in major functional disabilities, but do not preclude the re-
Clark MA, Thomas JM: Major amputation for soft-tissue sarcoma. Br J Surg
90:102-107, 2003
Paz IB: Major palliative amputations. Surg Clin N Am 13:543-547, 2004
Вам также может понравиться
- Hip Disorders in Children: Postgraduate Orthopaedics SeriesОт EverandHip Disorders in Children: Postgraduate Orthopaedics SeriesРейтинг: 3 из 5 звезд3/5 (2)
- AnastomosisДокумент7 страницAnastomosissuri84Оценок пока нет
- Traction in OrthopaedicДокумент32 страницыTraction in OrthopaedicFarry Doank100% (1)
- Microsurgical Skills: A Handbook of Experimental Microsurgical TechniquesОт EverandMicrosurgical Skills: A Handbook of Experimental Microsurgical TechniquesОценок пока нет
- Ao Principles Principles of Internal Fixation (Of Fractures)Документ18 страницAo Principles Principles of Internal Fixation (Of Fractures)Satya NagaraОценок пока нет
- Current Challenges with their Evolving Solutions in Surgical Practice in West Africa: A ReaderОт EverandCurrent Challenges with their Evolving Solutions in Surgical Practice in West Africa: A ReaderОценок пока нет
- Orthopaedics EmergenciesДокумент63 страницыOrthopaedics EmergencieszzooooeeeeeeОценок пока нет
- 9 Orthopaedic EmergenciesДокумент68 страниц9 Orthopaedic EmergenciesAndrew WdsmithОценок пока нет
- Lateral Condyle Fracture Tips and TricksДокумент33 страницыLateral Condyle Fracture Tips and TricksPurushotham NalamatiОценок пока нет
- Skeletal Injury in The ChildДокумент1 216 страницSkeletal Injury in The ChildRizki KokoОценок пока нет
- Total Hip Replacement PPДокумент22 страницыTotal Hip Replacement PPAnonymous dGfXuDd5Оценок пока нет
- Pfo IntroДокумент9 страницPfo IntroabdirashidОценок пока нет
- Tissue Repair: Kristine Krafts, M.D. - September 13, 2010Документ59 страницTissue Repair: Kristine Krafts, M.D. - September 13, 2010Antonino CassottaОценок пока нет
- PreviewДокумент24 страницыPreviewSabryОценок пока нет
- Clavicle AO Surgery Reference (2023)Документ399 страницClavicle AO Surgery Reference (2023)Wael GabrОценок пока нет
- Matary General Surgery 2013 (WWW - Afriqa Sat - Com)Документ310 страницMatary General Surgery 2013 (WWW - Afriqa Sat - Com)Ahmed AttiaОценок пока нет
- Total Knee Replacement: The Path ToДокумент6 страницTotal Knee Replacement: The Path ToMoses DhinakarОценок пока нет
- Approach To FractureДокумент17 страницApproach To FractureRebecca WongОценок пока нет
- Locked Plating: Sean E. Nork, MD James P. Stannard, MD and Philip J. Kregor, MDДокумент119 страницLocked Plating: Sean E. Nork, MD James P. Stannard, MD and Philip J. Kregor, MDDeep Katyan DeepОценок пока нет
- Infection in Orthopedic SurgeryДокумент17 страницInfection in Orthopedic SurgerykesramanujamОценок пока нет
- The Talonavicular and Subtalar Joints The Calcaneopedal Unit ConceptДокумент11 страницThe Talonavicular and Subtalar Joints The Calcaneopedal Unit ConceptAnonymous kdBDppigEОценок пока нет
- History Taking in OrthopaedicsДокумент23 страницыHistory Taking in OrthopaedicsVaibhav Krishna100% (5)
- Congenital Dysplasia & DislocatiДокумент558 страницCongenital Dysplasia & DislocatiWilson A. QuinteroОценок пока нет
- Fractures and Dislocations About The Elbow in The Pediatric PatientДокумент65 страницFractures and Dislocations About The Elbow in The Pediatric PatientPeter HubkaОценок пока нет
- Practical Procedures in Elective Orthopaedic Surgery - Pelvis & Lower ExtremityДокумент315 страницPractical Procedures in Elective Orthopaedic Surgery - Pelvis & Lower ExtremityNishil Modi100% (1)
- External FixationДокумент23 страницыExternal FixationJc LeeОценок пока нет
- Miles Operation - Abdominoperineal Excision - Rectal CAДокумент5 страницMiles Operation - Abdominoperineal Excision - Rectal CASpencer DempseyОценок пока нет
- Innovative Solutions in Hip ArthrosДокумент16 страницInnovative Solutions in Hip ArthrosGustavo Enrique Matson CarballoОценок пока нет
- A Regional Approach To Foot and Ankle MRIДокумент17 страницA Regional Approach To Foot and Ankle MRInior100% (1)
- Orthopaedic Emergencies: IC3 Musculoskeletal Teaching Week Gavin O'Reilly 6/1/15Документ13 страницOrthopaedic Emergencies: IC3 Musculoskeletal Teaching Week Gavin O'Reilly 6/1/15kylieverОценок пока нет
- Shoulder Joint ReplacementДокумент10 страницShoulder Joint ReplacementSiva ShanmugamОценок пока нет
- Ankle Foot OrthosisДокумент4 страницыAnkle Foot Orthosis楊畯凱Оценок пока нет
- Orthopedic Clinics Na 2007 Vol 38 ScoliosisДокумент102 страницыOrthopedic Clinics Na 2007 Vol 38 ScoliosisChanina BlacksteinОценок пока нет
- Any PDFДокумент252 страницыAny PDFRaja VeerappanОценок пока нет
- Humerus FractureДокумент18 страницHumerus FractureHęñøķ BęŕhãñęОценок пока нет
- Basics of Knee Arthroscopy: For The BeginnersДокумент40 страницBasics of Knee Arthroscopy: For The BeginnersPedro Zambrano100% (1)
- New Trends and Techniques in Open Reduction and Internal Fixation of Fractures of The Tibial PlateauДокумент8 страницNew Trends and Techniques in Open Reduction and Internal Fixation of Fractures of The Tibial PlateauCosmina BribanОценок пока нет
- Cavus FootДокумент14 страницCavus FootdrkbarryОценок пока нет
- Coxitis TB Hip KneeДокумент26 страницCoxitis TB Hip KneefajarvicОценок пока нет
- Posterior Tibialis Tendon Dysfunction (PTTD)Документ11 страницPosterior Tibialis Tendon Dysfunction (PTTD)bigpawn13Оценок пока нет
- AAOS Mini Open Rotator Cuff RepairДокумент10 страницAAOS Mini Open Rotator Cuff RepairHannah CoОценок пока нет
- BooksДокумент1 страницаBooksAnonymous atS3ugОценок пока нет
- Hip Fractures-Orthoinfo - AaosДокумент9 страницHip Fractures-Orthoinfo - Aaosapi-228773845Оценок пока нет
- Hip - Total Hip ArthroplastyДокумент13 страницHip - Total Hip ArthroplastyKholod AnwarОценок пока нет
- Shoulder PathologiesДокумент33 страницыShoulder PathologiesjermaineОценок пока нет
- Surgical Antibiotic Prophylaxis - Orthopaedic Surgery in AdultsДокумент7 страницSurgical Antibiotic Prophylaxis - Orthopaedic Surgery in AdultsConstantin BudinОценок пока нет
- PDFДокумент328 страницPDFBreak DerulsОценок пока нет
- Argenson - Partial Knee Arthroplasty2Документ160 страницArgenson - Partial Knee Arthroplasty2ValaMelkor100% (1)
- HIP JOINT Special Tests-WPS OfficeДокумент51 страницаHIP JOINT Special Tests-WPS OfficeManisha MishraОценок пока нет
- Mukharjee Regimen 321Документ16 страницMukharjee Regimen 321shreyahospital.motinagarОценок пока нет
- FR Distal HumerusДокумент55 страницFR Distal Humerusiisscribd100% (1)
- Vivek Sharm Acl ReconstructionДокумент7 страницVivek Sharm Acl ReconstructionJuan Pablo FuentesОценок пока нет
- Transient SynovitisДокумент9 страницTransient SynovitisMuhammad Taufik AdhyatmaОценок пока нет
- Bone Tumor: Daniel A. (Orthopedic Surgeon)Документ225 страницBone Tumor: Daniel A. (Orthopedic Surgeon)mebrieОценок пока нет
- Practical ProceduresДокумент315 страницPractical ProceduresAnil SoodОценок пока нет
- KS LE AmputationДокумент116 страницKS LE AmputationAstri ArfОценок пока нет
- Shoulder DislocationДокумент29 страницShoulder DislocationAndaleeb ZehraОценок пока нет
- Trauma Musculoskeletal - Spine FKK UMJ1Документ92 страницыTrauma Musculoskeletal - Spine FKK UMJ1Hendra Hash AwoОценок пока нет
- 2 Hip Examination - How To Examine Hip DR Prof Anil AroraДокумент112 страниц2 Hip Examination - How To Examine Hip DR Prof Anil AroraSaikatОценок пока нет
- Advances in Liposuction Five Key Principles With.7Документ9 страницAdvances in Liposuction Five Key Principles With.7alinutza_childОценок пока нет
- MastopexyДокумент16 страницMastopexyalinutza_childОценок пока нет
- Development of The Inframammary Fold and Ptosis in Breast Reconstruction PDFДокумент4 страницыDevelopment of The Inframammary Fold and Ptosis in Breast Reconstruction PDFalinutza_childОценок пока нет
- Re-Creation of The Inframammary Fold, BreastДокумент9 страницRe-Creation of The Inframammary Fold, Breastalinutza_childОценок пока нет
- Pedicled and Free Radial Forearm Flaps For Reconstruction of The Elbow Wrist and Hand - PRS 2008Документ12 страницPedicled and Free Radial Forearm Flaps For Reconstruction of The Elbow Wrist and Hand - PRS 2008alinutza_childОценок пока нет
- Skin Grafts PDFДокумент112 страницSkin Grafts PDFalinutza_childОценок пока нет
- Preplanning Vascularized Lymph Node Transfer With.4Документ7 страницPreplanning Vascularized Lymph Node Transfer With.4alinutza_childОценок пока нет
- Detergent Free Decellularized Nerve Grafts For.6Документ8 страницDetergent Free Decellularized Nerve Grafts For.6alinutza_childОценок пока нет
- 10 16 02CleftLipandPalatePart2 PDFДокумент93 страницы10 16 02CleftLipandPalatePart2 PDFalinutza_childОценок пока нет
- Clinical Evidence For The Relationship Between.4Документ7 страницClinical Evidence For The Relationship Between.4alinutza_childОценок пока нет
- Capsular Contracture and Genetic Profile of Ica.56Документ20 страницCapsular Contracture and Genetic Profile of Ica.56alinutza_childОценок пока нет
- Microtia Reconstruction and Postsurgical Grisel s.13Документ4 страницыMicrotia Reconstruction and Postsurgical Grisel s.13alinutza_childОценок пока нет
- Andrej Čretnik Achilles Tendon 0Документ154 страницыAndrej Čretnik Achilles Tendon 0alinutza_childОценок пока нет
- Clinical Evidence For The Relationship Between.4Документ7 страницClinical Evidence For The Relationship Between.4alinutza_childОценок пока нет
- Cranial Reconstruction Following The Removal of An.5Документ8 страницCranial Reconstruction Following The Removal of An.5alinutza_childОценок пока нет
- Minimal FaceliftДокумент13 страницMinimal Faceliftalinutza_childОценок пока нет
- FireДокумент7 страницFirealinutza_childОценок пока нет
- 6th Central Pay Commission Salary CalculatorДокумент15 страниц6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- Current Evidence On The Unit Equivalence of DifferentДокумент8 страницCurrent Evidence On The Unit Equivalence of Differentalinutza_childОценок пока нет
- A Comparison of Lipoatrophy and Aging PDFДокумент8 страницA Comparison of Lipoatrophy and Aging PDFalinutza_childОценок пока нет
- Malizos - Re Constructive Microsurgery (Landes Bio Science VademecumДокумент260 страницMalizos - Re Constructive Microsurgery (Landes Bio Science VademecumBudhi Nath Adhikari100% (5)
- Bioprosthetic Tissue Matrices in Complex Abdominal.2Документ7 страницBioprosthetic Tissue Matrices in Complex Abdominal.2alinutza_childОценок пока нет
- Classification of Masseter Hypertrophy For.11Документ10 страницClassification of Masseter Hypertrophy For.11alinutza_childОценок пока нет
- Full-Face Rejuvenation Using A Range of Hyaluronic AcidДокумент9 страницFull-Face Rejuvenation Using A Range of Hyaluronic Acidalinutza_childОценок пока нет
- Venous Thromboembolism Prophylaxis in Hospitalized Patients PDFДокумент9 страницVenous Thromboembolism Prophylaxis in Hospitalized Patients PDFalinutza_childОценок пока нет
- Cutaneous MelanomaДокумент55 страницCutaneous Melanomaalinutza_childОценок пока нет
- Achilles TendonДокумент154 страницыAchilles Tendonalinutza_childОценок пока нет
- Patient With Familial Multiple Lipomatosis and ReviewДокумент5 страницPatient With Familial Multiple Lipomatosis and Reviewalinutza_childОценок пока нет
- Carpal Tunnel Surgery, Hand Clinics, Volume 18, Issue 2, Pages 211-368 (May 2002)Документ151 страницаCarpal Tunnel Surgery, Hand Clinics, Volume 18, Issue 2, Pages 211-368 (May 2002)alinutza_childОценок пока нет
- Acceptance LetterДокумент1 страницаAcceptance LetterJayzel LaureanoОценок пока нет
- Cardiothoracic Surgery ST101.11.17Документ10 страницCardiothoracic Surgery ST101.11.17Javier Nicolas Pena DazaОценок пока нет
- Experiment 1 Plant MorphologyДокумент13 страницExperiment 1 Plant MorphologyZharif NizamОценок пока нет
- BMHRCДокумент8 страницBMHRCJeshiОценок пока нет
- Psydclpsy PDFДокумент55 страницPsydclpsy PDFBGangadharReddyОценок пока нет
- Temper Tantrums: A Normal Part of Growing UpДокумент2 страницыTemper Tantrums: A Normal Part of Growing UpAyudyah AnnishaОценок пока нет
- Week 2 - Motivation To Be A MidwifeДокумент4 страницыWeek 2 - Motivation To Be A MidwifemitaОценок пока нет
- Explaining Schilders Five Mechanical ObjectivesДокумент3 страницыExplaining Schilders Five Mechanical ObjectivesAmarili_2350% (2)
- 120 Random Questions For MCQ PDFДокумент41 страница120 Random Questions For MCQ PDFMostafa RezowanОценок пока нет
- Resume-Alvin Punzalan MangulabnanДокумент3 страницыResume-Alvin Punzalan MangulabnanMaestro JayОценок пока нет
- Colon Tumor Carcinoma WHO 2010Документ3 страницыColon Tumor Carcinoma WHO 2010Ronald MoraОценок пока нет
- Stem Cells and BioreactorДокумент1 страницаStem Cells and Bioreactorwillp200Оценок пока нет
- Des Moines Landmark ReviewДокумент147 страницDes Moines Landmark ReviewD.j. HaramieОценок пока нет
- Creating An Educational Plan That Meets The Learning Needs of Nursing StaffДокумент10 страницCreating An Educational Plan That Meets The Learning Needs of Nursing StaffJB VillanuevaОценок пока нет
- Motor, Sensory and Perceptual DevelopmentДокумент10 страницMotor, Sensory and Perceptual DevelopmentGlenda GalanganОценок пока нет
- Ravi ProjectДокумент92 страницыRavi ProjectAvinash Avii100% (1)
- Medicina InternaДокумент693 страницыMedicina InternaMaverick 18100% (5)
- Malignant Small Round Cell TumorsДокумент12 страницMalignant Small Round Cell TumorsSaptarshi Ghosh100% (1)
- The Modern Radiology DepartmentДокумент5 страницThe Modern Radiology DepartmentBeautederm ZamboangaОценок пока нет
- Analgesia Epidural Current Views and ApproachesДокумент168 страницAnalgesia Epidural Current Views and ApproachesManuel Ortega100% (2)
- Eye Hand CoordinationДокумент12 страницEye Hand CoordinationCharles JohnsonОценок пока нет
- Neurological ExaminationДокумент216 страницNeurological Examinationkid_latigo100% (4)
- Assessing Cephalopelvic Disproportion: Back To The BasicsДокумент27 страницAssessing Cephalopelvic Disproportion: Back To The Basicsbeechrissanty_807904Оценок пока нет
- The Ethics of Medical ReferralДокумент3 страницыThe Ethics of Medical Referralkajal907Оценок пока нет
- Supports of UterusДокумент16 страницSupports of UterusinnyОценок пока нет
- Original Research ReportДокумент4 страницыOriginal Research ReportSehrish SiddiqueОценок пока нет
- Designing of Manifold RoomДокумент4 страницыDesigning of Manifold RoomDurjoy_Sarker_143450% (2)
- [Advances in Neurosurgery 2] O. Stochdorph (Auth.), W. Klug, M. Brock, M. Klinger, O. Spoerri (Eds.) - Meningiomas Diagnostic and Therapeutic Problems Multiple Sclerosis Misdiagnosis Forensic Problems in NeurosurgДокумент461 страница[Advances in Neurosurgery 2] O. Stochdorph (Auth.), W. Klug, M. Brock, M. Klinger, O. Spoerri (Eds.) - Meningiomas Diagnostic and Therapeutic Problems Multiple Sclerosis Misdiagnosis Forensic Problems in Neurosurgbayu_gendeng666Оценок пока нет
- 101 - 36903 - Chapter 14 HairДокумент17 страниц101 - 36903 - Chapter 14 HairAaromal MaanasОценок пока нет
- MicrosurgeryFellowAugust2019Документ16 страницMicrosurgeryFellowAugust2019Navid ToyserkaniОценок пока нет
- Summary of The 4-Hour Body: An Uncommon Guide to Rapid Fat-Loss, Incredible Sex, and Becoming Superhuman by Timothy FerrissОт EverandSummary of The 4-Hour Body: An Uncommon Guide to Rapid Fat-Loss, Incredible Sex, and Becoming Superhuman by Timothy FerrissРейтинг: 4.5 из 5 звезд4.5/5 (81)
- The Obesity Code: Unlocking the Secrets of Weight LossОт EverandThe Obesity Code: Unlocking the Secrets of Weight LossРейтинг: 4 из 5 звезд4/5 (5)
- Briefly Perfectly Human: Making an Authentic Life by Getting Real About the EndОт EverandBriefly Perfectly Human: Making an Authentic Life by Getting Real About the EndОценок пока нет
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDОт EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDРейтинг: 5 из 5 звезд5/5 (1)
- Neville Goddard Master Course to Manifest Your Desires Into Reality Using The Law of Attraction: Learn the Secret to Overcoming Your Current Problems and Limitations, Attaining Your Goals, and Achieving Health, Wealth, Happiness and Success!От EverandNeville Goddard Master Course to Manifest Your Desires Into Reality Using The Law of Attraction: Learn the Secret to Overcoming Your Current Problems and Limitations, Attaining Your Goals, and Achieving Health, Wealth, Happiness and Success!Рейтинг: 5 из 5 звезд5/5 (284)
- Prisoners of Geography: Ten Maps That Explain Everything About the WorldОт EverandPrisoners of Geography: Ten Maps That Explain Everything About the WorldРейтинг: 4.5 из 5 звезд4.5/5 (1145)
- Really Very Crunchy: A Beginner's Guide to Removing Toxins from Your Life without Adding Them to Your PersonalityОт EverandReally Very Crunchy: A Beginner's Guide to Removing Toxins from Your Life without Adding Them to Your PersonalityРейтинг: 5 из 5 звезд5/5 (28)
- Gut: the new and revised Sunday Times bestsellerОт EverandGut: the new and revised Sunday Times bestsellerРейтинг: 4 из 5 звезд4/5 (392)
- The Bridesmaid: The addictive psychological thriller that everyone is talking aboutОт EverandThe Bridesmaid: The addictive psychological thriller that everyone is talking aboutРейтинг: 4 из 5 звезд4/5 (131)
- The Happiest Baby on the Block: The New Way to Calm Crying and Help Your Newborn Baby Sleep LongerОт EverandThe Happiest Baby on the Block: The New Way to Calm Crying and Help Your Newborn Baby Sleep LongerРейтинг: 4.5 из 5 звезд4.5/5 (58)
- How to Talk to Anyone: Learn the Secrets of Good Communication and the Little Tricks for Big Success in RelationshipОт EverandHow to Talk to Anyone: Learn the Secrets of Good Communication and the Little Tricks for Big Success in RelationshipРейтинг: 4.5 из 5 звезд4.5/5 (1135)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisОт EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisРейтинг: 4 из 5 звезд4/5 (1)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsОт EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsРейтинг: 4.5 из 5 звезд4.5/5 (169)
- Love Yourself, Heal Your Life Workbook (Insight Guide)От EverandLove Yourself, Heal Your Life Workbook (Insight Guide)Рейтинг: 5 из 5 звезд5/5 (40)
- No Mud, No Lotus: The Art of Transforming SufferingОт EverandNo Mud, No Lotus: The Art of Transforming SufferingРейтинг: 5 из 5 звезд5/5 (175)
- How to Walk into a Room: The Art of Knowing When to Stay and When to Walk AwayОт EverandHow to Walk into a Room: The Art of Knowing When to Stay and When to Walk AwayРейтинг: 4.5 из 5 звезд4.5/5 (5)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningОт EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningРейтинг: 4 из 5 звезд4/5 (3)
- Summary of The Art of Seduction by Robert GreeneОт EverandSummary of The Art of Seduction by Robert GreeneРейтинг: 4 из 5 звезд4/5 (46)
- Summary: I'm Glad My Mom Died: by Jennette McCurdy: Key Takeaways, Summary & AnalysisОт EverandSummary: I'm Glad My Mom Died: by Jennette McCurdy: Key Takeaways, Summary & AnalysisРейтинг: 4.5 из 5 звезд4.5/5 (2)
- The Babysitter: A gritty page-turning thriller from Gemma RogersОт EverandThe Babysitter: A gritty page-turning thriller from Gemma RogersРейтинг: 4.5 из 5 звезд4.5/5 (16)
- The Secret Teachings Of All Ages: AN ENCYCLOPEDIC OUTLINE OF MASONIC, HERMETIC, QABBALISTIC AND ROSICRUCIAN SYMBOLICAL PHILOSOPHYОт EverandThe Secret Teachings Of All Ages: AN ENCYCLOPEDIC OUTLINE OF MASONIC, HERMETIC, QABBALISTIC AND ROSICRUCIAN SYMBOLICAL PHILOSOPHYРейтинг: 4.5 из 5 звезд4.5/5 (4)


































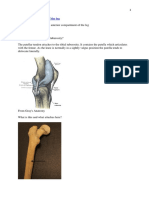















































































![[Advances in Neurosurgery 2] O. Stochdorph (Auth.), W. Klug, M. Brock, M. Klinger, O. Spoerri (Eds.) - Meningiomas Diagnostic and Therapeutic Problems Multiple Sclerosis Misdiagnosis Forensic Problems in Neurosurg](https://imgv2-2-f.scribdassets.com/img/document/375359245/149x198/fae4c10859/1522685798?v=1)































